Abstract
Alcohol is associated with nearly half of all violent crimes committed in the United States; yet, a potential neural basis for this type of pathological aggression remains elusive. Alcohol may act on N-methyl-d-aspartate receptors (NMDARs) within cortical circuits to impede processing and to promote aggression. Here, male mice were characterized as alcohol-heightened (AHAs) or alcohol non-heightened aggressors (ANAs) during resident–intruder confrontations after self-administering 1.0 g/kg alcohol (6% w/v) or water. Alcohol produced a pathological-like pattern of aggression in AHAs; these mice shifted their bites to more vulnerable locations on the body of a submissive animal, including the anterior back and ventrum after consuming alcohol. In addition, through immunoblotting, we found that AHAs overexpressed the NMDAR GluN2D subunit in the prefrontal cortex (PFC) as compared to ANAs while the two phenotypes expressed similar levels of GluN1, GluN2A and GluN2B. After identifying several behavioral and molecular characteristics that distinguish AHAs from ANAs, we tested additional mice for their aggression following preferential antagonism of GluN2D-containing NMDARs. In these experiments, groups of AHAs and ANAs self-administered 1.0 g/kg alcohol (6% w/v) or water before receiving intraperitoneal (i.p.) doses of ketamine or memantine, or infusions of memantine directly into the prelimbic (PLmPFC) or infralimbic medial PFC (ILmPFC). Moderate doses of IP ketamine, IP memantine, or intra-PLmPFC memantine increased aggression in AHAs, but only in the absence of alcohol. Prior alcohol intake blocked the pro-aggressive effects of ketamine or memantine. In contrast, only memantine, administered systemically or intra-PLmPFC, interacted with prior alcohol intake to escalate aggression in ANAs. Intra-ILmPFC memantine had no effect on aggression in either AHAs or ANAs. In sum, this work illustrates a potential role of GluN2D-containing NMDARs in the PLmPFC in alcohol-heightened aggression. GluN2D-containing NMDARs are highly expressed on cortical parvalbumin-containing interneurons, suggesting that, in a subset of individuals, alcohol may functionally alter signal integration within cortical microcircuits to dysregulate threat reactivity and promote aggression. This work suggests that targeting GluN2D-NMDARs may be of use in reducing the impact of alcohol-related violence in the human population.
Similar content being viewed by others
Introduction
Approximately half of all violent crimes committed in the United States are associated with alcohol consumption (Cherpitel, 2007). In describing aggressive individuals, two major subtypes have been identified: proactive or ‘cold-blooded’ aggressors tend to be manipulative and planning and may exhibit blunted affect and low autonomic reactivity; conversely, reactive or ‘hot-headed’ aggressors are impulsive, hostile and more likely to have deficits in information-processing (Giancola et al, 1996; Raine et al, 2006). Unlike proactive aggressors, reactive, violent individuals have a high risk of engaging in alcohol-escalated aggression (Giancola et al, 1996; Giancola, 2000). Reduced executive functioning and dysregulated medial prefrontal cortical (mPFC) control over subcortical, aggression-promoting brain regions may render reactive male aggressors more susceptible to the pro-aggressive effects of alcohol (Raine et al, 1998; Gan et al, 2015). Despite significant clinical research pointing to this relationship, the underlying neural bases for dysregulated cortical control and subsequent alcohol-escalated aggression remain unknown. Using a mouse model, we provide evidence to suggest that the inhibition of N-methyl-d-aspartate receptors (NMDARs) in the mPFC may be a mechanism by which alcohol, memantine, and ketamine escalate aggression in the same subset of individuals.
At physiologically relevant concentrations, alcohol can inhibit NMDAR-mediated excitatory currents (Lovinger et al, 1989). In the mammalian central nervous system, NMDARs are primarily comprised of two glutamate-sensitive GluN2 subunits, occurring in subtypes GluN2A-D, and two glycine-sensitive GluN1 subunits (Paoletti et al, 2013). Memantine, an NMDAR channel blocker (ie uncompetitive antagonist) with preferential action on GluN2C- or GluN2D-containing NMDARs (Parsons et al, 1999; Kotermanski and Johnson, 2009; Riebe et al, 2016), is clinically used for the treatment of Alzheimer’s disease, and has been proposed as a potential treatment option for alcohol use disorders (Goodwani et al, 2017). However, preclinical data indicate that memantine can facilitate aggressive behavior in mice when administered either after acute alcohol intake or during alcohol withdrawal (Newman et al, 2012; Hwa et al, 2015). Clinical evidence also suggests that memantine may disinhibit alcohol intake in a subset of individuals with higher baseline impulsivity (Krishnan-Sarin et al, 2015). Low doses of ketamine, another uncompetitive NMDAR antagonist has promising antidepressant effects (Berman et al, 2000); yet, it can also escalate aggression in some animals after acute (Newman et al, 2012) or chronic treatment (Becker et al, 2003; Becker and Grecksch, 2004).
In the present work, we extend our previous findings by first identifying a subset of outbred mice that is sensitive to the pro-aggressive effects of alcohol, memantine and ketamine. Memantine can reduce prefrontal cortical activity through its preferential blockade of GluN2C- or GluN2D-containing NMDARs expressed predominately on parvalbumin-containing interneurons (PVIs; Jackson et al, 2004; Homayoun and Moghaddam, 2007; Nakazawa et al, 2012; Gupta et al, 2016; Sapkota et al, 2016; Povysheva and Johnson, 2016). By reducing excitability of GABAergic PVIs that innervate glutamatergic projection neurons, NMDAR channel blockers can disinhibit subcortical brain areas that may promote aggressive behaviors. In rodents, functionally distinct subregions of the mPFC including the prelimbic (PLmPFC) and infralimbic (ILmPFC) areas have been tied to reward-seeking behavior and extinction conditioning, respectively (Gourley and Taylor 2016). Because both aggression and alcohol can serve as potent, positive reinforcers (Grahame and Cunningham; Fish et al, 2002; Golden et al, 2017), the PLmPFC is a region of interest for identifying the physiological correlates of pathological aggression following alcohol consumption. Based on this evidence, we postulate that a subset of outbred mice that is sensitive to the pro-aggressive effects of alcohol, memantine and ketamine will overexpress GluN2D in the mPFC, and that NMDAR channel blockade within the PLmPFC will escalate their aggressive behavior.
Here, we report that memantine, infused directly into the PLmPFC, but not the ILmPFC escalated aggression in alcohol-heightened aggressors (AHAs) and interacted with ethanol to heighten aggression in animals that were normally insensitive to the pro-aggressive effects of alcohol (ie alcohol non-heightened aggressors; ANAs). In addition, we report higher mPFC expression of the NMDAR GluN2D subunit in AHAs as compared to ANAs. This molecular difference was associated with a behaviorally distinct pattern of aggression. Most male mice engaged in species-typical aggression, directing their attack bites to the posterior back of a submissive conspecific. In contrast, after consuming a moderate dose of alcohol, AHAs attacked the more vulnerable anterior back and ventrum of a submissive male. This is the first evidence showing that alcohol can elicit a pattern of pathological and maladaptive social behavior in a subset of mice, and to suggest that this behavioral pattern may be associated with the dysregulation of excitatory signaling in the prelimbic mPFC.
Materials and methods
Animals
Eight-week-old resident male and female Swiss-derived mice (CFW mice; Charles River Laboratories, Wilmington, MA, USA) were housed in breeding pairs in clear polycarbonate cages (28 × 17 × 14 cm) lined with pine shavings. Intruder CFW males were group-housed in large polycarbonate cages (46 × 24 × 16 cm; n=10/cage) with corn cob bedding. Mice were cared for according to the NIH Guide for the Care and Use of Laboratory Animals (National Research Council, 2011) and procedures were approved by the Institutional Animal Care and Use Committee (IACUC) of Tufts University (see Supplementary Methods and Materials).
Alcohol Self-Administration Protocol and Resident–Intruder Aggression
Following a 1-week habituation period, residents were restricted to 3 h of daily water access, Monday–Friday, and were trained to self-administer 1.0 g/kg of 6% EtOH (w/v), diluted from 95% ethyl alcohol (Pharmco-AAPER; see Supplementary Methods and Materials). Self-administration sessions were terminated once mice consumed their final reward, drinking a total of 1 g/kg of 6% ethanol. All mice consistently self-administered ethanol or water in under 5 min.
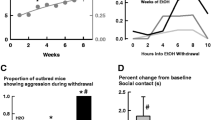
Males and females were housed for at least 3 weeks (ie until the first litter was born) prior to the males’ first session of resident–intruder aggression. Litters were consistently weaned between post-natal days 14 and 21 to prevent overcrowding. To screen resident males for aggression, the female and pups were removed and an intruder male was introduced to the resident’s home cage. Attack bites inflicted by the resident were recorded for 5 min following the initial attack (Miczek and O'Donnell, 1978). The session ended if no bites occurred within 5 min. Rarely, an intruder mouse would demonstrate defensive aggression toward a resident. In such cases, the intruder was promptly removed and replaced with a different, non-aggressive intruder. Resident–intruder confrontations occurred Mondays, Wednesdays, and Fridays, and each resident was paired with a consistent, familiar intruder. Attack bite frequencies stabilized after 6–8 interactions with <20% variability between three consecutive confrontations (Figure 1a).
Behavioral and molecular characterization of alcohol-heightened aggressors (AHAs). (a) Aggressive male residents were assessed for aggression toward submissive intruders and characterization began after attack bite frequencies stabilized. Residents that consumed 1.0 g/kg of 6% EtOH (w/v) and expressed an average bite frequency that was ⩾2 SD higher than their average baseline attack bite frequency were identified as alcohol-heightened aggressors (AHAs; n=7); males that were not sensitive to alcohol’s pro-aggressive effects were characterized as ANAs (n=8). Data are shown as group mean±SEM. Attack bite topography of (b) ANAs and (c) AHAs was assessed after water intake and after 1.0 g/kg EtOH intake. AHAs increased the number of attacks to the more vulnerable, anterior back after consuming alcohol as compared to ANAs. Alcohol increased the total number of bites comprising the initial bout and bites to the ventrum. The proportion of bites to the posterior back, anterior back, ventrum and head during the initial aggressive bout are illustrated in pie charts. The frequency of attacks to each location is tabulated below, showing average attack bites for each bite target±SEM for ANAs and AHAs; a indicates a main effect of alcohol; for interactions, *p<0.05 indicates statistical significance between AHAs and ANAs, and #p<0.05 indicates statistical significance between EtOH and H2O. Western blot analysis of NMDA receptor subunits revealed an increase in (f) GluN2D expression in the medial prefrontal cortex (mPFC) of AHAs compared to ANAs (n=6–8/phenotype group; *p=0.03) while there was no difference in PFC (d) GluN1 or (e) GluN2B. Data are shown as group mean±SEM.
Experiment 1: Behavioral and molecular characterization of alcohol-heightened aggressors
Resident males were evaluated for aggression 10 min after self-administering water or EtOH. Aggressive phenotypes were determined after six fluid self-administration and aggression assessments which were conducted every 48 h, alternating between water and EtOH self-administration (Figure 1a). Residents that consumed alcohol and expressed an average bite frequency that was ⩾2SD higher than their average baseline attack bite frequency were characterized as AHAs (Miczek et al, 1998). Resident males that were insensitive to alcohol’s pro-aggressive effects were characterized as ANAs.
AHA and ANA males were used to assess phenotype-dependent differences in attack bite topography. The initial aggressive bout was recorded under white light using a high-frame-rate digital camera (240 fps, Canon PowerShot ELPH 320 HS). Recordings were later analyzed frame-by-frame to identify where each bite was inflicted on the intruder’s body: the anterior back, posterior back, ventrum, or head (Blanchard et al, 1979). The first aggressive bout was operationally defined as the initial flurry of bites, separated from the second flurry by ≥10 s. Each animal was videotaped once after water self-administration and once after EtOH self-administration.
To evaluate NMDAR subunit protein expression, separate groups of AHA and ANA males were rapidly decapitated 1 week after their final aggressive encounter. Brains were removed and washed in ice-cold 1 × phosphate-buffered saline. The PFC, hypothalamus, thalamus, striatum, and hippocampus were dissected and flash frozen in liquid nitrogen (see Supplementary Methods and Materials). Twenty micrograms of protein were mixed with sample buffer and loaded into each lane for SDS-PAGE (6%). Protein was transferred to nitrocellulose membranes (Bio-Rad Laboratories, Hercules, CA) which were blocked for 1 h in TBS-T+5% skim milk, then incubated for an hour with primary antibodies against GluN1, GluN2A, GluN2B (BD Biosciences, San Jose, CA), GluN2D (Millipore, Billerica, MA), or tubulin (Sigma-Aldrich, St. Louis, MO). Membranes were probed with HRP-conjugated secondary antibodies and visualized by Pierce ECL (ThermoFisher Scientific, Waltham, MA) using the CCD based FujiFilm LAS 3000 system. Optical densities were quantified using the NIH ImageJ software.
Experiment 2: Alcohol, NMDAR antagonism and aggression
AHAs and ANAs were assigned to either the ketamine or memantine treatment group. On test days, mice self-administered water or EtOH, and received an intraperitoneal (i.p.) injection of ketamine (VedCo Inc.; 0.9% NaCl, 1.0–30.0 mg/kg) or memantine (Sigma-Aldrich; dH2O, 1.0–30.0 mg/kg) in a volume of 10 ml per kg of body weight. Residents were injected promptly after delivery of their final fluid reward and were tested for aggression 10 or 20 min following ketamine or memantine administration, respectively. Drug doses were given in a partially randomized order with the highest doses given last. Each subject was tested twice at each drug dose, once following water intake and once after EtOH intake. After receiving all doses, blood was collected from the residents’ submandibular vein 10 min after EtOH (1.0 g/kg) self-administration. Samples were centrifuged and blood plasma EtOH concentrations (BECs) were determined using the Analox Instruments AM1 Alcohol Analyzer (Analox Instruments Ltd., UK).
Experiment 3: Alcohol, intra-mPFC NMDAR antagonism and aggression
Following characterization, additional resident males were prepared for memantine microinfusions into the PLmPFC and ILmPFC (see Supplementary Methods and Materials). On drug testing days, obdurators were removed and mice self-administered water or EtOH. Three minutes after receiving their final fluid reward, a 33G microinjector (PlasticsOne) was inserted into the cannula. Microinjectors, extending 1 or 2 mm past the tip of the guide cannula for intra-PLmPFC or intra-ILmPFC infusions, respectively, were connected to polyethylene tubing (Intramedic PE-50) attached to a CMA/100 microinjection pump (CMA Microdialysis AB, Holliston, MA). Vehicle (aCSF) or memantine (3.75 or 7.5 μg) was microinjected into the mPFC in a volume of 0.3 μl at a rate of 0.1 μl/minute while the mouse moved freely in its home cage. Memantine doses were selected based on published microinfusion data (Eisenhardt et al, 2015) and a pilot study. Following the 3-min infusion, the microinjector remained in place for 2 min to allow the vehicle or drug solution to diffuse into the surrounding tissue.
The intruder was introduced to the resident’s home cage 10 min after the final fluid reward (ie 2 min after microinjector removal). The obdurator was placed back into the cannula after the 5-min aggressive confrontation. Each resident received 6–8 microinjections in a counterbalanced order into the PLmPFC via microinjectors projecting 1 mm past the tip of the guide cannula. One week after the final intra-PLmPFC infusion, all mice received 6–8 counterbalanced microinjections into the ILmPFC via microinjectors projecting 2 mm past the cannula tip. Following transcardial perfusion, cannula placements were verified microscopically following cresyl violet staining (Figure 2).
Histological verification of cannula placements in the right infralimbic medial prefrontal cortex (mPFC). Photomicrographs from a representative placement verified after cresyl violet staining (right) adjacent to atlas images with distance from bregma (Paxinos and Franklin, 2001). Solid lines depict verified placements in the infralimbic mPFC. One alcohol non-heightened aggressor was excluded due to a cannula placement outside of the mPFC (dashed line). Mice received infusions of memantine first into the right prelimbic mPFC via microinjectors projecting 1 mm past the end of the cannula, and subsequently, into the right infralimbic mPFC via microinjectors with a 2 mm projection.
For experiments 2 and 3, resident–intruder confrontations were videotaped under red light using a JVC Everio GZ-MG670 and analyzed by a trained researcher (intra-observed reliability: r>0.95) using The Observer XT software (Noldus, v. 9.0.436; Wageningen, the Netherlands). The frequency of attack bites, sideways threats, and tail rattles along with the duration of rearing, walking, grooming, and allogrooming (ie grooming of the intruder by the resident) was coded by key presses on a custom-made keyboard.
Statistical Analyses
The number of bites directed at the anterior back, posterior back, ventrum, and head was calculated for AHAs and ANAs that self-administered EtOH or water prior to aggressive confrontations. Bite frequencies were analyzed by two-way repeated-measures analyses of variance (two-way RM ANOVA; fluid × phenotype) and Holm–Sidak post-hoc comparisons were used in the case of significant interactions or main effects.
Western blot data were normalized by dividing the NMDAR subunit by the tubulin optical density. Two-tailed unpaired t-tests compared between AHA and ANA protein expression and were conducted for brain regions and subunits for which there were no directional a priori hypotheses. For the PFC, we hypothesized that AHAs would have elevated levels of GluN2B and GluN2D expression as compared with ANAs, warranting one-tailed t-tests.
For NMDAR antagonism studies, aggressive behaviors including the frequency of attack bites, sideways threats, and tail rattles as well as the duration of non-aggressive behaviors including walking, rearing, grooming, and allogrooming were analyzed within aggressive phenotype with two-way RM ANOVA (fluid × drug). A square root transform of the raw frequency or duration data was applied in cases when parametric assumptions were not met. To identify behaviors that were associated with alcohol-heightened or alcohol non-heightened aggression, one-way RM ANOVA or RM ANOVA on Ranks were conducted on vehicle data (phenotype × fluid). Attack bite data were transformed to percent change from vehicle baseline within the EtOH and water conditions and two-way RM ANOVA detected significant interactions and main effects within phenotype (fluid × drug). In the presence of a significant interaction or main effect, Holm–Sidak post-hoc comparisons were performed to detect differences between factor levels (H2O vs EtOH; vehicle vs drug dose). Two-way ANOVA was used to assess BECs in AHAs vs ANAs after EtOH self-administration. α was set at 0.05 for all analyses.
Results
Experiment 1: Behavioral and Molecular Characterization of Alcohol-Heightened Aggressors
In a subset of mice identified as AHAs (n=7), EtOH self-administration increased the frequency of attack bites (EtOH: M=40.6±4.7) as compared to the frequency of bites after water intake (H2O: M=20.5±2.3). In contrast, ANAs (n=8) were not sensitive to the pro-aggressive effects of 1.0 g/kg of alcohol (EtOH: M=22.3±3.2; H2O: M=23.2±3.5; Figure 1a). Slow-motion video footage was analyzed frame-by-frame to determine the target of each attack bite during the first aggressive bout after water or EtOH self-administration. After consuming water, both AHA and ANA residents showed species-typical attacks with bites mainly directed at an intruder's posterior back (Blanchard et al, 1979); however, after consuming 1.0 g/kg alcohol, AHAs inflicted significantly more bites to the anterior back (fluid × phenotype; [F(1,13)=5.04, p=0.043]; Figure 1b). Regardless of phenotype, alcohol increased the frequency of attacks made to the ventrum [F(1,13)=12.9, p=0.003] and the total number of bites comprising the first aggressive bout ([F(1,13)=5.33, p=0.038]; Figure 1b and c). BECs were not significantly different in AHAs (M=83.4±6 mg/dl) vs ANAs (M=80.9±6.1 mg/dl) 10 min after 1.0 g/kg EtOH self-administration.
Unpaired one-tailed t-test revealed elevated levels of GluN2D in the prefrontal cortex (PFC) of AHAs as compared to ANAs ([t(10)=2.07, p=0.03]; Figure 1f). There were no significant differences between AHA and ANA expression of GluN1 or GluN2B in the striatum, hippocampus, PFC (Figure 1d and e), hypothalamus or thalamus or of GluN2D in the striatum, hippocampus, or hypothalamus (Supplementary Table S1). Likewise, there were no significant differences between AHA and ANA expression of GluN2A in the striatum, hippocampus, or PFC (Supplementary Table S1).
Experiments 2 and 3: Effects of NMDAR Channel Blockers in Alcohol-Heightened and Alcohol Non-Heightened Aggressors
Alcohol-heightened aggressors: Low doses of ketamine and memantine escalate aggression
Compared to vehicle, low doses of ketamine (3–10 mg/kg) produced a twofold increase in attack bites inflicted by AHAs. In contrast, the highest dose of ketamine (30 mg/kg) had an anti-aggressive effect (drug: [F(5,45)=13.74, p<0.001]; Figure 3a). Consuming 1.0 g/kg EtOH blocked the pro-aggressive effect of low-dose ketamine without altering the serenic effect of the higher dose (fluid: [F(1,9)=42.43, p<0.001]; fluid × drug: [F(5,45)=3.58, p=0.008]; Figure 3a). Ketamine (30 mg/kg) reduced the frequency of attack bites [(F(5,45)=16.36, p<0.001], sideways threats [F(5,45)=6.29, p<0.001], and tail rattles [F(5,45)=16.81, p<0.001] without reducing the duration of walking, rearing, self-grooming or allogrooming, suggesting that, in the subanesthetic range, a higher dose of ketamine can have a selective, anti-aggressive effect (Supplementary Table S2). Ketamine (30 mg/kg) increased the duration of rearing after EtOH compared to water intake, though this behavior was often uncoordinated [F(5,45)=3.40, p=0.011].
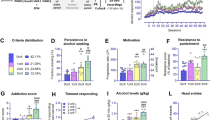
Aggression after alcohol or water intake and systemic NMDAR antagonist treatments. (a–d) Bar graphs depict baseline attack bite frequencies after 1.0 g/kg alcohol or water self-administration and vehicle injections. Alcohol-heightened aggressors (AHAs; left panels) attacked a submissive intruder more frequently after receiving a vehicle injection and consuming alcohol compared to water. Scatter plots display the percent change from baseline attack bite frequencies. In AHAs, low doses of (a) ketamine (n=10) or (c) memantine (n=8) escalated aggression; prior alcohol self-administration blocked these pro-aggressive effects. In alcohol non-heightened aggressors (ANAs; right panels), (b) ketamine (n=12) reduced aggression while (d) memantine (n=9) had a pro-aggressive effect when administered after alcohol self-administration. Higher doses of memantine and ketamine reduced aggression in (a,c) AHAs and (b,d) ANAs. Data are shown as mean±SEM; *p<0.05, **p<0.01 indicate statistical significance between vehicle and drug dose; #p<0.05, ##p<0.01 indicate statistical significance between H2O and EtOH.
Like ketamine, memantine (1–10 mg/kg) doubled the number of attack bites as compared to species-typical baseline levels (drug: [F(4,28)=7.29, p<0.001]; Figure 3c). This pro-aggressive effect was blocked by alcohol self-administration (fluid: [F(1,7)=12.37, p=0.01]; fluid × drug: [F(4,28)=3.12, p=0.031]; Figure 3c). In the absence of alcohol, low-dose memantine increased attack bites [F(4,28)=4.45, p=0.007] and sideways threats [F(4,28)=2.98, p=0.036] while reducing the duration of self-grooming [F(4,28)=2.87, p=0.041] (Supplementary Table S3). In contrast, the highest dose of memantine (30.0 mg/kg) reduced the number of attack bites [F(4,28)=9.23, p<0.001], sideways threats [F(4,28)=6.30, p<0.001], tail rattles [F(4,28)=9.82, p<0.001], and the duration of self-grooming [F(4,28)=8.40, p<0.001], while increasing allogrooming ([F(4,28)=4.49, p=0.006]; Supplementary Table S3).
When injected directly into the PLmPFC, memantine engendered a twofold escalation from baseline levels of aggression; this enhancement was absent when alcohol intake preceded memantine microinfusion (fluid × drug: [F(2, 12)=4.85, p=0.029]; fluid: [F(1,6)=27.20, p=0.002]; drug: [F(2,12)=4.72, p=0.031]; Figure 4a). In AHAs, memantine in the absence of alcohol increased the frequency of attacks [F(2,12)=5.45, p=0.021], and produced a trend toward increased sideways threats (p=0.054) without affecting the frequency of tail rattles, or the duration of walking, rearing, grooming, or allogrooming (Supplementary Table S4). In contrast, when infused into the ILmPFC, memantine had no detectable effect on aggressive or non-aggressive behaviors (Figure 4c, Supplementary Table S5).
Aggression after alcohol or water intake and intra-infralimbic or prelimbic mPFC memantine. Mice received intra-prelimbic (PLmPFC) and intra-infralimbic (ILmPFC) medial prefrontal cortical infusions of memantine after water or 1.0 g/kg alcohol self-administration. (a–d) Bar graphs depict baseline attack bite frequencies after alcohol or water self-administration and vehicle injections; scatter plots display the percent change from these baseline frequencies. Alcohol-heightened aggressors (AHAs; n=7; left panels) attacked a submissive intruder more frequently after receiving aCSF and consuming alcohol compared to water. In AHAs, memantine infused into the (a) PLmPFC, but not the (c) ILmPFC, escalated aggression. The pro-aggressive effect of intra-PLmPFC memantine was prevented when infusions were preceded by alcohol self-administration. In alcohol non-heightened aggressors (ANAs; n=9; right panels), (b) intra-PLmPFC memantine increased aggression when administered after alcohol consumption while (d) intra-ILmPFC memantine reduced the number of attack bites compared to baseline. Data are shown as mean±SEM; *p<0.05, **p<0.01 indicate statistical significance between vehicle and drug dose; #p<0.05, ##p<0.01 indicate statistical significance between H2O and EtOH.
Following vehicle treatment, AHAs had significantly higher attack bite frequencies after alcohol as compared to water intake, indicating that the aggressive phenotype remained consistent throughout systemic ketamine ([χ2(1)=10.0], p=0.002]; Figure 3a) and systemic memantine ([F(1,7)=15.26, p=0.006]; Figure 3c), intra-PLmPFC memantine ([χ2(1)=7.0, p=0.016]; Figure 4a) and intra-IL memantine ([F(1,6)=8.79, p=0.025]; Figure 4c) behavioral pharmacology experiments. All randomized memantine microinfusion doses were administered into the PLmPFC first, and then into the ILmPFC. Analyses of vehicle attack bite data with microinfusion order as a covariate revealed no interaction between fluid consumed (EtOH vs H2O) or injection site (PLmPFC vs ILmPFC) and order. This indicates that the initial 6–8 infusions into the PLmPFC did not disrupt alcohol-heightened aggression during the subsequent 6–8 aggressive encounters preceded by intra-ILmPFC infusions, and that aggression was similar following intra-PLmPFC (M=16.59±8.44) and intra-ILmPFC (M=16.07±6.59) vehicle infusions. Compared to water, alcohol also elicited a greater number of sideways threats in vehicle-treated AHAs during ketamine [χ2(1)=6.4, p=0.021] and memantine (ip.;[F(1,7)=18.90, p=0.003]; PLmPFC: [F(1,6)=7.80, p=0.031]) experiments (Supplementary Tables S2–S4).
Alcohol non-heightened aggressors: Divergent effects of ketamine and memantine
In ANAs, low-dose ketamine (3.0 mg/kg) diminished aggression. This effect was absent when alcohol intake preceded ketamine administration (fluid × drug: [F(5,55)=3.58, p=0.007]; Figure 3b). As in the AHAs, the highest dose of ketamine (30 mg/kg) reduced attack bites [F(5,55)=30.45, p<0.001], sideways threats [F(5,55)=21.62, p<0.001], and tail rattles [F(5,55)=7.85, p<0.001] in ANAs. Though drug administration did not reduce walking, rearing, or allogrooming, the highest dose of ketamine (30 mg/kg) decreased the amount of time that ANAs spent self-grooming ([F(5,55)=4.34, p=0.002]; Supplementary Table S2). Rodents may self-groom in order to thermoregulate (Spruijt et al, 1992); therefore, reduced self-grooming may reflect a more stable body temperature due to diminished aggression.
Reduced self-grooming was accompanied by an increase in allogrooming after ANAs received the highest dose of ketamine (30 mg/kg; drug: [F(5,55)=8.02, p<0.001]; Supplementary Table S2), indicating that, rather than inducing social avoidance, ketamine may increase the duration of time spent in pro-social interactions while decreasing agonistic behaviors. In addition, alcohol appears to shift the ketamine dose–effect curve leftward for allogrooming. Consuming alcohol prior to ketamine (17.0 mg/kg) increased the duration of allogrooming, producing durations similar to those observed after high-dose ketamine in the absence of alcohol (fluid × drug: [F(5,55)=2.94, p=0.02]; Supplementary Table S2). As observed previously (Newman et al, 2012), ketamine (17.0 mg/kg) can increase walking [F(5,55)=2.71, p=0.03]; however, this effect was not apparent at doses that reduced aggression, suggesting a specific serenic effect of high-dose ketamine (30 mg/kg).
Alcohol intake, followed by memantine treatment (3–10 mg/kg, i.p.) escalated the percent of baseline aggressive attacks by ANAs (fluid × drug: [F(4,32)=3.06, p=0.031]; fluid: [F(1,8)=10.49, p=0.012]; drug: [F(4,32)=7.69, p<0.001]; Figure 3d). Likewise, alcohol and low-dose memantine interacted to increase attack bites [F(4,32)=2.99, p=0.033] and sideways threats [F(4, 32)=5.36, p=0.002] (Supplementary Table S3). Like ketamine, a moderate dose of memantine increased walking in ANAs [F(4,32)=2.78, p=0.044]. In contrast, high-dose memantine (30.0 mg/kg) significantly reduced attack bites [F(4,32)=11.92, p<0.001], tail rattles [F(4,32)=18.21, p<0.001], and self-grooming [F(4,32)=9.82, p<0.001], while increasing allogrooming [F(4,32)=5.76, p=0.001] (Supplementary Table S3).
Infused directly into the PLmPFC of ANAs, memantine (3.75, 7.5 μg) interacted with alcohol to escalate aggression compared to baseline (fluid × drug: [F(2,16)=7.49, p=0.005]; fluid: [F(1,8)=56.25, p<0.001]; Figure 4b). Likewise, memantine escalated the frequency of attack bites after alcohol (fluid × drug: [F(2,16)=7.55, p=0.005]; fluid: [F(1,8)=5.58, p=0.046]), and produced a trend of increased sideways threats (p=0.06) (Supplementary Table S4). This increase in attack bite frequency occurred in the absence of any significant changes in locomotor behavior, self-grooming or allogrooming. In contrast, intra-ILmPFC, memantine (3.75 μg) reduced aggression after water or alcohol intake while the higher dose only reduced aggression following water consumption (fluid × drug: [F(2,16)=3.65, p=0.049]; drug: [F(2,16)=5.62, p=0.014]; Figure 4d). Intra- ILmPFC memantine also reduced attack bites [F(2,16)=8.98, p=0.002], sideways threats [F(2,16)=9.59, p=0.002], tail rattles [F(2,16)=4.3, p=0.032] and walking [F(2,16)=9.99, p=0.002] (Supplementary Table S5). Analyses of vehicle attack bite data conducted with order of infusion as a covariate revealed no significant interaction between fluid (EtOH vs H2O) or injection site (PLmPFC vs ILmPFC) and order, indicating that aggression following randomized vehicle infusions into the PLmPFC (M=16.83±7.88) did not affect later aggression preceded by randomized vehicle infusions into the ILmPFC (M=16.94±6.57).
Discussion
Though most people who consume alcohol do not become violent, a subset of individuals is prone to the pro-aggressive effects of moderate doses of alcohol. We identified a similar subset of mice, and characterized their aggression using qualitative and quantitative techniques (Blanchard et al, 1979; Miczek et al, 1998). These AHAs attacked a submissive intruder more frequently and with more potentially injurious bites after drinking alcohol. While alcohol increased the amount of aggression during the first bout regardless of phenotype, only AHAs accumulated a greater number of total bites during a complete, 5-min encounter, suggesting that AHAs may exhibit pathological persistence in their aggressive behavior after consuming alcohol. Conversely, aggression preceded by water intake was maintained at a species-typical level in AHAs.
Because alcohol can block NMDAR-mediated excitatory currents (Lovinger et al, 1989), we hypothesized that altered NMDAR function or expression may promote alcohol-heightened aggression. To address this, aggressive males consumed water or alcohol (1.0 g/kg) and were injected with an uncompetitive NMDAR antagonist before encountering a submissive intruder. This revealed a phenotype-dependent effect, with AHAs showing considerably more aggression following water intake and treatment with low-to-moderate doses of memantine or ketamine and reduced aggression when memantine or ketamine treatment was preceded by alcohol intake. This suggests that, at moderate doses, memantine and ketamine may compete with alcohol for a site of action on the NMDAR, and that this site could serve as a molecular basis for alcohol-heightened aggression.
The behavioral effects of systemically administered memantine and ketamine were dependent on aggressive phenotype. Interestingly, ketamine, but not memantine, can disinhibit brain-derived neurotrophic factor (BDNF) synthesis (Gideons et al, 2014). In humans, mutations in the BDNF gene have been associated with reduced BDNF signaling and increased impulsive aggression (Wagner et al, 2010) while a BDNF knockdown in mice escalates alcohol drinking, increases agonistic behavior, and reduces 5-HT1A receptor functioning (Lyons et al, 1999; Hensler et al, 2003; Maynard et al, 2016). Because AHAs have reduced 5-HT1A mRNA expression in the mPFC (Chiavegatto et al, 2010), future work must investigate whether these mice also have deficits in BDNF or its receptor, tropomyocin receptor kinase B (TrkB; Adachi et al, 2017). The pro-aggressive effect of ketamine observed in AHAs, but not in ANAs, may reflect dysregulated BDNF/TrkB or 5-HT/5-HT1A signaling in this subset of mice.
Memantine preferentially acts on GluN2C- or GluN2D-containing NMDARs and diminishes prefrontal cortical activity in rats, prompting our hypothesis that AHAs would express higher levels of GluN2D in the PFC as compared with ANAs (Monyer et al, 1994; Standaert et al, 1996; Sekar et al, 2013; Riebe et al, 2016; Sapkota et al, 2016). Protein quantification supported this hypothesis and identified overexpression of GluN2D in the PFC of AHAs without increased GluN1, suggesting a greater proportion of GluN2D-containing receptors rather than an overall increase in NMDARs. Despite the apparent role for GluN2B in ethanol’s antagonism of NMDAR-mediated currents (Fink and Gothert, 1996; Wills et al, 2012), we did not find any differences in GluN2B expression in AHAs vs ANAs. However, we must note that, due to the correlational nature of our western blotting data, GluN2D overexpression could either be a result of alcohol-heightened aggression or a molecular phenotype predictive of alcohol-heightened aggression.
To determine if systemic memantine treatments escalated aggression by acting on prefrontal cortical receptor populations, we infused memantine directly into the prefrontal cortex. Mirroring our findings with systemic administration, infusions of memantine into the PLmPFC, but not the ILmPFC escalated aggression in AHAs. By blocking GluN2D-containing NMDARs expressed on cortical PVIs, memantine may disinhibit mPFC pyramidal cells to promote glutamate release in subcortical brain areas (Jackson et al, 2004; Homayoun and Moghaddam, 2007; Gupta et al, 2016; Sapkota et al, 2016; Povysheva and Johnson, 2016). A subset of layer V prelimbic neurons innervates GABAergic interneurons in the dorsal raphé nucleus (DRN) that synapse onto serotonergic (5-HTergic) cells to modulate 5-HT output (Celada et al, 2001; Vertes, 2004; Challis and Berton, 2015). Memantine, infused directly into the PLmPFC, could disinhibit excitatory cells that innervate local inhibitory neurons in the DRN; a resultant reduction in 5-HT release could promote heightened aggression, specifically in AHAs (Davidson et al, 2000; Shearman et al, 2006; Heinz et al, 2011). To further characterize the functional implications of intra-mPFC GluN2D NMDAR overexpression in AHAs, immunohistochemistry experiments should focus on cell type specific receptor expression.
PV-interneuron dysfunction has been suggested in disorders that are commonly associated with social deficits and aggression, including autism spectrum disorder and schizophrenia (Saunders et al, 2013; Matson and Adams, 2014; Bicks et al, 2015; Thelin et al, 2017). In vivo, inclusion of the GluN2D subunit in NMDARs confers a weak Mg+ block and slow deactivation (Monyer et al, 1994). In combination with their extrasynaptic expression pattern, these features suggest that GluN2D-containing NMDARs play a vital role in detecting glutamate spillover and in engaging negative feedback to reduce glutamatergic transmission by pyramidal neurons (Perszyk et al, 2016; Povysheva and Johnson, 2016; Riebe et al, 2016; Dubois et al, 2016). In mice, NMDAR channel blockade can increase pyramidal cell firing rate and decrease delta network oscillations, suggesting long-distance desynchronization of thalamocortical inputs (Kargieman et al, 2007). Thus, memantine and ketamine may disrupt the integration of sensory inputs by mPFC microcircuits to compromise signaling of non-threatening stimuli and facilitate aggressive responding (Davidson et al, 2000).
Alcohol, memantine, and ketamine all have biphasic dose–effect curves, and because each of these compounds has effects on NMDARs, drug combinations appear to have complex additive effects on aggressive and non-aggressive behaviors. In addition, these curves appear phenotype-dependent, meaning that AHAs and ANAs have varying sensitivities to these drugs and to the interactions between them. We postulate that overexpression of GluN2D-NMDARs in AHAs might provide memantine with a greater proportion of preferred sites of action on parvalbumin interneurons. This increase in cell-type-specific sites could augment memantine’s capacity to inhibit parvalbumin interneurons and, consequently, to disinhibit the pyramidal cells that are innervated by these interneurons. Alcohol, ketamine, and memantine may each independently increase aggression in AHAs by producing functionally similar effects on parvalbumin interneurons, perhaps through inhibition of GluN2D-NMDAR-mediated currents. If so, alcohol pre-treatment may encourage ketamine or memantine either to act on non-preferred GluN2A- or GluN2B-NMDARs localized on interneurons and pyramidal cells or to act on off-target sites such as dopamine or nicotinic acetylcholine receptors (Aracava et al, 2005; Seeman et al, 2008). When NMDAR channel blockers are administered to AHAs following alcohol intake, their non-specific inhibition of NMDARs on interneurons and pyramidal cells could promote excitation/inhibition balance to prevent escalated aggression. We also observed that high doses of ketamine or memantine reduced aggression without reducing walking, rearing or allogrooming. This behaviorally specific, anti-aggressive effect may similarly result from antagonism of NMDARs in a non-cell-type-specific fashion or through off-target effects.
To understand the mechanisms underlying the observed interactions between alcohol and NMDAR channel blockers, future electrophysiology experiments must examine alcohol’s effects on PVIs in the presence and absence of memantine or ketamine in PFC slices from AHAs and ANAs. In behaving animals, short hairpin RNA used to knock down GluN2D in the mPFC could be used in conjunction with in vivo electrophysiology to establish the precise role of GluN2D-NMDARs in the disinhibition of pyramidal cells and in the escalation of aggression.
In the present work, we identified a subset of outbred mice that became highly aggressive after drinking a moderate dose of alcohol. These AHAs were distinguished from ANAs in that: (1) AHAs escalated both the number and the severity of their attacks toward a submissive intruder after consuming alcohol; (2) AHAs overexpressed the NMDAR subunit, GluN2D, in the PFC; and (3) AHAs were sensitive to the pro-aggressive effects of self-administered alcohol, systemically administered ketamine and memantine, and memantine that was infused directly into the PLmPFC. These findings suggest that alcohol-heightened aggression may involve dysregulated glutamatergic signaling via GluN2D-containing NMDARs expressed on interneurons in the mPFC of AHAs. In these mice, alcohol or NMDAR channel blockers may impede effective signal integration within the PFC and may functionally disinhibit signaling to subcortical, aggression-promoting brain regions. Recently developed, positive allosteric modulators that preferentially act on GluN2C- or GluN2D-containing NMDARs must be tested for their ability to reduce or block alcohol-heightened aggression in mice (Mullasseril et al, 2010; Perszyk et al, 2016). Such compounds will provide further insight into the mechanisms underlying alcohol-heightened aggression and may be of use in reducing the impact of alcohol-related violence in the human population.
Funding and disclosure
Research reported in this publication was supported by the National Institute on Alcohol Abuse and Alcoholism and the National Institute of Mental Health of the National Institutes of Health under award numbers R01AA013983 (KAM), F31AA025827 (ELN) and R01MH097446 (SJM). The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The authors declare no conflict of interest.
References
Adachi M, Autry AE, Mahgoub M, Suzuki K, Monteggia LM (2017). TrkB signaling in dorsal raphe nucleus is essential for antidepressant efficacy and normal aggression behavior. Neuropsychopharmacology 42: 886–894.
Aracava Y, Pereira EF, Maelicke A, Albuquerque EX (2005). Memantine blocks α7* nicotinic acetylcholine receptors more potently than N-methyl-D-aspartate receptors in rat hippocampal neurons. J Pharmacol Exp Ther 312: 1195–1205.
Becker A, Grecksch G (2004). Ketamine-induced changes in rat behaviour: a possible animal model of schizophrenia. Test of predictive validity. Prog Neuropsychopharmacol Biol Psychiatry 28: 1267–1277.
Becker A, Peters B, Schroeder H, Mann T, Huether G, Grecksch G (2003). Ketamine-induced changes in rat behaviour: a possible animal model of schizophrenia. Prog Neuropsychopharmacol Biol Psychiatry 27: 687–700.
Berman RM, Cappiello A, Anand A, Oren DA, Heninger GR, Charney DS et al (2000). Antidepressant effects of ketamine in depressed patients. Biol Psychiatry 47: 351–354.
Bicks LK, Koike H, Akbarian S, Morishita H (2015). Prefrontal cortex and social cognition in mouse and man. Front Psychol 6: 1805.
Blanchard RJ, O'Donnell V, Blanchard DC (1979). Attack and defensive behaviors in the albino mouse. Aggress Behav 5: 341–352.
Celada P, Puig MV, Casanovas JM, Guillazo G, Artigas F (2001). Control of dorsal raphe serotonergic neurons by the medial prefrontal cortex: involvement of serotonin-1 A, GABAA, and glutamate receptors. J Neurosci 21: 9917–9929.
Challis C, Berton O (2015). Top-down control of serotonin systems by the prefrontal cortex: a path toward restored socioemotional function in depression. ACS Chem Neurosci 6: 1040–1054.
Cherpitel CJ (2007). Alcohol and injuries: a review of international emergency room studies since 1995. Drug Alcohol Rev 26: 201–214.
Chiavegatto S, Quadros IM, Ambar G, Miczek KA (2010). Individual vulnerability to escalated aggressive behavior by a low dose of alcohol: decreased serotonin receptor mRNA in the prefrontal cortex of male mice. Genes Brain Behav 9: 110–119.
Davidson RJ, Putnam KM, Larson CL (2000). Dysfunction in the neural circuitry of emotion regulation—a possible prelude to violence. Science 289: 591–594.
Dubois CJ, Lachamp PM, Sun L, Mishina M, Liu SJ (2016). Presynaptic GluN2D receptors detect glutamate spillover and regulate cerebellar GABA release. J Neurophysiol 115: 271–285.
Eisenhardt M, Leixner S, Lujan R, Spanagel R, Bilbao A (2015). Glutamate receptors within the mesolimbic dopamine system mediate alcohol relapse behavior. J Neurosci 35: 15523–15538.
Fink K, Gothert M (1996). Both ethanol and ifenprodil inhibit NMDA-evoked release of various neurotransmitters at different, yet proportional potency: potential relation to NMDA receptor subunit composition. Naunyn Schmiedebergs Arch Pharmacol 354: 312–319.
Fish EW, DeBold JF, Miczek KA (2002). Aggressive behavior as a reinforcer in mice: activation by allopregnanolone. Psychopharmacology 163: 459–466.
Gan G, Sterzer P, Marxen M, Zimmermann US, Smolka MN (2015). Neural and behavioral correlates of alcohol-induced aggression under provocation. Neuropsychopharmacology 40: 2886–2896.
Giancola PR (2000). Executive functioning: a conceptual framework for alcohol-related aggression. Exp Clin Psychopharmacol 8: 576–597.
Giancola PR, Moss HB, Martin CS, Kirisci L, Tarter RE (1996). Executive cognitive functioning predicts reactive aggression in boys at high risk for substance abuse: a prospective study. Alcohol Clin Exp Res 20: 740–744.
Gideons ES, Kavalali ET, Monteggia LM (2014). Mechanisms underlying differential effectiveness of memantine and ketamine in rapid antidepressant responses. Proc Natl Acad Sci USA 111: 8649–8654.
Golden SA, Heins C, Venniro M, Caprioli D, Zhang M, Epstein DH et al (2017). Compulsive addiction-like aggressive behavior in mice. Biol Psychiatry 82: 239–248.
Goodwani S, Saternos H, Alasmari F, Sari Y (2017). Metabotropic and ionotropic glutamate receptors as potential targets for the treatment of alcohol use disorder. Neurosci Biobehav Rev 77: 14–31.
Gourley SL, Taylor JR (2016). Going and stopping: dichotomies in behavioral control by the prefrontal cortex. Nat Neurosci 19: 656–664.
Grahame NJ, Cunningham CL (1997). Intravenous ethanol self-administration in C57BL/6J and DBA/2J mice. Alcohol Clin Exp Res 21: 56–62.
Gupta SC, Ravikrishnan A, Liu J, Mao Z, Pavuluri R, Hillman BG et al (2016). The NMDA receptor GluN2C subunit controls cortical excitatory-inhibitory balance, neuronal oscillations and cognitive function. Sci Rep 6: 38321.
Heinz AJ, Beck A, Meyer-Lindenberg A, Sterzer P, Heinz A (2011). Cognitive and neurobiological mechanisms of alcohol-related aggression. Nat Rev Neurosci 12: 400–413.
Hensler JG, Ladenheim EE, Lyons WE (2003). Ethanol consumption and serotonin-1 A (5-HT1A receptor function in heterozygous BDNF (+/-) mice. J Neurochem 85: 1139–1147.
Homayoun H, Moghaddam B (2007). NMDA receptor hypofunction produces opposite effects on prefrontal cortex interneurons and pyramidal neurons. J Neurosci 27: 11496–11500.
Hwa LS, Nathanson AJ, Shimamoto A, Tayeh JK, Wilens AR, Holly EN et al (2015). Aggression and increased glutamate in the mPFC during withdrawal from intermittent alcohol in outbred mice. Psychopharmacology 232: 2889–2902.
Jackson ME, Homayoun H, Moghaddam B (2004). NMDA receptor hypofunction produces concomitant firing rate potentiation and burst activity reduction in the prefrontal cortex. Proc Natl Acad Sci USA 101: 8467–8472.
Kargieman L, Santana N, Mengod G, Celada P, Artigas F (2007). Antipsychotic drugs reverse the disruption in prefrontal cortex function produced by NMDA receptor blockade with phencyclidine. Proc Natl Acad Sci USA 104: 14843–14848.
Kotermanski SE, Johnson JW (2009). Mg2+ imparts NMDA receptor subtype selectivity to the Alzheimer's drug memantine. J Neurosci 29: 2774–2779.
Krishnan-Sarin S, O'Malley SS, Franco N, Cavallo DA, Morean M, Shi J et al (2015). N-methyl-D-aspartate receptor antagonism has differential effects on alcohol craving and drinking in heavy drinkers. Alcohol Clin Exp Res 39: 300–307.
Lovinger DM, White G, Weight FF (1989). Ethanol inhibits NMDA-activated ion current in hippocampal neurons. Science 243: 1721–1724.
Lyons WE, Mamounas LA, Ricaurte GA, Coppola V, Reid SW, Bora SH et al (1999). Brain-derived neurotrophic factor-deficient mice develop aggressiveness and hyperphagia in conjunction with brain serotonergic abnormalities. Proc Natl Acad Sci USA 96: 15239–15244.
Matson JL, Adams HL (2014). Characteristics of aggression among persons with autism spectrum disorders. Res Autism Spectr Disord 8: 1578–1584.
Maynard KR, Hill JL, Calcaterra NE, Palko ME, Kardian A, Paredes D et al (2016). Functional role of BDNF production from unique promoters in aggression and serotonin signaling. Neuropsychopharmacology 41: 1943–1955.
Miczek KA, Barros HM, Sakoda L, Weerts EM (1998). Alcohol and heightened aggression in individual mice. Alcohol Clin Exp Res 22: 1698–1705.
Miczek KA, O'Donnell JM (1978). Intruder-evoked aggression in isolated and nonisolated mice: Effects of psychomotor stimulants and l-dopa. Psychopharmacology 57: 47–55.
Monyer H, Burnashev N, Laurie DJ, Sakmann B, Seeburg PH (1994). Developmental and regional expression in the rat brain and functional properties of four NMDA receptors. Neuron 12: 529–540.
Mullasseril P, Hansen KB, Vance KM, Ogden KK, Yuan H, Kurtkaya NL et al (2010). A subunit-selective potentiator of NR2C- and NR2D-containing NMDA receptors. Nat Commun 1: 90.
Nakazawa K, Zsiros V, Jiang Z, Nakao K, Kolata S, Zhang S et al (2012). GABAergic interneuron origin of schizophrenia pathophysiology. Neuropharmacology 62: 1574–1583.
National Research Council (2011) Guide for the Care and Use of Laboratory Animals 8th edn National Academy Press: Washington DC. 248pp.
Newman EL, Chu A, Bahamón B, Takahashi A, DeBold JF, Miczek KA (2012). NMDA receptor antagonism: escalation of aggressive behavior in alcohol-drinking mice. Psychopharmacology (Berl) 224: 167–177.
Paoletti P, Bellone C, Zhou Q (2013). NMDA receptor subunit diversity: impact on receptor properties, synaptic plasticity and disease. Nat Rev Neurosci 14: 383–400.
Parsons CG, Danysz W, Bartmann A, Spielmanns P, Frankiewicz T, Hesselink M et al (1999). Amino-alkyl-cyclohexanes are novel uncompetitive NMDA receptor antagonists with strong voltage-dependency and fast blocking kinetics: in vitro and in vivo characterization. Neuropharmacology 38: 85–108.
Paxinos G, Franklin KBJ (2001) The Mouse Brain in Stereotaxic Coordinates 2nd edn Academic Press: San Diego.
Perszyk RE, DiRaddo JO, Strong KL, Low CM, Ogden KK, Khatri A et al (2016). GluN2D-containing N-methyl-d-aspartate receptors mediate synaptic transmission in hippocampal interneurons and regulate interneuron activity. Mol Pharmacol 90: 689–702.
Povysheva NV, Johnson JW (2016). Effects of memantine on the excitation-inhibition balance in prefrontal cortex. Neurobiol Dis 96: 75–83.
Raine A, Dodge K, Loeber R, Gatzke-Kopp L, Lynam D, Reynolds C et al (2006). The Reactive-Proactive Aggression Questionnaire: differential correlates of reactive and proactive aggression in adolescent boys. Aggress Behav 32: 159–171.
Raine A, Meloy JR, Bihrle S, Stoddard J, LaCasse L, Buchsbaum MS (1998). Reduced prefrontal and increased subcortical brain functioning assessed using positron emission tomography in predatory and affective murderers. Behav Sci Law 16: 319–332.
Riebe I, Seth H, Culley G, Dosa Z, Radi S, Strand K et al (2016). Tonically active NMDA receptors—a signalling mechanism critical for interneuronal excitability in the CA1 stratum radiatum. Eur J Neurosci 43: 169–178.
Sapkota K, Mao Z, Synowicki P, Lieber D, Liu M, Ikezu T et al (2016). GluN2D N-methyl-d-aspartate receptor subunit contribution to the stimulation of brain activity and gamma oscillations by ketamine: implications for schizophrenia. J Pharmacol Exp Ther 356: 702–711.
Saunders JA, Tatard-Leitman VM, Suh J, Billingslea EN, Roberts TP, Siegel SJ (2013). Knockout of NMDA receptors in parvalbumin interneurons recreates autism-like phenotypes. Autism Res 6: 69–77.
Seeman P, Caruso C, Lasaga M (2008). Memantine agonist action at dopamine D2High receptors. Synapse 62: 149–153.
Sekar S, Jonckers E, Verhoye M, Willems R, Veraart J, Van AJ et al (2013). Subchronic memantine induced concurrent functional disconnectivity and altered ultra-structural tissue integrity in the rodent brain: revealed by multimodal MRI. Psychopharmacology (Berl) 227: 479–491.
Shearman E, Rossi S, Szasz B, Juranyi Z, Fallon S, Pomara N et al (2006). Changes in cerebral neurotransmitters and metabolites induced by acute donepezil and memantine administrations: a microdialysis study. Brain Res Bull 69: 204–213.
Spruijt BM, van Hooff JARA, Gispen WH (1992). Ethology and neurobiology of grooming behavior. Physiol Rev 72: 825–852.
Standaert DG, Landwehrmeyer GB, Kerner JA, Penney JB Jr., Young AB (1996). Expression of NMDAR2D glutamate receptor subunit mRNA in neurochemically identified interneurons in the rat neostriatum, neocortex and hippocampus. Brain Res Mol Brain Res 42: 89–102.
Thelin J, Halje P, Nielsen J, Didriksen M, Petersson P, Bastlund JF (2017). The translationally relevant mouse model of the 15q13.3 microdeletion syndrome reveals deficits in neuronal spike firing matching clinical neurophysiological biomarkers seen in schizophrenia. Acta Physiol 220: 124–136.
Vertes RP (2004). Differential projections of the infralimbic and prelimbic cortex in the rat. Synapse 51: 32–58.
Wagner S, Baskaya O, Dahmen N, Lieb K, Tadic A (2010). Modulatory role of the brain-derived neurotrophic factor Val66Met polymorphism on the effects of serious life events on impulsive aggression in borderline personality disorder. Genes Brain Behav 9: 97–102.
Wills TA, Klug JR, Silberman Y, Baucum AJ, Weitlauf C, Colbran RJ et al (2012). GluN2B subunit deletion reveals key role in acute and chronic ethanol sensitivity of glutamate synapses in bed nucleus of the stria terminalis. Proc Natl Acad Sci USA 109: E278–E287.
Acknowledgements
The authors would like to acknowledge Colin Burnett and Kyle Aronson for their assistance with behavioral research.
Author contributions
ELN, JFD, SJM, and KAM designed the experiments and wrote the manuscript. ELN, TLW, NH, and MBB conducted the behavioral experiments. ELN performed surgeries and dissections, ELN, TLW, and NH analyzed the behavioral data, and ELN and MT conducted western blot experiments.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on the Neuropsychopharmacology website
Supplementary information
Rights and permissions
About this article
Cite this article
Newman, E., Terunuma, M., Wang, T. et al. A Role for Prefrontal Cortical NMDA Receptors in Murine Alcohol-Heightened Aggression. Neuropsychopharmacol. 43, 1224–1234 (2018). https://doi.org/10.1038/npp.2017.253
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2017.253
- Springer Nature Switzerland AG
This article is cited by
-
Behavioral analysis of kainate receptor KO mice and the role of GluK3 subunit in anxiety
Scientific Reports (2024)
-
To fight or not to fight: activation of the mPFC during decision to engage in aggressive behavior after ethanol consumption in a novel murine model
Psychopharmacology (2022)
-
Excessive alcohol consumption after exposure to two types of chronic social stress: intermittent episodes vs. continuous exposure in C57BL/6J mice with a history of drinking
Psychopharmacology (2022)
-
Rage Against the Machine: Advancing the study of aggression ethology via machine learning.
Psychopharmacology (2020)
-
A Role for Prefrontal Cortical NMDA Receptors in Murine Alcohol-Heightened Aggression
Neuropsychopharmacology (2018)