Abstract
LGI1 is a multifunctional brain protein whose dysfunction is related to several neurologic disorders as diverse as autosomal dominant lateral temporal epilepsy (ADLTE), autoimmune limbic encephalitis (LE), and glioma tumor progression. ADLTE is a genetic focal epilepsy characterized by auditory or aphasic aura and onset in infancy/adolescence, whereas autoimmune LE occurs in adult life and is characterized by amnesia, confusion, and seizures. The complex molecular mechanisms underlying these epileptic conditions are largely unknown. In this chapter, I outline the clinical features, the genetic or autoimmune causes, and a molecular mechanism possibly underlying both ADLTE and autoimmune LE.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
The leucine-rich, glioma inactivated 1 (LGI1) gene has been associated with clinical phenotypes as different as malignant glioma, autosomal dominant lateral temporal epilepsy (ADLTE) , a rare genetic focal epilepsy syndrome, and autoimmune limbic encephalitis (LE) , an acquired immunological disorder of the brain. Although very different in nature, these brain disorders result from a reduction of the physiological level of the Lgi1 protein.
In 1998, LGI1 was cloned due to its rearrangements in the T98G glioblastoma multiforme (GBM) cell line and was found to be downregulated in many malignant gliomas, suggesting a possible tumor suppressor function (Chernova et al. 1998). Subsequent studies failed to reveal point mutations in the LGI1 coding sequence and differential methylation of its core promoter region in GBM tumors, arguing against a role of LGI1 as a tumor suppressor gene (Somerville et al. 2000; Piepoli et al. 2006). However, LGI1 has been shown to control proliferation and invasiveness of glioma cell lines by regulating expression of the matrix metalloproteinases MMP1 and MMP3, suggesting that LGI1 may serve as a tumor metastasis suppressor gene (Kunapuli et al. 2003; 2004). In 2002, LGI1 heterozygous mutations were shown to cause ADLTE in several American and European families (Kalachikov et al. 2002; Morante-Redolat et al. 2002). Subsequent studies showed that LGI1 mutations account for about 50 % of ADLTE families (Michelucci et al 2003; Ottman et al. 2004). ADLTE is clinically characterized by auras with auditory features and is also named autosomal dominant partial epilepsy with auditory features (ADPEAF) . Finally, in 2010, LGI1 was implicated in acquired autoimmune limbic encephalitis, a neurological disorder of adulthood (Irani et al. 2010; Lai et al. 2010). Patients with autoantibodies directed against the Lgi1 protein suffer from psychiatric symptoms, including memory loss and confusion, as well as epilepsy.
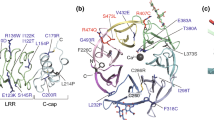
The LGI1 gene consists of eight exons with a coding region of 1671 bp. It is expressed mainly in neurons, particularly in the neocortex and limbic regions (Kalachikov et al. 2002; Senechal et al. 2005) and encodes a protein of 557 amino acids with no similarities to ion channels. The Lgi1 protein is secreted (Senechal et al. 2005), and its structure consists of an N-terminal signal peptide and two distinct structural domains: the N-terminal region contains four leucine-rich repeats (LRR) flanked by conserved cysteine clusters (Kobe and Kajava 2001), whereas the C-terminal region consists of seven copies of a repeat named EPTP (Staub et al. 2002), which form a beta-propeller structural domain (Paoli 2001). Both LRR and beta-propeller motifs mediate protein-protein interactions (Kobe and Kajava 2001; Paoli 2001).
In this chapter I describe the clinical features of ADLTE and LE, the role of LGI1 as a cause of these syndromes, and outline the current views about the possible functions of LGI1 .
ADLTE
Clinical Features
ADLTE is a rare familial condition characterized by focal seizures with prominent ictal auditory symptoms, negative MRI findings, and relatively benign evolution (Ottman et al. 1995; Michelucci et al. 2009). Its prevalence is unknown but it may account for about 19 % of genetic focal epilepsies (Ottman et al. 2004). Since the first description of the syndrome (Ottman et al. 1995), 39 families, most of which with unique LGI1 mutations have been reported. The syndrome segregates with an autosomal dominant inheritance pattern with reduced penetrance. Familial diagnosis is based on the existence of at least two cases with unprovoked focal or secondarily generalized seizures whose symptoms suggest a lateral temporal lobe onset.
The age of onset ranges between 1 and 60 years with a mean of 18 years. The ictal semiology includes focal seizures and secondarily generalized tonic-clonic seizures. Focal seizures are characterized by auditory auras in about 2/3 of the cases. In most cases, auditory symptoms are described as simple sounds (such as humming, buzzing, ringing); complex hallucinations (i.e. music, voices) are less frequent, and, sometimes, the aura is characterized by a distortion of sounds (becoming louder and louder or suddenly low). Aphasic seizures associated with auditory phenomena are reported, but may also be the only clinical symptom in some pedigrees (see Michelucci et al. 2003). Other less frequent auras include complex visual, psychic, autonomic, vertiginous, and other sensory symptoms, usually accompanying auditory phenomena.
Secondary tonic-clonic seizures are common, occurring in 90 % of cases, both during wakefulness and sleep, and may unmask an otherwise undiagnosed history of elementary focal seizures with auditory symptoms. Interictal EEGs show temporal abnormalities (described as mild slow/sharp waves) in about half of the patients, with a clear left predominance of the abnormalities in some families (Brodtkorb et al. 2005; Pisano et al. 2005). Standard MRI shows no abnormalities, but a study of 8 ADLTE patients with LGI1 mutations performed by voxel-based MRI and diffusion tensor imaging demonstrated a cluster of fractional anisotropy in the left lateral temporal cortex, suggesting a malformative origin of the abnormality (Tessa et al. 2007).
Genetic studies have revealed mutations of LGI1 in about 30–50 % of the families, providing evidence for genetic heterogeneity (Michelucci et al. 2003; 2013). Detailed analysis of families with and without LGI1 mutations showed no phenotypic differences between the pedigrees.
Sporadic, non-familial cases with auditory seizures have been reported (Bisulli et al. 2004a). Despite their negative family history, they had a clinical picture indistinguishable from that of ADLTE patients, characterized by focal seizures with auditory auras, a mean age of onset of 19 years, a high rate of secondary generalized tonic-clonic seizures, low seizure frequency, good response to antiepileptic treatment, unrevealing EEGs and normal MRIs. De novo LGI1 mutations have been found in two sporadic LTE cases (see below).
LGI1 Pathogenic Mutations
To date, a total of 37 LGI1 mutations have been described, either segregating in ADLTE families or occurring de novo in sporadic LTE patients (Fig. 1 and Table 1; nucleotide numbering uses the A of the ATG translation initiation start site as nucleotide + 1). Thirty-six mutations segregate in 39 affected families, whereas two, c.406C > T and c.1420C > T, are de novo mutations identified in non-familial cases, the latter occurring in both a family and a sporadic case (Morante-Redolat et al. 2002; Bisulli et al. 2004b). Of these mutations, 23 allow single amino acid substitutions, 13 result in protein truncation due to frameshift deletions or insertion, and to non-sense or splice site mutations, whereas one in frame deletion mutation (c. 377–379delACA) results in the deletion of an asparagine in the encoded protein. In addition, an internal deletion of exons 3–4, resulting from altered splicing (c.431 + 1G > A), and a genomic microdeletion spanning the first 4 LGI1 exons have been identified (Table 1). Thus, the majority of the mutations as yet identified are missense nucleotide changes. The mutation distribution along the gene is somewhat uniform, though a higher density of mutations appears to occur in exons 3–5, which correspond to the N-terminal LRR repeat 2–4 (Ho et al. 2012; see Fig. 1). The overall penetrance estimate of LGI1 mutations was 66 % (Rosanoff and Ottman 2008) and the proportion of families with penetrance > = 75 % was similar among those with missense vs truncation mutations (Ho et al. 2012).
The Lgi1 protein is expressed mainly in neurons and is secreted into the extracellular compartment (Senechal et al. 2005; Fukata et al. 2010). All but one LGI1 mutations reported so far inhibit protein secretion (Nobile et al. 2009), suggesting a loss-of-function effect of mutations. Only one missense mutation (R407C) has been shown to allow protein secretion (Striano et al. 2011), and its effect in the extracellular comparment of the brain is unclear. A three-dimensional protein model predicts that this mutation may perturb extracellular interactions of Lgi1 with other proteins, and that this effect may not be limited to this mutation (Leonardi et al. 2011).
Lgi1 Protein Function
The function of LGI1 and the mechanisms of LGI1-related epilepsy remain unclear. Three main functions have been proposed for LGI1 in the CNS: (1) inhibition of inactivation of the presynaptic voltage-gated potassium channel Kv1.1 (Schulte et al. 2006); (2) potentiation ofAMPA receptor-mediated synaptic transmission in the hippocampus through interaction with the transmembrane receptors ADAM22 and ADAM23 (Fukata et al. 2006; 2010; Ohkawa et al. 2013); (3) postnatal maturation of glutamatergic synapses, regulation of spine density, and dendritic pruning (Zhou et al. 2009). Remarkably, Lgi1- knockout mice (Fukata et al. 2010; Chabrol et al. 2010; Yu et al. 2010) display spontaneous seizures. Homozygous Lgi1 knockout (KO) mice have spontaneous seizures with onset at postnatal day 10 and all pups die before the end of the third postnatal week, while heterozygous Lgi1+/− mice exhibit increased susceptibility to sound-induced or pentylenetetrazole-induced seizures (Chabrol et al. 2010; Fukata et al. 2010). The “intermediate” phenotype of heterozygous +/− mice supports the loss-of-function model, whereas the phenotypic features of mice overexpressing a truncated protein in the presence of normal endogenous Lgi1 suggest that some mutations may have a dominant negative effect (Zhou et al. 2009).
Acquired Immune-Mediated Disorders
LE
The pivotal role of LGI1 in epileptic disorders has been expanded with the recent finding of autoantibodies against Lgi1 in patients with autoimmune LE, a neurological disorder of adulthood characterized by amnesia, confusion, seizures, which mostly involve the temporal lobes, and personality change or psychosis (Irani et al. 2010; Lai et al. 2010). Autoimmune LE belongs to the group of autoimmune synaptic encephalopathies, in which patients develop antibodies against synaptic proteins, including the excitatory N-Methyl-D-aspartate (NMDA) and alpha-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid (AMPA) receptors and voltage-gated potassium channel (VGKC)-complexes (Kv1). Because of the crucial role of these receptors in synaptic transmission and plasticity, the autoimmunity usually causes seizures and neuropsychiatric symptoms, ranging from alterations in memory, behaviour, and cognition, to psychosis. The resulting disorders are severe but treatable, and some of them can be individually classified on the basis of a particular immune response (for example, anti-NMDA receptor encephalitis (Dalmau et al. 2008; Gable et al. 2009); or anti-VGKC LE (Vincent et al. 2004; Tan et al. 2008). The VGKC complex antibodies have traditionally been measured by immunoprecipitation of VGKC Kv1 subunits solubilized in detergent from rabbit brain tissue and radioactively labeled by 125I-dendrotoxin, a snake toxin that binds very strongly to Kv1. Recently, a series of experiments has shown that the antibodies do not bind directly to Kv1 subunits but rather to other molecules that are complexed with the Kv1 in brain extracts. The most frequently associated molecules identified so far are Lgi1 and Contactin-associated protein 2 (CASPR2), with the great majority of the LE patients having antibodies to Lgi1 (Lai et al 2010). Commonly, these antibodies are detected using an immunofluorescence cell-based method which detects the binding of patients’ sera to the surface of cells transfected with cDNA encoding the protein.
LE patients with autoantibodies directed against Lgi1 protein suffer from psychiatric symptoms and epilepsy. Clinical seizures, generalized or involving the temporal lobes, occur in about 80 % of LE patients, whereas 40 % have myoclonus; 60 % of patients have hyponatraemia On MRI, increased T2 signal involving one or both medial temporal lobes are frequently observed (Lai et al. 2010). Lgi1-positive LE usually is not associated with tumors. Immunotherapy, consisting of intravenous immunoglobulin, glucocorticoids, plasma exchange, or a combination thereof, results in full recovery or mild residual memory impairment in most cases. Relapses only occur in a minority of cases.
In a proportion of patients, autoimmune LE is associated with faciobrachial dystonic seizures (FBDS), which is characterized by typical episodes of facial grimacing and ipsilateral arm dystonia (Irani et al. 2008; 2013). Seizures occur at high frequency (up to 360 episodes per day). The onset is variable (22–83 years) and is sometimes triggered by auditory stimuli or high emotion. EEG abnormalities, i.e. rhythmic frontotemporal spikes, are detectable in about one-fourth of FBDS cases. This syndrome has been found consistently associated with antibodies against Lgi1 (Irani et al. 2008; 2011; Vincent et al. 2011). Response to anti-epileptic drugs is poor whereas immunotherapy yields excellent results. Most FBDS patients subsequently develop the full LE phenotype, whereas in a minority of cases FBDS occur in isolation or follows LE. Early immunotherapy for faciobrachial dystonic seizures may postpone or even prevent progression to the cognitive impairment that characterizes LE (Irani et al. 2011).
Neuromyotonia and Morvan Syndrome
Lgi1 autoantibodies are also found in acquired immune-mediated peripheral nerve disorders neuromyotonia and Morvan syndrome, though often associated with other antibodies. Acquired neuromyotonia is characterized by the presence of spontaneous activity including positive sharp-waves and fibrillation potentials, fasciculations, myokymia, multiple discharges, muscle cramps and repetitive after-discharges in response to a voluntary contraction (Warmolts and Mendell 1980; Hart et al. 1997). Acquired neuromyotonia may be clinically misdiagnosed as amyotrophic lateral sclerosis (ALS), particularly in the early stages of ALS where widespread fasciculations may be evident in the absence of other clinical features of ALS.
Morvan’s syndrome has been recognized as a rare constellation of peripheral nerve neuromyotonia combined with sensory abnormalities and central nervous system (CNS) features, such as dysautonomia and encephalopathy with marked insomnia (Hart et al. 2002). Some of the patients had a thymoma, but many do not have a tumor. In patients with neuromyotonia or Morvan syndrome CASPR2 antibodies are mainly detected, whereas Lgi1 antibodies are much less frequent and, when occur, are frequently associated with CASPR2 antibodies (Irani et al. 2012).
Whether Lgi1 autoantibodies are pathogenic or represent an epiphenomenon is still uncertain. However, immunotherapies can lead to a marked improvement of these syndromes paralleling with antibody titer decrease, suggesting a possible direct role of antibodies on neuronal function.
LGI1 Functional Models
Despite definitive genetic evidence, the pathophysiological function of LGI1 in the brain remains controversial. Several studies have shown that the secreted Lgi1 protein binds to ADAM22 and ADAM23 receptors on the surface of neuronal cells and that these protein complexes exert various functions during neuronal maturation and synaptic transmission (Fukata et al. 2006; 2010; Owuor et al. 2009). The involvement of both ADAM22 and ADAM23 in epilepsy is suggested by studies of knock-out mice, showing that lack of expression of either of these genes results in spontaneous seizures (Owuor et al. 2009; Sagane et al. 2005). It has been shown that the ligand-receptor complexes between Lgi1 and ADAM22/ADAM23 regulates AMPA receptor-mediated synaptic transmission in the hippocampus, suggesting a possible molecular mechanism underlying ADLTE (Fukata 2006; 2010). This mechanism is further supported by recent findings showing that Lgi1 antibodies associated with LE neutralize the specific protein-protein interaction between LGI1 and ADAM22/ADAM23, and that disruption of this complex is sufficient to reduce AMPA receptors in rat hippocampal neurons (Ohkawa 2013). Thus, a unifying view is emerging, suggesting that reduced binding of Lgi1 to ADAM22/23 may be a pathogenic mechanism for both genetically inherited ADLTE and acquired LE, providing further support to the central role of LGI1 in mechanisms for regulating brain function and excitability.
References
Berghuis B, Brilstra EH, Lindhout D et al (2013) Hyperactive behavior in a family with autosomal dominant lateral temporal lobe epilepsy caused by a mutation in the LGI1/epitempin gene. Epilepsy Behav 28:41–46
Berkovic SF, Izzillo P, McMahon JM et al (2004) LGI1 mutations in temporal lobe epilepsies. Neurology 62:1115–1119
Bisulli F, Tinuper P, Avoni P et al (2004a) Idiopathic partial epilepsy with auditory features (IPEAF): a clinical and genetic study of 53 sporadic cases. Brain 127:1343–1352
Bisulli F, Tinuper P, Scudellaro E et al (2004b) A de novo LGI1 mutation in sporadic partial epilepsy with auditory features. Ann Neurol 56:455–456
Brodtkorb E, Michler RP, Gu W et al (2005) Speech-induced aphasic seizures in epilepsy caused by LGI1 mutation. Epilepsia 46:963–966
Chabrol E, Popescu C, Gourfinkel-An I et al (2007) Two novel epilepsy-linked mutations leading to a loss of function of LGI1. Arch Neurol 64:217–222
Chabrol E, Navarro V, Provenzano G et al (2010) Electroclinical characterization of epileptic seizures in leucine-rich, glioma-inactivated 1- deficient mice. Brain 133:2749–2762
Chernova OB, Somerville RP, Cowell JK (1998) A novel gene, LGI1, from 10q24 is rearranged and downregulated in malignant brain tumors. Oncogene 17:2873–2881
Dalmau J, Gleichman AJ, Hughes EG et al (2008) Anti-NMDA-receptor encephalitis: case series and analysis of the effects of antibodies. Lancet Neurol 7:1091–1098
de Bellescize J, Boutry N, Chabrol E et al (2009) A novel three base-pair LGI1 deletion leading to loss of function in a family with autosomal dominant lateral temporal epilepsy and migraine-like episodes. Epilepsy Res 85:118–122
Di Bonaventura C, Carni M, Diani E et al (2009) Drug resistant ADLTE and recurrent partial status epilepticus with dysphasic features in a family with a novel LGI1 mutation: electroclinical, genetic, and EEG/fMRI findings. Epilepsia 50:2481–2486
Di Bonaventura C, Operto FF, Busolin G et al (2011) Low penetrance and effect on protein secretion of LGI1 mutations causing autosomal dominant lateral temporal epilepsy. Epilepsia 52:1258–1264
Fertig E, Lincoln A, Martinuzzi A et al (2003) Novel LGI1 mutation in a family with autosomal dominant partial epilepsy with auditory features. Neurology 60:1687–1690
Fanciulli M, Santulli L, Errichiello L et al (2012) LGI1 microdeletion in autosomal dominant lateral temporal epilepsy. Neurology 78:1299–1303
Fukata Y, Adesnik H, Iwanaga T et al (2006) Epilepsy-related ligand/receptor complex LGI1 and ADAM22 regulate synaptic transmission. Science 313:1792–1795
Fukata Y, Lovero KL, Iwanaga T et al (2010) Disruption of LGI1-linked synaptic complex causes abnormal synaptic transmission and epilepsy. Proc Natl Acad Sci U S A 107:3799–3804
Gable MS, Gavali S, Radner A et al (2009) Anti-NMDA receptor encephalitis: report of ten cases and comparison with viral encephalitis. Eur J Clin Microbiol Infect Dis 28:1421–1429
Gu W, Brodtkorb E, Steinlein OK (2002) LGI1 is mutated in familial temporal lobe epilepsy characterized by aphasic seizures. Ann Neurol 52:364–367
Hart IK, Waters C, Vincent A et al (1997) Autoantibodies detected to expressed Kþ channels are implicated in neuromyotonia. Ann Neurol 41:238–246
Hart IK, Maddison P, Newsom-Davis J et al (2002) Phenotypic variants of autoimmune peripheral nerve hyperexcitability. Brain 125:1887–1895
Hedera P, Abou-Khalil B, Crunk AE et al (2004) Autosomal dominant lateral temporal epilepsy: two families with novel mutations in the LGI1 gene. Epilepsia 45:218–222
Heiman GA, Kamberakis K, Gill R et al (2010) Evaluation of depression risk in LGI1 mutation carriers. Epilepsia 51:1685–1690
Ho YY, Ionita-Laza I, Ottman R (2012) Domain-dependent clustering and genotype-phenotype analysis of LGI1 mutations in ADPEAF. Neurology 78:563–568
Irani SR, Buckley C, Vincent A et al (2008) Immunotherapy-responsive seizure-like episodes with potassium channel antibodies. Neurology 71:1647–1648
Irani SR, Alexander S, Waters P et al (2010) Antibodies to Kv1 potassium channel-complex proteins leucine-rich, glioma inactivated 1 protein and contactin-associated protein-2 in limbic encephalitis, Morvan’s syndrome and acquired neuromyotonia. Brain 133:2734–2748
Irani SR, Michell AW, Lang B et al (2011) Faciobrachial dystonic seizures precede Lgi1 antibody limbic encephalitis. Ann Neurol 69:892–900
Irani SR, Pettingill P, Kleopa KA et al (2012) Morvan syndrome: Clinical and serological observations in 29 cases. Ann Neurol 72:241–255
Irani SR, Charlotte JS, Schott JM et al (2013) Faciobrachial dystonic seizures: the influence of immunotherapy on seizure control and prevention of cognitive impairment in a broadening phenotype. Brain 136:3151–3162
Kalachikov S, Evgrafov O, Ross B et al (2002) Mutations in LGI1 cause autosomal-dominant partial epilepsy with auditory features. Nat Genet 30:335–341
Kawamata J, Ikeda A, Fujita Y et al (2010) Mutations in LGI1 gene in Japanese families with autosomal dominant lateral temporal lobe epilepsy: the first report from Asian families. Epilepsia 51:690–693
Kobe B, Kajava AV (2001) The leucine-rich repeat as a protein recognition motif. Curr Opin Struct Biol 11:725–732
Kunapuli P, Chitta KS, Cowell JK (2003) Suppression of the cell proliferation and invasion phenotypes in glioma cells by the LGI1 gene. Oncogene 22:3985–3991
Kunapuli P, Kasyapa CS, Hawthorn L et al (2004) LGI1, a putative tumor metastasis suppressor gene, controls in vitro invasiveness and expression of matrix metalloproteinases in glioma cells through the ERK1/2 pathway. J Biol Chem 279:23151–23157
Leonardi E, Andreazza S, Vanin S et al (2011) A computational model of the LGI1 protein suggests a common binding site for ADAM proteins. Plos One 6:e18142
Lai M, Huijbers MGM, Lancaster E et al (2010) Investigation of LGI1 as the antigen in limbic encephalitis previously attributed to potassium channels: a case series. Lancet Neurol 9:776–785
Lee MK, Kim SW, Lee JH et al (2014) A Newly discovery of LGI1 mutation in a Korean family with autosomal dominant lateral temporal lobe epilepsy. Seizure 23:69–73
Michelucci R, Poza JJ, Sofia V et al (2003) Autosomal dominant lateral temporal epilepsy: clinical spectrum, new epitempin mutations, and genetic heterogeneity in seven European families. Epilepsia 44:1289–1297
Michelucci R, Mecarelli O, Bovo G et al (2007) A de novo LGI1 mutation causing idiopathic partial epilepsy with telephone-induced seizures. Neurology 68:2150–2151
Michelucci R, Pasini E, Nobile C (2009) Lateral temporal lobe epilepsies: clinical and genetic features. Epilepsia 50(Suppl 5):52–54
Michelucci R, Pasini E, Malacrida S et al (2013) Low penetrance of autosomal dominant lateral temporal epilepsy in Italian families without LGI1 mutations. Epilepsia 54:1288–1297
Morante-Redolat JM, Gorostidi-Pagola A, Piquer-Sirerol S et al (2002) Mutations in the LGI1/Epitempin gene on 10q24 cause autosomal dominant lateral temporal epilepsy. Hum Mol Genet 11:1119–1128
Nobile C, Michelucci R, Andreazza S et al (2009) LGI1 mutations in autosomal dominant and sporadic lateral temporal epilepsy. Hum Mutat 30:530–536
Ohkawa T, Fukata Y, Yamasaki M et al (2013) Autoantibodies to Epilepsy-Related LGI1 in Limbic Encephalitis Neutralize LGI1-ADAM22 Interaction and Reduce Synaptic AMPA Receptors. J Neurosci 33:18161–18174
Owuor K, Harel NY, Englot DJ et al (2009) LGI1-associated epilepsy through altered ADAM23-dependent neuronal morphology. Mol Cell Neurosci 42:448–457
Ottman R, Risch N, Hauser WA et al (1995) Localization of a gene for partial epilepsy to chromosome 10q. Nat Genet 10:56–60
Ottman R, Winawer MR, Kalachikov S et al (2004) LGI1 mutations in autosomal dominant partial epilepsy with auditory features. Neurology 62:1120–1126
Paoli M (2001) Protein folds propelled by diversity. Prog Biophys Molec Biol 76:103–130
Piepoli T, Jakupoglu C, Gu W et al (2006) Expression studies in gliomas and glial cells do not support a tumor suppressor role for LGI1. Neuro Oncol 8:96–108
Pisano T, Marini C, Brovedani P et al (2005) Abnormal phonologic processing in familial lateral temporal lobe epilepsy due to a new LGI1 mutation. Epilepsia 46:118–123
Pizzuti A, Flex E, Di Bonaventura C et al (2003) Epilepsy with auditory features: a LGI1 gene mutation suggests a loss-of-function mechanism. Ann Neurol 53:396–399. Erratum in. Ann Neurol 2003;54:137
Rosanoff MJ, Ottman R (2008) Penetrance of LGI1 mutations in autosomal dominant partial epilepsy with auditory features. Neurology 71:567–571
Sadleir LG, Agher D, Chabrol E et al (2013) Seizure semiology in autosomal dominant epilepsy with auditory features, due to novel LGI1 mutations. Epilepsy Res 107:311–317
Sagane K, Hayakawa K, Kaj J et al (2005) Ataxia and peripheral nerve hypomyelination in ADAM22-deficient mice. BMC Neurosci 6:33
Schulte U, Thumfart JO, Klocker N et al (2006) The epilepsy-linked Lgi1 protein assembles into presynaptic kv1 channels and inhibits inactivation by Kvbeta1. Neuron 49:697–706
Senechal KR, Thaller C, Noebels JL (2005) ADPEAF mutations reduce levels of secreted LGI1, a putative tumor suppressor protein linked to epilepsy. Hum Mol Genet 14:1613–1620
Somerville RP, Chernova O, Liu S et al (2000) Identification of the promoter, genomic structure, and mouse ortholog of LGI1. Mamm Genome 11:622–627
Staub E, Perez-Tur J, Siebert R et al (2002) The novel EPTP repeat defines a superfamily of proteins implicated in epileptic disorders. Trends Biochem Sci 27:441–444
Striano P, de Falco A, Diani E et al (2008) A novel loss-of-function LGI1 mutation linked to autosomal dominant lateral temporal epilepsy. Arch Neurol 65:939–942
Striano P, Busolin G, Santulli L et al (2011) Familial temporal lobe epilepsy with psychic auras associated with a novel LGI1 mutation. Neurology 76:1173–1176
Tan KM, Lennon VA, Klein CJ et al (2008) Clinical spectrum of voltage-gated potassium channel autoimmunity. Neurology 70:1883–1890
Tessa C, Michelucci R, Nobile C et al (2007) Structural anomaly of left lateral temporal lobe in epilepsy due to mutated LGI1. Neurology 69:1298–1300
Vincent A, Buckley C, Schott JM et al (2004) Potassium channel antibodyassociated encephalopathy: a potentially immunotherapy-responsive form of limbic encephalitis. Brain 127:701–712
Vincent A, Bien CG, Irani SR et al (2011) Autoantibodies associated with diseases of the CNS: new developments and future challenges. Lancet Neurol 10:759–772
Warmolts JR, Mendell JR (1980) Neurotonia: impulse-induced repetitive discharges in motor nerves in peripheral neuropathy. Ann Neurol 7:245–250
Yu YE, Wen L, Silva J et al (2010) Lgi1 null mutant mice exhibit myoclonic seizures and CA1 neuronal hyperexcitability. Hum Mol Genet 19:1702–1711
Zhou YD, Lee S, Jin Z et al (2009) Arrested maturation of excitatory synapses in autosomal dominant lateral temporal lobe epilepsy. Nat Med 15:1208–1214
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2015 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Nobile, C. (2015). LGI1 Dysfunction in Inherited and Acquired Epileptic Disorders. In: Striano, P. (eds) Epilepsy Towards the Next Decade. Contemporary Clinical Neuroscience. Springer, Cham. https://doi.org/10.1007/978-3-319-12283-0_3
Download citation
DOI: https://doi.org/10.1007/978-3-319-12283-0_3
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-12282-3
Online ISBN: 978-3-319-12283-0
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)