Abstract
Diabetes mellitus is a chronic illness that affects the world on an epidemic scale. It requires complex healthcare and considerable economic resources. Diabetes disease management programs use a variety of strategies to improve clinical outcome measures and reduce costs. Studies have demonstrated the effectiveness of these programs on reducing glycosylated hemoglobin levels, improving cardiovascular risks, and reducing utilization of services. However, the most effective components of disease management strategies or combination of strategies remain unknown. This narrative review explores the components, impact, benefits, and barriers of current diabetes disease management models and also presents a novel hybrid model incorporating elements of both on-site and off-site programs.
On-site disease management programs include strategies characterized by unique patient identification and evaluation, implementation of intervention methods, on-site health provider team members, and specific environmental resources. Advantages of this model include the face-to-face encounter between patients and providers, the proximity of the healthcare team members to facilitate ease of communication and build independence and trust between patients and providers, and technology resources, such as the electronic medical record. A number of clinical trials have demonstrated the effectiveness and cost effectiveness of on-site diabetes disease management programs. However, because of the methodological limitations of many studies, further studies are needed to confirm such findings. Barriers to the implementation of on-site programs may include patient population characteristics such as complexity of co-morbid illness and social Stressors, including low health literacy, that require adaptation of the disease management model. In comparison, off-site disease management programs utilize administrative resources to identify patients with chronic illnesses. Other key elements include the evaluation of clinical care practices using established guidelines with auditing and feedback to providers based on their performance, and the use of reminders for both patients and providers to influence better processes of care. This process is often independent of the traditional on-site care delivered directly by providers.
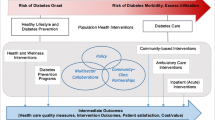
A hybrid disease management model that incorporates both on-site and off-site disease management components could be the ideal model for optimizing care of patients with chronic illness. The suggested hybrid model incorporates many features of previous models of disease management but gives a new construct that can be customized to different clinic settings, provider practices, and patient populations, including patients with other complex chronic illness. This hybrid model could be applied to a variety of individual or multiple chronic illnesses. This model would engage both on-site healthcare providers and support staff along with off-site administrative staff and electronic medical data to provide patients optimal care while potentially reducing overall costs.


Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.References
Wild S, Roglic G, Green A, et al. Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 2004 May; 27(5): 1047–53
Yach D, Hawkes C, Gould CL, et al. The global burden of chronic diseases: overcoming impediments to prevention and control. JAMA 2004 Jun 2; 291(21): 2616–22
Hogan P, Dall T, Nikolov P. Economic costs of diabetes in the US in 2002. Diabetes Care 2003 Mar; 26(3): 917–32
Klonoff DC, Schwartz DM. An economic analysis of interventions for diabetes. Diabetes Care 2000 Mar; 23(3): 390–404
Diabetes Quality Improvement Alliance. Measures and supporting documents [online]. Available from URL: http://www.nationaldiabetesalliance.org/measures.html [Accessed 2006 Nov 1]
The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993 Sep 30; 329(14): 977–86
UK Prospective Diabetes Study Group. Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38. BMJ 1998 Sep 12; 317(7160): 703–13
Goldberg RB, Mellies MJ, Sacks FM, et al. Cardiovascular events and their reduction with pravastatin in diabetic and glucose-intolerant myocardial infarction survivors with average cholesterol levels: subgroup analyses in the cholesterol and recurrent events (CARE) trial. The Care Investigators. Circulation 1998 Dec; 98(23): 2513–9
Saaddine JB, Cadwell B, Gregg EW, et al. Improvements in diabetes processes of care and intermediate outcomes: United States, 1988–2002. Ann Intern Med 2006 Apr; 144(7): 465–74
Asch SM, Kerr EA, Keesey J, et al. Who is at greatest risk for receiving poor-quality health care? N Engl J Med 2006 Mar; 354(11): 1147–56
Bodenheimer T. Disease management: promises and pitfalls. N Engl J Med 1999 Apr; 340(15): 1202–5
Epstein RS, Sherwood LM. From outcomes research to disease management: a guide for the perplexed. Ann Intern Med 1996 May; 124(9): 832–7
Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness: the chronic care model, part 2. JAMA 2002 Oct 16; 288(15): 1909–14
Bodenheimer T, Wagner EH, Grumbach K. Improving primary care for patients with chronic illness. JAMA 2002 Oct 9; 288(14): 1775–9
McCulloch DK, Price MJ, Hindmarsh M, et al. A population-based approach to diabetes management in a primary care setting: early results and lessons learned. Eff Clin Pract 1998 Aug–Sep; 1(1): 12–22
Wagner EH. Chronic disease management: what will it take to improve care for chronic illness? Eff Clin Pract 1998 Aug–Sep; 1(1): 2–4
Wagner EH, Groves T. Care for chronic diseases. BMJ 2002 Oct 26; 325(7370): 913–4
Krumholz HM, Currie PM, Riegel B, et al. A taxonomy for disease management: a scientific statement from the American Heart Association Disease Management Taxonomy Writing Group. Circulation 2006 Sep; 114(13): 1432–45
Burns H. Disease management and the drug industry: carve out or carve up? Lancet 1996 Apr 13; 347(9007): 1021–3
Harris Jr JM. Disease management: new wine in new bottles? Ann Intern Med 1996 May; 124(9): 838–42
Casalino L, Gillies RR, Shortell SM, et al. External incentives, information technology, and organized processes to improve health care quality for patients with chronic diseases. JAMA 2003 Jan 22–29; 289(4): 434–41
Welch WP, Bergsten C, Cutler C, et al. Disease management practices of health plans. Am J Manag Care 2002 Apr; 8(4): 353–61
Kanaya AM, Grady D, Barrett-Connor E. Explaining the sex difference in coronary heart disease mortality among patients with type 2 diabetes mellitus: a meta-analysis. Arch Intern Med 2002 Aug 12–26; 162(15): 1737–45
Rothman RL, Malone R, Bryant B, et al. A randomized trial of a primary care-based disease management program to improve cardiovascular risk factors and glycated hemoglobin levels in patients with diabetes. Am J Med 2005 Mar; 118(3): 276–84
D’Eramo-Melkus GA, Wylie-Rosett J, Hagan JA. Metabolic impact of education in NIDDM. Diabetes Care 1992 Jul; 15(7): 864–9
Gaede P, Vedel P, Larsen N, et al. Multifactorial intervention and cardiovascular disease in patients with type 2 diabetes. N Engl J Med 2003 Jan 30; 348(5): 383–93
Shojania KG, Ranji SR, McDonald KM, et al. Effects of quality improvement strategies for type 2 diabetes on glycemic control: a meta-regression analysis. JAMA 2006 Jul 26; 296(4): 427–40
Knight K, Badamgarav E, Henning JM, et al. A systematic review of diabetes disease management programs. Am J Manag Care 2005 Apr; 11(4): 242–50
Norris SL, Nichols PJ, Caspersen CJ, et al. The effectiveness of disease and case management for people with diabetes, a systematic review. Am J Prev Med 2002 May; 22 (4 Suppl.): 15–38
Ellis SE, Speroff T, Dittus RS, et al. Diabetes patient education: a meta-analysis and meta-regression. Patient Educ Couns 2004 Jan; 52(1): 97–105
Kim HS, Oh JA. Adherence to diabetes control recommendations: impact of nurse telephone calls. J Adv Nurs 2003 Nov; 44(3): 256–61
Piette JD, Weinberger M, Kraemer FB, et al. Impact of automated calls with nurse follow-up on diabetes treatment outcomes in a Department of Veterans Affairs Health Care System: a randomized controlled trial. Diabetes Care 2001 Feb; 24(2): 202–8
Vinicor F, Cohen SJ, Mazzuca SA, et al. DIABEDS: a randomized trial of the effects of physician and/or patient education on diabetes patient outcomes. J Chronic Dis 1987; 40(4): 345–56
Meigs JB, Cagliero E, Dubey A, et al. A controlled trial of web-based diabetes disease management: the MGH diabetes primary care improvement project. Diabetes Care 2003 Mar; 26(3): 750–7
Mangione CM, Gerzoff RB, Williamson DF, et al. The association between quality of care and the intensity of diabetes disease management programs. Ann Intern Med 2006 Jul 18; 145(2): 107–16
Smith S, Bury G, O’Leary M, et al. The North Dublin randomized controlled trial of structured diabetes shared care. Fam Pract 2004 Feb; 21(1): 39–45
Varroud-Vial M, Simon D, Attali J, et al. Improving glycaemic control of patients with type 2 diabetes in a primary care setting: a French application of the Staged Diabetes Management Programme. Diabet Med 2004 Jun; 21(6): 592–8
Gruesser M, Hartmann P, Schlottmann N, et al. Structured treatment and teaching programme for type 2 diabetic patients on conventional insulin treatment: evaluation of reimbursement policy. Patient Educ Couns 1996 Oct; 29(1): 123–30
Aubert RE, Herman WH, Waters J, et al. Nurse case management to improve glycemic control in diabetic patients in a health maintenance organization: a randomized, controlled trial. Ann Intern Med 1998 Oct 15; 129(8): 605–12
de Sonnaville JJ, Bouma M, Colly LP, et al. Sustained good glycaemic control in NIDDM patients by implementation of structured care in general practice: 2-year follow-up study. Diabetologia 1997 Nov; 40(11): 1334–40
Polonsky WH, Earles J, Smith S, et al. Integrating medical management with diabetes self-management training: a randomized control trial of the Diabetes Outpatient Intensive Treatment program. Diabetes Care 2003 Nov; 26(11): 3048–53
Kiel PJ, McCord AD. Pharmacist impact on clinical outcomes in a diabetes disease management program via collaborative practice. Ann Pharmacother 2005 Nov; 39(11): 1828–32
Leal S, Glover JJ, Herrier RN, et al. Improving quality of care in diabetes through a comprehensive pharmacist-based disease management program. Diabetes Care 2004 Dec; 27(12): 2983–4
Nichols-English GJ, Provost M, Koompalum D, et al. Strategies for pharmacists in the implementation of diabetes mellitus management programs: new roles in primary and collaborative care. Dis Manage Health Outcomes 2002; 10(12): 783–803
Choe HM, Mitrovich S, Dubay D, et al. Proactive case management of high-risk patients with type 2 diabetes mellitus by a clinical pharmacist: a randomized controlled trial. Am J Manag Care 2005 Apr; 11(4): 253–60
Norris SL, Engelgau MM, Narayan KM. Effectiveness of self-management training in type 2 diabetes: a systematic review of randomized controlled trials. Diabetes Care 2001 Mar; 24(3): 561–87
Diabetes Integrated Care Evaluation Team. Integrated care for diabetes: clinical, psychosocial, and economic evaluation. BMJ 1994 May 7; 308(6938): 1208–12
Kinmonth AL, Woodcock A, Griffin S, et al. Randomised controlled trial of patient centred care of diabetes in general practice: impact on current wellbeing and future disease risk. The Diabetes Care From Diagnosis Research Team. BMJ 1998 Oct 31; 317(7167): 1202–8
Terrin N, Schmid CH, Lau J, et al. Adjusting for publication bias in the presence of heterogeneity. Stat Med 2003 Jul 15; 22(13): 2113–26
Ménard J, Payette H, Baillargeon JP, et al. Efficacy of intensive multitherapy for patients with type 2 diabetes mellitus: a randomized controlled trial. CMAJ 2005 Dec 6; 173(12): 1457–66
Rothman RL, Elasy TA. Can diabetes management programs create sustained improvements in disease outcomes? CMAJ 2005 Dec 6; 173(12): 1467–8
Ofman JJ, Badamgarav E, Henning JM, et al. Does disease management improve clinical and economic outcomes in patients with chronic diseases? A systematic review. Am J Med 2004 Aug 1; 117(3): 182–92
Rubin RJ, Dietrich KA, Hawk AD. Clinical and economic impact of implementing a comprehensive diabetes management program in managed care. J Clin Endocrinol Metab 1998 Aug; 83(8): 2635–42
Sadur CN, Moline N, Costa M, et al. Diabetes management in a health maintenance organization. Efficacy of care management using cluster visits. Diabetes Care 1999 Dec; 22(12): 2011–7
Donohoe ME, Fletton JA, Hook A, et al. Improving foot care for people with diabetes mellitus—a randomized controlled trial of an integrated care approach. Diabet Med 2000 Aug; 17(8): 581–7
Acton K, Valway S, Helgerson S, et al. Improving diabetes care for American Indians. Diabetes Care 1993 Jan; 16(1): 372–5
Cook CB, Ziemer DC, El-Kebbi IM, et al. Diabetes in urban African-Americans. XVI. Overcoming clinical inertia improves glycemic control in patients with type 2 diabetes. Diabetes Care 1999 Sep; 22(9): 1494–500
Smedley BD, Stith AY, Nelson AR, editors. Institute of Medicine: unequal treatment: confronting racial and ethnic disparities in health care. Washington, DC: National Academy Press, 2002
The California Medi-Cal Type 2 Diabetes Study Group. Closing the gap: effect of diabetes case management on glycemic control among low-income ethnic minority populations: the California Medi-Cal type 2 Diabetes Study. Diabetes Care 2004 Jan; 27(1): 95–103
Health literacy: report of the Council on Scientific Affairs. Ad Hoc Committee on Health Literacy for the Council on Scientific Affairs, American Medical Association. JAMA 1999 Feb 10; 281(6): 552–7
Schwartzberg JG, VanGeest JB, Wang CC, editors. Understanding health literacy: implications for medicine and public health. Chicago (IL): AMA Press, 2005
Rothman RL, DeWalt DA, Malone R, et al. Influence of patient literacy on the effectiveness of a primary care-based diabetes disease management program. JAMA 2004 Oct 13; 292(14): 1711–6
Stroebel RJ, Gloor B, Freytag S, et al. Adapting the chronic care model to treat chronic illness at a free medical clinic. J Health Care Poor Underserved 2005 May; 16(2): 286–96
Siminerio LM, Piatt G, Zgibor JC. Implementing the chronic care model for improvements in diabetes care and education in a rural primary care practice. Diabetes Educ 2005 Mar–Apr; 31(2): 225–34
Renders CM, Valk GD, Griffin S, et al. Interventions to improve the management of diabetes mellitus in primary care, outpatient and community settings. Cochrane Database Syst Rev 2001; (1): CD001481
Anderson JE, Nelson DE, Wilson RW. Telephone coverage and measurement of health risk indicators: data from the National Health Interview Survey. Am J Public Health 1998 Sep; 88(9): 1392–5
Piette JD, Weinberger M, McPhee SJ, et al. Do automated calls with nurse follow-up improve self-care and glycemic control among vulnerable patients with diabetes? Am J Med 2000 Jan; 108(1): 20–7
Snyder JW, Malaskovitz J, Griego J, et al. Quality improvement and cost reduction realized by a purchaser through diabetes disease management. Dis Manag 2003 Winter; 6(4): 233–41
Goetzel RZ, Ozminkowski RJ, Villagra VG, et al. Return on investment in disease management: a review. Health Care Financ Rev 2005 Summer; 26(4): 1–19
Kreuter MW, Chheda SG, Bull FC. How does physician advice influence patient behavior? Evidence for a priming effect. Arch Fam Med 2000 May; 9(5): 426–33
Casalino LP. Disease management and the organization of physician practice. JAMA 2005 Jan 26; 293(4): 485–8
Villagra VG. Integrating disease management into the outpatient delivery system during and after managed care. Health Aff (Millwood) 2004 Jan–Jun; Suppl. Web Exclusives: W4-281-3
Steffens B. Cost-effective management of type 2 diabetes: providing quality care in a cost-constrained environment. Am J Manag Care 2000 Aug; 6 (13 Suppl.): S697-703; discussion S4-9
Cranor CW, Bunting BA, Christensen DB. The Asheville Project: long-term clinical and economic outcomes of a community pharmacy diabetes care program. J Am Pharm Assoc (Wash) 2003 Mar–Apr; 43(2): 173–84
Stevens DP, Wagner EH. Transform residency training in chronic illness care-now. Acad Med 2006 Aug; 81(8): 685–7
Acknowledgments
Drs Cavanaugh and White have no conflicts of interest directly relevant to the content of this review. Dr Rothman is funded by the National Institutes of Health (NIH), NIDDK, K23 Career Development Award (DK065294) to explore the role of chronic disease management in adolescents with diabetes. Dr Rothman has also received funding from the American Diabetes Association (Novo Nordisk Clincal Research Award), the Pfizer Clear Health Communication Initiative, and the Vanderbilt Diabetes Research and Training Centre (NIDDK 5P60DK020593) to examine the role of literacy and numeracy in diabetes disease management.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cavanaugh, K.L., White, R.O. & Rothman, R.L. Exploring Disease Management Programs for Diabetes Mellitus. Dis-Manage-Health-Outcomes 15, 73–81 (2007). https://doi.org/10.2165/00115677-200715020-00002
Published:
Issue Date:
DOI: https://doi.org/10.2165/00115677-200715020-00002