Abstract
Monitoring changes in opioid receptor binding with positron emission tomography (PET) could lead to a better understanding of tolerance and addiction because altered opioid receptor dynamics following agonist exposure has been linked to tolerance mechanisms. We have studied changes in kappa opioid receptor (KOR) binding availability in vivo with PET following kappa opioid agonist administration. Male Sprague–Dawley rats (n=31) were anesthetized and treated with the (KOR) agonist salvinorin A (0.01–1.8 mg/kg, i.v.) before administration of the KOR selective radiotracer [11C]GR103545. When salvinorin A was administered 1 min prior to injection of the radiotracer, [11C]GR103545 binding potential (BPND) was decreased in a dose-dependent manner, indicating receptor binding competition. In addition, the unique pharmacokinetics of salvinorin A (half-life ~8 min in non-human primates) allowed us to study the residual impact on KOR after the drug had eliminated from the brain. Salvinorin A was administered up to 5 h prior to [11C]GR103545, and the changes in BPND were compared with baseline, 2.5 h, 1 h, and 1 min pretreatment times. At lower doses (0.18 mg/kg and 0.32 mg/kg) we observed no prolonged effect on KOR binding but at 0.60 mg/kg salvinorin A induced a sustained decrease in KOR binding (BPND decreased by 40–49%) which persisted up to 2.5 h post administration, long after salvinorin A had been eliminated from the brain. These data point towards an agonist-induced adaptive response by KOR, the dynamics of which have not been previously studied in vivo with PET.
Similar content being viewed by others
INTRODUCTION
The opioid receptors (ORs) belong to the superfamily of G-protein coupled receptors (GPCR) and consist of at least three main subtypes: μ, κ, δ (Lord et al, 1977; Evans et al, 1992; Kieffer et al, 1992; Chen et al, 1993; Minami et al, 1993). The kappa OR (KOR) is the most abundant OR in the human brain (Minami and Satoh, 1995; Hiller and Fan, 1996). Activation of KOR by the endogenous ligand, the peptide dynorphin, results in a variety of physiological functions such as mood modulation, pain perception, consciousness, learning and memory, motor control, and behavioral response to drugs of abuse (Shirayama et al, 2004; Schwarzer, 2009). KOR antagonists are currently being pursued as treatment for depression and mood disorders (major depressive disorder, anxiety disorder, and substance abuse disorders; for review see Carroll and Carlezon, 2013). Although KORs are potential targets for drug development, the in vivo pharmacology is not well described. New imaging tools now exist that, combined with unique KOR drugs, can provide insights into receptor ligand interactions in vivo. In this report we combined positron emission tomography (PET) imaging using [11C]GR103545 with the unique kappa agonist salvinorin A.
Salvinorin A is a natural product derived from the sage plant, Salvia Divinorum (Valdes et al, 1984). In humans, salvinorin A displays remarkable onset and potency with a short duration, producing dissociative, hallucinogenic, and memory effects (Johnson et al, 2011; MacLean et al, 2013). In 2002, the NIMH Psychoactive Drug Screening Program determined that salvinorin A is a potent full agonist at KOR with extreme selectivity (Figure 1). Unlike other hallucinogens, salvinorin A does not target serotonin-2A (Roth et al, 2002). Although salvinorin A has been well characterized in vitro, in vivo quantification methods have proven challenging (Schmidt et al., 2005; Cunningham et al, 2011) owing to the rapid metabolism and pharmacokinetics (half-life ~8 min in non-human primates (NHPs); Hooker et al, 2008). In addition, salvinorin A causes differing behavioral effects in rodents when assessed immediately following drug administration compared with a delayed testing schedule (Potter et al, 2011). In vivo imaging assessment of salvinorin A at KORs could validate its unique characteristics and clarify existing in vitro and behavioral data.
KOR agonist salvinorin A and KOR PET radiotracer [11C]GR103545 with literature-reported values for affinity and selectivity for KOR. *In vitro radioligand binding of salvinorin A (Wang et al, 2008) and GR103545 (Schoultz et al, 2010) with [3H]diprenorphine, using membranes prepared from CHO cells expressing human KOR. (Ki±SD).
PET is a non-invasive imaging modality that can monitor changes in receptor availability in vivo following endogenous or exogenous stimuli. [11C]GR103545 is a KOR selective PET tracer (Figure 1) and has been evaluated in NHPs (Talbot et al, 2005; Tomasi et al, 2013) and humans (Naganawa et al, 2014a), displaying good uptake and specific binding in kappa-dense brain regions. PET studies following salvinorin A pretreatment have not been reported and with recently validated KOR PET ligands, we sought to investigate the neurochemical profile of this ligand/receptor interaction. In vivo occupancy measurements of agonists with PET can be challenging in some GPCR systems because of agonist-induced adaptive responses by the receptor (Laruelle, 2000; Skinbjerg et al, 2010). Salvinorin A causes internalization of KORs in vitro (Wang et al, 2008; White et al, 2015) and we hoped to exploit this property, allowing us to study not only occupancy of the drug at KORs but also the prolonged receptor binding changes caused by the agonist, long after it has cleared from the brain.
The aims of this study were to (i) evaluate the kappa agonist radiotracer [11C]GR103545 in rats with PET, (ii) determine the in vivo occupancy of salvinorin A at KORs, and (iii) monitor the immediate and prolonged effects of salvinorin A on KOR binding with [11C]GR103545. To explore these goals, [11C]GR103545 binding was evaluated in rats after administration of vehicle or blocking agents such as self-blocking with GR89696 (GR103545 racemate), the OR antagonist naloxone, KOR antagonist LY2795050, and the KOR agonist salvinorin A. Secondly, to determine the occupancy of salvinorin A at KOR in vivo, we administered escalating doses of salvinorin A to rats and monitored changes in [11C]GR103545 binding potential (BPND) at KOR. Lastly, given the rapid pharmacokinetics of salvinorin A and its ability to cause internalization of KORs in vitro, we examined the dynamics of this process in vivo using a time-delayed administration of salvinorin A and PET radiotracer.
MATERIALS AND METHODS
Subjects and Drug
A total of 31 male Sprague–Dawley rats (Charles River Labs) were used for this study and imaged between 2 and 4 months of age. Animals were pair housed until they reached a weight of 500 g, and were kept on a 12 h : 12 h light:dark cycle. All treatment and imaging experiments were performed according to procedures approved by the Institutional Animal Care and Use Committee at the Massachusetts General Hospital. Salvinorin A (~98% purity) was extracted from Salvia divinorum leaves using a method previously reported (Hooker et al, 2008). (R,S)-LY2795050 (racemate) was synthesized in our laboratory by methods previously reported (Mitch et al, 2011). (−)-Naloxone hydrochloride dihydrate was obtained from Sigma-Aldrich. GR103545 precursor (normethylcarbamoyl-GR103545) and reference standard (racemate, GR89696) were obtained from ABX advanced biochemical compounds.
Radiochemistry
(R)-(-)-[11C]GR103545 was synthesized from the normethylcarbamoyl precursor via carboxylation with CO2 and methylation of the carbamic acid with [11C]MeOTf using a modified literature procedure described previously (Nabulsi et al, 2011). The crude material was purified by reverse-phase HPLC with a 9.4 × 250 mm Agilent Eclipse XDB-C18-5 μm HPLC column eluting with 30% acetonitrile/70% H2O/0.1 M ammonium formate at 5 ml/min. Non-radioactive peaks were analyzed by UV (230 nm), and retention time of [11C]GR103545 was ~9 min. The collected product was diluted with water (20 ml), captured on a Waters C18 plus sep-pak cartridge (conditioned with 1 ml ethanol followed by 10 ml water). The sep-pak was washed with water (5 ml), and the radiotracer was eluted with USP absolute ethanol (1 ml), diluted with USP sterile saline (9 ml) and passed through a sterile membrane filter (0.22 μm) to afford an injectable solution of [11C]GR103545 with an average RCY of 15.2±6.1% (end of synthesis (EOS), non-decay corrected) and specific activity of 9.5±4.8 mCi/nmol, at the EOS). Total injected mass of GR103545 (except 0.1 mg/kg self-blocking experiment) based on specific activity of [11C]GR103545 at time of injection ranged from 0.099–0.226 μg/kg. [11C]Salvinorin A was synthesized according to a method previously reported (Hooker et al, 2008).
PET
Animals were anesthetized under isoflurane (3% for induction, 2% for maintenance) with oxygen carrier. A catheter was placed in a lateral tail vein of each animal and an extension line was used to attach the catheter to a syringe. Animals received a bolus injection of either vehicle (1 : 1 : 8 DMSO : Tween80 : saline, n=5) at 5 min pretreatment, GR89696 (0.1 mg/kg, 1 : 9 ethanol : saline, n=1) at 5 min pretreatment, LY2795050 (0.32 mg/kg, 1 : 9 ethanol : saline, n=1) at 5 min pretreatment or naloxone (2 mg/kg, saline, n=1) at 10 min pretreatment prior to the radiotracer. Salvinorin A (formulated in 1 : 1 : 8 DMSO : Tween80: saline) was administered at either 1 min (0.010, 0.018, 0.032, 0.060, 0.10, 0.18, 0.32, 0.60, 1 and 1.8 mg/kg; n=1 for each dose), 60 min (0.18 mg/kg, n=2; 0.32 mg/kg, n=3; 0.60 mg/kg, n=2), 2.5 h (0.60 mg/kg, n=3), or 5 h (0.60 mg/kg, n=3) prior to injection of the radiotracer. A bolus injection of the radiotracer (~1 mCi) was then administered and animals underwent a 60 min dynamic PET scan. Animals were then scanned in one of two instruments (GammaMedica Triumph PET/CT/SPECT scanner or Siemens P4 PET scanner). For scans completed in the GammaMedica Triumph, CT images of the animals were acquired for attenuation correction during image reconstruction. For animals imaged in the P4, a transmission scan was performed with a Cobalt (57Co) line source which generated an attenuation correction map used for image reconstruction. Dynamic scan data was binned into 32 frames (8 × 15 s, 8 × 1 min, 10 × 2 min, or 6 × 5 min) and each frame was reconstructed using an iterative MLEM (maximum likelihood expectation maximization) algorithm which consists of 16 iterations and yields an image resolution of~2 mm FWHM (full width at half maximum). Final reconstructed images have a 0.26 mm in-plane resolution with a 0.6 mm slice thickness.
Image Analysis
All image processing and kinetic analysis was performed using PMOD 3.3 (PMOD Technologies, Zurich, Switzerland). All image data derived from the Triumph scanner were coregistered to the corresponding CT image and data derived from the Siemens P4 were manually aligned and coregistered to a CT image acquired from a different animal of similar age and weight. These coregistered PET/CT images were spatially aligned to the Px Rat (Schiffer et al, 2006) rat brain template with predefined VOIs (volumes of interest; Schiffer et al, 2006) for regional analysis. Image analysis was performed on each animal and both regional standardized uptake value (SUV) and BPND, a measure of specific binding with respect to nondisplaceable uptake (Innis et al, 2007), were calculated. SUV was averaged from 50 to 60 min for comparison to all blocking agents. BPND was calculated using the Logan reference analysis method (Logan et al, 1996) with the cerebellum as a reference region (t*=20 min).
RESULTS
[11C]GR103545 Dynamic PET in Rats
The baseline [11C]GR103545 time-activity curve displays high uptake of the radiotracer in the rat brain with quantifiable kinetics and fast washout in the reference region, cerebellum (Figure 2a). Figure 2 displays only a subset of regions for clarity purposes but the Supplementary Table contains a thorough list of regional uptake values. Highest uptake at later time points was observed in the hypothalamus followed by periaqueductal gray, ventral tegmental area, midbrain and nucleus accumbens. Intermediate uptake was observed in the amygdala followed by insular cortex, olfactory tubercle, caudate putamen, superior colliculus, and thalamus. Lower uptake was observed in the hippocampus, frontal cortex, cingulate cortex, motor cortex, and lowest uptake was observed in the cerebellum. Administration of GR89696 (GR103545 racemate; 0.1 mg/kg, i.v.) 5 min prior to radiotracer injection resulted in significantly lower uptake in kappa-dense regions (60±5% average SUV decrease in nucleus accumbens, amygdala, caudate putamen, olfactory tubercle, midbrain, and thalamus) indicating saturable binding (Figure 2b). Administration of the opioid antagonist naloxone (2 mg/kg, i.v.) 10 min prior to radiotracer injection resulted in complete blocking at KOR (86±5% average SUV decrease) and demonstrated that [11C]GR103545 is exclusively binding at ORs (Figure 2c). The recently discovered KOR selective antagonist LY2795050 (Mitch et al, 2011) at 0.32 mg/kg significantly alters radiotracer binding in kappa-rich regions (77±4% average SUV decrease) and validates the in vivo specificity of [11C]GR103545 for KORs (Figure 2d). To examine the sensitivity of the radiotracer to kappa agonist challenge, we administered salvinorin A at 1 mg/kg (i.v.). We observed considerable blocking of the radiotracer (37±9% average SUV decrease) in kappa-dense regions, indicating binding competition between drug and radiotracer (Figure 2e). This prompted us to further investigate the in vivo occupancy of salvinorin A at KOR.
Validation of KOR occupancy imaging in rat by [11C]GR103545. Rats were administered either vehicle or a blocking agent prior to a bolus injection of the KOR-specific radiotracer [11C]GR103545 (a) Baseline scan with vehicle (1 : 1 : 8 DMSO : Tween80 : saline, i.v.). Highest uptake at later time was observed in the hypothalamus, nucleus accumbens, and caudate putamen. Lower uptake observed in the thalamus and hippocampus with the lowest uptake in cerebellum. (b) 0.1 mg/kg GR89696 (racemic GR103545; i.v.) administered 5 min prior to [11C]GR103545. (c) 2 mg/kg OR antagonist naloxone (i.v.) administered 10 min prior to [11C]GR103545. (d) 0.32 mg/kg KOR antagonist LY2795050 administered 5 min prior to [11C]GR103545. (e) 1 mg/kg KOR agonist salvinorin A (i.v.). administered 5 min prior to [11C]GR103545.
Salvinorin A in vivo Occupancy at KOR
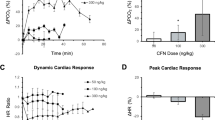
The in vivo KOR occupancy of salvinorin A in the rat brain is shown in Figure 3. Rats (n=15) were anesthetized with isoflurane (~2%) and administered salvinorin A at 1 of 10 doses (n=1 for each dose) ranging from 0.010 to 1.8 mg/kg (dose increments of 0.25 log units) and compared with the vehicle-treated animals (n=5). In each animal, [11C]GR103545 BPND values were averaged from six regions that had similar binding (baseline n=5; nucleus accumbens 0.66±0.15, midbrain 0.64±0.15, olfactory tubercle 0.61±0.12, amygdala 0.61±0.14, caudate putamen 0.57±0.14, and thalamus 0.55±0.20; mean±SD). As indicated by the dose–response decrease in BPND of [11C]GR103545, salvinorin A competitively blocks the radioligand from binding in KOR-rich regions in the rat brain. The administered dose producing 50% receptor binding potential (EC50) was obtained from Figure 3. On the basis of our data, salvinorin A achieves 50% occupancy at 0.36 mg/kg, and ~80% occupancy at 1.8 mg/kg when administered intravenously, 1 min prior to the radiotracer.
Occupancy of salvinorin A at KOR in vivo, estimated from [11C]GR103545 binding potential (BPND) in rat brain. Vehicle (n=5, mean±SEM) or salvinorin A (0.010–1.8 mg/kg, n=1 for each dose) was administered i.v. to rats 1 min prior to injection of [11C]GR103545. BPND represents the mean of nucleus accumbens, caudate putamen, amygdala, olfactory tubercle, midbrain, and thalamus (similar baseline regional binding levels). BPND was calculated using the Logan reference analysis method with the cerebellum as a reference region.
Prolonged Effects of Salvinorin A at KOR
When animals were treated with 0.18 and 0.32 mg/kg salvinorin A (n=1 for each dose) 1 min prior to [11C]GR103545, BPND is decreased to 70 and 60% of baseline (Figure 4a). Pretreating the animals at 1 h with the same doses of salvinorin A (0.18 mg/kg, n=2 and 0.32 mg/kg, n=3), BPND returns to near baseline, 91±7% and 87±12% of baseline (mean±SEM). Increasing the salvinorin A dose to 0.60 mg/kg (n=1) and pretreating at 1 min, specific binding decreased to 55% of baseline. A delayed radiotracer injection 1 h after salvinorin A (n=2) at the same dose resulted in a sustained, low BPND (51±5%), comparable to 1 min pretreated animals (Figure 4b). Extending the time between drug and [11C]GR103545 injection to 2.5 h, maintained a reduction in BPND, (60±8%), again consistent with 1 min and 1 h time points. Five hours after treatment with 0.60 mg/kg salvinorin A (n=3), [11C]GR103545 BPND returned to near baseline levels (88±5%).
Immediate and persistent effects of salvinorin A on KOR binding availability. Rats were treated with either vehicle or salvinorin A at 1 min, 1, 2.5, or 5 h prior to [11C]GR103545 and subsequent dynamic PET scan. (a) Rats pretreated with salvinorin A 1 h prior to the radioligand, had specific binding levels consistent with baseline for both 0.18 mg/kg (91±7%, n=2) and 0.32 mg/kg (87±12%, n=3). At 0.60 mg/kg, a sustained decrease in [11C]GR103545-specific binding was observed after 1 h, comparable to 1 min pretreatment (51±5%, n=2). (b) Pretreating rats with salvinorin A at 0.60 mg/kg for a longer period prior to [11C]GR103545 injection resulted in a persistent decrease in radioligand binding at 1 h (51±5%, n=2) and 2.5 h (60±8%, n=3). The radiotracer binding returned to near baseline levels when animals were treated with 0.6 mg/kg salvinorin A at 5 h before [11C]GR103545 (88±5%, n=3).
DISCUSSION
This is the first report of dynamic PET imaging with [11C]GR103545 in rats. Previously [11C]GR103545 has been evaluated in rats, but only following tissue dissection experiments (Ravert et al, 1999, 2002). [11C]GR103545 has been evaluated with PET in both NHPs (Talbot et al, 2005; Tomasi et al, 2013) and humans (Naganawa et al., 2014a). In comparison with the [11C]GR103545 in vivo tissue dissection experiments, we see a similar neuroanatomical localization of the radiotracer. Our results indicate highest radioligand binding in the hypothalamus followed by periaqueductal gray and ventral tegmental area. Previous autoradiography experiments with the KOR agonist [3H]U-69593 resulted in a similar neuroanatomical distribution (Nock et al, 1988), although we observed some differences compared with [11C]GR103545. [3H]U-69593 binding as reported in Nock et al (1988), was high in olfactory tubercle and only moderate in hypothalamus, contrast to both our findings and early reports with [11C]GR103545 mouse in vivo tissue dissection studies. We observed intermediate levels of radioligand binding in the caudate putamen, amygdala, and thalamus which is consistent with prior reports on neuroanatomical distribution of KORs in rat brain (Tempel and Zukin, 1987; Mansour et al, 1988; Unterwald et al, 1991). Our data indicate low binding in several cortical regions and lowest in the cerebellum, an area known to have little to undetectable levels of KOR density.
Self-blocking with GR89696 (racemic GR103545) at 0.1 mg/kg resulted in significant blocking of KOR binding sites (60% decrease), indicating the potency and high brain uptake of this kappa agonist (Figure 2b). Our results are consistent with in vivo tissue dissection studies which reported reduced radiotracer levels after administration of a similar dose of GR89696 (0.2 mg/kg).
The nonselective OR antagonist naloxone (in vitro Ki: μ=0.93 nM, κ=2.3 nM, δ=17 nM; Raynor et al, 1994) at 2 mg/kg completely blocked radioligand binding (86% decrease) indicating the specificity of [11C]GR103545 for ORs (Figure 2c). Recently, a new class of kappa-selective antagonists, aminobenzyloxyarylamides, have been identified (Mitch et al, 2011). Several compounds were evaluated pharmacologically (Lowe et al, 2014) and some as KOR radiotracers for PET (Zheng et al, 2013, 2014). LY2795050 has been evaluated as an antagonist PET tracer in both NHPs (Zheng et al, 2013; Kim et al, 2013) and humans (Naganawa et al., 2014b, 2015). According to Mitch et al (2011), LY2795050 binds preferentially at KORs in vitro with high affinity and selectivity (κ=0.72±0.22 nM, μ=25.8±12.6 nM, δ=153±50.3 nM). We administered 0.32 mg/kg LY2795050 (i.v., 5 min pretreatment) followed by [11C]GR103545 and observed significant blocking of the radiotracer at later time points (78% decrease) indicating the radiotracer is selective for KORs in vivo (Figure 2d). Quantifying salvinorin A levels in the brain has been difficult due to its rapid metabolism and pharmacokinetics (for review see Cunningham et al (2011)). We estimated the in vivo occupancy of salvinorin A at KOR using PET. To determine the sensitivity of [11C]GR103545 to agonist challenge, we administered salvinorin A at 1 mg/kg (i.v.) 5 min before the radiotracer. We observed a considerable reduction in binding of the radiotracer in kappa-dense regions (37% decrease) as evident in Figure 2e.
Self-blocking and naloxone blocking results also showed a decrease in radioligand binding in the cerebellum, compared with vehicle-treated animals. This result was unforeseen and is in contrast to previous in vivo tissue dissection experiments with [11C]GR103545 which reported no change in cerebellum levels after administration of blocking agents (Ravert et al, 2002). Kinetic modeling of [11C]GR103545 binding was executed using the Logan analysis method with the cerebellum as a reference region. We encompassed activity in the whole cerebellum because this resulted in the highest consistency between baseline animals. Encompassing the entire cerebellum may be subject to partial volume effects from nearby high-binding regions such as the periaqueductal gray, or nonspecific binding outside the brain. Attempts at encompassing smaller VOIs around the posterior lobe of the cerebellum resulted in undesirable low signal to noise and inconsistent baseline BPND values. Other low-binding regions (eg, motor cortex) were examined as reference regions but resulted in further underestimations of BPND.
The pharmacokinetics of [11C]Salvinorin A have been investigated previously in baboons (t1/2=8 min, bolus, i.v.) and rats (bolus, i.p.; Hooker et al, 2008, 2009). To guide our time-delayed administration experiments for measuring the immediate and prolonged effects of salvinorin A at KOR, we measured the pharmacokinetics of [11C]Salvinorin A in rats when administered intravenously (Supplementary Figure). [11C]Salvinorin A displayed rapid uptake (maximum activity in ~13 s; maximum uptake 0.2% injected dose/cc) and fast washout in the rat brain (t1/2=3.3 min). It is important to note that the data in the Supplementary Figure is uncorrected for radiometabolites which could explain the slow elimination after 5 min. Radioactive metabolites from [11C]Salvinorin A were reported by Hooker et al 2008 and it is well documented in the literature that salvinorin A undergoes rapid metabolism at the C-2 acetate (for review see Cunningham et al (2011)). The C-2 acetate group is also the labeling site of [11C]Salvinorin A, and cleavage leads to polar radioactive metabolites and potential accumulation in brain tissue. In addition, the pharmacokinetics of salvinorin A in rats following intraperitoneal administration has been previously reported. It was determined that intraperitoneal administration in rats resulted in a clearance rate from brain of 36 min t1/2 (Teksin et al, 2009). On the basis of the rapid clearance rate we observed, and also previously reported pharmacokinetics of salvinorin A, we chose a pretreatment time of 1 min for calculating occupancy at KOR. This pretreatment time maximized competition at KOR between drug challenge and radiotracer. We administered 10 different doses of salvinorin A followed by [11C]GR103545 and plotted the dose–response relationship with BPND. On the basis of high affinity and selectivity of salvinorin A in vitro, and its potent effects in vivo, we anticipated a lower EC50 than what resulted. Upon futher examination we determined that the occupancy reached at the administered doses is valid, given the low peak uptake of the drug in rat brain. The rapid metabolism of salvinorin A has been described in previous reports, and it was found that only 0.8% of the parent drug was detected in human urine (Pichini et al, 2005). In addition, Hooker et al (2008) reported an average maximum concentration of only 0.0175% ID/cc in baboon brain, and Butelman et al (2009) reported a maximum concentration of 1.01 ng/ml in NHP cerebrospinal fluid (0.032 mg/kg injected dose, i.v., measured 2 min after injection). In male Sprague–Dawley rats, Teksin et al (2009) reported a peak uptake of only 23.9 ng/ml (10 mg/kg injected dose, i.p.). From our [11C]Salvinorin A (i.v.) rat pharmacokinetic data, we observed a maximum uptake of 0.2% ID/cc. In addition, the rapid clearance of the drug could contribute to an underestimation of the salvinorin A-induced BPND change. This is under the assumption that by the time the radiotracer reaches KOR binding sites in the brain, salvinorin A has already started to clear and our measurements of receptor occupancy by salvinorin A would be underestimated. Regardless, this represents the first quantifiable measurement of salvinorin A occupancy at KOR in vivo.
These data offer some insight into the mechanism of tolerance to kappa agonist drugs. Upon agonist exposure, GPCRs can desensitize, internalize and traffic intracellularly into endosomes where they are either degraded by lysosomes (leading to downregulation), or recycled and re-inserted in the cell membrane (for review see Roth et al (1998)). KOR can also internalize following agonist exposure (Li et al, 2000, Liuchen, 2004) and this mechanism has been linked to behavioral tolerance from kappa agonists such as U50,488 (McLaughlin et al, 2004). Although KOR internalization has been well studied in vitro, the dynamics of this process in vivo have not been explored with PET (for review see Liuchen (2004)). To date, only a few reports have described the effect on PET measurements, and both reports were focused on the dopamine system (Skinbjerg et al, 2010; Quelch et al, 2014).
Salvinorin A causes desensitization and/or internalization of KORs from cell membranes in vitro (Wang et al, 2008; White et al, 2015), which prompted us to examine this process in vivo using salvinorin A as a ‘pharmacological tool’, taking advantage of its rapid pharmacokinetics. To test this, we designed a time-delayed administration of salvinorin A that would compare the immediate and persistent effects after the drug had eliminated. Guided by our initial pharmacokinetic and KOR occupancy data, we chose doses of salvinorin A that produced occupancy levels below and above the BPND EC50, and pretreatment times that allowed for complete clearance of salvinorin A in the rat brain. When 0.18 mg/kg salvinorin A was administered at 1 min, radioligand binding reduced by 30% compared with vehicle-treated animals. Introducing a 1 h delay between salvinorin A administration and radiotracer injection, BPND returned to near baseline at the same dose. Increasing the salvinorin A dose to 0.32 mg/kg, BPND decreased by ~35% from baseline at 1 min pretreatment but returned to near baseline levels when administered 1 h before the radioligand. Interestingly, increasing the salvinorin A dose to 0.60 mg/kg at 1 h pretreatment, we observed a prolonged effect on binding, consistent with 1 min pretreatment times. To explore the extent of prolonged binding reduction, we administered the same dose (0.60 mg/kg) of salvinorin A but increased the delay before radioligand injection. At 2.5 h pretreatment, we observed a consistent decrease in KOR binding, similar to 1 min and 1 h pretreatment time points. At 5 h following salvinorin A administration at 0.60 mg/kg, BPND of [11C]GR103545 returns to near baseline levels. The process of adaptive receptor trafficking following agonist exposure has been reported to occur within seconds to minutes for desensitization, minutes to hours for internalization, and hours to days for downregulation with the recovery rate from of each of those processes being similar (Li et al, 2000). Although we have no direct evidence of internalization, our timeline is consistent with other GPCR internalization and recycling dynamics (for review see Lefkowitz (1998)). On the basis of our kinetic data, we are confident salvinorin A has completely eliminated from rat brain at 1, 2.5, and 5 h time points, pointing towards an agonist-induced adaptive response by the receptor such as desensitization, internalization or downregulation of KOR.
We have reported the first rat PET study with the KOR selective radiotracer [11C]GR103545. This compliments previous NHP and human PET studies with [11C]GR103545, allowing for KOR translational PET research in rats. The interest in KOR as potential targets for non-addictive analgesics and antidepressants has been of considerable focus. Tools that aid in the study of this receptor class could expedite potential KOR therapeutics to market. The quantification of salvinorin A in vivo has been difficult due to its rapid metabolism and pharmacokinetics. We have demonstrated that [11C]GR103545 can be used to quantify salvinorin A levels in the brain. Our analysis estimates the in vivo occupancy of salvinorin A at KOR with BPND EC50~357 μg/kg in the rat brain.
Our results indicate salvinorin A has a prolonged effect on KOR binding availability, long after the drug has eliminated from the brain. This is the first PET study investigating this process in ORs and may aid in future occupancy studies following opioid agonist administration. Our results indicate when considerable occupancy of salvinorin A is reached, the drug has a prolonged impact on radioligand binding up to 2.5 h after treatment, and binding returns to near baseline levels at 5 h. Our results add to previous rat behavioral data that indicates opposite effects on intracranial self-stimulation thresholds when monitored immediately or 1 day after salvinorin A (Potter et al, 2011). In addition, our results are consistent with previous in vitro and ex vivo KOR internalization reports which suggest similar receptor trafficking rates. On the basis of these results, we have initiated an investigation of salvinorin A with multimodal imaging (PET/MR) in NHPs to further elucidate the neural mechanisms of this unique drug.
FUNDING AND DISCLOSURE
This research was carried out in whole or in part at the Athinoula A. Martinos Center for Biomedical Imaging at the Massachusetts General Hospital, using resources provided by the Center for Functional Neuroimaging Technologies, P41EB015896, a P41 Biotechnology Resource Grant supported by the National Institute of Biomedical Imaging and Bioengineering (NIBIB), National Institutes of Health. This work also involved the use of instrumentation supported by the NIH Shared Instrumentation Grant Program and/or High-End Instrumentation Grant Program; specifically, grant number(s) S10RR015728, S10RR026666, and S10RR017208, P41RR14075. NIH-NIDA T32 postdoctoral fellowship T32DA015036, DOE Training Grant DE-SC0008430, and NIH-NIDA K99DA037928. The authors declare no conflict of interest.
References
Butelman ER, Prisinzano TE, Deng H, Rus S, Kreek MJ (2009). Unconditioned behavioral effects of the powerful κ-opioid hallucinogen salvinorin A in nonhuman primates: fast onset and entry into cerebrospinal fluid. J Pharmacol Exp Ther 328: 588–597.
Carroll FI, Carlezon WA (2013). Development of κ opioid receptor antagonists. J Med Chem 56: 2178–2195.
Chen Y, Mestek A, Liu J, Hurley JA, Yu L (1993). Molecular cloning and functional expression of a mu-opioid receptor from rat brain. Mol Pharmacol 44: 8–12.
Cunningham CW, Rothman RB, Prisinzano TE (2011). Neuropharmacology of the naturally occurring–opioid hallucinogen salvinorin A. Pharmacological Reviews 63: 316–347.
Evans CJ, Keith DE, Morrison H, Magendzo K, Edwards RH (1992). Cloning of a delta opioid receptor by functional expression. Science 258: 1952–1955.
Hiller JM, Fan LQ (1996). Laminar distribution of the multiple opioid receptors in the human cerebral cortex. Neurochem Res 21: 1333–1345.
Hooker JM, Xu Y, Schiffer W, Shea C, Carter P, Fowler JS (2008). Pharmacokinetics of the potent hallucinogen, salvinorin A in primates parallels the rapid onset and short duration of effects in humans. Neuroimage 41: 1044–1050.
Hooker JM, Munro TA, Béguin C, Alexoff D, Shea C, Xu Y et al (2009). Salvinorin A and derivatives: Protection from metabolism does not prolong short-term, whole-brain residence. Neuropharmacology 57: 386–391.
Innis RB, Cunningham VJ, Delforge J, Fujita M, Gjedde A, Gunn RN et al (2007). Consensus nomenclature for in vivo imaging of reversibly binding radioligands. J Cereb Blood Flow Metab 27: 1533–1539.
Johnson MW, MacLean KA, Reissig CJ, Prisinzano TE, Griffiths RR (2011). Human psychopharmacology and dose-effects of salvinorin A, a kappa opioid agonist hallucinogen present in the plant Salvia divinorum. Drug Alcohol Depend 115: 150–155.
Kieffer BL, Befort K, Gaveriaux-Ruff C, Hirth CG (1992). The delta-opioid receptor: isolation of a cDNA by expression cloning and pharmacological characterization. PNAS 89: 12048–12052.
Kim SJ, Zheng M-Q, Nabulsi N, Labaree D, Ropchan J, Najafzadeh S et al (2013). Determination of the in vivo selectivity of a new κ-opioid receptor atagonist PET tracer 11C-LY2795050 in the Rhesus Monkey. J Nucl Med 54: 1668–1674.
Laruelle M (2000). Imaging synaptic neurotransmission with in vivo binding competition techniques: a critical review. J Cereb Blood Flow Metab 20: 423–451.
Li J-G, Benovic JL, Liu-Chen L-Y (2000). Mechanisms of agonist-induced down-regulation of the human κ-opioid receptor: internalization is required for down-regulation. Mol Pharmacol 58: 795–801.
Liuchen L (2004). Agonist-induced regulation and trafficking of κ opioid receptors. Life Sci 75: 511–536.
Logan J, Fowler JS, Volkow ND, Wang G-J, Ding Y-S, Alexoff DL (1996). Distribution volume ratios without blood sampling from graphical analysis of PET data. J Cereb Blood Flow Metab 16: 834–840.
Lord JAH, Waterfield AA, Hughes J, Kosterlitz HW (1977). Endogenous opioid peptides: multiple agonists and receptors. Nature 267: 495–499.
Lowe SL, Wong CJ, Witcher J, Gonzales CR, Dickinson GL, Bell RL et al (2014). Safety, tolerability, and pharmacokinetic evaluation of single- and multiple-ascending doses of a novel kappa opioid receptor antagonist LY2456302 and drug interaction with ethanol in healthy subjects. J Clin Pharmacol 54: 968–978.
Lefkowitz RJ (1998). G protein-coupled receptors. III. New roles for receptor kinases and beta-arrestins in receptor signaling and desensitization. J Biol Chem 273: 18677–18680.
MacLean KA, Johnson MW, Reissig CJ, Prisinzano TE, Griffiths RR (2013). Dose-related effects of salvinorin A in humans: dissociative, hallucinogenic, and memory effects. Psychopharmacology 226: 381–392.
Mansour A, Khachaturian H, Lewis ME, Akil H, Watson SJ (1988). Anatomy of CNS opioid receptors. Trends in Neurosciences 11: 308–314.
McLaughlin JP, Myers LC, Zarek PE, Caron MG, Lefkowitz RJ, Czyzyk TA et al (2004). Prolonged kappa opioid receptor phosphorylation mediated by G-protein receptor kinase underlies sustained analgesic tolerance. J Biol Chem 279: 1810–1818.
Minami M, Toya T, Katao Y, Maekawa K, Nakamura S, Onogi T et al (1993). Cloning and expression of a cDNA for the rat k-opioid receptor. FEBS Letters 329: 291–295.
Minami M, Satoh M (1995). Molecular biology of the opioid receptors: structures, functions and distributions. Neurosci Res 23: 121–145.
Mitch CH, Quimby SJ, Diaz N, Pedregal C, Torre MG, de la, Jimenez A et al (2011). Discovery of aminobenzyloxyarylamides as κ opioid receptor selective antagonists: application to preclinical development of a κ opioid receptor antagonist receptor occupancy tracer. J Med Chem 54: 8000–8012.
Nabulsi NB, Zheng M-Q, Ropchan J, Labaree D, Ding Y-S, Blumberg L et al (2011). [11C]GR103545: novel one-pot radiosynthesis with high specific activity. Nucl Med Biol 38: 215–221.
Naganawa M, Jacobsen LK, Zheng M-Q, Lin S-F, Banerjee A, Byon W et al (2014a). Evaluation of the agonist PET radioligand [11C]GR103545 to image kappa opioid receptor in humans: kinetic model selection, test-retest reproducibility and receptor occupancy by the antagonist PF-04455242. Neuroimage 99: 69–79.
Naganawa M, Zheng M-Q, Nabulsi N, Tomasi G, Henry S, Lin S-F et al (2014b). Kinetic modeling of 11C-LY2795050, a novel antagonist radiotracer for PET imaging of the kappa opioid receptor in humans. J Cereb Blood Flow Metab 34: 1818–1825.
Naganawa M, Zheng M-Q, Henry S, Nabulsi N, Lin S-F, Ropchan J et al (2015). Test-retest reproducibility of binding parameters in humans with 11C-LY2795050, an antagonist PET radiotracer for the κ opioid receptor. J Nucl Med 56: 243–248.
Nock B, Rajpara A, O'Connor LH, Cicero TJ (1988). Autoradiography of [3 H] U-69593 binding sites in rat brain: evidence for κ opioid receptor subtypes. Eur J Pharmacol 154: 27–34.
Pichini S, Abanades S, Farré V, Pellegrini M, Marchei E, Pacifici R et al (2005). Quantification of the plant-derived hallucinogen Salvinorin A in conventional and non-conventional biological fluids by gas chromatography/mass spectrometry after Salvia divinorum smoking. Rapid Commun Mass Spectrom 19: 1649–1656.
Potter DN, Damez-Werno D, Carlezon WA, Cohen BM, Chartoff EH (2011). Repeated exposure to the κ-opioid receptor agonist salvinorin A modulates extracellular signal-regulated kinase and reward sensitivity. Biol Psychiatry 70: 744–753.
Quelch DR, Withey SL, Nutt DJ, Tyacke RJ, Parker CA (2014). The influence of different cellular environments on PET radioligand binding: an application to D2/3-dopamine receptor imaging. Neuropharmacology 85: 305–313.
Ravert HT, Mathews WB, Musachio JL, Scheffel U, Finley P, Dannals RF (1999). [11C]-methyl 4-[(3, 4-dichlorophenyl) acetyl]-3-[(1-pyrrolidinyl) methyl]-1-piperazinecarboxylate ([11C]GR89696): synthesis and in vivo binding to kappa opiate receptors. Nucl Med Biol 26: 737–741.
Ravert HT, Scheffel U, Mathews WB, Musachio JL, Dannals RF (2002). [11C]-GR89696, a potent kappa opiate receptor radioligand; in vivo binding of the R and S enantiomers. Nucl Med Biol 29: 47–53.
Raynor K, Kong H, Chen Y, Yasuda K, Yu L, Bell GI et al (1994). Pharmacological characterization of the cloned kappa-, delta-, and mu-opioid receptors. Mol Pharmacol 45: 330–334.
Roth BL, Willins DL, Kroeze WK (1998). G protein-coupled receptor (GPCR) trafficking in the central nervous system: relevance for drugs of abuse. Drug Alcohol Depend 51: 73–85.
Roth BL, Baner K, Westkaemper R, Siebert D, Rice KC, Steinberg S et al (2002). Salvinorin A: a potent naturally occurring nonnitrogenous κ opioid selective agonist. Proc Natl Acad Sci USA 99: 11934–11939.
Schmidt MD, Schmidt MS, Butelman ER, Harding WW, Tidgewell K, Murry DJ et al (2005). Pharmacokinetics of the plant-derived κ-opioid hallucinogen salvinorin A in nonhuman primates. Synapse 58: 208–210.
Schiffer WK, Mirrione MM, Biegon A, Alexoff DL, Patel V, Dewey SL (2006). Serial microPET measures of the metabolic reaction to a microdialysis probe implant. J Neurosci Methods 155: 272–284.
Schoultz BW, Hjornevik T, Willoch F, Marton J, Noda A, Murakami Y et al (2010). Evaluation of the kappa-opioid receptor-selective tracer [11C]GR103545 in awake rhesus macaques. Eur J Nucl Med Mol Imaging 37: 1174–1180.
Schwarzer C (2009). 30 years of dynorphins—new insights on their functions in neuropsychiatric diseases. Pharmacol Therap 123: 353–370.
Shirayama Y, Ishida H, Iwata M, Hazama G, Kawahara R, Duman RS (2004). Stress increases dynorphin immunoreactivity in limbic brain regions and dynorphin antagonism produces antidepressant-like effects. J Neurochem 90: 1258–1268.
Skinbjerg M, Liow J-S, Seneca N, Hong J, Lu S, Thorsell A et al (2010). D2 dopamine receptor internalization prolongs the decrease of radioligand binding after amphetamine: A PET study in a receptor internalization-deficient mouse model. NeuroImage 50: 1402–1407.
Talbot PS, Narendran R, Butelman ER, Huang Y, Ngo K, Slifstein M et al (2005). 11C-GR103545, a radiotracer for imaging kappa-opioid receptors in vivo with PET: synthesis and evaluation in baboons. J Nucl Med 46: 484–494.
Teksin ZS, Lee IJ, Nemieboka NN, Othman AA, Upreti VV, Hassan HE et al (2009). Evaluation of the transport, in vitro metabolism and pharmacokinetics of Salvinorin A, a potent hallucinogen. Eur J Pharm Biopharm 72: 471–477.
Tempel A, Zukin RS (1987). Neuroanatomical patterns of the mu, delta, and kappa opioid receptors of rat brain as determined by quantitative in vitro autoradiography. PNAS 84: 4308–4312.
Tomasi G, Nabulsi N, Zheng M-Q, Weinzimmer D, Ropchan J, Blumberg L et al (2013). Determination of in vivo Bmax and Kd for 11C-GR103545, an agonist PET tracer for opioid receptors: a study in nonhuman primates. J Nucl Med 54: 600–608.
Unterwald EM, Knapp C, Zukin RS (1991). Neuroanatomical localization ofκ1and κ2 opioid receptors in rat and guinea pig brain. Brain Res 562: 57–65.
Valdes LJ, Butler WM, Hatfield GM, Paul AG, Koreeda M (1984). Divinorin A, a psychotropic terpenoid, and divinorin B from the hallucinogenic Mexican mint, Salvia divinorum. J Org Chem 49: 4716–4720.
Wang Y, Chen Y, Xu W, Lee DYW, Ma Z, Rawls SM et al (2008). 2-Methoxymethyl-salvinorin B is a potent κ opioid receptor agonist with longer lasting action in vivo than salvinorin A. J Pharmacol Exp Ther 324: 1073–1083.
White KL, Robinson JE, Zhu H, DiBerto JF, Polepally PR, Zjawiony JK et al (2015). The G protein-biased κ-opioid receptor agonist RB-64 is analgesic with a unique spectrum of activities in vivo. J Pharmacol Exp Ther 352: 98–109.
Zheng M-Q, Nabulsi N, Kim SJ, Tomasi G, Lin S -f ., Mitch C et al (2013). Synthesis and evaluation of 11C-LY2795050 as a opioid receptor antagonist radiotracer for PET imaging. J Nucl Med 54: 455–463.
Zheng M-Q, Kim SJ, Holden D, Lin S -f ., Need A, Rash K et al (2014). An improved antagonist radiotracer for the opioid receptor: synthesis and characterization of 11C-LY2459989. J Nucl Med 55: 1185–1191.
Acknowledgements
We thank Ramesh Neelamegam, Nathan Schauer, and Judit Sore for their assistance with PET radiotracer synthesis. We also thank Aijun Zhu, Al Schroeder, and Martin Strebl for assistance with animal preparation and scanner operation.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on the Neuropsychopharmacology website
Supplementary information
Rights and permissions
About this article
Cite this article
Placzek, M., Van de Bittner, G., Wey, HY. et al. Immediate and Persistent Effects of Salvinorin A on the Kappa Opioid Receptor in Rodents, Monitored In Vivo with PET. Neuropsychopharmacol 40, 2865–2872 (2015). https://doi.org/10.1038/npp.2015.159
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2015.159
- Springer Nature Switzerland AG
This article is cited by
-
Kappa-opioid receptors, dynorphin, and cocaine addiction: a positron emission tomography study
Neuropsychopharmacology (2019)