Abstract
Gastroesophageal reflux disease (GERD) affects 20–30% of the population and impairs the life quality due to the symptoms and cancer risk in those with Barrett’s esophagus (BE). Due to the anatomical properties of the esophagus, GERD causes a large spectrum of symptoms including heartburn, wheezing, coughing, burning throat, nose, ears, and eyes. Here, we propose a novel multidisciplinary GERD and BE management to eliminate the two major causes for GERD-induced impairment of the life quality: symptoms and cancer risk. In addition, GERD-related management is related to the perspective of an ancient Greek concept of reasoning, as coined by Hesiod and others. Finally, the chapter may motivate a positive and cause-related management of GERD and BE.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
14.1 Introduction
Symptomatic gastroesophageal reflux disease (GERD) affects 20–30% of the population, and thus represents one of the most frequent disorders of the upper gastrointestinal tract [1,2,3]. Factors associated with GERD include heredity, age, and lifestyle (nutrition, obesity, eating disorders, drug consumption) [1,2,3]. GERD affects the life quality and the well-being due to the symptoms (heartburn, wheezing, cough, asthma) and the morphological consequences including an increased cancer risk for those with Barrett’s esophagus (BE) [4,5,6,7]. Economically, GERD matters as a frequent reason for sick leave [7]. In addition, diagnosis and therapy of GERD and BE foster the development of novel technologies [1, 2, 4, 5, 7]. This continues to entertain new promising niches for the industry and health-related economies. Furthermore, diagnosis and therapy of GERD and BE cause economic burdens for private and public health security systems [1, 7].
Due to the anatomical associations of the esophagus, reflux can affect the esophagus, ear, nose, throat (ENT), mouth, tongue, teeth, and the lungs. Therefore, GERD and BE management requires a multi- and interdisciplinary approach [1, 3, 7]. Accordingly, this book aims to summarize a novel understanding regarding the diagnosis, therapy, and follow up of patients with GERD and BE. The incidence and frequency of asymptomatic reflux without and with BE are not known. Individuals without symptoms do not seek medical care. However, the majority of those developing esophageal cancer lack a GERD symptom positive medical history. Here we aim to elucidate the current difficulties related to the diagnosis and therapy of GERD and BE, and how they could be overcome. Special attention addresses the question, in as much the translation and application of ancient wisdom contribute to improve GERD and BE management [8,9,10,11].
Our scientific journey follows the idea that histopathology represents a sensitive diagnostic marker for reflux, GERD, and BE management (diagnosis, therapy monitoring, follow up) [12,13,14,15,16,17,18,19,20,21]. In contrast to symptomatology, endoscopy, and function test data, histopathology assesses reflux at the cellular level (increases resolution) [12,13,14,15,16,17,18,19,20,21]. According to this concept, the presence of columnar-lined esophagus (CLE) with and without cancer risk (BE) serves as a marker for reflux (no CLE without reflux) [14,15,16,17,18,19,20,21]. Reflux is considered a disease in the presence of life quality impairing symptoms and cancer risk. As such cancer risk (BE) ± symptoms or symptoms with cancer risk (BE) negative CLE defines disease. Columnar-lined esophagus (CLE) without cancer risk (BE) and symptoms defines abnormality. Absence of any CLE defines normalcy. Disease requires therapy (lifestyle, medical, interventional). The finding of abnormality and normalcy translates into strategies for disease prevention (lifestyle measures).
14.2 Symptoms and Signs
Conceptually, disease management should focus on the cause. Since many years, GERD management is based on a complex mixture of symptoms, endoscopic information, histopathological findings, measures obtained during esophageal function test (manometry, reflux pH-monitoring), and radiological examinations [22,23,24,25,26,27,28]. As a consequence GERD has been described, categorized, and assessed, using terms, which fostered the impression of a complicated and confusing babylonian linguistic confusion. While the moon shades light on changes, the beautiful spectrum of classifications tours from Montreal to Rome, from Vienna to Los Angeles, from Chicago to Prague, and from there to Milan [22,23,24,25,26,27,28]. Through the internet, physicians and patients learned about nonerosive reflux disease (NERD), erosive reflux disease (ERD), gastroesophageal reflux disease (GERD), functional heartburn (HB), hypersensitive esophagus, normal Z-line, irregular Z-line, small and large hernias, tongues, island and segments of columnar-lined esophagus (CLE), endoscopic Barrett’s esophagus, confirmed Barrett’s esophagus, ultra-short Barrett’s esophagus; definitions for normal and abnormal manometry and reflux monitoring [2, 7, 21, 26]. The problem was that we were not allowed to know: what is normal? What defines normalcy? Is it the absence of any reflux? Is it the absence of any symptoms? Is it the absence of any CLE? Does the presence of CLE, BE without symptoms define a disease or an abnormal condition? Does it need the presence of symptom negative, but low- or high-grade dysplasia positive CLE to be recognized as a disease? Which measures define normal, physiologic reflux? How many symptoms per week, per month, per year define normalcy? How often do you have to perceive symptoms to be categorized as abnormal, as having a disease? What means the term “troublesome”? What defines a symptom to be categorized as “troublesome”? Which measures, numbers and values define the landmark, and the cutting edge between normal and abnormal and between physiologic and pathologic? At which point do GERD and CLE start to become a disease? Why did we get into trouble at all? What are the reasons for the above insecurities? It seems that our current conduct of reasoning hides ourselves from a suitable and reliable marker for the definition of GERD. It seems that our current approach towards GERD and BE prevents us from recognizing the most valuable and reproducible indicator for reflux, GERD, and BE.
14.3 GERD and Cellular Pathology
Going in line with Carl von Rokitansky (1804–1878) and Rudolf Ludwig Karl Virchow (1821–1902), cellular pathology and histopathology define a disease [21, 29, 30]. As such histopathology defines diseases of the liver, pancreas, kidneys, lungs, thyroids, adrenals, colon, intestine, prostate, bone, muscle, skin, nerves, and brain. Would there be the possibility for a histopathological definition of GERD? Does it need the development of low- and high-grade dysplasia and cancer to get recognized as a disease in those without symptoms (heartburn, regurgitation)?
Twenty years ago, the pathologist Para Chandrasoma and the surgeon Tom DeMeester critically revisited the criteria used for the definition of GERD and did what medicine used to do since the times of Rokitansky and Virchow: to base the diagnosis of a disease on cellular pathology, i.e., histopathology [12,13,14,15,16]. Their cautious search correlated the histopathology to the function of the esophagus and aimed to examine the qualities, which contributed to the orchestration of symptoms, signs, and cancer risk [12,13,14,15,16, 31, 32]. And the articles collected within this book nicely demonstrate, what happens, if you allow the use of histopathology for the definition of a disease: you receive an advantage. Going in line with the above statement, that something prevents us from recognizing the most valuable marker for GERD, we are led to a very old concept of reasoning. Within this concept, man recognized the world as a spectrum of hidden atmospheres and unhidden perceptions. You cannot see an atmosphere, but something you see may evoke a particular atmosphere (astonishment, excitement, happiness, humility). Atmosphere may contribute to focus your attention into a specific direction. Therefore, the legacy of our ancient Greek forefathers contains important relevance for the understanding of GERD and BE. In addition, it motivates to search for a common, underlying cause of any observation, perception, and phenomenon, i.e., GERD, NERD, BE, heartburn [7,8,9,10,11]. Now we are going to explore and investigate the relevance of this approach for a distinct understanding of GERD and BE.
14.4 Hesiod Unfolds GERD and BE
Most excitingly, the GERD story contains a lot of similarities that have been expressed within the Theogony of the ancient Greek thinker Hesiod (around 700 B.C.), where we are allowed to read [33]:
But hateful Strife bore painful Toil and
Forgetfulness and Famine and tearful Sorrows and
Discord
This fascinating “fragment,” this wonderful poetic biopsy points out the reason and the major consequences of a disease (for example, GERD): the cause for painful toil, tearful sorrows, and discord [33]. The list of terms including painful toil, tearful sorrows, and discord describes the ancient version of so-called somatic and psychosomatic symptoms. Most strikingly, Hesiod understood and explained the reasons for the symptoms: forgetfulness and famine. Furthermore, forgetfulness and famine originated within “hateful strife.” In ancient Greek, forgetfulness (lethe) and famine (limos) describe the qualities of a very old concept serving the understanding of phenomena [10, 11].
Briefly: forgetfulness, lethe, is the famine (limos) of memory (lack of memory); as such the limos, the deficiency, the hunger, the absence, the lack of something, equals the very cause of all phenomena [10, 11]. Limos, the deficiency, the lack of something represents the reason and prerequisite for all things that we can perceive (without the well-oriented and distributed lack of the white background color we could not read the words in this book) [8, 9]. The entire ancient Greek mythology, tragedy and epic poetry (Hesiod, Homer, Sophocles, Euripides, Aeschylus, Pindar, Anaximander, Heraclitus, Parmenides) explains the world as the manifestations of limos (hunger, deficiency, lack of something) and lack of memory (forgetfulness; lethe) [11]. According to the ancient Greek reasoning, lethe and limos orchestrate the background against which we are allowed to reason, think, and consider perceptions (i.e., esophagitis, Schatzki ring, esophageal cancer) [10, 11].
Lethe describes the hidden (i.e., lack, limos, of perception), the things we are not allowed to see, because they are hidden, away from our perception, behind another thing, etc. At this point we arrive at the central aspect of our understanding: if you unhide the lethe, you will get a-letheia, and this is the term which simply describes the truth! Aletheia unhides the term, that all philosophy and thinking is about [11]. The ancient Greek thinkers Anaximander, Heraclitus, and Parmenides contributed their lives to explore the relations between lethe and a-letheia [11]. As such we understand, how the ancient Greeks, our forefathers, spoke about truth: truth for them was the unhidden, the things they were allowed to perceive, see, assess, measure, and diagnose. But they understood, that trouble and insecurity arise from those thing, that we were not allowed to see, because they were hidden to us, hidden from our perception: lethe. And here we face the essence of the ancient Greek reasoning and mythology (= the collection of ancient knowledge). The interplay between lethe and a-letheia, the hidden and the perceivable, Shakespeare’s, Hamlet’s “to be or not to be,” unfolds the tension-rich playground for Greek philosophy, poetry, epic, and architecture [8,9,10,11]. Ancient Greece is all about lethe and a-letheia and therefore about existence and being. And the circuit of reasoning is closed by the understanding that lethe represents the deficiency, lack, limos of a-letheia [11].
Based on the above considerations, the essential character of all perceptions unfolds as a manifestation of limos. Since limos indicates “deficiency,” “lack of something” it seems justified to follow that any perception equals a form of “lack limos” [8, 9]. Phenomenologically shadow represents lack limos of light, silence represents lack limos of sound, secret means lack limos of information, absence mirrors lack limos of presence, disease equals lack limos of health, and a-letheia is lack limos of lethe [8,9,10,11]. The latter mirrors the “cellular pathology” of our being, existence, and atmosphere. Taken together, the term “lack limos” indicates “deficiency” and/or “the lack of something.” If all perceptions (GERD symptoms, diagnostic signs) represent a form of lack limos, we have to search for a possibility to overcome (theory) and compensate (praxis) this state of deficiency.
Fortunately, Hesiod describes a way to unhide the lack limos of information and replace it by unhidden knowledge: the muse. The term “muse” can be traced back to the levantine cultures (1500 B.C.) and describes the concept of strict order and discipline for achieving success. At the beginning of the theogony, Hesiod calls the muses to support his project [34]. Now you may ask: what the hell does Hesiod and these terms have in common with GERD? Did Hesiod suffer from GERD? Basically we do not know that, there exists no record regarding the medical history of Hesiod, although it can be assumed that Hesiod had an esophagus (Greek: oiso—carry, transport; phagein—the food; i.e., the transporter of the food) [35], that presumably also has been lined by columnar epithelium, at least to some extent. Thus, it may be justified to assume that Hesiod had at least quiet asymptomatic reflux. We will go back to it later.
The poetry of Hesiod motivates us to take a look at GERD, using a different perspective. We may question, in as much GERD translates into a collection (Greek: logos) of “lack limos” forms of deficiencies, of absences, of limos and lethe. And what about forgetfulness, the absence of memory, the lack of remembrance within the patient history and the medical community [8,9,10,11]? May it be that GERD and BE collect a broad spectrum of forms of deficiencies? A collection of forms of lack limos? Could it be that Hesiod (700 B.C.) had given a future outlook containing major relevance for our present time (2019 A.D.)? Are we caught back to our roots after a time span of 2719 years?
14.5 GERD as a Collection (Greek: Logos) of Lack Limos Deficiencies
During the conduct of the book you saw, that the modern understanding of GERD in fact goes in line with the Hesiod concept of lack limos (deficiencies) and lethe (the hidden, out of memory, out of perception) [9,10,11]. As depicted in Table 14.1, GERD represents a “beautiful” collection of lack limos (deficiencies) and lethe-type phenomena. The reason for GERD is not the gastric acid, not the development of symptoms, stenosis, Barrett’s esophagus, and cancer. A modern understanding unhides, that the reason for GERD is the dysfunction of the lower esophageal sphincter: lack of adequate sphincter function, i.e., limos (deficit) of appropriate sphincter function [20, 36,37,38,39,40]. This has already been pointed out by the early papers of Tilestone 1906, Jackson 1929, Allison and Johnstone, and Norman Barrett in the 1940s [41,42,43,44,45,46]. But it seems that the medical community somehow did forget about it: lethe, forgetfulness, lack of remembrance comes into play.
Then around 1994, Chandrasoma and DeMeester synchronized their interests and started to unhide (a-letheia) and remember the sequence of events leading to GERD: dysfunction of the lower esophageal sphincter fosters reflux, which in turn causes the return of the gastric acid juice into the esophagus. As a consequence, the esophagus inflames and changes its lining, the squamous lining is replaced by a columnar-lined mucosa [47], and the so-called columnar-lined esophagus (CLE) [12,13,14,15,16,17,18,19,20]. And if the CLE contains goblet cells, we name it Barrett’s esophagus and we speak about Barrett’s esophagus [31]. Thus, we refer to the paper published by Norman Barrett in June 1957 in Surgery, where he coined the term columnar-lined esophagus [48].
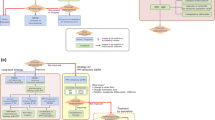
Going in line with the Hesiod terminology [33], lack, limos, deficiency of adequate function of the lower esophageal sphincter causes reflux, this reflux causes the lack, loss, limos of normal white squamous epithelium, which gets inflamed and replaced by columnar-lined esophagus, i.e., the esophagus loses its normal mucosa, this is lack limos of normalcy (Figs. 14.1 and 14.2). Over time progression of GERD causes lack limos of adequate esophageal and hiatal anatomy and geometry (Fig. 14.2) [16, 19, 49, 50]. In addition, the lack limos of sphincter function causes the symptoms (pain, sorrow) and inflammation, i.e., the discord of the immune system, using the words of Hesiod.
Antegrade endoscopic view into the lower end of the esophagus with the squamo-columnar junction (SCJ) at (arrow in a), and above the level of the diaphragmatic impression (b–d). Note the presence of endoscopically visible tongues and islands of columnar-lined esophagus (arrows in panels b, d) and prominent rugal folds (arrows in panel c). The histopathology of SCJ biopsies revealed columnar-lined esophagus (CLE) without (a–c) and with non-dysplastic Barrett’s esophagus (d)
Hill classification of the esophagogastric valve, as obtained during retrograde endoscopy. Note, that with increased Hill grade, the esophagogastric valve loses the capacity to adequately enwrap the endoscope. The lack limos of Hill valve integrity mirrors the failure of the lower esophageal sphincter function, geometry, and anchorage within the diaphragm, as described in the text
Over time the lack limos of appropriate function of the lower esophageal sphincter induces increased reflux (± acid pockets) which in turn affects the transport function of the esophageal body, resulting in lack limos of adequate esophageal bolus transport function. As such, GERD progresses with all its manifestations including symptoms, impaired patency, food intolerance, sleeping disorders, anxiety, depression, and cancer. Could we stop the progression of GERD? Is there a perfect point, at which progression of GERD should be stopped? May symptoms help to define that point?
14.6 Lack Limos of Symptoms
As a matter of fact, the large majority of those developing the most severe consequence and complication of GERD, esophageal cancer, appear without a preceding history of symptoms [2, 4,5,6,7]. So, symptoms did not work as a reliable marker for GERD in these patients. But how can people without symptoms, without having GERD symptoms, develop a GERD-induced cancer?
Here, morphology (the collection of tissue data) entered the stage: we discovered that Barrett’s esophagus is the precursor to cancer and may be assessed by histopathological examination within biopsies obtained from an irregular Z-line, tongue, or island of endoscopically visible columnar-lined esophagus [2, 4,5,6,7, 10, 11, 15]. But how should we deal with Barrett’s assessed at an endoscopically normal appearing esophago-gastric junction? [18]. Where and how do we define the normal esophago-gastric junction? What about Barrett’s within an endoscopically completely normal appearing esophago-gastric junction? What about dysplasia and early cancer within an endoscopically normal appearing esophago-gastric junction? What about the importance of magnification for the discrimination between normal and abnormal findings? For more than 30 years, symptoms and endoscopic criteria defined GERD [22,23,24,25]. Histopathology of biopsies obtained from the endoscopically visible squamo-columnar junction (SCJ) came into play, when Barrett’s esophagus was assessed [2, 18, 19]. Today we know that we can do much better. Today we see that the information gained at the highest light microscopical magnification resolution is most suitable for the definition of reflux, GERD, cancer risk, therapy monitoring, and follow-up [7, 15, 19,20,21]. And this intriguing aspect is also well taken by the book.
14.7 Lack Limos of LES Function
The correlation of function test data and histopathology demonstrated that the failure of the function of the lower esophageal sphincter (LES) represents the cause of GERD and BE [31, 32, 36, 51]. Over time, lack limos of LES function contributes to orchestrate symptoms and signs of the disease [7, 16, 27].
Conceptually, LES failure and dysfunction may be mediated by genetically weak formatting of the connective tissue, mechanical stress, which in turn contribute to unfold and open the LES; and drug-induced impairment of LES function. These are the reasons for LES failure:
-
1.
Hereditary factors: genetics for the formatting of weak tissue and sphincters (inguinal hernia, connective tissue disorders, i.e., scleroderma, etc.). Weak tissue fosters impaired resistance against mechanical stress [52].
-
2.
Mechanical stress due to increased abdominal pressure contributes to unfold the LES. Causes for increased abdominal pressure and tension forces towards the diaphragm include obesity, constipation (straining), eating behavior (overeating, large meals, food and beverages containing concentrated, artificial sugar; conservatives, E-substances; food (± concentrated sugar) induced post-prandial gastric contractions and spasms, associated with epigastric crampy pain; delayed gastric emptying, nausea and discomfort, repeated vomiting (eating disorder, migraine), lifting of heavy weights (street worker, sports, gym, etc.), diaphragmatic straining forces (singers, actors), and pregnancy [7, 53, 54].
-
3.
Medical causes: medications against depression, sleeping disorders, chronic painkiller consumption, regular use of nicotine, alcohol, drugs (cannabis, designer drugs) [7, 24].
All other GERD-related findings are the manifestations of LES failure: symptoms, tissues, and structural alterations of the esophagus (stenosis, diverticula, rings, webs) [7, 20, 24, 36].
14.8 CLE as a Marker for LES Failure: Cellular Instead of Endoscopic Pathology
The above functional changes of the esophagus (i.e., the shortening of the lower esophageal sphincter, impaired esophageal body transport function) are paralleled by morphological alterations (lack limos of adequate epithelial integrity and tissue resistance), as assessed by endoscopic resolution: esophagitis, hiatal hernia, increased grades of the distortion of the geometry of the esophago-gastric junction valve (Hill grades I–IV), and increased length of CLE [7, 16,17,18,19,20, 27, 36]. We point out here into a very fascinating topic, which is well described in detail within the book. Use of the larger magnification of the microscope enabled to demonstrate that what has been taken as gastric cardia during endoscopy, in fact represents reflux damaged columnar-lined, dilated, sphincter function lacking lower end of the esophagus [7, 11, 17,18,19,20]. The lack limos of sphincter function induces the reflux which alters the tissue, and CLE develops due to lack limos of normal squamous-lined esophagus. Due to the lack limos of sphincter and esophageal body transport function, the lower end of the esophagus forms CLE-lined folds [10, 11]. These folds are of gastric appearance during endoscopy and lack limos of appropriate magnification creates the idea of gastric cardia [10, 11, 15]. But there is a hidden thing behind, there is a lethe, and this lethe can be unfolded if we recognize that we should replace endoscopic pathology by cellular pathology. What is hidden, i.e., lethe during endoscopy becomes a-letheia, i.e., unhidden, if we apply the resolution of histopathology. As such, the so-called gastric cardia, as assessed by endoscopic resolution, is recognized as columnar-lined, reflux-damaged esophagus, as confirmed by the highly accurate means of histopathology [10, 11, 15, 20]. As quantum space time unfolds perception, magnification improves our resolution.
How did all that happen? It happened because physicians obtained biopsies from the so-called cardia, and the histopathology of these biopsies clearly showed that the tissues represented fragments of abnormal distal esophagus [11, 17,18,19,20], i.e., CLE, and this experience equals the lack limos of normalcy in the words of Hesiod. What does this mean? The endoscopic magnification is not appropriate (lack limos of resolution) for the assessment of the distal end of the esophagus and the proximal limit of the stomach. Why? Because the endoscopic appearance of the proximal stomach and the reflux injured inflamed dilated distal esophagus are the same [10, 11]. Interestingly, the same argument convinced Norman Barrett to write his CLE paper [48]. But forgetfulness (lethe) came over us and lack of remembrance avoided us from getting it right again. We have been in a state of lack limos of knowledge and awareness regarding the anatomy of the esophago-gastric junction. Correlation of anatomy, histology, histopathology, and esophageal function test contributed to reveal the hidden, i.e., lethe. Numerous studies demonstrated that the lack limos of lower esophageal sphincter (LES) function correlated with increased reflux, length of CLE and BE, and development of cancer [7, 12, 16, 31, 32, 36, 47]. In addition, effective anti-reflux surgery and ablation therapies reversed BE and cancer risk [55,56,57].
14.9 No CLE Without Reflux
Let us replace endoscopic by cellular pathology. If we aim to base our GERD management (diagnosis, grading of disease, therapy, therapy monitoring, cancer prevention) on the histopathology of CLE, we have to be sure that reflux is the only cause for the development of CLE and that the extent of CLE correlates with the severity of GERD. Fortunately, there exists a large body of evidence, which supports the notion that CLE represents a reproducible, sensitive marker for reflux at the cellular level (no CLE without reflux) [11, 12]. Thus, at least by theory, histopathology collects the information, which may serve as the fundamental and most reliable marker for GERD diagnosis, therapy, and follow-up. Those are the facts we have, which indicate that there develops no CLE without reflux.
Following subtotal esophagectomy and reconstruction of the upper GI tract with an esophago-gastric tube anastomosis served to elucidate the morphological consequences or reflux. After the surgery, squamous-lined esophagus connected to the mucosa of the proximal stomach. There existed no sphincter anymore and as a consequence reflux of gastric content into the remnant esophagus occurred. The histopathology of follow-up biopsies demonstrated that the stomach remained normal, and there were no abnormal chances observed within the mucosa of the stomach. In contrast to that, all patients developed CLE within their remnant esophagus, up to 36% developed BE [58, 59].
Following radiofrequency ablation (RFA) stenosis may occur in 2–4% of the cases. This prevents the reflux of gastric juice into the segment of the esophagus above the level of the stenosis. As a consequence, post RFA assessment showed absence of any CLE above the stenosis and CLE and neosquamous epithelium below the level of the stenosis [1, 4, 7].
Numerous studies correlated the presence and length of CLE, BE, and esophageal function [12, 13, 16, 20]. The studies demonstrated that the length and presence of CLE and BE correlated with a distorted geometry of the lower esophagus/diaphragm (hiatal hernia) increased reflux and the dysfunction of the lower esophageal sphincter (length, pressure) [12, 13, 16, 20].
Effective anti-reflux surgery (Nissen fundoplication, LINX system) contributed to foster the regression of BE in 25–30% of the cases [55,56,57]. Therefore, the parts of the puzzle-evidence are strong and highly convincing to support the notion, that the dysfunction of the lower esophageal sphincter fosters reflux, which in turn manifests in the form of CLE and BE [7].
During GERD, CLE interposes between the normal squamous-lined esophagus and the normal mucosa of the proximal stomach. Chandrasoma and DeMeester coined the term “squamo-oxyntic gap” (SOG) for this reflux-induced condition [15]. Their data indicate that the length of the SOG correlates with the severity of GERD. For example, the longer the SOG, the more advanced the stage of GERD and the higher the probability to have BE [12, 13, 15]. However, we still lack accurate correlation between the length of the SOG and esophageal function data (manometry, reflux monitoring). As such our book aims to motivate future clinical science for a better understanding of reflux, GERD, and BE. If these studies will proof, that SOG characteristics (length, cellular composition) correlate with other markers of the disease (symptoms, esophageal function, cancer risk), the SOG will serve as a novel, reliable, and sensitive marker for reflux, GERD, and BE management [20]. Then we will be allowed to close the diagnostic gap for the benefit of those affected by reflux, GERD, BE and cancer risk, who come to see us to seek medical care [7, 14].
14.10 Is There More Than LES Failure?
Going in line with the ideas of Hesiod, we have seen that the spectrum of GERD phenomena during diagnosis, therapy, therapy monitoring, and follow-up may in fact be seen as different forms of lack limos deficiencies. First, there is the spectrum of deficiencies of esophageal structure and function. Second, we know about the lack limos limitations regarding the level of magnification for the adequate assessment of the disease (endoscopic vs. histopathological diagnosis) [60, 61]. Third, there are the lack limos deficiencies regarding the knowledge of known and still unknown aspects of the disease. We still do not know: what is the normal length and function of the LES at birth and at adolescence. But we know that there are studies showing a max length of 6.0 cm [36,37,38,39]. We know that those presenting with shorter length than 6.0 cm all harbor CLE interposed between the normal squamous lining of the esophagus and the normal mucosa of the gastric body [15, 19, 62, 63]. In addition, CLE associates with increased acid exposure of the esophagus [12,13,14,15,16, 20, 62]. These data justify to assume that CLE developed at the cost of functioning LES. Fourth, there exists a lack limos of knowledge of the patients regarding adequate lifestyle, nutrition, and eating behavior to support the treatment of GERD and BE [53, 54]. Thus, reflux appears in the form of multiple lack limos phenomena. But there seems to be one more essential driver and cause.
14.11 Failure of Discipline
Hesiod names the very reason and cause of limos and lethe: he names it the “strife” [33]. According to Hesiod, it seems that strife causes the playground for lethe and limos. And this observation seems to be of major importance. What kind of strife is he talking about? Approximately 100 years after Hesiod, Heraclitus, and Parmenides created their imaginations of the world. Going in line with Hesiod, Heraclitus also came up with the conclusion that strife represents the underlying cause of every perception. He calls it: polemos! And we recall his saying, where he states: polemos is the father of all things. At this point we have to ask ourselves: what is the strife all about, who are the actors of the strife, of the polemos? A deeper reading reveals the essential understanding of Hesiod’s citation: the strife, the polemos between lethe and aletheia, between the hidden and unhidden is the world, is being, is existence, is all, and this all is one (Heraclitus) [11]. And this all equals our reasoning (Parmenides). Within the tensions of the hidden (lethe) and the unhidden (a-letheia), our reasoning creates the perceptions, which allow us to establish a diagnosis, design a therapy, and conduct therapy monitoring and follow-up [8,9,10,11]. The “strife” between lethe and a-letheia is driven by the lack limos of information. And here the circuit closes and continues to push forward. Going in line with Parmenides knowing (Greek: noein) and being (einai) are the same. Furthermore, there exists the strife, battle, confrontation, and dispute between healthy and unhealthy lifestyle aspects. It is well accepted that food and beverages containing concentrated sugar, artificial sugar, conservatives, and E-substances foster the development of reflux, GERD, BE, and esophageal cancer [4, 5, 53, 54]. Due to our culture and eating habits, it is hard for the patients to abandon these foods and beverages. As a consequence, nutrition therapy and diets face the strife between “what is allowed” and “what is not allowed.” Such tensions of strife also affect the well-being and the life quality. Is there a way out of the struggle? Well, there is a way and we know we can: Hesiod names the muse, the principle of strict order and discipline. As a consequence, discipline fosters to outbalance the tensions and to achieve balance, health, and well-being.
Taken together, the principle for reflux, GERD, and BE management seems to unhide (a-letheia) in the form of discipline for both the physician and the patient [11, 53, 54]. Following strict order and discipline, the physician should accurately diagnose and treat the cause of the disease, i.e., the dysfunction, the failure of the LES, which represents in the form of the CLE-lined squamo-oxyntic gap (SOG) [15, 32]. The patient should follow the recommendations of the physician for diagnosis and therapy [7]. As such, we are aware of the rich value of the legacy of old European reasoning for nowadays medicine and patient care [33, 34].
14.12 Reflux: Normalcy, Abnormality, and Disease
We hope that our journey motivates you to allow a different, histopathology-based perspective towards reflux, GERD, and BE management. As such, histopathology offers the possibility to differentiate between normality, abnormality, and disease (Table 14.2). When compared to symptomatology, endoscopy and function test data, histopathology offers the advantage of an increased resolution, i.e., resolution at the cellular level [28,29,30,31, 40, 62, 63].
Going in line with the above considerations, CLE represents the histopathological marker for reflux (no CLE without reflux) and may occur with and without symptoms and cancer risk (BE) [1, 2, 10, 47, 63]. Consequently, the presence of symptoms ± cancer risk (BE) or cancer risk (BE) without symptoms defines disease (GERD). The finding of BE-negative CLE without symptoms, defines abnormality. The absence of any CLE, i.e., squamo-oxyntic gap (SOG) negative individual, defines normalcy [4, 15, 63]. Future investigations may contribute to clarify the correlations between histopathology, endoscopy, and function test data. As a consequence, the multi- and interdisciplinary management will recommend:
-
Treatment of disease: elimination of symptoms and cancer risk, using lifestyle measures, medical, endoscopic, and surgical therapies.
-
Prevention of disease: prevent abnormality (symptom and cancer risk negative CLE) from becoming a disease, using lifestyle measures.
-
Normality: in the absence of any CLE, SOG, there is no need for intervention, and prevention may be recommended in order to prevent normality from becoming an abnormality.
Follow-up endoscopies will serve reflux-related management and monitoring.
The histopathology-based differentiation between normalcy, abnormality, and disease may offer an alternative approach for reflux management and cancer prevention [50, 64]. The fact, that individuals without symptoms are considered to be normal and are thus not seen by a physician, explains why there exist no data describing the progression from normalcy to disease, from health to cancer. Such studies would provide enormously valuable information for disease and cancer prevention. As such, Hesiod might have been categorized as having had asymptomatic, Barrett’s esophagus negative reflux. Otherwise, he would have reported on complex constellations between gods, goddess, nymphs, and heroes related to bile, acid, and gullet sounds of tube. So, what do we have?
There is a lot we have, and our book presents you the spectrum of new data related to the diagnosis, therapy, and follow-up of GERD and BE. As a consequence, the book summarizes how the individual aspects of the spectrum of manifestations of GERD translate into diagnosis and therapy. The inter- and multidisciplinary spectrum of contributions include GERD symptomatology, endoscopy, histopathology, endoscopic mucosal resections, transoral and laparoscopic anti-reflux surgeries, the management of Barrett’s esophagus (BE), esophageal cancer, palliation therapies, and cancer prevention. Most importantly, the book outlines the relevance of GERD for ear, throat, and nose (ENT) medicine and how modern GERD management recommends the involvement of ENT into diagnosis and therapy. As such, GERD-positive individuals working as singers and actors will benefit from the interdisciplinary approach.
Taken together, our goal is met if the book fosters a different understanding of reflux, GERD, and BE and contributes to improve your daily routine. Fun Do for You!
References
Kristo I, Schoppmann SF. Diagnosis and treatment of benign inflammatory esophageal disease. Eur Surg. 2015;47(4):188–98.
Labenz J, Chandrsoma PT, Knapp LJ, DeMeester TR. Proposed approach to the challenging management of progressive gastroesophageal reflux disease. World J Gastrointest Endosc. 2018;10(9):175–83.
Falk G, Vivian SJ. Laryngopharyngeal reflux: diagnosis, treatment and latest research. Eur Surg. 2016;48(2):74–91.
Riegler M, Kristo I, Nikolic M, et al. Update on the management of Barrett’s esophagus in Austria. Eur Surg. 2017;49(6):282–7.
Kristo I, Schoppmann SF, Riegler M, et al. Austrian expert panel recommendation for radiofrequency ablation of Barrett’s esophagus. Eur Surg. 2015;47(6):319–23.
Lenglinger J, Riegler M, Cosentini E, et al. Review on the annual cancer risk of Barrett’s esophagus in persons with symptoms of gastroesophageal reflux disease. Anticancer Res. 2012;32(12):5465–73.
Rieder E, Riegler M, Simic AP, et al. Alternative therapies for GERD: a way to personalized antireflux surgery. Ann N Y Acad Sci. 2018;1434(1):360–9.
Riegler M. The lemon taste of limos. Eur Surg. 2014;46(3):99–102.
Riegler M. Surgery, limos and shine keep things going. Eur Surg. 2015;47(5):215–7.
Riegler FM. Lessons learnt from the esophagogastric junction: the hidden counts. Eur Surg. 2013;45(4):185–6.
Riegler M, Asari R, Cosentini EP, Wrba F, Schoppmann SF. Critical assessment of a new endoscopic anatomic concept for the so-called cardia in the sense of the notions of Parmenides and Martin Heidegger. Z Gastroenterol. 2014;52:367–73.
Chandrasoma PT, Lokuhetty DM, DeMeester TR, et al. Definition of histopathologic changes in gastroesophageal reflux disease. Am J Surg Pathol. 2000;24:344–51.
Chandrasoma PT, Der A, Ma Y, et al. Histologic classification of patients based on mapping biopsies of the gastroesophageal junction. Am J Surg Pathol. 2003;27:929–36.
Chandrasoma P, Wijetung S, DeMeester S, et al. Columnar-lined esophagus without intestinal metaplasia has no proven risk of adenocarcinoma. Am J Surg Pathol. 2012;36:1–7.
Chandrasoma PT, Wijetunge S, DeMeester SR, et al. The histologic squamo-oxyntic gap: an accurate and reproducible diagnostic marker of gastroesophageal reflux disease. Am J Surg Pathol. 2010;34:1574–81.
Oberg S, Peters JH, DeMeester SR, et al. Endoscopic grading of the gastroesophageal valve in patients with symptoms of gastroesophageal reflux disease. Surg Endosc. 1999;13:1184–8.
Jain R, Aquino D, Harford WV, et al. Cardiac epithelium is found frequently in the gastric cardia. Gastroenterology. 1998;114:A160. (Abstract).
Marsman WA, van Sandick JW, Tytgat GNJ, et al. The presence and mucin histochemistry of cardiac type mucosa at the esophagogastric junction. Am J Gastroenterol. 2004;99(2):212–7.
Ringhofer C, Lenglinger J, Izay B, et al. Histopathology of the endoscopic esophagogastric junction in patients with gastroesophageal reflux disease. Wien Klin Wochenschr. 2008;120:350–9.
Chandrasoma PT. GERD. A new pathologic test of LES damage. In: Chandrasoma PT, editor. GERD; a new understanding. London: Academic Press, Elsevier; 2018. p. 5125–516.
Chandrasoma PT. Historical definitions of the gastroesophageal junction. In: Chandrasoma PT, editor. GERD; a new understanding. London: Academic Press, Elsevier; 2018. p. 163–4.
Sharma P, Dent J, Armstrong D, et al. The development and validation of an endoscopic grading system for Barrett’s esophagus: the Prague C&M criteria. Gastroenterology. 2006;131:1392–9.
Vakil N, van Zanten SV, Kahrilas P, et al. The Montreal definition and classification of gastroesophageal reflux disease: a global evidence-based consensus. Am J Gastroenterol. 2006;101:1900–20.
Kahrilas PJ, Bredenoord AJ, Fox M, et al. The Chicago classification of esophageal motility disorders. Neurogastroenterol Motil. 2015;27:160–74.
Frazzoni L, Frazzoni M, de Bortoli N, et al. Critical appraisal of Rome IV criteria: hypersensitive esophagus does belong to gastroesophageal reflux disease spectrum. Ann Gastroenterol. 2018;31(1):1–7.
Riegler M. Delphi comes to Milan to stop oracles on GERD and Barrett’s esophagus. Eur Surg. 2018;50(1):1–3.
Labenz J, Nocon M, Lind T, et al. Prospective follow up data from the pro GERD study suggest that GERD is not a categorial disease. Am J Gastroenterol. 2006;101(11):2457–62.
Chandrasoma PT. The past: historical evolution of columnar lined esophagus. In: Chandrasoma PT, editor. GERD; a new understanding. London: Academic Press, Elsevier; 2018. p. 300–17.
Rokitansky C. Entzündungen. In: Rokitansky C, editor. Handbuch der speziellen pathologischen Anatomie. 1. Band. Wien: Braumüller & Seidel; 1844. p. 50–65.
Virchow R. Cellularpathologie in ihrer Begründung auf physiologische und pathologische Gewebelehre. Berlin: Hirschwald; 1858. p. 32–48.
Theodorou D, Ayazi S, DeMeester SR, et al. Intraluminal pH and goblet cell density in Barrett’s esophagus. J Gastrointest Surg. 2012;16(3):469–74.
Chandrasoma PT. Correlation between lower esophageal sphincter damage and gastroesophageal reflux disease. In: Chandrasoma PT, editor. GERD; a new understanding. London: Academic Press, Elsevier; 2018. p. 236–7.
Hesiod. Theogony. https://msu.edu/~tyrrell/theogon.pdf. Lines 226–228.
Hesiod. Theogony. https://msu.edu/~tyrrell/theogon.pdf. Line 1.
Guttmann W. Medizinische Terminilogie. Ösophagus. Berlin: Urban und Schwarzenberg; 1917. p. 916.
Zaninotto G, DeMeester TR, Schwizer W, et al. The lower esophageal sphincter in health and disease. Am J Surg. 1988;155:104–11.
Do Carmo GC, Jafari J, Sifrim D, et al. Normal esophageal pressure topography metric for data derived from the Sandhill-Unisensor high-resolution manometry assembly in supine and sitting positions. Neurogastroenterol Motil. 2015;27(2):285–92.
Sivla RMBD, Herbella FAM, Gualberto D. Normative values for a new water-perfused high resolution manometry system. Arg Gastroenterol. 2018;55(Suppl 1):30–4.
Weijenborg PW, Kessing BE, Bredenord AJ. Normal values for solid-state esophageal high-resolution manometry in a European population; an overview of all current metrics. Neurogastroenterol Motil. 2014;26(5):654–9.
Chandrasoma P. How the pathologist can aid in the assessment of gastroesophageal reflux disease. Curr Opin Gastroenterol. 2018;34(4):233–42.
Tilestone W. Peptic ulcer of the esophagus. Am J Med Sci. 1906;132:240–65.
Jackson C. Peptic ulcer of the esophagus. JAMA. 1929;92:369–72.
Allison PR. Peptic ulcer of the oesophagus. Thorax. 1948;3:20–42.
Allison PR. Peptic ulcer of the oesophagus. J Thorax Surg. 1946;15:308–17.
Allison PR, Johnstone AS. The oesophagus lined with gastric mucous membrane. Thorax. 1953;8:87–101.
Barrett NR. Chronic peptic ulcer of the oesophagus and “oesophagitis”. Br J Surg. 1950;38:175–82.
Paull A, Trier JS, Dalton MD, et al. The histologic spectrum of Barrett’s esophagus. N Engl J Med. 1976;295:476–80.
Barrett NR. The lower oesophagus lined by columnar epithelium. Surgery. 1957;41:881–94.
Triadafilopoulos G, Zikos T, Regalia K, et al. Use of esophageal pH monitoring to minimize proton pump inhibitor utilization in patients with gastroesophageal reflux symptoms. Dig Dis Sci. 2018;63(10):2673–80.
Triadafilopoulos G, Clarke JO, Hawn M. Precision GERD management 21st century. Dis Esophagus. 2017;30(9):1–6.
Hvid-Jensen F, Pedersen L, Funch Jensen P, Drewes AM. Proton pump inhibitor use may not prevent high-grade dysplasia and oesophageal adenocarcinoma in Barrett’s oesophagus: a nationwide study in 9883 patients. Aliment Pharmacol Ther. 2014;39(9):984–91.
von Diemen V, Trindade EN, Trindade MR. Hiatal hernia and gastroesophageal reflux: study of collagen in the phrenoesophageal ligament. Surg Endosc. 2016;30(11):5091–8.
Riegler M, Kristo I, Asari R, et al. Dietary sugar and Barrett’s esophagus. Eur Surg. 2017;49(6):279–81.
Austin GL, Thiny MT, Westman EC, et al. A very low-carbohydrate diet improves gastroesophageal reflux and its symptoms. Dig Dis Sci. 2006;51(8):1307–12.
Alicuben ET, Tatum JM, Bildzukewicz N, et al. Regression of intestinal metaplasia following magnetic sphincter augmentation device placement. Surg Endosc. 2019;33(2):576–9.
Zehetner J, DeMeester SR, Ayazi S, et al. Long-term follow-up after anti-reflux surgery in patients with Barrett’s esophagus. J Gastrointest Surg. 2010;14(10):1483–91.
Zaninotto G, Parente P, Salvador R, et al. Long-term follow-up of Barrett’s epithelium: medical versus antireflux surgical therapy. J Gastrointest Surg. 2012;16(1):7–14.
Lord RV, Wickramasinghe K, Johansson JJ, et al. Cardiac mucosa in the remnant esophagus is an acquired epithelium with Barrett’s-like features. Surgery. 2004;136(3):633–40.
Dunn LJ, Burt AD, Hayes N, Griffin SM. Columnar metaplasia in the esophageal remnant after esophagectomy: a common occurrence and a valuable insight into the development of Barrett’s esophagus. Ann Surg. 2016;264(6):1016–21.
Skrobic O, Simic AP, Pesko P. Current treatment strategies in Barrett’s esophagus. In: Simic AP, Bonavina L, DeMeester SR, editors. Surgery for benign oesophageal disorders. Singapore: World Scientific; 2018. ISSN: 2045-0346. p. 133–48.
Herbella FA, Schlottmann F, Patti MG. Chicago classification: impact of HRM on the diagnosis and management of esophageal motility disorders. In: Simic AP, Bonavina L, DeMeester SR, editors. Surgery for benign oesophageal disorders. Singapore: World Scientific; 2018. ISSN: 2045-0346. p. 149–72.
Ringhofer C, Lenglinger J, Riegler M, et al. Waist to hip ratio is a better predictor of esophageal acid exposure than body mass index. Neurogastroenterol Motil. 2017;29(7) https://doi.org/10.1111/nmo.13033.
Chandrasoma PT, Der R, Ma Y, et al. Histology of the gastroesophageal junction: an autopsy study. Am J Surg Pathol. 2000;24(3):402–9.
Spechler S. Barrett esophagus and risk of esophageal cancer: a clinical review. JAMA. 2013;310(6):627–36.
Acknowledgments
The authors thank their families, friends, colleagues, and teachers for their passion, support, and understanding. Otherwise the project would not have been possible. Finally, the authors thank their patients, from whom they were allowed to borrow knowledge and perception, which fostered a deeper understanding of reflux, GERD, and BE.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Riegler, M., Schoppmann, S.F. (2021). Multidisciplinary Management: Alternative Perspectives for the Management of Gastroesophageal Reflux Disease (GERD) and Barrett’s Esophagus (BE). In: Schoppmann, S.F., Riegler, M. (eds) Multidisciplinary Management of Gastroesophageal Reflux Disease. Springer, Cham. https://doi.org/10.1007/978-3-030-53751-7_14
Download citation
DOI: https://doi.org/10.1007/978-3-030-53751-7_14
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-53750-0
Online ISBN: 978-3-030-53751-7
eBook Packages: MedicineMedicine (R0)