Abstract
The current treatment for massively bleeding patients is nearly identical to practices developed by physicians caring for thousands of injured combatants during World War I and II. After being forgotten for half a century, these techniques made a resurgence in the form of damage control resuscitation early in the twenty-first century, based on therapies employed during wars in Southwest Asia. The concepts include limiting crystalloid, whole blood, or balance blood component transfusions to achieve permissive hypotension, preventing hypothermia, and stopping bleeding as quickly as possible.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
It will be tragic if medical historian can look back on the WWII period and write of it as a time when so much was learned and so little remembered.—Dr. Henry Beecher (1951) [1]
With the exception of a few cases of whole blood transfusion, including four during the Civil War, crystalloid was the standard of therapy for hemorrhage shock in the nineteenth century and the first two decades of the twentieth century [2,3,4,5]. However, the onset of World War I and the subsequent great influx of severely injured combatants caused Allied surgeons to deem crystalloid “unsatisfactory” for treating massive hemorrhage because of the increased bleeding it caused [6]. That knowledge, along with advances in blood typing and preservation techniques at the beginning of the twentieth century, allowed whole blood to become the standard of care during the final year of World War I [5, 7, 8]. This persisted for the next four decades until dried plasma was developed just prior to WWII, and it became the standard early resuscitation fluid for US military surgeons during the war. It was transfused to maintain a systolic blood pressure of 85 mm Hg along with appropriate skin color and warmth while readying whole blood and attempting to stop the bleeding [1, 9,10,11]. Surgeons learned that warming the patient to physiologic temperature and transfusing whole blood to achieve a lower than normal blood pressure resulted in the “most dramatic improvement” [12, 13].
In the early 1960s, research by leading civilian trauma surgeons seemed to indicate that infusing Ringer’s lactate (LR) before whole blood improved survival for animals in hemorrhagic shock [14,15,16,17,18,19]. These models failed to take into account the chance for rebleeding from achieving a normal blood pressure and were not compared with whole blood resuscitation in scientific studies, but this did not prevent the adoption of crystalloids as a resuscitative fluid for bleeding casualties during the Vietnam War. An influential study published in the mid-1970s seemed to confirm the safety of crystalloid when it said that 1–2 l could be administered while waiting for whole blood to be crossmatched [20].
While increasing volumes of crystalloid were being incorporated into hemorrhagic shock resuscitation, advances in blood fractionation techniques permitted a unit of whole blood to be separated into separate units of red blood cells (RBCs), plasma, and platelets. This allowed for most patients requiring a blood transfusion to be treated with only the component in which they were deficient, thus conserving blood supplies while limiting exposure to potential pathogens and transfusion reactions [21,22,23,24]. At the time, experienced surgeons recommended moderation of crystalloid infusion and asserted that whole blood should be used to replace acute blood loss, but this did not prevent many busy trauma centers in the 1970s from exclusively infusing RBCs and LR in bleeding patients [18, 25,26,27].
The aggressive use of crystalloid and RBC resuscitation only grew in the last two decades of the twentieth century as studies proclaimed that transfusing platelets and plasma was not necessary until laboratory values demonstrated coagulopathy [28,29,30,31]. “Supranormal resuscitation” also became popular at this time because of subsequently refuted studies and HIV transmission was a concern for all blood transfusions [32,33,34,35,36,37,38,39,40,41].
19.1 Damage Control Resuscitation
At the beginning of the twenty-first century, complications resulting from large-volume crystalloid resuscitation, including cardiopulmonary dysfunction, abdominal compartment syndrome, multiple organ dysfunction syndrome, and mortality, were being identified and published [42, 43]. Coagulopathy was also identified in 25–33% of severely injured patients and was associated with increased mortality [44,45,46,47,48,49]. Observations of the clinical utility of whole blood were described from the 1993 Black Hawk Down episode [50]. As a result, the US military surgeons treating patients in Iraq and Afghanistan developed damage control resuscitation (DCR) as a way to mimic the lessons learned by Allied physicians treating thousands of combat casualties during the World Wars. DCR attempted to replicate the success of whole blood by transfusing balanced ratios of plasma and platelets to RBCs to achieve permissive hypotension while maintaining normal temperature and quickly stopping bleeding [51, 52]. This reduced the side effects associated with large-volume crystalloid infusion including dilutional coagulopathy, hypothermia from room temperature infusion, as well as increased inflammation, edema, and organ failure [53,54,55,56,57,58].
19.2 Limit Crystalloid
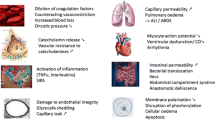
Large-volume crystalloid infusion worsens the “bloody vicious cycle” of coagulopathy, acidosis, and hypothermia by diluting clotting factors, cooling the patient, and worsening acidosis [27, 53, 54, 59, 60]. It also disrupts cellular mechanisms leading to inflammation and edema. This leads to increased mortality from cardiac, pulmonary, gastrointestinal, and immune system dysfunction as well as morbidity from decreased healing and increased incidences of anastomotic leak, abdominal compartment syndrome, and open abdomen [42, 43, 61,62,63,64,65,66, 56, 57,58,59]. Increased crystalloid resuscitation also results in more blood transfusions and more rapid clot breakdown (hyperfibrinolysis) [67,68,69,70].
19.3 Balanced Resuscitation
After implementing DCR in Iraq and Afghanistan, the military published their initial results with balanced resuscitation in 2007. The first retrospective trial showed improved survival for patients receiving higher ratios of plasma to RBCs [51]. These results were replicated in other military and civilian trials looking at both blunt and penetrating injuries [48, 71,72,73,74,75,76,77,78]. Similar results were found for balanced ratios of platelet transfusion [72, 79,80,81,82,83]. Civilian trauma centers quickly adopted balanced ratio massive resuscitation with 70–85% of level 1 centers now including it in their massive transfusion protocol, up from just a few centers a decade ago [84,85,86].
19.4 Survival Bias
A limitation to retrospective studies was highlighted in 2009 by a trial that examined the increased time required to thaw fresh frozen plasma (FFP) (93 min) for transfusion compared with RBCs (18 min) [87]. As a result, patients who survived ultimately received balance ratios of plasma, while those who died within the first few hours received RBCs but not other components which require longer to prepare. Prethawed plasma and never-frozen plasma are now available in more than 85% of surveyed trauma centers, to overcome the time required to thaw FFP [86, 88,89,90,91,92,93].
The PROPPR trial was a prospective, randomized, multicenter trial designed to evaluate the difference in outcomes between the two most common resuscitation ratios (1:1:1 and 1:1:2 (plasma/platelet/RBC)) [94]. While it did not show an improvement in 24 h or 30-day mortality, it did show the benefits of early balanced plasma and platelet resuscitation with decreased mortality at 3 h, decreased hemorrhagic death at 24 h, and increased median time to hemorrhage death [94,95,96,97]. PROPPR also showed no increase in complications for those treated with a 1:1:1 ratio, indicating that it is safe to transfuse higher ratios of plasma and platelets [94].
19.5 Whole Blood
While balance resuscitation was rapidly adopted in civilian trauma centers, the US military continued a long tradition of whole blood transfusions. Military physicians have safely transfused more than a million units of whole blood during wars over the past century, including more than 10,300 units of fresh whole blood to treat massively injured combatants in Iraq and Afghanistan [7, 8, 41, 98, 99]. Much of the transfused whole blood during these conflicts was provided by a walking blood bank of prescreened soldiers in rural settings. Retrospective reviews from these wars show improved 24-h and 30-day survival for massively transfused patients who received warm, fresh whole blood compared with those who received balanced ratios of blood components [100, 101]. This superiority is a result of the improved oxygen-carrying capacity, coagulation factors, platelet activity, flow characteristics, decreased dilution by storage solutions, and the superior hemostatic potential of whole blood compared to reconstituted component therapy [41, 98, 102].
19.6 Permissive Hypotension
In addition to replacing blood loss with whole blood or a balanced approximation, another component of damage control resuscitation is permissive hypotension. Originally described by World War I and II physicians, permissive hypotension contends that maintaining a lower than normal blood pressure decreases blood loss [9, 13]. The theory was confirmed by multiple animal models of uncontrolled hemorrhage [50, 103,104,105,106,107] and randomized trials in penetrating and blunt trauma patients [108,109,110].
19.7 Hypothermia
Hypothermia is common in severely injured trauma patients because of environmental exposure and infusion of room temperature fluids. It causes increased bleeding and mortality because of a reduction in coagulation enzyme activity and clot formation [27, 111,112,113,114,115]. Warming fluids and other rewarming techniques should be used to reverse these processes [57].
19.8 Stopping Hemorrhage
Rapid hemorrhage control is an important component of DCR because exsanguination is the leading cause of potentially survivable trauma deaths [116]. Tourniquets are effective for controlling extremity hemorrhage, and they have a low incidence of complications [117, 118]. Hemostatic dressings are effective for controlling compressible bleeding, but two-thirds of hemorrhagic deaths result from non-compressible torso trauma, so resuscitative endovascular balloon occlusion of the aorta (REBOA) has made a resurgence for quickly halting abdominal and pelvic hemorrhage with less morbidity than a resuscitative thoracotomy [116, 119,120,121,122]. Centers should implement a comprehensive hemorrhage control bundle, to begin prehospital and extend through the operating room [96].
19.9 Viscoelastic Hemostatic Assays
When bleeding slows, viscoelastic hemostatic assays (VHA), such as thromboelastography (TEG) and rotational thromboelastometry (ROTEM), can be used to guide resuscitation more precisely than fixed component ratios by evaluating clot formation, stability, and degradation as well as diagnose hypo- and hypercoagulable states [58, 123,124,125,126]. Rapid TEG is capable of predicting the need for component transfusions within 5 min, and a recent randomized control trial showed improved mortality and decreased blood component transfusions when comparing it with conventional coagulation tests [127, 128].
VHA also provide information on fibrinolysis, which is a spectrum of clot degradation ranging from hyperfibrinolysis with unmitigated hemorrhage to fibrinolysis shutdown causing excessive thrombus and subsequent organ dysfunction [129]. Fibrinolysis is diagnosed based on TEG LY30, and both extremes cause increased mortality [68, 129]. Administering tranexamic acid (TXA) within 3 h of injury reverses this laboratory abnormality, but it remains to be seen if this treatment for hyperfibrinolysis (LY30 > 3%) improves patient outcomes [130,131,132].
Conclusion
Cutting edge therapy for hemorrhage shock is nearly identical to the methods established while resuscitating thousands of critically wounded soldiers during WWI and WWII. The biggest difference is the currently accepted practice of balanced blood component therapy rather than whole blood, which was successfully used for half a century before being supplanted by crystalloid and RBCs, despite no comparison studies in uncontrolled hemorrhage. Because fractionated blood components are inferior to whole blood in oxygen-carrying capacity and coagulation, the best replacement for blood loss is almost assuredly whole blood. As a result, whole blood needs to be seriously evaluated as the therapy of choice for massively bleeding patients.
References
Beecher HK. Early care of the seriously wounded man. JAMA. 1951;145(4):193–200.
Jennings CE. The intra-venous injection of fluid for severe hæmorrhage. The Lancet. 1882;120(3081):436–7.
Jennings CE. The intra-venous injection of fluid for severe haemorrhage. The Lancet. 1883;121(3102):228–9.
Pye-Smith RJ. Sheffield public hospital and dispensary: five cases of intravenous injection of saline fluid for hæmorrhage and collapse. The Lancet. 1892;139(3582):913–5.
Schmidt PJ. Transfusion in America in the eighteenth and nineteenth centuries. N Engl J Med. 1968;279(24):1319–20.
Fraser J, Cowell EM. Clinical study of blood pressure in wound conditions. JAMA. 1918;70
Spinella PC. Warm fresh whole blood transfusion for severe hemorrhage: US military and potential civilian applications. Crit Care Med. 2008;36(7):S340–5.
Hess JR, Thomas MJ. Blood use in war and disaster: lessons from the past century. Transfusion. 2003;43(11):1622–33.
Beecher HK. Preparation of battle casualties for surgery. Ann Surg. 1945;121(6):769–92.
Beecher HK. Resuscitation, and anesthesia for wounded men, the management of traumatic shock. Springfield. Charles C: Thomas; 1949.
Giangrande PL. The history of blood transfusion. Br J Haematol. 2000;100:758–67.
Robertson OH. Transfusion with preserved red blood cells. Br Med J. 1918;1(2999):691.
Cannon, Walter B. Traumatic Shock. New York: D. Appl Ther 1923.
Fogelman MJ, Wilson BJA. different concept of volume replacement in traumatic hypovolemia observations on injured man and animal. Am J Surg. 1960;99(5):694–701.
Shires T, Williams J, Brown F. Acute change in extracellular fluids associated with major surgical procedures. Ann Surg. 1961;154:803–10.
Shires T, Jackson DE. Postoperative salt tolerance. Arch Surg. 1962;84:703–6. PMID: 13912108
Wolfman EF, Neill SA, Heaps DK, Zuidema GD. Donor blood and isotonic salt solution. Effect on survival after hemorrhagic shock and operation. Arch Surg. 1963;86:869–73.
Shires T, Coln D, Carrico J, Lightfoot S. Fluid therapy in hemorrhagic shock. Arch Surg. 1964;88:688–93.
McClelland RN, Shires GT, Baxter CR, Coln CD, Carrico J. Balanced salt solution in the treatment of hemorrhagic shock. JAMA. 1967;199:830–4.
Carrico CJ, Canizaro PC, Shires GT. Fluid resuscitation following injury: rationale for the use of balanced salt solutions. Crit Care Med. 1976;4(2):46–54.
Davidsohn I. Speculation on future use of blood or blood component therapy. JAMA. 1967;202(10):970–2.
Chaplin H Jr. Packed red blood cells. N Engl J Med. 1969;281(7):364–7.
Committee AMA. on Transfusion and Transplantation. Something old, something new. JAMA. 1970;212(1):147.
Westphal RG. Rational alternatives to the use of whole blood. Ann Intern Med. 1972;76(6):987–90.
Moore FD, Shires G. Moderation. Ann Surg. 1967;166:300–1.
Moore FD. Should blood be whole or in parts? N Engl J Med. 1969;280(6):327–8.
Kashuk JL, Moore EE, Millikan JS, Moore JB. Major Abdominal Vascular Trauma-A Unified Approach. Journal of Trauma and Acute Care Surgery. 1982 Aug 1;22(8):672–9. RJ Lowe in DiscussionKashuk JL, Moore EE, Millikan JS, Moore JB Major abdominal vascular trauma--a unified approach J Trauma 2008;65:261-270 RJ Lowe in Discussion
Counts RB, Haisch C, Simon TL, Maxwell NG, Heimbach DM, Carrico CJ. Hemostasis in massively transfused trauma patients. Ann Surg. 1979;190(1):91–9.
Shackford SR, Virgilio RW, Peters RM. Whole blood versus packed-cell transfusions: a physiologic comparison. Ann Surg. 1981;193(3):337–40.
Lucas CE, Ledgerwood AM. Clinical significance of altered coagulation tests after massive transfusion for trauma. Am Surg. 1981;47(3):125–30.
Reed RL 2nd, Ciavarella D, Heimbach DM, Baron L, Pavlin E, Counts RB, Carrico CJ. Prophylactic platelet administration during massive transfusion. A prospective, randomized, double-blind clinical study. Ann Surg. 1986;203:40–8.
Bland R, Shoemaker WC, Shabot MM. Physiologic monitoring goals for the critically ill patient. Surg Gynecol Obstet. 1978;147(6):833–41.
Shoemaker WC, Appel PL, Kram HB, Waxman K, Lee TS. Prospective trial of supranormal values of survivors as therapeutic goals in high-risk surgical patients. Chest J. 1988;94(6):1176–86.
Fleming A, Bishop M, Shoemaker W, Appel P, Sufficool W, Kuvhenguwha A, Kennedy F, Wo CJ. Prospective trial of supranormal values as goals of resuscitation in severe trauma. Arch Surg. 1992;127:1175–9. Discussion 1179-1181
Bishop MH, Wo CCJ, Appel PL, et al. Relationship between supranormal circulatory values, time delays, and outcome in severely traumatized patients. Crit Care Med. 1993;21:56–60.
Boyd O, Grounds RM, Bennett ED. A randomized clinical trial of the effect of deliberate perioperative increase of oxygen delivery on mortality in high-risk surgical patients. JAMA. 1993;270(22):2699–707.
Bishop MH, Shoemaker WC, Appel PL, Meade P, Ordog GJ, Wasserberger J, Wo CJ, Rimle DA, Kram HB, Umali R. Prospective, randomized trial of survivor values of cardiac index, oxygen delivery, and oxygen consumption as resuscitation endpoints in severe trauma. J Trauma. 1995;38(5):780–7.
Gattinoni L, Brazzi L, Pelosi P, Latini R, Tognoni G, Pesenti A, Fumagalli RA. trial of goal-oriented hemodynamic therapy in critically ill patients. N Engl J Med. 1995;333(16):1025–32.
Velmahos GC, Demetriades D, Shoemaker WC, Chan LS, Tatevossian R, Wo CC, Vassiliu P, Cornwell EE III, Murray JA, Roth B, Belzberg H. Endpoints of resuscitation of critically injured patients: normal or supranormal?: a prospective randomized trial. Ann Surg. 2000;232(3):409–18.
Lee L, Moore EE, Hansen KC, Silliman CC, Chandler JG, Banerjee A. It’s not your grandfather’s field plasma. Surgery. 2013;153(6):857–60.
Spinella PC, Pidcoke HF, Strandenes G, Hervig T, Fisher A, Jenkins D, Yazer M, Stubbs J, Murdock A, Sailliol A, Ness PM. Whole blood for hemostatic resuscitation of major bleeding. Transfusion. 2016;56(S2):S190–202.
Brandstrup B, Tønnesen H, Beier-Holgersen R, Hjortsø E, Ørding H, Lindorff-Larsen K, Rasmussen MS, Lanng C, Wallin L, Iversen LH, Gramkow CS. Effects of intravenous fluid restriction on postoperative complications: comparison of two perioperative fluid regimens: a randomized assessor-blinded multicenter trial. Ann Surg. 2003;238(5):641.
Balogh Z, McKinley BA, Cocanour CS, Kozar RA, Valdivia A, Sailors RM, Moore FA. Supranormal trauma resuscitation causes more cases of abdominal compartment syndrome. Arch Surg. 2003;138:637–42.
Simmons RL, Collins JA, Heisterkamp CA 3rd, Mills DE, Andren R, Phillips LL. Coagulation disorders in combat casualties, I: acute changes after wounding. Ann Surg 1969;169(4):455–482.
MacLeod JB, Lynn M, McKenney MG, Cohn SM, Murtha M. Early coagulopathy predicts mortality in trauma. J Trauma. 2003;55(1):39–44.
Brohi K, Singh J, Heron M, Coats T. Acute traumatic coagulopathy. J Trauma. 2003;54:1127–30.
Niles SE, McLaughlin DF, Perkins JG, Wade CE, Li Y, Spinella PC, Holcomb JB. Increased mortality associated with the early coagulopathy of trauma in combat casualties. J Trauma Injury Infect Crit Care. 2008;64(6):1459–63. discussion 1463-5
Gunter OL Jr, BK A, Isbell JM, Mowery NT, Young PP, Cotton BA. Optimizing outcomes in damage control resuscitation: identifying blood product ratios associated with improved survival. J Trauma Injury Infect Crit Care. 2008;65(3):527–34.
Pidcoke HF, Aden JK, Mora AG, Borgman MA, Spinella PC, Dubick MA, Blackbourne LH, Cap AP. Ten-year analysis of transfusion in Operation Iraqi Freedom and Operation Enduring Freedom: increased plasma and platelet use correlates with improved survival. J Trauma Acute Care Surg. 2012;73(6):S445–52.
Mabry RL, Holcomb JB, Baker AM, Cloonan CC, Uhorchak JM, Perkins DE, Canfield AJ, Hagmann JH. United States army rangers in Somalia: an analysis of combat casualties on an urban battlefield. J Trauma Acute Care Surg. 2000;49(3):515–29.
Borgman MA, Spinella PC, Perkins JG, Grathwohl KW, Repine T, Beekley AC, Sebesta J, Jenkins D, Wade CE, Holcomb JB. The ratio of blood products transfused affects mortality in patients receiving massive transfusions at a combat support hospital. J Trauma. 2007;63(4):805–13.
Holcomb JB, Jenkins D, Rhee P, Johannigman J, Mahoney P, Mehta S, Cox ED, Gehrke MJ, Beilman GJ, Schreiber M, Flaherty SF. Damage control resuscitation: directly addressing the early coagulopathy of trauma. J Trauma Acute Care Surg. 2007;62(2):307–10.
Maegele M, Lefering R, Yucel N, Tjardes T, Rixen D, Paffrath T, Simanski C, Neugebauer E, Bouillon B. AG Polytrauma of the German Trauma Society (DGU). Early coagulopathy in multiple injury: an analysis from the German Trauma Registry on 8724 patients. Injury. 2007;38:298.
Tieu BH, Holcomb JB, Schreiber MA. Coagulopathy: its pathophysiology and treatment in the injured patient. World J Surg. 2007;31:1055–64.
Cotton BA, Au BK, Nunez TC, Gunter OL, Robertson AM, Young PP. Predefined massive transfusion protocols are associated with a reduction in organ failure and postinjury complications. J Trauma. 2009;66:41–8. discussion 48-49
Shah SK, Uray KS, Stewart RH, Laine GA, Cox CS. Resuscitation-induced intestinal edema and related dysfunction: state of the science. J Surg Res. 2011;166(1):120–30.
Duchesne JC, Kimonis K, Marr AB, Rennie KV, Wahl G, Wells JE, Islam TM, Meade P, Stuke L, Barbeau JM, Hunt JP, Baker CC, NE MS Jr. Damage control resuscitation in combination with damage control laparotomy: a survival advantage. J Trauma. 2010;69:46–52.
Feinman M, Cotton BA, Haut ER. Optimal fluid resuscitation in trauma: type, timing, and total. Curr Opin Crit Care. 2014;20(4):366–72.
Cotton BA, Reddy N, Hatch QM, LeFebvre E, Wade CE, Kozar RA, Gill BS, Albarado R, McNutt MK, Holcomb JB. Damage control resuscitation is associated with a reduction in resuscitation volumes and improvement in survival in 390 damage control laparotomy patients. Ann Surg. 2011;254(4):598–605.
Myburgh JA, Mythen MG. Resuscitation fluids. N Engl J Med. 2013;369:1243–51.
Lobo DN, Bostock KA, Neal KR, Perkins AC, Rowlands BJ, Allison SP. Effect of salt and water balance on recovery of gastrointestinal function after elective colonic resection: a randomized control trial. Lancet. 2002;359:1812–8.
Balogh Z, McKinley BA, Cocanour CS, Kozar RA, Holcomb JB, Ware DN, Moore FA. Secondary abdominal compartment syndrome is an elusive early complication of traumatic shock resuscitation. Am J Surg. 2002;184(6):538–43. discussion 543-4
Cotton BA, Guy JS, Morris JA Jr, Abumrad NA. The cellular, metabolic, and systemic consequences of aggressive fluid resuscitation strategies. Shock. 2006;26:115–21.
Ley EJ, Clond MA, Srour MK, Barnajian M, Mirocha J, Margulies DR, Salim A. Emergency department crystalloid resuscitation of 1.5 L or more is associated with increased mortality in elderly and nonelderly trauma patients. J Trauma. 2011;70:398–400.
Hatch QM, Osterhout LM, Podbielski J, Kozar RA, Wade CE, Holcomb JB, Cotton BA. Impact of closure at the first take back: complication burden and potential overutilization of damage control laparotomy. J Trauma. 2011;71(6):1503–11.
Schnüriger B, Inaba K, Wu T, Eberle BM, Belzberg H, Demetriades D. Crystalloids after primary colon resection and anastomosis at initial trauma laparotomy: excessive volumes are associated with anastomotic leakage. J Trauma Acute Care Surg. 2011;70(3):603–10.
Spinella PC, Perkins JG, Grathwohl KW, Repine T, Beekley AC, Sebesta J, Jenkins D, Azarow K, Holcomb JB. 31st CSH Research Working Group. Fresh whole blood transfusions in coalition military, foreign national, and enemy combatant patients during Operation Iraqi Freedom at a US combat support hospital. World J Surg. 2008;32(1):2–6.
Cotton BA, Harvin JA, Kostousouv V, Minei KM, Radwan ZA, Schöchl H, Wade CE, Holcomb JB, Matijevic N. Hyperfibrinolysis at admission is an uncommon but highly lethal event associated with shock and prehospital fluid administration. J Trauma Acute Care Surg. 2012;73(2):365–70. discussion 370
Duchesne JC, Heaney J, Guidry C, McSwain N Jr, Meade P, Cohen M, Schreiber M, Inaba K, Skiada D, Demetriades D, Holcomb J. Diluting the benefits of hemostatic resuscitation: a multi-institutional analysis. J Trauma Acute Care Surg. 2013;75(1):76–82.
Shrestha B, Holcomb JB, Camp EA, Del Junco DJ, Cotton BA, Albarado R, Gill BS, Kozar RA, Kao LS, McNutt MK, Moore LJ, Love JD, Tyson GH 3rd, Adams PR, Khan S, Wade CE. Damage-control resuscitation increases successful nonoperative management rates and survival after severe blunt liver injury. J Trauma Acute Care Surg. 2015;78(2):336–41.
Spinella PC, Perkins JG, Grathwohl KW, Beekley AC, Niles SE, McLaughlin DF, Wade CE, Holcomb JB. Effect of plasma and red blood cell transfusions on survival in patients with combat related traumatic injuries. J Trauma. 2008;64(2 Suppl):S69–77. discussion S77–8
Holcomb JB, Wade CE, Michalek JE, Chisholm GB, Zarzabal LA, Schreiber MA, Gonzalez EA, Pomper GJ, Perkins JG, Spinella PC, Williams KL, Park MS. Increased plasma and platelet to red blood cell ratios improves outcome in 466 massively transfused civilian trauma patients. Ann Surg. 2008;248(3):447–58.
Duchesne JC, Hunt JP, Wahl G, Marr AB, Wang YZ, Weintraub SE, Wright MJ, McSwain NE Jr. Review of current blood transfusions strategies in a mature level I trauma center: were we wrong for the last 60 years. J Trauma. 2008;65:272–6. Discussion 276-278
Maegele M, Lefering R, Paffrath T, Tjardes T, Simanski C, Bouillon B. Working Group on Polytrauma of the German Society of Trauma Surgery (DGU). Red-blood-cell to plasma ratios transfused during massive transfusion are associated with mortality in severe multiple injury: a retrospective analysis from the Trauma Registry of the Deutsche Gesellschaft für Unfallchirurgie. Vox Sang. 2008;95(2):112–9.
Sperry JL, Ochoa JB, Gunn SR, Alarcon LH, Minei JP, Cuschieri J, Rosengart MR, Maier RV, Billiar TR, Peitzman AB, Moore EE. Inflammation the host response to injury investigators. An FFP:PRBC transfusion ratio >/=1:1.5 is associated with a lower risk of mortality after massive transfusion. J Trauma. 2008;65:986.
Teixeira PG, Inaba K, Shulman I, Salim A, Demetriades D, Brown C, Browder T, Green D, Rhee P. Impact of plasma transfusion in massively transfused trauma patients. J Trauma Injury Infect Crit Care. 2009;66(3):693–7.
Brown LM, Aro SO, Cohen MJ, Trauma Outcomes Group, Holcomb JB, Wade CE, Brasel KJ, Vercruysse G, MacLeod J, Dutton RP, Hess JR, Duchesne JC, NE MS, Muskat P, Johannigamn J, Cryer HM, Tillou A, Pittet JF, Knudson P, De Moya MA, Schreiber MA, Tieu B, Brundage S, Napolitano LM, Brunsvold M, Sihler KC, Beilman G, Peitzman AB, Zenait MS, Sperry J, Alarcon L, Croce MA, Minei JP, Kozar R, Gonzalez EA, Stewart RM, Cohn SM, Mickalek JE, Bulger EM, Cotton BA, Nunez TC, Ivatury R, Meredith JW, Miller P, Pomper GJ, Marin B. A high fresh frozen plasma: packed red blood cell transfusion ratio decreases mortality in all massively transfused trauma patients regardless of admission international normalized ratio. J Trauma. 2011;71(2 Suppl 3):S358–63.
Rowell SE, Barbosa RR, Diggs BS, Schreiber MA, Trauma Outcomes Group, Holcomb JB, Wade CE, Brasel KJ, Vercruysse G, MacLeod J, Dutton RP, Hess JR, Duchesne JC, NE MS, Muskat P, Johannigamn J, Cryer HM, Tillou A, Cohen MJ, Pittet JF, Knudson P, De Moya MA, Schreiber MA, Tieu B, Brundage S, Napolitano LM, Brunsvold M, Sihler KC, Beilman G, Peitzman AB, Zenait MS, Sperry J, Alarcon L, Croce MA, Minei JP, Kozar R, Gonzalez EA, Stewart RM, Cohn SM, Mickalek JE, Bulger EM, Cotton BA, Nunez TC, Ivatury R, Meredith JW, Miller P, Pomper GJ, Marin B. Effect of high product ratio massive transfusion on mortality in blunt and penetrating trauma patients. J Trauma. 2011;71(2 Suppl 3):S353–7.
Perkins JG, Cap AP, Spinella PC, Blackbourne LH, Grathwohl KW, Repine TB, Ketchum L, Waterman P, Lee RE, Beekley AC, Sebesta JA, Shorr AF, Wade CE, Holcomb JB. An evaluation of the impact of apheresis platelets used in the setting of massively transfused trauma patients. J Trauma. 2009;66:S77–85.
Zink KA, Sambasivan CN, Holcomb JB, Chisholm G, Schreiber MA. A high ratio of plasma and platelets to packed red blood cells in the first 6 hours of massive transfusion improves outcomes in a large multicenter study. Am J Surg. 2009;197(5):565–70. discussion 570
Inaba K, Branco BC, Rhee P, Blackbourne LH, Holcomb JB, Teixeira PG, Shulman I, Nelson J, Demetriades D. Impact of plasma transfusion in trauma patients who do not require massive transfusion. J Am Coll Surg. 2010;210(6):957–65.
Holcomb JB, Zarzabal LA, Michalek JE, Kozar RA, Spinella PC, Perkins JG, Matijevic N, Dong JF, Pati S, Wade CE, Trauma Outcomes Group, Holcomb JB, Wade CE, Cotton BA, Kozar RA, Brasel KJ, Vercruysse GA, JB ML, Dutton RP, Hess JR, Duchesne JC, NE MS, Muskat PC, Johannigamn JA, Cryer HM, Tillou A, Cohen MJ, Pittet JF, Knudson P, MA DM, Schreiber MA, Tieu BH, Brundage SI, Napolitano LM, Brunsvold ME, Sihler KC, Beilman GJ, Peitzman AB, Zenati MS, Sperry JL, Alarcon LH, Croce MA, Minei JP, Steward RM, Cohn SM, Michalek JE, Bulger EM, Nunez TC, Ivatury RR, Meredith JW, Miller PR, Pomper GJ, Marin B. Increased platelet:RBC ratios are associated with improved survival after massive transfusion. J Trauma. 2011;71(2 Suppl 3):S318–28.
Holcomb JB, del Junco DJ, Fox EE, Wade CE, Cohen MJ, Schreiber MA, Alarcon LH, Bai Y, Brasel KJ, Bulger EM, Cotton BA, Matijevic N, Muskat P, Myers JG, Phelan HA, White CE, Zhang J, Rahbar MH, PROMMTT Study Group. The prospective, observational, multicenter, major trauma transfusion (PROMMTT) study: comparative effectiveness of a time-varying treatment with competing risks. JAMA Surg. 201;148(2):127–36.
Malone DL, Hess JR, Fingerhut A. Massive transfusion practices around the globe and a suggestion for a common massive transfusion protocol. J Trauma. 2006;60(6 Suppl):S91–6.
Hess JR, Holcomb JB. Resuscitating properly. Transfusion. 2015;55(6):1362–4.
Treml AB, Gorlin JB, Dutton RP, Scavone BM. Massive transfusion protocols: a survey of academic medical centers in the United States. Anesth Anal. 2017;124(1):277–81.
Snyder CW, Weinberg JA, Jr MGG, Melton SM, George RL, Reiff DA, Cross JM, Hubbard-Brown J, Rue LW 3rd, Kerby JD. The relationship of blood product ratio to mortality: survival benefit or survival bias. J Trauma Injury Infect. Crit Care. 2009;66(2):358–62.
Zielinski MD, Johnson PM, Jenkins D, Goussous N, Stubbs JR. Emergency use of prethawed Group A plasma in trauma patients. J Trauma Acute Care Surg. 2013;74(1):69–75.
Matijevic N, Wang YW, Cotton BA, Hartwell E, Barbeau JM, Wade CE, Holcomb JB. Better hemostatic profiles of never-frozen liquid plasma compared with thawed fresh frozen plasma. J Trauma Acute Care Surg. 2013;74(1):84–90. discussion 90-1
Radwan ZA, Bai Y, Matijevic N, del Junco DJ, McCarthy JJ, Wade CE, Holcomb JB, Cotton BA. An emergency department thawed plasma protocol for severely injured patients. JAMA Surg. 2013;148(2):170–5.
Holcomb JB, Pati S. Optimal trauma resuscitation with plasma as the primary resuscitative fluid: the surgeon's perspective. Hematology Am Soc Hematol Educ Program. 2013;2013:656–9.
Norii T, Crandall C, Terasaka Y. Survival of severe blunt trauma patients treated with resuscitative endovascular balloon occlusion of the aorta compared with propensity score-adjusted untreated patients. J Trauma Acute Care Surg. 2015;78(4):721–8.
Ho AM, Zamora JE, Holcomb JB, Ng CS, Karmakar MK, Dion PW. The many faces of survivor bias in observational studies on trauma resuscitation requiring massive transfusion. Ann Emerg Med. 2015;66(1):45–8.
Holcomb JB, Tilley BC, Baraniuk S, Fox EE, Wade CE, Podbielski JM, del Junco DJ, Brasel KJ, Bulger EM, Callcut RA, Cohen MJ, Cotton BA, Fabian TC, Inaba K, Kerby JD, Muskat P, O’Keeffe T, Rizoli S, Robinson BR, Scalea TM, Schreiber MA, Stein DM, Weinberg JA, Callum JL, Hess JR, Matijevic N, Miller CN, Pittet JF, Hoyt DB, Pearson GD, Leroux B, van Belle G, PROPPR Study Group. Transfusion of plasma, platelets, and red blood cells in a 1:1:1 vs a 1:1:2 ratio and mortality in patients with severe trauma: the PROPPR randomized clinical trial. JAMA. 2015;313(5):471–82.
Demetriades D, Kimbrell B, Salim A, Velmahos G, Rhee P, Preston C, Gruzinski G, Chan L. Trauma deaths in a mature urban trauma system: is “trimodal” distribution a valid concept? J Am Coll Surg. 2005;201(3):343–8.
Oyeniyi BT, Fox EE, Scerbo M, Tomasek JS, Wade CE, Holcomb JB. Trends in 1029 trauma deaths at a level 1 trauma center: Impact of a bleeding control bundle of care. Injury. 2016;3
Fox EE, Holcomb JB, Wade CE, Bulger EM, Tilley BC. On behalf of the PROPPR study group. Earlier endpoints are required for hemorrhagic shock trials among severely injured patients. Shock. [Submitted for publication].
Kauvar DS, Holcomb JB, Norris GC, Hess JR. Fresh whole blood transfusion: a controversial military practice. J Trauma. 2006;61(1):181–4.
Murdock AD, BersÈus O, Hervig T, Strandenes G, Lunde TH. Whole blood: the future of traumatic hemorrhagic shock resuscitation. Shock. 2014;41:62–9.
Spinella PC, Perkins JG, Grathwohl KW, Beekley AC, Holcomb JB. Warm fresh whole blood is independently associated with improved survival for patients with combat-related traumatic injuries. J Trauma Injury Infect Crit Care. 2009;66(4 Suppl):S69–76.
Holcomb JB, Spinella PC. Optimal use of blood in trauma patients. Biologicals. 2010;38(1):72–7.
Repine TB, Perkins JG, Kauvar DS, Blackborne L. The use of fresh whole blood in massive transfusion. J Trauma Injury Infect Crit Care. 2006;60(6 suppl):S59–69.
Kowalenko T, Stern S, Dronen S, Wang X. Improved outcome with hypotensive resuscitation of uncontrolled hemorrhagic shock in a swine model. J Trauma Acute Care Surg. 1992;33(3):349–53.
Burris D, Rhee P, Kaufmann C, Pikoulis E, Austin B, Eror A, DeBraux S, Guzzi L, Leppäniemi A. Controlled resuscitation for uncontrolled hemorrhagic shock. J Trauma. 1999;46:216–23.
Holmes JF, Sakles JC, Lewis G, Wisner DH. Effects of delaying fluid resuscitation on an injury to the systemic arterial vasculature. Acad Emerg Med. 2002;9:267–74.
Holcomb JB. Fluid resuscitation in modern combat casualty care: lessons learned from Somalia. J Trauma. 2003;54(5 Suppl):S46–51. Review
Sondeen JL, Coppes VG, Holcomb JB. Blood pressure at which rebleeding occurs after resuscitation in swine with aortic injury. J Trauma Injury Infect. Crit Care. 2003;54(5 suppl):S110–7.
Bickell WH, Wall MJ Jr, Pepe PE, Martin RR, Ginger VF, Allen MK, Mattox KL. Immediate versus delayed fluid resuscitation for hypotensive patients with penetrating torso injuries. N Engl J Med. 1994;331(17):1105–9.
Wall MJ Jr, Granchi TS, Liscum K, Aucar J, Mattox KL. Delayed versus immediate fluid resuscitation in patients with penetrating trauma: subgroup analysis. J Trauma. 1995;39:173.
Schreiber MA, Meier EN, Tisherman SA, Kerby JD, Newgard CD, Brasel K, Egan D, Witham W, Williams C, Daya M, Beeson J. A controlled resuscitation strategy is feasible and safe in hypotensive trauma patients: results of a prospective randomized pilot trial. J Trauma Acute Care Surg. 2015;78(4):687.
Jurkovich GJ, Greiser WB, Luterman A, Curreri PW. Hypothermia in trauma victims: an ominous predictor of survival. J Trauma. 1987;27(9):1019–24.
Ferrara A, MacArthur JD, Wright HK, Modlin IM, McMillen MA. Hypothermia and acidosis worsen coagulopathy in the patient requiring massive transfusion. Am J Surg. 1990;160:515–8.
Cosgriff NM, Ernest E, Sauaia A, Kenny-Moynihan M, Burch JM, Galloway B. Predicting life-threatening coagulopathy in the massively transfused patient: hypothermia and acidosis revisited. J Trauma Injury Infect Crit Care. 1997;42(5):857–62.
Martini WZ, Holcomb JB. Acidosis and coagulopathy: the differential effects on fibrinogen synthesis and breakdown in pigs. Ann Surg. 2007;246(5):831–5.
Hess JR, Brohi K, Dutton RP, Hauser CJ, Holcomb JB, Kluger Y, Mackway-Jones K, Parr MJ, Rizoli SB, Yukioka T, Hoyt DB, Bouillon B. The coagulopathy of trauma: a review of mechanisms. J Trauma. 2008 Oct;65(4):748–54.
Eastridge BJ, Mabry RL, Seguin P, Cantrell J, Tops T, Uribe P, Mallett O, Zubko T, Oetjen-Gerdes L, Rasmussen TE, Butler FK. Death on the battlefield (2001–2011): implications for the future of combat casualty care. J Trauma Acute Care Surg. 2012;73(6):S431–7.
Kragh JF Jr, Walters TJ, Baer DG, Fox CJ, Wade CE, Salinas J, Holcomb JB. Practical use of emergency tourniquets to stop bleeding in major limb trauma. J Trauma Acute Care Surg. 2008;64(2):S38–50.
Scerbo MH, Mumm JP, Gates K, Love JD, Wade CE, Holcomb JB, Cotton BA. Safety and appropriateness of tourniquets in 105 civilians. Prehosp Emerg Care. 2016;May 31:1–11. [Epub ahead of print]
Shina A, Lipsky AM, Nadler R, Levi M, Benov A, Ran Y, Yitzhak A, Glassberg E. Prehospital use of hemostatic dressings by the Israel Defense Forces Medical Corps: A case series of 122 patients. J Trauma Acute Care Surg. 2015;79(4):S204–9.
Inaba K, Siboni S, Resnick S, Zhu J, Wong MD, Haltmeier T, Benjamin E, Demetriades D. Tourniquet use for civilian extremity trauma. J Trauma Acute Care Surg. 2015;79(2):232–7. quiz 332-3
Moore LJ, Brenner M, Kozar RA, Pasley J, Wade CE, Baraniuk MS, Scalea T, Holcomb JB. Implementation of resuscitative endovascular balloon occlusion of the aorta as an alternative to resuscitative thoracotomy for noncompressible truncal hemorrhage. J Trauma Acute Care Surg. 2015;79(4):523–30. discussion 530-2
Morrison JJ, Galgon RE, Jansen JO, Cannon JW, Rasmussen TE, Eliason JLA. systematic review of the use of resuscitative endovascular balloon occlusion of the aorta in the management of hemorrhagic shock. J Trauma Acute Care Surg. 2016;80(2):324–34.
Spinella PC, Holcomb JB. Resuscitation and transfusion principles for traumatic hemorrhagic shock. Blood Rev. 2009;23(6):231–40.
Otton BA, Minei KM, Radwan ZA, Matijevic N, Pivalizza E, Podbielski J, Wade CE, Kozar RA, Holcomb JB. Admission rapid thrombelastography predicts development of pulmonary embolism in trauma patients. J Trauma Acute Care Surg. 2012;72(6):1470–5.
Holcomb JB, Minei KM, Scerbo ML, Radwan ZA, Wade CE, Kozar RA, Gill BS, Albarado R, McNutt MK, Khan S, Adams PR, McCarthy JJ, Cotton BA. Admission rapid thrombelastography can replace conventional coagulation tests in the emergency department: experience with 1974 consecutive trauma patients. Ann Surg. 2012;256(3):476–86.
Johansson PI, Stensballe J, Oliveri R, Wade CE, Ostrowski SR, Holcomb JB. How I treat patients with massive hemorrhage. Blood. 2014;124(20):3052–8.
Cotton BA, Faz G, Hatch QM, Radwan ZA, Podbielski J, Wade C, Kozar RA, Holcomb JB. Rapid thrombelastography delivers real-time results that predict transfusion within 1 hour of admission. J Trauma. 2011;71(2):407–14. discussion 414-7
Gonzalez E, Moore EE, Moore HB, Chapman MP, Chin TL, Ghasabyan A, Wohlauer MV, Barnett CC, Bensard DD, Biffl WL, Burlew CC, Johnson JL, Pieracci FM, Jurkovich GJ, Banerjee A, Silliman CC, Sauaia A. Goal-directed hemostatic resuscitation of trauma-induced coagulopathy: a pragmatic randomized clinical trial comparing a viscoelastic assay to conventional coagulation assays. Ann Surg. 2016;263(6):1051–9.
Moore EE, Moore HB, Gonzalez E, Sauaia A, Banerjee A, Silliman CC. Rationale for the selective administration of tranexamic acid to inhibit fibrinolysis in the severely injured patient. Transfusion. 2016;56(Suppl 2):S110–4.
CRASH-2 Trial Collaborators, Shakur H, Roberts I, Bautista R, Caballero J, Coats T, Dewan Y, El-Sayed H, Gogichaishvili T, Gupta S, Herrera J, Hunt B, Iribhogbe P, Izurieta M, Khamis H, Komolafe E, Marrero MA, Mejía-Mantilla J, Miranda J, Morales C, Olaomi O, Olldashi F, Perel P, Peto R, Ramana PV, Ravi RR, Yutthakasemsunt S. Effects of tranexamic acid on death, vascular occlusive events, and blood transfusion in trauma patients with significant haemorrhage (CRASH-2): a randomised, placebo-controlled trial. Lancet. 2010;376(9734):23–32.
CRASH-2 Collaborators, Roberts I, Shakur H, Afolabi A, Brohi K, Coats T, Dewan Y, Gando S, Guyatt G, Hunt BJ, Morales C, Perel P, Prieto-Merino D, Woolley T. The importance of early treatment with tranexamic acid in bleeding trauma patients: an exploratory analysis of the CRASH-2 randomised controlled trial. Lancet. 2011;377:1096–101.
Harvin JA, Peirce CA, Mims MM, Hudson JA, Podbielski JM, Wade CE, Holcomb JB, Cotton BA. The impact of tranexamic acid on mortality in injured patients with hyperfibrinolysis. J Trauma Acute Care Surg. 2015;78(5):905–11.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Kalkwarf, K.J., Holcomb, J.B. (2018). Evolution of Resuscitation: What Is Damage Control Resuscitation?. In: Duchesne, J., Inaba, K., Khan, M. (eds) Damage Control in Trauma Care. Springer, Cham. https://doi.org/10.1007/978-3-319-72607-6_19
Download citation
DOI: https://doi.org/10.1007/978-3-319-72607-6_19
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-72606-9
Online ISBN: 978-3-319-72607-6
eBook Packages: MedicineMedicine (R0)