Abstract
Introduction
Not all Americans may benefit equally from current improvements in breast and colorectal cancer screening and mortality rates.
Methods
We performed a cross-sectional retrospective review of county-level screening, incidence, and mortality rates for breast and colon cancer utilizing three publicly available data sources from the Centers for Disease Control and Prevention (CDC), and their association with the Distressed Communities Index (DCI), a measure of local economic prosperity across communities.
Results
After controlling for other factors, DCI was associated with county-level screening, incidence, and death rates per 100,000 for breast and colorectal cancer. There was an absolute increase of 0.77 (95% confidence interval [CI] 0.67–0.85, p < 0.001) in the proportion of women aged 40 years or older who had a screening mammogram for every 10-point decrease in DCI, which in turn correlated with an increase in the age-adjusted incidence by 1.68 per 100,000 (95% CI 1.37–2.00, p < 0.001). While the age-adjusted death rate for breast cancer was highest in the most distressed communities, the overall incidence of age-adjusted death decreased by 0.28 per 100,000 (95% CI −0.37 to −0.19, p < 0.001) with every 10-point decrease in DCI. For colorectal cancer, every 10-point decrease in DCI was similarly associated with an absolute 0.60 (95% CI 0.52–0.69, p < 0.001) increase in the proportion of individuals who had screening endoscopy. Increased colorectal screening in low-DCI counties was associated with a lower age-adjusted incidence rate (−0.80 per 100,000; 95% CI −0.94 to −0.65) and age-adjusted death rate (−0.55 per 100,000; 95% CI −0.62 to −0.49) of colorectal cancer per every 10-point decrease in DCI (p < 0.001).
Conclusion
The association of county-level socioeconomic and healthcare factors with breast and colorectal cancer outcomes was notable, with level of community distress impacting cancer screening, incidence, and mortality rates.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Cancer is the second leading cause of mortality in the US, being responsible for more than one in five deaths in 2019.1 In particular, breast and colorectal cancer rank among the four most deadly cancers affecting 42,000 women and 52,547 Americans, respectively, on an annual basis.2 Of note, mortality from breast cancer is on the decline, with a 1% annual decrease from 2013 to 2018, whereas mortality from colorectal cancer has declined by almost 2% per year from 2014 to 2018.3 As case mortality decreases, screening rates for both breast and colorectal cancer are increasing, with a 1.6% increase between 2015 and 2018 and a 1.4% increase between 2016 and 2018, respectively.4,5 Despite these general improvements in screening and mortality, progress has not been universally realized by all Americans. Specifically, persistent disparities in cancer screening, as well as cancer-related mortality, exist relative to race and ethnicity.6 In particular, screening for breast and colorectal cancers may be lower among Black, Hispanic, Asian, and American Indian/Alaska Native patients relative to White patients.7 In addition, Black/African American patients have higher death rates than all other racial/ethnic groups for many cancer types.8 While racial and ethnic disparities have been reported, potential underlying mechanisms that drive these disparities have not been well-defined.9,10
Disparities in cancer screening and mortality may be related to underlying economic trends given the strong association between cancer screening, incidence, and mortality with community economic indicators such as employment and income.11,12,13,14,15 Regional economic improvement may manifest in increased employment opportunities, which, in turn, may afford residents higher income and increased ability to obtain health insurance, thereby improving access to healthcare including cancer screening. Given persistent economic inequality across the US, understanding how economic trends influence cancer screening, incidence, and mortality may be important to devise strategies to target these factors. To date, whether changes in regional economic prosperity may be associated with trends in screening, incidence, and mortality among patients with breast and colon cancer has not been investigated.
Therefore, the purpose of the current study was to characterize the relative impact of economic prosperity and distress on outcomes of patients with breast and colon cancer. To this end, we utilized the Economic Innovation Group (EIG) Distressed Communities Index (DCI), a composite metric that combines seven zip code-level economic variables to characterize the spatial distribution of US economic well-being.14 The DCI is designed to provide a single, holistic, and comparative measure of economic well-being across communities throughout the US. By combining these seven complementary economic indicators into a single summary statistic, the DCI can convey each community’s economic standing relative to other communities. We hypothesized that DCI was associated with county-level incidence, mortality, and screening rates for breast and colon cancer.
Methods
Cancer Screening, Incidence, and Mortality Data
County-level data on incidence and mortality among patients with breast and colon cancer were obtained from the State Cancer Profiles made available through the NIH National Cancer Institute and Centers for Disease Control and Prevention (CDC).16 Screening for breast cancer was defined as having had a mammogram in the past 2 years among women aged 40 years and older,17 while screening for colorectal cancer was defined as having had a colorectal endoscopy (i.e., sigmoidoscopy or colonoscopy) in adults aged 50 years and older.17 Screening estimates were reported as the proportion of eligible individuals who met the screening criteria within any given county. The most recent available estimates were based on 2008–2010 data derived from a statistical model that combined information from the Behavioral Risk Factor Surveillance System and the National Health Interview Survey to correct for nonresponse and undercoverage bias; the model also enhanced data from small areas by borrowing information from similar areas across the nation.18,19
The incidence of breast and colorectal cancer was reported by county for all stages (excluding in situ lesions) among patients of all ages; for breast cancer, only female individuals were included in the framing sample. Estimates were reported for 2013–2017, which was the latest 5-year average available. Estimates were age-adjusted incidence rates reported as cases per 100,000 individuals in the population.20,21 The 5-year trend in the incidence of cancer was reported for both breast and colorectal cancer. Breast and colorectal cancer mortality were similarly reported by county, using estimates from 2013 to 2017. Estimates were age-adjusted death rates reported as deaths per 100,000 individuals.22,23 Additionally, a 5-year trend in the death rate was determined for patients with breast or colorectal cancer.
Economic Prosperity and County Demographic Data
Economic prosperity was based on the DCI, which is composed of seven markers of economic activity drawn from the US Census Bureau’s American Community Survey (ACS) 5-Year Estimates and Business Patterns data sets; the data are available for all counties with more than 500 residents.24 The seven components of the index include (1) No High School Diploma; (2) Housing Vacancy Rate; (3) Adults Not Working; (4) Poverty Rate; (5) Median Income Ratio; (6) Percentage Change in Employment (i.e., percentage change in number of jobs from 2014 to 2018); and (7) Percentage Change in Establishments (i.e., percentage change in the number of business establishments from 2014 to 2018). Each community is ranked on each measure, after which each community’s rankings are averaged and weighted equally to create a preliminary score. This preliminary score is then normalized into a final score that ranges from approaching 0 (most prosperous) to 100 (most distressed).24 By combining these seven complementary economic indicators into a single summary statistic, the DCI is able to convey each community’s economic standing relative to other communities. For the purposes of the current study, the 2020 edition of the DCI was utilized, which was derived from US Census Bureau’s ACS 5-Year Estimates covering the years 2014–2018 and the Census Bureau’s Business Patterns datasets for the same years.
County-level demographic data, including total population, total population aged 40–64 years, percentage of female and male residents, and proportion of individuals of different races/ethnicities, were obtained from the US Census Bureau.25 County-level data for the number of primary care providers and hospital beds were obtained from the Health Resources and Services Administration Area Health Resource File.26
Outcomes and Analysis
The primary outcome was county-level estimates of breast and colorectal cancer screening relative to DCI, while secondary outcomes included county-level estimates of age-adjusted incidence and mortality rates of breast and colorectal cancer, relative to DCI. Secondary outcomes also included the 5-year trends in age-adjusted incidence and mortality rates of breast and colorectal cancer between 2013 and 2017.
Counties were divided into tertiles based on the DCI and outcomes were estimated across the DCI tertiles using generalized linear mixed models, which allowed for analysis of hierarchical data with non-normal distributions. The models included the DCI score as a continuous variable, as well the proportion of individuals who were female, Black, or Hispanic, proportion of patients with health insurance, as well as the number of primary care providers per 100,000 and hospitals per 100,000. Random effects for states were included to account for clustering of counties within states.
All analyses were performed in Stata 16 (StataCorp LLC, College Station, TX, USA). All tests were two-sided and significance was determined using a p-value <0.05. The study was deemed exempt by both the University of Michigan Institutional Review Board and The Ohio State University Review Board guidelines because it used publicly available data routinely collected for public health purposes.
Results
County Characteristics Relative to the Distressed Communities Index (DCI)
Among 3100 counties included in the analysis, median DCI was 16.7 (interquartile range [IQR] 8.3–25.0) for counties in the lowest tertile versus 50.1 (IQR 41.7–58.3) for intermediate counties and 83.4 (IQR 75.0–91.7) for counties in the highest tertile (Fig. 1). Across county tertiles, there was a stepwise decrease in median county population (lowest DCI 55,462.5 [IQR 19,146–176,954] vs. intermediate DCI 24,925 [IQR 10,025–57,325] vs. highest DCI 18,464 [IQR 9664.5–32,610]; p < 0.001); median age was similar across county DCIs (lowest DCI 39.8 years vs. intermediate DCI 41.3 years vs. highest DCI 40.1 years), as was the proportion of females (lowest DCI 50.6% vs. intermediate DCI 50.5% vs. highest DCI 51.1%; both p < 0.001) (Table 1). The proportion of non-Hispanic White individuals was lowest within counties in the highest DCI tertile (69.7%) versus counties in the lowest (86.5%) or intermediate (87.0%) tertiles (p < 0.001); the proportion of Hispanic/Latino individuals also decreased from the lowest to highest DCI counties (lowest DCI 4.8% vs. intermediate DCI 3.9% vs. highest DCI 3.3%; p < 0.001). In contrast, the proportion of Black/African American individuals was markedly higher within counties in the highest DCI tertile (5.0%) versus counties in the lowest (1.7%) or intermediate (1.5%) DCI tertiles (p < 0.001).

Source: Maps are based on the authors’ analysis of DCI and CDC cancer statistics data for breast and colorectal cancer. a US county DCI by tertiles. b US county breast cancer screening estimates by tertiles. c US county colorectal cancer screening estimates by tertiles. DCI Distressed Communities Index, CDC Centers for Disease Control and Prevention
Geographic distribution of counties by tertiles of DCI and breast and colorectal screening rates.
Socioeconomic and healthcare-related factors worsened in a stepwise fashion across DCI tertiles (Table 1). Specifically, while median income was highest in counties within the lowest DCI tertile ($58,392), median income was much lower among individuals who lived in intermediate ($47,633) or highest ($39,061) DCI counties (p < 0.001). In turn, the proportion of individuals in poverty increased relative to DCI (lowest DCI 10.3% vs. intermediate DCI 10.6% vs. highest DCI 14.6%; p < 0.001). Similarly, the percentage of adults not working, as well as the percentage of adults without a high school degree was related to county DCI (lowest DCI: not working, 18.5%/without high school diploma, 10.3% vs. intermediate DCI: not working, 23.6%/without high school diploma, 11.7% vs. highest DCI: not working, 32.3%/without high school diploma, 18.5%; p < 0.001). The percentage change in employment and business establishments also worsened across DCI tertiles. Specifically, while individuals living in the lowest DCI tertile county had a 7.8% increase in employment and a 4.4% increase in business establishments, individuals residing in the highest DCI counties had a 1.9% decrease in employment and a 2.2% decrease in business establishments (p < 0.001).
Of note, the proportion of adults aged 40–64 years without health insurance was also related to county DCI (lowest DCI 7.7% vs. intermediate DCI 10.0% vs. highest DCI 13.3%; p < 0.001). The number of primary care providers per 100,000 (lowest DCI 60.8 vs. intermediate DCI 47.3 vs. highest DCI 37.2; p < 0.001), as well as hospital beds per 100,000 (lowest DCI 167.2 vs. intermediate DCI 209.7 vs. highest DCI 195.2) also varied relative to DCI (both p < 0.001).
Impact of DCI on Cancer Screening and Outcomes
Breast and colorectal cancer screening, incidence, and death rates varied relative to county DCI (Table 2). Specifically, the percentage of women aged 40 years or older who had a mammogram in the past 2 years was lowest among individuals who lived in the most distressed communities (lowest DCI 71.5% vs. intermediate DCI 68.2% vs. highest DCI 64.6%; p < 0.001). Similarly, the proportion of adults aged 50 years or older who had ever had a colorectal endoscopy was lowest among individuals from highly distressed communities (lowest DCI 60.2% vs. intermediate DCI 56.8% vs. high DCI 52.6%; p < 0.001). Of note, the relationship between age-adjusted incidence per 100,000 and economic prosperity was different for breast and colorectal cancer. Specifically, the age-adjusted incidence of breast cancer per 100,000 was 128.4 within counties in the lowest DCI tertile versus 120.7 and 113.2 in intermediate and high tertile DCI communities, respectively (p < 0.001). Conversely, the age-adjusted incidence of colorectal cancer per 100,000 increased stepwise with increasing economic distress (lowest DCI 19.9 vs. intermediate DCI 21.2 vs. high DCI 22.9; p < 0.001).
Among women with breast cancer, the age-adjusted death rate per 100,000 incrementally increased with higher distress in the community in which the patient lived (low DCI 19.9 vs. intermediate DCI 21.2 vs. high DCI 22.0; p < 0.001). Similarly, the 5-year trend in breast cancer mortality per 100,000 was worse as community distress increased (low DCI −1.9 vs. intermediate DCI −1.6 vs. high DCI −1.4: p < 0.001). The age-adjusted mortality per 100,000 among patients with colorectal cancer was highest among individuals residing in very distressed communities (low DCI 13.3 vs. intermediate DCI 15.5 vs. high DCI 18.1; p < 0.001); 5-year trends in colorectal cancer mortality per 100,000 were similarly incrementally worse in highly distressed communities (5-year trend: low DCI −1.2 vs. intermediate DCI −2.0 vs. high DCI −2.4; p < 0.001).
After risk adjustment, DCI remained associated with county screening, incidence, and death rates per 100,000 among individuals with breast or colorectal cancer (Fig. 2a–c). In particular, there was an absolute increase of 0.77 (95% confidence interval [CI] 0.67–0.85; p < 0.001) in the proportion of women aged 40 years or older who had a screening mammogram for every 10-point decrease in DCI, which in turn correlated with an increase in the age-adjusted incidence by 1.68 per 100,000 (95% CI 1.37–2.00; p < 0.001). Notably, age-adjusted death rates decreased by 0.28 per 100,000 (95% CI −0.37 to −0.19; p < 0.001) with every 10-point decrease in DCI. For colorectal cancer, every 10-point decrease in DCI was similarly associated with an absolute 0.60 (95% CI 0.52–0.69; p < 0.001) increase in the proportion of individuals who had screening endoscopy. However, unlike breast cancer, increased colorectal screening in low DCI counties was associated with a lower age-adjusted incidence rate (0.80 per 100,000; 95% CI −0.94 to −0.65) and age-adjusted death rate (0.55 per 100,000; 95% CI −0.62 to −0.49) of colorectal cancer per every 10-point decrease in DCI (p < 0.001).

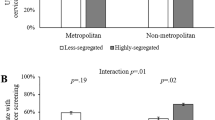
Source: Figures are based on the authors’ analysis of DCI and CDC cancer statistics data for breast and colorectal cancer. a County-level estimates of the percentage of individuals who had breast and colorectal screening across the DCI. b County-level estimates of the breast and colorectal incidence rate across the DCI. c County-level estimates of breast and colorectal death rates across the DCI. Models are adjusted for percentage of females, percentage of Black subjects, percentage of Hispanic subjects, percentage of individuals without health insurance, primary care provider per 100K, and hospital beds per 100K. Random effects for states were included to account for clustering of counties within states. DCI Distressed Communities Index, CDC Centers for Disease Control and Prevention
Risk-adjusted breast and colorectal screening a, incidence b, and death rates c, by DCI.
Overall, 5-year trends in the incidence rate of breast cancer did not change relative to DCI (0.009; 95% CI −0.04 to 0.06; p = 0.716); however, the overall death rate trend did decrease by 0.05 (95% CI −0.10 to −0.002; p = 0.041) for every 10-point decrease in the DCI. In examining colorectal cancer, 5-year trends in incidence rate and death rate decreased by 0.05 (95% CI −0.10 to −0.005; p = 0.031) and 0.14 (95% CI −0.18 to −0.11; p < 0.001), respectively, for every 10-point decrease in DCI.
In subset analyses that compared the least versus most distressed counties, the effect of DCI was even more pronounced. Specifically, individuals residing in the least distressed counties had a 4.44% (95% CI 3.77–5.11) higher likelihood of having had a screening mammogram in the last 2 years; similarly, individuals aged 50 years or older in these counties had a 3.44% (95% CI 2.85–4.02) higher likelihood of having had colorectal endoscopy (both p < 0.001) (Table 3). Furthermore, the most distressed counties had 1.51 more deaths per 100,000 (95% CI +0.88 to +2.14) for breast cancer and 3.2 more deaths per 100,000 (95% CI +2.74 to +3.65) for colorectal cancer. Interestingly, while the incidence of breast cancer was 10.29 (95% CI 8.14–12.44) cases greater per 100,000, the incidence of colorectal cancer was 4.7 (95% CI −5.371 to −3.71) cases fewer per 100,000 among the least distressed counties. Although there was no difference in trends of breast cancer age-adjusted death rates among the least versus most distressed counties, the trend in age-adjusted colorectal cancer death rate declined much more (−0.84, 95% CI −1.10 to −0.57) among individuals residing in the least distressed counties.
Discussion
Not all communities have benefitted equally from the long period of economic expansion that followed the 2008–2009 recession in the US.27 In fact, the gap in economic well-being between prosperous and impoverished areas in the US has only grown larger over the last decade.28,29,30 The consequences of geographic economic inequality on health may be particularly relevant for breast and colorectal cancer patients. Established screening programs exist for both breast and colorectal cancer, leading to earlier diagnosis and lower mortality for these two conditions.31,32 Specifically, guidelines recommend that most adults start screening for breast and colon cancer at 40 and 50 years of age, respectively—a period of time in which most Americans obtain their health insurance through their employer.33,34 As such, unfavorable community-level economic circumstances may offer residents fewer employment opportunities, limiting their ability to obtain health insurance and, in turn, to participate in cancer screening programs. The current study was important because we characterized the impact of county-level economic prosperity, as measured by DCI, on rates of breast and colorectal cancer screening, incidence, and mortality. Of note, more distressed counties had almost twice as many adult residents without health insurance as more prosperous counties, as well as fewer primary care providers per capita. Additionally, counties with high DCI scores had decidedly lower screening rates, as well as higher mortality for breast and colorectal cancer compared with counties with low DCI scores. Specifically, the least distressed counties had an estimated 6293 fewer annual deaths from breast (1251) and colorectal (5042) cancer versus individuals who lived in the most distressed counties. Collectively, these data suggest that geographic economic inequality resulted in an uneven application of screening programs for breast and colorectal cancer across the country, which may have contributed to the higher mortality for breast and colorectal cancer among residents of distressed communities.
Levels of health insurance coverage and access to primary care vary widely across different US counties.35,36 Notably, individuals with health insurance are more likely to have access to a usual source of care, preventative screenings, and early diagnosis of chronic conditions.37 In the current study, counties with the highest DCI scores had almost twice as many adult residents without health insurance as counties with the lowest DCI scores (13.3% vs. 7.7%; p < 0.001) [Table 1]. These data were in line with previous reports that demonstrated economic variables such as household income, unemployment and education level were associated with insurance status.36 In turn, insurance status has been associated with stage at diagnosis and outcomes among patients with breast and colorectal cancer.38,39,40 Insurance status may mediate the impact of county-level economic prosperity on breast and colorectal cancer screening, incidence, and mortality. Additionally, counties in the highest tertile of DCI had decidedly fewer primary care providers per 100,000 people compared with counties in the lowest tertile of DCI (median 37.2 vs. 60.8; p < 0.001) (Table 1). Of note, increased availability of primary care providers has been linked to a diagnosis of cancer at an earlier stage and lower mortality for both breast and colorectal cancer patients.41,42,43 As such, availability of coordinated primary care networks may represent an additional mechanism mediating the effects of county-level economic well-being on breast and colorectal cancer screening rates, incidence, and mortality.
Screening is effective at reducing colorectal cancer incidence and mortality through the removal of precancerous polyps and detection of early-stage colorectal cancer.44,45,46 Despite this, approximately one-third of US adults who are eligible for screening have not been screened.47 As a result, 46–63% of deaths due to colorectal cancer are attributable to lack of screening.48 In the current study, 56.5% of the total population had colorectal cancer screening. In contrast, the 2010 Behavioral Risk Factor Surveillance System (BRFSS) questionnaire reported that 66.4% of responders aged 50 years or older had ever had sigmoidoscopy or endoscopy in their life.49 This difference may be explained by the dissimilar composition of BRFSS responders versus the overall US population.50 Of note, the proportion of county residents aged 50 years or older who had ever had colorectal endoscopy decreased with increasing values of county-level DCI (Figs. 1 and 2a). Specifically, counties in the high DCI tertile had 7.5% fewer residents who had undergone colorectal cancer screening than individuals who resided in low DCI tertile counties (Table 2). The association of colorectal cancer screening uptake with socioeconomic status and neighborhood-level social determinants of health is well established.51,52,53,54 Additionally, stark regional differences in colorectal cancer screening rates have been described.55 To our knowledge, the current study is the first to report an association between county-level economic prosperity and colorectal cancer screening rates among residents. Since colorectal endoscopy is able to prevent colorectal cancer through the removal of adenomatous polyps, as well as diagnose cancer at an earlier stage, lower county-level economic prosperity and higher DCI also led to higher colorectal cancer incidence and mortality (Figs. 2b,c).45,56 Collectively, these findings can help identify communities in which an increase in colorectal screening rates would have the largest impact.57 Additionally, they suggest that interventions aimed at improving the economic conditions of distressed counties would have beneficial repercussions on residents at risk of or affected by colorectal cancer.
Regular breast cancer screening in eligible adults has also been demonstrated to reduce mortality, increase life expectancy, and reduce costs associated with treatment.58,59,60,61 However, according to 2018 CDC data, breast cancer screening rates in the US are still suboptimal. Additionally, notable disparities in breast cancer screening uptake exist among population subgroups.62 In the current study, 68.2% of women aged 40 years or older had breast cancer screening within the past 2 years (Table 2). This is slightly above the 2018 US rate of 66.7%.4 Of note, screening rates differed relative to county DCI tertile (median, low 71.5% vs. intermediate 68.2% vs. high 64.6%; p < 0.001), with the screening rate being below the national average for those individuals residing in counties with the highest DCI tertile. These results are consistent with data reported by other investigators.15,54,62,63 For example, a recent study by Kurani et al. noted that individuals living in areas of greater deprivation in the Midwest had 49% lower odds of completing recommended breast cancer screening.54 Furthermore, other studies have reported an association between breast cancer screening rates and regional disparities in breast cancer incidence and mortality.15,54,64,65,66 Specifically, Harding et al. analyzed data from 547 Surveillance, Epidemiology, and End Results (SEER) counties and noted that higher rates of breast cancer screening were associated with increased incidence of breast cancer in the same area.65 However, increased screening rates mostly resulted from the diagnosis of additional small, early-stage cancers, without a concomitant increase in the diagnosis of large, late-stage cancers. As a result, no benefit in terms of decreased breast cancer mortality was noted.65 In contrast, prior ecological studies conducted at the larger state level had demonstrated that breast cancer mortality decreased with increasing screening rates.67,68,69 Regardless, caution is recommended when drawing conclusions from the reported association between DCI and county-level breast cancer screening rates and mortality. In fact, the results of the current study demonstrated that breast cancer incidence increased in relation to screening rates and DCI tertile (Figs. 2a, b). In addition, a strong association was noted between DCI tertile and breast cancer mortality per 100,000 people (median, low 19.9 vs. intermediate 21.2 vs. high 22.9; p < 0.001) (Table 2). Taken together, these data suggest that area-level differences in economic prosperity impact screening rates, which, in turn, affect breast cancer incidence and mortality. However, the increased breast cancer mortality in more distressed communities could also be attributable to differences in access to surgical care or treatment patterns. Nonetheless, our findings provide novel and valuable insight on potential barriers to equitable care. By shedding light on community-level distress patterns in relation to breast and colon cancer outcomes, the data can inform the creation and implementation of strategies, as well as direct allocation of funding and resources to help alleviate geographical disparities among breast and colon cancer populations.
Several limitations should be considered when interpreting the results of the current study. For example, potential unmeasured confounding was likely, although several important demographic and healthcare-related variables were accounted for that have a plausible association with cancer screening, incidence, and mortality. In addition, data on screening estimates were from 2008–2010. While a decade old, these data were the most recent estimates available at the county level. Estimates were based on a statistical model that combined information from the Behavioral Risk Factor Surveillance System and the National Health Interview Survey to correct for nonresponse and undercoverage bias, and were enhanced in small areas by borrowing information from similar areas across the nation. Data on staging or tumor subtype were also not available, which impacted the ability to examine changes in DCI relative to disease characteristics. Because the data were aggregated at the county level, inferences at the individual level could not be made. Additionally, the findings may have been subject to residual heterogeneity within counties. For example, large, diverse counties may have residents and neighborhoods with a wide variation of distressed community indices. Despite these limitations, differences observed at the county level between the lowest and highest distressed counties were notable and should compel further research to mitigate disparities.
Conclusion
Disparities in breast and colorectal cancer outcomes are multifaceted. The association of area-level socioeconomic and healthcare factors with breast and colorectal cancer outcomes was notable, with level of community distress impacting cancer screening, incidence, and mortality rates. Future studies should focus on individual-level access to and utilization of preventive services to understand primary drivers of such disparities. Additionally, further examination of the longitudinal interplay between access to care, preventive services, and outcomes of breast and colon cancer are needed. DCI proved to be a valuable tool that can aid researchers in understanding socioeconomic barriers to accessing healthcare. As such, continued work in this area has the potential to support strategies and policies aimed at increasing health equity.
References
Kochanek KD, Xu J, Arias E. Mortality in the United States, 2019. NCHS Data Brief. 2020;395:1–8.
US Cancer Statistics Working Group. US Cancer Statistics Data Visualizations Tool, based on 2019 submission data (1999–2017). US Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute; 2020.
Cancer Facts and Figures 2021. American Cancer Society, NY, 2021.
Centers for Disease Control and Prevention. Health, United States, 2019 – Data Finder. Available at: https://www.cdc.gov/nchs/hus/contents2019.htm. Accessed 26 Apr 2021.
Centers for Disease Control and Prevention. Colorectal Cancer Screening Rates. 26 June 2020. Available at: https://www.cdc.gov/cancer/ncccp/screening-rates/. Accessed 26 Apr 2021.
Goel MS, Wee CC, McCarthy EP, et al. Racial and ethnic disparities in cancer screening: the importance of foreign birth as a barrier to care. J Gen Intern Med. 2003;18(12):1028–35.
Goding Sauer A, Siegel RL, Jemal A, et al. Current Prevalence of Major Cancer Risk Factors and Screening Test Use in the United States: Disparities by Education and Race/Ethnicity. Cancer Epidemiol Biomarkers Prev. 2019;28(4):629–42.
National Cancer Institute. Cancer Disparities. 17 November 2020. Available at: https://www.cancer.gov/about-cancer/understanding/disparities. Accessed 3 May 2021.
Zeng C, Wen W, Morgans AK, et al. Disparities by Race, Age, and Sex in the Improvement of Survival for Major Cancers: Results From the National Cancer Institute Surveillance, Epidemiology, and End Results (SEER) Program in the United States, 1990 to 2010. JAMA Oncol. 2015;1(1):88–96.
Warren Andersen S, Blot WJ, Lipworth L, et al. Association of Race and Socioeconomic Status With Colorectal Cancer Screening, Colorectal Cancer Risk, and Mortality in Southern US Adults. JAMA Netw Open. 2019;2(12):e1917995.
Freeman HP, Alshafie TA. Colorectal carcinoma in poor blacks. Cancer. 2002;94(9):2327–32.
Clegg LX, Reichman ME, Miller BA, et al. Impact of socioeconomic status on cancer incidence and stage at diagnosis: selected findings from the surveillance, epidemiology, and end results: National Longitudinal Mortality Study. Cancer Causes Control. 2009;20(4):417–35.
O’Connor JM, Sedghi T, Dhodapkar M, et al. Factors associated with cancer disparities among low-, medium-, and high-income US counties. JAMA Netw Open. 2018;1(6):e183146.
Reames BN, Birkmeyer NJ, Dimick JB, et al. Socioeconomic disparities in mortality after cancer surgery: failure to rescue. JAMA Surg. 2014;149(5):475–81.
Singh GK, Jemal A. Socioeconomic and Racial/Ethnic Disparities in Cancer Mortality, Incidence, and Survival in the United States, 1950–2014: Over Six Decades of Changing Patterns and Widening Inequalities. J Environ Public Health. 2017;2017:2819372.
State Cancer Profiles. Available at: https://www.statecancerprofiles.cancer.gov/index.html. Accessed April 20, 2021.
State Cancer Profiles. Data Types—Screening and Risk Factors Data Types. 16 May 2017. Available at: https://statecancerprofiles.cancer.gov/screening_risk_datatypes.html. Accessed 11 May 2021.
Liu B, Parsons V, Feuer EJ, et al. Small Area Estimation of Cancer Risk Factors and Screening Behaviors in US Counties by Combining Two Large National Health Surveys. Prev Chronic Dis. 2019;16:E119.
National Institutes of Health, National Cancer Institute. Methodology for the Model-based Small Area Estimates of Cancer Risk Factors and Screening Behaviors. Small Area Estimates for Cancer-Related Measures. 19 August 2019. Available at: https://sae.cancer.gov/nhis-brfss/methodology.html. Accessed 20 Apr 2021.
National Institutes of Health, National Cancer Institute. State Cancer Profiles. Breast cancer incidence rates table. Available at: https://www.statecancerprofiles.cancer.gov/incidencerates/index.php?stateFIPS=00&areatype=county&cancer=055&race=00&sex=2&age=001&stage=999&year=0&type=incd&sortVariableName=rate&sortOrder=default&output=0#results. Accessed 20 Apr 2021.
National Institutes of Health, National Cancer Institute. State Cancer Profiles. Colon and rectal cancer incidence rates table. Available at: https://www.statecancerprofiles.cancer.gov/incidencerates/index.php?stateFIPS=00&areatype=county&cancer=020&race=00&sex=0&age=001&stage=999&year=0&type=incd&sortVariableName=rate&sortOrder=default&output=0#results. Accessed 20 April 2021.
National Institutes of Health, National Cancer Institute. State Cancer Profiles. Breast cancer death rates table. Available at: https://www.statecancerprofiles.cancer.gov/deathrates/index.php?stateFIPS=00&areatype=county&cancer=055&race=00&sex=2&age=001&year=0&type=death&sortVariableName=rate&sortOrder=default#results. Accessed 20 Apr 2021.
National Institutes of Health, National Cancer Institute. State Cancer Profiles. Colon and rectal cancer death rates table. Available at: https://www.statecancerprofiles.cancer.gov/deathrates/index.php?stateFIPS=00&areatype=county&cancer=020&race=00&sex=0&age=001&year=0&type=death&sortVariableName=rate&sortOrder=default#results. Accessed 20 Apr 2021.
Economic Innovation Group. Distressed Communities Index: methodology. Available at: https://eig.org/dci/methodology. Accessed 20 Apr 2021.
US Census Bureau. Explore Census data. Available at: https://data.census.gov/cedsci/. Accessed 20 Apr 2021.
Health Resources and Services Information. Area health resources file. Available at: https://data.hrsa.gov/topics/health-workforce/ahrf. Accessed 20 Apr 2021.
Sommeiller E, Price M 2018 The new gilded age. Income inequality in the U.S. by state, metropolitan area, and county. Economic Policy Institute
Benzow A, Fikri K, et al. 2020 The Spaces Between Us. The Evolution of American Communities in the New Century. Economic Innovation Group
Shambaugh J, Nunn R et al. Place-based Policies for Shared Economic Growth. The Hamilton Project; 2018.
Florida R. America’s Worsening Geographic Inequality. 16 October 2018. Available at: https://www.bloomberg.com/news/articles/2018-10-16/geographic-economic-inequality-is-growing-in-the-u-s. Accessed 22 Apr 2021.
Siu AL, US Preventive Services Task Force. Screening for Breast Cancer: U.S. Preventive Services Task Force Recommendation Statement. Ann Intern Med. 2016;164(4):279–96.
US Preventive Services Task Force, Bibbins-Domingo K, Grossman DC, et al. Screening for Colorectal Cancer: US Preventive Services Task Force Recommendation Statement. JAMA 2016; 315(23):2564-2575.
State Health Facts. Health Insurance Coverage of the Total Population. 2021. Available at: https://www.kff.org/other/state-indicator/total-population/?dataView=1¤tTimeframe=0&selectedDistributions=employer&sortModel=%7B%22colId%22:%22Location%22,%22sort%22:%22asc%22%7D. Accessed 26 Apr 2021.
SHADAC analysis of the American Community Survey (ACS) Public Use Microdata Sample (PUMS) files. 2021. Available at: statehealthcompare.shadac.org. Accessed 26 Apr 2021.
Kirby JB, Yabroff KR. Rural-Urban Differences in Access to Primary Care: Beyond the Usual Source of Care Provider. Am J Prev Med. 2020;58(1):89–96.
Stone LC, Boursaw B, Bettez SP, et al. Place as a predictor of health insurance coverage: a multivariate analysis of counties in the United States. Health Place. 2015;34:207–14.
Institute of Medicine (US) Committee on Health Insurance Status and its Consequences. America’s Uninsured Crisis: Consequences for Health and Health Care. Washington (DC); National Academies Press (US);2009.
Ellis L, Canchola AJ, Spiegel D, et al. Trends in cancer survival by health insurance status in California from 1997 to 2014. JAMA Oncol. 2018;4(3):317–23.
Sun W, Cheng M, Zhuang S, et al. Impact of Insurance Status on Stage, Treatment, and Survival in Patients with Colorectal Cancer: A Population-Based Analysis. Med Sci Monit. 2019;25:2397–418.
de Moor JS, Cohen RA, Shapiro JA, et al. Colorectal cancer screening in the United States: Trends from 2008 to 2015 and variation by health insurance coverage. Prev Med. 2018;112:199–206.
Freeman VL, Naylor KB, Boylan EE, et al. Spatial access to primary care providers and colorectal cancer-specific survival in Cook County Illinois. Cancer Med. 2020;9(9):3211–23.
Chien LC, Deshpande AD, Jeffe DB, et al. Influence of primary care physician availability and socioeconomic deprivation on breast cancer from 1988 to 2008: a spatio-temporal analysis. PLoS One. 2012;7(4):35737.
Donohoe J, Marshall V, Tan X, et al. predicting Late-stage breast cancer diagnosis and receipt of adjuvant therapy: Applying current spatial access to care methods in Appalachia. Med Care. 2015;53(11):980–8.
Edwards BK, Ward E, Kohler BA, et al. Annual report to the nation on the status of cancer, 1975–2006, featuring colorectal cancer trends and impact of interventions (risk factors, screening, and treatment) to reduce future rates. Cancer. 2010;116(3):544–73.
Zauber AG, Winawer SJ, O’Brien MJ, et al. Colonoscopic polypectomy and long-term prevention of colorectal-cancer deaths. N Engl J Med. 2012;366(8):687–96.
Ladabaum U, Dominitz JA, Kahi C, et al. Strategies for colorectal cancer screening. Gastroenterology. 2020;158(2):418–32.
White A, Thompson TD, White MC, et al. Cancer Screening Test Use—United States, 2015. MMWR Morb Mortal Wkly Rep. 2017;66(8):201–6.
Meester RG, Doubeni CA, Lansdorp-Vogelaar I, et al. Colorectal cancer deaths attributable to nonuse of screening in the United States. Ann Epidemiol. 2015;25(3):208-213e1.
Behavioral Risk Factor Surveillance System. 2010 Codebook Report. Centers for Disease Control and Prevention 2011.
Schneider KL, Clark MA, Rakowski W, et al. Evaluating the impact of non-response bias in the behavioral risk factor surveillance system (BRFSS). J Epidemiol Community Health. 2012;66(4):290–5.
Doubeni CA, Laiyemo AO, Reed G, et al. Socioeconomic and racial patterns of colorectal cancer screening among Medicare enrollees in 2000 to 2005. Cancer Epidemiol Biomarkers Prev. 2009;18(8):2170–5.
Carethers JM, Doubeni CA. Causes of socioeconomic disparities in colorectal cancer and intervention framework and strategies. Gastroenterology. 2020;158(2):354–67.
Mohan G, Chattopadhyay S. Cost-effectiveness of leveraging social determinants of health to improve breast, cervical, and colorectal cancer screening: a systematic review. JAMA Oncol. 2020;6(9):1434–44.
Kurani SS, McCoy RG, Lampman MA, et al. Association of neighborhood measures of social determinants of health with breast, cervical, and colorectal cancer screening rates in the US Midwest. JAMA Netw Open. 2020;3(3):200618.
Cole AM, Jackson JE, Doescher M. Urban-rural disparities in colorectal cancer screening: cross-sectional analysis of 1998–2005 data from the Centers for Disease Control’s Behavioral Risk Factor Surveillance Study. Cancer Med. 2012;1(3):350–6.
Winawer SJ, Zauber AG, Ho MN, et al. Prevention of colorectal cancer by colonoscopic polypectomy. The National Polyp Study Workgroup. N Engl J Med. 1993;329(27):1977–81.
Siegel RL, Sahar L, Robbins A, et al. Where can colorectal cancer screening interventions have the most impact? Cancer Epidemiol Biomarkers Prev. 2015;24(8):1151–6.
Mandelblatt JS, Stout NK, Schechter CB, et al. Collaborative modeling of the benefits and harms associated with different us breast cancer screening strategies. Ann Intern Med. 2016;164(4):215–25.
National Institutes of Health, National Cancer Institute. Cancer Stat Facts: Female Breast Cancer. 2021. Available at: https://seer.cancer.gov/statfacts/html/breast.html. Accessed 26 Apr 2021.
Blumen H, Fitch K, Polkus V. Comparison of treatment costs for breast cancer, by Tumor Stage and type of service. Am Health Drug Benefits. 2016;9(1):23–32.
Subramanian S, Trogdon J, Ekwueme DU, et al. Cost of breast cancer treatment in Medicaid: implications for state programs providing coverage for low-income women. Med Care. 2011;49(1):89–95.
Hall IJ, Tangka FKL, Sabatino SA, et al. Patterns and trends in cancer screening in the United States. Prev Chronic Dis. 2018;15:E97.
Tatalovich Z, Zhu L, Rolin A, et al. Geographic disparities in late stage breast cancer incidence: results from eight states in the United States. Int J Health Geogr. 2015;14:31.
Verdial FC, Etzioni R, Duggan C, et al. Demographic changes in breast cancer incidence, stage at diagnosis and age associated with population-based mammographic screening. J Surg Oncol. 2017;115(5):517–22.
Harding C, Pompei F, Burmistrov D, et al. Breast cancer screening, incidence, and mortality across US counties. JAMA Intern Med. 2015;175(9):1483–9.
Obeng-Gyasi S, Timsina L, Bhattacharyya O, et al. Breast cancer presentation, surgical management and mortality across the rural-urban continuum in the national cancer database. Ann Surg Oncol. 2020;27(6):1805–15.
Elmore JG, Etzioni R. Effect of Screening Mammography on Cancer Incidence and Mortality. JAMA Intern Med. 2015;175(9):1490–1.
Das B, Feuer EJ, Mariotto A. Geographic association between mammography use and mortality reduction in the US. Cancer Causes Control. 2005;16(6):691–9.
Cooper GS, Yuan Z, Bowlin SJ, et al. An ecological study of the effectiveness of mammography in reducing breast cancer mortality. Am J Public Health. 1998;88(2):281–4.
Funding
Adrian Diaz receives funding from the University of Michigan Institute for Healthcare Policy and Innovation Clinician Scholars Program, and received salary support from the Veterans Affairs Office of Academic Affiliations during the conduct of this study/
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
DISCLOSURE
Chelsea Herbert, Alessandro Paro, Adrian Diaz, and Timothy M. Pawlik have no disclosures to declare.
Disclaimer
This study does not necessarily represent the views of the United States Government or the Department of Veterans Affairs.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Herbert, C., Paro, A., Diaz, A. et al. Association of Community Economic Distress and Breast and Colorectal Cancer Screening, Incidence, and Mortality Rates Among US Counties. Ann Surg Oncol 29, 837–848 (2022). https://doi.org/10.1245/s10434-021-10849-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-021-10849-7