Abstract
Lupus nephritis is a crucial complication of systemic lupus erythematosus. In this study, we investigated the roles of mouse natural killer T (NKT) cells in lupus nephritis. From 24 weeks of age, NZB/NZW F1 mice were injected with alpha-galactosylceramide (α-GalCer) or vehicle once a week for four weeks. In the α-GalCer group, the levels of proteinuria and blood urea nitrogen were significantly lower than those in the vehicle group. The histological evaluation showed a decrease in glomerular immune complex deposits and an alleviation of podocyte injury. The proportion of NKT cells in the mononuclear cell (MNC) fraction in the α-GalCer group was significantly decreased in the liver, kidney, and spleen. The proliferation and cytokine production in α-GalCer-stimulated liver MNCs were markedly diminished in the α-GalCer group (anergy). The IFN-γ production in liver MNCs stimulated by concanavalin A or an anti-CD3 antibody did not differ between the two groups, whereas the IL-4 production was significantly lower in the α-GalCer group. In addition, the IgM production in CpG-oligodeoxynucleotide-stimulated spleen MNCs was significantly lower in the α-GalCer group. These results suggest that α-GalCer suppressed Th2 immune responses in NKT cells and B cell function, thereby slowing the progression of lupus nephritis.
Similar content being viewed by others
Introduction
Systemic lupus erythematosus (SLE) is one of the representative systemic autoimmune diseases, which is characterized by the presence of autoantibodies and involves virtually any organ. Lupus nephritis represents a crucial complication because renal outcomes in patients with lupus nephritis are poor despite the use of immunosuppressive therapy1. A previous study has shown that approximately one-third of patients with lupus nephritis progress to end-stage renal disease within 20 years2. An understanding of its detailed pathogenesis is urgently needed to find better therapeutic approaches.
Mouse natural killer T (NKT) cells are innate immune cells that express both the NK1.1 antigen and the T cell receptor (TCR) and are abundant in the liver. Once activated by IL-12 or an anti-CD3 antibody (Ab), they produce cytokines and exert antitumor cytotoxicity3,4. Their TCRs are mainly encoded by the Vα14Jα18 and Vβ8 genes5,6. The gene arrangement for encoding the TCR is invariant, and therefore, they are also known as invariant NKT (iNKT) cells. The functions of NKT cells have been examined under stimulation with alpha-galactosylceramide (α-GalCer), a specific sphingoglycolipid ligand of these cells7.
Liver NKT cells activated by α-GalCer trigger a potent antitumor response mediated via NK cells and subsequently CD8+ T cells8,9. However, NKT cells themselves can cause multiple organ failure, especially in aged mice8,10. On the other hand, NKT cells may play protective roles in some glomerulonephritis or vasculitis models11,12. In a SLE model, the expansion of NKT cells is thought to be involved in the onset of lupus nephritis13, whereas their immunoregulatory roles were also reported both in human SLE and SLE models14,15,16.
The effects of α-GalCer in the progression of autoimmune disease models have also been controversial. For example, it was shown that α-GalCer prevented the onset of diabetes in non-obese diabetic (NOD) mice, a representative type 1 diabetes model17,18. Conversely, there have been contradictory reports regarding the effects of α-GalCer in NZB/NZW F1 (BWF1) mice, an experimental model of SLE in which lupus nephritis-like lesions develop. Thus, one report showed that α-GalCer-activated NKT cells exacerbated the experimental lupus nephritis19, whereas a long-term reduction in severe proteinuria following α-GalCer treatment was reported in another study20.
Therefore, in the present study, we have investigated the roles of NKT cells in lupus nephritis using BWF1 mice. We show that the repeated administration of α-GalCer into BWF1 mice induced beneficial effects, as follows: (i) it improved proteinuria which represents a hallmark of renal injury, by protecting nephrin, a key functional molecule in the slit diaphragm of the podocytes21; (ii) it suppressed B cell function and decreased glomerular immune complex deposits; (iii) it induced not only an anergic state to α-GalCer in NKT cells, but also decreased the number of NKT cells in multiple organs and the production of IL-4 by these cells.
Results
The effects of α-GalCer treatment on the progression of kidney dysfunction
The levels of proteinuria in the α-GalCer group were significantly lower than those in the vehicle group (Fig. 1a). Moreover, the incidence of proteinuria in the α-GalCer group was also significantly lower when analyzed using the log-rank test (Fig. 1b, p < 0.05), but was not statistically significant when using the Cox proportional hazard model (Supplementary Table S1, p = 0.10). Neither group displayed hematuria. The survival rate in the α-GalCer group tended to be higher than that in the vehicle group, although it was not statistically different (Fig. 1c, p = 0.20 and Supplementary Table S1, p = 0.33).
The effects of repeated alpha-galactosylceramide (α-GalCer) administration on proteinuria and survival rates. (a) The levels of proteinuria in each group, measured 8 weeks after the last α-GalCer or vehicle injection (n = 5–7 in each group). *p < 0.05 compared with the vehicle group. (b) The percentages of mice with free of proteinuria and (c) the survival rate in the α-GalCer and the vehicle groups (n = 8 and 10, respectively). Arrows show the timing of when the mice were injected with α-GalCer or vehicle.
The blood urea nitrogen (BUN) levels in the α-GalCer group were significantly lower than those in the vehicle group (Table 1). Moreover, the serum albumin levels in the α-GalCer group were significantly higher than those in the vehicle group, reflecting the difference in the levels of proteinuria between the two groups (Fig. 1a). Although no significant differences in the total serum protein levels or IgM levels were observed, the serum albumin/globulin ratio was significantly higher in the α-GalCer group. However, the serum IgG anti-dsDNA Ab levels did not differ between the two groups. The alanine aminotransferase levels were within the normal range and no significant difference was found between the two groups. Splenomegaly was observed in both groups; however, there was no difference in spleen weight or body weight. Furthermore, obvious lymphadenopathy was not observed in any of the mice.
Glomerular immune complex deposits and the infiltration of inflammatory cells decrease following α-GalCer treatment
A representative image of periodic acid-Schiff (PAS) staining in the vehicle group is shown in Fig. 2a, while that in the α-GalCer group is shown in Fig. 2b. The percentage of glomeruli containing immune complex deposits and that of sclerotic glomeruli in the α-GalCer group were significantly lower (Fig. 2c,d). Furthermore, although the difference was not statistically significant, the percentage of glomeruli with crescents in the α-GalCer group tended to be lower than that in the vehicle group (Fig. 2e).
Kidney pathology of experimental lupus nephritis is ameliorated by treatment with alpha-galactosylceramide (α-GalCer). Representative images of periodic acid-Schiff staining of kidney slices in the (a) vehicle and (b) α-GalCer groups. Arrows, immune complex deposits; arrowhead, segmentally sclerotic area. The percentages of (c) glomeruli with immune complex deposits, (d) sclerotic glomeruli, and (e) glomeruli with crescents in each group (vehicle group; n = 5, α-GalCer group; n = 7). *p < 0.05 compared with the vehicle group.
We also evaluated the infiltration of inflammatory cells in the kidney. Representative images for F4/80 and CD3 staining in both groups are shown in Fig. 3a,b. Both the F4/80 and CD3 positive areas were significantly smaller in the α-GalCer group than those in the vehicle group (Fig. 3c,d). The renal messenger RNA (mRNA) expression levels for a dendritic cell marker (CD11c) and a plasma cell marker (CD138) did not significantly differ between the two groups (Supplementary Fig. S1).
Alpha-galactosylceramide (α-GalCer) treatment decreases the infiltration of inflammatory cells into the kidney. Representative images of (a) F4/80-stained and (b) CD3-stained kidney slices in the vehicle (left) and α-GalCer (right) groups. In each panel, arrows indicate F4/80 or CD3-positive areas. The percentages of the (c) F4/80-positive area and (d) CD3-positive area in each group (vehicle group; n = 5, α-GalCer group; n = 7). *p < 0.05 compared with the vehicle group.
α-GalCer treatment decreases IgG deposition and ameliorates podocyte injury
Next, we assessed the deposition of glomerular immune complexes and the podocyte damage of the two groups. Figure 4a shows representative images of immunofluorescence (IF) IgG staining. In accordance with the light microscopy findings, the mean fluorescence intensity (MFI) of IgG staining in the α-GalCer group was significantly weaker (Fig. 4b).
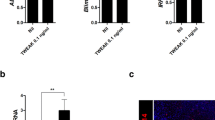
Alpha-galactosylceramide (α-GalCer) treatment decreases the deposition of glomerular immune complexes and ameliorates podocyte injury. Representative images of (a) immunofluorescence (IF) IgG staining, (c) immunoperoxidase WT-1 staining, and (e) IF nephrin staining of kidney slices in the vehicle (left) and α-GalCer (right) groups. In (c) and (e), arrows indicate positively stained cells or areas. (b) MFI (mean fluorescence intensity) of IgG staining, (d) WT-1 positive cells/glomeruli, and (f) semiquantitative nephrin IF score in each group (vehicle group; n = 5, α-GalCer group; n = 7). *p < 0.05, **p < 0.01 compared with the vehicle group. (g) Representative electron microscopy photomicrographs of kidney slices in the vehicle (left) and α-GalCer (right) groups. Widespread effacement of podocyte foot processes (red arrows) and electron dense immune deposits (red arrowheads) are shown in the vehicle group. Endocapillary infiltration of inflammatory cells was also observed (yellow asterisks).
Figure 4c shows representative images of WT-1 immunostaining, which represents a marker of podocyte damage22. Compared with that in the vehicle group, the number of WT-1 positive cells was significantly larger in the α-GalCer group (Fig. 4d). The IF nephrin staining score was also significantly higher in the α-GalCer group (Fig. 4e,f). These results suggested that podocyte injury was alleviated in the α-GalCer group.
Moreover, electron microscopy showed that although widespread effacement of podocyte foot processes was observed in the vehicle group, foot processes were relatively preserved in the α-GalCer group (Fig. 4g). Electron dense deposits, especially subepithelial deposits, were also smaller in the α-GalCer group.
Repeated α-GalCer injection decreases the proportion of NKT cells and the cytokine responses to α-GalCer stimulation
We performed flow cytometry analysis to assess the number of NKT cells in multiple organs. Figure 5a shows representative images in which liver mononuclear cells (MNCs) were stained with anti-TCR αβ and anti-NK1.1 Abs. The proportion of NKT cells in the liver in the α-GalCer group was significantly reduced compared to that in the vehicle group (Fig. 5b). Figure 5c,e and g show representative images in which liver, kidney, and spleen MNCs were stained with anti-TCR αβ Ab and the α-GalCer-loaded CD1d tetramer. The proportions of iNKT cells in the liver, kidney, and spleen in the α-GalCer group were significantly lower than those in the vehicle group (Fig. 5d,f and h).
Repeated alpha-galactosylceramide (α-GalCer) administration decreases the proportion of NKT cells in multiple organs. (a) Flow cytometry analysis of liver mononuclear cells (MNCs) in the vehicle (left) and α-GalCer (right) groups, stained with anti-TCR αβ and anti-NK1.1 antibodies. In both panels, black squares show NKT cells. Flow cytometry analysis of (c) liver, (e) kidney, and (g) spleen MNCs in the (left) vehicle and (right) α-GalCer groups. Isolated MNCs were double stained with anti-TCR αβ antibody and α-GalCer-loaded CD1d tetramer; invariant NKT (iNKT) cells are shown in black squares. The percentages of (b) whole NKT cells in the liver and iNKT cells in the (d) liver, (f) kidney, and (h) spleen are shown (n = 4 in each group). *p < 0.05 compared with the vehicle group.
Next, we assessed the cytokine responses under α-GalCer stimulation. The repeated administration of α-GalCer reduced the elevation of serum IFN-γ and IL-4 levels following α-GalCer injection in mice, and the levels of both cytokines decreased to undetectable levels (Fig. 6a,b). These results were also confirmed in vitro. Thus, α-GalCer-stimulated liver MNCs strongly proliferated in the vehicle group (Fig. 6c), whereas the proliferation was poor in the α-GalCer group (Fig. 6d). In addition, the IFN-γ and IL-4 levels produced by liver MNCs following α-GalCer stimulation were significantly lower in the α-GalCer group, even at 8 weeks after the last α-GalCer injection (Fig. 6e,f). Furthermore, not only BWF1, but also C57BL/6 J (B6) mice undergoing repeated α-GalCer administration showed similar cytokine responses both in in vivo and in vitro (Fig. 6a,b,e and f). These results suggested that the repeated administration of α-GalCer induced a state of anergy to α-GalCer, which was not specific to BWF1 mice.
Repeated alpha-galactosylceramide (α-GalCer) injection induces anergy in NKT cells to α-GalCer. (a) Serum IFN-γ levels 12 hours after α-GalCer injection and (b) IL-4 levels 3 hours after α-GalCer injection in (NZB/NZW) F1 (BWF1) and C57BL/6 J (B6) mice. The mice were injected with 2 μg/body of α-GalCer once a week for 4 weeks, and cytokine levels were evaluated after every injection (n = 4 in each group). *p < 0.05, **p < 0.01 compared with B6 mice. ††p < 0.01 compared with the levels after the first α-GalCer injection. †p < 0.05 compared with the levels after the second α-GalCer injection. Microphotographs of liver mononuclear cells (MNCs), stimulated by α-GalCer in the (c) vehicle and (d) α-GalCer groups (original magnification, 100×). In vitro production of (e) IFN-γ and (f) IL-4 from liver MNCs in BWF1 mice treated with α-GalCer or vehicle, and B6 mice treated with α-GalCer. Liver MNCs were obtained 8 weeks after the last α-GalCer or vehicle injection and were stimulated with α-GalCer for 48 hours (n = 4 in each group). **p < 0.01 compared with the vehicle group of BWF1 mice.
Repeated α-GalCer administration decreases B cell function through the suppression of Th2 immune responses
The cytokine production levels of MNCs were also evaluated under stimulation with other agents. Liver MNCs stimulated with concanavalin A (ConA), a T-cell stimulant23, proliferated well both in the vehicle and α-GalCer groups (Fig. 7a,b), and the levels of IFN-γ produced by these cells were comparable between the two groups (Fig. 7c). However, the IL-4 levels in the α-GalCer group were significantly lower than those in the vehicle group (Fig. 7d). Similar cytokine responses were observed when liver MNCs were stimulated with an anti-CD3 Ab. Although the levels of IFN-γ produced by liver MNCs did not differ between the two groups, the IL-4 levels in the α-GalCer group were significantly lower than those in the vehicle group (Fig. 7e,f). This suppression of IL-4 production was also observed in B6 mice, following the repeated administration of α-GalCer (Fig. 7c–f).
Th2 but not Th1 immune responses are suppressed by repeated alpha-galactosylceramide (α-GalCer) injections. Microphotographs of liver mononuclear cells (MNCs), stimulated by concanavalin A (ConA) in the (a) vehicle and (b) α-GalCer groups (original magnification, 100×). IFN-γ production and IL-4 production from liver MNCs, stimulated with (c,d) ConA or (e,f) anti-CD3 antibody for 48 hours in (NZB/NZW) F1 (BWF1) mice treated with α-GalCer or vehicle, and C57BL/6 J (B6) mice treated with α-GalCer (n = 4–5 in each group). **p < 0.01, ***p < 0.001 compared with the vehicle group of BWF1 mice. ††p < 0.01 compared with the α-GalCer group of BWF1 mice.
To assess the B cell function, we measured the IgM production levels of splenic MNCs. The number of B cells was also evaluated by flow cytometry. In the α-GalCer group, the expression of Toll-like receptor-9 (TLR-9) which recognizes the CpG-oligodeoxynucleotide (CpG-ODN), common bacterial DNA, in splenic F4/80+ CD11b+ macrophages was significantly lower (Fig. 8a). Moreover, the IgM levels produced by spleen MNCs following CpG-ODN stimulation were significantly lower (Fig. 8b), and those produced by lipopolysaccharide (LPS)-stimulated spleen MNCs also tended to be lower (Fig. 8c). The proportions of B cells in the liver, kidney, and spleen did not differ between the two groups (Supplementary Fig. S2).
A decrease in B cell function and augmentation of NK cell function is observed in (NZB/NZW) F1 (BWF1) mice treated with alpha-galactosylceramide (α-GalCer). (a) Representative histograms obtained by flow cytometry showing the expression of intracellular Toll-like receptor-9 (TLR-9) in splenic F4/80+ CD11b+ macrophages in the vehicle (left) and α-GalCer (right) groups of BWF1 mice. The data represent the mean ± SEM in each group (n = 4 in each group). IgM production by spleen mononuclear cells (MNCs) stimulated with (b) CpG-oligodeoxynucleotide (CpG-ODN) or (c) lipopolysaccharide for 48 hours in each group (n = 4–6 in each group). (d) IFN-γ production by liver MNCs stimulated by CpG-ODN for 48 hours in each group (n = 4 in each group). *p < 0.05 compared with the vehicle group.
On the other hand, the IFN-γ levels produced by liver MNCs following stimulation with CpG-ODN were significantly higher in the α-GalCer group (Fig. 8d), suggesting that the function of NK cells was enhanced24. TLR-9 expression in hepatic F4/80+ CD11b+ macrophages did not differ between the two groups (data not shown).
Discussion
To our knowledge, this is the first report to demonstrate that a repeated α-GalCer injection ameliorates podocyte injury, thereby inducing an anti-proteinuric effect. The number of WT-1 positive cells was significantly larger and the nephrin staining score was significantly higher in the α-GalCer group. Moreover, the preservation of podocyte foot processes was observed in the α-GalCer group. We assessed the proteinuria-free survival time in mice using two analysis methods; one showed a statistically significant difference, while another only suggested a tendency toward significance. Regarding this point, it has been reported that the log-rank test may show a tendency toward significant results25. Regardless, the daily levels of proteinuria in the α-GalCer group were significantly lower than those in the vehicle group.
In our study, the infiltration of F4/80-positive macrophages and CD3-positive T lymphocytes in the kidney was reduced, and the serum albumin/globulin ratio was higher in the α-GalCer group. A low albumin/globulin ratio reflects chronic inflammation26. Therefore, our data also suggested the resolution of inflammation following the repeated administration of α-GalCer.
It has been reported that NKT cells and B cells interact to generate Igs, including autoantibodies27,28, whereas inhibitory roles of NKT cells against autoreactive B cells have also been described29. In the present study, we showed another novel finding that the repeated administration of α-GalCer decreased glomerular immune complex deposits. Thus, the percentage of glomeruli containing immune complex deposits, as assessed by PAS staining, was significantly lower and the IgG deposition was significantly decreased in the α-GalCer group. These findings were also observed by electron microscopy. Moreover, the IgM levels produced by CpG-ODN-stimulated spleen MNCs were significantly lower. These data suggested the suppression of autoimmune responses mediated by a decrease in B cell function. The decreased TLR-9 expression of splenic macrophages in the α-GalCer group may also have been related to the improvement of kidney pathology, since TLR-9 has been implicated in the development of lupus nephritis30. Despite the alleviation of renal injuries, the administration of α-GalCer did not affect the levels of anti-dsDNA IgG Abs. However, in the present study, the levels of anti-dsDNA Abs did not correlate with the levels of proteinuria in BWF1 mice, suggesting that these autoantibodies are not pathogenetic markers. Similarly, a study using another SLE model demonstrated an improvement in skin lesions, without any changes in the levels of anti-dsDNA Abs31.
As previously reported32, a repeated α-GalCer injection induced anergy in NKT cells. In addition, the proportions of NKT cells in the liver, kidney, and spleen were significantly reduced in the α-GalCer group. In contrast, the IFN-γ levels remained constant following stimulation with ConA and anti-CD3 Abs, showing that the anergy observed in NKT cells was specific to α-GalCer.
On the other hand, the IL-4 levels produced by ConA and anti-CD3-stimulated liver MNCs were significantly reduced in the α-GalCer group, suggesting the suppression of Th2 immune responses. A predominant Th2 cytokine response in human membranous lupus nephritis has been reported33, and important roles for the Th2 immune responses in the pathogenesis of membranous lupus nephritis have been suggested34,35. Therefore, the present study strongly supported that the repeated administration of α-GalCer ameliorated the progression of lupus nephritis through the suppression of Th2 immune responses. However, it has also been reported that an α-GalCer injection modulates immune responses towards a Th2 phenotype in B6 mice36 and that Th2-biased immune responses induced by the administration of α-GalCer17,18 or its derivative37 prevented diabetes in NOD mice. Thus, the effects of α-GalCer could vary depending on the disease model.
Yang et al. demonstrated that a brief treatment with α-GalCer in 7-week-old BWF1 mice suppressed lupus nephritis20. On the other hand, Zeng et al. reported contradictory results, namely that multiple injections of α-GalCer in 20-week-old BWF1 mice exacerbated lupus nephritis19. Regarding this point, a complex role for NKT cells in SLE, that is, a potential protective role before the onset of the disease and a potential pathogenic role after the establishment of the disease has been proposed16. Moreover, the age of the mice and the α-GalCer dose or administration interval may have influenced these conflicting results. However, we considered that the administration of α-GalCer to young mice was clinically unsuitable, because current international guidelines do not recommend the treatment of patients with mild lupus nephritis using immunosuppressive therapies38. We, therefore, began the α-GalCer treatment at 24 weeks of age, when mice may already develop mild renal disease.
Although some experimental agents have been used in SLE models with favorable outcomes22,39, in the present study we did not use such agents. Instead, we administered α-GalCer, a synthetic but specific ligand of NKT cells, to investigate the role of these cells in lupus nephritis. Definitive natural ligands of NKT cells have not been so far identified. However, considering that α-GalCer is a glycolipid antigen and that some microbes may be antigenic candidates for NKT cells40,41, we think that NKT cells are involved in lupus nephritis via the glycolipid metabolism or in response to microbes.
We have recently demonstrated that the function of NKT cells was enhanced in the absence of NK cells (Uchida et al. in submission). In the present study, we have demonstrated that IFN-γ levels produced by CpG-ODN-stimulated liver MNCs were significantly higher in the α-GalCer group. Moreover, because we have previously reported that NK cells produced IFN-γ after CpG-ODN stimulation24, we proposed a compensatory augmentation in the function of NK cells. Although the precise mechanisms remain to be elucidated, complementary roles may be shared between NKT and NK cells to avoid immunosuppressive states.
Our study has several limitations. It has been reported that BWF1 mice are superior to other SLE models in that they resemble the human disease, and therefore, are most commonly used42. Indeed, these mice spontaneously develop lupus nephritis-like renal lesions. However, the renal disease observed in these mice does not fully recapitulate that in humans; for example, hematuria was not observed in BWF1 mice despite proliferative glomerulonephritis. The role of NKT cells in the progression of human lupus nephritis also remains to be resolved using α-GalCer. This is partly because human NKT cells, which express T cell receptors encoded by the Vα24Jα18 and Vβ11 genes and respond to α-GalCer, are rare in the liver as well as other organs. In addition, decreased levels of human CD56+ T cells, which are not activated by α-GalCer but have been proposed as a functional counterpart for mouse NKT cells8,43,44, might be associated with high levels of serum IgG and anti-dsDNA Abs in patients with SLE14, suggesting that CD56+ T cells may ameliorate SLE. Therefore, it should be carefully evaluated in the future whether human NKT cells or CD56+ T cells are really involved in lupus nephritis.
In conclusion, the repeated administration of α-GalCer decreased the number of NKT cells and suppressed Th2 immune responses in these cells. This led to the suppression of B cell function and the autoimmune response, and ameliorated proteinuria and kidney pathology in experimental lupus nephritis. Therefore, we propose that NKT cells collaborate with B cells and play significant roles in the induction of lupus nephritis through their Th2 immune responses. Thus, it is important to focus on NKT cells to further investigate the precise pathogenesis of lupus nephritis.
Methods
Mice and study protocols
Female BWF1 and B6 mice were obtained from Japan SLC, Inc. (Shizuoka, Japan), and were provided with water and standard chow ad libitum.
The baseline urinary protein excretion of BWF1 mice was measured at 20 weeks of age, and the mice were assigned to either the α-GalCer group (n = 8), which was intraperitoneally injected with 2 μg/body of α-GalCer (Funakoshi, Tokyo, Japan) once a week for 4 weeks from 24 weeks of age, or the vehicle group (n = 10). The baseline urinary protein excretion was balanced between the two groups and amounted to less than 1 mg/day. The urinary protein excretion was thereafter measured periodically, and was considered to be positive when greater than 1 mg/day.
B6 mice were intraperitoneally injected with 2 μg/body of α-GalCer once a week for 4 weeks from 24 weeks of age.
Mice were sacrificed under deep anesthesia at the end of the experiment (8 weeks after the last α-GalCer injection). All animal experiments were conducted in accordance with the National Defense Medical College guidelines for the care and use of laboratory animals in research. The study protocol (no. 15087) was approved by the Animal Ethics Committee of the National Defense Medical College.
Assessment of renal histopathology
Sections of formalin-fixed paraffin-embedded renal tissues were subjected to PAS staining, and 50 glomeruli were evaluated to assess glomeruli with immune complex deposits consisting of wire loop lesions and hyaline thrombi, sclerotic glomeruli including both globally and segmentally sclerotic glomeruli, and glomeruli with crescents.
Immunoperoxidase staining
Indirect immunoperoxidase staining for F4/80, CD3, or WT-1 was performed using rat anti-mouse F4/80 (Serotec, Oxford, UK), rabbit anti-human CD3 (Agilent, Santa Clara, CA), or rabbit anti-mouse WT-1 Abs (Santa Cruz Biotechnology Inc., Santa Cruz, CA), respectively.
Images of five non-overlapping areas from each section stained for F4/80 or CD3 were obtained with a digital camera at a magnification of 200×, and the percentages of the areas positive for each staining were measured using image analysis software (LuminaVision ver. 2.04, Mitani Corporation, Tokyo, Japan) and averaged. For WT-1 staining, 20 glomeruli were assessed, and the numbers of WT-1-positive cells per glomerulus were counted and averaged.
Real-time reverse transcription-polymerase chain reaction (RT-PCR)
Extraction of total RNA, reverse transcription into complementary DNA, and the subsequent real-time PCR were all performed as previously described45. We used primer/probe sets of the TaqMan Gene Expression Assays for mouse CD11c, CD138, and glyceraldehyde 3-phosphate dehydrogenase (GAPDH), all obtained from Thermo Fisher Scientific (Waltham, MA). The relative amount of mRNA was calculated using the comparative Ct (∆∆Ct) method. All amplification products were normalized against GAPDH mRNA, which was amplified in the same reaction as an internal control.
IF staining
Direct IF staining for IgG was performed using FITC-labeled anti-IgG Abs (MP Biomedicals, Santa Ana, CA), and indirect IF staining for nephrin was performed using anti-guinea pig nephrin Abs (Progen, Heidelberg, Germany).
The MFI for IgG staining was calculated by measuring and averaging the IF intensities of 20 randomly selected glomeruli under the same conditions using the image analysis software. For nephrin staining, 20 randomly selected glomeruli were graded semi-quantitatively as follows: 0, severely decreased staining; 1, mildly decreased staining; 2, intense staining. The nephrin IF score was then calculated using the formula: (0 × N0 + 1 × N1 + 2 × N2)/(N0 + N1 + N2), where N is the number of the glomeruli for each staining grade.
Electron microscopy
Renal cortical tissue fragments were examined under a transmission electron microscope, essentially as previously described46.
Cytokine measurements and biochemical parameters
The cytokine and IgM levels in the sera or culture supernatants, and the levels of serum IgG anti-dsDNA Abs were measured using ELISA kits (IL-4 and IFN-γ: BD Biosciences, San Diego, CA; IgM: Bethyl Laboratories, Inc., Montgomery, TX; IgG anti-dsDNA Abs: Shibayagi Co. Ltd., Gunma, Japan). BUN levels and serum albumin, total protein, and alanine aminotransferase levels were measured using a DRICHEM 3000 V system (Fuji Medical System, Tokyo, Japan). Urinary protein excretion was measured by a clinical laboratory testing company (SRL, Tokyo, Japan).
Flow cytometry
Kidney, liver, and spleen specimens were filtered through a stainless-steel mesh and dissolved. Kidney MNCs were thereafter isolated using a Percoll density gradient (67% and 33%) centrifugation. Liver MNCs were isolated without collagenase, essentially as previously described10.
For the identification of whole NKT or iNKT cells, the MNCs were stained with anti-TCR αβ Ab (H57-597, eBioscience, San Diego, CA) and either anti-NK1.1 Ab (PK136, eBioscience) or the α-GalCer-loaded CD1d tetramer (MBL, Nagoya, Japan), respectively. Macrophages were identified by staining MNCs with anti-F4/80 (BM8, eBioscience) and anti-CD11b Abs (M1/70, eBioscience), and their expression of TLR-9 was examined using anti-TLR-9 Ab (J15A7, BD Biosciences). B cells were identified by staining MNCs with anti-B220 Ab (RA3-6B2, eBioscience). Flow cytometry was performed on a Cytomics FC500 instrument (Beckman Coulter, Indianapolis, IN).
Cell culture for MNCs
MNCs (5 × 105 cells) of liver or splenic origin in 200 μL of medium were cultured with either α-GalCer (100 ng/mL), ConA (1 ng/mL, Vector Laboratories, Inc., Burlingame, CA), anti-CD3 Ab (10 μg/mL, eBioscience), CpG-ODN (20 μg/mL, Hycult Biotech, Uden, The Netherlands), or LPS from E. coli 0111:B4 (10 μg/mL, Sigma-Aldrich, St. Louis, MO) in 96-well flat-bottom plates. The culture supernatants were harvested 48 hours after seeding.
Statistics
Data are expressed as the mean ± SEM. Differences between two experimental groups were assessed using the Student’s t-test, and those among more than three experimental groups were assessed by one-way ANOVA with Tukey’s HSD post hoc test. Differences in the proteinuria-free survival time and the survival time of the groups were analyzed using the log-rank test and the Cox proportional hazard model. P-values of < 0.05 were considered statistically significant. All statistical analyses were performed using the JMP software (version 11; SAS Institute Inc., Cary, NC).
Data availability
All data generated or analyzed during this study are included in this published article (and its Supplementary Information files).
References
Fu, J. et al. Transcriptomic analysis uncovers novel synergistic mechanisms in combination therapy for lupus nephritis. Kidney Int. 93, 416–429 (2018).
Yang, J. et al. Long-term renal outcomes in a cohort of 1814 Chinese patients with biopsy-proven lupus nephritis. Lupus. 24, 1468–1478 (2015).
Hashimoto, W. et al. Cytotoxic NK1.1 Ag + alpha beta T cells with intermediate TCR induced in the liver of mice by IL-12. J Immunol. 154, 4333–4340 (1995).
Kawamura, T. et al. Cytotoxic activity against tumour cells mediated by intermediate TCR cells in the liver and spleen. Immunology. 89, 68–75 (1996).
Makino, Y. et al. Extrathymic differentiation of a T cell bearing invariant V alpha 14J alpha 281 TCR. Int Rev Immunol. 11, 31–46 (1994).
Lantz, O. & Bendelac, A. An invariant T cell receptor alpha chain is used by a unique subset of major histocompatibility complex class I-specific CD4 + and CD4-8- T cells in mice and humans. J Exp Med. 180, 1097–1106 (1994).
Kawano, T. et al. CD1d-restricted and TCR-mediated activation of valpha14 NKT cells by glycosylceramides. Science. 278, 1626–1629 (1997).
Seki, S., Nakashima, H., Nakashima, M. & Kinoshita, M. Antitumor immunity produced by the liver Kupffer cells, NK cells, NKT cells, and CD8 CD122 T cells. Clin Dev Immunol. 2011, 868345 (2011).
Nakagawa, R. et al. Mechanisms of the antimetastatic effect in the liver and of the hepatocyte injury induced by alpha-galactosylceramide in mice. J Immunol. 166, 6578–6584 (2001).
Inui, T. et al. Neutralization of tumor necrosis factor abrogates hepatic failure induced by alpha-galactosylceramide without attenuating its antitumor effect in aged mice. J Hepatol. 43, 670–678 (2005).
Riedel, J. H. et al. Immature renal dendritic cells recruit regulatory CXCR6( + ) invariant natural killer T cells to attenuate crescentic GN. J Am Soc Nephrol. 23, 1987–2000 (2012).
Mesnard, L. et al. Invariant natural killer T cells and TGF-beta attenuate anti-GBM glomerulonephritis. J Am Soc Nephrol. 20, 1282–1292 (2009).
Morshed, S. R. et al. Tissue-specific expansion of NKT and CD5 + B cells at the onset of autoimmune disease in (NZBxNZW)F1 mice. Eur J Immunol. 32, 2551–2561 (2002).
Green, M. R. et al. Natural killer T cells in families of patients with systemic lupus erythematosus: their possible role in regulation of IGG production. Arthritis Rheum. 56, 303–310 (2007).
Chen, J., Wu, M., Wang, J. & Li, X. Immunoregulation of NKT Cells in Systemic Lupus Erythematosus. J Immunol Res. 2015, 206731 (2015).
Godo, M., Sessler, T. & Hamar, P. Role of invariant natural killer T (iNKT) cells in systemic lupus erythematosus. Curr Med Chem. 15, 1778–1787 (2008).
Hong, S. et al. The natural killer T-cell ligand alpha-galactosylceramide prevents autoimmune diabetes in non-obese diabetic mice. Nat Med. 7, 1052–1056 (2001).
Sharif, S. et al. Activation of natural killer T cells by alpha-galactosylceramide treatment prevents the onset and recurrence of autoimmune Type 1 diabetes. Nat Med. 7, 1057–1062 (2001).
Zeng, D., Liu, Y., Sidobre, S., Kronenberg, M. & Strober, S. Activation of natural killer T cells in NZB/W mice induces Th1-type immune responses exacerbating lupus. J Clin Invest. 112, 1211–1222 (2003).
Yang, J. Q., Kim, P. J. & Singh, R. R. Brief treatment with iNKT cell ligand alpha-galactosylceramide confers a long-term protection against lupus. J Clin Immunol. 32, 106–113 (2012).
Kawachi, H. et al. Slit diaphragm dysfunction in proteinuric states: identification of novel therapeutic targets for nephrotic syndrome. Clin Exp Nephrol. 13, 275–280 (2009).
Xia, Y. et al. Deficiency of fibroblast growth factor-inducible 14 (Fn14) preserves the filtration barrier and ameliorates lupus nephritis. J Am Soc Nephrol. 26, 1053–1070 (2015).
Tiegs, G., Hentschel, J. & Wendel, A. A T cell-dependent experimental liver injury in mice inducible by concanavalin A. J Clin Invest. 90, 196–203 (1992).
Kawabata, T. et al. Functional alterations of liver innate immunity of mice with aging in response to CpG-oligodeoxynucleotide. Hepatology. 48, 1586–1597 (2008).
Berty, H. P., Shi, H. & Lyons-Weiler, J. Determining the statistical significance of survivorship prediction models. J Eval Clin Pract. 16, 155–165 (2010).
Suh, B. et al. Low albumin-to-globulin ratio associated with cancer incidence and mortality in generally healthy adults. Ann Oncol. 25, 2260–2266 (2014).
Takahashi, T. & Strober, S. Natural killer T cells and innate immune B cells from lupus-prone NZB/W mice interact to generate IgM and IgG autoantibodies. Eur J Immunol. 38, 156–165 (2008).
Tang, X. et al. Ly108 expression distinguishes subsets of invariant NKT cells that help autoantibody production and secrete IL-21 from those that secrete IL-17 in lupus prone NZB/W mice. J Autoimmun. 50, 87–98 (2014).
Yang, J. Q., Wen, X., Kim, P. J. & Singh, R. R. Invariant NKT cells inhibit autoreactive B cells in a contact- and CD1d-dependent manner. J Immunol. 186, 1512–1520 (2011).
Chauhan, S. K., Singh, V. V., Rai, R., Rai, M. & Rai, G. Distinct autoantibody profiles in systemic lupus erythematosus patients are selectively associated with TLR7 and TLR9 upregulation. J Clin Immunol. 33, 954–964 (2013).
Yang, J. Q. et al. Repeated alpha-galactosylceramide administration results in expansion of NK T cells and alleviates inflammatory dermatitis in MRL-lpr/lpr mice. J Immunol. 171, 4439–4446 (2003).
Uldrich, A. P. et al. NKT cell stimulation with glycolipid antigen in vivo: costimulation-dependent expansion, Bim-dependent contraction, and hyporesponsiveness to further antigenic challenge. J Immunol. 175, 3092–3101 (2005).
Akahoshi, M. et al. Th1/Th2 balance of peripheral T helper cells in systemic lupus erythematosus. Arthritis Rheum. 42, 1644–1648 (1999).
Miyake, K., Akahoshi, M. & Nakashima, H. Th subset balance in lupus nephritis. J Biomed Biotechnol. 2011, 980286 (2011).
Miyake, K. et al. Parasites alter the pathological phenotype of lupus nephritis. Autoimmunity. 47, 538–547 (2014).
Singh, N. et al. Cutting edge: activation of NK T cells by CD1d and alpha-galactosylceramide directs conventional T cells to the acquisition of a Th2 phenotype. J Immunol. 163, 2373–2377 (1999).
Mizuno, M. et al. Synthetic glycolipid OCH prevents insulitis and diabetes in NOD mice. J Autoimmun. 23, 293–300 (2004).
Hahn, B. H. et al. American College of Rheumatology guidelines for screening, treatment, and management of lupus nephritis. Arthritis Care Res (Hoboken). 64, 797–808 (2012).
Devarapu, S. K. et al. Dual blockade of the pro-inflammatory chemokine CCL2 and the homeostatic chemokine CXCL12 is as effective as high dose cyclophosphamide in murine proliferative lupus nephritis. Clin Immunol. 169, 139–147 (2016).
Kinjo, Y. et al. Recognition of bacterial glycosphingolipids by natural killer T cells. Nature. 434, 520–525 (2005).
Mattner, J. et al. Exogenous and endogenous glycolipid antigens activate NKT cells during microbial infections. Nature. 434, 525–529 (2005).
Peng, S. L. Experimental use of mouse models of systemic lupus erythematosus. Methods Mol Biol. 900, 135–168 (2012).
Kawarabayashi, N. et al. Decrease of CD56( + )T cells and natural killer cells in cirrhotic livers with hepatitis C may be involved in their susceptibility to hepatocellular carcinoma. Hepatology. 32, 962–969 (2000).
Seki, S. et al. The liver as a crucial organ in the first line of host defense: the roles of Kupffer cells, natural killer (NK) cells and NK1.1 Ag + T cells in T helper 1 immune responses. Immunol Rev. 174, 35–46 (2000).
Uchida, T. et al. Renoprotective effects of a dipeptidyl peptidase 4 inhibitor in a mouse model of progressive renal fibrosis. Ren Fail. 39, 340–349 (2017).
Nakashima, M. et al. Pivotal advance: characterization of mouse liver phagocytic B cells in innate immunity. J Leukoc Biol. 91, 537–546 (2012).
Acknowledgements
We are grateful to Dr. Takahiro Nakamura, at Laboratory for Mathematics of National Defense Medical College, for his valuable advice and discussions. We also thank Ms. Yayoi Ichiki and Ms. Aya Kotani for their technical assistance, and our colleague Ms. Keiko Komoda for expert secretarial assistance.
Author information
Authors and Affiliations
Contributions
T.U., H.N. and S.S. designed experiments. T.U., H.N., A.Y., S.I. and T.I. conducted experiments. T.U. acquired data, and T.U., H.N., M.N., S.S., H.K. and N.O. analyzed data. T.U. and H.N. wrote the draft of the manuscript, that was edited by S.S., H.K. and N.O.
Corresponding author
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Uchida, T., Nakashima, H., Yamagata, A. et al. Repeated administration of alpha-galactosylceramide ameliorates experimental lupus nephritis in mice. Sci Rep 8, 8225 (2018). https://doi.org/10.1038/s41598-018-26470-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-26470-w
- Springer Nature Limited
This article is cited by
-
Alpha-galactosylceramide pre-treatment attenuates clinical symptoms of LPS-induced acute neuroinflammation by converting pathogenic iNKT cells to anti-inflammatory iNKT10 cells in the brain
Inflammation Research (2024)
-
Unconventional T cells and kidney disease
Nature Reviews Nephrology (2021)