Abstract
Objective
Acute respiratory distress syndrome (ARDS) leads to life-threatening acute hypoxemic respiratory failure and requires mechanical ventilation. However, there is a lack of certainty regarding recruitment maneuvers (RMs) and positive end-expiratory pressure (PEEP) levels. Therefore, we performed a network meta-analysis to identify the optimal RM and PEEP levels of patients with ARDS.
Methods
We searched the PubMed, OVID and Cochrane Central Register of Controlled Trials (Central) databases for randomized controlled trials (RCTs). The primary outcome was death on the 28th day, and the secondary outcomes included in-hospital death, ventilator-free days, and barotrauma. The relative effect sizes were estimated by risk ratios (RRs) for binary variables and standard mean difference (SMD) for continuous variables. The efficacy of the interventions was ranked using surface under the cumulative ranking. Multiple intervention comparisons based on the Bayesian framework were performed to integrate the efficacy of all included strategies.
Results
Thirteen RCTs comprising 4410 patients were included in the network meta-analysis. In terms of death at 28 days, inconsistencies were found globally and locally in the tests. None of the ventilation strategies was significantly superior to the others on any outcomes. According to the relative rank probabilities, RM + lower PEEP levels showed the highest probability of reducing the risk of in-hospital death and reducing ventilator-free days. Lower PEEP levels showed the highest probability of benefitting barotrauma. The overall quality of the evidence per grade was moderate to low.
Conclusions
The no ventilation strategy is significantly superior to the other strategies. RM + lower PEEP levels has the highest probability of benefitting survival. The evidence has low overall quality and should be further studied.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Acute respiratory distress syndrome (ARDS) is an acute inflammatory lung injury characterized by damaged pulmonary capillary endothelial cells, damaged alveolar epithelial cells and increased vascular permeability, leading to life-threatening acute hypoxemic respiratory failure in the clinic [1]. ARDS was first reported 50 years ago [2], and a number of positive clinical trials have been conducted over the past decades to examine treatment strategies, such as mechanical ventilation with a low tidal volume [3], neuromuscular blockers in early ARDS [4], and prone positioning [5]. Approximately 40.1% of patients with ARDS need invasive ventilation. To date, mechanical ventilation is the firstline therapy for ARDS. On the basis of clinical research, guidelines endorsed by multiple professional societies recommend lowering the tidal volume and airway pressure as the basic strategies for ventilation [6, 7]. In addition to tidal volume, other parameters of mechanical ventilation, such as positive end-expiratory pressure (PEEP) levels and lung recruitment maneuvers, can affect the outcomes of patients with ARDS. In previous studies, higher PEEP levels for patients with ARDS responded to increased PEEP through improved oxygenation and reduced mortality [8]; additionally, some studies have shown that lung recruitment maneuvers (RMs) with higher PEEP levels may reduce mortality [9], while other studies have reached a different conclusion [10]. Traditional pairwise meta-analysis can only be used to compare specific parameters between ventilation strategies but not for the entire set of parameters relevant to different ventilation strategies. In this case, a network meta-analysis is advantageous for comparing the effectiveness of multiple interventions. To date, network meta-analysis has not been conducted to compare multiple mechanical ventilation strategies. We compared different PEEP levels with or without lung recruitment maneuvers in terms of low tidal volume ventilation to identify the optimal ventilation strategy for ARDS.
2 Methods
We performed our systematic review in accordance with the preferred reporting items for systematic reviews and meta-analyses extension statement for network meta-analysis [11].
2.1 Eligibility Criteria
The inclusion criteria of the studies were randomized controlled trials (RCTs) that were used to compare different mechanical ventilation strategies for adult patients with moderate to severe ARDS. The inclusion criteria of patients were adults with moderate to severe ARDS who received mechanical ventilation with low tidal volume mechanical ventilation strategies.
The types of mechanical strategies included lower PEEP, higher PEEP, RM + higher PEEP, RM + lower PEEP, and RM + PEEP titration. A lower PEEP level is defined as the minimum PEEP levels reaching the clinical goals, including the ARDSNet PEEP/FiO2 protocol [12] or minimum PEEP to maintain PaO2 > 60 mmHg and FiO2 < 0.6. A higher PEEP level is defined as the maximum PEEP without increasing the maximal inspiratory plateau pressure above 28–30 cm H2O or initial PEEP levels higher than a comparator strategy used to determine PEEP, including the high PEEP/FiO2 protocol. PEEP titration included PEEP titration according to the best respiratory-system static compliance, maximum SaO2, or esophageal pressure. RM is defined as the application of transient elevations to airway pressure during mechanical ventilation to open, including collapsed lung units and an increase in the number of alveoli participating in tidal ventilation, including extended sigh, staircase incremental PEEP levels or continuous positive airway pressure.
The primary outcome was 28-day mortality, and the secondary outcomes included in-hospital mortality, length of ventilator-free days, and barotrauma.
2.2 Data Sources and Searches
We searched the PubMed, OVID, and Cochrane Central Register of Controlled Trials (Central) databases to find relevant articles up to 30 December 2019 in all languages without limitations concerning publication dates and languages. We used combinations of the terms “acute respiratory distress syndrome” (or “acute lung injury” or “acute respiratory failure”) and “mechanical ventilation” (or “positive end-expiratory pressure” or “recruitment maneuver” or “open lung” or “lung recruitment” or “alveolar recruitment maneuver”). The electronic search strategy for the 4 databases is shown in the supplemental file.
2.3 Study Selection and Data Collection
Two reviewers (WH and PW) independently assessed the eligibility of all identified citations in accordance with the abovementioned criteria. Data were extracted, and the study quality was assessed independently by two reviewers (WH and PW). Disagreements between reviewers were settled by a third reviewer (FJ) when needed. During data collection, if the median and the first and third quartiles were recorded in clinical trial studies, then the equation \((X\approx (0.7+0.39/n) (q1+q3)/2+(0.3-0.39/n)\) m) [13] was used to transform information to the sample mean, and the equation (\(SD\approx (q3-q1)/1.35\)) was used to transform information to standard deviation [14] to avoid data loss.
2.4 Risk of Bias in Individual Studies
The risk of bias in individual studies was classified into three levels: low risk of bias, unclear risk of bias, and high risk of bias. Risk of bias analysis was performed using Review Manager® Version 5.3 for Windows (RevMan, The Cochrane Collaboration, Oxford, UK).
2.5 Statistical Analysis
Traditional pairwise meta-analysis was used with the meta module of STATA (Version 15.0; StataCorp, College Station, TX). Network meta-analyses in a Bayesian framework were performed using a Markov chain Monte Carlo simulation technique in Aggregate Data Drug Information System (ADDIS) software (version 1.16.8).
Risk ratios (RRs) were used to estimate the relative effect sizes for binary variables, while the standard mean difference (SMD) was used for continuous variables. The 95% confidence interval (CI) was used for the direct meta-analysis and Crl for the network meta-analysis.
Heterogeneity between studies was assessed with I2 statistics and p values. Statistical significance was set at a p value of 0.05. Heterogeneity was considered low, moderate, or high for the estimated I2 values under 25%, between 25 and 50%, and over 50%, respectively. If p < 0.05 or I2 > 50%, the random effects model was used for pairwise meta-analyses; otherwise, the fixed effects model was used.
The comparison of the fit of consistency and inconsistency models was evaluated to determine the global inconsistency. The node splitting approach was also used to calculate the inconsistency of the model, and p < 0.05 was considered significant heterogeneity. The random effects model was used to calculate the pooled effect size; otherwise, the consistency model was used to calculate the pooled effect size. The residual deviance statistics and deviance information criteria were used to evaluate the model fit for the consistent and inconsistent models.
The ranking probabilities for each mechanical ventilation strategy under different endpoints were assessed to provide a basis for selecting alternatives. For each ventilation strategy, the surface under the cumulative ranking (SUCRA) was used to estimate the ranking probabilities of assuming any possible rank. SUCRA was plotted using the cumulative ranking curves, and the surface under the curves was calculated. The SUCRA can be used to estimate the priority of the strategy. SUCRA was calculated using a previously reported equation [13]. The ranking probabilities were calculated using the Bayesian framework, and cumulative ranking probability curves were drawn using GraphPad Prism 5.
3 Results
3.1 Characteristics of Enrolled Studies
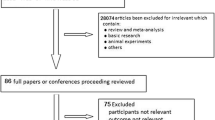
A total of 878 articles were obtained according to the search strategy. After screening, 31 articles were excluded due to duplicates. A total of 124 articles remained after screening based on their title and abstract. Among the 124 articles, 2 were case reports, 3 were letters, 48 were review articles, 17 were not randomized control trials, 16 had no relevant data, and 4 did not adopt a low tidal volume ventilation strategy in the control groups. Ultimately, 13 randomized controlled trials including 4410 patients were enrolled for the network meta-analysis. Patients with ARDS received one of the five mechanical ventilation strategies (recruitment maneuver combined with PEEP titration, recruitment maneuver combined with higher PEEP, recruitment maneuver combined with lower PEEP, higher PEEP, and lower PEEP). Literature screening and results are shown in Fig. 1A. The main characteristics of all studies are reported in Table 1.
3.2 Risk of Bias Within Studies
The risk of bias within studies is shown in Fig. 1B. An article [15] did not describe randomization methods. Three articles had a high risk of other bias, and one of them [12] modified the high-PEEP strategy by eliminating the steps with a PEEP of less than 12 cm of water and requiring a minimum PEEP of 14 cm of water for the first 48 h. An article reported by Meade et al. had a programming error occurring late in the study, thereby disrupting the specified randomization blocks. The bias in another study [26] was caused by different treatments between focal ARDS and nonfocal ARDS.
3.3 Heterogeneity and Inconsistency Assessment
In the pairwise meta-analyses, moderate to high heterogeneity was detected; for death in 28 days, the I2 of RM + PEEP titration versus RM + lower PEEP was 64.5%. For ventilator-free days, the I2 of RM + PEEP titration versus lower PEEP is 56.8% and that for higher PEEP versus lower PEEP is 71.3%. For barotrauma, the I2 of RM + PEEP titration versus lower PEEP is 55.5%. The comparisons of other strategies show low heterogeneity. The results of the pairwise meta-analyses are shown in Supplemental file 1.
The fit of the consistency model for all outcomes was similar to that of the inconsistency model (Supplemental file 2), suggesting low global inconsistency. The node-splitting analysis for death in 28 days, RM + PEEP titration versus RM + lower PEEP and RM + lower PEEP versus lower PEEP had local inconsistency (p < 0.05). The other outcomes showed no significant inconsistency between the direct effects and indirect effects (Supplemental file 3).
3.4 Network Structure and Geometry
The network plot for all outcomes is shown in Fig. 2. The size of the node is proportional to the number of patients randomized to receive the treatment. The width of each line is proportional to the number of trials comparing the connected treatments. The most common comparison was RM + PEEP titration versus lower PEEP, and the most common subjects were RM + PEEP titration versus lower PEEP.
Network plots for all outcomes. A Network plots for death in 28 days. B Network plots for death in hospital. C Network plots for ventilator-free days. D Network plots for barotrauma. Treatments are represented by nodes and head-to-head comparisons with edges. The size of the nodes is proportional to the number of the patients, while the thickness of the edges is proportional to the number of studies
3.5 Network Meta-analysis for Outcomes
For the primary outcomes in terms of death at 28 days, five ventilation strategies were included. None of the ventilation strategies were significantly superior to others, and the 95% CI included 1 in the Bayesian analysis (Fig. 3A).
Pooled estimates of network meta-analysis. A Risk ratios (95% credible intervals) for death in 28 days (upper triangle) and death in the hospital (lower triangle) in the Bayesian framework. B Risk ratios (95% credible intervals) for barotrauma (upper triangle) and standard mean difference (95% credible intervals) for ventilator-free days (lower triangle) in the Bayesian framework. Result in each cell is presented as risk ratio or standard mean difference (95% credible interval) for the comparison of row-defining treatment versus column-defining treatment. For the outcomes, if the range of 95% CI of 1, the difference between the two strategies is not significant
For the secondary outcomes, the ventilation strategies were compared in terms of ventilator-free days. The results of the network meta-analysis indicated that the differences among the strategies were not significant (Fig. 3B) with a 95% CI of 0. In terms of the other two secondary outcomes, the results suggested that no strategy was superior in terms of hospital deaths (Fig. 3A) and barotrauma (Fig. 3B).
3.6 Rank Probabilities
The relative ranking of the ventilation strategies was estimated using SUCRA. In our study, the results indicate that the higher the SUCRA is, the more superior the strategy. The ranking results are shown in Table 2, and the SUCRA values are shown in Fig. 4.
Rankograms and the SUCRA for each ventilation strategy for A Death in 28 days in the Bayesian framework. B Death in the hospital in the Bayesian framework. C Ventilator-free days in the Bayesian framework. D Barotrauma in the Bayesian framework. Horizontal axis shows possible ranks and vertical axis shows cumulative probability at each rank. The larger SUCRA, the better ranking
In terms of death at 28 days, higher PEEP had the highest SUCRA value (0.701), and RM + lower PEEP had the lowest SUCRA value (0.546). RM + lower PEEP had the highest SUCRA value in terms of hospital deaths (0.925) and ventilator-free days (0.759). Higher PEEP had the lowest SUCRA value (0.410) in terms of hospital deaths. The lower PEEP strategy had the lowest SUCRA value (0.470) in terms of ventilator-free days. In terms of barotrauma, lower PEEP had the highest SUCRA value (0.734), whereas RM + PEEP titration had the lowest SUCRA value (0.435).
4 Discussion
In our systematic review and network meta-analysis, we summarized mechanical ventilation strategies based on the low tidal volume among patients with moderate to severe ARDS. To the best of our knowledge, this study is the first to use network meta-analysis to compare different mechanical ventilation strategies. The major findings from our present analysis are as follows. (1) No ventilation strategy was significantly superior to other strategies in terms of in-hospital death, ventilator-free days, and barotrauma. (2) This technique is not applicable to studies involving deaths in 28 days because of the considerable inconsistency found in global and local inconsistency tests. (3) The overall quality of the evidence is moderate-to-low or low for the primary and secondary outcomes. Given that the use of ventilators should be monitored at all times and the parameters should be adjusted by the clinician according to the condition of the patients, blinding is not suitable for these random clinical trials. Thus, it is difficult to improve the overall quality of RCTs. The research population in our meta-analysis was mainly European and American, and 4 RCTs were conducted in Asia [15, 19, 20, 25]. The sample size was 334, accounting for 7.57% of the total. We analyzed 9 RCTs conducted in European and American countries, and the results were the same as before. The heterogeneous study population did not influence the results.
The optimal lung recruitment maneuvers and PEEP levels for patients with ARDS remain unclear. Sarina et al. summarized approaches to setting PEEP, but the optimal approach to setting PEEP has not yet been firmly established [27]. A pairwise meta-analysis suggested that the use of higher PEEP is unlikely to improve clinical outcomes among unselected patients with ARDS [28]. Our network meta-analysis also showed that no approaches to setting PEEP were significantly superior to others. The reason may be that the theoretical beneficial effects of higher PEEP on oxygenation can be offset by heart–lung interactions. Therefore, the approach to find the optimal PEEP needs more study. The recruitment maneuver can open up the collapsed lung, and PEEP can maintain alveolar stability, but a recent study suggested that RM + PEEP titration and RM + lower PEEP had no difference in terms of 28-day mortality and ICU mortality in patients with moderate–severe ARDS [29], and another two pairwise meta-analyses suggested that RM had no advantageous effect on mortality [10, 30]. These results were consistent with the results of our network meta-analysis. The negative result may be caused by studies that did not take into account the lung recruitability. ARDS patients enrolled in the RCTs were randomized, and they did not receive an assessment of lung recruitability, which influences the effect of RM and PEEP. In these RCTs, more pneumonia patients were recruited, except two RCTs [18, 20]. Pneumonia patients have low lung recruitability, which may cause negative results. Guo et al. found that high PEEP reduced mortality in a subgroup of patients with ARDS who responded to increased PEEP by improved oxygenation [8]. This study demonstrated that lung recruitability is important for the effect of RM and PEEP level. Lung recruitability should be considered for further RCTs.
In our network meta-analysis, five combinations of RM and PEEP levels were enrolled, and RM + PEEP titration versus low PEEP were the most common points of comparison. In our study, the PEEP level in the lower PEEP group was 7.1 ± 1.8 mmHg [17] to 12 ± 3 mmHg [25] on day 1, which was lower than that in the control groups. The high PEEP-FIO2 strategy proposed by the ALVEOLI trial was included in the higher PEEP group. The PEEP level in the higher PEEP group was 14.6 ± 3.2 mmHg [17] to 16 ± 4 mmHg [24] on day 1. The PEEP level in the PEEP titration group was 13 ± 3 mmHg [25] to 17 ± 6 mmHg [24] on day 1. In Beitler's research, the PEEP level in the higher group was lower than that in the titration group, which may be caused by the inconsistent baseline PEEP between the two groups.
Network meta-analysis is a technique to meta-analyze more than two treatments at the same time. The advantage of network meta-analysis is that it can be used to estimate the probability that a particular treatment is the best, the second best, etc. [31]. As such, we used network meta-analysis to provide relative efficacy estimates among all interventions; however, some techniques have never been directly compared. In this study, the differences among in-hospital death, ventilator-free days, and barotrauma were not significant. This finding is consistent with previous conventional pairwise meta-analyses. In terms of death at 28 days, an inconsistency was found globally and locally in the tests, so the network meta-analysis was improper for death at 28 days. For ranking probabilities, in terms of in-hospital death and ventilator-free days, RM + lower PEEP had the highest SUCRA and the highest Rank 1 possibility. These results were beyond our expectations. PEEP titration is a personalized treatment for obtaining the optimal PEEP; several methods have been proposed for PEEP titration in an individual patient with ARDS, including gas change, compliance, pressure–volume curve, and esophageal pressure [32]. However, RM + PEEP titration was not the best recommended strategy in our network meta-analysis. Among the studies enrolled in our analysis, a PEEP titration strategy based on respiratory-system compliance [19, 22, 23], oxygen saturation [21, 26], and esophageal pressure [18, 24] was conducted. The different approaches for RM and PEEP titration may be the reason. Although the decrease in driving pressure is strongly associated with increased survival, no studies have used this parameter as the PEEP titration strategy [33]. These factors may explain why RM + PEEP titration was not the first choice in our analysis. The rank possibility of RM + lower PEEP is superior to RM + PEEP titration, and the low lung recruitability was the main reason. A recent finding showed that the open lung strategy is not satisfactory using PEEP up to 15 cmH2O and plateau pressure up to 30 cmH2O; high pressure levels are required for opening the lung [34]. This result is attributed to the heterogeneity of pulmonary lesions among patients with severe ARDS; maximum compliance was determined by overdistending the normal tissue, thereby resulting in adverse effects compared with alveolar recruitment.
In terms of barotrauma, lower PEEP is the safest strategy according to the SUCRA, which is consistent with theoretical and clinical understanding. However, RM + PEEP titration had the highest risk of barotrauma. One reason is that the baseline level of PEEP was higher in the titration group than in the higher group in Bietler’s research. Another reason is ascribed to the RM + higher PEEP strategy recruiting more collapsed alveoli, which can reduce shear stress [35] and improve ventilation-to-perfusion mismatch.
5 Limitations
This study has several limitations. First, the modes of ventilation are diverse. Ventilator models used in clinical trials are inconsistent, and we classified the mechanical ventilation strategies, which may cause bias. Second, ventilator parameters may change anytime according to patients, and the same strategy may include different parameters that may influence the judgment of outcomes. A few articles used the median and the first and third quartiles to describe the results. We used an equation to transform the data, which may decrease the reliability of the results.
6 Conclusion
In this network meta-analysis, we classified mechanical ventilation strategies on the basis of recruitment maneuvers and different PEEP levels for mechanical ventilation among patients with ARDS. None of the strategies were significantly superior to the others. According to the relative ranking recommended by the Bayesian frameworks, RM + lower PEEP showed the highest probability of reducing the risk of in-hospital death and reducing ventilator-free days, whereas lower PEEP showed the highest probability of benefitting barotrauma. The overall quality of the evidence is low, and thus, further research should be conducted.
Availability of Data and Materials
All data analysed during this study are included in this published article.
Abbreviations
- ARDS:
-
Acute respiratory distress syndrome
- DIC:
-
Deviance information criterion
- ICU:
-
Intensive care unit
- PEEP:
-
Positive end-expiratory pressure
- RM:
-
Recruitment maneuver
- RR:
-
Risk ratios
- SMD:
-
Standard mean difference
References
Howell MD, Davis AM. Management of ARDS in adults. JAMA. 2018;319(7):711–2.
Ashbaugh DG, Bigelow DB, Petty TL, Levine BE. Acute respiratory distress in adults. Lancet. 1967;2(7511):319–23.
Brower RG, Matthay MA, Morris A, Schoenfeld D, Thompson BT, Wheeler A, Acute Respiratory Distress Syndrome N. Ventilation with lower tidal volumes as compared with traditional tidal volumes for acute lung injury and the acute respiratory distress syndrome. N Engl J Med. 2000;342(18):1301–8.
Papazian L, Forel JM, Gacouin A, Penot-Ragon C, Perrin G, Loundou A, Jaber S, Arnal JM, Perez D, Seghboyan JM, et al. Neuromuscular blockers in early acute respiratory distress syndrome. N Engl J Med. 2010;363(12):1107–16.
Guerin C, Reignier J, Richard JC, Beuret P, Gacouin A, Boulain T, Mercier E, Badet M, Mercat A, Baudin O, et al. Prone positioning in severe acute respiratory distress syndrome. N Engl J Med. 2013;368(23):2159–68.
Ferguson ND, Fan E, Camporota L, Antonelli M, Anzueto A, Beale R, Brochard L, Brower R, Esteban A, Gattinoni L, et al. The Berlin definition of ARDS: an expanded rationale, justification, and supplementary material. Intensive Care Med. 2012;38(10):1573–82.
Fan E, Del Sorbo L, Goligher EC, Hodgson CL, Munshi L, Walkey AJ, Adhikari NKJ, Amato MBP, Branson R, Brower RG, et al. An Official American Thoracic Society/European Society of Intensive Care Medicine/Society of Critical Care Medicine Clinical Practice Guideline: mechanical ventilation in adult patients with acute respiratory distress syndrome. Am J Respir Crit Care Med. 2017;195(9):1253–63.
Guo L, Xie J, Huang Y, Pan C, Yang Y, Qiu H, Liu L. Higher PEEP improves outcomes in ARDS patients with clinically objective positive oxygenation response to PEEP: a systematic review and meta-analysis. BMC Anesthesiol. 2018;18(1):172.
Goligher EC, Hodgson CL, Adhikari NKJ, Meade MO, Wunsch H, Uleryk E, Gajic O, Amato MPB, Ferguson ND, Rubenfeld GD, et al. Lung recruitment maneuvers for adult patients with acute respiratory distress syndrome. A systematic review and meta-analysis. Ann Am Thorac Soc. 2017;14(Supplement_4):S304–11.
Pensier J, de Jong A, Hajjej Z, Molinari N, Carr J, Belafia F, Chanques G, Futier E, Azoulay E, Jaber S. Effect of lung recruitment maneuver on oxygenation, physiological parameters and mortality in acute respiratory distress syndrome patients: a systematic review and meta-analysis. Intensive Care Med. 2019;45(12):1691–702.
Hutton B, Salanti G, Caldwell DM, Chaimani A, Schmid CH, Cameron C, Ioannidis JP, Straus S, Thorlund K, Jansen JP, et al. The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: checklist and explanations. Ann Intern Med. 2015;162(11):777–84.
Brower RG, Lanken PN, MacIntyre N, Matthay MA, Morris A, Ancukiewicz M, Schoenfeld D, Thompson BT, National Heart L, Blood Institute ACTN. Higher versus lower positive end-expiratory pressures in patients with the acute respiratory distress syndrome. N Engl J Med. 2004;351(4):327–36.
Salanti G, Ades AE, Ioannidis JP. Graphical methods and numerical summaries for presenting results from multiple-treatment meta-analysis: an overview and tutorial. J Clin Epidemiol. 2011;64(2):163–71.
Wan X, Wang W, Liu J, Tong T. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol. 2014;14:135.
Lim CM, Jung H, Koh Y, Lee JS, Shim TS, Lee SD, Kim WS, Kim DS, Kim WD. Effect of alveolar recruitment maneuver in early acute respiratory distress syndrome according to antiderecruitment strategy, etiological category of diffuse lung injury, and body position of the patient. Crit Care Med. 2003;31(2):411–8.
Meade MO, Cook DJ, Guyatt GH, Slutsky AS, Arabi YM, Cooper DJ, Davies AR, Hand LE, Zhou Q, Thabane L, et al. Ventilation strategy using low tidal volumes, recruitment maneuvers, and high positive end-expiratory pressure for acute lung injury and acute respiratory distress syndrome: a randomized controlled trial. JAMA. 2008;299(6):637–45.
Mercat A, Richard JC, Vielle B, Jaber S, Osman D, Diehl JL, Lefrant JY, Prat G, Richecoeur J, Nieszkowska A, et al. Positive end-expiratory pressure setting in adults with acute lung injury and acute respiratory distress syndrome: a randomized controlled trial. JAMA. 2008;299(6):646–55.
Talmor D, Sarge T, Malhotra A, O’Donnell CR, Ritz R, Lisbon A, Novack V, Loring SH. Mechanical ventilation guided by esophageal pressure in acute lung injury. N Engl J Med. 2008;359(20):2095–104.
Huh JW, Jung H, Choi HS, Hong SB, Lim CM, Koh Y. Efficacy of positive end-expiratory pressure titration after the alveolar recruitment manoeuvre in patients with acute respiratory distress syndrome. Crit Care. 2009;13(1):R22.
Xi XM, Jiang L, Zhu B, group RM. Clinical efficacy and safety of recruitment maneuver in patients with acute respiratory distress syndrome using low tidal volume ventilation: a multicenter randomized controlled clinical trial. Chin Med J (Engl). 2010;123(21):3100–5.
Hodgson CL, Tuxen DV, Davies AR, Bailey MJ, Higgins AM, Holland AE, Keating JL, Pilcher DV, Westbrook AJ, Cooper DJ, et al. A randomised controlled trial of an open lung strategy with staircase recruitment, titrated PEEP and targeted low airway pressures in patients with acute respiratory distress syndrome. Crit Care. 2011;15(3):R133.
Kacmarek RM, Villar J, Sulemanji D, Montiel R, Ferrando C, Blanco J, Koh Y, Soler JA, Martinez D, Hernandez M, et al. Open lung approach for the acute respiratory distress syndrome: a pilot randomized controlled trial. Crit Care Med. 2016;44(1):32–42.
Cavalcanti AB, Suzumura EA, Laranjeira LN, Paisani DM, Damiani LP, Guimaraes HP, Romano ER, Regenga MM, Taniguchi LNT, Writing Group for the Alveolar Recruitment for Acute Respiratory Distress Syndrome Trial I, et al. Effect of lung recruitment and titrated positive end-expiratory pressure (PEEP) vs low PEEP on mortality in patients with acute respiratory distress syndrome: a randomized clinical trial. JAMA. 2017;318(14):1335–45.
Beitler JR, Sarge T, Banner-Goodspeed VM, Gong MN, Cook D, Novack V, Loring SH, Talmor D, Group EP-S. Effect of titrating positive end-expiratory pressure (PEEP) with an esophageal pressure-guided strategy vs an empirical high PEEP-Fio2 strategy on death and days free from mechanical ventilation among patients with acute respiratory distress syndrome: a randomized clinical trial. JAMA. 2019;321(9):846–57.
Kung SC, Hung YL, Chen WL, Wang CM, Chang HC, Liu WL. Effects of stepwise lung recruitment maneuvers in patients with early acute respiratory distress syndrome: a prospective, randomized, controlled trial. J Clin Med. 2019;8(2):231.
Constantin JM, Jabaudon M, Lefrant JY, Jaber S, Quenot JP, Langeron O, Ferrandiere M, Grelon F, Seguin P, Ichai C, et al. Personalised mechanical ventilation tailored to lung morphology versus low positive end-expiratory pressure for patients with acute respiratory distress syndrome in France (the LIVE study): a multicentre, single-blind, randomised controlled trial. Lancet Respir Med. 2019;7(10):870–80.
Wilke T, Mueller S, Bauer S, Pitura S, Probst L, Ratsch BA, Salwender H. Treatment of relapsed refractory multiple myeloma: which new PI-based combination treatments do patients prefer? Patient Prefer Adherence. 2018;12:2387–96.
Walkey AJ, Del Sorbo L, Hodgson CL, Adhikari NKJ, Wunsch H, Meade MO, Uleryk E, Hess D, Talmor DS, Thompson BT, et al. Higher PEEP versus lower PEEP strategies for patients with acute respiratory distress syndrome a systematic review and meta-analysis. Ann Am Thorac Soc. 2017;14(Suppl 4):S297–303.
Zheng X, Jiang Y, Jia H, Ma W, Han Y, Li W. Effect of lung recruitment and titrated positive end-expiratory pressure (PEEP) versus low PEEP on patients with moderate-severe acute respiratory distress syndrome: a systematic review and meta-analysis of randomized controlled trials. Ther Adv Respir Dis. 2019;13:1753466619858228.
Cui Y, Cao R, Wang Y, Li G. Lung recruitment maneuvers for ARDS patients: a systematic review and meta-analysis. Respiration. 2019;99:1–13.
Mills EJ, Thorlund K, Ioannidis JP. Demystifying trial networks and network meta-analysis. BMJ. 2013;346:f2914.
Hess DR. Recruitment maneuvers and PEEP titration. Respir Care. 2015;60(11):1688–704.
Amato MB, Meade MO, Slutsky AS, Brochard L, Costa EL, Schoenfeld DA, Stewart TE, Briel M, Talmor D, Mercat A, et al. Driving pressure and survival in the acute respiratory distress syndrome. N Engl J Med. 2015;372(8):747–55.
Cressoni M, Chiumello D, Algieri I, Brioni M, Chiurazzi C, Colombo A, Colombo A, Crimella F, Guanziroli M, Tomic I, et al. Opening pressures and atelectrauma in acute respiratory distress syndrome. Intensive Care Med. 2017;43(5):603–11.
Lachmann B. Open up the lung and keep the lung open. Intensive Care Med. 1992;18(6):319–21.
Acknowledgements
We thank Bin Xiong, Li Xu, and Yi Liu, from the Second Affiliated Hospital of Chongqing Medical University, for their assistance in analysing data and formatting the manuscript.
Funding
This work was supported by grants from the Chongqing medical scientific research project (Joint project of Chongqing Health Commission and Science and Technology Bureau) (Grant No. 2020FYYX025) and the Science and Technology Research Program of Chongqing Municipal Education Commission Grant (No. KJQN202000411).
Author information
Authors and Affiliations
Contributions
W.H., P.W. searched the scientific literature, W.H. drafted the manuscript. W.H., B.H., X.C. and H.S. performed the statistical analyses and revised the manuscript. W.H., H.D. and Y.C. participated in data interpretation and drafted the report. A.Z. conceived of the study and contributed data. A.Z. made important revisions to the draft report. A.Z. contributed equally to this paper and are joint corresponding authors. W.H. is first author. All authors have read and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Ethics Approval and Consent to Participate
Not applicable.
Consent for Publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Huang, W., Wang, P., Huang, B. et al. Efficacy and Safety of Different Mechanical Ventilation Strategies for Patients with Acute Respiratory Distress Syndrome: Systematic Review and Network Meta-analysis. Intensive Care Res 3, 50–60 (2023). https://doi.org/10.1007/s44231-022-00015-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s44231-022-00015-2