Abstract
Extracellular vesicles (EVs) are membrane-enclosed organelles that serve as biological messengers that mediate cell-cell communication and have been implicated in disease progression. EVs are secreted by various cell types and can be assayed from tissue, cell culture media, and biological fluids collected from animals and human subjects. A special subtype of EVs known as matrix vesicles has been studied as nucleating sites for mineralization in skeletal tissues. More recently, studies have found that EVs derived from calcified vascular tissues have similar properties to matrix vesicles released within bone. This opens up novel avenues for a deeper mechanistic understanding and characterization of vascular calcification through analysis of these EVs. However, these analyses are limited by the small size and extremely complex and heterogeneous nature of the vesicles. The advent of new technologies, many of which were originally developed for analysis of synthetic nanoparticles, has provided new insight into EV properties and function. This chapter focuses on the characterization of EV properties demonstrated by various physical, structural, and biomolecular analyses that have allowed for a more comprehensive description of the initiation of calcification. We will begin by briefly reviewing the properties of calcifying EVs that promote mineralization, followed by a focus on the current discussion on commonly utilized and emerging techniques to measure EV properties. We outline several methodologies and detail the advantages and limitations of each technique, along with possible solutions.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Extracellular vesicles
- Calcification
- Microcalcification
- Mineralization
- Nanoparticle characterization
- Nanoparticle tracking analysis
- Tunable resistive pulse sensing
- Electron microscopy
Extracellular Vesicles in Physiological and Pathological Calcification
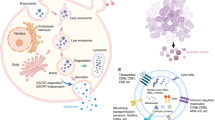
Extracellular vesicles (EVs) are membrane-enclosed vesicles secreted from cells that contain cellular-derived content such as lipids, proteins, and cytokines [1]. EVs have received increased attention for their role as vehicles for intracellular communication as they have the ability to transfer content via membrane fusion to target cells, thereby modulating various physiological and pathological processes in both the target and parental cells. EVs incorporate into target cells through endocytosis, pinocytosis, or phagocytosis [2]. Mammalian cells release a broad range of EVs with diverse features. In the cardiovascular system, EVs have a myriad of physiological roles, including regulation of inflammation and coagulation, as well as activation of endothelial cells and platelets [3,4,5]. These EV-mediated processes are induced by stimulating the target cell surface receptors through bioactive ligands and proteins. The transfer of content to target cells is tightly regulated by the lipid composition in the EV membrane, and reports suggest that the phospholipid phosphatidylserine plays a major role to facilitate the membrane fusion process [6].
In physiological calcification , EVs known as matrix vesicles are enriched in membrane proteins that regulate extracellular matrix mineralization (see Chaps. 16 and 17 for thorough discussions on bone mineralization). Some of the membrane proteins involved in these processes include the calcium-dependent phospholipid-binding annexin protein (annexins I, II, V and VI), as well as enzymes such as tissue non-specific alkaline phosphatase (TNAP) and ectonucleotide pyrophosphatase/phosphodiesterase-1 (ENPP1). These proteins and enzymes are essential to maintain the balance of pyrophosphate and inorganic phosphate for the formation of hydroxyapatite crystals and remodeling of the extracellular matrix [7]. The mineralization process is initiated by inhibition of pyrophosphate generated through the cleavage of nucleotide triphosphates by ENPP1 [8]. Inorganic phosphates that are derived from TNAP-mediated hydrolysis of pyrophosphate are loaded into EVs via transmembrane phosphate transporter proteins and react with calcium ions immobilized on the EV phospholipid bilayer. We have recently shown in silico that negatively charged phosphatidylserine is important in immobilizing positively charged calcium ions [9]. Phosphatidylserine-rich membrane of the EVs coupled with annexin proteins sequesters calcium and phosphate, driving the nucleation of immature minerals [10]. The phosphatidylserine-calcium-phosphate complex functions as an intravesicular niche to form mature apatite. As mineral matures and becomes increasingly crystalline, it can rupture the EV membrane and fuse with the underlying cartilaginous matrix [11], which leads to early mineralization events that are required for bone development and regeneration.
Calcifying EVs are reported to have a diameter in the range of 100–300 nm. In models of medial calcification, calcifying EVs released from vascular smooth muscle cells cultured in media with elevated calcium and phosphate have an average diameter of ~140 nm [12, 13]. Conversely, vascular smooth muscle cells cultured in a pro-calcific media that may recapitulate inflammation-driven intimal calcification (with β-glycerophosphate and L-ascorbic acid) release EVs that appear larger in size with a diameter of >150 nm. Minerals formed during early bone mineralization have similar chemical properties to the minerals deposited during pathological calcification, especially those found in medial and intimal layers of the coronary arteries [14]. This observation suggests that EVs released during pathological calcification may be underpinned by similar mechanisms that control bone mineralization. However, the cellular derivation of calcifying EVs in cardiovascular tissues appears different than those described in bone. One of the mechanisms by which calcifying EVs are formed intracellularly involves the protein sortilin [15]. Sortilin is elevated in calcifying arteries of both the human and murine atheroma and plays a vital role in mineral formation in vitro. The presence of serum sortilin in circulation also predicts the presence and abundance of abdominal aortic calcification [16]. In accordance with the risk predication power of cardiovascular calcification (Chap. 23), the level of serum sortilin also predicts the rate of event-free mortality in 8-year follow-up studies.
Sortilin directly modulates calcification potential by regulating the intracellular trafficking of TNAP into the EVs, which serves to hydrolyze calcification inhibitors (e.g., pyrophosphate) into free phosphate for mineralization. Once released into the extracellular space, these TNAP-positive EVs begin the process of depositing mineral in the vascular wall. We have previously reported that the formation of microcalcification in human smooth muscle cells and a murine model of vascular calcification occurs in four stages (Fig. 5.1) [17]. First, microcalcification is initiated when calcifying EVs accumulate within collagen-poor regions of an atherosclerotic plaque. Second, interactions between these calcifying EVs lead to the formation of aggregates. Third, the nucleation of calcium phosphate within EVs leads to fusion of the EV membranes, forming microcalcifications. Finally, the microcalcification grows through interactions with additional EVs. When formed within a collagen-poor fibrous cap of an atherosclerotic plaque, these microcalcifications contribute to stress accumulation and the detrimental effects of plaque rupture. Indeed, clinical data and in silico studies suggest that plaque stability can be determined by calcification size and morphology of the fibrous cap collagen content in atherosclerosis [18]. Based on these studies, we can better understand how calcifying EVs are initiated and formed during calcification and the implications on cardiovascular morbidity. Future studies are needed to target these processes in order to intervene at an early stage of mineral formation and potentially prevent or reverse microcalcification.
Microcalcification formation within vulnerable fibrous caps of atherosclerotic plaques occurs in four stages. First, calcifying EVs accumulate in collage-poor regions. Second, the EVs aggregate to form a larger structure. Third, the EVs merge as mineralization begins. Fourth, the mature mineral grows from this nucleation niche. (Figure adapted from Ref. [17])
It is clear that EVs are emerging as key players in the development of calcification. It is, however, worth noting that EVs are highly complex and heterogeneous in nature and may exert opposite functional effects in the vasculature. For example, endothelium-derived vesicles show both beneficial and harmful effects through reducing neointima formation [19] and inducing endothelial dysfunction [20], respectively. Therefore, additional efforts should be put in place to standardize the methodologies used to characterize the multifaceted aspect of EVs, so that data generated from these studies can be more comparable. We and others have comprehensively reviewed the roles of EVs in cardiovascular calcification [21,22,23,24,25] and will summarize a few key mediators that are commonly involved in the pathogenesis of vascular calcification in the following section.
Extracellular Vesicles in Vascular Calcification
It is well-established that vascular smooth muscle cell proliferation plays a vital role in the development of the atherosclerotic plaque [26]. More recently, vascular smooth muscle cell-derived EVs have been described as important mediators in vascular calcification in late stages of atherogenesis [17, 27]. Proteomic analysis reveals that intracellular contents of EVs released by vascular cells [28] show similar protein composition to those derived from chondrocytes and osteoblasts [29, 30]. Specifically, EVs derived from these cell types have comparable calcium binding proteins, surface receptors, cytoskeletal proteins, and extracellular matrix components. One of the calcium-dependent enzymes that cross-links with an extracellular matrix protein, transglutaminase 2 (TGM2), was found to be upregulated in EVs derived from the aorta of a rat model of medial calcification [31]. On the other hand, osteoprotegerin (OPG), a crucial regulator of bone homeostasis, was found in EVs derived from vascular smooth muscle cells, which also contained the calcium-binding protein annexin A6 [32]. In this study, Schoppet et al. reported that OPG has anti-calcification effects at physiological concentrations to inhibit the EV-driven mineral nucleation and accumulation of hydroxyapatite on the vascular wall. The initiation and rate of mineralization likely depend on the balance of factors within EVs that promote and inhibit mineral formation.
Pathological changes in calcium homeostasis trigger significant alterations in EV composition, including the formation of nucleating phosphatidylserine-annexin A6 and calcium-phosphate complexes, as well as a deficit in matrix gla protein, which would otherwise inhibit calcification [12, 28]. TNAP is one of the key enzymes that is involved in the pathogenesis of vascular calcification [15, 33]. However, the role of TNAP in vascular smooth muscle cells-derived EVs under pro-calcific conditions is controversial, as some studies reported increased in TNAP activity [34, 35], whereas others reported no changes in TNAP activity after short-term treatment [28]. These contradictory data suggest that the components within pro-calcific media used and duration of experiments may be a crucial point to consider when comparing EVs released under different calcifying conditions. Indeed, studies that reported increased TNAP activity used the combination of β-glycerophosphate and L-ascorbic acid to induce osteogenic differentiation, whereas studies that reported a reduction in TNAP used a high calcium-phosphate media. A recent study that tested the calcification potential of valve interstitial cells (VICs) under different calcifying conditions yielded similar results to that of the smooth muscle cells [36]. Goto et al. reported increased in TNAP activity in VICs cultured in media containing β-glycerophosphate and L-ascorbic acid, an effect that was also passage-dependent. TNAP-dependent calcification was not observed in these primary VICs cultured in high-phosphate media , and these observations are consistent with previous studies in vascular cells. In short, vascular smooth muscle cell- or VIC-derived EVs play a major role in pathological calcification when the balance between pro-calcific activators and anti-calcific regulators is lost. In addition to the role of vascular smooth muscle cells and VICs, macrophages may serve as an important contributor to EVs that nucleate mineral. Particularly in the context of atherosclerosis, EVs are localized to areas of mineral deposition, and this process is highly driven by inflammatory cells and potentiates rupture of vulnerable plaques [37]. Macrophage-derived EVs also play an important role in promoting microcalcification [38]. New et al. found that the calcium-binding proteins S100A9 and annexin A5 are upregulated in calcifying macrophage-derived EVs, and these proteins interact with each other to form a S100A9-annexin A5-phosphatidylserine complex, which serves as a nucleation site for hydroxyapatite. The exact changes that lead to EV-mediated phenomena may depend on the extracellular cues that initiate calcification and the particular cell phenotypes that respond to these cues.
Methods to Analyze Extracellular Vesicle Properties
Recent interest in EV research has led to the advent of various characterization methods to identify EVs released from cells under physiological and pathological conditions. Despite the advances in methodologies to characterize EVs, uncertainty remains in regard to the most appropriate methods of data collection and interpretation due to the small size and complex nature of EVs. In this chapter, we will review the strengths and weaknesses associated with each of the commonly used methodological approaches for the identification of calcifying EVs. In particular, we detail the different methods used for structural analysis of EVs, which can be used in conjunction with conventional physical characterization methods. These fundamental analyses are important in the classification of EVs into subgroups, which can lead to further characterization using techniques such as mass spectroscopy. Through extensive characterization and understanding of the biological functions of these calcifying EVs, potential therapeutic strategies will soon become available by targeting the probable source of mineral formation.
Physical Analysis of Extracellular Vesicles
General Characterization of Extracellular Vesicles
Electromagnetic radiation and its interaction with biological constructs have proven to be an essential tool in research used to study molecular properties of macromolecular structures. Both absorption and scattering by characteristic determinants in molecules result in changes in the energy level or frequency of light. Specifically, analysis of scattered light through subsequent light polarization, angular allocation, and intensity can be used to identify physical properties of matter [39]. Light scattering techniques can be used to study particles in either dynamic or static states. Studying particles in their dynamic state, through a technique known as dynamic light scattering (DLS) , offers a sensitive technique for particle detection. Particles in a solution constantly move due to a random walk motion that becomes apparent at small length scales and through subsequent interaction with neighboring solvent particles. The random walk phenomenon, known as Brownian motion , is related to particle size. Time-dependent measurements in the intensity of scattered light from the particles can determine their hydrodynamic radius based upon Brownian motion relationships [40]. In DLS measurements, incident light exposure on a particular sample leads to light scattering from all particles within the sample. The summation of scattered light gathered from each particle is recorded as a net intensity value. As the particles move, this net intensity fluctuates at a rate dependent on the particle size [40]. Larger particles diffuse at a slower rate, resulting in less fluctuation in net intensity. An autocorrelation function, measuring net intensity at different time intervals, is then used to determine the translational diffusion coefficient (D) for the particles in solution. This diffusion coefficient is incorporated into the Stokes-Einstein relationship (Eq. 5.1) to determine the average hydrodynamic radius (R h) of the particles within the solution, when both the viscosity (η) and absolute temperature (T) of the solution are known [40].
DLS also allows for determination of particle zeta potential, an indication of surface charge. A voltage applied across a sample will result in particle movement. Negatively and positively charged particles move with faster velocities toward positive and negative electrodes, respectively, with the velocity proportional to the magnitude of the particle charge. The particle velocity measured by changes in the DLS frequency can be used to calculate the electrophoretic mobility of the particle , which is then applied to Henry’s equation for zeta potential measurements [41]. This size characterization technique has been used to study both time- and temperature-dependent calcification through the precipitation of primary calciprotein particles (CPPs) to an insoluble, crystalline structure [42, 43]. These studies looked at fetuin-A as a natural inhibitor of calcification and evaluated the endogenous capacity of the protein to limit the progression of calcification. While one group was working to create a more accessible light scattering technique for clinical use, both groups show similar results in their analysis of these CPPs. In relation to both intensity of the subsequent light and measured hydrodynamic radius of particles, a clear distinction was made as the CPPs transitioned from their soluble and smaller state to an insoluble precipitate structure [42, 43].
While DLS measurements provide an efficient and rapid means of analyzing average properties of monodisperse nanoparticles, it is limited in characterization of heterogeneous particles, such as EVs released by cells. DLS sensitivity can only distinguish particles that differ in size by a factor of 3, restricting its utility in differentiating different populations of EVs that have similar size characteristics [44]. Measuring the intensity of scattered light from all the particles within the solution can lead to bias measurements for large particles whose fluctuations in intensity are much lower than smaller particles. Moreover, the use of the Stokes-Einstein relationship to determine the hydrodynamic radius of particles within a sample assumes these particles are of a spherical shape [45].
In short, DLS measurements serve as a general data collection tool that provides average properties of EVs suspended in a media but cannot yield an accurate quantitative measure of EV heterogeneity within a sample. Nonetheless, DLS can be used as a preliminary tool to validate the presence and general characteristics of EVs.
Particle-by-Particle Analysis of Extracellular Vesicles
Nanoparticle tracking analysis (NTA) uses similar methodologies as DLS measurements to determine hydrodynamic size of particles based on Brownian motion [44]. NTA is preferred over DLS measurements, due to the fact that it is capable of distinguishing the hydrodynamic size properties of each particle in a solution by calculating the mean squared displacement of light scattered from individual particles, rather than average intensity fluctuations analyzed by DLS in a frame-by-frame analysis [44]. This technique not only allows for the determination of individual particle characteristics but also provides visualization of these particles in the solution. Since the volume of the imaging window is known, the number of particles visualized at any given time also provides a measure of EV concentration within a sample. In addition to providing concentration data, NTA has other obvious advantages over DLS measurements, with the most important being the removal of bias and increased sensitivity for polydisperse samples [44, 46]. NTA has been used to characterize calcifying EVs released from vascular smooth muscle cells cultured in pro-calcific media to evaluate the relationship between EV aggregation and mineral growth [12, 15, 17, 35, 38] (Fig. 5.2). This is particularly important, as information on aggregation of EVs will determine their fusion mineralization capacity of either forming microcalcification or macrocalcification.
Nanoparticle tracking analyses show increase in diameter as EVs merge to build mineral over the course of 7 days in vitro. (Figure adapted from Ref. [17])
It is, however, worth noting that the accuracy of NTA in particle measurement remains challenging because of the nature of the technique by which particle displacement is calculated. Once a particle diffuses from the field of view, it can no longer be analyzed [46], and relatively low abundance EV populations may not be counted at a significantly high numbers to allow statistically meaningful analyses of properties. This may be a particular problem for analysis of calcifying EV samples, which may represent a small portion of the total EV population in a sample that consists of exosomes, microvesicles, and microparticles.
Flow cytometry (FCM) techniques have recently been developed for EV analyses, and several studies have shown the potential of this technique in analyzing different EV populations [47, 48]. Conventionally, FCM is used to quantitatively assess cells based on their chemical and physical properties [49], and this technique has recently taken its turn into the growing field of EV research. The use of FCM for EV analysis is feasible, as the necessary machinery is already utilized in most laboratories for cell sorting. However, this technique is limited by its sensitivity to collect scattered light from smaller particles, as the setup is only able to reach 200 nm in size [50]. Researchers have worked to normalize FCM measurements for EV detection through a high-sensitive approach which increased concentration detection as well as the detection limit [51], but is it enough for such a novel field of research knowing that EV size can reach a lower limit of around 30 nm? An alternative look at FCM moved from the use of light scattering to properties determined by fluorescence. This enhanced technology which was successfully used by Brussaard et al. in the detection of different viruses offered up to a 50x increase in concentration of detected EVs than conventional methods dependent solely on light scattering [52, 53].
More recently, tunable resistive pulse sensing (TRPS) emerged as a powerful technique to provide particle-by-particle characterization of size and charge properties. It uses the Coulter principle to provide a highly sensitive system for quantitative particle-by-particle characterization (Fig. 5.3). The Coulter principle, originally developed to determine size and concentration of cells in hematological analyses, measures the impedance of nonconductive particles as they disrupt an electric current within a conductive medium. TRPS incorporates a two-compartment setup, divided by a nano-sized pore with electrodes on either side. A voltage is applied to the system with electrolyte solution in each compartment to induce a current through the pore. Particles diluted within electrolyte solution are placed in the upper fluid well compartment. Both applied pressure and electrophoretic mobility result in particle translocation through the pore, increasing the resistivity of the pore to current flow [54]. The current disruption is proportional to the size and charge properties of each particle.
Three different aspects of particle measurements using TRPS can be modified throughout sample reading to ensure maximum sensitivity and accuracy in particle detection. (i) Increasing the voltage applied to the system will increase the current, allowing higher resistivity for particles of smaller sizes. (ii) Increasing the pressure within the system will accelerate particle flow, allowing more accurate measurement of particles from a larger sample pool. (iii) Applying stretch to the nanopore can adapt the measurement to different particle sizes and help prevent blockages. Duration of the current disruption serves as an indicator of charge for each particle. Absolute calculation of zeta potential is also possible from the particle transit time using the Smoluchowski approximation (Eq. 2) [54, 55]. Particle translocation through the nanopore depends on electrophoretic mobility and convective mobility due to pressure applied to the system. The relative contribution of electrophoretic and convective mobility can be measured using calibration particles of a known size and charge prior to sample velocity measurements at a constant voltage (V) and pressure (P), providing the constant values, \( {v}_{x\ Cal}^V \) and \( {v}_{x\ Cal}^P. \)Determination of calibration particle translocation time can be compared to those time-dependent measurements obtained from the sample at different points within the pore. This will provide a particle’s respective velocity relative to its intrinsic and pressure-driven movement. The summation of these velocity values \( \left({v}_{x\ Sample}^i\right) \) is averaged respective to each particle at that point. The zeta potential of both the calibration particles (ξ net Cal) and of the pore itself (ξ m) are known constants and are taken into account during this approximation, as well.
The limitations of TRPS include the short lifespan of the nanopore and difficulties related to choosing the correct nanopore for heterogeneous biological samples. Nanopore sizing is a critical determinant of the range of EVs that can be measured. Therefore, heterogeneous EV samples must be separated by size (e.g., through size chromatography column-based approaches) and measured using size-appropriate nanopores. Biological samples are also prone to aggregation, which can lead to blockage of the nanopore, preventing proper particle-by-particle analysis. The inclusion of nonionic detergents in the electrolyte solution may help prevent aggregation of particles in biological samples.
Adaptation of TRPS methods in newer resistive pulse sensing (RPS) technologies has increased sensitivity in particle analysis. A recently developed RPS technology uses a multifunctional nanopipette that simultaneously measures changes in ionic current and potential through the similar translocation mechanism unique to TRPS analysis but utilizes a nanopipette system that may enhance controllability and reduce blockages [56].
In short, TRPS offers the most accurate quantification of small EVs based upon the Coulter principle, but the technique remains technically challenging and laborious compared to NTA. As TRPS and related techniques continue to develop, physical properties such as size, charge, and concentration of EVs may provide new information on characteristics of EVs released under various conditions (healthy vs diseased). This may contribute to therapeutic advances that can target these EVs to treat vascular calcification.
Structural Analysis of Extracellular Vesicles
The analyses discussed in the previous section have begun to elucidate size and charge characteristics of EVs, but they do not provide direct visualization of EV structure. The smallest EVs are around 30 nm in diameter, smaller than the resolution limits of a standard light microscope. The limitations in light microscopy lie in the consolidation of diffracted light from smaller particles that have a higher index of refraction at the visible light range, resulting in a blurred image [57]. The discovery that moving matter acts similarly to light, a phenomenon described as the wave-particle duality, led to the development of microscopy techniques using electron emission [58]. Due to electron mass being considerably larger than that of a photon, the corresponding wavelength is much lower (based on the matter-wave equation), resulting in lower level diffraction of smaller-sized samples, easy consolidation of light, and resolution below 0.05 nm. All electron microscopy techniques allow for the structural determination of EVs, but methods differ in both sample preparation and output image. Deciding which technique is best for EV analysis is dependent on the purpose of study [59].
Transmission electron microscopy (TEM) analyzes electrons that were able to pass through a specimen. Sample preparation for TEM involves fixation and dehydration of EVs, thus losing their natural conformation. After dehydration, the samples are sectioned into nanometer-sized films and placed on a carbon-coated grid for imaging, which provides the structural analysis of the EVs. TEM offers a higher-resolution image by capturing not only transmitted electrons for structural determination but also those scattered, thus increasing the contrast of the output image. On the other hand, scanning electron microscopy (SEM) offers topographic image of EVs by collecting electrons scattered from the surface. We have previously visualized calcifying EVs released from smooth muscle cells cultured under pro-calcific conditions that mimic those observed in calcified human plaques (Fig. 5.4) [17]. SEM, though similar in sample preparation with fixation and dehydration, does not necessitate the sectioning required for TEM. One limitation of SEM is the production of false ring-like images that can interfere with accurate structural and concentration analyses. Both TEM and SEM require dehydration and fixation of EVs prior to analysis, which can deform the EVs and hinder final size verification. These limitations, while apparent, are known sources of error that should be accounted for during data analysis.
Aggregation of EV and calcification within a calcified human carotid artery plaque. (a) Density-dependent color SEM shows calcifying EVs composing mineral (dense, orange features) in human atheroma. Bar = 2 μm. (b) Magnified image of a large calcification within human atheroma (a, white rectangle). Bar = 500 nm. (c) Calcifying EVs seeded into a three-dimensional collagen hydrogel recapitulate these structures. Bar = 500 nm. White arrows depict dense, orange features of calcium phosphate-rich calcifying EVs. (Figure adapted from Ref. [17])
Cryo-electron microscopy (cryo-EM) provides a more realistic imaging technique for EVs, by utilizing a different fixation method that avoids dehydration and preserves the natural structure [60]. Through the cryo-immobilization technique, water is cooled to a glass-like state with liquid ethane, allowing for particles to remain hydrated [59]. TEM and cryo-TEM are often coupled with immunogold labeling, allowing for further quantification to identify specific surface proteins, verifying the presence of a particular subgroup of EVs [61]. In the context of vascular calcification, calcifying EVs that mediate mineralization contain TNAP, which can be targeted and labeled using this technique to confirm their presence [27].
Atomic force microscopy (AFM) is another common technique used to gain topographic information on EVs. While SEM and TEM techniques involve the direct interaction of an electron beam with the sample, AFM uses laser light to study the deflection of a cantilever coupled with a sharp tip interacting along the surface of particles [62]. Additionally, stiffness of the particles can be obtained through AFM measurements. As the cantilever moves closer to the surface of the particles, molecular forces (e.g., Van der Waals forces) increase the strength of the interaction between the EV surface and the tip. The displacement curve obtained during retraction of the cantilever can be used to determine the stiffness of the particle [63]. Rastering the cantilever across the EV surface results in a high-resolution 3D image, as well as the radius determination [62]. Sample preparation for AFM is straightforward and only involves immobilization of the sample along a mica surface [62, 64]. Though this can disrupt the natural state of the EV, embedding molecules that interact with EV surface proteins can mitigate deformation and allow for accurate size determination [62]. Moreover, similar to immunogold labeling for TEM, the mica surface for AFM can be modified to include antibodies from which EVs can specifically bind. This enhances quantification of differential subgroups of EVs within a sample defined by unique surface proteins [62].
In short, these techniques provide a means for EV structural analyses. As discussed previously, during NTA and DLS analyses, EVs are assumed to be spherical. While less high-throughput, the methods discussed here do not require a priori assumptions about EV shape, and additional structural analyses using these microscopy techniques can help validate assumptions made in the indirect measurements of EV properties.
Biomolecular Analysis of Extracellular Vesicles
The ultimate goal of EV research is usually to determine biomolecular function. Beyond characterizing EV size and structure, methods are needed to analyze EV content. Of particular interest for calcifying EVs is the analysis of proteins and lipid moieties involved in mineralization. Insight into the molecular drivers of mineralization may ultimately lead to the discovery of relevant therapeutic targets.
Mass spectroscopy (MS) is one of the most common screening techniques used to identify the mass-to-charge ratio of ions within a sample, and the use of this technique, specifically high-throughput MS, has been used in protein analysis of EVs [65]. The use of MS in clinical settings has evolved greatly from drug testing, to newborn screening, to identification of blood-borne infections, to most recently providing a real-time look at cancerous tissue during surgery [66]. This screening technique can essentially be used to determine the presence of EVs and the specific lipidomic or proteomic profiles of these EVs, which will provide important clues on their biological functions. For example, MS is used as an unbiased tool to identify proteins that are enriched in calcifying EVs using common gene ontology database [35]. Functional annotation of these specific proteins can be applied to further classify these EVs into subgroups and identify their distinct roles in vascular calcification. Additionally, MS also allows for the determination of cellular derivation and mechanisms of calcifying EV formation from the vascular smooth muscle cells [13, 15]. Data obtained from mass spectroscopy can also be used as biomarkers in the future based on the specific subgroups of lipid or protein that are misregulated under pro-calcific conditions.
An increasing body of evidence from metabolomics analyses suggests that lipids play an important role in directing the physiological and pathophysiological functions of EVs. EVs derived from various sources are enriched in sphingomyelin, cholesterol, phosphatidylserine, and glycosphingolipids [67]. Analysis of these lipid species will help us to characterize the specific lipid composition in the EV bilayer and contribute significantly to our knowledge about the distinct lipid profiles that are essential in maintaining the structural and physical constituents of EVs released under pro-calcific conditions. In brief, EV lysis and lipid extraction methods are typically carried out in a single step through liquid-liquid phase extraction. Analysis of the lipid species is achieved with lysis and extraction using a 4:1 tetrahydrofuran/water phase, followed by the separation of phospholipids and glycophospholipids by diethyl ether and water partitioning [68]. Additionally, EV lipids may be extracted by the Bligh and Dyer liquid-liquid phase extraction method, whereby most lipid species are dissolved in the organic layer of a chloroform/methanol/water (1:1:1 by volume) solution [69]. Lipid species from the organic phase are then separated and analyzed by gas chromatography (GC)-MS, liquid chromatography (LC)-MS, or direct infusion electrospray ionization into a high-resolution mass spectrometer. Due to the complexity and heterogeneity of EVs, accurate mass measurement is often ambiguous for the identification of specific lipid or metabolite species. To overcome the issue, additional analysis from MS experiments is often supplemented by obtaining the elution time (compared to known standards), fragmentation (tandem MS), ion mobility measurements, and relative isotope intensities [70, 71]. Analyses of these distinct lipid compositions present in the EVs will inform us about the stability of these vesicles in various extracellular environments. This may contribute to our knowledge about the specific lipids that confer the stability of EVs in vascular calcification, which is important for future clinical applications that involve liposomal drug delivery method. To ensure sufficient information is gathered regarding a particular subgroup of EVs, robust analyses of the particles such as quantification methods, biodistribution, circulating levels, and their pharmacokinetics must first be established.
In addition to lipid [72] and protein analysis, mass spectroscopy has the ability to identify possible genomic profile [73] of the EVs as well, which is typically determined by next-generation sequencing. Collectively , mass spectroscopy represents a powerful and reliable tool for biomolecular analysis of EVs, which would help to advance the field by identifying specific properties of calcifying EVs that participate in mineralization.
Analysis of Extracellular Vesicle Mineralization
Chapter 11 provides a thorough discussion on methods to visualize and analyze mineral properties. In this section, we briefly discuss methods to analyze and quantify EV-mediated mineralization. The properties discussed in the previous sections (size, charge, and biomolecular content) provide insight into the properties of EVs that may be important in directing calcification. However, analyses of these properties do not directly assess the mineralization potential of EVs. Assays for mineralization in cell cultures and tissue sections are well established and involve the utilization of colorimetric or fluorescent dyes that bind calcium or phosphate. Traditionally, alizarin red S staining of calcium and von Kossa staining of phosphate provide visualization of calcified regions in cultures and tissues and allow for quantification through light absorbance measurements of extracted dye. A method utilizing the color change that occurs when o-cresolphthalein complex 1 reacts with free calcium has also been used to quantify calcium extracted from mineralized tissue and cultures using hydrochloric acid [17, 34, 38]. More recently, the development of fluorescent probes specific to calcium phosphate-based minerals has yielded higher-resolution, and more sensitive, assessment of mineral abundance and morphology (Fig. 5.5) [17, 35]. Longitudinal injection of fluorescent probes into mouse models has also provided a means to track changes in both bone and cardiovascular mineral formation over time [17, 74, 75]. Adaptation of these established assays to measure mineralization directly from EVs, however, is often not straightforward due to EVs’ small size.
Imaging of a near-infrared fluorescent calcium mineral probe (red fluorescence) shows increased mineralization from (a) day 14 to (b) day 21 in smooth muscle cells cultured in pro-calcific media. (c) High-resolution images show calcifications forming within a collagen (green fluorescence) network. Bar = 1 μm. (Figure adapted from Ref. [17])
Similar to difficulties in measurement of the physical and biomolecular properties of EVs, limited starting material and small size present complications when trying to measure mineralization directly from EVs. Initial studies into EV mineralization relied solely on static characterization of associations between mineral and EVs within calcified tissues using electron microscopy (as discussed in section “Structural Analysis of Extracellular Vesicles”). Early seminal studies in the dynamic mechanisms of EV calcification used EVs isolated from mineralized tissue by protease digestion of the extracellular matrix [76, 77]. Nascent mineral scatters light at 340 nm. By suspending isolated EVs in a high calcium-phosphate solution and monitoring absorbance at 340 nm over time, the relative mineralization potential of EVs can be measured. EV samples with higher potential exhibit an increase in absorbancy at 340 nm at earlier time points compared to those with lower mineralization potential. Similar studies have used fluorescent mineral dyes [35] or the colorimetric o-cresolphthalein complex 1 method [38] to measure mineral formation in suspended EVs, which allow for a lower amount of starting material and measurement of EV mineral from cell culture samples. These methods, however, are not conducive to visualize EV-directed mineralization.
Interactions with collagen fibers dictate mineral patterning by EVs in both physiological bone mineralization and pathological vascular calcification. Studies by Chen et al. used the known associations between calcifying EVs and collagen to measure EV-mediated mineral formation on collagen-coated coverslips using the o-cresolphthalein complex 1 method [34]. Building upon these studies, we seeded EVs from human coronary artery smooth muscle cells cultured in pro-calcific media on three-dimensional collagen hydrogels to visualize and quantify mineralization potential [17]. The mineral formed within the hydrogels recapitulates aspects of mineral observed in calcified atheroma, and fluorescent labeling of the EVs with CellTracker™ dyes enabled super-resolution optical imaging of calcifications formed from the merger of individual EVs (Fig. 5.6). The collagen fibers trap and dictate EV associations, serving as a scaffold for mineral morphology. The size and shape of microcalcifications within atherosclerotic plaques determine the accumulation of local stresses that can destabilize the plaque [18]. Subsequent plaque rupture results in artery occlusion and tissue infarction . Therefore, quantification of mineral formation and associated morphologies can provide insight into the pathological consequences of EV-mediated calcification and therapeutic strategies to reduce cardiovascular morbidity.
(a) Structured illumination super-resolution microscopy shows fluorescently labeled EVs aggregating to build a (b, c) microcalcification. Bar = 500 nm. Arrows depict the near-infrared labeled EVs. (Figure adapted from Ref. [17])
Future Perspectives
EVs are vectors that have important roles in the biological system which could modify the pathophysiological mechanisms during the progression of vascular calcification, by releasing either good or harmful mediators. The characterization of EVs released into cell culture media serves as an invaluable step to study the biological functions of these vesicles under pro-calcific conditions in a controlled environment and reproducible manner. This fundamental knowledge gained from in vitro study will provide us with meaningful information on the cellular activation of these EVs during disease progression and could be used as diagnostic or prognostic biomarkers in the future. In this chapter, we have outlined several common analyses used to characterize EVs. It is, however, worth mentioning that there remains the need to overcome some of the common technical challenges to quantify EVs. While extensive efforts have been made to accurately measure both the EV concentration and protein content [78], there is still an unmet need to standardize the EV isolation procedures across laboratories. Hence, a strong research effort is necessary to establish procedures for EV isolation in order to compare the downstream analyses of different EV subgroups. This is especially important for allowing comparison of biological data to define EV dosage for clinical trial purposes. A combination of physical and biomolecular analysis of EVs may represent a major breakthrough in the field to define the concentration, size, and charge of EVs, as well as the protein and/or lipid content in these vesicles under pro-calcific conditions. This would give us valuable information on the dosage to use for clinical applications by titrating the concentration of EVs relative to the protein ratio. As outlined above, the opportunity to employ highly sensitive and accurate methodologies to characterize EVs continues to emerge in the field, and this will certainly help with advancement in the understanding of EV biology. Of note, a better understanding of EV biology together with standardized methods for EV isolation and quantification, functional characterization, as well as establishing potency assays will immensely enhance the future promise for EV-based diagnostic and therapeutic applications for the treatment of vascular calcification.
At present, the limitations of using EV-based diagnostics or therapeutics as a tool for clinical purposes include its applicability in vivo, particularly in the area of calcification. Despite the enormous promise of EVs as therapeutic vectors that can be delivered to different targeted locations within the body system, it requires laborious engineering expertise to optimize the interaction of these EVs with target cells [79]. Moreover, a majority of the current knowledge is derived from studies done in vitro, or with supraphysiological concentrations of EVs that are irrelevant to clinical scenarios observed in patients with vascular calcification. Hence, with the hope to better understand the roles of EVs in vivo, new methods are needed to delineate the mechanisms by which EVs are released temporally and spatially within the vascular wall, as well as from circulating cells. Furthermore, as detailed in section “Biomolecular Analysis of Extracellular Vesicles”, proteomic and lipidomic mapping using matrix-assisted laser desorption/ionization (MALDI) approaches in intact tissue may provide vital information on biomolecular changes in EVs during the progression of calcification. In summary, various methods to assess the characteristics of EVs released in vascular calcification represent a potential path toward future therapeutic avenues that reduce cardiovascular morbidity and mortality.
References
Colombo M, Raposo G, Thery C. Biogenesis, secretion, and intercellular interactions of exosomes and other extracellular vesicles. Annu Rev Cell Dev Biol. 2014;30:255–89.
Mulcahy LA, Pink RC, Carter DR. Routes and mechanisms of extracellular vesicle uptake. Journal Extracell Vesicles. 2014;3:24641.
Brill A, Dashevsky O, Rivo J, Gozal Y, Varon D. Platelet-derived microparticles induce angiogenesis and stimulate post-ischemic revascularization. Cardiovasc Res. 2005;67(1):30–8.
Jansen F, Yang X, Franklin BS, Hoelscher M, Schmitz T, Bedorf J, et al. High glucose condition increases NADPH oxidase activity in endothelial microparticles that promote vascular inflammation. Cardiovasc Res. 2013;98(1):94–106.
Owens AP 3rd, Mackman N. Microparticles in hemostasis and thrombosis. Circ Res. 2011;108(10):1284–97.
Chernomordik L, Kozlov MM, Zimmerberg J. Lipids in biological membrane fusion. J Membr Biol. 1995;146(1):1–14.
Anderson HC. Molecular biology of matrix vesicles. Clin Orthop Relat Res. 1995;314:266–80.
Huang MS, Sage AP, Lu J, Demer LL, Tintut Y. Phosphate and pyrophosphate mediate PKA-induced vascular cell calcification. Biochem Biophys Res Commun. 2008;374(3):553–8.
Pokhrel R, Gerstman BS, Hutcheson JD, Chapagain PP. In silico investigations of calcium phosphate mineralization in extracellular vesicles. J Phys Chem B. 2018;122(14):3782–9.
Wuthier RE, Wu LN, Sauer GR, Genge BR, Yoshimori T, Ishikawa Y. Mechanism of matrix vesicle calcification: characterization of ion channels and the nucleational core of growth plate vesicles. Bone Miner. 1992;17(2):290–5.
Skrtic D, Eanes ED. Membrane-mediated precipitation of calcium phosphate in model liposomes with matrix vesicle-like lipid composition. Bone Miner. 1992;16(2):109–19.
Kapustin AN, Chatrou ML, Drozdov I, Zheng Y, Davidson SM, Soong D, et al. Vascular smooth muscle cell calcification is mediated by regulated exosome secretion. Circ Res. 2015;116(8):1312–23.
Kapustin AN, Schoppet M, Schurgers LJ, Reynolds JL, McNair R, Heiss A, et al. Prothrombin loading of vascular smooth muscle cell-derived exosomes regulates coagulation and calcification. Arterioscler Thromb Vasc Biol. 2017;37(3):e22–32.
New SE, Aikawa E. Role of extracellular vesicles in de novo mineralization: an additional novel mechanism of cardiovascular calcification. Arterioscler Thromb Vasc Biol. 2013;33(8):1753–8.
Goettsch C, Hutcheson JD, Aikawa M, Iwata H, Pham T, Nykjaer A, et al. Sortilin mediates vascular calcification via its recruitment into extracellular vesicles. J Clin Invest. 2016;126(4):1323–36.
Goettsch C, Iwata H, Hutcheson JD, O’Donnell CJ, Chapurlat R, Cook NR, et al. Serum Sortilin associates with aortic calcification and cardiovascular risk in men. Arterioscler Thromb Vasc Biol. 2017;37(5):1005–11.
Hutcheson JD, Goettsch C, Bertazzo S, Maldonado N, Ruiz JL, Goh W, et al. Genesis and growth of extracellular-vesicle-derived microcalcification in atherosclerotic plaques. Nat Mater. 2016;15(3):335–43.
Kelly-Arnold A, Maldonado N, Laudier D, Aikawa E, Cardoso L, Weinbaum S. Revised microcalcification hypothesis for fibrous cap rupture in human coronary arteries. Proc Natl Acad Sci U S A. 2013;110(26):10741–6.
Jansen F, Stumpf T, Proebsting S, Franklin BS, Wenzel D, Pfeifer P, et al. Intercellular transfer of miR-126-3p by endothelial microparticles reduces vascular smooth muscle cell proliferation and limits neointima formation by inhibiting LRP6. J Mol Cell Cardiol. 2017;104:43–52.
Brodsky SV, Zhang F, Nasjletti A, Goligorsky MS. Endothelium-derived microparticles impair endothelial function in vitro. Am J Physiol Heart Circ Physiol. 2004;286(5):H1910–5.
Yang W, Zou B, Hou Y, Yan W, Chen T, Qu S. Extracellular vesicles in vascular calcification. Clin Chim Acta. 2019;499:118–22.
Bakhshian Nik A, Hutcheson JD, Aikawa E. Extracellular vesicles as mediators of cardiovascular calcification. Front Cardiovasc Med. 2017;4:78.
Blaser MC, Aikawa E. Roles and regulation of extracellular vesicles in cardiovascular mineral metabolism. Front Cardiovasc Med. 2018;5:187.
Zhang C, Zhang K, Huang F, Feng W, Chen J, Zhang H, et al. Exosomes, the message transporters in vascular calcification. J Cell Mol Med. 2018;22(9):4024–33.
Liberman M, Marti LC. Vascular calcification regulation by exosomes in the vascular wall. Adv Exp Med Biol. 2017;998:151–60.
Libby P, Ridker PM, Hansson GK. Inflammation in atherosclerosis: from pathophysiology to practice. J Am Coll Cardiol. 2009;54(23):2129–38.
Krohn JB, Hutcheson JD, Martinez-Martinez E, Aikawa E. Extracellular vesicles in cardiovascular calcification: expanding current paradigms. J Physiol. 2016;594(11):2895–903.
Kapustin AN, Davies JD, Reynolds JL, McNair R, Jones GT, Sidibe A, et al. Calcium regulates key components of vascular smooth muscle cell-derived matrix vesicles to enhance mineralization. Circ Res. 2011;109(1):e1–12.
Balcerzak M, Malinowska A, Thouverey C, Sekrecka A, Dadlez M, Buchet R, et al. Proteome analysis of matrix vesicles isolated from femurs of chicken embryo. Proteomics. 2008;8(1):192–205.
Xiao Z, Camalier CE, Nagashima K, Chan KC, Lucas DA, de la Cruz MJ, et al. Analysis of the extracellular matrix vesicle proteome in mineralizing osteoblasts. J Cell Physiol. 2007;210(2):325–35.
Chen NX, O'Neill K, Chen X, Kiattisunthorn K, Gattone VH, Moe SM. Transglutaminase 2 accelerates vascular calcification in chronic kidney disease. Am J Nephrol. 2013;37(3):191–8.
Schoppet M, Kavurma MM, Hofbauer LC, Shanahan CM. Crystallizing nanoparticles derived from vascular smooth muscle cells contain the calcification inhibitor osteoprotegerin. Biochem Biophys Res Commun. 2011;407(1):103–7.
Hutcheson JD, Blaser MC, Aikawa E. Giving calcification its due: recognition of a diverse disease: a first attempt to standardize the field. Circ Res. 2017;120(2):270–3.
Chen NX, O’Neill KD, Chen X, Moe SM. Annexin-mediated matrix vesicle calcification in vascular smooth muscle cells. J Bone Miner Res. 2008;23(11):1798–805.
Hutcheson JD, Goettsch C, Pham T, Iwashita M, Aikawa M, Singh SA, et al. Enrichment of calcifying extracellular vesicles using density-based ultracentrifugation protocol. J Extracell Vesicles. 2014;3:25129.
Goto S, Rogers MA, Blaser MC, Higashi H, Lee LH, Schlotter F, et al. Standardization of human calcific aortic valve disease in vitro modeling reveals passage-dependent calcification. Front Cardiovasc Med. 2019;6:49.
Hutcheson JD, Maldonado N, Aikawa E. Small entities with large impact: microcalcifications and atherosclerotic plaque vulnerability. Curr Opin Lipidol. 2014;25(5):327–32.
New SE, Goettsch C, Aikawa M, Marchini JF, Shibasaki M, Yabusaki K, et al. Macrophage-derived matrix vesicles: an alternative novel mechanism for microcalcification in atherosclerotic plaques. Circ Res. 2013;113(1):72–7.
Berne BJ, Pecora R. Dynamic light scattering: with applications to chemistry, biology, and physics. Mineola, New York: Dover Publications; 2000.
Hassan PA, Rana S, Verma G. Making sense of Brownian motion: colloid characterization by dynamic light scattering. Langmuir. 2015;31(1):3–12.
Bhattacharjee S. DLS and zeta potential – what they are and what they are not? J Control Release. 2016;235:337–51.
Pasch A, Farese S, Gräber S, Wald J, Richtering W, Floege J, et al. Nanoparticle-based test measures overall propensity for calcification in serum. J Am Soc Nephrol. 2012;23(10):1744–52.
Heiss A, Duchesne A, Denecke B, Grötzinger J, Yamamoto K, Renné T, et al. Structural basis of calcification inhibition by α2-HS glycoprotein/Fetuin-A. J Biol Chem. 2003;278(15):13333–41.
Filipe V, Hawe A, Jiskoot W. Critical evaluation of Nanoparticle Tracking Analysis (NTA) by NanoSight for the measurement of nanoparticles and protein aggregates. Pharm Res. 2010;27(5):796–810.
Svedberg T, Rinde H. The determination of the distribution of size of particles in disperse systems1. J Am Chem Soc. 1923;45(4):943–54.
Malloy A, Carr B. Nanoparticle tracking analysis – the Halo™ System. Particle & Particle Systems Characterization. 2006;23(2):197–204.
de Rond L, Libregts S, Rikkert LG, Hau CM, van der Pol E, Nieuwland R, et al. Refractive index to evaluate staining specificity of extracellular vesicles by flow cytometry. J Extracell Vesicles. 2019;8(1):1643671.
Shen W, Guo K, Adkins GB, Jiang Q, Liu Y, Sedano S, et al. A single Extracellular Vesicle (EV) flow cytometry approach to reveal EV heterogeneity. Angew Chem Int Ed Engl. 2018;57(48):15675–80.
Shapiro HM. Practical flow cytometry. Hoboken, New Jersey: Wiley; 2005.
Chandler W, Yeung W, Tait J. A new microparticle size calibration standard for use in measuring smaller microparticles using a new flow cytometer. J Thromb Haemost. 2011;9(6):1216–24.
Robert S, Lacroix R, Poncelet P, Harhouri K, Bouriche T, Judicone C, et al. High-sensitivity flow cytometry provides access to standardized measurement of small-size microparticles–brief report. Arteriosclerosis, Thrombosis, and Vascular Biology. 2012;32(4):1054–8.
Brussaard CPD, Marie D, Bratbak G. Flow cytometric detection of viruses. J Virol Methods. 2000;85(1–2):175–82.
Arraud N, Gounou C, Linares R, Brisson AR. A simple flow cytometry method improves the detection of phosphatidylserine-exposing extracellular vesicles. J Thromb Haemost. 2015;13(2):237–47.
Blundell ELCJ, Vogel R, Platt M. Particle-by-particle charge analysis of DNA-modified nanoparticles using tunable resistive pulse sensing. Langmuir. 2016;32(4):1082–90.
Vogel R, Pal AK, Jambhrunkar S, Patel P, Thakur SS, Reátegui E, et al. High-resolution single particle zeta potential characterisation of biological nanoparticles using tunable resistive pulse sensing. Sci Rep. 2017;7:17479.
Panday N, Qian G, Wang X, Chang S, Pandey P, He J. Simultaneous ionic current and potential detection of nanoparticles by a multifunctional nanopipette. ACS Nano. 2016;10(12):11237–48.
Shaked NT, Zalevsky Z, Satterwhite LL. Biomedical optical phase microscopy and nanoscopy. Oxford, UK: Elsevier Science; 2012.
Goodhew PJ, Humphreys J. Electron microscopy and analysis. Boca Raton, Florida: CRC Press; 2000.
Chuo ST-Y, Chien JC-Y, Lai CP-K. Imaging extracellular vesicles: current and emerging methods. J Biomed Sci. 2018;25:91.
Choi H, Mun JY. Structural analysis of exosomes using different types of electron microscopy. Appl Microscopy. 2017;47(3):171–5.
Cizmar P, Yuana Y. Detection and characterization of extracellular vesicles by transmission and cryo-transmission electron microscopy, Extracellular vesicles. New York, NY: Springer; 2017. p. 221–32.
Szatanek R, Baj-Krzyworzeka M, Zimoch J, Lekka M, Siedlar M, Baran J. The methods of choice for Extracellular Vesicles (EVs) characterization. Int J Mol Sci. 2017;18(6):1153.
Sokolov I, Dokukin ME, Guz NV. Method for quantitative measurements of the elastic modulus of biological cells in AFM indentation experiments. Methods. 2013;60(2):202–13.
Binnig G, Quate CF, Gerber C. Atomic force microscope. Phys Rev Lett. 1986;56(9):930–3.
Choi D-S, Kim D-K, Kim Y-K, Gho YS. Proteomics of extracellular vesicles: exosomes and ectosomes. Mass Spectrom Rev. 2015;34(4):474–90.
Jannetto PJ, Fitzgerald RL. Effective use of mass spectrometry in the clinical laboratory. Clin Chem. 2016;62(1):92–8.
Record M, Carayon K, Poirot M, Silvente-Poirot S. Exosomes as new vesicular lipid transporters involved in cell-cell communication and various pathophysiologies. Biochim Biophys Acta. 2014;1841(1):108–20.
Del Boccio P, Raimondo F, Pieragostino D, Morosi L, Cozzi G, Sacchetta P, et al. A hyphenated microLC-Q-TOF-MS platform for exosomal lipidomics investigations: application to RCC urinary exosomes. Electrophoresis. 2012;33(4):689–96.
Bligh EG, Dyer WJ. A rapid method of total lipid extraction and purification. Can J Biochem Physiol. 1959;37(8):911–7.
Kliman M, May JC, McLean JA. Lipid analysis and lipidomics by structurally selective ion mobility-mass spectrometry. Biochim Biophys Acta. 2011;1811(11):935–45.
Ecker J, Scherer M, Schmitz G, Liebisch G. A rapid GC-MS method for quantification of positional and geometric isomers of fatty acid methyl esters. J Chromatogr B Analyt Technol Biomed Life Sci. 2012;897:98–104.
Hu T, Zhang JL. Mass-spectrometry-based lipidomics. J Sep Sci. 2018;41(1):351–72.
Gupta N, Benhamida J, Bhargava V, Goodman D, Kain E, Kerman I, et al. Comparative proteogenomics: combining mass spectrometry and comparative genomics to analyze multiple genomes. Genome Res. 2008;18(7):1133–42.
Aikawa E, Aikawa M, Libby P, Figueiredo JL, Rusanescu G, Iwamoto Y, et al. Arterial and aortic valve calcification abolished by elastolytic cathepsin S deficiency in chronic renal disease. Circulation. 2009;119(13):1785–94.
Aikawa E, Nahrendorf M, Figueiredo JL, Swirski FK, Shtatland T, Kohler RH, et al. Osteogenesis associates with inflammation in early-stage atherosclerosis evaluated by molecular imaging in vivo. Circulation. 2007;116(24):2841–50.
Genge BR, Wu LN, Wuthier RE. Kinetic analysis of mineral formation during in vitro modeling of matrix vesicle mineralization: effect of annexin A5, phosphatidylserine, and type II collagen. Anal Biochem. 2007;367(2):159–66.
Genge BR, Wu LN, Wuthier RE. In vitro modeling of matrix vesicle nucleation: synergistic stimulation of mineral formation by annexin A5 and phosphatidylserine. J Biol Chem. 2007;282(36):26035–45.
Webber J, Clayton A. How pure are your vesicles? J Extracell Vesicles. 2013;2:19861.
Vader P, Mol EA, Pasterkamp G, Schiffelers RM. Extracellular vesicles for drug delivery. Adv Drug Deliv Rev. 2016;106(Pt A):148–56.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Ng, H.H., Molina, J.E., Hutcheson, J.D. (2020). Calcifying Extracellular Vesicles: Biology, Characterization, and Mineral Formation. In: Aikawa, E., Hutcheson, J. (eds) Cardiovascular Calcification and Bone Mineralization. Contemporary Cardiology. Humana, Cham. https://doi.org/10.1007/978-3-030-46725-8_5
Download citation
DOI: https://doi.org/10.1007/978-3-030-46725-8_5
Published:
Publisher Name: Humana, Cham
Print ISBN: 978-3-030-46724-1
Online ISBN: 978-3-030-46725-8
eBook Packages: MedicineMedicine (R0)