Abstract
Post-traumatic seizures (PTS) and epilepsy (PTE) are serious and debilitating complications occurring commonly after traumatic brain injury (TBI). PTE accounts for approximately 6% of all epilepsy cases and is often medically refractory. A clear correlation between the severity of TBI and the likelihood of developing PTS or PTE has been demonstrated. Clinical studies have attempted to use anti-seizure and other medications after TBI to prevent the development of PTE, but none have been successful. The occurrence of several structural, physiological, and biochemical modifications in the brain promotes epileptogenesis, and there is great interest in developing therapeutic options aimed at these mechanisms to prevent the development of PTE. This chapter will review the epidemiology, genetic and risk factors, and natural history of PTS and PTE. We will also provide an overview of the diagnostic workup of suspected PTE and medical and surgical treatment options. Finally, we provide a brief overview of animal models being used to investigate PTE, possible mechanisms behind epileptogenesis, and experimental treatments that have recently been explored.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Post-traumatic epilepsy
- Post-traumatic seizures
- Epilepsy
- Status epilepticus
- Traumatic brain injuries
- Brain injury
- Closed-head injury
- Head trauma
- Epileptogenesis
- Epilepsy prevention
Introduction
Epilepsy is a common neurologic complication of traumatic brain injury (TBI) [1,2,3]. Five percent of all referrals to specialized epilepsy centers are due to confirmed post-traumatic epilepsy (PTE) [4]. Patients with PTE comprise a regular part of the care provided by epilepsy specialists, as well as general neurologists and primary care physicians throughout the world [5]. The objective of this chapter is to provide an overview of post-traumatic seizures and epilepsy by reviewing the definition, epidemiology, and risk factors of epileptic events in TBI. Subsequently, we will discuss the pathophysiology of PTE particularly through animal studies. Finally, the clinical aspects of PTE will be discussed, and we provide a summary of the clinical approach to epileptic events associated with TBI, including diagnostic and therapeutic measures.
Definition
An epileptic seizure is defined as “a transient occurrence of signs and/or symptoms due to abnormal excessive or synchronous neuronal activity in the brain” [6]. According to the latest definition proposed by the task force of the International League Against Epilepsy (ILAE ), epilepsy is “a disease of the brain defined by any of the following conditions: (1) At least two unprovoked (or reflex) seizures occurring >24 h apart; (2) one unprovoked (or reflex) seizure and a probability of further seizures similar to the general recurrence risk (at least 60%) after two unprovoked seizures, occurring over the next 10 years; (3) diagnosis of an epilepsy syndrome” [6].
The epileptic events occurring following TBI are classified in one of these categories: [1, 7] immediate post-traumatic seizures (PTSs) occur less than 24 h after TBI, while early PTSs occur within the first week post-injury. Both immediate and early seizures after TBI are considered provoked seizures. They do not meet the definition of epilepsy since they are not necessarily mediated by the pathogenic mechanisms that predispose the patient to manifest spontaneous seizures [6]. Late recurring seizures, or PTE, are unprovoked seizures occurring more than 1 week after TBI.
Epidemiology
Post-traumatic Seizures
The incidence of immediate seizures is reported to be 1–4% and of early seizures is 4–25% in civilian head injuries [2, 8, 9]. The occurrence of early PTSs depends in part on TBI severity [2, 8]. There are several classification systems for TBI severity. A widely used system is that of Annegers and colleagues (Table 7.1) [1]. Recently, a newer classification, the Mayo Classification System for TBI Severity, has been designed to distinguish between different severities of TBI correlated with the general outcome of the patients after injury (Table 7.2) [10]. Age also plays an important role in the development of PTSs, as children seem to be more likely to develop PTSs compared to adults [1]. In children PTSs are more common than later development of PTE (97% vs 3%) [11]. In addition, other important risk factors have been implicated in the development of PTS, listed in Table 7.3.
Subclinical seizures are seizures which show electrophysiological changes with electroencephalogram (EEG ) recordings but display no overt behavioral changes [12]. Subclinical seizures, including nonconvulsive status epilepticus (NCSE ), are relatively common after severe TBI in the intensive care unit (ICU) setting [13, 14]. Thirty-three percent of adult TBI patients requiring ICU were reported to have seizures as detected by continuous EEG monitoring [15]. In a pediatric study, the reported incidence of seizures was as high as 42.5%, of whom 7% only had subclinical seizures [14]. Intracranial EEG with electrodes implanted after TBI was able to detect electrographic seizures in 71% of patients that were not apparent on scalp EEG [16], suggesting seizure rates may be even higher than reported. Detection of subclinical seizures is crucial as reports have shown early nonconvulsive PTSs are associated with increased intracranial pressure, metabolic derangements, and long-term hippocampal atrophy [17, 18].
The occurrence of status epilepticus (SE) at onset is high, estimated to be 6.39% in an adult population, comprising 28.57% of the patients with moderate to severe TBI who developed clinical and subclinical PTS [13]. SE rates are even higher in the pediatric population compared to adults. In one study, an average of 18.4% of children with acute TBI developed SE in a pediatric ICU, ranging between 12.5% and 31.3%, depending on the severity of TBI [14]. Seventy percent of these children showed subclinical SE [14]. Younger age, abusive head trauma, and intracranial hemorrhage were the risk factors of developing SE in this study.
Post-traumatic Epilepsy
PTE accounts for 5–6% of all epilepsies [19]. The frequency rate of PTE varies in different studies between 1.9% and 53% [1, 2, 8, 9, 20, 21], depending on injury severity and mechanism. Patients with TBI have increased risk of developing epilepsy compared to the general population, and the relative risks of developing epilepsy after mild, moderate, and severe TBI are 1.5, 2.9, and 17, respectively [2]. Furthermore, the mechanism of injury in penetrating head trauma and closed-head injuries is different, and the former is more likely associated with PTE (50% in penetrating injuries versus up to 23.6% for the closed-head injuries) [2, 3, 9]. The bone and iron-containing metal fragments in the wounds of war survivors are potentially more epileptogenic than lead fragments from bullets. Hence, civilian injuries with bone fragments alone do not significantly increase the risk for PTE [9, 21, 22]. Furthermore, the duration of epilepsy, seizure frequency, and response to antiepileptic drug (AED) therapy is correlated with severity of TBI [2, 23]. In 27% of patients with penetrating war injuries, epilepsy persisted up to 15-year post-injury as compared with the risk in the general population [9]. Whether early PTS is a risk factor for PTE is a matter of controversy. While some studies found that PTSs were not an independent risk factor for PTE [2], other studies have demonstrated the presence of early PTSs as a precursor [21, 24], or even the most consistently significant risk factor for PTE in adults [7, 24], but this is certainly not true for children [7].
Family History/Genetic Associations
Hereditary predisposition to PTE and related genetic polymorphisms has been long debated [26,27,27]. Although some studies have linked certain genes to PTE, many of them need to be duplicated.
While Schaumann and colleagues showed that family history of epilepsy could precipitate individuals into early PTSs and PTE [28], others found that family history of epilepsy increases the risk of PTE in children [29, 30] but not in older patients [9, 31].
Genetic association studies propose that there might be a genetic element to the development of PTE. A study showed that TBI patients with an apolipoprotein Eε4 (APOEε4 ) allele , a gene encoding a cholesterol transporter into neurons, experienced a higher risk of PTS [32]. In a review made by Cotter and colleagues, the most promising candidates were the pro-inflammatory gene Interleukin-1beta (IL-1b) SNP (rs1143634) and A1 adenosine receptor (A1AR) SNP (rs10920573) by which the individuals with heterozygous genotype seemed to be at higher risk for developing PTE. However, other genes such as glutamic acid decarboxylase 1 (GAD1 ) and methylenetetrahydrofolate reductase (MTHFR ) C677T have been associated with early PTSs [33].
More recently, a genetic variation in solute carrier family 1 member 1 (SLC1A1 ), a gene encoding the neuronal glutamate transporters, was associated with reduced time to first seizure and increased seizure risk up to 3-year post-injury. When individuals were homozygous (GG) for the SLC1A1 SNP rs10974620 minor allele, the risk of seizure over this period increased significantly. Likewise, in individuals who were homozygous (TT) for the SLC1A1 SNP rs7858819 minor allele, the risk of PTE was higher when follow-up began on day 2 post-injury [34].
Mechanistic target of rapamycin (mTOR) complex 1 (mTORC1) is a protein involved in the regulation of cell proliferation and cell metabolism that widely has been associated with tumors including tuberous sclerosis. In a review recently published by Myers and colleagues, mTORC1 activation was considered as a contributing factor causing mossy fiber sprouting and neurogenesis, predisposing the patients to develop epilepsy after TBI although the significance of it has not been confirmed yet [35].
Pathophysiology
Human studies and animal models have attempted to discover the pathophysiological mechanisms for PTE, and various mechanisms have been proposed. A number of animal models have been employed at different developmental stages and with injuries of varying severity and location. One of the most well-studied models is fluid percussion injury (FPI ), a model of closed-head TBI [36]. In this model, injury is delivered through a craniotomy by rapid fluid injection. The fluid pulse first strikes the intact dura and then moves into the epidural space [37]. Craniotomies can be applied to the midline to produce more diffuse injuries or laterally to produce mixed focal and diffuse injury [37]. Early electrophysiological changes [38] as well as PTE have been described [36, 39, 40]. Controlled cortical impact (CCI ) injury is another widely used experimental model of closed-head injury that was recently identified as a model of injury-induced epilepsy [41]. This model often utilizes an electronically controlled pneumatic impactor to apply a focal contusion injury to the brain surface through a craniotomy [42].
Experimental models have described potential biological changes after TBI in three distinct temporal phases. The first phase ranges from a few seconds to minutes [43], consisting of immediate release of excitatory neurotransmitters including glutamate, followed by ion channel activation and calcium influx [44]. Hyperexcitation results in energy depletion and cell death [44]. One of the underlying ionic changes identified early after the injury is potassium accumulation that is caused by failure of the ionic ATP pump [45] leading to altered resting membrane potential and neuronal excitability, with a loss of inhibitory postsynaptic potentials [46]. In addition, an increase in extracellular potassium converts spikers to a burster state in the CA3 region of the hippocampus [47]. Also, hyperexcitability in the CA1 subregion of the hippocampus has been reported by in vitro studies [48, 49].
Secondary injury is characterized by altered local cerebral blood flow regulation, breakdown in the blood brain barrier (BBB ), and initiation of inflammatory and neuronal death, occurring within hours to days after TBI. During the inflammatory response, cytokines are released [50] which inhibit the uptake of glutamate by astrocytes [51] and modulate excitatory neurotransmission in the brain through glutamate receptors [52, 53]. For instance, IL-1β modulates neuronal hyperexcitability through Ca2+, glutamatergic, and GABAergic pathways [54]. Glial glutamate transporter protein (GLT) which regulates the extracellular glutamate level also decreases after TBI, particularly in the neocortical and hippocampal regions leading to increased level of glutamate and hyperexcitability [55, 56]. Patients with PTE are more likely to show BBB disruption compared to non-epileptic patients after TBI, and slow waves are identified in EEG in 70% of cases [57].Tomkins and colleagues also showed that the size of lesion with BBB disruption was significantly larger in PTE patients [57].
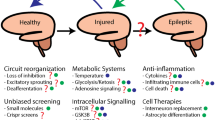
The third phase is the latent period between the injury and the first successive seizure and is when epileptogenesis takes places [58]. It is characterized by morphological changes including mossy fiber sprouting, dendritic modifications, interneuron loss, rewiring of synaptic circuits, glial cell activation, ectopic cell proliferation, and gliosis [41, 61,62,63,62]. During this phase, excitability is increased both in CA1 [63] and dentate gyrus [64]. Loss of GABAergic interneurons decreases the inhibition on pyramidal cells [67,68,67]. Moreover, not only mossy fiber sprouting and loss of inhibition but also the increased connections on the dentate granule cells together enhance the excitability of hippocampus [47, 70,71,72,73,72]. This could also explain how injury at the neocortex progresses to mesial temporal seizures at a later time. Some groups have shown that seizures are originally neocortical at onset, but over time, the mesial temporal region transforms to an epileptogenic zone [73]. In fact, in approximately 61% of patients with PTE, seizures emanate from the temporal lobe [74], and magnetic resonance imaging (MRI) has shown that about 35% of these patients have mesial temporal lobe sclerosis (MTS). It is unclear, however, if MTS could be a secondary phenomenon [74]. Furthermore, prolonged seizures at the acute post-TBI phase have been implicated in hippocampal atrophy at the later phase of injury [18]. It is, however, worth mentioning that it is not uncommon that TBI results in multifocal pathology [74]. In conclusion, neuronal loss, chronic neuroinflammation, and network reorganization in the overlaying cortical regions are implicated in epileptogenesis.
Clinical or Natural History
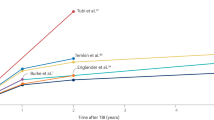
Forty-seven percent of late PTSs recur after 1 month, while an 86% recurrence rate is observed within 2 years after injury [75]. In general, the relative risk of developing PTE after severe TBI remains significantly high even after 10 years both in adults [2] and in children [30], whereas patients with mild TBI exhibit a normalization of the risk after the first 5 years [2]. Christensen and colleagues believe that the absolute risk of PTE decreases significantly, and the yearly absolute risk remains below 1% for all types of brain injury including severe TBI by 5 years of follow-up [76]. One study showed that the mean latency to seizure was 3.5 years [77], ranging from 2.1 years for MTS to 5.1 years for all lesional neocortical cases. Age may be a determining factor in the latency period of seizures after trauma. There was a latency period of about 3 years in the patients who were over 15 years at time of injury versus a 13-year latency period in those who were 2 years or younger at the time of injury [78].
Seizure onset location can be very variable after TBI. In a study of 60 patients with moderate to severe TBI and PTE, 52% developed generalized seizures, 34% had focal seizures, and 15% showed focal seizures with secondary generalization; however, this was based on seizure semiology and not electrophysiology [75]. By contrast, in a 10-year retrospective study based on EEG recordings from the epilepsy monitoring unit, 93% had localization-related epilepsy arising most commonly from temporal or frontal lobes [77], and 4.8% displayed generalized epilepsy. Of temporal lobe epilepsy cases, just under half had MTS, and about one-third were nonlesional. In humans, owing to the shape of the skull, the frontal and temporal cortices are susceptible to contusion, accounting for the greater prevalence of post-traumatic contusion [81,82,81]. Likewise, in most animal studies, frontal neocortical or limbic epilepsy are more common than parietal/occipital seizures regardless of FPI location [82]. The other explanation for the predilection of the frontal lobe to epileptogenesis, although not well established, could be higher intrinsic susceptibility to tissue damage or the known tendency of prefrontal neurons to burst discharges and hypersynchronization [82]. In experimental models, frontal neocortical foci develop within 1 month following FPI , while it takes several months for limbic regions to transform to an epileptogenic zone [73]. Whether frontal neocortical seizures are capable to kindle the hippocampus through propagation [73] is a proposed explanation. Direct hippocampal injury could also cause limbic epileptogenesis although more slowly [82]. In two studies, 24% to 35% of patients had mesial TLE (MTLE ), while neocortical foci were identified in 12–48% of patients [74, 83]. TBI can induce MTLE in children younger than 5 years, while neocortical epilepsy tends to occur later in life [74]. However, recently, Gupta and colleagues reported that 83% of patients with MTS following TBI had their injury after the age of 5 years. Englander and colleagues believe that although TBI has a propensity toward frontal and temporal lobes, parietal lobe involvement may also reduce the overall seizure threshold [21].
The remission rates of seizures vary between 25% and 40% once PTE is diagnosed (and treated), and up to half of patients with PTE show prolonged periods of seizure freedom [84].This is slightly lower than remission rates in other epilepsy populations [85]. Patients with high frequencies of seizures during the first year following injury are less likely to achieve remission [86].
Investigations
Following a seizure associated with acute head injury, investigation should involve assessment of the biochemical parameters, such as hyponatremia, along with exploring for possible intracranial hemorrhage. Hyponatremia induced by head trauma may lower the seizure threshold [86]. Acute brain edema, perioperative events including cerebral interventions or stress from general anesthesia, and metabolic disturbances account for a high proportion of seizures which develop during the first month after brain injury [21]. In patients developing PTS after moderate to severe TBI, CT scan should be performed urgently. If the seizures occur after initial imaging, a repeat CT is indicated.
Patients with PTE should be approached similarly to patients with a first non-traumatic epileptic seizure. All patients with epilepsy should be asked specifically about head trauma, since patients do not usually volunteer certain incidences of head trauma such as sports-related concussions [87]. In addition, psychogenic non-epileptic seizures (PNES ) are common after TBI [88, 89] and are frequently mistaken for epileptic seizures [90]. They should be ruled out with appropriate investigations, including video-EEG monitoring if necessary.
Magnetic resonance imaging (MRI) is the most sensitive means in identifying the extent and severity of brain injury and is the recommended neuroimaging modality in patients with PTE. Conventional MRI sequences, including T1-weighted, T2-weighted, gradient echo, and diffusion-weighted imaging, may discover parenchymal hemorrhages, extra-axial blood products (hemosiderin deposits), early ischemia, edema, and gliosis [91]. While the epileptogenic role of hemosiderin deposits has been established [20], precocious formation of a gliotic scar around a hemosiderin deposit reduces the risk of PTE [92]. Advanced MRI modalities including diffusion tensor imaging (DTI ) and functional MRI (fMRI) identify early and late changes that might correlate with epileptogenic foci [93]. Susceptibility-weighted imaging and DTI are more sensitive to microhemorrhages and white matter injury, respectively [94].
The EEG findings in TBI are usually nonspecific, and the presence of epileptiform activity does not predict the development of PTE [95] or disability outcome [96]. As described earlier, continuous EEG monitoring is worthwhile to rule out subclinical seizures, particularly NCSE in the ICU setting. The scalp EEG is negative in more than 20% of patients with PTE during the first 3 months after TBI [95]. However, it remains useful for localization of the epileptogenic zone as well as measurements of the extent of damage and in predicting relapse before AED is withdrawn [97]. Intracranial recordings also have demonstrated interictal spikes and fast ripples early during the epileptogenic process in patients with established PTE, representing a more sensitive method than routine scalp recordings in identifying the epileptic activity in these patients [16].
Management
The decision to initiate pharmacotherapy depends on the temporal relationship between the inciting brain injury and onset of seizures. In immediate seizures which occur immediately following head trauma, antiepileptic therapy is not indicated. Indeed, the pathophysiological mechanism of immediate seizures might be related to transient functional decerebration with loss of cortical inhibition and is characterized by initial tonic phase within 2 s of impact, followed by a clonic or myoclonic phase, which may last for several minutes. Immediate seizures do not lead to development of PTE [98].
In contrast, since early seizures increase cerebral perfusion pressure and intracranial pressure, seizure prophylaxis is the recommended therapy during the first 7 days of moderate to severe TBI based on the latest guideline (2016) of the Brain Trauma Foundation. Phenytoin treatment significantly reduces the incidence of early PTSs (3.6–14.2%) [99]. While phenytoin has been widely used to prevent early PTS, levetiracetam recently has gained attention for seizure prophylaxis in TBI [100]. However, a high-quality, head-to-head randomized clinical trial (RCT) between phenytoin and levetiracetam is lacking. Levetiracetam has demonstrated comparable efficacy to phenytoin in non-controlled studies [103,104,103] and is associated with fewer adverse effects, monitoring considerations [104], and better long-term outcomes [103]. An observational study on severe TBI revealed that epileptiform EEG abnormalities are more likely to persist in patients treated with levetiracetam compared to phenytoin [105]. Compared to placebo, carbamazepine has been documented to be effective in the prevention of early PTSs only in one true RCT [106]. Although similar results have been reported for valproate [107], this drug has lesser capacity to prevent early PTSs compared with phenytoin.
Compared to the established efficacy of early PTS, there is no evidence for pharmacological prophylaxis of the development of PTE [86, 99, 108]. Nevertheless, patients with early PTS, dural-penetrating injuries, multiple contusions, and/or SDH requiring evacuation may benefit from antiepileptic therapy beyond the first week post-injury [21, 107, 109, 110]. Principles of AED selection in PTE are identical to other patients with epilepsy, and no specific AED has been recommended for PTE [111, 112]. Neuropsychological consideration is required to be taken prior to starting AEDs [22]. Inappropriate treatment with AEDs may impair neurorehabilitation after TBI [113], and patients with post-TBI PNES could benefit from antidepressants, such as selective serotonin reuptake inhibitors and/or cognitive–behavioral therapy [114] rather than AEDs. There is no doctrine on duration of AED therapy, and much depends on a patient’s age, personal preference , and drug tolerability. However, as a rule of thumb, AED withdrawal can be considered after at least 2 years of seizure freedom, though waiting up to 4 years has been suggested as well [115].
Experimental Interventions
One of the main goals of PTE studies is to develop a therapeutic strategy which could be delivered during the latent period after TBI in order to prevent epileptogenesis and the development of PTE. Investigators have focused on various mechanistic pathways as potential therapeutic targets. Many studies have attempted to find antioxidant and neuroprotective drugs which prevent the lipid peroxidation of neuronal membranes. Based on the knowledge that magnesium blocks glutamate transmission at NMDA receptors, continuous infusion of magnesium sulfate was carried out within 8 h after moderate or severe TBI. However, this double-blinded RCT did not appear to prevent PTE [23]. The effect of magnesium on PTS could not be assessed because of concomitant use of phenytoin. In a ferrous chloride animal model, tochopherol (vitamin E) use was associated with a delay in the onset of electrical seizures on EEG [116]. The use of adenosine and its derivatives in post-traumatic animal models showed suppression of epileptic discharges through scavenging free radicals such as OH [117]. Subsequently, Malhotra et al. demonstrated that adenosine and its analogues protect against seizures induced by chemical agents through their action on A1 receptors [118].
Although the efficacy of corticosteroids has been established in spinal cord injury, the administration of these agents is controversial in TBI. Previously, Hoeppner had shown that prednisone prevents epileptogenesis in a metallic aluminum-injected animal model [119]. However, in a randomized placebo-controlled trial, the risk of death within 2 weeks after brain injury was higher in the group that received corticosteroids compared with placebo. The prevalence of seizure did not differ significantly between the two groups during this period [120]. In a retrospective study, corticosteroids treatment within the first day of head trauma resulted in increased seizure activity and was not associated with any decrease in PTE [121].
As discussed earlier, TBI initiates a cascade of neuroinflammation in the brain, which may induce epileptogenesis and contribute to development of PTE. As such, recent investigations have attempted to focus on neuroinflammatory agents as the novel therapeutic targets in the post-traumatic phase. Diamond and colleagues demonstrated that patients who developed PTE had a higher ratio of cerebrospinal fluid (CSF)/serum IL-1β and lower levels of serum IL-1β, whereas the difference between CSF IL-1β levels was not significant [122]. Dextromethorphan derivative is an experimental treatment which reduces both neuroinflammation and nonconvulsive seizures in a penetrating ballistic-like brain injury (PBBI ) model [123]. Minozac prevents experimental seizure susceptibility by suppression of cytokine upregulation in the hippocampus in a “two-hit” injury model [124]. Most recently, perampanel, an antiepileptic drug, has been shown to have neuroprotective effects through reduced neuronal apoptosis, inhibition of lipid peroxidation, and suppression of pro-inflammatory cytokines such as tumor necrosis factor-α (TNF-α) and IL-1β, as well as increase in the levels of anti-inflammatory cytokines IL-10 and transforming growth factor-β (TGF-β 1) [125] although its prophylactic effect on PTS or PTE has not been studied. Recently, cooling has gained attention as a prophylactic treatment in PTE, possibly via anti-inflammatory mechanisms. Focal mild cooling prevented the onset of epileptic seizures in a rostral parasagittal PFI model both during and after the treatment. Rare remaining seizures were shorter than in controls [126].
Studies have demonstrated that the mTOR signaling pathway is abnormally activated in TBI, and rapamycin, an mTOR inhibitor, suppresses epileptogenesis of dentate gyrus granule cells in the ipsilateral temporal lobe in CCI models [127, 128]. Inhibition of mTOR also showed antiepileptogenic and neuroprotective effect in an organotypic hippocampal culture model of PTE [129]. While exogenous insulin-like growth factor-1 (IGF-1) has neuroprotective effect early after TBI, in long term, it contributes to epileptogenesis through activation of mTOR cascade [130]. In animal epilepsy models, activation of cannabinoid type-1 (CB1) receptor prevents the seizure [131]. Cannabinoid receptors downregulate after TBI, leading to hyperexcitability. This is followed by upregulation in 4 weeks. Despite the protective role of the CB1receptor agonists [131], Echegoyen et al. showed that a single use of a CB1receptor antagonist immediately after TBI could disrupt the epileptogenic process and prevent PTE occurrence [132]. In contrast, Nissinen J and colleagues showed that either immediate single dosage or long-term treatment with SR141716 (a CB1 receptor antagonist) initiated 30 min after injury did not have antiepileptic effect in a lateral FPI model [133]. This difference was attributed to later timepoint assessment, different types of assessment of seizure susceptibility, and the number of included animals.
Surgical Intervention
The presence of focal cerebral pathology in patients with PTE prompts the consideration of surgical options in medically refractory patients [91]. Indeed, the success rate of surgical resection appears to be comparable to that in the non-traumatic population [77, 134]. Therefore, PTE patients should be worked up similarly to non-traumatic patients with epilepsy in terms of determining surgical candidacy. In an optimal treatment plan, both pharmacological and surgical options should be considered when appropriate, since early surgery prevents progressive secondary injury from recurrent seizures [77]. The likelihood of seizure freedom depends on the ictal onset zone as well as the presence of an identifiable lesion [135]. Rates of seizure freedom in PTE patients with MTLE who undergo temporal lobectomy can be as high as 69–90% [77, 136, 137], compared with 33% in patients with frontal lobe epilepsy, similar to what is seen in the non-traumatic population [77]. While neocortical seizures are less ideal surgical candidates [74, 83], the presence of focal encephalomalacia predicts a good outcome with electrocorticography-guided resections [138].
Nevertheless, in the surgical approach in patients with medically refractory PTE, several challenges might be encountered. Firstly, diffuse cerebral injury induced by TBI can result in multifocal epilepsy which may not be surgically amenable. Secondly, owing to prior craniotomies and breach rhythms, seizure foci might be difficult to localize precisely [139]. In addition, orbitofrontal cortex is commonly involved, impacting accurate localization of the epileptogenic zone [83].
Neuromodulation is a palliative treatment which is reserved for medically refractory patients who are not suitable candidates for conventional resective surgery, either because the seizure onset zone cannot be adequately localized or because it involves eloquent cortex which is not safe to remove. Neuromodulation is believed to provide high-frequency stimulation which desynchronizes the cerebral cortex and prevents seizure. Neuromodulation modalities which are used currently in the treatment of patients with medically refractory epilepsy are deep brain stimulation (DBS ), vagal nerve stimulation (VNS ), and responsive neurostimulation (RNS ).
VNS in post-traumatic patients is thought to be comparable to the non-traumatic population. However, one case-control study indicated that VNS was associated with more than 50% reduction in seizure frequency in 78% of patients with PTE as opposed to 61% in patients with non-traumatic epilepsy at 2-year follow-up, suggesting it may have greater efficacy in this group [140]. Similarly, DBS of the anterior nucleus of the thalamus (ATN ) showed a seizure frequency reduction by 40.4% in refractory PTE patients [141]. However, the seizure reduction effect was only significant if the seizures originated from one or both temporal lobes compared with seizures arising from frontal, parietal, and occipital regions or multifocal/diffuse seizures. In addition, the number of responders during the blinded evaluation period was not significantly different between the groups. However, the seizure frequency reduction and responder rates increased significantly in long-term nonblinded follow-up by 56% and 54%, respectively.
Unlike the other two modalities, RNS is a closed-loop system that prevents seizures by detecting epileptiform activities and stimulating the seizure onset zone. Two studies showed a significant difference in seizure frequency reduction (37.9–41.5%) between active and control groups [142, 143]. However, the percentage of the responder was not significant. Similar to DBS , improved efficacy was observed in long-term stimulation. However, there have been no reports of RNS specifically in patients with PTE, and therefore, it is not clear whether efficacy is similar in this population.
Conclusion
PTE is a serious common complication of TBI, comprising 5% of all epilepsies. Several risk factors have been identified, anticipating the likelihood of developing PTS and PTE. Severe TBI is correlated with an increased risk of developing PTS and PTE. Whether PTS increases the risk of PTE is controversial. Recently, genetic association studies have identified a number of genetic variants predisposing patients with TBI to PTS or PTE. Numerous experimental studies have attempted to identify the nature of hyperexcitability after TBI. The post-traumatic animal models have recently highlighted the putative role of inflammation as one of the underlying pathophysiology of neuronal hyperexcitability. Localization-related epilepsy represents the most common epilepsy occurring after TBI, and there is a high predilection for temporal and frontal lobe epilepsy in this regard. High percentage of recurrence is observed within the first 2 years after injury. Although the role of AEDs in prophylactic treatment of PTS has been well established, they are not able to prevent PTE. Phenytoin is a highly recommended prophylactic therapy within the first week after TBI although levetiracetam has shown comparable effect to phenytoin. No neuroprotective agent has been proved to prevent PTE or PTS in human. Clinical approach and principles of AED selection in PTE are identical to other epilepsy syndromes, and surgery may be indicated in patients who do not respond properly to AEDs.
References
Annegers JF, Grabow JD, Groover RV, Laws ER, Elveback LR, Kurland LT. Seizures after head trauma: a population study. Neurology. 1980;30(7 Pt 1):683–9.
Annegers JF, Hauser WA, Coan SP, Rocca WA. A population-based study of seizures after traumatic brain injuries. N Engl J Med. 1998;338(1):20–4.
Annegers JF, Coan SP. The risks of epilepsy after traumatic brain injury. Seizure. 2000;9(7):453–7.
Semah F, Picot M, Adam C, Broglin D, Arzimanoglou A, Bazin B, et al. Is the underlying cause of epilepsy a major prognostic factor for recurrence? Neurology. 1998;51:1256–62.
Lowenstein DH. Epilepsy after head injury: an overview. Epilepsia. 2009;50(SUPPL. 2):4–9.
Fisher RS, Acevedo C, Arzimanoglou A, Bogacz A, Cross JH, Elger CE, et al. A practical clinical definition of epilepsy. Epilepsia. 2014;55(4):475–82.
Frey LC. Epidemiology of posttraumatic epilepsy: a critical review. Epilepsia. 2003;44:11–7.
Asikainen I, Kaste M, Sarna S. Early and late posttraumatic seizures in traumatic brain injury rehabilitation patients: brain injury factors causing late seizures and influence of seizures on long-term outcome. Epilepsia. 1999;40(5):584–9.
Salazar AM, Jabbari B, Vance SC, Grafman J, Amin D, Dillon JD. Epilepsy after penetrating head injury. I. Clinical correlates: a report of the Vietnam head injury study. Neurology. 1985;35(10):1406–14.
Malec JF, Brown AW, Leibson CL, Flaada JT, Mandrekar JN, Diehl NN, et al. The Mayo classification system for traumatic brain injury severity. J Neurotrauma. 2007;24(9):1417–24.
Hahn YS, Fuchs S, Flannery AM, Barthel MJ, McLone DG. Factors influencing posttraumatic seizures in children. Neurosurgery. 1988;22(5):864–7.
Maganti RK, Rutecki P. EEG and epilepsy monitoring. CONTINUUM Lifelong Learn Neurol. 2013;19:598–622.
Vespa PM, Nuwer MR, Nenov V, Ronne-Engstrom E, Hovda DA, Bergsneider M, et al. Increased incidence and impact of nonconvulsive and convulsive seizures after traumatic brain injury as detected by continuous electroencephalographic monitoring. J Neurosurg. 1999;91:750–60.
Arndt DH, Lerner JT, Matsumoto JH, Madikians A, Yudovin S, Valino H, et al. Subclinical early posttraumatic seizures detected by continuous EEG monitoring in a consecutive pediatric cohort. Epilepsia. 2013;54(10):1780–8.
Ronne-Engstrom E, Winkler T. Continuous EEG monitoring in patients with traumatic brain injury reveals a high incidence of epileptiform activity. Acta Neurol Scand. 2006;114(1):47–53.
Waziri A, Claassen J, Morgan Stuart R, Arif H, Michael Schmidt J, Mayer SA, et al. Intracortical electroencephalography in acute brain injury. Ann Neurol. 2009;66(3):366–77.
Vespa P, Miller C, McArthur D, Eliseo M, Etchepare M, Hirt D, et al. Nonconvulsive electrographic seizures after traumatic brain injury result in a delayed, prolonged increase in intracranial pressure and metabolic crisis. Crit Care Med. 2007;35(12):2830–6.
Vespa PM, McArthur DL, Xu Y, Eliseo M, Etchepare M, Dinov I, et al. Nonconvulsive seizures after traumatic brain injury are associated with hippocampal atrophy. Neurology. 2010;75(9):792–8.
Hauser WA, Annegers JF, Kurland LT. Incidence of epilepsy and unprovoked seizures in Rochester, Minnesota: 1935–1984. Epilepsia. 1993;34(3):453–8.
Angeleri F, Majkowski J, Cacchio G, Sobieszek A, D’Acunto S, Gesuita R, et al. Posttraumatic epilepsy risk factors: one-year prospective study after head injury. Epilepsia. 1999;40(9):1222–30.
Englander J, Bushnik T, Duong TT, Cifu DX, Zafonte R, Wright J, et al. Analyzing risk factors for late posttraumatic seizures: a prospective, multicenter investigation. Arch Phys Med Rehabil. 2003;84(3 SUPPL. 1):365–73.
Agrawal A, Timothy J, Pandit L, Manju M. Post-traumatic epilepsy: an overview. Clin Neurol Neurosurg. 2006;108(5):433–9.
Temkin NR, Anderson GD, Winn HR, Ellenbogen RG, Britz GW, Schuster J, et al. Magnesium sulfate for neuroprotection after traumatic brain injury: a randomised controlled trial. Lancet Neurol. 2007;6(1):29–38.
Temkin NR. Risk factors for posttraumatic seizures in adults. Epilepsia. 2003;44(SUPPL. 10):18–20.
Pitkänen A, Lukasiuk K. Molecular and cellular basis of epileptogenesis in symptomatic epilepsy. Epilepsy Behav. 2009;14(1 SUPPL. 1):16–25.
Davidson J, Cusimano MD, Bendena WG. Post-traumatic brain injury: genetic susceptibility to outcome. Neurosci. 2015;21(4):424–41.
Scheffer IE. Epilepsy genetics revolutionizes clinical practice. Neuropediatrics. 2014;45:70–4.
Schaumann BA, Annegers JF, Johnson SB, Moore KJ, Lubozynski MF, Salinsky MC. Family history of seizures in posttraumatic and alcohol-associated seizure disorders. Epilepsia. 1994;35(1):48–52.
Christensen J, Pedersen MG, Pedersen CB, Sidenius P, Olsen J, Vestergaard M. Long-term risk of epilepsy after traumatic brain injury in children and young adults: a population-based cohort study. Lancet. 2009;373(9669):1105–10.
Hung R, Carroll LJ, Cancelliere C, Cote P, Rumney P, Keightley M, et al. Systematic review of the clinical course, natural history, and prognosis for pediatric mild traumatic brain injury: results of the international collaboration on mild traumatic brain injury prognosis. Arch Phys Med Rehabil. 2014;95(3 Suppl):S174–91.
Raymont V, Salazar AM, Krueger F, Grafman J. “Studying injured minds” - the Vietnam head injury study and 40 years of brain injury research. Front Neurol. 2011;2:15.
Diaz-Arrastia R, Gong Y, Fair S, Scott KD, Garcia MC, Carlile MC, et al. Increased risk of late posttraumatic seizures associated with inheritance of APOE e4 allele. Arch Neurol. 2003;60:818–22.
Cotter D, Kelso A, Neligan A. Genetic biomarkers of posttraumatic epilepsy: a systematic review. Seizure. 2017;46:53–8.
Ritter AC, Kammerer CM, Brooks MM, Conley YP, Wagner AK. Genetic variation in neuronal glutamate transport genes and associations with posttraumatic seizure. Epilepsia. 2016;57(6):984–93.
Myers KA, Scheffer IE. DEPDC5 as a potential therapeutic target for epilepsy. Expert Opin Ther Targets. 2017;21:591–600.
Pitkänen A, McIntosh TK. Animal models of post-traumatic epilepsy. J Neurotrauma. 2006;23(2):241–61.
Lifshitz J. Fluid percussion injury model. In: Animal models of acute neurological injuries; 2009. p. 369–84.
Bragin A, Li L, Almajano J, Alvarado-Rojas C, Reid AY, Staba RJ, et al. Pathologic electrographic changes after experimental traumatic brain injury. Epilepsia. 2016;57(5):735–45.
Reid AY, Bragin A, Giza CC, Staba RJ, Engel J. The progression of electrophysiologic abnormalities during epileptogenesis after experimental traumatic brain injury. Epilepsia. 2016;57(10):1558–67.
D’Ambrosio R, Fairbanks JP, Fender JS, Born DE, Doyle DL, Miller JW. Post-traumatic epilepsy following fluid percussion injury in the rat. Brain. 2004;127(Pt 2):304–14.
Hunt RF, Scheff SW, Smith BN. Posttraumatic epilepsy after controlled cortical impact injury in mice. Exp Neurol. 2009;215(2):243–52.
Edward Dixon C, Clifton GL, Lighthall JW, Yaghmai AA, Hayes RL. A controlled cortical impact model of traumatic brain injury in the rat. J Neurosci Methods. 1991;39(3):253–62.
Laurer HL, Lenzlinger PM, McIntosh TK. Models of traumatic brain injury. Eur J Trauma. 2000;26:95–110.
Hunt RF, Boychuk JA, Smith BN. Neural circuit mechanisms of post–traumatic epilepsy. Front Cell Neurosci. 2013;7(June):1–14.
Mautes AE, Thome D, Steudel WI, Nacimiento AC, Yang Y, Shohami E. Changes in regional energy metabolism after closed head injury in the rat. J Mol Neurosci. 2001;16(1):33–9.
Chandel S, Gupta SK, Medhi B. Epileptogenesis following experimentally induced traumatic brain injury - a systematic review. Rev Neurosci. 2016;27(3):329–46.
Golarai G, Greenwood a C, Feeney DM, Connor JA. Physiological and structural evidence for hippocampal involvement in persistent seizure susceptibility after traumatic brain injury. J Neurosci. 2001;21(21):8523–37.
Reeves TM, Kao CQ, Phillips LL, Bullock MR, Povlishock JT. Presynaptic excitability changes following traumatic brain injury in the rat. J Neurosci Res. 2000;60(3):370–9.
Griesemer D, Mautes AM. Closed head injury causes hyperexcitability in rat hippocampal CA1 but not in CA3 pyramidal cells. J Neurotrauma. 2007;24(12):1823–32.
Morganti-Kossmann MC, Rancan M, Stahel PF, Kossmann T. Inflammatory response in acute traumatic brain injury: a double-edged sword. Curr Opin Crit Care. 2002;8(2):101–5.
Hu S, Sheng WS, Ehrlich LC, Peterson PK, Chao CC. Cytokine effects on glutamate uptake by human astrocytes. Neuroimmunomodulation. 2000;7(3):153–9.
Balosso S, Ravizza T, Pierucci M, Calcagno E, Invernizzi R, Di Giovanni G, et al. Molecular and functional interactions between tumor necrosis factor-alpha receptors and the glutamatergic system in the mouse hippocampus: implications for seizure susceptibility. Neuroscience. 2009;161(1):293–300.
Pickering M, Cumiskey D, O’Connor JJ. Actions of TNF-alpha on glutamatergic synaptic transmission in the central nervous system. Exp Physiol. 2005;90(5):663–70.
Zhu G, Okada M, Yoshida S, Mori F, Ueno S, Wakabayashi K, et al. Effects of interleukin-1?? On hippocampal glutamate and GABA releases associated with Ca2+−induced Ca2+ releasing systems. Epilepsy Res. 2006;71(2–3):107–16.
Samuelsson C, Kumlien E, Flink R, Lindholm D, Ronne-Engström E. Decreased cortical levels of astrocytic glutamate transport protein GLT-1 in a rat model of posttraumatic epilepsy. Neurosci Lett. 2000;289(3):185–8.
Rao VL, Dogan A, Bowen KK, Todd KG, Dempsey RJ. Antisense knockdown of the glial glutamate transporter GLT-1 exacerbates hippocampal neuronal damage following traumatic injury to rat brain. Eur J Neurosci. 2001;13(1):119–28.
Tomkins O, Feintuch A, Benifla M, Cohen A, Friedman A, Shelef I. Blood-brain barrier breakdown following traumatic brain injury: a possible role in posttraumatic epilepsy. Cardiovasc Psychiatry Neurol. 2011;2011:765923.
Loscher W, Brandt C. Prevention or modification of Epileptogenesis after brain insults: experimental approaches and translational research. Pharmacol Rev. 2010;62(4):668–700.
Gao X, Deng P, Xu ZC, Chen J. Moderate traumatic brain injury causes acute dendritic and synaptic degeneration in the hippocampal dentate gyrus. PLoS One. 2011;6(9):e24566.
Robinson S, Berglass JB, Denson JL, Berkner J, Anstine CV, Winer JL, et al. Microstructural and microglial changes after repetitive mild traumatic brain injury in mice. J Neurosci Res. 2017;95(4):1025–35.
Shitaka Y, Tran HT, Bennett RE, Sanchez L, Levy MA, Dikranian K, et al. Repetitive closed-skull traumatic brain injury in mice causes persistent multifocal axonal injury and microglial reactivity. J Neuropathol Exp Neurol. 2011;70(7):551–67.
Chirumamilla S, Sun D, Bullock MR, Colello RJ. Traumatic brain injury induced cell proliferation in the adult mammalian central nervous system. J Neurotrauma. 2002;19(6):693–703.
Griesemer D, Mautes AM. Closed head injury causes Hyperexcitability in rat hippocampal CA1 but not in CA3 pyramidal cells. J Neurotrauma. 2007;24(12):1823–32.
Zhang B-L, Chen X, Tan T, Yang Z, Carlos D, Jiang R-C, et al. Traumatic brain injury impairs synaptic plasticity in hippocampus in rats. Chin Med J. 2011;124(5):740–5.
Prince DA, Parada I, Scalise K, Graber K, Jin X, Shen F. Epilepsy following cortical injury: cellular and molecular mechanisms as targets for potential prophylaxis. Epilepsia. 2009;50:30–40.
Li H, Prince DA. Synaptic activity in chronically injured, epileptogenic sensory-motor neocortex. J Neurophysiol. 2002;88(1):2–12.
Cantu D, Walker K, Andresen L, Taylor-Weiner A, Hampton D, Tesco G, et al. Traumatic brain injury increases cortical glutamate network activity by compromising GABAergic control. Cereb Cortex. 2015;25(8):2306–20.
Swartz BE, Houser CR, Tomiyasu U, Walsh GO, DeSalles A, Rich JR, et al. Hippocampal cell loss in posttraumatic human epilepsy. Epilepsia. 2006;47(8):1373–82.
Atkins CM, Truettner JS, Lotocki G, Sanchez-Molano J, Kang Y, Alonso OF, et al. Post-traumatic seizure susceptibility is attenuated by hypothermia therapy. Eur J Neurosci. 2010;32(11):1912–20.
Hu B, Liu C, Bramlett H, Sick TJ, Alonso OF, Chen S, et al. Changes in trkB-ERK1/2-CREB/Elk-1 pathways in hippocampal mossy fiber organization after traumatic brain injury. J Cereb Blood Flow Metab. 2004;24(8):934–43.
Hunt RF, Scheff SW, Smith BN. Regionally localized recurrent excitation in the dentate gyrus of a cortical contusion model of posttraumatic epilepsy. J Neurophysiol. 2010;103(3):1490–500.
Hunt RF, Haselhorst LA, Schoch KM, Bach EC, Rios-Pilier J, Scheff SW, et al. Posttraumatic mossy fiber sprouting is related to the degree of cortical damage in three mouse strains. Epilepsy Res. 2012;99(1–2):167–70.
D’Ambrosio R, Fender JS, Fairbanks JP, Simon EA, Born DE, Doyle DL, et al. Progression from frontal-parietal to mesial-temporal epilepsy after fluid percussion injury in the rat. Brain. 2005;128(1):174–88.
Diaz-Arrastia R, Agostini MA, Frol a B, Mickey B, Fleckenstein J, Bigio E, et al. Neurophysiologic and neuroradiologic features of intractable epilepsy after traumatic brain injury in adults. Arch Neurol. 2000;57(11):1611–6.
Haltiner AM, Temkin NR, Dikmen SS. Risk of seizure recurrence after the first late posttraumatic seizure. Arch Phys Med Rehabil. 1997;78(8):835–40.
Christensen J. The epidemiology of posttraumatic epilepsy epidemiology of traumatic. Brain Inj. 2015;35(3):218–22.
Gupta PK, Sayed N, Ding K, Agostini MA, Van Ness PC, Yablon S, et al. Subtypes of post-traumatic epilepsy: clinical, electrophysiological, and imaging features. J Neurotrauma. 2014;31(16):1439–43.
Manaka S, Takahashi H, Sano K. The difference between children and adults in the onset of post-traumatic epilepsy. Psychiatry Clin Neurosci. 1981;35(3):301–4.
Pohlmann-Eden B, Bruckmeir J. Predictors and dynamics of posttraumatic epilepsy. Acta Neurol Scand. 1997;95(5):257–62.
Adams JH, Scott G, Parker LS, Graham DI, Doyle D. The contusion index: a quantitative approach to cerebral contusions in head injury. Neuropathol Appl Neurobiol. 1980;6(4):319–24.
Bešenski N, Broz R, Jadro-Šantel D, Pavić D, Mikulić D. The course of the traumatising force in acceleration head injury: CT evidence. Neuroradiology. 1996;38(SUPPL. 1):S36.
Curia G, Levitt M, Fender JS, Miller JW, Ojemann J, D’Ambrosio R. Impact of injury location and severity on posttraumatic epilepsy in the rat: role of frontal neocortex. Cereb Cortex. 2011;21(7):1574–92.
Marks DA, Kim J, Spencer DD, Spencer SS. Seizure localization and pathology following head injury in patients with uncontrolled epilepsy. Neurology. 1995;4Marks, D(11):2051–7.
Jennett B. Posttraumatic epilepsy. Adv Neurol. 1979;22:137–47.
Kwan P. The natural history of epilepsy: an epidemiological view. J Neurol Neurosurg Psychiatry. 2004;75(10):1376–81.
Ilaria Casetta EC. Post-traumatic epilepsy: review. J Neurol Neurophysiol. 2011;s2(1):009.
Hung C, Chen JWY. Treatment of post-traumatic epilepsy. Curr Treat Options Neurol. 2012;14(4):293–306.
Chen LLK, Baca CB, Choe J, Chen JW, Ayad ME, Cheng EM, et al. Posttraumatic epilepsy in operation enduring freedom / operation Iraqi freedom veterans. Mil Med. 2014;179(May):492–7.
Salinsky M, Storzbach D, Goy E, Evrard C. Traumatic brain injury and psychogenic seizures in veterans. J Head Trauma Rehabil. 2015;30(February):E65–70.
Barry E, Krumholz A, Bergey GK, Chatha H, Alemayehu S, Grattan L. Nonepileptic posttraumatic seizures. Epilepsia. 1998;39(4):427–31.
Rao V, Parko K. Clinical approach to posttraumatic epilepsy. Semin Neurol. 2015;35(1):057–63.
Messori A, Polonara G, Carle F, Gesuita R, Salvolini U. Predicting posttraumatic epilepsy with MRI: prospective longitudinal morphologic study in adults. Epilepsia. 2005;46(9):1472–81.
Diaz-Arrastia R, Agostini MA, Madden CJ, Van Ness PC. Posttraumatic epilepsy: the endophenotypes of a human model of epileptogenesis. Epilepsia. 2009;50(SUPPL. 2):14–20.
Kou Z, Wu Z, Tong KA, Holshouser B, Benson RR, Hu J, et al. The role of advanced MR imaging findings as biomarkers of traumatic brain injury. J Head Trauma Rehabil. 2010;25(4):267–82.
Jennett B, van de Sande J. EEG prediction of post-Traumatic epilepsy. Epilepsia. 1975;16(2):251–6.
Steinbaugh LA, Lindsell CJ, Shutter LA, Szaflarski JP. Initial EEG predicts outcomes in a trial of levetiracetam vs. fosphenytoin for seizure prevention. Epilepsy Behav. 2012;23(3):280–4.
Heikkinen ER, Ronty HS, Tolonen U, Pyhtinen J. Development of posttraumatic epilepsy. Stereotact Funct Neurosurg. 1990;54–55:25–33.
McCrory PR, Bladin PF, Berkovic SF. Retrospective study of concussive convulsions in elite Australian rules and rugby league footballers: phenomenology, aetiology, and outcome. BMJ. 1997;314(7075):171.
Temkin NR, Dikmen SS, Wilensky AJ, Keihm J, Chabal S, Winn HR. A randomized, double-blind study of phenytoin for the prevention of post-traumatic seizures. N Engl J Med. 1990;323(8):497–502.
Kruer RM, Harris LH, Goodwin H, Kornbluth J, Thomas KP, Slater LA, et al. Changing trends in the use of seizure prophylaxis after traumatic brain injury: a shift from phenytoin to levetiracetam. J Crit Care. 2013;28(5):883.e9.
Yang Y, Zheng F, Xu X, Wang X. Levetiracetam versus phenytoin for seizure prophylaxis following traumatic brain injury: a systematic review and meta-analysis. CNS Drugs. 2016;30(8):677–88.
Khan NR, Vanlandingham MA, Fierst TM, Hymel C, Hoes K, Evans LT, et al. Should Levetiracetam or phenytoin be used for posttraumatic seizure prophylaxis? A systematic review of the literature and meta-analysis. Neurosurgery. 2016;79(6):775–81.
Szaflarski JP, Sangha KS, Lindsell CJ, Shutter LA. Prospective, randomized, single-blinded comparative trial of intravenous levetiracetam versus phenytoin for seizure prophylaxis. Neurocrit Care. 2010;12(2):165–72.
Torbic H, Forni AA, Anger KE, Degrado JR, Greenwood BC. Use of antiepileptics for seizure prophylaxis after traumatic brain injury. Am J Health Syst Pharm. 2013;70:759–66.
Jones KE, Puccio AM, Harshman KJ, Falcione B, Benedict N, Jankowitz BT, et al. Levetiracetam versus phenytoin for seizure prophylaxis in severe traumatic brain injury. Neurosurg Focus. 2008;25(4):E3.
Glotzner FL, Haubitz I, Miltner F, Kapp G, Pflughaupt KW. Seizure prevention using carbamazepine following severe brain injuries. Neurochirurgia (Stuttg). 1983;26(0028–3819):66–79.
Temkin NR, Dikmen SS, Anderson GD, Wilensky AJ, Holmes MD, Cohen W, et al. Valproate therapy for prevention of posttraumatic seizures: a randomized trial. J Neurosurg. 1999;91(4):593–600.
Temkin NR. Preventing and treating posttraumatic seizures: the human experience. In: Epilepsia; 2009. p. 10–3.
Chadwick D. Seizures and epilepsy after traumatic brain injury. Lancet. 2000;355(9201):334–6.
Dikmen SS, Temkin NR, Miller B, Machamer J, Winn HR. Neurobehavioral effects of phenytoin prophylaxis of posttraumatic seizures. JAMA. 1991;265(10):1271–7.
Langendorf FG, Pedley TA, Temkin NR. Chapter 253 Posttraumatic Seizures.
Burneo JG, Sirven JI, Kiesel LW, Vecht CJ, Jehi L, Chung SS, et al. Managing common complex symptomatic epilepsies: tumors and trauma. Epilepsy Curr. 2013;13:232–5.
Hernandez TD. Preventing post-traumatic epilepsy after brain injury: weighing the costs and benefits of anticonvulsant prophylaxis. Trends Pharmacol Sci. 1997;18:59–62.
LaFrance WC, Deluca M, MacHan JT, Fava JL. Traumatic brain injury and psychogenic nonepileptic seizures yield worse outcomes. Epilepsia. 2013;54(4):718–25.
Camfield P, Camfield C. When is it safe to discontinue AED treatment? Epilepsia. 2008;49:25–8.
Levy SL, Burnham WM, Hwang PA. An evaluation of the anticonvulsant effects of vitamin E. Epilepsy Res. 1990;6:12–7.
Yokoi I, Toma J, Liu J, Kabuto H, Mori A. Adenosines scavenged hydroxyl radicals and prevented posttraumatic epilepsy. Free Radic Biol Med. 1995;19(4):473–9.
Malhotra J, Gupta YK. Effect of adenosine receptor modulation on pentylenetetrazole-induced seizures in rats. Br J Pharmacol. 1997;120(2):282–8.
Hoeppner TJ, Morrell F. Control of scar formation in experimentally induced epilepsy. Exp Neurol. 1986;94(3):519–36.
Roberts I, Yates D, Sandercock P, Farrell B, Wasserberg J, Lomas G, et al. Effect of intravenous corticosteroids on death within 14 days in 10008 adults with clinically significant head injury (MRC CRASH trial): randomised placebo-controlled trial. Lancet. 2004;364(9442):1321–8.
Watson NF, Barber JK, Doherty MJ, Miller JW, Temkin NR. Does glucocorticoid administration prevent late seizures after head injury? Epilepsia. 2004;45(6):690–4.
Diamond ML, Ritter AC, Failla MD, Boles JA, Conley YP, Kochanek PM, et al. IL-1β associations with posttraumatic epilepsy development: a genetics and biomarker cohort study. Epilepsia. 2015;56(7):991–1001.
Lu X-CM, Shear DA, Graham PB, Bridson GW, Uttamsingh V, Chen Z, et al. Dual therapeutic effects of C-10068, a dextromethorphan derivative, against post-traumatic nonconvulsive seizures and Neuroinflammation in a rat model of penetrating ballistic-like brain injury. J Neurotrauma. 2015;32(20):1621–32.
Chrzaszcz M, Venkatesan C, Dragisic T, Watterson DM, Wainwright MS. Minozac treatment prevents increased seizure susceptibility in a mouse “two-hit” model of closed skull traumatic brain injury and electroconvulsive shock-induced seizures. J Neurotrauma. 2010;27(7):1283–95.
Chen T, Dai SH, Jiang ZQ, Luo P, Jiang XF, Fei Z, et al. The AMPAR antagonist Perampanel attenuates traumatic brain injury through anti-oxidative and anti-inflammatory activity. Cell Mol Neurobiol. 2017;37(1):43–52.
D’Ambrosio R, Eastman CL, Darvas F, Fender JS, Verley DR, Farin FM, et al. Mild passive focal cooling prevents epileptic seizures after head injury in rats. Ann Neurol. 2013;73(2):199–209.
Butler CR, Boychuk JA, Smith BN. Differential effects of rapamycin treatment on tonic and phasic GABAergic inhibition in dentate granule cells after focal brain injury in mice. Exp Neurol. 2016;280:30–40.
Butler CR, Boychuk JA, Smith BN. Effects of rapamycin treatment on neurogenesis and synaptic reorganization in the dentate gyrus after controlled cortical impact injury in mice. Front Syst Neurosci. 2015;9:163.
Berdichevsky Y, Dryer AM, Saponjian Y, Mahoney MM, Pimentel CA, Lucini CA, et al. PI3K-Akt signaling activates mTOR-mediated Epileptogenesis in Organotypic hippocampal culture model of post-traumatic epilepsy. J Neurosci. 2013;33(21):9056–67.
Song Y, Pimentel C, Walters K, Boller L, Ghiasvand S, Liu J, et al. Neuroprotective levels of IGF-1 exacerbate epileptogenesis after brain injury. Sci Rep. 2016;6(1):32095.
Kozan R, Ayyildiz M, Agar E. The effects of intracerebroventricular AM-251, a CB1-receptor antagonist, and ACEA, a CB1-receptor agonist, on penicillin-induced epileptiform activity in rats. Epilepsia. 2009;50(7):1760–7.
Echegoyen J, Armstrong C, Morgan RJ, Soltesz I. Single application of a CB1 receptor antagonist rapidly following head injury prevents long-term hyperexcitability in a rat model. Epilepsy Res. 2009;85(1):123–7.
Nissinen J, Andrade P, Natunen T, Hiltunen M, Malm T, Kanninen K, et al. Disease-modifying effect of atipamezole in a model of post-traumatic epilepsy. Epilepsy Res. 2017;136:18–34.
Hartzfeld P, Elisevich K, Pace M, Smith B, Gutierrez JA. Characteristics and surgical outcomes for medial temporal post-traumatic epilepsy. Br J Neurosurg. 2008;22(2):224–30.
Benbadis SR, Tatum WO, Vale FL. When drugs don’t work: an algorithmic approach to medically intractable epilepsy. Neurology. 2000;55(12):1780–4.
Elliott RE, Bollo RJ, Berliner JL, Silverberg A, Carlson C, Geller EB, et al. Anterior temporal lobectomy with amygdalohippocampectomy for mesial temporal sclerosis: predictors of long-term seizure control. J Neurosurg. 2013;119:261–72.
Spencer S, Huh L. Outcomes of epilepsy surgery in adults and children. Lancet Neurol. 2008;7:525–37.
Hakimian S, Kershenovich A, Miller JW, Ojemann JG, Hebb AO, D’Ambrosio R, et al. Long-term outcome of extratemporal resection in posttraumatic epilepsy. Neurosurg Focus. 2012;32(3):E10.
Brigo F, Cicero R, Fiaschi A, Bongiovanni LG. The breach rhythm. Clin Neurophysiol. 2011;122:2116–20.
Englot DJ, Chang EF, Auguste KI. Vagus nerve stimulation for epilepsy: a meta-analysis of efficacy and predictors of response. J Neurosurg. 2011;115(6):1248–55.
Fisher R, Salanova V, Witt T, Worth R, Henry T, Gross R, et al. Electrical stimulation of the anterior nucleus of thalamus for treatment of refractory epilepsy. Epilepsia. 2010;51(5):899–908.
Heck CN, King-Stephens D, Massey AD, Nair DR, Jobst BC, Barkley GL, et al. Two-year seizure reduction in adults with medically intractable partial onset epilepsy treated with responsive neurostimulation: final results of the RNS system pivotal trial. Epilepsia. 2014;55(3):432–41.
Morrell MJ. Responsive cortical stimulation for the treatment of medically intractable partial epilepsy. Neurology. 2011;77(13):1295–304.
Author Disclosures
Arezoo Rezazadeh
This author declares no financial or intellectual conflicts of interest.
Aylin Reid
This author declares no financial or intellectual conflicts of interest.
Danielle M Andrade
This author declares no financial or intellectual conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Rezazadeh, A., Andrade, D.M., Reid, A. (2018). Post-traumatic Epilepsy. In: Anghinah, R., Paiva, W., Battistella, L., Amorim, R. (eds) Topics in Cognitive Rehabilitation in the TBI Post-Hospital Phase. Springer, Cham. https://doi.org/10.1007/978-3-319-95376-2_7
Download citation
DOI: https://doi.org/10.1007/978-3-319-95376-2_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-95374-8
Online ISBN: 978-3-319-95376-2
eBook Packages: MedicineMedicine (R0)