Abstract
Background
Single-event multilevel surgery (SEMLS) approach is regarded as the golden standard in developed countries to improve gait and functional mobility in children with cerebral palsy (CP). However, this approach is not always feasible in developing countries. Therefore, orthopedic surgery based on an interval surgery approach (ISA) is still commonly used in developing countries, although little is known about the long term outcomes of an ISA. Therefore, the aim of this study was to describe the gait patterns of adults with CP, who have been treated with ISA, which started more than 15 years ago.
Materials and Methods
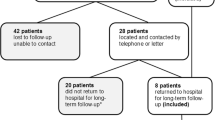
Thirty adults with CP and spastic diplegia, who received ISA treatment 21.6–33.7 years ago, were recruited for this study and participated in three-dimensional gait analysis. Twenty kinematic and nondimensional temporal-distance parameters were captured, while the overall gait deviation index (GDI) was also calculated. Data of the adults with CP were compared to normative data of typically developing (TD) adults.
Results
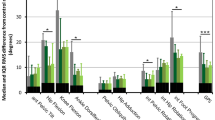
Although all adults with CP were still ambulant, their gait parameters significantly differed from TD adults, with a lower GDI in the adults with CP. The CP gait patterns were characterized by excessive hip flexion and hip internal rotation as well as a stiff-knee gait.
Conclusion
Although different to TD adults, the gait patterns observed in the adult with CP treated with ISA is in line with other studies. Gait patterns suggest that derotation osteotomies potentially could have improved the long term gait patterns. Although SEMLS might be the preferred treatment method, potentially resulting in better outcomes, ISA can also be used to treat children with CP in developing countries as India and South Africa, where a SEMLS approach is not always feasible.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Rosenbaum P, Paneth N, Leviton A, Goldstein M, Bax M, Damiano D, et al. A report: The definition and classification of cerebral palsy April 2006. Dev Med Child Neurol Suppl 2007;109:8–14.
Narayanan UG. Management of children with ambulatory cerebral palsy: An evidence-based review. J Pediatr Orthop 2012;32 Suppl 2:S172–81.
Novak I, McIntyre S, Morgan C, Campbell L, Dark L, Morton N, et al. A systematic review of interventions for children with cerebral palsy: State of the evidence. Dev Med Child Neurol 2013;55:885–910.
Morgan P, McGinley J. Gait function and decline in adults with cerebral palsy: A systematic review. Disabil Rehabil 2014;36:1–9.
McGinley JL, Dobson F, Ganeshalingam R, Shore BJ, Rutz E, Graham HK. Single-event multilevel surgery for children with cerebral palsy: A systematic review. Dev Med Child Neurol 2012;54:117–28.
Lamberts RP, Burger M, du Toit J, Langerak NG. A systematic review of the effects of single-event multilevel surgery on gait parameters in children with spastic cerebral palsy. PLoS One 2016;11:e0164686.
Wilson DJ, Scully WF, Min KS, Harmon TA, Eichinger JK, Arrington ED. Biomechanical analysis of intramedullary vs. superior plate fixation of transverse midshaft clavicle fractures. J Shoulder Elbow Surg 2016;25:949–53.
Wilson NC, Chong J, Mackey AH, Stott NS. Reported outcomes of lower limb orthopaedic surgery in children and adolescents with cerebral palsy: A mapping review. Dev Med Child Neurol 2014;56:808–14.
Hanna SE, Rosenbaum PL, Bartlett DJ, Palisano RJ, Walter SD, Avery L, et al. Stability and decline in gross motor function among children and youth with cerebral palsy aged 2 to 21 years. Dev Med Child Neurol 2009;51:295–302.
Rang M. Cerebral Palsy. In: Morrissy R, editor. Lovell and Winter’s Peadiatric Orthopaedics. Philadelphia: JB Lippincott Co.; 1990. p. 465–506.
Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, Galuppi B. Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol 1997;39:214–23.
Palisano RJ, Rosenbaum P, Bartlett D, Livingston MH. Content validity of the expanded and revised gross motor function classification system. Dev Med Child Neurol 2008;50:744–50.
Micklesfield LK, Levitt NS, Carstens MT, Dhansay MA, Norris SA, Lambert EV. Early life and current determinants of bone in South African children of mixed ancestral origin. Ann Hum Biol 2007;34:647–55.
Langerak NG, Tam N, Vaughan CL, Fieggen AG, Schwartz MH. Gait status 17–26 years after selective dorsal rhizotomy. Gait Posture 2012;35:244–9.
Hof AL. Scaling gait data to body size. Gait Posture 1996;4:222–3.
Schwartz MH, Rozumalski A. The gait deviation index: A new comprehensive index of gait pathology. Gait Posture 2008;28:351–7.
Maanum G, Jahnsen R, Stanghelle JK, Sandvik L, Larsen KL, Keller A. Face and construct validity of the gait deviation index in adults with spastic cerebral palsy. J Rehabil Med 2012;44:272–5.
Palisano RJ, Cameron D, Rosenbaum PL, Walter SD, Russell D. Stability of the gross motor function classification system. Dev Med Child Neurol 2006;48:424–8.
Alriksson-Schmidt A, Nordmark E, Czuba T, Westbom L. Stability of the gross motor function classification system in children and adolescents with cerebral palsy: A retrospective cohort registry study. Dev Med Child Neurol 2017;59:641–6.
Donald KA, Samia P, Kakooza-Mwesige A, Bearden D. Pediatric cerebral palsy in Africa: A systematic review. Semin Pediatr Neurol 2014;21:30–5.
Donald KA, Kakooza AM, Wammanda RD, Mallewa M, Samia P, Babakir H, et al. Pediatric cerebral palsy in Africa: Where are we? J Child Neurol 2015;30:963–71.
Wren TA, Gorton GE 3rd, Ounpuu S, Tucker CA. Efficacy of clinical gait analysis: A systematic review. Gait Posture 2011;34:149–53.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Langerak, N.G., Tam, N., du Toit, J. et al. Gait Pattern of Adults with Cerebral Palsy and Spastic Diplegia More Than 15 Years after Being Treated with an Interval Surgery Approach: Implications for Low-Resource Settings. IJOO 53, 655–661 (2019). https://doi.org/10.4103/ortho.IJOrtho_113_19
Published:
Issue Date:
DOI: https://doi.org/10.4103/ortho.IJOrtho_113_19