Abstract
The tumor microenvironment (TME) represents a milieu that enables tumor cells to acquire the hallmarks of cancer. The TME is heterogeneous in composition and consists of cellular components, growth factors, proteases, and extracellular matrix. Concerted interactions between genetically altered tumor cells and genetically stable intratumoral stromal cells result in an “activated/reprogramed” stroma that promotes carcinogenesis by contributing to inflammation, immune suppression, therapeutic resistance, and generating premetastatic niches that support the initiation and establishment of distant metastasis. The lungs present a unique milieu in which tumors progress in collusion with the TME, as evidenced by regions of aberrant angiogenesis, acidosis and hypoxia. Inflammation plays an important role in the pathogenesis of lung cancer, and pulmonary disorders in lung cancer patients such as chronic obstructive pulmonary disease (COPD) and emphysema, constitute comorbid conditions and are independent risk factors for lung cancer. The TME also contributes to immune suppression, induces epithelial-to-mesenchymal transition (EMT) and diminishes efficacy of chemotherapies. Thus, the TME has begun to emerge as the “Achilles heel” of the disease, and constitutes an attractive target for anti-cancer therapy. Drugs targeting the components of the TME are making their way into clinical trials. Here, we will focus on recent advances and emerging concepts regarding the intriguing role of the TME in lung cancer progression, and discuss future directions in the context of novel diagnostic and therapeutic opportunities.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Microenvironment
- Lung cancer
- Inflammation
- Immune cells
- Angiogenesis
- Endothelial cells
- Bone marrow
- Hypoxia
- Therapy
- Immunotherapy
- Radiation
- Resistance
1 The Tumor Microenvironment: An Overview
The TME has been recognized as a major contributor to tumor progression and metastasis [1–4]. The TME is heterogeneous in composition, and concerted heterotypic reciprocal interactions between genetically altered tumor epithelial cells and intratumoral stromal cells regulate major hallmarks of cancer including angiogenesis, inflammation, immune suppression, epithelial-to-mesenchymal transition (EMT), and metastasis [1, 3]. Importantly, strategies that target the TME are being considered in cancer prevention [5–7].
The stromal cells recruited to the tumor beds are “educated” and “reprogramed” by the paracrine activity of tumor epithelial cells to acquire an “activated” protumorigenic phenotype [8–10]. Examples of tumor-activated stromal cells include macrophages (classically activated M1 to alternatively-activated M2 phenotype) [11, 12], neutrophils (N1 to N2 conversion) [11], fibroblasts (conversion to activated cancer-associated fibroblasts (CAFs)) [13], endothelial cells [14] and immune cells [15]. These activated stromal cells promote tumor growth and have begun to emerge as attractive targets for anti-cancer therapy [1, 5, 16, 17].
The “angiogenic switch” is a critical step in tumor growth and in the progression of micrometastasis to lethal macrometastasis [1, 18, 19]. The molecular players and mechanisms underlying the angiogenic switch have been intensely investigated, and a variety of pro-angiogenic factors and angiogenic inhibitors that play critical roles during the angiogenic switch have been identified and characterized. Insights from these investigations have led to the development of various pro- and anti-angiogenic therapies that are currently tested in clinical trials or are already in clinical use. Inhibition of angiogenesis by neutralizing antibodies against vascular endothelial growth factor (VEGF) is effective at reducing progression of certain tumors despite having little effect on most tumor cells [7]. In addition to endothelial cells, the inflammatory cells, particularly cells of the myeloid lineages (monocytes, macrophages, and neutrophils) and CAFs progressively accumulate in tumors, where they establish an inflammatory protumorigenic TME [12, 20]. Inflammation is now accepted as an underlying or enabling characteristic that contributes to key hallmarks of cancer, and non-steroidal anti-inflammatory drugs have shown a reduction in cancer risk [21, 22] and may prevent distant metastasis [23]. Myeloid cells also secrete VEGF, basic fibroblast growth factor (bFGF), platelet-derived growth factor (PDGF), placental growth factor (PIGF), and Bv8, that contribute to vascular remodeling during tumor progression [24, 25]. Myeloid cells also secrete proteases such as urokinase-type plasminogen activator (uPA) and matrix metalloproteinases (MMPs), which degrade extracellular matrix (ECM) components to release VEGF and other sequestered mitogenic factors that facilitate endothelial migration and tumor invasion [26].
Tumor-associated macrophages (TAMs) accumulate in regions of hypoxia [27] and support multiple aspects of tumor progression [28]. Studies from breast cancer and glioblastoma have shown that TAMs promote invasive cellular phenotypes [29], through a paracrine signaling loop that involves tumor-derived colony-stimulating factor 1 (CSF-1) and macrophage-derived epidermal growth factor (EGF) [30–32]. TAMs also secrete proteases, such as cysteine cathepsins, which support tumor progression and confer therapeutic resistance [33, 34]. The therapeutic potential of targeting TAMs has been demonstrated in breast cancer and in glioblastoma [6, 34, 35].
The stromal cells also generate inflammatory conditions that contribute to tumorigenesis [20, 36, 37]. The inflammation-responsive Ikappa B kinase (IKK)-beta and its target nuclear factor kappa B (NF-κB) have important tumor-promoting functions within malignant cells and inflammatory cells (macrophages, lymphocytes) [38]. From a clinical perspective, a strong tumor-associated inflammatory response can be initiated by cancer therapy. For example, radiation and chemotherapy cause massive necrotic death of cancer cells and surrounding tissues, which in turn trigger an inflammatory reaction. Therapy-induced inflammation may have tumor-promoting functions [39, 40], or may enhance the cross-presentation of tumor antigens and subsequent induction of an anti-tumor immune response [41].
Cells and molecules of the immune system are a fundamental component of the TME. The tumor-infiltrating immune cells constitute two distinct compartments mediating the innate and adaptive immune responses. The innate immune system consists of phagocytes including neutrophils, mast cells/macrophages (CD68+), dendritic cells (DC), natural killer NK cells (CD56+ CD3–), and NK T cells (CD56+ CD3+), and mainly serves as the first-line defense against both foreign pathogens and transformed cells. However, the tumor “reprogramed” innate immune system stimulates tumor growth by promoting tumor angiogenesis, invasion, and metastasis; whereas the adaptive immune system tends to repress tumor growth. The adaptive immune system is mediated by two major T lymphocyte subsets; cytotoxic T cells (CTL) (CD8+) and helper T cells (Th) (CD4+), and B cells (CD20+). The adaptive immune system is the second-line defense, acting via antigen-specific molecules and requiring clonal expansion following the recognition of foreign antigens. However, in the TME, cancer cells often induce an immunosuppressive microenvironment, which favors the development of immunosuppressive populations of immune cells, such as myeloid-derived suppressor cells (MDSCs) and regulatory T cells (Treg). Understanding the complexity of immunomodulation by tumors is important for the development of immunotherapy, and among the most promising approaches to activating therapeutic antitumor immunity is the blockade of immune checkpoint pathways [42].
MDSCs are a heterogeneous population of immature myeloid progenitors, and precursors of macrophages, granulocytes and dendritic cells [43, 44]. In general, MDSCs from cancer patients express the common myeloid markers CD33 and CD11b, display heterogeneous expression of CD14 (monocytic) and CD15 (granulocytic) markers, but lack mature myeloid or lymphoid markers such as HLA-DR [45, 46]. Clinical correlation studies in breast, colorectal, pancreatic, esophageal, and gastric cancer patients demonstrated that MDSC levels confer an independent prognostic factor for survival [47, 48]. Since MDSCs the major regulators of the immune response due to their ability to suppress both the cytotoxic activities of natural killer (NK) and NKT cells, and the adaptive immune response mediated by CD4+ and CD8+ T cells [44, 49, 50], this cell type has generated much attention. While the mechanism of NK cell inhibition is currently not well understood, multiple pathways are responsible for MDSC-mediated T cell suppression including: (1) production of Arginase 1 (ARG1), which depletes L-Arginine from the microenvironment, and (2) production of nitric oxide synthase 2 (NOS2). Both pathways block translation of the T cell CD3 zeta chain, inhibit T cell proliferation, and promote T cell apoptosis [51]. Not much is known regarding upstream regulators of these suppressive mediators. However recent studies have demonstrated the importance of key signaling pathways such as PI3K, Ras, JAK-STAT, and TGFβ—STAT3 signaling [52, 53]. In mice, MDSCs have been defined as CD11b+ Gr1+ cells and can be subdivided into granulocytic (CD11b+ Ly6G+ Ly6Clow) or monocytic (CD11b+ Ly6G–Ly6Chi) [54]. The mechanisms by which MDSCs are generated and contribute to immune suppression is being exploited for developing anti-MDSC agents [55]. Approaches to inhibit MDSCs include use of phosphodiesterase (PDE) inhibitors, nitroaspirins, synthetic triterpenoids, COX2 inhibitors, ARG1 inhibitors, anti-glycan antibodies, CSF-1R antagonists, IL-17 inhibitors, and histamine-based approaches. In another approach, MDSCs differentiate by using all-trans retinoic acid (ATRA), vitamins A or D3, or IL-12 [56]. Some compounds , such as ATRA, PDE5 inhibitors, nitroaspirins (e.g. NCX-4016), or tyrosine kinase inhibitors, are being tested in clinical trials to mediate suppression of MDSCs, and improve the efficacy of immune modulating therapies (immune checkpoint inhibitors or cancer vaccines). Notably, pre-clinical evidence suggests that cancer vaccines are more effective in tumor-bearing mice that have been depleted of MDSCs.
2 TME in Lung Cancer Prognosis
Lung cancer is the leading cause of cancer-related deaths worldwide [57]. Lung cancer is generally classified into two histopathological subtypes, small-cell lung carcinoma (SCLC) and non–small cell lung carcinoma (NSCLC) . NSCLC accounts for 80% of all lung malignancies, and the overall 5-year survival of patients with this disease remains approximately 15% [58]. A major research focus in lung cancer has been directed to cancer cell intrinsic properties [59–61], which has led to the discovery of important driver mutations and the development of targeted therapies, such as the receptor tyrosine kinase (RTK) inhibitors gefitinib/erlotinib (EGFR inhibitors) and crizotinib (EML4-ALK inhibitor) [62–64]. However, these treatments benefit only a small proportion (15–20%) of patients harboring these driver mutations, and acquired resistance to these therapies presents a major impediment to the effective treatment of NSCLC patients with these mutations [65–67]. More recent studies have begun to elucidate the prognostic and pathophysiological role of the TME in lung cancer.
Many studies have examined the contribution of tumor epithelial molecular markers for prognosis and guidance of cancer therapy, yet only a few have focused on the analysis of the tumor-associated stroma for the identification of prognostic and predictive markers in cancer therapy. More recent studies have begun to demonstrate the prognostic role of TME in cancer with the promise to advance discovery of prognostic and predictive molecular markers for patient management and cancer therapy. For example, stromal gene signatures have been shown to predict clinical outcome and resistance to therapy in breast cancer [68, 69], and fibroblast-derived transcriptional signatures were associated with cancer progression and poor outcome in human breast and lung cancer [70, 71]. In patients with stage I NSCLC, the presence of CAFs is a poor prognostic indicator typically associated with nodal metastases and a higher risk of recurrence [72]. Interestingly, a specific 11-gene expression signature in CAFs stratified NSCLC patients into low and high-risk groups, and was associated with survival [71]. Similarly, prognostic gene signatures from bulk NSCLC tissue analysis included prominent stromal genes such as glypican 3, ICAM-1, laminin B1, L-selectin, P-selectin, and SPARC [73, 74]. High numbers of circulating endothelial cells (CECs) and high levels of soluble CD146 (sCD146) in the plasma have been shown to correlate with poor prognosis and may be useful for the prediction of clinical outcome in patients undergoing surgery for NSCLC [75].
Recently, several groups have demonstrated that the immune fraction of the TME has prognostic value in lung cancer. Elevated numbers of MDSCs have been associated with poor clinical outcomes [76, 77]. Similarly, leukocyte infiltrates, particularly increased numbers of neutrophils, were significantly associated with a worse outcome in patients with bronchioalveolar carcinoma [78–80]. Tumor-infiltrating mature dendritic cells have been suggested to identify patients with early-stage NSCLC who have a high risk of relapse [81, 82]. High density of stromal CD56+ NK cells was shown to be an independent factor associated with improved prognosis in resected NSCLC [81]. TAMs are abundant components of NSCLC, and clinical data correlating the apoptotic index and/or macrophage densities and polarization status (M1/M2) with outcome in NSCLC patients has been recently reviewed [83]. The number of macrophages in NSCLC stroma is an independent predictor of survival time in NSCLC patients [84]. Similarly, mast cells [85], cytotoxic T cells [86], and helper T cells [87] have been reported as potential prognostic factors following resection in patients with NSCLC. Recently, tumor-infiltrating FOXP3+ Treg cells were positively correlated with intratumoral COX-2 expression and were associated with a worse recurrence-free survival (RFS), especially among patients with node-negative NSCLC [88]. Stromal CD99 expression has been described as a novel prognostic marker in human NSCLC [89], and humoral immune response immunoglobulin kappa C (IGKC) expression in tumor-infiltrating plasma cells was shown to have prognostic value in NSCLC [90].
3 TME in Lung Cancer Progression and Metastasis
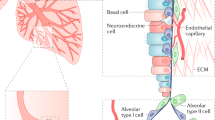
The stroma in NSCLC is heterogeneous, comprised of many different populations of cells, including bone marrow-derived immune and inflammatory cells, fibroblasts, and endothelial cells (Fig. 1). The contribution of these cell types to tumor growth is illustrated below.
Infiltration of BM hematopoietic cells in the adenocarcinoma and matched adjacent lung. (a) H&E staining of lung tissue from an adenocarcinoma patient (×20 magnification). (b) Representative immunofluorescence image of tumor and matched adjacent non-neoplastic lung of adenocarcinoma patient stained for epithelial cells (EpCAM+, red) and BM-derived hematopoietic cells (CD45+, green). DAPI (blue) was used to label cell nuclei
3.1 Cancer-Associated Fibroblasts (CAFs)
As is the case for many solid tumors, the TME of human NSCLC often demonstrates significant desmoplasia, which is characterized by stromal changes depicted by the presence of activated stromal fibroblasts [91–93]. In addition, several mouse explant studies have suggested a pro-tumorigenic role for tumor-derived lung fibroblasts in NSCLCs [94–96]. CAFs, which differ morphologically and functionally from normal fibroblasts (NFs), exhibit similar activities with wound-activated fibroblasts, suggesting that the supportive and reparative roles of activated fibroblasts in wound healing contribute to the pro-tumorigenic activities of CAFs. The origin of CAFs is not clear, yet it is likely that they arise from a reprogramming of tissue resident fibroblasts [97] as well as differentiate from BM cells recruited to the tumor [98].
CAFs have been reported to support tumor progression, metastasis, and chemotherapy resistance by a wide variety of mechanisms, including direct paracrine support of cancer cells via the secretion of growth factors, cytokines, and chemokines, through pro-angiogenic effects, as well as by remodeling the extracellular matrix [99–102].
A number of different mechanisms have been specifically reported for the pro-tumorigenic activity of CAFs in NSCLC. A paracrine crosstalk between fibroblasts and NSCLC cells involves IL-6 and TGFβ-enhanced EMT and tumor progression [97, 103]. Cross-species functional characterization of mouse and human lung CAFs identified a secreted gene signature, and functional studies identified important roles for cardiotrophin-like cytokine factor 1 (CLCF1)-Ciliary Neurotrophic Factor Receptor (CNTFR) and interleukin (IL)-6–IL-6R signaling in promoting growth of NSCLCs [104]. A paracrine network was described, involving Insulin-like growth factor-II (IGFII)/IGF1 receptor (IGF1R)-Nanog signaling pathway by which CAFs contributed to cancer stem cell enrichment in NSCLC [105]. Importantly, this paracrine signaling predicted overall and relapse-free survival in stage I NSCLC patients. Similarly, pulmonary fibroblasts induced EMT and stem cell potential in NSCLC [106]. Fibroblast-derived hepatocyte growth factor (HGF) was shown to induce EGFR-tyrosine kinase inhibitor (TKI) resistance in NSCLC with EGFR-activating mutations [107, 108].
The lack of a single pro-tumorigenic activity likely reflects the heterogeneity of CAFs within a tumor. Although there are several markers of CAFs (e.g. α-smooth muscle actin (αSMA), fibroblast-activating protein (FAP), and fibroblast-specific protein (FSP)), no distinct single marker of CAFs exist, and none of the commonly used markers for CAFs are unique to CAFs [94]. Compounding this heterogeneity of CAFs within a tumor is the heterogeneity of CAFs among different tumors. It is likely that specific cancer cells require distinct support from CAFs. For example, in a recent study, metabolic reprogramming in NSCLC-CAFs was shown to correlate with increased glycolytic metabolism of the tumor, indicating tumor-specific specialization of CAFs [109].
3.2 Endothelial Cells
Endothelial cells that form the vasculature have key functions in providing nutrients and oxygen to the tumor. However, emerging studies have begun to describe “angiocrine” regulation as a major endothelial function in cancer [110]. Vascular endothelial cells actively participate in and regulate the inflammatory response in both normal and diseased tissues [111], and emerging data suggests that endothelial cells directly influence tumor behavior [18, 112]. In NSCLC, the degree of tumor-associated angiogenesis correlates with disease progression and predicts unfavorable survival outcome [113]. In particular, high vascularity at the tumor periphery has been correlated with tumor progression [114]. However, high steady state vessel density in the lung has imposed challenges in accurate identification and quantification of neoangiogenic microvessels in the tumor tissue. Notably, some NSCLCs do not display an angiogenic phenotype and these tumors are invasive, exploiting the pre-existing alveolar vessels for growth [115, 116].
In a recent study, endothelial-derived angiocrine signals were shown to induce regenerative lung alveolarization. Particularly, activation of VEGFR2 and FGFR1 in pulmonary capillary endothelial cells induced MMP14 expression that unmasked EGF receptor ligands to enhance alveologenesis [117]. Lung endothelial cells also control lung stem cell differentiation, as bone morphogenetic protein 4 (BMP4)-BMPR1A signaling triggers calcineurin/NFATc1-dependent expression of thrombospondin-1 (Tsp-1) in lung endothelial cells to promote alveolar lineage-specific bronchioalveolar stem cell differentiation [118]. Using a mouse model of lung adenocarcinoma , it was shown that perlecan , a component of the ECM, secreted by endothelial cells in a paracrine fashion blocked proliferation and invasiveness of lung cancer by impacting pro-inflammatory pathways [112].
3.3 Hypoxia in Lung Cancer
Hypoxia is typically present in solid tumors, like lung cancer, and is known to enhance tumor progression and therapy resistance [119]. The effects of hypoxia are largely mediated by the hypoxia-inducible factors (HIFs) HIF-1α and HIF-2α, as they activate the transcription of genes implicated in tumor angiogenesis, cell survival, and resistance to chemotherapeutic drugs [120]. The overexpression of HIF-1α confers cellular resistance to the EGFR-blocking mAb cetuximab in epidermoid carcinoma cells. In addition, knocking down HIF-1α substantially restores cellular sensitivity to cetuximab-mediated antitumor activities [121]. These findings suggest that HIF-1α expression is associated with the therapeutic responses of cancer cells to EGFR-targeted therapies. More recently, the involvement of hypoxia in the resistance to EGFR-TKIs , such as gefitinib and erlotinib, in NSCLC with an EGFR-sensitive mutation was shown to be mediated by TGFβ [122]. The hypoxic microenvironment is an important stem cell niche that promotes the persistence of cancer stem cells (CSCs) in tumors. Importantly, hypoxia was shown to increase the population of lung CSCs resistant to gefitinib in EGFR mutation-positive NSCLC by activating IGF1R [123].
3.4 Inflammation
Chronic lung inflammation has been associated with an increased risk of lung cancer. Carcinogens including asbestos, cigarette smoke, and other pollutants are known to cause a chronic inflammatory state, which in turn promotes tumorigenesis [20]. Moreover, pulmonary disorders such as COPD/emphysema and pulmonary fibrosis, which are associated with greater risk for developing lung cancer, are characterized by copious inflammation [124–126]. It remains unclear whether inflammation affects the incidence of driver oncogenic mutations. However, inflammation has been shown to enhance tumor progression. Lipopolysaccharide (LPS) , a potent endotoxin eliciting chronic lung inflammation, significantly increased the risk of carcinogen-mediated lung tumorigenesis in mice through K-ras gene activation by point mutations [127]. Recently, it was demonstrated that mucin 1 (MUC1) contributes to smoking-induced lung cancers that are driven by inflammatory signals from macrophages, and a signaling pathway involving PPAR-γ, ERK, and MUC1 resulted in TNFα secretion in macrophages [128].
Inflammation has also been described in the generation of lung metastasis from extrapulmonary neoplasms . Clinical studies suggested a correlation between smoking and an increased risk of lung metastasis in patients with breast cancer [129, 130] and esophageal cancer [131]. In addition, inflammation caused by smoke inhalation in mice was also correlated with increased incidence of lung metastasis [132]. Data on autoimmune arthritis showed that lung inflammation in arthritic mice, characterized by neutrophil and mast cell infiltration, as well as increase in circulating levels of pro-inflammatory cytokines, was associated with enhanced lung metastasis [133, 134]. Recently, several mechanisms explaining the metastasis-promoting effects of inflammation have been elucidated. LPS-induced acute lung inflammation dramatically increased breast cancer cell metastasis to lung via a ubiquitin/CXCR4-dependent mechanism [135]. Systemic LPS-induced inflammation led to elevated levels of E-selectin expression in lung tissue and enhanced lung metastasis of breast cancer cells [136]. Induction of lung inflammation by specific NF-κB activation in airway epithelial cells increased lung metastasis via a macrophage-dependent mechanism [137]. Bladder cancer cells expressing the proteoglycan versican metastasize to the lungs via a mechanism involving increased lung CCL2 chemokine expression and macrophage infiltration [138]. The recruitment of CCR2 (the receptor for chemokine CCL2)-expressing monocytes/macrophages to the metastatic site in response to CCL2 enhances breast tumor metastasis to lungs [139]. Lewis lung carcinoma (LLC) cells express versican and subsequently activate TLR2: TLR6 complexes on myeloid cells, inducing TNFα secretion and thus enhancing LLC metastatic growth [140]. Another study showed that CD11+ Gr1+ Ly6Chigh myeloid progenitor cells express versican in the premetastatic lung, leading to stimulation of mesenchymal-to-epithelial transition of metastatic tumor cells, increasing cell proliferation and accelerating metastasis [8]. Furthermore, these pre-metastatic niches are characterized by the induction of chemoattractants such as, S100A8, growth factors, ECM proteins including fibronectin, and ECM-modifying proteins like lysyl oxidase [141–144], creating a permissive microenvironment for metastasis [145]. Importantly, S100A8/A9 expression in the pre-metastatic niche in turn induces expression of serum amyloid A (SAA) 3, which through the Toll-like receptor 4 (TLR4) leads to the activation of NF-κB signaling and further amplification of inflammatory responses, accelerating lung metastasis [146].
3.5 Immune Cells
Tumors utilize various mechanisms to evade destruction by the immune system. One of the key immunomodulatory mechanisms is via immune checkpoint pathways, which play a key role in regulating T-cell responses. Under normal circumstances, the immune checkpoints are important to maintain self-tolerance by preventing autoimmunity and protecting the tissue from damage when the immune system is activated. The expression of immune checkpoint proteins are usually exploited by the tumor cells to develop resistance mechanisms.
3.5.1 T-Cells
Tumor-infiltrating lymphocytes (TILs) are often found in the TME, suggesting an immune response against the tumor. Among the TILs, CD8+ cytotoxic T lymphocytes (CTLs) are directly capable of killing tumor cells, whereas CD4+ T helper lymphocytes (Th) are a heterogeneous cytokine-secreting class of T lymphocytes. Th1 subtypes activate CTLs, whereas Th2 lymphocytes stimulate humoral immunity. Besides the Th1 and Th2 subsets, the CD4+ regulatory T lymphocyte (Treg) subset suppresses effector T lymphocytes. In cancer, Tregs preferentially traffic to tumors, as a result of chemokines produced by tumor cells and microenvironmental macrophages. While active immunotherapy such as adoptive T cell-transfer represents one promising therapeutic approach in lung cancer, more recently, immune checkpoint blockade has received tremendous attention as a potential therapy in solid tumors including lung cancer. The two major immune checkpoint inhibitory pathways involve the programmed cell death-1, PD-1/ PD-L1 pathway and the cytotoxic T-lymphocyte antigen-4, CTLA-4 pathway [147]. PD-1 is a surface receptor member of the B7-CD28 superfamily. It is expressed on many cell types, including activated T cells, B cells, NK cells, and host tissues. PD-1 binds with its ligand PD-L1 (B7-H1, CD274) on antigen presenting cells (APCs), and this interaction inhibits downstream NF-κB transcription and downregulates interferon (IFN)-γ secretion, resulting in T-cell tolerance. Similarly , PD1 can also interact with PD-L2 on dendritic cells, and PD-L2 also has effective inhibitory activity upon T cells. CTLA-4 is expressed on the surface of activated cytotoxic T cells, and it competes with the costimulatory molecule CD28 for mutually shared ligands, B7-1 (CD80) or B7-2 (CD86), and these interactions inhibit the antitumor activity of T-cells.
Recent understanding of the functioning of the immune system and its relation to tumor evasion have led to the development of novel agents that have promising results in the treatment of NSCLC. These agents include immune checkpoint inhibitors such as anti-PD-1 antibodies (nivolumab and MK-3475), anti-PD-L1 antibody (MPDL3280A, MEDI4736), and CTLA-4 inhibitors (tremelimumab and ipilimumab), as well as vaccines.
3.5.2 γδ T Cells
γδ T cells contribute to lymphoid antitumor surveillance and bridge the gap between innate and adaptive immunity [148]. γδ T cells constitute 1%–5% of peripheral blood T lymphocytes and recognize phosphoantigens via polymorphic γδ T-cell antigen receptors (TCR), and develop strong cytolytic and Th1-like effector functions [149]. Therefore, γδ T cells are attractive candidate effector cells for cancer immunotherapy, as they can secrete cytokines abundantly and exert potent cytotoxicity against a wide range of cancer cells. Clinical trials have been conducted to evaluate the safety and efficacy of γδ T-cell-based immunotherapies for non-Hodgkin’s lymphoma, multiple myeloma, and solid tumors. In lung cancer, the therapeutic impact of adoptive immunotherapy with expanded γδ T-cells is being assessed [150, 151], and in one study, remission of lung metastasis following adoptive immunotherapy using activated autologous γδ T-cells in a patient with renal cell carcinoma was observed [152].
3.5.3 Myeloid-Derived Suppressor Cells
Increase in the number of MDSCs induces a strong immunosuppressive activity in cancer patients [153–155]. In a mouse model of lung cancer, MDSC depletion increased APC activity and augmented the frequency and activity of NK and T cell effectors that led to impaired tumor growth, enhanced therapeutic vaccination responses, and conferred immunological memory [156, 157]. Immune suppressive MDSCs, defined as Lin−HLA-DR−CD33+ and CD14−CD11b+ CD33+ [158] were increased in patients with lung cancer. Analysis of 89 patients with NSCLC showed an increase in both frequency and absolute number of MDSCs in the peripheral blood and indicated an association with metastasis, response to chemotherapy, and progression-free survival [159].
4 TME of Premetastatic Niche in the Lung
The lung is one of the most frequent sites of metastasis from extrapulmonary neoplasms including breast and colon cancer. As early as 1889, Steven Paget proposed his “seed” and “soil” hypothesis establishing the concept that primary tumors metastasize to specific organs which harbor a receptive microenvironment [160]. More recently, experimental support for this hypothesis has been provided by studies showing that primary tumors release specific cytokines such as VEGF, SDF-1, TGFβ, and TNFα, which systemically initiate premetastatic niches. These premetastatic niches are characterized by the accumulation of BM-derived cells, and selective induction of organ-specific chemoattractants, growth factors, and ECM-related proteins, which provide permissive local microenvironments for recruiting the incoming tumor cells, leading to the initiation and establishment of micrometastases [145]. Pioneering studies by Lyden and colleagues have shown that the premetastatic niche is comprised of BM-derived VEGFR1+ hematopoietic progenitor cells, which express VLA-4 (also known as integrin α4β1), and that tumor-specific growth factors upregulate fibronectin, a VLA-4 ligand in resident fibroblasts, suggesting a possible mechanism by which the permissive niche recruits incoming tumor cells [143, 161]. Similarly, Hiratuska et al. have demonstrated that tumor-secreted factors including VEGF-A, TGFβ, and TNFα induce expression of chemoattractants, such as S100A8 and S100A9 by lung endothelial cells and Mac1+ myeloid cells [143, 161], that facilitate the homing of tumor cells to the premetastatic sites, via induction of serum amyloid A3 (SAA3). Notably, SAA3 stimulated NF-κB signaling in the macrophages via TLR4 and facilitated metastasis [146], suggesting the therapeutic potential of blocking SAA3-TLR4 for the prevention of pulmonary metastasis. Giaccia and colleagues have shown that lysyl oxidase (LOX) secreted by hypoxic tumors accumulates in the lungs and supports premetastatic niche formation. LOX remodels ECM by crosslinking collagen IV, which recruits CD11b+ myeloid cells that cleave collagen by secreting MMP2, enhancing the invasion and recruitment of BM cells and metastasizing tumor cells. LOX inhibition prevents CD11b+ cell recruitment and metastatic growth. CD11b+ cells and LOX were also shown to colocalize in biopsies of human metastases [142, 162, 163].
In another mechanism, within the premetastatic niche, fibroblasts expressed periostin which contributed to cancer stem cell maintenance and expansion through Wnt signaling leading to metastasis [164]. In a similar study, metastatic tumor cells, by secreting tenascin C, enhanced stem cell signaling via Notch in the metastatic niche [165]. In the premetastatic lung, BM-derived myeloid progenitor cells were shown to secrete the proteoglycan versican, which induced mesenchymal -to- epithelial transition (MET) of disseminated metastatic tumor cells, accelerating tumor outgrowth in the lungs [8, 166]. Notably, this tumor outgrowth was facilitated by BM-derived endothelial progenitor cells (EPCs), which by initiating the angiogenic switch resulted in the progression of micro- to macrometastases [167]. The premetastatic niche has become an exciting area of research in the quest for novel therapeutic and prophylactic strategies against metastasis [168]. In contrast, a novel mechanism was recently described, whereby metastasis-incompetent tumors generate metastasis-suppressive microenvironments in the lungs by inducing the expression of a potent antiangiogenic factor, thrombospondin 1 (Tsp-1) , in the recruited BM-derived myeloid cells [169]. Tsp-1 induction is mediated by the activity of prosaposin (PSAP), a protein secreted by poorly metastatic cells, which acts systemically to reprogram myeloid cells into metastasis-inhibitory cells [169].
5 The Contribution of TME to Therapeutic Resistance
A major research focus to determine the mechanisms of therapeutic resistance has largely been the analysis of tumor cells, and resistance mechanisms involving secondary pathway mutations or bypass mechanisms within the tumor cells, such as EGFR (T790M) mutations or MET receptor amplification have been identified. Importantly, more recent studies have begun to unravel that heterologous cell types within tumors can actively influence therapeutic response and elicit resistance [170, 171].
5.1 Contribution of TME to Resistance to Radiation Therapy
Given that lung cancer is one of the leading causes of death from cancer worldwide, new and effective treatments are urgently needed [172, 173]. Approximately 70% of NSCLC patients receive radiotherapy (RT), either alone or in combination with other treatment modalities such as surgery or chemotherapy [174]. In patients who are unable to tolerate surgical resection because of medical co-morbidities, conventional RT is an alternative, but with poor long-term survival of 15–30% and local failure of up to 50% [175–177]. Retrospective and nonrandomized prospective data suggest that further dose escalation in NSCLC may be associated with better outcomes [178–181]. Additional improvement of the therapeutic ratio for NSCLC will likely come from different radiation dosing schedules. However, for patients with locally advanced disease, the benefit of dose escalation beyond 60 Gy has not been supported by level I evidence. A recent randomized study by the Radiation Therapy Oncology Group (RTOG) in patients with locally advanced NSCLC showed worse survival rates for patients receiving 74 Gy versus 60Gy with concurrent chemotherapy [182].
Accurate delivery of the ionizing radiation (IR) that allows more precise deposition of dose in the tumor while progressively reducing any unwanted dose to surrounding normal tissues has motivated hypofractionated radiation schedules [174]. Stereotactic body RT (SBRT) takes advantage of this favorable dose distribution and gained credence recently as a result of phase II studies with promising outcomes for early-stage medically inoperable NSCLC [183]. However, lack of pathological confirmation of primary tumor control, different definitions of NSCLC control after SBRT, and serious toxicity, particularly for centrally placed tumor, raises concerns about the utility of dose escalation [184, 185]. Clinical factors can explain some of the failures, such as a large tumor and/or advanced tumor stage, but many failures still go unexplained, for tumors with apparently similar sizes, stages, grades, and delivered doses.
It is clear from such clinical considerations and from a wealth of experimental research, that biological factors also have a crucial role in determining treatment success. The main biological factors affecting outcome after RT [186] include intrinsic radioresistance of the tumor cells [187], the ability of the surviving cells, including cancer stem cells, to repopulate [188], and the extent of hypoxia. Sensitizing strategies commonly focus on either targeting intrinsic properties of tumor cells or the vasculature . Recently, targeting the TME has become an even more compelling option to impede tumor progression and augment RT responses [189, 190]. For example, the recognition that tumor infiltration by inflammatory cells and other BM-derived cells contributes to RT responses, particularly tumor regrowth, provides a new route to augment RT efficacy [191, 192].
There is considerable evidence that the microenvironment regulates many tumor responses to radiation, thus providing novel routes for manipulating the response to radiotherapy [193–195]. Of particular interest is the activity of TGFβ, which is a critical signal in cancer and plays a detrimental role to tumor responses to RT. In NSCLC, increased TGFβ activity correlates with tumor progression, increased tumor growth and angiogenesis [196]. TGFβ signaling activation in TME has been identified as a key factor for chemotherapy resistance in NSCLC [197]. Although little is known about how TGFβ modulates the irradiated TME, given its pleiotropic roles in NSCLC, TGFβ inhibition may increase tumor cell radiosensitivity and shift the microenvironment to augment NSCLC response to radiotherapy. TGFβ ligands are enriched in the TME, where their production by stromal or tumor cells varies according to tumor phenotype [198]. The use of clinically viable TGFβ inhibitors in oncology is motivated by rationales to reduce metastasis, augment existing cancer therapies, and to improve tumor vaccines [199]. TGFβ signaling blockade enhances glioblastoma (GBM) response to chemoradiation in preclinical models [200, 201], and specifically inhibits GBM cancer stem cell renewal in vitro and in vivo [202].
In addition to a well recognized phenomenon of the impact of TGFβ on tumor-promoting effects and metastasis [203], TGFβ mediates an effective DNA damage response in epithelial cells via control of ATM kinase activity [204]. TGFβ activity is controlled by production as a latent complex that requires extracellular modification to initiate ligand binding to ubiquitous receptors; this activation is efficiently induced by ionizing radiation, in part due to the presence of a redox sensitive motif in the latency associated peptide (reviewed in [189]). As a consequence, we have shown that inhibiting TGFβ promotes clonogenic cell death of mouse and human breast cancer and GBM cells in vitro and that systemically neutralizing TGFβ enhances RT action in GBM and breast cancer preclinical models [205, 206]. Given that radiation-induced TGFβ is also a significant factor in lung fibrosis , a late tissue toxicity that limits effective tumor control [207], the application of TGFβ antagonists in radiation treatment of NSCLC is clinically viable.
Recent preclinical studies support the potential for improving radiotherapy by use of TGFβ inhibitors (Du and Barcellos-Hoff, unpublished data). As observed for brain and breast tumors [205, 208], most murine and human lung cancer cells were sensitized by TGFβ inhibition prior to radiation, as measured by in vitro clonogenic assays . Using the Lewis lung cancer syngeneic subcutaneous tumors , tumor growth control was significantly improved by use of TGFβ neutralizing antibodies concurrent with single or fractionated radiation treatment. Notably, even though irradiated tumors treated with TGFβ inhibition were significantly smaller at experiment termination, hypoxia was higher and vessel density was also significantly more decreased than that of non-irradiated, bigger tumors. Martin Brown has shown that hypoxia promoted mobilization of CD11b+ monocytes, which secrete the pro-angiogenic factor MMP9 into the TME in preclinical GBM, and blockade of this crucial event prevents tumor recurrence [207]. The combined treatment of radiation and TGFβ inhibition decreased CD11b+/MMP9 monocytes, suggesting that TGFβ is necessary for the recruitment of the CD11b+/MMP9 cells and tumor regrowth.
Given that radiation-induced immunity is critical for long term benefit [209], we also studied the effect of combined treatment of fractionated radiation and TGFβ inhibition on the peripheral anti-tumor immune response. Analysis of monocyte maturation and activation markers CD11b and F4/80 in tumors suggests that distinct BM cells are recruited as a function of treatment : the F4/80+ macrophage population is more differentiated, while CD11b+ cells are more immature. TGFβ inhibition concurrent with radiation treatment also affects systemic maturation as evidenced by analysis of cells from spleens of treated mice. These preliminary data suggest that TGFβ inhibition concurrent with fractionated radiation treatment may cooperate in directing both the microenvironment and the immune system towards an anti-tumor response, which could lead not only to better control of primary tumor growth but also to abrogation of relapse.
5.2 Contribution of TME to Resistance to Antiangiogenic Therapies and EGFR-TKIs
BM-derived cells have also been shown to provide resistance to cancer therapeutics. For example, BM-derived Gr1+ myeloid cells [210] have been shown to make tumors refractory to anti-VEGF treatment [211], by obviating the necessity for VEGF signaling and reinitiating angiogenesis. In another study, administration of vascular disruptive agents (VDA) or chemotherapeutics caused acute hypoxia and necrosis in tumors and triggered an accumulation of endothelial progenitor cells at the tumor leading edge to reinitiate angiogenesis [212]. This appears to be an adaptive response of the tumor to develop evasive resistance to potent anti-angiogenesis therapy. In lung cancer, the tumor-stroma cross talk was implicated in mediating resistance to EGFR-TKIs. For example, fibroblast-derived hepatocyte growth factor (HGF) was shown to induce EGFR-TKI (gefitinib) resistance in NSCLC with EGFR-activating mutations [107, 108].
6 The TME as a Therapeutic Target in Lung Cancer
Lung cancer is a global public health problem with an estimated 1.3 million new cases each year [213]. In the United States, approximately 226,160 new cases of lung cancer are diagnosed per year with over 160,000 deaths. Despite advances in treatment options, including minimally invasive surgical resection, stereotactic radiation, and novel chemotherapeutic regimens, the 5-year survival rate in NSCLC remains at approximately 15%. Available targeted therapies such as EGFR TKIs (erlotinib and gefitinib) and EML4-ALK inhibitor (crizotinib) benefit only 15–20% of NSCLC patients who carry specific drug-sensitive mutations. Even in these patients, acquired resistance is a major impediment to a durable therapeutic response [65–67]. Moreover, a majority of the patients with lung cancer patients do not exhibit an actionable molecular aberration. Therefore, traditional standard cytotoxic chemotherapies remain the only treatment option for the majority of advanced NSCLC patients, and these treatments also usually fail, resulting in an aggressive metastatic relapse . As such, there is an unmet medical need for the development of additional targeted therapies for lung cancer patients. In this context, more recent studies have begun to focus on the TME as an unexplored target for drug discovery, with an increased interest in evaluating anti-angiogenic, immunomodulatory, and anti-inflammatory agents in the treatment of various malignancies , including NSCLC [214] (Table 1).
6.1 Antiangiogenic Therapies in Lung Cancer
Drugs that either block tumor vascularization or interfere with the activity of growth factor receptors and molecular pathways that are triggered by activation of these receptors have already been used in clinical practice [215]. Bevacizumab , a humanized monoclonal antibody against VEGF, has been approved in many countries for use in combination with first-line platinum-based chemotherapy (carboplatin and paclitaxel) for the treatment of NSCLC patients with advanced stage disease [216, 217]. Approvals were based upon an improvement in response rate (RR) and progression-free survival (PFS) observed with the addition of bevacizumab to chemotherapy in two large phase III studies, the North American Eastern Cooperative Oncology Group (ECOG) 4599 [218] and the European AVAiL [219]. The encouraging results with bevacizumab has led to approval of Aflibercept (VEGF Trap), which is a recombinant VEGF receptor-antibody protein fusion with affinity for VEGF-A, VEGF-B and placental growth factor (PlGF), which acts as a decoy receptor preventing angiogenesis [220]. Aflibercept , has been approved for metastatic colorectal cancer, and it has been evaluated in second-line therapy of NSCLC. A randomized phase III trial of second-line docetaxel with or without aflibercept in platinum-pretreated patients with advanced non-squamous NSCLC failed its primary endpoint of overall survival, despite higher response rates and progression free survival in the experimental arm [221].
Other promising anti-angiogenic agents include small molecule TKIs targeting the VEGF receptor (VEGFR). Motesanib , a selective oral inhibitor of VEGF receptors-1, 2, and 3, platelet-derived growth factor receptor (PDGFR), and c-Kit was tested in a randomized phase II trial in combination with carboplatin/paclitaxel as frontline therapy for patients with advanced NSCLC, and results showed that RR, PFS, and OS were comparable in those patients receiving either motesanib or bevacizumab [222]. However, an international randomized phase III trial with carboplatin/paclitaxel either alone or in combination with motesanib in patients with advanced NSCLC showed no improvement in overall survival compared with placebo; despite an improvement in PFS and overall response [223, 224]. Another phase III trial evaluated the addition of the multi-kinase inhibitor (including VEGFR2) sorafenib to chemotherapy in patients with advanced non-squamous NSCLC. Again, despite a slight but statistically significant improvement in PFS, there was no improvement in OS, the trial’s primary end-point [225]. A recently reported phase III trial assigned patients with advanced NSCLC who failed first-line therapy to docetaxel with and without nintedanib, a multi-angiogenic kinase inhibitor (VEGFR1-3/FGFR1-3/PDGFR/FLT3). Nintedanib in combination with docetaxel was associated with significant improvement in PFS and OS especially in patients with adenocarcinomas [226]. This is the first and only trial to demonstrate an improvement in OS using a targeted agent in the second-line setting. Finally, a phase III placebo-controlled trial of carboplatin and paclitaxel with and without the vascular disrupting agent vadimezan (ASA404) as first-line therapy for patients with advanced lung cancer did not meet the specified primary and secondary endpoints of OS and PFS [227–229]. Results from recently completed and ongoing phase III trials will determine if these newer antiangiogenic agents will be incorporated into clinical practice [230].
6.2 Anti-inflammatory Therapies in Lung Cancer
Compared to advances with antiangiogenic therapies, success with anti-inflammatory treatments have been less impactful. Previous clinical trials have indicated that long-term use of aspirin or other NSAIDs decreases the incidence of colorectal, esophageal, breast, lung, and bladder cancers [231]. While initial studies had focused on various broad-spectrum NSAIDs (which non-specifically inhibit both COX-1 and COX-2), more recent studies have examined COX-2 specific agents, such as celecoxib [125]. Significant pre-clinical and clinical data support the importance of COX-2 in the development and progression of NSCLC. Despite this, a protective effect of NSAIDs was not observed on lung cancer development in either the general or high-risk COPD populations [232]. Moreover, clinical trials of COX-2 inhibition in NSCLC have been disappointing [233]. The lack of clinical benefit in the Cancer and Leukemia Group B (CALGB) 30203 trial may be that COX-2 inhibition would be of value in COX-2-overexpressing tumors, emphasizing the need for a prospective, randomized trial that selects patients for therapy on the basis of COX-2 expression [234]. CALGB 30801 is a randomized phase III double-blind trial evaluating selective COX-2 inhibition in COX-2-expressing advanced NSCLC. However, given the gastrointestinal (GI) toxicity and non-specific activity of NSAIDs, and the cardiotoxicity of specific COX-2 inhibitors, the use of such agents continues to remain controversial [235].
Two recent studies have shed light on the future therapeutic potential of the NF-κB-mediated inflammatory pathway in lung cancer. Logsdon and colleagues found that in the presence of oncogenic Ras, inflammatory stimuli initiate a positive feedback loop involving NF-κB that further amplifies Ras activity to pathological levels [236]. Because a large proportion of lung cancer patients possess Ras mutations, disruption of this positive feedback loop may be an important strategy for cancer prevention. In another study, using mouse models of lung cancer, Verma and colleagues found that therapies targeting the enzyme IKK2 (involved in inflammation) and Timp1, which help activate the body’s inflammatory response , may effectively treat certain lung cancers [237].
6.3 Immune Checkpoint Inhibitors in Lung Cancer
Utilizing the immune system to eliminate cancer holds great potential, and therefore understanding the complexity of immunomodulation by tumors is important for the development of immunotherapy . A large numbers of different factors have been implicated in the inhibition of tumor-specific immune responses. These include regulatory T cells (Treg), MDSCs, various soluble factors and cytokines, and inhibitory molecules expressed by immune and tumor cells. As such, various strategies are being developed to enhance anti-tumor immune responses, including DC-based vaccines and antagonists of inhibitory signaling pathways to overcome ‘immune checkpoints’. The immune checkpoint pathway is a series of cell-cell interactions that inhibit effector T cells from being overactive under normal conditions [147, 238]. A major arm of the immune checkpoint pathway consists of the T cell surface receptor CTLA-4 . CTLA-4 is an inhibitory receptor expressed upon activation of a cytotoxic T cell, competing with the co-stimulatory receptor CD28 for their shared ligands CD80 and CD86 on antigen-presenting cells (APCs) [239]. Lung cancer can co-opt this mechanism to evade immune surveillance by stimulating abnormal expression of CTLA-4 on T-cells, leading to T cell anergy. The monoclonal antibodies, tremelimumab and ipilimumab, which inhibit CTLA-4, are being tested for the treatment of lung cancer. Although tremelimumab treatment did not enhance PFS in a phase II trial, objective radiological responses in 5% of participants was observed using tremelimumab. Ipilimumab treatment, on the other hand, showed slight improvement in immune-related progression-free survival (irPFS) in NSCLC patients when administered in a phased manner with platinum-based chemotherapy [240]. Interestingly, ipilimumab treatment showed high activity in squamous carcinomas [241]. These results prompted the phase III trial, testing ipilimumab in squamous NSCLC using the phased ipilimumab schedule [147].
PD-1 pathway is a major immune checkpoint by which tumors suppress lymphocyte function within the TME. PD-1 is a surface receptor on activated T cells, B cells, and NK cells. It binds to its ligands PD-L1 and PD-L2 on the surface of APCs or dendritic cells, leading to T cell anergy. Cancers can co-opt this pathway and aberrantly express PD-L1 on their cell surface, leading to T cell inactivation. It has been reported that sarcomatoid and adenocarcinoma subtypes of lung cancer express PD-L1, and its expression correlated with poor prognosis [242, 243].
Antibody blockade of PD-1 with its ligands (B7-H1/PD-L1 and B7-DC/PD-L2) showed promising activity in several malignancies [42]. In particular, blocking antibodies against PD-1 and PD-L1 have shown clinical activity in NSCLC [244, 245]. Nivolumab , a monoclonal antibody targeting PD-1, as been shown to restore cytokine secretion and proliferation of CD8+ T cells within lung tumors [246]. A phase I trial of Nivolumab showed a response rate of 17% in previously treated patients with advanced NSCLC, with responses persisting for a median duration of 17 months [244, 247]. As with any type of therapy, a main consideration for the implementation of an immunotherapy regimen is toxicity. For instance, Ipilimumab in combination with chemotherapy exhibited 14% to 17% higher incidence of all-cause grade 3/4 adverse events (AE) compared to chemotherapy alone [248]. Furthermore, a fatal side effect that occurs in a small proportion of patients following anti-CTLA-4 antibody treatment is hypophysitis, inflammation of the pituitary gland [249]. Nivolumab treatment exhibited 9% rate of treatment-related grade 3/4 AE [250], with three drug-related deaths due to pneumonitis [147]. Nivolumab treatment in combination with platinum-based chemotherapy yielded an objective response rate of 33% and a grade 3/4 AE rate of 49% [147]. A current phase I trial is testing the combination of nivolumab with ipilimumab for SCLC [147]. Another antibody targeting PD-1 is MK-3475. A phase I trial in 38 NSCLC patients showed an objective response rate of 24%, with a median PFS of 9.7 weeks and median OS of 51 weeks. 53% of patients had drug-related AEs, most of which were mild. Another approach to targeting the PD-1/PD-L1 pathway is using antibodies that target PD-L1 on cancer cells. One such antibody, MPDL3280A, yielded a 23% overall response rate, with only 11% drug-related grade 3–4 AEs in a phase I trial that included 85 patients with NSCLC [147].
Another avenue being explored to block tumor-driven immunosuppression is based on NK cell activity. NK cells express killer cell immunoglobulin-like receptors (KIRs) that downregulate NK cytotoxic activity, in response to HLA class I molecules on target cells. A higher incidence of the suppressive KIR2DL3 and its ligand HLA-C2 is observed in NSCLC [251] leading to reduced NK activity and protection of cancer cells from NK-mediated killing. A monoclonal antibody to KIR, Lirilumab (IPH2102), has demonstrated efficacy in combination with nivolumab in preclinical models. A trial combining nivolumab with lirilumab in human solid tumors, including 32 NSCLC patients is being conducted, as well as a trial combining lirilumab with ipilimumab [147].
6.4 MDSC as a Therapeutic Target in Lung Cancer
MDSCs have prognostic importance in multiple solid tumors. Emerging data has begun to support the utility of circulating MDSCs as a predictive marker for cancer immunotherapy and for predicting clinical response to systemic chemotherapy in patients with advanced solid tumors [252]. An increase in the number of MDSCs evokes strong immune suppressive activity in cancer patients [153–155], and greatly limits the efficacy of immune therapy. In a randomized phase II clinical trial of advanced stage SCLC, depletion of MDSCs with ATRA substantially improved the immune response to vaccination, suggesting that this approach can be used to enhance the effect of immune interventions in cancer [253]. These studies are consistent with the demonstration that targeting MDSCs augments antitumor activity against lung cancer in mice [157].
7 Future Directions
Analysis of TME in lung cancer is a relatively new area of investigation. Therefore, major efforts are required to identify individual stromal components and unravel heterotypic reciprocal crosstalk signaling pathways between the stroma and tumor cells in NSCLC. This is a major challenge given the high heterogeneity of genetic and epigenetic alterations present in the tumor, differences in host genetic background, as well as tissue-specific responses. Understanding the cellular and molecular mechanisms underlying these processes will provide novel avenues leading to the discovery of biomarkers for disease stratification, molecular diagnosis and prognosis, and devising therapeutic strategies against lung cancer. Over 10 years ago, it was suggested that treatments options for NSCLC other than chemotherapy needed to be investigated [254]. So far, only one phase III clinical trial showed survival benefit of combining an anti-angiogenic agent to standard platinum-based chemotherapy in patients with advanced stage NSCLC. Selected groups of patients responded to antiangiogenic therapies that result in tumor shrinkage and disease stabilization; however, in aggregate, antiangiogenic therapy has not yet had a major clinical impact in most of the trials conducted so far [215]. Many clinical benefits are short-lived; while numerous trials have shown an increase in survival of patients treated with antiangiogenic therapy, the increase for many has been a matter of months [255]. Several possibilities have been suggested to explain why anti-angiogenic trials have not yielded significant benefit in NSCLC. For example, lack of predictive biomarkers continues to be a major hurdle in the selection of adequate patient cohorts that are most likely to benefit. In fact, some studies have alluded to a possible link between antiangiogenic therapy and increased metastasis in multiple tumor types [256, 257].
Immunotherapy has been heralded as a new era of lung cancer therapy. Blocking PD1-PDL1 or CTLA-4 immune checkpoints has resulted in striking and durable responses, with global overall response rates of 20% to 25% as monotherapy in metastatic NSCLC. In order to increase response rates, it has been suggested that identifying patients who might respond to immunotherapy would be particularly useful, as correlations between PD-L1 expression and EGFR mutation, and PD-1 expression and KRAS mutations has been observed (D’Incecco et al. Journal of Thoracic Oncology 2014). Notably, activation of the PD-1 pathway was shown to contribute to immune escape in mutant EGFR-driven lung tumors in mice, and blockade of this escape pathway improved survival [258]. These findings support further investigation of anti-PD-L1 or anti-PD-1 agents in combination with various targeted therapies, including epigenetic therapy. While immune checkpoint inhibitors such as ipilimumab (anti-CTLA-4 antibody) have been approved for the treatment of melanoma, they have yet not been approved for lung cancer. However, several classes of new drugs appear to be active in various ongoing clinical trials, and their impending approval for use in lung cancer is presumed. At present, several new therapeutic agents are being tested in more than 600 clinical trials in patients with advanced NSCLC, and based on early phase data exhibiting potential, some of these new agents have the capacity to translate to phase III trials, and eventually benefit patients.
References
Gao D, Mittal V (2009) The role of bone-marrow-derived cells in tumor growth, metastasis initiation and progression. Trends Mol Med 15:333–343
Hanahan D, Coussens LM (2012) Accessories to the crime: functions of cells recruited to the tumor microenvironment. Cancer Cell 21:309–322
Hanahan D, Weinberg RA (2011) Hallmarks of cancer: the next generation. Cell 144:646–674
Joyce JA, Pollard JW (2009) Microenvironmental regulation of metastasis. Nat Rev Cancer 9:239–252
Albini A, Sporn MB (2007) The tumour microenvironment as a target for chemoprevention. Nat Rev Cancer 7:139–147
DeNardo DG, Brennan DJ, Rexhepaj E, Ruffell B, Shiao SL, Madden SF, Gallagher WM, Wadhwani N, Keil SD, Junaid SA et al (2011) Leukocyte complexity predicts breast cancer survival and functionally regulates response to chemotherapy. Cancer Discov 1:54–67
Ebos JM, Kerbel RS (2011) Antiangiogenic therapy: impact on invasion, disease progression, and metastasis. Nat Rev Clin Oncol 8:210–221
Gao D, Vahdat LT, Wong S, Chang JC, Mittal V (2012) Microenvironmental regulation of epithelial-mesenchymal transitions in cancer. Cancer Res 72:4883–4889
Lee G, Walser TC, Dubinett SM (2009) Chronic inflammation, chronic obstructive pulmonary disease, and lung cancer. Curr Opin Pulm Med 15:303–307
Punturieri A, Szabo E, Croxton TL, Shapiro SD, Dubinett SM (2009) Lung cancer and chronic obstructive pulmonary disease: needs and opportunities for integrated research. J Natl Cancer Inst 101:554–559
Fridlender ZG, Sun J, Kim S, Kapoor V, Cheng G, Ling L, Worthen GS, Albelda SM (2009) Polarization of tumor-associated neutrophil phenotype by TGF-beta: “N1” versus “N2” TAN. Cancer Cell 16:183–194
Mantovani A, Sica A (2010) Macrophages, innate immunity and cancer: balance, tolerance, and diversity. Curr Opin Immunol 22:231–237
Orimo A, Gupta PB, Sgroi DC, Arenzana-Seisdedos F, Delaunay T, Naeem R, Carey VJ, Richardson AL, Weinberg RA (2005) Stromal fibroblasts present in invasive human breast carcinomas promote tumor growth and angiogenesis through elevated SDF-1/CXCL12 secretion. Cell 121:335–348
Zeng Q, Li S, Chepeha DB, Giordano TJ, Li J, Zhang H, Polverini PJ, Nor J, Kitajewski J, Wang CY (2005) Crosstalk between tumor and endothelial cells promotes tumor angiogenesis by MAPK activation of Notch signaling. Cancer Cell 8:13–23
Coussens LM, Werb Z (2002) Inflammation and cancer. Nature 420:860–867
Gadea BB, Joyce JA (2006) Tumour-host interactions: implications for developing anti-cancer therapies. Expert Rev Mol Med 8:1–32
Joyce JA (2005) Therapeutic targeting of the tumor microenvironment. Cancer Cell 7:513–520
Bergers G, Benjamin LE (2003) Angiogenesis: tumorigenesis and the angiogenic switch. Nat Rev Cancer 3:401–410
Hanahan D, Folkman J (1996) Patterns and emerging mechanisms of the angiogenic switch during tumorigenesis. Cell 86:353–364
Mantovani A, Allavena P, Sica A, Balkwill F (2008) Cancer-related inflammation. Nature 454:436–444
Gupta RA, Dubois RN (2001) Colorectal cancer prevention and treatment by inhibition of cyclooxygenase-2. Nat Rev Cancer 1:11–21
Rothwell PM, Fowkes FG, Belch JF, Ogawa H, Warlow CP, Meade TW (2011) Effect of daily aspirin on long-term risk of death due to cancer: analysis of individual patient data from randomised trials. Lancet 377:31–41
Rothwell PM, Wilson M, Price JF, Belch JF, Meade TW, Mehta Z (2012) Effect of daily aspirin on risk of cancer metastasis: a study of incident cancers during randomised controlled trials. Lancet 379:1591–1601
Murdoch C, Muthana M, Coffelt SB, Lewis CE (2008) The role of myeloid cells in the promotion of tumour angiogenesis. Nat Rev Cancer 8:618–631
Shojaei F, Wu X, Zhong C, Yu L, Liang XH, Yao J, Blanchard D, Bais C, Peale FV, van Bruggen N et al (2007) Bv8 regulates myeloid-cell-dependent tumour angiogenesis. Nature 450:825–831
Kessenbrock K, Plaks V, Werb Z (2010) Matrix metalloproteinases: regulators of the tumor microenvironment. Cell 141:52–67
Lewis CE, Pollard JW (2006) Distinct role of macrophages in different tumor microenvironments. Cancer Res 66:605–612
Qian B, Deng Y, Im JH, Muschel RJ, Zou Y, Li J, Lang RA, Pollard JW (2009) A distinct macrophage population mediates metastatic breast cancer cell extravasation, establishment and growth. PLoS One 4, e6562
Condeelis J, Pollard JW (2006) Macrophages: obligate partners for tumor cell migration, invasion, and metastasis. Cell 124:263–266
Coniglio SJ, Eugenin E, Dobrenis K, Stanley ER, West BL, Symons MH, Segall JE (2012) Microglial stimulation of glioblastoma invasion involves epidermal growth factor receptor (EGFR) and colony stimulating factor 1 receptor (CSF-1R) signaling. Mol Med 18:519–527
Goswami S, Sahai E, Wyckoff JB, Cammer M, Cox D, Pixley FJ, Stanley ER, Segall JE, Condeelis JS (2005) Macrophages promote the invasion of breast carcinoma cells via a colony-stimulating factor-1/epidermal growth factor paracrine loop. Cancer Res 65:5278–5283
Wyckoff J, Wang W, Lin EY, Wang Y, Pixley F, Stanley ER, Graf T, Pollard JW, Segall J, Condeelis J (2004) A paracrine loop between tumor cells and macrophages is required for tumor cell migration in mammary tumors. Cancer Res 64:7022–7029
Gocheva V, Zeng W, Ke D, Klimstra D, Reinheckel T, Peters C, Hanahan D, Joyce JA (2006) Distinct roles for cysteine cathepsin genes in multistage tumorigenesis. Genes Dev 20:543–56
Shree T, Olson OC, Elie BT, Kester JC, Garfall AL, Simpson K, Bell-McGuinn KM, Zabor EC, Brogi E, Joyce JA (2011) Macrophages and cathepsin proteases blunt chemotherapeutic response in breast cancer. Genes Dev 25:2465–2479
Pyonteck SM, Akkari L, Schuhmacher AJ, Bowman RL, Sevenich L, Quail DF, Olson OC, Quick ML, Huse JT, Teijeiro V et al (2013) CSF-1R inhibition alters macrophage polarization and blocks glioma progression. Nat Med 19:1264–1272
Balkwill F, Charles KA, Mantovani A (2005) Smoldering and polarized inflammation in the initiation and promotion of malignant disease. Cancer Cell 7:211–217
Grivennikov SI, Greten FR, Karin M (2010) Immunity, inflammation, and cancer. Cell 140:883–899
Ben-Neriah Y, Karin M (2011) Inflammation meets cancer, with NF-κB as the matchmaker. Nat Immunol 12:715–723
Ammirante M, Luo JL, Grivennikov S, Nedospasov S, Karin M (2010) B-cell-derived lymphotoxin promotes castration-resistant prostate cancer. Nature 464:302–305
Vakkila J, Lotze MT (2004) Inflammation and necrosis promote tumour growth. Nat Rev Immunol 4:641–648
Zitvogel L, Apetoh L, Ghiringhelli F, Kroemer G (2008) Immunological aspects of cancer chemotherapy. Nat Rev Immunol 8:59–73
Pardoll DM (2012) The blockade of immune checkpoints in cancer immunotherapy. Nat Rev Cancer 12:252–264
Chioda M, Peranzoni E, Desantis G, Papalini F, Falisi E, Solito S, Samantha S, Mandruzzato S, Bronte V (2011) Myeloid cell diversification and complexity: an old concept with new turns in oncology. Cancer Metastasis Rev 30:27–43
Gabrilovich DI, Nagaraj S (2009) Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev Immunol 9:162–174
Greten TF, Manns MP, Korangy F (2011) Myeloid derived suppressor cells in human diseases. Int Immunopharmacol 11:802–807
Serafini P, Borrello I, Bronte V (2006) Myeloid suppressor cells in cancer: recruitment, phenotype, properties, and mechanisms of immune suppression. Semin Cancer Biol 16:53–65
Gabitass RF, Annels NE, Stocken DD, Pandha HA, Middleton GW (2011) Elevated myeloid-derived suppressor cells in pancreatic, esophageal and gastric cancer are an independent prognostic factor and are associated with significant elevation of the Th2 cytokine interleukin-13. Cancer Immunol Immunother 60:1419–1430
Solito S, Falisi E, Diaz-Montero CM, Doni A, Pinton L, Rosato A, Francescato S, Basso G, Zanovello P, Onicescu G et al (2011) A human promyelocytic-like population is responsible for the immune suppression mediated by myeloid-derived suppressor cells. Blood 118:2254–2265
Hoechst B, Voigtlaender T, Ormandy L, Gamrekelashvili J, Zhao F, Wedemeyer H, Lehner F, Manns MP, Greten TF, Korangy F (2009) Myeloid derived suppressor cells inhibit natural killer cells in patients with hepatocellular carcinoma via the NKp30 receptor. Hepatology 50:799–807
Talmadge JE, Gabrilovich DI (2013) History of myeloid-derived suppressor cells. Nat Rev Cancer 13:739–752
Ostrand-Rosenberg S, Sinha P (2009) Myeloid-derived suppressor cells: linking inflammation and cancer. J Immunol 182:4499–4506
Trikha P, Carson WE (2014) Signaling pathways involved in MDSC regulation. Biochim Biophys Acta 1846:55–65
Vasquez-Dunddel D, Pan F, Zeng Q, Gorbounov M, Albesiano E, Fu J, Blosser RL, Tam AJ, Bruno T, Zhang H et al (2013) STAT3 regulates arginase-I in myeloid-derived suppressor cells from cancer patients. J Clin Invest 123:1580–1589
Movahedi K, Guilliams M, Van den Bossche J, Van den Bergh R, Gysemans C, Beschin A, De Baetselier P, Van Ginderachter JA (2008) Identification of discrete tumor-induced myeloid-derived suppressor cell subpopulations with distinct T cell-suppressive activity. Blood 111:4233–4244
Markowitz J, Wesolowski R, Papenfuss T, Brooks TR, Carson WE (2013) Myeloid-derived suppressor cells in breast cancer. Breast Cancer Res Treat 140:13–21
Kusmartsev S, Cheng F, Yu B, Nefedova Y, Sotomayor E, Lush R, Gabrilovich D (2003) All-trans-retinoic acid eliminates immature myeloid cells from tumor-bearing mice and improves the effect of vaccination. Cancer Res 63:4441–4449
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61:69–90
Herbst RS, Heymach JV, Lippman SM (2008) Lung cancer. N Engl J Med 359:1367–1380
Slebos RJ, Kibbelaar RE, Dalesio O, Kooistra A, Stam J, Meijer CJ, Wagenaar SS, Vanderschueren RG, van Zandwijk N, Mooi WJ (1990) K-ras oncogene activation as a prognostic marker in adenocarcinoma of the lung. N Engl J Med 323:561–565
Takahashi T, Nau MM, Chiba I, Birrer MJ, Rosenberg RK, Vinocour M, Levitt M, Pass H, Gazdar AF, Minna JD (1989) p53: a frequent target for genetic abnormalities in lung cancer. Science 246:491–494
Zochbauer-Muller S, Gazdar AF, Minna JD (2002) Molecular pathogenesis of lung cancer. Annu Rev Physiol 64:681–708
Haber DA, Bell DW, Sordella R, Kwak EL, Godin-Heymann N, Sharma SV, Lynch TJ, Settleman J (2005) Molecular targeted therapy of lung cancer: EGFR mutations and response to EGFR inhibitors. Cold Spring Harb Symp Quant Biol 70:419–426
Lynch TJ, Bell DW, Sordella R, Gurubhagavatula S, Okimoto RA, Brannigan BW, Harris PL, Haserlat SM, Supko JG, Haluska FG et al (2004) Activating mutations in the epidermal growth factor receptor underlying responsiveness of non-small-cell lung cancer to gefitinib. N Engl J Med 350:2129–2139
Sequist LV, Martins RG, Spigel D, Grunberg SM, Spira A, Jänne PA, Joshi VA, McCollum D, Evans TL, Muzikansky A et al (2008) First-line gefitinib in patients with advanced non-small-cell lung cancer harboring somatic EGFR mutations. J Clin Oncol 26:2442–2449
Choi YL, Soda M, Yamashita Y, Ueno T, Takashima J, Nakajima T, Yatabe Y, Takeuchi K, Hamada T, Haruta H et al (2010) EML4-ALK mutations in lung cancer that confer resistance to ALK inhibitors. N Engl J Med 363:1734–1739
Engelman JA, Zejnullahu K, Mitsudomi T, Song Y, Hyland C, Park JO, Lindeman N, Gale CM, Zhao X, Christensen J et al (2007) MET amplification leads to gefitinib resistance in lung cancer by activating ERBB3 signaling. Science 316:1039–1043
Pao W, Miller VA, Politi KA, Riely GJ, Somwar R, Zakowski MF, Kris MG, Varmus H (2005) Acquired resistance of lung adenocarcinomas to gefitinib or erlotinib is associated with a second mutation in the EGFR kinase domain. PLoS Med 2, e73
Farmer P, Bonnefoi H, Anderle P, Cameron D, Wirapati P, Becette V, André S, Piccart M, Campone M, Brain E et al (2009) A stroma-related gene signature predicts resistance to neoadjuvant chemotherapy in breast cancer. Nat Med 15:68–74
Finak G, Bertos N, Pepin F, Sadekova S, Souleimanova M, Zhao H, Chen H, Omeroglu G, Meterissian S, Omeroglu A et al (2008) Stromal gene expression predicts clinical outcome in breast cancer. Nat Med 14:518–527
Chang HY, Sneddon JB, Alizadeh AA, Sood R, West RB, Montgomery K, Chi JT, van de Rijn M, Botstein D, Brown PO (2004) Gene expression signature of fibroblast serum response predicts human cancer progression: similarities between tumors and wounds. PLoS Biol 2, E7
Navab R, Strumpf D, Bandarchi B, Zhu CQ, Pintilie M, Ramnarine VR, Ibrahimov E, Radulovich N, Leung L, Barczyk M et al (2011) Prognostic gene-expression signature of carcinoma-associated fibroblasts in non-small cell lung cancer. Proc Natl Acad Sci U S A 108:7160–7165
Ito M, Ishii G, Nagai K, Maeda R, Nakano Y, Ochiai A (2012) Prognostic impact of cancer-associated stromal cells in stage I lung adenocarcinoma patients. Chest 142:151–8
Nakamura H, Saji H, Ogata A, Hosaka M, Hagiwara M, Saijo T, Kawasaki N, Kato H (2003) cDNA microarray analysis of gene expression in pathologic stage IA nonsmall cell lung carcinomas. Cancer 97:2798–2805
Ramaswamy S, Ross KN, Lander ES, Golub TR (2003) A molecular signature of metastasis in primary solid tumors. Nat Genet 33:49–54
Ilie M, Long E, Hofman V, Selva E, Bonnetaud C, Boyer J, Vénissac N, Sanfiorenzo C, Ferrua B, Marquette CH et al (2014) Clinical value of circulating endothelial cells and of soluble CD146 levels in patients undergoing surgery for non-small cell lung cancer. Br J Cancer 110:1236–1243
Diaz-Montero CM, Salem ML, Nishimura MI, Garrett-Mayer E, Cole DJ, Montero AJ (2009) Increased circulating myeloid-derived suppressor cells correlate with clinical cancer stage, metastatic tumor burden, and doxorubicin-cyclophosphamide chemotherapy. Cancer Immunol Immunother 58:49–59
Sharma S, Dubinett S, Salgia R (2012) CD14(+)S100A9(+) myeloid-derived suppressor cells portend decreased survival in patients with advanced lung cancer. Am J Respir Crit Care Med 186:940–941
Bellocq A, Antoine M, Flahault A, Philippe C, Crestani B, Bernaudin JF, Mayaud C, Milleron B, Baud L, Cadranel J (1998) Neutrophil alveolitis in bronchioloalveolar carcinoma: induction by tumor-derived interleukin-8 and relation to clinical outcome. Am J Pathol 152:83–92
Eck M, Schmausser B, Scheller K, Brändlein S, Müller-Hermelink HK (2003) Pleiotropic effects of CXC chemokines in gastric carcinoma: differences in CXCL8 and CXCL1 expression between diffuse and intestinal types of gastric carcinoma. Clin Exp Immunol 134:508–515
Kimura YN, Watari K, Fotovati A, Hosoi F, Yasumoto K, Izumi H, Kohno K, Umezawa K, Iguchi H, Shirouzu K et al (2007) Inflammatory stimuli from macrophages and cancer cells synergistically promote tumor growth and angiogenesis. Cancer Sci 98:2009–2018
Al-Shibli K, Al-Saad S, Donnem T, Persson M, Bremnes RM, Busund LT (2009) The prognostic value of intraepithelial and stromal innate immune system cells in non-small cell lung carcinoma. Histopathology 55:301–312
Dieu-Nosjean MC, Antoine M, Danel C, Heudes D, Wislez M, Poulot V, Rabbe N, Laurans L, Tartour E, de Chaisemartin L et al (2008) Long-term survival for patients with non-small-cell lung cancer with intratumoral lymphoid structures. J Clin Oncol 26:4410–4417
Becker M, Müller CB, De Bastiani MA, Klamt F (2014) The prognostic impact of tumor-associated macrophages and intra-tumoral apoptosis in non-small cell lung cancer. Histol Histopathol 29:21–31
Dai F, Liu L, Che G, Yu N, Pu Q, Zhang S, Ma J, Ma L, You Z (2010) The number and microlocalization of tumor-associated immune cells are associated with patient’s survival time in non-small cell lung cancer. BMC Cancer 10:220
Takanami I, Takeuchi K, Naruke M (2000) Mast cell density is associated with angiogenesis and poor prognosis in pulmonary adenocarcinoma. Cancer 88:2686–2692
Al-Shibli KI, Donnem T, Al-Saad S, Persson M, Bremnes RM, Busund LT (2008) Prognostic effect of epithelial and stromal lymphocyte infiltration in non-small cell lung cancer. Clin Cancer Res 14:5220–5227
Wakabayashi O, Yamazaki K, Oizumi S, Hommura F, Kinoshita I, Ogura S, Dosaka-Akita H, Nishimura M (2003) CD4+ T cells in cancer stroma, not CD8+ T cells in cancer cell nests, are associated with favorable prognosis in human non-small cell lung cancers. Cancer Sci 94:1003–1009
Shimizu K, Nakata M, Hirami Y, Yukawa T, Maeda A, Tanemoto K (2010) Tumor-infiltrating Foxp3+ regulatory T cells are correlated with cyclooxygenase-2 expression and are associated with recurrence in resected non-small cell lung cancer. J Thorac Oncol 5:585–590
Edlund K, Lindskog C, Saito A, Berglund A, Pontén F, Göransson-Kultima H, Isaksson A, Jirström K, Planck M, Johansson L et al (2012) CD99 is a novel prognostic stromal marker in non-small cell lung cancer. Int J Cancer 131:2264–2273
Lohr M, Edlund K, Botling J, Hammad S, Hellwig B, Othman A, Berglund A, Lambe M, Holmberg L, Ekman S et al (2013) The prognostic relevance of tumour-infiltrating plasma cells and immunoglobulin kappa C indicates an important role of the humoral immune response in non-small cell lung cancer. Cancer Lett 333:222–228
Demarchi LM, Reis MM, Palomino SA, Farhat C, Takagaki TY, Beyruti R, Saldiva PH, Capelozzi VL (2000) Prognostic values of stromal proportion and PCNA, Ki-67, and p53 proteins in patients with resected adenocarcinoma of the lung. Mod Pathol 13:511–520
Maeshima AM, Niki T, Maeshima A, Yamada T, Kondo H, Matsuno Y (2002) Modified scar grade: a prognostic indicator in small peripheral lung adenocarcinoma. Cancer 95:2546–2554
Shimosato Y, Suzuki A, Hashimoto T, Nishiwaki Y, Kodama T, Yoneyama T, Kameya T (1980) Prognostic implications of fibrotic focus (scar) in small peripheral lung cancers. Am J Surg Pathol 4:365–373
Augsten M (2014) Cancer-associated fibroblasts as another polarized cell type of the tumor microenvironment. Front Oncol 4:62
Madar S, Goldstein I, Rotter V (2013) ‘Cancer associated fibroblasts’–more than meets the eye. Trends Mol Med 19:447–453
Polanska UM, Orimo A (2013) Carcinoma-associated fibroblasts: non-neoplastic tumour-promoting mesenchymal cells. J Cell Physiol 228:1651–1657
Bremnes RM, Dønnem T, Al-Saad S, Al-Shibli K, Andersen S, Sirera R, Camps C, Marinez I, Busund LT (2011) The role of tumor stroma in cancer progression and prognosis: emphasis on carcinoma-associated fibroblasts and non-small cell lung cancer. J Thorac Oncol 6:209–217
Direkze NC, Hodivala-Dilke K, Jeffery R, Hunt T, Poulsom R, Oukrif D, Alison MR, Wright NA (2004) Bone marrow contribution to tumor-associated myofibroblasts and fibroblasts. Cancer Res 64:8492–8495
Kalluri R, Zeisberg M (2006) Fibroblasts in cancer. Nat Rev Cancer 6:392–401
Ostman A, Augsten M (2009) Cancer-associated fibroblasts and tumor growth–bystanders turning into key players. Curr Opin Genet Dev 19:67–73
Tripathi M, Billet S, Bhowmick NA (2012) Understanding the role of stromal fibroblasts in cancer progression. Cell Adh Migr 6:231–235
Xing F, Saidou J, Watabe K (2010) Cancer associated fibroblasts (CAFs) in tumor microenvironment. Front Biosci 15:166–179
Abulaiti A, Shintani Y, Funaki S, Nakagiri T, Inoue M, Sawabata N, Minami M, Okumura M (2013) Interaction between non-small-cell lung cancer cells and fibroblasts via enhancement of TGF-β signaling by IL-6. Lung Cancer 82:204–213
Vicent S, Sayles LC, Vaka D, Khatri P, Gevaert O, Chen R, Zheng Y, Gillespie AK, Clarke N, Xu Y et al (2012) Cross-species functional analysis of cancer-associated fibroblasts identifies a critical role for CLCF1 and IL-6 in non-small cell lung cancer in vivo. Cancer Res 72:5744–5756
Chen WJ, Ho CC, Chang YL, Chen HY, Lin CA, Ling TY, Yu SL, Yuan SS, Chen YJ, Lin CY et al (2014) Cancer-associated fibroblasts regulate the plasticity of lung cancer stemness via paracrine signalling. Nat Commun 5:3472
Shintani Y, Abulaiti A, Kimura T, Funaki S, Nakagiri T, Inoue M, Sawabata N, Minami M, Morii E, Okumura M (2013) Pulmonary fibroblasts induce epithelial mesenchymal transition and some characteristics of stem cells in non-small cell lung cancer. Ann Thorac Surg 96:425–433
Wang W, Li Q, Yamada T, Matsumoto K, Matsumoto I, Oda M, Watanabe G, Kayano Y, Nishioka Y, Sone S et al (2009) Crosstalk to stromal fibroblasts induces resistance of lung cancer to epidermal growth factor receptor tyrosine kinase inhibitors. Clin Cancer Res 15:6630–6638
Yano S, Yamada T, Takeuchi S, Tachibana K, Minami Y, Yatabe Y, Mitsudomi T, Tanaka H, Kimura T, Kudoh S et al (2011) Hepatocyte growth factor expression in EGFR mutant lung cancer with intrinsic and acquired resistance to tyrosine kinase inhibitors in a Japanese cohort. J Thorac Oncol 6:2011–2017
Chaudhri VK, Salzler GG, Dick SA, Buckman MS, Sordella R, Karoly ED, Mohney R, Stiles BM, Elemento O, Altorki NK et al (2013) Metabolic alterations in lung cancer-associated fibroblasts correlated with increased glycolytic metabolism of the tumor. Mol Cancer Res 11:579–592
Franses JW, Edelman ER (2011) The evolution of endothelial regulatory paradigms in cancer biology and vascular repair. Cancer Res 71:7339–7344
Pober JS, Sessa WC (2007) Evolving functions of endothelial cells in inflammation. Nat Rev Immunol 7:803–815
Franses JW, Baker AB, Chitalia VC, Edelman ER (2011) Stromal endothelial cells directly influence cancer progression. Sci Transl Med 3:66ra65
Dundar E, Oner U, Peker BC, Metintas M, Isiksoy S, Ak G (2008) The significance and relationship between mast cells and tumour angiogenesis in non-small cell lung carcinoma. J Int Med Res 36:88–95
Herbst RS, Onn A, Sandler A (2005) Angiogenesis and lung cancer: prognostic and therapeutic implications. J Clin Oncol 23:3243–3256
Hu J, Bianchi F, Ferguson M, Cesario A, Margaritora S, Granone P, Goldstraw P, Tetlow M, Ratcliffe C, Nicholson AG et al (2005) Gene expression signature for angiogenic and nonangiogenic non-small-cell lung cancer. Oncogene 24:1212–1219
Offersen BV, Pfeiffer P, Hamilton-Dutoit S, Overgaard J (2001) Patterns of angiogenesis in nonsmall-cell lung carcinoma. Cancer 91:1500–1509
Ding BS, Nolan DJ, Guo P, Babazadeh AO, Cao Z, Rosenwaks Z, Crystal RG, Simons M, Sato TN, Worgall S et al (2011) Endothelial-derived angiocrine signals induce and sustain regenerative lung alveolarization. Cell 147:539–553
Lee JH, Bhang DH, Beede A, Huang TL, Stripp BR, Bloch KD, Wagers AJ, Tseng YH, Ryeom S, Kim CF (2014) Lung stem cell differentiation in mice directed by endothelial cells via a BMP4-NFATc1-thrombospondin-1 axis. Cell 156:440–455
Harris AL (2002) Hypoxia–a key regulatory factor in tumour growth. Nat Rev Cancer 2:38–47
Semenza GL (2003) Targeting HIF-1 for cancer therapy. Nat Rev Cancer 3:721–732
Li X, Lu Y, Liang K, Pan T, Mendelsohn J, Fan Z (2008) Requirement of hypoxia-inducible factor-1alpha down-regulation in mediating the antitumor activity of the anti-epidermal growth factor receptor monoclonal antibody cetuximab. Mol Cancer Ther 7:1207–1217
Minakata K, Takahashi F, Nara T, Hashimoto M, Tajima K, Murakami A, Nurwidya F, Yae S, Koizumi F, Moriyama H et al (2012) Hypoxia induces gefitinib resistance in non-small-cell lung cancer with both mutant and wild-type epidermal growth factor receptors. Cancer Sci 103:1946–1954
Murakami A, Takahashi F, Nurwidya F, Kobayashi I, Minakata K, Hashimoto M, Nara T, Kato M, Tajima K, Shimada N et al (2014) Hypoxia increases gefitinib-resistant lung cancer stem cells through the activation of insulin-like growth factor 1 receptor. PLoS One 9, e86459
Houghton AM (2013) Mechanistic links between COPD and lung cancer. Nat Rev Cancer 13:233–245
Lee JM, Yanagawa J, Peebles KA, Sharma S, Mao JT, Dubinett SM (2008) Inflammation in lung carcinogenesis: new targets for lung cancer chemoprevention and treatment. Crit Rev Oncol Hematol 66:208–217
Yao H, Rahman I (2009) Current concepts on the role of inflammation in COPD and lung cancer. Curr Opin Pharmacol 9:375–383
Keohavong P, Kahkonen B, Kinchington E, Yin J, Jin J, Liu X, Siegfried JM, DI YP (2011) K-ras mutations in lung tumors from NNK-treated mice with lipopolysaccharide-elicited lung inflammation. Anticancer Res 31:2877–2882
Xu X, Padilla MT, Li B, Wells A, Kato K, Tellez C, Belinsky SA, Kim KC, Lin Y (2014) MUC1 in macrophage: contributions to cigarette smoke-induced lung cancer. Cancer Res 74:460–470
Murin S, Inciardi J (2001) Cigarette smoking and the risk of pulmonary metastasis from breast cancer. Chest 119:1635–1640
Scanlon EF, Suh O, Murthy SM, Mettlin C, Reid SE, Cummings KM (1995) Influence of smoking on the development of lung metastases from breast cancer. Cancer 75:2693–2699
Abrams JA, Lee PC, Port JL, Altorki NK, Neugut AI (2008) Cigarette smoking and risk of lung metastasis from esophageal cancer. Cancer Epidemiol Biomarkers Prev 17:2707–2713
Murin S, Pinkerton KE, Hubbard NE, Erickson K (2004) The effect of cigarette smoke exposure on pulmonary metastatic disease in a murine model of metastatic breast cancer. Chest 125:1467–1471
Das Roy L, Pathangey LB, Tinder TL, Schettini JL, Gruber HE, Mukherjee P (2009) Breast-cancer-associated metastasis is significantly increased in a model of autoimmune arthritis. Breast Cancer Res 11:R56
Roy LD, Curry JM, Sahraei M, Besmer DM, Kidiyoor A, Gruber HE, Mukherjee P (2013) Arthritis augments breast cancer metastasis: role of mast cells and SCF/c-Kit signaling. Breast Cancer Res 15:R32
Yan L, Cai Q, Xu Y (2013) The ubiquitin-CXCR4 axis plays an important role in acute lung infection-enhanced lung tumor metastasis. Clin Cancer Res 19:4706–4716
Jiang M, Xu X, Bi Y, Xu J, Qin C, Han M (2014) Systemic inflammation promotes lung metastasis via E-selectin upregulation in mouse breast cancer model. Cancer Biol Ther 15:789–796
Stathopoulos GT, Sherrill TP, Han W, Sadikot RT, Yull FE, Blackwell TS, Fingleton B (2008) Host nuclear factor-kappaB activation potentiates lung cancer metastasis. Mol Cancer Res 6:364–371
Said N, Sanchez-Carbayo M, Smith SC, Theodorescu D (2012) RhoGDI2 suppresses lung metastasis in mice by reducing tumor versican expression and macrophage infiltration. J Clin Invest 122:1503–1518
Qian BZ, Li J, Zhang H, Kitamura T, Zhang J, Campion LR, Kaiser EA, Snyder LA, Pollard JW (2011) CCL2 recruits inflammatory monocytes to facilitate breast-tumour metastasis. Nature 475:222–225
Kim S, Takahashi H, Lin WW, Descargues P, Grivennikov S, Kim Y, Luo JL, Karin M (2009) Carcinoma-produced factors activate myeloid cells through TLR2 to stimulate metastasis. Nature 457:102–106
Carlini MJ, De Lorenzo MS, Puricelli L (2011) Cross-talk between tumor cells and the microenvironment at the metastatic niche. Curr Pharm Biotechnol 12:1900–1908
Erler JT, Bennewith KL, Cox TR, Lang G, Bird D, Koong A, Le QT, Giaccia AJ (2009) Hypoxia-induced lysyl oxidase is a critical mediator of bone marrow cell recruitment to form the premetastatic niche. Cancer Cell 15:35–44
Hiratsuka S, Watanabe A, Aburatani H, Maru Y (2006) Tumour-mediated upregulation of chemoattractants and recruitment of myeloid cells predetermines lung metastasis. Nat Cell Biol 8:1369–1375
Kaplan RN, Psaila B, Lyden D (2006) Bone marrow cells in the ‘pre-metastatic niche’: within bone and beyond. Cancer Metastasis Rev 25:521–529
Psaila B, Lyden D (2009) The metastatic niche: adapting the foreign soil. Nat Rev Cancer 9:285–293
Hiratsuka S, Watanabe A, Sakurai Y, Akashi-Takamura S, Ishibashi S, Miyake K, Shibuya M, Akira S, Aburatani H, Maru Y (2008) The S100A8-serum amyloid A3-TLR4 paracrine cascade establishes a pre-metastatic phase. Nat Cell Biol 10:1349–1355
Creelan BC (2014) Update on immune checkpoint inhibitors in lung cancer. Cancer Control 21:80–89
Fisher JP, Heuijerjans J, Yan M, Gustafsson K, Anderson J (2014) γδ T cells for cancer immunotherapy: a systematic review of clinical trials. Oncoimmunology 3:e27572
Bonneville M, O’Brien RL, Born WK (2010) Gammadelta T cell effector functions: a blend of innate programming and acquired plasticity. Nat Rev Immunol 10:467–478
Kang N, Zhou J, Zhang T, Wang L, Lu F, Cui Y, Cui L, He W (2009) Adoptive immunotherapy of lung cancer with immobilized anti-TCRgammadelta antibody-expanded human gammadelta T-cells in peripheral blood. Cancer Biol Ther 8:1540–1549
Nakajima J, Murakawa T, Fukami T, Goto S, Kaneko T, Yoshida Y, Takamoto S, Kakimi K (2010) A phase I study of adoptive immunotherapy for recurrent non-small-cell lung cancer patients with autologous gammadelta T cells. Eur J Cardiothorac Surg 37:1191–1197
Kobayashi H, Tanaka Y, Shimmura H, Minato N, Tanabe K (2010) Complete remission of lung metastasis following adoptive immunotherapy using activated autologous gammadelta T-cells in a patient with renal cell carcinoma. Anticancer Res 30:575–579
Kusmartsev SA, Kusmartseva IN, Afanasyev SG, Cherdyntseva NV (1998) Immunosuppressive cells in bone marrow of patients with stomach cancer. Adv Exp Med Biol 451:189–194
Young MR, Lathers DM (1999) Myeloid progenitor cells mediate immune suppression in patients with head and neck cancers. Int J Immunopharmacol 21:241–252
Young MR, Wright MA, Pandit R (1997) Myeloid differentiation treatment to diminish the presence of immune-suppressive CD34+ cells within human head and neck squamous cell carcinomas. J Immunol 159:990–996
Srivastava MK, Andersson Å, Zhu L, Harris-White M, Lee JM, Dubinett S, Sharma S (2012) Myeloid suppressor cells and immune modulation in lung cancer. Immunotherapy 4:291–304
Srivastava MK, Zhu L, Harris-White M, Kar UK, Kar U, Huang M, Johnson MF, Lee JM, Elashoff D, Strieter R et al (2012) Myeloid suppressor cell depletion augments antitumor activity in lung cancer. PLoS One 7, e40677
Nagaraj S, Youn JI, Weber H, Iclozan C, Lu L, Cotter MJ, Meyer C, Becerra CR, Fishman M, Antonia S et al (2010) Anti-inflammatory triterpenoid blocks immune suppressive function of MDSCs and improves immune response in cancer. Clin Cancer Res 16:1812–1823
Huang A, Zhang B, Wang B, Zhang F, Fan KX, Guo YJ (2013) Increased CD14(+)HLA-DR (-/low) myeloid-derived suppressor cells correlate with extrathoracic metastasis and poor response to chemotherapy in non-small cell lung cancer patients. Cancer Immunol Immunother 62:1439–1451
Paget S (1989) The distribution of secondary growths in cancer of the breast. 1889. Cancer Metastasis Rev 8:98–101
Kaplan RN, Riba RD, Zacharoulis S, Bramley AH, Vincent L, Costa C, MacDonald DD, Jin DK, Shido K, Kerns SA et al (2005) VEGFR1-positive haematopoietic bone marrow progenitors initiate the pre-metastatic niche. Nature 438:820–827
Chang J, Erler J (2014) Hypoxia-mediated metastasis. Adv Exp Med Biol 772:55–81
Erler JT, Bennewith KL, Nicolau M, Dornhöfer N, Kong C, Le QT, Chi JT, Jeffrey SS, Giaccia AJ (2006) Lysyl oxidase is essential for hypoxia-induced metastasis. Nature 440:1222–1226
Malanchi I, Santamaria-Martínez A, Susanto E, Peng H, Lehr HA, Delaloye JF, Huelsken J (2012) Interactions between cancer stem cells and their niche govern metastatic colonization. Nature 481:85–89
Oskarsson T, Acharyya S, Zhang XH, Vanharanta S, Tavazoie SF, Morris PG, Downey RJ, Manova-Todorova K, Brogi E, Massagué J (2011) Breast cancer cells produce tenascin C as a metastatic niche component to colonize the lungs. Nat Med 17:867–874
Gao D, Joshi N, Choi H, Ryu S, Hahn M, Catena R, Sadik H, Argani P, Wagner P, Vahdat LT et al (2012) Myeloid progenitor cells in the premetastatic lung promote metastases by inducing mesenchymal to epithelial transition. Cancer Res 72:1384–1394
Gao D, Nolan DJ, Mellick AS, Bambino K, McDonnell K, Mittal V (2008) Endothelial progenitor cells control the angiogenic switch in mouse lung metastasis. Science 319:195–198
Stefanovic S, Schuetz F, Sohn C, Beckhove P, Domschke C (2013) Bone marrow microenvironment in cancer patients: immunological aspects and clinical implications. Cancer Metastasis Rev 32:163–178
Catena R, Bhattacharya N, El Rayes T, Wang S, Choi H, Gao D, Ryu S, Joshi N, Bielenberg D, Lee SB et al (2013) Bone marrow-derived gr1+ cells can generate a metastasis-resistant microenvironment via induced secretion of thrombospondin-1. Cancer Discov 3:578–589
Junttila MR, de Sauvage FJ (2013) Influence of tumour micro-environment heterogeneity on therapeutic response. Nature 501:346–354
Meads MB, Gatenby RA, Dalton WS (2009) Environment-mediated drug resistance: a major contributor to minimal residual disease. Nat Rev Cancer 9:665–674
Paull T, Cortez D, Bowers B, Elledge S, Gellert M (2001) Direct DNA binding by Brca1. Proc Natl Acad Sci U S A 98:6086–6091
Ye Q, Hu Y, Zhong H, Nye A, Belmont A, Li R (2001) BRCA1-induced large-scale chromatin unfolding and allele-specific effects of cancer-predisposing mutations. J Cell Biol 155:911–921
Xu X, Wagner K, Larson D, Weaver Z, Li C, Ried T, Hennighausen L, Wynshaw-Boris A, Deng C (1999) Conditional mutation of Brca1 in mammary epithelial cells results in blunted ductal morphogenesis and tumour formation. Nat Genet 22:37–43
Thakur S, Croce C (1999) Positive regulation of the BRCA1 promoter. J Biol Chem 274:8837–8843
Xu C, Brown M, Chambers J, Griffiths B, Nicolai H, Solomon E (1995) Distinct transcription start sites generate two forms of BRCA1 mRNA. Hum Mol Genet 4:2259–2264
Xu C-F, Chambers J, Solomon E (1997) Complex regulation of the BRCA1 gene. J Biol Chem 272:20994–20997
Dimitrov S, Matouskova E, Forejt J (2001) Expression of BRCA1, NBR1 and NBR2 genes in human breast cancer cells. Folia Biol 47:120–127
Gudas J, Li T, Nguyen H, Jensen D, Rauscher F, Cowan K (1996) Cell cycle regulation of BRCA1 messenger RNA in human breast epithelial cells. Cell Growth Differ 7:717–723
Spillman M, Bowcock A (1996) BRCA1 and BRCA2 mRNA levels are coordinately elevated in human breast cancer cells in response to estrogen. Oncogene 13:1639–1645
Suen T, Goss P (1999) Transcription of BRCA1 is dependent on the formation of a specific protein-DNA complex on the minimal BRCA1 Bi-directional promoter. J Biol Chem 274:31297–31304
Romagnolo D, Annab L, Thompson T, Risinger J, Terry L, Barrett J, Afshari C (1998) Estrogen upregulation of BRCA1 expression with no effect on localization. Mol Carcinog 22:102–109
Atlas E, Stramwasser M, Whiskin K, Mueller C (2000) GA-binding protein alpha/beta is a critical regulator of the BRCA1 promoter. Oncogene 19:1933–1940
Marquis S, Rajan J, Wynshaw-Boris A, Xu J, Yin G, Abel K, Weber B, Chodosh L (1995) The developmental pattern of Brca1 expression implies a role in differentiation of the breast and other tissues. Nat Genet 11:17–26
Welcsh P, Lee M, Gonzalez-Hernandez R, Black D, Mahadevappa M, Swisher E, Warrington J, King M (2002) BRCA1 transcriptionally regulates genes involved in breast tumorigenesis. Proc Natl Acad Sci U S A 99:7560–7565
Hennighausen L, Robinson G (1998) Think globally, act locally: the making of a mouse mammary gland. Genes Dev 12:449–455
Blackshear P, Goldsworthy S, Foley J, McAllister K, Bennett L, Collins N, Bunch D, Brown P, Wiseman R, Davis B (1998) Brca1 and Brca2 expression patterns in mitotic and meiotic cells of mice. Oncogene 16:61–68
Rajan J, Marquis S, Gardner H, Chodosh L (1997) Developmental expression of Brca2 colocalizes with Brca1 and is associated with proliferation and differentiation in multiple tissues. Dev Biol 184:385–401
Du S, Barcellos-Hoff MH (2013) Biologically augmenting radiation therapy by inhibiting TGFβ actions in carcinomas. Semin Radiat Oncol 23:242–251
Vignard J, Mirey G, Salles B (2013) Ionizing-radiation induced DNA double-strand breaks: a direct and indirect lighting up. Radiother Oncol 108:362–369
Borges FT, Melo SA, Özdemir BC, Kato N, Revuelta I, Miller CA, Gattone VH, LeBleu VS, Kalluri R (2013) TGF-β1–containing exosomes from injured epithelial cells activate fibroblasts to initiate tissue regenerative responses and fibrosis. J Am Soc Nephrol 24:385–392
Kioi M, Vogel H, Schultz G, Hoffman RM, Harsh GR, Brown JM (2010) Inhibition of vasculogenesis, but not angiogenesis, prevents the recurrence of glioblastoma after irradiation in mice. J Clin Invest 120:694–705
Barcellos-Hoff MH, Park C, Wright EG (2005) Radiation and the microenvironment—tumorigenesis and therapy. Nat Rev Cancer 5:867–875
Begg AC, Stewart FA, Vens C (2011) Strategies to improve radiotherapy with targeted drugs. Nat Cancer Rev 11:239–253
Erickson AC, Barcellos-Hoff MH (2003) The not-so innocent bystander: microenvironment as a target of cancer therapy. Expert Opin Ther Targets 7:71–88
Hasegawa Y, Takanashi S, Kanehira Y, Tsushima T, Imai T, Okumura K (2001) Transforming growth factor-beta1 level correlates with angiogenesis, tumor progression, and prognosis in patients with nonsmall cell lung carcinoma. Cancer 91:964–971
Goldstraw P, Ball D, Jett JR, Le Chevalier T, Lim E, Nicholson AG, Shepherd FA (2011) Non-small-cell lung cancer. Lancet 378:1727–1740
Jarvis E, Kirk J, Clarke C (1998) Loss of nuclear BRCA1 expression in breast cancers is associated with a highly proliferative tumor phenotype. Cancer Genet Cytogenet 101:109–115
Akhurst RJ, Hata A (2012) Targeting the TGF[beta] signalling pathway in disease. Nat Rev Drug Discov 11:790–811
Mengxian Z, Kleber S, Roehrich M, Timke C, Han N, Tuettenberg J, Martin-Villalba A, Debus J, Peschke P, Wirkner U et al (2011) Blockade of TGF-beta signaling by the TGF{beta}R-I kinase Inhibitor LY2109761 enhances radiation response and prolongs survival in glioblastoma. Cancer Res 71:155–67
Zhang M, Herion TW, Timke C, Han N, Hauser K, Weber KJ, Peschke P, Wirkner U, Lahn M, Huber PE (2011) Trimodal glioblastoma treatment consisting of concurrent radiotherapy, temozolomide, and the novel TGF-β receptor I kinase inhibitor LY2109761. Neoplasia 13:537–549
Peñuelas S, Anido J, Prieto-Sánchez RM, Folch G, Barba I, Cuartas I, García-Dorado D, Poca MA, Sahuquillo J, Baselga J et al (2009) TGF-[beta] increases glioma-initiating cell self-renewal through the induction of LIF in human glioblastoma. Cancer Cell 15:315–327
Barcellos-Hoff MH, Akhurst RJ (2010) Transforming growth factor-beta in breast cancer: too much, too late. Breast Cancer Res Treat 11:202–208
Kirshner J, Jobling MF, Pajares MJ, Ravani SA, Glick A, Lavin M, Koslov S, Shiloh Y, Barcellos-Hoff MH (2006) Inhibition of TGFb1 signaling attenuates ATM activity in response to genotoxic stress. Cancer Res 66:10861–10868
Bouquet SF, Pal A, Pilones KA, Demaria S, Hann B, Akhurst RJ, Babb JS, Lonning SM, DeWyngaert JK, Formenti S et al (2011) Transforming growth factor β1 inhibition increases the radiosensitivity of breast cancer cells in vitro and promotes tumor control by radiation in vivo. Clin Cancer Res 17:6754–6765
Taylor J, Lymboura M, Pace P, A’hern R, Desai A, Shousha S, Coombes R, Ali S (1998) An important role for BRCA1 in breast cancer progression is indicated by its loss in a large proportion of non-familial breast cancers. Int J Cancer 79:334–342
Jones LP, Li M, Halama ED, Ma Y, Lubet R, Grubbs CJ, Deng CX, Rosen EM, Furth PA (2005) Promotion of mammary cancer development by tamoxifen in a mouse model of Brca1-mutation-related breast cancer. Oncogene 24:3554–3562
Barcellos-Hoff MH, Lyden D, Wang TC (2013) The evolution of the cancer niche during multistage carcinogenesis. Nat Rev Cancer 13:511–518
Formenti SC, Demaria S (2009) Systemic effects of local radiotherapy. Lancet Oncol 10:718–726
Yang L, DeBusk LM, Fukuda K, Fingleton B, Green-Jarvis B, Shyr Y, Matrisian LM, Carbone DP, Lin PC (2004) Expansion of myeloid immune suppressor Gr+ CD11b+ cells in tumor-bearing host directly promotes tumor angiogenesis. Cancer Cell 6:409–421
Shojaei F, Wu X, Malik AK, Zhong C, Baldwin ME, Schanz S, Fuh G, Gerber HP, Ferrara N (2007) Tumor refractoriness to anti-VEGF treatment is mediated by CD11b+ Gr1+ myeloid cells. Nat Biotechnol 25:911–920
Shaked Y, Ciarrocchi A, Franco M, Lee CR, Man S, Cheung AM, Hicklin DJ, Chaplin D, Foster FS, Benezra R et al (2006) Therapy-induced acute recruitment of circulating endothelial progenitor cells to tumors. Science 313:1785–1787
Jemal A, Tiwari RC, Murray T, Ghafoor A, Samuels A, Ward E, Feuer EJ, Thun MJ (2004) Cancer statistics, 2004. CA Cancer J Clin 54:8–29
Blumenschein GR (2012) Developmental antiangiogenic agents for the treatment of non-small cell lung cancer (NSCLC). Invest New Drugs 30:1802–1811
Korpanty G, Smyth E, Carney DN (2011) Update on anti-angiogenic therapy in non-small cell lung cancer: are we making progress? J Thorac Dis 3:19–29
Herbst RS (2008) Bevacizumab/chemotherapy in non-small-cell lung cancer: looking for a few good men? Clin Lung Cancer 9:75–76
Planchard D (2011) Bevacizumab in non-small-cell lung cancer: a review. Expert Rev Anticancer Ther 11:1163–1179
Sandler A, Gray R, Perry MC, Brahmer J, Schiller JH, Dowlati A, Lilenbaum R, Johnson DH (2006) Paclitaxel-carboplatin alone or with bevacizumab for non-small-cell lung cancer. N Engl J Med 355:2542–2550
Reck M, von Pawel J, Zatloukal P, Ramlau R, Gorbounova V, Hirsh V, Leighl N, Mezger J, Archer V, Moore N et al (2009) Phase III trial of cisplatin plus gemcitabine with either placebo or bevacizumab as first-line therapy for nonsquamous non-small-cell lung cancer: AVAil. J Clin Oncol 27:1227–1234
Huang J, Frischer JS, Serur A, Kadenhe A, Yokoi A, McCrudden KW, New T, O’Toole K, Zabski S, Rudge JS et al (2003) Regression of established tumors and metastases by potent vascular endothelial growth factor blockade. Proc Natl Acad Sci U S A 100:7785–7790
Neal JW, Wakelee HA (2013) Aflibercept in lung cancer. Expert Opin Biol Ther 13:115–120
Blumenschein GR, Kabbinavar F, Menon H, Mok TS, Stephenson J, Beck JT, Lakshmaiah K, Reckamp K, Hei YJ, Kracht K et al (2011) A phase II, multicenter, open-label randomized study of motesanib or bevacizumab in combination with paclitaxel and carboplatin for advanced nonsquamous non-small-cell lung cancer. Ann Oncol 22:2057–2067
Das M, Wakelee H (2012) Anti-angiogenic agents in Non-Small-Cell Lung Cancer (NSCLC): a perspective on the MONET1 (Motesanib NSCLC Efficacy and Tolerability) study. J Thorac Dis 4:558–561
Scagliotti GV, Vynnychenko I, Park K, Ichinose Y, Kubota K, Blackhall F, Pirker R, Galiulin R, Ciuleanu TE, Sydorenko O et al (2012) International, randomized, placebo-controlled, double-blind phase III study of motesanib plus carboplatin/paclitaxel in patients with advanced nonsquamous non-small-cell lung cancer: MONET1. J Clin Oncol 30:2829–2836
Paz-Ares LG, Biesma B, Heigener D, von Pawel J, Eisen T, Bennouna J, Zhang L, Liao M, Sun Y, Gans S et al (2012) Phase III, randomized, double-blind, placebo-controlled trial of gemcitabine/cisplatin alone or with sorafenib for the first-line treatment of advanced, nonsquamous non-small-cell lung cancer. J Clin Oncol 30:3084–3092
Reck M, Kaiser R, Mellemgaard A, Douillard JY, Orlov S, Krzakowski M, von Pawel J, Gottfried M, Bondarenko I, Liao M et al (2014) Docetaxel plus nintedanib versus docetaxel plus placebo in patients with previously treated non-small-cell lung cancer (LUME-Lung 1): a phase 3, double-blind, randomised controlled trial. Lancet Oncol 15:143–155
Lara PN, Douillard JY, Nakagawa K, von Pawel J, McKeage MJ, Albert I, Losonczy G, Reck M, Heo DS, Fan X et al (2011) Randomized phase III placebo-controlled trial of carboplatin and paclitaxel with or without the vascular disrupting agent vadimezan (ASA404) in advanced non-small-cell lung cancer. J Clin Oncol 29:2965–2971
McKeage MJ, Reck M, Jameson MB, Rosenthal MA, Gibbs D, Mainwaring PN, Freitag L, Sullivan R, Von Pawel J (2009) Phase II study of ASA404 (vadimezan, 5,6-dimethylxanthenone-4-acetic acid/DMXAA) 1800mg/m(2) combined with carboplatin and paclitaxel in previously untreated advanced non-small cell lung cancer. Lung Cancer 65:192–197
McKeage MJ, Von Pawel J, Reck M, Jameson MB, Rosenthal MA, Sullivan R, Gibbs D, Mainwaring PN, Serke M, Lafitte JJ et al (2008) Randomised phase II study of ASA404 combined with carboplatin and paclitaxel in previously untreated advanced non-small cell lung cancer. Br J Cancer 99:2006–2012
Aggarwal C, Somaiah N, Simon G (2012) Antiangiogenic agents in the management of non-small cell lung cancer: where do we stand now and where are we headed? Cancer Biol Ther 13:247–263
Wang D, Dubois RN (2006) Prostaglandins and cancer. Gut 55:115–122
Wall RJ, Shyr Y, Smalley W (2007) Nonsteroidal anti-inflammatory drugs and lung cancer risk: a population-based case control study. J Thorac Oncol 2:109–114
McCormack VA, Hung RJ, Brenner DR, Bickeböller H, Rosenberger A, Muscat JE, Lazarus P, Tjønneland A, Friis S, Christiani DC et al (2011) Aspirin and NSAID use and lung cancer risk: a pooled analysis in the International Lung Cancer Consortium (ILCCO). Cancer Causes Control 22:1709–1720
Edelman MJ, Hodgson L, Wang X, Kratzke RA, Vokes EE (2012) Cyclooxygenase-2 (COX-2) as a predictive marker for the use of COX-2 inhibitors in advanced non-small-cell lung cancer. J Clin Oncol 30:2019–2020; author reply 2020
Drazen JM (2005) COX-2 inhibitors–a lesson in unexpected problems. N Engl J Med 352:1131–1132
Daniluk J, Liu Y, Deng D, Chu J, Huang H, Gaiser S, Cruz-Monserrate Z, Wang H, Ji B, Logsdon CD (2012) An NF-κB pathway-mediated positive feedback loop amplifies Ras activity to pathological levels in mice. J Clin Invest 122:1519–1528
Xia Y, Yeddula N, Leblanc M, Ke E, Zhang Y, Oldfield E, Shaw RJ, Verma IM (2012) Reduced cell proliferation by IKK2 depletion in a mouse lung-cancer model. Nat Cell Biol 14:257–265
Langer CJ (2015) Emerging immunotherapies in the treatment of non-small cell lung cancer (NSCLC): the role of immune checkpoint inhibitors. Am J Clin Oncol 38:422–30
Callahan MK, Wolchok JD, Allison JP (2010) Anti-CTLA-4 antibody therapy: immune monitoring during clinical development of a novel immunotherapy. Semin Oncol 37:473–484
Wolchok JD, Hoos A, O’Day S, Weber JS, Hamid O, Lebbé C, Maio M, Binder M, Bohnsack O, Nichol G et al (2009) Guidelines for the evaluation of immune therapy activity in solid tumors: immune-related response criteria. Clin Cancer Res 15:7412–7420
Drilon A, Rekhtman N, Ladanyi M, Paik P (2012) Squamous-cell carcinomas of the lung: emerging biology, controversies, and the promise of targeted therapy. Lancet Oncol 13:e418–426
Konishi J, Yamazaki K, Azuma M, Kinoshita I, Dosaka-Akita H, Nishimura M (2004) B7-H1 expression on non-small cell lung cancer cells and its relationship with tumor-infiltrating lymphocytes and their PD-1 expression. Clin Cancer Res 10:5094–5100
Mu CY, Huang JA, Chen Y, Chen C, Zhang XG (2011) High expression of PD-L1 in lung cancer may contribute to poor prognosis and tumor cells immune escape through suppressing tumor infiltrating dendritic cells maturation. Med Oncol 28:682–688
Brahmer JR (2014) Immune checkpoint blockade: the hope for immunotherapy as a treatment of lung cancer? Semin Oncol 41:126–132
Sznol M, Chen L (2013) Antagonist antibodies to PD-1 and B7-H1 (PD-L1) in the treatment of advanced human cancer. Clin Cancer Res 19:1021–1034
Zhang Y, Huang S, Gong D, Qin Y, Shen Q (2010) Programmed death-1 upregulation is correlated with dysfunction of tumor-infiltrating CD8+ T lymphocytes in human non-small cell lung cancer. Cell Mol Immunol 7:389–395
Forde PM, Kelly RJ, Brahmer JR (2014) New strategies in lung cancer: translating immunotherapy into clinical practice. Clin Cancer Res 20:1067–1073
Lynch TJ, Bondarenko I, Luft A, Serwatowski P, Barlesi F, Chacko R, Sebastian M, Neal J, Lu H, Cuillerot JM et al (2012) Ipilimumab in combination with paclitaxel and carboplatin as first-line treatment in stage IIIB/IV non-small-cell lung cancer: results from a randomized, double-blind, multicenter phase II study. J Clin Oncol 30:2046–2054
Iwama S, De Remigis A, Callahan MK, Slovin SF, Wolchok JD, Caturegli P (2014) Pituitary expression of ctla-4 mediates hypophysitis secondary to administration of ctla-4 blocking antibody. Sci Transl Med 6:230ra245
Brahmer JR, Tykodi SS, Chow LQ, Hwu WJ, Topalian SL, Hwu P, Drake CG, Camacho LH, Kauh J, Odunsi K et al (2012) Safety and activity of anti-PD-L1 antibody in patients with advanced cancer. N Engl J Med 366:2455–2465
Al Omar S, Middleton D, Marshall E, Porter D, Xinarianos G, Raji O, Field JK, Christmas SE (2010) Associations between genes for killer immunoglobulin-like receptors and their ligands in patients with solid tumors. Hum Immunol 71:976–981
Diaz-Montero CM, Finke J, Montero AJ (2014) Myeloid-derived suppressor cells in cancer: therapeutic, predictive, and prognostic implications. Semin Oncol 41:174–184
Iclozan C, Antonia S, Chiappori A, Chen DT, Gabrilovich D (2013) Therapeutic regulation of myeloid-derived suppressor cells and immune response to cancer vaccine in patients with extensive stage small cell lung cancer. Cancer Immunol Immunother 62:909–918
Carney DN (2002) Lung cancer–time to move on from chemotherapy. N Engl J Med 346:126–128
Kerbel RS (2008) Tumor angiogenesis. N Engl J Med 358:2039–2049
Ebos JM, Lee CR, Cruz-Munoz W, Bjarnason GA, Christensen JG, Kerbel RS (2009) Accelerated metastasis after short-term treatment with a potent inhibitor of tumor angiogenesis. Cancer Cell 15:232–239
Paez-Ribes M, Allen E, Hudock J, Takeda T, Okuyama H, Vinals F, Inoue M, Bergers G, Hanahan D, Casanovas O (2009) Antiangiogenic therapy elicits malignant progression of tumors to increased local invasion and distant metastasis. Cancer Cell 15:220–231
Akbay EA, Koyama S, Carretero J, Altabef A, Tchaicha JH, Christensen CL, Mikse OR, Cherniack AD, Beauchamp EM, Pugh TJ et al (2013) Activation of the PD-1 pathway contributes to immune escape in EGFR-driven lung tumors. Cancer Discov 3:1355–1363
Acknowledgement
We thank Sharell Lee for reading the manuscript.
Author information
Authors and Affiliations
Corresponding authors
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Mittal, V., El Rayes, T., Narula, N., McGraw, T.E., Altorki, N.K., Barcellos-Hoff, M.H. (2016). The Microenvironment of Lung Cancer and Therapeutic Implications. In: Ahmad, A., Gadgeel, S. (eds) Lung Cancer and Personalized Medicine: Novel Therapies and Clinical Management. Advances in Experimental Medicine and Biology, vol 890. Springer, Cham. https://doi.org/10.1007/978-3-319-24932-2_5
Download citation
DOI: https://doi.org/10.1007/978-3-319-24932-2_5
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-24931-5
Online ISBN: 978-3-319-24932-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)