Abstract
Background
Daylight photodynamic therapy (DL-PDT) is an effective and convenient treatment for multiple actinic keratosis (AKs). There are limited tools to evaluate the outcome of AK treatment. Recently, the actinic keratosis area and severity index (AKASI) has been proposed as a quantitative tool for assessing AK severity.
Objectives
To investigate patient satisfaction and efficacy of DL-PDT for severe AKs and to validate AKASI scoring as a quantitative tool for assessing the outcome of DL-PDT treatment.
Materials & methods
In this prospective single-centre study, we analysed the results of patients treated with one or two cycles of DL-PDT for severe AKs in the facial or scalp area.
Results
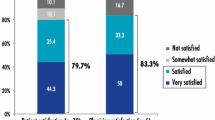
Forty patients (37 male and three female) with a mean age of 74 years (range: 56–87 years) were included and received either one (n = 20) or two (n = 20) cycles of DL-PDT. At baseline, most patients (95%) had 20 or more lesions. Patients treated with one cycle of DL-PDT showed a mean AKASI reduction of 45.5% (p < 0.001). Patients eligible for two cycles of DL-PDT demonstrated a mean AKASI reduction of 23.7% (p < 0.05) after one and 48.2% (p < 0.001) after two cycles. Patients participating in this study were either very satisfied (67.5%) or satisfied (32.5%). Almost all patients (97.5%) would recommend DL-PDT to other patients.
Conclusions
DL-PDT is a well-tolerated, safe and efficient treatment option for field cancerisation in the facial and scalp area with high patient satisfaction. AKASI scoring has proven useful as a quantitative tool for assessing the outcome of DL-PDT treatment.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Flohil SC, van der Leest RJ, Dowlatshahi EA, Hofman A, de Vries E, Nijsten T. Prevalence of actinic keratosis and its risk factors in the general population: the Rotterdam Study. J Invest Dermatol 2013; 133: 1971–8.
Schaefer I, Augustin M, Spehr C, Reusch M, Kornek T. Prevalence and risk factors of actinic keratoses in Germany-analysis of multisource data. J Eur Acad Dermatol Venereol 2014; 28: 309–13.
Glogau RG. The risk of progression to invasive disease. J Am Acad Dermatol 2000;42: 23–4.
Werner RN, Stockfleth E, Connolly SM, et al. Evidence- and consensus-based (S3) Guidelines for the Treatment of Actinic Keratosis - International League of Dermatological Societies in cooperation with the European Dermatology Forum - Short version. J Eur Acad Dermatol Venereol 2015; 29: 2069–79.
Arenberger P, Arenbergerova M. New and current preventive treatment options in actinic keratosis. J Eur Acad Dermatol Venereol 2017; 31: 13–7.
Fargnoli MC, Piccioni A, Neri L, Tambone S, Pellegrini C, Peris K. Conventional vs. daylight methyl aminolevulinate photodynamic therapy for actinic keratosis of the face and scalp: an intra-patient, prospective, comparison study in Italy. J Eur Acad Dermatol Venereol 2015; 29: 1926–32.
Rubel DM, Spelman L, Murrell DF, et al. Daylight photodynamic therapy with methyl aminolevulinate cream as a convenient, similarly effective, nearly painless alternative to conventional photodynamic therapy in actinic keratosis treatment: a randomized controlled trial. Br J Dermatol 2014; 171: 1164–71.
Sotiriou E, Apalla Z, Vrani F, et al. Daylight photodynamic therapy vs. conventional photodynamic therapy as skin cancer preventive treatment in patients with face and scalp cancerization: an intra-individual comparison study. J Eur Acad Dermatol Venereol 2017; 31: 1303–7.
Sotiriou E, Evangelou G, Papadavid E, et al. Conventional vs. daylight photodynamic therapy for patients with actinic keratosis on face and scalp: 12-month follow-up results of a randomized, intra-individual comparative analysis. J Eur Acad Dermatol Venereol 2018; 32: 595–600.
Dirschka T, Pellacani G, Micali G, et al. A proposed scoring system for assessing the severity of actinic keratosis on the head: actinic keratosis area and severityindex. J Eur Acad Dermatol Venereol 2017; 31: 1295–302.
Schmitz L, Gambichler T, Gupta G, Stucker M, Dirschka T. Actinic keratosis area and severity index (AKASI) is associated with the incidence of squamous cell carcinoma. J Eur Acad Dermatol Venereol 2018; 32: 752–6.
Schmitz L, von Dobbeler C, Gupta G, et al. Photodynamic therapy leads to significant improvement of actinic keratosis area and severity index (AKASI). Photodiagnosis Photodyn Ther 2018; 21: 66–70.
Olsen EA, Abernethy ML, Kulp-Shorten C, et al. A double-blind, vehicle-controlled study evaluating masoprocol cream in the treatment of actinic keratoses on the head and neck. J Am Acad Dermatol 1991; 24: 738–43.
Szeimies RM, Atanasov P, Bissonnette R. Use of lesion response rate in actinic keratosis trials. Dermatol Ther (Heidelb) 2016; 6: 461–4.
Skov T, Stockfleth E, Szeimies RM, Berman B. Efficacy endpoints in clinical trials in actinic keratosis. Dermatol Ther (Heidelb) 2018: 1–9.
Genovese G, Fai D, Fai C, Mavilia L, Mercuri SR. Daylight methyl-aminolevulinate photodynamic therapy versus ingenol mebutate for the treatment of actinic keratoses: an intraindividual comparative analysis. Dermatol Ther 2016; 29: 191–6.
Lacour JP, Ulrich C, Gilaberte Y, et al. Daylight photodynamic therapy with methyl aminolevulinate cream is effective and nearly painless in treating actinic keratoses: a randomised, investigator-blinded, controlled, phase III study throughout Europe. J Eur Acad Dermatol Venereol 2015; 29: 2342–8.
Wiegell SR, Fabricius S, Gniadecka M, et al. Daylight-mediated photodynamic therapy of moderate to thick actinic keratoses of the face and scalp: a randomized multicentre study. Br J Dermatol 2012; 166: 1327–32.
Wiegell SR, Fabricius S, Stender IM, et al. A randomized, multi-centre study of directed daylight exposure times of 1(1/2) vs. 2(1/2) h in daylight-mediated photodynamic therapy with methyl aminolae-vulinate in patients with multiple thin actinic keratoses of the face and scalp. Br J Dermatol 2011; 164: 1083–90.
Wiegell SR, Haedersdal M, Eriksen P, Wulf HC. Photodynamic therapy of actinic keratoses with 8% and 16% methyl aminolaevulinate and home-based daylight exposure: a double-blinded randomized clinical trial. Br J Dermatol 2009; 160: 1308–14.
Pellacani G, Gupta G, Micali G, et al. Actinic keratosis area severity index (AKASI): reproducibility study and comparison with total lesion count. Br J Dermatol 2018; 179: 763–4.
Kellner C, Bauriedl S, Hollstein S, Reinhold U. Simulated-daylight photodynamic therapy with BF-200 aminolaevulinic acid for actinic keratosis: assessment of the efficacy and tolerability in a retrospective study. Br J Dermatol 2015; 172: 1146–8.
Neittaanmaki-Perttu N, Gronroos M, Karppinen TT, Tani TT, Snellman E. Hexyl-5-aminolaevulinate 0.2% vs. methyl-5-aminolaevulinate 16% daylight photodynamic therapy for treatment of actinic keratoses: results of a randomized double-blinded pilot trial. Br J Dermatol 2016; 174: 427–9.
Neittaanmaki-Perttu N, Karppinen TT, Gronroos M, Tani TT, Snellman E. Daylight photodynamic therapy for actinic keratoses: a randomized double-blinded nonsponsored prospective study comparing 5-aminolaevulinic acid nanoemulsion (BF-200) with methyl-5-aminolaevulinate. Br J Dermatol 2014; 171: 1172–80.
Neittaanmaki-Perttu N, Karppinen TT, Tani T, Snellman E, Gronroos M. Long-term outcome of low-concentration hexyl-5-aminolaevulinate daylight photodynamic therapy for treatment of actinic keratoses. Acta Derm Venereol 2017; 97: 120–1.
Fargnoli MC, Ibbotson SH, Hunger RE, et al. Patient and physician satisfaction in an observational study with methyl aminolevulinate daylight photodynamic therapy in the treatment of multiple actinic keratoses of the face and scalp in six European countries. J Eur Acad Dermatol Venereol 2018; 32: 757–62.
See JA, Gebauer K, Wu JK, Manoharan S, Kerrouche N, Sullivan J. High patient satisfaction with daylight-activated methyl aminole-vulinate cream in the treatment of multiple actinic keratoses: results of an observational study in Australia. Dermatol Ther 2017; 7: 525–33.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Jordan, M., Ghoreschi, K. & Eberle, F.C. Daylight photodynamic therapy for severe facial and scalp actinic keratosis: a prospective non-sponsored single-centre study employing the actinic keratosis area and severity index (AKASI). Eur J Dermatol 29, 67–74 (2019). https://doi.org/10.1684/ejd.2018.3492
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1684/ejd.2018.3492