Abstract
Most pediatric nail conditions are benign but remain a source of anxiety for parents or physicians inexperienced in onychology and may be a cosmetic issue or a cause of functional impairment. This review includes the most relevant articles from the last 5 years. Physiologic alterations at birth are frequent and important to recognize. Nails are involved in many congenital disorders and part of a larger clinical spectrum of many genetic syndromes. Among infectious diseases, periungual warts are very challenging to treat. On the contrary, onychomycosis seems easier to treat in children than in adults. As in adults, nail psoriasis is associated with a higher risk of psoriatic arthritis and metabolic comorbidities. Crushing injury of finger by a door is the most common cause of acute nail trauma. The management of subungual hematomas and nail bed laceration still remains controversial. Podiatric abnormalities are underestimated and should be considered as a potential cause of nail dystrophy in children. Children who suck their thumbs or bite their nails are less likely to have atopic sensitization. Topical steroids should be the first-line treatment for retronychia and surgery only restricted to nonresponsive cases. Longitudinal melanonychia in children displays more worrisome melanoma-associated features than in adults, but the very vast majority are benign, and a wait-and-see policy is the gold standard. Yellow nail syndrome is extremely rare in children but should raise the potential role of titanium in candies and toothpastes.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
Introduction
Nail disorders in children can be classified into seven categories: physiologic, congenital and/or hereditary, infectious, inflammatory, traumatic or mechanical, neoplastic, systemic, and/or iatrogenic [1]. Most pediatric nail conditions are benign but are a source of anxiety for parents or physicians inexperienced in onychology and may be a cosmetic issue or a cause of functional impairment [1, 2]. To date, very few studies have been conducted to determine the overall prevalence of nail disorders in children [3,4,5]. This prevalence has been estimated at 11.1% and 6.8% in two studies [3, 4]. A very recent study examined the span of nail conditions in a pediatric onychology center and highlighted the ten most frequent diagnoses (Table 14.1) [6].
This study also demonstrated that some diagnoses were more frequently encountered depending on the age category (Table 14.2). Another publication has classified nail diseases in children according to age [7].
This chapter collects the recent findings and updates found in the literature on children’s nail disorders. This review includes the most relevant articles from the last 5 years. Search engines were Google Scholar and the Medline database through PubMed and MeSH. Keywords included “nails,” “children,” “infants,” and “teenagers,” as well as specific keywords for many nail disorders.
Physiologic Alterations
Very few papers have described physiologic nail alterations in children, especially in newborns. A recent study from Chinazzo et al. described the normal nail features in newborns. It showed that koilonychia, onycholysis, and onychoschizia were frequent findings on toenails, while the absence of lunula was a usual feature of both finger- and toenails. The authors also reported an apparent hypertrophy of the proximal nail fold of the hallux in 1/3 of the toddlers and of the lateral folds of the hallux in 3/4 of the newborns. This hypertrophy was accentuated by koilonychia and a triangular shape of the nail plate. All dark-skinned newborns showed hyperpigmentation of the proximal fold of both hands and feet, especially between 2 and 6 months, that faded before the age of 1 [8].
One article reviewed the literature on koilonychia, which is a common feature on toenails in infants. Although mostly transient and idiopathic in young children, some familial and syndromic cases have been reported [9].
Key Points
-
Koilonychia, onycholysis, and onychoschizia are frequent findings on toenails in newborns, as well as the absence of lunula on both finger- and toenails.
Congenital Disorders
Congenital Malalignment of the Great Toenails
This entity is probably underdiagnosed, and most of the recent publications are case reports [10,11,12,13]. Congenital malalignment usually appears at birth or during the first years of life [10]. Mean age for medical consultation is 3 years old [6]. However, a few studies reported cases of great toenail malalignment with onset in adolescence or young adulthood without any history of nail surgery or acute trauma, raising the possibility of a late-onset presentation of this condition [11, 14]. Congenital malalignment of the great toenail spontaneously improved in 58% of a recent case series of 25 patients, similar to the 50% rate quoted in the literature [6, 15]. Clinical observation with photographic follow-up along with podiatric care is the rule. For severe forms, or those that don’t resolve spontaneously, surgical realignment may be considered to avoid unsightly and persistent nail dystrophy [10, 16]. In the most recent series, four patients underwent a whole nail unit rotation surgery, with an improvement of the nail dystrophy in three cases [6].
Congenital Hypertrophy of the Lateral Nail Folds
Congenital hypertrophy of the lateral nail folds affects children around the age of 1 (Fig. 14.1). Great toenails are mainly involved, both in 67% of cases. Spontaneous improvement occurs in around 3/4 of cases, reason for which conservative care and follow-up is usually sufficient. Surgery is infrequent and restricted to very prominent or recalcitrant cases [6].
Pachyonychia Congenita
Pachyonychia congenita (PC) is a group of autosomal dominant disorders resulting from mutations in one of five keratin genes [17, 18]. The last classification, validated by phenotype-genotype correlations, divides PC into subtypes according to the mutation found in the keratin-encoding genes KRT6A, KRT6B, KRT6C, KRT16, and KRT17 [19]. PC prevalence in Western countries is 0.9 cases per million with a worldwide PC population estimated between five to ten thousand. In a large case-cohort study of 815 patients conducted by Samuelov et al., the earliest and most common clinical feature of PC was nail dystrophy, appearing during the first year of life in most cases. The median number of affected fingernails and toenails was ten, while the mean number was 6.4 and 8, respectively. Fifty-one percent of PC patients had all 20 nails affected [18]. Nail dystrophy may be responsible for pain, infection, and functional and psychosocial impairment [17, 18]. It deeply affects social interactions and function of adolescents. Among patients with a detectable mutation, PC manifests with nail thickening and plantar keratoderma before school age in more than 3/4 of affected children, allowing early diagnosis [19]. KTR6A mutations were associated with a younger age at diagnosis and a higher number of fingernails/toenails involvement. Conversely, a lack of fingernail involvement was most commonly associated with KRT16 and KRT6B mutations [18, 20]. An increased number of affected toenails and earlier age of toenails involvement predicted fingernail dystrophy, while an increased number of affected fingernails correlated with toenails involvement. Earlier onset of toenails involvement correlated with the development of plantar keratoderma, while age of fingernail dystrophy onset and walking aids use predicted palmar keratoderma. Finally, oral leukokeratosis and natal teeth correlated with an earlier toenail involvement, while hoarseness correlated with an increased number of involved fingernails [18]. No specific histopathological feature is identified in PC nails. Parakeratosis and plasma globules are the most prominent features in both clinically affected and unaffected PC nails. The presence of onychomycosis in a nail plate does not exclude a diagnosis of PC [20]. Nail removal remains a therapeutic option and seems to have an overall positive outcome [17].
Nail-Patella Syndrome
Nail-patella syndrome (NPS) is a rare autosomal dominant condition characterized by variable nail, skeletal, renal, and ocular anomalies [21]. The incidence of NPS is usually given as 1 per 50,000, but an epidemiologically based incidence estimate is still lacking [22, 23]. LMX1B is the major gene responsible for NPS and explains around 95% of all cases [24]. To date, over 180 heterozygous mutations of LMX1B have been reported in NPS [22]. A new mutation in WIF1 gene has also been identified, suggesting a potential novel cause of NPS [24]. Mean age at the time of clinical diagnosis is 6.54 years [25]. Almost all patients have nail abnormalities, the most frequent being hyponychia. Other findings include triangular lunula, absence of lunula, anonychia, nail splitting, pterygium, koilonychia, as well as the loss of the dorsal creases in the skin overlying the distal interphalangeal joints [21, 25]. These nail changes may be present since birth and are commonly bilateral and symmetrical [25]. Each individual nail is usually more severely affected on its ulnar side [23, 26]. Thumbnails are the most affected, and the severity tends to decrease towards the little finger [23, 25, 26]. When toenails are involved, the abnormalities tend to be less severe, and the little toenail is most commonly affected [23]. Triangular lunula is a pathognomonic finding, but it is not encountered in all cases [25]. When present, it is mainly associated with a dystrophy of the medial part of the nail, ranging from a simple longitudinal crease to pseudopterygium and median nail fracture. These findings are detectable only in forms of NPS with severe nail involvement [26]. The severity of the nail signs is unrelated to visceral involvement [25, 26].
Key Points
-
Congenital hypertrophy of the lateral nail folds is a benign condition that spontaneously improves in 3/4 of cases. Surgery should be restricted to resistant cases.
-
Congenital malalignment of the great toenail spontaneously improves in around 50% of cases. Clinical observation and photographic follow-up are a must. Severe cases and non-improving cases should be proposed surgery.
-
Pachyonychia congenita is responsible for severe psychosocial impairment. By the age of 5, more than 3/4 of patients have nail alterations, allowing early diagnosis.
-
Nail alterations are constant in nail-patella syndrome. Triangular lunula is pathognomonic but not always present.
Infectious Diseases
Periungual Warts
Periungual warts are a therapeutic challenge (Fig. 14.2). Treatment modalities include salicylic acid, cryotherapy, bleomycin, contact immunotherapy – with diphenylcyclopropenone or squaric acid dibutyl ester – and laser ablation [27]. A shorter sensitization period and a more severe sensitization reaction (characterized by a higher “erythema and blister index”) contribute to a shorter time period required for a complete cure of the periungual warts with diphenylcyclopropenone immunotherapy [28]. Another type of immunotherapy that can be used is Vitamin D3 injections in an oily base, just beneath the warts, every 2 weeks for a maximum of four sessions. This new treatment seems promising. However, pain during injection is the limiting factor. It is a safe, inexpensive, and effective treatment for periungual warts [29]. Topical cidofovir is a possible alternative for recalcitrant periungual warts or those that fail to respond to the conventional treatment. Nonetheless, its high price and its limited availability are major limitations [30]. The application of a nitric-zinc complex solution (Verrutop®) twice a month on warts resulted in a complete clearance in 83.9% with excellent cosmetic results and tolerance , according to a recent study [31]. In a small case series of 11 patients, translesional bleomycin delivered via a multipuncture technique using an ablative carbon dioxide fractional laser before the application of bleomycin on the wart resulted in a complete clearance – recurrence-free for 6 months – in 70% of cases [32]. Finally, a combination of superficial shaving with photodynamic therapy also seems to be an effective and safe treatment for recalcitrant , multiple, and thick periungual warts [33].
Nail Scabies
To date, only five cases of pediatric nail scabies have been reported in the literature [34,35,36]. In the study of Chinazzo et al. including 47 children with confirmed scabies, a nail involvement was found in 6.4% of children, all infants. In two of the three cases, scabies was surprisingly found in a great toenail rather than in fingernails. According to Chinazzo et al., the nail area may constitute a reservoir of mites and may be a risk factor for scabies recurrence. Nails should not be overlooked during scabies treatment [34]. Some authors recommend to cut, brush, and apply a topical scabicide on the nails, even in classic scabies [35].
Acute Paronychia
Neonates with oral self-soothing behaviors may be more at risk for developing paronychia of mixed anaerobic and aerobic infections. Initial therapy with broad-spectrum antibiotics amoxicillin/clavulanate or clindamycin is suggested [37].
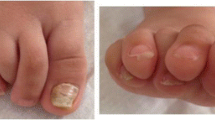
Onychomycosis
Onychomycosis in childhood is rare and affects approximately 0.2–2.6% of all children [38, 39]. However, an increased incidence has been reported in the pediatric population [38]. Trichophyton rubrum is the most commonly isolated pathogen, as in adults [39, 40]. Children are more likely to respond to monotherapy since they have thinner and faster-growing nails [41]. New topical treatments for onychomycosis have an increased nail penetration and sometimes additional delivery routes to the site of infection [42, 43]. Tavaborole may be a good candidate to treat children with onychomycosis. It penetrates the nail plate very well and is effective when used in monotherapy [41]. It was found to be safe and well tolerated in the pediatric population [44]. When a systemic treatment has to be prescribed, terbinafine is the first choice. It is recommended to perform a baseline transaminase monitoring. On a study with 261 children treated with terbinafine, the authors discovered that 12.5% of patients had grade 1 laboratory abnormalities – such as liver alterations – prior to (8.3%) or during therapy (4.2%). However, if the pretreatment’ routine laboratory is within normal limits, further monitoring is unnecessary, considering the low incidence of clinically significant adverse effects, costs of laboratory tests, and patient discomfort [45].
Key Points
-
Periungual warts remain a therapeutic challenge.
-
Nail scabies may be a risk factor for resistance to therapy and recurrence.
-
Neonates with oral self-soothing behaviors may be more at risk for developing paronychia.
-
New topical treatments with better nail penetration may be used in monotherapy for onychomycosis.
Inflammatory Disorders
Nail Lichen Planus
In Goettmann et al.’s study , among 67 patients with nail lichen planus, around 11% were children [46]. In a more recent study from Morocco, among the 20 cases of nail lichen planus, amazingly 40% were children, highlighting the frequency of pediatric forms in this country [47]. Nail alterations are reported in 13.9% of children presenting with skin lichen planus [48].
Nail Lichen Striatus
In a report of seven cases by Kim et al., four were children, between 4 and 11 years old. All patients had both typical skin lesions and nail abnormalities, although lichen striatus can be limited to the nail. Nail lichen striatus usually involved a single digit. The most common nail change was longitudinal fissuring (Fig. 14.3) [49]. Iorizzo et al. described the dermoscopic features of nail lichen striatus: involvement of only one part of the nail plate with linear longitudinal fissuring, ridging, and distal splitting, especially if seen with perionychial skin lesions, is characteristic. This dermoscopic pattern may help in the diagnosis of nail lichen striatus [50]. In the study of Kim et al., most nail lesions resolved within a mean of 4 months after the initiation of a topical corticosteroid cream and 0.1% tacrolimus ointment for both skin and nail lesions [49].
Trachyonychia
In a recent series of 26 patients, trachyonychia mainly affected children between 6 and 12 years old, with a mean age of 8 years [6]. Biopsies for diagnostic purposes are not recommended because whatever the cause, trachyonychia doesn’t lead to nail destruction [51]. A favorable evolution was observed in 75% of cases, confirming the good prognosis previously published, regardless of treatment (Fig. 14.4) [6, 51, 52]. Nonetheless, an annual photographic follow-up is usually suggested to reassure parents and their child. In a recent series, trachyonychia did not appear to regress faster in patients receiving topical treatment, in contrast with the study of Park et al., which reported a significant nail improvement in 98.6% of cases with calcipotriol/betamethasone ointment applied once daily for 6 months [6, 53].
Nail Psoriasis
The prevalence of nail involvement in psoriatic children varies widely between studies. In recent series, nail involvement was reported between 15.7% and 32.3% of psoriatic children [54,55,56]. This prevalence increases with age [55, 56]. Fingernails are involved more frequently than toenails [55]. The main clinical features are pitting on fingernails and onycholysis as well as pachyonychia on toenails. Other common features include Beau’s lines, oil drop, paronychia, leukonychia, and splinter hemorrhages. All fingers are involved at similar frequencies, whereas the big toenails are involved twice as often as the others, suggesting a Koebner phenomenon. Nail involvement is significantly associated with male gender, palmoplantar psoriasis, and a higher PASI (Psoriasis Area Severity Index) score, indicating a more severe disease course over time [55, 56]. When comparing the mean NAPSI (Nail Psoriasis Severity Index) and the mean PASI according to nail lesions, a study found that subungual hyperkeratosis and nail fold psoriasis were significantly associated with the severity of both nail psoriasis and cutaneous psoriasis [57]. As in adults, nail psoriasis is closely associated with psoriatic arthritis [55]. Nail involvement in children is also associated with metabolic comorbidities such as abdominal obesity, overweight, or metabolic syndrome [58]. The microscopic nail features such as the presence of neutrophils and serous lakes in the nail plate have also been associated with higher PASI and NAPSI scores in psoriatic children. Nail clippings remain very useful to help the diagnosis and to rule out onychomycosis [59].
Key Points
-
Nail lichen planus is rare in children, accounting for about 11% of all nail lichen planus cases.
-
Nail lichen striatus is characterized by a linear longitudinal fissuring, ridging, and distal splitting of one part of the nail plate.
-
Trachyonychia spontaneously improves in most cases and never leads to nail destruction, whatever the cause. Biopsies are therefore unnecessary.
-
Nail psoriasis is associated with psoriatic arthritis and with a higher PASI score, indicating a more severe course of the disease.
Traumatic and/or Mechanical Disorders
Pediatric Finger Injuries/Acute Trauma
Fingertip injuries are common in children, affecting mostly boys under 5 years old, probably because of an imbalance between gross motor abilities and cognitive development [60,61,62,63]. Younger children are also naturally curious and use their hands to probe and explore their environment [62, 64]. Among all finger injuries, nail bed injuries and fractures are the most prevalent [60, 62]. Nail bed injuries can be classified as subungual hematomas, simple or stellate lacerations, avulsions, and crush injuries [65]. Crushing injury of finger by door or window is still the most common mechanism of injury among younger children and accounts for a large number of hospital admissions. The door is often closed by another child, at home, in the presence of an adult. The right hand is usually involved and the most commonly injured finger is the middle finger (Fig. 14.5) [60, 62]. Imaging rules out bone fractures [64]. The management of subungual hematomas and nail bed lacerations remains controversial. Most hematomas caused by nail bed lacerations do not usually require nail removal and repair, if the nail/nail margins are intact. Small hematomas are often left to reabsorb without treatment [66]. For larger and painful subungual hematomas, there is much debate about removal of the nail plate for repair of a nail bed laceration compared with simple trephination – i.e., the creation of a hole in the nail plate to release trapped blood [65, 66]. Satku et al. compared the results of nail removal and formal nail bed reconstruction with trephination of a subungual hematoma after a fingernail crush injury. They found that simple nail trephination was equal or superior to removal of the nail with nail bed repair, with significantly lower cost [61]. The rate of accidents is not reduced by the presence of adults, which highlights the need for preventive measures and health education [60, 63]. Satku et al. suggested techniques to prevent door crush injuries in children, including placing door stoppers and using plastic hinge protectors [61, 62]. The cost of prevention of fingertip injuries by using safety equipment is less than the cost of treating them [61, 63]. Sports injuries are most common among the 13- to 18-year-old age group [62].
Podiatric Disorders
Podiatric abnormalities remain underestimated and should be considered as potential causes of nail abnormalities in children. It includes toe malposition, difference in shape/size between the two feet, abnormal gait, or improper shoes. Toe malpositioning results in nail thickening, nail bed hyperkeratosis, or onycholysis, which may mimic other nail disorders such as onychomycosis or nail psoriasis. If not treated, it can eventually lead to permanent dystrophies in adulthood and sequelae related to feet malposition, like back pain. It is therefore crucial to examine the whole foot and recognize the toe position. Medical treatment is usually not necessary. Conservative measures are recommended, such as nail debridement or orthodigital devices. Referral to a podiatric practitioner is useful. Surgery is not recommended in children [67].
Onychotillomania and Onychophagia
Onychophagia affects all age groups but is more prevalent in children and adolescents, predisposing to psychosocial issues and complications including paronychia and dental problems. According to the study of Winebrake et al. including 281 patients, the prevalence of nail biting for more than 1 month was 37%, with a median age of onset of 5 years old. Only fingernails were involved in 88% of cases. There was a history of nail biting in 63% of cases. Biters were 3.34 times more likely to have a diagnosis of a psychiatric disorder than non-biters [68]. The study of Lynch et al. showed that children who suck their thumbs or bite their nails were less likely to have atopic sensitization in childhood and adulthood. On the contrary, no association was found with asthma or hay fever [69]. The application of bitter nail lacquers produced significant improvement in terms of odds of frequent nail biting [68]. Management of onychophagia includes a combination of pharmacotherapy, such as N-acetylcysteine and antidepressant therapy, stimulus control, habit reversal training, as well as cognitive behavioral and aversion therapy [68, 70]. N-Acetylcysteine warrants consideration as an efficacious pharmacological intervention due to its relative safety [68, 71]. Auricular acupressure appears to improve the efficacy of habit reversal treatment, likely by reducing anxiety [72]. Halteh et al. discourage practitioners to tell children that no treatment is needed and that they will outgrow it [73].
Retronychia
Retronychia is mostly described in adults, but pediatric cases have also been reported, with the same clinical features (Fig. 14.6) [74]. Until recently, nail avulsion was the treatment of choice. A study from Lencastre et al. evaluated the efficacy of potent topical steroids in retronychia. The youngest patient included in the study was 12 years old. Topical steroids were used under occlusion for an average duration of 8 weeks, with a complete or partial response in 41.1% and 28.5% of cases, respectively. Response correlated with milder paronychia and longer treatment durations. Topical steroids should therefore be the first-line treatment of retronychia, especially in milder forms, associated with shoewear and gait biomechanics assessment [75, 76]. Nail avulsion should still be performed if there is no improvement after 10 weeks [75].
Ingrown Nails
In the study of Arica et al., a positive family history of ingrown nail was present in 15.7% of patients. High prevalence of incorrect nail cutting (72.1%), trauma (36.1%), poorly fitting shoes (29%), hyperhidrosis (12.9%), and obesity (9.7%) were determined among the patients with ingrown toenails. The mean age at presentation was 15 years [77]. Ingrown toenails in children and adolescents should be treated in first instance by nonoperative methods, such as taping and nail brace application [78,79,80]. Operative options can be considered for resistant cases or in case of recurrence [80]. Partial nail avulsion with chemical matrix cauterization is considered as the technique of choice [81]. However, Livingston et al. suggested to consider the Vandenbos procedure – a large debulking of the lateral folds with secondary intention healing – which is associated with a low recurrence rate in children, adolescents, and young adults with ingrown toenails. Patient-reported recovery time, complication rate, functional outcomes, and satisfaction are excellent [82].
Key Points
-
Fingertip injuries are common in children, mostly crushing by a door or a window. This should be preventable with adequate measures.
-
Topical steroids are the first-line treatment of retronychia, especially in milder forms.
-
Nail biting is common in children. It is associated with psychiatric disorders but reduces the risk of atopic sensitization.
-
Ingrown toenails in children and adolescents should be first treated conservatively.
Nail Tumors
Subungual Exostosis
Subungual exostosis (SE) is an uncommon, benign osteocartilaginous tumor of the distal phalanx [83]. Half of the patients are under 18, with an equal female/male ratio [83,84,85]. The hallux is the most common location [83, 84]. Fingernails are rarely affected. Pain is a common complaint [83].
A history of trauma is present in about 30% of cases [84]. One study suggested that trauma, including surgeries, may have a dual function of induction and regression of SE [86]. Infections are also frequently implicated in the etiology of the disease [83]. A study focusing on dermoscopic features of subungual exostosis showed that vascular ectasia (Fig. 14.7) was the most common dermoscopic finding, followed by hyperkeratosis, onycholysis, and ulceration [87].
Longitudinal Melanonychia
The mean age at time of consultation for longitudinal melanonychia (LM) is 8 years old [6]. In a recent histopathological study of 30 childhood cases of melanonychia conducted in the USA, Cooper et al. reported subungual lentigo in 20 cases, subungual nevus in 5 cases, and atypical melanocytic hyperplasia in 5 cases [88, 89]. Childhood LM due to a benign nail matrix nevus (NMN) displays more melanoma-associated features compared with those of adults [90, 91]. Those features include a sharply demarcated pigment band of even width, a Hutchinson’s sign – usually observed at the hyponychium and/or proximal nail fold cuticles – and a longitudinal brush pigmentation [91]. A pseudo-Hutchinson sign, a triangular sign, an irregular pattern, as well as dots and globules are also detected more commonly in children. NMN in children are darker and multicolored. Pigmentation also tends to be broader in children, but without statistical significance [90]. There is still no consensus on how to manage or follow up NMN in children. It has been shown that the predictive scoring model for dermoscopy of nail melanoma in situ couldn’t be applied to the pediatric population (Fig. 14.8) [92,93,94]. Nail melanoma is exceedingly rare in children, with less than 20 cases of pediatric subungual melanoma in the literature, without any deaths reported to date [89, 92, 95]. Only two cases were subungual invasive melanomas that subsequently metastasized to regional lymph nodes without distant metastases, providing evidence that subungual melanoma with metastatic potential does occur in children , albeit exceptionally rarely [92]. Therefore, the vast majority of excised lesions are in fact benign, even if they display worrisome clinical, dermoscopic, or sometimes histopathological features [88, 96]. Considering the morbidity associated with surgical excision of the nail matrix and the rarity of nail unit melanoma in children, the overwhelming majority of cases can be managed conservatively with photographic and dermoscopic follow-up, especially under 14 years old, with biopsy only required in selected cases [88, 89, 92, 96]. When LM appears in older teenagers, a closer follow-up is required [89]. Piraccini et al. decide to biopsy only when the band rapidly enlarges and involves the whole nail and when its color is dark black. This management remains difficult, especially when dealing with anxious parents [94, 97].
Onychopapilloma
Onychopapilloma is a benign nail unit tumor that is usually seen in adults. Two cases of onychopapilloma in children – aged 9 and 10 years old – and one in a teenager have been recently described [98, 99].
Key Points
-
Subungual exostosis affects mainly young patients; half of them are <18 years old.
-
Longitudinal melanonychia is benign in children in the vast majority of cases, even if it frequently displays worrisome features. A wait-and-see policy is most of the time appropriate.
-
Onychopapilloma is a benign longitudinal nail tumor which can occur in children and teenagers.
Systemic and/or Iatrogenic Disorders
Fever-Related Beau’s Lines or Onychomadesis
A temporary cessation in matrix growth from a systemic shock like a thermal peak may result in a Beau’s line or an onychomadesis, according to the duration of the injury [100]. This condition is observed mainly in the group 2 to 6 years old, most probably because of the fragile nail matrix in young children [6, 101]. Thirty percent of children with hand, foot and mouth disease (HFMD) have such nail abnormalities [102]. Fingernails are more commonly involved than toenails. Nail changes typically occur synchronously [101]. It is still debated whether the inhibition of the nail matrix proliferation results from direct inflammation spreading from skin lesions of HFMD around nails or a coxsackievirus-specific nail matrix involvement, or HFMD’s severe systemic impact on the general condition of the small children [100]. In HMFD, nail changes usually occur within 1 or 2 months after onset and last for 1 to 8 weeks [101].
Yellow Nail Syndrome
YNS is a rare disorder and is even more rarely reported in children with around 20 cases described in the literature. As in adults, yellow nails and recurrent respiratory infections are the most common presentations. Lymphedema was also noted in 12 of 19 cases in the literature. There seem to be two age peaks in the incidence of YNS. Most pediatric cases presented at birth, maybe because of a transplacental crossing of titanium from the mother to the fetus. The second peak appears between the age of 6 and 10 and may be related to the high exposure to candy or children’s toothpastes that contain titanium dioxide at this age. Avoiding titanium exposure could alleviate the symptoms of YNS [103]. The prognosis of YNS in children is not known [104].
Key Points
-
Beau’s lines and onychomadesis occur in 30% of children with hand, foot and mouth disease, within 2 months after the infection.
-
Yellow nail syndrome is an extremely rare disorder in children, although severe. It may be related to titanium absorption from candies and toothpastes.
Abbreviations
- HFMD:
-
Hand, foot and mouth disease
- LM:
-
Longitudinal melanonychia
- NAPSI:
-
Nail Psoriasis Severity Index
- NMN:
-
Nail matrix nevius
- NPS:
-
Nail-patella syndrome
- PASI:
-
Psoriasis Area Severity Index
- PC:
-
Pachyonychia congenita
- SE:
-
Subungual exostosis
- YNS:
-
Yellow nail syndrome
References
Richert B, André J. Nail disorders in children: diagnosis and management. Am J Clin Dermatol. 2011;12(2):101–12.
de Berker D. Childhood nail diseases. Dermatol Clin. 2006;24(3):355–63.
Iglesias A, Tamayo L, Sosa-de-Martínez C, Durán-McKinster C, Orozco-Covarrubias L, Ruiz-Maldonado R. Prevalence and nature of nail alterations in pediatric patients. Pediatr Dermatol. 2001;18(2):107–9.
Sarifakioglu E, Yilmaz AE, Gorpelioglu C. Nail alterations in 250 infant patients: a clinical study. J Eur Acad Dermatol Venereol. 2008;22(6):741–4.
Sobjanek M, Michajłowski I, Konczalska M, Włodarkiewicz A, Roszkiewicz J. Childhood nail alterations in Polish population. Acta Dermatovenerol Croat. 2012;20(2):95–7.
Tasia M, Lecerf P, Richert B, André J. Paediatric nail consultation in an academic centre in Belgium: a 10-year retrospective study. J Eur Acad Dermatol Venereol. 2019;33(9):1800–5.
Starace M, Alessandrini A, Piraccini BM. Nail disorders in children. Skin Appendage Disord. 2018;4(4):217–29.
Chinazzo M, Lorette G, Baran R, Finon A, Saliba É, Maruani A. Nail features in healthy term newborns: a single-centre observational study of 52 cases. J Eur Acad Dermatol Venereol. 2017;31(2):371–5.
Walker J, Baran R, Vélez N, Jellinek N. Koilonychia: an update on pathophysiology, differential diagnosis and clinical relevance. J Eur Acad Dermatol Venereol. 2016;30(11):1985–91.
Catalfo P, Musumeci ML, Lacarrubba F, Dinotta F, Micali G. Congenital malalignment of the great toenails: a review. Skin Appendage Disord. 2018;4(4):230–5.
Decker A, Scher RK, Avarbock A. Acquired congenital malalignment of the great toenails. Skin Appendage Disord. 2016;1(3):147–9.
Lipner SR, Scher RK. Congenital malalignment of the great toenails with acute paronychia. Pediatr Dermatol. 2016;33(5):e288–9.
Ko D, Lipner S. Congenital malalignment of the great toenail. J Cutan Med Surg. 2018;22(3):326.
Wang CY, Kern J, Howard A. Late-onset malalignment of the great toenails. Australas J Dermatol. 2019;60(4):315–7.
Baran R, Haneke E. Etiology and treatment of nail malalignment. Dermatol Surg. 1998;24(7):719–21.
Domínguez-Cherit J, García-Galaviz R, Gatica-Torres M. Successful surgical treatment of bilateral congenital malalignment of the great toenail and hypertrophic lateral nail folds. Dermatol Surg. 2019;45(9):1211–3.
DeKlotz CMC, Schwartz ME, Milstone LM. Nail removal in pachyonychia congenita: patient-reported survey outcomes. J Am Acad Dermatol. 2017;76(5):990–2.
Samuelov L, Smith FJD, Hansen CD, Sprecher E. Revisiting pachyonychia congenita: a case-cohort study of 815 patients. Br J Dermatol. 2020;182(3):738–46.
Shah S, Boen M, Kenner-Bell B, Schwartz M, Rademaker A, Paller AS. Pachyonychia congenita in pediatric patients: natural history, features, and impact. JAMA Dermatol. 2014;150(2):146–53.
Stewart CL, Takeshita J, Hansen CD, Rubin AI. The histopathological features of the nail plate in pachyonychia congenita. J Cutan Pathol. 2020;47(4):357–62.
Ghoumid J, Petit F, Holder-Espinasse M, et al. Nail-Patella Syndrome: clinical and molecular data in 55 families raising the hypothesis of a genetic heterogeneity. Eur J Hum Genet. 2016;24(1):44–50.
Harita Y, Kitanaka S, Isojima T, Ashida A, Hattori M. Spectrum of LMX1B mutations: from nail-patella syndrome to isolated nephropathy. Pediatr Nephrol. 2017;32(10):1845–50.
Price A, Cervantes J, Lindsey S, Aickara D, Hu S. Nail-patella syndrome: clinical clues for making the diagnosis. Cutis. 2018;101(2):126–9.
Jones MC, Topol SE, Rueda M, Oliveira G, Phillips T, Spencer EG, Torkamani A. Mutation of WIF1: a potential novel cause of a Nail-Patella-like disorder. Genet Med. 2017;19(10):1179–83.
Figueroa-Silva O, Vicente A, Agudo A, et al. Nail-patella syndrome: report of 11 pediatric cases. J Eur Acad Dermatol Venereol. 2016;30(9):1614–7.
Neri I, Piccolo V, Balestri R, Piraccini BM, Patrizi A. Median nail damage in nail-patella syndrome associated with triangular lunulae. Br J Dermatol. 2015;173(6):1559–61.
Sterling JC, Gibbs S, Haque Hussain SS, Mohd Mustapa MF, Handfield-Jones SE. British association of dermatologists’ guidelines for the management of cutaneous warts 2014. Br J Dermatol. 2014;171(4):696–712.
Park HK, Kim JS. Factors contributing to the treatment duration of diphenylcyclopropenone immunotherapy for periungual warts. Dermatol Ther. 2016;29(2):114–9.
Jakhar D, Kaur I, Misri R. Intralesional vitamin D3 in periungual warts. J Am Acad Dermatol. 2019;80(5):e111–2.
Padilla España L, Del Boz J, Fernández Morano T, Arenas-Villafranca J, de Troya M. Successful treatment of periungual warts with topical cidofovir. Dermatol Ther. 2014;27(6):337–42.
Giacaman A, Granger C, Aladren S, et al. Use of topical nitric-zinc complex solution to treat palmoplantar and periungual warts in a pediatric population. Dermatol Ther (Heidelberg). 2019;9(4):755–60.
Suh JH, Lee SK, Kim MS, Lee UH. Efficacy of bleomycin application on periungual warts after treatment with ablative carbon dioxide fractional laser: a pilot study. J Dermatolog Treat. 2020;31(4):410–4.
Wu L, Chen W, Su J, et al. Efficacy of the combination of superficial shaving with photodynamic therapy for recalcitrant periungual warts. Photodiagn Photodyn Ther. 2019;27:340–4.
Chinazzo M, Desoubeaux G, Leducq S, et al. Prevalence of nail scabies: a French prospective multicenter study. J Pediatr. 2018;197:154–7.
Finon A, Desoubeaux G, Nadal M, Georgescou G, Baran R, Maruani A. Scabies of the nail unit in an infant. Ann Dermatol Venereol. 2017;144(5):356–61.
Sechi A, Chessa MA, Patrizi A, Savoia F, Neri I. Periungual scabies in infants: a tough reservoir of mites presenting with lamellar desquamation. Arch Dis Child. 2020;105(7):703.
Grome L, Borah G. Neonatal Acute Paronychia. Hand (N Y). 2017;12(5):NP99–NP100.
Solís-Arias MP, García-Romero MT. Onychomycosis in children. A review. Int J Dermatol. 2017;56(2):123–30.
Totri CR, Feldstein S, Admani S, Friedlander SF, Eichenfield LF. Epidemiologic analysis of onychomycosis in the San Diego pediatric population. Pediatr Dermatol. 2017;34(1):46–9.
Wlodek C, Trickey A, de Berker D, Johnson E. Trends in pediatric laboratory-diagnosed onychomycosis between 2006 and 2014 in the southwest of England. Pediatr Dermatol. 2016;33(6):e358–9.
Gupta AK, Versteeg SG. Tavaborole - a treatment for onychomycosis of the toenails. Expert Rev Clin Pharmacol. 2016;9(9):1145–52.
Feldstein S, Totri C, Friedlander SF. Antifungal therapy for onychomycosis in children. Clin Dermatol. 2015;33(3):333–9.
Eichenfield LF, Friedlander SF. Pediatric onychomycosis: the emerging role of topical therapy. J Drugs Dermatol. 2017;16(2):105–9.
Rich P, Spellman M, Purohit V, Zang C, Crook TJ. Tavaborole 5% topical solution for the treatment of toenail onychomycosis in pediatric patients: results from a phase 4 open-label study. J Drugs Dermatol. 2019;18(2):190–5.
Patel D, Castelo-Soccio LA, Rubin AI, Streicher JL. Laboratory monitoring during systemic terbinafine therapy for pediatric onychomycosis. JAMA Dermatol. 2017;153(12):1326–7.
Goettmann S, Zaraa I, Moulonguet I. Nail lichen planus: epidemiological, clinical, pathological, therapeutic and prognosis study of 67 cases. J Eur Acad Dermatol Venereol. 2012;26(10):1304–9.
Chiheb S, Haim H, Ouakkadi A, Benchikhi H. Clinical characteristics of nail lichen planus and follow-up: a descriptive study of 20 patients. Ann Dermatol Venereol. 2015;142(1):21–5.
Pandhi D, Singal A, Bhattacharya SN. Lichen planus in childhood: a series of 316 patients. Pediatr Dermatol. 2014;31(1):59–67.
Kim M, Jung HY, Eun YS, Cho BK, Park HJ. Nail lichen striatus: report of seven cases and review of the literature. Int J Dermatol. 2015;54(11):1255–60.
Iorizzo M, Rubin AI, Starace M. Nail lichen striatus: is dermoscopy useful for the diagnosis? Pediatr Dermatol. 2019;36(6):859–63.
Jacobsen AA, Tosti A. Trachyonychia and twenty-nail dystrophy: a comprehensive review and discussion of diagnostic accuracy. Skin Appendage Disord. 2016;2(1–2):7–13.
Kumar MG, Ciliberto H, Bayliss SJ. Long-term follow-up of pediatric trachyonychia. Pediatr Dermatol. 2015;32(2):198–200.
Park JM, Cho HH, Kim WJ, et al. Efficacy and safety of calcipotriol/betamethasone dipropionate ointment for the treatment of trachyonychia: an open-label study. Ann Dermatol. 2015;27(4):371–5.
Piraccini BM, Triantafyllopoulou I, Prevezas C, et al. Nail psoriasis in children: common or uncommon? Results from a 10-year double-center study. Skin Appendage Disord. 2015;1(1):43–8.
Pourchot D, Bodemer C, Phan A, et al. Nail psoriasis: a systematic evaluation in 313 children with psoriasis. Pediatr Dermatol. 2017;34(1):58–63.
Bronckers IMGJ, Bruins FM, van Geel MJ, et al. Nail involvement as a predictor of disease severity in paediatric psoriasis: follow-up data from the Dutch ChildCAPTURE registry. Acta Derm Venereol. 2019;99(2):152–7.
Choi JW, Kim BR, Seo E, Youn SW. Identification of nail features associated with psoriasis severity. J Dermatol. 2017;44(2):147–53.
Kelati A, Baybay H, Najdi A, Zinoune S, Mernissi FZ. Pediatric psoriasis: should we be concerned with comorbidity? Cross-sectional study. Pediatr Int. 2017;59(8):923–8.
Uber M, Carvalho VO, Abagge KT, Robl Imoto R, Werner B. Clinical features and nail clippings in 52 children with psoriasis. Pediatr Dermatol. 2018;35(2):202–7.
Liu WH, Lok J, Lau MS, et al. Mechanism and epidemiology of paediatric finger injuries at Prince of Wales Hospital in Hong Kong. Hong Kong Med J. 2015;21(3):237–42.
Satku M, Puhaindran ME, Chong AK. Characteristics of fingertip injuries in children in Singapore. Hand Surg. 2015;20(3):410–4.
Yorlets RR, Busa K, Eberlin KR, et al. Fingertip injuries in children: epidemiology, financial burden, and implications for prevention. Hand (N Y). 2017;12(4):342–7.
Weir Y. Fingertip injuries in children: a review of the literature. Emerg Nurse. 2018;26(3):17–20.
Sullivan MA, Cogan CJ, Adkinson JM. Pediatric hand injuries. Plast Surg Nurs. 2016;36(3):114–20.
Patel L. Management of simple nail bed lacerations and subungual hematomas in the emergency department. Pediatr Emerg Care. 2014;30(10):742–5.
Ramirez EG, Hoyt KS. Management of hand injuries: part II. Adv Emerg Nurs J. 2016;38(4):266–78.
Iorizzo M, Lipner S, Vlahovic TC. Nail dystrophy due to toe malposition in children. Eur J Pediatr. 2017;176(8):1089–91.
Winebrake JP, Grover K, Halteh P, Lipner SR. Pediatric onychophagia: a survey-based study of prevalence, etiologies, and co-morbidities. Am J Clin Dermatol. 2018;19(6):887–91.
Lynch SJ, Sears MR, Hancox RJ. Thumb-sucking, nail-biting, and atopic sensitization, asthma, and hay fever. Pediatrics. 2016;138(2):e20160443.
Magid M, Mennella C, Kuhn H, Stamu-O'Brien C, Kroumpouzos G. Onychophagia and onychotillomania can be effectively managed. J Am Acad Dermatol. 2017;77(5):e143–4.
Braun TL, Patel V, DeBord LC, Rosen T. A review of N-acetylcysteine in the treatment of grooming disorders. Int J Dermatol. 2019;58(4):502–10.
Sun D, Reziwan K, Wang J, et al. Auricular acupressure improves habit reversal treatment for nail biting. J Altern Complement Med. 2019;25(1):79–85.
Halteh P, Scher RK, Lipner SR. Onychotillomania: diagnosis and management. Am J Clin Dermatol. 2017;18(6):763–70.
Piraccini BM, Richert B, de Berker DA, et al. Retronychia in children, adolescents, and young adults: a case series. J Am Acad Dermatol. 2014;70(2):388–90.
Lencastre A, Iorizzo M, Caucanas M, et al. Topical steroids for the treatment of retronychia. J Eur Acad Dermatol Venereol. 2019;33(9):e320–2.
Laird ME, Lo Sicco KI, Rich P. Conservative treatment of retronychia: a retrospective study of 25 patients. Dermatol Surg. 2019;45(4):614–6.
Arica IE, Bostanci S, Koçyigit P, Arica DA. Clinical and sociodemographic characteristics of ingrown nails in children. J Am Podiatr Med Assoc. 2019;109(4):272–6.
Watabe A, Yamasaki K, Hashimoto A, Aiba S. Retrospective evaluation of conservative treatment for 140 ingrown toenails with a novel taping procedure. Acta Derm Venereol. 2015;95(7):822–5.
Shih YH, Huang CY, Lee CC, Lee WR. Nail brace application: a noninvasive treatment for ingrown nails in pediatric patients. Dermatol Surg. 2019;45(2):323–6.
Gera SK, Zaini DKH, Wang S, Abdul Rahaman SHB, Chia RF, Lim KBL. Ingrowing toenails in children and adolescents: is nail avulsion superior to nonoperative treatment? Singap Med J. 2019;60(2):94–6.
André MS, Caucanas M, André J, Richert B. Treatment of ingrowing toenails with phenol 88% or trichloroacetic acid 100%: a comparative, prospective, randomized, double-blind study. Dermatol Surg. 2018;44(5):645–50.
Livingston MH, Coriolano K, Jones SA. Nonrandomized assessment of ingrown toenails treated with excision of skinfold rather than toenail (NAILTEST): an observational study of the Vandenbos procedure. J Pediatr Surg. 2017;52(5):832–6.
Göktay F, Atış G, Güneş P, Macit B, Çelik NS, Gürdal KE. Subungual exostosis and subungual osteochondromas: a description of 25 cases. Int J Dermatol. 2018;57(7):872–81.
DaCambra MP, Gupta SK, Ferri-de-Barros F. Subungual exostosis of the toes: a systematic review. Clin Orthop Relat Res. 2014;472(4):1251–9.
Piccolo V, Russo T, Rezende LL, Argenziano G. Subungual exostosis in an 8-year-old child: clinical and dermoscopic description. An Bras Dermatol. 2019;94(2):233–5.
Nakamura Y, Maruyama H, Fujisawa Y, et al. Subungual exostosis with postoperative recurrence followed by spontaneous regression. J Dermatol. 2019;46(3):e86–7.
Piccolo V, Argenziano G, Alessandrini AM, Russo T, Starace M, Piraccini BM. Dermoscopy of subungual exostosis: a retrospective study of 10 patients. Dermatology. 2017;233(1):80–5.
Cooper C, Arva NC, Lee C, et al. A clinical, histopathologic, and outcome study of melanonychia striata in childhood. J Am Acad Dermatol. 2015;72(5):773–9.
Koga H. Dermoscopic evaluation of melanonychia. J Dermatol. 2017;44(5):515–7.
Ohn J, Choe YS, Mun JH. Dermoscopic features of nail matrix nevus (NMN) in adults and children: a comparative analysis. J Am Acad Dermatol. 2016;75(3):535–40.
Lee JH, Lim Y, Park JH, et al. Clinicopathologic features of 28 cases of nail matrix nevi (NMNs) in Asians: comparison between children and adults. J Am Acad Dermatol. 2018;78(3):479–89.
Khatri SS, Wang M, Harms KL, et al. Subungual atypical lentiginous melanocytic proliferations in children and adolescents: a clinicopathologic study. J Am Acad Dermatol. 2018;79(2):327–336.e2.
Ohn J, Jo G, Cho Y, Sheu SL, Cho KH, Mun JH. Assessment of a predictive scoring model for dermoscopy of subungual melanoma in situ. JAMA Dermatol. 2018;154(8):890–6.
Stefanaki C, Soura E, Sgouros D, et al. Nail matrix nevi in children: a prospective study. J Eur Acad Dermatol Venereol. 2020;34(4):e203–5.
Starace M, Alessandrini A, Brandi N, Piraccini BM. Use of nail dermoscopy in the M-management of melanonychia: review. Dermatol Pract Concept. 2019;9(1):38–43.
Tseng YT, Liang CW, Liau JY, et al. Longitudinal melanonychia: differences in etiology are associated with patient age at diagnosis. Dermatology. 2017;233(6):446–55.
Piraccini BM, Dika E, Fanti PA. Tips for diagnosis and treatment of nail pigmentation with practical algorithm. Dermatol Clin. 2015;33(2):185–95.
Delvaux C, Richert B, Lecerf P, André J. Onychopapillomas: a 68-case series to determine best surgical procedure and histologic sectioning. J Eur Acad Dermatol Venereol. 2018;32(11):2025–30.
Beggs S, Butala N, Heymann WR, Rubin AI. Onychopapilloma presenting as longitudinal erythronychia in an adolescent. Pediatr Dermatol. 2015;32(4):e173–4.
Hardin J, Haber RM. Onychomadesis: literature review. Br J Dermatol. 2015;172(3):592–6.
Long DL, Zhu SY, Li CZ, Chen CY, Du WT, Wang X. Late-onset nail changes associated with hand, foot, and mouth disease: a clinical analysis of 56 cases. Pediatr Dermatol. 2016;33(4):424–8.
Nag SS, Dutta A, Mandal RK. Delayed cutaneous findings of hand, foot, and mouth disease. Indian Pediatr. 2016;53(1):42–4.
Hsu TY, Lin CC, Lee MD, Chang BP, Tsai JD. Titanium dioxide in toothpaste causing yellow nail syndrome. Pediatrics. 2017;139(1):e20160546.
Dessart P, Deries X, Guérin-Moreau M, Troussier F, Martin L. Yellow nail syndrome: two pediatric case reports. Ann Dermatol Venereol. 2014;141(10):611–9.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Tasia, M., Richert, B. (2021). What’s New in Pediatric Nail Disorders?. In: Baran, R.L. (eds) Advances in Nail Disease and Management. Updates in Clinical Dermatology. Springer, Cham. https://doi.org/10.1007/978-3-030-59997-3_14
Download citation
DOI: https://doi.org/10.1007/978-3-030-59997-3_14
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-59996-6
Online ISBN: 978-3-030-59997-3
eBook Packages: MedicineMedicine (R0)