Abstract
Amorphous solid dispersions enhance solubility and oral bioavailability of poorly water-soluble drugs. The escalating number of drugs with poor aqueous solubility, poor dissolution, and poor oral bioavailability is an unresolved problem that requires adequate interventions. This review article highlights recent solubility and bioavailability enhancement advances using amorphous solid dispersions (ASDs). The review also highlights the mechanism of enhanced dissolution and the challenges faced by ASD-based products, such as stability and scale-up. The role of process analytical technology (PAT) supporting continuous manufacturing is highlighted. Accurately predicting interactions between the drug and polymeric carrier requires long experimental screening methods, and this is a space where computational tools hold significant potential. Recent advancements in data science, computational tools, and easy access to high-end computation power are set to accelerate ASD-based research. Hence, particular emphasis has been given to molecular modeling techniques that can address some of the unsolved questions related to ASDs. With the advancement in PAT tools and artificial intelligence, there is an increasing interest in the continuous manufacturing of pharmaceuticals. ASDs are a suitable option for continuous manufacturing, as production of a drug product from an ASD by direct compression is a reality, where the addition of multiple excipients is easy to avoid. Significant attention is necessary for ongoing clinical studies based on ASDs, which is paving the way for the approval of many new ASDs and their introduction into the market.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
One of the most significant hurdles in bringing a new drug candidate to the market is poor aqueous solubility, consequent low dissolution rate, and poor oral bioavailability. This has become more pronounced with the arrival of combinatorial tools and high-throughput technologies for screening for the medicine discovery phase (1). The proportion of molecules that face this challenge, most commonly belonging to BCS class II and IV, is rising with each passing year (2,3,4). Low dissolution rate and poor bioavailability have an impact on the marketability of these drugs, with limited formulation strategies available to address the challenges (5), especially for BCS class II drugs, which display dissolution-limited absorption (6).
For a drug to be absorbed via the gastrointestinal epithelium, the dosage form first disintegrates, and the drug dissolves in the gastrointestinal fluids. To make this possible, newer formulation strategies need to be applied to enhance dissolution rate and solubility (1). There are multiple approaches that can be employed to achieve these goals, including prodrug formation (7), complexation (8), micronization (9), salt formation (10), micelles (11), nanoemulsions (12), solid–lipid nanoparticles (13), and nanocrystals (14). One strategy is to employ supersaturation-based formulations (15). A supersaturated solution is formed when the total solute concentration surpasses the equilibrium solubility. The augmented concentrations attained through the formation of a supersaturated solution consequently enhance the oral bioavailability of the molecule. A key drawback of a supersaturated solution is its metastability and the intrinsic inclination for the drug candidate to crystallize; thus, the solubility advantage is lost. One of the supersaturating formulation strategies, the amorphous solid dispersion (ASD), comprises a mixture of both amorphous drug and polymer at the molecular level, with increasing oral bioavailability in comparison to crystalline systems (16,17,18,19).
Although the precise factors that improve the dissolution of drug molecules from an ASD that lead to the formation of supersaturated solutions are not yet fully deciphered (Fig. 1), it has already been identified that the polymer employed in the formation of the ASD plays an essential role in facilitating drug release from the ASD and in delaying consequent crystallization (20). This is especially significant for drugs that crystallize rapidly because once crystallization begins, solubility enhancement is compromised as the supersaturation level goes down. Therefore, the polymer employed in an ASD should possess both hydrophobic and hydrophilic moieties to prevent crystallization of the drug in the aqueous environment while also facilitating drug release from the ASD (21,22,23).
Although the concept of ASDs has created immense interest within the scientific community, this has not been translated into the desired commercial success. ASD-based formulations that have reached the market remain in double digits. This low number originates from problems with scale-up and instability of the ASD during the manufacturing process (24, 25). The experimental screening of different candidates as polymeric carriers while developing an ASD system is a slow, tedious, and costly process. Another difficulty lies in ensuring long-term product physical stability, as drug recrystallization from its initial amorphous state and phase separation between the drug and polymeric carrier can cause unacceptable variations in oral bioavailability (26). Even though ASDs came into existence more than half a century ago, the concepts of formation and physical stability of ASDs are still not fully understood. Accurately predicting interactions between the drug and polymeric carrier requires long experimental screening methods. As a result, product development is attained through trial-and-error methods that end up increasing cost and stretching timelines (27). The time can be lessened by acquiring suitable knowledge about the behavior of ASD formation, dissolution, and subsequently drug release from the carrier matrix. This is where molecular modeling tools come into the picture. Computational tools hold the potential to act as a novel paradigm in the research and development of ASDs.
Technologies that may be employed to manufacture ASDs include hot melt extrusion (HME), KinetiSol®, spray drying, supercritical fluid (SCF) technology, and electrospinning (28). HME is an organic solvent-free continuous operation in which a physical mixture of active pharmaceutical ingredient (API) and polymeric carrier is melted, extruded, and solidified, with varying processing parameters which include feed rate, temperature, shear force, die size, geometry, screw type, and speed (29, 30). KinetiSol® is a novel high shear-based technology that also employs the fusion principle wherein shear force and friction rapidly transform the physical mixture into the melted state to give a homogeneous ASD (19). Spray drying is another technology commonly employed in the production of ASD systems. Spray drying is a fast-drying process that causes kinetic entrapment of the API in the amorphous state. Spray drying conditions, such as solvent content, can have a significant influence on spray-dried dispersion characteristics (31). It has been proven that supercritical fluid technology maintains polymeric structure more than any other methodology, and it is a one-step process. It may be utilized at low temperatures, enabling thermolabile drugs to be processed without surpassing the glass transition temperature (Tg). The residual solvent content in processed samples is kept to a bare minimum (32). Electrospinning (ES) is a unique technique for making ASDs out of a polymer mixture or melt. Using ES, micro- and nanometric polymer fibers are created by the generation and elongation of an electrified fluid element. ES, in contrast to the abovementioned ASD-producing techniques, functions at ambient temperatures, making it a mild process at a low cost. The API is distributed in a polymer matrix at the molecular level, resulting in a nano-scale amorphous solid dispersion in electrospun fibers with a large surface area (33).
Continuous manufacturing refers to the production of a pharmaceutical product in a single continuous process. The entire process takes place in one location, from beginning to end, with no waiting times. Continuous manufacturing is a more flexible method than batch processing that allows for better production scaling. Generally, high-volume goods drive the adoption of continuous processing, which is the motivation for using continuous processes mostly in the commodity chemical industry. While high capacity is still an important aspect of continuous manufacturing, reducing development costs for novel drugs and increasing flexibility to create capabilities of tailored therapeutics for specific patient populations are other factors for the shift from batch to continuous manufacturing (34). Continuous manufacturing offers high-quality products as the whole process may be controlled using process analytical technology (PAT).
This review addresses new advances in the field of ASDs that aim to overcome the issues that limit the marketability of such formulations and considers new approaches that can enable the formulation of ASDs with more confidence. Special emphasis has been given to molecular modeling techniques that can be used to address some of the burning questions related to ASDs today. It also throws new light upon the continuous manufacturing techniques that can overcome the challenge of scale-up for ASDs.
Amorphous Solid Dispersions and Mechanism of Enhanced Dissolution
Amorphous materials exist in a thermodynamically metastable state, and because of the significantly higher free energy compared to crystalline solids, amorphous forms are more soluble (35). Amorphous materials may exist as supercooled liquids that can be achieved by fast cooling of a melt. As the material is further cooled, the molecular mobility is gradually reduced, and the viscosity increases simultaneously. The temperature at which this transition happens is called the glass transition temperature (Tg), and below the Tg the material is called “glassy” (35, 36). The Tg is related to alterations in a number of thermodynamic parameters, including enthalpy, entropy, and volume (36).
ASDs represent a promising formulation strategy to increase the aqueous solubility and dissolution rate and oral bioavailability of poorly water-soluble drugs (37). In an ASD, the API, which is initially crystalline and hydrophobic, is made to disperse in a carrier matrix that is hydrophilic in nature. This strategy offers advantages of amorphization associated with decreased particle size and enhanced wettability (38). For example, Harmon et al. performed research on the mechanism of dissolution-induced nanoparticle formation from a copovidone-based solid dispersion. The surfactant inside the ASD particle inhibited “hydrophobic capture,” a process that resulted in fast, local drug domain aggregation. This inhibition enabled amorphous drug domains to diffuse into the bulk solution where they were characterized as nanoparticles (42). Similarly, Han F et al. investigated the impact of phase separation morphology on the mechanism of drug release from ASDs and found that release at low drug loadings was influenced by erosion of the polymer and embedded drug-rich droplets (39), while at high drug loadings, the creation of a drug-rich domain continuous morphology resulted in the preferential release of polymer-rich domains (43).
ASDs hold the potential to address bioavailability issues as the drug molecule exists in its amorphous form, which is known to have higher solubility. This solubility enhancement, along with higher rates of dissolution and improved solid-state stability, can be accomplished by the selection of a suitable polymeric carrier. The spring and parachute concept was explained, where a higher spring effect (dissolution) and enhanced parachute effect (crystallization inhibition) were observed (40). The “spring and parachute” mechanism of enhanced dissolution by amorphous solid dispersions is depicted in Fig. 2, with the polymer providing the parachute, which maintains the supersaturation of the drug. “Spring” is a descriptive word for the initial drug dissolution. After supersaturation is achieved, liquid-liquid phase separation or drug crystallization can causes drug concentration to decrease, and interaction of drug and polymer is required in order to provide a “parachute” and maintenance of drug supersaturation (41). The spring and parachute must be thoroughly adjusted so that an appropriate degree of drug supersaturation can be achieved (an optimal spring) and sustained over time (an effective parachute) (42). The polymeric carrier also plays a vital role in stabilizing the ASD system in the solid state also, by decreasing the molecular mobility and increasing its Tg, maintaining the drug in the amorphous state. The stability of such a system is influenced by the drug-polymeric carrier interactions and intermolecular interactions in the drug’s crystal lattice.
Absorption of drugs from ASD is a multistep process that has three stages. In the first step, the ASD undergoes dissolution in the surrounding medium, followed by the uptake across the intestinal membrane of the solubilized drug from the medium, with the final step causing the drug to attain equilibrium of drug in the drug solution (43). During dissolution, the ASD system exists in a state of metastable equilibrium such that, due to the lack of any crystalline substance, a transition state between the drug’s amorphous phase and its solution form exists. Drug-rich particles are said to be naturally metastable in an amorphous liquid phase transition. The amorphization contributes to a better dissolution as amorphous compounds possess higher energies and apparent solubilities as compared to their crystalline counterparts. This is due to their disordered structure and higher energetic state, which does not have the prerequisite of breaking down the crystal lattice before dissolution (44). A crucial step in the enhanced dissolution profile of the drug is the formation of dissolved ASD, as it is directly associated with oral bioavailability. Two possible mechanism of drug release from an ASD are (a) carrier-controlled release and (b) drug-controlled release, which have been proposed to explain the mechanism of dissolution of ASD (45, 46). The diagrammatic representation of the overall enhancement of aqueous solubility and oral bioavailability by ASDs is depicted in Fig. 3.
Carrier-Controlled Release
In carrier-controlled release, polymer employed does not dissolve, and after ingression of dissolution medium, they form a viscous gel like structure. This viscous gel layer structure shows two layers; one is diffusion layer (between dissolved and undissolved API), and another is erosion layer (between viscous gel and dissolution medium) (47). Erosion and release of drug from these layers depends on the nature and interaction of drugs and polymers (48). There are multiple reports where carrier-controlled release is found congruent. Indulkar et al. studied that hydrophilic polymer shows carrier-controlled release at low drug loading (22). Saboo et al. observed the formation of nano-droplets through the amorphous liquid phase separation (ALPS). Nanodroplets are drug-rich aggregates which forms when the drug amorphous solubility is exceeded and ALPS happens (49). It has been observed that some ASDs with a low drug loading dissolve to a concentration higher than the amorphous solubility of the drug which leads to ALPS. This ALPS further cause generation of drug-rich amorphous aggregates of nanometer size. These aggregates are colloidal in nature, and they coexist with the aqueous phase. The aqueous phase already contains drug concentration equivalent to the amorphous solubility. Once the dissolved drug absorbs, these aggregates release drug in to the medium and maintains the amorphous solubility and membrane flux (47).
Drug-Controlled Release
In drug-controlled release, the employed polymer dissolved completely, and due to which no viscous gel layer formation happens (46). As the polymer and drug dissolves at different rates (noncongruent), super-saturation happens at fast pace which further increases the chances for crystallization. Amorphous drug-rich aggregate (nano-droplet) formation does not happen in this scenario as amorphous drug state is not stable. Indulkar et al. and Saboo et al. observed that hydrophilic polymer shows drug-controlled release at high drug loading (22, 48, 49).
Amorphous Solid Dispersion Development.
ASDs represent a formulation approach that has been extensively used to improve drug solubility, enhance oral bioavailability, and mask taste. One or more active pharmaceutical ingredients (APIs) are distributed in a nonreactive polymer or matrix (50). It is recognized that molecular level mixing with a polymer of hydrophilic nature improves the release of poorly water-soluble chemicals from ASDs. The polymer type and drug loading in the ASD have been proven to affect the release rate. Rapid release of ASD components happens in some cases, often with minimal drug loading, resulting in apparent solution concentrations greater than the amorphous solubility of the drug (51). Figure 1 describes the factors affecting the development of ASDs. Cho and co-workers 3D-printed orodispersible films loaded with amorphous olanzapine (52). Tres et al. generated amorphous materials from supersaturated aqueous solutions of ritonavir and lopinavir by antisolvent addition and showed that the dissolution of both the drugs was improved when made into ASDs compared to the crystalline form (53). Feng et al. focused on using an ASD-based polymer-surfactant system to improve the aqueous solubility and oral bioavailability of itraconazole and efavirenz (54). Kwon et al. used a spray drying process, where a hydrophilic polymer was successfully employed to incorporate the hydrophobic drug atorvastatin, into solid dispersions. Atorvastatin in the ASD form resulted in higher solubility and an improved dissolution profile compared to the crystalline drug (55). Solid dispersions of dolutegravir prepared by quench cooling and solvent evaporation methods showed increased bioavailability over its crystalline equivalent (56). Posaconazole kinetic solubility was improved by ASDs prepared by solvent evaporation, which resulted in an improved dissolution and bioavailability compared to the crystalline free drug (57). Figueirêdo et al. employed the ASD approach to combine two synergistic antichagasic drugs, posaconazole, and benznidazole, in the amorphous form demonstrating improved solubility and potentially enhanced bioavailability (58). In one study, it was found that using HME technology to prepare ASDs of lacidipine with Soluplus and PVP VA64 improved the drug’s solubility and bioavailability (59). ASDs prepared using the KinetiSol technology improved abiraterone’s solubility and pharmacokinetics (60). Ketoconazole was converted into an amorphous state with drug-polymer interactions, which yielded positive results (61). The researchers prepared PVAs with varying levels of cross-linking and hydrolysis, which were then evaluated in their solid dispersion formulations with amenamevir and looked into the differences in solubility improvement produced by different degrees of hydrolysis and degrees of polymerization (62). Candesartan and cilexetil ASDs were successfully developed using a ball milling approach (63). Quercetin ASDs were prepared using HME, which resulted in an increased dissolution rate and oral bioavailability. Similarly, celecoxib ASDs prepared by hot melt extrusion showed an improved dissolution rate (64). Ibuprofen ASDs generated using supercritical fluid technology showed improved absorption and oral bioavailability (65). Alhayali et al. investigated the ASD formulations of ezetimibe and the supersaturation-precipitation-permeation interactions and bioavailability increase of the API (66). The wettability improvement and bioavailability enhancement proved the success of the ASD approach in improving griseofulvin (GF) release from a ternary GF-Soluplus-SDS ASD (67). Solvent evaporation was used to create lacidipine-spironolactone co-amorphous solid dispersion (LCDP-SPLCASDs) systems. In vitro release characteristics and physical stability were improved in the LCDP-SPLC ASDs systems compared to free drugs (68). These studies demonstrate that ASDs is a promising technique to fine-tune the release of drugs that are poorly soluble.
Due to the unique benefits and qualities of ASDs, the pharmaceutical industry has become extremely interested in methods for their manufacture. For instance, academics have been interested in HME, an environmentally friendly technique, because of its capacity for continuous manufacturing. However, the industry also recognizes the value of spray drying for manufacturing solid dispersions which cannot be handled by HME. HME is not suitable for heat sensitive drugs and polymers with higher heat processing temperatures, a drawback that can often be resolved by using plasticizers. The KinetiSol® dispersion technology is a revolutionary alternative thermal processing method that relies on the combinatorial principle of shear force and friction to quickly turn the physical mixture into a molten state and create a homogenous ASD. The physicochemical characteristics of the drug and the polymers required to produce a thermally and chemically stable product must be considered when choosing an effective technique for manufacturing ASDs. Himawan et al. formulated ASDs of BCS class II drug valsartan by solvent evaporation to increase its oral bioavailability (69). Muller et al. formulated regorafenib amorphous solid dispersions to increase the biopharmaceutical performance (70). Similarly lumafentrine (71), filgotinib (72), atorvastatin (73), celecoxib (74), berberine (75), and tacrolimus (76) ASDs were prepared using solvent evaporation to enhance their biopharmaceutical properties. Nieto et al. prepared ASDs by a solvent casting method for solubility enhancement of fenretinide (77). Ewings et al. prepared ASDs of indomethacin using HME to increase the solubility (78). Sarode et al. enhanced the aqueous dissolution and biphasic partitioning by preparing ASDs of felodipine (79). Jijun et al. prepared nimodipine ASDs by HME with polyvinylpyrrolidone/vinyl acetate copolymer to increase the dissolution (80). Hassouna et al. prepared ASDs of ibuprofen by an emulsification-diffusion method to enhance its biopharmaceutical properties (81). Similarly ascorbic acid ASDs was prepared by Christina and co-workers (82). Paclitaxel ASDs were also prepared by freeze drying (83). Thombre et al. prepared ASDs of ziprasidone to enhance its solubility (84). Kim et al. increased the bioavailability of clopidogrel by preparing ASDs (85). In the same way sibutramine, ASDs were prepared by spray drying to enhance its biopharmaceutical properties (86). Deng et al. prepared ferulic acid ASDs by electrospinning (87). Mehanna et al. prepared ASDs of tadafil by a fusion method for dissolution enhancement (88). Similarly, many more APIs were made into ASDs by different technologies as reported in Table I.
Trend of Continuous Manufacturing of Pharmaceuticals
Over the last two decades, there has been a steep rise in the reports in the scientific literature on continuous manufacturing (Fig. 4).
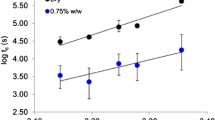
When applying the term “continuous manufacturing” to “pharmaceuticals,” a similar trend with respect to the scientific literature was observed, with exponential growth from 2017 onwards (Fig. 5), reflecting increasing adaptation of continuous processing in pharmaceutical manufacture.
Continuous Manufacturing for ASDs
Amorphous materials can be manufactured using processes that can be categorized into three different types: solvent evaporation, melt-cool, mechanical procedures using a ball mill, etc. The difference between batch and continuous manufacturing is illustrated in Fig. 6. Hot melt extrusion (89) and KinetiSol technology (19) currently appear to be the most promising techniques for continuous manufacturing of ASDs. HME is a stable technique that can enable the production of ASDs without the use of solvents. Additionally, HME is a continuous process that is easily expanded from a small-scale laboratory extruder to production-scale machinery. For research, validation, manufacture, and maintenance, this approach is thought to be cost-efficient. For example, Thiry et al. performed an experiment that explored HME as a continuous technique to create cyclodextrin inclusion complexes in order to improve itraconazole’s solubility and dissolution rate (90). Similarly, Maniruzzaman et al. reported that the HME technique demonstrated its processing abilities to develop different solid dosage forms, like pellets, capsules, films, or tablets (91). KinetiSol is another technology that quickly converts the physical mix into a melted form and produces a uniform solid dispersion and can also be used for continuous manufacturing. Similarly, LaFountaine et al. prepared ASD of ritonavir-polyvinyl alcohol by KinetiSol technology (92). Gala and coworkers prepared the amorphous solid dispersions of abiraterone and hydroxypropyl beta cyclodextrin by KinetiSol technology (16). The physicochemical characteristics of the API and the polymers that can result in a product that is physically and thermally stable are the basis for the choice of an optimal technique for preparing ASDs(19, 93).
Continuous manufacturing methods are well suited to the production of active pharmaceutical components as well as the manufacture of final dosage forms. Ivacaftor, an API from Vertex Pharmaceuticals, has relatively poor dissolution characteristics and bioavailability in the crystalline form. Vertex generated ASDs of ivacaftor using both spray-drying and HME, which showed improved dissolution and oral bioavailability. Continuous manufacturing processes are suitable for ASDs due to high-quality criteria and good manufacturing practice norms. Several pharmaceutical companies have recently focused their attention on the continuous processing in pharmaceutical production. The FDA sees continuous processes as having a lot of potential since they can open new avenues for producing high-quality medicinal products. Increasing yields in production is a difficult task which can be achieved by continuous manufacturing techniques, where the manufacturing is controlled using artificial intelligence and PAT tools. Continuous manufacturing of drug-loaded ASDs also gives new possibilities for automation (94).
Hot-Melt Extrusion
Hot-melt extrusion (HME) is one of the most popular methods for manufacturing amorphous solid dispersions. In HME, an extruder feeds raw materials into an apparatus with one or two revolving screws that are heated to varying temperatures, after which the material is treated and fed through a die to generate the desired shape and size. Muvva et al. reported increased bioavailability of apremilast when processed by the HME method (95, 96). Similarly, Lee et al. also performed research on improving the solubility and bioavailability of rivaroxaban (RXB) which is poorly water-soluble. They prepared RXB-containing hot-melt extruded ASD (HME-ASD) by altering the API: polymer (polyvinyl pyrrolidone-vinyl acetate 64) ratio and barrel temperature (1:1–1:4) (200–240°C). Solomon et al. worked on felodipine to form ASDs by the HME process without the use of a solvent (97). Emam et al. generated meloxicam ASD by HME, which resulted in an improvement in dissolution and bioavailability (98). Using HME technology, researchers built a microenvironment pH-modulated ASD system of telmisartan. The microenvironment pH adjustment produced by the inclusion of an alkalizer was one of the reasons for the improved solubility, bioavailability, better wettability, and increased drug release in a favorable pH environment (99). One-step co-extrusion as a continuous production process in ASD manufacture is growing rapidly in the industry and academia. In one study, Maniruzzaman et al. used magnesium alumina metasilicate as a carrier for continuous extrusion processing to create ASDs of indomethacin which showed enhanced solubility and dissolution rate. Under stability studies, the extruded solid dispersions displayed good flowability and physical properties without indomethacin crystallization or changes in physical stability (100). A one-step HME technique was used to successfully manufacture an ASD of nisoldipine with Kollidon VA64. It disintegrated faster when compared to commercial tablets and their physical mixture (101). These examples show that the process of one-step extrusion will likely be more useful than other commonly used technologies like spray-drying, solvent evaporation method, and fluid bed technology method for continuous manufacturing of ASD-based formulations.
A predictive tool for the selection of various formulation components for ASDs in HME processes is based on Flory-Huggins thermodynamic modeling (102). The Flory-Huggins solution concept is a lattice model of the thermodynamics of mixing polymeric solutions. This theory provides a useful framework for creating an ASD design space (103). Moseson et al. used the Flory-Huggins-based model, where melting temperature depression measurement was used to create the phase diagram for indomethacin and polyvinylpyrrolidone/vinyl acetate copolymer (93). Suryvanshi et al. used this theory for the evaluation of Kollidon®SR matrix–mediated amorphous filament extrusion of norfloxacin prepared by HME (104). The Hildebrand and Scott solubility factor was calculated at 25°C, and the melting point depression of the drugs in polymer blend at the melting temperature was used to determine the Flory-Huggins (F-H) interaction parameter for the drug and polymer at varying temperatures which indicates enthalpic and entropic changes in solubility and defines the thermodynamic features of drug-polymer solutions. Numerous investigations have discovered that, within a small compositional range, fluctuates proportionally to the opposite of the melting point of the drug (105). The Flory–Huggin’s theory of the fusion power of mixing allows for the entropic contributions of polymers and intraspecies interaction; however, the corrective entropy element provided by Hildebrand and Scott has been omitted in the computational techniques that are extensively used for calculations. Turpin et al. highlighted some of the novel in silico screening methods for ASD for troubleshooting solubility parameters, arguing for the adoption of PC-SAFT2 (perturbed-chain statistical associating fluid theory) (102).
Spray-Drying
Spray-drying is a drying method that can produce nano to micron-sized particles in a short period of time. Spray-dryers can turn crystalline starting materials into amorphous products. Ha et al. used spray-dried Eudragit E/HCl, which is a cationic polymer, to create an ASD of trans-resveratrol. The amorphous Eudragit E/HCl solid dispersion displayed supersaturation without precipitation for 48 h. The absolute oral bioavailability of trans-resveratrol solid dispersion was found to be increased (106). Mudie et al. manufactured spray-dried ASD for tablets and achieved improved bioavailability (107). Similarly, Costa et al. proved that spray-drying can be employed as a continuous manufacturing technique suited to the manufacture of ASD-based tablets, and they also stated that skipping the demixing step (API-carrier solubility), which is an alternative to prepared supersaturated API-polymer solid solutions by spray-drying, resulted in a highly supersaturated liquid that delivered efavirenz from ASD formulations in seconds (108). Ziaee et al. prepared ibuprofen ASDs by spray-drying, and they indicated that it would be a suitable technique for continuous manufacturing of ASDs. The ASD gave a higher dissolution rate and solubility profile for ibuprofen than the crystalline drug (109). ASDs of dutasteride were prepared by spray-drying, and the link between supersaturation behavior assessed during dissolution and in vivo absorption improvement was evaluated (110). Raloxifene ASD nanoparticles were successfully generated by spray-drying aqueous solutions, demonstrating a case of green manufacturing as no organic solvents were used or produced in the process (111). The increase in the dissolution rate through the dextrin-based polymer dispersion system, the bioavailability enhancement, and the permeability enhancement by inclusion of SLS resulted in a considerable increase in oral absorption of amlodipine-free base ASD (18). Rivaroxaban-polymer ASDs have shown higher biopharmaceutical efficiency, including solubility and dissolution rate, than crystalline API in a pharmacokinetic trial with in vitro permeability analysis (112). With these examples, it may be reasonably expected that ASDs of other APIs could also be manufactured by spray-drying and that spray drying could be employed in continuous processing of ASDs.
Electrospraying Technology
The electrospraying technique is a relatively new method for producing ASDs. A solution of API and the inert polymer is gently forced through a nozzle to make solid dispersions via electrospraying. The liquid stream becomes highly charged when a high voltage is applied to the nozzle, generating electrostatic stress inside the fluid leaving the nozzle. The electric forces will counteract the surface tension of the liquid when there is enough electric potential between the vessel and the nozzle. A Taylor cone is formed when the meniscus of a liquid drop developing at the nozzle tip deflects into a conical shape. The free surface charges are accelerated and concentrated at the cone’s tip, resulting in the generation of a jet that accelerates downwards before breaking up into droplets, and has a high potential for continuous manufacturing. This technique allows fine-tuning of powder morphological properties and API release characteristics. Smeets et al. explained the utility of electrospraying for the creation of a fixed-dose combination product containing three APIs. Smeets et al. also studied the feasibility of coaxial electrospraying for the creation of gastro-resistant microparticles of darunavir ASD-based formulations. The formulation of darunavir had a burst release, and the API was readily available for dissolution (113). Although researchers have shown that electrospraying can successfully generate ASDs, there have also been reports highlighting the difficulty of electrospraying in the preparation of ASDs. Mohammadi et al. discovered that when clarithromycin ASDs were generated by electrospraying, the medication was only partially amorphized. Similarly, Zhang et al. generated ASDs, which showed significantly improved drug release; however, partial amorphization was detected in the formulation. Apart from the API characteristics, one of the elements that cause inadequate amorphization during electrospraying is the ambient pressure (114). Using coaxial electrospraying, which allows for the generation of highly monodisperse droplets, reducing the number of satellite droplets, a solid core-shell solid dispersion was generated to solve the problem of the low solubility of fenofibrate. Dissolution and gastrointestinal absorption behaviors were greatly improved by the reduction in particle size as well as improvement in dispersion efficiency (115). Electrospraying should be explored further as a general amorphization technology, as it has been demonstrated to be favorable for the amorphization of ketoprofen and many other APIs which cannot be prepared from other methods, which are thermally labile (116). Different polymers typically employed in the formation of solid dispersions have been studied with electrospraying technology and the impact of process variables evaluated. The experiments have assessed the significance of experimental parameters such as the electric potential differential, flow rate, and nozzle tip to collector distance. The nature of the solvent and the quantity of polymeric solutions, concentration, and viscosity are recognized as critical formulation characteristics. This information is critical for rationally designing future electrospraying technologies for creating ASDs (116).
Coprecipitation Method
Coprecipitation means that the API and polymer must quickly shift from one solvent environment to another. In the first environment with a common solvent, both API and the polymer are soluble; however, in the second environment, both are insoluble (common anti-solvent). The polymer-API solid dispersion in the slurry must also be in a glassy state, i.e., the glass transition temperature of the amorphous mixture as plasticized by the anti-solvent environment must be higher than the precipitation temperature. Coprecipitation is the simultaneous precipitation of a normally soluble component (API-polymer) with a macro-component (solvent) from the same solution by forming a mixed composite by adsorption, occlusion, or mechanical entrapment. Sichen et al. produced a sorafenib ASD using coprecipitation technology. They showed that instant-release tablets manufactured using sorafenib ASD resulted in enhanced oral bioavailability (117). Duarte et al. prepared an ASD of carbamazepine, a weakly water-soluble drug with solubility restricted absorption, by a novel solvent-controlled precipitation (SCP) approach called microfluidization to form carbamazepine-amorphous solid dispersions (118). The production of indomethacin-ASD by coprecipitation was carried out by Lim et al. and co-workers, resulting in improved dissolution (119). A curcumin-CaCO3 combination resulted in a significant increase in curcumin solubility when using the coprecipitation approach to create ASDs (120). An ASD formulated with a ratio of 1:10 diosgenin to Soluplus had enhanced solubility and stability. It was made via a coprecipitation technique, and the diosgenin-ASD showed a substantial increase in solubility (121). Wang et al. explained the process of coprecipitation where quercetin ASDs were successfully prepared when employing HPMCAS as a polymeric carrier (122). The coprecipitation-based tablets disintegrated reasonably slower than the spray-dried dispersion-based tablets in dissolution trials, but both attained the full release. The tablets showed comparable dissolution patterns.
PAT Tool-Assisted Continuous Manufacturing
The application of process analytical technology (PAT) in pharmaceutical manufacturing was initiated in 2004 by the US Food and Drug Administration (FDA). PAT supports the transition from batch to continuous manufacturing operations, and an increasing number of organizations are relying on it as a critical component of a real-time product release system. As a result, one of the many advantages that PAT may provide is a reduction in cycle time, faster process design, and faster response to market demand. PAT tools are the framework for designing, analyzing, and controlling production through timely measured data (i.e., during processing) of essential quality and performance characteristics of raw materials, end products, and methods, with the aim of maintaining final product quality (123). PAT tools have primarily been used for the design, analysis, and control of diverse processes involved in production. PAT can be used to provide the necessary information on a range of parameters that could have a substantial impact on several critical quality attributes (CQA). PAT is effective for evaluating the physical and chemical quality of raw materials and finished products, which can lower engineering and production costs. PAT tools have enhanced operational control and amenability, which has led to continual and immediate improvements in product quality. PAT involves evaluating the level of quality at various intermediate (in- or out-line processing) stages and ensuring transfer of quality to the final product. This technology has become a revolutionary instrument in the industrial sector and is the subject of extensive research.
Continuous manufacturing is emerging as next-generation manufacturing and will be widely accepted by pharmaceutical industries with the help of advanced PAT tools (Fig. 7) (124). The key objectives of PAT tools are to improve process understanding and real-time quality monitoring (125). PAT techniques, such as spectral sensors and chemometric models, are used to check product quality in real-time. In the pharmaceutical sector, as shown in Fig. 8 (126), near-infrared spectroscopy has been and continues to be widely utilized to check product quality during continuous manufacturing procedures (123, 127). Similarly, Raman spectroscopy is also one of the PAT technologies where method compatibility, validation, and convenience of use are all factors to consider when using Raman spectroscopy for pharmaceutical solids analysis. Fiber-optic probes are used in PAT Raman spectroscopy, with fiber designs with low separation between the activation and collection fibers (128). PAT tools make the process easier to monitor throughout, from raw material introduction to the finished products (Fig. 7). For example, in HME, in-line UV-Vis was employed as a quick PAT instrument to identify critical process parameters (CPPs) and their critical quality attributes (CQAs). A systematic strategy based on the continuous design of experiments was utilized to screen, optimize, and verify processing conditions using multivariable statistical analysis (CQAs) (129, 130). In the same way, Korasa et al. gave an overview of PAT in the monitoring of film coating unit operations (131). Galata et al. employed a PAT tool for monitoring continuous blending processes for tablets, including the steps of dry granulation (132), wet granulation (132), tableting (132, 133), and film coating (131). Chalbani et al. also incorporated NIR spectroscopy as a PAT tool for moisture content determination (134). Silva et al. used PAT tools for monitoring the coating of microspheres in a bench scale fluid bed dryer (135) and continuous manufacturing of tablets (136). Krier et al. developed PAT tools capable of monitoring four CQAs involved in implant manufacturing. PAT instruments, both in-line and off-line (using Raman imaging), offered great insights into the process and could be effectively integrated into a real-time release or expedited release strategy (137). A PAT system built on digital photography was utilized for continual blending processes with a colorful API (riboflavin, RI). It was shown that this method could measure the RI at levels as low as 0.05 w/w percent (138). The comparable UV/Vis imaging-based techniques can be utilized to gather real-time data on the product quality; therefore, the proposed system might develop into a PAT tool (139). Similarly, the design of a multivariate light induced fluorescence PAT tool for in-line quantification of pharmaceutical substances (140). Chavez et al. performed optimization of a pharmaceutical tablet formulation based on a design space approach and using vibrational spectroscopy as a PAT tool. The above examples shown how PAT can be used in the production of different pharmaceutical dosage forms and can also help in continuous manufacturing of amorphous solid dispersions. The potential use of PAT tools in ASD and final dosage form continuous manufacturing is shown in Figs. 7 and 8.
Medicines Commercially Available as ASDs
ASD-based formulations are commercially viable and have been shown to be well accepted in terms of safety. ASD manufacturing technologies such as HME or spray drying are ideal for continuous manufacturing if well assisted by the necessary PAT tools. MICARDIS is a commercially marketed telmisartan product. Giri and his co-workers combined the API with Soluplus, 30–90% w/w, by a HME method. Giri and his colleagues used an ASD-based drug delivery strategy to improve telmisartan’s solubility, dissolving, and pharmacokinetic properties, and thus, the dose could be reduced up to 5.34-fold (99). The extended-release tablet, Envarsus XR®, used in conjunction with other drugs to help prevent organ rejection in kidney transplant recipients, was prepared by melt extrusion technology, with different polymers at a 10% w/w drug loading (tacrolimus), and it is one of the marketed formulations in the form of amorphous solid dispersions (141). Table II summarizes the US Food and Drug Administration (FDA)-approved marketed products based on ASDs. There has been an increase in the number of ASDs under development and reaching the market over the last decade. Lynparza (olaparib), Belsomra (suvorexant), Mavyret (glecaprevir/pibrentasvir), Venclexta Viekira Pak (ombitasvir/paritaprevir/ritonavir), and Onmel (itraconazole) are all ASD-based formulations where the ASD is prepared by HME (142). Stivarga (regorafenib), Zepatier elbasvir/grazoprevir, Isoptin (verapamil), Kaletra (lopinavir/ritonavir), Orkambi (lumacaftor/ivacaftor), Zortress (everolimus), Prograf (tacrolimus), Intelence (etravirine), Epclusa (sofosbuvir/velpatasvir), Harvoni (ledipasvir/sofosbuvir), Kalydeco (ivacaftor), and Incivek (telaprevir) are some examples of marketed formulations of ASDs prepared by spray drying (142). Zelboraf is an ASD-based formulation of vemurafenib where the ASD is prepared by solvent-antisolvent precipitation (142). These are some of the commercially available dosage forms of ASDs listed in Table II. According to the trend, the most frequently used preparation methods for ASDs in marketed products are HME and the spray-drying method.
Molecular Modeling For ASDs
Molecular modeling is a vast research field; the two most frequently applied elements of computational modeling are molecular docking and molecular dynamics simulations, both of which have proved critical in the rapid identification of prospects for in vitro and in vivo assessment, as shown in Fig. 9 (143).
Virtual screening using molecular docking identifies hit compounds with both the highest binding affinity and correct binding interactions. The lack of or incorrect simulation of receptors’ flexibilities is sometimes a drawback (144). There have been simulations which are reported abnormal transit-time dispersion using multiple-trapping Monte Carlo methods. Monte Carlo algorithm makes use of multiple exponential allocation trapping. The findings of the simulations are the change from nondispersive to dispersive transients as a function of temperature is the result of repeated carrier entrapment and disrupted surface release (145). The implementation of the Monte Carlo algorithm-based simulation of surface dynamics has criteria for choosing which atoms are permitted to be moved about during the simulation and for determining how many MMC cycles should pass before the simulation is terminated (146). Molecular modeling involves model building and computation to study molecular structure and functions. Modeling of molecular systems is often carried out through quantum mechanics (QM), molecular mechanics (MM), and hybrid QM/MM that describes molecular energies and geometries using cumulative physical forces. Molecular dynamics encompasses the observation of system behavior over time using molecular mechanics (147). Molecular dynamics is a significant computational tool for deducing the function of biological macromolecules, the physical basis of the structure, and the dynamic evolution of the system (148). Molecular simulations have the potential to serve as a significant tool for the future development of ASDs as molecular modeling, when applied to ASDs, enables one to observe the microscopic interactions of the system and extrapolate them to macroscopic scales to better predict physical stability and phase separation. Thus, microscopic mechanisms can be associated with collective properties of the system (149,150,151,152,153).
In an ASD, the active pharmaceutical ingredient (API) dispersed in the polymeric carrier undergoes nonbonding interactions such as van der Waals, acid-base/ionic, dipole-dipole, and hydrogen bonding. These interactions are not only responsible for preventing self-association between like molecules but also play a significant role in promoting the physical stability of the ASD via enhancement in API-carrier interaction energy (154,155,156). Determining the extent and types of such interactions helps understand the miscibility between the API and carriers.
Docking Studies
Docking studies are generally helpful in generating favorable preliminary binding confirmations between the API and the polymeric carrier in an ASD system. Molecular docking simulations help in more in-depth analysis and energy refinement of the constituents post rapid screening and scoring via docking studies (157). Fule et al. performed docking studies of the antimalarial lumefantrine and polymers Kollidon VA-64 and Soluplus. The docking results showed a strong hydrogen bond between the drug’s hydroxyl, amine, and chlorine groups and the monomers of vinylpyrrolidone-vinyl acetate and Soluplus (158). Docking can also screen the stable tautomers before applying MD simulations. In one such study, Gangurde et al. used docking to analyze the binding energy of keto-enol and diketo forms of curcumin with Eudragit EPO. It was found that the diketo tautomer was more stable, with binding primarily being governed by van der Waal’s forces. MD simulations were then applied after these docking studies, which afforded a more comprehensive structural insight into the interactions between curcumin-Eudragit EPO (159). Macháˇcková et al. undertook a detailed docking study wherein they performed systematic docking simulations with chitosan, L/D-polylactide, PEG, polyglycolic acid, and cellulose with cyclosporin A. Each extensible polymer produced a million complexes with static cyclosporin A. Based on the binding energy, cellulose and chitosan were expected to be more miscible with cyclosporin A (160).
Molecular Dynamics (MD)
ASDs are large and complex systems, and studying such systems requires advanced tools. Molecular dynamics (MD) is a tool that facilitates the study of such phenomena from a more physically realistic point of view. The application of MD necessitates that all constituent components of the system are parametrized by a molecular mechanics-based force field assigning the system’s total energy as a sum of empirical potential energy functions (potentials) (161). Force fields commonly applied to API-excipient ASD modeling include polymer consistent force field (PCFF) (17), condensed-phase optimized molecular potentials for atomistic simulation studies (COMPASS) (162, 163), assisted model building with energy refinement (AMBER) (164), optimized potential for liquid simulations (OPLS) (165), and chemistry at Harvard macromolecular mechanics (CHARMM) (166, 167). These force fields describe energy as dependent on atomic positions. The subcomponent potentials can be divided into those for bonded atoms accounting for bond lengths, angles, torsions, and nonbonded atoms describing van der Waals and Coulombic interactions (168, 169).
Using force field COMPASS, Gupta et al. demonstrated the ability of molecular modeling to simulate and predict solubility parameters. MD was used to study the miscibility of indomethacin in polyethylene oxide (PEO), glucose, and sucrose. MD simulations revealed that indomethacin was miscible with PEO, borderline miscible with sucrose, and immiscible with glucose (170). Employing CHARMM, miscibility parameters between ibuprofen and carbamazepine were evaluated in polymeric carriers polyvinyl caprolactam-polyvinyl acetate-polyethylene glycol graft copolymer/polyethylene glycol. Strong molecular interactions were observed between these components, which was confirmed by DSC and FTIR analysis (157). Kapourani et al. used PCFF to determine miscibility parameters between simvastatin and PVP, which were further verified by DSC and hot stage polarized microscopy (171).
Yani et al. utilized Hilderbrand and Hansen solubility parameters to investigate miscibility between the APIs and polymers. Before the preparation of ASDs, MD simulations predicted Hansen solubility parameters and calculated total hydrogen bond interaction energy and the average hydrogen bond lifetime per monomer between polymer functional groups and API. As per the predicted solubility, ASDs of fenofibrate/PVP-VA 64, ibuprofen/PVP–VA 64, and ibuprofen/Eudragit EPO were then manufactured using HME. The relative intermolecular interaction was predicted to be weakest for fenofibrate/PVP-VA 64. This result was further validated by the observed recrystallization of this system (172). Han et al. envisaged preparing a ternary ASD system comprising glipizide (API), PEG (polymeric carrier), and Tween 80 (surfactant). MD simulations were used to study ASD formation, dissolution, and molecular mobility (173). Razmimanesh et al. evaluated ASDs of gemcitabine as the API and chitosan as the polymeric carrier. MD simulations were used to investigate the effects of hydration on API loading efficiency with varying concentrations of API. The strongest molecular interactions and the maximum loading efficiency in simulated aqueous conditions were found to occur at the intermediate concentration (40%) of gemcitabine (174). Xiang et al. used MD simulations to study the effect of hydration on HPMC with the aim of investigating any alterations in its properties. It was found that increasing water fractions led to an enhanced structural relaxation and increased molecular mobility (175).
Barmpalexis et al. used docking models involving ibuprofen and carbamazepine interaction using mixtures of Soluplus, PEG polymer, and plasticizer which are the most stable forms. The miscibility of the system was evaluated by means of Hoftyzer-Van Krevelen and Hildebrand solubility parameters. The ternary systems were found to be miscible as per the calculated solubility parameters and DSC experiment results. In addition to this, FTIR spectroscopy was used to analyze the intermolecular interactions within the ASD system. Strong H-bonding which was observed between the carbamazepine primary amine group and the carbonyl and amide groups from docking and MD was further confirmed in this way (157).
Quantum Mechanics
Quantum mechanics (QM) methods can be used to study the API-carrier nonbonding interactions. Density functional theory (DFT) is one such computational modeling tool that may be used to study solid-state pharmaceutical compounds. The nonbonding interactions that occur between the API and the polymeric carrier in an ASD can be studied using methods such as DFT, through which hypothesized molecular complexes can be directly constructed, and their associated interaction energy calculated. It is a rapid and powerful computational methodology that can identify ionic and strong hydrogen bonding interactions and predict the energy of model complexes (176). This pure QM approach produces a static snapshot while ASD modeling and therefore calls for adequate, sometimes manual, conformational space sampling. When applying DFT to large chemical systems, the calculation time can be drastically reduced by truncating the polymers to their monomeric and dimeric forms in the model systems. This permits a more systematic and detailed structural investigation of the ASD system. DFT applications are being used to study hydrogen bonding and charge interactions. A critical step toward ASD formulation and rational excipient screening is considering both of these parameters, whether relying on complexes formed between the API and carrier is comprehending the crucial interactions which determine ASD stabilization and solubilization (177). In one such study to understand these interactions, Maniruzzaman et al. investigated the interactions between a cationic API and an anionic polymeric carrier (91, 178).
Nie et al. probed the molecular interactions between the anti-leprotic drug, clofazimine, and the polymeric carrier, hypromellose phthalate, in an ASD system. Potential strong donors and acceptors were identified using partial charge analysis. DFT geometry and energy calculations utilized a truncated model system with acetic acid as a structural substitution for hypromellose phthalate carboxylic acid. Based on the results of the calculations and spectroscopic studies, it was proposed that the formation of an ion-pair complex is crucial for API-carrier miscibility (179).
DFT calculations have also been used to predict ASD storage stability. Wang et al. investigated the ability of polyvinyl pyrrolidone (PVP) to inhibit the crystallization of PVP-griseofulvin and PVP-resveratrol ASDs. DFT calculations and FTIR spectroscopy were used to investigate the relative interaction strengths between API-API and API-polymer complexes. Greater stabilizing hydrogen bond interactions were found to occur between the PVP-resveratrol ASDs as compared to PVP-griseofulvin ASD. The stronger interaction energy between PVP and resveratrol was found to be the contributing factor to the storage stability of the ASD and also yielded a continuous high dissolution rate of up to 90 days of storage, whereas a lower dissolution rate was observed for the PVP-griseofulvin system (180).
Machine Learning for ASDs from Molecular Modeling
Machine learning (ML) is increasingly being used in several aspects of the pharmaceutical sector, including drug development, allowing the industry to grow as a whole (181). Machine learning capabilities and their utility in drug development and simulations are becoming important, so it is critical that ML be included in future breakthroughs in the field of ASDs. The inclusion of a novel drug molecule into a suitable pharmaceutical ASD with desirable delivery characteristics follows the development of the novel therapeutic molecule. In this case, artificial intelligence (AI) may be able to take over the role of the classic trial and error methods for product development (182). AI integration in manufacturing could be beneficial to pharmaceutical manufacturing and business (183). Quantitative structure-activity relationship (QSAR) modeling has been used to predict features such as adsorption, distribution, metabolism, elimination, and toxicity (ADMET) or compound oral bioavailability (184). The QSAR comparison cluster prediction approach requires structured similarity searching, in which a cluster of chemicals with similar systems to the test molecule is identified in the learning data set and utilized to construct a model that serves as the foundation for toxicological prediction. So, in this way, AI, ML, and QSAR can play a major role in the development of ASDs. The screening of suitable polymeric carriers when developing an ASD system of a poorly water-soluble drug is a tedious process that requires a huge amount of time, leading to high development times and slower progression to clinical trials. This time can be lessened by acquiring suitable knowledge about the behavior of ASD formation, dissolution, and subsequently drug release from the carrier matrix. This knowledge enables one to guide and streamline the choice of suitable excipient candidates for ASD formulation.
The mechanism of dissolution of the API is crucial to understand when designing an ASD. This mechanism can include either rapid dissolution, which results in a fluid phase that promotes the formation of crystalline or amorphous API nanostructures inside the polymer carrier, the progressive release of amorphous API-polymer compounds from the larger bulk ASD complex, or the subtle release of API-polymer, but gelation by water can cause crystalline API-polymer agglomerations to develop at the ASD-solvent interface (185), (186). Chan et al. investigated the formation and dissolution of ASDs composed of ibuprofen, PEG, PVP, and poloxamer 188 (P188) using MD simulations. The simulated annealing method was used to model ASD formation. This was followed by water immersion with the aim of investigating dissolution behavior. While smaller ASD particles displayed rapid dissolution, the dissolution of larger particles was found to be dependent on the polymer. API mobility was found to be higher within PEG and PVP polymers that led to API aggregation and consequently recrystallization of API, while P188 slowed API aggregation, thus better stability and dissolution (187). Jha et al. utilized MD simulations to study the intermolecular interactions and dissolution behavior of ASDs comprising phenytoin, a poorly soluble API, and cellulose-type polymeric carriers. The phenytoin diffusion rate was analyzed by determining the variation in a water weight ratio in order to determine the dissolution behavior. As the water weight increased, the diffusion constants were found to increase exponentially (188).
Challenges for ASD-Based Formulations: Regulatory Constraints
ASDs have shown potential in the delivery of poorly water-soluble drugs. There was not much research on ASDs until 2010; however, the interest in ASD-based research has gained much attention since then. Our literature review revealed that ASDs had been used to deliver multiple drugs, including griseofulvin, verapamil, ritonavir, tacrolimus, troglitazone, antifungal agents (e.g., itraconazole), and immunosuppressant agents (e.g., cyclosporin A). Because the increased bioavailability of ASD is due to the increased energy of the amorphous form, this drug delivery strategy has several drawbacks in manufacturing and storage. The key challenges associated with ASDs are their physical instability during manufacturing and after manufacturing and their humidity and temperature sensitivity/susceptibility, which impacts storage lifetime, although the type of packaging employed can reduce the risk of water uptake and crystallization.
Although our understanding has progressed dramatically in recent years, there are still numerous unanswered problems associated with ASDs. More research is needed to improve the predictability of ASD’s unique physical and chemical properties and in vivo performance, including the molecular interactions between the drug and the polymer carrier.
The HME process to produce ASDs is gaining popularity in pharmaceutical companies, despite the fact that more than half of all polymer-carriers lack a temperature range (defined by thermal plus elastomeric properties) suited to using HME. Furthermore, several polymer-carriers have wide temperature ranges, which could make it difficult to process thermolabile APIs continuously (189).
Similarly, spray-drying has been recognized as one of the valuable methods to generate ASDs. However, it is a multistep process. The spray-drying process entails: (1) a solvent system is used to dissolve the drug and inactive ingredients; (2) pumping the concentrated solution into the spray nozzle; (3) atomizing the solution flow into fine droplets through an external unit; (4) drying the fine droplets inside a drying chamber; and (5) dividing and accumulating the dried particles via an appropriate collector. Screening with milligram amounts of API has been made possible by miniaturized spray-dryers. Many experiments have shown that ASDs produced by small-scale or lab-scale spray-driers could be replicated at a bigger scale. The spray-drying technique for amorphization of a low Tg drug has limitations because of the requirement to keep the output temperature low (below 35°C). For example, Shetty et al. prepared ASDs of ciprofloxacin by spray drying and found the outlet temperature to affect the degree of crystallization and also aerosol performance for pulmonary drug delivery (190). Similarly, Mangal et. Al. prepared ASDs based on colistin on the surfaces of colistin-meropenem co-sprayed particulates. This has been attributed to an increase in particle porosity in conjunction with an increase in colistin concentration, resulting in a reduction in meropenem co-sprayed particulate. Any ASD that becomes physically unstable when exposed to humidity because of porosity it should be carefully packaged or protected from moisture (191).
The use of pharmaceutical ASDs will be hastened further if a technological breakthrough delivers a scaled miniaturized solvent-free equipment, such as HME or KinetiSol technology, which allows for the assessment of solvent-free ASDs utilizing milligram quantities of API. For some APIs, the introduction of new polymer, like Soluplus, has improved stability and dissolution profiles. ASD matrices of HPMCAS, which is a common polymer with high Tg and low hygroscopicity, were improved by the inclusion of Soluplus®. The choice of new, unproven additives is a regulatory and policy decision as well as a pharmacologic safety risk. In respect of patent protection, pioneers of new polymers suitable for ASDs have a significant advantage. Nevertheless, gaining regulatory approval for novel excipients requires a significant amount of time and money.
In the case of ASD-based formulations, unfortunately, devitrification can occur during storage. Since the product may be subject to change during storage, it needs to satisfy regulatory requirements such as solubility and crystallization tendencies.
Quality by design (QbD) is a platform in which quality is determined by the finished product instead of quality control quantitative assays. By leveraging new technology and computational tools, critical quality attributes (CQA) are employed in QbD to analyze, regulate, and monitor essential manufacturing operations (by multivariate analysis). To obtain a product with the critical quality attributes (CQAs), QbD methods such as DoE and PAT are frequently used, which helps to discover the optimal design space of critical material attributes (CMAs) and critical process parameters (CPPs). The essential nature of these critical attributes in the drug products is based on their identification and screening. The use of a risk assessment tool as a QbD approach is commonly used to achieve this criticality (192). Multivariate analysis approaches are used to detect, classify, and measure statistically relevant variable effects on essential product qualities (193). The design and development of formulations and manufacturing procedures that ensure pre-defined product characteristics are all part of the QbD strategy. A QbD approach based on the factorial design of experiments (DoE) was used to successfully develop a Carbopol 940 topical gel containing an aceclofenac-crospovidone ASD (194). QbD was also used to optimize the solid dispersion formulation and process factors for polypeptide-k (PPK-SD) manufactured by spray-drying. The resulting product powder flow characteristics and yield were found to be greatly improved when the ratio of trehalose to PPK was raised (195). In order to improve the dissolution rate and solubility of the poorly water-soluble drug efavirenz, QbD methods were used to produce and optimize an ASD (196).
Current Scenario
The present regulatory framework is supportive of advances in scientific research, which includes deserting old-style manufacturing processes in favor of dynamic continuous manufacturing. Regulatory authorities are encouraging manufacturers to embrace new technologies, as represented by ICH Q3, Q7, Q8 (R2), Q9, Q10, and Q11, and the introduction of QbD concepts, emphasizing science as well as risk-based methods to ensure product quality (197).
As the API and non-active component(s) do not exist in the same crystal lattice and often do not require stoichiometry, ASDs differ from salts and solvates. A quasi component is a non-covalently attached component, including a carrier, additive, or other excipients, that is added to the ASD to enhance properties. The co-processed API may not be deemed a new API according to FDA guidelines for industry, Regulatory Classification of Pharmaceuticals. It is crucial to define an ASD as an effective dosage form since it clarifies that all these materials are not in-process materials, an API mixture, or an active pharmaceutical intermediate. The alternative categorization of an ASD intermediate would have ramifications for both expiry dating and GMP production, posing major barriers to commercialization. Through a scientific-technical advice (STA) request, an input on continuous manufacturing techniques for a future phase 1 clinical study was recently received, from the Federal Agency for Medicines and Health Products (FAMHP) of Belgium: “From a regulatory standpoint, the Agency agrees with the Applicant’s proposal to consider continuous manufacturing as a drug substance because it is regarded as vital for the (physical) convergence of amorphous form of the drug molecule, and thus its bioavailability and clinical outcomes.” While the approach has certain flaws, it is a potential first step that could pave the door for broader adoption of continuous production (193).
Regulatory Harmonization and Convergence
To reach the quality target profile, the requirement for an ASD formulation, a complicated composition, should be adequately justified, and this should be done from a clinical perspective: to enhance the bioavailability, physical stability, and pharmacological burden and strengthen the product’s actual safety profile. The application of this type of formulation is to enhance the efficacy of the drug. In the case of inactive ingredients, only those that are generally regarded as safe (GRAS) are established for human use at precise doses are listed in the FDA’s inactive ingredient registry. A full pharmacology study, including carcinogenic effects and chronic toxicity, is required to ensure that all necessary excipients are suitable for use in humans. This is particularly true in ASD-based formulations, where polymer quantities are often much higher than in traditional dosage forms. All types of equipment used in pharmaceutical ASD manufacturing must meet GMP guidelines and validation standards. The surfaces that come into direct touch with the finished product must comply with GMP guidelines. The regulatory guideline states that “the level of pertinent scientific knowledge given in the application for registration determines the degree of regulatory flexibility.” Science- and risk-based filings and regulatory evaluations are based on the information gained and provided to authorities. All of the aforementioned guidelines, as well as the recently emphasized QbD framework, have the potential to make a substantial impact on the creation, optimization, and deployment of continuous manufacturing processes.
Conclusion and Future Perspective
The increasing number of drugs with low aqueous solubility, poor dissolution, and poor oral bioavailability remains an unresolved issue that needs to be addressed with suitable interventions. Many potential drug candidates are aborted in the developmental pipeline as they are unable to exert their therapeutic benefit due to poor solubility. This obstacle of insolubilization can be overcome by employing suitable formulation strategies, and ASD is one such strategy that can help enhance the solubility and dissolution rate of poorly soluble drugs. Although the technology of ASD has come a long way since its advent more than half a century ago, it has not yet been utilized to its full potential in the best possible manner. The problems that exist today with ASDs include screening, stability, and scale-up issues, which may be overcome by employing computational molecular modeling tools and continuous manufacturing techniques. For large dosage drugs, direct compression-based continuous manufacturing holds a lot of potential, and amorphous solid dispersions will play a significant role in that process. However, thorough investigations are necessary for amorphous material-based tablets as there is the possibility of crystallization, particularly at high compaction pressure. The chances of heterogeneous crystallization (on the surface or in the interior of the amorphous material) exist, even at lower compaction pressure. Specialized 2D X-ray diffractometry techniques with high-intensity synchrotron radiation can be useful to detect phase transformation in tablets. Thakral et al. have provided detailed information on the compaction of amorphous APIs (198). To step further in this arena, a meticulous understanding of such concepts need to be attained. Further research in this field will enable the translation of preclinical evidence into clinical reality and bring more ASD-based formulations to the market.
References
Van den Mooter GJDDTT. The use of amorphous solid dispersions: a formulation strategy to overcome poor solubility and dissolution rate. Drug Disc Today. 2012;9(2):e79–85.
Ojo AT, Ma C, Lee PIJIJoP. Elucidating the effect of crystallization on drug release from amorphous solid dispersions in soluble and insoluble carriers. Int J Pharm. 2020;591:120005.
Benet LZJJops. The role of BCS (biopharmaceutics classification system) and BDDCS (biopharmaceutics drug disposition classification system) in drug development. J Pharm Sci. 2013;102(1):34–42.
Fahr A, Liu XJEoodd. Drug delivery strategies for poorly water-soluble drugs. Expert opinion on drug delivery. 2007;4(4):403–16.
Wilson VR, Lou X, Osterling DJ, Stolarik DF, Jenkins GJ, Nichols BL, et al. Amorphous solid dispersions of enzalutamide and novel polysaccharide derivatives: Investigation of relationships between polymer structure and performance. Scientific reports. 2020;10(1):1–12.
Kawabata Y, Wada K, Nakatani M, Yamada S, Onoue SJIjop. Formulation design for poorly water-soluble drugs based on biopharmaceutics classification system: basic approaches and practical applications. Int J Pharm. 2011;420(1):1–10.
Rautio J, Kumpulainen H, Heimbach T, Oliyai R, Oh D, Järvinen T, et al. Prodrugs: design and clinical applications. Natures. 2008;7(3):255–70.
Loftsson T, Duchene DJIjop. Cyclodextrins and their pharmaceutical applications. Int J Pharm. 2007;329(1–2):1–11.
Rabinow BEJNrDd. Nanosuspensions in drug delivery. Natures. 2004;3(9):785–96.
Berge SM, Bighley LD. Monkhouse DCJJops. Pharmaceutical salts. J Pharm Sci. 1977;66(1):1–19.
Lavasanifar A, Samuel J, Kwon GSJAddr. Poly (ethylene oxide)-block-poly (L-amino acid) micelles for drug delivery. Adv Drug Delivery Rev. 2002;54(2):169–90.
Fatouros DG, Deen GR, Arleth L, Bergenstahl B, Nielsen FS, Pedersen JS, et al. Structural development of self nano emulsifying drug delivery systems (SNEDDS) during in vitro lipid digestion monitored by small-angle X-ray scattering. Pharmaceutical research. 2007;24(10):1844–53.
Potta SG, Minemi S, Nukala RK, Peinado C, Lamprou DA, Urquhart A, et al. Development of solid lipid nanoparticles for enhanced solubility of poorly soluble drugs. J Biomed Nanotech. 2010;6(6):634–40.
Patel VR, Agrawal YJJoapt, research. Nanosuspension: an approach to enhance solubility of drugs. J Advanc Pharma Tech 2011;2(2):81.
Gao P, Shi YJTAj. Characterization of supersaturatable formulations for improved absorption of poorly soluble drugs. AAPS journal. 2012;14(4):703–13.
Gala UH, Miller DA, Su Y, Spangenberg A, Williams ROB 3rd. The effect of drug loading on the properties of abiraterone-hydroxypropyl beta cyclodextrin solid dispersions processed by solvent free KinetiSol(R) technology. Eur J Pharm Biopharm. 2021;165:52–65.
Maple JR, Dinur U. Hagler ATJPotNAoS. Derivation of force fields for molecular mechanics and dynamics from ab initio energy surfaces. Proceedings of the National Academy of Sciences. 1988;85(15):5350–4.
Jang D-J, Sim T, Oh EJD. pharmacy i. Formulation and optimization of spray-dried amlodipine solid dispersion for enhanced oral absorption. J Drug develop. 2013;39(7):1133–41.
Ellenberger DJ, Miller DA, Williams ROJAP. Expanding the application and formulation space of amorphous solid dispersions with KinetiSol®: a review. AAPS Pharmscitech. 2018;19(5):1933–56.
Wu JX, Yang M, van den Berg F, Pajander J, Rades T, Rantanen JJEjops. Influence of solvent evaporation rate and formulation factors on solid dispersion physical stability. Eur J Pharm Sci. 2011;44(5):610–20.
Mosquera-Giraldo LI, Borca CH, Meng X, Edgar KJ, Slipchenko LV, Taylor LSJB. Mechanistic design of chemically diverse polymers with applications in oral drug delivery. Biomacromolecules. 2016;17(11):3659–71.
Indulkar AS, Lou X, Zhang GGZ, Taylor LS. Insights into the dissolution mechanism of ritonavir-copovidone amorphous solid dispersions: importance of congruent release for enhanced performance. Mol Pharm. 2019;16(3):1327–39.
Mosquera-Giraldo LI, Li N, Wilson VR, Nichols BL, Edgar KJ, Taylor LSJMP. Influence of polymer and drug loading on the release profile and membrane transport of telaprevir. Mol Pharm. 2018;15(4):1700–13.
Martínez LM, Videa M, Sosa NG, Ramírez JH, Castro SJM. Long-term stability of new co-amorphous drug binary systems: Study of glass transitions as a function of composition and shelf time. Molecules. 2016;21(12):1712.
Van den Mooter G, Weuts I, De Ridder T, Blaton NJIjop. Evaluation of Inutec SP1 as a new carrier in the formulation of solid dispersions for poorly soluble drugs. Int J Pharm. 2006;316(1–2):1–6.
Medarević D, Djuriš J, Barmpalexis P, Kachrimanis K, Ibrić SJP. Analytical and computational methods for the estimation of drug-polymer solubility and miscibility in solid dispersions development. Pharmaceutics. 2019;11(8):372.
DeBoyace K, Wildfong PLJJoPS. The application of modeling and prediction to the formation and stability of amorphous solid dispersions. J Pharm Sci. 2018;107(1):57–74.
Mendonsa N, Almutairy B, Kallakunta V, Sarabu S, Thipsay P, Bandari S. Manufacturing strategies to develop amorphous solid dispersions: an overview. J Drug Deliv Sci Technol. 2020;55(101459):2019.
Crowley MM, Zhang F, Repka MA, Thumma S, Upadhye SB, Kumar Battu S, et al. Pharmaceutical applications of hot-melt extrusion: part I. Drug development industrial pharmacy. 2007;33(9):909–26.
Repka MA, Battu SK, Upadhye SB, Thumma S, Crowley MM, Zhang F, et al. Pharmaceutical applications of hot-melt extrusion: Part II. J Drug Develop. 2007;33(10):1043–57.
Li N, Cape JL, Mankani BR, Zemlyanov DY, Shepard KB, Morgen MM, et al. Water-induced phase separation of spray-dried amorphous solid dispersions. Mol Pharm. 2020;17(10):4004–17.
Obaidat RM, Tashtoush BM, Awad AA, Al Bustami RTJAP. Using supercritical fluid technology (SFT) in preparation of tacrolimus solid dispersions. AAPS PharmSciTech. 2017;18(2):481–93.
Fülöp G, Balogh A, Farkas B, Farkas A, Szabó B, Démuth B, et al. Homogenization of amorphous solid dispersions prepared by electrospinning in low-dose tablet formulation. Pharmaceutics. 2018;10(3):114.
Burcham CL, Florence AJ, Johnson MDJAroc, engineering b. Continuous manufacturing in pharmaceutical process development and manufacturing. Annual review of chemical biomolecular engineering 2018;9:253–281.
Lapuk S, Mukhametzyanov T, Schick C, Gerasimov AJIJoP. Kinetic stability of amorphous dipyridamole: a fast scanning calorimetry investigation. Int J Pharm. 2020;574:118890.
Newman A, Zografi GJAP. Commentary: considerations in the measurement of glass transition temperatures of pharmaceutical amorphous solids. AAPS PharmSciTech. 2020;21(1):1–13.
Neilly JP, Yin L, Leonard S-E, Kenis PJ, Danzer GD, Pawate ASJJoPS. Quantitative measures of crystalline fenofibrate in amorphous solid dispersion formulations by X-ray microscopy. J Pharm Sci. 2020;109(10):3078–85.
Jha DK, Shah DS, Amin PDJIJoP. Thermodynamic aspects of the preparation of amorphous solid dispersions of Naringenin with enhanced dissolution rate. Int J Pharm. 2020;583:119363.
Han YR, Ma Y, Lee PI. Impact of phase separation morphology on release mechanism of amorphous solid dispersions. Eur J Pharm Sci. 2019;136:104955.
Shi NQ, Wang SR, Zhang Y, Huo JS, Wang LN, Cai JH, et al. Hot melt extrusion technology for improved dissolution, solubility and "spring-parachute" processes of amorphous self-micellizing solid dispersions containing BCS II drugs indomethacin and fenofibrate: Profiles and mechanisms. Eur J Pharm Sci. 2019;130:78–90.
Chen Y, Wang S, Wang S, Liu C, Su C, Hageman M, et al. Initial drug dissolution from amorphous solid dispersions controlled by polymer dissolution and drug-polymer interaction. Pharm Res. 2016;33(10):2445–58.
Liu C, Chen Z, Chen Y, Lu J, Li Y, Wang S, et al. Improving oral bioavailability of sorafenib by optimizing the “spring” and “parachute” based on molecular interaction mechanisms. Mol Pharm. 2016;13(2):599–608.
Arca HÇ, Mosquera-Giraldo LI, Dahal D, Taylor LS, Edgar KJJMP. Multidrug, anti-HIV amorphous solid dispersions: nature and mechanisms of impacts of drugs on each other’s solution concentrations. Mol Pharm. 2017;14(11):3617–27.
Graeser KA, Patterson JE, Zeitler JA, Rades TJP. The role of configurational entropy in amorphous systems. Pharmaceutics. 2010;2(2):224–44.
Craig DQJIjop. The mechanisms of drug release from solid dispersions in water-soluble polymers. Int J Pharm. 2002;231(2):131–44.
Schittny A, Huwyler J, Puchkov M. Mechanisms of increased bioavailability through amorphous solid dispersions: a review. J Drug Deliv. 2020;27(1):110–27.
Sun DD, Lee PI. Probing the mechanisms of drug release from amorphous solid dispersions in medium-soluble and medium-insoluble carriers. J Control Release. 2015;211:85–93.
Pandi P, Bulusu R, Kommineni N, Khan W, Singh M. Amorphous solid dispersions: an update for preparation, characterization, mechanism on bioavailability, stability, regulatory considerations and marketed products. Int J Pharm. 2020;586:119560.
Saboo S, Mugheirbi NA, Zemlyanov DY, Kestur US, Taylor LS. Congruent release of drug and polymer: A "sweet spot" in the dissolution of amorphous solid dispersions. J Control Release. 2019;298:68–82.
Li J, Li C, Zhang H, Gao X, Wang T, Wang Z, et al. Preparation of azithromycin amorphous solid dispersion by hot-melt extrusion: an advantageous technology with taste masking and solubilization effects. Polymers. 2022;14(3):495.
Indulkar AS, Lou X, Zhang GG, Taylor LSJPR. Role of surfactants on release performance of amorphous solid dispersions of ritonavir and copovidone. Pharm Res. 2022;39(2):381–97.
Cho H-W, Baek S-H, Lee B-J, Jin H-EJP. Orodispersible polymer films with the poorly water-soluble drug, olanzapine: hot-melt pneumatic extrusion for single-process 3D printing. Pharmaceutics 2020;12(8):692.
Tres F, Posada MM, Hall SD, Mohutsky MA, Taylor LSJIJoP. Mechanistic understanding of the phase behavior of supersaturated solutions of poorly water-soluble drugs. Int J Pharm. 2018;543(1–2):29–37.
Feng D, Peng T, Huang Z, Singh V, Shi Y, Wen T, et al. Polymer–surfactant system based amorphous solid dispersion: Precipitation inhibition and bioavailability enhancement of itraconazole. Pharmaceutics. 2018;10(2):53.
Kwon J, Giri BR, Song ES, Bae J, Lee J, Kim DWJP. Spray-dried amorphous solid dispersions of atorvastatin calcium for improved supersaturation and oral bioavailability. Pharmaceutics. 2019;11(9):461.
Lakshman D, Chegireddy M, Hanegave GK, Sree KN, Kumar N, Lewis SA, et al. Investigation of drug-polymer miscibility, biorelevant dissolution, and bioavailability improvement of Dolutegravir-polyvinyl caprolactam-polyvinyl acetate-polyethylene glycol graft copolymer solid dispersions. Eur J pharm Sci. 2020;142:105137.
de Alencar Danda LJ, de Medeiros BL, Melo VCS, Sobrinho JLS, Soares MFdLRJEJoPS. Combining amorphous solid dispersions for improved kinetic solubility of posaconazole simultaneously released from soluble PVP/VA64 and an insoluble ammonio methacrylate copolymer. Eur J Pharm Sci. 2019;133:79–85.
Figueirêdo CBM, Nadvorny D, de Medeiros Vieira ACQ, de Medeiros Schver GCR, Sobrinho JLS, Neto PJR, et al. Enhanced delivery of fixed-dose combination of synergistic antichagasic agents posaconazole-benznidazole based on amorphous solid dispersions. Eur J Pharm Sci. 2018;119:208–18.
Xi L, Song H, Wang Y, Gao H, Fu QJAP. Lacidipine amorphous solid dispersion based on hot melt extrusion: good miscibility, enhanced dissolution, and favorable stability. AAPS Pharm Sci Tech. 2018;19(7):3076–84.
Gala U, Miller D, Williams ROJP. Improved dissolution and pharmacokinetics of abiraterone through KinetiSol® enabled amorphous solid dispersions. Pharmaceutics. 2020;12(4):357.
Monschke M, Kayser K, Wagner KGJAP. Influence of particle size and drug load on amorphous solid dispersions containing pH-dependent soluble polymers and the weak base ketoconazole. AAPS PharmSciTech. 2021;22(1):1–11.
Umemoto Y, Uchida S, Yoshida T, Shimada K, Kojima H, Takagi A, et al. An effective polyvinyl alcohol for the solubilization of poorly water-soluble drugs in solid dispersion formulations. J Drug Deliv Sci Tech. 2020;55:101401.
Pinto JMO, Leão AF, Alves GF, Mendes C, França MT, Fernandes D, et al. New supersaturating drug delivery system as strategy to improve apparent solubility of candesartan cilexetil in biorelevant medium. Pharm Develop. 2020;25(1):89–99.
Shi X, Fan N, Zhang G, Sun J, He Z, Li JJPD, et al. Quercetin amorphous solid dispersions prepared by hot melt extrusion with enhanced solubility and intestinal absorption. J Pharm Develop Tech. 2020;25(4):472–81.
Han F, Zhang W, Wang Y, Xi Z, Chen L, Li S, et al. Applying supercritical fluid technology to prepare ibuprofen solid dispersions with improved oral bioavailability. pharmaceutics. 2019;11(2):67.
Alhayali A, Selo MA, Ehrhardt C, Velaga SJEJoPS. Investigation of supersaturation and in vitro permeation of the poorly water soluble drug ezetimibe. Eur J Pharm Sci. 2018;117:147–53.
Rahman M, Ahmad S, Tarabokija J, Parker N, Bilgili EJP. Spray-dried amorphous solid dispersions of griseofulvin in HPC/Soluplus/SDS: elucidating the multifaceted impact of sds as a minor component. Pharmaceutics. 2020;12(3):197.
Wang Z, Sun M, Liu T, Gao Z, Ye Q, Tan X, et al. Co-amorphous solid dispersion systems of lacidipine-spironolactone with improved dissolution rate and enhanced physical stability. Asian J Pharm Sci. 2019;14(1):95–103.
Himawan A, Djide NJN, Mardikasari SA, Utami RN, Arjuna A, Donnelly RF, et al. A novel in vitro approach to investigate the effect of food intake on release profile of valsartan in solid dispersion-floating gel in-situ delivery system. Eur J Pharm Sci. 2022;168:106057.
Müller M, Wiedey R, Hoheisel W, Serno P, Breitkreutz JJEJoP, Biopharmaceutics. Impact of co-administered stabilizers on the biopharmaceutical performance of regorafenib amorphous solid dispersions. Eur J Pharm Biopharm. 2021;169:189–199.
Trasi NS, Bhujbal SV, Zemlyanov DY, Zhou QT, Taylor LSJIjopX. Physical stability and release properties of lumefantrine amorphous solid dispersion granules prepared by a simple solvent evaporation approach. Int J Pharm. 2020;2:100052.
Ren F, Sun H, Cui L, Si Y, Chen N, Ren G, et al. Antisolvent recrystallization strategy to screen appropriate carriers to stabilize filgotinib amorphous solid dispersions. J Pharm Sci. 2018;107(6):1624–32.
Dong W, Su X, Xu M, Hu M, Sun Y, Zhang PJAjops. Preparation, characterization, and in vitro/vivo evaluation of polymer-assisting formulation of atorvastatin calcium based on solid dispersion technique. Asian journal of pharmaceutical sciences. 2018;13(6):546–54.
Xie T, Taylor LSJJops. Effect of temperature and moisture on the physical stability of binary and ternary amorphous solid dispersions of celecoxib. J Pharm Sci. 2017;106(1):100–10.
Shi C, Tong Q, Fang J, Wang C, Wu J, Wang WJEJoPS. Preparation, characterization and in vivo studies of amorphous solid dispersion of berberine with hydrogenated phosphatidylcholine. Eur J Pharm Sci. 2015;74:11–7.
Rahman Z, Siddiqui A, Bykadi S, Khan MAJIJoP. Determination of tacrolimus crystalline fraction in the commercial immediate release amorphous solid dispersion products by a standardized X-ray powder diffraction method with chemometrics. Int J Pharm. 2014;475(1–2):462–70.
Nieto K, Mallery SR, Schwendeman SPJIjop. Microencapsulation of amorphous solid dispersions of fenretinide enhances drug solubility and release from PLGA in vitro and in vivo. Int J Pharm. 2020;586:119475.
Ewing AV, Clarke GS, Kazarian SGJEJoPS. Stability of indomethacin with relevance to the release from amorphous solid dispersions studied with ATR-FTIR spectroscopic imaging. Eur J Pharm Sci. 2014;60:64–71.
Sarode AL, Malekar SA, Cote C, Worthen DRJCP. Hydroxypropyl cellulose stabilizes amorphous solid dispersions of the poorly water soluble drug felodipine. Carbohydrate Polymers. 2014;112:512–9.
Jijun F, Lishuang X, Xiaoguang T, Min S, Mingming Z, Haibing H, et al. The inhibition effect of high storage temperature on the recrystallization rate during dissolution of nimodipine-Kollidon VA64 solid dispersions (NM-SD) prepared by hot-melt extrusion. J Pharm Sci. 2011;100(5):1643–7.
Hassouna F, El Dahab MA, Fulem M, Haiek ADL, Laachachi A, Kopecký D, et al. Multi-scale analysis of amorphous solid dispersions prepared by freeze drying of ibuprofen loaded acrylic polymer nanoparticles. J Drug Deliv Sci. 2019;53:101182.
Christina B, Taylor LS, Mauer LJJFRI. Physical stability of l-ascorbic acid amorphous solid dispersions in different polymers: a study of polymer crystallization inhibitor properties. Food Res Int. 2015;76:867–77.
Moes J, Koolen S, Huitema A, Schellens J, Beijnen J, Nuijen BJEjop, et al. Development of an oral solid dispersion formulation for use in low-dose metronomic chemotherapy of paclitaxel. Eur J Pharm Biopharm 2013;83(1):87–94.
Thombre AG, Shah JC, Sagawa K, Caldwell WB. In vitro and in vivo characterization of amorphous, nanocrystalline, and crystalline ziprasidone formulations. Int J Pharm. 2012;428(1–2):8–17.
Kim YI, Kim KS, Suh KH, Shanmugam S, Woo JS, Yong CS, et al. New clopidogrel napadisilate salt and its solid dispersion with improved stability and bioequivalence to the commercial clopidogrel bisulphate salt in beagle dogs. Int J Pharm. 2011;415(1–2):129–39.
Lim HT, Balakrishnan P, Oh DH, Joe KH, Kim YR, Hwang DH, et al. Development of novel sibutramine base-loaded solid dispersion with gelatin and HPMC: physicochemical characterization and pharmacokinetics in beagle dogs. Int J Pharm. 2010;397(1–2):225–30.
Yu DG, Yang JM, Branford-White C, Lu P, Zhang L, Zhu LM. Third generation solid dispersions of ferulic acid in electrospun composite nanofibers. Int J Pharm. 2010;400(1–2):158–64.
Mehanna MM, Motawaa AM, Samaha MW. In sight into tadalafil - block copolymer binary solid dispersion: Mechanistic investigation of dissolution enhancement. Int J Pharm. 2010;402(1–2):78–88.
Thiry J, Lebrun P, Vinassa C, Adam M, Netchacovitch L, Ziemons E, et al. Continuous production of itraconazole-based solid dispersions by hot melt extrusion: preformulation, optimization and design space determination. Int J Pharm. 2016;515(1–2):114–24.
Thiry J, Krier F, Ratwatte S, Thomassin J-M, Jerome C, Evrard BJEJoPS. Hot-melt extrusion as a continuous manufacturing process to form ternary cyclodextrin inclusion complexes. Eur. J Pharm Pharm Sci. 2017;96:590–7.
Maniruzzaman M, Morgan DJ, Mendham AP, Pang J, Snowden MJ, Douroumis DJIjop. Drug–polymer intermolecular interactions in hot-melt extruded solid dispersions. Int J Pharm. 2013;443(1–2):199–208.
LaFountaine JS, Jermain SV, Prasad LK, Brough C, Miller DA, Lubda D, et al. Enabling thermal processing of ritonavir-polyvinyl alcohol amorphous solid dispersions by KinetiSol(R) Dispersing. Eur J Pharm Biopharm. 2016;101:72–81.
Moseson DE, Taylor LS. The application of temperature-composition phase diagrams for hot melt extrusion processing of amorphous solid dispersions to prevent residual crystallinity. Int J Pharm. 2018;553(1–2):454–66.
Szabó E, Démuth B, Galata DL, Vass P, Hirsch E, Csontos I, et al. Continuous formulation approaches of amorphous solid dispersions: significance of powder flow properties and feeding performance. Pharmaceutics. 2019;11(12):654.
Muvva A, Lakshman D, Dwibhashyam VM, Dengale S, Lewis SAJJoDDS, Technology. In vitro-in silico evaluation of Apremilast solid dispersions prepared via Corotating Twin Screw Extruder. J Drug Deliv Sci Tech. 2020;59:101844.
Manne ASN, Hegde AR, Raut SY, Rao RR, Kulkarni VI, Mutalik SJD, et al. Hot liquid extrusion assisted drug-cyclodextrin complexation: a novel continuous manufacturing method for solubility and bioavailability enhancement of drugs. J Drug Deliv. 2021;11(3):1273–87.
Solomon S, Iqbal J, Albadarin ABJEJoP, Biopharmaceutics. Insights into the ameliorating ability of mesoporous silica in modulating drug release in ternary amorphous solid dispersion prepared by hot melt extrusion. Eur J Pharm Biopharm. 2021;165:244–258.
Emam MF, Taha NF, Emara LHJJoAPS. A novel combination of Soluplus® and Poloxamer for Meloxicam solid dispersions via hot melt extrusion for rapid onset of action—part 1: dissolution and stability studies. Journal of Applied Pharmaceutical. Science. 2021;11(02):141–50.
Giri BR, Kwon J, Vo AQ, Bhagurkar AM, Bandari S, Kim DWJP. Hot-melt extruded amorphous solid dispersion for solubility, stability, and bioavailability enhancement of telmisartan. Pharmaceuticals. 2021;14(1):73.
Maniruzzaman M, Nair A, Scoutaris N, Bradley MS, Snowden M, Douroumis DJIjop. One-step continuous extrusion process for the manufacturing of solid dispersions. Int J Pharm. 2015;496(1):42–51.
Fu Q, Fang M, Hou Y, Yang W, Shao J, Guo M, et al. A physically stabilized amorphous solid dispersion of nisoldipine obtained by hot melt extrusion. Powder Technology. 2016;301:342–8.
Turpin ER, Taresco V, Al-Hachami WA, Booth J, Treacher K, Tomasi S, et al. In silico screening for solid dispersions: the trouble with solubility parameters and chiFH. Mol Pharm. 2018;15(10):4654–67.
Tian Y, Jacobs E, Jones DS, McCoy CP, Wu H, Andrews GP. The design and development of high drug loading amorphous solid dispersion for hot-melt extrusion platform. Int J Pharm. 2020;586:119545.
Suryavanshi P, Banerjee S. Exploration of theoretical and practical evaluation on Kollidon®SR matrix mediated amorphous filament extrusion of norfloxacin by melt extrusion. Journal of Drug Delivery Science and Technology. 2022;67.
Zhao Y, Inbar P, Chokshi HP, Malick AW, Choi DSJJops. Prediction of the thermal phase diagram of amorphous solid dispersions by Flory–Huggins theory. J Pharm Sci. 2011;100(8):3196–3207.
Ha E-S, Choi DH, Baek I-h, Park H, Kim M-SJA. Enhanced oral bioavailability of resveratrol by using neutralized eudragit E solid dispersion prepared via spray drying. Antioxidants. 2021;10(1):90.
Mudie DM, Buchanan S, Stewart AM, Smith A, Shepard KB, Biswas N, et al. A novel architecture for achieving high drug loading in amorphous spray dried dispersion tablets. Int J Pharm. 2020;2:100042.
Costa B, Sauceau M, Del Confetto S, Sescousse R, Ré M-IJEJoP, Biopharmaceutics. Determination of drug-polymer solubility from supersaturated spray-dried amorphous solid dispersions: a case study with Efavirenz and Soluplus®. Eur J Pharm Biopharm. 2019;142:300–306.
Ziaee A, Albadarin AB, Padrela L, Faucher A, O'Reilly E, Walker GJEJoP, et al. Spray drying ternary amorphous solid dispersions of ibuprofen–an investigation into critical formulation and processing parameters. Eur J Pharm Biopharm. 2017;120:43–51.
Beak I-H, Kim M-SJC, Bulletin P. Improved supersaturation and oral absorption of dutasteride by amorphous solid dispersions. Chemical. Pharmaceutical Bulletin. 2012;60(11):1468–73.
Tran TH, Poudel BK, Marasini N, Chi S-C, Choi H-G, Yong CS, et al. Preparation and evaluation of raloxifene-loaded solid dispersion nanoparticle by spray-drying technique without an organic solvent. Int J Pharm. 2013;443(1–2):50–7.
Metre S, Mukesh S, Samal SK, Chand M, Sangamwar ATJMp. Enhanced biopharmaceutical performance of rivaroxaban through polymeric amorphous solid dispersion. Mol Pharm. 2018;15(2):652–68.
Smeets A, Koekoekx R, Ruelens W, Smet M, Clasen C, Van den Mooter GJIJoP. Gastro-resistant encapsulation of amorphous solid dispersions containing darunavir by coaxial electrospraying. Int J Pharm. 2020;574:118885.
Kawakami K, Miyazaki A, Fukushima M, Sato K, Yamamura Y, Mohri K, et al. Physicochemical properties of solid phospholipid particles as a drug delivery platform for improving oral absorption of poorly soluble drugs. Pharm Res. 2017;34(1):208–16.
Kawakami K, Zhang S, Chauhan RS, Ishizuka N, Yamamoto M, Masaoka Y, et al. Preparation of fenofibrate solid dispersion using electrospray deposition and improvement in oral absorption by instantaneous post-heating of the formulation. Int J Pharm. 2013;450(1–2):123–8.
Browne E, Charifou R, Worku ZA, Babu RP, Healy AMJIjop. Amorphous solid dispersions of ketoprofen and poly-vinyl polymers prepared via electrospraying and spray drying: a comparison of particle characteristics and performance. Int J Pharm. 2019;566:173–84.
Song S, Wang C, Wang S, Siegel RA, Sun CCJIJoP. Efficient development of sorafenib tablets with improved oral bioavailability enabled by coprecipitated amorphous solid dispersion. Int J Pharm. 2021;610:121216.
Duarte Í, Corvo ML, Serôdio P, Vicente J, Pinto JF, Temtem MJEJoPS. Production of nano-solid dispersions using a novel solvent-controlled precipitation process—Benchmarking their in vivo performance with an amorphous micro-sized solid dispersion produced by spray drying. Eur J Pharm Sci. 2016;93:203–14.
Lim RTY, Ng WK, Tan RBJPt. Dissolution enhancement of indomethacin via amorphization using co-milling and supercritical co-precipitation processing. Powder Technology. 2013;240:79–87.
Zhou H, Wang W, Hu H, Ni X, Ni S, Xu Y, et al. Co-precipitation of calcium carbonate and curcumin in an ethanol medium as a novel approach for curcumin dissolution enhancement. J Drug Deliv Sci Tech. 2019;51:397–402.
Liu P, Zhou J-y, Chang J-h, Liu X-g, Xue H-f, Wang R-x, et al. Soluplus-mediated diosgenin amorphous solid dispersion with high solubility and high stability: development, characterization and oral bioavailability. Drug Design, Develop 2020;14:2959.
Wang Y, Fang Y, Zhou F, Liang Q, Deng YJJoPS. The amorphous quercetin/hydroxypropylmethylcellulose acetate succinate solid dispersions prepared by co-precipitation method to enhance quercetin dissolution. J Pharm Sci. 2021;110(9):3230–7.
Islam MT, Scoutaris N, Maniruzzaman M, Moradiya HG, Halsey SA, Bradley MS, et al. Implementation of transmission NIR as a PAT tool for monitoring drug transformation during HME processing. Eur J Pharm Biopharm. 2015;96:106–16.
Saerens L, Vervaet C, Remon JP, De Beer T. Process monitoring and visualization solutions for hot-melt extrusion: a review. J Pharm Pharmacol. 2014;66(2):180–203.
Sacher S, Poms J, Rehrl J, Khinast JGJIjop. PAT implementation for advanced process control in solid dosage manufacturing–a practical guide. Int J Pharm. 2021;121408.
Rehrl J, Karttunen AP, Nicolai N, Hormann T, Horn M, Korhonen O, et al. Control of three different continuous pharmaceutical manufacturing processes: Use of soft sensors. Int J Pharm. 2018;543(1–2):60–72.
Pauli V, Roggo Y, Pellegatti L, Nguyen Trung NQ, Elbaz F, Ensslin S, et al. Process analytical technology for continuous manufacturing tableting processing: a case study. J Pharm Biomed Anal. 2019;162:101–11. https://doi.org/10.1016/j.jpba.2018.09.016.
Esmonde-White KA, Cuellar M, Uerpmann C, Lenain B, Lewis IR. Raman spectroscopy as a process analytical technology for pharmaceutical manufacturing and bioprocessing. Anal Bioanal Chem. 2017;409(3):637–49. https://doi.org/10.1007/s00216-016-9824-1.
Schlindwein W, Bezerra M, Almeida J, Berghaus A, Owen M, Muirhead G. In-Line UV-Vis Spectroscopy as a Fast-Working Process Analytical Technology (PAT) during Early Phase Product Development Using Hot Melt Extrusion (HME). Pharmaceutics. 2018;10(4). https://doi.org/10.3390/pharmaceutics10040166.
Yamanaka T, Kano S. Patent term extension systems differentiate Japanese and US drug lifecycle management. Drug Discov Today. 2016;21(1):111–7. https://doi.org/10.1016/j.drudis.2015.09.005.
Korasa K, Vrečer FJEJoPS. Overview of PAT process analysers applicable in monitoring of film coating unit operations for manufacturing of solid oral dosage forms. Eur J Pharm Sci. 2018;111:278–92.
Harting J, Kleinebudde PJEJoP, Biopharmaceutics. Optimisation of an in-line Raman spectroscopic method for continuous API quantification during twin-screw wet granulation and its application for process characterisation. Eur J Pharm Biopharm. 2019;137:77–85.
Vargas JM, Nielsen S, Cárdenas V, Gonzalez A, Aymat EY, Almodovar E, et al. Process analytical technology in continuous manufacturing of a commercial pharmaceutical product. Int J Pharm. 2018;538(1–2):167–78.
Chablani L, Taylor MK, Mehrotra A, Rameas P, Stagner WCJAP. Inline real-time near-infrared granule moisture measurements of a continuous granulation–drying–milling process. AAPS PharmSciTech. 2011;12(4):1050–5.
Silva BS, Colbert M-J, Santangelo M, Bartlett JA, Lapointe-Garant P-P, Simard J-S, et al. Monitoring microsphere coating processes using PAT tools in a bench scale fluid bed. Eur J Pharm Sci. 2019;135:12–21.
Domokos A, Pusztai É, Madarász L, Nagy B, Gyürkés M, Farkas A, et al. Combination of PAT and mechanistic modeling tools in a fully continuous powder to granule line: rapid and deep process understanding. Powder Technology. 2021;388:70–81.
Krier F, Mantanus J, Sacre PY, Chavez PF, Thiry J, Pestieau A, et al. PAT tools for the control of co-extrusion implants manufacturing process. Int J Pharm. 2013;458(1):15–24.
Galata DL, Meszaros LA, Ficzere M, Vass P, Nagy B, Szabo E, et al. Continuous blending monitored and feedback controlled by machine vision-based PAT tool. J Pharm Biomed Anal. 2021;196:113902.
Meszaros LA, Galata DL, Madarasz L, Kote A, Csorba K, David AZ, et al. Digital UV/VIS imaging: a rapid PAT tool for crushing strength, drug content and particle size distribution determination in tablets. Int J Pharm. 2020;578:119174.
Guay JM, Lapointe-Garant PP, Gosselin R, Simard JS, Abatzoglou N. Development of a multivariate light-induced fluorescence (LIF) PAT tool for in-line quantitative analysis of pharmaceutical granules in a V-blender. Eur J Pharm Biopharm. 2014;86(3):524–31.
Ponnammal P, Kanaujia P, Yani Y, Ng WK, Tan RBJP. Orally disintegrating tablets containing melt extruded amorphous solid dispersion of tacrolimus for dissolution enhancement. Pharmaceutics. 2018;10(1):35.
Anane-Adjei AB, Jacobs E, Nash SC, Askin S, Soundararajan R, Kyobula M, et al. Amorphous solid dispersions: Utilization and challenges in preclinical drug development within AstraZeneca. Int J Pharm. 2022;614:121387.
Adelusi TI, Oyedele A-QK, Boyenle ID, Ogunlana AT, Adeyemi RO, Ukachi CD, et al. Molecular modeling in drug discovery. Informatics in Medicine Unlocked. 2022;100880.
Glaab EJBiB. Building a virtual ligand screening pipeline using free software: a survey. Briefings in Bioinformatics. 2016;17(2):352–66.
Silver M, Cohen L. Monte Carlo simulation of anomalous transit-time dispersion of amorphous solids. Physical Review B. 1977;15(6):3276–8.
Eckert M, Neyts E, Bogaerts A. Modeling adatom surface processes during crystal growth: a new implementation of the Metropolis Monte Carlo algorithm. CrystEngComm. 2009;11(8).
Schlick T. Molecular modeling and simulation: an interdisciplinary guide: Springer; 2010.
McCammon JA, Gelin BR. Karplus MJn. Dynamics of folded proteins. Natures. 1977;267(5612):585–90.
Cui YJJoPS. Using molecular simulations to probe pharmaceutical materials. J Pharm Sci. 2011;100(6):2000–19.
Vogiatzis GG, Theodorou DNJAoCMiE. Multiscale molecular simulations of polymer-matrix nanocomposites. Archives of Computational Methods in Engineering. 2018;25(3):591–645.
Ojo AT, Lee PIJJoPS. A mechanistic model for predicting the physical stability of amorphous solid dispersions. J Pharm Sci. 2021;110(4):1495–512.
Huynh L, Grant J, Leroux J-C, Delmas P, Allen CJPr. Predicting the solubility of the anti-cancer agent docetaxel in small molecule excipients using computational methods. Pharm Res. 2008;25(1):147–57.
Giulini M, Rigoli M, Mattiotti G, Menichetti R, Tarenzi T, Fiorentini R, et al. From system modeling to system analysis: The impact of resolution level and resolution distribution in the computer-aided investigation of biomolecules. Frontiers in Molecular Biosciences. 2021;8.
Wegiel LA, Mauer LJ, Edgar KJ, Taylor LSJJops. Crystallization of amorphous solid dispersions of resveratrol during preparation and storage—Impact of different polymers. J Pharm Sci. 2013;102(1):171–84.
Yang F, Su Y, Small J, Huang C, Martin GE, Farrington AM, et al. Probing the molecular-level interactions in an active pharmaceutical ingredient (API)-polymer dispersion and the resulting impact on drug product formulation. Pharm Res. 2020;37(6):1–16.
Telang C, Mujumdar S, Mathew MJJops. Improved physical stability of amorphous state through acid base interactions. J Pharm Sci. 2009;98(6):2149–59.
Barmpalexis P, Karagianni A, Katopodis K, Vardaka E, Kachrimanis KJEJoPS. Molecular modelling and simulation of fusion-based amorphous drug dispersions in polymer/plasticizer blends. Eur J Pharm Sci. 2019;130:260–8.
Fule R, Meer T, Sav A, Amin PJJopi. Solubility and dissolution rate enhancement of lumefantrine using hot melt extrusion technology with physicochemical characterisation. Journal of pharmaceutical investigation. 2013;43(4):305–21.
Gangurde AB, Kundaikar HS, Javeer SD, Jaiswar DR, Degani MS, Amin PDJJoDDS, et al. Enhanced solubility and dissolution of curcumin by a hydrophilic polymer solid dispersion and its insilico molecular modeling studies. J Drug Deliv Sci Tech 2015;29:226–237.
Macháčková M, Tokarský J, Čapková PJEJoPS. A simple molecular modeling method for the characterization of polymeric drug carriers. Eur J Pharm Sci. 2013;48(1–2):316–22.
Ma S-M, Zhao L, Wang Y-L, Zhu Y-L, Lu Z-YJPCCP. The coarse-grained models of poly (ethylene oxide) and poly (propylene oxide) homopolymers and poloxamers in big multipole water (BMW) and MARTINI frameworks. Phys Chem Chem Phys. 2020;22(28):15976–85.
Rigby D, Sun H, Eichinger BJPI. Computer simulations of poly (ethylene oxide): force field, pvt diagram and cyclization behaviour. Polymer Int. 1997;44(3):311–30.
Sun HJTJoPCB. COMPASS: an ab initio force-field optimized for condensed-phase applications overview with details on alkane and benzene compounds. J Phy Chem. 1998;102(38):7338–64.
Wang J, Wang W, Kollman PA. Case DAJJomg, modelling. Automatic atom type and bond type perception in molecular mechanical calculations. J Mol Graphics. 2006;25(2):247–60.
Jorgensen WL, Maxwell DS, Tirado-Rives JJJotACS. Development and testing of the OPLS all-atom force field on conformational energetics and properties of organic liquids. Journal of the American Chemical Society 1996;118(45):11225–11236.
Brooks BR, Bruccoleri RE, Olafson BD, States DJ, Sa S, Karplus MJJocc. CHARMM: a program for macromolecular energy, minimization, and dynamics calculations. Journal of computational chemistry. 1983;4(2):187–217.
MacKerell AD Jr, Banavali N, Foloppe NJBORoB. Development and current status of the CHARMM force field for nucleic acids. Biopolymers. 2000;56(4):257–65.
Bhattacharya S, Suryanarayanan RJJops. Local mobility in amorphous pharmaceuticals—characterization and implications on stability. J Pharm Sci. 2009;98(9):2935–53.
Kothari K, Ragoonanan V, Suryanarayanan RJMp. Influence of molecular mobility on the physical stability of amorphous pharmaceuticals in the supercooled and glassy states. Mol Pharm. 2014;11(9):3048–55.
Gupta J, Nunes C, Vyas S, Jonnalagadda SJTJoPCB. Prediction of solubility parameters and miscibility of pharmaceutical compounds by molecular dynamics simulations. J Phys Chem. 2011;115(9):2014–23.
Kapourani A, Chatzitheodoridou M, Kontogiannopoulos KN, Barmpalexis PJMP. Experimental, thermodynamic, and molecular modeling evaluation of amorphous simvastatin-poly (vinylpyrrolidone) solid dispersions. Mol Pharm. 2020;17(7):2703–20.
Yani Y, Kanaujia P, Chow PS, Tan RBJI, Research EC. Effect of API-Polymer miscibility and interaction on the stabilization of amorphous solid dispersion: a molecular simulation study. Ind Eng Chem Res. 2017;56(44):12698–707.
Han R, Huang T, Liu X, Yin X, Li H, Lu J, et al. Insight into the dissolution molecular mechanism of ternary solid dispersions by combined experiments and molecular simulations. AAPS PharmSciTech. 2019;20(7):1–14.
Razmimanesh F, Amjad-Iranagh S, Modarress HJJoMM. Molecular dynamics simulation study of chitosan and gemcitabine as a drug delivery system. J Mol Model. 2015;21(7):1–14.
Xiang T-X, Anderson BDJJops. Molecular dynamics simulation of amorphous hydroxypropylmethylcellulose and its mixtures with felodipine and water. J Pharm Sci. 2017;106(3):803–16.
Mazurek AH, Szeleszczuk Ł, Pisklak DMJP. Periodic DFT calculations—review of applications in the pharmaceutical sciences. Pharmaceutics. 2020;12(5):415.
Meng F, Trivino A, Prasad D, Chauhan HJEJoPS. Investigation and correlation of drug polymer miscibility and molecular interactions by various approaches for the preparation of amorphous solid dispersions. Eur J Pharm Sci. 2015;71:12–24.
Maniruzzaman M, Pang J, Morgan DJ, Douroumis DJMp. Molecular modeling as a predictive tool for the development of solid dispersions. Mol Pharm. 2015;12(4):1040–9.
Nie H, Mo H, Zhang M, Song Y, Fang K, Taylor LS, et al. Investigating the interaction pattern and structural elements of a drug–polymer complex at the molecular level. Mol Pharm. 2015;12(7):2459–68.
Wang B, Wang D, Zhao S, Huang X, Zhang J, Lv Y, et al. Evaluate the ability of PVP to inhibit crystallization of amorphous solid dispersions by density functional theory and experimental verify. Eur J Pharm Sci. 2017;96:45–52.
Elbadawi M, Gaisford S, Basit AW. Advanced machine-learning techniques in drug discovery. J Drug Deliv Sci Tech. 2021;26(3):769–77.
Mehta CH, Narayan R, Nayak UYJDDT. Computational modeling for formulation design. Drug Discovery Today. 2019;24(3):781–8.
Rantanen J, Khinast JJJops. The future of pharmaceutical manufacturing sciences. J Pharm Sci. 2015;104(11):3612–38.
Yoshida F, Topliss JGJJomc. QSAR model for drug human oral bioavailability. J Medi Chem. 2000;43(13):2575–85.
Huang Y, Dai W-GJAPSB. Fundamental aspects of solid dispersion technology for poorly soluble drugs. Acta Pharmaceutica Sinica B. 2014;4(1):18–25.
Ricarte RG, Van Zee NJ, Li Z, Johnson LM, Lodge TP, Hillmyer MAJMp. Recent advances in understanding the micro-and nanoscale phenomena of amorphous solid dispersions. Mol Pharm. 2019;16(10):4089–103.
Chan T. Ouyang DJajops. Investigating the molecular dissolution process of binary solid dispersions by molecular dynamics simulations. asian journal of pharmaceutical sciences. 2018;13(3):248–54.
Jha PK, Larson RGJMp. Assessing the efficiency of polymeric excipients by atomistic molecular dynamics simulations. Mol Pharm. 2014;11(5):1676–86.
LaFountaine JS, McGinity JW, Williams ROJAP. Challenges and strategies in thermal processing of amorphous solid dispersions: a review. AAPS Pharmscitech. 2016;17(1):43–55.
AboulFotouh K, Zhang Y, Maniruzzaman M, Williams III RO, Cui ZJIJoP. Amorphous solid dispersion dry powder for pulmonary drug delivery: Advantages and challenges. Int J Pharm. 2020;587:119711.
Mangal S, Park H, Zeng L, Heidi HY, Lin Y-w, Velkov T, et al. Composite particle formulations of colistin and meropenem with improved in-vitro bacterial killing and aerosolization for inhalation. Int J Pharm. 2018;548(1):443–53.
Pawar J, Tayade A, Gangurde A, Moravkar K, Amin P. Solubility and dissolution enhancement of efavirenz hot melt extruded amorphous solid dispersions using combination of polymeric blends: a QbD approach. Eur J Pharm Sci. 2016;88:37–49. https://doi.org/10.1016/j.ejps.2016.04.001.
Rathod V, Stagner WC, Gajera B, Haware RV. Hybridized nanoamorphous micellar dispersion using a QbD-DM(3) linked rational product design strategy for ritonavir: A BCS IV drug. Int J Pharm. 2020;588:119727. https://doi.org/10.1016/j.ijpharm.2020.119727.
Jana S, Ali SA, Nayak AK, Sen KK, Basu SKJCER, Design. Development of topical gel containing aceclofenac-crospovidone solid dispersion by “quality by design (QbD)” approach. Chemical Engineering Research. 2014;92(11):2095–105.
Kaur P, Singh SK, Garg V, Gulati M, Vaidya YJPT. Optimization of spray drying process for formulation of solid dispersion containing polypeptide-k powder through quality by design approach. Powder Technology. 2015;284:1–11.
Pawar J, Suryawanshi D, Moravkar K, Aware R, Shetty V, Maniruzzaman M, et al. Study the influence of formulation process parameters on solubility and dissolution enhancement of efavirenz solid solutions prepared by hot-melt extrusion: a QbD methodology. Drug Delivery Translational Research. 2018;8(6):1644–57.
Chavan RB, Thipparaboina R, Yadav B, Shastri NRJD. research t. Continuous manufacturing of co-crystals: challenges and prospects. Drug delivery translational research. 2018;8(6):1726–39.
Thakral NK, Mohapatra S, Stephenson GA, Suryanarayanan R. Compression-induced crystallization of amorphous indomethacin in tablets: characterization of spatial heterogeneity by two-dimensional X-ray diffractometry. Mol Pharm. 2015;12(1):253–63.
Acknowledgments
The authors are grateful to the Indian Institute of Technology (Banaras Hindu University), Varanasi, for providing infrastructure facilities. AM Healy acknowledges funding from Science Foundation Ireland under grant number 12/RC/2275_P2 co-funded under the European Regional Development Fund.
Author information
Authors and Affiliations
Contributions
Amritha G. Nambiar: conceptualization, literature survey, a compilation of data, and original draft writing. Maan Singh: writing, reviewing, and editing. Abhishek R Mali: writing, review, and editing. Dolores R. Serano: writing, editing, and reviewing. Rajnish Kumar: writing, editing, and reviewing. Anne Marie Healy: conceptualization, writing, editing, and reviewing. Ashish Kumar Agrawal: writing, editing, and reviewing. Dinesh Kumar: conceptualization, writing, editing, reviewing, overall modification, and correction. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nambiar, A.G., Singh, M., Mali, A.R. et al. Continuous Manufacturing and Molecular Modeling of Pharmaceutical Amorphous Solid Dispersions. AAPS PharmSciTech 23, 249 (2022). https://doi.org/10.1208/s12249-022-02408-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1208/s12249-022-02408-4