Abstract
Type 1 diabetes mellitus (T1D) is a chronic autoimmune disease characterized by β cell destruction, insulin deficiency and hyperglycemia. Activated macrophages and autoimmune T cells play a crucial role in the pathogenesis of hyperglycemia in NOD murine diabetes models, but the molecular mechanisms of macrophage activation are unknown. We recently identified pigment epithelium-derived factor (PEDF) as an adipocyte-derived factor that activates macrophages and mediates insulin resistance. Reasoning that PEDF might participate as a proinflammatory mediator in murine diabetes, we measured PEDF levels in NOD mice. PEDF levels are significantly elevated in pancreas, in parallel with pancreatic TNF levels in NOD mice. To identify experimental therapeutics, we screened 2,327 compounds in two chemical libraries (the NIH Clinical Collection and Pharmakon-1600) for leads that inhibit PEDF mediated TNF release in macrophage cultures. The lead molecule selected, “emetine” is a widely used emetic. It inhibited PEDF-mediated macrophage activation with an EC50 or 146 nmol/L. Administration of emetine to NOD mice and to C57Bl6 mice subjected to streptozotocin significantly attenuated hyperglycemia, reduced TNF levels in pancreas and attenuated insulitis. Together, these results suggest that targeting PEDF with emetine may attenuate TNF release and hyperglycemia in murine diabetes models. This suggests that further investigation of PEDF and emetine in the pathogenesis of human diabetes is warranted.
Similar content being viewed by others
Introduction
Type 1 diabetes mellitus (T1D) is a chronic autoimmune disease characterized by β cell destruction resulting in insulin deficiency and hyperglycemia. The incidence of T1D is increasing worldwide, and in the United States the prevalence is 1 in 300 by the age of 18 years, with associated annual costs of $14.9 billion (1,2). The chronicity of T1D beginning early in life leads to serious long-term complications affecting the renal, cardiovascular, retinal and neural systems (3). Despite extensive research and significant advances in patient care, the treatment of T1D is mainly limited to multiple daily insulin injections that inadequately prevent severe hyperglycemia and diabetes related complications.
Experimental models of T1D include the non-obese diabetic (NOD) mice, and streptozotocin (STZ)-induced diabetes in C57Bl6 mice. Studies in NOD mice reveal a role for several immune cell phenotypes in β cell death, including CD4 + and CD8 + T cells [4–6] and macrophages (7). Macrophages and dendritic cells are the first to infiltrate the pancreas during the development of experimental T1D in NOD mice (8,9). Non-invasive cytofluorometric analysis shows progressive infiltration of the pancreas by CD11b +/CD11c- macrophages in the BDC2.5_NOD T cell receptor transgenic murine model of T1D (10). Inhibition of complement receptor 3 (CR3 or CD11b/CD18) prevents macrophage and T cell infiltration of pancreatic islets and ameliorates disease in NOD mice (11). Depletion of macrophages from the pancreas arrests the development of T1D (12,13). Macrophages mediate the pathogenesis of T1D in this model by secreting tumor necrosis factor (TNF) and other proinflammatory cytokines that modulate β cell cytotoxicity (14,15). In NOD mice, anti-TNF antibody treatment confers significant protection against the development of diabetes (15). Furthermore, TNF receptor 1 (TNFR1) deficient NOD mice show a reduction in the development of hyperglycemia as well as improved survival (14). Together these data indicate an important role of macrophages and TNF in the pathogenesis of murine diabetes. However, the mechanisms that initiate macrophage activation resulting in increased TNF release are poorly understood.
Pigment epithelium-derived factor (PEDF), also known as serpin F1 (SER-PINF1), is a 50 kDa protein member of the serpin family of protease inhibitors that has been studied for its anti-angiogenic, anti-tumorigenic and neurotrophic properties. Recently, we discovered that PEDF as an adipocyte-derived factor that can stimulate macrophage TNF activation and mediate insulin resistance (16). It was initially discovered as a factor secreted by retinal epithelial cells, but we and others have found that PEDF is also released by adipocytes and hepatocytes, and mediates inflammatory phenotype in macrophages (16–18). The cytokine activities of PEDF include activation of macrophages to increase expression of proinflammatory cytokines, differentiation of neurons, inhibition of endothelial cell migration and proliferation, prevention of angiogenesis and suppression of tumor growth (16,19). PEDF modulates target cell responses by signaling via a family of unrelated high affinity receptors. The anti-angiogenic activity of PEDF is mediated by the laminin receptor (19–21); low-density lipoprotein receptor-related protein 6 (LPR6; Wnt co-receptor) (22); and cell surface F1F0-ATP synthase (23). The macrophage stimulating (16) and neurotrophic activities (24) of PEDF are mediated by adipose triglyceride lipase (ATGL), also known as patatin-like phospholipase domain containing 2 (PNPLA2; PEDF-RN).
Elevated levels of PEDF have been observed in humans with type 2 diabetes mellitus, obesity, metabolic syndrome, vascular inflammation and cardiovascular diseases (25–27). In type 1 diabetes patients, microvascular complications, vascular stiffness, inflammation and diabetic retinopathy have been significantly correlated with increased serum levels of PEDF (28,29). Systemic PEDF administration to naïve animals induced activation of proinflammatory cytokine responses, and reduced insulin sensitivity (16,18). Inhibition or blockade of PEDF in obese, insulin-resistant mice, significantly improves whole-body insulin sensitivity, even when initial dosing of inhibitors was delayed until after the onset of frank obesity (18).
Here we reasoned that the cytokine-like proinflammatory role of PEDF might be exploited as a potential target in T1D. Accordingly, we developed a high throughput screen to identify PEDF inhibitors, and discovered that emetine Di-HCl attenuates PEDF mediated cytokine production and hyperglycemia in NOD and streptozotocin-induced murine diabetes.
Materials and Methods
Animals
NOD female mice (15–20 g) and C57Bl/6 male mice (20–25 g) acquired from Taconic were housed at 25°C under light-controlled conditions with a 12-h light/dark cycle. Mice were given free access to water and standard rodent chow and were acclimated to their environment for 1 wk before experimentation. All animal studies were approved by the Institutional Animal Care and Use Committee of the Feinstein Institute for Medical Research, Northwell Health.
Induction of Diabetes
T1D was induced by administration of streptozotocin (Sigma-Aldrich) (50 mg/kg dissolved in sodium citrate buffer, pH 4.5) to 6 to 8 wk old C57Bl/6 mice intraperitoneally (i.p.) once each day for 5 consecutive days. Mice were given water supplemented with 10% sucrose (Sigma-Aldrich) for six days to prevent sudden hypoglycemia during streptozotocin administration. For time course studies, body weight and blood glucose were measured every other day. Blood glucose was measured with a FreeStyle Lite blood glucose meter (Abbot Diabetes Care, Inc.). For studies with emetine (EMD Millipore), mice received daily administration of emetine dihydrochloride (0.002, 0.02, 0.2 and 2 mg/kg) or saline. Blood glucose with either FreeStyle Lite blood glucose meter (Abbot Diabetes Care, Inc.) or Bayer Contour blood glucose meter (Bayer HealthCare, LLC.) and body weight were measured once weekly. At the end of each study, mice were euthanized by CO2 asphyxiation. Blood and pancreas were collected for cytokine analysis.
NOD Mice
NOD female mice received i.p. administrations of emetine (0,0.002, 0.02, 0.2 and 2 mg/kg) daily beginning at 5 wks of age. Blood glucose and body weight were recorded weekly. At the end of the studies, mice were euthanized by CO2 asphyxiation. Blood and pancreas collected for cytokine analysis.
Histology
Pancreas were fixed in 10% formalin, and processed for paraffin embedding (AML Laboratory and Genecopoeia). 7-µm-thick sections were stained with hematoxylin/eosin (Genecopoeia) and the degree of insulitis was evaluated microscopically. Islets were analyzed in multiple sections at 20×. Images were captured by Zeiss Axiovert 20-inverted microscope, using the AxioVision V5 software (Zeiss). Insulitis was scored by infiltration grade 0 to 4 (0 = no visible infiltration; 1 = perivascular/periductular infiltrates with leukocytes touching islet perimeters, but not penetrating; 2 = leukocytic penetration of up to 25% of islet mass; 3 = leukocytic penetration of up to 75% of islet mass; 4 = end-stage insulitis) (30).
Cytokine Analysis
Pancreas tissues were homogenized with 1:1 zirconium oxide 1.0 mm beads in two volumes of T-PER Tissue Protein Extraction Reagent (Thermo Fisher Scientific Inc.), supplemented with complete protease inhibitor cocktail (Roche Applied Science). Samples were homogenized using a BBX24 Bullet Blender homogenizer (Next Advance Inc.) at speed 8 for 5 min. Supernatants were collected by centrifugation at 10,000g for 10 min at 4°C. Levels of TNF (R&D systems) and PEDF (BioProducts MD, LLC) were evaluated using commercially available enzyme-linked immunosorbent assay (ELISA) kits as per manufacturer’s instructions.
Cell Culture
Murine macrophage-like RAW 264.7 cells (American Type Culture Collection) were cultured in Dulbecco’s Modified Eagle’s Medium supplemented with 10%FBS, 1% penicillin-streptomycin and 1% L-Glutamine (Life Technologies). For high-throughput screening, cells were seeded onto 96-well plates at 5 × 105 cells/mL and incubated overnight in a humidified chamber at 37°C with 5% CO2. Cells were washed twice with optimum then pre-incubated with compounds from drug libraries (NIH Clinical Collection, Evotec US, Inc. and Pharmakon-1600, MicroSource Discovery Systems, Inc.) for 30 min prior to challenge with his-sumo-rhPEDF (0.05 μg/mL). Supernatant was collected after 2.5 h and TNF levels were analyzed by ELISA. Cell viability was assessed either by 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) assay (EMD Millipore) or by quantitating lactate dehydrogenase (LDH) levels (Takara Bio, Inc.) in the supernatants. The IC50 value of emetine was calculated using ED50 Plus v1.0 online software.
Surface Plasmon Resonance
The Biacore T200 instrument (GE Healthcare) was used for real time binding interaction experiments. For binding analysis, recombinant ATGL (Abnova) was immobilized onto CM5 dextran biosensor chips. The biosensor chip was activated by amine coupling using 0.4 mol/L 1-ethyl-3-(3-dimethylaminopropyl)-carbodiimide (EDC) and 0.1 mol/L N-hydroxysuccinimide. Immobilization of a 75 µg/mL concentration of ATGL (Abnova) to the sample flow-cell was accomplished by injection at a flow rate of 30 µL/min until the SPR reached ~ 100 to 300 RU. Binding assays were performed at a flow rate of 30 µL/min for 60 s at 25°C in 1 × PBS buffer, pH 5.5 and 0.1% surfactant p20. For ATGL-emetine binding, increasing concentrations of emetine (0 to 500 µmol/L) were flowed over immobilized ATGL. For ATGL-PEDF binding, increasing concentrations rhPEDF (Abcam) (0 to 1, 000 nmol/L) were used as the analyte. A sample of running buffer alone was subtracted from the resulting reaction surface data. Results were analyzed using Biacore T200 Evaluation Software version 2.0 (GE Healthcare). The equilibrium disassociation binding constant (KD) was determined with Biacore T200 Evaluation Software version 2.0 supposing a 1:1 binding ratio.
Statistical Analysis
Data are presented as means ± SEM. A two-way ANOVA (Turkey), one-way ANOVA with Fischer’s protected, chi-square test for trend, chi-square test, log rank test or Student t test was used where specified; then least significant difference test was conducted.
Results
Pancreatic PEDF and TNF Levels in Murine Streptozotocin (STZ)-Induced Hyperglycemia
To determine the expression kinetics of PEDF in pancreas, we measured PEDF levels in a standard murine model of T1D. In this model, streptozotocin, an alkylating agent, enters the β cell via a glucose transporter (GLUT2) and alkylates DNA, leading to β cell death, resulting in severe insulin deficiency and hyperglycemia (31,32). Plasma glucose concentrations in streptozotocin-injected mice were more than >200 mg/dL by d 7, and remained at that level thereafter (Figure 1A). Pancreatic PEDF levels increased in time-dependent manner following streptozotocin administration (Figure 1B). Pancreatic PEDF was >12,000 pg/mg protein by d 12, and remained elevated for the entire observation period. Increasing PEDF levels in pancreatic tissue were significantly correlated with increasing levels of blood glucose (Figure 1C). Moreover, we observed that TNF levels in the pancreas were also significantly increased (Figure 1D), and were strongly correlated with pancreatic PEDF levels (Figure 1E). Serum PEDF and TNF levels did not change significantly in the streptozotocin animals as compared with vehicle control animals (data not shown).
Blood glucose, pancreatic TNF and pancreatic PEDF are elevated in a low-dose streptozotocin model of T1D. (A) Blood glucose, (B) PEDF and (D) TNF levels increase over time in mice streptozotocin-induced type 1 diabetes. Levels of PEDF and TNF and were monitored in blood and pancreas over time. Pancreatic PEDF levels are correlated with (C) blood glucose and (E) pancreatic TNF levels. (A) Days: 0 (n = 84); 7 (n = 62); 5, 11, 13, 15, 17, 19 and 21 (n = 7). (B, D) n = 7. (C, E) Data are shown as mean ± SEM with a linear regression fit model (n = 7).
PEDF Induces Inflammatory Cytokine Secretion by Macrophages
Previous studies demonstrated that PEDF induces an inflammatory phenotype and cytokine release in macrophages and other cells (16–18). Here, we analyzed the profile of inflammatory mediators released by macrophages in response to PEDF. Murine macrophage like cells RAW 264.7 were stimulated with increasing concentration of PEDF and an array of cytokines was analyzed using a multiplex assay. PEDF induced a concentration dependent increase in TNF, IL-6, KC/GRO, IL-12p40 and IL-10, but not IL-1β or IFNγ, secretion by macrophages as measured in culture medium at 6 h (Table 1) and 24 h post stimulation (Table 2).
Identification of a novel PEDF Antagonist
Reasoning that it might be possible to identify PEDF inhibitors, we next established a high-throughput bioassay to screen 2,327 compounds derived from two libraries: the NIH Clinical Collection and Pharmakon-1600. These compound libraries are a collection of small molecules that are either federal drug administration (FDA) approved, or are experimental therapeutics that have been previously used in clinical phase trials. Macrophages were pre-exposed to test compounds for 30 min, and then challenged with PEDF for 2.5 h. TNF levels were subsequently measured in the supernatants.
From the NIH clinical collection we selected 503 compounds that reduced TNF secretion from macrophages by 25% or greater at a concentration of 5 µmol/L. Next, macrophages were pre-exposed to increasing concentrations of 503 test compounds, and then stimulated with PEDF. We eliminated compounds that induced cell viability of less than 60% as determined by MTT assay. Next we selected 44 candidates from 503 previously selected compounds that inhibited PEDF induced TNF release (50% reduction) at a concentration of 5 µmol/L. Finally, we screened increasing concentrations of these 44 compounds along with an additional 1,600 compounds from the Pharmakon-1600 library to identify candidate drugs that at a ten-fold lower concentration (0.5 µmol/L) can reduce at least 50% of secreted TNF from PEDF-challenged macrophages (Figure 2A).
High-throughput screening for antagonists of PEDF-mediated macrophage activation. (A) Raw 264.7 cells were pre-exposed to 5 µM concentrations of compounds from the NIH Clinical Collection library then challenged with his-sumo- rhPEDF (0.05 µg/mL) for 2.5 h. The supernatant was collected for TNF analysis. Five hundred and three compounds that show at least 25% suppression of TNF release were re-tested with 2 concentrations (0.5 µmol/L and 5 µmol/L), and TNF levels and cell viability was assessed (see Materials and Methods). Forty-four compounds that had at least 50% suppression at 5µM as well as at least 60% viability by MTT were re-tested at various concentrations along with 1,600 additional compounds from the Pharmakon-1600 library (0.005, 0.05, 0.5 and 5 µmol/L). TNF analysis and viability, by MTT, were analyzed. Three candidate drug targets that yield a concentration-dependent response, at least 50% suppression at 0.5 µmol/L and at least 60% viability at 0.5 µmol/L concentration were identified. Emetine is one of the three-candidate drug targets that was studied in detail. (B) Summary of lead compounds. (C) Emetine inhibits PEDF induced TNF release in concentration dependent manner. Horizontal dashed line represents the lower limit of assay detection at 31.5 pg/mL. Emetine does not induce cell toxicity at the concentrations tested. Cell viability was analyzed by (D) LDH Assay and (E) MTT Assay. (D and E) Data are mean ± SEM. Statistical analysis was measured by one-way ANOVA.
Compounds that showed a concentration-dependent reduction in TNF and a viability of greater than 60% were selected as lead clinical candidates. Results show that 62% of the identified leading compounds were corticosteroids, while a composite of other known antiinflammatory compounds represented 11% of these leading candidates (Figure 2B). Among the screened drug candidates, emetine was identified as a lead compound with significant concentration dependent suppression of PEDF-induced TNF secretion and an IC50 of 146 nmol/L (Figure 2C). Analysis of supernatants for cell toxicity did not show increased LDH leakage from emetine-treated cells (Figure 2D). Additionally, mitochondrial activity was unaffected by emetine as determined by MTT cytotoxicity assay (Figure 2E) indicating that emetine inhibits PEDF-mediated TNF release without affecting cell viability.
Emetine Binds ATGL with High Affinity
To elucidate the underlying molecular mechanism of emetine-mediated inhibition of PEDF-induced TNF release, we examined whether emetine interferes with the binding of PEDF to its receptor ATGL. Surface plasmon resonance analysis demonstrated that emetine binds to PEDF receptor ATGL with high-binding affinity (KD = 14.3 nmol/L) (Figure 3A).
Emetine binds to ATGL with high affinity. Surface plasmon resonance analysis was conducted by immobilizing ATGL on a CM5 dextran biosensor chip surface (see Materials and Methods). (A) ATGL ligand of ∼300 RU and emetine analyte (0-500 µmol/L). (B) ATGL ligand at ~ 100 RU, then PEDF (0-1,000 nmol/L) added as an analyte.
This binding affinity was ten-fold greater than that of PEDF to its receptor ATGL (KD = 214 nmol/L) (Figure 3B).
Emetine Administration Attenuates Hyperglycemia and Reduces Pancreatic TNF Levels in T1D
To evaluate the therapeutic potential of emetine, we next studied whether emetine can improve disease severity in T1D mice. C57Bl/6 male mice with streptozotocin-induced T1D received a daily administration of emetine, and changes in body weight and blood glucose were monitored. Emetine did not induce any significant difference in body weight in mice with low-dose streptozotocin model of T1D (Figure 4A). In contrast, administration of emetine not only attenuated blood glucose levels in dose-dependent way but also induced a persistent attenuation of blood glucose levels. Daily administration of emetine dose-dependently attenuated hyperglycemic response by d 21 (Figure 4B). Consistent with this observation, administration of emetine, but not the vehicle control, resulted in a sustained attenuation of blood glucose levels (Figure 4C). Accordingly, mice from the vehicle control group demonstrated significantly increased insulitis scores as compared with mice receiving emetine (Figure 4D, E). Levels of TNF in homogenized pancreas were significantly attenuated by emetine administration in doses of 2 mg/kg (Figure 4F).
Emetine improves disease severity in a streptozotocin model of T1D. (A) Emetine administration did not induce any significant changes in body weight. Body weights collected at the end of the study are shown here. (B) Emetine administration attenuated blood glucose levels in a dose dependent manner. Blood glucose measured at d 21 in all the dose groups is shown here. (n = 10/group, one way ANOVA: † p < 0.01) (C) Emetine (2 mg/kg) induced a persistent attenuation of blood glucose levels. Data are mean ± SEM. (n = 10/group, two way ANOVA: † p < 0.01, # p < 0.0001). (D) Representative images of hematoxylin and eosin stained pancreatic islets from mice receiving saline or emetine (2 mg/kg). Islet from a naïve animal is shown as a representation of a normal islet. Scale bar-50 µm. (E) Emetine (2 mg/kg) induces decrease in insulitis severity. Data are mean ± SEM. (n = 5; islets: saline = 81 and emetine = 53, Student t-test, p = 0.72). (F) Emetine induces significant attenuation of pancreatic TNF levels. Data are mean ± SEM. (n = 10/group, one way ANOVA: *p < 0.05).
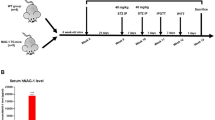
Next, we assessed the efficacy of emetine in attenuating disease severity in a spontaneous model of T1D. NOD female mice received either saline or emetine once daily for 14 wks, and body weight and blood glucose levels were monitored over time. Body weight was unaffected by emetine administration to animals as compared with control animals exposed to saline (Figure 5A). In the saline group, 80% of animals developed hyperglycemia at 19 wks of age, whereas NOD mice receiving emetine were significantly and dose-dependently protected from hyperglycemia (Figure 5B). Only 40% of the NOD mice receiving emetine developed hyperglycemia (Figure 5B). There was also a time-dependent delay in the onset and progression of hyperglycemia in mice treated with emetine when compared with saline-treated animals (Figure 5C). Although 40% of the animals from the emetine treated group developed hyperglycemia, the levels of blood glucose were significantly lower in emetine receiving animals as compared with the saline group (Figure 5D). We observed a small fraction of non-responders in the emetine treated group (~30%) that maintained high levels of blood glucose even after emetine administration (Figure 5D). Insulitis scores were significantly reduced in animals exposed to emetine as compared with saline-treated mice (Figure 5E, F, G). In line with our observations in the streptozotocin model, pancreatic TNF levels were also significantly in the emetine treated NOD mice (Figure 5H). Taken together, these results indicate that emetine attenuates hyperglycemia and insulitis in two independent murine models of diabetes.
Emetine improves disease severity in a spontaneous model of NOD T1D. (A) Emetine administration did not induce any significant changes in body weight. Body weights collected at the end of the study (19 wks) are shown here. (B) Emetine dose-dependently protects animals from hyperglycemia. Total number of animals, at wk 19, developing hyperglycemia is shown here. Mice with blood glucose levels above 200 mg/dL were considered hyperglycemic, p = 0.01. (C) Time course of the percent of mice that are hyperglycemic (200 mg/dL) in saline and emetine (2 mg/kg) treated animals, p = 0.02. (D) Individual blood glucose levels measured at 19 wks of age. Red data points signify the last measured blood glucose level of mice that did not survive until the end of the study. (E) Representative images of hematoxylin & eosin (H&E) stained pancreatic islets of Langerhans from either saline or emetine (0.2mg/kg) treated animals. Scale bar, 50 µm. (F) Insulitis scores of top slice of H&E stained pancreatic islets from saline and emetine (0.2 mg/kg) treated animals, p = 0.0037. (G) Percentage of total islets are sectioned into score categories, p < 0.0001. (H) Emetine induces significant attenuation of pancreatic TNF levels. (A-D) 0 mg/kg (n = 14), 0.002 mg/kg (n = 14), 0.02 mg/kg (n = 13), 0.2 mg/kg (n = 14), 2 mg/kg (n = 13). (H) 0 mg/kg (n = 12), 0.002 mg/kg (n = 14), 0.02 mg/kg (n = 11), 0.2 mg/kg (n = 12), 2 mg/kg (n = 13). (F, G) n = 4 (islets: saline = 29, emetine = 48). Data are mean ± SEM. Statistical analysis was measured by (A and D, H) one-way ANOVA, (B) chi-square test for trend, (C) Kaplan-Meier curve with a log rank test for trend, (G) chi-square test, and (F) Student t test, p ≤ 0.05(*).
Discussion
The principal findings here indicate that PEDF levels are increased in experimental murine T1D, and that administration of a PEDF inhibitor emetine significantly attenuates disease severity. PEDF is a ubiquitous protein in a wide range of human tissues (33), and PEDF levels are significantly associated with various metabolic diseases (25,34–36). In the present results from murine streptozotocininduced diabetes, PEDF and TNF levels are significantly increased in pancreas, and expression significantly correlated with blood glucose levels. Results from high-throughput screenings revealed that emetine is a potent inhibitor of PEDF-induced macrophage activation. Emetine binds the PEDF receptor ATGL and attenuates TNF release mediated by PEDF. In low-dose streptozotocin and NOD mouse models of T1D, emetine administration attenuates hyperglycemia, reduces insulitis and decreases levels of pancreatic TNF.
To our knowledge, these are the first results implicating increased pancreatic PEDF in this model of T1D. In agreement with our prior findings that PEDF stimulates macrophage TNF release, rising PEDF levels in pancreas correlate with increasing levels of pancreatic TNF. On the contrary, circulating levels of PEDF did not change significantly, and did not correlate with levels of blood glucose (data not shown). In an experimental model of ethanol-induced pancreatitis, immunohistochemical analysis showed increased levels of PEDF in the acinus of the inflamed pancreas (37). It is possible that pancreatic PEDF may be locally derived from acinar cells in experimental T1D, and local accumulation of PEDF may induce inflammatory phenotype. Pancreatic levels of PEDF were positively correlated with both TNF and increased levels of blood glucose, suggesting that PEDF may contribute to the pathogenesis of disease in T1D.
We observed an initial decrease in pancreatic levels of PEDF and TNF within the first week of administration of streptozotocin to animals. This may be a result of an increase in insulin release from cytotoxic β cells (38). Insulin has previously been shown to reduce PEDF expression in adipose tissue of T2D patients (39). It is possible that insulin reduces the levels of PEDF in the pancreas and, as a result, TNF levels are also decreased in the first week of streptozotocin-induced T1D. Together, these findings indicate that PEDF may act as an inflammatory mediator in experimental T1D.
We have previously demonstrated that PEDF activates macrophages and induces the release of TNF (16). At a concentration of 0.05 µg/mL, the concentration of PEDF used for the high-throughput screening of test compounds and in vitro studies with emetine, TNF secretion was significantly enhanced from macrophages as compared with other cytokines. At higher concentrations, PEDF also stimulated the release of the inflammatory cytokines IL-6, KC/GRO, IL-12p40 and the antiinflammatory cytokine IL-10. TNF and IL-6 are regulated by both P38MAPK and extracellular signal-regulated kinases (ERK) phosphorylation (16,40). KC/GRO, IL-12p40, and IL-10 require P38MAPK activation and is necessary for the regulation of macrophage-derived IL-6, KC/GRO and IL-10 (40–42). It is interesting to consider that both proinflammatory cytokines IL-1β and IFNγ were not increased in this experiment, even at 24 h. IL-1β and IFNγ production require caspase-1 activation (43,44). This suggests that PEDF induces the activation of macrophages and promotes the release of cytokines through P38MAPK and ERK signaling, independent of caspase-1. Collectively, this suggests that PEDF is a specific activator of TNF release from macrophages.
Emetine is an alkaloid that has been tested in Phase I and II clinical trials against solid tumors (45). Emetine has been used as an anti-protozoal drug and a cough suppressant, although its use is limited by cardiotoxicity (46,47). Exposure of macrophages to emetine reduces PEDF stimulated TNF release with an IC50 of 146 nmol/L. At these concentrations, emetine does not induce cytotoxicity as demonstrated by both LDH and MTT assays. Additionally in vivo, in the doses used here, emetine did not mediate significant changes in body weight. We have previously shown that macrophages express PEDF receptors, and PEDF mediated its inflammatory phenotype through its receptor ATGL. Here, we demonstrated that emetine binds to PEDF receptor, ATGL, with almost 15-fold higher affinity than PEDF. It is plausible that emetine mediates its inhibition of TNF release by direct binding to ATGL. The cardiotoxicity of emetine may limit its chronic use in humans, suggesting that a search for other, less toxic PEDF inhibitors is warranted.
The increased levels of PEDF in pancreatic tissue indicate its importance in the pathogenesis of murine type 1 diabetes. To address the role of PEDF, we treated streptozotocin induced T1D mice with a PEDF-antagonist, emetine. As expected, emetine treatment attenuated blood glucose levels and improved insulitis. Unlike the streptozotocin model of T1D, NOD mice are genetically susceptible to spontaneously develop T1D-like symptoms, including hyperglycemia (31). Similar to both the streptozotocin model and human T1D, NOD mice exhibit autoimmune responses that lead to the development of hyperglycemia (31). Emetine administration not only significantly delayed the onset of hyperglycemia and reduced the total number of hyperglycemic animals, it also attenuated the development of insulitis. We did notice that some NOD mice failed to respond to emetine, which began at 5 wks of age. The basis of this observation is not clear from our studies. It is plausible that in a subset of NOD mice, the disease onset and progression may have preceded emetine treatment, as macrophage infiltration occurs as early as 3 wks in animals that develop T1D (9). Together, these studies suggests that PEDF as an early mediator in T1D, which may influence immune cell migration into islets. Furthermore, these findings also show that emetine, perhaps through inhibition of TNF from macrophages, can suppress immune cell translocation into the islets of Langerhans.
Conclusion
We observed a reduction in pancreas levels of TNF with emetine enterprise. Remarkably, emetine at 2 mg/kg for mice, the highest dose used in these experiments, is equivalent to 0.167 mg/kg in humans (48). This is 11% of the clinically tested dosage for cancer treatment, which is an intravenous at a dose of 1.5 mg/kg (55.5 mg/m2) (48,49). Currently clinical trials exist for the prevention of T1D in genetically at-risk patients (50,51). It is plausible to consider the use of emetine in patients at high risk for T1D. Collectively these data suggest that PEDF is a local inflammatory mediator in T1D and that emetine, or other PEDF inhibitors, may represent a novel therapeutic strategy.
Disclosure
The authors declare they have no competing interests as defined by Molecular Medicine, or other interests that might be perceived to influence the results and discussion reported in this paper.
References
Dabelea D et al. (2014) Prevalence of type 1 and type 2 diabetes among children and adolescents from 2001 to 2009. JAMA. 311: 1778–86. doi:10.1001/jama.2014.3201
Dall TM et al. (2009) Distinguishing the economic costs associated with type 1 and type 2 diabetes. Popul Health Manag. 12:103–10. Available: http://www.ncbi.nlm.nih.gov/pubmed/19361253
Daneman D (2006) Type 1 diabetes. Lancet. 367:847–58. doi:10.1016/S0140-6736(06)68341-4
Roep BO, Peakman M (2011) Diabetogenic T lymphocytes in human Type 1 diabetes. Curr Opin Immunol. 23:746–53. doi:10.1016/j.coi.2011.10.001
Burton AR et al. (2008) the pathogenicity of autoantigen-specific T-cell receptors. Diabetes 57:1321–30. doi:10.2337/db07-1129
DiLorenzo TP, Serreze DV (2005) The good turned ugly: immunopathogenic basis for diabetogenic CD8+ T cells in NOD mice. Immunol. Rev. 204:250–63. doi:10.1111/j.0105-2896.2005.00244.x
Calderon B, Suri A, Unanue ER (2006) In CD4+ T-Cell-Induced Diabetes, Macrophages Are the Final Effector Cells that Mediate Islet β-Cell Killing. Am. J. Pathol. 169:2137–2147. doi:10.2353/ajpath.2006.060539
Cvetkovic I et al. (2005) Critical role of macrophage migration inhibitory factor activity in experimental autoimmune diabetes. Endocrinology146:2942–51. doi:10.1210/en.2004-1393
Jansen A, Homo-Delarche F, Hooijkaas H, Leenen PJ, Dardenne M, Drexhage HA (1994) Immunohistochemical characterization of monocytes-macrophages and dendritic cells involved in the initiation of the insulitis and beta-cell destruction in NOD mice. Diabetes 43:667–675. doi:10.2337/diabetes.43.5.667
Denis MC, Mahmood U, Benoist C, Mathis D, Weissleder R (2004) Imaging inflammation of the pancreatic islets in type 1 diabetes. Proc. Natl. Acad. Sci. U. S. A. 101:12634–9. doi:10.1073/pnas.0404307101
Hutchings P, Rosen H, O’Reilly L, Simpson E, Gordon S, Cooke A (1990) Transfer of diabetes in mice prevented by blockade of adhesion-promoting receptor on macrophages. Nature 348:639–42. doi:10.1038/348639a0
Jun HS, Yoon CS, Zbytnuik L, van Rooijen N, Yoon JW (1999) The role of macrophages in T cell-mediated autoimmune diabetes in non-obese diabetic mice. J. Exp. Med. 189:347–358. doi:10.1084/jem.189.2.347
Jun HS, Santamaria P, Lim HW, Zhang ML, Yoon JW (1999) Absolute requirement of macrophages for the development and activation of β-cell cytotoxic CD8+ T-cells in T-cell receptor transgenic NOD mice. Diabetes 48:34–42. doi:10.2337/diabetes.48.1.34.
Chee J et al. (2011) TNF receptor 1 deficiency increases regulatory T cell function in nonobese diabetic mice. J. Immunol. 187:1702–12. doi:10.4049/jimmunol.1100511
Lee L-F et al. (2005) The role of TNF-alpha in the pathogenesis of type 1 diabetes in the non-obese diabetic mouse: analysis of dendritic cell maturation. Proc. Natl. Acad. Sci. U. S. A. 102:15995–6000. doi:10.1073/pnas.0508122102
Chavan SS et al. (2012) Identification of pigment epithelium-derived factor as an adipocyte-derived inflammatory factor. Mol. Med. 18:1161–8. doi:10.2119/molmed.2012.00156
Famulla S et al. (2011) Pigment epithelium-derived factor (PEDF) is one of the most abundant proteins secreted by human adipocytes and induces insulin resistance and inflammatory signaling in muscle and fat cells. Int J Obes (Lond). Nature 35:762–72. doi:10.1038/ijo.2010.212
Crowe S et al. (2009) Pigment epithelium-derived factor contributes to insulin resistance in obesity. Cell Metab. 10:40–7. doi:10.1016/j.cmet.2009.06.001
Filleur S, Nelius T, de Riese W, Kennedy RC (2009) Characterization of PEDF: a multi-functional serpin family protein. J. Cell. Biochem. 106:769–75. doi:10.1002/jcb.22072
Bernard A, Gao-Li J, Franco C-A, Bouceba T, Huet A, Li Z (2009) Laminin receptor involvement in the anti-angiogenic activity of pigment epithelium-derived factor. J Biol. Chem. 284:10480–90. doi:10.1074/jbc.M809259200
Alberdi E, Aymerich MS, Becerra SP (1999) Binding of Pigment Epithelium-derived Factor (PEDF) to Retinoblastoma Cells and Cerebellar Granule Neurons: EVIDENCE FOR A PEDF RECEPTOR. J Biol. Chem. 274:31605–31612. doi:10.1074/jbc.274.44.31605
Qi W et al. (2014) High Levels of Pigment Epithelium-derived Factor in Diabetes Impair Wound Healing through Suppression of Wnt Signaling. Diabetes 5:1–67. doi:10.2337/db14-1111
Notari L, Arakaki N, Mueller D, Meier S, Amaral J, Becerra SP (2010) Pigment epithelium-derived factor binds to cell-surface F(1)-ATP synthase. FEBS J. 277:2192–205. doi:10.1111/j.1742–4658.2010.07641.x
Notari L et al. (2006) Identification of a lipase-linked cell membrane receptor for pigment epithelium-derived factor. J Biol. Chem. 281:38022–37. doi:10.1074/jbc.M600353200
Nakamura K, Yamagishi S-I, Adachi H, Kurita-Nakamura Y, Matsui T, Inoue H (2009) Serum levels of pigment epithelium-derived factor (PEDF) are positively associated with visceral adiposity in Japanese patients with type 2 diabetes. Diabetes Metab Res Rev. 25:52–6. doi:10.1002/dmrr.820
Yamagishi S-I (2006) et al. Elevated serum levels of pigment epithelium-derived factor in the metabolic syndrome. J. Clin. Endocrinol. Metab. 91:2447–50. doi:10.1210/jc.2005-2654
Jenkins A et al. (2008) Increased serum pigment epithelium derived factor levels in Type 2 diabetes patients. Diabetes Res Clin Pract. 82:e5–7. doi:10.1016/j.diabres.2008.06.019
Jenkins AJ et al. (2007) Increased serum pigment epithelium-derived factor is associated with microvascular complications, vascular stiffness and inflammation in Type 1 diabetes. Diabet Med. 24:1345–51. doi:10.1111/j.1464-5491.2007.02281.x
Katakami N, Kaneto H, Yamasaki Y, Matsuhisa M (2008) Increased serum pigment epithelium-derived factor levels in type 1 diabetic patients with diabetic retinopathy. Diabetes Res Clin Pract. 81:e4–7. doi:10.1016/j.diabres.2008.03.009
Leiter EH (2001) The NOD mouse: a model for insulin-dependent diabetes mellitus. Curr Protoc Immunol. Chapter 15:Unit 15.9. doi:10.1002/0471142735.im1509s24
Van Belle TL, von Herrath MG (2009) Mouse Models of Type1 Diabetes. Drug Discov Today Dis Model. 6:41–45. doi:10.1016/j.ddmod.2009.03.008. Mouse
Szkudelski T (2001) The mechanism of alloxan and streptozotocin action in B cells of the rat pancreas. Physiol Res. 50:537–546.
Tombran-Tink J, Barnstable CJ (2003) PEDF: a multifaceted neurotrophic factor. Nat Rev Neurosci. Nature 4:628–36. doi:10.1038/nrn1176
Gattu AK et al. (2012) Insulin resistance is associated with elevated serum pigment epithelium-derived factor (PEDF) levels in morbidly obese patients. Acta Diabetol. 49 Suppl 1:S161–9. doi:10.1007/s00592-012-0397-y
Jenkins AJ et al. (2014) Clinical correlates of serum pigment epithelium-derived factor in type 2 diabetes patients. J Diabetes Complications 28:353–9. doi:10.1016/j.jdiacomp.2014.01.008
Tryggestad JB, Wang JJ, Zhang SX, Thompson DM, Short KR (2014) Elevated plasma pigment epithelium-derived factor in children with type 2 diabetes mellitus is attributable to obesity. Pediatr Diabetes. 1–6. doi:10.1111/pedi.12226
Schmitz JC et al. (2011) Pigment epithelium-derived factor regulates early pancreatic fibrotic responses and suppresses the profibrotic cytokine thrombospondin-1. Am. J. Pathol. 179:2990–9. doi:10.1016/j.ajpath.2011.08.009
Lenzen S (2008) The mechanisms of alloxan- and streptozotocin-induced diabetes. Diabetologia 51:216–226. doi:10.1007/s00125-007-0886-7
Zhou Y et al. (2013) PEDF expression is inhibited by insulin treatment in adipose tissue via suppressing 11β-HSD1. PLoS One 8:e84016. doi:10.1371/journal.pone.0084016
Leonard M, Ryan MP, Watson AJ, Schramek H, Healy E (1999) Role of MAP kinase pathways in mediating IL-6 production in human primary mesangial and proximal tubular cells. Kidney Int. 56:1366–77. doi:10.1046/j.1523-1755.1999.00664.x
Feng WG, Wang YB, Zhang JS, Wang XY, Li CL, Chang ZL (2002) cAMP elevators inhibit LPS-induced IL-12 p40 expression by interfering with phosphorylation of p38 MAPK in murine peritoneal macrophages. Cell Res. 12:331–7. doi:10.1038/sj.cr.7290135
Schnyder-Candrian S et al. (2005) Dual Effects of p38 MAPK on TNF-Dependent Bronchoconstriction and TNF-Independent Neutrophil Recruitment in Lipopolysaccha-ride-Induced Acute Respiratory Distress Syndrome. J. Immunol. 175:262–269. doi:10.4049/jimmunol.175.1.262
Kim YM, Talanian R V, Li J, Billiar TR (1998) Nitric oxide prevents IL-1beta and IFN-gamma-inducing factor (IL-18) release from macrophages by inhibiting caspase-1 (IL-1beta-converting enzyme). J. Immunol. 161:4122–4128. Available: http://www.ncbi.nlm.nih.gov/pubmed/9780184
Ghayur T et al. (1997) Caspase-1 processes IFN-gamma-inducing factor and regulates LPS-induced IFN-gamma production. Nature 386:619–23. doi:10.1038/386619a0
Akinboye ES, Bakare O (2011) Biological Activities of Emetine 8–15.
Cushny AR (1918) A Textbook of pharmacology and therapeutics, or, the Action of drugs in health and disease Am. ed [Internet]. Lea & Febinger. Available: http://books.google.com/books?id=gjGrgW-J9q1oC&pgis=1
Raeburn JA (1914) SUBCUTANEOUS INJECTIONS OF EMETINE IN PULMONARY TUBERCULOSIS. Br Med J. 1:703–704. doi:10.1136/bmj.1.2778.703
Freireich EJ, Gehan EA, Rall DP, Schmidt LH, Skipper HE (1966) Quantitative comparison of toxicity of anticancer agents in mouse, rat, hamster, dog, monkey, and man. Cancer Chemother Rep. 50:219–244. Available: http://www.ncbi.nlm.nih.gov/pubmed/4957125
Barceloux DG (2012) Medical Toxicology of Drug Abuse: Synthesized Chemicals and Psychoactive Plants [Internet]. John Wiley & Sons. Available: https://books.google.com/books?id=OWFiVaDZnkQC&pgis=1
Skyler JS et al. (2005) Effects of oral insulin in relatives of patients with type 1 diabetes: The Diabetes Prevention Trial—Type 1. [Internet]. Diabetes care. doi:10.2337/diacare.28.5.1068
Gale EAM, Bingley PJ, Emmett CL, Collier T (2004) European Nicotinamide Diabetes Intervention Trial (ENDIT): a randomised controlled trial of intervention before the onset of type 1 diabetes. Lancet 363:925–31. doi:10.1016/S0140-6736(04)15786-3
Acknowledgments
We thank Dee Prieto for expert administrative assistance; Yanexy Portal and the Center for Comparative Physiology at for animal care and expert technical assistance; Dr. Amanda Chan, PhD, from the Microscopy Facility for expert microscopy assistance; and Dr. Barbara Sherry, PhD, and Head of the Center for Immunology & Inflammation for critically reading the manuscript. This work was supported by a grant from the Juvenile Diabetes Research Fund.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, and provide a link to the Creative Commons license. You do not have permission under this license to share adapted material derived from this article or parts of it.
The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder.
To view a copy of this license, visit (http://creativecommons.org/licenses/by-nc-nd/4.0/)
About this article
Cite this article
Hudson, L.K., Dancho, M.E., Li, J. et al. Emetine Di-HCl Attenuates Type 1 Diabetes Mellitus in Mice. Mol Med 22, 585–596 (2016). https://doi.org/10.2119/molmed.2016.00082
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.2119/molmed.2016.00082