Abstract
Background
Subungual exostosis is a relatively common benign bone tumor that occurs in the distal phalanges of the toes and can be a source of pain and nail deformity. There is controversy about the treatment of these lesions and there are few studies that have synthesized what is known and provided meaningful information on treatment.
Questions/purposes
We performed a systematic review to address the following questions: (1) What is the best surgical approach for excising these lesions? (2) What is the age range, sex distribution, and presenting symptoms of subungual exostoses and which toe is most frequently affected? (3) What complications arise from treatment?
Methods
Two authors independently searched multiple databases (Medline, 1950–May 2013; Cochrane EBM database, and EMBASE, 1980–May 2013 provided by OVID; ACP Journal Club, 2003–May 2013; CINAHL by EBSCO, 1937–May 2013; and PubMed by NLM, 1940–May 2013), and key words were chosen to achieve a broad search strategy. We included studies on the management of toe exostoses with > 10 cases and we excluded studies that reported on upper extremity exostoses or osteochondromas. Demographic and treatment data were collected from each article by two independent authors and collated. A total of 124 abstracts were screened, and 116 articles were reviewed in full, of which 13 met the inclusion criteria.
Results
Complete marginal excision through a fish mouth incision protecting the nail led to a recurrence rate of 4% and satisfactory clinical results, defined as no requirement for postoperative intervention and a satisfactory clinical appearance in 73%. Most studies provided incomplete descriptions of specific surgical techniques used. Fifty-five percent of the patients were younger than 18 years of age. A history of toe trauma before diagnosis was present in approximately 30% of the cases. Delayed diagnosis occurred in approximately 10% of the cases and onychodystrophy occurred in more than 10%.
Conclusions
There is weak evidence to guide management of subungual exostosis. Adequate wound management postexcision aiming to minimize disruption to the nail bed and matrix may prevent onychodystrophy, which is a common complication of treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Subungual exostosis is a relatively uncommon, osteocartilaginous tumor that affects the distal phalanx of the toes or fingers [2, 5, 12, 24] (Fig. 1). This benign lesion has also been reported as part of multiple hereditary exostoses [1, 24, 28, 32]. Dupuytren described in 1817 a bony growth of the distal phalanx of the great toe that became known as “Dupuytren’s exostosis.” The exact pathogenesis of subungual exostosis is unclear, although trauma, infection, tumor, hereditary abnormality, or activation of a cartilaginous cyst all have been suggested as possible etiologies of subungual exostosis. Most consider it to be a reactive metaplasia resulting from microtrauma [3, 33, 35]; however, there is no conclusive evidence to support a single pathogenesis [14, 32, 34]. There is debate whether subungual osteochondroma is the same clinical entity as subungual exostosis. Histologically, the cartilaginous cap of exostoses is made of fibrocartilage, whereas in osteochondromas, it is hyaline cartilage and is confluent with the underlying trabecular and cortical bone [16, 25] (Fig. 2). In exostoses, bone is formed directly from fibrous tissue, whereas in conventional osteochondromas, it is derived from enchondral ossification [12, 16, 24]. The translocation t(X;6)(q22;q13-14) has been reproducibly linked to subungual exostosis [7, 33], implying it is a true neoplasm instead of being a reactive process in response to trauma. Other lesions of the bone surface such as bizarre parosteal osteochondromatous proliferation (BPOP or Nora lesion), once thought to be a related proliferative process to subungual exostoses, have unique chromosomal rearrangements and represent a distinct molecular pathogenesis [33].
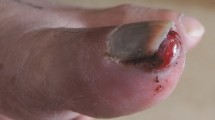
Clinical photographs and radiographs of the same subungual exostosis in the right hallux of a 15-year-old girl presenting with pain and an enlarging mass for 3 months. (A) Dorsal and (B) medial clinical photographs and (C) posterior-anterior and (D) lateral radiographs of the same lesion. Reproduced with permission from BMJ Case Reports [6].
Light microscopic image of a histological specimen taken intraoperatively from the great toe of a 15-year-old girl. It shows dermal tissue with normal trabecular bone and fibrocartilaginous overgrowth, consistent with subungual exostosis. Reproduced with permission from BMJ Case Reports [6].
The most common clinical presentation is that of several months of pain, erythema, and deformity of the nail bed [8, 12, 33, 38], which cause a deleterious impact on health-related quality of life [8, 36]. Examination usually reveals a firm, fixed nodule with a hyperkeratotic smooth surface at the distal end of the nail plate. Because misdiagnosis and delayed diagnosis of this lesion are common, appropriate treatment often is not rendered [31, 37]. Radiographs show a pedunculated radioopaque mass on the dorsomedial surface of the distal phalanx. The role of nonoperative management is limited because the condition is generally progressive. The mainstay of treatment has been marginal surgical excision of the exostosis, which typically alleviates the symptoms [25–27]. However, surgical techniques have varied [2, 11, 17, 33], and the most recent literature review on this topic was published by Davis and Cohen in 1996 [8]. The hypothesis is that complete marginal excision with minimal trauma to the nail bed results in the fewest recurrences and optimal cosmesis.
We therefore sought to do a systematic review of the literature to address the following questions: (1) What is the best surgical approach for excising these lesions? (2) What is the age range, sex distribution, and presenting symptoms of subungual exostoses and which toe is most frequently affected? (3) What complications arise from treatment?
Search Strategy and Criteria
We performed the literature search in Medline (1950–May 2013), Cochrane EBM database, and EMBASE (1980–May 2013) provided by OVID; ACP Journal Club (2003–May 2013); CINAHL by EBSCO (1937–May 2013); and PubMed by NLM (1940–May 2013). We used the search terms “subungual exostoses/exostosis”, “toe exostoses/exostosis”, and “subungual osteochondroma”, and we limited our search to human populations. The review was limited to English, French, and Spanish languages. Two authors (MPD, SKG) independently reviewed the abstracts according to predetermined inclusion criteria. Disagreement about inclusion was resolved by consensus with input from the senior author (FFB).
We included studies of diverse designs that reported treatment outcomes for toe exostoses, which comprised 10 or more patients, and excluded case reports and small case series. Two authors (MPD, SKG) independently reviewed the full-text articles (and their respective references) for those that met our inclusion criteria. We graded the articles according to levels of evidence as depicted by Wright et al. [39, 40] and used PRISMA (Preferred Reporting Items for Systematic reviews and Meta-Analyses) guidelines for relevance as determined by Liberati et al. [22].
One of the authors (MPD) collected demographic and treatment data and collated in an Excel spreadsheet (Microsoft Inc, Redmond, WA, USA). All authors contributed to final data analysis and writing of the article.
One hundred twenty-four abstracts were initially identified and screened. Eight articles were excluded because they addressed only upper extremity exostoses or osteochondromas. The remaining 116 full-text articles were reviewed and 13 studies met our inclusion criteria, which were all Level IV retrospective case series comprising 10 or more patients. No experimental or quasiexperimental studies were identified (Fig. 3).
The total number of reported cases in the 13 included studies was 287. A wide variety of medical journals reported on subungual exostosis, suggesting that physicians of diverse specialties have managed this condition. Dermatology journals published 25% of all articles followed by orthopaedics (19%), foot/ankle (13%), and others (44%). Eleven (85%) articles were published in English (Table 1).
Results
Specific operative and nonoperative strategies varied widely and no article compared one technique with another. Histological characterization was mentioned in most of the articles but details regarding tissue preparation, fixation techniques, and staining methods were only included in one [10]. The most successful principles involved curettage, burr, or ronguer débridement down to the base of the stalk to avoid recurrence, with preservation of the nail bed when possible.
Fifty-five percent of the patients were younger than 18 years of age. The female:male ratio was approximately equal (146:143). The average age at the time of presentation was 25.7 years. The hallux was the most common location of the exostoses (204 of 255 [80%]) followed by the second toe (16 of 255 [6%]), third toe (17 of 255 [7%]), fourth toe (12 of 255 [5%]), and the fifth toe (six of 255 [2%]) (Fig. 4). Pain was the most common complaint (193 of 250 [77%]) followed by mass/swelling in the nail (77 of 250 [31%]), nail change (38 of 250 [15%]), or other complaints such as shoe wear rubbing or stiffness (eight of 250 [3%]) (Table 2). With respect to the history at presentation, the duration of symptoms ranged widely from 2 to 48 months. A history of toe trauma before diagnosis was present in 46 of 160 (29%) documented cases, and a history of previous infection was noted in 21 of 153 (14%) documented cases. There were no reported cases of positive family history or malignant degeneration of the lesion (Table 2). Only those articles reporting antecedent conditions were included in these percentages.
The most prevalent complication was onychodystrophy (malformation or discoloration of the nail), which occurred in 20 of 124 (16.1%) of cases. Strategies aiming to minimize trauma to the nail bed yielded better cosmetic results, mitigating the incidence of onycholysis (loosening or separation of the nail from its bed). A missed, incorrect, or delayed diagnosis occurred in three of 124 (2%) of cases. For all treatments reviewed, recurrence occurred in five of 124 (4.0%) cases, and postoperative infections occurred in four of 124 (3.2%). Other complications such as chronic regional pain syndrome occurred in one of 124 (0.8%) (Table 2). Not all articles reported complications and only those reporting them specifically were included in these percentages.
Discussion
Subungual exostoses are relatively uncommon in both the general and pediatric orthopaedic populations. Currently there is a paucity of evidence to define the demographics of this group and to guide management. Most reports on this topic are case series and the most recent attempt at a systematic review is more than 15 years old [8]. The current study extends the scope of that review by including numerous cases reported on since that time and providing a more robust consensus of both the complication profile and successful surgical strategies. This systematic review sought to identify the best treatment approaches, the demographics and common presentations of subungual exostosis, and the complications arising from treatment.
The main limitation of this review is that it is based on a series of Level IV studies, each containing different treatment methodologies and result parameters. This is the result of the fact that the condition is uncommon; thus, designing experimental research comparing different treatment options is a challenge. The synthesis of current literature provided here does, however, establish the demographics and optimal treatment strategies on this topic, which is relatively underrepresented in the orthopaedic literature.
We found from our review that the principle of treatment is to achieve complete excision of the lesion by curetting or burring down to normal trabecular bone while minimizing deformity to the nail plate (Fig. 5). This approach seemed to lead to the lowest incidence of recurrence. De Berker and Langtry [9] described the use of a ronguer to adequately resect lesional tissue, whereas Davis and Cohen [8] used a curette to create a “saucer-like defect” into normal trabecular bone. Suga and Mukouda [34] introduced the idea that if the nail bed was intact, a fish mouth incision distally with a proximally based flap could be raised lifting the nail bed off of the lesion, thus sparing the nail. If the lesion invaded the nail bed, however, a direct dorsal approach should be used (Fig. 5) because the nail bed is already compromised and the priority should be shifted to complete lesional excision. Lokiec et al. [23] showed in his six-patient series that reasonable results in terms of recurrence and cosmesis can be achieved with only partial nail resection using a distally based flap, which is reattached. Recurrence was related to incomplete excision in most described cases; however, overly aggressive dissection was thought to lead to onychodsytrophy and poor cosmesis [8, 9, 33, 34], particularly when the lesion invaded the germinal matrix [9]. In the single podiatric article included in the study, Valinsky et al. [37] used local anesthesia, a laterally based incision, and a single application of intralesional corticosteroid and antibiotics. There is no mention, however, of results or complications.
Intraoperative images of a marginal excision of subungual exostosis of the great toe in a 15-year-old girl. (A) The lesion invaded the nail bed, which was not salvageable; thus, a direct dorsal exostectomy was performed. (B) The osteocartilaginous lesion was marginally resected and the base of the stalk was curetted, ronguered, and burred down creating a “saucer-like defect.” The sample was sent for pathological analysis and found to be consistent with subungual exostosis. Reproduced with permission from BMJ Case Reports [6].
Although multiple specific surgical techniques and postoperative wound closure strategies have been reported [6, 8, 9, 23, 34, 37], as a result of a lack of comparative analyses, no one technique has significant evidence to show its superiority. The principle, however, of a balance between complete lesional excision and delicate separation from underlying nail bed structures is the most important factor in mitigating recurrence and nail problems.
Our review has shown some similarities as well as some differences as compared with previous reviews with respect to the epidemiology of subungual exostoses of the toes. The average age of onset of 26 years and the preponderance for the great toe (80%) corroborate with numbers published previously [8, 33, 34]. Conversely, we found that there is a much higher proportion of cases in the pediatric population (55%), and the female:male ratio is closer to 1:1 (compared with 16% and 2:1, respectively, as reported by Davis and Cohen [8]). Also, this review finds that the association with previous trauma or infection is high (29% and 14%, respectively). Although Fikry et al. [13] showed a relationship to previous trauma in 21 of 28 (75%), the remainder of the studies reporting on this was much lower. Similarly, Landon et al. [18] showed prior infection was observed in 15 of 39 (38%), but multiple others showed very little correlation (Table 2). The differences in our results compared with the next most recent review by Davis and Cohen in 1996 [8] are likely attributable to the fact that five of 13 of the articles that met our comprehensive inclusion criteria have been published since the Davis and Cohen study, representing a more recent summary of the current literature.
The complication profile presented in this review shows that important, potentially avoidable morbidity is associated with the treatment of subungual exostosis, including postsurgical deformity (16%), recurrence (4%), and delayed diagnosis (2%). Although the complication of postsurgical nail deformity is related to the size and location of the lesion at presentation, meticulous surgical technique and wound closure can minimize deformity [9, 19, 33]. Although the actual rate of defined “delayed diagnosis” was found to be only 2%, this number is likely much higher. This can be inferred from the duration of symptoms ranging in many cases well beyond 6 months and up to many years (Table 2). Delayed diagnosis probably stems from the wide differential diagnosis, the broad spectrum of health practitioners from whom patients first seek care, the requirement for appropriate pathological analysis, and the lack of experience of some of those providers in clinically recognizing and managing these relatively rare conditions. Radiographs of the involved toe play an important role in making the differential diagnosis. The recurrence rate likely is a result of incomplete surgical excision. Some authors describe no onycholysis even after they excised a portion of the nail bed through a fish mouth incision and allowed the wound to close secondarily. This seems counterintuitive but may represent the fact that the healing potential is greater in skeletally immature individuals as long as the germinal matrix is maintained. Suga and Mukouda [34] suggest that in the case in which the lesion creates a significant nail bed defect, you can either allow the defect to heal spontaneously or augment the wound with artificial skin and allow it to epithelialize. Recently, DaCambra et al. [6] suggested a novel method of wound management using a vacuum-assisted closure device to promote faster healing with good results. With this variability of management, onycholysis remains an important complication, which can be mitigated with preservation of the nail bed and germinal matrix.
In conclusion, there is weak evidence to guide management of subungual exostosis, a condition that has a relatively high complication rate and which affects children and adults. This topic is underrepresented in the orthopaedic literature, because many of the important clinical series have been published in journals from other specialties [4, 8, 9, 12, 15, 20, 21, 29, 30, 33, 34, 41], reflecting the fact that the condition is treated by many kinds of nonorthopaedic providers. Complete marginal excision of the exostosis appears to mitigate recurrence. Adequate wound management postexcision aiming to minimize disruption to the nail bed and matrix may prevent onychodystrophy, which is a common complication of treatment. Further empirical research is required to compare the outcomes of diverse strategies for wound management postexostosis resection.
References
Baran R, Bureau H. Multiple exostoses syndrome. J Am Acad Dermatol. 1991;25:333–335.
Bendl B. Subungual exostosis. Cutis. 1980;26:260.
Bervar M. [Subungual exostosis of the toe and its etiology] [in Serbian]. Vojnosanit Pregl. 1958;15:452–455.
Bostanci S, Ekmekçi P, Ekinci C, Akçaboy B, Gürgey E. Subungual osteochondroma: a case report. Dermatol Surg. 2001;27:591–593.
Cohen HJ, Frank SB, Minkin W, Gibbs RC. Subungual exostoses. Arch Dermatol. 1973;107:431.
DaCambra MP, Gupta SK, Ferri-de-Barros F. A novel management strategy for subungual exostosis. BMJ Case Rep. 2013 Aug 30;2013. pii: bcr2013200396. doi: 10.1136/bcr-2013-200396.
Dal Cin P, Pauwels P, Poldermans LJ, Sciot R, Van den Berghe H. Clonal chromosome abnormalities in a so-called Dupuytren’s subungual exostosis. Genes Chromosomes Cancer. 1999;24:162–164.
Davis D, Cohen P. Subungual exostosis: case report and review of the literature. Pediatr Dermatol. 1996;13:212–218.
De Berker D, Langtry J. Treatment of subungual exostoses by elective day case surgery. Br J Dermatol. 1999;140:915–918.
De Palma L, Gigante A, Specchia N. Subungual exostosis of the foot. Foot Ankle Int. 1996;17:758–63.
DiCenso A, Bayley L, Haynes RB. Accessing pre-appraised evidence: fine-tuning the 5S model into a 6S model. Evid Based Nurs. 2009;12:99–101.
Evison G, Price CH. Subungual exostosis. Br J Radiol. 1966;39:451–455.
Fikry T, Dkhissi M, Harfaoui A, Adil A, Haddoun A, Zryouil B. Subungual exostosis: a retrospective study of 28 cases. Acta Orthop Belg. 1998;64:35–40.
Grisafi PJ, Lombardi CM, Sciarrino AL, Rainer GF, Buffone WF. Three select subungual pathologies: subungual exostosis, subungual osteochondroma, and subungual hematoma. Clin Podiatr Med Surg. 1989;6:355–364.
Guarneri C, Guarneri F, Risitano G, Lentini M, Vaccaro M. Solitary asymptomatic nodule of the great toe. Int J Dermatol. 2005;44:245–247.
Ippolito E, Falez F, Tudisco C, Balus L, Fazio M, Morrone A. Subungual exostosis. Histological and clinical considerations on 30 cases. Ital J Orthop Traumatol. 1987;13:81–87.
Kim S, Park K, Son S. Subungual osteochondroma presenting as verruca vulgaris in a 6-year-old boy. Pediatr Dermatol. 2007;24:584–585.
Landon GC, Johnson KA, Dahlin DC. Subungual exostoses. J Bone Joint Surg Am. 1979;61:256–259.
Lee SK, Jung MS, Lee YH, Gong HS, Kim JK, Baek GH. Two distinctive subungual pathologies: subungual exostosis and subungual osteochondroma. Foot Ankle Int. 2007;28:595–601.
Letts M, Davidson D, Nizalik E. Subungual exostosis: diagnosis and treatment in children. J Trauma Acute Care Surg. 1998;44:346–349.
Li Y, Yue T, Han Y. Subungual exostosis. 1991;6:169–171.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JPA, Clarke M, Devereaux PJ, Kleijnen J, Moher D. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700–b2700.
Lokiec F, Ezra E, Krasin E, Keret D, Wientroub S. A simple and efficient surgical technique for subungual exostosis. J Pediatr Orthop. 2001;21:76.
Mavrogenis A, Papagelopoulos P, Soucacos P. Skeletal osteochondromas revisited. Orthopedics. 2008;31:1018–1028.
Mertens F, Möller E, Mandahl N, Picci P, Perez-Atayde AR, Samson I, Sciot R, Debiec-Rychter M. The t(X;6) in subungual exostosis results in transcriptional deregulation of the gene for insulin receptor substrate 4. Int J Cancer. 2011;128:487–491.
Miller-Breslow A, Dorfman H. Dupuytren’s (subungual) exostosis. Am J Surg Pathol. 1988;12:368.
Multhopp-Stephens H, Walling A. Subungual (Dupuytren’s) exostosis. J Pediatr Orthop. 1995;15:582.
Murphey MD, Choi JJ, Kransdorf MJ, Flemming DJ, Gannon FH. Imaging of osteochondroma: variants and complications with radiologic-pathologic correlation. Radiographics. 2000;20:1407–1434.
Oliveira AS, Picoto AS, Verde SF, Martins O. Subungual exostosis: treatment as an office procedure. J Dermatol Surg Oncol. 1980;6:555–558.
Ortega ORM, Sanchez HG. 23 observations of subungual exostosis. Med Cut ILA. 1988;16:11–14.
Smith LC, Funkhouser WK, Campion ER, Morrell DS. A firm nodule on the great toe of a 13-year-old boy. Pediatr Dermatol. 2009;26:747–748.
Stark JD, Adler NN, Robinson WH. Hereditary multiple exostoses. Radiology. 1952;59:212–215.
Storlazzi C, Wozniak A, Panagopoulos I, Sciot R, Mandahl N, Mertens F, Debiec-Rychter M. Rearrangement of the COL12A1 and COL4A5 genes in subungual exostosis: molecular cytogenetic delineation of the tumor-specific translocationt (X; 6)(q13-14; q22). Int J Cancer. 2006;118:1972–1976.
Suga H, Mukouda M. Subungual exostosis. Ann Plast Surg. 2005;55:272–275.
Toyoda M, Morohashi M. An ultrastructural study of subungual exostosis, with specila reference to intranuclear inclusions. Medical Electron Microscopy. 1998;31:142–146.
Tuzuner T, Kavak A, Ustundag N, Parlak A. A painful subungual nodule: subungual exostosis. Acta Orthop Traumatol Turc. 2004;38:71.
Valinsky MS, Hettinger DF, Gennet PM. Subungual exostosis removal utilizing a minimal incision technique. Curr Podiatr Med. 1991;40:10–15.
Webber J, Miller M. Subungual exostosis in a young woman. Pathology. 1994;26:339–341.
Wright JG, Kocher MS, Sanders JO. Evidence-based pediatric orthopaedics: an introduction, Part I. J Pediatr Orthop. 2012;32:S83–S90.
Wright JG, Swiontkowski MF, Heckman JD. Introducing levels of evidence to the journal. J Bone Joint Surg Am. 2003;85:1–3.
Zambrano E, Nosé V, Perez-Atayde A, Gebhardt M, Hresko MT, Kleinman P, Richkind KE, Kozakewich HP. Distinct chromosomal rearrangements in subungual (Dupuytren) exostosis and bizarre parosteal osteochondromatous proliferation (Nora lesion). Am J Surg Pathol. 2004;28:1033.
Author information
Authors and Affiliations
Corresponding author
Additional information
Each author certifies that he or she, or a member of his or her immediate family, has no funding or commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
All ICMJE Conflict of Interest Forms for authors and Clinical Orthopaedics and Related Research editors and board members are on file with the publication and can be viewed on request.
This work was performed at the Alberta Children’s Hospital, Calgary, Alberta, Canada.
About this article
Cite this article
DaCambra, M.P., Gupta, S.K. & Ferri-de-Barros, F. Subungual Exostosis of the Toes: A Systematic Review. Clin Orthop Relat Res 472, 1251–1259 (2014). https://doi.org/10.1007/s11999-013-3345-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-013-3345-4