Abstract
Host defense peptides are effector molecules of the innate immune system. They show broad antimicrobial action against gram-positive and -negative bacteria, and they likely play a key role in activating and mediating the innate as well as adaptive immune response in infection and inflammation. These features make them of high interest for wound healing research. Non-healing and infected wounds are a major problem in patient care and health care spending. Increasing infection rates, growing bacterial resistance to common antibiotics, and the lack of effective therapeutic options for the treatment of problematic wounds emphasize the need for new approaches in therapy and pathophysiologic understanding. This review focuses on the current knowledge of host defense peptides affecting wound healing and infection. We discuss the current data and highlight the potential future developments in this field of research.
Similar content being viewed by others
Introduction
Skin and soft tissue infections account for 7% to 10% of hospitalizations and represent one of the most common indications for the use of antimicrobial therapy in the United States (1). Wound infections and sepsis are an increasing cause of death in severely ill patients (2), and the treatment of chronic and complex wounds puts a significant burden on the health care system and on the economy as a whole (3). The progressive decline of therapeutic efficacies of available antibiotics due to antimicrobial resistance and the limited therapeutic approaches in wound healing emphasize the urgency for further pathophysiological insights and the development of new classes of drugs for the treatment of soft tissue and skin infections (4,5).
The human skin is constitutively colonized with various microorganisms. The epidermal and dermal layers present an important physical barrier against invading mircroorganisms; disruption of this barrier allows pathogens to invade the body and drastically increases the risk of infection and mortality of severely ill patients (2,6). As an immune reaction, the skin is able to activate the innate immune response (7–9), in which host defense peptides work on the effector side of the immune response of the human host (10,11). Host defense peptides (HDPs) are peptide molecules <100 amino acids, coded by an individual gene (12). They have been identified in all kinds of species, including plants, insects, animals, and humans (13). The total number of known HDPs is increasing every year, with >900 HDPs listed in three databases to date (14–16).
Host defense peptides, also known as antimicrobial peptides (AP), play an important role in the innate immune system as antimicrobial and immunomodulating agents and present an important link between the innate and adaptive immune response (17,18). Owing to their multiple functions, they are considered promising agents for new therapeutic approaches in infectious diseases and wound healing (19–21).
Host Defense (Antimicrobial) Peptides
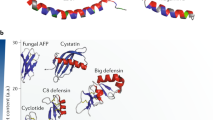
According to their molecular composition, size, conformational structure, or predominant amino acid structure, host defense peptides can be divided into four main classes: linear α-helical structure, β-sheet structure stabilized by characteristic disulfide bridges, peptides with predominance of one or more amino acids, and loop-structured peptides (Table 1) (22–25). In humans, two main classes of host defense peptides have been identified: cathelicidins and defensins. Cathelicidins were first described in 1995 to classify peptides containing both a cathelin and a c-terminal antimicrobial peptide domain expressed in mammalian myeloid cells (26,27). The molecular structure of cathelicidins is a bipartite molecule, characterized by a stable N-terminal cathelin domain and an antimicrobial C-terminal domain (28). To date, hCAP18/LL-37 is the only human cathelicidin described. The cathelicidin family has great variance but only the hCAP-18, with a cathelicidin gene on chromosome 3, can be produced as a propeptide. It is stored as a precursor in human neutrophil granules (29) and various cells and tissues such as T cells, monocytes, lymphocytes, natural killer (NK) cells, B cells, and mast cells. The epithelia of the airways, mouth, tongue, esophagus, intestine, cervix, vagina, salivary glands, epididymis, and testis have been shown to express LL-37 (30,31). Furthermore, LL-37 is secreted in human wound, sweat, and airway surface fluids (28,32–36) and is upregulated in response to cutaneous infection or injury (36,37). Its C-terminal antimicrobial domain, LL-37, can be liberated by proteinase 3 after degranulation and secretion (27,38).
Cathelicidin has broad activity against bacterial, viral, and fungal pathogens (39,40). Inflammation or injury seems to be the trigger for upregulation of the LL-37/hCAP-18 gene, particularly in keratinocytes and leukocytes (27,41). An indirect immune-modulating effect of LL-37/hCAP-18 is its chemotactic effect in the peripheral blood flow on monocytes, neutrophils, and CD4− cells (30,42,43). In an animal model, a mast cell degranulation effect by LL-37 (43) and a chemoattractant effect of neutrophils with the initiation of a specific immune response by phagocytosis of opsonized bacteria (44) have been shown. LL-37 shows the direct binding of lipopolysaccharide (LPS) and the inhibition of LPS-induced cell responses like release of tumor necrosis factor (TNF)-α, nitric oxide, and tissue factor (45–47).
One of the best-characterized families of host defense peptides in vertebrates are defensins, which represent the second important class of HDPs in humans (48). Defensins are small, cationic cystine-rich peptides with a characteristic molecular β-sheet structure, including three disulfide bridges with an amphiphilic charge distribution (49,50). Defensins are subclassified into α-defensins, also called human neutrophil peptides (HNPs), and β-defensins (hBD). Their molecular configuration enables defensins to interact with cell membranes of target cells and disrupt them (51). It ensures broad antimicrobial activity that functions by forming channels in the target membrane, leading to cell lysis and consecutive cell death (17,52–54).
The human α-defensin was isolated from myeloid-derived cells like neutrophils and macrophages (55). Five different human α-defensin genes and six different human α-defensin molecules are called HNP-1 to -6 (56–59). HNP-1 to -4 are localized in azurophilic granules of neutrophil granulocytes, where they contribute to the oxygen-independent killing of phagocytosed microorganisms (55,60). HNP-5 and -6 are enteric defensins, first discovered in Paneth cells. As immune modulators, HNP-1, -2, and -3 upregulate TNF-α and interleukin (IL)-1 in human monocytes that have been activated by bacteria (61,62). Furthermore, HNP-1 and -2 have the ability to directly kill gram-negative and -positive bacteria (48), Candida albicans (63), and enveloped viruses such as members of the herpes family (64,65). HNP-5 has concentration-dependent microbicidal activity against Escherichia coli, Listeria monocytogenes, Salmonella typhimurium, and C. albicans (66).
The human β-defensin (hBD-1) was identified and purified in 1995 from blood plasma of patients with renal disease (67). HBD-1 is constitutively expressed in different tissues with primary expression in the epithelial lining of the respiratory and urinary tracts (7,68–72). Different studies have shown that hBD-1 expression can be upregulated by LPS, heat-inactivated Pseudomonas aeruginosa, and interferon (IFN)-γ (73–78). In contrast to many other antimicrobial peptides in cutaneous wounds, hBD-1 does not seem to be involved in a specific manner. However, it shows special activity against gram-negative bacterial strains like E. coli and P. aeruginosa (71).
The initial isolation of human β-defensin-2 (hBD-2) occurred in 1997 from psoriatic skin lesions (79). The most prevalent expression of hBD-2 is observed in keratinocytes, the gastrointestinal tract, and the respiratory tract (80,81). Stored in lamellar bodies of keratinocytes (82), hBD-2 can be upregulated directly by bacterial pathogens (62,83) or inflammatory cells like monocyte-derived, macrophage-derived (73,84–86), and lymphocyte-derived (76,87) cells. Several mechanisms and signaling pathways are involved in the expression of hBD-2. Detection of bacterial LPS by CD14 and Toll-like receptor 2 and subsequent activation of the NF-κB cascade induces human β-defensin 2 (88,89). Furthermore, human Toll-like receptor 2 mediates induction of the antimicrobial peptide hBD-2 in response to bacterial lipoprotein (88,90,91). HBD-2 signaling pathways involve NF-κB (89) and mitogen-activated protein kinase (92), including Src-dependent Raf-MEK1/2-ERK (93). The promoter of hBD-2 has binding sites for NF-κB and putative binding sequences for AP-1, NF-IL6, and STATs (85,89,91). After upregulation, hBD-2 shows immune-stimulating properties by chemoattracting immature dendritic cells and T cells to modify the adaptive immune reaction (94).
As an inducible HDP, hBD-2 seems to be involved in wound repair by activating the intrinsic immunity after destruction of epidermal skin layers and inflammation (95). Mediators upregulating hBD-2 in epithelial tissue are proinflammatory cytokines like IL-1 (84), IL-22 (96), bacterial LPS (97), and direct bacterial contact with epithelial cells (79,98,99). After activation, hBD-2 shows direct activity against P. aeruginosa, E. coli, and C. albicans (100). Furthermore, hBD-2 shows a synergistic effect with LL-37 in increased activity against S. aureus (101). In the setting of chronic skin disorders, Ong et al. (101) showed a continuous upregulation of hBD-2 in psoriatic skin scale with a low susceptibility for skin infections.
In burn wounds, decreased hBD-2 activity was shown, indicating that innate immune defects contribute to the risk of burn wound infection and sepsis (102).
The human β-defensin-3 (hBD-3) was originally discovered from psoriatic skin lesions and isolated nearly simultaneously from two groups in 2001 (103, 104). HBD-3 was further detected in many other tissues such as heart, liver, fetal thymus, and placenta cells (103, 105,106). In skin, hBD-3 is stored like hBD-2 in lamellar bodies of keratinocytes (107). TNF-α, transforming growth factor (TGF)-α, insulin-like growth factor 1 (IGF-1), Toll-like receptor 5, IL-1β, IFN-γ, TGF-α, and IGF-1 as well as various bacteria play an important role in activation of the synthesis of hBD-3 (103,108).
After testing a large number of bacterial strains, the broad bactericidal activity of hBD-3 against gram-positive and -negative bacteria was reported, including multidrug-resistant strains of S. aureus and P. aeruginosa (109,110).
Human β-defensin-4 is primarily expressed in testis and epididymis (111) and inducible in primary keratinocytes (112). These data are based on detection of mRNA, and a partial characterization of this defensin relies on recombinant preparation by Garcia et al. (111). The activation of hBD-4 seems similar to that of hBD-2 and hBD-3 (112).
Human β-defensins promote histamine release and prostaglandin-2 production in mast cells (43,113), connect the innate and adaptive immune system by chemoattraction of immature dendritic cells and T cells (94), and increase the expression of TNF-α and IL-1 in human monocytes following activation by bacterial stimulus (61).
Host defense peptides in human skin are primarily produced by keratinocytes, eccrin glands, and neutrophile granulocytes (114). Constitutively produced HDPs of the human skin are dermicidin (115), protease inhibitor antileucoprotease (ALP) (116,117), RNAse 7 (118), psoriasin (119), lysozyme (120), β-defensin-1, (69) and secretory phospholipase A2 (121). Inducible HDPs of the human skin are cathelicidin LL-37 (35) produced in keratinocytes, α-defensins (HNP 1–4, human neutrophil peptide) produced by neutrophils (55,122), and β-defensins-2 and -3 (79,103,104).
Properties of Host Defense Peptides
Host defense peptides show great variance of effects and interactions. One major function of HDPs is to inactivate microbes, including bacteria, fungi, parasites, and viruses, through multiple direct effects on their membranes (9,23,36,123) (Table 1).
HDPs have the ability to attack specific external targets simultaneously, such as the cytoplasmic membrane of bacteria, by building perturbing peptides and attacking internal targets by invading the barrier of the bacterial cell wall and permitting passage of various molecules into the cell (23,124).
Another major function is their active role in the transition to the adaptive immune response by being chemotactic for human monocytes, neutrophils, and T cells and by exhibiting adjuvant and polarizing effects in influencing dendritic cell development (125).
Ahigh endotoxin-neutralization capacity after bacterial infections slows down the acute immune reaction and prevents septic shock in severely ill patients (17,23,126–128); host defense peptides have a direct influence on the adaptive immune responses by activation of different immune factors such as TNF-α, IL-1, and IFN-γ without employing the NF-κB pathway (129–131).
Host Defense Peptides in Wounds
Host defense peptides, synthesized in the skin at sites of potential microbial entry, provide a soluble barrier that acts as an impediment to infection (62). If the skin is intact, bacterial growth will be controlled by bacteriostatic and bactericidal compounds such as psoriasin and RNAse 7 (6). However, in injury and infection of the skin, expression of host defense peptides will be upregulated owing to increased synthesis by keratinocytes and deposition from degranulation of recruited neutrophils. Constitutive and inducible expression of human cathelicidin (hCAP18/LL-37), as well as hBD-2 and -3, have been observed in epidermal keratinocytes (36,41,104).
In a wound, IGF-1 and TGF-α are stimulators for the human cathelicidin hCAP18/LL-37 to a comparable level as the proinflammatory cytokine IL-1 (36,132). Both play important roles in wound healing by activating epidermal cells and fibroblasts to form granulation tissue, mediate angiogenesis, and chemoattract macrophages and fibroblasts (133–135). In a feedback mechanism, cathelicidin from activated leukocytes in pigs (PR-39) has shown a direct influence on dermal fibroblasts by increasing synthesis of the extracellular matrix proteoglycans, syndecan-1 and -4 (136), which are required for the activity of many growth factors (137–140). In an animal model, syndecan production was delayed and ineffective wound repair (141,142) was reported.
Heilborn et al. (143) described a receptor K67-dependent, continuous increase of LL-37 produced by keratinocytes and granulocytes (36), with a peak maximum after 48 h and high expression in the wound fluid and wound tissue of healing skin. Expression decreased after wound closure, and a lack of LL-37 in chronic wounds was reported (143). Different authors have shown a protective function of LL-37 from invasive bacterial skin infections, particularly against P. aeruginosa, S. aureus, and group A Streptococcus (36,101,144,145). Comparing wild-type mice with Cnlp-deficient mice (targeted deletion of the cathelicidin gene), a prolonged period of wound healing and an increase in bacterial colonization for Cnlp-deficient mice was reported (145). These findings were confirmed by Nizet et al. (144), who reported a better outcome for wild-type mice versus Cnlp-deficient mice after challenge with necrotic skin infections of Group A Streptococcus.
Ong et al. (101) showed better immune response against S. aureus in patients with psoriasis caused by a higher LL-37 expression level, whereas patients suffering from topical dermatitis showed decreased expression (146). These findings may provide an explanation for the susceptibility of patients suffering from atopic dermatitis to skin infection compared with patients with psoriasis (147).
We demonstrated a bactericidal effect of LL-37 in a rat animal model following transient adenoviral gene therapy to P. aeruginosa-infected burn wounds (148).
LL-37 has a direct effect on wound healing by promoting neovascularization and angiogenesis. Koczulla et al. (149) showed the impact of LL-37 to angiogenesis in a chorionallantoic membrane assay and by a revascularization model in an animal after hind-limb ischemia. The authors found a direct effect of LL-37 by activating vessel growth in cultivated epithelial cells, and after injection of LL-37 in the ischemic limb of a rabbit, they noted increased blood supply. They found direct participation of the formyl peptide receptor like 1 (FPRL1) in activation of hCAP-18 and following neovascularization (149). We confirmed the angiogenetic effect of LL-37 in a skinfold chamber model in mice (150).
Another study analyzed visualization and localization of the cathelicidin LL-37, neutrophil defensin α (human neutrophil peptide), and human β-defensin-1, -2, and -3 in normal and burned skin and determined the cell types in which these host defense peptides were localized using fluorescence microscopy. The authors showed that in normal skin, human β-defensin-1 was localized to the perinuclear region of keratinocytes and human β-defensin-2 was primarily localized to the stratum germinativum; human β-defensin-3 was detected in the stratum spinosum, whereas human α-defensins (HNPs) were randomly distributed in the papillary dermis. The cathelicidin LL-37 was concentrated in the stratum corneum and along ducts.
In burned skin, human β-defensin-1 was expressed in dermal glands, including hair shafts; human β-defensin-2 and -3 were found in the remaining keratin layers and glands of the lower dermis; human neutrophil peptides were localized to hair shafts and in residual keratin layers. Interestingly, LL-37 was detected in very high concentrations in the epithelium of sweat ducts. The authors concluded that the cells in the lower dermal and subdermal regions of burned skin produce host defense peptides after burn injury to maintain a barrier against infection (151,152).
HNPs promote wound healing. Oono et al. (153) showed that synthetic HNP-1 increases the expression of pro-collagen mRNA and protein in dermal fibroblast cultures. In contrast, the expression of matrix-metalloproteinase-1 was decreased. The authors suggest that HNP-1 may promote wound repair by enhancing extracellular matrix deposition (153). Another study showed mitogenic activity of HNPs in epithelial and fibroblast cell lines in vitro (154).
For β-defensins, Supp et al. (155) showed expression of the β-defensin-1, -2, and -3 in keratinocyte cultures and split skin grafts from healthy and burned donors. Later studies reported that β -defensins stimulate migration and proliferation of epidermal keratinocytes and thus might promote cutaneous wound healing (156). In chronic and acute wounds, β-defensin-2 seems to be upregulated, whereas it is not detectable in healthy skin (157).
Expression of human β-defensin-3 in keratinocytes is induced by skin infection with S. aureus via Toll-like receptor 2 and epidermal growth factor receptor (EGFR) (76,158), and Kisich et al. (159) demonstrated that the capacity of human keratinocytes to fight bacterial infections (S. aureus) depends on its β-defensin-3 expression. We have demonstrated that gene transfer of human β-defensin-3 to infected diabetic porcine wounds enhances wound closure by 25% (unpublished data).
In a rat burn model, we showed that the host defense peptide histone 1.2 is effective against P. aeruginosa wound infection, with a threefold reduction in bacterial burden (160). In a recent published study, we analyzed host defense peptide expression in burned skin in humans. In this study, we showed that concentrations of LL-37 and human β-defensin-1, -2, and -3 change significantly in burntraumatized skin. Whereas human β-defensin-1 showed only a moderately lower expression in burn wounds compared with healthy tissue, hBD-2 expression changed drastically: burn wound tissue showed an upregulation of 380fold compared with controls. hBD-3 showed a 10-fold increase in mRNA expression.
Tissue sections taken from the center of burn wounds showed no direct changes in LL-37 expression compared with comparable sections from unburned patients. However, it became evident that in the edges of burn wounds a 10-fold reduction in LL-37 expression occurs. This might be due to the presence of more viable, traumatized cells, whereas in the center, cells are already dead (161). These combined data show that host defense peptides play a major role in wound healing and wound infection. In contrast to clinically used antibiotics, HDPs have interesting features for topical application to treat wound infection and promote healing. However, there are few data investigating their role in wounds in detail. Thus, more experimental and clinical studies are needed to gain further insights into this important field of research.
From Bench to Bedside
Despite the seemingly successful application of host defense peptides in in vitro experiments and animal models, cytotoxicity could be a serious limitation to clinical studies. We demonstrated that application of the host defense peptide protegrin-1, a mammalian HDP, led to increased bacterial reduction but decreased survival in a sepsis model in mice. These data indicate that protegrin-1 induces extensive endotoxin release and thus elicits large alterations in host innate immune response (20). Another study showed that neonatal rats that developed LPS-induced sepsis died within 5-8 h when more than 300 µg/kg LL-37 was applied (162). However, mortality was significantly reduced in groups that received lower doses of LL-37 (162). In fact, LL-37 has shown nonselective cell toxicity and hemolytic activity (163) and causes DNA fragmentation in cell cultures (164). Recently, we detected high cytotoxicity of human β-defensin-3 after gene transfer to primary keratinocyte cell cultures (unpublished data). Many other host defense peptides were shown to be cytotoxic (165).
These setbacks led to increased efforts to develop novel synthetic host defense peptides with less cytotoxic effects and improved antimicrobial activity. We demonstrated that the designer peptide proline-novispirin G10 possesses low hemolytic and cytotoxic activities combined with broad-spectrum microbicidal activities against gram-positive and -negative bacteria in vitro. These findings were confirmed in a large animal wound healing model against S. aureus (166) and in a P. aeruginosa-infected rat burn model (21).
Ciornei et al. (167) presented a modified truncated LL-37 peptide. Although LPS binding and neutralization was not affected and concentration-dependent chemotactic activity was similar, it caused significantly less hemolysis than the native LL-37 (167). Another study described an active domain of LL-37, and demonstrated the possibility to use shorter and less-toxic variants of LL-37 with retained or improved antimicrobial and endotoxin-neutralizing activities (168). Another strategy was reported by Braunstein et al. (169) in which D-amino acids substituted several of the L-amino acids in host defense peptides, thus markedly reducing toxicity in mice (170).
Bacterial resistance to conventional antibiotics is a major concern and the main reason for extensive, ongoing research to develop new therapeutics. Microorganisms have also developed ways to escape direct killing by human host defense peptides (171–174), which emphasizes their important and ancient role in the innate immune system (172). However, resistance mechanisms are generally related to the direct killing of bacteria and are not comparable to the resistance mechanisms of conventional antibiotics. Furthermore, the potent immunomodulatory functions are not hampered.
A promising aspect in improving antimicrobial therapy is the combination of common therapeutic antibiotics with host defense peptides. The application of the host defense peptide temporin L combined with β-lactams in a murine model of gram-negative sepsis led to the lowest plasma endotoxin and TNF-α levels measured in the study, the highest antimicrobial activities, and the highest survival rates (175).
In rat models, β-lactams even increased plasma endotoxin and TNF-α levels, whereas the combination with cecropin B proved to be the most effective treatment affecting survival rates, antimicrobial activity, and reduction in plasma endotoxin and TNF-α levels (176). Cirioni et al. (177) tested the efficacy of a combination of two α-helical antimicrobial peptides (cecropin Aand maigainin II) and vancomycin against S. aureus with intermediate resistance to glycopeptides in a murine sepsis model. The authors demonstrated that the combination showed low lethality rates (5%–15%), low bacterial blood counts, and the strongest reduction in TNF-α and IL-6 in the plasma (177). Host defense peptides seem to be impaired by bacteriostatic antibiotics. If the growth of E. coli and S. aureus is suppressed by chloramphenicol and erythromycin, the susceptibility of bacteria to cathelicidin antimicrobial peptides is markedly diminished (178). These findings indicate the importance and relevance of the development of new therapeutic strategies, including host defense peptides, in the treatment of wound infections.
To gain a better understanding of the role of host defense peptides, it is crucial to determine their kinetics in systemic and local infection and inflammation. In general, only a few clinical studies deal with host defense peptides to date (179); however, four host defense peptides were successful in therapeutic clinical trials (180).
Children suffering from meningococcal sepsis were treated with the designer host defense peptide rBPI21 (Neuprex, derived from bactericidal/permeability-increasing protein [BPI]), a human host defense protein synthesized by polymorphonuclear leukocytes (181). The investigators reported significantly reduced morbidity and improved functional outcome; however, there was no significant benefit in mortality (182). Currently, there is an ongoing clinical trial investigating therapeutic effects of rBPI21 in burn patients. Other studies investigated the treatment of diabetic foot ulcers and impetigo with the modified host defense peptide MSI-78. The bovine indolicin-derived Migenix MX-226 has already proceeded to a phase 3b study for the treatment and prevention of catheter-associated infections (179,180, 183). Promising candidates for the treatment of acne are the designer peptides XOMA 629 and MBI 594AN with bactericidal effects against Propionibacterium acnes (184). This agent is expected to be available for clinical therapy in the near future.
To date, no clinical trial for the treatment of wounds using host defense peptides is published. Other ongoing trials are promising, however, and clinical studies using host defense peptides for the treatment of impaired and infected wounds are expected in the near future.
Conclusion
Despite the loss of epidermal barrier function and subsequent exposure to environmental microorganisms, superficial epidermal wounds in vertebrates usually heal without major complications. One reason is that the skin innate immune defense function creates a soluble antimicrobial peptide barrier. After injury, host defense peptide levels in the skin rise rapidly due to increased synthesis by keratinocytes and deposition from degranulation of recruited neutrophils. In addition to the direct antimicrobial effect, host defense peptides have emerged as important effectors in infection and inflammation by modulating the innate immune reaction and activating adaptive immunity.
The growing problem of resistance to conventional antibiotics and the need for new ones has stimulated interest in the development of antimicrobial peptides as potential therapeutic agents. The main impediments to the development of host defense peptides as systemic therapy include that many of the naturally occurring peptides (such as magainin), although active in vitro, are effective in animal models of infection only at very high doses, often at close to toxic concentrations. Most pharmaceutical research has been devoted to the development of topically applied agents, such as the magainin analog pexiganan, largely because of the relative safety of topical therapy and the uncertainty surrounding the long-term toxicology of any new class of drug administered systemically (17). The potential use of HDPs as future therapeutics depends on factors such as toxicity, stability, and immunogenicity of the substances in the host.
Protegrin-1, a member of the cathelicidin family in pigs, and novospirin G10, a modified ovospirin-1, were applied as a topical ointment, successfully reducing bacterial load and promoting healing of burn wounds in an animal model (21,185). By using the neovascularization and antibacterial effect of LL-37, we could show a high potential of LL-37 in skin reconstruction in a biopolymer assay as a future option for clinical therapy.
Beyond single-therapy regimens, there is a promising future approach: the application of new complex therapeutic regimens, such as host defense peptides combined with conventional and established antibiotic agents or the application of multiple host defense peptides. These therapies could both affect the pathogens and simultaneously activate and modulate innate and adaptive immune systems of the host.
These developments and insights in host defense peptides and are promising and may contribute significantly to the therapeutic endeavors to fight systemic and local infection and inflammation in the near future.
References
Vinh DC, Embil JM. (2005) Rapidly progressive soft tissue infections. Lancet Infect. Dis. 5:501–13.
Wilson MA. (2003) Skin and soft-tissue infections: impact of resistant gram-positive bacteria. Am. J. Surg. 186:35S–41S; discussion 42S–3S, 41S–4S.
Kalorama-Informations. (2002) Woundcare Markets, Volume I: Chronic Ulcers. Kalorama Informations, a Division of https://doi.org/Market.Research.com.
Rice LB. (2003) Do we really need new anti-infective drugs? Curr. Opin. Pharmacol. 3:459–63.
Grundmann H, Aires-de-Sousa M, Boyce J, Tiemersma E. (2006) Emergence and resurgence of meticillin-resistant Staphylococcus aureus as a public-health threat. Lancet 368:874–85.
Schroder JM, Harder J. (2006) Antimicrobial skin peptides and proteins. Cell Mol. Life Sci. 63:469–86.
Fulton C, Anderson GM, Zasloff M, Bull R, Quinn AG. (1997) Expression of natural peptide antibiotics in human skin. Lancet 350:1750–1.
Beisswenger C, Bals R. (2005) Functions of antimicrobial peptides in host defense and immunity. Curr. Protein Pept. Sci. 6:255–64.
Ganz T. (2003) Defensins: antimicrobial peptides of innate immunity. Nat. Rev. Immunol. 3:710–20.
Fearon DT, Locksley RM. (1996) The instructive role of innate immunity in the acquired immune response. Science 272:50–3.
Medzhitov R, Janeway CA Jr. (1997) Innate immunity: the virtues of a nonclonal system of recognition. Cell 91:295–8.
Bals R. (2000) Antimicrobial peptides and pep ide antibiotics [in German]. Med. Klin. (Munich) 95:496–502.
Hancock RE, Scott MG. (2000) The role of antimicrobial peptides in animal defenses. Proc. Natl. Acad. Sci. U. S. A. 97:8856–61.
Brahmachary M, et al. 2004. ANTIMIC: a database of antimicrobial sequences. Nucleic Acids Res. [Internet]. [cited 2007 Dec 20];32(database issue): D586–9. Available from: https://doi.org/nar.oxfordjournals.org/cgi/content/full/32/suppl_1/D586.
Antimicrobial Sequences Database (ASDb) [Internet]. 2004-. Trieste (Italy): Antiinfective Peptides Laboratory Tossi Group, Department of Biochemistry, Biophysics, and Macromolecular Chemistry, University of Trieste. [cited 2007 Dec 20]. Available from: https://doi.org/www.bbcm.units.it/∼tossi/amsdb.html.
Wang Z, Wang G. 2004. APD: the Antimicrobial Peptide Database. Nucleic Acids Res. [Internet]. [cited 2007 Dec 20];32(database issue):D590–2. vailable from: https://doi.org/nar.oxfordjournals.org/cgi/content/full/32/suppl_1/D590.
Zasloff M. (2002) Antimicrobial peptides of multicellular organisms. Nature 415:389–95.
Hoffmann JA, Kafatos FC, Janeway CA, Ezekowitz RA. (1999) Phylogenetic perspectives in innate immunity. Science 284:1313–8.
Hancock RE. (2001) Cationic peptides: effectors in innate immunity and novel antimicrobials. Lancet Infect. Dis. 1:156–64.
Steinstraesser L, et al. (2003) Protegrin-1 increases bacterial clearance in sepsis but decreases survival. Crit. Care Med. 31:221–6.
Steinstraesser L, et al. (2002) Activity of novispirin G10 against Pseudomonas aeruginosa in vitro and in infected burns. Antimicrob. Agents Chemother. 46:1837–44.
Andreu D, Rivas L. (1998) Animal antimicrobial peptides: an overview. Biopolymers 47:415–33.
Hancock RE. (1997) Peptide antibiotics. Lancet 349:418–22.
van’t Hof W, Veerman EC, Helmerhorst EJ, Amerongen AV. (2001) Antimicrobial peptides: properties and applicability. Biol. Chem. 382:597–619.
Koczulla AR, Bals R. (2003) Antimicrobial peptides: current status and therapeutic potential. Drugs 63:389–406.
Larrick JW, Hirata M, Balint RF, Lee J, Zhong J, Wright SC. (1995) Human CAP18: a novel antimicrobial lipopolysaccharide-binding protein. Infect. Immun. 63:1291–7.
Sorensen OE, et al. (2001) Human cathelicidin, hCAP-18, is processed to the antimicrobial peptide LL-37 by extracellular cleavage with proteinase 3. Blood 97:3951–9.
Zanetti M, Gennaro R, Romeo D. (1995) Cathelicidins: a novel protein family with a common proregion and a variable C-terminal antimicrobial domain. FEBS Lett. 374:1–5.
Ganz T, Lehrer RI. (1997) Antimicrobial peptides of leukocytes. Curr. Opin. Hematol. 4:53–8.
Agerberth B, et al. (2000) The human antimicrobial and chemotactic peptides LL-37 and alpha-defensins are expressed by specific lymphocyte and monocyte populations. Blood 96:3086–93.
Yang D, et al. (2000) LL-37, the neutrophil granule- and epithelial cell-derived cathelicidin, utilizes formyl peptide receptor-like 1 (FPRL1) as a receptor to chemoattract human peripheral blood neutrophils, monocytes, and T cells. J. Exp. Med. 192:1069–74.
Ong PY, et al. (2002) Endogenous antimicrobial peptides and skin infections in atopic dermatitis. N. Engl. J. Med. 347:1151–60.
Sorensen O, Arnljots K, Cowland JB, Bainton DF, Borregaard N. (1997) The human antibacterial cathelicidin, hCAP-18, is synthesized in myelocytes and metamyelocytes and localized to specific granules in neutrophils. 114 90:2796–803.
Gallo RL, Nizet V. (2003) Endogenous production of antimicrobial peptides in innate immunity and human disease. Curr. Allergy Asthma Rep. 3:402–9.
Gallo RL, Murakami M, Ohtake T, Zaiou M. (2002) Biology and clinical relevance of naturally occurring antimicrobial peptides. J. Allergy Clin. Immunol. 110:823–31.
Dorschner RA, et al. (2001) Cutaneous injury induces the release of cathelicidin anti-microbial peptides active against group A Streptococcus. J. Invest. Dermatol. 117:91–7.
Turner J, Cho Y, Dinh NN, Waring AJ, Lehrer RI. (1998) Activities of LL-37, a cathelin-associated antimicrobial peptide of human neutrophils. Antimicrob. Agents Chemother. 42:2206–14.
Frohm M, et al. (1996) Biochemical and antibacterial analysis of human wound and blister fluid. Eur. J. Biochem. 237:86–92.
Travis SM, et al. (2000) Bactericidal activity of mammalian cathelicidin-derived peptides. Infect. Immun. 68:2748–55.
Zanetti M, Gennaro R, Skerlavaj B, Tomasinsig L, Circo R. (2002) Cathelicidin peptides as candidates for a novel class of antimicrobials. Curr. Pharm. Des. 8:779–93.
Frohm M, et al. (1997) The expression of the gene coding for the antibacterial peptide LL-37 is induced in human keratinocytes during inflammatory disorders. J. Biol. Chem. 272:15258–63.
De Y, et al. (2000) LL-37, the neutrophil granule-and epithelial cell-derived cathelicidin, utilizes formyl peptide receptor-like 1 (FPRL1) as a receptor to chemoattract human peripheral blood neutrophils, monocytes, and T cells. J. Exp. Med. 192:1069–74.
Niyonsaba F, Someya A, Hirata M, Ogawa H, Nagaoka I. (2001) Evaluation of the effects of peptide antibiotics human beta-defensins-1/-2 and LL-37 on histamine release and prostaglandin D(2) production from mast cells. Eur. J. Immunol. 31:1066–75.
Feger F, Varadaradjalou S, Gao Z, Abraham SN, Arock M. (2002) The role of mast cells in host defense and their subversion by bacterial pathogens. Trends Immunol. 23:151–8.
Hirata M, et al. (1994) Characterization of a rabbit cationic protein (CAP18) with lipopolysaccharide-inhibitory activity. Infect. Immun. 62:1421–6.
Larrick JW, et al. (1994) A novel granulocyte-derived peptide with lipopolysaccharide-neutralizing activity. J. Immunol. 152:231–40.
Scott MG, Davidson DJ, Gold MR, Bowdish D, Hancock RE. (2002) The human antimicrobial peptide LL-37 is a multifunctional modulator of innate immune responses. J. Immunol. 169:3883–91.
Lehrer RI, Lichtenstein AK, Ganz T. (1993) Defensins: antimicrobial and cytotoxic peptides of mammalian cells. Annu. Rev. Immunol. 11:105–28.
Lehrer RI, Ganz T, Selsted ME. (1991) Defensins: endogenous antibiotic peptides of animal cells. Cell 64:229–30.
White SH, Wimley WC, Selsted ME. (1995) Structure, function, and membrane integration of defensins. Curr. Opin. Struct. Biol. 5:521–7.
Lehrer RI, Barton A, Daher KA, Harwig SS, Ganz T, Selsted ME. (1989) Interaction of human defensins with Escherichia coli: mechanism of bactericidal activity. J. Clin. Invest. 84:553–61.
Ganz T, Oren A, Lehrer RI. (1992) Defensins: microbicidal and cytotoxic peptides of mammalian host defense cells. Med. Microbiol. Immunol. (Berlin) 181:99–105.
Lehrer RI, Ganz T. (2002) Defensins of vertebrate animals. Curr. Opin. Immunol. 14:96–102.
Selsted ME, et al. (1993) Purification, primary structures, and antibacterial activities of beta-defensins, a new family of antimicrobial peptides from bovine neutrophils. J. Biol. Chem. 268:6641–8.
Ganz T, et al. (1985) Defensins: natural peptide antibiotics of human neutrophils. J. Clin. Invest. 76:1427–35.
Mallow EB, et al. (1996) Human enteric defensins. Gene structure and developmental expression. J. Biol. Chem. 271:4038–45.
Selsted ME, Harwig SS. (1989) Determination of the disulfide array in the human defensin HNP-2: a covalently cyclized peptide. J. Biol. Chem. 264:4003–7.
Skalicky JJ, Selsted ME, Pardi A. (1994) Structure and dynamics of the neutrophil defensins NP-2, NP-5, and HNP-1: NMR studies of amide hydrogen exchange kinetics. Proteins 20:52–67.
Wilde CG, Griffith JE, Marra MN, Snable JL, Scott RW. (1989) Purification and characterization of human neutrophil peptide 4, a novel member of the defensin family. J. Biol. Chem. 264:11200–3.
Selsted ME, Harwig SS, Ganz T, Schilling JW, Lehrer RI. (1985) Primary structures of three human neutrophil defensins. J. Clin. Invest. 76:1436–9.
Chaly YV, Paleolog EM, Kolesnikova TS, Tikhonov, II, Petratchenko EV, Voitenok NN. (2000) Neutrophil alpha-defensin human neutrophil peptide modulates cytokine production in human monocytes and adhesion molecule expression in endothelial cells. Eur. Cytokine Netw. 11:257–66.
Braff MH, Bardan A, Nizet V, Gallo RL. (2005) Cutaneous defense mechanisms by antimicrobial peptides. J. Invest. Dermatol. 125:9–13.
Lehrer RI, Ganz T, Szklarek D, Selsted ME. (1988) Modulation of the in vitro candidacidal activity of human neutrophil defensins by target cell metabolism and divalent cations. J. Clin. Invest. 81:1829–35.
Schroder JM, Harder J. (1999) Human beta-defensin-2. Int. J. Biochem. Cell Biol. 31:645–51.
Daher KA, Selsted ME, Lehrer RI. (1986) Direct inactivation of viruses by human granulocyte defensins. J. Virol. 60:1068–74.
Porter EM, van Dam E, Valore EV, Ganz T. (1997) Broad-spectrum antimicrobial activity of human intestinal defensin 5. Infect. Immun. 65:2396–401.
Bensch KW, Raida M, Magert HJ, Schulz-Knappe P, Forssmann WG. (1995) hBD-1: a novel beta-defensin from human plasma. FEBS Lett. 368:331–5.
Ali RS, Falconer A, Ikram M, Bissett CE, Cerio R, Quinn AG. (2001) Expression of the peptide antibiotics human beta defensin-1 and human beta defensin-2 in normal human skin. J. Invest. Dermatol. 117:106–11.
Zhao C, Wang I, Lehrer RI. (1996) Widespread expression of beta-defensin hBD-1 in human secretory glands and epithelial cells. FEBS Lett. 396:319–22.
Mathews M, et al. (1999) Production of beta-defensin antimicrobial peptides by the oral mucosa and salivary glands. Infect. Immun. 67:2740–5.
Goldman MJ, Anderson GM, Stolzenberg ED, Kari UP, Zasloff M, Wilson JM. (1997) Human beta-defensin-1 is a salt-sensitive antibiotic in lung that is inactivated in cystic fibrosis. Cell 88:553–60.
Valore EV, Park CH, Quayle AJ, Wiles KR, McCray PB Jr, Ganz T. (1998) Human beta-defensin-1: an antimicrobial peptide of urogenital tissues. J. Clin. Invest. 101:1633–42.
Duits LA, Ravensbergen B, Rademaker M, Hiemstra PS, Nibbering PH. (2002) Expression of beta-defensin 1 and 2 mRNA by human monocytes, macrophages and dendritic cells. Immunology 106:517–25.
Feng Z, Jiang B, Chandra J, Ghannoum M, Nelson S, Weinberg A. (2005) Human beta-defensins: differential activity against candidal species and regulation by Candida albicans. J. Dent. Res. 84:445–50.
Joly S, Organ CC, Johnson GK, McCray PB Jr, Guthmiller JM. (2005) Correlation between beta-defensin expression and induction profiles in gingival keratinocytes. Mol. Immunol. 42:1073–84.
Sorensen OE, Thapa DR, Rosenthal A, Liu L, Roberts AA, Ganz T. (2005) Differential regulation of beta-defensin expression in human skin by microbial stimuli. J. Immunol. 174:4870–9.
Hiratsuka T, et al. (2003) Increased concentrations of human beta-defensins in plasma and bronchoalveolar lavage fluid of patients with diffuse panbronchiolitis. Thorax 58:425–30.
Zhu BD, Feng Y, Huang N, Wu Q, Wang BY. (2003) Mycobacterium bovis bacille Calmette-Guerin (BCG) enhances human beta-defensin-1 gene transcription in human pulmonary gland epithelial cells. Acta Pharmacol. Sin. 24:907–12.
Harder J, Bartels J, Christophers E, Schroder JM. (1997) Apeptide antibiotic from human skin. Nature 387:861.
O’Neil DA, et al. (1999) Expression and regulation of the human beta-defensins hBD-1 and hBD-2 in intestinal epithelium. J. Immunol. 163:6718–24.
Bals R, et al. (1998) Human beta-defensin 2 is a salt-sensitive peptide antibiotic expressed in human lung. J. Clin. Invest. 102:874–80.
Oren A, Ganz T, Liu L, Meerloo T. (2003) In human epidermis, beta-defensin 2 is packaged in lamellar bodies. Exp. Mol. Pathol. 74:180–2.
Liu AY, et al. (2002) Human beta-defensin-2 production in keratinocytes is regulated by interleukin-1, bacteria, and the state of differentiation. J. Invest. Dermatol. 118:275–81.
Liu L, Roberts AA, Ganz T. (2003) By IL-1 signaling, monocyte-derived cells dramatically enhance the epidermal antimicrobial response to lipopolysaccharide. J. Immunol. 170:575–80.
Tsutsumi-Ishii Y, Nagaoka I. (2003) Modulation of human beta-defensin-2 transcription in pulmonary epithelial cells by lipopolysaccharide-stimulated mononuclear phagocytes via proinflammatory cytokine production. J. Immunol. 170:4226–36.
Fang XM, et al. (2003) Differential expression of alpha- and beta-defensins in human peripheral blood. Eur. J. Clin. Invest. 33:82–7.
Selsted ME, Ouellette AJ. (2005) Mammalian defensins in the antimicrobial immune response. Nat. Immunol. 6:551–7.
Birchler T, et al. (2001) Human Toll-like receptor 2 mediates induction of the antimicrobial peptide human beta-defensin 2 in response to bacterial lipoprotein. Eur. J. Immunol. 31:3131–7.
Tsutsumi-Ishii Y, Nagaoka I. (2002) NF-kappa B-mediated transcriptional regulation of human beta-defensin-2 gene following lipopolysaccharide stimulation. J. Leukoc. Biol. 71:154–62.
Hertz CJ, et al. (2003) Activation of Toll-like receptor 2 on human tracheobronchial epithelial cells induces the antimicrobial peptide human beta defensin-2. J. Immunol. 171:6820–6.
Wang X, Zhang Z, Louboutin JP, Moser C, Weiner DJ, Wilson JM. (2003) Airway epithelia regulate expression of human beta-defensin 2 through Toll-like receptor 2. FASEB J. 17:1727–9.
Krisanaprakornkit S, Kimball JR, Dale BA. (2002) Regulation of human beta-defensin-2 in gingival epithelial cells: the involvement of mitogen-activated protein kinase pathways, but not the NF-kappaB transcription factor family. J. Immunol. 168:316–24.
Moon SK, et al. (2002) Activation of a Srcdependent Raf-MEK1/2-ERK signaling pathway is required for IL-1alpha-induced upregulation of beta-defensin 2 in human middle ear epithelial cells. Biochim. Biophys. Acta 1590:41–51.
Yang D, et al. (1999) Beta-defensins: linking innate and adaptive immunity through dendritic and T cell CCR6. Science 286:525–8.
Schmid P, Grenet O, Medina J, Chibout SD, Osborne C, Cox DA. (2001) An intrinsic antibiotic mechanism in wounds and tissue-engineered skin. J. Invest. Dermatol. 116:471–2.
Wolk K, Kunz S, Witte E, Friedrich M, Asadullah K, Sabat R. (2004) IL-22 increases the innate immunity of tissues. Immunity 21:241–54.
Kawai K, Shimura H, Minagawa M, Ito A, Tomiyama K, Ito M. (2002) Expression of functional Toll-like receptor 2 on human epidermal keratinocytes. J. Dermatol. Sci. 30:185–94.
Diamond G, Russell JP, Bevins CL. (1996) Inducible expression of an antibiotic peptide gene in lipopolysaccharide-challenged tracheal epithelial cells. Proc. Natl. Acad. Sci. U. S. A. 93:5156–60.
Harder J, et al. (2000) Mucoid Pseudomonas aeruginosa, TNF-alpha, and IL-1beta, but not IL-6, induce human beta-defensin-2 in respiratory epithelia. Am. J. Respir. Cell Mol. Biol. 22:714–21.
Singh PK, et al. (1998) Production of beta-defensins by human airway epithelia. Proc. Natl. Acad. Sci. U. S. A. 95:14961–6.
Ong PY, et al. (2002) Endogenous antimicrobial peptides and skin infections in atopic dermatitis. N. Engl. J. Med. 347:1151–60.
Milner SM, Ortega MR. (1999) Reduced antimicrobial peptide expression in human burn wounds. Burns 25:411–3.
Garcia JR, et al. (2001) Identification of a novel, multifunctional beta-defensin (human beta-defensin 3) with specific antimicrobial activity: its interaction with plasma membranes of Xenopus oocytes and the induction of macrophage chemoattraction. Cell Tissue Res. 306:257–64.
Harder J, Bartels J, Christophers E, Schroder JM. (2001) Isolation and characterization of human beta-defensin-3, a novel human inducible peptide antibiotic. J. Biol. Chem. 276:5707–13.
Dunsche A, Acil Y, Dommisch H, Siebert R, Schroder JM, Jepsen S. (2002) The novel human beta-defensin-3 is widely expressed in oral tissues. Eur. J. Oral Sci. 110:121–4.
Hattenbach LO, Gumbel H, Kippenberger S. (1998) Identification of beta-defensins in human conjunctiva. Antimicrob. Agents Chemother. 42:3332.
Sawamura D, et al. (2005) Beta defensin-3 engineered epidermis shows highly protective effect for bacterial infection. Gene Ther. 12:857–61.
Miller LS, et al. (2005) TGF-alpha regulates TLR expression and function on epidermal keratinocytes. J. Immunol. 174:6137–43.
Sahly H, et al. (2003) Burkholderia is highly resistant to human Beta-defensin 3. Antimicrob. Agents Chemother. 47:1739–41.
Maisetta G, et al. (2006) In vitro bactericidal activity of human beta-defensin 3 against multidrug-resistant nosocomial strains. Antimicrob. Agents Chemother. 50:806–9.
Garcia JR, et al. (2001) Human beta-defensin 4: a novel inducible peptide with a specific saltsensitive spectrum of antimicrobial activity. FASEB J. 15:1819–21.
Harder J, Meyer-Hoffert U, Wehkamp K, Schwichtenberg L, Schroder JM. (2004) Differential gene induction of human beta-defensins (hBD-1, -2, -3, and -4) in keratinocytes is inhibited by retinoic acid. J. Invest. Dermatol. 123:522–9.
Niyonsaba F, Iwabuchi K, Matsuda H, Ogawa H, Nagaoka I. (2002) Epithelial cell-derived human beta-defensin-2 acts as a chemotaxin for mast cells through a pertussis toxin-sensitive and phospholipase C-dependent pathway. Int. Immunol. 14:421–6.
Gallo RL, Huttner KM. (1998) Antimicrobial peptides: an emerging concept in cutaneous biology. J. Invest. Dermatol. 111:739–43.
Schittek B, et al. (2001) Dermcidin: a novel human antibiotic peptide secreted by sweat glands. Nat. Immunol. 2:1133–7.
Wiedow O, Harder J, Bartels J, Streit V, Christophers E. (1998) Antileukoprotease in human skin: an antibiotic peptide constitutively produced by keratinocytes. Biochem. Biophys. Res. Commun. 248:904–9.
Wingens M, et al. (1998) Induction of SLPI (ALP/HUSI-I) in epidermal keratinocytes. J. Invest. Dermatol. 111:996–1002.
Harder J, Schroder JM. (2002) RNase 7, a novel innate immune defense antimicrobial protein of healthy human skin. J. Biol. Chem. 277:46779–84.
Glaser R, Harder J, Lange H, Bartels J, Christophers E, Schroder JM. (2005) Antimicrobial psoriasin (S100A7) protects human skin from Escherichia coli infection. Nat. Immunol. 6:57–64.
Chen VL, France DS, Martinelli GP. (1986) De novo synthesis of lysozyme by human epidermal cells. J. Invest. Dermatol. 87:585–7.
Qu XD, Lehrer RI. (1998) Secretory phospholipase A2 is the principal bactericide for staphylococci and other gram-positive bacteria in human tears. Infect. Immun. 66:2791–7.
Ganz T. (1987) Extracellular release of antimicrobial defensins by human polymorphonuclear leukocytes. Infect. Immun. 55:568–71.
Steinstraesser L, et al. (2005) Inhibition of early steps in the lentiviral replication cycle by cathelicidin host defense peptides. Retrovirology 2:2.
Brogden KA. (2005) Antimicrobial peptides: pore formers or metabolic inhibitors in bacteria? Nat. Rev. Microbiol. 3:238–50.
Territo MC, Ganz T, Selsted ME, Lehrer R. (1989) Monocyte-chemotactic activity of defensins from human neutrophils. J. Clin. Invest. 84:2017–20.
Giacometti A, et al. (2004) Cathelicidin peptide sheep myeloid antimicrobial peptide-29 prevents endotoxin-induced mortality in rat models of septic shock. Am. J. Respir. Crit. Care Med. 169:187–94.
Gough M, Hancock RE, Kelly NM. (1996) Antiendotoxin activity of cationic peptide antimicrobial agents. Infect. Immun. 64:4922–7.
Cirioni O, et al. (2006) LL-37 protects rats against lethal sepsis caused by gram-negative bacteria. Antimicrob. Agents Chemother. 50:1672–9.
Elsbach P. (2003) What is the real role of antimicrobial polypeptides that can mediate several other inflammatory responses? J. Clin. Invest. 111:1643–5.
Ganz T. (2002) Immunology: versatile defensins. Science 298:977–9.
Niyonsaba F, Ushio H, Nagaoka I, Okumura K, Ogawa H. (2005) The human beta-defensins (-1, -2, -3, -4) and cathelicidin LL-37 induce IL-18 secretion through p38 and ERK MAPK activation in primary human keratinocytes. J. Immunol. 175:1776–84.
Sorensen OE, Cowland JB, Theilgaard-Monch K, Liu L, Ganz T, Borregaard N. (2003) Wound healing and expression of antimicrobial peptides/polypeptides in human keratinocytes, a consequence of common growth factors. J. Immunol. 170:5583–9.
Singer AJ, Clark RA. (1999) Cutaneous wound healing. N. Engl. J. Med. 341:738–46.
Gartner MH, Benson JD, Caldwell MD. (1992) Insulin-like growth factors I and II expression in the healing wound. J. Surg. Res. 52:389–94.
Rappolee DA, Mark D, Banda MJ, Werb Z. (1988) Wound macrophages express TGF-alpha and other growth factors in vivo: analysis by mRNA phenotyping. Science 241:708–12.
Chan YR, Gallo RL. (1998) PR-39, a syndecaninducing antimicrobial peptide, binds and affects p130(Cas). J. Biol. Chem. 273:28978–85.
Ho G, Broze GJ Jr, Schwartz AL. (1997) Role of heparan sulfate proteoglycans in the uptake and degradation of tissue factor pathway inhibitor-coagulation factor Xa complexes. J. Biol. Chem. 272:16838–44.
Penc SF, Pomahac B, Eriksson E, Detmar M, Gallo RL. (1999) Dermatan sulfate activates nuclear factor-kappaB and induces endothelial and circulating intercellular adhesion molecule-1. J. Clin. Invest. 103:1329–35.
Proudfoot AE, et al. (2001) The BBXB motif of RANTES is the principal site for heparin binding and controls receptor selectivity. J. Biol. Chem. 276:10620–6.
Rix DA, Douglas MS, Talbot D, Dark JH, Kirby JA. (1996) Role of glycosaminoglycans (GAGs) in regulation of the immunogenicity of human vascular endothelial cells. Clin. Exp. Immunol. 104:60–5.
Echtermeyer F, et al. (2001) Delayed wound repair and impaired angiogenesis in mice lacking syndecan-4. J. Clin. Invest. 107:R9–14.
Gallo RL. (2000) Proteoglycans and cutaneous vascular defense and repair. J. Invest. Dermatol. Symp. Proc. 5:55–60.
Heilborn JD, et al. (2003) The cathelicidin antimicrobial peptide LL-37 is involved in reepithelialization of human skin wounds and is lacking in chronic ulcer epithelium. J. Invest. Dermatol. 120:379–89.
Nizet V, et al. (2001) Innate antimicrobial peptide protects the skin from invasive bacterial infection. Nature 414:454–7.
Braff MH, Zaiou M, Fierer J, Nizet V, Gallo RL. (2005) Keratinocyte production of cathelicidin provides direct activity against bacterial skin pathogens. Infect. Immun. 73:6771–81.
Leung DY, Boguniewicz M, Howell MD, Nomura I, Hamid QA. (2004) New insights into atopic dermatitis. J. Clin. Invest. 113:651–7.
Christophers E, Henseler T. (1987) Contrasting disease patterns in psoriasis and atopic dermatitis. Arch. Dermatol. Res. 279 Suppl:S48–51.
Jacobsen F, et al. (2005) Transient cutaneous adenoviral gene therapy with human host defense peptide hCAP-18/LL-37 is effective for the treatment of burn wound infections. Gene Ther. 12:1494–502.
Koczulla R, von Degenfeld G, Kupatt C, et al. (2003) An angiogenic role for the human peptide antibiotic LL-37/hCAP-18. J. Clin. Invest. 111:1665–72.
Steinstraesser L, Ring A, Bals R, Steinau HU, Langer S. (2006) The human host defense peptide LL37/hCAP accelerates angiogenesis in PEGT/ PBT biopolymers. Ann. Plast. Surg. 56:93–8.
Poindexter BJ. (2005) Immunofluorescence deconvolution microscopy and image reconstruction of human defensins in normal and burned skin. J. Burns Wounds 4:e7.
Poindexter BJ, Bhat S, Buja LM, Bick RJ, Milner SM. (2006) Localization of antimicrobial peptides in normal and burned skin. Burns 32:402–7.
Oono T, Shirafuji Y, Huh WK, Akiyama H, Iwatsuki K. (2002) Effects of human neutrophil peptide-1 on the expression of interstitial collagenase and type I collagen in human dermal fibroblasts. Arch. Dermatol. Res. 294:185–9.
Murphy CJ, Foster BA, Mannis MJ, Selsted ME, Reid TW. (1993) Defensins are mitogenic for epithelial cells and fibroblasts. J. Cell Physiol. 155:408–13.
Supp DM, Karpinski AC, Boyce ST. (2004) Expression of human beta-defensins HBD-1, HBD-2, and HBD-3 in cultured keratinocytes and skin substitutes. Burns 30:643–8.
Niyonsaba F, et al. (2006) Antimicrobial peptides human beta-defensins stimulate epidermal keratinocyte migration, proliferation and production of proinflammatory cytokines and chemokines. J. Invest. Dermatol. 127:510–2.
Butmarc J, Yufit T, Carson P, Falanga V. (2004) Human beta-defensin-2 expression is increased in chronic wounds. Wound Repair Regen. 12:439–43.
Menzies BE, Kenoyer A. (2006) Signal transduction and nuclear responses in Staphylococcus aureus-induced expression of human beta-defensin 3 in skin keratinocytes. 74 74:6847–54.
Kisich KO, Howell MD, Boguniewicz M, Heizer HR, Watson NU, Leung DY. (2007) The constitutive capacity of human keratinocytes to kill Staphylococcus aureus is dependent on beta-defensin 3. J. Invest. Dermatol. 127:2368–80.
Jacobsen F, et al. (2005) Activity of histone H1.2 in infected burn wounds. J. Antimicrob. Chemother. 55:735–41.
Kaus A, et al. (2008) Host defence peptides in human burns. Burns. 34:32–40.
Fukumoto K, et al. (2005) Effect of antibacterial cathelicidin peptide CAP18/LL-37 on sepsis in neonatal rats. Pediatr. Surg. Int. 21:20–4.
Oren Z, Lerman JC, Gudmundsson GH, Agerberth B, Shai Y. (1999) Structure and organization of the human antimicrobial peptide LL-37 in phospholipid membranes: relevance to the molecular basis for its non-cell-selective activity. Biochem. J. 341.
Ciornei CD, Egesten A, Bodelsson M. (2003) Effects of human cathelicidin antimicrobial peptide LL-37 on lipopolysaccharide-induced nitric oxide release from rat aorta in vitro. Acta Anaesthesiol. Scand. 47:213–20.
Risso A, Zanetti M, Gennaro R. (1998) Cytotoxicity and apoptosis mediated by two peptides of innate immunity. Cell. Immunol. 189:107–15.
Jacobsen F, et al. (2007) Antimicrobial activity of the recombinant designer host defence peptide P-novispirin G10 in infected full-thickness wounds of porcine skin. J. Antimicrob. Chemother. 59:493–8.
Ciornei CD, Sigurdardottir T, Schmidtchen A, Bodelsson M. (2005) Antimicrobial and chemoattractant activity, lipopolysaccharide neutralization, cytotoxicity, and inhibition by serum of analogs of human cathelicidin LL-37. Antimicrob. Agents Chemother. 49:2845–50.
Sigurdardottir T, Andersson P, Davoudi M, Malmsten M, Schmidtchen A, Bodelsson M. (2006) In silico identification and biological evaluation of antimicrobial peptides based on human cathelicidin LL-37. Antimicrob. Agents Chemother. 50:2983–9.
Braunstein A, Papo N, Shai Y. (2004) In vitro activity and potency of an intravenously injected antimicrobial peptide and its DL amino acid analog in mice infected with bacteria. Antimicrob. Agents Chemother. 48:3127–9.
Shai Y. (2002) From innate immunity to de-novo designed antimicrobial peptides. Curr. Pharm. Des. 8:715–25.
Peschel A, Sahl H-G. (2006) The co-evolution of host cationic antimicrobial peptides and microbial resistance. Nature 4:529–36.
Peschel A. (2002) How do bacteria resist human antimicrobial peptides? Trends Microbiol. 10:179–86.
Yount NY, Bayer AS, Xiong YQ, Yeaman MR. (2006) Advances in antimicrobial peptide immunobiology. Biopolymers (Peptide Sci.) 84:435–58.
Hamilton A, Popham DL, Carl DJ, Lauth X, Nizet V, Jones AL. (2006) Penicillin-binding protein 1a promotes resistance of group B streptococcus to antimicrobial peptides. Infect. Immun. 74:6179–87.
Giacometti A, et al. (2006) Interaction of antimicrobial peptide temporin L with lipopolysaccharide in vitro and in experimental rat models of septic shock caused by gram-negative bacteria. Antimicrob. Agents Chemother. 50:2478–86.
Ghiselli R, et al. (2004) Cecropin B enhances betalactams activities in experimental rat models of gram-negative septic shock. Ann. Surg. 239:251–6.
Cirioni O, et al. (2006) Experimental study on the efficacy of combination of alpha-helical antimicrobial peptides and vancomycin against Staphylococcus aureus with intermediate resistance to glycopeptides. Peptides 27:2600–6.
Kristian SA, et al. (2007) Impairment of innate immune killing mechanisms by bacteriostatic antibiotics. FASEB J. 21:1107–16.
Zhang L, Falla TJ. (2006) Antimicrobial peptides: therapeutic potential. Expert Opin. Pharmacother. 7:653–63.
Hancock RE, Sahl HG. (2006) Antimicrobial and host-defense peptides as new anti-infective therapeutic strategies. Nat. Biotech. 24:1551–7.
Levin M, et al. (2000) Recombinant bactericidal/ permeability-increasing protein (rBPI21) as adjunctive treatment for children with severe meningococcal sepsis: a randomised trial. rBPI21 Meningococcal Sepsis Study Group. Lancet 356:961–7.
Giroir BP, Scannon PJ, Levin M. (2001) Bactericidal/permeability-increasing protein: lessons learned from the phase III, randomized, clinical trial of rBPI21 for adjunctive treatment of children with severe meningococcemia. Crit. Care Med. 29:S130–5.
Mookherjee N, Hancock RE. (2007) Cationic host defense peptides: innate immune regulatory peptides as a novel approach for treating infections. Cell Mol. Life Sci. 64:922–33.
Hancock RE, Patrzykat A. (2002) Clinical development of cationic antimicrobial peptides: from natural to novel antibiotics. Curr. Drug Targets Infect. Disord. 2:79–83.
Steinstraesser L, et al. (2001) Protegrin-1 enhances bacterial killing in thermally injured skin. Crit. Care Med. 29:1431–7.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is published under license to BioMed Central Ltd. This is an Open Access article is distributed under the terms of the Creative Commons Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Steinstraesser, L., Koehler, T., Jacobsen, F. et al. Host Defense Peptides in Wound Healing. Mol Med 14, 528–537 (2008). https://doi.org/10.2119/2008-00002.Steinstraesser
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.2119/2008-00002.Steinstraesser