Abstract
We theoretically know that metabolic disorders, including overweight/obesity, insulin resistance, diabetes, dyslipidemia, and relevant tissue/organ damage, play a critical role in elevating blood pressure and developing hypertension. However, staying abreast of the ever-evolving and current research on the various metabolic disorder topics is difficult. At the same time, as hypertension in childhood and adolescence is attracting significant attention globally, it is becoming increasingly evident that metabolic disorders exert an important role in its pathogenesis. In order to effectively prevent hypertension, it is essential to appropriately approach metabolic disorders, and importantly, this approach must be practiced continuously throughout all generations. Thus, focusing on metabolic disorders is the first and essential step in effectively managing and preventing hypertension. In this Mini-Review, we introduce cutting-edge research findings on “Metabolism,” published in 2023 by Hypertension Research, and discuss relevant topics and therapeutic and future perspectives.

Similar content being viewed by others
Introduction
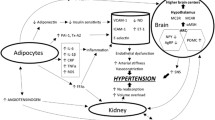
Metabolic disorders, including obesity, diabetes, and dyslipidemia, are foundational pathogenesis of metabolic syndrome (MetS) and cardiovascular diseases (CVD). Also, such metabolic disorders are closely associated with increased blood pressure (BP) and hypertension in conjunction with insulin resistance, chronic inflammation, and vascular failure [1, 2]. Therefore, prevention and treatment strategies against these conditions should be widely implemented over generations. However, there are still insufficient countermeasures, and the incidence of metabolic disorder-related disease conditions, including CVD and even cancer [3], is expected to continually increase globally. Updating the ever-evolving research on metabolic disorders and accelerating further research and its application to clinical practice is urgently required. In this Mini-Review, we introduce cutting-edge research findings on “Metabolism” published in 2023 by Hypertension Research, the official journal of the Japanese Society of Hypertension, and discuss relevant topics and perspectives (Fig. 1). Each section is divided into three parts: an overview of each topic related to metabolism, an introduction of research papers recently reported in Hypertens Res, and a therapeutic perspective based on recent evidence.
Overweight/obesity
The prevalence of overweight/obesity has reached a pandemic level globally, imposing substantial medical, economic, and social burdens [4]. Overweight/obesity is characterized by accumulated visceral fat and various metabolic alterations, contributing to the hypertensive state and the risk of subsequent CVD [5, 6]. It is therefore urgently required to identify at-risk individuals with overweight/obesity early to facilitate appropriate interventions [7].
Kawasoe et al. [8] investigated which anthropometric indices, including body mass index (BMI), waist circumference (WC), body roundness index (BRI), and body shape index, predict the future incidence of hypertension in the Japanese general population by sex and age categories. Among those indices, BMI, WC, and BRI were similarly associated with the study outcome; they were more prominent in women and the younger generation (30 s and 40 s). At the same time, Ishida et al. [9] reported that visceral fat and the anthropometric indices were also positively associated with the presence of individual components of MetS, including hypertension, hyperglycemia, and hyperglycemia in a cohort of community-based participants receiving health checkups. Interestingly, Wu et al. [10] investigated the association between menopausal age and BP levels and the mediating effects of obesity indices in a population-based cohort of female residents from Guangzhou. The authors found that older age (50 years or more) was positively associated with higher BP levels, which was modestly mediated by several obesity indicators, such as BMI and WC. Their findings suggest that prolonged estrogen exposure promotes visceral fat accumulation and is partially responsible for menopausal hypertension. This potentially contributes to the women’s health promotion for hypertension, according to the menopause information. In a study by Fukumine and Nakamura [11], noting that the Okinawa Prefecture has one of the highest obesity percentages in Japan, the authors conducted a cross-sectional study examining the association between obesity and hypertension among residents of Yonaguni Island, a remote island of Okinawa. Among the residents analyzed, 54.3% of men and 32.3% of women had obesity with a BMI of 25 kg/m2 or higher. Furthermore, among the people with hypertension, 49.5% of men and 37.9% of women were obese. Although Japan is generally considered to have a lower rate of obesity compared with the Western population, their findings suggest the need to promote quality health care for obesity and obesity-related diseases even in Japan according to the local-specific characteristics.
Overweight/obesity is a major culprit for the risk of hypertension and CVD events. Lifestyle modification is an essential part of prevention and therapy. Aerobic exercise alone or in combination with resistance training is favorable for improving the CVD risk profile, including BP, in people with overweight/obesity [12]. However, lifestyle modification alone is often insufficient to improve the condition and reduce the risk of relevant cardiovascular events. Given the degree of body weight reduction from bariatric surgery (20% or more) and its apparent beneficial effect on cardiovascular mortality [13], it is reasonable to assume that anti-obesity medications with greater weight-loss effects may be useful in reducing the risk of CVD events [14]. In this context, glucagon-like peptide-1 receptor agonist (GLP-1RA) and tirzepatide, a novel dual agonist of glucose-dependent insulinotropic polypeptide and GLP-1 receptor, have demonstrated a substantial body weight reduction in people with overweight/obesity [15,16,17,18]. Several large-scale randomized clinical trials with GLP-1RA and a systematic review and meta-analysis showed a significant risk reduction in cardiovascular events and mortality [19, 20]. More recently, GLP-1RA (semaglutide) therapy proved to be clinically effective for improving the symptoms and physical limitations in patients with heart failure with preserved ejection fraction and obesity [21]. This sheds light on the potential therapeutic role of GLP-1RA in this patient population [22].
Diabetes
Diabetes and hypertension often coexist and enhance the risk of CVD events synergistically. Approximately 50% of patients with diabetes have hypertension, and 20% of patients with hypertension have diabetes in Japan. The risk of CVD events increases by three to six-fold in patients with both conditions compared with people without [23]. In a recently reported cohort study of 590,000 Japanese individuals, the incidence of CVD events rose with increasing systolic and diastolic BP levels, regardless of diabetes status [24]. Therefore, better BP control is essential for cardiovascular and renal protection in patients with diabetes or prediabetes. At the same time, it is also necessary to distinguish the patients at risk and intervene via a patient-centric approach [25].
Suzuki et al. [26] assessed the impact of diabetes status, such as diabetes and prediabetes, and BP on the risk of CVD events using the Japan Morning Surge-Home Blood Pressure study dataset. The authors found that prediabetes is potentially associated with the risk of future CVD events, while diabetes predicts it. Additionally, elevated systolic BP at the office and home imposed a risk of future CVD events in diabetes but not prediabetes. Their findings indicate that we should recognize that prediabetes is already a risk for CVD events, but it is also a requisite to determine potential factors other than BP to mediate that risk. Insulin resistance and hyperinsulinemia are primary pathologies of obesity, prediabetes, and diabetes. They contribute to BP elevation via several adverse actions, such as increased renal sodium reabsorption and fluid retention, vascular remodeling, and sympathetic tone activation [27]. Among the indices of insulin resistance is the triglyceride-glucose (TyG) index, a parameter composed of fasting triglyceride and fasting plasma glucose, which is strongly associated with the risk of incident hypertension and CVD events in the general population [28,29,30,31,32,33]. Miao et al. [34] tested whether the association between individual TyG-related parameters, including TyG-BMI, TyG-WC, TyG-waist-to-hip ratio (TyG-WHR), and TyG-waist-to-height-ratio and the presence of hypertension and 10-year atherosclerotic CVD (ASCVD) risk differ in residents from a community in Beijing, China. Among TyG-parameters, TyG-WC and TyG-WHR exhibited a superior ability to distinguish the patients with hypertension and those with high 10-year ASCVD risk status, respectively. Their findings highlight the need for longitudinal studies using those parameters in the Asian population, especially in a primary care setting. Sakoda et al. [35] examined whether the TyG index predicts the risk of chronic kidney disease (CKD) onset in Japanese middle-aged men. The authors found that the TyG index was a more stable indicator of the outcome than individual components of the index. This predictive ability was consistent across BP categories, such as normotensive, hypertensive, isolated systolic, or diastolic hypertensive status. Thus, the TyG index, initially recognized as an indicator of insulin resistance, has recently emerged as a clinically important predictor of cardiovascular and renal event risk.
Several clinical questions exist concerning BP control in diabetes, e.g., target BP threshold and how to reduce BP to improve the prognosis in patients with diabetes [36]. In this context, two glucose-lowering agents, sodium-glucose cotransporter 2 inhibitor (SGLT2i) and GLP-1RA, have modest but significant BP-lowering effects and proven benefits for cardiovascular and renal events [37]. Those agents potentially reduce BP via direct and indirect approaches to the key pathophysiology of diabetes-related hypertension, such as attenuation of sodium reabsorption and body weight reduction [36]. According to our experience, in a sub-analysis of a randomized clinical trial [38], SGLT2i ipragliflozin therapy modestly reduced systolic BP over 24 months in patients with type 2 diabetes who had been receiving standard therapy for type 2 diabetes and relevant comorbidities including hypertension. Interestingly, the BP reduction was positively correlated with the degree of weight loss, suggesting that weight loss was, at least in part, responsible for the BP reduction after initiating SGLT2i therapy. Furthermore, in another sub-analysis of a placebo-controlled trial for patients with type 2 diabetes and established CVD, we found that 24 weeks of SGLT2i empagliflozin therapy modestly but significantly reduced systolic/diastolic BPs and mean arterial pressure. The systolic BP reduction was almost consistent across background clinical features and usage status of conventional anti-hypertensive medications [39]. Thus, the glucose-lowering agents that have the combined effect of weight loss and BP-lowering will attract more attention for better BP control with the idea of preventing cardiovascular and renal diseases in overweight/obesity and diabetes.
Dyslipidemia and related liver diseases
Dyslipidemia is an established risk factor of CVD, and metabolic dysfunction-associated fatty liver disease (MAFLD) has also recently been proven to be associated with diverse CVDs, including ASCVD, heart failure, and arrhythmia [40, 41]. Although there have been numerous studies on low-density lipoprotein (LDL)-cholesterol concerning dyslipidemia, knowledge is limited with respect to other lipid indices, including triglycerides. At the same time, cardiologists, including ourselves, are still not fully knowledgeable about MAFLD and its relationship with hypertension and CVD. Apart from LDL-cholesterol, those issues may represent residual CVD risk factors, which we need to address in the next decade.
Ishida et al. [42] investigated whether serum triglyceride levels could predict the development of hypertension among the general Japanese population. The authors found that high triglyceride levels, irrespective of fasting or non-fasting sampling, were associated with the outcome in men but not in women, highlighting a potential need for a sex-specific approach for clinically managing hypertriglyceridemia. Although the precise mechanisms underlying this association remain to be fully determined, the authors discussed the hypertriglyceridemia-induced alteration of LDL-cholesterol into an atherogenic one, namely small dense LDL (sdLDL), and its adverse effects on arterial function and construction as one of the mechanisms [42]. In this context, Tanaka et al. [43] reported that among relevant lipid profiles, sdLDL-cholesterol, calculated by the Sampson equation [44], was the most powerful predictor of new-onset hypertension over 10 years in the Japanese general population. Moreover, Uemura et al. [45] examined the association between a novel indicator of dyslipidemia triglyceride-to-high-density lipoprotein-cholesterol (TG/HDL-C) and the risk of incident CVD and end-stage kidney disease (ESKD) in patients with biopsy-proven diabetic nephropathy. They concluded that the TG/HDL-C ratio was independently associated with the risk of incident CVD but not ESKD, suggesting its different impact on cardiovascular and renal outcomes. Regarding relevant fatty liver diseases, Wu et al. [46] found that the calculated fatty liver index [47] could predict the risk of hypertension onset in the Japanese general population irrespective of diabetes status. Furthermore, Mori et al. [48] demonstrated that MAFLD enhanced the temporal increase in systolic BP over 10 years, compared with individuals without fatty liver and even those with ultrasonography-proven nonalcoholic fatty liver disease (non-metabolic disorder features). These studies highlight the importance of further research collaboration with hepatologists in the areas of hypertension and cardiology.
Fibrates effectively modify atherogenic lipid profiles, including lowering serum triglyceride levels. In contrast, the impact of fibrates on the risk of cardiovascular events has been controversial for a long time [49, 50]. In a recent large-scale randomized clinical trial with a newer fibrate pemafibrate for patients with type 2 diabetes and hypertriglyceridemia (the PROMINENT trial), pemafibrate therapy, compared with placebo, did not reduce the incidence of cardiovascular events, despite improving atherogenic lipid profiles [51]. On the other hand, a more recent case-control study showed that fibrate use was associated with a reduced risk of cardiovascular events in Japanese people with CKD [52]. Given the potential benefit of fibrates on albuminuria [53], fibrate-mediated lipid modulation may be a promising therapeutic target in patients with CKD [54]. Finally, there is accumulating evidence on the beneficial effects of SGLT2i and GLP-1RA on relevant liver diseases, including MAFLD and even liver cancer [55,56,57,58,59]. This potentially underpins the expansion of these agents into therapeutic advantages across organs.
Hypertension in the young generation
An epidemiology study revealed a global trend of the increasing prevalence of pediatric hypertension during the past two decades [60]. Hypertension in childhood and adolescence is often related to obesity and suboptimal lifestyles, leading to target organ damage and the development of cardiovascular and renal diseases in adulthood [61, 62]. However, these facts are still underrecognized, and further academic and public efforts are urgently and globally warranted to better identify young individuals with hypertension, optimize their BP levels, and improve their future prognosis [63].
Li et al. [64] showed that disturbed levels of adipokines, including leptin, were associated with hypertension in young Chinese individuals, and the association was substantially mediated through obesity-related insulin resistance. Van Niekerk et al. [65] also demonstrated that 24-h ambulatory BP was positively correlated with the serum leptin level in young African adults with overweight/obesity, indicating a central role of adiposity in the elevation of BP during youth. Cui et al. [66] examined the longitudinal impact of weight change trajectories on BP levels and the incidence of hypertension in Chinese adolescents. The authors showed that weight gain over time and persistent overweight/obesity enhanced the risk of the endpoints, while weight loss reduced it. These findings strongly support the importance of earlier management of overweight/obesity to optimize BP in childhood and adolescence and reduce the risk of cardiovascular and renal events in later life.
Importantly, the evidence on accurate screening for high BP and long-term health outcomes after BP screening and intervention in childhood and adolescence is still inconclusive [67]. Nevertheless, the prevalence of hypertension in that generation is rising in the United States, China, and South Korea [68,69,70]. Moreover, a recent systematic review and meta-analysis revealed that the prevalence of masked hypertension (MH) in the general pediatric population was 10.4% (95% confidence interval, 8.0–12.8%), being accelerated by the risk of conditions such as CKD. Children diagnosed with MH had more evident subclinical cardiovascular risks, including left ventricular hypertrophy and increased arterial stiffness [71]. However, little is known about the current BP situation in childhood and adolescence in Japan. In a pilot study attempting to assess this issue, we found that the prevalence of hypertension in a junior and senior high school in Saga Prefecture, Japan, was 8.7% in junior high school students and 6.2% in senior high school students [72]. To measure and manage their BP appropriately, it is essential to spread knowledge and awareness about BP, especially at schools and in the community.
Conclusion
We herein introduced the recent progress of hypertension research in the area of metabolic disorders. Along with advances and developments in the treatment of hypertension, the importance of hypertension prevention throughout all generations is expected to increase. In this context, focusing on metabolic disorders is the first and essential step in effectively preventing hypertension. Finally, we will meet in the early autumn and learn about the latest updates in hypertension science, including anti-hypertensive metabolic modulations and social prevention of hypertension, at the Annual Scientific meeting of the Japanese Society of Hypertension held in Fukuoka, Japan [73].
References
Ferrannini E, Natali A. Essential hypertension, metabolic disorders, and insulin resistance. Am Heart J. 1991;121:1274–82.
Inoue T, Node K. Vascular failure: a new clinical entity for vascular disease. J Hypertens. 2006;24:2121–30.
Liu C, Liu T, Zhang Q, Song M, Zhang Q, Shi J, et al. Temporal relationship between inflammation and metabolic disorders and their impact on cancer risk. J Glob Health. 2024;14:04041.
Blüher M. Obesity: global epidemiology and pathogenesis. Nat Rev Endocrinol. 2019;15:288–98.
Seravalle G, Grassi G. Obesity and hypertension. Pharm Res. 2017;122:1–7.
Nakamura K, Okamura T, Hayakawa T, Hozawa A, Kadowaki T, Murakami Y, et al. The proportion of individuals with obesity-induced hypertension among total hypertensives in a general Japanese population: NIPPON DATA80, 90. Eur J Epidemiol. 2007;22:691–8.
Zhang L, Dai S, Chen Y, Jin T, Li W, Wang W, et al. Scoping review of obesity interventions: Research frontiers and publication status. iScience. 2024;27:109240.
Kawasoe S, Kubozono T, Salim AA, Ojima S, Yamaguchi S, Ikeda Y, et al. Association between anthropometric indices and 5-year hypertension incidence in the general Japanese population. Hypertens Res. 2024;47:867–76.
Ishida A, Taira H, Shinzato T, Ohya Y. Association between visceral fat mass and arterial stiffness among community-based screening participants. Hypertens Res. 2023;46:2488–96.
Wu YJ, Jiang CQ, Zhu T, Jin YL, Zhu F, Zhou BJ, et al. Obesity indicators as mediators of the association between age at menopause and blood pressure values. Hypertens Res. 2023;46:1100–9.
Fukumine Y, Nakamura K. Obesity and hypertension from a public health perspective in a small remote island of Okinawa, Japan. Hypertens Res. 2023;46:1850–9.
Lee DC, Brellenthin AG, Lanningham-Foster LM, Kohut ML, Li Y. Aerobic, resistance, or combined exercise training and cardiovascular risk profile in overweight or obese adults: the CardioRACE trial. Eur Heart J. 2024;45:1127–42.
Cardoso L, Rodrigues D, Gomes L, Carrilho F. Short- and long-term mortality after bariatric surgery: a systematic review and meta-analysis. Diabetes Obes Metab. 2017;19:1223–32.
Sawami K, Tanaka A, Node K. Anti-obesity therapy for cardiovascular disease prevention: potential expected roles of glucagon-like peptide-1 receptor agonists. Cardiovasc Diabetol. 2022;21:176.
Kadowaki T, Isendahl J, Khalid U, Lee SY, Nishida T, Ogawa W, et al. Semaglutide once a week in adults with overweight or obesity, with or without type 2 diabetes in an east Asian population (STEP 6): a randomised, double-blind, double-dummy, placebo-controlled, phase 3a trial. Lancet Diabetes Endocrinol. 2022;10:193–206.
Ryan DH, Lingvay I, Colhoun HM, Deanfield J, Emerson SS, Kahn SE, et al. Semaglutide effects on cardiovascular outcomes in people with overweight or obesity (SELECT) rationale and design. Am Heart J. 2020;229:61–9.
Wilding JPH, Batterham RL, Calanna S, Davies M, Van Gaal LF, Lingvay I, et al. Once-weekly semaglutide in adults with overweight or obesity. N Engl J Med. 2021;384:989–1002.
Tan B, Pan XH, Chew HSJ, Goh RSJ, Lin C, Anand VV, et al. Efficacy and safety of tirzepatide for treatment of overweight or obesity. A systematic review and meta-analysis. Int J Obes (Lond). 2023;47:677–85.
Lincoff AM, Brown-Frandsen K, Colhoun HM, Deanfield J, Emerson SS, Esbjerg S, et al. Semaglutide and cardiovascular outcomes in obesity without diabetes. N Engl J Med. 2023;389:2221–32.
Sattar N, Lee MMY, Kristensen SL, Branch KRH, Del Prato S, Khurmi NS, et al. Cardiovascular, mortality, and kidney outcomes with GLP-1 receptor agonists in patients with type 2 diabetes: a systematic review and meta-analysis of randomised trials. Lancet Diabetes Endocrinol. 2021;9:653–62.
Kosiborod MN, Abildstrøm SZ, Borlaug BA, Butler J, Rasmussen S, Davies M, et al. Semaglutide in patients with heart failure with preserved ejection fraction and obesity. N Engl J Med. 2023;389:1069–84.
Cimino G, Vaduganathan M, Lombardi CM, Pagnesi M, Vizzardi E, Tomasoni D, et al. Obesity, heart failure with preserved ejection fraction, and the role of glucagon-like peptide-1 receptor agonists. ESC Heart Fail. 2024;11:649–61.
Tatsumi Y, Ohkubo T. Hypertension with diabetes mellitus: significance from an epidemiological perspective for Japanese. Hypertens Res. 2017;40:795–806.
Yamada MH, Fujihara K, Kodama S, Sato T, Osawa T, Yaguchi Y, et al. Associations of systolic blood pressure and diastolic blood pressure with the incidence of coronary artery disease or cerebrovascular disease according to glucose status. Diabetes Care. 2021;44:2124–31.
Tanaka A, Node K. Evidence-based and tailored medication in type 2 diabetes: a pathway learned from clinical trials. Cardiovasc Diabetol. 2019;18:19.
Suzuki D, Hoshide S, Kario K. Impact of diabetic status and contribution of office and home blood pressure across diabetic status for cardiovascular disease: the J-HOP study. Hypertens Res. 2023;46:1684–93.
Ferrannini E, Cushman WC. Diabetes and hypertension: the bad companions. Lancet. 2012;380:601–10.
Gao Q, Lin Y, Xu R, Luo F, Chen R, Li P, et al. Positive association of triglyceride-glucose index with new-onset hypertension among adults: a national cohort study in China. Cardiovasc Diabetol. 2023;22:58.
Lee JH, Heo SJ, Kwon YJ. Sex-specific comparison between triglyceride glucose index and modified triglyceride glucose indices to predict new-onset hypertension in middle-aged and older adults. J Am Heart Assoc. 2023;12:e030022.
Xin F, He S, Zhou Y, Jia X, Zhao Y, Zhao H. The triglyceride glucose index trajectory is associated with hypertension: a retrospective longitudinal cohort study. Cardiovasc Diabetol. 2023;22:347.
Liang S, Wang C, Zhang J, Liu Z, Bai Y, Chen Z, et al. Triglyceride-glucose index and coronary artery disease: a systematic review and meta-analysis of risk, severity, and prognosis. Cardiovasc Diabetol. 2023;22:170.
Liu X, Tan Z, Huang Y, Zhao H, Liu M, Yu P, et al. Relationship between the triglyceride-glucose index and risk of cardiovascular diseases and mortality in the general population: a systematic review and meta-analysis. Cardiovasc Diabetol. 2022;21:124.
Lopez-Jaramillo P, Gomez-Arbelaez D, Martinez-Bello D, Abat MEM, Alhabib KF, Avezum Á, et al. Association of the triglyceride glucose index as a measure of insulin resistance with mortality and cardiovascular disease in populations from five continents (PURE study): a prospective cohort study. Lancet Healthy Longev. 2023;4:e23–e33.
Miao H, Zhou Z, Yang S, Zhang Y. The association of triglyceride-glucose index and related parameters with hypertension and cardiovascular risk: a cross-sectional study. Hypertens Res. 2024;47:877–86.
Sakoda T, Akasaki Y, Sasaki Y, Kawasoe S, Kubozono T, Ikeda Y, et al. Triglyceride-glucose index predicts future chronic kidney disease development in all populations, including normotensive and isolated diastolic hypertension. Hypertens Res. 2024;47:149–56.
Sawami K, Tanaka A, Node K. Recent understandings about hypertension management in type 2 diabetes: What are the roles of SGLT2 inhibitor, GLP-1 receptor agonist, and finerenone? Hypertens Res. 2023;46:1892–9.
Tanaka A, Node K. Hypertension in diabetes care: emerging roles of recent hypoglycemic agents. Hypertens Res. 2021;44:897–905.
Saito Y, Tanaka A, Imai T, Nakamura I, Kanda J, Matsuhisa M, et al. Long-term effects of ipragliflozin on blood pressure in patients with type 2 diabetes: insights from the randomized PROTECT trial. Hypertens Res. 2024;47:168–76.
Tanaka A, Shimabukuro M, Teragawa H, Yoshida H, Okada Y, Takamura T, et al. Blood pressure reduction with empagliflozin in Japanese patients with type 2 diabetes and cardiovascular diseases: a post-hoc sub-analysis of the placebo-controlled randomized EMBLEM trial. Hypertens Res. 2024. (in press).
Kasper P, Martin A, Lang S, Kütting F, Goeser T, Demir M, et al. NAFLD and cardiovascular diseases: a clinical review. Clin Res Cardiol. 2021;110:921–37.
Stahl EP, Dhindsa DS, Lee SK, Sandesara PB, Chalasani NP, Sperling LS. Nonalcoholic fatty liver disease and the heart: JACC state-of-the-art review. J Am Coll Cardiol. 2019;73:948–63.
Ishida S, Kondo S, Funakoshi S, Abe M, Satoh A, Kawazoe M, et al. Serum triglyceride levels and incidence of hypertension in a general Japanese population: ISSA-CKD study. Hypertens Res. 2023;46:1122–31.
Tanaka M, Sato T, Endo K, Inyaku M, Mori K, Hosaka I, et al. An increase in calculated small dense low-density lipoprotein cholesterol predicts new onset of hypertension in a Japanese cohort. Hypertens Res. 2023;46:2635–45.
Sampson M, Wolska A, Warnick R, Lucero D, Remaley AT. A new equation based on the standard lipid panel for calculating small dense low-density lipoprotein-cholesterol and its use as a risk-enhancer test. Clin Chem. 2021;67:987–97.
Uemura T, Nishimoto M, Eriguchi M, Tamaki H, Tasaki H, Furuyama R, et al. Association of triglycerides to high-density lipoprotein cholesterol ratio with incident cardiovascular disease but not end-stage kidney disease among patients with biopsy-proven diabetic nephropathy. Hypertens Res. 2023;46:1423–32.
Wu D, Hirata A, Hirata T, Imai Y, Kuwabara K, Funamoto M, et al. Fatty liver index predicts the development of hypertension in a Japanese general population with and without dysglycemia. Hypertens Res. 2023;46:879–86.
Bedogni G, Bellentani S, Miglioli L, Masutti F, Passalacqua M, Castiglione A, et al. The Fatty Liver Index: a simple and accurate predictor of hepatic steatosis in the general population. BMC Gastroenterol. 2006;6:33.
Mori K, Tanaka M, Hosaka I, Mikami T, Endo K, Hanawa N, et al. Metabolic dysfunction-associated fatty liver disease is associated with an increase in systolic blood pressure over time: linear mixed-effects model analyses. Hypertens Res. 2023;46:1110–21.
Jakob T, Nordmann AJ, Schandelmaier S, Ferreira-González I, Briel M. Fibrates for primary prevention of cardiovascular disease events. Cochrane Database Syst Rev. 2016;11:Cd009753.
Lim GB. Limited benefit of triglyceride lowering with fibrates in statin-treated patients. Nat Rev Cardiol. 2023;20:4.
Das Pradhan A, Glynn RJ, Fruchart JC, MacFadyen JG, Zaharris ES, Everett BM, et al. Triglyceride lowering with pemafibrate to reduce cardiovascular risk. N Engl J Med. 2022;387:1923–34.
Goto H, Iseri K, Hida N. Fibrates and the risk of cardiovascular outcomes in chronic kidney disease patients. Nephrol Dial Transplant. 2023:gfad248. https://doi.org/10.1093/ndt/gfad248. Epub ahead of print.
Hadjivasilis A, Kouis P, Kousios A, Panayiotou A. The effect of fibrates on kidney function and chronic kidney disease progression: a systematic review and meta-analysis of randomised studies. J Clin Med. 2022;11:768.
Mitrofanova A, Merscher S, Fornoni A. Kidney lipid dysmetabolism and lipid droplet accumulation in chronic kidney disease. Nat Rev Nephrol. 2023;19:629–45.
Borisov AN, Kutz A, Christ ER, Heim MH, Ebrahimi F. Canagliflozin and metabolic associated fatty liver disease in patients with diabetes mellitus: new insights from CANVAS. J Clin Endocrinol Metab. 2023;108:2940–9.
Suzuki Y, Kaneko H, Okada A, Ohno R, Yokota I, Fujiu K, et al. Comparison of SGLT2 inhibitors vs. DPP4 inhibitors for patients with metabolic dysfunction associated fatty liver disease and diabetes mellitus. J Endocrinol Invest. 2024;47:1261–70.
Targher G, Mantovani A, Byrne CD. Mechanisms and possible hepatoprotective effects of glucagon-like peptide-1 receptor agonists and other incretin receptor agonists in non-alcoholic fatty liver disease. Lancet Gastroenterol Hepatol. 2023;8:179–91.
Wester A, Shang Y, Toresson Grip E, Matthews AA, Hagström H. Glucagon-like peptide-1 receptor agonists and risk of major adverse liver outcomes in patients with chronic liver disease and type 2 diabetes. Gut. 2024.
Moon JS, Hong JH, Jung YJ, Ferrannini E, Nauck MA, Lim S. SGLT-2 inhibitors and GLP-1 receptor agonists in metabolic dysfunction-associated fatty liver disease. Trends Endocrinol Metab. 2022;33:424–42.
Song P, Zhang Y, Yu J, Zha M, Zhu Y, Rahimi K, et al. Global prevalence of hypertension in children: a systematic review and meta-analysis. JAMA Pediatr. 2019;173:1154–63.
Yang L, Magnussen CG, Yang L, Bovet P, Xi B. Elevated blood pressure in childhood or adolescence and cardiovascular outcomes in adulthood: a systematic review. Hypertension. 2020;75:948–55.
Chung J, Robinson CH, Yu A, Bamhraz AA, Ewusie JE, Sanger S, et al. Risk of target organ damage in children with primary ambulatory hypertension: a systematic review and meta-analysis. Hypertension. 2023;80:1183–96.
Falkner B, Gidding SS, Baker-Smith CM, Brady TM, Flynn JT, Malle LM, et al. Pediatric primary hypertension: an underrecognized condition: a scientific statement from the American Heart Association. Hypertension. 2023;80:e101–11.
Li B, Hou C, Li L, Li M, Gao S. The associations of adipokines with hypertension in youth with cardiometabolic risk and the mediation role of insulin resistance: The BCAMS study. Hypertens Res. 2023;46:1673–83.
van Niekerk E, Botha-Le Roux S, Mels CMC, Swanepoel M, Delles C, Welsh P, et al. Twenty-four-hour ambulatory, but not clinic blood pressure associates with leptin in young adults with overweight or obesity: The African-PREDICT study. Hypertens Res. 2024;47:478–86.
Cui Y, Zhang F, Wang H, Wu J, Zhang D, Xing Y, et al. Children who appeared or remained overweight or obese predict a higher follow-up blood pressure and higher risk of hypertension: a 6-year longitudinal study in Yantai, China. Hypertens Res. 2023;46:1840–9.
Gartlehner G, Vander Schaaf EB, Orr C, Kennedy SM, Clark R, Viswanathan M. U.S. preventive services task force evidence syntheses, formerly systematic evidence reviews. In: Screening for Hypertension in Children and Adolescents: Systematic Review for the US Preventive Services Task Force. Rockville (MD). Agency for Healthcare Research and Quality (US); 2020.
Hardy ST, Sakhuja S, Jaeger BC, Urbina EM, Suglia SF, Feig DI, et al. Trends in blood pressure and hypertension among US children and adolescents, 1999–2018. JAMA Netw Open. 2021;4:e213917.
Wang L, Song L, Liu B, Zhang L, Wu M, Cao Z, et al. Trends and status of the prevalence of elevated blood pressure in children and adolescents in China: a systematic review and meta-analysis. Curr Hypertens Rep. 2019;21:88.
Park PG, Park E, Kang HG. Increasing trend in hypertension prevalence among Korean adolescents from 2007 to 2020. BMC Public Health. 2024;24:617.
Chung J, Robinson C, Sheffield L, Paramanathan P, Yu A, Ewusie J, et al. Prevalence of pediatric masked hypertension and risk of subclinical cardiovascular outcomes: a systematic review and meta-analysis. Hypertension. 2023;80:2280–92.
Tanaka A, Yajima A, Kitaoka K, Natsuaki M, Yoshioka G, Kaneko H, et al. Blood pressure in Japanese junior and senior high school students. Hypertens Res. 2024;47:195–6.
Node K, Tanaka A. Our mission in the Japanese Society of Hypertension (JSH) Future Plan: a baton-connection from JSH Osaka 2023 to Fukuoka 2024. Hypertens Res. 2024;47:1097–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
AT received honoraria from Boehringer Ingelheim Japan and Mochida and research funding from GlaxoSmithKline, Takeda, Bristol Myers Squibb, and Novo Nordisk. KN has received honoraria from AstraZeneca, Bayer Yakuhin, Boehringer Ingelheim Japan, Daiichi Sankyo, Eli Lilly Japan, Kowa, Mitsubishi Tanabe Pharma, Mochida Pharmaceutical, MSD, Novartis Pharma, Novo Nordisk Pharma, Otsuka; Research grant from Astellas, Bayer Yakuhin, Boehringer Ingelheim Japan, Fuji Yakuhin, Mitsubishi Tanabe, Pharma Corporation, Mochida Pharmaceutical, Novartis Pharma; Scholarship from Abbott, Boehringer Ingelheim Japan, Daiichi Sankyo Healthcare, Mitsubishi Tanabe Pharma, Teijin Pharma.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tanaka, A., Node, K. Associations of metabolic disorders with hypertension and cardiovascular disease: recent findings and therapeutic perspectives. Hypertens Res (2024). https://doi.org/10.1038/s41440-024-01737-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41440-024-01737-0
- Springer Nature Singapore Pte Ltd.