Abstract
Data sources
PubMed, Ovid, EMBASE and LILACS were searched up to December 2011. In addition, the reference lists of the selected review papers were further hand searched. Language was limited to studies published only in English.
Study selection
Human and animal randomised clinical trials (RCT), systematic reviews of RCTs, non-randomised trials, case series that reported on the clinical, radiographic, and/or histological outcomes of dental/oral implants exposed to excessive load were considered eligible for inclusion.
Data extraction and synthesis
Identified studies were evaluated by one non-blinded reviewer according to the selection criteria. When doubt arose co-authors assisted until consensus was reached. The data extracted from the clinical studies included study design, patients/implants/prostheses/loading time/follow-up time, type of intervention/methods, outcome, and, specific to animal studies, the animal model, intention to overload (ie yes or no), load mode, type of loading (ie dynamic or static), and microbial control if any. The heterogeneity among studies did not allow data to be combined.
Results
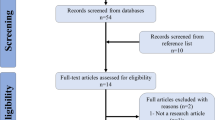
The search strategy in addition to hand searching retrieved 726 potentially eligible studies after de-duplication. After screening the 41 full-text relevant studies and applying the selection criteria assessment, only three non-randomised split-mouth animal studies and one systematic review of animal experimental data were considered for inclusion. The non-randomised studies could not reveal any relationship between increased leverage on dental implants and marginal loss. The systematic review suggested that supra-occlusal contacts on uninflamed peri-implant bone tissue did not cause catabolism, whereas supra-occlusal contacts combined with inflammation significantly increased the plaque-induced catabolism.
Conclusions
The effect of implant overload on bone/implant loss in clinically well-integrated implants is poorly reported and provides little unbiased evidence to support a cause-and-effect relationship.
Similar content being viewed by others
Commentary
Previous to this review, studies derived from clinical and animal observations have suggested that biomechanical and occlusal overload on a well-osseointegrated oral implant can result in loss of the marginal bone or even in late implant failure.1,2,3,4,5,6_ENREF_3 However, there is still a need to clarify the biological consequences that overloading might have on osseointegrated oral implants.
The title of this review lacked clear identification as a systematic review. The review question, inclusion criteria, hand searching and search strategy were conversely clearly described. The review was limited to English language articles. The authors described all information sources well and contacted study authors to request further information. Yet, if this search strategy were better designed, it likely would have retrieved the primary studies cited in the included systematic review. In addition, the authors failed to mention the method for data extraction and the number of authors who participated at each step. The reasons for exclusion of the studies that were eliminated after quality assessment were well described and the risk of bias was clearly defined. However, the authors did not report the score of each of the included studies but rather they presented them grouped in tables: those eliminated due to high risk of bias and those included for the review. For the final study selection it was thus surprising that they considered a system review.7 On the whole, most of the potential limitations were well addressed.
It was difficult to reveal any correlation between occlusal overload and marginal bone loss or implant failures from the few well-conducted studies retrieved as their scope was short term and their conclusions were weak. The authors acknowledge the need to interpret the results on overload of stable osseointegrated implants with caution since the literature is very limited and mostly biased. They also note the introduction of a language bias by restricting the review to studies published only in English. Most of the knowledge in this field, moreover, is derived from animal experimental studies. In turn, this left the PICO question unanswered.
References
Esposito M, Hirsch JM, Lekholm U, Thomsen P . Biological factors contributing to failures of osseointegrated oral implants. (II). Etiopathogenesis. Eur J Oral Sci 1998; 106:721–764.
Adell R, Lekholm U, Rockler B, Brånemark PI . A 15-year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg 1981; 10:387–416.
Isidor F . Influence of forces on peri-implant bone. Clin Oral Implants Res 2006; 17:8–18.
Jovanovic SA . The management of peri-implant breakdown around functioning osseointegrated dental implants. J Periodontol 1993; 64:1176–1183.
Afrashtehfar KI, Qadeer S . Computerized occlusal analysis as an alternative occlusal indicator. Cranio 2016; 34:52–57.
Afrashtehfar KI, Manfredini D . Five things to know about bruxism. J N J Dent Assoc 2013; 84:26.
Chambrone L, Chambrone LA, Lima LA . Effects of occlusal overload on peri-implant tissue health: a systematic review of animal-model studies. J Periodontol 2010; 81:1367–1378.
Gotfredsen K, Berglundh T, Lindhe J . Bone reactions adjacent to titanium implants subjected to static load. A study in the dog (I). Clin Oral Implants Res 2001; 12:1–8.
Kozlovsky A, Tal H . Laufer B-Z, et al. Impact of implant overloading on the peri-implant bone in inflamed and non-inflamed peri-implant mucosa. Clin Oral Implants Res 2007; 18:601–610.
Splawinski J, Kuzniar J . Clinical trials: active control vs placebo--what is ethical? Sci Eng Ethics 2004; 10:73–79.
Fu JH, Hsu YT, Wang HL . Identifying occlusal overload and how to deal with it to avoid marginal bone loss around implants. Eur J Oral Implantol 2012; 5:S91–S103.
Acknowledgements
To Dr. Ben Balevi, faculty at the University of British Columbia and private practitioner in Vancouver, Canada, for his valuable guidance in the appraisal of this summary review.
Author information
Authors and Affiliations
Additional information
Address for correspondence: Prof. Ignace Naert, KU Leuven (Catholic University of Leuven), Kapucijnenvoer 7 blok a bus 7001, BE-3000 Leuven, Belgium. Tel. 0032 16 33 24 58/38, Fax: 0032 16 33 23 09. E-mail: Ignace.Naert@med.kuleuven.be
Naert I, Duyck J, Vandamme K. Occlusal overload and bone/implant loss. Clin Oral Implants Res 2012; 23: 95–107. doi: 10.1111/j.1600-0501.2012.02550.x.
Rights and permissions
About this article
Cite this article
Afrashtehfar, K., Afrashtehfar, C. Lack of association between overload and peri-implant tissue loss in healthy conditions. Evid Based Dent 17, 92–93 (2016). https://doi.org/10.1038/sj.ebd.6401193
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.ebd.6401193
- Springer Nature Limited
This article is cited by
-
Titanium-base abutments may have similar long-term peri-implant effects as non-bonded one-piece abutments
Evidence-Based Dentistry (2022)