Abstract
As mentioned in Chap. 3, terminal ballistics is the scientific discipline concerned with the interaction between projectiles or rounds and the objects they impact; when they impact biological tissue this study is called wound ballistics. This chapter seeks to distil the multiple, complex and interacting factors that influence gunshot wounding (GSW) into a more coherent but comprehensive and clinical-relevant text.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
-
1.
Projectiles or rounds affect tissues in casualties by three mechanisms: generation of a shockwave, formation of a temporary cavity and finally the resultant permanent cavity or wound tract.
-
2.
Wounding patterns are idiosyncratic and difficult to predict.
-
3.
Significant tissue damage can sometimes be produced by lower-energy firearms and, paradoxically, minimal wounding can sometimes be seen from higher-energy firearms.
-
4.
Fragmentation of the round and bone-strike are typically associated with greater energy transfer and therefore more severe wounds
Many of the varieties between one gun-shot wound and another, arise from the difference in the velocity of the body projected; and they are principally the following. If the velocity of the ball is small, then the mischief is less.—Sir John Hunter, 1794 [1]
5.1 Introduction
As mentioned in Chap. 2, terminal ballistics is the scientific discipline concerned with the interaction between projectiles or rounds and the objects they impact; when they impact biological tissue this study is called wound ballistics . This chapter seeks to distil the multiple, complex and interacting factors that influence gunshot wounding (GSW) into a more coherent but comprehensive and clinical-relevant text.
The behaviour of a round in flight (external ballistics) is predictable enough that a skilled sniper can consistently hit targets at distances of over a kilometre. However, the behaviour of rounds as they pass through tissue becomes idiosyncratic and extremely challenging to predict. Although still governed by Newtonian physics, wound ballistics describes a very complex set of interactions and therefore, there are few reliable rules or patterns to guide the clinician aside from gaining experience of these injuries. This chapter will examine the specifics of these interactions between projectile and tissues rather than detailed techniques of surgical management of such wounds.
Reduced to its fundamental form for the clinical context, wound ballistics concerns the work done by the transfer of kinetic energy (KE) from the round leading to crushing, lacerating, stretching and shearing of the tissues [2]. The KE transferred into tissues is simply the difference between the KE of the round as it strikes the body and that which remains should it exit the tissues. If the round does not exit the tissues, all of its KE will be transferred into the body.
There are three specific mechanisms that will be addressed which allow this transfer of energy to occur: The shockwave preceding the round; the temporary cavity formed in the wake of the round and finally the permanent cavity or wound tract left in the tissue [3].
5.2 Shockwave
This is an area of controversy within ballistic literature as the significance of this component is not fully understood [4, 5]. It has long been recognised that when a projectile strikes tissue, a tiny region of very high pressure is generated. This propagates through the tissue slightly faster than the speed of sound in water (1434 ms−1), and therefore ahead of the projectile with a duration of 15–25 μs [6]. Whether or not this subsequently has any significant clinical effect on tissues is disputed: some investigators, particularly those examining actual shootings and animal models, believe a significant degree of the observed effect of GSW can be attributed to the shockwave [7, 8]. There is also a belief amongst some investigators that neural tissue might be particularly sensitive to the shockwave [7, 9]. However, others discount the wounding potential of the shockwave and regard it as insignificant or even non-existent when compared to the damage created by the temporary and permanent cavity [10] (Fig. 5.1).
5.3 Temporary Cavity
The temporary cavity is the stretching of the tissue radially away from the path of the round, and occurs in its wake as it passes through tissue [11]. When the projectile strikes the tissue it is subjected to a significant increase in retardant forces from the increased drag and is decelerated [12]. This deceleration involves the rapid transfer of KE from the round into the surrounding causing those tissues to radially accelerate away from the path of the round [13]. The process takes place over milliseconds as it must overcome the inertia of the tissues, hence occurs, and continues, after passage of the round. As the tissues accelerate away from the passage of the round, a temporary space or cavity at sub-atmospheric pressure is formed, creating a vacuum which potentially draws air and surface contaminants into the cavity via the entrance (or exit) wound [14, 15]. As the tissues are stretched, those tissues which stretch beyond their capacity to absorb such deformation will tear or fracture [3].
Ultimately, once balance between the radial acceleration of the tissue and the energy the tissue absorbs as it is deformed is reached, the temporary cavity will cease its expansion and collapse back in on itself; it will then expand again, albeit with less available energy. This is visible within modelling as an oscillating or pulsating wave of expansion and collapse which continues over milliseconds until all of the available transferred energy is completely dissipated even when a projectile has left the body [6].
The size of the temporary cavity formed is proportional to the amount of energy delivered. It is important to recognise that cavitation does not occur equally throughout the wound tract: it will be larger wherever the contact surface area of the round is greater, allowing for that greater delivery of KE, such as if the round becomes unstable or fragments as described in greater detail in Sect. 5.6.1 below.
5.4 Permanent Cavity
The round crushes, cuts and shears tissue as it passes through the casualty creating a tract that is typically of a similar size to that of the contact area of the projectile. The permanent cavity is typically a continuation of the trajectory of the projectile though it must be remembered that this trajectory can be deflected by tissue planes, bone strike or otherwise from the instability of the round itself as it traverses the tissues [16]. The entrance wound will usually be predictably minimal in size if the round strikes the body nose first, whereas the exit wound can be more variable; a large exit wound tends to only be present if significant temporary cavitation occurs at the point where the projectile leaves the body [17].
If a round fragments, which can occur either in soft tissue or after bone strike, then each fragment will subsequently continue passage to create a permanent cavity and possibly even a generate a temporary cavity, if the fragments possess enough energy, dramatically increasing the volume of tissue damage in the wound [17, 18].
With regard to the weapon systems and calibres of ammunition available, the number of variables make it difficult for a clinician to predict the injury pattern of a GSW as a casualty arrives; however, lower energy handgun projectiles (e.g. 9 × 19 mm), travelling at lower velocities typically only produce a minimal temporary cavity and may not exit the body [17]. GSWs produced by these rounds usually involve damage limited to structures and organs lying in the path of the projectile. Therefore, in ‘through and through’ injuries, where both entry and exit wounds exist, the structures damaged can be predicted with a fair degree of accuracy where the path of the round is known [19, 20]. However it is important to recognise that higher energy handgun rounds can sometimes form a more significant or clinically relevant temporary cavity: where the round has not been recovered, or the weapon type is unknown, it is perilous to assume that damage from cavitation will not have been caused where the entrance and exit wounds appear minimal as this can mask catastrophic internal tissue injury.
It should also be remembered that paradoxically the higher energy round of a larger calibre (e.g. 7.62 × 39 mm) which passes “through and through” the tissues over a short distance may cause minimal damage; whereas in converse, the lower energy round of a lower calibre (e.g. again, 9 × 19 mm) which does not exit the tissues will dump its entire energy load causing potentially far more devastation to structures by comparison [10].
5.5 Anatomic Injury Patterns
When considering the effect of GSW, it is important to differentiate the anatomic effect and the functional effect of the injury. A high-energy transfer wound to the thigh might involve a relatively large amount of tissue, but if no significant vessels are damaged and the femur is preserved from fracture, the damage may be relatively minimal where, as previously mentioned, muscle tissue is able to tolerate significant deformity and stretch from temporary cavitation without significant injury. Conversely, far less anatomic disruption involving the Central Nervous System (CNS) or the heart and great vessels can be rapidly fatal.
This is evident when one looks at the anatomic distribution of injuries in armed conflict as shown in Table 5.1 below. It is important to remember that military personnel are normally wearing body armour, and therefore will sustain proportionally fewer injuries to their chest and head than unprotected civilian casualties. However, the small proportion of survivors with chest and head injuries relative to those with limb injuries gives some measure of the likely preponderance of extremity injury in a civilian mass-shooting event.
5.6 Tissue Injury Patterns
Chapter 2 described how a round is slowed down by the effect of drag, and that this is quantified by the following formula:
where Fd is the drag force acting to slow the bullet, Cd is the drag coefficient, ρ is the mass density of the gas or liquid the bullet is passing through, v is the velocity of the projectile, and A is the cross-sectional surface area of the projectile.
The greater the Fd, then the greater the rate of transfer of kinetic energy (KE) is from the round (or fragment) into the tissue. It is important to note that the cross sectional area presented by the round and the density of the tissue it is traversing is proportional to the drag force and therefore the energy transfer [3, 21]. Specific gravity values of different tissues are shown below in Table 5.2. This lead to the conclusion that if the round directly strikes tissue of higher density, it will likely cause more damage e.g. a direct strike to bone will cause more damage than a direct strike to lung tissue.
This helps explain the earlier observation that wound severity is increased with the following factors:
-
Tumbling or fragmentation of the round
-
Bone Strike
Conversely, if a round traverses a limb without fragmenting or striking a bone then very little energy may be transferred into the tissue. Skeletal muscle is resilient to the stretching seen with temporary cavitation and while some tissue will be crushed in the formation of the permanent cavity, overall the wound may be minor with little tissue necrosis and require only limited surgical intervention [23,24,25].
5.6.1 Tumbling and Fragmentation
As described in Chap. 2, military rounds are designed to resist drag. The effect of the tissue on the round increases drag, however if the round tumbles or fragments, drag is dramatically increased and therefore so is the energy transfer. This explains why temporary cavities are at their greatest at the point in the wound tract where the round tumbles [17] as shown schematically in Fig. 5.2 below.
A gyroscopically stable, high-ogive (“sharper” nose or Spitzer) round will pass through tissue for some distance without significant yaw away from its central axis, thus will likely exit the body with much of its kinetic energy retained [26]. Conversely, an unstable, low-ogive (“blunter” nose), expanding or fragmenting round, will strike tissues with an increased contact surface area, allowing transfer of a proportionally larger amount of energy. As the projectile passes through tissue, the torque or spin conferred upon it by the rifling is slowed (for those rounds fired from an appropriately rifled weapon system), further reducing its stability and increasing the opportunity for yaw away from the central axis. The drag coefficient is also increased, and the resultant rapid deceleration also leads to the round being subjected to bending and stressing which can result in fragmentation of the round [3].
Finally, it is worth remembering that many modern rifle rounds are designed such that the centre of mass lies further towards the tail than the nose, so as stability is lost once it enters tissues (or even before it enters the body), it can mean the round will reverse its orientation by 180° or even 360° during its forward passage, otherwise known as tumbling [11, 27]. If the penetration distance through tissue is sufficient, or if the projectile strikes tissue of higher density, such as bone, it is likely that the bullet will yaw significantly and may begin to tumble unpredictably, such as when its long axis is at 90° to its trajectory; as previously mentioned, the rate of energy transfer and cavitation is greatest due to the maximal surface area being in contact with tissues.
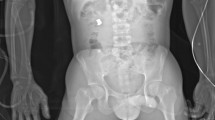
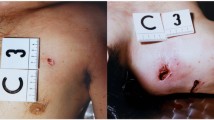
When the round fragments, there is an overall increased surface area of the projectile in contact with the tissues; as such the components are subject to considerably greater drag so, again, there is greater energy transfer and tissue damage. This is shown in the clinical photograph and radiograph shown in Fig. 5.3 above.
Radiograph and clinical photograph of a casualty injured by a negligent discharge of a 5.56 × 45 mm round at close range. The round has fragmented as shown in the CT scouting image as it traversed across both legs, causing excessive soft tissue damage shown in the clinical photograph taken after the first surgical episode. © 2017 Crown Copyright
If initial radiographs demonstrate round fragmentation, then it should be assumed that there is significant energy transfer and therefore significant soft tissue damage [28, 29].
5.6.2 Tissue Density
Whilst specific gravities of different tissues were examined earlier, it is now important to consider the clinical implications. The tissue that presents the greatest resistance to the passage of a round is bone. If a round strikes bone, there is normally rapid slowing of the round and therefore energy transfer and tissue damage. A strike to a long bone shaft appears to result in a fracture with significant comminution [22]. Figure 5.4 above demonstrates the significant energy transfer when a high energy round strikes a long bone.
Radiograph and clinical photograph illustrating a gun-shot wound in which the round has struck the tibia causing a multi-fragmentary fracture associated with significant energy transfer and soft-tissue damage as shown in the clinical photograph. This photograph was taken as part of the assessment in the operating theatre prior to the second. © 2017 Crown Copyright
When lower energy weapons such as handguns are used, there is a higher proportion of incomplete fracture seen [30]. Whilst comminution occurs at a higher rate in high energy GSWs, incomplete fracture can also be seen with higher energy rounds in areas of bone that are more cancellous in nature appear to undergo “drilling” as the round passes through with little apparent damage away from the passage of the round, leaving a ‘drilled-out’ permanent wound tract [22] as shown in Fig. 5.5 below.
Radiograph, CT image and clinical photographs showing a gun-shot wound to the heel with a low-energy open fracture of the calcaneum. There has been little energy transferred and the wound healed without complication only requiring superficial scrubbing of the entry and exit wounds and irrigation with saline. © 2017 Crown Copyright
When considering tissue of less density, lung tissue is at the opposite end of the tissue density spectrum from bone and therefore offers little drag to rounds as they pass through the lungs. Lung parenchyma is also is an elastic tissue, which can tolerate the stretch that occurs with the formation of a temporary cavity [31] However, if a round strikes a rib as it either enters or exits the chest, there can be significant energy transfer as the round is destabilised, fragments or accelerates splinters of rib bone as shown in Fig. 5.6 below.
Conclusion
This chapter has examined the mechanisms by which a projectile transfers energy into the tissue following gunshot and the resultant effect in terms of the wounds that are created. The mechanisms of wounding have been discussed with particular focus on the creation of temporary and permanent cavities.
The typical features of wounds with higher energy transfer and therefore more severe wounds i.e. round fragmentation and bone-strike have been explained with clinical examples.
References
Hunter JFRS, Home ESB. A Treatise on the Blood, inflammation, and gunshot wounds, … to which is prefixed a short account of the author’s life by … Everard Home [the Editor]. London: James Webster; 1794.
Hopkinson DA, Marshall TK. Firearm injuries. Br J Surg. 1967;54(5):344–53.
Coupland RM, Rothschild MA, Thali MJ. Wound ballistics-basics and application. 3rd ed. Berlin: Springer; 2008.
Fackler ML, Peters CE. Ascribing local, regional, and distant injuries to the sonic pressure wave. J Trauma. 1989;1455:29–10.
Fackler ML. The ‘Strasbourg tests:’ another gunwriter/bullet salesman fraud? Wound Ballistics Rev. 1992;1(4):10–1.
Harvey EN, McMillen JH. An experimental study of shock waves resulting from the impact of high velocity missiles on animal tissues. J Exp Med. 1947;85(3):321–8.
Suneson A, Hansson HA, Kjellstrom BT, Lycke E, Seeman T. Pressure waves caused by high-energy missiles impair respiration of cultured dorsal root ganglion cells. J Trauma. 1990;30(4):484–8.
Marshall EP, Sanow EJ. Handgun stopping power: the definitive study, vol. xi. Boulder, CO: Paladin Press; 1992. p. 224.
Suneson A, Hansson HA, Seeman T. Peripheral high-energy missile hits cause pressure changes and damage to the nervous system: experimental studies on pigs. J Trauma. 1987;27(7):782–9.
Fackler ML. Wound ballistics. A review of common misconceptions. JAMA. 1988;259(18):2730–6.
Peters CE, Sebourn CL. Wound ballistics of unstable projectiles. Part II: temporary cavity formation and tissue damage. J Trauma. 1996;40(3 Suppl):S16–21.
Berlin R, Gelin LE, Janzon B, Lewis DH, Rybeck B, Sandegard J, Seeman T. Local effects of assault rifle bullets in live tissues. Acta Chir Scand Suppl. 1976;459:1–76.
Albreht M, Scepanovic D, Ceramilac A, Milivojevic V, Berger S, Tasic G, Tatic V, Todoric M, Popovic D, Nanusevic N. Experimental soft tissue wounds caused by standard military rifles. Acta Chir Scand Suppl. 1979;489:185–98.
Thoresby FP, Watts JC. Gas gangrene of the high-velocity missile wound. Br J Surg. 1967;54(1):25–9.
Adams DB. Wound ballistics: a review. Mil Med. 1982;147(10):831–5.
Fackler ML. Muscle devitalization in high-energy missile wounds, and its dependence on energy transfer. J Trauma. 1986;26(3):297.
Fackler ML, Malinowski JA. The wound profile: a visual method for quantifying gunshot wound components. J Trauma. 1985;25(6):522–9.
Fackler ML, O'Benar JD. Basic physics of the projectile-tissue interaction. Mil Med. 1987;152(10):531–4.
Hollerman JJ, Fackler ML, Coldwell DM, Ben-Menachem Y. Gunshot wounds: 1. Bullets, ballistics, and mechanisms of injury. AJR Am J Roentgenol. 1990;155(4):685–90.
Hollerman JJ, Fackler ML, Coldwell DM, Ben-Menachem Y. Gunshot wounds: 2. Radiology. AJR Am J Roentgenol. 1990;155(4):691–702.
Danel RA. Bullet wounds of the lungs. An experimental study. Surgery. 1944;15:774.
DeMuth WE Jr, Smith JM. High-velocity bullet wounds of muscle and bone: the basis of rational early treatment. J Trauma. 1966;6(6):744–55.
Hopkinson DA, Watts JC. Studies in experimental missile injuries of skeletal muscle. Proc R Soc Med. 1963;56:461–8.
Fackler ML, Breteau JP, Courbil LJ, Taxit R, Glas J, Fievet JP. Open wound drainage versus wound excision in treating the modern assault rifle wound. Surgery. 1989;105(5):576–84.
Bowyer GW, Rossiter ND. Management of gunshot wounds of the limbs. J Bone Joint Surg Br. 1997;79(6):1031–6.
DeMuth WE Jr. Bullet velocity and design as determinants of wounding capability: an experimental study. J Trauma. 1966;6(2):222–32.
Peters CE, Sebourn CL, Crowder HL. Wound ballistics of unstable projectiles. Part I: projectile yaw growth and retardation. J Trauma. 1996;40(Suppl 3):S10–5.
Penn-Barwell JG, Sargeant ID, Severe Lower Extremity Combat Trauma Study G. Gun-shot injuries in UK military casualties - features associated with wound severity. Injury. 2016;47(5):1067–71.
Coupland RM, Hoikka V, Sjoeklint OG, Cuenod P, Cauderay GC, Doswald-Beck L. Assessment of bullet disruption in armed conflicts. Lancet. 1992;339(8784):35–7.
Knapp TP, Patzakis MJ, Lee J, Seipel PR, Abdollahi K, Reisch RB. Comparison of intravenous and oral antibiotic therapy in the treatment of fractures caused by low-velocity gunshots. A prospective, randomized study of infection rates. J Bone Joint Surg Am. 1996;78(8):1167–71.
DeMuth WE Jr. High velocity bullet wounds of the thorax. Am J Surg. 1968;115(5):616–25.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG
About this chapter
Cite this chapter
Penn-Barwell, J.G., Stevenson, T. (2017). The Effect of Projectiles on Tissues. In: Breeze, J., Penn-Barwell, J., Keene, D., O'Reilly, D., Jeyanathan, J., Mahoney, P. (eds) Ballistic Trauma. Springer, Cham. https://doi.org/10.1007/978-3-319-61364-2_5
Download citation
DOI: https://doi.org/10.1007/978-3-319-61364-2_5
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-61363-5
Online ISBN: 978-3-319-61364-2
eBook Packages: MedicineMedicine (R0)