Abstract
Exposure to environmental contaminants is thought to be important in the development of adverse effects on reproductive health. While the adverse effects of environmental contaminants on semen quality and testicular function have been well studied, effects on ovarian function are less well defined. Epidemiological studies have linked exposure to environmental contaminants with adverse effects on menstrual cycle characteristics, infertility, and earlier age of menopause onset; yet direct evidence of effects on ovarian function is lacking. Environmental contaminant concentrations have been quantified in human ovarian follicular fluid establishing target tissue exposure; however, such data is sporadic and limited to women undergoing assisted reproductive therapies making generalization of results to the broader population of women difficult. We note that the relationship between serum and follicular fluid concentrations can be orders of magnitude different and thus target tissue distribution requires further study. Animal studies revealed effects of environmental contaminants on ovarian follicle dynamics, oocyte maturation, steroidogenesis, and epigenetic changes. Issues of dosing such as concentration of test chemicals used, route of administration, and use of multiple dose groups remain important limitations of the current literature. While animal studies establish a basis for biological plausibility of effects and support conclusions of reproductive hazard, we conclude that exposures in the general human population are too low to present a demonstrable risk to human ovarian function.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Worldwide, estimates of infertility range widely from 50 to 186 million couples of which 7.3 million American women alone are infertile (Boivin et al. 2007; Chandra et al. 2005; Mascarenhas et al. 2012; Rutstein and Shah 2004; Stephen and Chandra 2006). Established risk factors for infertility include: advanced age, diet, prescription medication use, pre-existing health status, genetic mutations, and infections; however, for many women the cause of their infertility is unknown. Thus, exposures to environmental contaminants are thought to adversely affect human fertility. Indeed, an association between farm or industrial work and infertility was demonstrated using a questionnaire on reproductive and occupational health histories, lifestyle and demographics (Fuortes et al. 1997), while residue levels of specific compounds were not measured. Infertile women had higher odds of working in industry (OR, 95 % CI = 6.7, 2.3–19.6) or farms (1.8, 1.2–2.7), adjusted for age, date of outcome and smoking compared to a fertile control group. Among specific infertility types, ovulatory dysfunction was highest and shows an association with industry/occupation (10.9, 3.5–33.7). In a National survey conducted in French in vitro fertilization (IVF) clinics between 2011 and 2012 (Alvarez and Devouche 2012), one in eight women reported sexual problems (mostly dyspareunia, insensitivity and bleeding). Of the 348 responding women (mean age: 34.9 ± 5.3 years), 20 % smoked cigarettes, 1.4 % cannabis, and 23 % consumed alcohol, whereas 8.6 % reported occupational exposure to chemicals. Work stress was reported by 41 % and family stress by 14 %. Taken together, these data suggest that exposures to environmental contaminants are potentially associated with reduced fertility, however, the strength of this association and potential mechanisms are poorly defined.
While the effects of environmental contaminants on male reproductive health have received research attention, the effects on female fertility and ovarian function in particular remain to be elucidated. We propose that environmental contaminants affect reproductive health in part via impaired ovarian function (Augood et al. 1998; Foster 2003; Pocar et al. 2003; Sadeu et al. 2010). Moreover, we postulate that the ovary is potentially vulnerable to the adverse effects of environmental contaminant exposure owing to its rich blood supply, rapid cell division associated with follicle development, and ovulation. Moreover, environmental contaminant effects on the ovary have far reaching consequences on reproduction and general health owing to its central role in the production of the gonadal steroids estradiol (E2) and progesterone (P4), the finite and non-renewable number of follicles present in the ovary at birth, and development of female gametes (oocytes).
2 Epidemiology
Determining the effect of environmental contaminants on reproductive health in women and on ovarian function in particular is difficult to assess. The relationship between environmental contaminant exposure and reproductive function in women has primarily been limited to measurement of time-to-pregnancy (TTP), infertility, menstrual cycle characteristics, duration of menstrual bleeding, amenorrhea, dysmenorrhea, age at menopause, and premature ovarian failure (POF). Measurement of circulating follicle stimulating hormone (FSH), ovarian hormones (activin and inhibin), gonadal steroid hormones (E2 and P4), and more recently quantification of anti-Müllerian hormone (AMH) concentrations have been employed as markers of impaired reproductive health that provide indirect insight into ovarian function.
A questionnaire on reproductive health and lifestyle histories of women who presented with natural menopause revealed that only women who had been breastfed as babies showed a significantly earlier natural menopause (p = 0.014), while alcohol consumption (p = 0.080) and smoking (p = 0.081) had no significant effect on timing of natural menopause (Dvornyk et al. 2006). Other factors such as the use of oral contraceptives also had no significant effect. In contrast, a survey of 443 hairdressers, aged 21–55, revealed a greater likelihood of premature ovarian failure (POF; 3.2 vs. 1.4 %, p = 0.06) compared to 508 women employed in other occupations (Gallicchio et al. 2009). While hairdressers also smoked significantly more than the controls, the overall relative risk (RR, 95 % CI) for POF was 1.90, (0.76–4.72) and thus was non-significant. Hairdressers are exposed to several chemicals such as solvents, bleaches, hair dyes, non-lye relaxers, alcohols, ethylene glycol, methacrylate and phthalates; all of which are potentially hazardous to ovarian function. Sub-analysis of the data revealed that Caucasians over 40 years had a RR of 5.58 (1.24–25.22) illustrating that age is an important variable in assessing the impact of environmental factors on ovarian function. In another study, ovarian failure was reported (Koh et al. 1998) in 16 laborers exposed to cleaning solvent containing 2-bromopropane (n-propyl bromide). Amenorrhea was reported in 26 women after occupational exposure in South Korea, of which 16 were diagnosed with primary ovarian failure. Between these two groups, there were significant differences (P < 0.05) in levels of LH: 32.9 mIU/ml (range = 10.1–93.0) vs. 8.5 (1.1–13.9); FSH: 87.7 mIU/ml (31.8–119.7) vs. 9.8 (3.3–28.3); and E2: 11.0 pg/ml (7.0–28.0) vs. 48.0 (12.0–205.0). While the effects of occupational exposure to environmental contaminants are well known, effects arising from exposure to environmental contaminants at exposure levels representative of the concentrations reported in contemporary biomonitoring studies involving the general population are less clear.
Persistent Organic Pollutants (POPs ) are a group of chemicals including the chlorinated organic chemicals that have been used in the manufacture of a diverse group of chemical compounds such as pesticides, chlorine, bleaches, plastics, flame-retardants and metal production. Since they are stable and lipophilic, they easily accumulate in the food chain, and humans may acquire them via food or direct (occupational or accidental) exposure (Hombach-Klonisch et al. 2005). Polybrominated diphenyl ethers (PBDEs ) are a family of structurally related chemicals used as flame retardants, and have been detected in human follicular fluid (Johnson et al. 2012). Several organochlorine compounds including the polychlorinated biphenyls (PCBs) and metabolites of the pesticide DDT, have also been quantified in follicular fluid (De Felip et al. 2004; Foster 1995; Mahalingaiah et al. 2012; Meeker et al. 2009; Petro et al. 2012; Schlebusch et al. 1989; Younglai et al. 2002) (Table 7.1). In a longitudinal study of 501 couples who discontinued contraception to achieve pregnancy (Bloom et al. 2007) the fecundability odds ratios (FOR) was decreased by 18–21 % in women with PCB congeners 118, 167 & 219. The strongest effect found was for PCB167 (FOR = 0.79; 95 % CI = 0.64–0.97). These correlations suggest that PCB exposure is associated with adverse effects on fertility although the direct ovarian effects of PCBs remain equivocal. Mean total PCB concentrations (3.1 ± 1.9 μg/L) were positively correlated with menstrual cycle length reported by 2314 women (p = 0.02) (Cooper et al. 2005). The majority of 37 follicular fluid samples from an IVF clinic contained 0–1 and 1–2 μg/kg of PCB138, 153, or 180, but the highest levels reached 15–16 μg/kg (Schlebusch et al. 1989). In women attending a fertility clinic, follicular fluid concentrations of PCB180 were lower in women who became pregnant vs. those who did not (85 ± 14 vs. 147 ± 11 pg/ml, respectively, p < 0.05). German women had higher serum PCB concentrations (0.35 ± 0.049 vs. 0.17 ± 0.02 μg/kg, p < 0.01) compared to women in Tanzania (Weiss et al. 2006). In contrast, follicular fluid levels did not show regional differences (0.26 ± 0.02 vs. 0.22 ± 0.06 μg/kg). These studies suffer from relatively small sample sizes and recruitment exclusively from women attending fertility clinics and thus generalization of results to the entire population is difficult. Although 2,3,7,8 tetrachlorodibenzo-p-dioxin (TCDD ) is widely regarded as one of the most toxic environmental contaminants, adverse effects on ovarian function are poorly defined. A long-term study was carried out in Italy after a chemical plant explosion in 1976 that exposed a town to TCDD (Eskenazi et al. 2005). Serum residue concentrations of 43.7 ppt (range, 2.5–6320) were found in 616 women that were exposed between 1 month and 40 years of age. While there was a trend toward earlier menopause with increasing TCDD concentrations, suggesting potential effects on ovarian function, significance could not be documented.
The common pesticide 1,1-bis-(4-chlorophenyl)-2,2,2-trichloroethane ( p,p′-DDT ) has been banned in many industrialized countries, but continues to be used in developing nations. Although widely studied, the relationship between exposure to this pesticide and its metabolites on fertility and ovarian function remains equivocal. The DDT metabolite 1,1-bis-(4-chlorophenyl) 2,2-dichloroethene ( p,p′-DDE ) is frequently detected in serum and follicular fluid (De et al. 2004; Mahalingaiah et al. 2012; Petro et al. 2012; Younglai et al. 2002) although effects on fertility have been mixed (Table 7.1). A study that compared the fertility of 289 women born in the USA between 1960 and 1963 to that of their daughters’ 30 years later showed a 32 % decrease in the probability of pregnancy of the daughters for every 10 μg/L in maternal serum DDT, but also an unexpected 16 % increase in the probability of pregnancy for every 10 μg/L in maternal serum DDE (Cohn et al. 2003). While in Brazil, sales of pesticides in 1985 were correlated with reproductive alterations and cancer rates a decade later (Koifman et al. 2002), no association between serum DDE levels (mean value: 30.0 ± 19.6 μg/L) and menstrual cycle dysfunction (cycle length and missed periods) was found in two American studies (Cooper et al. 2005; Mahalingaiah et al. 2012). A study comparing German and Tanzanian women attending fertility clinics (Weiss et al. 2006) found that Tanzanian women had higher DDE levels (12.77 ± 9.7 vs. 0.78 ± 0.75 μg/kg, P < 0.01). In contrast, in a Canadian study (Younglai et al. 2002), pesticide concentrations in the follicular fluid were not related to pregnancy rates whereas in a Belgian study of infertility patients (Petro et al. 2012), an association between follicular fluid DDE levels (392 ± 348 pg/ml) and reduced fertilization rates and embryo quality was described. We postulate that equivocal findings may be related to study design, sample size, analytical methods, regional differences, and potential interactions amongst the myriad chemicals to which people are exposed.
Organophosphates are a widely used family of pesticides to increase crop productivity by eradicating pests. Despite substantial available information involving the impact of organophosphates on the environment and different animal species (Patel et al. 2007), evidence of toxicity in humans remains scarce. Exposures to high concentrations of organophosphates in a short period, especially during the manufacture, formulation, and application of chemicals can lead to toxic effects (Dyer et al. 2001). In Iowa and North Carolina, the association between pesticide use and menstrual function among 3103 women living on farms was examined (Farr et al. 2004). These women were premenopausal, between the ages of 21–40 years of age, not pregnant or breastfeeding, and not taking hormonal contraceptives. Results revealed that women who were exposed to pesticides experienced a non-significant increase in menstrual cycle length (odds ratio = 1.2, 95 % CI: 0.66, 2.2) and increased odds of missed periods (odds ratio = 1.5, 95 % CI: 1.2, 1.9) compared with women who have never used pesticides (Farr et al. 2004). Women who were exposed to organophosphates experienced longer menstrual cycles (odds ratio = 1.3, 95 % CI: 0.55, 2.9) and increased odds of missed periods (odds ratio = 1.4, 95 % CI: 0.93, 2.2) compared with women who had never used pesticides. Women with suspected exposure to hormonally active or ovotoxic pesticides (parathion and trichlorfon) had fewer cases of irregular menstrual cycles (odds ratio = 0.53, 95 % CI: 0.37, 0.78) but 60–100 % increased odds of long cycles (odds ratio = 1.6, 95 % CI: 1.0, 2.5), missed periods (odds ratio = 1.7, 95 % CI: 1.3, 2,2), and intermenstrual bleeding (odds ratio = 1.3, 95 % CI: 1.0, 1.6) than women who had never used pesticides (Farr et al. 2004). The findings suggest a possible but weak correlation between the use of certain hormonally active pesticides and decreased menstrual function among women living on farms. Further detailed data on menstrual cycle and organophosphate exposure is required to strengthen the association between organophosphate exposure and menstrual cycle characteristics.
Of the metals , exposure to cadmium (Cd), mercury (Hg), lead (Pb), selenium (Se) and zinc (Zn) are the most commonly encountered and linked with adverse reproductive effects (Dickerson et al. 2011; Jackson et al. 2011; Pollack et al. 2011; Yang et al. 2002). Cd, Hg and Pb have been measured in follicular fluid (Al-Saleh et al. 2008; Bloom et al. 2012b) providing direct evidence of target tissue exposure (Table 7.2). The effects of metals including Cd on ovarian function have been evaluated by several research groups (Davis et al. 2001; Laughlin et al. 1987; Zhang and Jia 2007; Zhang et al. 2008). An inverse relationship between serum Cd concentrations and circulating concentrations of FSH were reported in the absence of any effect on circulating E2 concentrations (Pollack et al. 2011). The relationship between menstrual cycle characteristics and circulating metal concentrations was investigated previously; however, only Cd was associated with higher serum E2 concentrations (Jackson et al. 2011) which contrast with the results described by others who could not find an effect (Pollack et al. 2011). For each μg/l increase in Cd there was a 24.3 % increase in circulating E2 concentrations during the follicular phase (95 % CI = 1.1–52.9). Although the source of exposure was not confirmed, cigarette smoking is thought to be the primary source. Cigarette smoking is associated with elevated levels of blood Cd that are 2.5–4 times higher than in non-smokers (Batariova et al. 2006; Wong and Lye 2008; Zhang and Jia 2007). However, these results contrast with studies that have reported decreased circulating concentrations of E2 in female smokers (Windham et al. 2005).
While a positive association between blood Pb concentrations and circulating P4 levels have been reported (Pollack et al. 2011) an inverse association between follicular fluid Pb concentrations and fertilization rates (relative risk = 0.68, P = 0.026) was found in women undergoing fertility treatments in another study (Bloom et al. 2012b). The mean blood and follicular fluid Pb concentrations were 0.82 ± 0.31 and 0.25 ± 0.31 μg/L, respectively. In another study (Jackson et al. 2011), Pb levels of 0.87 μg/dl were reported in human whole blood samples, but were not associated with toxic effects. An increased odds ratio for dysmenorrhea (1.66; 1.07–2.59) compared to non-exposed controls was found in a study of normal cycling women with occupational exposure to Hg vapor in a Chinese lamp factory (Yang et al. 2002). In another study (Dickerson et al. 2011), Hg, Zn and Se concentrations were measured in patients attending a fertility clinic. Only Hg showed a negative correlation with the number of oocytes collected and follicle number after ovarian stimulation, after adjusting for age and BMI. There were no effects on fertilization, cleavage rates or embryo quality. Despite evidence of reproductive hazard, the literature relating metal exposure with reproductive effects lacks consistency across studies and thus the evidence is judged as weak.
Unlike POPs and metals, newer generation commercial chemicals are engineered to be more labile and hydrophilic in order to obviate concerns with bioaccumulation and toxicity to mammalian systems. Of these bisphenol A (BPA) has received extensive research attention and has been linked with reproductive effects in women, yet considerable controversy continues to surround the health risk associated with this chemical. For example, urinary concentrations of BPA have recently been associated with a shorter luteal phase but not with adverse effects on the follicular phase length, TTP or early pregnancy loss (Jukic et al. 2015). In a subsequent study of women (n = 44) attending a fertility clinic (Fujimoto et al. 2011), serum unconjugated (free) BPA concentrations were measured by HPLC. In this study, the median unconjugated BPA was 2.53 ng/ml and ranged from non-detectable to 67.4 ng/ml. Serum BPA concentrations were inversely associated with E2 (β = −0.16; 95 % CI = −0.32, 0.01) and with E2 concentration normalized to the number of mature-sized follicles at the human chorionic gonadotropin (hCG) trigger (β = −0.14; 95 % CI = −0.24, −0.03). However, the concentration of unconjugated BPA in the serum was not associated with oocyte maturation rate, but intracytoplasmic sperm injection (ICSI) or conventional IVF patients had a 55 % decrease in the probability of fertilization for each doubling in BPA levels (adjusted relative risk = 0.45, 95 % CI = 0.21–0.66). Although preliminary, these data suggest that free BPA in the circulation is potentially associated with a reduced serum E2 response to ovarian stimulation in IVF and reduced fertility. Limitations of the above studies are the focus on study participants who are attending fertility programs and thus are not necessarily representative of the population overall.
3 Exposure Data
Insight into whole body and target tissue exposure is essential for dose setting in experimental studies as well as for transparent and defensible evidence-based regulatory decisions and advice to guide industry action. However, exposure data is frequently lacking for many environmental contaminants and quantification of target tissue exposure is complicated by difficulty in accessing the ovary and ovarian follicular fluid. Therefore, understanding the relationship between circulating concentrations of contaminants and the concentrations in the follicular fluid is potentially valuable. Herein we summarize the available exposure data and explore the relationship between serum and follicular fluid concentrations .
Advances in analytical chemistry have enabled the measurement of increasingly smaller concentrations of environmental contaminants, many with reproductive and developmental toxicity, in the human circulation and reproductive fluids (Calafat et al. 2008; Silva et al. 2004). Environmental contaminants have been quantified in serum (Bloom et al. 2007, 2011; Fujimoto et al. 2011; Mahalingaiah et al. 2012; Younglai et al. 2002) and ovarian follicular fluid (Baukloh et al. 1987; Foster et al. 1995; Ikezuki et al. 2002; Jarrell et al. 1993; Jirsova et al. 2010; Neal et al. 2008; Trapp et al. 1984, 1990; Younglai et al. 2002) of women participating in assisted reproductive therapy (ART) programs . Although exposure to environmental contaminants has been linked to adverse effects on fertility (Bloom et al. 2011; Fujimoto et al. 2011; Ikezuki et al. 2002; Mahalingaiah et al. 2012; Takeuchi et al. 2004; Younglai et al. 2002), the available literature is limited to studies involving patients attending ART programs and thus is not representative of the general population. Thus improved methods of estimating target tissue exposure are needed.
Organofluorine compounds include the surfactants perfluorooctane sulfonic acid (PFOS) and perfluorooctanoic acid (PFOA); used as stain repellents in the manufacture of textiles, carpets and furniture (La Rocca et al. 2012), have been measured in follicular fluid (Petro et al. 2014). A study on the effects of long-term PFOS exposure in drinking water (Knox et al. 2011) found serum levels of 16.9 ± 9.9 19.1 ± 12.9 and 24.8 ± 16.3 ng/ml for 3 age groups (18–42, 43–51 and 52–65 years, respectively). PFOS exposure was negatively associated with estrogen levels (E2 decreased from ~88 to 72 pg/ml, p < 0.0001 and ~32 to 22 pg/ml, p < 0.007, for the 1st compared to the 5th quintile of PFOS levels, respectively) in the two oldest age groups described above. Similarly there was an increased odds of experiencing early menopause for the 5th vs. the 1st quintile of PFOS concentrations (OR, 95 % CI = 1.4, 1.1–1.8 and 2.1, 1.6–2.8 for both age groups, respectively). A positive effect of PFOA levels in follicular fluid on fertilization rate and proportion of viable embryos collected from IVF patients has been described (Petro et al. 2014); however, the mechanism for this effect is unclear. A study of 53 couples attending a fertility clinic in Italy (La Rocca et al. 2012) revealed that patients with unexplained infertility had detectable PFOS (>0.5 ng/g whole blood). Of those exhibiting infertility factors (PCOS, endometriosis or male-factor infertility), 30 women had >20-fold lower limit (3–144 ng/g). Whole blood PFOA concentrations were below the detection limit in 90 % of samples. It is worth noting that serum and follicular fluid concentrations of the perfluorinated compounds are close to identical (Petro et al. 2014) suggesting that serum concentrations are useful surrogate markers of target tissue exposure.
The concentrations of total BPA (free + conjugated) in the serum from healthy non-pregnant and pregnant women, and follicular fluid from women attending an IVF clinic have been reported (Ikezuki et al. 2002). Concentrations ranged from 1.4 ± 0.9 to 2.4 ± 0.8 ng/ml in most cases suggesting exposure to BPA in women. While these data suggest exposure of estrogen sensitive target tissues at critical stages of steroid regulated development, these reports are limited to measures of total BPA and thus the concentration of the bioactive form of BPA, free BPA, in ovarian follicular fluid remains unknown. Polycystic ovarian syndrome (PCOS) and serum concentrations of BPA were linked through two independent studies, one conducted in Japan and the other in Greece (Kandaraki et al. 2011; Tsutsumi 2005). Serum BPA concentrations were 0.64 ± 0.1 for normal cycling women compared to 1.04 ± 0.1 ng/ml for women with PCOS (Tsutsumi 2005). In the second study (Kandaraki et al. 2011), women referred to a PCOS clinic were stratified by BMI and serum BPA concentrations were again higher in women with PCOS and a BMI ≥25 (0.96 ± 0.46 vs. 0.72 ± 0.39 ng/ml, p < 0.05) or <25 (1.13 ± 0.63 vs. 0.70 ± 0.36 ng/ml, p < 0.001) compared to healthy cycling women, respectively. However, the antibody based ELISA method employed to quantify circulating BPA concentrations in these studies employed an antibody with significant cross reactivity with BPA metabolites and thus the assay cannot discriminate between free (bioactive) BPA and its metabolites. Therefore, it is unclear, on the basis of this evidence, what role if any BPA may play in the development or progression of this disease. Free BPA could not be detected in the follicular fluid of women (Krotz et al. 2012) raising further concern that the reported link between BPA and PCOS may be spurious; however, we note that the data in this study is limited to only five study subjects and thus cannot be taken as conclusive. Regardless of the findings with free BPA, the authors were able to quantify phthalate metabolites in ovarian follicular fluid of these same five women suggesting that technical limitations are unlikely to account for the failure to detect free BPA in these samples. The phthalate metabolites quantified in the follicular fluid included: mono-2-ethylhexyl phthalate (m-EHP, 9.34 ± 3.33 ng/mL), monoethyl phthalate (m-EP, 3.19 ± 2.97 ng/mL), mono-n-butyl phthalate (m-BuP, 1.62 ± 0.59 ng/mL) and monomethyl phthalate (m-MP, 1.19 ± 0.25 ng/mL) (Krotz et al. 2012) but these concentrations are considered to be 200–1000 times lower than those harmful to reproductive function in laboratory animals (Kay et al. 2013). Therefore, although human exposure is recognized as wide-spread, the concentrations present in the ovary are thought too low to have an adverse effect. While regulatory action seems inappropriate, health conscious individuals who remain concerned can minimize their personal exposures to these chemicals through consumption of fresh foods and reducing personal exposure to plastics and canned goods.
Finally, parabens are another group of contemporary chemicals used as anti-microbial agents in the production of cosmetics, food and pharmaceuticals (Ahn et al. 2012; Taxvig et al. 2008). Urinary parabens concentrations were measured in patients attending a fertility clinic (Smith et al. 2013) yielding median concentrations of 158, 35.5 and 1.53 μg/L for methyl, propyl and butyl parabens (mPB, pPB and bPB), respectively. Although serum or follicle fluid levels were not measured, the authors suggested a correlation between urinary paraben concentrations and ovarian reserve. This provocative suggestion requires additional study in both clinical samples and animal studies to confirm and explore potential mechanisms of action. Although widely appreciated, we feel compelled to remind the reader that evidence of exposure cannot be equated with evidence of an adverse health effect or increased risk of an adverse health outcome at a later date. Risk is the product of exposure, evidence of a health hazard usually derived from experimental animal studies and an uncertainty factor that accounts for differences between experimental animals and humans.
4 Experimental Animal Evidence
Well-controlled animal studies allow for testing with known concentrations of pure test compounds, using relevant routes of exposure, to genetically homogenous animals at well-defined developmental stages, and under carefully regulated environmental conditions that cannot be replicated in human populations. Consequently, animal studies are important to understanding the potential health hazards associated with exposure to environmental contaminants and contribute essential data to evidence based regulatory decisions.
Different reproductive and developmental toxicology test protocols have been developed by government bodies such as the Organization for Economic Cooperation and Development (OECD), the United States-Environmental Protection Agency (US-EPA), and the National Toxicology Program (NTP). While these protocols exploit good laboratory practices rendering their results highly reproducible and thus attractive for regulatory purposes, they have been criticized for the superficial nature of the outcome measures employed and lack of mechanistic insight. Animal testing for reproductive and developmental effects using these protocols provides indirect evidence for toxicant effects on ovarian function as shown by changes in estrous cycle length, sexual maturation, fertility index, weight of reproductive organs and histology, and circulating reproductive hormone concentrations. By comparison, academic scientists operate in less restrictive environments and thus are able to develop innovative protocols designed to assess reproductive function and provide mechanistic insight that is lacking in traditional regulatory toxicity testing paradigms. For example, a series of elegant studies have shown that BPA exposure can affect oogenesis and aneuploidy in mouse and non-human primate oocytes (Hunt et al. 2003, 2012), insight that could not be achieved through traditional testing paradigms. Moreover, access to primary (Haney et al. 1984) and immortalized ovarian granulosa cell lines (Kwintkiewicz et al. 2010) has also allowed for direct assessment of test chemical effects. Recent developments have seen the introduction of isolated ovarian follicle cultures employed to assess test chemical effects on stage dependent effects of follicle growth, steroidogenesis, follicle survival, and ovulation (Cortvrindt et al. 1998; Cortvrindt and Smitz 2002; Lenie et al. 2004; Lenie and Smitz 2009; Neal et al. 2007, 2010; Sadeu and Foster 2011a, b; Van Wemmel et al. 2005), a model that has been extended to three dimensional cultures of follicles (Songsasen et al. 2011). While these studies provide much needed mechanistic insight, they suffer from the need for sophisticated testing, and high level of expertise in the field. Regardless of their limitations, results arising from both regulatory and academic scientific studies contribute essential data to the risk assessment process and thus are central to evidence based regulatory decisions. Chief among the effects detected are depletion of the ovarian follicle reserve, interference with the cumulus oocyte complex (COC) communication, and steroidogenesis.
4.1 Effects on Ovarian Reserve
With each menstrual cycle, a cohort of primordial follicles enters one of the waves of growing follicles (Baerwald et al. 2003a, b). Typically one follicle from the growing pool of follicles is selected to ovulate while the remainder become atretic. Of the estimated 500,000 follicles present in the human ovary at the start of reproductive life, only about 400 reach the pre-ovulatory stage and ovulate whereas follicle atresia is the fate for the vast majority of female germ cells (Byskov 1978). The number of follicles formed in utero, the rate of recruitment into the growing pool, and rate of follicle destruction are all potentially modifiable by environmental contaminant exposure with important implications to fertility, sterility, premature ovarian failure, and menopause. Indeed, contaminant exposures that disrupt the number of follicles formed during development, affect the rate of follicle recruitment, follicle development, or follicle loss can have serious implications for circulating steroid concentrations, fertility, and ultimately the reproductive life span for a woman. Since estrogens are important mediators of cell proliferation, neurogenesis, growth and maintenance of bone, and cardiovascular health, the consequences to general health arising from ovarian toxicity are potentially profound and reach across the life span with important implications to health care needs and costs.
Contaminant exposure in adult animals has been shown to decrease ovarian follicle counts but the most sensitive follicle stage to the toxic effects of environmental contaminants is variable. For example, 4 vinylcyclohexene diepoxide (VCD) has been shown to selective target primordial and primary follicles (Appt et al. 2006; Sahambi et al. 2008; Sobinoff et al. 2010), the follicles at the earliest stages of development. Similar effects have also been shown with polycyclic aromatic hydrocarbons such as 9,10- dimethyl benzanthracene, 3-methylcholanthrene, and benzo[a]pyrene and (Borman et al. 2000), all of which involve activation of the apoptosis pathway. Of note, repeated exposure to low concentrations may be more toxic that exposure to a single high concentration of an environmental contaminant (Borman et al. 2000), an effect that could have important implications for humans who are typically exposed to low concentrations of contaminants over long periods of time. Similar effects on follicle counts have been demonstrated with several different POPs. For example, PCB treatment-related increase in ovarian follicle loss (Baldridge et al. 2003) has been documented with fewer preantral follicles (15 ± 0.6 vs. 56 ± 0.7/section, p < 0.05), and fewer small and large antral follicles (18 ± 0.9 vs. 41 ± 2 and 8 ± 0.9 vs. 30 ± 0.6/section, respectively, p < 0.05), as well as more atretic follicles (59 ± 0.9 vs. 26 ± 1.2, p < 0.05). Similarly, in a study on the long-term reproductive effects of dioxin exposure (Franczak et al. 2006), prepubertal rats were treated orally with vehicle or 10 μg TCDD/kg at 29 days of age (acute treatment) while pregnant rats were treated (0, 50 or 200 ng/kg) on GD 14, 21 and postnatal D7 and 14. Subsequently, the female pups were given the same weekly doses until 8 months of age (chronic treatment). The acute treatment delayed (p < 0.05) vaginal opening (37.8 ± 1.5 vs. 33.2 ± 1.0 d), reduced reproductive lifespan (287.2 ± 9.7 vs. 319.2 ± 4.1d), and prolonged diestrus (0.65 ± 0.01 vs. 0.58 ± 0.02 of cycle). Treatment also reduced E2 output (p < 0.05). Chronic treatment had no effect on follicle and corpus luteum numbers or structure but at 8 months only 25–30 % of treated females showed normal cycles (vs. 100 % in controls, p < 0.05). Although the two largest doses of TCDD used accelerated reproductive ageing (fewer had normal cycles at 9 and 11 months, p < 0.05), there was no effect of TCDD treatment on follicle counts (Shi et al. 2007). In another study TCDD (0 or 5 μg/kg, i.p.) treatment decreased ER gene expression in the ovary and other tissues in 6-to-8-week-old mice (Tian et al. 1998). Available studies have primarily evaluated the effect of test chemicals under basal conditions. In a provocative study (Jung et al. 2010), TCDD treatment decreased ovulation rate (2.7 ± 1.9 vs. 20.3 ± 3.6, p < 0.05) and increased Aryl hydrocarbon Receptor (AhR) expression in granulosa cells in 25-day-old rats treated with 1 dose of TCDD (0 or 32 μg/kg, by gavage) plus hCG and LH (1 and 3 d later, respectively) to induce follicle development and ovulation. Treatment also decreased the number of follicles available for ovulation. Taken together these data suggest that TCDD may have direct effects upon the ovary although the mechanisms remain to be determined.
In addition to direct effects of TCDD in adults, evidence has been brought forward in the literature that suggests effects may be transmitted across generations. In a transgenerational study (Nilsson et al. 2012), F3 females also exhibited fewer primordial follicles than controls (~14 to 9, p < 0.005), with no effect on antral follicle counts, but developed cystic structures similar to PCOS following treatment of pregnant rats with TCDD (0 or 100 ng/kg BW/d i.p.) on gestation day (GD) 8–14. However, the underlying mechanisms remain unclear.
Clinical markers of adverse effects of environmental contaminants on ovarian function are sparse; however, AMH has received increasing interest as a marker of ovarian reserve and has been used in toxicology to access Methoxychlor (MXC) effects on the ovary. In a developmental study (Masutomi et al. 2003), rats were treated with MXC (0, 24, 240, or 1200 ppm in the diet) from GD 3 to PND 21. Only the highest dose (1200 ppm) decreased body and ovarian weight, accelerated vaginal opening, and caused irregular estrous cycles. Furthermore, longer estrous cycles (6.28 ± 1.91 vs. 3.76 ± 0.25 days, p < 0.001), fewer corpora albicantia from previous cycles, fewer corpora hemorrhagica, and more degenerate oocytes were found in MXC treated rats (Quignot et al. 2012a, b). MXC (0, 1, 10, 50, 100, or 500 mg/kg/d) exposure from 3 to 10 days of age resulted in antral follicle loss but increased the growing follicle pool, and increased AMH expression at 20 days of age (Uzumcu et al. 2006). Doses of 50, 100, and 500 led to 1.6 ± 0.2, 1.85 ± 0.6 and 2.2 ± 0.5 times the AMH expression of the control group (p < 0.05), as measured using immunohistochemistry. Antral follicle counts were reduced (~6/section after 100 or 500 mg, vs. ~17 in controls, p < 0.05), whereas preantral follicles increased (~13 and 15 after 100 and 500 mg, vs. ~8 in controls, p < 0.05). The effects of VCD on circulating AMH concentrations (Sahambi et al. 2008) further support the notion that AMH is a potentially useful minimally invasive marker of toxicant effect.
The adverse effects of legacy chemicals such as the POPs on ovarian follicle counts are not unique and can be extended to contemporary commercial chemicals such as BPA. In a study on prenatal exposure (Markey et al. 2003), pregnant mice were exposed to BPA on GD 9 to term (via s.c. pump delivering 0, 25 or 250 μg/kg/day). Treatment did not affect age at vaginal opening, but more mice showed persistent estrus/metestrus (≥4 days) after exposure to 25 μg (55.7 %) and 250 μg (55.6 %) than controls (37.1 %, p < 0.05). A proportion of exposed females showed blood-filled ovarian bursae at 3 months (11 and 16 vs. 0 %), and those exposed to 250 μg had a greater ovarian area occupied by antral follicles (15.5 ± 2.7 vs. 6.4 ± 2.8 %, p < 0.05). In a transgenerational study (Nilsson et al. 2012), pregnant rats were treated with BPA (0 or 50 mg/kg BW/d i.p.) on GD 8–14, F3 females exhibited fewer primordial follicles than controls (~14 to 9, p < 0.005), with no effect on antral follicle counts, but developed cystic structures similar to PCOS.
In another study on pre- and postnatal exposure (Signorile et al. 2012), pregnant mice were treated with BPA (0, 100 or 1000 μg/kg) on GD 1-PND 7. Exposed females showed fewer primordial follicles (median numbers: 7.75, 3.8 and 2.65, respectively, p < 0.001), reduced numbers of developing follicles (11.9, 5.5 and 4.5, p < 0.001), and increased the number of atretic follicles (1.55, 3.3 and 3.4, p < 0.001). In another study (Xi et al. 2011), female mice and their pups were treated with BPA (0, 12, 25 or 50 mg/kg/d, by gavage) from GD 1 to PND 20, and from PND 20 to 49, respectively. Exposure led to a dose-dependent increase in E2 (~150, 300, 550 and 600 pMol/L), which altered feedback signals within the hypothalamic- pituitary-gonadal axis.
Neonatal exposure to BPA (PND 1, 3, 5 and 7) was examined (Rodriguez et al. 2010) in rats treated with oil (negative control), DES (positive control, 0.2 or 20 μg/kg) or BPA (0.05 or 20 mg/kg). BPA treatments (20 mg/kg) led to the highest proportion of recruited follicles on PND 8: ~30 % of follicles for control, ~45 % for DES0.2 (p < 0.001), ~40 % for DES20 (p < 0.01), ~55 % for BPA20 (p < 0.001), and ~30 % for BPA0.05 (NS). The BPA (20 mg/kg) dose also led to more EsR1-positive follicles than negative controls (~65 vs. 15 %, p < 0.05), which may explain the higher recruitment rate. In contrast, EsR2 positive staining was not affected by treatment. Taken together the data consistently show BPA exposure induced primordial follicle loss and suggest accelerated follicle recruitment into the growing pool.
In contrast to the examples of BPA, more primordial follicles and more primary follicles and altered gene expression for steroidogenic enzymes such as StAR and Cyp11a1 were found (Ahn et al. 2012) in rats treated with methyl, propyl or butyl parabens (mPB, pPB and bPB, respectively, at 0, 62.5, 250 or 1000 mg/kg/d each, s.c.) or E2 (40 μg/kg/d, positive control) for 7 days (PND 1-7). In a gestational exposure study (Taxvig et al. 2008), rats were exposed to s.c. oil, ethyl paraben (ePB, 400 mg/kg/d) or bBP (200 or 400 mg/kg/d) on GD 7-21. The females and the fetuses showed no histologic alterations in the ovaries, but treatment increased EsR2 gene expression. Additionally, female rats maternally exposed to bPB from GD 6 to PND 20 (100 mg/kg/day) presented early vaginal opening with no alterations in ovarian weight and histology (Kang et al. 2002), possibly due to the estrogenic action of parabens in the female HPG axis during development. In contrast, prepubertal mPB and isopropyl paraben exposure (250 and 1000 mg/kg from PND 21-40) leads to a delay in vaginal opening, a decrease in the number of corpora lutea and an increase in the number of cystic follicles in the ovary (Vo et al. 2010).
In summary, multiple contaminants from different chemical classes have been shown to affect ovarian follicle counts and thus establish the ovary as a potentially important target organ for adverse effects of environmental contaminant exposure. Moreover, we postulate that the accelerated loss of primordial follicles has the potential to shorten reproductive life span as well as advance the age of onset for health problems such as osteoporosis and cardiovascular disease arising from loss of estrogen. The mechanisms of ovarian follicle loss are unclear and may include decreased number of oocytes and follicles formed during development (Yin et al. 2015), increased recruitment of follicles into the growing pool (Rodriguez et al. 2010), and increased rate of follicle loss through either apoptosis (Jurisicova et al. 2007; Matikainen et al. 2001; Takai et al. 2003) or autophagy (Gannon et al. 2012, 2013). Regardless of the mechanism, the underlying initiating events remain to be elucidated and have important implications for fertility preservation as well as life-long health benefits. Tissue culture studies have shown that the adverse effects of polycyclic aromatic hydrocarbons such as benzyo[a]pyrene can be attenuated by co-treatment with AhR antagonists such as resveratrol and 3,4 dimethoxyflavone (Casper et al. 1999; Neal et al. 2010). These data raise the encouraging possibility that the ovary can be protected from the adverse effects of some contaminants on ovarian follicle loss. Fertility preservation is an exciting area of reproductive biology that is receiving renewed interest which we anticipate will uncover novel therapeutic interventions to protect ovarian function.
4.2 Steroidogenesis
Steroid production in the ovary is regulated by gonadotrophins and involves androgen production by theca cells and subsequent conversion of androgens to estrogens by granulosa cells . Results of animal studies demonstrate that CdCl2 exposure decreased serum E2 and P4 concentrations by altering expression and/or activity of granulosa cell steroidogenic enzymes P450scc and StAR in adult female rats injected s.c. with CdCl2 (0, 2.5, 5 and 7.5 mg/kg) (Zhang and Jia 2007; Zhang et al. 2008). CdCl2 has a MW of 183, but only 112 of it is Cd. 1M would be 112 g/L; 1 μM would be 112 μg/L; 20 μM (lowest significant effect) would be 2.24 mg/L, a level much higher than the 0.29 ± 0.30 μg/l reported in follicular fluid in Saudi Arabian women for both controls and women under fertility treatment (Al-Saleh et al. 2008). Lead acetate was given to adult rhesus monkeys over several years at different doses (3.6, 5.9 and 8.1 mg/kg/d) in drinking water (Laughlin et al. 1987). Lead was detected in blood at concentrations that ranged between 51 and 88 μg/dl. Although the monkeys were still fertile, treated females showed menstrual cycles that were longer (50.9 vs. 32.9 days) and more variable, with shorter menses (2.3 vs. 3.4 d, p < 0.05). Chronic lead exposure suppressed circulating concentrations of LH, FSH and E2 in cynomolgus monkeys (Foster 1992) and suppressed luteal function at moderate blood levels (Foster et al. 1996).
Toxic effects of phthalates and phenols in experimental animal studies have been examined by several authors (Guerra et al. 2010; Kimura et al. 2006; Laskey and Berman 1993; Masutomi et al. 2003; Nagao et al. 2000; Willoughby et al. 2005) and have recently been reviewed elsewhere (Kay et al. 2013). Pregnant rats were exposed to di-η-butyl-phthalate (DBP) from GD 12 to PND 21 (0 or 100 mg/kg/d by gavage); the dose used did not affect ovarian development, puberty, hormone levels or fertility (Guerra et al. 2010). In another study (Masutomi et al. 2003), rats were treated with diisononyl phthalate (DINP, 0, 400, 4000, or 20,000 ppm in the diet) from GD 3 to PND 21; the highest dose decreased body and ovarian weight, whereas the lower doses had no adverse effects. Using a different approach, adult rats were treated with bis(2-diethylhexyl) phthalate (DEHP) (0 or 1500 mg/kg/day by gavage) for 10 days and their ovaries collected at different cycle stages for culture and measurement of steroid output (Laskey and Berman 1993). In diestrus, treated rats produced more E2 and testosterone than controls, whereas in estrus, they produced more E2. Another study (Mlynarcikova et al. 2009) also evaluated the effects of phenols and phthalates, by treating cumulus-oocyte- complexes (COCs) with 4-Chloro-3-methyl phenol (CMP), di(2-ethylhexyl) phthalate (DEHP) and benzyl butyl phthalate (BBP), in a range of 102–10−4 μM. Only the highest levels of CMP and BBP decreased COC expansion rate. The highest level of CMP decreased oocyte maturation rate (50.0 % reached metaphase II (MII) vs. 81.5 % in controls; p < 0.001) and only the second highest level of DEHP increased P4 output (~50 % more than control p < 0.05). In another study from this group (Mlynarcikova et al. 2007), porcine granulosa cells were treated with 10−8M to 10−4M 4-octylphenol (OP), 4-nonylphenol (NP), and 4-tert-octylphenol (tOP), diisononyl phthalate (DiNP), diisodecyl phthalate (DiDP) or dioctyl phthalate (DOP), with or without FSH. OP (10−5M) reduced P4 output (p < 0.05), and NP (10−8 M) decreased E2 output (p < 0.05). FSH stimulated E2 concentration in the media was reduced by OP, NP (p < 0.05), as well as DiDP and DiNP (p < 0.01) treatment. Taken together these data suggest that ovarian steroidogenesis can be affected by some of the phenols and phthalates used as plasticizers. To evaluate the effect of phthalate treatment on oocyte maturation equine COCs were incubated with di-(2-ethylhexyl) phthalate (DEHP) at 0, 0.12, 12 or 1200 μM (Ambruosi et al. 2011). The lowest concentration of DEHP (0.12 μM) inhibited oocyte maturation (P < 0.05) with increased apoptosis and reduced ROS levels (p < 0.001). Higher concentrations did not affect oocyte maturation, but apoptosis and ROS were higher (p < 0.0001). Treated oocytes also exhibited higher ATP content (p < 0.05). Taken together these data suggest that the COC is sensitive to the adverse effects of environmental contaminants; however, the underlying mechanisms are uncertain. We postulate that contaminant effects on gap junction communication are an area that may yield interesting results (Ganesan and Keating 2014; Gittens et al. 2003, 2005; Kidder and Mhawi 2002; Li et al. 2007).
While contaminant effects on ovarian steroidogenesis have been established, the mechanisms remain ill-defined and thus different culture methods have been employed in an effort to clarify this issue. Cocultures of granulosa and theca cells were isolated from pig antral follicles (Ptak et al. 2006) and treated with 4-Chlorobiphenyl (PCB3) or two of its metabolites (4-OH or 3,4-diOH PCB3, at 6 ng/ml). PCB3 and metabolite treatment decreased P4 output by 55–65 % and 70–80 % of control (p < 0.05), respectively. All 3 compounds increased E2 output (130–330 % of controls, p < 0.05), via increasing P4 conversion to androgen and subsequently androgen aromatization. Chronic TCDD exposure upregulated the expression of 19 genes of known function (e.g. Cyp1a1, indicating activation of AHR) and downregulated the expression of 31 genes (e.g. 17α-OHase); FSH receptor, aromatase and inhibin were not affected (Valdez et al. 2009). Thus, TCDD alters ovarian steroidogenesis by affecting genes related to androgen synthesis. Similarly, rat granulosa cells from punctured follicles treated with 2,2-bis-(p-hydroxyphenyl)-1,1,1-trichloroethane (HPTE, the main metabolite of methoxychlor) produced a dose-dependent inhibition of P4 output, blocked FSH-induced P450scc, 3β-HSD and P450arom mRNAs, but not StAR (Zachow and Uzumcu 2006). Thus, HPTE alters steroidogenesis by inhibiting several of the corresponding enzymes. The cells were incubated for 48 h with androgens (as aromatase substrates) and FSH (30 ng/ml) in the presence or absence of HPTE (0.1, 1, or 10 μM). The effects of methoxychlor (MXC) on ovarian steroidogenesis have been demonstrated by treating granulosa cells from pig antral follicles for 48 h with DDE (100–103 μM) or MXC (10−2–101 μM), E2 (0.1 μM, positive control) or negative control (10 % new born calf serum), with a final FSH exposure (Chedrese and Feyles 2001). In addition to stimulating cell proliferation, DDE affected FSH-induced cAMP production. MXC inhibited P4 but not cAMP. The authors concluded that the mechanism appeared to be non-estrogenic. In rats, exposed prenatally (GD 19–22) and postnatally (PND 0–7) to 0, 20 or 100 μg/kg/d MXC exhibited 83–100, 78─100 and 0–11 % regular cycles and E2 levels of ~27, 20, 18 pg/ml, respectively (p < 0.05), at 13–15 months of age (Gore et al. 2011).
In tissue culture experiments (Grasselli et al. 2010), granulosa cells aspirated from pig antral follicles were treated with BPA (0, 0.1, 1, or 10 μM) and cell proliferation, E2, P4, and VEGF output were measured. Cell proliferation was not affected by BPA whereas the lowest dose of BPA increased estradiol, while the two higher ones inhibited it (p < 0.001), and all BPA levels inhibited progesterone (p < 0.01). VEGF output was increased after treatment with 1 and 10 μM BPA (p < 0.05). The authors concluded that BPA alters follicle steroidogenesis and VEGF production. In one study (Mlynarcikova et al. 2005), granulosa cells from pig antral follicles were treated with BPA or BPA-dimethacrylate (DMA) at 10−4–10−8 M and E2 and P4 output was determined. P4 concentrations were increased by 10−6 BPA treatment (p < 0.05) whilst 10−4 BPA inhibited P4 output (p < 0.001). At all concentrations tested, BPA inhibited FSH-induced E2 production (p < 0.05). In another study (Mlynarcikova et al. 2009), porcine COCs were treated with BPA (102–10−4 μM) during FSH-induced oocyte maturation. Subsequently, cumulus expansion, oocyte maturation and P4 output were determined. Only the highest BPA concentration tested reduced the COC expansion rate compared to controls (16.9 % vs. 39.3 %, p < 0.05), oocyte maturation rate (50.0 % reached MII vs. 81.5 %, p < 0.001), and P4 output (47.4 % less than controls, p < 0.01). Although equivocal, the data lend some support to the observation that BPA is associated with an impaired response to ovulation induction (Fujimoto et al. 2011).
Human cells have also been used to study potential ovariotoxic effects. KGN cells, an ovarian granulosa-like tumour cell line that expresses a functional FSH receptor, as well as human granulosa cells (GLC) from IVF patients were treated with BPA (0, 40, 60, 80 or 100 μM), with or without FSH (Kwintkiewicz et al. 2010). In the KGN cells, BPA exhibited a dose-dependent reduction on FSH-induced IGF1, aromatase and E2. In the GLC, only aromatase was examined, with similar effects to those seen in KGN cells (but the cells were more sensitive to lower doses). BPA also induced PPARγ, an aromatase inhibitor, which was seen as a possible mechanism for lower aromatase expression. Human fetal (21–22 weeks) ovarian explants were incubated with BPA (0 or 30 μM) for 1, 2 and 3 weeks (Brieno-Enriquez et al. 2012). Oocytes and fibroblasts were isolated for RNA extraction. BPA led to higher expression (p < 0.05) of genes related to double-strand break generation, signaling and repair (Rpa, Spo11, H2ax, Blm, Stra8, Nalp5), onset of meiosis (Stra8), estrogen receptors and primordial follicle formation (Nalp5). However, the importance of these findings to risk assessment is unclear in the absence of accurate measures of free BPA concentrations in the follicular fluid. Assuming that the total BPA concentrations previously reported in follicular fluid were composed entirely of free BPA then the concentrations as added to the culture media used in this study would be approximately 4500 times greater than the concentrations measured in follicular fluid.
Isolated ovarian follicle culture techniques have been developed to assess the effect of test chemicals on stage-dependent follicle development and ovulation (Sun et al. 2004). In one study (Lenie and Smitz 2009), mouse follicles were isolated and cultured for 12 days to determine follicular development. Ovulation was stimulated (with recombinant hCG and recombinant epidermal growth factor), and evaluated on day 13. During development, follicles were exposed to the active metabolite of di (2-ethylhexyl) phthalate (DEHP), mono (2-ethylhexyl) phthalate (MEHP, 10–200 μM). MEHP led to a fivefold increase in P4 output by day 12, but no change after ovulation stimulus. Testosterone/E2 ratios showed that, despite increased testosterone output, less E2 was produced with increasing MEHP. In another study (Treinen et al. 1990), MEHP was added to cultures of rat granulosa cells collected from freshly ruptured follicles (the rats had been treated with DES to induce granulosa cell proliferation). MEHP decreased up to 40 % cAMP production. Treatments containing 10, 25, 50 and 100 μM MEHP produced 30, 35, 40 and 70 % less P4 than controls (p < 0.05), and cAMP production was similarly inhibited. Human granulosa cells from IVF patients were treated with MEHP (0 or 0.6–500 μM) and aromatase mRNA, cell viability and steroid output were measured. MEHP decreased aromatase and E2 output (Reinsberg et al. 2009) whereas P4 output and cell viability decreased only at the highest dose. The large variety of phthalate compounds appears to have varying effects, and again, most studies involve laboratory animals, where significant effects are seen only at higher concentrations. The lowest dose with an effect was 0.12 μM of DEHP (Ambruosi et al. 2011), a dose equivalent to 47 μg/L (or ng/mL); a concentration that is substantially higher than the highest concentration of a phthalate metabolite (9.3 ng/ml) previously measured in follicular fluid (Krotz et al. 2012). In preliminary data from our lab, using an isolated mouse ovarian follicle culture system, BPA treatment significantly decreased the number of follicles as a percentage of the controls progressing to the preantral (18.04 ± 5.5 %), antral (28 ± 13.7 %) and preovulatory (54.5 ± 20.4 %) stage, and follicle survival (50.6 ± 18.8 %), but only at the highest concentration (5.0 μM) tested (Fig. 7.1). Treatments had no effect on gonadal steroid output in these cultures (Fig. 7.2). Thus, effective concentrations as added in cultures ranged between 1.14 and 2.28 mg of BPA/ml; concentrations far in excess of human exposure.
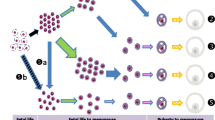
Effect of BPA-exposure on in vitro follicle growth and survival.
Follicular development at (a) 4, (b) 8, and (c) 12 days of culture and (d) follicular survival at 12 days of culture. All the follicles were follicular at day 0 (start) of culture. Each experiment was repeated at least 3 times in duplicate plate/condition, n = 826 follicles (10–16 follicles/plate). Bars with different letters (within the same follicular stages) differ significantly (p < 0.05)
Effect of BPA-exposure on steroid outputs during in vitro follicle growth. (a) Estradiol (E2) and (c) progesterone (P4) outputs after antral (Day 8) and preovulatory (Day 12) follicle development. Relative average increase of (b) E2 between Days 8 and 12 [(Day 12/Day 8) × 100] and of (d) P4 between Days 12 and 13 [(Day 13/Day 12) × 100]. Values are means ± S.E.M. E2: n = 4–8 replicates; P4: n = 4–5 replicates
4.3 Genetic and Epigenetic Effects
The mutagenic effects of environmental toxicants have been well documented and effects on DNA repair mechanisms have also been described (Ganesan et al. 2013, 2014; Ganesan and Keating 2015). In addition to transcriptional regulation of genes through toxicant changes in transcription factor expression and microRNA (miRNA), contemporary studies have revealed that contaminant exposures are also associated with changes in the epigenome involving histone modifications including DNA methylation. Marks on the DNA that regulate gene expression and may be carried across generations.
Epigenetic effects of dietary factors such as phytoestrogens and environmental contaminants have been documented on the rodent uterus and lung whereas effects on the ovary remain largely unexplored (Zama and Uzumcu 2010). In one study identified in our literature search (Zama and Uzumcu 2009), MXC induced treatment-related effects on estrous cyclicity, ovarian steroidogenesis, and produced changes in DNA methylation with potential effects across generations. Effects of MXC on DNA methylation have been documented in pregnant rats exposed to MXC (0, 20 μg or 100 mg/kg/d i.p.) from GD 19 to PND 7. Female pups were also treated from day 0 to PND 7 and euthanized after a cycle on PND 50-60. DNA methylation showed that 10 ovarian genes were hypermethylated after the highest MXC dose, including genes related to follicle maturation and ovulation, such as PAPP-A. Ovarian EsR1 was not affected, but EsR2 expression was reduced with 100 mg MXC (19.9 ± 1.06 vs. 36.7 ± 5.47, p < 0.05). Environmental contaminant-induced changes in ovarian epigenetic marks is an important emerging area in reproductive biology that holds great promise for increased mechanistic insight.
5 Future Directions
Understanding the hazard to reproductive health and ovarian function arising from exposure to environmental contaminants is difficult to appreciate in the absence of direct measures of exposure and more sensitive markers of an adverse effect. While circulating concentrations of AMH provides insight into the primordial follicle count/ovarian reserve, there are a number of limitations with this marker that have yet to be adequately resolved. Specifically, changes in circulating concentrations of AMH as women age as well as relationship with BMI and health status such as PCOS and diabetes are yet to be defined and normal ranges are only generally established.
While the concentrations of some chemicals in the serum are representative of concentrations that can be measured in ovarian follicular fluid (e.g. perfluorinated compounds), this is not always the case as shown for p,p′-DDE which can be three times higher in the serum than the follicular fluid (Younglai et al. 2002). It is encouraging that good correlation has been shown between serum and ovarian follicular fluid concentrations of DDT and its metabolites (Mahalingaiah et al. 2012). Therefore, we suggest that the pharmacokinetics and pharmacodynamics of environmental contaminants are essential data for establishing relevant target doses for animal and tissue culture studies as well as for risk assessment purposes.
We note that animal studies are clearly indispensable in the assessment of potential hazards to human health and reproductive function. We propose that their contribution to the risk assessment process could be enhanced with greater attention to issues of comparative endocrinology. For example, emerging evidence suggests that women may have more than one wave of follicles developing for ovulation in a given cycle (Baerwald et al. 2003a, b; Baerwald and Pierson 2004). However, many questions remain and the relevance of these observations to human health, fertility and toxicology has yet to be defined. We further postulate that while the academic investigators enjoy a much less restrictive environment that favors development of innovative testing strategies to enhance understanding of the mechanisms underlying toxic phenomenon, greater insight into the dose used, route of exposure, and use of multiple dose groups would enhance uptake of study results by regulatory bodies. Finally, there have been many calls for studies of mixtures and we add to the cacophony of voices calling for such testing.
Finally, although the literature suggests that effects of environmental contaminants at concentrations typically measured in contemporary biomonitoring studies are unlikely, precaution is never a poor option. Overall, regulatory decisions appear to be effective in protecting the health of general population against adverse effects on ovarian function; however, we note that chemicals continue to enter the environment. Manufacturing practices have improved substantially over the last decades with reductions in chemical emissions or releases into the environment. However, leaching of chemicals from finished products continues to be a problem and thus is an issue for engineering to insure safety. While calls to regulatory authorities for chemical bans continue, we caution against replacement of suspected chemicals with alternatives that are potentially more hazardous to human health such as Bisphenol S and Bisphenol F, replacements for BPA (Eladak et al. 2015; Rosenmai et al. 2014). Toxicity testing has progressed substantially over the last several decades as techniques have improved and understanding of reproductive physiology and endocrinology have advanced. We note that it will never be possible to prove absolute safety; however, enhancements to existing regulatory testing paradigms and continued interest of academic investigators promises to insure that potential health effects of environmental contaminants are identified and brought forward in the literature for use in the risk assessment process. In addition to partnering with chemical engineers to identify safer alternatives, academic investigators are encouraged to explore mechanisms of action as well as potential therapeutic interventions that can protect the ovary and aid in fertility preservation. Renewed interest in this area could have spill-over benefits for women undergoing cancer therapies that are well known to damage ovarian health.
6 Conclusions
Human exposure to potential ovarian toxicants has not been well defined and of greater concern is the lack of data on internal exposure dose and measurement of parent and metabolite concentrations in the ovary. While there is a robust animal literature illustrating the potential hazard to ovarian function and reproductive health from exposure to environmental contaminants, the concentrations at which effects were documented were frequently orders of magnitude beyond human exposure. While a robust literature was uncovered, the environmental contaminants addressed represent only a very small proportion of the many thousands of chemicals in commercial use that enter the environment, the food chain, and ultimately result in human exposure. Thus the available literature provides only an incomplete picture of the potential impact of environmental contaminants on reproductive health and ovarian function. We note that some environmental contaminant exposures have been linked with decreased circulating concentrations of E2, shorter or longer menstrual cycle length, attenuated response to ovulation induction strategies, impaired fertility, and earlier menopause. However, the available literature is equivocal and highly variable with respect to study design, populations studied, sample size, exposure assessment, analytical methods employed, and outcomes assessed. Therefore, we propose that the state-of-the science is presently inadequate to conclude that exposure to environmental contaminants are or are not associated with adverse effects on ovarian function or human fertility.
References
Ahn HJ, An BS, Jung EM, Yang H, Choi KC, Jeung EB (2012) Parabens inhibit the early phase of folliculogenesis and steroidogenesis in the ovaries of neonatal rats. Mol Reprod Dev 79:626–636
Al-Saleh I, Coskun S, Mashhour A, Shinwari N, El-Doush I, Billedo G, Jaroudi K, Al-Shahrani A, Al-Kabra M, El Din Mohamed G (2008) Exposure to heavy metals (lead, cadmium and mercury) and its effect on the outcome of in-vitro fertilization treatment. Int J Hyg Environ Health 211:560–579
Alvarez S, Devouche E (2012) First French national survey on lifestyle and toxic factors in infertile couples. Gynecol Obstet Fertil 40:765–771
Ambruosi B, Uranio MF, Sardanelli AM, Pocar P, Martino NA, Paternoster MS, Amati F, Dell’Aquila ME (2011) In vitro acute exposure to DEHP affects oocyte meiotic maturation, energy and oxidative stress parameters in a large animal model. PLoS One 6:e27452
Appt SE, Kaplan JR, Clarkson TB, Cline JM, Christian PJ, Hoyer PB (2006) Destruction of primordial ovarian follicles in adult cynomolgus macaques after exposure to 4-vinylcyclohexene diepoxide: a nonhuman primate model of the menopausal transition. Fertil Steril 86(Suppl 4):1210–1216
Augood C, Duckitt K, Templeton AA (1998) Smoking and female infertility: a systematic review and meta-analysis. Hum Reprod 13:1532–1539
Baerwald AR, Pierson RA (2004) Endometrial development in association with ovarian follicular waves during the menstrual cycle. Ultrasound Obstet Gynecol 24:453–460
Baerwald AR, Adams GP, Pierson RA (2003a) Characterization of ovarian follicular wave dynamics in women. Biol Reprod 69:1023–1031
Baerwald AR, Adams GP, Pierson RA (2003b) A new model for ovarian follicular development during the human menstrual cycle. Fertil Steril 80:116–122
Baldridge MG, Stahl RL, Gerstenberger SL, Tripoli V, Hutz RJ (2003) Modulation of ovarian follicle maturation in Long-Evans rats exposed to polychlorinated biphenyls (PCBs) in-utero and lactationally. Reprod Toxicol 17:567–573
Batariova A, Spevackova V, Benes B, Cejchanova M, Smid J, Cerna M (2006) Blood and urine levels of Pb, Cd and Hg in the general population of the Czech Republic and proposed reference values. Int J Hyg Environ Health 209:359–366
Baukloh V, Bohnet HG, Trapp M, Heeschen W, Feichtinger W, Kemeter P (1987) Biocides in human follicular fluid. Ann N Y Acad Sci 442:240–250
Bloom MS, Buck Louis GM, Schisterman EF, Liu A, Kostyniak PJ (2007) Maternal serum polychlorinated biphenyl concentrations across critical windows of human development. Environ Health Perspect 115:1320–1324
Bloom MS, Kim D, vom Saal FS, Taylor JA, Cheng G, Lamb JD, Fujimoto VY (2011) Bisphenol A exposure reduces the estradiol response to gonadotropin stimulation during in vitro fertilization. Fertil Steril 96:672–677
Bloom MS, Fujimoto VY, Steuerwald AJ, Cheng G, Browne RW, Parsons PJ (2012a) Background exposure to toxic metals in women adversely influences pregnancy during in vitro fertilization (IVF). Reprod Toxicol 34:471–481
Bloom MS, Kim K, Kruger PC, Parsons PJ, Arnason JG, Steuerwald AJ, Fujimoto VY (2012b) Associations between toxic metals in follicular fluid and in vitro fertilization (IVF) outcomes. J Assist Reprod Genet 29:1369–1379
Boivin J, Bunting L, Collins JA, Nygren KG (2007) International estimates of infertility prevalence and treatment-seeking: potential need and demand for infertility medical care. Hum Reprod 22:1506–1512
Borman SM, Christian PJ, Sipes IG, Hoyer PB (2000) Ovotoxicity in female Fischer rats and B6 mice induced by low-dose exposure to three polycyclic aromatic hydrocarbons: comparison through calculation of an ovotoxic index. Toxicol Appl Pharmacol 167:191–198
Brieno-Enriquez MA, Reig-Viader R, Cabero L, Toran N, Martinez F, Roig I, Garcia Caldes M (2012) Gene expression is altered after bisphenol A exposure in human fetal oocytes in vitro. Mol Hum Reprod 18:171–183
Byskov AGS (1978) Follicle atresia. In: Jones R (ed) The vertebrate ovary. Plenum Press, New York, pp 533–562
Calafat AM, Ye X, Wong LY, Reidy JA, Needham LL (2008) Exposure of the U.S. population to bisphenol A and 4-tertiary-octylphenol: 2003–2004. Environ Health Perspect 116:39–44
Casper RF, Quesne M, Rogers IM, Shirota T, Jolivet A, Milgrom E, Savouret JF (1999) Resveratrol has antagonist activity on the aryl hydrocarbon receptor: implications for prevention of dioxin toxicity. Mol Pharmacol 56:784–790
Chandra A, Martinez GM, Mosher WD, Abma JC, Jones J (2005) Fertility, family planning, and reproductive health of U.S. women: data from the 2002 National Survey of Family Growth. Vital Health Stat 23:1–160
Chedrese PJ, Feyles F (2001) The diverse mechanism of action of dichlorodiphenyldichloroethylene (DDE) and methoxychlor in ovarian cells in vitro. Reprod Toxicol 15:693–698
Cohn BA, Cirillo PM, Wolff MS, Schwingl PJ, Cohen RD, Sholtz RI, Ferrara A, Christianson RE, van den Berg BJ, Siiteri PK (2003) DDT and DDE exposure in mothers and time to pregnancy in daughters. Lancet 361:2205–2206
Cooper GS, Klebanoff MA, Promislow J, Brock JW, Longnecker MP (2005) Polychlorinated biphenyls and menstrual cycle characteristics. Epidemiology 16:191–200
Cortvrindt RG, Smitz JE (2002) Follicle culture in reproductive toxicology: a tool for in-vitro testing of ovarian function? Hum Reprod Update 8:243–254
Cortvrindt RG, Hu Y, Liu J, Smitz JE (1998) Timed analysis of the nuclear maturation of oocytes in early preantral mouse follicle culture supplemented with recombinant gonadotropin. Fertil Steril 70:1114–1125
Davis BJ, Price HC, O’Connor RW, Fernando R, Rowland AS, Morgan DL (2001) Mercury vapor and female reproductive toxicity. Toxicol Sci 59:291–296
De FE, Porpora MG, Di DA, Ingelido AM, Cardelli M, Cosmi EV, Donnez J (2004) Dioxin-like compounds and endometriosis: a study on Italian and Belgian women of reproductive age. Toxicol Lett 150:203–209
De Felip E, di Domenico A, Miniero R, Silvestroni L (2004) Polychlorobiphenyls and other organochlorine compounds in human follicular fluid. Chemosphere 54:1445–1449
Dickerson EH, Sathyapalan T, Knight R, Maguiness SM, Killick SR, Robinson J, Atkin SL (2011) Endocrine disruptor & nutritional effects of heavy metals in ovarian hyperstimulation. J Assist Reprod Genet 28:1223–1228
Dvornyk V, Long JR, Liu PY, Zhao LJ, Shen H, Recker RR, Deng HW (2006) Predictive factors for age at menopause in Caucasian females. Maturitas 54:19–26
Dyer SM, Cattani M, Pisaniello DL, Williams FM, Edwards JW (2001) Peripheral cholinesterase inhibition by occupational chlorpyrifos exposure in Australian termiticide applicators. Toxicology 169:177–185
Eladak S, Grisin T, Moison D, Guerquin MJ, N’Tumba-Byn T, Pozzi-Gaudin S, Benachi A, Livera G, Rouiller-Fabre V, Habert R (2015) A new chapter in the bisphenol A story: bisphenol S and bisphenol F are not safe alternatives to this compound. Fertil Steril 103:11–21
Eskenazi B, Warner M, Marks AR, Samuels S, Gerthoux PM, Vercellini P, Olive DL, Needham L, Patterson D Jr, Mocarelli P (2005) Serum dioxin concentrations and age at menopause. Environ Health Perspect 113:858–862
Farr SL, Cooper GS, Cai J, Savitz DA, Sandler DP (2004) Pesticide use and menstrual cycle characteristics among premenopausal women in the Agricultural Health Study. Am J Epidemiol 160:1194–1204
Foster WG (1992) Reproductive toxicity of chronic Lead exposure in the female cynomolgus monkey. Reprod Toxicol 6:123–131
Foster WG (1995) The reproductive toxicity of Great Lakes contaminants. Environ Health Perspect 103(Suppl 9):63–69
Foster WG (2003) Do environmental contaminants adversely affect human reproductive physiology? J Obstet Gynaecol Can 25:33–44
Foster WG, McMahon A, Younglai EV, Jarrell JF, Lecavalier P (1995) Alterations in circulating ovarian steroids in hexachlorobenzene-exposed monkeys. Reprod Toxicol 9:541–548
Foster WG, McMahon A, Rice DC (1996) Subclinical changes in luteal function in cynomolgus monkeys with moderate blood lead levels. J Appl Toxicol 16:159–163
Franczak A, Nynca A, Valdez KE, Mizinga KM, Petroff BK (2006) Effects of acute and chronic exposure to the aryl hydrocarbon receptor agonist 2,3,7,8-tetrachlorodibenzo-p-dioxin on the transition to reproductive senescence in female Sprague-Dawley rats. Biol Reprod 74:125–130
Fujimoto VY, Kim D, vom Saal FS, Lamb JD, Taylor JA, Bloom MS (2011) Serum unconjugated bisphenol A concentrations in women may adversely influence oocyte quality during in vitro fertilization. Fertil Steril 95:1816–1819
Fuortes L, Clark M, Kirchner H, Smith E (1997) Association between female infertility and agricultural work history. Am J Ind Med 31:445–451
Gallicchio L, Miller S, Greene T, Zacur H, Flaws JA (2009) Premature ovarian failure among hairdressers. Hum Reprod 24:2636–2641
Ganesan S, Keating AF (2014) Impact of 7,12-dimethylbenz[a]anthracene exposure on connexin gap junction proteins in cultured rat ovaries. Toxicol Appl Pharmacol 274:209–214
Ganesan S, Keating AF (2015) Phosphoramide mustard exposure induces DNA adduct formation and the DNA damage repair response in rat ovarian granulosa cells. Toxicol Appl Pharmacol 282:252–258
Ganesan S, Bhattacharya P, Keating AF (2013) 7,12-Dimethylbenz[a]anthracene exposure induces the DNA repair response in neonatal rat ovaries. Toxicol Appl Pharmacol 272:690–696
Ganesan S, Nteeba J, Keating AF (2014) Enhanced susceptibility of ovaries from obese mice to 7,12-dimethylbenz[a]anthracene-induced DNA damage. Toxicol Appl Pharmacol 281:203–210
Gannon AM, Stampfli MR, Foster WG (2012) Cigarette smoke exposure results in significant follicle loss via an alternative ovarian cell death pathway in mice. Toxicol Sci 125:274–284
Gannon AM, Stampfli MR, Foster WG (2013) Cigarette smoke exposure elicits increased autophagy and dysregulation of mitochondrial dynamics in murine granulosa cells. Biol Reprod 88:1–11
Gittens JE, Mhawi AA, Lidington D, Ouellette Y, Kidder GM (2003) Functional analysis of gap junctions in ovarian granulosa cells: distinct role for connexin 43 in early stages of folliculogenesis. Am J Physiol Cell Physiol 284:C880–C887
Gittens JE, Barr KJ, Vanderhyden BC, Kidder GM (2005) Interplay between paracrine signaling and gap junctional communication in ovarian follicles. J Cell Sci 118:113–122
Gore AC, Walker DM, Zama AM, Armenti AE, Uzumcu M (2011) Early life exposure to endocrine-disrupting chemicals causes lifelong molecular reprogramming of the hypothalamus and premature reproductive aging. Mol Endocrinol 25:2157–2168
Grasselli F, Baratta L, Baioni L, Bussolati S, Ramoni R, Grolli S, Basini G (2010) Bisphenol A disrupts granulosa cell function. Domest Anim Endocrinol 39:34–39
Guerra MT, Scarano WR, de Toledo FC, Franci JA, Kempinas Wde G (2010) Reproductive development and function of female rats exposed to di-eta-butyl-phthalate (DBP) in utero and during lactation. Reprod Toxicol 29:99–105
Haney AF, Hughes SF, Hughes CL Jr (1984) Screening of potential reproductive toxicants by use of porcine granulosa cell cultures. Toxicology 30:227–241
Hombach-Klonisch S, Pocar P, Kietz S, Klonisch T (2005) Molecular actions of polyhalogenated arylhydrocarbons (PAHs) in female reproduction. Curr Med Chem 12:599–616
Hunt PA, Koehler KE, Susiarjo M, Hodges CA, Ilagan A, Voigt RC, Thomas S, Thomas BF, Hassold TJ (2003) Bisphenol a exposure causes meiotic aneuploidy in the female mouse. Curr Biol 13:546–553
Hunt PA, Lawson C, Gieske M, Murdoch B, Smith H, Marre A, Hassold T, Vandevoort CA (2012) Bisphenol A alters early oogenesis and follicle formation in the fetal ovary of the rhesus monkey. Proc Natl Acad Sci U S A 109:17525–17530
Ikezuki Y, Tsutsumi O, Takai Y, Kamei Y, Taketani Y (2002) Determination of bisphenol A concentrations in human biological fluids reveals significant early prenatal exposure. Hum Reprod 17:2839–2841
Jackson LW, Howards PP, Wactawski-Wende J, Schisterman EF (2011) The association between cadmium, lead and mercury blood levels and reproductive hormones among healthy, premenopausal women. Hum Reprod 26:2887–2895
Jarrell JF, Villeneuve D, Franklin C, Bartlett S, Wrixon W, Kohut J, Zouves CG (1993) Contamination of human ovarian follicular fluid and serum by chlorinated organic compounds in three Canadian cities. CMAJ 148:1321–1327
Jirsova S, Masata J, Jech L, Zvarova J (2010) Effect of polychlorinated biphenyls (PCBs) and 1,1,1-trichloro-2,2,-bis (4-chlorophenyl)-ethane (DDT) in follicular fluid on the results of in vitro fertilization-embryo transfer (IVF-ET) programs. Fertil Steril 93:1831–1836
Johnson PI, Altshul L, Cramer DW, Missmer SA, Hauser R, Meeker JD (2012) Serum and follicular fluid concentrations of polybrominated diphenyl ethers and in-vitro fertilization outcome. Environ Int 45:9–14
Jukic AM, Calafat AM, McConnaughey DR, Longnecker MP, Hoppin JA, Weinberg CR, Wilcox AJ, Baird DD (2015) Urinary concentrations of phthalate metabolites and bisphenol a and associations with follicular-phase length, luteal-phase length, fecundability, and early pregnancy loss. Environ Health Perspect. doi:10.1289/ehp.1408164
Jung NK, Park JY, Park JH, Kim SY, Park JK, Chang WK, Lee HC, Kim SW, Chun SY (2010) Attenuation of cell cycle progression by 2,3,7,8-tetrachlorodibenzo-p-dioxin eliciting ovulatory blockade in gonadotropin-primed immature rats. Endocr J 57:863–871
Jurisicova A, Taniuchi A, Li H, Shang Y, Antenos M, Detmar J, Xu J, Matikainen T, Benito HA, Nunez G, Casper RF (2007) Maternal exposure to polycyclic aromatic hydrocarbons diminishes murine ovarian reserve via induction of Harakiri. J Clin Invest 117:3971–3978
Kandaraki E, Chatzigeorgiou A, Livadas S, Palioura E, Economou F, Koutsilieris M, Palimeri S, Panidis D, Diamanti-Kandarakis E (2011) Endocrine disruptors and polycystic ovary syndrome (PCOS): elevated serum levels of bisphenol A in women with PCOS. J Clin Endocrinol Metab 96:E480–E484
Kang KS, Che JH, Ryu DY, Kim TW, Li GX, Lee YS (2002) Decreased sperm number and motile activity on the F1 offspring maternally exposed to butyl p-hydroxybenzoic acid (butyl paraben). J Vet Med Sci 64:227–235
Kay VR, Chambers C, Foster WG (2013) Reproductive and developmental effects of phthalate diesters in females. Crit Rev Toxicol 43:200–219
Kidder GM, Mhawi AA (2002) Gap junctions and ovarian folliculogenesis. Reproduction 123:613–620
Kimura N, Kimura T, Suzuki M, Totsukawa K (2006) Effect of gestational exposure to nonylphenol on the development and fertility of mouse offspring. J Reprod Dev 52:789–795
Knox SS, Jackson T, Javins B, Frisbee SJ, Shankar A, Ducatman AM (2011) Implications of early menopause in women exposed to perfluorocarbons. J Clin Endocrinol Metab 96:1747–1753
Koh JM, Kim CH, Hong SK, Lee KU, Kim YT, Kim OJ, Kim GS (1998) Primary ovarian failure caused by a solvent containing 2-bromopropane. Eur J Endocrinol 138:554–556
Koifman S, Koifman RJ, Meyer A (2002) Human reproductive system disturbances and pesticide exposure in Brazil. Cad Saude Publica 18:435–445
Krotz SP, Carson SA, Tomey C, Buster JE (2012) Phthalates and bisphenol do not accumulate in human follicular fluid. J Assist Reprod Genet 29:773–777
Kwintkiewicz J, Nishi Y, Yanase T, Giudice LC (2010) Peroxisome proliferator-activated receptor-gamma mediates bisphenol A inhibition of FSH-stimulated IGF-1, aromatase, and estradiol in human granulosa cells. Environ Health Perspect 118:400–406
La Rocca C, Alessi E, Bergamasco B, Caserta D, Ciardo F, Fanello E, Focardi S, Guerranti C, Stecca L, Moscarini M, Perra G, Tait S, Zaghi C, Mantovani A (2012) Exposure and effective dose biomarkers for perfluorooctane sulfonic acid (PFOS) and perfluorooctanoic acid (PFOA) in infertile subjects: preliminary results of the PREVIENI project. Int J Hyg Environ Health 215:206–211
Laskey JW, Berman E (1993) Steroidogenic assessment using ovary culture in cycling rats: effects of Bis(2-Diethylhexyl) phthalate on ovarian steroid production. Reprod Toxicol 7:25–33
Laughlin N, Bowman R, Franks P, Dierschke D (1987) Altered menstrual cycles in rhesus monkeys induced by lead. Fundam Appl Toxicol 9:722–729
Lenie S, Smitz J (2009) Steroidogenesis-disrupting compounds can be effectively studied for major fertility-related endpoints using in vitro cultured mouse follicles. Toxicol Lett 185:143–152
Lenie S, Cortvrindt R, Adriaenssens T, Smitz J (2004) A reproducible two-step culture system for isolated primary mouse ovarian follicles as single functional units. Biol Reprod 71:1730–1738
Li TY, Colley D, Barr KJ, Yee SP, Kidder GM (2007) Rescue of oogenesis in Cx37-null mutant mice by oocyte-specific replacement with Cx43. J Cell Sci 120:4117–4125
Mahalingaiah S, Missmer SA, Maity A, Williams PL, Meeker JD, Berry K, Ehrlich S, Perry MJ, Cramer DW, Hauser R (2012) Association of hexachlorobenzene (HCB), dichlorodiphenyltrichloroethane (DDT), and dichlorodiphenyldichloroethylene (DDE) with in vitro fertilization (IVF) outcomes. Environ Health Perspect 120:316–320
Markey CM, Coombs MA, Sonnenschein C, Soto AM (2003) Mammalian development in a changing environment: exposure to endocrine disruptors reveals the developmental plasticity of steroid-hormone target organs. Evol Dev 5:67–75
Mascarenhas MN, Flaxman SR, Boerma T, Vanderpoel S, Stevens GA (2012) National, regional, and global trends in infertility prevalence since 1990: a systematic analysis of 277 health surveys. PLoS Med 9:e1001356
Masutomi N, Shibutani M, Takagi H, Uneyama C, Takahashi N, Hirose M (2003) Impact of dietary exposure to methoxychlor, genistein, or diisononyl phthalate during the perinatal period on the development of the rat endocrine/reproductive systems in later life. Toxicology 192:149–170
Matikainen T, Perez GI, Jurisicova A, Pru JK, Schlezinger JJ, Ryu HY, Laine J, Sakai T, Korsmeyer SJ, Casper RF, Sherr DH, Tilly JL (2001) Aromatic hydrocarbon receptor-driven Bax gene expression is required for premature ovarian failure caused by biohazardous environmental chemicals. Nat Genet 28:355–360
Meeker JD, Missmer SA, Altshul L, Vitonis AF, Ryan L, Cramer DW, Hauser R (2009) Serum and follicular fluid organochlorine concentrations among women undergoing assisted reproduction technologies. Environ Health 8:32
Mlynarcikova A, Kolena J, Fickova M, Scsukova S (2005) Alterations in steroid hormone production by porcine ovarian granulosa cells caused by bisphenol A and bisphenol A dimethacrylate. Mol Cell Endocrinol 244:57–62
Mlynarcikova A, Fickova M, Scsukova S (2007) The effects of selected phenol and phthalate derivatives on steroid hormone production by cultured porcine granulosa cells. Altern Lab Anim 35:71–77
Mlynarcikova A, Nagyova E, Fickova M, Scsukova S (2009) Effects of selected endocrine disruptors on meiotic maturation, cumulus expansion, synthesis of hyaluronan and progesterone by porcine oocyte-cumulus complexes. Toxicol In Vitro 23:371–377
Nagao T, Saito Y, Usumi K, Nakagomi M, Yoshimura S, Ono H (2000) Disruption of the reproductive system and reproductive performance by administration of nonylphenol to newborn rats. Hum Exp Toxicol 19:284–296
Neal MS, Zhu J, Holloway AC, Foster WG (2007) Follicle growth is inhibited by benzo-[a]-pyrene, at concentrations representative of human exposure, in an isolated rat follicle culture assay. Hum Reprod 22:961–967
Neal MS, Zhu J, Foster WG (2008) Quantification of benzo[a]pyrene and other PAHs in the serum and follicular fluid of smokers versus non-smokers. Reprod Toxicol 25:100–106
Neal MS, Mulligan Tuttle AM, Casper RF, Lagunov A, Foster WG (2010) Aryl hydrocarbon receptor antagonists attenuate the deleterious effects of benzo[a]pyrene on isolated rat follicle development. Reprod Biomed Online 21:100–108
Nilsson E, Larsen G, Manikkam M, Guerrero-Bosagna C, Savenkova MI, Skinner MK (2012) Environmentally induced epigenetic transgenerational inheritance of ovarian disease. PLoS One 7:e36129
Patel S, Bajpayee M, Pandey AK, Parmar D, Dhawan A (2007) In vitro induction of cytotoxicity and DNA strand breaks in CHO cells exposed to cypermethrin, pendimethalin and dichlorvos. Toxicol In Vitro 21:1409–1418
Petro EM, Leroy JL, Covaci A, Fransen E, De ND, Dirtu AC, De PI, Bols PE (2012) Endocrine-disrupting chemicals in human follicular fluid impair in vitro oocyte developmental competence. Hum Reprod 27:1025–1033
Petro EM, D’Hollander W, Covaci A, Bervoets L, Fransen E, De Neubourg D, De Pauw I, Leroy JL, Jorssen EP, Bols PE (2014) Perfluoroalkyl acid contamination of follicular fluid and its consequence for in vitro oocyte developmental competence. Sci Total Environ 496:282–288
Pocar P, Brevini TA, Fischer B, Gandolfi F (2003) The impact of endocrine disruptors on oocyte competence. Reproduction 125:313–325
Pollack AZ, Schisterman EF, Goldman LR, Mumford SL, Albert PS, Jones RL, Wactawski-Wende J (2011) Cadmium, lead, and mercury in relation to reproductive hormones and anovulation in premenopausal women. Environ Health Perspect 119:1156–1161
Ptak A, Ludewig G, Robertson L, Lehmler HJ, Gregoraszczuk EL (2006) In vitro exposure of porcine prepubertal follicles to 4-chlorobiphenyl (PCB3) and its hydroxylated metabolites: effects on sex hormone levels and aromatase activity. Toxicol Lett 164:113–122
Quignot N, Arnaud M, Robidel F, Lecomte A, Tournier M, Cren-Olive C, Barouki R, Lemazurier E (2012a) Characterization of endocrine-disrupting chemicals based on hormonal balance disruption in male and female adult rats. Reprod Toxicol 33:339–352
Quignot N, Tournier M, Pouech C, Cren-Olive C, Barouki R, Lemazurier E (2012b) Quantification of steroids and endocrine disrupting chemicals in rat ovaries by LC-MS/MS for reproductive toxicology assessment. Anal Bioanal Chem 403:1629–1640
Reinsberg J, Wegener-Toper P, van der Ven K, van der Ven H, Klingmueller D (2009) Effect of mono-(2-ethylhexyl) phthalate on steroid production of human granulosa cells. Toxicol Appl Pharmacol 239:116–123
Rodriguez HA, Santambrosio N, Santamaria CG, Munoz-de-Toro M, Luque EH (2010) Neonatal exposure to bisphenol A reduces the pool of primordial follicles in the rat ovary. Reprod Toxicol 30:550–557
Rosenmai AK, Dybdahl M, Pedersen M, Alice van Vugt-Lussenburg BM, Wedebye EB, Taxvig C, Vinggaard AM (2014) Are structural analogues to bisphenol a safe alternatives? Toxicol Sci 139:35–47
Rutstein SO, Shah IH (2004) Infecundity, infertility, and childlessness in developing countries. ORC Macro, Calverton
Sadeu JC, Foster WG (2011a) Cigarette smoke condensate exposure delays follicular development and function in a stage-dependent manner. Fertil Steril 95:2410–2417
Sadeu JC, Foster WG (2011b) Effect of in vitro exposure to Benzo[a]pyrene, a component of cigarette smoke, on folliculogenesis, steroidogenesis, and oocyte maturation. Reprod Toxicol 31:402–408
Sadeu JC, Hughes CL, Agarwal S, Foster WG (2010) Alcohol, drugs, caffeine, tobacco, and environmental contaminant exposure: reproductive health consequences and clinical implications. Crit Rev Toxicol 40:633–652
Sahambi SK, Visser JA, Themmen AP, Mayer LP, Devine PJ (2008) Correlation of serum anti-Mullerian hormone with accelerated follicle loss following 4-vinylcyclohexene diepoxide-induced follicle loss in mice. Reprod Toxicol 26:116–122
Schlebusch H, Wagner U, van der Ven H, Al-Hasani S, Diedrich K, Krebs D (1989) Polychlorinated biphenyls: the occurrence of the main congeners in follicular and sperm fluids. J Clin Chem Clin Biochem 27:663–667
Shi Z, Valdez KE, Ting AY, Franczak A, Gum SL, Petroff BK (2007) Ovarian endocrine disruption underlies premature reproductive senescence following environmentally relevant chronic exposure to the aryl hydrocarbon receptor agonist 2,3,7,8-tetrachlorodibenzo-p-dioxin. Biol Reprod 76:198–202
Signorile PG, Spugnini EP, Citro G, Viceconte R, Vincenzi B, Baldi F, Baldi A (2012) Endocrine disruptors in utero cause ovarian damages linked to endometriosis. Front Biosci (Elite Ed) 4:1724–1730
Silva MJ, Slakman AR, Reidy JA, Preau JL Jr, Herbert AR, Samandar E, Needham LL, Calafat AM (2004) Analysis of human urine for fifteen phthalate metabolites using automated solid-phase extraction. J Chromatogr B Analyt Technol Biomed Life Sci 805:161–167
Smith KW, Souter I, Dimitriadis I, Ehrlich S, Williams PL, Calafat AM, Hauser R (2013) Urinary paraben concentrations and ovarian aging among women from a fertility center. Environ Health Perspect 121:1299–1305
Sobinoff AP, Pye V, Nixon B, Roman SD, McLaughlin EA (2010) Adding insult to injury: effects of xenobiotic-induced preantral ovotoxicity on ovarian development and oocyte fusibility. Toxicol Sci 118:653–666
Songsasen N, Woodruff TK, Wildt DE (2011) In vitro growth and steroidogenesis of dog follicles are influenced by the physical and hormonal microenvironment. Reproduction 142:113–122
Stephen EH, Chandra A (2006) Declining estimates of infertility in the United States: 1982–2002. Fertil Steril 86:516–523
Sun F, Betzendahl I, Shen Y, Cortvrindt R, Smitz J, Eichenlaub-Ritter U (2004) Preantral follicle culture as a novel in vitro assay in reproductive toxicology testing in mammalian oocytes. Mutagenesis 19:13–25
Takai Y, Canning J, Perez GI, Pru JK, Schlezinger JJ, Sherr DH, Kolesnick RN, Yuan J, Flavell RA, Korsmeyer SJ, Tilly JL (2003) Bax, caspase-2, and caspase-3 are required for ovarian follicle loss caused by 4-vinylcyclohexene diepoxide exposure of female mice in vivo. Endocrinology 144:69–74
Takeuchi T, Tsutsumi O, Ikezuki Y, Takai Y, Taketani Y (2004) Positive relationship between androgen and the endocrine disruptor, bisphenol A, in normal women and women with ovarian dysfunction. Endocr J 51:165–169
Taxvig C, Vinggaard AM, Hass U, Axelstad M, Boberg J, Hansen PR, Frederiksen H, Nellemann C (2008) Do parabens have the ability to interfere with steroidogenesis? Toxicol Sci 106:206–213
Tian Y, Ke S, Thomas T, Meeker RJ, Gallo MA (1998) Regulation of estrogen receptor mRNA by 2,3,7,8-tetrachlorodibenzo-p-dioxin as measured by competitive RT-PCR. J Biochem Mol Toxicol 12:71–77
Trapp M, Baukloh V, Bohnet H-G, Heeschen W (1984) Pollutants in human follicular fluid. Fertil Steril 42(1):146–148
Treinen KA, Dodson WC, Heindel JJ (1990) Inhibition of FSH-stimulated cAMP accumulation and progesterone production by mono(2-ethylhexyl) phthalate in rat granulosa cell cultures. Toxicol Appl Pharmacol 106:334–340
Tsutsumi O (2005) Assessment of human contamination of estrogenic endocrine-disrupting chemicals and their risk for human reproduction. J Steroid Biochem Mol Biol 93:325–330
Uzumcu M, Kuhn PE, Marano JE, Armenti AE, Passantino L (2006) Early postnatal methoxychlor exposure inhibits folliculogenesis and stimulates anti-Mullerian hormone production in the rat ovary. J Endocrinol 191:549–558
Valdez KE, Shi Z, Ting AY, Petroff BK (2009) Effect of chronic exposure to the aryl hydrocarbon receptor agonist 2,3,7,8-tetrachlorodibenzo-p-dioxin in female rats on ovarian gene expression. Reprod Toxicol 28:32–37
Van Wemmel K, Gobbers E, Eichenlaub-Ritter U, Smitz J, Cortvrindt R (2005) Ovarian follicle bioassay reveals adverse effects of diazepam exposure upon follicle development and oocyte quality. Reprod Toxicol 20:183–193
Vo TT, Yoo YM, Choi KC, Jeung EB (2010) Potential estrogenic effect(s) of parabens at the prepubertal stage of a postnatal female rat model. Reprod Toxicol 29:306–316
Weiss JM, Bauer O, Bluthgen A, Ludwig AK, Vollersen E, Kaisi M, Al-Hasani S, Diedrich K, Ludwig M (2006) Distribution of persistent organochlorine contaminants in infertile patients from Tanzania and Germany. J Assist Reprod Genet 23:393–399
Willoughby KN, Sarkar AJ, Boyadjieva NI, Sarkar DK (2005) Neonatally administered tert-octylphenol affects onset of puberty and reproductive development in female rats. Endocrine 26:161–168
Windham GC, Mitchell P, Anderson M, Lasley BL (2005) Cigarette smoking and effects on hormone function in premenopausal women. Environ Health Perspect 113:1285–1290
Wong SL, Lye EJ (2008) Lead, mercury and cadmium levels in Canadians. Health Rep 19:31–36
Xi W, Lee CK, Yeung WS, Giesy JP, Wong MH, Zhang X, Hecker M, Wong CK (2011) Effect of perinatal and postnatal bisphenol A exposure to the regulatory circuits at the hypothalamus-pituitary-gonadal axis of CD-1 mice. Reprod Toxicol 31:409–417
Yang JM, Chen QY, Jiang XZ (2002) Effects of metallic mercury on the perimenstrual symptoms and menstrual outcomes of exposed workers. Am J Ind Med 42:403–409
Yin S, Song C, Wu H, Chen X, Zhang Y (2015) Adverse effects of high concentrations of fluoride on characteristics of the ovary and mature oocyte of mouse. PLoS One 10:e0129594
Younglai EV, Foster WG, Hughes EG, Trim K, Jarrell JF (2002) Levels of environmental contaminants in human follicular fluid, serum, and seminal plasma of couples undergoing in vitro fertilization. Arch Environ Contam Toxicol 43:121–126
Zachow R, Uzumcu M (2006) The methoxychlor metabolite, 2,2-bis-(p-hydroxyphenyl)-1,1,1-trichloroethane, inhibits steroidogenesis in rat ovarian granulosa cells in vitro. Reprod Toxicol 22:659–665
Zama AM, Uzumcu M (2009) Fetal and neonatal exposure to the endocrine disruptor methoxychlor causes epigenetic alterations in adult ovarian genes. Endocrinology 150:4681–4691
Zama AM, Uzumcu M (2010) Epigenetic effects of endocrine-disrupting chemicals on female reproduction: an ovarian perspective. Front Neuroendocrinol 31:420–439
Zhang W, Jia H (2007) Effect and mechanism of cadmium on the progesterone synthesis of ovaries. Toxicology 239:204–212
Zhang W, Pang F, Huang Y, Yan P, Lin W (2008) Cadmium exerts toxic effects on ovarian steroid hormone release in rats. Toxicol Lett 182:18–23
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Dominguez, M.A., Sadeu, J.C., Guerra, M.T., Furlong, H.C., Baines, S., Foster, W.G. (2016). Ovarian Toxicity of Environmental Contaminants: 50 Shades of Grey. In: Hughes, C., Waters, M. (eds) Translational Toxicology. Molecular and Integrative Toxicology. Humana Press, Cham. https://doi.org/10.1007/978-3-319-27449-2_7
Download citation
DOI: https://doi.org/10.1007/978-3-319-27449-2_7
Published:
Publisher Name: Humana Press, Cham
Print ISBN: 978-3-319-27447-8
Online ISBN: 978-3-319-27449-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)