Abstract
Certain endocrine and metabolic disorders cause mild to moderate weight gain and fat deposition. Excess fat storage in turn can have profound effects on intermediary metabolism and endocrine function. We begin this section with a brief discussion of endocrine disorders that promote excess weight gain. We then review the effects of obesity on linear growth and bone maturation, thyroid function, sexual development, adrenal function, and calcium homeostasis and bone mineralization. Subsequent chapters in this volume discuss the implications of obesity for insulin production and action and the regulation of glucose tolerance, blood pressure, lipid metabolism and atherogenesis, sleep hygiene, and hepatic function.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Key Words
- Growth hormone
- insulin-like growth factor (IGF)
- thyroid hormone
- cortisol
- prolactin
- pseudohypoparathyroidism
- adrenarche
- puberty
- gynecomastia
- vitamin D
- bone
Certain endocrine and metabolic disorders cause mild to moderate weight gain and fat deposition. Excess fat storage in turn can have profound effects on intermediary metabolism and endocrine function. We begin this section with a brief discussion of endocrine disorders that promote excess weight gain. We then review the effects of obesity on linear growth and bone maturation, thyroid function, sexual development, adrenal function, and calcium homeostasis and bone mineralization. Subsequent chapters in this volume discuss the implications of obesity for insulin production and action and the regulation of glucose tolerance, blood pressure, lipid metabolism and atherogenesis, sleep hygiene, and hepatic function.
Metabolic and Hormonal Disorders Causing Excess Fat Deposition
Hormonal disorders commonly associated with weight gain and increases in the ratio of fat to lean body mass include growth hormone (GH) deficiency, hypothyroidism, glucocorticoid excess, and the polycystic ovarian syndrome (PCOS, Table 1). Fat deposition in GH deficiency results from heightened insulin sensitivity, impaired lipolysis, sarcopenia, and induction of 11β-hydroxysteroid dehydrogenase 1 (11β-HSD1) in visceral or abdominal fat, which favors local overproduction of cortisol ( 1 ). Hypothyroidism promotes weight gain by reducing resting energy expenditure, while glucocorticoid excess causes hyperphagia, adipogenesis, and muscle wasting. Ovarian hyperandrogenism/PCOS is associated with insulin resistance and hyperinsulinemia; given the ability of insulin to stimulate ovarian androgen production (see below), it may be a consequence as well as a cause of obesity.
Hypothalamic damage or disease can cause insatiable appetite and progressive weight gain. Reductions in basal metabolic rate and physical activity contribute to hypothalamic obesity (see Chapter 2 by Lustig). Deficiencies of GH, thyroid hormone, and glucocorticoids are common in this setting and some patients have precocious puberty, which can promote fat deposition, particularly in girls. The insatiable appetite and obesity probably result from central leptin resistance and heightened vagal tone with hyperinsulinemia. The use of high-dose glucocorticoids around the time of surgery facilitates weight gain; hyperprolactinemia, which has been associated with weight gain in adults and children ( 2 , 3 ), may also contribute.
GH deficiency, hypothyroidism, glucocorticoid excess, and pseudohypoparathyroidism (which can be accompanied by hypothyroidism as well as GH deficiency) are associated with short stature and/or decreased height velocity. In contrast, stature and height velocity are normal or increased in “exogenous” obesity (see below). Laboratory testing in an obese child is unlikely to reveal an underlying hormonal disorder (other than insulin resistance and glucose intolerance) if the height, growth velocity, pubertal development, and menstrual function are appropriate for age and family history. It should be noted, however, that linear growth and bone maturation may not be reduced in children with adrenal tumors that produce androgens as well as cortisol. Moreover, linear growth may appear normal or even increased in GH-deficient or hypothyroid patients who also have precocious puberty.
Effects of Obesity on Linear Growth and Bone Maturation
Final adult height in otherwise normal obese children generally falls within two standard deviations of target height. However, rates of linear growth and bone maturation are often increased in obese pre- and peri-pubertal children despite marked reductions in basal and stimulated plasma growth hormone (GH) concentrations and a reduction in circulating GH half-life ( 4 ). The reduction in GH secretion in obese children and adults has been ascribed to negative feedback by free fatty acids, a reduction in plasma ghrelin (a GH secretagogue produced by the stomach), and nutrient-stimulated increases in IGF-1 production. Total IGF-1 and IGF binding protein (BP)-3 concentrations in obese subjects are typically normal or only mildly elevated; this may reflect in part the production of IGF-1 and IGF BP-3 by white adipose tissue ( 5 , 6 ) and/or an increase in hepatic GH sensitivity, resulting from induction of hepatic GH receptors by hyperinsulinemia (Fig. 1). Induction of GH receptor expression in obesity is suggested by an increase in levels of GH binding protein ( 7 ), the circulating form of the extracellular GH receptor domain, and by heightened production of IGF-1 following a single dose of GH ( 8 ).
Mechanisms that may explain the normal or increased rates of growth and bone maturation in pre- and peri-pubertal obese children. IGF, insulin-like growth factor; BP, binding protein. An increase in adrenal androgen production in obese children with precocious adrenarche may also accelerate bone maturation.
Total IGF-2 concentrations were elevated in obese adults in two studies but were normal in a study of obese adolescents ( 9 ). Many investigations find reductions in serum IGF binding proteins 1 and 2 (IGFBP-1 and BP-2), which correlate inversely with plasma insulin concentrations and liver fat content ( 10 , 11 ). The reductions in IGFBPs 1 and 2 are postulated to increase the bioavailability of IGF-1, which may thereby maintain or increase linear growth in obesity despite diminished GH secretion. “Free” IGF-1 levels have been found to be elevated in some, but not all, studies of obese adults ( 12 , 13 ); however, a recent investigation found that the bioactivity of IGF-1, as assessed by a kinase receptor activation assay, was normal in obese women. The ratio of bioactive IGF-1 to total IGF-1, however, was increased ( 14 ).
Reductions in plasma IGF BP-1 or 2 concentrations in insulin-resistant obese subjects may facilitate weight gain because overexpression of IGFBP-1 or 2 in transgenic mice reduces adipogenesis and prevents diet-induced obesity. Interestingly BP-1 excess reduces insulin sensitivity but BP-2 excess improves glucose tolerance ( 15 , 16 )
The effects of IGF-1 on growth and bone maturation may be potentiated by insulin-induced increases in adrenal androgen production (Fig. 1 and below); bone age may be advanced as much as 1 year in children with precocious adrenarche, which is more common in obese children. The hyperleptinemia of obesity also appears to play a role (Fig. 1). Circulating leptin levels rise in proportion to body (particularly subcutaneous) fat stores and are higher in girls than in boys. Leptin stimulates proliferation of isolated mouse and rat osteoblasts and increases the width of the chondroprogenitor zone of the mouse mandible in vivo. Conversely, leptin deficiency in ob/ob mice reduces cortical bone mass but increases trabecular mass ( 17 ); leptin treatment increases femoral length, bone area, and bone mineral content ( 18 ) and may promote the differentiation of osteoblasts from bone marrow stem cells ( 17 ). The effects of leptin may be exerted in concert with IGF-1 because leptin increases IGF-1 receptor expression in mouse chondrocytes ( 19 ). Nevertheless, linear growth is normal in patients with congenital deficiencies of leptin or the leptin receptor ( 20 , 21 ).
Thyroid Function
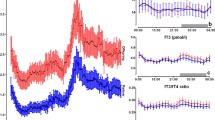
Plasma T4 and TSH levels generally fall within the normal range in obese subjects but tri-iodothyronine concentrations are mildly elevated, a consequence of nutrient-dependent T4 to T3 conversion [( 4 ), Fig. 2]. The elevation of T3 increases resting energy expenditure and may thereby limit further weight gain. Caloric restriction and weight loss, on the other hand, decrease total and free T4 and T3 levels, reducing energy expenditure and thereby facilitating weight regain.
The effects of caloric excess and deprivation on thyroid hormone levels are mediated in part by leptin-dependent effects on hypothalamic TRH production (Fig. 2; see also Chapter 28 by Lechan and Fekete). Thyroid hormone levels are variably low in leptin receptor-deficient humans and are reduced in leptin receptor-deficient db/db mice. Leptin treatment reverses the loss of TSH pulsatility that accompanies short-term fasting and normalizes thyroid hormone levels following longer-term caloric restriction. These actions are mediated by direct effects of leptin/STAT-3 signaling on TRH transcription and indirect effects on TRH production mediated by increases in ∝MSH and reductions in agouti-related peptide (AgRP) and neuropeptide Y ( 22 , 23 ).
Gonadal Function and Pubertal Development
A recent study found that obesity in early childhood (age 36–54 months) and excessive weight gain between 3 and 9 years of age increase the risks of precocious thelarche and may reduce the age of menarche ( 24 ). Since leptin promotes gonadotropin secretion and rises transiently before the onset of puberty in normal weight children, it is possible that the hyperleptinemia of obesity promotes early sexual maturation, at least in girls.
More commonly, obese girls and boys develop precocious adrenarche without true puberty, and teenage obese girls are prone to ovarian hyperandrogenism with mild hirsutism, acne, anovulation, and menstrual irregularity. The pathogenesis of precocious adrenarche and ovarian hyperandrogenism remains poorly understood. However, insulin and IGF-1 in excess act in synergy with adrenocorticotrophic hormone (ACTH) and luteinizing hormone (LH) to stimulate the production of androgens from adrenocortical cells and ovarian theca cells, respectively. These effects are mediated through induction of P450c17α hydroxylase activity. The biologic availability of ovarian and adrenal androgens is increased because insulin suppresses hepatic sex hormone binding globulin (SHBG) expression and reduces plasma SHBG concentrations. Free androgens increase the frequency of gonadotropin-releasing hormone (GnRH) pulses and the ratio of LH to follicle-stimulating hormone (FSH), thereby exacerbating thecal androgen production. The increase in free androgens may induce precocious adrenarche in pre-pubertal girls and boys and may cause anovulation and hirsutism in adolescent girls and young women [( 25 , 26 ), Fig. 3; see also Chapter 24 by Franks and Joharatnam].
Free and total testosterone levels are generally normal in obese boys but may decline with dramatic weight gain in association with a fall in gonadotropin levels. These changes can reverse with weight loss. Aromatization of androstenedione in adipose tissue increases plasma estrone concentrations, causing gynecomastia in adolescent boys.
In rare cases the gynecomastia and ovarian hyperandrogenism in obese children are caused by hyperprolactinemia. Prolactin levels are typically normal or low in obese children or adults. However, hyperprolactinemia deriving from a pituitary tumor may be associated with weight gain in children as well as adults ( 2 , 3 ).
Glucocorticoid Production and Turnover
The abdominal weight gain, striae, hirsutism, and menstrual irregularity that may accompany obesity are often confused with Cushing’s syndrome. In contrast to “exogenous” obesity, Cushing’s syndrome is typically associated with linear growth failure and delayed bone maturation (unless a primary adrenal tumor produces excess androgens as well as glucocorticoids) as well as hemorrhagic/violaceous, rather than pink, striae. Basal plasma, salivary, and urinary free cortisol concentrations and basal ACTH levels in obese, non-Cushingoid children generally fall within the normal range, and diurnal variation and the response to dexamethasone are maintained ( 27 ). However, body fat mass correlates with total excretion of glucocorticoid metabolites, suggesting that obesity is accompanied by increased cortisol secretion and turnover.
Changes in tissue glucocorticoid metabolism may modulate fat distribution and peripheral insulin sensitivity ( 28 ). For example, polymorphisms in the glucocorticoid receptor have been associated with obesity, hypertension, and insulin resistance in some studies in adults. Additional investigations suggest that overexpression of 11 beta hydroxysteroid dehydrogenase type 1 (11βHSD1) in visceral adipose tissue may exacerbate weight gain by increasing local production of cortisol from inactive cortisone. In contrast, other studies find lower expression of 11βHSD1 in preadipocytes of obese, non-diabetic adults ( 29 ); the expected reduction in tissue cortisol concentrations is postulated to counteract the insulin resistance and weight gain in obese patients. An increase in 11βHSD1 expression after weight loss may facilitate adipose cortisol production, adipogenesis, and weight rebound.
Calcium Homeostasis, Bone Mineralization, and Fractures
Adolescents and adults with severe obesity, particularly those with dark skin, often have reduced circulating levels of 25-hydroxyvitamin D (25OHD). One study ( 30 ) found that 25OHD levels were less than 20 ng/ml in 78.4% of markedly obese (BMI 43.3) African-American teenage girls (mean age 14 years). The prevalence of vitamin D deficiency is lower in obese whites than in black or Hispanic children ( 31 ): in a total of 127 obese adolescents (mean age 13 years, BMI 36.4), vitamin D deficiency was noted in 43.6% of Hispanics and 48.7% of African-Americans but only 10.2% of Caucasians; levels of 25OHD correlated inversely with serum parathyroid hormone (PTH). A more recent investigation ( 32 ) showed that 17 of 58 obese adolescents (mean 14.9 years, BMI 36, 66% female, 14% black) had 25OHD levels below 20 ng/ml; however, none had elevated (>65 ng/ml) PTH levels, and bone mineral content and density fell within the normal range.
The reductions in 25OH vitamin D levels in obese children may be explained by decreased intake of vitamin D-containing dairy products, decreased cutaneous synthesis of vitamin D3 (in persons of color), and/or reduced bioavailability of vitamin D3 owing to deposition in adipose tissue ( 33 ). 25OHD levels in adults are inversely proportional to visceral and subcutaneous fat stores and measures of insulin sensitivity ( 34 ). Recent evidence suggests that 1,25 diOH vitamin D inhibits expression of peroxisome-proliferator-activated receptor gamma (PPARγ) and c/EBPα, providing a mechanism by which vitamin D deficiency may promote adipogenesis ( 35 ). However, no studies thus far have demonstrated that Vitamin D treatment can prevent or reverse weight gain in obese subjects.
Some studies show variable decreases in bone mineral content in obese subjects; others find that overweight and obese children have normal or increased bone mass compared with lean children. Yet the incidence of extremity fractures appears to be higher in obese than in lean children ( 36 , 37 ); experiments in mice suggests that high-fat feeding increases bone density but reduces bone strength, bending stiffness, and fracture resistance ( 38 ). Overall bone quality appears to reflect a number of genetic and environmental factors including milk intake and sun exposure, consumption of carbonated beverages, and physical activity, which promotes bone accrual and strength ( 39 ).
References
Agha A, Monson JP. Modulation of glucocorticoid metabolism by the growth hormone: IGF-1 axis. Clin Endocrinol (Oxford). 2007;66:459–65.
Colao A, Sarno AD, Cappabianca P, Briganti F, Pivonello R, Somma CD, Faggiano A, Biondi B, Lombardi G. Gender differences in the prevalence, clinical features and response to cabergoline in hyperprolactinemia. Eur J Endocrinol. 2003;148(3):325–31.
Gillam MP, Molitch ME, Lombardi G, Colao A. Advances in the treatment of prolactinomas. Endocr Rev. 2006;27:485–534.
Douyon L, Schteingart DE. Effect of obesity and starvation on thyroid hormone, growth hormone and cortisol secretion. Endocrinol Metab Clin North Am. 2002;31:173–89.
Wabitsch M, Heinze E, Debatin KM, Blum WF. IGF-I- and IGFBP-3-expression in cultured human preadipocytes and adipocytes. Horm Met Res. 2000;32:555–9.
Peter MA, Winterhalter KH, Boni-Schnetzler M, Froesch ER, Zapf J. Regulation of insulin-like growth factor-I (IGF-I) and IGF-binding proteins by growth hormone in rat white adipose tissue. Endocrinology. 1993;133:2624–31.
Kratzsch J, Dehmel B, Pulzer F, et al. Increased serum GHBP levels in obese pubertal children and adolescents: relationship to body composition, leptin and indicators of metabolic disturbances. Int J Obes. 1997;21:1130–6.
Gleeson HK, Lissett CA, Shalet SM. Insulin-like growth factor-I response to a single bolus of growth hormone is increased in obesity. J Clin Endocrinol Metab. 2005;90:1061–7.
Wabitsch M, Blum WF, Muche R, Heinze E, Haug C, Mayer H, Teller W. Insulin-like growth factors and their binding proteins before and after weight loss and their associations with hormonal and metabolic parameters in obese adolescent girls. Int J Obes Relat Metab Disord. 1996;20(12):1073–80.
Wheatcroft SB, Kearney MT. IGF-dependent and IGF-independent actions of IGF-binding protein-1 and -2: implications for metabolic homeostasis. Trends Endocrinol Metab. 2009;20:153–62.
Kotronen A, Lewitt M, Hall K, Brismar K, Yki-Jarvinen H. Insulin-like growth factor binding protein 1 as a novel specific marker of hepatic insulin sensitivity. J Clin Endocrinol Metab. 2008;93:4867–72.
Frystyk J, Skjaerbaek C, Vestbo E, Fisker S, Orskov H. Circulating levels of free insulin-like growth factors in obese subjects: the impact of type 2 diabetes. Diabetes Metab Res Rev. 1999;15:314–22.
Rasmussen MH, Juul A, Kjems LL, Hilsted J. Effects of short-term caloric restriction on circulating free IGF-I, acid-labile subunit, IGF-binding proteins (IGFBPs)-1-4, and IGFBPs-1-3 protease activity in obese subjects. Eur J Endocrinol. 2006;155(4):575–81.
Frystyk J, Brick DJ, Gerweck AV, Utz AL, Miller KK. Bioactive insulin-like growth factor-1 in obesity. J Clin Endocrinol Metab. 2009;94:3093–7.
Rajkumar K, Modric T, Murphy LJ. Impaired adipogenesis in insulin-like growth factor binding protein-1 transgenic mice. J Endocrinol. 1999;162(3):457–65.
Wheatcroft SB, Kearney MT, Shah AM, Ezzat VA, Miell JR, Modo M, Williams SC, Cawthorn WP, Medina-Gomez G, Vidal-Puig A, Sethi JK, Crossey PA. IGF-binding protein-2 protects against the development of obesity and insulin resistance. Diabetes. 2007;56(2):285–94.
Cirmanova V, Bayer M, Starka L, Zajickova K. The effect of leptin on bone: an evolving concept of action. Physiol Res. 2008;57(Suppl 1):S143–51.
Steppan CM, Crawford DT, Chidsey-Frink KL, Ke H, Swick AG. Leptin is a potent stimulator of bone growth in ob/ob mice. Regul Pept. 2000;92:73–8.
Maor G, Rochwerger M, Segev Y, Phillip M. Leptin acts as a growth factor on the chondrocytes of skeletal growth centers. J Bone Miner Res. 2002;17:1034–43.
Montague CT, Farooqi IS, Whitehead JP, Soos MA, Rau H, Wareham NJ, Sewter CP, Digby JE, Mohammed SN, Hurst JA, Cheetham CH, Earley AR, Barnett AH, Prins JB, O’Rahilly S. Congenital leptin deficiency is associated with severe early-onset obesity in humans. Nature. 1997;387(6636):903–8.
Farooqi IS, Wangensteen T, Collins S, Kimber W, Matarese G, Keogh JM, Lank E, Bottomley B, Lopez-Fernandez J, Ferraz-Amaro I, Dattani MT, Ercan O, Myhre AG, Retterstol L, Stanhope R, Edge JA, McKenzie S, Lessan N, Ghodsi M, De Rosa V, Perna F, Fontana S, Barroso I, Undlien DE, O’Rahilly S. Clinical and molecular genetic spectrum of congenital deficiency of the leptin receptor. N Engl J Med. 2007;356(3):237–47.
Feldt-Rasmussen U. Thyroid and leptin. Thyroid. 2007;17:413–9.
Hollenberg AN. The role of the thyrotropin-releasing hormone (TRH) neuron as a metabolic sensor. Thyroid. 2008;18:131–8.
Lee JM, Appugliese D, Kaciroti N, Corwyn RF, Bradley RH, Lumeng JC. Weight status in young girls and the onset of puberty. Pediatrics. 2007;119:e624–30.
Sam S, Dunaif A. Polycystic ovary syndrome: syndrome XX? Trends Endocrinol Metab. 2003;14:365–70.
Chang RJ. The reproductive phenotype in polycystic ovary syndrome. Nat Clin Pract Endocrinol Metab. 2007;3(10):688–95.
Artz E, Haqq A, Freemark M. Hormonal and metabolic consequences of childhood obesity. Endocrinol Metab Clin North Am. 2005;34(3):643–58.
Wake DJ, Rask E, Livingstone DEW, Soderberg S, Olsson T, Walker BR. Local and systemic impact of transcriptional up-regulation of 11β-hydroxysteroid dehydrogenase type 1 in adipose tissue in human obesity. J Clin Endocrinol Metab. 2003;88:3983–8.
Tomlinson JW, Moore JS, Clark PM, Holder G, Shakespeare L, Stewart PM. Weight loss increases 11β-hydroxysteroid dehydrogenase type 1 expression in human adipose tissue. J Clin Endocrinol Metab. 2004;89:2711–6.
Ashraf A, Alvarez J, Saenz K, Gower B, McCormick K, Franklin F. Threshold for effects of vitamin D deficiency on glucose metabolism in obese female African-American adolescents. J Clin Endocrinol Metab. 2009;94:3200–6.
Alemzadeh R, Kichler J, Babar G, Calhoun M. Hypovitaminosis D in obese children and adolescents: relationship with adiposity, insulin sensitivity, ethnicity, and season. Metabolism. 2008;57:183–91.
Lenders CM, Feldman HA, Von Scheven E, et al. Relation of body fat indexes to vitamin D status and deficiency among obese adolescents. Am J Clin Nutr. 2009;90:459–67.
Wortsman J, Matsuoka LY, Chen TC, Lu Z, Holick MF. Decreased bioavailability of vitamin D in obesity. Am J Clin Nutr. 2000;72(3):690–3.
Cheng S, Massaro JM, Fox CS, Larson MG, Keyes MJ, McCabe EL, Robins SJ, O’Donnell CJ, Hoffmann U, Jacques PF, Booth SL, Vasan RS, Wolf M, Wang TJ. Adiposity, cardiometabolic risk, and vitamin D status: the Framingham Heart Study. Diabetes. 2010; 59(1):242–8.
Wood RJ. Vitamin D and adipogenesis: new molecular insights. Nutr Rev. 2008;66:40–6.
Taylor ED, Theim KR, Mirch MC, Ghorbani S, Tanofsky-Kraff M, Adler-Wailes DC, Brady S, Reynolds JC, Calis KA, Yanovski JA. Orthopedic complications of overweight in children and adolescents. Pediatrics. 2006;117(6):2167–74.
Rana AR, Michalsky MP, Teich S, Groner JI, Caniano DA, Schuster DP. Childhood obesity: a risk factor for injuries observed at a level-1 trauma center. J Pediatr Surg. 2009;44:1601–5.
Ionova-Martin SS, Do SH, Barth HD, et al. Reduced size-independent mechanical properties of cortical bone in high fat diet-induced obesity. Bone. 2010;46(1):217–25.
Manias K, McCabe D, Bishop N. Fractures and recurrent fractures in children: varying effects of environmental factors as well as bone size and mass. Bone. 2006;39:652–7.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2010 Springer Science+Business Media, LLC
About this chapter
Cite this chapter
Freemark, M. (2010). Childhood Obesity and the Regulation of Growth, Thyroid Function, Sexual Development, and Calcium Homeostasis. In: Freemark, M. (eds) Pediatric Obesity. Contemporary Endocrinology. Humana Press, New York, NY. https://doi.org/10.1007/978-1-60327-874-4_12
Download citation
DOI: https://doi.org/10.1007/978-1-60327-874-4_12
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-60327-873-7
Online ISBN: 978-1-60327-874-4
eBook Packages: MedicineMedicine (R0)