Abstract
Data from dry bone samples, collected from anatomical or archaeological collections, can improve the knowledge regarding accessory foot bones, including prevalence, size, shape and laterality, that can be useful in disparate fields of research, from medicine to bioarcheology. In the present study, the prevalence of six accessory foot bones (os trigonum, calcaneus secundarium, accessory navicular bone, os vesalianum, os sustentaculum and os intermetatarseum) was assessed in a sample of 486 individuals (226 females, 260 males) from the Coimbra Identified Skeletal Collection (CISC). The most frequent accessory bones are os trigonum (9.9%; 48/485) and calcaneus secundarium (6.0%; 29/486), while the most uncommon is os sustentaculum (0.4%; 2/486). No sex differences were observed. All accessory bones occur more often unilaterally, with the exception of the accessory navicular bone that, in the majority of cases, occurs bilaterally. The unilateral expression of os trigonum, calcaneus secundarium and os vesalianum was mostly in the right foot. The co-occurrence of accessory foot bones was recorded in 1.7% of the individuals (8/486), and the combinations of os trigonum and calcaneus secundarium were the most frequently observed. This research emphasizes the relevance of conducting studies on reference skeletal collections in order to gain a comprehensive understanding of anatomical variations in the foot. This understanding is crucial for accurate diagnoses and successful treatment in clinical settings, as well as for establishing population comparison standards in the fields of bioarchaeology and forensic anthropology.
Similar content being viewed by others
Introduction
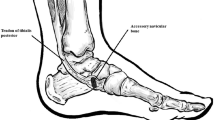
The human foot is characterized by an intricate and distinctive anatomy, and has been comprehensively studied in both evolutionary and clinical contexts1. Several skeletal variations, including accessory bones, bipartitions and coalitions, have been described since the sixteenth century2 (Fig. 1), but particularly after the second half of the nineteenth century, with the contribution of different researchers, such as Wenzel Gruber3, Ludwig Stieda4, Karl von Bardeleben5, William Pfitzner6, Thomas Dwight7, and Emil Geist8.
According to Kelikian and Sarrafian9, accessory bones, or accessory ossicles, are defined as developmental anomalies that stem from an abnormal division of a normal primary ossification center or from the failure of union of a secondary ossification center to the main bone. A plethora of accessory bones of the foot have been described in the literature and documented in identified skeletal or anatomical collections, cadaver dissections and in vivo through medical imaging10,11. Some are uncommon and unacknowledged, while others are known under different designations stirring some bewilderment in the research landscape concerning accessory bones of the foot. Their reported prevalence is varied, and mostly derived from clinical/epidemiological contexts, e.g.,12,13,14,15,16,17, but also from anthropological studies, e.g.,18,19,20,21,22. In general, these skeletal variations are asymptomatic23, but sometimes can cause complications that result in painful syndromes or degenerative changes secondary to trauma, overuse or chronic stress10,11,24.
Accruing an extensive knowledge about the epidemiology of accessory ossicles in the foot can be beneficial in various domains, including the surgical and medical management of the foot, bioarchaeology, and forensic anthropology. Their potential use as an indicator of genetic relatedness in anthropological and archaeological studies has been emphasized18,19,22,25,26,27,28, while in medico-legal contexts, their documentation improves the assessment of the biological profile of an individual and, particularly in the presence of rare skeletal variants, contributes to a positive identification29.
In the medical practice, particularly in the emergency hospital context, they are frequently confused with fractures11,30, a problem already recognized since the end of the nineteenth century6,7,8. Given the potential for misinterpretation, emergency physicians should be familiar with uncommon normal variants of the foot and ankle, and their skeletal development and radiographic appearances, to enable the correct diagnosis, thus avoiding unnecessary complications and treatments14,23,31.
This study aims to thoroughly document the frequency of six types of accessory foot bones, namely os trigonum, os calcaneus secundarium, accessory navicular bone, os sustentaculum, os vesalianum, and os intermetatarseum, according to biological sex, size and morphology, co-occurrence and laterality, in a sample from the Coimbra Identified Skeletal Collection, imparting a template for the improvement of the diagnosis and interpretation of accessory ossicles in both the clinical and anthropological contexts.
Materials and methods
Study sample
The present study was implemented at the Coimbra Identified Skeletal Collection (CISC), a reference skeletal collection assembled during the twentieth century that includes 505 skeletons of individuals predominantly collected in shallow graves of the largest public cemetery of Coimbra (Portugal), Cemitério da Conchada. Biographical information for the skeletal individuals includes, among others, the place of birth, occupation, biological sex, age at death and cause of death. The individuals in the collection are primarily Portuguese nationals of lower socioeconomic status, and involved in unskilled manual work. They were born between 1822 and 1921, and deceased between 1904 and 193632,33. The study-base comprises 486 individuals (226 females, 260 males), with ages-at-death ranging from twelve to 96 years old.
The accessory ossicles of the foot
Although the majority of the skeletons are complete and well-preserved, it is impossible to fathom if every small accessory and sesamoid bones were collected during excavation. This constrained the selection of accessory bones; accordingly, six were included in this study: os trigonum, os calcaneus secundarium, accessory navicular bone, os sustentaculum, os vesalianum, and os intermetatarseum.
In archaeological samples or skeletal collections, the presence of accessory ossicles will mainly be identified by the presence of more or less pronounced notches with some expositions of internal trabecular bone, since rarely the accessory bone is collected19.
Os trigonum
The posterior region of the talus (or processus posterior tali) includes the posterolateral and the posteromedial tubercles, separated by the fibro-osseous tunnel for the flexor hallucis longus tendon. Between the ages of eight and 11/13 years a secondary ossification center appears posteriorly to the posterolateral process15. Usually, this ossification center fuses within one year of its appearance, leading to a large posterolateral process named Stieda’s process, trigonal process or fused os trigonum. If it remains separate from the talus, due to the failure of the secondary ossification center to fuse, it is identified as os trigonum34. This developmental skeletal variation was scored as present when a notch was identified in the posterolateral process of the talus. The cases of fused os trigonum, recognized by the presence of a fusion line visible on plantar view, were also documented.
Measurements included the maximum mesio-lateral length of the defect along the border of the articular surface, maximum width (measurement perpendicular to the previous one) and depth of the notch (Supplementary material: Figure S1). If preserved, the size and morphology of the accessory bone was recorded.
Os calcaneus secundarium
The os calcaneus secundarium is an ossicle located in the anterior calcaneal facet, specifically in the interval between the anteromedial aspect of the calcaneus, the cuboid, the talar head and the tarsal navicular, and it is mostly recognized as a notch in this area. It can be round but it is more often triangular10,11.
Measurements included the maximum anteroposterior length and the depth of the notch, following Mann35, and maximum breadth (Supplementary material: Figure S2).
Accessory navicular bone
The accessory navicular bone, also named os naviculare secundarium, os tibiale, tibiale externum, accessory scaphoid, pre-hallux, bifurcate navicular, divided navicular, and accessory tarsal scaphoid, is a supernumerary foot bone located medially to the navicular tuberosity. It ensues as a preformed cartilage at the gestational age of around two months9,22. The main body of the navicular commences ossification at the end of the second year of life in females, and at the beginning of the fourth year in males. Between the ages of nine and 13, a secondary center of ossification may appear, and fuses shortly thereafter36. When it fails to fuse to the main body of the navicular, an accessory navicular bone occurs.
Three types of this anatomical variant have been defined in the biomedical literature: Types I, II and III10,11. A new subtype, Type II.a, is described in this study.
Type I: Freestanding spherical shape ossicle, partially embedded within the tibialis posterior tendon. This ossicle has been often confused with sesamoid of the tibialis posterior tendon due to their association.
Type II: Triangular or heart-shaped accessory bone attached to the navicular tuberosity by a cartilaginous or fibrocartilaginous bridge37. This type is identified by flattened and porous surface of the navicular tuberosity (as well as the ossicle), being easily identified in dry bone—even in the absence of the small ossicle. It was considered necessary to create a new subtype, Type II.a, when the ossicle was fused and the fusion line was still visible (Supplementary material: Figure S3). Performed measurements included the maximum length at the fusion margin and maximum height.
Type III: Fusion of the accessory bone to the navicular tuberosity, forming a large, hook-like protuberance classified as cornuate navicular38.
Type I does not leave any anatomical evidence of its presence since the freestanding ossicle does not articulate with the navicular tuberosity. Therefore, it is almost impossible to identify it in skeletal collections. Subjectivity regarding the definition of type III precluded its inclusion in this study. Henceforth, only types II and II.a were scored as present or absent.
Os sustentaculum
The sustentaculum tali is a shelf-like projection on the medial aspect of the calcaneus that supports the anterior articular facet of the talus. On its inferior aspect, a groove is present for the flexor hallucis longus tendon. An accessory ossicle, os sustentaculum, is uncommonly found at its posterior end. It is usually bridged to the calcaneus via a fibrous or fibrocartilaginous tissue. The os sustentaculum forms through the extension of the fibrocartilaginous talocalcaneal bridge originating from the posterior part of the sustentaculum tali9,10.
Measurements collected included the maximum anteroposterior length, and the maximum width (Supplementary material: Figure S4).
Os vesalianum
This rare accessory ossicle is located proximally to the base of the fifth metatarsal, within the peroneus brevis tendon, and sometimes it articulates with the cuboid11,39. The fifth metatarsal ossifies from two main ossification centers during development: a primary center for the shaft, and a secondary ossification center for the head. The ossification of the former starts at about the third month of gestation, and for the latter, it appears between the third and fourth years. These ossification centers unite at about 14 to 16 years of age. At the age of 10 years in girls and 12 years in boys another apophyseal line appears at the base of the fifth metatarsal. The fusion of the apophysis and the metatarsal base typically ensues in the following two to four years. The failure of this fusion seems to be the cause of this anatomical variant36.
Collected measurements included the maximum length along the proximal basal articulation and the maximum height (Supplementary material: Figure S5).
Os intermetatarseum
This ossicle is located between the medial cuneiform and the base of the first and the second metatarsals, and ossifies during adolescence or shortly before. Although presenting with variable size and morphology, it is usually spindle-shaped. Os intermetatarseum can occur free or fused with one of the three previously mentioned bones9,40. In this study only fused cases were recorded, confirmed through the recognition of a fusion line. Measurements taken in this ossicle included the length along the fusion line and the maximum height (Supplementary material: Figure S6).
Statistical analysis
The frequency of each accessory ossicle was estimated as its prevalence and reported as a percentage. A chi-square (X2) test of independence was performed under the null hypothesis that the proportion of individuals presenting with an accessory ossicle is the same in each sex. The proportion of accessory ossicles in each foot was compared through a Pearson's chi-square test with n-1 correction. A student’s t-test (independent samples) was employed to evaluate the null hypothesis that the mean age-at-death was equal in individuals with and without accessory ossicles of the foot. All statistical analyses were performed with JASP (v. 0.17.2).
Results
Accessory bones of any type were observed in 89 individuals (18.3%; 89/486), 44 females (19.5%; 44/226) and 45 (17.3%; 45/260) males. There is no significant association between biological sex and presence of accessory bones (X2: 0.378, df = 1, p = 0.539). The average age at death of individuals with (mean = 46.1 years; sd = 19.7) and without (mean = 46.1 years; sd = 17.9) accessory bones is virtually the same (Student’s t-test: 0.008, df = 483, p = 0.994). The prevalence of the different foot ossicles per individual is summarized in Table 1. Likewise, the prevalence of foot ossicles in each foot is depicted in Tables 2 and 3.
In eight individuals, four females (1.8%; 4/226) and four males (1.5%; 4/260), the co-occurrence of accessory foot bones was recorded (1.6%; 8/486). Co-occurrence is thus present in 9.0% (8/89) of the individuals with accessory ossicles. The most frequent combination, documented in five individuals (two females and three males), was the presence of os trigonum and calcaneus secundarium. The co-occurrence of calcaneus secundarium and os intermetatarseum was observed in only one male, of calcaneus secundarium and os vesalianum in one female, and of os trigonum and os vesalianum in one female (Table 4). No pathological conditions—including fractures and degenerative joint diseases—were identified in direct association with any of the recorded accessory bones, with the exception of a mild degenerative change in a left accessory navicular bone (see below).
Os trigonum
Os trigonum was the most frequently observed accessory bone in this study, being present in 48 individuals (9.9%, 48/485; Table 1). The prevalence was 8.9% in females (20/225) and 10.8% in males (28/260); the proportion of individuals with this type of accessory bone did not differ by sex (X2: 0.478, df = 1, p = 0.489). Seventeen individuals (35.4%, 17/48), five females and twelve males, presented the ossicle bilaterally (Fig. 2). Among them, one female and three males exhibited bilateral fusion. In ten males (five in the left and five in the right foot) and five females (three in the left and two in the right foot), it was recorded a unilateral fusion of this accessory bone (Fig. 3). In total, 19 individuals (37.5%; 19/48) exhibited a fused os trigonum.
The prevalence is 7.9% (38/479) in the left foot (Table 2), 6.8% in females (15/222) and 8.9% in males (23/257). Three of the affected females (20.0%, 3/15) and eight of the affected males (34.8%, 8/23) exhibited a fused os trigonum in the left foot. In the right foot, the frequency is 5.6% (27/481), 10 females (4.5%, 10/222) and 17 males (6.6%, 17/259, Table 3). Of those affected, three females (30.0%; 3/10) and eight males (47.1%; 8/17) showed a fused os trigonum in the right foot. This ossicle was observed bilaterally in 35.5% (17/48) of the individuals.) Most of the unilateral cases were found on the left foot (67.7%; 21/31), while only 32.3% (10/31) of the unilateral cases were observed on the right foot. The difference in the prevalence between the left and right feet is not statistically significant (X2: 2.016, df = 1, p = 0.156).
The more frequent location of this accessory bone is in a notch/indentation along the posterolateral tubercle. A less frequent location was also observed, namely an extension of the ossicle in the superodistal direction, into the trochlear surface, and so depthless (Fig. 4). This location was recorded in five individuals (bilaterally in two males, unilaterally on the left foot in two females, and unilaterally on the right foot in one male). Length varies between 6.0 mm and 16.5 mm, the width between 2.0 mm and 10.0 mm, and the depth between 0.5 mm and 1.0 mm.
Diverse studies, namely the ones based on radiological images, can only detect cases of free ossicles. In order to allow comparisons, more detailed results are presented in Table 5. In sum, 6.7% (65/960) observed feet display os trigonum (free + fused), 25 belonging to females, and 40 to males.
Four ossicles belonging to three individuals (one female and two male) were recovered (Fig. 5). Length ranges between 8 and 10mm, while maximum height, between 4 and 7mm.
Calcaneus secundarium
The total prevalence of calcaneus secundarium per individual is 6.0% (29/486, Table 1). This ossicle was present in 16 females (7.1%; 16/226) and 13 males (5.0%; 13/260), with no significant association between sex and this ossicle’s presence (X2: 0.932, df = 1, p = 0.334). Eight individuals, three females and five males, displayed this ossicle in both feet (27.6%, 8/29; Fig. 6). Only one fused calcaneus secundarium was documented for a right unilateral expression on a male individual (Fig. 7).
In the left foot, the prevalence is 3.1% (15/478, Table 2), being 3.1% in both females (7/223) and males (8/255). The prevalence in the right foot is 4.6% (22/476, Table 3), 5.4% in females (12/222) and 3.9% in males (10/254). This accessory bone is expressed bilaterally in 27.6% of the individuals. Among the unilateral cases, 66.7% (14/21) were observed on the right foot. There is no association between laterality and the presence of calcaneus secundarium (X2: 1.449, df = 1, p = 0.229). Maximum anteroposterior length ranges from 0.4 to 18 mm, maximum breadth, from 0.2 to 0.6 mm, and depth, between 0.1 and 0.4mm.
Accessory navicular bone
Accessory navicular of Type II, including the subtype II.a, was observed in nine individuals (1.9%, 9/485), seven females (3.1%, 7/226) and two males (0.8%, 2/259, Table 1). There was not a statistically significant association between sex and the presence of accessory navicular bone (Fisher’s exact test: p = 0.089). Six individuals (66.7%, 6/9), five females and a male, presented with a bilateral occurrence (Fig. 8). These included four bilateral Type II cases, one bilateral Type II.a case, and another with a combination of Types II and II.a. The unilateral cases were observed in three individuals, two females (one on each foot) and one male (left foot). In the female with bilateral Type II, both ossicles were recovered, measuring 1.8 × 1.2 mm and 1.7 × 1.5 mm, respectively maximum length and height. In the left bones, some degenerative changes were visible in the attachment area (Fig. 9).
The prevalence of accessory navicular bone in the left foot is 1.5% (7/481, Table 2), 2.2% in females (5/225) and 0.8% in males (2/257). In the right foot, the prevalence is 1.5% (7/481, Table 3), varying from 2.7% in females (6/224) and 0.4% in males (1/257). Maximum length of the accessory navicular bone ranges from 7.0 to 18.0 mm, while width ranges from 4.0 to 12.0 mm.
Os sustentaculum
Only two individuals (0.4%, 2/486) presented os sustentaculum (Table 1). One female (0.4%, 1/226) was affected in both feet (Fig. 10), while a male (0.4%, 1/260) was affected in the left foot (Fig. 11).
The bilateral case is unusually large, with the affected area measuring 28 × 11 mm and 22 × 10 mm, respectively for the left and right bones. Both ossicles were recovered, measuring 25mm × 10 mm (left) and 20mm × 0.85 mm (right). A small area without exposure of the trabecular bone is visible on their margins. In the male individual the defect is small, measuring 8 × 2 mm, and it is located on the posterior end of the posterior articular surface (Fig. 11).
Os vesalianum
This accessory bone was found in six individuals (1.2%, 6/485, Table 1), four females (1.8%, 4/226) and two males (0.8%, 2/259). The difference between the sexes is not significant (Fisher’s exact test: p = 0.424). There were two bilateral cases (33.3%, 2/6), one female and one male (Fig. 12). In two individuals (one bilateral and one right unilateral case), the accessory bone was recovered, revealing a triangular shape.
The prevalence of os vesalianum in the left side is 0.4% (2/477, Table 2), 0.4% in both females (1/226) and males (1/251). In the right foot, the total prevalence is 1.3% (6/480, Table 3), 1.8% in females (4/224) and 0.8% in males (2/256). The frequency is not significantly different between the left and right feet (X2: 2.293, df = 1, p = 0.130). All unilateral cases were observed on the right foot, with the only fused ossicle observed in the right foot of a male individual (Fig. 13). Maximum length varies between 12.0 and 16.0 mm, and maximum height between 7.5 and 12 mm.
Os intermetatarseum
Os intermetatarseum was identified in four individuals (0.8%, 4/486, Table 1), all of them males (1.5%, 4/260). Nevertheless, the difference between sexes does not reach statistical significance (Fisher’s exact test: p = 0.127). In three cases, the ossicle was fused to the medial cuneiform (Fig. 14) and in one case it was fused to the second metatarsal. The ossicle occurrs bilaterally in two individuals (50.0%, 2/4), and both unilateral cases are on the right foot. The total prevalence in the right foot is 0.8% (4/480), being 1.5% in males (4/259). In the left side, the prevalence is 0.4% (2/476), 0.8% in males (2/256; X2: 0.640, df = 1, p = 0.424). Maximum length varies between 3.0 and 7.0 mm, while maximum height ranges from 3.0 to 8.0 mm.
Discussion
A systematic assessment of accessory foot bones, including their prevalence, location, morphology and size, is essential to differentiate between normal anatomical variants and pathological processes in the clinical practice, but also in past population studies11,14,16,39. The frequency of accessory ossicles of the foot and ankle in different populations is heteroclite, varying from 18.0 to 49.2%10,13,41,42. In the present analysis, the prevalence of accessory foot ossicles is in the vicinity of the lower end of reported population frequencies; however, these miscellaneous studies recorded a different suite of accessory foot and ankle bones. Keles-Celik et al.11, for example, list 24 accessory ossicles of the foot and ankle, while only six were assessed in this study design. Sex differences in the prevalence of accessory foot bones are negligible, an epidemiological outline also observed in other population samples13,42.
The co-occurrence of accessory bones is infrequently documented but not completely unnoticed. Already in 1925, Heimerzheim described an individual presenting with os trigonum, os supranaviculare, os vesalianum, os peroneum and an accessory navicular bone. There is a scarcity of studies investigating the prevalence of the simultaneous presence of two or more distinct accessory bones, but recent epidemiological surveys have explored the co-occurrence of accessory ossicles, with frequencies ranging from 3.4% to 10.6%13,41,42,43. Several co-occurrences were identified in the CISC sample, but the prevalence is considerably lower than the ones listed in the epidemiological studies. In this study, os trigonum is frequently associated with calcaneus secundarium, an outline that is absent in other studies13,44. Interestingly, os sustentaculum and accessory navicular bone did not occur together with any other of the studied accessory ossicles. This is noteworthy since the accessory navicular bone is one of the most common accessory foot bones43.
Os trigonum
Os trigonum is one of the most documented accessory foot bones in the anatomical and clinical literature11,42. During the first half of the twentieth century, different authors discussed this ossicle recognizing its origin as an unfused secondary ossification center of the posterolateral talar tubercle45,46,47,48. In medical imaging studies, this ossicle is commonly an incidental finding, and can be confused with a fracture – Shepherd’s fracture—of the lateral posterior process of the talus. The prevalence of os trigonum in the present study is congruent with previous studies, which range from 1.7 to 25.0%10,13,42 (Table 6). However, the comparison of data from reports that use different scoring methods or that present frequencies per individual or per foot is not straightforward. Some studies only consider free cases of this accessory bone, while others include both free and fused cases. Moreover, the interpretation of fused cases raises another relevant question, namely the distinction between an enlarged posterolateral process and a fused os trigonum in the absence of visible fusion line, as previously noted by Zwiers et al.15, and here confirmed. In order to surpass this constraint, in the present study, fused os trigonum were only scored if a fusing line was identified.
This ossicle displays a wide spectrum of size and shape. It is usually single (rarely bipartite), and small (less than 1 cm), triangular, round or oval in shape, presenting three surfaces: anterior, inferior and posterior. The former attaches to the lateral tubercle by fibrous, fibrocartilaginous, or cartilaginous tissue and the inferior, articulates with the calcaneus. The posterior surface is non-articular9,10,16. In skeletal collections, the free ossicle is frequently not recovered, and its size can only be estimated considering the maximum length along the notch present in the posterolateral process. In the CISC sample, all the recovered free ossicles are solitary and triangular.
Heimerzheim49 and Kelikian and Sarrafian9 asserted that this ossicle occurs bilaterally most frequently. Nonetheless, in other studies—including the present one—unilateral cases have been recorded more often15,41, regardless of the scoring method (Table 6). Results are diverse concerning side dominance in unilateral cases, with no side differences. In general, the differences in prevalence between sexes are not significant (Table 7).
Calcaneus secundarium
Reported prevalence rates for calcaneus secundarium are heteroclite, ranging from 0.1 to 15.0% (Table 8). Laterality and sex dominance are rarely explored for this accessory ossicle, probably due to its low frequency. Mann35 observed that bilaterality was infrequent, without sex or side dominance—similarly to the results of the present study. On the other hand, Pfitzner6 documented a tendency for the bilateral expression of CS.
Accessory navicular bone
According to clinical literature, the accessory navicular bone is the most common accessory bone of the foot, being usually asymptomatic43,50. Still, it is also the most likely to present symptoms, as pain (chronic or acute) on the medial aspect of the foot, and several foot problems, such as posterior tibial tendon pathology and flattening of the medial longitudinal arch51. In clinical studies, its prevalence ranges from 1.2 to 13.7%6,8,41,45,49,52 (Table 9). Prevalence in skeletal remains from three anatomical and two archaeological collections ranged between 1.2% and 3.5%22. The prevalence of the accessory navicular in the CISC sample is among the values obtained in both archaeological and clinical studies, being the second most common accessory bone.
Several studies depict a higher frequency among females50,52,53,54, although others—including the present study—document a similar prevalence in both sexes22,41,55. The higher prevalence in modern females can be related to the type of shoes worn and ligamentous laxity56.
Laterality reports are also conflicting, as different studies claim that this accessory bone is most often bilateral6,53,55, unilateral8,22,41, or without differences between unilateral and bilateral expressions39. In the present study, most of the cases are bilateral.
Os sustentaculum
This accessory bone rarely occurs as a distinct bone, with an estimated prevalence of 0.3—1.0%9,10. Correspondingly, the prevalence obtained in the CISC sample is within these limits. This ossicle is usually asymptomatic10, but can become symptomatic secondarily to trauma, chronic stress or degenerative changes57,58. This ossicle can also be confused with a fracture in the region of the sustentaculum tali10. The bilateral case observed in a female from the CISC stands out due to the large size of the accessory bone, while the unilateral left case observed in a male is similar to the one described by Pfitzner (1896: Fig. 11)6.
Os vesalianum
The uncommonness of this accessory ossicle was already noted by Pfitzner6 and Dwight7. The documented prevalence of this anatomical variant ranges from 0.1 to 1.0%10,41, but slightly higher frequencies are also reported59 (Table 10). Accordingly, it is seldom mentioned in the anthropological literature. In the present study, six individuals (1.2%) exhibit this ossicle, which corresponds to one of the highest reported frequencies. No sex or side differences were found, similarly to recent radiological surveys13,59,60.
Os intermetatarseum
Reported prevalences of os intermetatarseum are diverse (Table 11). In general, anatomical studies report higher prevalences than radiographic studies, which tend to document prevalence rates below 2.0%6,7,14,21,41. These differences can be justified, at least in part, with the difficulty to properly identify this ossicle in standard radiographic views. However, in anatomical collections of individuals without soft tissues, only two of the three discrete ossicle types can be observed. Thus, prevalence comparison between different studies is hampered. In the CISC sample, the observed prevalence (0.8%) is comparable to the radiological studies, even if only fused cases could be detected and scored.
Conclusions
In this study of a large sample of the Coimbra Identified Skeletal Collection, diverse anatomical and demographic data, including overall and sex-related prevalence, laterality, size and shape, regarding six accessory foot bones (os trigonum, os intermetatarseum, calcaneus secundarium, accessory navicular bone, os vesalianum and os sustentaculum), were collected. The most frequent accessory bones in the CISC sample are os trigonum and calcaneus secundarium, while os sustentaculum is the least prevalent. Age and sex differences are negligible, and while some accessory bones occurred unilaterally more frequently, the accessory navicular bone was bilateral in the majority of cases. The unilateral expression of os trigonum, calcaneus secundarium and os vesalianum is mostly in the right foot. The co-occurrence of accessory foot bones was also noted, with frequent combinations between os trigonum and calcaneus secundarium.
Accessory foot bones were only of interest to the anatomists for a long time but, following the discovery of X-rays, their significance for the clinical practice of surgeons and orthopedists soared49. They were—and still are—frequently disregarded in patients with feet pain and discomfort41 and a thorough knowledge of these ossicles is paramount to avoid the misdiagnosis of fractures, as early diagnosis and conservative treatment are crucial if unnecessary surgery is to be avoided10. As such, this research underscores the importance of examining reference skeletal collections in order to gain a complete comprehension of foot anatomical variations, which is essential for an accurate diagnosis and effective therapeutics in clinical contexts. Furthermore, it contributes to establishing population standards for comparison in the fields of bioarchaeology and forensic anthropology. Limitations of this study include the cross-sectional nature of the data and the collecting biases of an identified skeletal collection such as the CISC.
Data availability
The datasets generated during the current study are available from the corresponding author on reasonable request.
References
Cazeau, C. Foot Surgery Viewed Through the Prism of Comparative Anatomy. Foot Surgery Viewed Through the Prism of Comparative Anatomy (Wiley-ISTE, 2020).
Vesalius, A. De Humani Corporis Fabrica. (Joannes Oporinus, 1543).
Gruber, W. Vorläufige mittheilung über die secundären fusswurzelknochen des menschen. Arch. für Anat. Physiol. Wissenschaftliche Medizin 31, 286–290 (1864).
Stieda, L. Ueber secundäre fusswurzelknochen. Arch. für Anat. Physiol. und Wissenschaftliche Med. 108–111 (1869).
Bardeleben, K. Tarsus and Carpus. J. Anat. Physiol. 19, 509–510 (1885).
Pfitzner, W. Beiträge zur Kenntniss des menschlichen Extremitätenskelets. Morphol. Arb. 6, (1896).
Dwight, T. A Clinical Atlas, Variations of the Bones of the Hands and Feet (Lippincott Williams & Wilkins, 1907).
Geist, E. S. Supernumerary bones of the foot—a Röntgen study of the feet of one hundred normal individuals. JBJS 2, 413–414 (1915).
Kelikian, A. & Sarrafian, S. K. Sarrafian’s Anatomy of the Foot and Ankle: Descriptive, Topographic, Functiona (Lippincott Williams & Wilkins, 2011).
Mellado, J. M. et al. Accessory ossicles and sesamoid bones of the ankle and foot: Imaging findings, clinical significance and differential diagnosis. Eur. Radiol. 13, L164–L177 (2003).
Keles-Celik, N. et al. Accessory Ossicles of the foot and ankle: Disorders and a review of the literature. Cureus 9, e1881 (2017).
Keles Coskun, N., Arican, R. Y., Utuk, A., Ozcanli, H. & Sindel, T. The incidence of accessory navicular bone types in Turkish subjects. Surg. Radiol. Anat. 31, 675–679 (2009).
Kalbouneh, H. et al. Accessory ossicles in the region of the foot and ankle: An epidemiologic survey in a jordanian population. Med. 57, 1–10 (2021).
Cilli, F. & Akçaoglu, M. The incidence of accessory bones of the foot and their clinical significance. Acta Orthop. Traumatol. Turc. 39, 243–246 (2005).
Zwiers, R., Baltes, T. P. A., Opdam, K. T. M., Wiegerinck, J. I. & van Dijk, C. N. Prevalence of Os Trigonum on CT Imaging. Foot Ankle Int. 39, 338–342 (2018).
Kose, O. The accessory Ossicles of the foot and ankle; a diagnostic pitfall in emergency department in context of foot and ankle trauma. J. Acad. Emerg. Med. 11, 106–114 (2012).
Kepka, S. et al. A case of an injured calcaneus secundarius in a professional soccer player. BMC Musculoskelet. Disord. https://doi.org/10.1186/s12891-021-04246- (2021).
Anderson, T. Calcaneus secundarius: An osteo-archaeological note. Am. J. Phys. Anthropol. 77, 529–531 (1988).
Silva, A. M. Foot anomalies in the late Neolithic/Chalcolithic population exhumed from the rock cut cave of São Paulo 2 (Almada, Portugal). Int. J. Osteoarchaeol. 21, 420–427 (2011).
Mann, R. W. & Owsley, D. W. Os trigonum. Variation of a common accessory ossicle of the talus. J. Am. Podiatr. Med. Assoc. 80, 536–539 (1990).
Troy Case, D., Ossenberg, N. S. & Burnett, S. E. Os intermetatarseum: A heritable accessory bone of the human foot. Am. J. Phys. Anthropol. 107, 199–209 (1998).
Offenbecker, A. M. & Case, D. T. Accessory navicular: A heritable accessory bone of the human foot. Int. J. Osteoarchaeol. 22, 158–167 (2012).
Szaro, P., Polaczek, M., Świątkowski, J. & Kocoń, H. How to increase the accuracy of the diagnosis of the accessory bone of the foot?. Radiol. Medica 125, 188–196 (2020).
Guo, S., Yan, Y. Y., Lee, S. S. Y. & Tan, T. J. Accessory ossicles of the foot—an imaging conundrum. Emerg. Radiol. 26, 465–478 (2019).
Liagre, E. B. K., Hoogland, M. L. P. & Schrader, S. A. It runs in the family: Kinship analysis using foot anomalies in the cemetery of Middenbeemster (Netherlands, 17th to 19th century). Int. J. Osteoarchaeol. 32, 769–782 (2022).
Silva, A. M. Non-osseous calcaneonavicular coalition in the Portuguese prehistoric population: Report of two cases. Int. J. Osteoarchaeol. 15, 449–453 (2005).
Silva, A. M. & Silva, A. L. Unilateral non-osseous calcaneonavicular coalition: Report of a Portuguese archeological case. Anthropol. Sci. 118, 61–64 (2010).
Case, D. T., Jones, L. B. & Offenbecker, A. M. Skeletal Kinship Analysis Using Developmental Anomalies of the Foot. Int. J. Osteoarchaeol. 27, 192–205 (2017).
Verna, E., Piercecchi-Marti, M. D., Chaumoitre, K. & Adalian, P. Relevance of discrete traits in forensic anthropology: From the first cervical vertebra to the pelvic girdle. Forensic Sci. Int. 253(134), e1-134.e7 (2015).
Summers, A. Accessory ossicles and sesamoid bones: Recognition and treatment. Emerg. Nurse 22, 27–32 (2015).
Lee, J. H., Kyung, M. G., Cho, Y. J., Go, T. W. & Lee, D. Y. Prevalence of accessory bones and tarsal coalitions based on radiographic findings in a healthy, asymptomatic population. CiOS Clin. Orthop. Surg. 12, 245–251 (2020).
Cunha, E. & Wasterlain, S. The Coimbra identified osteological collections. In Skeletal Series in their Socioeconomic Context Vol. 5 (eds Grupe, G. & Peters, J.) 23–33 (Leidorf, 2007).
Curate, F. & Tavares, A. Maternal mortality, marital status and bone mineral density in young women from the coimbra identified skeletal collection. Anthropol. Anzeiger 75, 233–242 (2018).
McAlister, J. E. & Urooj, U. Os Trigonum syndrome. Clin. Podiatr. Med. Surg. 38, 279–290 (2021).
Mann, R. W. Calcaneus secundarius: Description and frequency in six skeletal samples. Am. J. Phys. Anthropol. 81, 17–25 (1990).
Scheuer, L. & Black, S. Developmental Juvenile Osteology (Elsevier, 2000).
Zadek, I. & Gold, A. M. The accessory tarsal scaphoid. J. Bone Jt. Surg. 30, 957–968 (1948).
Miller, T. T. et al. The symptomatic accessory tarsal navicular bone: Assessment with MR imaging. Radiology 195, 849–853 (1995).
Nwawka, O. K. et al. Sesamoids and accessory ossicles of the foot: Anatomical variability and related pathology. Insights Imaging 4, 581–593 (2013).
Reichmister, J. P. The painful os intermetatarseum: A brief review and case reports. Clin. Orthop. Relat. Res. 153, 201–203 (1980).
Coskun, N. et al. Incidence of accessory ossicles and sesamoid bones in the feet: A radiographic study of the Turkish subjects. Surg. Radiol. Anat. 31, 19–24 (2009).
Candan, B., Torun, E. & Dikici, R. The prevalence of accessory ossicles, sesamoid bones, and biphalangism of the foot and ankle: A radiographic study. Foot Ankle Orthop. https://doi.org/10.1177/24730114211068792 (2022).
Kir, H., Kandemir, S., Olgaç, M., Yıldırım, O. & Şen, G. The incidence and distribution of accessory ossicles of the foot. Med. Bull. Sisli Etfal Hosp. 45, 44–47 (2011).
Gursoy, M., Dirim Mete, B., Cetinoglu, K., Bulut, T. & Gulmez, H. The coexistence of os trigonum, accessory navicular bone and os peroneum and associated tendon and bone pathologies. Foot 50, 101886 (2022).
Bizarro, A. H. On sesamoid and supernumerary bones of the limbs. J. Anat. 55, 256–268 (1921).
Holland, T. On rarer ossifications seen during X-ray examinations. Arch. Radiol. Electrother. 26, 105–118 (1921).
Meisenbach, R. Fracture of os trigonum: Report of two cases. J. Am. Med. Assoc. 89, 199–200 (1927).
Sewell, R. B. A Study of the Astragalus. J. Anat. Physiol. 39, 74-88 7 (1904).
Heimerzheim, A. Über einige akzessorische Fußwurzelknochen nebst ihrer chirurgischen Bedeutung. Dtsch. Zeitschrift für Chir. 190, 96–112 (1925).
Mosel, L. D., Kat, E. & Voyvodic, F. Imaging of the symptomatic type II accessory navicular bone. Australas. Radiol. 48, 267–271 (2004).
Cheong, I. Y. et al. Genetic influence on accessory Navicular bone in the foot: A Korean twin and family study. Twin Res. Hum. Genet. 20, 236–241 (2017).
Riepert, T., Drechsler, T., Schild, H., Nafe, B. & Mattern, R. Estimation of sex on the basis of radiographs of the calcaneus. Forensic Sci. Int. 77, 133–140 (1996).
Mygind, H. B. The accessory tarsal scaphoid: Clinical features and treatment. Acta Orthop. 23, 142–151 (1953).
Ugolini, P. A. & Raikin, S. M. The accessory navicular. Foot Ankle Clin. 9, 165–180 (2004).
Shands, A. R. & Wentz, I. J. Congenital anomalies, accessory bones, and osteochondritis in the feet of 850 children. Surg. Clin. North Am. 33, 1643–1666 (1953).
Macnicol, M. F. & Voutsinas, S. Surgical treatment of the symptomatic accessory navicular. J. Bone Jt. Surg. Br. 66, 218–226 (1984).
Bencardino, J., Rosenberg, Z. S., Beltran, J. & Sheskier, S. Os sustentaculi: Depiction on MR images. Skeletal Radiol. 26, 505–506 (1997).
Huria, G., Atay, A. O., Leblebicioǧlu, G. A. & Doral, M. N. Fracture of the sustentaculum tali of the calcaneus in pediatric age: A case report. J. Pediatr. Orthop. B 18, 354–356 (2009).
Vasiljevic, V. et al. Accessory bones of the feet: Radiological analysis of frequency. Vojnosanit. Pregl. 67, 469–472 (2010).
Pitchandi, M., Mallikarjun, A. & Bhuvaneswari, V. Radiological study on the Incidence and clinical importance of Os Vesalianum of 5th Metatarsal Bone. Int. J. Anatomy Radiol. Surg. 8, 9–11 (2019).
Acknowledgements
The authors are thankful to the Research Centre for Anthropology and Health (PEst-OE/SADG/UI0283/2021).
Author information
Authors and Affiliations
Contributions
Author contributions Ana Maria Silva: Conceptualization; Data collection; Formal analysis; Methodology; Roles/Writing—original draft. Francisco Curate: Conceptualization; Formal analysis; Methodology; Roles/Writing—original draft.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Silva, A.M., Curate, F. Accessory foot bones in a Portuguese identified skeletal collection. Sci Rep 14, 17169 (2024). https://doi.org/10.1038/s41598-024-68211-2
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-024-68211-2
- Springer Nature Limited