Abstract
In the quest for developing more effective immune therapy strategies for cancer, to date, unraveling and successful modulation of the mechanisms of tumor escape in the microenvironment became an urgent challenge. While immune suppression is considered an important mode of immune escape, this overview will deal with another important mechanism of immune escape in the tumor microenvironment: the microenvironment-regulated resistance of tumor cells toward the cytotoxic machinery of immune effector cells. We have recently studied the impact of the microenvironment to the development of immune resistance in multiple myeloma (MM) and will outline the backgrounds and current knowledge about the mechanisms and modulation of this type of immune escape.
No conflict statement: No potential conflicts of interest were disclosed.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Cytotoxic T cells
- Cancer immunotherapy
- Bone marrow
- Microenvironment
- Apoptosis
- Drug resistance
- Immune resistance
- Multiple myeloma
1 Introduction
Eradication of malignant cells through the cytotoxic machinery of immune cells such as cytotoxic T cells (CTLs) and natural killer (NK) cells is the ultimate aim of cellular immunotherapy of cancer. Starting from the early applications of allogeneic stem cell transplantation, followed by successful donor lymphocyte infusions, clinicians and immunologists have witnessed and appreciated the potential power of cellular immunotherapy in the battle of hematological and non-hematological malignancies [1]. Over the past two decades, the rapid identification of tumor-associated antigens [2, 3], development of new technologies such as T cell receptor (TCR)-gene transfer [4] and recently the remarkable successes of virus-specific T cells [5], tumor infiltrating lymphocytes (TIL) [6] and chimeric antigen receptor (CAR)-engineered T cells [7–9] in the treatment of various hematologic cancers, have elevated cancer immunotherapy to a new level, with high expectations. Nonetheless, despite the optimal activation and infiltration of abundant numbers of tumor-reactive CTLs or NK cells at tumor sites, human cancers, mainly due to genetic heterogeneity as well as micro-environmental influences, display various mechanisms to evade the immune attack [10, 11]. To date, the unraveling and the successful modulation of the mechanisms of tumor escape in the microenvironment became the most urgent challenges to achieve the next level of success in the immunotherapy of cancer [12, 13].
Currently, most scientists consider immune suppression as the main mechanism of immune escape in the tumor microenvironment [14–17]. There is, indeed, a large body of evidence that the tumor microenvironment is a suppressive inflammatory niche [18, 19], with the presence of several immune suppressive soluble factors, such as IDO, Arginase, INOS or TGF-β [20–22], secreted either from tumor cells [23], accessory cells (vascular endothelium, stromal cells, fibroblasts) [24] or from suppressive immune cells such as regulatory T cells [25], tumor associated macrophages [26], and myeloid derived suppressor cells [27, 28], many of which are recruited or induced in the microenvironment through crosstalk with tumor cells and tumor stroma [29]. This immune suppressive milieu also involves the strong upregulation of the immune checkpoint molecules PD1 on T cells and PD-L1/2 on tumor cells [30–35], and in some reported cases through interaction with stroma [36].
This chapter will, however, deal with another, entirely distinct mechanism of immune escape in the tumor microenvironment: the microenvironment-regulated resistance of tumor cells toward the cytotoxic machinery of immune effector cells. This resistance of tumor cells against cytotoxic attack, although extensively documented in the melanoma setting, and may be as important as “immune suppression”, has not received sufficient attention yet, probably because it has not been seen as a microenvironment-mediated phenomenon. We have recently studied the impact of the microenvironment to the development of immune resistance in multiple myeloma (MM) and will outline below the backgrounds and current knowledge about the mechanisms and modulation of this type of immune escape.
2 MM the Model for Investigating the Role of the Microenvironment in Human Cancers
MM is the malignant disorder of antibody producing clonal plasma cells [37]. It is the second most common hematological malignancy worldwide. Despite four exciting decades of drug development, MM remains incurable by chemotherapy due to the induction of drug resistance [38, 39]. Although experimental and clinical studies indicate the immune competence of MM cells and possibility to treat the disease with cellular immunotherapy [40–42], the overall outcome of allo-SCT, DLI or other experimental immunotherapies in MM is at most moderate, underscoring the ability of MM cells to evade the cellular immune attack.
Traditionally, the biology of MM and its therapy-response is studied preferably in the context of the microenvironment [43–46] because MM, especially in the initial phases of the disease, is entirely dependent on its natural habitat, the bone marrow (BM). Over the past decades, it has been extensively documented that the BM provides MM cells an ideal sanctuary by the production of several survival cytokines such as IL-6 and IL-8, VEGF, SDF-1 and many others, and by interactions of MM cells with extracellular matrix and BM accessory cells, in particular with stromal cells (BMSCs) and vascular endothelial cells (VECs) [47, 48]. In fact, once taken out of this natural niche, primary human MM cells rapidly die, and are very difficult to engraft even in the BM of immune deficient mice [49–51].
3 Importance of the Tumor Microenvironment in Drug Resistance
Investigations aiming at understanding the molecular basis of drug resistance of MM have demonstrated that the many soluble factors produced in the BM microenvironment not only provide proliferative and survival signals to MM cells, but also -individually or collectively- contribute to the development of drug resistance [52]. Perhaps, more important is the induction of drug resistance through the (integrin-mediated) adhesion of MM cells to BMSCs and VECs. This type of environmentally, thus epigenetically, regulated drug resistance, which is generally known as “Cell Adhesion-Mediated Drug Resistance” (CAM-DR), has originally been demonstrated for MM cells in the late nineties [53], and has subsequently been described also for several other hematological and non-hematological malignancies [54–58]. While integrins were initially shown to play a key role in this type of drug resistance, another important molecule appears to be NOTCH [59–61]. The relation of this environmentally regulated drug resistance with immune resistance will become obvious upon outlining the molecular nature of both types of resistance mechanisms.
4 The Apoptotic Pathways: Immune Resistance Meets Drug Resistance
Studies have shown that the molecular basis of CAM-DR is the cell adhesion-dependent triggering of a complex series of signaling events resulting in the transcriptional or posttranscriptional regulation of intracellular molecules involved in apoptotic signaling for programmed cell death [45, 46]. This ability of the microenvironment to modulate apoptotic pathways was, in fact, for us a major reason to start studying the relation of the microenvironment with immune resistance, because not only drugs, but also cytotoxic immune cells kill the tumor cells via the induction of apoptosis.
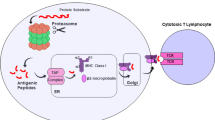
In general terms, apoptosis involves a complex cascade of molecular events that can be initiated inside the cell or by external dead signals. Accordingly, two main apoptotic pathways have been described: the intrinsic or mitochondrial pathway and the extrinsic or death receptor pathway [62, 63] (Fig. 7.1). Several pro-apoptotic anticancer drugs are designed for activating either of these pathways [64–71]. While immune cells can trigger the extrinsic death receptor pathway [72], a major mechanism of tumor cell lysis by CTLs and NK cells is the apoptosis induced by the degranulation of granzyme/perforin from the cytotoxic granules upon engagement with the target cells [73]. This specific mechanism has traditionally been defined as a separate pathway, although it is also initiated by external signals. As will be outlined below, more important is the considerable overlap between these pathways. All three signaling pathways eventually converge and mediate the execution phase of apoptosis via the activation of caspase-3. Hence, although immune cells may in some cases kill drug resistant tumor cells, specific drug resistance mechanisms may overlap with immune resistance mechanisms, with potentially important clinical consequences.
Apoptotic pathways activated by immune effector cells (CTLs/NK cells) and their regulation by the microenvironment. The simplified scheme demonstrates the key molecules and the overlap between the intrinsic, extrinsic and granzyme pathways of apoptosis. Also note the convergence of these pathways at the level of caspase 3 (Cas-3). The molecules that are known to be modulated by the stroma-tumor interactions are indicated with red (downregulated) and green (upregulated) boxes. Cas-3 caspase 3, Cas-8 caspase 8, Cas-9 caspase 9, Cyt-C cytochrome C, Gr-B granzyme B
5 The Modulation of Intrinsic, Extrinsic and Granzyme/Perforin Mediated Pathways of Apoptosis by the Microenvironment
The intrinsic apoptosis pathway, which involves mitochondrial depolarization, is initiated with the activation of pro-apoptotic proteins BAX and BAK, by BIM and BID, respectively [74] (Fig. 7.1). Oligomers or multimers of activated BAX and BAK engage with the mitochondrial membrane [75], induce the formation of mitochondrial pores and cause the release of cytochrome-c and SMAC/Diablo from the mitochondria into the cytosol [76]. By binding to the APAF-1 protein, cytochrome-c generates a large cytoplasmic complex, the apoptosome [77]. This complex binds and activates caspase-9, which in turn can activate several executioner caspases including the caspase-3 [78]. Several members of the BCL-2 family of proteins are important regulators of this pathway. Briefly, the mitochondrial membrane-associated BCL-2, BCL-2A1, BCL-W BCL-XL and MCL-1 proteins protect the cells form apoptosis by inhibiting the oligomerization of BAX and BAK. In contrast, the other members, such as PUMA and NOXA, improve the oligomerization of BAX and BAK via competitive binding to the former anti-apoptotic members of the BCL-2 family of proteins [79]. It has been extensively demonstrated that the mediator and regulatory molecules of the intrinsic pathway are significantly influenced by stroma-derived soluble factors and adhesion. For instance, IL-6, through activation of STAT3 upregulates the transcription of BCL-XL [80], induces adhesion of MM cells to stroma, downregulates BIM [81, 82] and BAX [83] and upregulates the anti-apoptotic BCL-2 proteins [83], especially of MCL-1 [44, 84]. Upregulation of MCL-1 and BCL-2 importantly contributes to drug resistance in MM, acute myeloid leukemia and B-cell acute lymphoblastic leukemia [85, 86]. Several studies indicate that not only integrins but also Notch signaling can have a major impact on the protection of tumor cells from apoptosis via modulation of the intrinsic pathway [59–61].
The signaling of the extrinsic apoptosis pathway involves the triggering of the tumor necrosis factor (TNF) family of death receptors including FAS (CD95), TNF-related apoptosis-inducing ligand-receptor 1 (TRAIL-R1), TRAIL-R2 and TNF receptor apoptosis-mediating protein (TRAMP). CTLs, especially of the CD4+ phenotype, frequently trigger FAS to activate the extrinsic pathway [87–93]. Triggering of death receptors activates FADD and then caspase-8, which in turn either directly activates caspase-3 or cleaves BID to signal via the intrinsic pathway [94]. In this pathway, the FLICE-like inhibitory protein FLIP can inhibit recruitment and activation of caspase-8. Soluble factors produced by BMSCs have been shown to upregulate FLIP expression [95]. In addition, integrin-mediated adhesion inhibits activation of caspase-8 due to increased cellular redistribution of FLIP [96]. In addition, we have recently shown that MM cell-stroma interactions significantly downregulates MM cell surface FAS expression [97].
Finally, the Granzyme/perforin pathway, which is exclusively utilized by CTLs and NK cells, is initiated by the degranulation of the preformed cytotoxic granules containing granzymes, perforin and serglycin into the immune synapse upon engagement of immune effector cells with target cells. Perforin, with its complement-like structure, generates membrane pores in the target cell to enable the cytotosolic entry of granzymes, which are the key molecules to induce signaling for cytotoxic cell-mediated apoptosis [98]. Among the 12 granzymes described until now, the granzyme B is the most abundantly present one in cytotoxic granules. It cleaves proteins after aspartate residues and can directly activate caspase-3 to trigger apoptosis. But, similar to caspase 8, granzyme-B can also trigger the intrinsic pathway of apoptosis through the activation of BID [98]. This clear overlap between the intrinsic pathway and granzyme-mediated lysis may have important consequences: for instance, melanoma cells that have been made resistant to CTL killing display signatures for hyperactivation of the NF-κB pathway, and overexpression of BCL-2, BCL-XL, and MCL-1 [99]. In fact, the efficacy of (CAR) T cell therapy can be significantly upregulated by inhibition of BCL-2 family of proteins [100, 101]. Thus the above described microenvironment-mediated drug resistance mechanisms of intrinsic pathway, may very well influence the outcome of CTL therapy.
In human cells, granzyme B can be inhibited by the proteinase inhibitor-9 (PI-9) [102]. The expression levels of this molecule in pediatric ALL cells correlate with their resistance against immune cell mediated lysis [103]. In the clinical setting, PI-9 expression is an important predictor of disease-free survival in melanoma patients treated with immunotherapy [104]. Interestingly, PI-9 gene expression can be induced by NF-κB signaling [105] as well as by hypoxia [106], which is a typical feature of the bone marrow microenvironment and has been shown to induce resistance against NK mediated lysis of MM cells [107].
Since all major apoptotic pathways converge at the level of caspase-3 activation, the (microenvironment-mediated) signals that regulate the activity of this executioner caspase may contribute to the development of both immune- and drug resistance. A specific group of molecules that regulates the activation of caspases is the IAP family of proteins [108–110]. XIAP, one of the best characterized IAPs, inhibits the activity of caspase-3, -7, and -9. Survivin (BIRC5), another well-known IAP, is frequently expressed in human tumor cells, and inhibits caspase-3 and -7. The activities of these molecules can be controlled, in turn, by the proapoptotic protein SMAC/Diablo, which is released upon mitochondrial depolarization [111, 112]. IAPs are indeed important in mediating both drug and immune resistance: for instance, in a recent study, cis-platinum resistant human ovarian cancer cells were found less susceptible toward NK-cell mediated killing than the parental cells partly due to the upregulation of cIAP-1 and -2 [113], Also survivin-3B, an alternative splice variant of survivin, was recently associated with chemotherapy resistance as well as with resistance to FAS-mediated immune cell toxicity [114]. Taken together, these and some earlier studies [115] demonstrate that drug resistance mechanisms show substantial overlap with the documented mechanisms of immune resistance. Unfortunately, however, the impact of the microenvironment on the induction of immune resistance has not been widely studied, except for MM.
The first indirect evidence for the microenvironment-mediated immune resistance in MM was provided by a study in which BM stroma conferred resistance to Apo2 ligand/TRAIL induced lysis in part by regulating c-FLIP [95]. In this case, soluble factors were found responsible for immune resistance. Using mainly an in vitro co-culture system, which was originally developed to study BMSC-induced drug resistance [44], we and other investigators have recently questioned whether the BM microenvironment can also cause a CAM-DR like immune resistance. Indeed, MM cells were protected against NK cells by co-culture with autologous BMSCs [116]. Subsequently, we have reported in vitro and in vivo evidence that MM cells are protected from CD4+ and CD8+ CTL-mediated lysis upon direct cellular interactions with VECs and BMSCs derived either from MM patients or from healthy individuals [97]. In our study, the protection of MM cells by accessory cells could be observed in the absence of immune suppression; hence, analogous to CAM-DR, we designated this type of cell adhesion-mediated immune resistance as CAM-IR. In further analysis, we discovered that MM cell-stroma interactions significantly downregulated MM cell FAS surface expression, but correction of FAS expression by bortezomib, did not entirely abrogate CAM-IR. By contrast, upregulation of survivin/MCL-1 appeared a central mechanism of CAM-IR, since we could entirely neutralize the immune resistance, in vitro as well as in a recently developed MM model in vivo [51], by combining T cells with the small molecule YM155, a suppressant of survivin and MCL-1 [117, 118]. Although we have not elucidated the entire mechanisms of CAM-IR yet, we have observed that CAM-IR, like CAM-DR, can be inhibited by interfering with integrin binding on intact cells, but unlike CAM-DR, cannot be induced by sole binding of MM cells to fibronectin, vitronectin, or laminin. Signals initiating CAM-IR are therefore most likely triggered by the collective action of integrins with other receptor-ligand systems. A possible candidate is the NOTCH signaling pathway, since we have recently observed that CAM-IR could also be abrogated by inhibition of the NOTCH pathway by gamma secretase inhibitors (GSI) (unpublished observations).
6 Towards the Design of Immune-Chemotherapy Strategies to Overcome Microenvironment-Mediated Immune Resistance
Our findings as well as evidence provided from other studies underscore the notion that the interactions between tumor cells and the cells of the microenvironment can induce resistance toward the cytotoxic machinery of immune cells through upregulation of anti-apoptotic molecules such as survivin, BCL-2 and MCL-1. Thus, successful anti-tumor immunotherapy may rely not only on eliminating the immune suppressive factors from the microenvironment, but also on modulation of the mechanisms that induce or mediate immune resistance. Among several theoretically conceivable strategies, specific attention needs to be paid for modulating the target molecules/pathways without compromising T cell function. With this respect, neutralizing survivin/MCL-1 with YM155 is a suitable strategy as we have not observed any T cell compromising effects of YM155. Several other pathways such as the PI3-K/AKT pathway, that are activated by microenvironmental influences play important roles in tumor development, survival, proliferation and drug resistance through induction of anti-apoptotic molecules [119]. The modulation of these pathways may be beneficial but need to be cautiously explored as these pathways may also play essential roles in T cell activation. For instance, the popular MEK inhibitors appear to impair T cell functions and are probably not suitable candidates to combine with immune therapy. On the other hand, selective inhibitors of BRAF were shown to enhance T-cell recognition of melanoma without affecting lymphocyte function [120]. More practical choices may be the general regulators of epigenetic mechanisms, such as histone deacetylase (HDAC) inhibitors as they have been shown to modulate drug resistance as well as to improve CTL-mediated lysis of tumor cells through upregulation of death receptors [121], and downregulating intracellular c-IAP-2 and BCL-XL expressions [122].
Among all these choices, however, the most appealing strategies may be disrupting the tumor-stroma interactions. Since T cells require integrins to generate a proper immune synapse, targeting integrin-mediated adhesion may not be feasible. However, in the BM an effective disruption of stroma-tumor interactions may be achieved using CXCR4 inhibitors, which induce mobilization of stem cells and myeloma cells from the BM. Such a strategy has already been shown to successfully overcome stroma-mediated activation of STAT3 [123] and HGF/MET [124] pathways, and to prevent the drug resistance of myeloma cells induced by BMSCs [125]. Furthermore, disturbing the stroma-tumor interactions may also prevent the upregulation of immune checkpoint molecules [36]. Finally, since NOTCH signaling also seems important in the microenvironment-mediated drug resistance and similarly may induce immune resistance, its modulation can also be explored. Nonetheless, more investigation is required on NOTCH, as there are conflicting reports on its role, especially on the cytotoxic activity of T cells [126–128].
7 Concluding Remarks
The appreciation of the role of the microenvironment, not only in the induction of immune suppressive events but also in the protection of tumor cells against cytotoxic T cell attack, will stimulate the research and encourage the scientists and clinicians to combine immunotherapy not only with agents that can modulate immune suppression but also with those that can eliminate the resistance mechanisms induced by the microenvironment. Furthermore, the increasing consciousness that drug resistance may in several cases also cause immune-resistance may stimulate the discussion whether heavily pretreated and multidrug resistant patients are suitable candidates for clinical testing of cellular immunotherapy strategies.
Abbreviations
- BM:
-
Bone marrow
- BMSC:
-
Bone marrow mesenchymal stromal cells
- CTL:
-
Cytotoxic T cell
- MM:
-
Multiple myeloma
- MSC:
-
Mesenchymal stromal cells
- NK cell:
-
Natural killer cells
References
Ringden O. Immunotherapy by allogeneic stem cell transplantation. Adv Cancer Res. 2007;97:25–60.
Wang RF, Rosenberg S. A human tumor antigens for cancer vaccine development. Immunol Rev. 1999;170:85–100.
Lewis JD, Reilly BD, Bright RK. Tumor-associated antigens: from discovery to immunity. Int Rev Immunol. 2003;22:81–112.
Schumacher TN. T-cell-receptor gene therapy. Nat Rev Immunol. 2002;2:512–9.
Bollard CM, Rooney CM, Heslop HE. T-cell therapy in the treatment of post-transplant lymphoproliferative disease. Nat Rev Clin Oncol. 2012;9:510–9.
Rosenberg SA, Dudley ME. Adoptive cell therapy for the treatment of patients with metastatic melanoma. Curr Opin Immunol. 2009;21:233–40.
Maus MV, Grupp SA, Porter DL, June CH. Antibody-modified T cells: CARs take the front seat for hematologic malignancies. Blood. 2014;123:2625–35.
Kochenderfer JN, Rosenberg SA. Treating B-cell cancer with T cells expressing anti-CD19 chimeric antigen receptors. Nat Rev Clin Oncol. 2013;10:267–76.
Brentjens RJ, Curran KJ. Novel cellular therapies for leukemia: CAR-modified T cells targeted to the CD19 antigen. Hematology Am Soc Hematol Educ Program. 2012;2012:143–51.
Gajewski TF, Meng Y, Blank C, Brown I, Kacha A, Kline J, Harlin H. Immune resistance orchestrated by the tumor microenvironment. Immunol Rev. 2006;213:131–45.
Runger TM, Klein CE, Becker JC, Brocker EB. The role of genetic instability, adhesion, cell motility, and immune escape mechanisms in melanoma progression. Curr Opin Oncol. 1994;6:188–96.
Gajewski TF, Fuertes M, Spaapen R, Zheng Y, Kline J. Molecular profiling to identify relevant immune resistance mechanisms in the tumor microenvironment. Curr Opin Immunol. 2011;23:286–92.
Leen AM, Rooney CM, Foster AE. Improving T cell therapy for cancer. Annu Rev Immunol. 2007;25:243–65.
Kim R, Emi M, Tanabe K, Arihiro K. Tumor-driven evolution of immunosuppressive networks during malignant progression. Cancer Res. 2006;66:5527–36.
Becker JC, Andersen MH, Schrama D, Thor Straten P. Immune-suppressive properties of the tumor microenvironment. Cancer Immunol Immunother. 2013;62:1137–48.
Zumsteg A, Christofori G. Corrupt policemen: inflammatory cells promote tumor angiogenesis. Curr Opin Oncol. 2009;21:60–70.
Gajewski TF, Meng Y, Harlin H. Immune suppression in the tumor microenvironment. J Immunother. 2006;29:233–40.
Mantovani A, Romero P, Palucka AK, Marincola FM. Tumour immunity: effector response to tumour and role of the microenvironment. Lancet. 2008;371:771–83.
Yu H, Pardoll D, Jove R. STATs in cancer inflammation and immunity: a leading role for STAT3. Nat Rev Cancer. 2009;9:798–809.
Munn DH. Indoleamine 2,3-dioxygenase, tumor-induced tolerance and counter-regulation. Curr Opin Immunol. 2006;18:220–5.
Ochoa AC, Zea AH, Hernandez C, Rodriguez PC. Arginase, prostaglandins, and myeloid-derived suppressor cells in renal cell carcinoma. Clin Cancer Res. 2007;13:721s–6s.
Wakefield LM, Hill CS. Beyond TGFbeta: roles of other TGFbeta superfamily members in cancer. Nat Rev Cancer. 2013;13:328–41.
Rabinovich GA, Gabrilovich D, Sotomayor EM. Immunosuppressive strategies that are mediated by tumor cells. Annu Rev Immunol. 2007;25:267–96.
Anderson KC. Targeted therapy of multiple myeloma based upon tumor-microenvironmental interactions. Exp Hematol. 2007;35:155–62.
Wang HY, Wang RF. Regulatory T cells and cancer. Curr Opin Immunol. 2007;19:217–23.
Pollard JW. Macrophages define the invasive microenvironment in breast cancer. J Leukoc Biol. 2008;84:623–30.
Diaz-Montero CM, Finke J, Montero AJ. Myeloid-derived suppressor cells in cancer: therapeutic, predictive, and prognostic implications. Semin Oncol. 2014;41:174–84.
Lindau D, Gielen P, Kroesen M, Wesseling P, Adema GJ. The immunosuppressive tumour network: myeloid-derived suppressor cells, regulatory T cells and natural killer T cells. Immunology. 2013;138:105–15.
Gabrilovich DI, Ostrand-Rosenberg S, Bronte V. Coordinated regulation of myeloid cells by tumours. Nat Rev Immunol. 2012;12:253–68.
Blank C, Brown I, Peterson AC, Spiotto M, Iwai Y, Honjo T, Gajewski TF. PD-L1/B7H-1 inhibits the effector phase of tumor rejection by T cell receptor (TCR) transgenic CD8+ T cells. Cancer Res. 2004;64:1140–5.
Myklebust JH, Irish JM, Brody J, Czerwinski DK, Houot R, Kohrt HE, Timmerman J, Said J, Green MR, Delabie J, Kolstad A, Alizadeh AA, Levy R. High PD-1 expression and suppressed cytokine signaling distinguish T cells infiltrating follicular lymphoma tumors from peripheral T cells. Blood. 2013;121:1367–76.
Deng L, Liang H, Burnette B, Beckett M, Darga T, Weichselbaum RR, Fu YX. Irradiation and anti-PD-L1 treatment synergistically promote antitumor immunity in mice. J Clin Invest. 2014;124:687–95.
Topalian SL, Drake CG, Pardoll DM. Targeting the PD-1/B7-H1(PD-L1) pathway to activate anti-tumor immunity. Curr Opin Immunol. 2012;24:207–12.
Thompson RH, Kuntz SM, Leibovich BC, Dong H, Lohse CM, Webster WS, Sengupta S, Frank I, Parker AS, Zincke H, Blute ML, Sebo TJ, Cheville JC, Kwon ED. Tumor B7-H1 is associated with poor prognosis in renal cell carcinoma patients with long-term follow-up. Cancer Res. 2006;66:3381–5.
Yang H, Bueso-Ramos C, DiNardo C, Estecio MR, Davanlou M, Geng QR, Fang Z, Nguyen M, Pierce S, Wei Y, Parmar S, Cortes J, Kantarjian H, Garcia-Manero G. Expression of PD-L1, PD-L2, PD-1 and CTLA4 in myelodysplastic syndromes is enhanced by treatment with hypomethylating agents. Leukemia. 2014;28:1280–8.
Tamura H, Ishibashi M, Yamashita T, Tanosaki S, Okuyama N, Kondo A, Hyodo H, Shinya E, Takahashi H, Dong H, Tamada K, Chen L, Dan K, Ogata K. Marrow stromal cells induce B7-H1 expression on myeloma cells, generating aggressive characteristics in multiple myeloma. Leukemia. 2013;27:464–72.
Raab MS, Podar K, Breitkreutz I, Richardson PG, Anderson KC. Multiple myeloma. Lancet. 2009;374:324–39.
Dalton WS. Drug resistance and drug development in multiple myeloma. Semin Oncol. 2002;29:21–5.
Kastritis E, Palumbo A, Dimopoulos MA. Treatment of relapsed/refractory multiple myeloma. Semin Hematol. 2009;46:143–57.
Kroger N, Badbaran A, Lioznov M, Schwarz S, Zeschke S, Hildebrand Y, Ayuk F, Atanackovic D, Schilling G, Zabelina T, Bacher U, Klyuchnikov E, Shimoni A, Nagler A, Corradini P, Fehse B, Zander A. Post-transplant immunotherapy with donor-lymphocyte infusion and novel agents to upgrade partial into complete and molecular remission in allografted patients with multiple myeloma. Exp Hematol. 2009;37:791–8.
van de Donk NW, Kröger N, Hegenbart U, Corradini P, San Miguel JF, Goldschmidt H, Perez-Simon JA, Zijlmans M, Raymakers RA, Montefusco V, Ayuk FA, van Oers MH, Nagler A, Verdonck LF, Lokhorst HM. Prognostic factors for donor lymphocyte infusions following non-myeloablative allogeneic stem cell transplantation in multiple myeloma. Bone Marrow Transplant. 2006;37:1135–41.
Lokhorst HM, Schattenberg A, Cornelissen JJ, van Oers MH, Fibbe W, Russell I, Donk NW, Verdonck LF. Donor lymphocyte infusions for relapsed multiple myeloma after allogeneic stem-cell transplantation: predictive factors for response and long-term outcome. J Clin Oncol. 2000;18:3031–7.
McMillin DW, Mitsiades CS. High-throughput approaches to discover novel immunomodulatory agents for cancer. Oncoimmunology. 2012;1:1406–8.
McMillin DW, Delmore J, Weisberg E, Negri JM, Geer DC, Klippel S, Mitsiades N, Schlossman RL, Munshi NC, Kung AL, Griffin JD, Richardson PG, Anderson KC, Mitsiades CS. Tumor cell-specific bioluminescence platform to identify stroma-induced changes to anticancer drug activity. Nat Med. 2010;16:483–9.
Dalton WS. The tumor microenvironment: focus on myeloma. Cancer Treat Rev. 2003;29 Suppl 1:11–9.
Mahtouk K, Moreaux J, Hose D, Rème T, Meissner T, Jourdan M, Rossi JF, Pals ST, Goldschmidt H, Klein B. Growth factors in multiple myeloma: a comprehensive analysis of their expression in tumor cells and bone marrow environment using Affymetrix microarrays. BMC Cancer. 2010;10:198.
Mitsiades CS, Hayden PJ, Anderson KC, Richardson PG. From the bench to the bedside: emerging new treatments in multiple myeloma. Best Pract Res Clin Haematol. 2007;20:797–816.
Hideshima T, Mitsiades C, Tonon G, Richardson PG, Anderson KC. Understanding multiple myeloma pathogenesis in the bone marrow to identify new therapeutic targets. Nat Rev Cancer. 2007;7:585–98.
Tassone P, Neri P, Burger R, Di Martino MT, Leone E, Amodio N, Caraglia M, Tagliaferri P. Mouse models as a translational platform for the development of new therapeutic agents in multiple myeloma. Curr Cancer Drug Targets. 2012;12:814–22.
Mitsiades CS, Anderson KC, Carrasco DR. Mouse models of human myeloma. Hematol Oncol Clin North Am. 2007;21:1051–69.
Groen RW, Noort WA, Raymakers RA, Prins HJ, Aalders L, Hofhuis FM, Moerer P, van Velzen JF, Bloem AC, van Kessel B, Rozemuller H, van Binsbergen E, Buijs A, Yuan H, de Bruijn JD, de Weers M, Parren PW, Schuringa JJ, Lokhorst HM, Mutis T, Martens AC. Reconstructing the human hematopoietic niche in immunodeficient mice: opportunities for studying primary multiple myeloma. Blood. 2012;120:e9–16.
Shain KH, Dalton WS. Environmental-mediated drug resistance: a target for multiple myeloma therapy. Expert Rev Hematol. 2009;2:649–62.
Damiano JS, Cress AE, Hazlehurst LA, Shtil AA, Dalton WS. Cell adhesion mediated drug resistance (CAM-DR): role of integrins and resistance to apoptosis in human myeloma cell lines. Blood. 1999;93:1658–67.
Nakagawa Y, Nakayama H, Nagata M, Yoshida R, Kawahara K, Hirosue A, Tanaka T, Yuno A, Matsuoka Y, Kojima T, Yoshitake Y, Hiraki A, Shinohara M. Overexpression of fibronectin confers cell adhesion-mediated drug resistance (CAM-DR) against 5-FU in oral squamous cell carcinoma cells. Int J Oncol. 2014;44:1376–84.
Mraz M, Zent CS, Church AK, Jelinek DF, Wu X, Pospisilova S, Ansell SM, Novak AJ, Kay NE, Witzig TE, Nowakowski GS. Bone marrow stromal cells protect lymphoma B-cells from rituximab-induced apoptosis and targeting integrin alpha-4-beta-1 (VLA-4) with natalizumab can overcome this resistance. Br J Haematol. 2011;155:53–64.
Li ZW, Dalton WS. Tumor microenvironment and drug resistance in hematologic malignancies. Blood Rev. 2006;20:333–42.
Damiano JS, Hazlehurst LA, Dalton WS. Cell adhesion-mediated drug resistance (CAM-DR) protects the K562 chronic myelogenous leukemia cell line from apoptosis induced by BCR/ABL inhibition, cytotoxic drugs, and gamma-irradiation. Leukemia. 2001;15:1232–9.
Mudry RE, Fortney JE, York T, Hall BM, Gibson LF. Stromal cells regulate survival of B-lineage leukemic cells during chemotherapy. Blood. 2000;96:1926–32.
Roodhart JM, He H, Daenen LG, Monvoisin A, Barber CL, van Amersfoort M, Hofmann JJ, Radtke F, Lane TF, Voest EE, Iruela-Arispe ML. Notch1 regulates angio-supportive bone marrow-derived cells in mice: relevance to chemoresistance. Blood. 2013;122:143–53.
Nefedova Y, Sullivan DM, Bolick SC, Dalton WS, Gabrilovich DI. Inhibition of Notch signaling induces apoptosis of myeloma cells and enhances sensitivity to chemotherapy. Blood. 2008;111:2220–9.
Nefedova Y, Cheng P, Alsina M, Dalton WS, Gabrilovich DI. Involvement of Notch-1 signaling in bone marrow stroma-mediated de novo drug resistance of myeloma and other malignant lymphoid cell lines. Blood. 2004;103:3503–10.
Debatin KM. Apoptosis pathways in cancer and cancer therapy. Cancer Immunol Immunother. 2004;53:153–9.
Zimmermann KC, Green DR. How cells die: apoptosis pathways. J Allergy Clin Immunol. 2001;108:S99–103.
Hu W, Kavanagh JJ. Anticancer therapy targeting the apoptotic pathway. Lancet Oncol. 2003;4:721–9.
Cao X, Bennett RL, May WS. c-Myc and caspase-2 are involved in activating Bax during cytotoxic drug-induced apoptosis. J Biol Chem. 2008;283:14490–6.
Corazza N, Kassahn D, Jakob S, Badmann A, Brunner T. TRAIL-induced apoptosis: between tumor therapy and immunopathology. Ann N Y Acad Sci. 2009;1171:50–8.
Ledgerwood EC, Morison IM. Targeting the apoptosome for cancer therapy. Clin Cancer Res. 2009;15:420–4.
Kang MH, Reynolds CP. Bcl-2 inhibitors: targeting mitochondrial apoptotic pathways in cancer therapy. Clin Cancer Res. 2009;15:1126–32.
Papenfuss K, Cordier SM, Walczak H. Death receptors as targets for anti-cancer therapy. J Cell Mol Med. 2008;12:2566–85.
Akiyama T, Dass CR, Choong PF. Bim-targeted cancer therapy: a link between drug action and underlying molecular changes. Mol Cancer Ther. 2009;8:3173–80.
Lessene G, Czabotar PE, Colman PM. BCL-2 family antagonists for cancer therapy. Nat Rev Drug Discov. 2008;7:989–1000.
Wajant H. CD95L/FasL and TRAIL in tumour surveillance and cancer therapy. Cancer Treat Res. 2006;130:141–65.
Bleackley RC. A molecular view of cytotoxic T lymphocyte induced killing. Biochem Cell Biol. 2005;83:747–51.
Sarosiek KA, Chi X, Bachman JA, Sims JJ, Montero J, Patel L, Flanagan A, Andrews DW, Sorger P, Letai A. BID preferentially activates BAK while BIM preferentially activates BAX, affecting chemotherapy response. Mol Cell. 2013;51:751–65.
Westphal D, Kluck RM, Dewson G. Building blocks of the apoptotic pore: how Bax and Bak are activated and oligomerize during apoptosis. Cell Death Differ. 2014;21:196–205.
Luo X, Budihardjo I, Zou H, Slaughter C, Wang X. Bid, a Bcl2 interacting protein, mediates cytochrome c release from mitochondria in response to activation of cell surface death receptors. Cell. 1998;94:481–90.
Rodriguez J, Lazebnik Y. Caspase-9 and APAF-1 form an active holoenzyme. Genes Dev. 1999;13:3179–84.
Slee EA, Harte MT, Kluck RM, Wolf BB, Casiano CA, Newmeyer DD, Wang HG, Reed JC, Nicholson DW, Alnemri ES, Green DR, Martin SJ. Ordering the cytochrome c-initiated caspase cascade: hierarchical activation of caspases-2, -3, -6, -7, -8, and -10 in a caspase-9-dependent manner. J Cell Biol. 1999;144:281–92.
Kale J, Liu Q, Leber B, Andrews DW. Shedding light on apoptosis at subcellular membranes. Cell. 2012;151:1179–84.
Catlett-Falcone R, Landowski TH, Oshiro MM, Turkson J, Levitzki A, Savino R, Ciliberto G, Moscinski L, Fernández-Luna JL, Nuñez G, Dalton WS, Jove R. Constitutive activation of Stat3 signaling confers resistance to apoptosis in human U266 myeloma cells. Immunity. 1999;10:105–15.
Reginato MJ, Mills KR, Paulus JK, Lynch DK, Sgroi DC, Debnath J, Muthuswamy SK, Brugge JS. Integrins and EGFR coordinately regulate the pro-apoptotic protein Bim to prevent anoikis. Nat Cell Biol. 2003;5:733–40.
Hazlehurst LA, Argilagos RF, Dalton WS. Beta1 integrin mediated adhesion increases Bim protein degradation and contributes to drug resistance in leukaemia cells. Br J Haematol. 2007;136:269–75.
de la Fuente MT, Casanova B, Garcia-Gila M, Silva A, Garcia-Pardo A. Fibronectin interaction with alpha4beta1 integrin prevents apoptosis in B cell chronic lymphocytic leukemia: correlation with Bcl-2 and Bax. Leukemia. 1999;13:266–74.
Balakrishnan K, Burger JA, Wierda WG, Gandhi V. AT-101 induces apoptosis in CLL B cells and overcomes stromal cell-mediated Mcl-1 induction and drug resistance. Blood. 2009;113:149–53.
Matsunaga T, Takemoto N, Sato T, Takimoto R, Tanaka I, Fujimi A, Akiyama T, Kuroda H, Kawano Y, Kobune M, Kato J, Hirayama Y, Sakamaki S, Kohda K, Miyake K, Niitsu Y. Interaction between leukemic-cell VLA-4 and stromal fibronectin is a decisive factor for minimal residual disease of acute myelogenous leukemia. Nat Med. 2003;9:1158–65.
Wang L, Fortney JE, Gibson LF. Stromal cell protection of B-lineage acute lymphoblastic leukemic cells during chemotherapy requires active Akt. Leuk Res. 2004;28:733–42.
Paludan C, Bickham K, Nikiforow S, Tsang ML, Goodman K, Hanekom WA, Fonteneau JF, Stevanović S, Münz C. Epstein-Barr nuclear antigen 1-specific CD4(+) Th1 cells kill Burkitt’s lymphoma cells. J Immunol. 2002;169:1593–603.
Silva CL, Lowrie DB. Identification and characterization of murine cytotoxic T cells that kill Mycobacterium tuberculosis. Infect Immun. 2000;68:3269–74.
Wilson AD, Redchenko I, Williams NA, Morgan AJ. CD4+ T cells inhibit growth of Epstein-Barr virus-transformed B cells through CD95–CD95 ligand-mediated apoptosis. Int Immunol. 1998;10:1149–57.
Yi S, Feng X, Wang Y, Kay TW, Wang Y, O’Connell PJ. CD4+ cells play a major role in xenogeneic human anti-pig cytotoxicity through the Fas/Fas ligand lytic pathway. Transplantation. 1999;67:435–43.
Doherty PC, Topham DJ, Tripp RA, Cardin RD, Brooks JW, Stevenson PG. Effector CD4+ and CD8+ T-cell mechanisms in the control of respiratory virus infections. Immunol Rev. 1997;159:105–17.
Komada Y, Zhou YW, Zhang XL, Chen TX, Tanaka S, Azuma E, Sakurai M. Fas/APO-1 (CD95)-mediated cytotoxicity is responsible for the apoptotic cell death of leukaemic cells induced by interleukin-2-activated T cells. Br J Haematol. 1997;96:147–57.
Hahn S, Gehri R, Erb P. Mechanism and biological significance of CD4-mediated cytotoxicity. Immunol Rev. 1995;146:57–79.
Shelton SN, Shawgo ME, Robertson JD. Cleavage of Bid by executioner caspases mediates feed forward amplification of mitochondrial outer membrane permeabilization during genotoxic stress-induced apoptosis in Jurkat cells. J Biol Chem. 2009;284:11247–55.
Perez LE, Parquet N, Shain K, Nimmanapalli R, Alsina M, Anasetti C, Dalton W. Bone marrow stroma confers resistance to Apo2 ligand/TRAIL in multiple myeloma in part by regulating c-FLIP. J Immunol. 2008;180:1545–55.
Shain KH, Landowski TH, Dalton WS. Adhesion-mediated intracellular redistribution of c-Fas-associated death domain-like IL-1-converting enzyme-like inhibitory protein-long confers resistance to CD95-induced apoptosis in hematopoietic cancer cell lines. J Immunol. 2002;168:2544–53.
de Haart SJ, van de Donk NW, Minnema MC, Huang JH, Aarts-Riemens T, Bovenschen N, Yuan H, Groen RW, McMillin DW, Jakubikova J, Lokhorst HM, Martens AC, Mitsiades CS, Mutis T. Accessory cells of the microenvironment protect multiple myeloma from T-cell cytotoxicity through cell adhesion-mediated immune resistance. Clin Cancer Res. 2013;19:5591–601.
Barry M, Bleackley RC. Cytotoxic T lymphocytes: all roads lead to death. Nat Rev Immunol. 2002;2:401–9.
Jazirehi AR, Baritaki S, Koya RC, Bonavida B, Economou JS. Molecular mechanism of MART-1+/A*0201+ human melanoma resistance to specific CTL-killing despite functional tumor-CTL interaction. Cancer Res. 2011;71:1406–17.
Karlsson H, Lindqvist AC, Fransson M, Paul-Wetterberg G, Nilsson B, Essand M, Nilsson K, Frisk P, Jernberg-Wiklund H, Loskog A. CAR T cells and the Bcl-2 family apoptosis inhibitor ABT-737 for treating B-cell malignancy. Cancer Gene Ther. 2013;20:386–93.
Thakur A, Lum LG, Schalk D, Azmi A, Banerjee S, Sarkar FH, Mohommad R. Pan-Bcl-2 inhibitor AT-101 enhances tumor cell killing by EGFR targeted T cells. PLoS One. 2012;7:e47520.
Medema JP, de Jong J, Peltenburg LT, Verdegaal EM, Gorter A, Bres SA, Franken KL, Hahne M, Albar JP, Melief CJ, Offringa R. Blockade of the granzyme B/perforin pathway through overexpression of the serine protease inhibitor PI-9/SPI-6 constitutes a mechanism for immune escape by tumors. Proc Natl Acad Sci U S A. 2001;98:11515–20.
Classen CF, Ushmorov A, Bird P, Debatin KM. The granzyme B inhibitor PI-9 is differentially expressed in all main subtypes of pediatric acute lymphoblastic leukemias. Haematologica. 2004;89:1314–21.
van Houdt IS, Oudejans JJ, van den Eertwegh AJ, Baars A, Vos W, Bladergroen BA, Rimoldi D, Muris JJ, Hooijberg E, Gundy CM, Meijer CJ, Kummer JA. Expression of the apoptosis inhibitor protease inhibitor 9 predicts clinical outcome in vaccinated patients with stage III and IV melanoma. Clin Cancer Res. 2005;11:6400–7.
Kannan-Thulasiraman P, Shapiro DJ. Modulators of inflammation use nuclear factor-kappa B and activator protein-1 sites to induce the caspase-1 and granzyme B inhibitor, proteinase inhibitor 9. J Biol Chem. 2002;277:41230–9.
Holmquist-Mengelbier L, Fredlund E, Löfstedt T, Noguera R, Navarro S, Nilsson H, Pietras A, Vallon-Christersson J, Borg A, Gradin K, Poellinger L, Påhlman S. Recruitment of HIF-1alpha and HIF-2alpha to common target genes is differentially regulated in neuroblastoma: HIF-2alpha promotes an aggressive phenotype. Cancer Cell. 2006;10:413–23.
Sarkar S, Germeraad WT, Rouschop KM, Steeghs EM, van Gelder M, Bos GM, Wieten L. Hypoxia induced impairment of NK cell cytotoxicity against multiple myeloma can be overcome by IL-2 activation of the NK cells. PLoS One. 2013;8:e64835.
Roy N, Deveraux QL, Takahashi R, Salvesen GS, Reed JC. The c-IAP-1 and c-IAP-2 proteins are direct inhibitors of specific caspases. EMBO J. 1997;16:6914–25.
Deveraux QL, Roy N, Stennicke HR, Van Arsdale T, Zhou Q, Srinivasula SM, Alnemri ES, Salvesen GS, Reed JC. IAPs block apoptotic events induced by caspase-8 and cytochrome c by direct inhibition of distinct caspases. EMBO J. 1998;17:2215–23.
Liston P, Roy N, Tamai K, Lefebvre C, Baird S, Cherton-Horvat G, Farahani R, McLean M, Ikeda JE, MacKenzie A, Korneluk RG. Suppression of apoptosis in mammalian cells by NAIP and a related family of IAP genes. Nature. 1996;379:349–53.
Du C, Fang M, Li Y, Li L, Wang X. Smac, a mitochondrial protein that promotes cytochrome c-dependent caspase activation by eliminating IAP inhibition. Cell. 2000;102:33–42.
Verhagen AM, Ekert PG, Pakusch M, Silke J, Connolly LM, Reid GE, Moritz RL, Simpson RJ, Vaux DL. Identification of DIABLO, a mammalian protein that promotes apoptosis by binding to and antagonizing IAP proteins. Cell. 2000;102:43–53.
Hahne JC, Meyer SR, Gambaryan S, Walter U, Dietl J, Engel JB, Honig A. Immune escape of AKT overexpressing ovarian cancer cells. Int J Oncol. 2013;42:1630–5.
Vegran F, Mary R, Gibeaud A, Mirjolet C, Collin B, Oudot A, Charon-Barra C, Arnould L, Lizard-Nacol S, Boidot R. Survivin-3B potentiates immune escape in cancer but also inhibits the toxicity of cancer chemotherapy. Cancer Res. 2013;73:5391–401.
Classen CF, Fulda S, Friesen C, Debatin KM. Decreased sensitivity of drug-resistant cells towards T cell cytotoxicity. Leukemia. 1999;13:410–8.
McMillin DW, Delmore J, Negri JM, Vanneman M, Koyama S, Schlossman RL, Munshi NC, Laubach J, Richardson PG, Dranoff G, Anderson KC, Mitsiades CS. Compartment-specific bioluminescence imaging platform for the high-throughput evaluation of antitumor immune function. Blood. 2012;119:e131–8.
Nakahara T, Kita A, Yamanaka K, Mori M, Amino N, Takeuchi M, Tominaga F, Hatakeyama S, Kinoyama I, Matsuhisa A, Kudoh M, Sasamata M. YM155, a novel small-molecule survivin suppressant, induces regression of established human hormone-refractory prostate tumor xenografts. Cancer Res. 2007;67:8014–21.
Tang H, Shao H, Yu C, Hou J. Mcl-1 downregulation by YM155 contributes to its synergistic anti-tumor activities with ABT-263. Biochem Pharmacol. 2011;82:1066–72.
Datta SR, Dudek H, Tao X, Masters S, Fu H, Gotoh Y, Greenberg ME. Akt phosphorylation of BAD couples survival signals to the cell-intrinsic death machinery. Cell. 1997;91:231–41.
Boni A, Cogdill AP, Dang P, Udayakumar D, Njauw CN, Sloss CM, Ferrone CR, Flaherty KT, Lawrence DP, Fisher DE, Tsao H, Wargo JA. Selective BRAFV600E inhibition enhances T-cell recognition of melanoma without affecting lymphocyte function. Cancer Res. 2010;70:5213–9.
Jazirehi AR, Kurdistani SK, Economou JS. Histone deacetylase inhibitor sensitizes apoptosis-resistant melanomas to cytotoxic human T lymphocytes through regulation of TRAIL/DR5 pathway. J Immunol. 2014;192:3981–9.
Hodge JW, Garnett CT, Farsaci B, Palena C, Tsang KY, Ferrone S, Gameiro SR. Chemotherapy-induced immunogenic modulation of tumor cells enhances killing by cytotoxic T lymphocytes and is distinct from immunogenic cell death. Int J Cancer. 2013;133:624–36.
Li J, Favata M, Kelley JA, Caulder E, Thomas B, Wen X, Sparks RB, Arvanitis A, Rogers JD, Combs AP, Vaddi K, Solomon KA, Scherle PA, Newton R, Fridman JS. INCB16562, a JAK1/2 selective inhibitor, is efficacious against multiple myeloma cells and reverses the protective effects of cytokine and stromal cell support. Neoplasia. 2010;12:28–38.
Straussman R, Morikawa T, Shee K, Barzily-Rokni M, Qian ZR, Du J, Davis A, Mongare MM, Gould J, Frederick DT, Cooper ZA, Chapman PB, Solit DB, Ribas A, Lo RS, Flaherty KT, Ogino S, Wargo JA, Golub TR. Tumour micro-environment elicits innate resistance to RAF inhibitors through HGF secretion. Nature. 2012;487:500–4.
Azab AK, Runnels JM, Pitsillides C, Moreau AS, Azab F, Leleu X, Jia X, Wright R, Ospina B, Carlson AL, Alt C, Burwick N, Roccaro AM, Ngo HT, Farag M, Melhem MR, Sacco A, Munshi NC, Hideshima T, Rollins BJ, Anderson KC, Kung AL, Lin CP, Ghobrial IM. CXCR4 inhibitor AMD3100 disrupts the interaction of multiple myeloma cells with the bone marrow microenvironment and enhances their sensitivity to therapy. Blood. 2009;113:4341–51.
Gogoi D, Dar AA, Chiplunkar SV. Involvement of Notch in activation and effector functions of gammadelta T cells. J Immunol. 2014;192:2054–62.
Sandy AR, Chung J, Toubai T, Shan GT, Tran IT, Friedman A, Blackwell TS, Reddy P, King PD, Maillard I. T cell-specific notch inhibition blocks graft-versus-host disease by inducing a hyporesponsive program in alloreactive CD4+ and CD8+ T cells. J Immunol. 2013;190:5818–28.
Zhang Y, Sandy AR, Wang J, Radojcic V, Shan GT, Tran IT, Friedman A, Kato K, He S, Cui S, Hexner E, Frank DM, Emerson SG, Pear WS, Maillard I. Notch signaling is a critical regulator of allogeneic CD4+ T-cell responses mediating graft-versus-host disease. Blood. 2011;117:299–308.
Acknowledgments
We thank Prof. Dr. H. Lokhorst and Dr. A. Martens from VUmc Amsterdam, the Netherlands and for Dr. C. Mitsiades from Dana Farber Cancer Institute, Boston US for significant conceptual contributions, inputs with experimental models, critical reading, and stimulating discussions.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Mutis, T., van de Donk, N.W.C.J., Groen, R.W.J. (2015). Mechanisms and Modulation of Tumor Microenvironment-Induced Immune Resistance. In: Bonavida, B., Chouaib, S. (eds) Resistance of Cancer Cells to CTL-Mediated Immunotherapy. Resistance to Targeted Anti-Cancer Therapeutics, vol 7. Springer, Cham. https://doi.org/10.1007/978-3-319-17807-3_7
Download citation
DOI: https://doi.org/10.1007/978-3-319-17807-3_7
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-17806-6
Online ISBN: 978-3-319-17807-3
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)