Abstract
Acute kidney injury (AKI) is characterized by tubular cell death and interstitial inflammation. TWEAK promotes experimental kidney injury and activates the transcription factor NF-κB, a key regulator of genes involved in cell survival and inflammatory response. In search of potential therapeutic targets for AKI, we compared a transcriptomics database of NF-κB-related genes from murine AKI-kidneys with a transcriptomics database of TWEAK-stimulated cultured tubular cells. Four out of twenty-four (17%) genes were significantly upregulated (false discovery rate, FDR<0.05), while nine out of twenty-four (37%) genes were significantly upregulated at FDR <0.1 in both databases. Bcl3 was the top upregulated NF-κB-related gene in experimental AKI and one of the most upregulated genes in TWEAK-stimulated tubular cells. Quantitative reverse transcription PCR (qRT-PCR), western blot and immunohistochemistry confirmed Bcl3 upregulation in both experimental conditions and localized increased Bcl3 expression to tubular cells in AKI. Transcriptomics database analysis revealed increased Bcl3 expression in numerous experimental and human kidney conditions. Furthermore, systemic TWEAK administration increased kidney Bcl3 expression. In cultured tubular cells, targeting Bcl3 by siRNA resulted in the magnification of TWEAK-induced NF-κB transcriptional activity, chemokine upregulation and Klotho downregulation, and in the sensitization to cell death induced by TWEAK/TNFα/interferon-γ. In contrast, Bcl3 overexpression decreased NF-κB transcriptional activity, inflammatory response and cell death while dampening the decrease in Klotho expression. In conclusion, Bcl3 expressed in response to TWEAK stimulation decreases TWEAK-induced inflammatory and lethal responses. Therefore, therapeutic upregulation of Bcl3 activity should be explored in kidney disease because it has advantages over chemical inhibitors of NF-κB that are known to prevent inflammatory responses but can also sensitize the cells to apoptosis.
Similar content being viewed by others
Introduction
Acute kidney injury (AKI) is characterized by an acute rise in serum creatinine levels or a decrease in urine output and is associated with the progression of chronic kidney disease (CKD) and to an increase in short-term and long-term mortality.1 There is no satisfactory treatment for this condition.2 Recent consensus in definitions allows for the recognition of AKI at earlier stages and thus even the knowledge of incipient AKI has been advanced lately.3, 4 This will hopefully facilitate clinical research examining early management strategies of AKI. Correct understanding of the pathophysiology of AKI will allow for the identification of specific therapeutic agents and earlier biomarkers for clinical practice.
The tumor necrosis factor (TNF) superfamily cytokine TWEAK is a key promoter of acute and chronic kidney injury.5, 6, 7, 8, 9, 10 Neutralizing anti-TWEAK antibodies have gone to clinical trials in lupus nephritis.10 The bulk of the renal cell mass is composed of tubular cells, and it is the tubular cell death or injury that is the main morphological feature of AKI.11 In tubular cells, TWEAK induces inflammatory responses, downregulates Klotho and, in presence of additional inflammatory cytokines, promotes cell death.12, 13, 14 These actions are thought to contribute to kidney injury and are related to the activation of the transcription factor NF-κB.13 TWEAK promotes both the early canonical NF-κB pathway activation characterized by nuclear translocation of RelA and the prolonged activation of the non-canonical pathway characterized by increased DNA-binding activity of the p52/RelB NF-κB complex.9, 15 Parthenolide is an inhibitor of the canonical pathway of NF-κB activation. TWEAK induces the parthenolide-sensitive expression of monocyte chemoattractant protein 1 (MCP-1)/CCL2 and RANTES/CCL5 chemokines13 and downregulation of Klotho expression.8
There is histological evidence of NF-κB activation in human diabetic nephropathy, glomerular disease and AKI.15 NF-κB was found to be activated in glomerular and tubular cells and correlated with the parameters associated with severe renal diseases, such as proteinuria or inflammation.16, 17, 18, 19, 20 In experimental renal disease, NF-κB is activated in podocytes and mesangial cells during glomerular injury and in tubular cells during the course of proteinuria. It is also activated in primary tubulointerstitial diseases, including ischemia/reperfusion injury, urinary tract obstruction and septic or toxic AKI.9, 13, 15, 21, 22, 23 NF-κB activation promotes inflammation, regulates fibrosis and may protect from cytokine-induced cell death.15 However, there is little information on the contribution of individual NF-κB-regulatory proteins in these actions. This knowledge is required to design better therapeutic approaches. Hence, there has not yet been any approach specifically targeting NF-κB in the clinic for kidney disease.
We recently showed that the NF-κB-regulatory protein NFκBiz was decreased during AKI, despite having higher than normal mRNA levels.24 Evidence from functional assessment have shown that in kidney cells, NFκBiz downregulation increased chemokine production, dampened TWEAK-induced Klotho downregulation and rendered the cells more resistant to inflammation-induced apoptosis. This suggests that NFκBiz may have anti-inflammatory properties in tubular epithelium. However, it can also result in cell death and downregulation of the anti-aging and tissue-protective protein Klotho. Overall, the properties of NFκBiz are thus not well suited for therapeutic intervention, given its opposing effects on inflammation and cell death. Here we have explored the function of B-cell leukemia protein 3 (Bcl3) in kidney cells. Bcl3 is yet another NF-κB regulator, and through a transcriptomics analysis of kidney tissues, we have identified it for its potential relevance in kidney injury.
Bcl3 is a member of the IκB family of NF-κB regulatory proteins that was first identified as a candidate proto-oncogene in patients with chronic lymphocytic leukemia.25 However, Bcl3 may have different functions in different cell types. Unlike other IκBs, Bcl3 is a predominantly nuclear protein containing a trans-activation domain, and it can be recruited to NF-κB-responsive promoters, resulting in transcriptional activation or repression depending on the subunit composition of NF-κB complexes.26, 27, 28, 29 Thus, Bcl3 specifically inhibits the DNA binding of homodimeric p50 or p52.28 By blocking ubiquitination of p50, Bcl3 stabilizes the p50 complex that inhibits gene transcription. Moreover, Bcl3 can also act as a co-activator for p50 and p52 dimers.27 It associates tightly with p52 homodimers, forming a ternary complex with DNA at κB sites. Tethering of Bcl3 to DNA via the p52 homodimer allows Bcl3 to trans-activate directly, which is not possible for p52 homodimers alone.27 In addition, Bcl3 can interact with other transcriptional regulators, including the AP-1 transcription factors c-Jun and c-fos,30 STAT131 and PPARγ.32 Because of these properties, elevated Bcl3 expression has been shown to promote increased cell proliferation, survival and malignant potential in breast cancer cell lines.33
To date, there are no data on Bcl3 expression or function in kidney cells. However, Bcl3 was the top upregulated NF-κB-related gene found in experimental AKI, and one of the most upregulated genes in TWEAK-stimulated tubular cells. In this study, we explored the regulation of Bcl3 expression and Bcl3 function in kidney tubular cells. We found that inflammatory stimuli induce Bcl3 expression and, in turn, Bcl3 contributes to block inflammatory and lethal responses to inflammatory stimuli in tubular cells. Thus, Bcl3 overexpression could have advantages over chemical inhibitors of NF-κB which, despite being able to prevent inflammatory responses, also sensitize the cells to apoptosis.8, 13, 34
Materials and methods
Cells and reagents
Mouse cortical tubule cells (MCT) murine tubular epithelial cells were grown in Roswell Park Memorial Institute (RPMI) 1640 (Life Technologies, Grand Island, NY, USA) medium with 10% heat inactivated fetal bovine serum, 2 mM glutamine, 100 U ml−1 penicillin, 100 μg ml−1 streptomycin, in 5% carbon dioxide at 37 °C.35 For experiments, the cells were rested in serum-free media for 24 h prior to the addition of stimuli. Two hundred thousand cells were seeded in 60-mm-coated plates (Costar, Sigma-Aldrich, St Louis, MO, USA) for RNA extraction and western blot or in 12-well plates (Costar, Sigma-Aldrich) for flow cytometry experiments. Cells were stimulated with TWEAK (Millipore, Bedford, MA, USA), interferon-γ (INFγ) and TNFα (PeproTech, Rocky Hill, NJ, USA). The concentrations of TWEAK, TNFα and INFγ used were derived from prior detailed dose–response studies.12, 13 Unless otherwise specified, TWEAK was used at 100 ng ml−1 based on these past studies and dose–response studies of the effect on Bcl3 expression.
Transfection of small interfering RNA
Cells were grown in six-well plates (Costar, Cambridge, MA, USA) and transfected with a mixture of 35 nmol ml−1 Bcl3 siRNA (Santa Cruz Biotechnology, Santa Cruz, CA, USA), Opti-MEM I Reduced Serum Medium and Lipofectamine RNAiMAX Transfection Reagent (Invitrogen, Paisley, UK; Life Technologies). After 18 h, the cells were washed and cultured in complete medium for 24 h and serum-depleted for 24 h before stimulation. A scrambled siRNA construct (Ambion, Applied Biosystems, Foster City, CA, USA) was used as the control. Cells were silenced for Bcl3 and 48 h later stimulated with TWEAK for 24 h.
Bcl3 transfection
Cells were grown in six-well plates (Costar) and transfected with a mixture of 0.5 μg Bcl3 overexpressing plasmid in the pCMV6 vector (OriGene, Rockville, MD, USA), Opti-MEM I Reduced Serum Medium and Lipofectamine 3000 transfection reagent (Invitrogen) following the manufacturer’s instructions. The transfected cells were selected with neomycin.
Cell death
Morphological characterization of apoptosis was assessed by fixation of cells with formalin and staining of nuclei with 4′,6-diamidino-2-phenylindole (Sigma-Aldrich) to observe the typical morphological changes as previously described.12 For assessment of apoptosis by flow cytometry, cells were silenced using Bcl3 or scrambled siRNA, rested in serum-free media for 24 h and then stimulated for 24 h with a lethal cytokine cocktail (100 ng ml−1 TWEAK, 30 ng ml−1 TNFα and 30 UI ml−1 interferon-γ (IFNγ)) for 24 h.12 The adherent cells were pooled with the spontaneously detached cells and incubated in propidium iodide (PI) 100 μg ml−1, NP-40 0.05%, RNAse A 10 μg ml−1 in phosphate-buffered saline at 4 °C for >3 h. This assay permeabilized the cells, allowing PI to stain both live and dead cells. The percentage of apoptotic cells with decreased DNA staining (hypodiploid cells) was quantified by flow cytometry using BD CellQuest Software (BD Biosciences, San Jose, CA, USA).
RNA extraction and real-time polymerase chain reaction
Total RNA was extracted from tissues and cells by the TRI Reagent method (Roche, Mannheim, Germany) and 1 or 4 μg RNA was reverse-transcribed with High-Capacity cDNA Archive Kit (Applied Biosystems). Pre-developed primers and probe assays (PDAR) were acquired from Applied Biosystems. Quantitative PCR was performed on an ABI Prism 7500 sequence detection PCR system (Applied Biosystems) according to the manufacturer’s protocol using the ΔΔCt method. Expression levels are given as ratios to GAPDH.
Western blot
Western blots were performed as previously described.36 The membranes were incubated overnight at 4 °C with rabbit polyclonal anti-Bcl3 antibody (1:500, Santa Cruz Biotechnology), caspase-3 (1:1000, Cell Signaling, Danvers, MA, USA), PCNA (1:1000, Cell Signaling), Klotho (1:1000, Calbiochem, San Diego, CA, USA) or mouse anti-tubulin monoclonal antibody (1:10 000, Sigma-Aldrich) followed by incubation with horseradish peroxidase-conjugated secondary antibody (1:2000, Amersham, Aylesbury, UK). The blots were developed with the enhanced chemiluminescence method (ECL) following the manufacturer’s instructions (Amersham).
Enzyme-linked immunosorbent assay
Cells were stimulated with TWEAK at 100 ng ml−1 for 3 h. The concentration of murine MCP-1 in the cell culture supernatants was determined by enzyme-linked immunosorbent assay following the manufacturer’s instructions (R&D Systems, Minneapolis, MN, USA).
Confocal microscopy
Cells were fixed in 4% paraformaldehyde and permeabilized in 0.2% Triton X-100 in phosphate-buffered saline for 10 min, washed in phosphate-buffered saline and incubated overnight at 4 °C with rabbit polyclonal anti-Bcl3 (1:50, Santa Cruz Biotechnology), followed by 1 h incubation with the appropriate FITC secondary antibody (1:300, Sigma-Aldrich). Filamentous actin was stained with phalloidin (1:1000) and cell nuclei were counterstained with 4′,6-diamidino-2-phenylindole. After washing, the cells were mounted in ProLong Gold Antifade Reagent (Life Technologies), and analyzed with a DM-IRB confocal microscope (Leica DM, Bannockburn, IL, USA).
NF-κB luciferase reporter gene assay
The silenced cells or cells overexpressing Bcl3 were transfected with Lipofectamine 3000 transfection reagent (Invitrogen, Life Technologies) according to the manufacturer’s instructions. pNF-κB-Luc (Stratagene, La Jolla, CA, USA) and pRLTK vectors, containing the luciferase gene Renilla (Promega, Madison, WI, USA), were used in a ratio of 10:1. The medium was replaced with RPMI without serum 6 h after transfection. The following day, the cells were treated with 100 ng ml−1 TWEAK for 3 h. Luciferase activity was determined by a luciferase assay system (Promega) and a luminometer (Berthold, Nashua, NH, USA) and normalized to Renilla activity to control for differences in transfection efficiency. TNF-α was used as a control.
Electrophoretic mobility shift assay
Cells were resuspended in buffer A (10 mmol l−1 HEPES, pH 7.8, 15 mmol l−1 KCl, 2 mmol l−1 MgCl2, 1 mmol l−1 PMSF, 0.1 mmol l−1 EDTA and 1 mmol l−1 DDT) and homogenized. Nuclei and cytosolic fractions were separated by centrifugation at 1000 g for 10 min. The nuclei (pellet) were washed twice in buffer A and resuspended in the same buffer, with a final concentration of 0.39 mol l−1 KCl. Nuclear proteins were extracted for 1 h at 4 °C and centrifuged at 100 000 g for 30 min. Supernatants containing the nuclear proteins were dialyzed in buffer C (50 mmol l−1 HEPES, pH 7.8, 50 mmol l−1 KCl, 10% glycerol, 1 mmol l−1 PMSF, 0.1 mmol l−1 EDTA and 1 mmol l−1 DDT) and then cleared by centrifugation and stored at −80 °C. The protein concentration was determined by the bicinchoninic acid method. Electrophoretic mobility shift assay was carried out as previously described.13
Animal models
These studies were approved by the IIS-FJD animal ethics committee and followed Directive 2010/63/EU on the protection of animals used for scientific purposes.
For experimental AKI, 12- to 14-week-old female WT or FN14 KO C57/BL6 mice37 received a single intraperitoneal (i.p.) injection of folic acid (Sigma-Aldrich) at 250 mg kg−1 in 0.3 mol l−1 sodium bicarbonate (AKI) or vehicle alone (controls) and were killed 1, 2, 3, 7 and 14 days later as previously described.9, 38 C57/BL6 mice (12- to 14-week old) received a single i.p. injection of 20 mg kg−1 cisplatin (Sigma-Aldrich) or saline (controls) and were killed 3 days later (n=5 per group). In addition, healthy 12- to 14-week-old mice were killed 48 or 72 h after a single i.p. injection of either 0.5 μg per mouse TWEAK (Alexis, Läufelfingen, Switzerland) or vehicle (200 μl 0.9% NaCl).39 The dose of TWEAK was estimated from cell culture dose–response studies, adjusted for the estimated extracellular volume of mice and validated as promoting TWEAK-induced signaling in the kidneys in vivo.
The mouse kidneys were perfused with cold saline in situ before removal. One kidney from each mouse was fixed in buffered formalin, embedded in paraffin and stained with hematoxylin–eosin or used for immunohistochemistry. The other kidney was snap-frozen in liquid nitrogen for protein and RNA studies.
Immunohistochemistry and immunofluorescence
Immunohistochemistry was carried out in 3-μm-thick paraffin-embedded tissue sections as previously described.37 The samples were incubated with primary anti-Bcl3 (1:100 Santa Cruz Biotechnology) antibody overnight at 4 °C. Secondary horseradish peroxidase-conjugated antibody was applied on the samples for 1 h. The sections were counterstained with Carazzi’s hematoxylin. The samples were dehydrated and mounted in Depex. Images were analyzed with Image-Pro Plus software (Media Cybernetics, Silver Spring, MD, USA).
For immunofluorescence, the samples were incubated with anti-Bcl3 (1:100 Santa Cruz Biotechnology) overnight at 4 °C, followed by a secondary Alexa Fluor 488- or 633-conjugated antibodies for 1 h. Cell nuclei were counterstained with 4′,6-diamidino-2-phenylindole. After washing, the cells were mounted in ProLong Gold Antifade Reagent (Life Technologies) and analyzed. Some sections were subsequently incubated with the proximal tubule marker, fluorescein-conjugated tetragonolobus lotus lectin (1:33, Sigma-Aldrich).40
Six human kidney tissue samples were obtained from the IIS-FJD biobank (age 65–80 years, three males, serum creatinine 0.73–3.1 mg dl−1) with or without AKI. AKI was defined by a serum creatinine increase of 0.3 mg dl−1 within 48 h or by histological evidence of AKI.
AKI transcriptomics
Affymetrix transcriptomic arrays of kidney tissue were analyzed at Unidad Genómica Moncloa, Fundación Parque Científico de Madrid, Madrid, Spain, following the manufacturer’s protocol.7 Image files were initially obtained through the Affymetrix GeneChip Command Console Software. Subsequently, Robust Multichip Analysis was performed using the Affymetrix Expression Console Software. Starting from the normalized Robust Multichip Analysis, the Significance Analysis of Microarrays was performed using the limma package (Babelomics, http://www.babelomics.org), using a false discovery rate (FDR) of 5% to identify genes that were significantly differentially regulated between the analyzed groups. Transcriptomic analysis was performed in cultured MCT cells exposed to 100 ng ml−1 TWEAK or vehicle for 6 h and in kidney samples from mice 24 h after being injected with folic acid (AKI) or vehicle.
Database search
The following databases were searched for Bcl3 expression in kidney disease: GEO profiles (http://www.ncbi.nlm.nih.gov/geoprofiles/?term=bcl3+kidney), Kidney & Urinary Pathway Knowledge Base (kupkb at http://www.kupkb.org/) and Nephromine (http://www.nephromine.org/).
Statistics
Statistical analyses were performed using SPSS 17.0 statistical software. The results are expressed as the mean±s.e.m. Significance at the P<0.05 level was assessed by Student’s t-test for two groups and analysis of variance for three or more groups of data.
Results
Bcl3 expression is increased in AKI
TWEAK targeting protects from experimental AKI induced by a folic acid overdose or ischemia/reperfusion13, 41 as well as from other experimental nephropathies.10 TWEAK promotes the activation of NF-κB.15 To search for potential mediators of TWEAK effects during AKI, we performed a transcriptomics analysis of NF-κB-related genes in a model of folic acid-induced AKI and in cultured murine renal tubular cells stimulated with 100 ng ml−1 TWEAK for 6 h. This analysis disclosed that 4/24 (17%) NF-κB-related genes were significantly upregulated (FDR<0.05) while 9/24 (37%) genes were upregulated at FDR<0.1 in both databases. No gene was downregulated at FDR<0.05 in both databases simultaneously. When assessing the mean fold-change in upregulated genes in both databases, Bcl3 topped the list (Table 1). Bcl3 was upregulated in kidney tissue during AKI (Figure 1a) where expression of Bcl3 mRNA correlated with that of Fn14 (TWEAK receptor) mRNA (Figure 1b). Bcl3 was also upregulated in cultured tubular cells exposed to TWEAK (Figure 1c) qRT-PCR confirmed an increased in Bcl3 mRNA expression in whole kidneys from day 1 through day 7 after AKI induction, with partial recovery by day 14 (Figure 2a). By contrast, serum creatinine, a marker of renal dysfunction, peaked at days 1–3 and returned to normal values by day 7.8 Western blot assessment of Bcl3 protein expression confirmed its upregulation during AKI (Figure 2b). Immunohistochemistry revealed that Bcl3 was localized in the nuclei of tubular cells (Figure 2c), supporting the hypothesis that tubular cells may be targets of TWEAK during kidney injury. Lectin staining further revealed that Bcl3 was expressed in the nuclei of proximal as well as non-proximal tubular cells (Figure 2d). Tubular Bcl3 expression was also increased in human AKI (Supplementary Figure 1) and in a cisplatin-induced AKI model (Supplementary Figure 2).
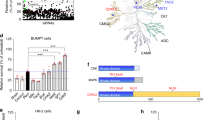
Kidney Bcl3 expression is increased during AKI and TWEAK increases Bcl3 in cultured tubular cells. (a) Transcriptomics analysis of Bcl3 expression in kidney samples from experimental AKI, expressed as the mean±s.e.m. Mice were injected with folic acid or vehicle 24 h before killing. Control values were considered to be 100%. N=3, *P<0.01. (b) Transcriptomics show a positive correlation between Bcl3 and TWEAK receptor Fn14 mRNA in AKI. (c) Transcriptomics of murine renal tubular cells showed increased Bcl3 mRNA expression upon stimulation with TWEAK at 100 ng ml−1 for 6 h (N=3, *P<0.001). Mean±s.e.m. from three independent experiments.
Increased kidney Bcl3 expression in AKI is localized to tubular cells. Mice were injected with folic acid and killed at days 1, 2, 3, 7 and 14 (5 mice per group). Serum creatinine, a marker of renal dysfunction, peaked at days 1–3 and returned to normal values by day 7.8 (a) Kidney Bcl3 mRNA levels. Quantitative PCR with reverse transcription (qRT-PCR). Mean±s.e.m. *P<0.004, #P<0.02 vs control. (b) Bcl3 protein assessed by western blot. Mean±s.e.m., *P<0.002 vs control. (c) Bcl3 protein immunohistochemistry. Note nuclear Bcl3 staining in AKI tubules (arrowheads). (d) Bcl3 protein immunofluorescence. Tetragonolobus lotus lectin stains of proximal tubular cells. Note nuclear Bcl3 staining in AKI proximal and non-proximal tubules.
Database search
Our database search disclosed that Bcl3 is also upregulated in a variety of experimental and human nephropathies, both acute and chronic (Table 2). Thus, understanding the role of Bcl3 in tubular cells may be relevant for nephropathies beyond AKI in both humans and experimental animals.
TWEAK increases Bcl3 expression in tubular cells in vitro and in vivo
On the basis of the transcriptomics data that showed upregulation of Bcl3 expression in cultured proximal tubular cells and immunohistochemistry data that showed upregulation of nuclear Bcl3 levels in tubular cells during AKI, further studies were conducted in cultured tubular cells. In cultured tubular cells, 100 ng ml−1 TWEAK increased Bcl3 mRNA expression in dose-dependent (Figure 3a) and time-dependent manners (Figure 3b). TWEAK also increased Bcl3 protein expression assessed by western blot (Figure 3c). In addition, immunofluorescence showed that TWEAK promoted Bcl3 translocation to the nucleus (Figure 3d). To study the effects of TWEAK on Bcl3 in vivo, healthy mice received a single TWEAK injection intraperitoneally. Both Bcl3 mRNA and protein expression increased in kidneys from TWEAK-injected mice in a time-dependent manner (Figure 4a and b). To further confirm the effect of TWEAK on Bcl3 expression, we explored the effect of Fn14 deficiency on Bcl3 expression in AKI in mice. Both Bcl3 mRNA and protein expressions were lower in kidneys from mice deficient in the TWEAK receptor Fn14 than in wild-type controls after induction of AKI with folic acid (Figure 4c and d).
TWEAK increases Bcl3 expression in dose-dependent and time-dependent manners in cultured tubular cells. (a) Tubular cells were exposed to different concentrations of TWEAK for 1 h. Quantitative PCR with reverse transcription. Mean±s.e.m. of three independent experiments, *P<0.02, #P<0.035 vs control. (b) Tubular cells were exposed to 100 ng ml−1 TWEAK for 1–24 h. N=3, *P<0.001, #P<0.027 vs control. (c) Western blot shows that TWEAK at 100 ng ml−1 for 6 h increased nuclear Bcl3 protein in tubular cells. Histone-3 was used as loading control. N=3, *P<0.004 vs control. (d) TWEAK at 100 ng ml−1 increased nuclear Bcl3 assessed by immunofluorescence.
TWEAK increases Bcl3 expression in healthy kidneys in vivo and Fn14 targeting prevents Bcl3 upregulation in AKI. (a) Systemic TWEAK administration increased kidney Bcl3 mRNA expression assessed by qRT-PCR. Mean±s.e.m. of five mice per group. *P<0.04, **P<0.002, vs control. (b) Immunohistochemistry showed the increased Bcl3 protein levels in kidney in response to TWEAK localized to tubular nuclei. (c) FN14 knockout (KO) and wild-type (WT) mice were injected with folic acid 24 or 72 h before killing. Bcl3 mRNA was assessed by qRT-PCR. N=6 animals per group, mean±s.e.m., *P<0.02, #P<0.014 vs control. (d) FN14 KO and WT mice were injected with folic acid 24 or 72 h before killing. Bcl3 protein expression was assessed by western blot. N=6 animals per group, mean±s.e.m., *P<0.013, #P<0.029 vs control.
Bcl3 silencing results in increased inflammatory gene expression in response to TWEAK
In tubular cells, TWEAK activates NF-κB as assessed by increased DNA-binding activity and reporter gene transcription (Supplementary Figures 3 and 4). To investigate the function of Bcl3 in tubular cells, Bcl3 expression was downregulated with a specific siRNA (Figure 5a and b). Then, the cells were stimulated with 100 ng ml−1 TWEAK for 24 h. Bcl3 downregulation did not significantly modify the proliferation or apoptosis rates, neither serum-deprived nor in TWEAK-treated cells (Figure 5c and d). Because TWEAK upregulates the expression of inflammatory genes in tubular cells in an NF-κB-dependent manner,13 we tested the impact of Bcl3 silencing on TWEAK-induced expression of these inflammatory genes. Bcl3 targeting increased the inflammatory response to TWEAK, increasing MCP-1, CXCL10 and RANTES mRNA levels assessed by quantitative PCR with reverse transcription (Figure 5e) and protein expression of the chemokine MCP-1 (Figure 5f). NF-κB transcriptional activity, assayed with an NF-κB reporter construct, was higher in Bcl3-silenced cells treated with TWEAK than in non-silenced cells (Supplementary Figure 4).
Bcl3 silencing results in an increased tubular cell inflammatory response to TWEAK. (a) Bcl3 siRNA silences Bcl3 protein expression assessed by western blot. Tubular cells were transfected with Bcl3 or control siRNA for 18 h and then washed and collected at 24, 48 and 72 h. (b) Bcl3 siRNA silences Bcl3 mRNA expression. Tubular cells were transfected with Bcl3 or control siRNA. Bcl3 mRNA expression was measured by qRT-PCR. N=3, *P<0.002. (c) Bcl3 downregulation did not modify the apoptosis rate in cells stimulated with 100 ng ml−1 TWEAK for 24 h. N=3. (d) Bcl3 downregulation did not modify the proliferation rate in cells stimulated with 100 ng ml−1 TWEAK for 24 h. N=3. (e) In Bcl3-targeted cells, 100 ng ml−1 TWEAK increased MCP-1 mRNA expression at 3 h to a greater extent than in control cells. N=3, *P<0.025. (f) In Bcl3-targeted cells, 100 ng ml−1 TWEAK increased supernatant MCP-1 protein at 3 h to a greater extent than in control cells. N=3, *P<0.025. (g) In Bcl3-targeted cells, 100 ng ml−1 TWEAK increased CXCL10 mRNA expression at 3 h to a greater extent than in control cells. N=3, *P<0.001. (h) In Bcl3-targeted cells, 100 ng ml−1 TWEAK increased RANTES mRNA expression at 3 h to a greater extent than in control cells. N=3, *P<0.002.
Bcl3 silencing increases apoptosis in cultured tubular cells exposed to an inflammatory milieu
To determine the role of Bcl3 in apoptosis, tubular cells were exposed to a lethal cytokine cocktail composed of TWEAK–TNFα–IFNγ that upregulated Bcl3 expression, and this was inhibited by parthenolide (Figure 6a). Because we had previously characterized parthenolide as an inhibitor of NF-κB in this system,8 these data indicated that the Bcl3 upregulation was NF-κB-dependent. TWEAK–TNFα–IFNγ increased both Bcl3 mRNA and protein expressions in a time-dependent manner, which peaked at 3 h (Supplementary Figure 5a and b). Bcl3 silencing rendered the cells more sensitive to TWEAK–TNFα–IFNγ-induced apoptosis, confirmed by the presence of both hypodiploid cells and the typical apoptotic, pyknotic and fragmented nuclei from morphological assessment (Figure 6b–d). This sensitivity to apoptosis due to Bcl3 silencing may have been occurring through caspase activation, due to the fact that Bcl3 silencing magnified the appearance of cleaved (active) caspase-3 in response to TWEAK–TNFα–IFNγ (Figure 6e).
Bcl3 expression is increased under pro-apoptotic conditions and Bcl3 has anti-apoptotic properties. (a) The lethal cytokine cocktail 100 ng ml−1 TWEAK/30 ng ml−1 TNFα/30 UI ml−1 IFNγ (TTI) for 3 h increased Bcl3 protein levels in cultured tubular cells. This increment was prevented by pretreatment with 2.5 μg ml−1 parthenolide. N=3, *P<0.009. (b) Bcl3-silenced cells were exposed to TTI for 24 h and the number of hypodiploid cells was analyzed by flow cytometry. Representative flow cytometry results. (c) Apoptosis rate assessed by the percentage of hypodiploid cells was increased in Bcl3-silenced cells exposed to TTI for 24 h. N=3, *P<0.002. (d) Cells fixed with formalin were stained with 4′,6-diamidino-2-phenylindole (DAPI). Bcl3-silenced cells were more sensitive to apoptosis (nuclear fragmentation and pyknotic nuclei) induced by TTI than control cells. (e) Caspase-3 cleavage was assessed by western blot. Bcl3 silencing increased caspase-3 cleavage in response to TTI. Note the appearance of an additional fragment in TTI-treated cells which is magnified by Bcl2 siRNA. N=3, *P<0.025.
Bcl3 overexpression prevents apoptosis in cultured tubular cells exposed to an inflammatory milieu
To confirm the function of Bcl3 in tubular cells, Bcl3 was overexpressed by means of a specific plasmid (Figure 7a). Bcl3 upregulation did not modify the baseline proliferation or apoptosis rates (Figure 7a and e). However, in Bcl3-overexpressing cells, the inflammatory response to TWEAK was milder, with lower MCP-1, RANTES and CXCL10 mRNA levels (Figure 7b–d). NF-κB transcriptional activity in response to TWEAK was also milder in Bcl3-overexpressing cells than in wild-type cells (Supplementary Figure 4). To confirm the role of Bcl3 in apoptosis, tubular cells were exposed to the lethal cytokine cocktail TWEAK–TNFα–IFNγ for 24 h. Bcl3 upregulation protected the cells from TWEAK–TNFα–IFNγ-induced apoptosis (Figure 7e and f).
Bcl3 overexpression results in a reduced tubular cell inflammatory response to TWEAK and protection against apoptosis. (a) Bcl3 plasmid transfection increased Bcl3 protein expression without modulating proliferation, as showed by PCNA protein expression assessed by western blot. (b–d) In Bcl3-transfected cells, 100 ng ml−1 TWEAK increased MCP-1, RANTES and CXCL10 mRNA expression at 3 h to a lesser extent than in control cells. (b) MCP-1 mRNA expression. N=3, *P<0.001. (c) RANTES mRNA expression. N=3, *P<0.001. (d) CXCL10 mRNA expression. N=3, *P<0.001. (e) Bcl3-transfected cells were exposed to 100 ng ml−1 TWEAK/30 ng ml−1 TNFα/30 UI ml−1 IFNγ (TTI) for 24 h and the number of hypodiploid cells was analyzed by flow cytometry. Representative flow cytometry results. (f) The apoptosis rate assessed as percentage of hypodiploid cells was reduced in Bcl3-transfected cells exposed to TTI for 24 h. N=4, *P<0.001.
Bcl3 modulates Klotho expression in cultured tubular cells
Klotho, a kidney-expressed protein with anti-aging and nephroprotective functions, is decreased by inflammatory stimuli such as TWEAK.8, 42, 43, 44 Bcl3 targeting reduced Klotho mRNA and protein expression and magnified the decrease in Klotho expression induced by TWEAK stimulation (Figure 8a and b). In contrast, Bcl3 overexpression increased Klotho expression and lessened TWEAK-induced Klotho downregulation (Figure 8c).
Bcl3 dampens TWEAK downregulation of Klotho expression. (a) Klotho mRNA was assessed by qRT-PCR in control or Bcl3-silenced cells treated with 100 ng ml−1 TWEAK for 24 h. N=3, *P<0.003 vs the respective scrambled siRNA control. (b) Klotho protein was assessed by western blot in Bcl3-silenced cells exposed to TWEAK for 24 h. Representative western blot. N=3, *P<0.005 vs the respective scrambled siRNA control. The exaggerated response to TWEAK in terms of Klotho downregulation when endogenous Bcl3 is silenced is consistent with the role of Bcl3 in dampening TWEAK signaling, possibly by downregulating NF-κB activation, due to the fact that proinflammatory gene expression and Klotho downregulation are NF-κB-dependent responses. (c) Enforced Bcl3 overexpression dampened TWEAK downregulation of Klotho expression. N=3, *P<0.025 vs control.
Discussion
For the first time, we have explored the regulation of the expression and the function of Bcl3 in kidney tubular epithelium. The main findings are that Bcl3 expression is increased in the tubular epithelium during AKI and that in tubular cells, Bcl3 is induced by pro-inflammatory stimuli. In turn, Bcl3 contributes to the quenching of inflammatory responses, which protects the cells from apoptosis and increases the expression of the protective and anti-aging protein Klotho. Bcl3 was found to be upregulated in numerous kidney conditions both in humans and experimental animals, suggesting that these results likely have an impact beyond AKI.
Unlike other members of the IκB family, Bcl3 contains a transactivation domain, and can be recruited to promoters, resulting in transcriptional activation or repression, depending on the transcriptional complex formed.45, 46, 47 We have observed Bcl3 upregulation in AKI, a process characterized by release of cytokines, inflammation and tubular cell death. Furthermore, we have confirmed that Bcl3 is upregulated in tubular cells by the pro-inflammatory cytokine TWEAK, a promoter of AKI, and translocates to the nucleus where it regulates gene expression. Bcl3 expression in tubules is also increased in vivo and translocates to the nucleus upon TWEAK injection, while Fn14 (TWEAK receptor) deficiency prevents Bcl3 upregulation in AKI. Thus, TWEAK is a key Bcl3 regulator both in cell culture and in vivo in tubular cells.
Bcl3 silencing and overexpression studies have provided some insights into the function of inducible Bcl3 in tubular cells in response to cytokines. The results showed that except for cell proliferation, Bcl3 targeting magnified all the cellular responses that were studied, including increased chemokine expression and cell death, and further decreased Klotho expression, while Bcl3 overexpression had the opposite effect. Upregulation of chemokine expression and downregulation of Klotho expression are mediated by the classical NF-κB activation pathway in tubular cells.7, 8, 15 Induction of inflammation, reduction of Klotho expression and promotion of tubular cell death are all thought to contribute to the severity of AKI. Secretion of inflammatory mediators by inflammatory cells promotes further tubular cell injury. In addition, Klotho, originally described as an anti-aging factor,48 also has nephroprotective functions, including anti-inflammatory, pro-survival and anti-fibrotic actions.14, 42, 49, 50 Overall, these studies suggest that in kidney cells, Bcl3 dampens the cellular responses to inflammatory stress, and, thus, potentiating Bcl3 expression should be explored as a nephroprotective strategy. However, Bcl3 did not antagonize all NF-κB-dependent responses to TWEAK. Thus, no impact on TWEAK-induced cell proliferation, an NF-κB-dependent process,39 was observed. This argues for some selectivity of Bcl3 in the regulation of TWEAK-induced, NF-κB-activated genes that should be clarified in further detailed studies.
The observed anti-inflammatory function of Bcl3 in tubular cells is also consistent with observations in leukocytes. In these cells, Bcl3 has been described as an essential negative regulator of NF-κB during Toll-Like Receptor and TNF receptor signaling in macrophages. Deletion of Bcl3 in macrophages results in an increase in NF-κB p50 ubiquitination and proteasomal degradation, and increased inflammatory gene expression after lipopolysaccharide exposure.46, 47 In RAW cells, Bcl3 acts as an IL-10-inducible molecule that suppresses lipopolysaccharide-induced TNF-α production.51 Furthermore, Bcl3 silencing increased mRNA expression and secretion of pro-inflammatory cytokines IL-8 and IL-17 in cutaneous T-cell lymphoma cells.33
Unfortunately, we were unable to study the role of Bcl3 in AKI in vivo. However, the results reported here identifying Bcl3 as a negative regulator of deleterious cellular responses suggest that the therapeutic utility of Bcl3 in kidney injury appears to lie in identifying mechanisms to further increase its expression or mimic its activation to protect the cells from death or stress responses. Strategies aimed at increasing Bcl3 activity should therefore be developed. These may include cell-permeable Bcl3 agonist peptides or small molecule activators. In this regard, the role of Bcl3 in attenuating its own expression in a TNFα-induced manner has been recently characterized to be dependent on an incoherent feed-forward loop. In this regulatory loop, TNFα-induced NF-κB signaling activates the expression of both the TNFα and Bcl3 genes, but with distinct temporal expression profiles, which allows the modulation of expression dynamics and inflammatory responses while minimizing the risk of pathological hyper-inflammation.52
Inhibitors of NF-κB have been shown to prevent expression of inflammatory molecules and downregulation of Klotho in response to inflammatory cytokines of the TNF superfamily.8, 13 However, they also promote apoptosis when the cells are exposed to TNF superfamily cytokines.34 By contrast, Bcl3 protects the cells from apoptosis, inflammation upregulation and Klotho downregulation. Thus, the therapeutic upregulation of Bcl3 activity may have advantages over small-molecule inhibitors of NF-κB.
Characterizing the role of Bcl3 in kidney cell NF-κB signaling is a further step toward the goal of therapeutically manipulating this transcription factor. In this regard, we recently observed that the NFκBiz protein is decreased in tubular cells during AKI and that targeting NFκBiz increased chemokine production and dampened Klotho downregulation induced by TWEAK without modulating cell proliferation.24 NFκBiz targeting also rendered cells more resistant to apoptosis induced by inflammatory cytokines. Thus, there are similarities but also differences between the roles of NFκBiz and Bcl3 in the modulation of cell responses elicited by pro-inflammatory stimuli (Table 3).
In conclusion, Bcl3 is a regulator of NF-κB that is inducible during kidney injury by inflammatory stimuli such as TWEAK. In kidney cells, Bcl3 limits pro-inflammatory and lethal responses induced by TWEAK and other cytokines (Figure 9). Thus, therapeutic strategies aimed at increasing Bcl3 expression or activity should be explored as potential approaches for kidney disease.
Bcl3 regulation of tubular cell biology in response to inflammatory cytokines. TWEAK alone promotes tubular cell proliferation, upregulation of chemokine expression and downregulation of Klotho expression in an NF-κB-dependent, parthenolide-sensitive manner. In the presence of additional inflammatory cytokines such as TNFα and IFNγ, TWEAK promotes cell death. However, inducible Bcl3 expression does not modulate cell proliferation in response to inflammatory stimuli but prevents downregulation of Klotho gene expression while dampening the upregulation of the chemokine genes. Furthermore, Bcl3 prevents tubular cell death in an inflammatory milieu.
References
Moe S, Drueke T, Cunningham J, Goodman W, Martin K, Olgaard K et al. Definition, evaluation, and classification of renal osteodystrophy: a position statement from Kidney Disease: Improving Global Outcomes (KDIGO). Kidney Int 2006; 69: 1945–1953.
Bellomo R, Kellum JA, Ronco C . Acute kidney injury. Lancet 2012; 380: 756–766.
Perazella MA, Coca SG . Three feasible strategies to minimize kidney injury in 'incipient AKI'. Nat Rev Nephrol 2013; 9: 484–490.
Acute Kidney Injury Work Group. KDIGO Clinical Practice Guideline for Acute Kidney Injury. Kidney Int Suppl 2012; 2: 1–138.
Sanz AB, Aroeira LS, Bellon T, del PG, Jimenez-Heffernan J, Santamaria B et al. TWEAK promotes peritoneal inflammation. PLoS ONE 2014; 9: e90399.
Ucero AC, Benito-Martin A, Fuentes-Calvo I, Santamaria B, Blanco J, Lopez-Novoa JM et al. TNF-related weak inducer of apoptosis (TWEAK) promotes kidney fibrosis and Ras-dependent proliferation of cultured renal fibroblast. Biochim Biophys Acta 2013; 1832: 1744–1755.
Izquierdo MC, Sanz AB, Mezzano S, Blanco J, Carrasco S, Sanchez-Nino MD et al. TWEAK (tumor necrosis factor-like weak inducer of apoptosis) activates CXCL16 expression during renal tubulointerstitial inflammation. Kidney Int 2012; 81: 1098–1107.
Moreno JA, Izquierdo MC, Sanchez-Nino MD, Suarez-Alvarez B, Lopez-Larrea C, Jakubowski A et al. The inflammatory cytokines TWEAK and TNFalpha reduce renal klotho expression through NFkappaB. J Am Soc Nephrol 2011; 22: 1315–1325.
Sanz AB, Sanchez-Nino MD, Izquierdo MC, Jakubowski A, Justo P, Blanco-Colio LM et al. TWEAK activates the non-canonical NFkappaB pathway in murine renal tubular cells: modulation of CCL21. PLoS ONE 2010; 5: e8955.
Sanz AB, Izquierdo MC, Sanchez-Nino MD, Ucero AC, Egido J, Ruiz-Ortega M et al. TWEAK and the progression of renal disease: clinical translation. Nephrol Dial Transplant 2014; 29 (Suppl 1): i54–i62.
Ortiz A, Justo P, Sanz A, Lorz C, Egido J . Targeting apoptosis in acute tubular injury. Biochem Pharmacol 2003; 66: 1589–1594.
Justo P, Sanz AB, Sanchez-Nino MD, Winkles JA, Lorz C, Egido J et al. Cytokine cooperation in renal tubular cell injury: the role of TWEAK. Kidney Int 2006; 70: 1750–1758.
Sanz AB, Justo P, Sanchez-Nino MD, Blanco-Colio LM, Winkles JA, Kreztler M et al. The cytokine TWEAK modulates renal tubulointerstitial inflammation. J Am Soc Nephrol 2008; 19: 695–703.
Sanchez-Nino MD, Sanz AB, Ortiz A . Klotho to treat kidney fibrosis. J Am Soc Nephrol 2013; 24: 687–689.
Sanz AB, Sanchez-Nino MD, Ramos AM, Moreno JA, Santamaria B, Ruiz-Ortega M et al. NF-kappaB in renal inflammation. J Am Soc Nephrol 2010; 21: 1254–1262.
Loverre A, Ditonno P, Crovace A, Gesualdo L, Ranieri E, Pontrelli P et al. Ischemia-reperfusion induces glomerular and tubular activation of proinflammatory and antiapoptotic pathways: differential modulation by rapamycin. J Am Soc Nephrol 2004; 15: 2675–2686.
Zheng L, Sinniah R, Hsu SI . In situ glomerular expression of activated NF-kappaB in human lupus nephritis and other non-proliferative proteinuric glomerulopathy. Virchows Arch 2006; 448: 172–183.
Mezzano SA, Barria M, Droguett MA, Burgos ME, Ardiles LG, Flores C et al. Tubular NF-kappaB and AP-1 activation in human proteinuric renal disease. Kidney Int 2001; 60: 1366–1377.
Sakai N, Wada T, Furuichi K, Iwata Y, Yoshimoto K, Kitagawa K et al. p38 MAPK phosphorylation and NF-kappa B activation in human crescentic glomerulonephritis. Nephrol Dial Transplant 2002; 17: 998–1004.
Ashizawa M, Miyazaki M, Abe K, Furusu A, Isomoto H, Harada T et al. Detection of nuclear factor-kappaB in IgA nephropathy using Southwestern histochemistry. Am J Kidney Dis 2003; 42: 76–86.
Ruiz-Ortega M, Bustos C, Hernandez-Presa MA, Lorenzo O, Plaza JJ, Egido J . Angiotensin II participates in mononuclear cell recruitment in experimental immune complex nephritis through nuclear factor-kappa B activation and monocyte chemoattractant protein-1 synthesis. J Immunol 1998; 161: 430–439.
Ruiz-Ortega M, Lorenzo O, Ruperez M, Blanco J, Egido J . Systemic infusion of angiotensin II into normal rats activates nuclear factor-kappaB and AP-1 in the kidney: role of AT(1) and AT(2) receptors. Am J Pathol 2001; 158: 1743–1756.
Lopez-Franco O, Suzuki Y, Sanjuan G, Blanco J, Hernandez-Vargas P, Yo Y et al. Nuclear factor-kappa B inhibitors as potential novel anti-inflammatory agents for the treatment of immune glomerulonephritis. Am J Pathol 2002; 161: 1497–1505.
Poveda J, Sanz AB, Rayego-Mateos S, Ruiz-Ortega M, Carrasco S, Ortiz A et al. NFkappaBiz protein downregulation in acute kidney injury: modulation of inflammation and survival in tubular cells. Biochim Biophys Acta 2016; 1862: 635–646.
Ohno H, Takimoto G, McKeithan TW . The candidate proto-oncogene bcl-3 is related to genes implicated in cell lineage determination and cell cycle control. Cell 1990; 60: 991–997.
Wulczyn FG, Naumann M, Scheidereit C . Candidate proto-oncogene bcl-3 encodes a subunit-specific inhibitor of transcription factor NF-kappa B. Nature 1992; 358: 597–599.
Bours V, Franzoso G, Azarenko V, Park S, Kanno T, Brown K et al. The oncoprotein Bcl-3 directly transactivates through kappa B motifs via association with DNA-binding p50B homodimers. Cell 1993; 72: 729–739.
Nolan GP, Fujita T, Bhatia K, Huppi C, Liou HC, Scott ML et al. The bcl-3 proto-oncogene encodes a nuclear I kappa B-like molecule that preferentially interacts with NF-kappa B p50 and p52 in a phosphorylation-dependent manner. Mol Cell Biol 1993; 13: 3557–3566.
Zhang Q, Didonato JA, Karin M, McKeithan TW . BCL3 encodes a nuclear protein which can alter the subcellular location of NF-kappa B proteins. Mol Cell Biol 1994; 14: 3915–3926.
Na SY, Choi JE, Kim HJ, Jhun BH, Lee YC, Lee JW . Bcl3, an IkappaB protein, stimulates activating protein-1 transactivation and cellular proliferation. J Biol Chem 1999; 274: 28491–28496.
Jamaluddin M, Choudhary S, Wang S, Casola A, Huda R, Garofalo RP et al. Respiratory syncytial virus-inducible BCL-3 expression antagonizes the STAT/IRF and NF-kappaB signaling pathways by inducing histone deacetylase 1 recruitment to the interleukin-8 promoter. J Virol 2005; 79: 15302–15313.
Yang J, Williams RS, Kelly DP . Bcl3 interacts cooperatively with peroxisome proliferator-activated receptor gamma (PPARgamma) coactivator 1alpha to coactivate nuclear receptors estrogen-related receptor alpha and PPARalpha. Mol Cell Biol 2009; 29: 4091–4102.
Chang TP, Vancurova I . Bcl3 regulates pro-survival and pro-inflammatory gene expression in cutaneous T-cell lymphoma. Biochim Biophys Acta 2014; 1843: 2620–2630.
Lorz C, Benito-Martin A, Boucherot A, Ucero AC, Rastaldi MP, Henger A et al. The death ligand TRAIL in diabetic nephropathy. J Am Soc Nephrol 2008; 19: 904–914.
Haverty TP, Kelly CJ, Hines WH, Amenta PS, Watanabe M, Harper RA et al. Characterization of a renal tubular epithelial cell line which secretes the autologous target antigen of autoimmune experimental interstitial nephritis. J Cell Biol 1988; 107: 1359–1368.
Poveda J, Sanchez-Nino MD, Glorieux G, Sanz AB, Egido J, Vanholder R et al. p-cresyl sulphate has pro-inflammatory and cytotoxic actions on human proximal tubular epithelial cells. Nephrol Dial Transplant 2014; 29: 56–64.
Sanchez-Nino MD, Poveda J, Sanz AB, Mezzano S, Carrasco S, Fernandez-Fernandez B et al. Fn14 in podocytes and proteinuric kidney disease. Biochim Biophys Acta 2013; 1832: 2232–2243.
Wen X, Peng Z, Li Y, Wang H, Bishop JV, Chedwick LR et al. One dose of cyclosporine A is protective at initiation of folic acid-induced acute kidney injury in mice. Nephrol Dial Transplant 2012; 27: 3100–3109.
Sanz AB, Sanchez-Nino MD, Izquierdo MC, Jakubowski A, Justo P, Blanco-Colio LM et al. Tweak induces proliferation in renal tubular epithelium: a role in uninephrectomy induced renal hyperplasia. J Cell Mol Med 2009; 13: 3329–3342.
Lorz C, Ortiz A, Justo P, Gonzalez-Cuadrado S, Duque N, Gomez-Guerrero C et al. Proapoptotic Fas ligand is expressed by normal kidney tubular epithelium and injured glomeruli. J Am Soc Nephrol 2000; 11: 1266–1277.
Hotta K, Sho M, Yamato I, Shimada K, Harada H, Akahori T et al. Direct targeting of fibroblast growth factor-inducible 14 protein protects against renal ischemia reperfusion injury. Kidney Int 2011; 79: 179–188.
Buendia P, Carracedo J, Soriano S, Madueno JA, Ortiz A, Martin-Malo A et al. Klotho prevents NFkappaB translocation and protects endothelial cell from senescence induced by uremia. J Gerontol A Biol Sci Med Sci 2015; 70: 1198–1209.
Sastre C, Rubio-Navarro A, Buendia I, Gomez-Guerrero C, Blanco J, Mas S et al. Hyperlipidemia-associated renal damage decreases Klotho expression in kidneys from ApoE knockout mice. PLoS ONE 2013; 8: e83713.
Izquierdo MC, Perez-Gomez MV, Sanchez-Nino MD, Sanz AB, Ruiz-Andres O, Poveda J et al. Klotho, phosphate and inflammation/ageing in chronic kidney disease. Nephrol Dial Transplant 2012; 27 (Suppl 4): iv6–10.
Wang VY, Huang W, Asagiri M, Spann N, Hoffmann A, Glass C et al. The transcriptional specificity of NF-kappaB dimers is coded within the kappaB DNA response elements. Cell Rep 2012; 2: 824–839.
Carmody RJ, Ruan Q, Palmer S, Hilliard B, Chen YH . Negative regulation of toll-like receptor signaling by NF-kappaB p50 ubiquitination blockade. Science 2007; 317: 675–678.
Collins PE, Kiely PA, Carmody RJ . Inhibition of transcription by B cell leukemia 3 (Bcl-3) protein requires interaction with nuclear factor kappaB (NF-kappaB) p50. J Biol Chem 2014; 289: 7059–7067.
Kuro-o M, Matsumura Y, Aizawa H, Kawaguchi H, Suga T, Utsugi T et al. Mutation of the mouse klotho gene leads to a syndrome resembling ageing. Nature 1997; 390: 45–51.
Carracedo J, Buendia P, Merino A, Madueno JA, Peralbo E, Ortiz A et al. Klotho modulates the stress response in human senescent endothelial cells. Mech Ageing Dev 2012; 133: 647–654.
Zhou L, Li Y, Zhou D, Tan RJ, Liu Y . Loss of Klotho contributes to kidney injury by derepression of Wnt/beta-catenin signaling. J Am Soc Nephrol 2013; 24: 771–785.
Kuwata H, Watanabe Y, Miyoshi H, Yamamoto M, Kaisho T, Takeda K et al. IL-10-inducible Bcl-3 negatively regulates LPS-induced TNF-alpha production in macrophages. Blood 2003; 102: 4123–4129.
Walker T, Adamson A, Jackson DA . BCL-3 attenuation of TNFA expression involves an incoherent feed-forward loop regulated by chromatin structure. PLoS ONE 2013; 8: e77015.
Schmid H, Boucherot A, Yasuda Y, Henger A, Brunner B, Eichinger F et al. Modular activation of nuclear factor-kappaB transcriptional programs in human diabetic nephropathy. Diabetes 2006; 55: 2993–3003.
Ju W, Nair V, Smith S, Zhu L, Shedden K, Song PX et al. Tissue transcriptome-driven identification of epidermal growth factor as a chronic kidney disease biomarker. Sci Transl Med 2015; 7: 316ra193.
Reich HN, Tritchler D, Cattran DC, Herzenberg AM, Eichinger F, Boucherot A et al. A molecular signature of proteinuria in glomerulonephritis. PLoS ONE 2010; 5: e13451.
Hodgin JB, Borczuk AC, Nasr SH, Markowitz GS, Nair V, Martini S et al. A molecular profile of focal segmental glomerulosclerosis from formalin-fixed, paraffin-embedded tissue. Am J Pathol 2010; 177: 1674–1686.
Sarwal M, Chua MS, Kambham N, Hsieh SC, Satterwhite T, Masek M et al. Molecular heterogeneity in acute renal allograft rejection identified by DNA microarray profiling. N Engl J Med 2003; 349: 125–138.
Flechner SM, Kurian SM, Solez K, Cook DJ, Burke JT, Rollin H et al. De novo kidney transplantation without use of calcineurin inhibitors preserves renal structure and function at two years. Am J Transplant 2004; 4: 1776–1785.
Teramoto K, Negoro N, Kitamoto K, Iwai T, Iwao H, Okamura M et al. Microarray analysis of glomerular gene expression in murine lupus nephritis. J Pharmacol Sci 2008; 106: 56–67.
Berthier CC, Bethunaickan R, Gonzalez-Rivera T, Nair V, Ramanujam M, Zhang W et al. Cross-species transcriptional network analysis defines shared inflammatory responses in murine and human lupus nephritis. J Immunol 2012; 189: 988–1001.
Okada S, Misaka T, Tanaka Y, Matsumoto I, Ishibashi K, Sasaki S et al. Aquaporin-11 knockout mice and polycystic kidney disease animals share a common mechanism of cyst formation. FASEB J 2008; 22: 3672–3684.
Attanasio M, Uhlenhaut NH, Sousa VH, O'Toole JF, Otto E, Anlag K et al. Loss of GLIS2 causes nephronophthisis in humans and mice by increased apoptosis and fibrosis. Nat Genet 2007; 39: 1018–1024.
Wright J, Morales MM, Sousa-Menzes J, Ornellas D, Sipes J, Cui Y et al. Transcriptional adaptation to Clcn5 knockout in proximal tubules of mouse kidney. Physiol Genomics 2008; 33: 341–354.
Puig O, Wang IM, Cheng P, Zhou P, Roy S, Cully D et al. Transcriptome profiling and network analysis of genetically hypertensive mice identifies potential pharmacological targets of hypertension. Physiol Genomics 2010; 42A: 24–32.
Manoli I, Sysol JR, Li L, Houillier P, Garone C, Wang C et al. Targeting proximal tubule mitochondrial dysfunction attenuates the renal disease of methylmalonic acidemia. Proc Natl Acad Sci USA 2013; 110: 13552–13557.
Rokushima M, Fujisawa K, Furukawa N, Itoh F, Yanagimoto T, Fukushima R et al. Transcriptomic analysis of nephrotoxicity induced by cephaloridine, a representative cephalosporin antibiotic. Chem Res Toxicol 2008; 21: 1186–1196.
Yasui N, Kajimoto K, Sumiya T, Okuda T, Iwai N . The monocyte chemotactic protein-1 gene may contribute to hypertension in Dahl salt-sensitive rats. Hypertens Res 2007; 30: 185–193.
Dweep H, Sticht C, Kharkar A, Pandey P, Gretz N . Parallel analysis of mRNA and microRNA microarray profiles to explore functional regulatory patterns in polycystic kidney disease: using PKD/Mhm rat model. PLoS ONE 2013; 8: e53780.
Acknowledgements
We thank María del Mar González García-Parreño for her assistance with the confocal microscope. This work was supported by grants from the Instituto de Salud Carlos III FEDER funds ISCIII RETIC REDINREN RD12/0021 and RD16/0009, PI16/02057, PI16/01900, PI13/00047, PI15/00298, CP14/00133, PIE13/00051, Comunidad de Madrid (CIFRA S2010/BMD-2378), Sociedad Española de Nefrología. Programa Intensificación Actividad Investigadora (ISCIII/Agencia Laín-Entralgo/CM) to AO, Miguel Servet to ABS, MDSN, MECD to JP. IIS-FJD biobank PT13/0010/0012.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on Experimental & Molecular Medicine website
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/4.0/
About this article
Cite this article
Poveda, J., Sanz, A., Carrasco, S. et al. Bcl3: a regulator of NF-κB inducible by TWEAK in acute kidney injury with anti-inflammatory and antiapoptotic properties in tubular cells. Exp Mol Med 49, e352 (2017). https://doi.org/10.1038/emm.2017.89
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/emm.2017.89
- Springer Nature Limited
This article is cited by
-
Mechanisms of norcantharidin against renal tubulointerstitial fibrosis
Pharmacological Reports (2024)
-
Regulation of Apoptosis and Autophagy During Anoxia in the Freshwater Crayfish, Faxonius virilis
Marine Biotechnology (2022)
-
The TWEAK/Fn14/CD163 axis—implications for metabolic disease
Reviews in Endocrine and Metabolic Disorders (2022)
-
The hepatic senescence-associated secretory phenotype promotes hepatocarcinogenesis through Bcl3-dependent activation of macrophages
Cell & Bioscience (2021)
-
Albuminuria Downregulation of the Anti-Aging Factor Klotho: The Missing Link Potentially Explaining the Association of Pathological Albuminuria with Premature Death
Advances in Therapy (2020)