Abstract
Definition: An invasive, permeative, and progressive tumor uniformly composed of fibroblasts and abundant collagen.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Definition: An invasive, permeative, and progressive tumor uniformly composed of fibroblasts and abundant collagen.
Epidemiology: Children and young males. Peak incidence 25–35 years.
Localization: Proximal part of the limbs (shoulder and buttock), then trunk, thigh, popliteal fossa, sura, arm, and forearm. Usually in the deep soft tissues. Skin invasion when the tumor expands to the superficial fascia.

Clinical: Deep, painless, firm or hard, and poorly circumscribed mass that may be adherent to the skin or bone and that grows insidiously and slowly for several months. Tumor mass is elongated along the muscle, or it is made up of large masses disseminated along the limb and joined together. The tumor grows by infiltrative ramifications along the muscle, the aponeuroses, and the tendons. When large, muscular retraction phenomena and limited joint motion occur. Pain, numbness, hypoesthesia, and motor weakness when it infiltrates a large nerve.
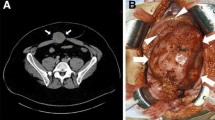
Imaging: On X-ray a dense mass interrupts the adjacent intermuscular and soft tissue planes. Adherent to bone (37 %) with saucerized cortex without periosteal reaction. On angiography a thick intratumoral capillary network, with few vessels of large caliber. On CT intensely and diffusely takes up contrast medium, easily distinguished from surrounding muscles, irregular shape of the tumor, many nodules joined together, and faded boundaries and digitations along the fascial and interstitial planes. On MRI infiltrative pattern (63 %) in youngsters and nodular pattern (81 %) in adults; hypo-/isointense to muscle on T1 and intermediate on T2; inhomogeneous (75 %), bright in the center (cellular area) and dark in the periphery (collagen area) on T2; on T2 white zones enhance after gadolinium administration, whereas dark zones remain hypointense; bright mass on T2 are aggressive lesions; natural evolution shows proximal migration; and gradual decrease of enhancing cellular areas and increasing of nonenhancing collagen zones.
Histopathology: Dense, white, firm lesion that may be of large size (up to 20 cm). Ill-defined margins, digitations, and satellite nodules near the tumoral limits. Firmly adherent to the aponeuroses, tendons, joint capsule, vessels, and nerves. These are compressed but not invaded. Rarely, compression on the bone causes a superficial scalloping of the cortex. A densely collagenized mature fibrous connective tissue with a relatively sparse number of fibroblasts. Mitoses are rare or absent. Variably prominent ectatic blood vessels. Spindle cells in intertwined bundles that are wavy and have no particular order. Infiltration of the muscle and the surrounding tissues. On immunohistochemistry, desmoid tumor is diffusely positive for vimentin and shows nuclear expression of beta-catenin in 85 % of cases. It may be positive for pan-muscle actin and smooth muscle actin.
Course and Staging: Locally aggressive tumor not associated with metastases. Stage 3. An involution to stage 2 or even stage 1 lesion is possible. Local recurrence is frequent even if removed with adequate margins. Malignant transformation has never been observed.
Treatment: Wide or better radical excision. When adequate excision is not possible, radiotherapy may give favorable results if it is used in addition to surgery. When the tumor compresses and surrounds main vessels of the limb, recurs several times, and pushes toward the pelvis and the axilla, wide amputation is necessary. Prognosis quoad vitam is good, but 2 % of patients die from vascular and/or interference from vital internal organs if the tumor enters the neck, chest, and abdomen. Low-dose, long-term chemotherapy with methotrexate shows good results and is used for recurrent disease or tumors that are difficult to excise.
FormalPara Immunohistochemical PanelVIM | + |
MS Act | ± |
Smooth M Act | ± |
Beta-catenin | + (nuclear staining, 70–75 %) |

Heavily collagenized tissue with low cellularity, spindle cells with bland appearance, intersected fascicles, and ectatic vascular clefts
Selected Bibliography
Desmoid Lazar AJ, Hajibashi S, Lev D (2009) Tumor: from surgical extirpation to molecular dissection. Curr Opin Oncol 21(4):352–359. Review
Guglielmi G, Cifaratti A, Scalzo G, Magarelli N (2009) Imaging of superficial and deep fibromatosis. Radiol Med 114(8):1292–1307. Review
Lee JC, Thomas JM, Phillips S, Fisher C, Moskovic E (2006) Aggressive fibromatosis: MRI features with pathologic correlation. AJR Am J Roentgenol 186(1):247–254
McCarville MB, Hoffer FA, Adelman CS, Khoury JD, Li C, Skapek SX (2007) MRI and biologic behavior of desmoid tumors in children. AJR Am J Roentgenol 189(3):633–640
Murphey MD, Ruble CM, Tyszko SM, Zbojniewicz AM, Potter BK, Miettinen M (2009) From the archives of the AFIP: musculoskeletal fibromatoses: radiologic-pathologic correlation. Radiographics 29(7):2143–2173
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Fabbri, N. (2014). Extra-abdominal Fibromatosis. In: Picci, P., Manfrini, M., Fabbri, N., Gambarotti, M., Vanel, D. (eds) Atlas of Musculoskeletal Tumors and Tumorlike Lesions. Springer, Cham. https://doi.org/10.1007/978-3-319-01748-8_61
Download citation
DOI: https://doi.org/10.1007/978-3-319-01748-8_61
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-01747-1
Online ISBN: 978-3-319-01748-8
eBook Packages: MedicineMedicine (R0)