Abstract
Owing to over three decades of research, we now have a good understanding of the genetic and molecular control of enteric nervous system (ENS) development during embryonic and prenatal stages. On the other hand, it has only just become clear that a substantial process of ENS maturation occurs after birth (Hao et al. 2013a). During postnatal stages, in addition to genetic influences, ENS development is also potentially affected by the external environment. Thus it is possible that manipulating certain environmental factors could help prevent or reduce motility disorders. However the genetic and environmental factors that regulate postnatal ENS development remain unknown. Researchers have used a variety of animal models that are easy to manipulate genetically or experimentally, and have short gestational periods, to understand the development of the ENS. Notably, due to the availability of mouse models for several human enteric neuropathies, many studies have used the mature and developing murine ENS as a model. Here, I will discuss recent advances in knowledge about postnatal development of the murine ENS, and highlight future directions for this emerging research field.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Owing to over three decades of research, we now have a good understanding of the genetic and molecular control of enteric nervous system (ENS) development during embryonic and prenatal stages. On the other hand, it has only just become clear that a substantial process of ENS maturation occurs after birth (Hao et al. 2013a). During postnatal stages, in addition to genetic influences, ENS development is also potentially affected by the external environment. Thus it is possible that manipulating certain environmental factors could help prevent or reduce motility disorders . However the genetic and environmental factors that regulate postnatal ENS development remain unknown. Researchers have used a variety of animal models that are easy to manipulate genetically or experimentally, and have short gestational periods, to understand the development of the ENS. Notably, due to the availability of mouse models for several human enteric neuropathies, many studies have used the mature and developing murine ENS as a model. Here, I will discuss recent advances in knowledge about postnatal development of the murine ENS, and highlight future directions for this emerging research field.
Development of Enteric Ganglionated Plexuses
The ENS is a network of neurons and glia residing within two major ganglionated plexuses embedded along the wall of the gastrointestinal tract (Furness 2012). The submucous plexus lies between the mucosa and circular muscle, the myenteric plexus is sandwiched between the longitudinal and circular muscles.
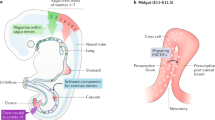
The ENS derives mainly from the vagal neural crest. Similar to other parts of the nervous system, development of the ENS comprises of a series of overlapping stages: migration, proliferation, differentiation and formation of synapses (Hao et al. 2013a; Sasselli et al. 2012). While the formation of the myenteric plexus precedes the submucous plexus in mice (Jiang et al. 2003; Uesaka et al. 2013), much is still unknown about how development of neurons in one plexus influences the other. The mature and developing myenteric plexus has been well studied compared to the submucous plexus.
Maturation of Cholinergic and Nitrergic Neurons
In the mature ENS, cholinergic (express the enzyme choline acetyltransferase, ChAT) and nitrergic (express the enzyme neuronal nitric oxide synthase, nNOS) neurons are typically characterized as separate neuronal populations (Foong et al. 2014; Sang and Young 1998). Cholinergic neurons are excitatory neurons and function as motor neurons, interneurons and sensory neurons, while nitrergic neurons can be inhibitory motor neurons or interneurons.
Significant numbers of myenteric neurons are still being born (exiting the cell cycle) between P0 and P10 in mice (Bergner et al. 2014; Laranjeira et al. 2011; Pham et al. 1991). Submucosal neurons tend to exit the cell cycle and differentiate later than myenteric neurons (McKeown et al. 2001; Pham et al. 1991). Some neuronal precursors transiently express certain neurotransmitter synthetic enzymes during fetal or early postnatal development (Baetge and Gershon 1989; Bergner et al. 2014; Gershon et al. 1993; Hao et al. 2013b; Obermayr et al. 2013). For example, in the small intestine, some submucosal and myenteric neurons that do not express nNOS in the mature gut transiently express nNOS during embryonic and early postnatal development (Bergner et al. 2014; Young and Ciampoli 1998). Nonetheless, segregation between nitrergic and cholinergic neurons seems to be established early in development (Hao et al. 2013b).
The proportion of nNOS myenteric neurons in the small intestine does not change significantly postnatally, whereas nNOS submucosal neurons decline from 50 % at P0 to only 3 % in adult mice (Young and Ciampoli 1998). Research into the development of ChAT neurons has been limited by technical difficulties until very recently. Uptake of 3[H]-choline at E10–E12 suggested that ChAT+ cells appear very early in development (Rothman and Gershon 1982). However, several ChAT antisera failed to detect any neurons in the gut until late embryonic stages. To overcome this problem, two recent studies used mouse fluorescent reporter lines to detect ChAT (Hao et al. 2013b; Erickson et al. 2014). The first used Cre-lox technology (ChAT-Cre mice in combination with a fluorescent reporter line) and detected the first ChAT+ neurons in the gut at E11.5. In this ChAT-Cre:R26R line, cholinergic neurons gradually increase in number during late embryonic and postnatal stages, and at birth, the proportion of cholinergic neurons at birth is still less than half of that in the adult small intestine (Hao et al. 2013b). The second study extended these findings and found that in ChAT-GFP mice GFP+ neurons are already present at E10.5; this study was also able to detect ChAT immunoreactive neurons in the gut E10.5 (Erickson et al. 2014). Furthermore, the proportion of cholinergic neurons in the small intestine was found to achieve adult levels as early as E13.5 (Erickson et al. 2014).
Little is known about the mechanisms regulating neuronal differentiation postnatally, although the role of two transcription factors in postnatal neuronal differentiation has been examined. Hand2 haploinsufficiency results in a reduction of nNOS neurons in embryos, and this reduction persists through to postnatal weeks 6–8 (D’Autreaux et al. 2011). Homeodomain interacting protein kinase 2 ( HIPK2 ) is a transcriptional cofactor of bone morphogenetic proteins. Loss of HIPK2 did not affect enteric neurons during embryogenesis, but caused a progressive decrease in the number of myenteric and submucosal neurons in the caudal gut with increasing postnatal age (Chalazonitis et al. 2011). Thus HIPK2 may be important for survival and differentiation of enteric neurons postnatally (Chalazonitis et al. 2011). Although not specifically studied, many other transcription factors, including Ascl1 (formally known as Mash1) (Okamura and Saga 2008), implicated in prenatal neuronal differentiation could also be involved in the postnatal development of enteric neurons.
Some external factors have been reported to affect enteric neuron differentiation postnatally. For example, the colonization of the intestine by microbiota has been shown to affect ENS postnatal development. The jejunum and ileum of germ-free mice have decreased myenteric nerve density and ganglion size, but an increase in proportion of myenteric nitrergic neurons (Collins et al. 2014). However, whether this is a direct effect of a lack of microbiota remains to be elucidated, as there are other defects in germ-free mice and the ENS defects might be indirect (Yi and Li 2012). Diet has also been shown to affect the postnatal development of the ENS; mice fed on a high fat diet for 8 weeks have decreased numbers of myenteric neurons in the small and large intestine, but submucosal neurons were unaffected (Stenkamp-Strahm et al. 2013; Voss et al. 2013). Notably in the duodenum, nitrergic neurons were particularly affected, while cholinergic neurons were spared (Stenkamp-Strahm et al. 2013). In contrast, a high fat diet was reported to be neuroprotective in the stomach, preventing age-associated loss of nitrergic myenteric neurons (Baudry et al. 2012).
Maturation of Neuronal Morphology
As in other species, adult enteric neurons in the mouse have either a single axon or multiple axons (Dogiel type II, DII) (Foong et al. 2012, 2014; Nurgali et al. 2004; Wong et al. 2008). Most myenteric uniaxonal neurons only have lamellar dendrites, while DII neurons have smooth cell bodies and typically project their axons circumferentially (Foong et al. 2012; Nurgali et al. 2004).
The first enteric neurons to differentiate have single long, anally-projecting axon-like processes (Hao et al. 2013a; Young et al. 2002, 2014). Orally and circumferentially-projecting neurons appear later. Unlike adults, most uniaxonal embryonic and early postnatal myenteric neurons have multiple filamentous dendrite-like structures instead of lamellar dendrites (Foong et al. 2012). Maturation of dendritic morphology and axonal projection lengths of uniaxonal neurons persists in postnatal stages, even after P10. DII neurons are present by birth and their long processes project nearly around the entire gut circumference at P10. Despite significant growth in gut circumference between P10 and adult, the lengths of DII neuron axons do not increase after P10 (Foong et al. 2012). The morphological changes in dendrites and axons after birth suggests that synapse formation remains dynamic postnatally; raising the possibility that ENS connectivity is vulnerable to environmental factors.
Maturation of Electrophysiological Properties
Enteric neurons are usually characterized into two classes. One group fires action potentials with short repolarizations (S-type) , while the other group of neurons fires action potentials with long after-hyperpolarization potentials (AH-type) . S-type myenteric neurons are typically uniaxonal while AH-type neurons exhibit DII morphology (Foong et al. 2012; Nurgali et al. 2004).
The electrophysiological properties of early postnatal myenteric neurons have been examined only very recently. At birth, the two adult-like classes of myenteric neurons are present, with distinctive electrophysiological and corresponding morphological properties, but these properties are not yet mature (Foong et al. 2012). Furthermore, the two classes of neurons develop asynchronously. S-type neurons seem to mature electrophysiologically first. A prominent Ca2+-mediated after-depolarizing potential is observed in DII neurons at P0 and P10 that is significantly larger than that recorded in their adult counterparts (Foong et al. 2012). In other parts of the nervous system, neuronal activity and increased intracellular calcium concentration affect development (Young et al. 2014), however, the mechanisms regulating the postnatal maturation of enteric neurons remain to be identified.
Maturation of Synaptic Profile
Adult enteric neurons receive a variety of synaptic inputs including fast and slow excitatory postsynaptic potentials (EPSPs ), and inhibitory postsynaptic potentials (IPSPs ) (Foong et al. 2012, 2014; Nurgali et al. 2004; Wong et al. 2008). The vast majority of enteric neurons exhibit fast EPSPs and only the neurotransmitters mediating fast transmission have been investigated in mice to date. Acetylcholine activating nicotinic receptors is the main mode of fast transmission, but ATP acting via P2X receptors is also involved (Foong et al. 2012, 2014; Nurgali et al. 2004; Wong et al. 2008).
At P0, S-type neurons exhibit fast EPSPs, and by P10, like adults, these fast EPSPs are mediated by nicotinic receptors (Foong et al. 2012). At P10-11, there is still few, if any, slow EPSPS or IPSPs (Foong et al. 2012). Thus, in combination with the significant growth of gut size, maturation of dendritic structure and axonal projection that occurs from P10 to adulthood, it is evident that the formation and maturation of synapses occurs over a protracted period of time.
Little is known about the regulation of synaptogenesis in the ENS. However, loss of Hipk2 and the absence of gut microbiota reduced intraganglionic synapses and nerve density respectively in postnatal myenteric plexus (Chalazonitis et al. 2011; Collins et al. 2014).
Maturation of Neurally-Mediated Motility Patterns
Motility in the mature intestine involves interactions between enteric neurons, interstitial cells of Cajal and intrinsic smooth muscle (Huizinga and Lammers 2009). Motility patterns differ in different regions of the gut, but mainly involves a combination of mixing behaviours to facilitate digestion and absorption of nutrients, and propulsion, to push the gut contents along the GIT (Bornstein et al. 2004; Burns et al. 2009; Costa et al. 2013; Huizinga and Lammers 2009).
It is essential for the duodenum to be functional by birth in order for the newborn to digest and absorb milk nutrients. The first propagating motility patterns detected in the gut are non-neuronal. In the duodenum, neurally-mediated motility commences just prior to birth, at E18.5 (Roberts et al. 2010). Conversely, neurally-mediated motility in the colon commences several days after birth. By P6, the neural circuit underlying colonic migrating motor complexes (CMMCs ) is present; however, CMMCs are only induced by blocking NOS (Roberts et al. 2007). In E18.5 and P0 duodenum, inhibition of nNOS induced or increases the frequency of contraction complexes (Roberts et al. 2010). In addition, during development the circular muscle appears to receive innervation from nNOS+ fibres prior to ChAT+ fibres. The number and density of ChAT+ fibres increase significantly after birth (Hao et al. 2013b; Roberts et al. 2007). Thus overall these pharmacological and immunohistochemical studies suggest that smooth muscle cells are tonically inhibited by NO until sufficient ChAT+ fibres are present to induce contractions. However, a re-examination of the number and density of ChAT+ fibres during development is now necessary since ChAT+ neurons are recently reported to achieve adult proportions by E13 in the small intestine and by P0 in the proximal colon (Erickson et al. 2014). In both duodenum and colon, motility patterns seem to be mature by P10 (Hao et al. 2013b; Roberts et al. 2007, 2010).
Some genetic and environmental factors that affect postnatal development of neurons also elicit profound effects on gut motility. Indeed, abnormal numbers of neuronal subtypes and nerve density due to impaired trophic factor signalling, absence of gut microbiota and prolonged ingestion of high fat diets all led to altered gut motility (Baudry et al. 2012; Chalazonitis et al. 2011; Collins et al. 2014; Mushref and Srinivasan 2013).
Postnatal Gut and Therapy
Understanding how the ENS develops postnatally could assist in developing therapies for gut motility disorders. Defects in ENS development result in pediatric motility disorders including Hirschprung disease, a congenital disorder affecting 1:4000–5000 newborns, in which enteric neurons are absent from the distal gut. These patients suffer from severe constipation and require surgery. Current therapies for Hirschprung patients and other gut motility disorders are life-saving, but remain inadequate in addressing other complications including dysmotility and incontinence that can last for years (Hotta et al. 2009).
A potential treatment plan would be to restore the ENS at the aganglionic region of Hirschprung patients. In recent years, the idea of transplanting progenitor cells as therapy for gut motility disorders has generated a lot of interest (Burns and Thapar 2014). Diagnosis of enteric neuropathies typically occurs after birth, thus cell therapy has to be administered postnatally. In fact, it is ideal for progenitor cells to be obtained from a “healthy” gut region of the patients themselves. Neural progenitors can be obtained the postnatal mouse and human gut and that their developmental potential appear to be similar to those obtained from fetal gut (Bondurand et al. 2003; Hotta et al. 2013; Metzger et al. 2009). Furthermore, it has recently been shown that after transplantation into the colon of postnatal mice, ENS progenitors isolated from postnatal gut successfully developed into neurons with the appropriate enteric neuronal subtype properties, including electrophysiological properties (Hotta et al. 2013). While this shows that cell therapy is a promising strategy, there are still significant obstacles to be overcome. In particular, these progenitors need to be able to generate a functional ENS over the patient’s aganglionic region (average length 7–10 cm) (Burns and Thapar 2014).
External factors such as diet and gut microbiota found to affect postnatal development could potentially be manipulated to prevent or help rescue the defected ENS. This strategy can be applied on its own or coupled with cell therapies to improve treatment of enteric neuropathies.
Conclusions
Substantial development of enteric neuronal properties continues postnatally. During this time the ENS is vulnerable to factors present in the extra uterine environment. Interaction between the environment and the yet to be identified intrinsic factors regulating ENS maturation will be a fertile source of research in the future.
References
Baetge G, Gershon MD (1989) Transient catecholaminergic (TC) cells in the vagus nerves and bowel of fetal mice: relationship to the development of enteric neurons. Dev Biol 132(1):189–211
Baudry C, Reichardt F, Marchix J, Bado A, Schemann M, des Varannes SB, Neunlist M, Moriez R (2012) Diet-induced obesity has neuroprotective effects in murine gastric enteric nervous system: involvement of leptin and glial cell line-derived neurotrophic factor. J Physiol 590(Pt 3):533–544
Bergner AJ, Stamp LA, Gonsalvez DG, Allison MB, Olson DP, Myers MG Jr, Anderson CR, Young HM (2014) Birthdating of myenteric neuron subtypes in the small intestine of the mouse. J Comp Neurol 522(3):514–527
Bondurand N, Natarajan D, Thapar N, Atkins C, Pachnis V (2003) Neuron and glia generating progenitors of the mammalian enteric nervous system isolated from foetal and postnatal gut cultures. Development 130(25):6387–6400
Bornstein JC, Costa M, Grider JR (2004) Enteric motor and interneuronal circuits controlling motility. Neurogastroenterol Motil 16(Suppl 1):34–38
Burns AJ, Thapar N (2014) Neural stem cell therapies for enteric nervous system disorders. Nat Rev Gastroenterol Hepatol 11(5):317–328
Burns AJ, Roberts RR, Bornstein JC, Young HM (2009) Development of the enteric nervous system and its role in intestinal motility during fetal and early postnatal stages. Semin Pediatr Surg 18(4):196–205
Chalazonitis A, Tang AA, Shang Y, Pham TD, Hsieh I, Setlik W, Gershon MD, Huang EJ (2011) Homeodomain interacting protein kinase 2 regulates postnatal development of enteric dopaminergic neurons and glia via BMP signaling. J Neurosci 31(39):13746–13757
Collins J, Borojevic R, Verdu EF, Huizinga JD, Ratcliffe EM (2014) Intestinal microbiota influence the early postnatal development of the enteric nervous system. Neurogastroenterol Motil 26(1):98–107
Costa M, Dodds KN, Wiklendt L, Spencer NJ, Brookes SJ, Dinning PG (2013) Neurogenic and myogenic motor activity in the colon of the guinea pig, mouse, rabbit, and rat. Am J Physiol Gastrointest Liver Physiol 305(10):G749–G759
D’Autreaux F, Margolis KG, Roberts J, Stevanovic K, Mawe G, Li Z, Karamooz N, Ahuja A, Morikawa Y, Cserjesi P, Setlick W, Gershon MD (2011) Expression level of Hand2 affects specification of enteric neurons and gastrointestinal function in mice. Gastroenterology 141(2):576–587, 587.e571–576
Erickson CS, Lee SJ, Barlow-Anacker AJ, Druckenbrod NR, Epstein ML, Gosain A (2014) Appearance of cholinergic myenteric neurons during enteric nervous system development: comparison of different ChAT fluorescent mouse reporter lines. Neurogastroenterol Motil 26(6):874–884
Foong JP, Nguyen TV, Furness JB, Bornstein JC, Young HM (2012) Myenteric neurons of the mouse small intestine undergo significant electrophysiological and morphological changes during postnatal development. J Physiol 590(Pt 10):2375–2390
Foong JP, Tough IR, Cox HM, Bornstein JC (2014) Properties of cholinergic and non-cholinergic submucosal neurons along the mouse colon. J Physiol 592(Pt 4):777–793
Furness JB (2012) The enteric nervous system and neurogastroenterology. Nat Rev Gastroenterol Hepatol 9(5):286–294
Gershon MD, Chalazonitis A, Rothman TP (1993) From neural crest to bowel: development of the enteric nervous system. J Neurobiol 24(2):199–214
Hao MM, Bornstein JC, Vanden Berghe P, Lomax AE, Young HM, Foong JP (2013a) The emergence of neural activity and its role in the development of the enteric nervous system. Dev Biol 382(1):365–374
Hao MM, Bornstein JC, Young HM (2013b) Development of myenteric cholinergic neurons in ChAT-Cre;R26R-YFP mice. J Comp Neurol 521(14):3358–3370
Hotta R, Natarajan D, Thapar N (2009) Potential of cell therapy to treat pediatric motility disorders. Semin Pediatr Surg 18(4):263–273
Hotta R, Stamp LA, Foong JP, McConnell SN, Bergner AJ, Anderson RB, Enomoto H, Newgreen DF, Obermayr F, Furness JB, Young HM (2013) Transplanted progenitors generate functional enteric neurons in the postnatal colon. J Clin Invest 123(3):1182–1191
Huizinga JD, Lammers WJ (2009) Gut peristalsis is governed by a multitude of cooperating mechanisms. Am J Physiol Gastrointest Liver Physiol 296(1):G1–G8
Jiang Y, Liu MT, Gershon MD (2003) Netrins and DCC in the guidance of migrating neural crest-derived cells in the developing bowel and pancreas. Dev Biol 258(2):364–384
Laranjeira C, Sandgren K, Kessaris N, Richardson W, Potocnik A, Vanden Berghe P, Pachnis V (2011) Glial cells in the mouse enteric nervous system can undergo neurogenesis in response to injury. J Clin Invest 121(9):3412–3424
McKeown SJ, Chow CW, Young HM (2001) Development of the submucous plexus in the large intestine of the mouse. Cell Tissue Res 303(2):301–305
Metzger M, Caldwell C, Barlow AJ, Burns AJ, Thapar N (2009) Enteric nervous system stem cells derived from human gut mucosa for the treatment of aganglionic gut disorders. Gastroenterology 136(7):2214–2225, e2211–2213
Mushref MA, Srinivasan S (2013) Effect of high fat-diet and obesity on gastrointestinal motility. Ann Transl Med 1(2):14
Nurgali K, Stebbing MJ, Furness JB (2004) Correlation of electrophysiological and morphological characteristics of enteric neurons in the mouse colon. J Comp Neurol 468(1):112–124
Obermayr F, Stamp LA, Anderson CR, Young HM (2013) Genetic fate-mapping of tyrosine hydroxylase-expressing cells in the enteric nervous system. Neurogastroenterol Motil 25(4):e283–e291
Okamura Y, Saga Y (2008) Notch signaling is required for the maintenance of enteric neural crest progenitors. Development 135(21):3555–3565
Pham TD, Gershon MD, Rothman TP (1991) Time of origin of neurons in the murine enteric nervous system: sequence in relation to phenotype. J Comp Neurol 314(4):789–798
Roberts RR, Murphy JF, Young HM, Bornstein JC (2007) Development of colonic motility in the neonatal mouse-studies using spatiotemporal maps. Am J Physiol Gastrointest Liver Physiol 292(3):G930–G938
Roberts RR, Ellis M, Gwynne RM, Bergner AJ, Lewis MD, Beckett EA, Bornstein JC, Young HM (2010) The first intestinal motility patterns in fetal mice are not mediated by neurons or interstitial cells of Cajal. J Physiol 588(Pt 7):1153–1169
Rothman TP, Gershon MD (1982) Phenotypic expression in the developing murine enteric nervous system. J Neurosci 2(3):381–393
Sang Q, Young HM (1998) The identification and chemical coding of cholinergic neurons in the small and large intestine of the mouse. Anat Rec 251(2):185–199
Sasselli V, Pachnis V, Burns AJ (2012) The enteric nervous system. Dev Biol 366(1):64–73
Stenkamp-Strahm CM, Kappmeyer AJ, Schmalz JT, Gericke M, Balemba O (2013) High-fat diet ingestion correlates with neuropathy in the duodenum myenteric plexus of obese mice with symptoms of type 2 diabetes. Cell Tissue Res 354(2):381–394
Uesaka T, Nagashimada M, Enomoto H (2013) GDNF signaling levels control migration and neuronal differentiation of enteric ganglion precursors. J Neurosci 33(41):16372–16382
Voss U, Sand E, Olde B, Ekblad E (2013) Enteric neuropathy can be induced by high fat diet in vivo and palmitic acid exposure in vitro. PLoS One 8(12), e81413
Wong V, Blennerhassett M, Vanner S (2008) Electrophysiological and morphological properties of submucosal neurons in the mouse distal colon. Neurogastroenterol Motil 20(6):725–734
Yi P, Li L (2012) The germfree murine animal: an important animal model for research on the relationship between gut microbiota and the host. Vet Microbiol 157(1-2):1–7
Young HM, Ciampoli D (1998) Transient expression of neuronal nitric oxide synthase by neurons of the submucous plexus of the mouse small intestine. Cell Tissue Res 291(3):395–401
Young HM, Jones BR, McKeown SJ (2002) The projections of early enteric neurons are influenced by the direction of neural crest cell migration. J Neurosci 22(14):6005–6018
Young HM, Bergner AJ, Simpson MJ, McKeown SJ, Hao MM, Anderson CR, Enomoto H (2014) Colonizing while migrating: how do individual enteric neural crest cells behave? BMC Biol 12(1):23
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Foong, J.P.P. (2016). Postnatal Development of the Mouse Enteric Nervous System. In: Brierley, S., Costa, M. (eds) The Enteric Nervous System. Advances in Experimental Medicine and Biology(), vol 891. Springer, Cham. https://doi.org/10.1007/978-3-319-27592-5_13
Download citation
DOI: https://doi.org/10.1007/978-3-319-27592-5_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-27590-1
Online ISBN: 978-3-319-27592-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)