Abstract
The endocannabinoid (eCB) system comprises endogenously produced cannabinoids (CBs), enzymes of their production and degradation, and CB-sensing receptors and transporters. The eCB system plays a critical role in virtually all stages of animal development. Studies on eCB system components and their physiological role have gained increasing attention with the rising legalization and medical use of marijuana products. The latter represent exogenous interventions that target the eCB system. This chapter summarizes knowledge in the field of CB contribution to gametogenesis, fertilization, embryo implantation, fetal development, birth, and adolescence-equivalent periods of ontogenesis. The material is complemented by the overview of data from our laboratory documenting the functional presence of the eCB system within cerebral arteries of baboons at different stages of development.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
2.1 Introduction
Humans have been consuming cannabis in the form of herbs since ancient times [1]. Although adverse reactions and high doses of cannabinoid preparations may trigger dysphoria [2], low-to-moderate consumption confers analgesic, anxiolytic, and antiemetic properties [3,4,5,6]. The modern understanding of mechanisms that stand behind physiological effects of cannabis consumption started to emerge in the middle of twentieth century with the isolation and characterization of the main psychoactive substance in Cannabis sativa plant – Δ9-tetrahydrocannabinol (THC) [1]. These findings were followed by the discovery of the first cannabinoid receptor (CB1), also by structure elucidation and isolation of endogenously produced cannabinoids anandamide (AEA) and 2-arachidonoylglycerol (2-AG) [1]. Although cannabis preparations currently are used primarily for recreational purposes, they are also consumed for medical reasons: to reduce nausea and vomiting, relieve symptoms associated with neurological disorders, reduce intraocular pressure in glaucoma patients, and as an analgesic remedy [1, 7]. Moreover, CB-based preparations have been increasingly recognized as having therapeutic potential for treatment of numerous pathological conditions, including depression, epilepsy, anxiety-related disorders, and obesity [8,9,10,11,12].
The endocannabinoid (eCB) system is comprised of endogenously produced CBs, their receptors, as well as eCB synthesis, degradation enzymes, and transporting molecules [13]. The eCB system plays a crucial role at all stages of human early development, stemming from the influence over gametogenesis and embryo implantation, spreading into control of nervous system development, peripheral organogenesis, and finishing with postnatal development [14]. Thus, studies of the eCB system help to delineate fundamentals of development and pinpoint potential sites of pharmacological interventions against prevalent developmental disorders. In addition, the understanding of mechanisms that govern eCB-mediated control over ontogenesis will help to expand our knowledge on the consequences of prenatal exposure to marijuana . The latter is reported to affect 3.9–7% of pregnancies [15], reaching even higher numbers (13% of meconium samples) within high-risk populations [16].
Remarkably, there is no acute toxicity to the major psychoactive substance in marijuana – THC [2]. Yet, THC consumption leads to a plethora of physiological and psychological effects [2, 17, 18], reflecting the complexity of the eCB system and its susceptibility to exogenous interventions. Widening legalization of marijuana use, development of synthetic approaches to obtain a “transgenic pot,” and the growing number of pharmaceutical agents that target eCB signaling are reasons that call for comprehensive understanding of the side effects and risks associated with modifications of eCB function.
This chapter summarizes knowledge in the field of CB contribution into gametogenesis, fertilization, embryo implantation, fetal development, birth, and adolescence-equivalent periods of ontogenesis. The literature overview in each section starts with the data on rodents and then gradually shifts to humans. The material is complemented by data from our laboratory documenting the functional presence of the eCB system within cerebral arteries of baboons at different stages of development.
2.2 Brief Overview of eCB System: From Genes to Products
Upon demand, eCBs are synthesized de novo using hydrolyzed lipid precursors from cellular membrane [14]. The two most widely studied endogenously produced CBs are AEA and 2-AG . AEA belongs to the N-acylethanolamine (NAE) family of lipid mediators that represent CB-related compounds. For instance, N-palmitoylethanolamine is able to activate cannabinoid receptors [19, 20]. The physiological role of NAEs is being actively investigated [21,22,23]. AEA synthesis originates from the rate-limiting step of the N-acylation of phosphatidylethanolamine rendering N-acylphosphatidylethanolamine (NAPE) [24]. One of the major pathways in AEA synthesis is mediated by N-acylphosphatidylethanolamine-specific phospholipase D (NAPE-PLD) that hydrolyses NAPE into AEA [24]. Other pathways engage phosphatase PTPN22 [25], α,β-hydrolase domain 4 (ABHD4) [26], and glycerophosphodiesterase (GDE1) [27].
The major synthetic pathway of 2-AG is presented as a two-step reaction. The first step is initiated upon phospholipase C activation and results in the generation of diacylglycerol from phosphatidylinositol. The second step, resulting in 2-AG release, is carried out by a membrane-bound diacylglycerol lipase (DAGLα/β) [24, 28].
Cell types that are most actively involved with eCB production are still under investigation, but likely represent quite an exhaustive catalog [29]. Upon production and release, eCBs are quickly degraded by hydrolytic enzymes. Fatty acid amide hydrolase (FAAH) largely enables AEA degradation, with additional contribution from other enzymes such as cyclooxygenase-2 (COX-2) [30,31,32,33]. 2-AG is largely processed by the monoacylglycerol lipase (MAGL) with additional contribution from α,β-hydrolases 6 and 12 [34, 35]. The relative contribution of these enzymes into 2-AG catabolism is tissue/cell specific [34, 35].
CB receptors are presented by canonical receptors of type 1 (CB1) and 2 (CB2) that are Gi/o protein-coupled receptors exhibiting constitutive activity [36,37,38,39,40,41].
CB1 receptors are widely expressed in numerous neuronal populations [42], within glia [43, 44], and are also found in peripheral organs such as adrenal gland, heart, lung, prostate, uterus, ovary, testis, bone marrow, thymus, and tonsils [45, 46]. Presence of a “pre-nervous” eCB system operating via transient receptor potential (TRP) protein orthologs has been proposed in invertebrate echinoderms (sea urchin, starfish) [47]. However, mammalian CB1 receptor ortholog-coding genes are absent in commonly studied nonvertebrate species such as Drosophila melanogaster and Caenorhabditis elegans [48]. To some extent, the lack of a CB1 receptor ortholog in invertebrate species poses limitations on the choice of animal models for CB-related studies. However, human CB1 ortholog-coding genes are described in a variety of vertebrates including fish, amphibians, avian species, and nonhuman primates [48,49,50].
Although CB2 receptors have been detected in glia [51, 52] and in specific areas of the brain [52,53,54,55], they are also attributed as CB receptors of predominantly peripheral tissue locations that play a central role in immunity [42, 45, 46, 56].
Stimulation of CB receptors results in a number of signaling events, including inhibition of adenylate cyclase, activation of mitogen-activated protein kinase (MAPK) signaling, and modulation of ion channels’ activity [36, 37, 57,58,59,60,61,62,63,64,65]. For instance, CBs target calcium, potassium, and TRP channel families [66, 67], either directly or via secondary signaling events. Besides canonical CB receptors, G protein-coupled receptors GPR55 and GPR119 are advanced as eCB sensors [68].
One must recognize that the eCB system is under constant control from various physiological stimuli, such as hormonal levels. For example, progesterone and estrogen regulate AEA level and expression of FAAH [69]. Also, FAAH in human lymphocytes is upregulated by progesterone [70]. Neither AEA nor THC modifies the level of follicle stimulating hormone; however, AEA decreases while THC increases growth hormone production [71]. In rats, prolonged glucocorticoid treatment decreases CB1 receptor density in the hippocampus [72].
ECB controls a wide range of physiological processes that include, but are not limited to, energy metabolism , inflammation, cardiovascular function, etc. [11, 12]. Thus, it comes as no surprise that a dysfunctional eCB system frequently underlies common human pathologies. The search for mechanisms of prevalent disorders, and studies of novel medications, both feed interest in eCB system functions, including its role in ontogenesis.
2.3 Cannabinoids in Fertility and Gametogenesis
ECB system components are present in virtually any reproductive tissue/organ [13, 73]. Early work described the ability of AEA to diminish sperm fertilizing capacity in sea urchins by inhibiting the acrosome reaction [74]. The CB2 receptor is detected in mouse Sertoli cells [75]. In human oocytes, both CB1 and CB2 receptors have been detected by means of reverse transcription polymerase chain reaction (PCR) and Western blotting [76].
The selective activation of the CB2 receptor induces progression of spermatogonia towards meiosis, and thus plays a critical role in spermatogenesis [77]. Notably, a mouse study reports a high amount of 2-AG in the caput (head) of the epididymis [78]. In this compartment, sperm cells are immobile or do not possess consistent motility. However, in the epididymis tail, 2-AG amount is lower, and such a gradient in 2-AG levels is believed to empower caudal spermatozoa with physiologically necessary motility via a CB1 receptor-mediated mechanism that involves the CB1 receptor on the sperm cell membrane [78]. In humans, reduction in viability characteristics and acrosome reaction of mature sperm is documented in response to AEA and is mediated by the CB1 receptor [69, 79].
Plasma levels of AEA fluctuate with the female cycle. The highest levels are observed during ovulation and follicular phase, while the lowest are reported during luteal phase [80,81,82]. ECB activity exerts an effect on hormonal production, as reported for AEA- and THC-driven downregulation of luteinizing hormone and prolactin levels in ovariectomized rats [71]. THC, however, has been found to inhibit ovulation by suppressing the plasma levels of follicle-stimulating hormone and luteinizing hormone in rats when animals were exposed to THC on the day of proestrus [83].
Clinical observations in human population concur on the risks of CB exposure during periconception [84, 85]. In particular, heavy use of marijuana and cannabis-derived psychoactive products is associated with decreased female fertility, loss of pregnancy, and embryotoxicity [86, 87]. Chronic marijuana use also decreases male fertility in humans and in animal models due to reduced testosterone production, sperm mobility and viability [88,89,90]. Linkage between the phenomenology of CB’s effect on fertility and molecular players that enable such action represents an area of active investigation [84, 85].
2.4 Embryonic Development
Zebrafish Danio rerio has been emerging as an important model for studying the role of eCB and consequences of environmental CB exposure in development [91, 92]. Use of this model allows tracing of eCB system gene expression using qPCR in zebrafish embryos throughout 1–120 h post-fertilization. Analysis reveals diverse patterns of eCB system gene expression [91]. For example, low levels of cnr1, gpr55a, and abhd6 expression are detected throughout development [91]. In contrast, expression levels of cnr2, cnrip1a and dagl family are relatively high [91]. Expression levels of naaa1a and abhd12 are progressively decreased, while expression of ptgs2a and mgll is increased throughout development [91].
A whole-mount in situ hybridization study on chick embryos detects the presence of CB1 gene expression within the first-appeared neurons of the central nervous system (within hindbrain, as early as stage 10 in the chick), followed by appearance within the peripheral nervous system (ophthalmic trigeminal placode) at stage 11 [93]. After these early milestones, CB1 expression is detected in other neuronal populations, such as within vestibuloacoustic, epibranchial ganglions and dorsal root ganglia. Notably, CB1 expression is not uniquely present in neurons. For example, CB1 expression is detected in the ventral forebrain that does not produce neurons in early development [93]. In addition, CB1 expression is detected in the mesoderm. Although neurons are showing CB1 expression very early on, the expression disappears at later stages of chick development [93]. Expression of CB2, TRPV1 and GPR55 is not apparent in chick embryonic central nervous system during development [94]. At early stages of nervous system establishment, eCB system is believed to play a critical role in axonal growth and formation of synaptic connections. Indeed, treatment of chick embryo central nervous system explants with CB1 receptor antagonist AM251 results in defective axonal growth and fasciculation [94]. With regards to other component of the eCB system, DAGL α and β isoforms are widely expressed throughout the embryonic chicken brain, while MAGL is only expressed at later stages [94].
A combination of qPCR, mass spectroscopy, immunohistochemistry and Western blotting detects the presence of eCB system components in chick and mouse embryos at stages 9–11 and E8.75, respectively [41]. These time points correspond to the pre-neuronal phase of early development [95] and represent post-coital days 22–26 of human gestation [41]. An additional study utilizing an agonist-stimulated [35S]GTPγS binding assay documents G protein activation in the brain primordium of chick embryos at stages 9 to 11 in presence of CB1 receptor agonist CP-55,940 [41]. This activation vanishes following pre-treatment of samples with the inverse agonist of CB1 receptor SR141716A [41].
In mammals, a balanced eCB system is crucial for successful early pregnancy. At this stage, synchronization of embryo development with uterine receptivity for implantation is central for maintaining viable pregnancy. The eCB system has been shown to play a critical role at all stages of such synchronization, starting from the development of the preimplantation embryo, its movement through oviduct, throughout implantation and placenta development. AEA synthesis and degradation enzymes NAPE-PLD and FAAH, respectively, are expressed at the two-cell stage of embryonic development [69, 96]. While the CB1 receptor is detected from the four-cell stage, CB2 is found as early as the one-cell stage of embryonic development [69, 96]. Systematic studies point at the CB1 receptor and CB1-mediated signaling as critical players in early development. In the mouse model, only CB1 receptor is present in the maternal oviduct and uterus, while both CB1 and CB2 receptors are detected in preimplantation embryo [86, 87, 97]. Cross-talk between maternal and embryonic CB systems is at the center of successful early pregnancy and development. Indeed, CB1, CB2, or double knock-out mice show asynchronous embryo development during early pregnancy [86, 87, 97]. Remarkably, the development is rescued when knock-out females are mated with wild-type males, pointing at the ability of heterozygous embryos to navigate the proper timing of development and disregard the abnormal maternal CB knock-out environment [86, 87, 97].
Movement of the preimplantation embryo through the maternal oviduct ensures a path to implantation. CB1 knock-out mice show 40% pregnancy loss at this stage [86, 87, 97]. Unlike embryo development, movement along the oviduct cannot be restored by mating CB1 knock-out females with wild type males [86, 87, 97]. Thus, at this stage, maternal factors gain critical weight over embryonic characteristics of the CB system. It is noted that embryos that fail to move to implantation site, still retain their quality, as they could be implanted into pseudopregnant recipient uteri [86, 87, 97]. Implantation of normal embryos into pseudopregnant recipient uteri of CB1 knock-out mice also renders non-developing pregnancies [86, 87, 97]. This finding provides independent verification of the critical role of maternal CB characteristics in controlling embryo movement through the oviduct.
Mechanistic studies reveal a closely coordinated cross-talk between CB1-mediated and adrenergic signaling in control of oviduct motility. Loss of CB1 function increases noradrenaline release from adrenergic nerve terminals and increases smooth muscle contractility via alpha-adrenergic receptor (α-AR) preventing embryo movement. In contrast, CB1 receptor stimulation relaxes oviduct muscle and promotes embryo movement [97]. Consistent with observations in animal models, reduced CB1 expression in Fallopian tubes is detected during ectopic pregnancy in humans [98].
Last but not least, CB tone is central for embryo implantation. This process is tightly controlled by hormonal release of estrogens and progesterone. While progesterone primes the uterus for implantation, estradiol and its metabolite 4-hydroxy-17β-estradiol, produced in the uterus, mediate blastocyst activation for implantation [87, 99]. It has been well established that lower levels of CB1 receptors in the blastocyst and a decrease in uterine AEA levels are crucial for sustaining the “window” of uterine receptivity [86, 87, 97,98,99,100]. In the blastocyst, CB1 expression is lower during the activated state when compared to the dormant blastocyst [101]. In uterus, higher levels of AEA, NAPE-PLD activity, and NAPE-PLD mRNA are detected in nonreceptive uterine states compared to receptive uteri [102, 103]. Of note, AEA levels in the uterus, similar to other organs (see below), are dramatically lower than those of 2-AG [13].
Studies in animal models are closely correlated with findings in humans: elevated plasma AEA levels are detected in women with nonviable pregnancies, while lower AEA is associated with positive pregnancy outcome [82, 104,105,106]. Moreover, decreased FAAH activity is detected in peripheral lymphocytes of women with pregnancy failure [82, 104, 105]. Low activity of placental FAAH, together with elevated CB1 levels, characterize human miscarriages, while higher FAAH activity is detected in placentas during normal pregnancies [107].
Notably, NAPE-PLD has been shown to play a critical role in maintaining uterine AEA levels [103] despite the fact that NAPE-PLD knock-out mice are characterized by near-normal AEA levels [108]. In the uterus, the implanting blastocyst exerts an inhibitory effect on NAPE-PLD activity [103], ensuring coordination in CB signaling between embryonic and maternal sites. NAPE-PLD has also been identified in human placental tissue and is believed to mediate AEA production in the placenta [105].
Further on in the process, successful implantation relies on the differentiation and invasion of a trophoblast originating from the blastocyst trophectoderm during early stages of pregnancy [109]. Low levels of AEA promote trophoblast growth, while elevated AEA inhibits the development of embryos [14]. Exploration of potential mechanisms that underlie the dual role of AEA in early pregnancy suggests two distinct pathways. In the murine model, low concentrations of AEA activate blastocyst extracellular-signal-regulated kinase (ERK) signaling and promote implantation [87, 99]. In the murine model and sheep pregnancy, higher levels of AEA inhibit calcium mobilization, induce cell apoptosis, and inhibit blastocyst cell proliferation thereby precluding successful implantation [87, 99, 110]. In a rat model, CB1 receptor activation results in ceramide release and p38 MAPK-mediated mitochondrial stress, leading to production of reactive oxygen species and apoptosis of uterine decidual cells [111]. MAPK triggers the COX-2 oxidative metabolism of AEA. Such metabolic pathways result in the formation of prostaglandin-like compounds termed “prostamides” [112]. The COX-2 metabolic pathway for AEA is competing with the conventional FAAH pathway [113]. In addition to COX-2-mediated oxidative metabolism resulting in oxidative stress, AEA-induced apoptotic effect is also associated with NF-kB activation [112].
When compared to CB1, the role of the CB2 receptor in early stages of pregnancy is less established. However, CB2 receptor transcript has been identified in both placenta and trophoblasts [114]. During hematopoietic differentiation of murine embryonic stem cell-derived embryoid bodies, CB1 and CB2 antagonists (AM251 and AM630, respectively) induce stem cell death and inhibition of cannabinoid agonist-induced chemotaxis [115].
A study on rat species utilizing RT-PCR, Western blot, and immunohistochemistry documents the presence of CB1 and CB2 receptors, TRPV1 transcripts, and protein products of corresponding encoding genes in rat mesometrial decidua [116]. While transcripts and protein products for CB1, CB2, and TRPV1 decrease throughout pregnancy overall, the CB1 protein amount shows a remarkable spike during day 12 of rat pregnancy. The spike is not detected in the CB1 transcript [116]. This fact underscores the importance of post-transcriptional regulatory mechanisms in maintaining optimal levels of key players within the eCB system.
In addition to direct targeting of eCB receptors within embryonic and maternal tissues, the eCB system has been proposed as exerting a modulatory effect on early pregnancy outcome via immunity [24]. Indeed, eCB system components are present in immune cells [117]; interestingly, immune response has been put forth as an important player in pregnancy initiation and maintenance [118, 119]. Possible cross-talk between the eCB system, immune cells, and reproductive success resulting in a formation of an “endocannabinoid-immune-reproductive axis” requires multifaceted experimental validation [24].
2.5 Midgestation
AEA and 2-AG are produced throughout the prenatal period, but their amounts are not constant [43, 120]. AEA levels in rat brain remain low throughout perinatal period, but then gradually increase as animals reach adulthood [120]. In contrast, changes in 2-AG level show a different time course. They remain relatively constant with the exception of a significant spike at day 21 of rat gestation [43, 120]. This is a full-term pregnancy in rats and in terms of brain development milestones, corresponds to approximately 23 weeks of pregnancy in humans [121].
The CB1 receptor is critical for placental development, as Cnr knock-out mice have smaller placentas and higher resorption rate at mid gestation when compared to their wild-type (CB1 receptor-containing) counterparts [122]. With regards to fetal tissue, CB1 receptor transcript is detected in rat embryo neural tube structures at E11 [114]. CB2 receptor messenger RNA is detected in rat embryonic liver as early as at E13 [114].
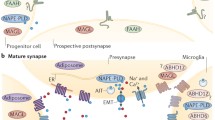
The occurrence and functional characterization of the eCB system has been actively studied within the developing nervous system [55, 123]. Establishment of critical structural components and connectivity within neuronal networks relies on several critical events, such as neuronal progenitor cell proliferation and differentiation, neuronal migration to target regions, and formation of synapses. All aforementioned events are connected with the functionality of eCB system components at various levels of resolution as shown in different experimental models [124].
Immunofluorescence labeling of rat fetuses detects the presence of CB1 receptors in E12.5-16.5 in migrating post-mitotic neurons during corticogenesis [125, 126]. Moreover, prenatal exposure to CB1 receptor agonist WIN 55,212-2 (0.75 mg/kg) via daily subcutaneous (s.c.) delivery to pregnant dams results in significant increases in the number of post-mitotic neurons [126]. However, this increase is not accompanied by a corresponding increase in gamma-aminobutyric acid (GABA)-positive immunostaining. In contrast, WIN 55,212-2 exposure increases immunofluorescence associated with T-box transcription factor Tbr2 that is characteristic of progenitor cells destined for glutamatergic development [126]. In contrast, the marker of post-mitotic glutamatergic neurons Tbr1 responds with transient decreases at E12.5 and E14.5 in brain samples from WIN 55,212-2-exposed fetuses [126]. Thus, the CB1 receptor plays a critical role in neuronal migration and corticogenesis. Variations in fetal CB1 receptor activity and functioning of the eCB system result in a complex reshaping of neuronal development, thus affecting formation of neuronal networks [127]. Studies in knock-out mouse lines demonstrate that lack of CB1 and CB2 receptors leads to impairment of neural progenitor cell proliferation [128, 129]. Mice lacking the CB1 receptor are characterized by diminished cortical progenitor cell proliferation and astrogliogenesis [128, 130]. Notably, work on cultured cell lines indicates that CB1 receptor activation can induce either neurite growth or retraction, depending on the CB1 receptor activation-triggered downstream signaling pathway [55, 131, 132]. Despite the fact that experimental probing of the CB1 receptor impact on the direction of neuronal development renders somewhat conflicting results, the overall picture seems to support positive correlations between CB1 receptor activation and neuronal cell proliferation and migration [124]. Yet, diminished CB1 receptor activity would likely favor cell differentiation, formation of a neuronal phenotype, and synaptogenesis [124].
Analysis of the CB1 receptor expression pattern in human fetuses during midgestation (17–22 weeks) reveals region-specific presence of CB1 receptor mRNA: while CB1 receptor expression is high in limbic structures, only moderate levels are detected in cerebral cortex, thalamus, medial/ventral striatum, and subventricular zone [133]. This expression profile remains unaltered by cannabis exposure in utero [133]. However, maternal cannabis use is associated with a significant decrease in dopamine receptor subtype 2 (D2) mRNA in the amygdala of male, but not female fetuses [133, 134]. D2 mRNA decrease is also detected in striatum; however, dopamine receptor subtype 1 (D1) expression remains unchanged [133, 134]. In addition, prenatal rat THC exposure leads to fluctuations in brain mRNA levels of the enzyme tyrosine hydroxylase that represents a rate-limiting step in dopamine synthesis [135]. This effect exhibits marked sexual dimorphism, the latter being characteristic of alterations in dopaminergic system by prenatal exposure to cannabinoids [43].
With regards to the opioid system, prenatal cannabis exposure is associated with increased mu opioid receptor expression in amygdala [133]. Yet, proenkephalin RNA levels are decreased in fetal striatum from cannabis-using mothers, while prodynorphin levels remain unchanged [133].
In addition to alterations in dopaminergic and opioid systems, prenatal and postnatal exposure to THC in a rat model (from gestational day 5 to postnatal day 20) is reported to result in a decreased immunoreactivity against the GluR1 subunit in Bergmann glial cells and the GluR2/3 subunit in Purkinje neurons when evaluated at postnatal day 20 [136]. These changes persist after THC withdrawal at postnatal days 30 and 70 [136]. Moreover, the expression of glial (GLAST) and neuronal (EAAC1) glutamate transporters in astroglial cells and Purkinje neurons, respectively, is decreased in THC-exposed rat offspring compared to saline-treated controls [137].
The eCB system in the developing brain also represents a target for a drug of abuse other than cannabis itself – alcohol [138, 139]. Data from our laboratory show alcohol-induced decreases in blood velocity in the fetal middle cerebral artery during baboon maternal alcohol intoxication during second trimester-equivalent of human pregnancy [50, 140]. This drop is consistent with fetal cerebral artery dilation, and the latter is replicated using in vitro pressurized arteries from fetal baboons [50]. Notably, alcohol-induced (63 mg/dL ethyl alcohol) dilation of fetal cerebral arteries is blocked in the presence of AM251 in a mixture with AM630 (Fig. 2.1) [50]. The fact that an alcohol effect in vitro is sensitive to CB receptor block, and is mimicking the in vivo scenario, strongly suggests an active eCB system within fetal cerebral arteries of nonhuman primates .
Ethanol-induced dilation of fetal cerebral arteries is mediated by CB receptors. (a) Original diameter trace showing fetal cerebral artery dilation in response to 63 mg/dL ethanol. (b) Averaged data showing diminished ethanol-induced dilation of fetal cerebral arteries in presence of CB1 and CB2 receptor blockers AM251 and AM630, respectively. ∗Statistically significant difference (P < 0.05 by t-test). With modifications from [50]
In human brain, the CB1 receptor is immune-detected in the cortical plate as early as gestational week 9 [141]. It is notable that in the case of brain malformation, CB1 receptors are still present in dysplastic neurons [141]. By the second trimester (20 weeks of human gestation), the CB1 receptor mRNA is spiked within hippocampal CA region and basal nuclear group of the amygdaloid complex [142]. Notably, the adult brain, cerebral cortex, caudate nucleus, putamen and cerebellar cortex are also characterized by high mRNA levels of CB1, in addition to high levels in hippocampus and amygdala [142]. Thus, CB1 receptor occurrence is brain region-specific.
With regards to the relative distribution of CB1 and CB2 receptors across cell types, a differential expression pattern is documented at early stages of development. For example, while CB1 receptors are traced to astrocytes, CB2 receptors are present in microglia [141].
Prenatal marijuana use in humans does not alter fetal growth rates, evident from the analysis of human fetuses aborted at midgestation (17–22 weeks of pregnancy) [143]. However, there is a significant reduction in fetal foot length and body weight in the group of marijuana-exposed fetuses when compared to controls. Moreover, fetal foot length growth is inversely correlated with the amount and frequency of marijuana use reported by the mothers [143]. The consequences of maternal marijuana use are long-lasting. For instance, prenatal marijuana exposure significantly correlates with the age of onset and frequency of marijuana use among 14-year-old teens [144]. Overall, the early appearance, wide distribution, differential expression pattern, and physiological function of eCB system components support the hypothesis of a critical role of eCB signaling in physiology and pathology during midgestation.
2.6 Neonatal and Postnatal Development
At birth, eCB system components are widely distributed in maternal and fetal tissues [14, 49, 145]. While AEA remains low during normal pregnancy [82], its level increases dramatically as labor approaches [14]. Upon delivery, eCBs continue to play a central role in maternal-fetal interaction, as 2-AG is present in maternal milk [13]. 2-AG in milk exceeds that of AEA by 100–1000-fold and serves as a critical contributor into the initiation of milk suckling [146, 147]. Indeed, injections of CB1 receptor antagonist SR141716 (5–20 mg/kg s.c.) into newborn but not older mouse pups drastically reduces milk ingestion and pup growth [146]. This effect is not specific to the particular antagonist, as it has been replicated by another CB receptor antagonist VCHSR [13]. Interestingly, when CB receptor antagonist-treated mouse pups are introduced to a dish with a milk/cream mixture, they are able to lick and ingest this food [13]. Thus, CB1 receptor block is specifically altering suckling behavior, presumably via alterations in synaptogenesis required for neuromuscular coupling within tongue tissue [13].
Around early postnatal development (postnatal day 5), a peak in rat brain 2-AG level is observed when compared to prenatal and adult 2-AG content [13, 148]. In contrast to the bell-shaped ontogeny of 2-AG, AEA levels in rat brain progressively increase from birth into adulthood [13, 148]. Levels of 2-AG detected in rat brain are much higher than those of AEA in rat brain: 2000–8000 pmol/g of tissue versus 3–6 pmol/g of tissue, respectively [43, 120]. However, regional patterns of 2-AG and AEA ontogeny do not always follow net levels, this variability being further complicated by a gender-specific component [42].
With regard to CB receptors, rodent and human brain CB1 receptor levels in fetal and juvenile tissues are generally higher than in adulthood [42, 120, 149, 150]. Yet, CB1 receptor distribution also shows region-specific variability with the predominant location within fetal white matter [148, 149], while CB1 expression in adulthood is predominantly located within grey matter [42, 148].
In a study utilizing C57BL/6 mouse strain, it was shown that the amount of CB1 receptor and its co-localization with GABA and glutamatergic synapses in the visual cortex is modulated by developmental plasticity and by visual input [151]. In particular, immunostaining against CB1 receptor reveals differential distribution of this protein across various layers of mouse visual cortex. The highest intensity of anti CB1 receptor staining is detected in layers II/III and VI. Moreover, CB1 receptor co-localization with presynaptic GABA transporter is detected by vesicular GABA transporter (VGAT)-positive staining and with vesicular glutamate transporter (VGluT)-positive staining. The former is attributed to localization of CB1 receptor within nerve terminals of inhibitory neurons, while the latter is associated with excitatory neurotransmission [151]. Dark rearing of mouse pups up to P30 results in the overall decrease of CB1 receptor-associated staining, decrease in co-localization of CB1 receptor with VGluT in deep layer of visual cortex, but produces an increase in co-localization of CB1 receptor with VGAT in this layer [151]. Notably, naturally uneven distribution of immunostaining signal among visual cortex layers remains unaltered by rearing conditions. Moreover, dark rearing until P50 does not modify the overall level of CB1 receptors, suggesting that visual input only exerts a modulatory role in the developmentally-programmed trajectory of CB1 receptor amounts in the deep layer of visual cortex [151]. At postnatal day 100, the overall amount of CB1 receptor in mouse primary visual cortex as detected by Western blotting, is significantly higher than the amount at an earlier postnatal age (P20) [151].
Targeting of the eCB system by administration of five daily AEA injections (20 mg/kg s.c.) to newborn mice from day 6 of age does not result in any effects on open field performance of the progeny until 4 weeks of age [152]. However, from 40 days of age, the offsprings from AEA-treated dams are characterized by a decrease in open field activity, catalepsy, and hypothermia [152]. It is noteworthy that a fully functional eCB system does not seem to emerge until adulthood, as acute challenge of mouse pups with AEA (20 mg/kg i.p.) does not produce anticipated analgesia and motor depression [152]. This outcome could be explained by the fact that the effects of CB challenge require complex interplay between several components of the eCB system that are only reaching their final levels and patterns of distribution in adulthood [42, 43].
THC exposure during the perinatal period (2.5–5 mg/kg per os, from gestational day 15 to postnatal day 9) results in an increased rate of vocalization in 12-day-old rat pups [153, 154]. However, acute treatment of 11–13-day-old rat pup with CB receptor agonist (-)-cis-3-[2-hydroxy-4-(1,1-dimethylheptyl) phenyl]-trans-4-(3-hydroxypropyl)cyclohexanol (CP 55,940) shows a dose-dependent decrease in ultrasonic vocalizations, with a 1000-μg/kg CP55,940 causing an almost complete shutdown of vocalized calls [155]. CB receptor antagonist SR 141716A (20 mg/kg) reverses this effect [155]. Thus, there are critical windows of vulnerability to eCB system targeting that enable differential outcomes of eCB challenge on physiology/behavior.
In addition to nearly immediate effects, targeting of eCB system during in utero development has long-lasting consequences on developmental trajectories [156,157,158,159]. For example, treatment of rats with cannabinoid receptor agonist HU-210 (25 μg/kg throughout gestation and lactation) results in decreased corticosterone levels in adult male progeny [160].
Altered gene expression in progeny born to THC-treated rat dams has been described for 112 brain genes [161], including elevated pre-proenkephalin mRNA expression in the nucleus accumbens and central and medial amygdala [162], as well as modifications of cortical genes related to glutamatergic system and also to noradrenergic transmission [163]. Alterations in gene expression are associated with a decrease in the cortical extracellular levels of both neurotransmitters [163]. Within the serotoninergic system, perinatal THC exposure (5 mg/kg body weight from gestational day 5 through postnatal day 24) leads to a reduced serotonin level in rat brain samples [164].
Prenatal exposure to CB1 receptor agonist WIN55,212-2 (0.5 mg/kg s.c.) disrupts memory retention in 40- and 80-day-old rat progeny [165]. This memory impairment is correlated with alterations of hippocampal long-term potentiation (LTP) and glutamate release. LTP in hippocampal CA3-CA1 synapses decays faster in brain slices of progeny that was prenatally exposed to WIN55,212-2 when compared to a control group [165]. The effect is specific to a particular parameter of LTP, as post-tetanic and short-term potentiation is similar in WIN55,212-2-exposed and control groups [165]. In vivo microdialysis studies detect a decrease in basal and potassium-induced glutamate levels in the cerebral cortex of adolescent and adult rats born to WIN55,212-2-treated dams (0.5 mg/kg s.c.) when compared to a vehicle-treated group [166]. This decrease is reported to be associated with a WIN55,212-2-triggered increase in glutamate uptake through overexpression of GLT1 and EAAC1 glutamate transporter subtypes, as demonstrated in rat frontal cerebral cortex [167]. Moreover, while WIN55,212-2 treatment (0.1 mg/kg i.p.) increases dialysate glutamate levels in adult rats, blockade of the CB1 receptors with the selective antagonist SR141716A only ablates the WIN55,212-2-induced increase of glutamate in a control group of rats, but not in rats that were prenatally exposed to WIN55,212-2 [166]. It is noteworthy that, while prenatal stimulation of eCB system does not generally result in severe fetal malformations or exert apparent toxicity, prenatal exposure to WIN55,212-2 is reported to be associated with impaired neuronal growth/neurite branching [168]. In synthesis, in utero exposure to exogenous cannabinoids reshapes the eCB system and its communication with major neurotransmission systems [163, 168, 169].
Outside the central nervous system, consequences of exposure to cannabinoids during the perinatal period include long-term alterations in cytochrome P-450 levels [170], enkephalin and norepinephrine sensitivity in vas deferens [171], and neurochemical response to stress [43, 172].
Behavioral consequences of prenatal THC exposure may last into adulthood. Following THC exposure (2 mg/kg twice daily, s.c. gestational days 1-22, postnatal days 2–10), adult (90-day-old) male progeny exhibits decreased time in the inner part of the open field and increased investigation time in the test of social interaction [173]. Moreover, rats that were exposed to THC (0.15 mg/kg, from gestational day 5 to postnatal day 2) exhibit higher heroin-seeking activity at postnatal day 62 [162]. Likewise, daily oral THC administration (5 mg/kg, starting from gestational day 5 throughout postnatal day 24 at weaning) modifies rat brain mu opioid receptor density in a region- and gender-specific manner and facilitates morphine self-administration behavior [162, 174].
Alterations in the eCB system during neonatal and perinatal periods can be achieved not only by exposure to cannabinoids, but also by common stressors such as maternal deprivation. For example, maternal deprivation of neonatal rat pups leads to increased 2-AG content in male hippocampus [175]. Maternal deprivation for 24 h at postnatal day 9 induces a significant increase in DAGLα but not DAGLβ levels upon immunostaining of hippocampi from rat male and female progeny (13-day-old pups) [176]. Maternal deprivation also decreases CB1 receptor expression while CB2 receptor levels are increased [177]. The former phenomenon (decreased CB1 receptor expression and lack of CB1 receptor function) in turn increases progeny’s susceptibility to stress [178]. MAGL protein and mRNA levels are decreased in deprived males [176]. A similar paradigm of maternal deprivation (24 h, postnatal days 9–10) renders increased expression of eCB system component-coding genes in frontal cortex and hippocampus of adolescent (postnatal day 46) male and female rat progeny, respectively [179]. Sexual dimorphisms observed within eCB system distribution and function has been extensively discussed in recent literature [180,181,182,183,184]. Based on studies showing a link between stress and the eCB system, it has been proposed that cannabinoids serve as modulators of the hypothalamic-pituitary-adrenal axis; this modulatory effect may be critical in shaping brain maturation during development [185].
The role of nutrition as another environmental factor that shapes eCB system development has been studied in a model of variable postnatal nutrition in cross-fostering mouse dams [186]. In this study, mouse pups are assigned to new mothers upon birth, and different pup-to-mother ratios are used to regulate nutritional intake (3, 6, or 10 pups per mother). Conceivably, groups with 3 pups per mother show higher growth measures when compared to 6 and 10 pups/mother groups [186]. ECB system components evaluated at postnatal day 50 show progressive decreases in FAAH and MAGL gene expression in liver as pup-to-mother ratio was increased [186]. Visceral adipose tissue does not render significant changes in FAAH gene expression level as a function of early postnatal nutrition, yet MAGL expression level is decreased with increased pup-to-mother ratio. Moreover, expression of NAPE-PLD and DAGLα in visceral adipose tissue is also progressively decreased as pup-to-mother ratio is increased [186]. This study promotes the peripheral eCB system as a sensor of early postnatal nutrition. Conceivably, maternal high-fat diet (≈29% of calories from fat) in a rat model results in profound modification of the eCB system protein levels of progeny [187, 188]. In particular, male offspring of mothers subjected to high-fat diet exhibit significant increase in hypothalamus CB1 receptor protein level, while females show increased CB2 receptor protein level in this brain region when evaluated at birth [188]. In brown fat tissue, a maternal high-fat diet results in increased FAAH level in male and increased CB2 receptor protein level in female progeny, respectively [188]. However, unlike the hypothalamic CB1 receptor, the brown fat tissue CB1 receptor is decreased in male progeny from mothers fed a high-fat diet [188]. These findings reiterate the tissue- and gender-specific nature of the eCB system, showing sensitivity to modulation by exogenous interventions.
In addition to nutrition, alcohol exposure in rodent models emerges as another critical modulator of eCB system function during perinatal/early postnatal development. Indeed, ethyl alcohol treatment of C57BL/6J mice at postnatal day 7 (2.5 g/kg s.c. twice) increases AEA levels [189]. Unlike AEA, 2-AG level remains unchanged due to alcohol-induced up-regulation of both DAGLβ and MAGL activities [190]. Alcohol treatment also results in up-regulated CB1 receptor protein expression in the cortex and hippocampus [189]. Moreover, such alcohol treatment triggers neurodegeneration that is absent in CB1 receptor knock-out mice [189]. These findings reinforce the concept of a cross-talk between the eCB system and the molecular targets of another drug of abuse, alcohol [138, 139].
Data from nonhuman primates are consistent with reports on predominant abundance of 2-AG over AEA: mass spectroscopy analyses of baboon samples from our laboratory show ≈30 times higher 2-AG levels when compared to AEA in the blood circulation of near-term fetuses and their corresponding mothers (Fig. 2.2). Similarly, the relative abundance of 2-AG in baboon cerebral arteries is higher than AEA in both mothers and near-term fetuses (Fig. 2.2). Data from our laboratory also present evidence of dynamic changes in CB1 receptor function within baboon cerebral arteries during development. In particular, application of AM251 (1 μM) to in vitro-pressurized branches of middle cerebral arteries, harvested from fetal baboons at the end of second trimester equivalent of human pregnancy, renders artery constriction (Fig. 2.3) [50]. However, identical pharmacological probing results in artery dilation in near-term fetal and their maternal cerebral artery segments (Fig. 2.3).
Blood and tissue eCB levels in baboon ( Papio spp .). (a) AEA levels in circulating blood of near-term fetal baboons and their corresponding mothers. Here and in B-D, data from a given fetus-mother pair are connected by a solid line. Different symbols correspond to data-points from separate fetus-mother pairs. (b) Circulating 2-AG levels in near-term fetal baboons and their corresponding mothers. (c) AEA levels in cerebral artery lysates of near-term fetal baboons and their corresponding mothers. Here and in D, the eCB reading within each sample was normalized to protein amount. (d) 2-AG levels in cerebral artery lysates of near-term fetal baboons and their corresponding mothers
Averaged Changes in cerebral artery diameter were assessed by probing of in vitro pressurized branches of fetal and maternal middle cerebral arteries harvested from baboons (Papio spp.). Effect of AM251 (1 μM) is presented as a percent change in artery diameter from pre-AM251 level. ∗Statistically significant difference (P < 0.05 by one-way ANOVA with Tukey post-test). dGa: days of gestational age
With regards to other nutritional interventions, maternal high-fat diet (12% fat) during pregnancy leads to decreased fetal baboon circulating 2-AG levels near–term, independent of fetal gender [191]. Interestingly, maternal baboon circulating 2-AG levels are increased by high-fat diet. In addition to modification of fetal circulating 2-AG level, fetal hepatic CB2 receptor, FAAH, and COX-2 expression values are lower in fetuses of both genders from the high-fat group. Within this group, DAGLα expression is selectively decreased in male fetuses [191].
In humans, a qPCR study on post-mortem samples from the middle frontal gyrus area of the donors between 39 days and 49 years of age unveils complex developmental trajectories for critical players within the eCB system [192]. In particular, expression of the CB1 receptor is progressively decreasing from infancy into adulthood with a slight local peak at toddler age. A similar profile is followed by MAGL [192]. In sharp contrast, NAPE-PLD, FAAH, and ABHD6 are progressively increased from infancy into adulthood. Finally, DAGLα mRNA shows a bell-shaped pattern with the peak around school age [192].
Consequences of in utero cannabis exposure on developmental trajectories in humans have been studied in several longitudinal cohort studies, and are found to be long-lasting. Several early reports describe increased tremors, startle response, and poor visual responsiveness of cannabis-exposed infants [193]. These characteristics are apparent in the absence of effect on morphometric (growth) parameters, such as weight and head circumference [194]. Notably, characteristics of infants born to cannabis users disappear by 30 days of age [193], demonstrating a remarkable plasticity that allows the development of compensatory measures in response to cannabis-driven alterations in physiological processes. Later in childhood, however, prenatal cannabis exposure negatively reflects on attention processes [195] and cognitive performance within executive function [154, 196]. In utero CB exposure leads to more aggressive behavior and attention problems in 18-month-old girls [17]. Moreover, maternal light-to-moderate marijuana use during pregnancy is associated with deficits in Wide Range Achievement Test-Revised reading and spelling scores and a lower rating on the teachers’ evaluations of the children’s performance in 10-year-olds [197]. Functional magnetic resonance imaging on eighteen-to-twenty two-year-old adults that were prenatally exposed to cannabis demonstrates alteration in visuospatial working memory processing [198]. Increased impulsive behavior has also been reported as a consequence of prenatal cannabis exposure [133, 199]. Yet, maternal marijuana use does not affect growth parameters of the progeny in puberty [200].
2.7 Adolescence
Although exact age limits of the adolescent period are poorly defined, adolescence usually refers to as a period of pubertal maturation [201]. Adolescence is a period of active brain development, representing the transition between childhood and adulthood [201, 202]. It is also often characterized by cannabis use [202, 203]. Considering that eCB system controls several fundamental processes of neuronal and glial development, such as cell proliferation, migration, and differentiation [1, 204, 205], alterations in the eCB system during adolescence are expected to impact neuronal maturation.
Studies in rat species describe a peak of CB1 receptor expression in prefrontal cortex, limbic, striatal, and midbrain areas during adolescence (postnatal days 25–29 in rats), this peak later declines to adult levels [185, 206, 207]. Consistent with this peak in CB1 receptor expression, studies in rodent models show that the adolescent brain is particularly vulnerable to CB stimulation when compared to adults. Rats that were exposed to THC (1.5 mg/kg i.p. every third day) at postnatal days 28 (early adolescence) to 49 (late adolescence) show profound alterations in the endocannabinoid levels in prefrontal cortex and nucleus accumbens regions [208]. Adolescent rats that were repeatedly exposed to THC (5 mg/kg i.p. starting from postnatal day 28) show less vocalization during the THC administration procedure when compared to adults (starting from postnatal day 60) [209]. This result suggests that THC is less aversive to adolescent rats. Also, after THC withdrawal, THC-exposed adolescent rats exhibit impaired object recognition memory. Proteomics analysis of hippocampal samples detects significant changes in 27 proteins following THC exposure in adolescence, compared to only 10 proteins in adults. The former are represented by oxidative stress/mitochondrial and cytoskeletal targets [209]. This finding confirms the greater vulnerability of the adolescent brain to cannabis exposure compared to the adult brain. Similarly, synthetic cannabinoid agonist WIN 55,212-2 (1.2 mg/kg i.p.) treatment of pubertal rats results in poorer recognition memory when compared to identical treatment of adult rats [210]. Also, working memory impairment and a significant decrease in social interaction is reported in female rats in response to CB receptor agonist CP 55,940 administered daily for 21 days at 150, 200, and 300 μg/kg i.p. for 3, 8 and 10 days, respectively [211]. In addition, in a study on rats using eCB system stimulation with CP 55,940, it is concluded that chronic CB exposure leads to long-term memory impairments and increased anxiety, irrespective of the age at which drug exposure occurs (either at the perinatal period, adolescence, or young adulthood) [212].
In a different experimental paradigm, adolescent male rats were administered AEA hydrolysis inhibitor URB597 (0, 0.1, or 0.5 mg/kg/day at postnatal days 38–43) [213]. Following this treatment, a decrease in CB1 receptor is detected in caudate-putamen, nucleus accumbens, ventral tegmental area, and hippocampus, while an opposite effect is observed in the locus coeruleus [213]. Similar treatment with FAAH inhibitor URB597 (0.3 mg/kg i.p.) reverts depressive-like symptoms induced by adolescent exposure to THC in female rats [214]. Moreover, MAGL inhibitor JZL 184 ameliorates a deficit in presynaptic long-term plasticity triggered by exposure of adolescent mice to WIN 55,212-2 [215]. These findings demonstrate the possibility of persistent attenuation in AEA and 2-AG levels as an underlying cause of neuronal deficits associated with adolescent THC exposure.
In addition to alterations within the eCB system, adolescent exposure to CB stimulation interferes with sensitivity to other drugs of abuse. For example, exposure of adolescent rats to THC (1.5 mg/kg i.p., every third day during postnatal days 28–49) results in increased sensitivity to opiates and heroin self-administration in adulthood (postnatal days 57 and 102) [216]. Mu opioid receptor GTP-coupling is potentiated in mesolimbic and nigrostriatal brainstem regions in THC-exposed animals, with mu opioid receptor function in the nucleus accumbens shell being specifically correlated with heroin intake [216]. Thus, the consequences of eCB alteration during adolescence are likely region-specific.
There is also a gender-specific component in responses of the adolescent brain to eCB stimulation. THC administration to rats twice a day (2.5 mg/kg at postnatal days 35–37, 5 mg/kg at postnatal days 38–41, and 10 mg/kg at postnatal days 42–45, i.p) results in significant decreases of CB1 receptor level and CB1/G-protein coupling in the amygdala, ventral tegmental area, and nucleus accumbens in females [217]. However, males only exhibit these alterations in the amygdala and hippocampus. Additional neuronal consequences of adolescence THC exposure include dendritic atrophy and decreases in markers of neuroplasticity [218, 219]. At the behavioral level, females present behavioral despair in a forced swim test, which is accompanied by anhedonia in a sucrose preference test [217]. Males only present anhedonia [217].
Ontogeny of CB1 receptor expression in humans somewhat differs from that of rats. In particular, a gradual increase in CB1 expression in the human brain towards adulthood is reported [149]. The function of these receptors is successfully assessed by [35S]GTPγS autoradiography. Moreover, high levels of CB receptors are detected during prenatal development in fiber-enriched areas, these areas being devoid of CB receptor signal in adulthood [149]. Several other reports on human dorsolateral prefrontal cortex samples also fail to detect a rodent-characteristic peak in brain CB1 receptor level in adolescence [192, 220]. While species-specific expression pattern of the CB1 receptor and, perhaps, eCB system function, should be considered as a primary cause for such discrepancy, it has been proposed that such inconsistency between reports might reflect overall instability of the developing eCB system [42].
Computer-assisted attention testing that addresses visual scanning, alertness, divided attention, flexibility, and working memory in humans detects a significant impairment in visual scanning reaction times in early-onset (before age 16) cannabis users but not in late-onset (after age 16) users [221]. This outcome suggests that the brain in early adolescence is particularly vulnerable to alterations in the eCB system upon exposure to exogenous cannabis. Adolescent cannabis use has also been suggested to exert a modulatory effect over anxiety-related behaviors and depression [154]. In the latter case, a link between adolescent cannabinoid exposure and serotonergic hypoactivity has been proposed [222].
2.8 Concluding Remarks
Ample data from invertebrate and vertebrate species, including humans, document the complex roles of the eCB system in development. Gender, timing, and pharmacological routes of eCB challenge are all-important in establishing the final trajectory of eCB ontogenesis and its role in physiology and pathology.
Continuous growth in proposed CB-based pharmacological remedies and increasing THC content in recreational cannabis preparations [223, 224] call for concerns over incomplete understanding of eCB function. Despite the fact that the eCB system represents an attractive therapeutics target for various conditions that represent developmental pathology, the major difficulty in developing eCB-targeting pharmacotherapy arises from the complexity of the eCB system. We are far from finalizing complete characterization of all eCB components, therefore the process of fully characterizing the eCB system continues.
Abbreviations
- ABHD4:
-
α/β-hydrolase domain 4
- AEA:
-
anandamide
- CB:
-
cannabinoid
- COX-2:
-
cyclooxygenase-2
- CP55,940:
-
(-)-cis-3-[2-hydroxy-4-(1,1-dimethylheptyl)phenyl]-trans-4-(3-hydroxypropyl)cyclohexanol
- DAGL:
-
diacylglycerol lipase
- eCB:
-
endocannabinoid (system)
- ERK:
-
extracellular-signal-regulated kinase
- FAAH:
-
fatty acid amide hydrolase
- GABA:
-
gamma aminobutyric acid
- LTP:
-
long-term potentiation
- MAPK:
-
mitogen-activated protein kinase
- MAGL:
-
monoacylglycerol lipase
- NAE:
-
N-acylethanolamine
- NAPE:
-
N-acylphosphatidylethanolamine
- NAPE-PLD:
-
N-acylphosphatidylethanolamine-specific phospholipase D
- PCR:
-
polymerase chain reaction
- THC:
-
Δ9-tetrahydrocannabinol
- TRP:
-
transient receptor potential (protein, channel)
- VGAT:
-
vesicular GABA transporter
- 2-AG:
-
2-arachidonoylglycerol.
References
Mechoulam R, Parker LA (2013) The endocannabinoid system and the brain. Annu Rev Psychol 64:21–47
Hall W, Solowij N (1998) Adverse effects of cannabis. Lancet 352:1611–1616
Green B, Kavanagh D, Young R (2003) Being stoned: a review of self-reported cannabis effects. Drug Alcohol Rev 22:453–460
Cheung JT, Mann RE, Ialomiteanu A, Stoduto G, Chan V, Ala-Leppilampi K, Rehm J (2010) Anxiety and mood disorders and cannabis use. Am J Drug Alcohol Abuse 36:118–122
Hunault CC, Böcker KB, Stellato RK, Kenemans JL, de Vries I, Meulenbelt J (2014) Acute subjective effects after smoking joints containing up to 69 mg Δ9-tetrahydrocannabinol in recreational users: a randomized, crossover clinical trial. Psychopharmacology 231:4723–4733
Temple EC, Driver M, Brown RF (2014) Cannabis use and anxiety: is stress the missing piece of the puzzle? Front Psychiatry 5:168
Schonhofen P, Bristot IJ, Crippa JA, Hallak JEC, Zuardi AW, Parsons RB, Klamt F (2018) Cannabinoid-based therapies and brain development: potential harmful effect of early modulation of the endocannabinoid system. CNS Drugs 32:697–712
Bortolato M, Mangieri RA, Fu J, Kim JH, Arguello O, Duranti A, Tontini A, Mor M, Tarzia G, Piomelli D (2007) Antidepressant-like activity of the fatty acid amide hydrolase inhibitor URB597 in a rat model of chronic mild stress. Biol Psychiatry 62:1103–1110
Mangieri RA, Piomelli D (2007) Enhancement of endocannabinoid signaling and the pharmacotherapy of depression. Pharmacol Res 56:360–366
Hill TD, Cascio MG, Romano B, Duncan M, Pertwee RG, Williams CM, Whalley BJ, Hill AJ (2013) Cannabidivarin-rich cannabis extracts are anticonvulsant in mouse and rat via a CB1 receptor-independent mechanism. Br J Pharmacol 170:679–692
Kaur R, Ambwani SR, Singh S (2016) Endocannabinoid system: a multi-facet therapeutic target. Curr Clin Pharmacol 11:110–117
Lu Y, Anderson HD (2017) Cannabinoid signaling in health and disease. Can J Physiol Pharmacol 95:311–327
Fride E (2008) Multiple roles for the endocannabinoid system during the earliest stages of life: pre- and postnatal development. J Neuroendocrinol 20:75–81
Correa F, Wolfson ML, Valchi P, Aisemberg J, Franchi AM (2016) Endocannabinoid system and pregnancy. Reproduction 152:R191–R200
Ko JY, Farr SL, Tong VT, Creanga AA, Callaghan WM (2015) Prevalence and patterns of marijuana use among pregnant and nonpregnant women of reproductive age. Am J Obstet Gynecol 213:e201–e210
Williamson S, Jackson L, Skeoch C, Azzim G, Anderson R (2006) Determination of the prevalence of drug misuse by meconium analysis. Arch Dis Child Fetal Neonatal Ed 91:F291–F292
El Marroun H, Hudziak JJ, Tiemeier H, Creemers H, Steegers EA, Jaddoe VW, Hofman A, Verhulst FC, van den Brink W, Huizink AC (2011) Intrauterine cannabis exposure leads to more aggressive behavior and attention problems in 18-month-old girls. Drug Alcohol Depend 118:470–474
Marco EM, Laviola G (2012) The endocannabinoid system in the regulation of emotions throughout lifespan: a discussion on therapeutic perspectives. J Psychopharmacol 26:150–163
Sun YX, Tsuboi K, Okamoto Y, Tonai T, Murakami M, Kudo I, Ueda N (2004) Biosynthesis of anandamide and N-palmitoylethanolamine by sequential actions of phospholipase A2 and lysophospholipase D. Biochem J 380:749–756
Romero TR, Resende LC, Guzzo LS, Duarte ID (2013) CB1 and CB2 cannabinoid receptor agonists induce peripheral antinociception by activation of the endogenous noradrenergic system. Anesth Analg 116:463–472
Borrelli F, Izzo AA (2009) Role of acylethanolamides in the gastrointestinal tract with special reference to food intake and energy balance. Best Pract Res Clin Endocrinol Metab 23:33–49
Hansen HS, Diep TA (2009) N-acylethanolamines, anandamide and food intake. Biochem Pharmacol 78:553–560
Caraceni P, Viola A, Piscitelli F, Giannone F, Berzigotti A, Cescon M, Domenicali M, Petrosino S, Giampalma E, Riili A, Grazi G, Golfieri R, Zoli M, Bernardi M, Di Marzo V (2010) Circulating and hepatic endocannabinoids and endocannabinoid-related molecules in patients with cirrhosis. Liver Int 30:816–825
Bambang KN, Lambert DG, Lam PM, Quenby S, Maccarrone M, Konje JC (2012) Immunity and early pregnancy events: are endocannabinoids the missing link? J Reprod Immunol 96:8–18
Liu J, Wang L, Harvey-White J, Osei-Hyiaman D, Razdan R, Gong Q, Chan AC, Zhou Z, Huang BX, Kim HY, Kunos G (2006) A biosynthetic pathway for anandamide. Proc Natl Acad Sci U S A 103:13345–13350
Liu J, Wang L, Harvey-White J, Huang BX, Kim HY, Luquet S, Palmiter RD, Krystal G, Rai R, Mahadevan A, Razdan RK, Kunos G (2008) Multiple pathways involved in the biosynthesis of anandamide. Neuropharmacology 54(1):1–7
Simon GM, Cravatt BF (2008) Anandamide biosynthesis catalyzed by the phosphodiesterase GDE1 and detection of glycerophospho-N-acyl ethanolamine precursors in mouse brain. J Biol Chem 283:9341–9349
Bisogno T, Howell F, Williams G, Minassi A, Cascio MG, Ligresti A, Matias I, Schiano-Moriello A, Paul P, Williams EJ, Gangadharan U, Hobbs C, Di Marzo V, Doherty P (2003) Cloning of the first sn1-DAG lipases points to the spatial and temporal regulation of endocannabinoid signaling in the brain. J Cell Biol 163:463–468
Taylor AH, Ang C, Bell SC, Konje JC (2007) The role of the endocannabinoid system in gametogenesis, implantation and early pregnancy. Hum Reprod Update 13:501–513
Maccarrone M, van der Stelt M, Rossi A, Veldink GA, Vliegenthart JF, Agrò AF (1998) Anandamide hydrolysis by human cells in culture and brain. J Biol Chem 273:32332–32339
Burstein SH, Rossetti RG, Yagen B, Zurier RB (2000) Oxidative metabolism of anandamide. Prostaglandins Other Lipid Mediat 61:29–41
Kozak KR, Crews BC, Morrow JD, Wang LH, Ma YH, Weinander R, Jakobsson PJ, Marnett LJ (2002) Metabolism of the endocannabinoids, 2-arachidonylglycerol and anandamide, into prostaglandin, thromboxane, and prostacyclin glycerol esters and ethanolamides. J Biol Chem 277:44877–44885
Ross RA, Craib SJ, Stevenson LA, Pertwee RG, Henderson A, Toole J, Ellington HC (2002) Pharmacological characterization of the anandamide cyclooxygenase metabolite: prostaglandin E2 ethanolamide. J Pharmacol Exp Ther 301:900–907
Blankman JL, Simon GM, Cravatt BF (2007) A comprehensive profile of brain enzymes that hydrolyze the endocannabinoid 2-arachidonoylglycerol. Chem Biol 14:1347–1356
Muccioli GG, Xu C, Odah E, Cudaback E, Cisneros JA, Lambert DM, López Rodríguez ML, Bajjalieh S, Stella N (2007) Identification of a novel endocannabinoid-hydrolyzing enzyme expressed by microglial cells. J Neurosci 27:2883–2889
Matsuda LA, Lolait SJ, Brownstein MJ, Young AC, Bonner TI (1990) Structure of a cannabinoid receptor and functional expression of the cloned cDNA. Nature 346:561–564
Slipetz DM, O’Neill GP, Favreau L, Dufresne C, Gallant M, Gareau Y, Guay D, Labelle M, Metters KM (1995) Activation of the human peripheral cannabinoid receptor results in inhibition of adenylyl cyclase. Mol Pharmacol 48:352–361
Shire D, Calandra B, Rinaldi-Carmona M, Oustric D, Pessègue B, Bonnin-Cabanne O, Le Fur G, Caput D, Ferrara P (1996) Molecular cloning, expression and function of the murine CB2 peripheral cannabinoid receptor. Biochim Biophys Acta 1307:132–136
Mukhopadhyay S, McIntosh HH, Houston DB, Howlett AC (2000) The CB(1) cannabinoid receptor juxtamembrane C-terminal peptide confers activation to specific G proteins in brain. Mol Pharmacol 57:162–170
Kenakin T, Onaran O (2002) The ligand paradox between affinity and efficacy: can you be there and not make a difference? Trends Pharmacol Sci 23:275–280
Psychoyos D, Vinod KY, Cao J, Xie S, Hyson RL, Wlodarczyk B, He W, Cooper TB, Hungund BL, Finnell RH (2012) Cannabinoid receptor 1 signaling in embryo neurodevelopment. Birth Defects Res B Dev Reprod Toxicol 95:137–150
Lee TT, Hill MN, Lee FS (2016) Developmental regulation of fear learning and anxiety behavior by endocannabinoids. Genes Brain Behav 15:108–124
Fernández-Ruiz JJ, Berrendero F, Hernández ML, Romero J, Ramos JA (1999) Role of endocannabinoids in brain development. Life Sci 65:725–736
Oliveira da Cruz JF, Robin LM, Drago F, Marsicano G, Metna-Laurent M (2016) Astroglial type-1 cannabinoid receptor (CB1): a new player in the tripartite synapse. Neuroscience 323:35–42
Galiègue S, Mary S, Marchand J, Dussossoy D, Carrière D, Carayon P, Bouaboula M, Shire D, Le Fur G, Casellas P (1995) Expression of central and peripheral cannabinoid receptors in human immune tissues and leukocyte subpopulations. Eur J Biochem 232:54–61
Barutta F, Mastrocola R, Bellini S, Bruno G, Gruden G (2018) Cannabinoid receptors in diabetic kidney disease. Curr Diab Rep 18:9
Buznikov GA, Nikitina LA, Bezuglov VV, Francisco ME, Boysen G, Obispo-Peak IN, Peterson RE, Weiss ER, Schuel H, Temple BR, Morrow AL, Lauder JM (2010) A putative ‘pre-nervous’ endocannabinoid system in early echinoderm development. Dev Neurosci 32:1–18
Elphick MR, Egertová M (2001) The neurobiology and evolution of cannabinoid signalling. Philos Trans R Soc Lond Ser B Biol Sci 356:381–408
Rodriguez-Sanchez IP, Guindon J, Ruiz M, Tejero ME, Hubbard G, Martinez-de-Villarreal LE, Barrera-Saldaña HA, Dick EJ Jr, Comuzzie AG, Schlabritz-Loutsevitch NE (2016) The endocannabinoid system in the baboon (Papio spp.) as a complex framework for developmental pharmacology. Neurotoxicol Teratol 58:23–30
Seleverstov O, Tobiasz A, Jackson JS, Sullivan R, Ma D, Sullivan JP, Davison S, Akkhawattanangkul Y, Tate DL, Costello T, Barnett S, Li W, Mari G, Dopico AM, Bukiya AN (2017) Maternal alcohol exposure during mid-pregnancy dilates fetal cerebral arteries via endocannabinoid receptors. Alcohol 61:51–61
Cabral GA, Raborn ES, Griffin L, Dennis J, Marciano-Cabral F (2008) CB2 receptors in the brain: role in central immune function. Br J Pharmacol 153:240–251
Li Y, Kim J (2017) Distinct roles of neuronal and microglial CB2 cannabinoid receptors in the mouse hippocampus. Neuroscience 363:11–25
Van Sickle MD, Duncan M, Kingsley PJ, Mouihate A, Urbani P, Mackie K, Stella N, Makriyannis A, Piomelli D, Davison JS, Marnett LJ, Di Marzo V, Pittman QJ, Patel KD, Sharkey KA (2005) Identification and functional characterization of brainstem cannabinoid CB2 receptors. Science 310:329–332
Onaivi ES, Ishiguro H, Gong JP, Patel S, Perchuk A, Meozzi PA, Myers L, Mora Z, Tagliaferro P, Gardner E, Brusco A, Akinshola BE, Liu QR, Hope B, Iwasaki S, Arinami T, Teasenfitz L, Uhl GR (2006) Discovery of the presence and functional expression of cannabinoid CB2 receptors in brain. Ann N Y Acad Sci 1074:514–536
Galve-Roperh I, Palazuelos J, Aguado T, Guzmán M (2009) The endocannabinoid system and the regulation of neural development: potential implications in psychiatric disorders. Eur Arch Psychiatry Clin Neurosci 259:371–382
Rom S, Persidsky Y (2013) Cannabinoid receptor 2: potential role in immunomodulation and neuroinflammation. J NeuroImmune Pharmacol 8:608–620
Felder CC, Joyce KE, Briley EM, Mansouri J, Mackie K, Blond O, Lai Y, Ma AL, Mitchell RL (1995) Comparison of the pharmacology and signal transduction of the human cannabinoid CB1 and CB2 receptors. Mol Pharmacol 48:443–450
Gebremedhin D, Lange AR, Campbell WB, Hillard CJ, Harder DR (1999) Cannabinoid CB1 receptor of cat cerebral arterial muscle functions to inhibit L-type Ca2+ channel current. Am J Phys 276:H2085–H2093
Hillard CJ (2000) Biochemistry and pharmacology of the endocannabinoids arachidonylethanolamide and 2-arachidonylglycerol. Prostaglandins Other Lipid Mediat 61:3–18
Demuth DG, Molleman A (2006) Cannabinoid signalling. Life Sci 78:549–563
Turu G, Hunyady L (2010) Signal transduction of the CB1 cannabinoid receptor. J Mol Endocrinol 44:75–85
Franklin JM, Carrasco GA (2013) Cannabinoid receptor agonists upregulate and enhance serotonin 2A (5-HT(2A)) receptor activity via ERK1/2 signaling. Synapse 67:145–159
Sánchez-Pastor E, Andrade F, Sánchez-Pastor JM, Elizalde A, Huerta M, Virgen-Ortiz A, Trujillo X, Rodríguez-Hernández A (2014) Cannabinoid receptor type 1 activation by arachidonylcyclopropylamide in rat aortic rings causes vasorelaxation involving calcium-activated potassium channel subunit alpha-1 and calcium channel, voltage-dependent, L type, alpha 1C subunit. Eur J Pharmacol 729:100–106
Szabó GG, Lenkey N, Holderith N, Andrási T, Nusser Z, Hájos N (2014) Presynaptic calcium channel inhibition underlies CB1 cannabinoid receptor-mediated suppression of GABA release. J Neurosci 34:7958–7963
Bondarenko AI, Panasiuk O, Okhai I, Montecucco F, Brandt KJ, Mach F (2018) Ca2+-dependent potassium channels and cannabinoid signaling in the endothelium of apolipoprotein E knockout mice before plaque formation. J Mol Cell Cardiol 115:54–63
Hillard CJ (2000) Endocannabinoids and vascular function. J Pharmacol Exp Ther 294:27–32
Caterina MJ (2014) TRP channel cannabinoid receptors in skin sensation, homeostasis, and inflammation. ACS Chem Neurosci 5:1107–1116
Godlewski G, Offertáler L, Wagner JA, Kunos G (2009) Receptors for acylethanolamides-GPR55 and GPR119. Prostaglandins Other Lipid Mediat 89:105–111
Bambang KN, Karasu T, Gebeh A, Taylor AH, Marczylo TH, Lam P, Willets JM, Konje JC (2010) From fertilization to implantation in mammalian pregnancy-modulation of early human reproduction by the endocannabinoid system. Pharmaceuticals (Basel) 3:2910–2929
Maccarrone M, Valensise H, Bari M, Lazzarin N, Romanini C, Finazzi-Agrò A (2001) Progesterone up-regulates anandamide hydrolase in human lymphocytes: role of cytokines and implications for fertility. J Immunol 166:7183–7189
Wenger T, Tóth BE, Martin BR (1995) Effects of anandamide (endogen cannabinoid) on anterior pituitary hormone secretion in adult ovariectomized rats. Life Sci 56:2057–2063
Hill MN, Carrier EJ, Ho WS, Shi L, Patel S, Gorzalka BB, Hillard CJ (2008) Prolonged glucocorticoid treatment decreases cannabinoid CB1 receptor density in the hippocampus. Hippocampus 18:221–226
Maccarrone M, Finazzi-Agrò A (2004) Anandamide hydrolase: a guardian angel of human reproduction? Trends Pharmacol Sci 25:353–357
Schuel H, Goldstein E, Mechoulam R, Zimmerman AM, Zimmerman S (1994) Anandamide (arachidonylethanolamide), a brain cannabinoid receptor agonist, reduces sperm fertilizing capacity in sea urchins by inhibiting the acrosome reaction. Proc Natl Acad Sci U S A 91:7678–7682
Maccarrone M, Cecconi S, Rossi G, Battista N, Pauselli R, Finazzi-Agrò A (2003) Anandamide activity and degradation are regulated by early postnatal aging and follicle-stimulating hormone in mouse Sertoli cells. Endocrinology 144:20–28
Peralta L, Agirregoitia E, Mendoza R, Expósito A, Casis L, Matorras R, Agirregoitia N (2011) Expression and localization of cannabinoid receptors in human immature oocytes and unfertilized metaphase-II oocytes. Reprod BioMed Online 23:372–379
Grimaldi P, Orlando P, Di Siena S, Lolicato F, Petrosino S, Bisogno T, Geremia R, De Petrocellis L, Di Marzo V (2009) The endocannabinoid system and pivotal role of the CB2 receptor in mouse spermatogenesis. Proc Natl Acad Sci U S A 106:11131–11136
Cobellis G, Ricci G, Cacciola G, Orlando P, Petrosino S, Cascio MG, Bisogno T, De Petrocellis L, Chioccarelli T, Altucci L, Fasano S, Meccariello R, Pierantoni R, Ledent C, Di Marzo V (2010) A gradient of 2-arachidonoylglycerol regulates mouse epididymal sperm cell start-up. Biol Reprod 82:451–458
Rossato M, Ion Popa F, Ferigo M, Clari G, Foresta C (2005) Human sperm express cannabinoid receptor Cb1, the activation of which inhibits motility, acrosome reaction, and mitochondrial function. J Clin Endocrinol Metab 90:984–991
Lazzarin N, Valensise H, Bari M, Ubaldi F, Battista N, Finazzi-Agrò A, Maccarrone M (2004) Fluctuations of fatty acid amide hydrolase and anandamide levels during the human ovulatory cycle. Gynecol Endocrinol 18:212–218
El-Talatini MR, Taylor AH, Konje JC (2010) The relationship between plasma levels of the endocannabinoid, anandamide, sex steroids, and gonadotrophins during the menstrual cycle. Fertil Steril 93:1989–1996
Habayeb OM, Taylor AH, Bell SC, Taylor DJ, Konje JC (2008) Expression of the endocannabinoid system in human first trimester placenta and its role in trophoblast proliferation. Endocrinology 149:5052–5060
Ayalon D, Nir I, Cordova T, Bauminger S, Puder M, Naor Z, Kashi R, Zor U, Harell A, Lindner HR (1977) Acute effect of delta1-tetrahydrocannabinol on the hypothalamo-pituitary-ovarian axis in the rat. Neuroendocrinology 23:31–42
Du Plessis SS, Agarwal A, Syriac A (2015) Marijuana, phytocannabinoids, the endocannabinoid system, and male fertility. J Assist Reprod Genet 32:1575–1588
Brents LK (2016) Marijuana, the endocannabinoid system and the female reproductive system. Yale J Biol Med 89:175–191
Wang H, Dey SK, Maccarrone M (2006) Jekyll and hyde: two faces of cannabinoid signaling in male and female fertility. Endocr Rev 27:427–448
Wang H, Xie H, Dey SK (2006) Endocannabinoid signaling directs periimplantation events. AAPS J 8:E425–E432
Wenger T, Ledent C, Csernus V, Gerendai I (2001) The central cannabinoid receptor inactivation suppresses endocrine reproductive functions. Biochem Biophys Res Commun 284:363–368
Nahas GG, Frick HC, Lattimer JK, Latour C, Harvey D (2002) Pharmacokinetics of THC in brain and testis, male gametotoxicity and premature apoptosis of spermatozoa. Hum Psychopharmacol 17:103–113
Schuel H, Burkman LJ (2005) A tale of two cells: endocannabinoid-signaling regulates functions of neurons and sperm. Biol Reprod 73:1078–1086
Oltrabella F, Melgoza A, Nguyen B, Guo S (2017) Role of the endocannabinoid system in vertebrates: Emphasis on the zebrafish model. Develop Growth Differ 59:194–210
Ahmed KT, Amin MR, Shah P, Ali DW (2018) Motor neuron development in zebrafish is altered by brief (5-hr) exposures to THC (∆9-tetrahydrocannabinol) or CBD (cannabidiol) during gastrulation. Sci Rep 8:10518
Begbie J, Doherty P, Graham A (2004) Cannabinoid receptor, CB1, expression follows neuronal differentiation in the early chick embryo. J Anat 205:213–218
Watson S, Chambers D, Hobbs C, Doherty P, Graham A (2008) The endocannabinoid receptor, CB1, is required for normal axonal growth and fasciculation. Mol Cell Neurosci 38:89–97
Newgreen DF, Howard MJ, Nishi R (2009) Encyclopedia of neuroscience. Autonomic nervous system development, pp 837–848
Taylor AH, Amoako AA, Bambang K, Karasu T, Gebeh A, Lam PM, Marzcylo TH, Konje JC (2010) Endocannabinoids and pregnancy. Clin Chim Acta 411:921–930
Wang H, Guo Y, Wang D, Kingsley PJ, Marnett LJ, Das SK, DuBois RN, Dey SK (2004) Aberrant cannabinoid signaling impairs oviductal transport of embryos. Nat Med 10:1074–1080
Horne AW, Phillips JA 3rd, Kane N, Lourenco PC, McDonald SE, Williams AR, Simon C, Dey SK, Critchley HO (2008) CB1 expression is attenuated in Fallopian tube and decidua of women with ectopic pregnancy. PLoS One 3:e3969
Wang H, Matsumoto H, Guo Y, Paria BC, Roberts RL, Dey SK (2003) Differential G protein-coupled cannabinoid receptor signaling by anandamide directs blastocyst activation for implantation. Proc Natl Acad Sci U S A 100:14914–14919
Wang H, Xie H, Guo Y, Zhang H, Takahashi T, Kingsley PJ, Marnett LJ, Das SK, Cravatt BF, Dey SK (2006) Fatty acid amide hydrolase deficiency limits early pregnancy events. J Clin Invest 116:2122–2131
Paria BC, Song H, Wang X, Schmid PC, Krebsbach RJ, Schmid HH, Bonner TI, Zimmer A, Dey SK (2001) Dysregulated cannabinoid signaling disrupts uterine receptivity for embryo implantation. J Biol Chem 276:20523–20528
Schmid PC, Paria BC, Krebsbach RJ, Schmid HH, Dey SK (1997) Changes in anandamide levels in mouse uterus are associated with uterine receptivity for embryo implantation. Proc Natl Acad Sci U S A 94:4188–4192
Guo Y, Wang H, Okamoto Y, Ueda N, Kingsley PJ, Marnett LJ, Schmid HH, Das SK, Dey SK (2005) N-acylphosphatidylethanolamine-hydrolyzing phospholipase D is an important determinant of uterine anandamide levels during implantation. J Biol Chem 280:23429–23432
Habayeb OM, Taylor AH, Finney M, Evans MD, Konje JC (2008) Plasma anandamide concentration and pregnancy outcome in women with threatened miscarriage. JAMA 299:1135–1136
Habayeb OM, Taylor AH, Evans MD, Cooke MS, Taylor DJ, Bell SC, Konje JC (2004) Plasma levels of the endocannabinoid anandamide in women – a potential role in pregnancy maintenance and labor? J Clin Endocrinol Metab 89:5482–5487
Taylor AH, Finney M, Lam PM, Konje JC (2011) Modulation of the endocannabinoid system in viable and non-viable first trimester pregnancies by pregnancy-related hormones. Reprod Biol Endocrinol 9:152
Trabucco E, Acone G, Marenna A, Pierantoni R, Cacciola G, Chioccarelli T, Mackie K, Fasano S, Colacurci N, Meccariello R, Cobellis G, Cobellis L (2009) Endocannabinoid system in first trimester placenta: low FAAH and high CB1 expression characterize spontaneous miscarriage. Placenta 30:516–522
Tsuboi K, Okamoto Y, Ikematsu N, Inoue M, Shimizu Y, Uyama T, Wang J, Deutsch DG, Burns MP, Ulloa NM, Tokumura A, Ueda N (1811) Enzymatic formation of N-acylethanolamines from N-acylethanolamine plasmalogen through N-acylphosphatidylethanolamine-hydrolyzing phospholipase D-dependent and -independent pathways. Biochim Biophys Acta 2011:565–577
Straszewski-Chavez SL, Abrahams VM, Mor G (2005) The role of apoptosis in the regulation of trophoblast survival and differentiation during pregnancy. Endocr Rev 26:877–897
Turco MY, Matsukawa K, Czernik M, Gasperi V, Battista N, Della Salda L, Scapolo PA, Loi P, Maccarrone M, Ptak G (2008) High levels of anandamide, an endogenous cannabinoid, block the growth of sheep preimplantation embryos by inducing apoptosis and reversible arrest of cell proliferation. Hum Reprod 23:2331–2338
Fonseca BM, Correia-da-Silva G, Teixeira NA (2013) The endocannabinoid anandamide induces apoptosis of rat decidual cells through a mechanism involving ceramide synthesis and p38 MAPK activation. Apoptosis 18:1526–1535
Almada M, Piscitelli F, Fonseca BM, Di Marzo V, Correia-da-Silva G, Teixeira N (1851) Anandamide and decidual remodelling: COX-2 oxidative metabolism as a key regulator. Biochim Biophys Acta 2015:1473–1481
Weber A, Ni J, Ling KH, Acheampong A, Tang-Liu DD, Burk R, Cravatt BF, Woodward D (2004) Formation of prostamides from anandamide in FAAH knockout mice analyzed by HPLC with tandem mass spectrometry. J Lipid Res 45:757–763
Buckley NE, Hansson S, Harta G, Mezey E (1998) Expression of the CB1 and CB2 receptor messenger RNAs during embryonic development in the rat. Neuroscience 82:1131–1149
Jiang S, Fu Y, Williams J, Wood J, Pandarinathan L, Avraham S, Makriyannis A, Avraham S, Avraham HK (2007) Expression and function of cannabinoid receptors CB1 and CB2 and their cognate cannabinoid ligands in murine embryonic stem cells. PLoS One 2:e641
Fonseca BM, Correia-da-Silva G, Taylor AH, Konje JC, Bell SC, Teixeira NA (2009) Spatio-temporal expression patterns of anandamide-binding receptors in rat implantation sites: evidence for a role of the endocannabinoid system during the period of placental development. Reprod Biol Endocrinol 7:121
Cabral GA, Ferreira GA, Jamerson MJ (2015) Endocannabinoids and the immune system in health and disease. Handb Exp Pharmacol 231:185–211
Moffett-King A (2002) Natural killer cells and pregnancy. Nat Rev Immunol 2:656–663
Xu YY, Wang SC, Li DJ, Du MR (2017) Co-signaling molecules in maternal-fetal immunity. Trends Mol Med 23:46–58
Berrendero F, Sepe N, Ramos JA, Di Marzo V, Fernández-Ruiz JJ (1999) Analysis of cannabinoid receptor binding and mRNA expression and endogenous cannabinoid contents in the developing rat brain during late gestation and early postnatal period. Synapse 33:181–191
Semple BD, Blomgren K, Gimlin K, Ferriero DM, Noble-Haeusslein LJ (2013) Brain development in rodents and humans: identifying benchmarks of maturation and vulnerability to injury across species. Prog Neurobiol 106–107:1–16
Sun X, Xie H, Yang J, Wang H, Bradshaw HB, Dey SK (2010) Endocannabinoid signaling directs differentiation of trophoblast cell lineages and placentation. Proc Natl Acad Sci U S A 107:16887–16892
Basavarajappa BS, Nixon RA, Arancio O (2009) Endocannabinoid system: emerging role from neurodevelopment to neurodegeneration. Mini-Rev Med Chem 9:448–462
Gaffuri AL, Ladarre D, Lenkei Z (2012) Type-1 cannabinoid receptor signaling in neuronal development. Pharmacology 90:19–39
Vitalis T, Lainé J, Simon A, Roland A, Leterrier C, Lenkei Z (2008) The type 1 cannabinoid receptor is highly expressed in embryonic cortical projection neurons and negatively regulates neurite growth in vitro. Eur J Neurosci 28:1705–1718
Saez TM, Aronne MP, Caltana L, Brusco AH (2014) Prenatal exposure to the CB1 and CB2 cannabinoid receptor agonist WIN 55,212-2 alters migration of early-born glutamatergic neurons and GABAergic interneurons in the rat cerebral cortex. J Neurochem 129:637–648
Berghuis P, Rajnicek AM, Morozov YM, Ross RA, Mulder J, Urbán GM, Monory K, Marsicano G, Matteoli M, Canty A, Irving AJ, Katona I, Yanagawa Y, Rakic P, Lutz B, Mackie K, Harkany T (2007) Hardwiring the brain: endocannabinoids shape neuronal connectivity. Science 316:1212–1216
Aguado T, Monory K, Palazuelos J, Stella N, Cravatt B, Lutz B, Marsicano G, Kokaia Z, Guzmán M, Galve-Roperh I (2005) The endocannabinoid system drives neural progenitor proliferation. FASEB J 19:1704–1706
Palazuelos J, Aguado T, Egia A, Mechoulam R, Guzmán M, Galve-Roperh I (2006) Non-psychoactive CB2 cannabinoid agonists stimulate neural progenitor proliferation. FASEB J 20:2405–2407
Aguado T, Palazuelos J, Monory K, Stella N, Cravatt B, Lutz B, Marsicano G, Kokaia Z, Guzmán M, Galve-Roperh I (2006) The endocannabinoid system promotes astroglial differentiation by acting on neural progenitor cells. J Neurosci 26:1551–1561
Rueda D, Navarro B, Martinez-Serrano A, Guzman M, Galve-Roperh I (2002) The endocannabinoid anandamide inhibits neuronal progenitor cell differentiation through attenuation of the Rap1/B-Raf/ERK pathway. J Biol Chem 277:46645–46650
Bromberg KD, Ma’ayan A, Neves SR, Iyengar R (2008) Design logic of a cannabinoid receptor signaling network that triggers neurite outgrowth. Science 320:903–909
Jutras-Aswad D, DiNieri JA, Harkany T, Hurd YL (2009) Neurobiological consequences of maternal cannabis on human fetal development and its neuropsychiatric outcome. Eur Arch Psychiatry Clin Neurosci 259:395–412
Wang X, Dow-Edwards D, Anderson V, Minkoff H, Hurd YL (2004) In utero marijuana exposure associated with abnormal amygdala dopamine D2 gene expression in the human fetus. Biol Psychiatry 56:909–915
Bonnin A, de Miguel R, Castro JG, Ramos JA, Fernandez-Ruiz JJ (1996) Effects of perinatal exposure to delta 9-tetrahydrocannabinol on the fetal and early postnatal development of tyrosine hydroxylase-containing neurons in rat brain. J Mol Neurosci 7:291–308
Suárez I, Bodega G, Fernández-Ruiz J, Ramos JA, Rubio M, Fernández B (2004) Down-regulation of the AMPA glutamate receptor subunits GluR1 and GluR2/3 in the rat cerebellum following pre- and perinatal delta9-tetrahydrocannabinol exposure. Cerebellum 3:66–74
Suárez I, Bodega G, Rubio M, Fernández-Ruiz JJ, Ramos JA, Fernández B (2004) Prenatal cannabinoid exposure down- regulates glutamate transporter expressions (GLAST and EAAC1) in the rat cerebellum. Dev Neurosci 26:45–53
Basavarajappa BS (2015) Fetal alcohol spectrum disorder: potential role of endocannabinoids signaling. Brain Sci 5:456–493
Bukiya AN, Dopico AM (2018) Fetal cerebral circulation as target of maternal alcohol consumption. Alcohol Clin Exp Res 42:1006–1018
Tobiasz AM, Duncan JR, Bursac Z, Sullivan RD, Tate DL, Dopico AM, Bukiya AN, Mari G (2018) The effect of prenatal alcohol exposure on fetal growth and cardiovascular parameters in a baboon model of pregnancy. Reprod Sci 25:1116–1123
Zurolo E, Iyer AM, Spliet WG, Van Rijen PC, Troost D, Gorter JA, Aronica E (2010) CB1 and CB2 cannabinoid receptor expression during development and in epileptogenic developmental pathologies. Neuroscience 170:28–41
Wang X, Dow-Edwards D, Keller E, Hurd YL (2003) Preferential limbic expression of the cannabinoid receptor mRNA in the human fetal brain. Neuroscience 118:681–694
Hurd YL, Wang X, Anderson V, Beck O, Minkoff H, Dow-Edwards D (2005) Marijuana impairs growth in mid-gestation fetuses. Neurotoxicol Teratol 27:221–229
Day NL, Goldschmidt L, Thomas CA (2006) Prenatal marijuana exposure contributes to the prediction of marijuana use at age 14. Addiction 101:1313–1322
Brocato B, Zoerner AA, Janjetovic Z, Skobowiat C, Gupta S, Moore BM 2nd, Slominski A, Zhang J, Schenone M, Phinehas R, Ferry RJ Jr, Dick E Jr, Hubbard GB, Mari G, Schlabritz-Loutsevitch N (2013) Endocannabinoid crosstalk between placenta and maternal fat in a baboon model (Papio spp.) of obesity. Placenta 34:983–989
Fride E, Ginzburg Y, Breuer A, Bisogno T, Di Marzo V, Mechoulam R (2001) Critical role of the endogenous cannabinoid system in mouse pup suckling and growth. Eur J Pharmacol 419:207–214
Fride E, Gobshtis N, Dahan H, Weller A, Giuffrida A, Ben-Shabat S (2009) The endocannabinoid system during development: emphasis on perinatal events and delayed effects. Vitam Horm 81:139–158
Fernández-Ruiz J, Berrendero F, Hernández ML, Ramos JA (2000) The endogenous cannabinoid system and brain development. Trends Neurosci 23:14–20
Mato S, Del Olmo E, Pazos A (2003) Ontogenetic development of cannabinoid receptor expression and signal transduction functionality in the human brain. Eur J Neurosci 17:1747–1754
Gomes FV, Edelson JR, Volk DW, Grace AA (2018) Altered brain cannabinoid 1 receptor mRNA expression across postnatal development in the MAM model of schizophrenia. Schizophr Res 201:254–260
Yoneda T, Kameyama K, Esumi K, Daimyo Y, Watanabe M, Hata Y (2013) Developmental and visual input-dependent regulation of the CB1 cannabinoid receptor in the mouse visual cortex. PLoS One 8:e53082
Fride E, Mechoulam R (1996) Developmental aspects of anandamide: ontogeny of response and prenatal exposure. Psychoneuroendocrinology 21:157–172
Trezza V, Campolongo P, Manduca A, Morena M, Palmery M, Vanderschuren LJ, Cuomo V (2012) Altering endocannabinoid neurotransmission at critical developmental ages: impact on rodent emotionality and cognitive performance. Front Behav Neurosci 6:2
Trezza V, Campolongo P, Cassano T, Macheda T, Dipasquale P, Carratù MR, Gaetani S, Cuomo V (2008) Effects of perinatal exposure to delta-9-tetrahydrocannabinol on the emotional reactivity of the offspring: a longitudinal behavioral study in Wistar rats. Psychopharmacology 198:529–537
McGregor IS, Dastur FN, McLellan RA, Brown RE (1996) Cannabinoid modulation of rat pup ultrasonic vocalizations. Eur J Pharmacol 313:43–49
Navarro M, Rubio P, de Fonseca FR (1995) Behavioural consequences of maternal exposure to natural cannabinoids in rats. Psychopharmacology 122:1–14
Fried PA, Smith AM (2001) A literature review of the consequences of prenatal marihuana exposure. An emerging theme of a deficiency in aspects of executive function. Neurotoxicol Teratol 23:1–11
Schneider M (2009) Cannabis use in pregnancy and early life and its consequences: animal models. Eur Arch Psychiatry Clin Neurosci 259:383–393
Campolongo P, Trezza V, Ratano P, Palmery M, Cuomo V (2011) Developmental consequences of perinatal cannabis exposure: behavioral and neuroendocrine effects in adult rodents. Psychopharmacology 214:5–15
del Arco I, Muñoz R, Rodríguez De Fonseca F, Escudero L, Martín-Calderón JL, Navarro M, Villanúa MA (2000) Maternal exposure to the synthetic cannabinoid HU-210: effects on the endocrine and immune systems of the adult male offspring. Neuroimmunomodulation 7:16–26
Economidou D, Mattioli L, Ubaldi M, Lourdusamy A, Soverchia L, Hardiman G, Campolongo P, Cuomo V, Ciccocioppo R (2007) Role of cannabinoidergic mechanisms in ethanol self-administration and ethanol seeking in rat adult offspring following perinatal exposure to Delta9-tetrahydrocannabinol. Toxicol Appl Pharmacol 223:73–85
Spano MS, Ellgren M, Wang X, Hurd YL (2007) Prenatal cannabis exposure increases heroin seeking with allostatic changes in limbic enkephalin systems in adulthood. Biol Psychiatry 61:554–563
Campolongo P, Trezza V, Cassano T, Gaetani S, Morgese MG, Ubaldi M, Soverchia L, Antonelli T, Ferraro L, Massi M, Ciccocioppo R, Cuomo V (2007) Perinatal exposure to delta-9-tetrahydrocannabinol causes enduring cognitive deficits associated with alteration of cortical gene expression and neurotransmission in rats. Addict Biol 12:485–495
Molina-Holgado F, Alvarez FJ, Gonzalez I, Antonio MT, Leret ML (1997) Maternal exposure to delta 9-tetrahydrocannabinol (delta 9-THC) alters indolamine levels and turnover in adult male and female rat brain regions. Brain Res Bull 43:173–178
Mereu G, Fà M, Ferraro L, Cagiano R, Antonelli T, Tattoli M, Ghiglieri V, Tanganelli S, Gessa GL, Cuomo V (2003) Prenatal exposure to a cannabinoid agonist produces memory deficits linked to dysfunction in hippocampal long-term potentiation and glutamate release. Proc Natl Acad Sci U S A 100:4915–4920
Antonelli T, Tanganelli S, Tomasini MC, Finetti S, Trabace L, Steardo L, Sabino V, Carratu MR, Cuomo V, Ferraro L (2004) Long-term effects on cortical glutamate release induced by prenatal exposure to the cannabinoid receptor agonist (R)-(+)-[2,3-dihydro-5-methyl-3-(4-morpholinyl-methyl)pyrrolo[1,2,3-de]-1,4-benzoxazin-6-yl]-1-naphthalenylmethanone: an in vivo microdialysis study in the awake rat. Neuroscience 124:367–375
Castaldo P, Magi S, Gaetani S, Cassano T, Ferraro L, Antonelli T, Amoroso S, Cuomo V (2007) Prenatal exposure to the cannabinoid receptor agonist WIN 55,212-2 increases glutamate uptake through overexpression of GLT1 and EAAC1 glutamate transporter subtypes in rat frontal cerebral cortex. Neuropharmacology 53:369–378
Ferraro L, Tomasini MC, Beggiato S, Gaetani S, Cassano T, Cuomo V, Amoroso S, Tanganelli S, Antonelli T (2009) Short- and long-term consequences of prenatal exposure to the cannabinoid agonist WIN55,212-2 on rat glutamate transmission and cognitive functions. J Neural Transm (Vienna) 116:1017–1027
Antonelli T, Tomasini MC, Tattoli M, Cassano T, Tanganelli S, Finetti S, Mazzoni E, Trabace L, Steardo L, Cuomo V, Ferraro L (2005) Prenatal exposure to the CB1 receptor agonist WIN 55,212-2 causes learning disruption associated with impaired cortical NMDA receptor function and emotional reactivity changes in rat offspring. Cereb Cortex 15:2013–2020
Dalterio S, Thomford PJ, Michael SD, DeAngelo L, Mayfield D (1986) Perinatal cannabinoid exposure: effects on hepatic cytochrome P-450 and plasma protein levels in male mice. Teratology 33:195–201
Dalterio S, Blum K, DeLallo L, Sweeney C, Briggs A, Bartke A (1980) Perinatal exposure to delta 9-THC in mice: altered enkephalin and norepinephrine sensitivity in vas deferens. Subst Alcohol Actions Misuse 1:467–471
Mokler DJ, Robinson SE, Johnson JH, Hong JS, Rosecrans JA (1987) Neonatal administration of delta-9-tetrahydrocannabinol (THC) alters the neurochemical response to stress in the adult Fischer-344 rat. Neurotoxicol Teratol 9:321–327
Newsom RJ, Kelly SJ (2008) Perinatal delta-9-tetrahydrocannabinol exposure disrupts social and open field behavior in adult male rats. Neurotoxicol Teratol 30:213–219
Vela G, Martín S, García-Gil L, Crespo JA, Ruiz-Gayo M, Fernández-Ruiz JJ, García-Lecumberri C, Pélaprat D, Fuentes JA, Ramos JA, Ambrosio E (1998) Maternal exposure to delta9-tetrahydrocannabinol facilitates morphine self-administration behavior and changes regional binding to central mu opioid receptors in adult offspring female rats. Brain Res 807:101–109
Llorente R, Llorente-Berzal A, Petrosino S, Marco EM, Guaza C, Prada C, López-Gallardo M, Di Marzo V, Viveros MP (2008) Gender-dependent cellular and biochemical effects of maternal deprivation on the hippocampus of neonatal rats: a possible role for the endocannabinoid system. Dev Neurobiol 68:1334–1347
Suárez J, Rivera P, Llorente R, Romero-Zerbo SY, Bermúdez-Silva FJ, de Fonseca FR, Viveros MP (2010) Early maternal deprivation induces changes on the expression of 2-AG biosynthesis and degradation enzymes in neonatal rat hippocampus. Brain Res 1349:162–173
Suárez J, Llorente R, Romero-Zerbo SY, Mateos B, Bermúdez-Silva FJ, de Fonseca FR, Viveros MP (2009) Early maternal deprivation induces gender-dependent changes on the expression of hippocampal CB(1) and CB(2) cannabinoid receptors of neonatal rats. Hippocampus 19:623–632
Fride E, Suris R, Weidenfeld J, Mechoulam R (2005) Differential response to acute and repeated stress in cannabinoid CB1 receptor knockout newborn and adult mice. Behav Pharmacol 16:431–440
Marco EM, Echeverry-Alzate V, López-Moreno JA, Giné E, Peñasco S, Viveros MP (2014) Consequences of early life stress on the expression of endocannabinoid-related genes in the rat brain. Behav Pharmacol 25:547–556
Viveros MP, Llorente R, Suarez J, Llorente-Berzal A, López-Gallardo M, de Fonseca FR (2012) The endocannabinoid system in critical neurodevelopmental periods: sex differences and neuropsychiatric implications. J Psychopharmacol 26:164–176
Craft RM, Marusich JA, Wiley JL (2013) Sex differences in cannabinoid pharmacology: a reflection of differences in the endocannabinoid system? Life Sci 92:476–481
Dow-Edwards D, Frank A, Wade D, Weedon J, Izenwasser S (2016) Sexually-dimorphic alterations in cannabinoid receptor density depend upon prenatal/early postnatal history. Neurotoxicol Teratol 58:31–39
Wagner EJ (2016) Sex differences in cannabinoid-regulated biology: a focus on energy homeostasis. Front Neuroendocrinol 40:101–109
Cooper ZD, Craft RM (2018) Sex-dependent effects of cannabis and cannabinoids: a translational perspective. Neuropsychopharmacology 43:34–51
Lee TT, Gorzalka BB (2012) Timing is everything: evidence for a role of corticolimbic endocannabinoids in modulating hypothalamic-pituitary-adrenal axis activity across developmental periods. Neuroscience 204:17–30
Schreiner F, Ackermann M, Michalik M, Hucklenbruch-Rother E, Bilkei-Gorzo A, Racz I, Bindila L, Lutz B, Dötsch J, Zimmer A, Woelfle J (2017) Developmental programming of somatic growth, behavior and endocannabinoid metabolism by variation of early postnatal nutrition in a cross-fostering mouse model. PLoS One 12:e0182754
Almeida MM, Dias-Rocha CP, Souza AS, Muros MF, Mendonca LS, Pazos-Moura CC, Trevenzoli IH (2017) Perinatal maternal high-fat diet induces early obesity and sex-specific alterations of the endocannabinoid system in white and brown adipose tissue of weanling rat offspring. Br J Nutr 118:788–803
Dias-Rocha CP, Almeida MM, Santana EM, Costa JCB, Franco JG, Pazos-Moura CC, Trevenzoli IH (2018) Maternal high-fat diet induces sex-specific endocannabinoid system changes in newborn rats and programs adiposity, energy expenditure and food preference in adulthood. J Nutr Biochem 51:56–68
Subbanna S, Shivakumar M, Psychoyos D, Xie S, Basavarajappa BS (2013) Anandamide-CB1 receptor signaling contributes to postnatal ethanol-induced neonatal neurodegeneration, adult synaptic, and memory deficits. J Neurosci 33:6350–6366
Subbanna S, Psychoyos D, Xie S, Basavarajappa BS (2015) Postnatal ethanol exposure alters levels of 2-arachidonylglycerol-metabolizing enzymes and pharmacological inhibition of monoacylglycerol lipase does not cause neurodegeneration in neonatal mice. J Neurochem 134:276–287
Gandhi K, Li C, German N, Skobowiat C, Carrillo M, Kallem RR, Larumbe E, Martinez S, Chuecos M, Ventolini G, Nathanielsz P, Schlabritz-Loutsevitch N (2018) Effect of maternal high-fat diet on key components of the placental and hepatic endocannabinoid system. Am J Physiol Endocrinol Metab 314:E322–E323
Long LE, Lind J, Webster M, Weickert CS (2012) Developmental trajectory of the endocannabinoid system in human dorsolateral prefrontal cortex. BMC Neurosci 13:87
Fried PA (1982) Marihuana use by pregnant women and effects on offspring: an update. Neurobehav Toxicol Teratol 4:451–454
Fried PA, O’Connell CM (1987) A comparison of the effects of prenatal exposure to tobacco, alcohol, cannabis and caffeine on birth size and subsequent growth. Neurotoxicol Teratol 9:79–85
Leech SL, Richardson GA, Goldschmidt L, Day NL (1999) Prenatal substance exposure: effects on attention and impulsivity of 6-year-olds. Neurotoxicol Teratol 21:109–118
Fried PA, Watkinson B, Gray R (1998) Differential effects on cognitive functioning in 9- to 12-year olds prenatally exposed to cigarettes and marihuana. Neurotoxicol Teratol 20:293–306
Goldschmidt L, Richardson GA, Cornelius MD, Day NL (2004) Prenatal marijuana and alcohol exposure and academic achievement at age 10. Neurotoxicol Teratol 26:521–532
Smith AM, Fried PA, Hogan MJ, Cameron I (2006) Effects of prenatal marijuana on visuospatial working memory: an fMRI study in young adults. Neurotoxicol Teratol 28:286–295
Smith A, Fried P, Hogan M, Cameron I (2004) The effects of prenatal and current marijuana exposure on response inhibition: a functional magnetic resonance imaging study. Brain Cogn 54:147–149
Fried PA, James DS, Watkinson B (2001) Growth and pubertal milestones during adolescence in offspring prenatally exposed to cigarettes and marihuana. Neurotoxicol Teratol 23:431–436
Spear LP (2000) The adolescent brain and age-related behavioral manifestations. Neurosci Biobehav Rev 24:417–463
Meruelo AD, Castro N, Cota CI, Tapert SF (2017) Cannabis and alcohol use, and the developing brain. Behav Brain Res 325:44–50
Hall W, Degenhardt L (2009) Adverse health effects of non-medical cannabis use. Lancet 374:1383–1391
Galve-Roperh I, Chiurchiù V, Díaz-Alonso J, Bari M, Guzmán M, Maccarrone M (2013) Cannabinoid receptor signaling in progenitor/stem cell proliferation and differentiation. Prog Lipid Res 52:633–650
Kozela E, Juknat A, Vogel Z (2017) Modulation of astrocyte activity by cannabidiol, a nonpsychoactive cannabinoid. Int J Mol Sci 18:E1669
Rodríguez de Fonseca F, Ramos JA, Bonnin A, Fernández-Ruiz JJ (1993) Presence of cannabinoid binding sites in the brain from early postnatal ages. Neuroreport 4:135–138
Heng L, Beverley JA, Steiner H, Tseng KY (2011) Differential developmental trajectories for CB1 cannabinoid receptor expression in limbic/associative and sensorimotor cortical areas. Synapse 65:278–286
Ellgren M, Artmann A, Tkalych O, Gupta A, Hansen HS, Hansen SH, Devi LA, Hurd YL (2008) Dynamic changes of the endogenous cannabinoid and opioid mesocorticolimbic systems during adolescence: THC effects. Eur Neuropsychopharmacol 18:826–834
Quinn HR, Matsumoto I, Callaghan PD, Long LE, Arnold JC, Gunasekaran N, Thompson MR, Dawson B, Mallet PE, Kashem MA, Matsuda-Matsumoto H, Iwazaki T, McGregor IS (2008) Adolescent rats find repeated Delta(9)-THC less aversive than adult rats but display greater residual cognitive deficits and changes in hippocampal protein expression following exposure. Neuropsychopharmacology 33:1113–1126
Schneider M, Koch M (2003) Chronic pubertal, but not adult chronic cannabinoid treatment impairs sensorimotor gating, recognition memory, and the performance in a progressive ratio task in adult rats. Neuropsychopharmacology 28:1760–1769
O’Shea M, Singh ME, McGregor IS, Mallet PE (2004) Chronic cannabinoid exposure produces lasting memory impairment and increased anxiety in adolescent but not adult rats. J Psychopharmacol 18:502–508
O’Shea M, McGregor IS, Mallet PE (2006) Repeated cannabinoid exposure during perinatal, adolescent or early adult ages produces similar long-lasting deficits in object recognition and reduced social interaction in rats. J Psychopharmacol 20:611–621
Marco EM, Rubino T, Adriani W, Viveros MP, Parolaro D, Laviola G (2009) Long-term consequences of URB597 administration during adolescence on cannabinoid CB1 receptor binding in brain areas. Brain Res 1257:25–31
Realini N, Vigano’ D, Guidali C, Zamberletti E, Rubino T, Parolaro D (2011) Chronic URB597 treatment at adulthood reverted most depressive-like symptoms induced by adolescent exposure to THC in female rats. Neuropharmacology 60:235–243
Lovelace JW, Corches A, Vieira PA, Hiroto AS, Mackie K, Korzus E (2015) An animal model of female adolescent cannabinoid exposure elicits a long-lasting deficit in presynaptic long-term plasticity. Neuropharmacology 99:242–255
Ellgren M, Spano SM, Hurd YL (2007) Adolescent cannabis exposure alters opiate intake and opioid limbic neuronal populations in adult rats. Neuropsychopharmacology 32:607–615
Rubino T, Viganò D, Realini N, Guidali C, Braida D, Capurro V, Castiglioni C, Cherubino F, Romualdi P, Candeletti S, Sala M, Parolaro D (2008) Chronic delta 9-tetrahydrocannabinol during adolescence provokes sex-dependent changes in the emotional profile in adult rats: behavioral and biochemical correlates. Neuropsychopharmacology 33:2760–2771
Rubino T, Realini N, Braida D, Alberio T, Capurro V, Viganò D, Guidali C, Sala M, Fasano M, Parolaro D (2009) The depressive phenotype induced in adult female rats by adolescent exposure to THC is associated with cognitive impairment and altered neuroplasticity in the prefrontal cortex. Neurotox Res 15:291–302
Rubino T, Realini N, Braida D, Guidi S, Capurro V, Viganò D, Guidali C, Pinter M, Sala M, Bartesaghi R, Parolaro D (2009) Changes in hippocampal morphology and neuroplasticity induced by adolescent THC treatment are associated with cognitive impairment in adulthood. Hippocampus 19:763–772
Choi K, Le T, McGuire J, Xing G, Zhang L, Li H, Parker CC, Johnson LR, Ursano RJ (2012) Expression pattern of the cannabinoid receptor genes in the frontal cortex of mood disorder patients and mice selectively bred for high and low fear. J Psychiatr Res 46:882–889
Ehrenreich H, Rinn T, Kunert HJ, Moeller MR, Poser W, Schilling L, Gigerenzer G, Hoehe MR (1999) Specific attentional dysfunction in adults following early start of cannabis use. Psychopharmacology 142:295–301
Bambico FR, Nguyen NT, Katz N, Gobbi G (2010) Chronic exposure to cannabinoids during adolescence but not during adulthood impairs emotional behavior and monoaminergic neurotransmission. Neurobiol Dis 37:641–655
Pijlman FT, Rigter SM, Hoek J, Goldschmidt HM, Niesink RJ (2005) Strong increase in total delta-THC in cannabis preparations sold in Dutch coffee shops. Addict Biol 10:171–180
Mehmedic Z, Chandra S, Slade D, Denham H, Foster S, Patel AS, Ross SA, Khan IA, ElSohly MA (2010) Potency trends of Δ9-THC and other cannabinoids in confiscated cannabis preparations from 1993 to 2008. J Forensic Sci 55:1209–1217
Acknowledgements
The author is thankful to Dr. Dejian Ma and Dr. Wei Li (Dept. Pharmaceutical Sciences, University of Tennessee Health Science Center) for mass spectroscopy quantifications of cannabinoid levels in baboon blood and tissue samples. The author also extends gratitude to Dr. Syed Ali (US Food and Drug Administration) for critical reading of the manuscript and Dr. Richard Redfearn (Office of Scientific Writing, Office of Research, University of Tennessee Health Science Center) for editorial assistance. This work was supported by the National Institutes of Health grant number R21 AA022433 [ANB].
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Bukiya, A.N. (2019). Physiology of the Endocannabinoid System During Development. In: Bukiya, A. (eds) Recent Advances in Cannabinoid Physiology and Pathology. Advances in Experimental Medicine and Biology, vol 1162. Springer, Cham. https://doi.org/10.1007/978-3-030-21737-2_2
Download citation
DOI: https://doi.org/10.1007/978-3-030-21737-2_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-21736-5
Online ISBN: 978-3-030-21737-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)