Abstract
The pulmonary artery catheter (PAC) has lost its popularity during the last years giving way to supposedly less invasive hemodynamic monitoring devices such as transpulmonary thermodilution techniques, pulse contour analysis, and echocardiography. Nevertheless, it is still the gold standard for cardiac output measurements via pulmonary artery thermodilution (PATD). Furthermore, a PAC is the only device offering the possibility to assess and monitor pulmonary artery pressure and right ventricular function continuously. PATD is valuable in situations where a comprehensive view of the hemodynamic situation is needed.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Pulmonary artery catheter
- Thermodilution
- Pulmonary artery thermodilution
- Hemodynamic monitoring
- Cardiac output monitoring
1 Pulmonary Artery Catheter and Pulmonary Artery Thermodilution
A pulmonary artery catheter (PAC), also known as Swan-Ganz catheter, named after the American cardiologists Swan and Ganz, who introduced it into clinical practice in 1970 [1], provides the clinician with right-sided pressures and related parameters as well as mixed venous saturation. It is a useful monitoring device in situations, in which the knowledge of cardiac output (CO), pulmonary artery pressure (PAP), pulmonary artery occlusion pressure (PAOP), and oxygenation parameters is needed. It is the only device offering the possibility to assess and monitor right ventricular function and corresponding PAP continuously [2]. To date, cardiac output measurement using pulmonary artery thermodilution (PATD) is still considered the gold standard for bedside CO monitoring.
2 Background of Pulmonary Artery Thermodilution
In a structurally normal heart (without any intracardiac recirculation or shunting), blood flow through the right ventricular outflow tract (RVOT) is equal to a time-averaged CO of the left ventricle, commonly referred to as the cardiac output. Techniques to measure this blood flow are based on measuring the dilution of a known quantity of an indicator substance by the passing blood flow. The method most commonly used in clinical practice is thermodilution, which was first described by Branthwaite and Bradley in 1968 [3].
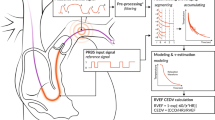
For PATD and CO monitoring using a PAC, a defined bolus of cool fluid is injected through a lumen at the central venous site. While the fluid bolus is then carried with the bloodstream through the right heart and into the pulmonary arteries, it mixes with the blood and is therefore diluted. Thus, the bolus gets warmer, whereas the blood temperature drops. This drop in temperature is recorded with a thermistor close to the tip of the catheter. With this blood temperature curve over time, the specific heat capacity and specific gravity of both blood and injectate as well as the volume of the injectate, the blood flow through RVOT and hence CO can be determined using the Stewart-Hamilton equation.
In addition to this bolus method, continuous cardiac output measurement is possible using modified catheters equipped with thermal filaments. These thermal elements generate heat pulses that are used for thermodilution similar to the cold bolus principle.
3 Derived and Calculated Hemodynamic Variables
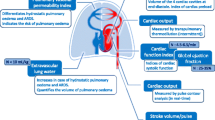
PATD does not only provide the clinician with CO; additional variables can be derived or calculated from the measured parameters (Table 6.1).
3.1 Vascular Resistances
Physiologically, resistances are altered for circulatory regulation and for demand-based distribution of the blood into certain organs. Only the right heart catheterization enables the clinician to determine both systemic and pulmonary vascular resistances. In clinical practice, systemic vascular resistance (SVR) can help to differentiate between the various forms of shock, especially between hypotension with vasoconstriction or vasodilatation. Therefore, SVR can be a tool to guide therapy with vasopressors and/or inotropes.
Pulmonary vascular resistance (PVR) is the ratio of transpulmonary pressure gradient to pulmonary blood flow. Despite numerous attempts to quantify PAP and vascular resistance with less invasive means such as echocardiography or computed tomography imaging, none of them has proven accurate enough. Thus, right heart catheterization remains the method of choice to determine those parameters [4].
PVR itself or indexed to body surface area (BSA) as pulmonary vascular resistance index (PVRI) is used for diagnosis and guidance of treatment of pulmonary hypertension, for assessment of suitability for closure of atrial and ventricular septal defects [5], and for candidacy for cardiac transplantation [6]. In intensive care settings, PVR(I) commonly serves as a surrogate for right ventricular afterload, therefore guiding vasopressor and inotropic therapy of right ventricular dysfunction and failure [7].
Practical Advice
Particularly with poor contractile function, cardiac output is strongly dependent on afterload. Thus, when treating low cardiac output, information on afterload given by vascular resistances is important.
3.2 Stroke Work Index
Stroke work can be used for the evaluation of contractility. For better interindividual comparability, stroke work is often indexed to body surface area, resulting in stroke work index (SWI). Stroke work calculation is done separately for each ventricle as pressure-volume-work, neglecting kinetic work. It represents the area bound by corresponding pressure-volume loops.
Left ventricular stroke work index (LVSWI) will decrease in the case of heart failure and usually increase in response to treatment with inotropes. However, LVSWI only represents the area within the pressure-volume loop, but not its position on the axes. Several factors can simultaneously influence the left ventricular performance. Changes in preload, ventricular compliance, and function can displace the pressure-volume-loops and the area between the slopes. Inferences about the cause of altered function cannot be made, and LVSWI as a single parameter should not be used to guide therapy. However, it can provide information on left ventricular systolic function, especially in cases where left ventricular ejection fraction does not reliably represent cardiac performance, e.g., in cases with mitral regurgitation [8].
Also, preoperative LVSWI has been found to be a significant predictor of outcome after mitral valve surgery for functional regurgitation in non-ischemic dilated cardiomyopathy: lower preoperative values of LVSWI are associated with worse outcome [9].
During the cardiac cycle, the right ventricle pumps an equal stroke volume as the left ventricle, but at markedly lesser stroke work. A high right ventricular stroke work index (RVSWI) is associated with worse kidney function in patients with heart failure with preserved ejection fraction [10]. In contrast, patients with low RVSWI show an increased risk for the need of a right ventricular assist device after left ventricular assist device implantation [11].
3.3 Right Ventricular Function Index (RVFI)
RVFI is a measure of load-adaptability, i.e., it can be used to evaluate the extent to which (elevated) PAP is associated with right ventricular function. A right ventricle, which can increase its contractility and therefore preserve its stroke volume in response to an increased afterload, should stay well compensated—albeit at increased workload. In contrast, with right heart failure, a previously elevated PAP may decrease [12]. An increase in RVFI is then interpreted as a ventricular-vascular mismatch and is associated with poor survival in critically ill patients with severe pulmonary hypertension and in patients undergoing cardiac surgery [13, 14].
3.4 Capacitance
Capacitance quantifies the stiffness of the pulmonary arteries. Pulmonary arterial stiffness plays an important role in right ventricular remodeling and therefore might be a target for altering right ventricular failure. It can also predict survival independently from resistance in heart failure with reduced or preserved ejection fraction as well as in idiopathic pulmonary arterial hypertension [15,16,17].
4 Step-by-Step Approach for Clinical Practice
4.1 Step 1. Indication
In critically ill patients, a PAC should be used if a hemodynamic situation raises a specific question that remains unanswered by clinical examination or less invasive methods. Possible indications are listed in Table 6.2, contraindications (Table 6.3) need to be considered to avoid harm to patients. Figure 6.1 may be a helpful approach in decision-making. Monitoring and treatment of right ventricular dysfunction and pulmonary arterial hypertension remain the domain of the right heart catheterization and PATD [2].
Practical Advice
Pulmonary artery catheterization and thermodilution should not routinely be used in patients with shock but should be considered in patients with refractory shock and in particular when right ventricular dysfunction is present or suspected.
4.2 Step 2. Preparation and Obtaining Pulmonary Artery Occlusion Pressure
To achieve high-quality and reliable results, the preparation is equally essential as the performance of the PATD itself. Therefore, check that all catheters are in place, connected to the monitor, zeroed to atmospheric pressure, and the specific waveforms (arterial, central venous, and pulmonary arterial) with reasonable values are displayed. A so-called flush-test can be useful to check for damping. At this stage, performing a pulmonary artery occlusion maneuver can help to verify the correct position of the PAC and determine PAOP (which is needed for later calculations) at the same time. For reliable calculation of PVR(I), the tip of the catheter needs to be located in West zone III, where pulmonary artery pressure and pulmonary venous pressure are greater than alveolar pressure, thus ensuring continuity in the fluid column between the left atrium and the catheter tip [18].
Practical Advice
When the tip of the PAC is in West zone III, PAOP should be lower than diastolic pulmonary artery pressure and should be altered less than 50% of changes in positive end-expiratory or plateau pressures during mechanical ventilation.
Make sure that the proximal and distal thermistors are connected to the monitor and that the proximal thermistor is connected to the central venous port of the PAC. After verifying the settings at the CO monitor (patient’s data, set injectate type (commonly NaCl 0.9%), volume, and constants), prepare syringes with cooled solution respecting hygiene rules in order to avoid catheter-associated bloodstream infections. For the injectate volume, refer to the settings of the CO monitor. The colder and the larger the volume, the better the signal-to-noise ratio [19]. The highest reproducibility of CO measurements in critically ill patients was demonstrated with 10-mL iced injectate, which also reflects the common clinical practice.
4.3 Step 3. Performing Pulmonary Artery Thermodilution
Due to a short indicator transit time from the injection site at the right atrium to the thermistor at the pulmonary artery, a single PATD measurement is usually shorter than a respiratory cycle. The right ventricular output may vary due to cyclic changes in venous return and right ventricular afterload during both spontaneous breathing and mechanical ventilation. Thus, for performing PATD, certain aspects on the timing of the injections need to be considered: performing PATD at the same moment of the respiratory cycle should create reproducible values for subsequent comparison. On the other hand, measurements performed in that manner might still not represent the mean CO or even the relative phasic changes in the flow; therefore, pseudorandomized injections at different positions at the respiratory cycle could better reflect the current CO and better enable comparison [20].
In order to reduce errors and to average results, a series of injections should be performed. Clear recommendations on the number can not be given, but it seems that three injections, although clinically mostly performed, are insufficient with regard to accuracy and reproducibility [21, 22]. Injections need to be done as fast and smoothly as possible. The results of the individual measurements should be within a 10% range. Reject aberrant measurements (outside the 10% range) and the sets with highest and lowest results. If necessary, repeat PATD.
4.4 Step 4. Calculation and Interpretation of Hemodynamic Variables
Analysis and interpretation should always take the patient’s context and the current clinical situation into account. In contemporary CO monitors, calculations are performed automatically. With attention to typical reasons for erroneous results in PATD (Table 6.3), use all available findings to guide therapy. Consider preexisting clinical conditions and diseases as well as medication and functional or laboratory monitoring of organs that are most likely affected by cardiac dysfunction (i.e., the brain, kidneys, liver, and gut).
Therapy goals should be defined and aimed at individually for every patient. Choose the therapy in accordance to pharmacology and physiology with the help of corresponding guidelines [23].
5 Risks and Limitations of Pulmonary Artery Thermodilution
As a result of the SUPPORT trial [24, 25], a high number of intensivists is reluctant to use the PAC in monitoring critically ill patients, most likely due to persistent doubts about its safety and its efficacy in guiding beneficial therapy. In addition, the PAC faces competition from supposedly less invasive hemodynamic monitoring devices such as transpulmonary thermodilution, pulse contour analysis, and echocardiography.
Like any other device, the PAC and therefore PATD have risks that need to be considered (Table 6.4). However, careful operation of the catheter will reduce them to a minimum. The PAC-specific risks (0.3% severe complications, 0.1% attributable mortality) have been reported to be lower as the risks associated with transesophageal echocardiography.
Specific conditions can lead to erroneous results (Table 6.5), but even with correctly determined variables, misinterpretation with potential consecutive inappropriate therapies is a well-known phenomenon [26].
For the so-called continuous CO monitoring PAC, it must be taken into account that it cannot be used for CO surveillance in rapidly changing hemodynamic situations. They have a certain delay in displaying CO (3–12 min) as the CO is averaged over several cardiac cycles [27].
6 Conclusion
PATD still is the gold standard for CO measurement. The proper use requires a profound theoretical and clinical knowledge, not only about patients’ pre-existing conditions but also about the limitations, pitfalls, and difficulties in interpreting measurement results. For the experienced user, PAC/PATD provides a comprehensive view of the hemodynamic situation, which can help optimize global oxygen balance.
Keynotes
-
Pulmonary artery thermodilution (PATD) is a valuable tool to determine cardiac output and derived parameters in critically ill patients.
-
Right ventricular failure and associated and contributing diseases in the critical care setting are the domain of PATD. In addition, derived parameters can help in decision-making in interventional or surgical therapy of cardiac conditions.
-
The complexity of parameters needs careful and skilled interpretation in the context of the individual patient.
References
Swan HJ, Ganz W, Forrester J, Marcus H, Diamond G, Chonette D. Catheterization of the heart in man with use of a flow-directed balloon-tipped catheter. N Engl J Med. 1970;283:447–51.
Ventetuolo CE, Klinger JR. Management of acute right ventricular failure in the intensive care unit. Ann Am Thorac Soc. 2014;11:811–22.
Branthwaite MA, Bradley RD. Measurement of cardiac output by thermal dilution in man. J Appl Physiol. 1968;24:434–8.
Weir-McCall JR, Struthers AD, Lipworth BJ, Houston JG. The role of pulmonary arterial stiffness in COPD. Respir Med. 2015;109:1381–90.
Galiè N, Humbert M, Vachiery J-L, Gibbs S, Lang I, Torbicki A, Simonneau G, Peacock A, Vonk Noordegraaf A, Beghetti M, Ghofrani A, Gomez Sanchez MA, Hansmann G, Klepetko W, Lancellotti P, Matucci M, McDonagh T, Pierard LA, Trindade PT, Zompatori M, Hoeper M. 2015 ESC/ERS guidelines for the diagnosis and treatment of pulmonary hypertension: the joint task force for the diagnosis and treatment of pulmonary hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS): endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC), International Society for Heart and Lung Transplantation (ISHLT). Eur Heart J. 2016;37:67–119.
Mehra MR, Canter CE, Hannan MM, Semigran MJ, Uber PA, Baran DA, Danziger-Isakov L, Kirklin JK, Kirk R, Kushwaha SS, Lund LH, Potena L, Ross HJ, Taylor DO, Verschuuren EAM, Zuckermann A. The 2016 International Society for Heart Lung Transplantation listing criteria for heart transplantation: a 10-year update. J Heart Lung Transpl. 2016;35:1–23.
Lankhaar J-W, Westerhof N, Faes TJC, Marques KMJ, Marcus JT, Postmus PE, Vonk-Noordegraaf A. Quantification of right ventricular afterload in patients with and without pulmonary hypertension. Am J Physiol Heart Circ Physiol. 2006;291:H1731–7.
Choi J-O, Lee S-C, Choi SH, Kim SM, Choi JH, Park JR, Song BG, Chang S-A, Park S-J, Park SW, Park PW. Noninvasive assessment of left ventricular stroke work index in patients with severe mitral regurgitation: correlation with invasive measurement and exercise capacity. Echocardiography (Mount Kisco, N.Y.). 2010;27:1161–9.
Kashiyama N, Toda K, Miyagawa S, Yoshikawa Y, Hata H, Yoshioka D, Sawa Y. Left ventricular stroke work index associated with outcome after mitral valve surgery for functional regurgitation in nonischemic dilated cardiomyopathy. Semin Thorac Cardiovasc Surg. 2020;32(4):698–709.
Kanjanahattakij N, Sirinvaravong N, Aguilar F, Agrawal A, Krishnamoorthy P, Gupta S. High right ventricular stroke work index is associated with worse kidney function in patients with heart failure with preserved ejection fraction. Cardior Med. 2018;8:123–9.
Fukamachi K, McCarthy PM, Smedira NG, Vargo RL, Starling RC, Young JB. Preoperative risk factors for right ventricular failure after implantable left ventricular assist device insertion. Ann Thorac Surg. 1999;68:2181–4.
Vonk-Noordegraaf A, Haddad F, Chin KM, Forfia PR, Kawut SM, Lumens J, Naeije R, Newman J, Oudiz RJ, Provencher S, Torbicki A, Voelkel NF, Hassoun PM. Right heart adaptation to pulmonary arterial hypertension: physiology and pathobiology. J Am Coll Cardiol. 2013;62:D22–33.
Robitaille A, Denault AY, Couture P, Belisle S, Fortier A, Guertin M-C, Carrier M, Martineau R. Importance of relative pulmonary hypertension in cardiac surgery: the mean systemic-to-pulmonary artery pressure ratio. J Cardiothorac Vasc Anesth. 2006;20:331–9.
Saydain G, Awan A, Manickam P, Kleinow P, Badr S. Pulmonary hypertension an Independent risk factor for death in intensive care unit: correlation of hemodynamic factors with mortality. Clin Med Insights Circ Respir Pulm Med. 2015;9:27–33.
Dupont M, Mullens W, Skouri HN, Abrahams Z, Wu Y, Taylor DO, Starling RC, Tang WHW. Prognostic role of pulmonary arterial capacitance in advanced heart failure. Circ Heart Fail. 2012;5:778–85.
Al-Naamani N, Preston IR, Hill NS, Roberts KE. The prognostic significance of pulmonary arterial capacitance in pulmonary arterial hypertension: single-center experience. Pulm Circ. 2016;6:608–10.
Mahapatra S, Nishimura RA, Sorajja P, Cha S, McGoon MD. Relationship of pulmonary arterial capacitance and mortality in idiopathic pulmonary arterial hypertension. J Am Coll Cardiol. 2006;47:799–803.
Kane PB, Askanazi J, Neville JF, Mon RL, Hanson EL, Webb WR. Artifacts in the measurement of pulmonary artery wedge pressure. Crit Care Med. 1978;6:36–8.
Nadeau S, Noble WH. Misinterpretation of pressure measurements from the pulmonary artery catheter. Can Anaesth Soc J. 1986;33:352–63.
Synder JV, Powner DJ. Effects of mechanical ventilation on the measurement of cardiac output by thermodilution. Crit Care Med. 1982;10:677–82.
Woods M, Scott RN, Harken AH. Practical considerations for the use of a pulmonary artery thermistor catheter. Surgery. 1976;79:469–75.
Stevens JH, Raffin TA, Mihm FG, Rosenthal MH, Stetz CW. Thermodilution cardiac output measurement. Effects of the respiratory cycle on its reproducibility. JAMA. 1985;253:2240–2.
Rajaram SS, Desai NK, Kalra A, Gajera M, Cavanaugh SK, Brampton W, Young D, Harvey S, Rowan K. Pulmonary artery catheters for adult patients in intensive care. Cochrane Database Syst Rev. 2013:CD003408.
Connors AF, Speroff T, Dawson NV, Thomas C, Harrell FE, Wagner D, Desbiens N, Goldman L, Wu AW, Califf RM, Fulkerson WJ, Vidaillet H, Broste S, Bellamy P, Lynn J, Knaus WA. The effectiveness of right heart catheterization in the initial care of critically ill patients. SUPPORT investigators. JAMA. 1996;276:889–97.
Singh K, Mayo P. Critical care echocardiography and outcomes in the critically ill. Curr Opin Crit Care. 2018;24(4):316–21.
Squara P, Bennett D, Perret C. Pulmonary artery catheter: does the problem lie in the users? Chest. 2002;121:2009–15.
Poli de Figueiredo LF, Malbouisson LM, Varicoda EY, Carmona MJ, Auler JO, Rocha e Silva M. Thermal filament continuous thermodilution cardiac output delayed response limits its value during acute hemodynamic instability. J Trauma. 1999;47:288–93.
Reuter DA, Huang C, Edrich T, Shernan SK, Eltzschig HK. Cardiac output monitoring using indicator-dilution techniques: basics, limits, and perspectives. Anesth Analg. 2010;110:799–811.
Tewelde SZ, Liu SS, Winters ME. Cardiogenic shock. Cardiol Clin. 2018;36:53–61.
Saugel B, Vincent J-L. Cardiac output monitoring: how to choose the optimal method for the individual patient. Curr Opin Crit Care. 2018;24:165–72.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Zitzmann, A., Reuter, D.A., Löser, B. (2021). Pulmonary Artery Thermodilution. In: Kirov, M.Y., Kuzkov, V.V., Saugel, B. (eds) Advanced Hemodynamic Monitoring: Basics and New Horizons. Springer, Cham. https://doi.org/10.1007/978-3-030-71752-0_6
Download citation
DOI: https://doi.org/10.1007/978-3-030-71752-0_6
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-71751-3
Online ISBN: 978-3-030-71752-0
eBook Packages: MedicineMedicine (R0)