Abstract Volume-sensitive outwardly rectifying anion channels (VSOACs) are expressed in pulmonary artery smooth muscle cells (PASMCs) and have been implicated in cell proliferation, growth, apoptosis and protection against oxidative stress. In this chapter, we review the properties of native VSOACs in PASMCs, and consider the evidence that ClC-3, a member of the ClC superfamily of voltage dependent Cl- channels, may be responsible for native VSOACs in PASMCs. Finally, we examine whether or not native VSOACs and heterologously expressed ClC-3 channels function as bona fide chloride channels or as chloride/proton antiporters.
Access provided by Autonomous University of Puebla. Download conference paper PDF
Similar content being viewed by others
Keywords
1 Introduction
Volume-sensitive outwardly rectifying anion channels (VSOACs) are ubiquitously expressed in mammalian cells and play a vitally important physiological role in a variety of cellular functions, including cell volume homeostasis, proliferation, apoptosis, and the regulation of electrical activity.1 VSOACs have been implicated in a number of these functions in vascular smooth muscle cells (SMCs) as well. For example, the magnitude of VSOAC currents in actively growing SMCs is higher than in growth-arrested or differentiated SMCs, suggesting that VSOACs may be important for SMC proliferation.2 There is evidence that pressure-induced depolarization and contraction of cerebral artery smooth muscle may be partially mediated by VSOACs.3
Although the exact identification of the proteins responsible for native VSOACs has proven to be elusive, the short isoform of ClC-3 (sClC-3), a member of the ClC superfamily of voltage-dependent chloride channels, has been proposed to be the molecular correlate of the native VSOAC in some cells, including cardiac myocytes and vascular SMCs.4,5 This hypothesis has been corroborated by a series of other independent studies from different laboratories.6-11 Despite these data, the role of ClC-3 as a constituent of native VSOACs remains controversial.12-14 Much of this controversy comes from results reported from the first transgenic ClC-3 global knockout (ClCn3 -/-) mouse produced by Jentsch and coworkers.15 They reported the apparent presence of native VSOACs in at least two different cell types from ClCn3 -/- mice. However, later experiments using global ClCn3 -/- transgenic mice revealed that the properties of native VSOACs were actually altered in heart, and there appeared to be significant compensatory changes in expression of a variety of other membrane proteins (including upregulation of two other members of the ClC chloride channel family), raising fundamental questions about the usefulness of the global ClCn3 -/- mouse model to assess ClC-3 function.16 It has been demonstrated that transgenic mice with cardiac-specific overexpression of the human short ClC-3 (hsClC-3) isoform exhibit enhanced VSOAC currents and accelerated regulatory volume decreases,17 which is consistent with a molecular role for sClC-3 in native VSOAC function.
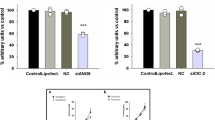
It has been demonstrated that ClC-3 is expressed in human aortic SMCs18 and pulmonary artery SMCs (PASMCs).5 It was demonstrated that antisense oligonucleotide-mediated downregulation of ClC-3 dramatically inhibits cell proliferation of rat aortic SMCs.19 The ClCn-3 gene appears to be upregulated in rat pulmonary artery and heart in response to monocrotaline-induced pulmonary hypertension and in canine cultured PASMCs incubated with inflammatory mediators. PASMCs infected to overexpress ClC-3 exhibited enhanced viability against H2O2, thus suggesting that ClC-3 may improve the resistance of VSMCs to reactive oxygen species (ROS) in an environment of elevated inflammatory cytokines in hypertensive pulmonary arteries.20 These and other studies suggested that activation of ClC-3 channels may indeed play a role in proliferation, growth, volume regulation, and apoptosis of vascular SMCs (see Ref. 21 for review).
2 Properties of Native VSOACs in PASMCs
Quantitative reverse-transcription polymerase chain reaction (RT-PCR) has been used to test for molecular expression of ClC-3 in canine pulmonary smooth muscle. Primers were designed to be specific for ClC-3 and do not cross hybridize to other members of the ClC gene family. The competitive “mimic” strategy of quantitative PCR was employed.12 As shown in Fig. 15.1a, quantitative RT-PCR detected significant levels of ClC-3 transcriptional expression from pulmonary arteries. The figure illustrates a representative gel used in digital analysis and comparison of mimic and ClC-3 amplification. Digital analysis and comparison of mimic and ClC-3-specific amplification products was performed on the 10-4 dilution of mimic DNA and was repeated on three independently generated samples. ClC-3 expression was 48.0% of β-actin in pulmonary artery. Figure 15.1b, c illustrate the activation of native VSOACs in canine PASMCs by exposure to hypotonic (230 mOsm) extracellular solutions. Exposure to a hypotonic solution causes cells to swell, which results in the delayed activation of VSOACs. Membrane currents at -100 and +100 mV were almost negligible in the isotonic solution but began to increase following a delay of some 3-4 min after changing to the hypotonic solution. Figure 15.1b shows raw current traces evoked by step pulses, which developed during exposure to hypotonic solution, and these were completely abolished by a 10-min perfusion with a hypertonic solution. In these experiments, possible contamination by cation currents was prevented using impermeant cations and appropriate blockers. Figure 15.1c is a plot of the current-voltage relations obtained from several cells in solutions with different osmolarities. In these experiments, both bath and pipet solutions contained 115 mM Cl-, and the currents activated during exposure to hypotonic solution exhibited clear outward rectification. The reversal potential was approximately 0 mV, which is the predicted equilibrium potential for Cl- (0 mV). The hypotonically activated currents were reduced by subsequent exposure to hypertonic solutions at each membrane potential. Membrane currents activated by exposure to hypotonic solutions were also markedly inhibited by the stilbene compound DIDS (4,4′-diisothiocyanatostilbene-2,2′-disulphonic acid).
ClC-3 expression and native VSOACs in canine PASMCs. (a) Representative gel of quantitative RT-PCR for ClC-3 in canine pulmonary arteries; competitive PCR products were resolved on 2% ethidium bromide agarose gels. Tenfold serial dilutions of mimic DNA were included in the PCRs, while target cDNA (ClC-3) concentration remained constant. The actual concentrations of target complementary DNA (cDNA) were calculated and expressed as percent of β-actin RNA concentration. (b) Raw VSOAC currents activated by hypotonic solutions during 150-ms voltage steps from 0 mV to potentials ranging from -100 to 50 mV. The cell was first equilibrated with the isotonic solution and then exposed to the hypotonic solution. Activations of VSOACs were reversed by exposure to hypertonic solutions. (c) Current-voltage relations for volume-regulated currents in the isotonic, hypotonic, and hypertonic solutions with 115 mM [Cl-]o and 115 mM [Cl-]i (n = 4). Modified with permission5
Figure 15.2 illustrates the effects of intracellular dialysis with an anti-ClC-3 carboxyl terminus antibody (C670-687 Ab) on native VSOAC currents in PASMCs. Membrane currents were obtained by applying 100-ms step pulses to ±80 mV from a holding potential of -40 mV every 30 s. In Fig. 15.2a, b, the time courses of change in the amplitudes of membrane currents measured at ±80 mV are shown, and original current traces obtained at the time points indicated by small letters are depicted in the insets. In a cell dialyzed with 10 μg mL-1 C670-687 Ab for over 10 min, basal membrane currents gradually declined in isotonic bath solution. Subsequent hypotonic cell swelling failed to induce any increase of the current amplitude (Fig. 15.2a). To know whether the observed inhibitory effects of C670-687 Ab on VSOACs were due to specific binding, similar experiments were repeated with the antigen-preabsorbed C670-687 Ab. Figure 15.2b shows a representative experiment. In contrast to the effects observed with the C670-687 Ab alone, dialysis with 10 μg mL-1 antigen-preabsorbed C670-687 Ab for over 10 min did not prevent activation of VSOACs on hypotonic cell swelling. Subsequent exposure of the cell to hypertonic bath solution totally reversed the swelling-induced VSOAC currents.
Inhibition of native VSOACs in canine PASMCs by anti-ClC-3 C670-687 Ab intracellular dialysis. Membrane currents were induced by repetitive 100-ms voltage steps to ±80 mV from a holding potential of -40 mV every 30 s. (a, b) Time courses of change in current amplitude measured at both -80 mV (filled circles) and +80 mV (open circles) in two representative cells intracellular dialyzed with either 10 μg mL-1 ClC-3 C670-687 Ab (a) or the antigen-preabsorbed C670-687 Ab (b). The bars underneath the current traces indicate different bath solutions. Original current recordings obtained at the time points indicated by small letters are shown in the corresponding insets. Modified with permission32
3 Anion Selectivity of Native VSOACs in PASMCs and sClC-3 Heterologously Expressed in NIH/3T3 Cells
To examine Cl- dependence, the reversal potentials E rev for the volume-sensitive currents were measured using either voltage steps or ramps in hypotonic solutions containing six different concentrations of external Cl- ([Cl-]o), replaced with aspartate. As shown in Fig. 15.3a, reducing [Cl-]o from 115 to 28 and 9 mM shifted E rev rightward, indicating a strong Cl- dependence of the volume-sensitive conductance. The inset shows the relationship between [Cl-]o and E rev of the volume-sensitive conductance obtained from a number of pulmonary cells. The straight line represents a theoretical slope of 57 mV per tenfold decrease in [Cl-]o, which is predicted from the Nernst equation assuming that Cl- is the only permeable ion. The slope of the relationship measured experimentally closely followed the predicted slope of 57 mV per tenfold change in [Cl-]o for changes in [Cl-]o greater than 40 mM but deviated from the predicted slope at [Cl-]o less than 40 mM, suggesting that the replacement anion, Asp-, may exhibit some limited permeability through these channels.
Effect of [Cl-]o (a) and anion substitution (b) on current-voltage relations of VSOAC currents elicited in canine pulmonary arterial smooth muscle cells by voltage steps or ramps. (a) The pipet solution contained 24 mM Cl- (n = 5). Inset, relation between the reversal potential (E rev) and [Cl-]o. Each circle indicates the mean value of E rev with standard errors of the means (SEM) from N observations indicated in the parentheses. The straight line indicates the theoretical slope of 57 mV per tenfold decrease in [Cl-]o, which is predicted from the Nernst equation. (b) NaCl (115 mM) in the bath solution was entirely replaced with the same concentration of NaI, NaBr, NaSCN, or Na aspartate. The pipet solution contained 115 mM Cl-. Modified with permission5
Relative anion selectivity was determined by total replacement of Cl- with other anions in the hypotonic solutions. Figure 15.3b shows typical hypotonically activated membrane currents elicited in a pulmonary cell by voltage ramps applied in the presence of different extracellular anions. I- appeared to be slightly more permeable, compared to Br-, which was more permeable than Cl- in this example. Likewise, SCN- appeared to be more permeable compared to Cl-, which was more permeable than aspartate-. The mean data accumulated from a group of cells gave E rev values (in mV) of -8.29 ± 0.92 (n = 7), -4.67 ± 1.49 (n = 12), -3.30 ± 1.16 (n = 10), 0.46 ± 1.01 (n = 13) and 12.40 ± 1.69 (n = 5) for SCN-, I-, Br-, Cl- and aspartate-, respectively. Accordingly, the relative permeability for each anion (X-) to Cl- \({\rm Cl}^- (P_{{\rm x}^-}/P_{{\rm Cl}^-})\) was estimated using the Goldman-Hodgkin-Katz equation. The sequence of \(P_{{\rm x}^-}/P_{{\rm Cl}^-}\) was SCN- (1.36 ± 0.06) > I- (1.19 ± 0.06) > Br- (1.09 ± 0.04) > Cl- (1.00) > aspartate- (0.63 ± 0.05). These data indicate that these membrane currents activated by hypotonic cell swelling in PASMCs can be identified as VSOACs.
sClC-3 has been successfully expressed in NIH/3T3 cells4 and in A10 vascular SMCs.11 In both cell types, sClC-3 transfection gives rise to larger volume-sensitive Cl- currents, compared to untransfected cells, with properties resembling those of native VSOACs. VSOACs in A10 sClC-3-transfected cells are completely abolished by intracellular dialysis of an anti-ClC-3 antibody and by ClC-3 antisense oligonucleotides.
We have examined the relative anion selectivity of expressed sClC-3 currents in NIH/3T3 cells to determine if it is similar to the anion permeability properties of native VSOACs in canine PASMCs (cf. Fig. 15.3). The results of these experiments are summarized in Table 15.1. To measure relative whole-cell anion permeability, external NaCl was replaced by the sodium salt of various anions. Reversal potentials were measured for each Cl- substitute (X) and the relative shifts in reversal potential (E X - E Cl) were used to calculate the relative permeability ratio (P X/P Cl) for each anion. The relative anion permeability (P X/P Cl) of expressed sClC-3 currents activated by hypotonic cell swelling was SCN-(1.50) > I-(1.34) > NO3 -(1.27) > Br-(1.15) > Cl-(1.00) > F-(0.57) > isethionate(0.25) > gluconate(0.09). These results demonstrate that sClC-3 channels exhibit a lyotropic anion permeability similar to native VSOACs in PASMCs and most mammalian cells.1
4 Do Native VSOACs in PASMCs and Heterologously Expressed sClC-3 Behave as Chloride/Proton Antiporters?
The molecular structure of the ClC family of voltage-gated proteins has been determined by X-ray crystallography of the bacterial homologue EcClC.22, 23 EcClC is a homodimer with each subunit consisting of 18 α-helical transmembrane-spanning domains and a cytoplasmic domain containing two cystathionine β-synthetase (CBS) subdomains. A selectivity filter has been identified that contains three selective anion-binding sites.24 Surprisingly, a study25 demonstrated that the bacterial homologue EcClC functions as an H+-Cl--exchange transporter, not as an ion channel. This was convincingly demonstrated since membrane currents associated with EcClC are relatively voltage independent and changes in proton gradients produced easily measurable shifts in current reversal potential, as predicted for an exchange transport mechanism. Efforts have been made to extend these results to the mammalian family of ClC Cl- channels. Conservation of a putative “proton” glutamate (Glu-203) in the selectivity region between EcClC and the mammalian homologues ClC-3-ClC-7 has suggested the possibility that these proteins may also function as proton exchange transporters.26 The major evidence for this proposal is indirect and comes from studies heterologously expressing ClC-4 and ClC-5. The difficulty is that expressed ClC-4 and ClC-5 currents exhibit strong outward rectification, making it impossible to measure reversal potentials or shifts in reversal potentials with changes in extracellular anion or proton concentrations. As an alternative approach, changes in intracellular pH were measured in ClC-4- and ClC-5-transfected tsA201 cells27 or changes in extracellular pH in ClC-4- and ClC-5-transfected oocytes28 to monitor proton fluxes attributable to electrogenic Cl-/H+ exchange.
We have examined whether native VSOACs in cultured canine PASMCs behave as Cl- channels or as Cl-/H+ antiporters. As shown in Fig. 15.4a, VSOAC currents activated by hypotonic cell swelling in canine PASMCs were strongly inhibited at both positive and negative membrane potentials when the extracellular hypotonic solution pH was changed from 7.3 to 4.5. Raw traces of VSOAC currents recorded over the voltage range -100 to +100 mV are illustrated in Fig. 15.4b, c. Figure 15.4d shows the current-voltage relationships of VSOACs recorded in the presence of hypotonic (pH 7.3) solutions and hypotonic (pH 4.5) solutions for a number of cells. Both inward and outward VSOAC currents were inhibited by extracellular acidification; significantly, there was no observed change in membrane current reversal potential.
Inhibition of VSOACs by extracellular acidification in cultured canine PASMCs. (a) Time course of membrane currents activated at ±80 mV by hypotonic (230 mOsm, pH 7.4) solution. Following maximal activation, the extracellular solution was changed to a hypotonic (230 mOsm, pH 4.5) solution at the time indicated by the horizontal bars. External acidification inhibited both outward and inward VSOAC currents, and the remaining currents were reversed by reexposure to isotonic solution. Traces of membrane currents elicited by voltage steps over the range -100 to +125 mV in hypotonic (230 mOsm, pH 7.4) solution (b) and after changing to a hypotonic (230 mOsm, pH 4.5) solution (c). (d) Current-voltage (IV) relationships of membrane currents shown in (b, c). Extracellular acidification inhibited VSOACs without inducing any significant change in current reversal potential (G.-X. Wang and J.R. Hume unpublished data)
If the transport mechanism involves Cl-/H+ exchange, the membrane current reversal potential V r is defined by the following equation25:
where E Cl is the equilibrium potential for Cl-, E H is the equilibrium potential for protons, and r is the proton-anion coupling ratio. For a Cl-/H+ exchange transport protein, significant changes in the proton gradient should produce measurable changes in the membrane current reversal potential, which we failed to observe (Fig. 15.4d) for native VSOACs in PASMCs. This is quite different from the findings on the bacterial homologue EcClC, for which extracellular acidification produced a negative shift in measured reversal potentials.25
We have also examined whether hsClC-3 currents measured in transfected NIH/3T3 cells behave as Cl- channels or as Cl-/H+ antiporters. As shown in Fig. 15.5a, b, hypotonically activated hsClC-3 currents were significantly inhibited by extracellular acidification. Extracellular acidification produced no measurable change in hsClC-3 current reversal potential (Fig. 15.5c), suggesting that hsClC-3 exhibits properties more consistent with a Cl- channel electrodiffusion mechanism compared to a Cl-/H+ countertransport mechanism.
Effect of extracellular acidification on hsClC-3 currents in transfected NIH/3T3 cells. Traces of membrane currents elicited by voltage steps over the range ±100 mV in hypotonic (230 mOsm, pH 7.4) solution (a) and after changing to a hypotonic (230 mOsm, pH 4.5) solution (b). (c) Current-voltage (IV) relationships of membrane currents shown in (a, b). hsClC-3 currents were inhibited by extracellular acidification, but acidification had no effect on membrane current reversal potential (G.-X. Wang and J.R. Hume unpublished data)
5 Summary and Conclusions
Native VSOACs in cardiac and SMCs share many properties with recombinant sClC-3 channels expressed in heterologous expression systems, including outwardly rectifying Cl- currents activated by cell swelling and inhibited by cell shrinkage; current inhibition at strong positive membrane potentials; and inhibition by extracellular nucleotides, stilbene derivatives such as DIDS and 4-Acetamido-4'-isothiocyanato-2,2'-stilbenedisulfonic acid (SITS), intracellular dialysis by anti-ClC-3 antibodies and by the antiestrogen compound tamoxifen.29 Moreover, as shown in this chapter, native VSOACs in PASMCs and expressed recombinant cClC-3 channels exhibit a similar lyotrophic permeability selectivity of SCN->I->NO3 ->Br->Cl->F-> isethionate > gluconate. Despite suggestions that some members of the mammalian ClC Cl- channel family may function as chloride/proton antiporters like the bacterial homologue EcClC, membrane current reversal potential measurements on native VSOACs in PASMCs and recombinant sClC-3 currents failed to provide any evidence supporting a role for chloride/proton antiporter function.
Native VSOACs and ClC-3 have been implicated in a wide variety of SMC functions, including proliferation, growth, apoptosis, and protection against oxidative stress. It is possible that all of these might be explained by the role that VSOACs and ClC-3 normally play in normal cell volume homeostasis. However, it is possible that an important physiological function of these channels may extend beyond their normal role in cell volume regulation.30 For example, it has been demonstrated31 that ClC-3 Cl- channels in the endothelial cell plasma membrane may be a prominent route for transmembrane flux of ROS. Future studies will certainly focus on such a possibility in PASMCs.
References
Nilius B, Droogmans G (2003) Amazing chloride channels: an overview. Acta Physiol Scand 177:119-147
Voets T, Wei L, De Smet P et al (1997) Downregulation of volume-activated Cl- currents during muscle differentiation. Am J Physiol 272:C667-C674
Nelson M, Conway MA, Knot HJ, Brayden JE (1997) Chloride channel blockers inhibit myogenic tone in rat cerebral arteries. J Physiol 502(2):259-264
Duan D, Winter C, Cowley S, Hume JR, Horowitz B (1997) Molecular identification of a volume-regulated chloride channel. Nature 390:417-421
Yamazaki J, Duan D, Janiak R, Kuenzli K, Horowitz B, Hume JR (1998) Functional and molecular expression of volume-regulated chloride channels in canine vascular smooth muscle cells. J Physiol 507:729-736
Do CW, Lu W, Mitchell CH, Civan MM (2005) Inhibition of swelling-activated Cl- currents by functional anti-ClC-3 antibody in native bovine non-pigmented ciliary epithelial cells. Invest Ophthalmol Vis Sci 46:948-955
Jin NG, Kim JK, Yang DK et al (2003) Fundamental role of ClC-3 in volume-sensitive Cl- channel function and cell volume regulation in AGS cells. Am J Physiol Gastrointest Liver Physiol 285:G938-G948
Petrunkina AM, Harrison RA, Ekhlasi-Hundrieser M, Topfer-Petersen E (2004) Role of volume-stimulated osmolyte and anion channels in volume regulation by mammalian sperm. Mol Hum Reprod 10:815-823
Vessey JP, Shi C, Jollimore CA et al (2004) Hyposmotic activation of I Cl, swell in rabbit nonpigmented ciliary epithelial cells involves increased ClC-3 trafficking to the plasma membrane. Biochem Cell Biol 82:708-718
Wang L, Chen L, Jacob TJ (2000) The role of ClC-3 in volume-activated chloride currents and volume regulation in bovine epithelial cells demonstrated by antisense inhibition. J Physiol 524:63-75
Zhou JG, Ren JL, Qiu QY, He H, Guan YY (2005) Regulation of intracellular Cl- concentration through volume-regulated ClC-3 chloride channels in A10 vascular smooth muscle cells. J Biol Chem 280:7301-7308
Jentsch TJ, Stein V, Weinreich F, Zdebik AA (2002) Molecular structure and physiological function of chloride channels. Physiol Rev 82:503-568
Li X, Shimada K, Showalter LA, Weinman SA (2000) Biophysical properties of ClC-3 differentiate it from swelling-activated chloride channels in Chinese hamster ovary-K1 cells. J Biol Chem 275:35994-35998
Weylandt KH, Valverde MA, Nobles M et al (2001) Human ClC-3 is not the swelling-activated chloride channel involved in cell volume regulation. J Biol Chem 276:17461-17467
Stobrawa SM, Breiderhoff T, Takamori S et al (2001) Disruption of ClC-3, a chloride channel expressed on synaptic vesicles, leads to a loss of the hippocampus. Neuron 29:185-196
Yamamoto-Mizuma S, Wang GX, Liu LL et al (2004) Altered properties of volume-sensitive osmolyte and anion channels (VSOACs) and membrane protein expression in cardiac and smooth muscle myocytes from ClCn3-/- mice. J Physiol 557:439-456
Xiong D, Wang G-X, Burkin D et al (2008) Cardiac specific overexpression of the human short ClC-3 chloride channel isoform in mice. Clin Exp Pharmacol Physiol 36:386-393, 2009
Lamb FS, Clayton GH, Liu BX, Smith RL, Barna TJ, Schutte BC (1999) Expression of CLCN voltage-gated chloride channel genes in human blood vessels. J Mol Cell Cardiol 31:657-666
Wang GL, Wang XR, Lin MJ, He H, Lan XJ, Guan YY (2002) Deficiency in ClC-3 chloride channels prevents rat aortic smooth muscle cell proliferation. Circ Res 91:e28-e32
Dai Y-P, Bongalon S, Hatton WJ, Hume JR, Yamboliev IA (2005) ClC-3 chloride channel is upregulated by hypertrophy and inflammation in rat and canine pulmonary artery. Br J Pharmacol 145:5-14
Guan YY, Wang GL, Zhou JG (2006) The ClC-3 Cl- channel in cell volume regulation, proliferation and apoptosis in vascular smooth muscle cells. Trends Pharmacol Sci 27:290-296
Arianzi EA, Gpuld MN (1996) Identifying differential gene expression in monoterpene-treated mammary carcinomas using subtractive display. J Biol Chem 271:29286-29294
Dutzler R, Campbell EB, MacKinnon R (2002) X-ray structure of a ClC chloride channel at 3.0 Å reveals the molecular basis of anion selectivity. Nature 415:287-294
Dutzler R (2006) The ClC family of chloride channels and transporters. Curr Opin Struct Biol 16:1-8
Accardi A, Miller C (2004) Secondary active transport mediated by a prokaryotic homologue of ClC Cl-channels. Nature 427:803-807
Zdebik AA, Zifarelli G, Bersforf E-Y et al (2008) Determinants of anion-proton coupling in mammalian endosomal CLC proteins. J Biol Chem 283:4219-4227
Scheel O, Zdebik AA, Lourdel S, Jentsch TJ (2005) Voltage-dependent electrogenic chloride/proton exchange by endosomal CLC proteins. Nature 436:424-427
Picollo A, Pusch M (2005) Chloride/proton antiporter activity of mammalian CLC proteins ClC-4 and ClC-5. Nature 436:420-423
Hume JR, Duan D, Collier ML, Yamazaki J, Horowitz B (2000) Anion transport in heart. Physiol Rev 80:31-81
Remillard CV, Yuan X-J (2005) ClC-3: more than just a volume-sensitive Cl- channel. Br J Pharmacol 145:1-2
Hawkins BJ, Madesh M, Kirkpatrick CJ, Fisher AB (2007) Superoxide flux in endothelial cells via the chloride channel-3 mediated intracellular signaling. Mol Biol Cell 18:2002-2012
Wang G-X, Hatton WJ, Wang GL et al (2003) Functional effects of novel anti-ClC-3 antibodies on native volume-sensitive osmolyte and anion channels (VSOACs) in cardiac and smooth muscle cells. Am J Physiol 285:H1453-H1463
Acknowledgments
Our work was supported by National Institutes of Health grants HL-49254 and P20RR1581 from the National Center for Research Resources.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2010 Humana Press, a part of Springer Science+Business Media, LLC
About this paper
Cite this paper
Hume, J.R., Wang, GX., Yamazaki, J., Ng, L.C., Duan, D. (2010). CLC-3 Chloride Channels in the Pulmonary Vasculature. In: Yuan, JJ., Ward, J. (eds) Membrane Receptors, Channels and Transporters in Pulmonary Circulation. Advances in Experimental Medicine and Biology, vol 661. Humana Press, Totowa, NJ. https://doi.org/10.1007/978-1-60761-500-2_15
Download citation
DOI: https://doi.org/10.1007/978-1-60761-500-2_15
Published:
Publisher Name: Humana Press, Totowa, NJ
Print ISBN: 978-1-60761-499-9
Online ISBN: 978-1-60761-500-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)