Abstract
Langerhans cells (LCs) are immune cells that reside in the stratified epithelium of the skin and mucosal membranes. They play a range of roles in the skin, including antigen presentation and maintenance of peripheral tolerance. Reports of LC numbers have been variable in different cancer types, with the majority of studies indicating a reduction in their number. Changes in the cytokine profile and other secreted molecules, downregulation of surface molecules on cells and hypoxia all contribute to the regulation of LCs in the tumour microenvironment. Functionally, LCs have been reported to regulate immunity and carcinogenesis in different cancer types. An improved understanding of the function and biology of LCs in tumours is essential knowledge that underpins the development of new cancer immunotherapies.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Langerhans cell
- Tumour microenvironment
- Cancer
- Cytokines
- Surface molecules
- Hypoxia
- Antigen presentation
- Carcinogenesis
- Immunity
- Immune cells
- Angiogenesis
- Lymphangiogenesis
- Immunotherapy
- Human
- Mice
8.1 Langerhans Cells
Langerhans cells (LCs) are unique antigen-presenting cells that reside in the stratified squamous epidermis of cutaneous and mucosal epithelium. LCs were discovered in 1868 by Paul Langerhans, who initially believed that these cells were neurons due to their dendritic morphology [39]. Nearly 100 years later, the antigen-presenting function of these cells was determined.
Langerhans cells can be identified based on the expression of the C-type lectin receptor, langerin (CD207) [81], along with other less-specific markers such as CD1a in humans [21, 66] and major histocompatibility complex (MHC) class II [37]. Langerin is involved in antigen capture and induces the formation of Birbeck granules [8]. Birbeck granules are unique rod or tennis racket-shaped endocytic vesicles that are considered the hallmark of LCs. LCs express the epithelial cell adhesion molecule (EpCAM) in mice [4, 55], which enables LC motility and migration to lymph nodes and modulates responses to epicutaneously applied protein antigen in a mouse model.
8.2 Ontogeny of Langerhans Cells
Cutaneous LCs originate from embryonic macrophages and foetal liver monocytes [29]. LC precursors seed the epidermis during murine embryonic development, but are not able to enter the adult epidermis in the steady state. These precursors differentiate into LCs in the epidermis immediately [29]. These newly differentiated LCs rapidly proliferate to form a radio-resistant cellular network that is capable of self-renewal throughout life [45]. During inflammation, the skin is permissive for the entry of circulating precursors to the epidermis that differentiate locally to LCs. Monocytes are the first bone marrow precursors that differentiate into LCs during inflammation [25, 54]. Unlike the skin, mucosal epithelium has better accessibility to circulating precursors in the steady state. Mucosal LCs arise from adult bone marrow precursors, unlike the embryonic precursor origin of cutaneous LCs [12].
Despite the differing ontogeny in the steady state, skin and mucosal LCs share similarities in anatomic location, phenotype, transcriptomic signature and function [30]. Mouse mucosal LCs can be controlled by the microbiota via regulation of epithelial differentiation signals, which may contribute to their generally less-dendritic appearance [30].
8.3 Langerhans Cell Function
The role of LCs in the skin was initially believed to be primarily one of antigen presentation. Through a number of studies using mice that are selectively depletable of skin antigen presenting cell subsets, langerin-positive dermal dendritic cells (dDCs) have now been identified as the primary antigen-presenting cells in the skin. LCs are not considered necessary for the initiation of an adaptive T-cell response to skin-expressed antigen.
In the steady state, LCs survey the epidermis and migrate to the lymph nodes where they present self or commensal microbial antigens to T cells to induce tolerance and maintain tissue homeostasis (reviewed in [19]). LCs play an important role in maintaining the population of memory T cells in the epidermis [73]. Mucosal LCs express the lipopolysaccharide receptor CD14 and have a high-affinity receptor for IgE [2]. LCs have regulatory roles and may either promote or suppress disease progression depending on the condition (reviewed in [61]).
8.4 LCs in the Tumour Microenvironment
The tumour microenvironment includes neoplastic and non-neoplastic cells along with the extracellular matrix, and cytokines, chemokines and growth factors that may be derived from those cells [68]. LCs have been identified in the tumour microenvironment in a range of cancer types, particularly skin cancers [75]. There is a body of evidence showing the presence of LCs in head and neck [35], gastric [80] and cervical cancers [43], and papillary thyroid carcinoma [70]. Some studies have also identified LCs in breast [79] and prostate cancers [7]. In this chapter, we explore the regulation and function of LCs in cancers, summarised in Fig. 8.1.
Langerhans cell regulation and role in the tumour microenvironment. Regulation of Langerhans cells (LCs) in the tumour microenvironment (TME) occurs due to several factors. Production of cytokines and other soluble molecules by the tumour cells can either attract or inhibit the migration of LCs into the TME. Changes to surface molecules such as E-cadherin and BMP7 can affect the retention of LCs in the TME. Hypoxic conditions cause downregulation of langerin and CD1a on LCs, and they become more rounded and less functional. The role of LCs in the TME includes detoxification of toxins in the skin that can result in carcinogenesis via HRAS mutation. LCs regulate immunity in the TME by recruiting immune cells and also mediating anti-tumour T-cell responses. LIGHT is upregulated in LCs during inflammation, promoting lymphangiogenesis in skin. It is currently unclear if this also occurs in tumours
8.5 Regulation of LC Numbers and Location in the Tumour Microenvironment
Generally, there is a reduced number of LCs observed in cancer, particularly skin cancer. LC numbers in squamous cell carcinoma (SCC) and basal cell carcinoma (BCC) are significantly decreased when compared to normal skin [75]. The LC count is reported to be higher in benign compared with malignant skin tumours, suggesting that carcinogenesis is associated with a reduction in the number of LCs [75]. Similarly, increased LC numbers are associated with less aggressive forms of BCC [69]. Increased numbers of LCs in the normal epidermis at the margin of less aggressive tumours could be indicative of greater immunological resistance, limiting the aggressiveness of the neoplasm [69].
LC numbers in the lesion may have utility as a prognostic marker; however, this may only be the case in certain cancer types. Increased LC numbers in the lesion are correlated with better prognosis in gastric carcinoma [80], thyroid carcinoma, ductal breast cancer [38] and lung carcinoma [14]. Higher LC numbers are associated with increased survival of the patients, particularly with stage III gastric cancer [80]. CD1a and S100 have been used to identify LCs in some studies; however, CD207 (langerin) is considered to be the most robust marker for the identification of LCs [6]. For laryngeal SCC, using S100 as a marker for LCs, numbers were not considered a reliable marker of prognosis in clinical practice [33]. Similarly, using CD1a as a marker for LCs, numbers were increased when compared to normal tissue, but there was no association with the prognosis for laryngeal cancer [20]. However, these differences in results could also arise from the use of antibodies against markers other than langerin for the identification of LCs.
The changes in LC number in the tumour are a consequence of cytokine and chemokine regulation in the microenvironment. Macrophage inflammatory protein-3/C-C motif chemokine ligand 20 produced by tumour cells is selectively chemotactic to LCs [56]. Interleukin (IL)-10, transforming growth factor β (TGFβ) [32], IL-1β [17] and vascular endothelial growth factor (VEGF) [76] may also regulate the recruitment and migration in the tumour microenvironment. IL-10 is a known inhibitor of LC migration [18] that is increased in tumour cells [85]. IL-1β is a critical mediator of chronic inflammation and has been implicated in tumour pathogenesis [3]. When oral SCC cells are treated with IL-1β, they proliferate and their pro-tumorigenic cytokine network is stimulated [40]. Elevated levels of IL-1β, tumour necrosis factor-α and prostaglandin E2 in chronic periodontitis stimulate dendritic cell (DC) maturation and migration. Environmental factors, such as smoking, could lead to changes in the cytokine profile, which can contribute to a reduction in LC levels or change the phenotype of LCs. There is an increase in LC density in the lateral border of the tongue and lip of patients with oral SCC with a history of smoking [16]. Cytokine profiles compared between tobacco users and non-tobacco users change significantly, with increased VEGF [74]. Further analysis is needed to study the direct relationships between these cytokines and LCs. However, the varied cytokine profiles in different cancers or even in the same cancer present a formidable challenge for the development of immunomodulatory drugs.
CD10 is a zinc dependent metalloproteinase that can be detected in peritumoural fibroblast-like stromal cells within the invasive area of various cancers. CD10 expression is low in precancerous lesions and normal skin tissues [78]. Immunohistochemical analysis indicates increased induction of CD10 in stromal cells in epidermal tumours, especially in SCC, which could be contributing to the tumorigenesis and reduction in LCs [78]. There is a positive correlation between Ki67 levels with LCs and stromal CD10-positive cells but a negative correlation with CD1a-positive cells in the tumour [78], suggesting a potential suppressive role for the CD10-positive cells in the tumour microenvironment on the number of LCs. However, further in vitro analyses are required to confirm the exact relationship.
A pronounced reduction in LCs has been observed in low-grade cervical intraepithelial neoplasia (CIN) [15, 27]. However, LC numbers are increased in cervical cancer, when compared to precancerous CIN lesions [11]. The interaction between LCs and keratinocytes (KCs) is mediated by E-cadherin. Immature LCs adhere to KCs via E-cadherin, which is constitutively expressed by KCs in the basal and suprabasal layers. This interaction is important for both LC localisation and retention. The detachment of LCs from the surrounding KCs is an essential step in the initiation of their migration from the epidermis. Reduced E-cadherin expression in CIN reduces the retention of LCs, which is proposed to contribute to immune evasion in human papillomavirus (HPV) pre-cancer [44]. Similarly, E-cadherin levels are reduced in oral [34] and cutaneous SCC samples [86], compared with normal skin. More poorly differentiated tumours express less than 40% E-cadherin, which could be leading to the reduced LC levels [83]. There is a loss of cell-to-cell adhesion and gain of cell-to-matrix adhesion when E-cadherin expression is lost, promoting the transformation of pre-malignant to malignant cells. However, in a recent study using a CD11c-specific E-cadherin knockout, it was shown that an absence of E-cadherin-mediated cell adhesion on LCs did not affect their stability in epidermal sheets [10]. The LCs did exhibit altered morphology with fewer dendrites and a more rounded body. However, the lack of E-cadherin on LCs did not affect their proliferation or retention in the skin [10].
HPV type 16 E7 is a cell cycle deregulating protein that contributes to the oncogenesis of HPV16-related cervical cancer [63]. The K14 E7 transgenic mouse expresses HPV16 E7 in the epidermal KCs, which was associated with increased numbers of skin-resident LCs in the skin [1]. The increased LC number was attributed to the chronic inflammatory environment of the skin in this transgenic mouse model. LCs were atypically activated and functionally impaired in this model; however, they were functionally active when extracted from the skin and matured in vitro [1].
Changes to the cell polarity and adhesive properties of cells enable malignant conversion of cells. LCs could contribute to epithelial–mesenchymal transition (EMT) in cutaneous cancers. Many of the cytokines involved in mediating LC migration have also been associated with EMT processes [28], such as TGFβ [26]. BMP7 is important for the maintenance of LCs in the epidermis. Immunohistological analysis of LC niches in early prenatal epidermis and adult basal (KCs) show high levels of BMP7 expression. Mice deficient of BMP7 have diminished levels of LCs, and any remaining LCs are less dendritic [84]. In melanoma, BMP7 can induce mesenchymal–epithelial transition (MET), which can inhibit metastasis in vitro [50].
A common feature of most tumours is the presence of regions that have low levels of oxygen. In increasingly proliferating and expanding tumour tissue, the oxygen demand surpasses the oxygen supply, which creates hypoxic regions [72]. The severity of hypoxia varies in different cancers [49]. Increased hypoxia is associated with poorer prognosis of patients [67].
The hypoxic conditions of cancers could have an effect on the regulation of LCs in tumours. In response to hypoxic conditions, cells rapidly upregulate genes under the control of the transcription factor hypoxia-inducible factor-1α (HIF-1α). HIF-1α can downregulate LC functions in vivo [52]. The phenotypic features and surface expression markers of LC-like cells generated from human monocytes cultured in hypoxic and normoxic conditions have been assessed [60]. The expression of langerin and the activation markers CD86 and CD83 were significantly decreased on cells from the majority of the donors, while CD1a and E-cadherin were reduced in cells from some donors. These results suggest that there could be downregulation of cell surface markers on LCs, creating an apparent loss of the cells rather than actual depletion of LCs from the tumour [60].
Hypoxic conditions also impaired the LCs’ ability to stimulate T-cell responses. More LCs in hypoxic regions were shown to be viable, as indicated by the lower percentage of early and late apoptosis, when compared to LCs grown in normoxic cultures [60]. The impairment of LC function in hypoxia could contribute to tumour cell evasion of the immune response.
8.6 LCs Regulate Immunity in the Cancer Microenvironment
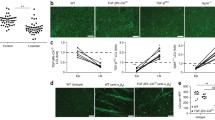
Langerhans cells are associated with infiltration of immune cells into the tumour. An increase in FoxP3+ Tregs as a percentage of total CD4+ T cells was observed in melanoma patient samples [71]. To test if there was a direct association between increased FoxP3+ Tregs in melanoma and LCs, the authors assessed co-localisation of the two cell populations [71]. However, LCs were not co-located with infiltrating Tregs, which led the authors to propose that LCs have a tolerogenic role in melanomas but not by directly effecting Tregs [71]. Melanoma-infiltrating LCs expressed less CD40 and are more likely to express the inhibitory programmed cell death-ligand 1 (PD-L1) marker [71]. Further in vitro studies may help to shed light on the increased Treg accumulation and LCs in melanoma. An analysis of cell infiltrates in radiation therapy demonstrated that a favourable prognosis was associated with LC infiltration [51]. T-cell infiltration into the tumour was associated with the presence of LCs [51], suggesting that they may induce a T-cell-mediated anti-tumour response that can improve the local response in radiation therapy.
Immature LCs express the programmed cell death protein 1 (PD-1) receptor, which helps to maintain tolerance in the skin [59]. As LCs mature, there is a decline in PD-1 receptor expression [59]. Blockade of PD-1 upregulates T-cell responses that can help fight off tumour cells [59]. However, the cells that provide the PD-L1/PD-L2 signal to PD-1 on the LCs are yet to be determined. KCs express high levels of PD-L1/PD-L2 during chronic inflammation [22]. Fujita et al. [24] have shown that LCs from SCC in particular are more mature, which could contribute to a reduced anti-tumour response [24].
LCs do contribute to the anti-tumour response to ovalbumin (OVA)-expressing melanoma cells following epicutaneous immunisation with OVA protein in the mouse, as do dermal dendritic cells [77]. The CD8+ T-cell response that is initiated following the presentation of antigen inhibited growth of the OVA-expressing transplanted melanoma [77]. Depletion of LCs at any point during the process resulted in susceptibility of the mice to the tumour [77].
8.7 Langerhans Cells Regulate Carcinogenesis
The epidermis is exposed to a variety of DNA-damaging chemicals . Cutaneous LCs play an important role in the detoxification of molecules such as polyaromatic hydrocarbons (PAH) in the skin. When toxins such as 2,4-dimethoxybenzaldehyde (DMBA) are detoxified by LCs, a carcinogenic intermediate is produced. The carcinogenic intermediate leads to increased HRAS mutations in the KCs , contributing to their malignant transformation. LC-intact mice are more susceptible to chemical carcinogenesis provoked by DMBA than mice without LCs [47]. The expression of p450 enzyme CYP1B1 is required for the rapid induction of DNA damage within the KCs to enable efficient neoplastic transformation [41]. Depletion of LCs worsened the progression of SCC in a temporarily LC-depletable mouse model. In the absence of LCs, there was reduced recruitment of natural killer (NK) cells into the tumour microenvironment [53]. NK cells are crucial for the elimination of DNA-damaged KCs during the tumour initiation step of chemical carcinogenesis [53]. These results need to be replicated in the same mouse model to make conclusive statements regarding the contribution of LCs in carcinogenesis.
8.8 LCs Regulate Lymphangiogenesis and Angiogenesis in the Tumour Microenvironment
Tumour growth and metastasis depend on angiogenesis and lymphangiogenesis triggered by chemical signals produced by tumour cells in a rapid growth phase [57]. In the absence of vascular support, tumours may become apoptotic or necrotic [58]. A role for LCs in tumour lymphatic development has not been defined; however, LCs do contribute to lymphatic vessel formation in the skin [54, 82]. LIGHT (an acronym for homologous to lymphotoxins, exhibits inducible expression, and competes with HSV glycoprotein D for herpesvirus entry mediator, a receptor expressed by T lymphocytes) is an important ligand that is required for lymphoid tissue development and homeostasis [23, 87]. LIGHT expression is significantly upregulated in skin LCs during inflammation, and LC signals play a dominant role in lymph endothelial cell activation [82]. A direct role for LCs in tumour lymphangiogenesis is still to be confirmed.
Lymphangiogenesis occurs following angiogenesis and relies on angiogenic factors in order for it to occur [42]. Pericytes contribute to angiogenesis in the tumour microenvironment [9], by producing pericyte-derived milk fat globulin E8 (MFG-E8) [48]. MFG-E8 is also produced by other immune cells, especially LCs [46], also implicating them in angiogenesis. Further investigation of their role in angiogenesis is warranted.
8.9 Langerhans Cells in Tumour Immunotherapy
Through translational studies it has been shown that DC-based immunisation is safe and feasible for patients with cancer. Most DC-based vaccines have used monocyte-derived DCs, but LCs derived from CD34+ haematopoietic cells are superior at activating a cytotoxic T-cell response [62]. Peptide-loaded LC vaccinations against melanoma elicited tumour responses that were comparable to monocyte-derived DCs in vivo [65]. A Phase I study of LCs electroporated with tyrosinase-related protein-2 (TRP-2) mRNA, a melanosomal differentiation antigen, in patients with melanoma was conducted [13]. The vaccines induced greater T-cell activation and diversity against the TRP-2 antigen, which correlated with clinical benefits [13]. Apart from mild delayed-type hypersensitivity reactions, no major toxicities were observed post vaccination [13]. LCs electroporated with Wilms Tumour 1 (WT1) induced sufficiently strong WT1-specific cytotoxic T lymphocytes in vitro [64]. These studies along with other clinical study data [5] highlight the feasibility and safety of LC immunisation, and the use of vaccination in combination with other immune therapies could further improve clinical outcomes for cancer patients.
8.10 Future Directions
The potential for LCs to amplify immune function in an antigen-specific manner makes them ideal candidates for cancer immunotherapy, which attempts to eradicate tumours through the manipulation of host immunity. The superior ability of LCs over other skin DCs to induce cytotoxic T-cell responses in vitro [62, 77] makes them ideal to be exploited for therapy. Protein antigen applied onto barrier-disrupted skin induces a long-lasting cytotoxic T-cell response that is potent enough to control and inhibit tumour growth [77]. In order for immunotherapies to be maximally effective, a thorough understanding of LC biology and function is required.
The identification of the distinct DC subset – langerin+ dermal DCs, has revealed that many of the functions attributed to LCs are in fact being carried out by dermal DCs. Many of these studies need to be revisited to separate the role of langerin-positive DCs from LCs. The inducible LC depletion mouse model, such as the Langerin-diphtheria toxin receptor (DTR) mouse, [36] depletes both the populations of langerin-positive cells (LCs and dDCs). Using the langerin-diphtheria toxin subunit A (DTA) model [31], or the generation of a specific mouse model that enables the inducible-targeted depletion of LCs over the DCs, would be highly useful to confirm the roles of the two langerin-positive populations in cancer. Single-cell sequencing would be highly beneficial to further define the roles of the different types of langerin-positive cells in cancer. This technology might help to uncover any potential subsets of LCs that could play a role in tumorigenesis and cancer. This may also help to clarify the controversy over the roles that have been attributed to LCs that may instead be a function of DCs, further paving the way for the targeting of antigen presentation for immune therapy against cancer.
8.11 Conclusion
Although there are varied levels of LCs reported in different cancers, the general trend is for numbers to be reduced. This could be an immune evasion mechanism that occurs in the neoplastic environment. The regulation of LCs in cancer could be mediated by changes in the cytokine milieu, downregulation of cell surface adhesion molecules, such as E-cadherin, or a result of the infiltration of other immune cells. Studies involving a LC-only depletable mouse model, single sequencing and standardised immunohistochemical protocols are necessary to further elucidate the function of LCs in cancers.
References
Abd Warif NM, Stoitzner P, Leggatt GR, Mattarollo SR, Frazer IH, Hibma MH (2015) Langerhans cell homeostasis and activation is altered in hyperplastic human papillomavirus type 16 E7 expressing epidermis. PLoS One 10(5):e0127155. https://doi.org/10.1371/journal.pone.0127155
Allam JP, Niederhagen B, Bucheler M, Appel T, Betten H, Bieber T, Berge S, Novak N (2006) Comparative analysis of nasal and oral mucosa dendritic cells. Allergy 61(2):166–172. https://doi.org/10.1111/j.1398-9995.2005.00965.x
Apte RN, Krelin Y, Song X, Dotan S, Recih E, Elkabets M, Carmi Y, Dvorkin T, White RM, Gayvoronsky L, Segal S, Voronov E (2006) Effects of micro-environment- and malignant cell-derived interleukin-1 in carcinogenesis, tumour invasiveness and tumour-host interactions. Eur J Cancer 42(6):751–759. https://doi.org/10.1016/j.ejca.2006.01.010
Balzar M, Winter MJ, de Boer CJ, Litvinov SV (1999) The biology of the 17-1A antigen (Ep-CAM). J Mol Med 77(10):699–712
Banchereau J, Palucka AK, Dhodapkar M, Burkeholder S, Taquet N, Rolland A, Taquet S, Coquery S, Wittkowski KM, Bhardwaj N, Pineiro L, Steinman R, Fay J (2001) Immune and clinical responses in patients with metastatic melanoma to CD34(+) progenitor-derived dendritic cell vaccine. Cancer Res 61(17):6451–6458
Bancroft H, Stewart R, Naidu B, Trotter S (2015) The use of immunohistochemical stains to identify Langerhans cell in pulmonary histiocytosis. Eur Respir J 46:PA3886. https://doi.org/10.1183/13993003.congress-2015.PA3886
Bigotti G, Coli A, Castagnola D (1991) Distribution of Langerhans cells and HLA class II molecules in prostatic carcinomas of different histopathological grade. Prostate 19(1):73–87. https://doi.org/10.1002/pros.2990190108
Birbeck MS, Breathnach AS, Everall JD (1961) An electron microscope study of basal melanocytes and high-level clear cells (Langerhans cells) in vitiligo. J Invest Dermatol 37(1):51–64. https://doi.org/10.1038/jid.1961.80
Birbrair A, Zhang T, Wang ZM, Messi ML, Olson JD, Mintz A, Delbono O (2014) Type-2 pericytes participate in normal and tumoral angiogenesis. Am J Physiol Cell Physiol 307(1):C25–C38. https://doi.org/10.1152/ajpcell.00084.2014
Brand A, Diener N, Zahner SP, Tripp C, Backer RA, Karram K, Jiang A, Mellman I, Stoitzner P, Clausen BE (2019) E-cadherin is dispensable to maintain Langerhans cells in the epidermis. J Invest Dermatol. https://doi.org/10.1016/j.jid.2019.06.132
Campaner AB, Nadais RF, Galvao MA, Santos RE, Aoki T (2007) Evaluation of density of Langerhans cells in human cervical intraepithelial neoplasia. Acta Obstet Gynecol Scand 86(3):361–366. https://doi.org/10.1080/00016340601133871
Capucha T, Mizraji G, Segev H, Blecher-Gonen R, Winter D, Khalaileh A, Tabib Y, Attal T, Nassar M, Zelentsova K, Kisos H, Zenke M, Sere K, Hieronymus T, Burstyn-Cohen T, Amit I, Wilensky A, Hovav AH (2015) Distinct murine mucosal Langerhans cell subsets develop from pre-dendritic cells and monocytes. Immunity 43(2):369–381. https://doi.org/10.1016/j.immuni.2015.06.017
Chung DJ, Carvajal RD, Postow MA, Sharma S, Pronschinske KB, Shyer JA, Singh-Kandah S, Dickson MA, D’Angelo SP, Wolchok JD, Young JW (2017) Langerhans-type dendritic cells electroporated with TRP-2 mRNA stimulate cellular immunity against melanoma: results of a phase I vaccine trial. Onco Targets Ther 7(1):e1372081. https://doi.org/10.1080/2162402X.2017.1372081
Colasante A, Poletti V, Rosini S, Ferracini R, Musiani P (1993) Langerhans cells in Langerhans cell histiocytosis and peripheral adenocarcinomas of the lung. Am Rev Respir Dis 148(3):752–759. https://doi.org/10.1164/ajrccm/148.3.752
Connor JP, Ferrer K, Kane JP, Goldberg JM (1999) Evaluation of Langerhans’ cells in the cervical epithelium of women with cervical intraepithelial neoplasia. Gynecol Oncol 75(1):130–135. https://doi.org/10.1006/gyno.1999.5559
Cruchley AT, Williams DM, Farthing PM, Speight PM, Lesch CA, Squier CA (1994) Langerhans cell density in normal human oral mucosa and skin: relationship to age, smoking and alcohol consumption. J Oral Pathol Med 23(2):55–59. https://doi.org/10.1111/j.1600-0714.1994.tb00256.x
Cumberbatch M, Bhushan M, Dearman RJ, Kimber I, Griffiths CE (2003) IL-1beta-induced Langerhans’ cell migration and TNF-alpha production in human skin: regulation by lactoferrin. Clin Exp Immunol 132(2):352–359. https://doi.org/10.1046/j.1365-2249.2003.02146.x
Cumberbatch M, Singh M, Dearman RJ, Young HS, Kimber I, Griffiths CEM (2006) Impaired Langerhans cell migration in psoriasis. J Exp Med 203(4):953–960. https://doi.org/10.1084/jem.20052367
Deckers J, Hammad H, Hoste E (2018) Langerhans cells: sensing the environment in health and disease. Front Immunol 9:93. https://doi.org/10.3389/fimmu.2018.00093
Esteban F, Ruiz-Cabello F, Gonzalez-Moles MA, Lopez-Gonzalez MA, Funez R, Redondo M (2012) Clinical significance of Langerhans cells in squamous cell carcinoma of the larynx. J Oncol 2012:753296. https://doi.org/10.1155/2012/753296
Fithian E, Kung P, Goldstein G, Rubenfeld M, Fenoglio C, Edelson R (1981) Reactivity of Langerhans cells with hybridoma antibody. Proc Natl Acad Sci U S A 78(4):2541–2544. https://doi.org/10.1073/pnas.78.4.2541
Freeman GJ, Long AJ, Iwai Y, Bourque K, Chernova T, Nishimura H, Fitz LJ, Malenkovich N, Okazaki T, Byrne MC, Horton HF, Fouser L, Carter L, Ling V, Bowman MR, Carreno BM, Collins M, Wood CR, Honjo T (2000) Engagement of the PD-1 immunoinhibitory receptor by a novel B7 family member leads to negative regulation of lymphocyte activation. J Exp Med 192(7):1027–1034. https://doi.org/10.1084/jem.192.7.1027
Fu YX, Chaplin DD (1999) Development and maturation of secondary lymphoid tissues. Annu Rev Immunol 17:399–433. https://doi.org/10.1146/annurev.immunol.17.1.399
Fujita H, Suarez-Farinas M, Mitsui H, Gonzalez J, Bluth MJ, Zhang S, Felsen D, Krueger JG, Carucci JA (2012) Langerhans cells from human cutaneous squamous cell carcinoma induce strong type 1 immunity. J Invest Dermatol 132(6):1645–1655. https://doi.org/10.1038/jid.2012.34
Ginhoux F, Tacke F, Angeli V, Bogunovic M, Loubeau M, Dai X-M, Stanley ER, Randolph GJ, Merad M (2006) Langerhans cells arise from monocytes in vivo. Nat Immunol 7(3):265–273. https://doi.org/10.1038/ni1307
Glick AB, Kulkarni AB, Tennenbaum T, Hennings H, Flanders KC, O’Reilly M, Sporn MB, Karlsson S, Yuspa SH (1993) Loss of expression of transforming growth factor beta in skin and skin tumors is associated with hyperproliferation and a high risk for malignant conversion. Proc Natl Acad Sci U S A 90(13):6076–6080. https://doi.org/10.1073/pnas.90.13.6076
Hawthorn RJ, Murdoch JB, MacLean AB, MacKie RM (1988) Langerhans’ cells and subtypes of human papillomavirus in cervical intraepithelial neoplasia. BMJ 297(6649):643–646. https://doi.org/10.1136/bmj.297.6649.643
Hieronymus T, Zenke M, Baek JH, Sere K (2015) The clash of Langerhans cell homeostasis in skin: should I stay or should I go? Semin Cell Dev Biol 41:30–38. https://doi.org/10.1016/j.semcdb.2014.02.009
Hoeffel G, Wang Y, Greter M, See P, Teo P, Malleret B, Leboeuf M, Low D, Oller G, Almeida F, Choy SHY, Grisotto M, Renia L, Conway SJ, Stanley ER, Chan JKY, Ng LG, Samokhvalov IM, Merad M, Ginhoux F (2012) Adult Langerhans cells derive predominantly from embryonic fetal liver monocytes with a minor contribution of yolk sac–derived macrophages. J Exp Med 209(6):1167–1181. https://doi.org/10.1084/jem.20120340
Hovav AH (2018) Mucosal and skin Langerhans cells - nurture calls. Trends Immunol 39(10):788–800. https://doi.org/10.1016/j.it.2018.08.007
Kaplan DH, Jenison MC, Saeland S, Shlomchik WD, Shlomchik MJ (2005) Epidermal Langerhans cell-deficient mice develop enhanced contact hypersensitivity. Immunity 23(6):611–620. https://doi.org/10.1016/j.immuni.2005.10.008
Kaplan DH, Li MO, Jenison MC, Shlomchik WD, Flavell RA, Shlomchik MJ (2007) Autocrine/paracrine TGFbeta1 is required for the development of epidermal Langerhans cells. J Exp Med 204(11):2545–2552. https://doi.org/10.1084/jem.20071401
Karakok M, Bayazit YA, Ucak R, Ozer E, Kanlikama M, Mumbuc S, Sari I (2003) Langerhans cell related inflammatory reaction in laryngeal squamous cell carcinoma. Auris Nasus Larynx 30(1):81–84. https://doi.org/10.1016/s0385-8146(02)00025-1
Kaur G, Carnelio S, Rao N, Rao L (2009) Expression of E-cadherin in primary oral squamous cell carcinoma and metastatic lymph nodes: an immunohistochemical study. Indian J Dent Res 20(1):71–76
Kindt N, Descamps G, Seminerio I, Bellier J, Lechien JR, Pottier C, Larsimont D, Journe F, Delvenne P, Saussez S (2016) Langerhans cell number is a strong and independent prognostic factor for head and neck squamous cell carcinomas. Oral Oncol 62:1–10. https://doi.org/10.1016/j.oraloncology.2016.08.016
Kissenpfennig A, Henri S, Dubois B, Laplace-Builhe C, Perrin P, Romani N, Tripp CH, Douillard P, Leserman L, Kaiserlian D, Saeland S, Davoust J, Malissen B (2005) Dynamics and function of Langerhans cells in vivo: dermal dendritic cells colonize lymph node areas distinct from slower migrating Langerhans cells. Immunity 22(5):643–654. https://doi.org/10.1016/j.immuni.2005.04.004
Klareskog L, Tjernlund U, Forsum U, Peterson PA (1977) Epidermal Langerhans cells express Ia antigens. Nature 268(5617):248–250. https://doi.org/10.1038/268248a0
La Rocca G, Anzalone R, Corrao S, Magno F, Rappa F, Marasa S, Czarnecka AM, Marasa L, Sergi C, Zummo G, Cappello F (2008) CD1a down-regulation in primary invasive ductal breast carcinoma may predict regional lymph node invasion and patient outcome. Histopathology 52(2):203–212. https://doi.org/10.1111/j.1365-2559.2007.02919.x
Langerhans P (1868) Ueber die Nerven der menschlichen Haut. Archiv für pathologische Anatomie und Physiologie und für klinische Medicin 44(2):325–337. https://doi.org/10.1007/BF01959006
Lee CH, Chang JS, Syu SH, Wong TS, Chan JY, Tang YC, Yang ZP, Yang WC, Chen CT, Lu SC, Tang PH, Yang TC, Chu PY, Hsiao JR, Liu KJ (2015) IL-1beta promotes malignant transformation and tumor aggressiveness in oral cancer. J Cell Physiol 230(4):875–884. https://doi.org/10.1002/jcp.24816
Lewis JM, Burgler CD, Fraser JA, Liao H, Golubets K, Kucher CL, Zhao PY, Filler RB, Tigelaar RE, Girardi M (2015) Mechanisms of chemical cooperative carcinogenesis by epidermal Langerhans cells. J Invest Dermatol 135(5):1405–1414. https://doi.org/10.1038/jid.2014.411
Li T, Yang J, Zhou Q, He Y (2012) Molecular regulation of lymphangiogenesis in development and tumor microenvironment. Cancer Microenviron 5(3):249–260. https://doi.org/10.1007/s12307-012-0119-6
Manickam A, Sivanandham M, Tourkova IL (2007) Immunological role of dendritic cells in cervical cancer. Adv Exp Med Biol 601:155–162. https://doi.org/10.1007/978-0-387-72005-0_16
Matthews K, Leong CM, Baxter L, Inglis E, Yun K, Bäckström BT, Doorbar J, Hibma M (2003) Depletion of Langerhans cells in human papillomavirus type 16-infected skin is associated with E6-mediated down regulation of E-cadherin. J Virol 77(15):8378–8385. https://doi.org/10.1128/JVI.77.15.8378-8385.2003
Merad M, Manz MG, Karsunky H, Wagers A, Peters W, Charo I, Weissman IL, Cyster JG, Engleman EG (2002) Langerhans cells renew in the skin throughout life under steady-state conditions. Nat Immunol 3(12):1135–1141. https://doi.org/10.1038/ni852
Miyasaka K, Hanayama R, Tanaka M, Nagata S (2004) Expression of milk fat globule epidermal growth factor 8 in immature dendritic cells for engulfment of apoptotic cells. Eur J Immunol 34(5):1414–1422. https://doi.org/10.1002/eji.200424930
Modi BG, Neustadter J, Binda E, Lewis J, Filler RB, Roberts SJ, Kwong BY, Reddy S, Overton JD, Galan A, Tigelaar R, Cai L, Fu P, Shlomchik M, Kaplan DH, Hayday A, Girardi M (2012) Langerhans cells facilitate epithelial DNA damage and squamous cell carcinoma. Science 335(6064):104–108. https://doi.org/10.1126/science.1211600
Motegi S, Leitner WW, Lu M, Tada Y, Sardy M, Wu C, Chavakis T, Udey MC (2011) Pericyte-derived MFG-E8 regulates pathologic angiogenesis. Arterioscler Thromb Vasc Biol 31(9):2024–2034. https://doi.org/10.1161/ATVBAHA.111.232587
Muz B, de la Puente P, Azab F, Azab AK (2015) The role of hypoxia in cancer progression, angiogenesis, metastasis, and resistance to therapy. Hypoxia 3:83–92. https://doi.org/10.2147/HP.S93413
Na YR, Seok SH, Kim DJ, Han JH, Kim TH, Jung H, Lee BH, Park JH (2009) Bone morphogenetic protein 7 induces mesenchymal-to-epithelial transition in melanoma cells, leading to inhibition of metastasis. Cancer Sci 100(11):2218–2225. https://doi.org/10.1111/j.1349-7006.2009.01301.x
Nakano T, Oka K, Takahashi T, Morita S, Arai T (1992) Roles of Langerhans’ cells and T-lymphocytes infiltrating cancer tissues in patients treated by radiation therapy for cervical cancer. Cancer 70(12):2839–2844. https://doi.org/10.1002/1097-0142(19921215)70:12<2839::aid-cncr2820701220>3.0.co;2-7
Nakjima S, Moniaga C, Miyachi Y, Kabashima K (2016) Hypoxia inducible factor-1α of Langerhans cell plays a critical role in a murine irritant dermatitis model. J Dermatol Sci 84(1):e3
Ortner D, Tripp CH, Komenda K, Dubrac S, Zelger B, Hermann M, Doppler W, Tymoszuk PZ, Boon L, Clausen BE, Stoitzner P (2017) Langerhans cells and NK cells cooperate in the inhibition of chemical skin carcinogenesis. Onco Targets Ther 6(2):e1260215. https://doi.org/10.1080/2162402X.2016.1260215
Otsuka M, Egawa G, Kabashima K (2018) Uncovering the mysteries of Langerhans cells, inflammatory dendritic epidermal cells, and monocyte-derived Langerhans cell-like cells in the epidermis. Front Immunol 9:1768. https://doi.org/10.3389/fimmu.2018.01768
Ouchi T, Nakato G, Udey MC (2016) EpCAM expressed by murine epidermal Langerhans cells modulates immunization to an epicutaneously applied protein antigen. J Invest Dermatol 136(8):1627–1635. https://doi.org/10.1016/j.jid.2016.04.005
Ouwehand K, Spiekstra SW, Waaijman T, Breetveld M, Scheper RJ, de Gruijl TD, Gibbs S (2012) CCL5 and CCL20 mediate immigration of Langerhans cells into the epidermis of full thickness human skin equivalents. Eur J Cell Biol 91(10):765–773. https://doi.org/10.1016/j.ejcb.2012.06.004
Paduch R (2016) The role of lymphangiogenesis and angiogenesis in tumor metastasis. Cell Oncol 39(5):397–410. https://doi.org/10.1007/s13402-016-0281-9
Parangi S, O’Reilly M, Christofori G, Holmgren L, Grosfeld J, Folkman J, Hanahan D (1996) Antiangiogenic therapy of transgenic mice impairs de novo tumor growth. Proc Natl Acad Sci U S A 93(5):2002–2007. https://doi.org/10.1073/pnas.93.5.2002
Pena-Cruz V, McDonough SM, Diaz-Griffero F, Crum CP, Carrasco RD, Freeman GJ (2010) PD-1 on immature and PD-1 ligands on migratory human Langerhans cells regulate antigen-presenting cell activity. J Invest Dermatol 130(9):2222–2230. https://doi.org/10.1038/jid.2010.127
Pierobon D, Raggi F, Cambieri I, Pelassa S, Occhipinti S, Cappello P, Novelli F, Musso T, Eva A, Castagnoli C, Varesio L, Giovarelli M, Bosco MC (2016) Regulation of Langerhans cell functions in a hypoxic environment. J Mol Med 94(8):943–955. https://doi.org/10.1007/s00109-016-1400-9
Rajesh A, Wise L, Hibma M (2019) The role of Langerhans cells in pathologies of the skin. Immunol Cell Biol 97(8):700–713. https://doi.org/10.1111/imcb.12253
Ratzinger G, Baggers J, de Cos MA, Yuan J, Dao T, Reagan JL, Munz C, Heller G, Young JW (2004) Mature human Langerhans cells derived from CD34+ hematopoietic progenitors stimulate greater cytolytic T lymphocyte activity in the absence of bioactive IL-12p70, by either single peptide presentation or cross-priming, than do dermal-interstitial or monocyte-derived dendritic cells. J Immunol 173(4):2780–2791. https://doi.org/10.4049/jimmunol.173.4.2780
Roman A, Munger K (2013) The papillomavirus E7 proteins. Virology 445(1–2):138–168. https://doi.org/10.1016/j.virol.2013.04.013
Romano E, Cotari JW, Barreira da Silva R, Betts BC, Chung DJ, Avogadri F, Fink MJ, St Angelo ET, Mehrara B, Heller G, Munz C, Altan-Bonnet G, Young JW (2012) Human Langerhans cells use an IL-15R-alpha/IL-15/pSTAT5-dependent mechanism to break T-cell tolerance against the self-differentiation tumor antigen WT1. Blood 119(22):5182–5190. https://doi.org/10.1182/blood-2011-09-382200
Romano E, Rossi M, Ratzinger G, de Cos MA, Chung DJ, Panageas KS, Wolchok JD, Houghton AN, Chapman PB, Heller G, Yuan J, Young JW (2011) Peptide-loaded Langerhans cells, despite increased IL15 secretion and T-cell activation in vitro, elicit antitumor T-cell responses comparable to peptide-loaded monocyte-derived dendritic cells in vivo. Clin Cancer Res 17(7):1984–1997. https://doi.org/10.1158/1078-0432.CCR-10-3421
Rowden G, Lewis MG, Sullivan AK (1977) Ia antigen expression on human epidermal Langerhans cells. Nature 268(5617):247–248. https://doi.org/10.1038/268247a0
Rudat V, Stadler P, Becker A, Vanselow B, Dietz A, Wannenmacher M, Molls M, Dunst J, Feldmann HJ (2001) Predictive value of the tumor oxygenation by means of pO2 histography in patients with advanced head and neck cancer. Strahlenther Onkol 177(9):462–468
Ruiter D, Bogenrieder T, Elder D, Herlyn M (2002) Melanoma-stroma interactions: structural and functional aspects. Lancet Oncol 3(1):35–43. https://doi.org/10.1016/s1470-2045(01)00620-9
Santos I, de Mello RJV, dos Santos IB, dos Santos RA (2010) Quantitative study of Langerhans cells in basal cell carcinoma with higher or lower potential of local aggressiveness. An Bras Dermatol 85(2):165–171. https://doi.org/10.1590/S0365-05962010000200006
Schroder S, Schwarz W, Rehpenning W, Loning T, Bocker W (1988) Dendritic/Langerhans cells and prognosis in patients with papillary thyroid carcinomas. Immunocytochemical study of 106 thyroid neoplasms correlated to follow-up data. Am J Clin Pathol 89(3):295–300. https://doi.org/10.1093/ajcp/89.3.295
Seidel JA, Otsuka A, Kabashima K (2017) Investigating the role of Langerhans cells in primary cutaneous melanoma. J Dermatol Sci 86(2):e73. https://doi.org/10.1016/j.jdermsci.2017.02.214
Semenza GL (2000) Hypoxia, clonal selection, and the role of HIF-1 in tumor progression. Crit Rev Biochem Mol Biol 35(2):71–103. https://doi.org/10.1080/10409230091169186
Seneschal J, Clark RA, Gehad A, Baecher-Allan CM, Kupper TS (2012) Human epidermal Langerhans cells maintain immune homeostasis in skin by activating skin resident regulatory T cells. Immunity 36(5):873–884. https://doi.org/10.1016/j.immuni.2012.03.018
Sgambato JA, Jones BA, Caraway JW, Prasad GL (2018) Inflammatory profile analysis reveals differences in cytokine expression between smokers, moist snuff users, and dual users compared to non-tobacco consumers. Cytokine 107:43–51. https://doi.org/10.1016/j.cyto.2017.11.013
Shevchuk Z, Filip A, Shevchuk V, Kashuba E (2014) Number of Langerhans cells is decreased in premalignant keratosis and skin cancers. Exp Oncol 36(1):34–37
Staquet MJ, Godefroy S, Jacquet C, Viac J, Schmitt D (2001) Vascular endothelial growth factor (VEGF) induces human Langerhans cell migration. Arch Dermatol Res 293(1–2):26–28. https://doi.org/10.1007/s004030000193
Stoitzner P, Green LK, Jung JY, Price KM, Tripp CH, Malissen B, Kissenpfennig A, Hermans IF, Ronchese F (2008) Tumor immunotherapy by epicutaneous immunization requires Langerhans cells. J Immunol 180(3):1991–1998. https://doi.org/10.4049/jimmunol.180.3.1991
Takahara M, Chen S, Kido M, Takeuchi S, Uchi H, Tu Y, Moroi Y, Furue M (2009) Stromal CD10 expression, as well as increased dermal macrophages and decreased Langerhans cells, are associated with malignant transformation of keratinocytes. J Cutan 36(6):668–674. https://doi.org/10.1111/j.1600-0560.2008.01139.x
Tsuge T, Yamakawa M, Tsukamoto M (2000) Infiltrating dendritic/Langerhans cells in primary breast cancer. Breast Cancer Res Treat 59(2):141–152. https://doi.org/10.1023/a:1006396216933
Tsujitani S, Furukawa T, Tamada R, Okamura T, Yasumoto K, Sugimachi K (1987) Langerhans cells and prognosis in patients with gastric carcinoma. Cancer 59(3):501–505. https://doi.org/10.1002/1097-0142(19870201)59:3<501::aid-cncr2820590325>3.0.co;2-h
Valladeau J, Ravel O, Dezutter-Dambuyant C, Moore K, Kleijmeer M, Liu Y, Duvert-Frances V, Vincent C, Schmitt D, Davoust J, Caux C, Lebecque S, Saeland S (2000) Langerin, a novel C-type lectin specific to Langerhans cells, is an endocytic receptor that induces the formation of birbeck granules. Immunity 12(1):71–81. https://doi.org/10.1016/S1074-7613(00)80160-0
Wang Z, Wang W, Chai Q, Zhu M (2019) Langerhans cells control lymphatic vessel function during inflammation via LIGHT-LTbetaR signaling. J Immunol 202(10):2999–3007. https://doi.org/10.4049/jimmunol.1801578
Wu H, Lotan R, Menter D, Lippman SM, Xu XC (2000) Expression of E-cadherin is associated with squamous differentiation in squamous cell carcinomas. Anticancer Res 20(3A):1385–1390
Yasmin N, Bauer T, Modak M, Wagner K, Schuster C, Koffel R, Seyerl M, Stockl J, Elbe-Burger A, Graf D, Strobl H (2013) Identification of bone morphogenetic protein 7 (BMP7) as an instructive factor for human epidermal Langerhans cell differentiation. J Exp Med 210(12):2597–2610. https://doi.org/10.1084/jem.20130275
Zhang H, Wang Y, Hwang ES, He YW (2016) Interleukin-10: an immune-activating cytokine in cancer immunotherapy. J Clin Oncol 34(29):3576–3578. https://doi.org/10.1200/JCO.2016.69.6435
Zhang W, Alt-Holland A, Margulis A, Shamis Y, Fusenig NE, Rodeck U, Garlick JA (2006) E-cadherin loss promotes the initiation of squamous cell carcinoma invasion through modulation of integrin-mediated adhesion. J Cell Sci 119(Pt 2):283–291. https://doi.org/10.1242/jcs.02738
Zhu M, Fu YX (2011) The role of core TNF/LIGHT family members in lymph node homeostasis and remodeling. Immunol Rev 244(1):75–84. https://doi.org/10.1111/j.1600-065X.2011.01061.x
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 The Editor(s) (if applicable) and The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Rajesh, A., Hibma, M. (2020). Novel Concepts: Langerhans Cells in the Tumour Microenvironment. In: Birbrair, A. (eds) Tumor Microenvironment. Advances in Experimental Medicine and Biology, vol 1273. Springer, Cham. https://doi.org/10.1007/978-3-030-49270-0_8
Download citation
DOI: https://doi.org/10.1007/978-3-030-49270-0_8
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-49269-4
Online ISBN: 978-3-030-49270-0
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)