Abstract
Background
Nearly 15% colorectal cancer (CRC) patients received ileostomy, while surgical site infection (SSI) is a common complication after ileostomy wound closure. Purse-string closure was reported to reduce SSI rate in ileostomy wound closure compared with conventional linear closure, but had never been systematically reported in CRC patients. The present study aimed to compare the short-term outcomes between purse-string and conventional closure in Chinese CRC patients.
Patients and methods
A total of 57 CRC patients underwent ileostomy wounds closure in the Second Affiliated Hospital of Zhejiang University during November, 2015 and October, 2017 were retrospectively reviewed. Twenty-nine received purse-string closure while the others received conventional closure. The short-term outcomes including SSI rate, scar length, pain score and hospital stay were reviewed and analyzed.
Results
There were no significant differences in the characteristics of the patients between two groups. The SSI rate was similar within two groups (10.3% vs 10.7%, p = 1.000). The purse-string closure group had a significantly short scar length (1.66 cm vs 5.30 cm, p < 0.0001), but had no difference in operation time, hospital stay and postoperative pain.
Conclusion
The present study did not find superiority of Purse-string closure in SSI rate control. It seemed only had a cosmetic effect according to its shorter scar length.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
There were an increasing number of patients receiving temporarily ileostomy, and one of the most common causes is colorectal cancer (CRC) [1,2,3]. CRC has been one of the leading cancers both worldwide and in China [4, 5]. Radical resection is the major therapy for non-metastatic and resectable metastatic CRC patients. However, nearly 15% CRC patients require simultaneous temporarily ileostomy to reduce anastomotic leakage risk [6, 7]. In general, rectal cancer patients who underwent neoadjuvant radiotherapy occupy the largest percentage in these patients, as preoperative radiotherapy was reported to increase anastomotic leakage risk [8].
Temporally ileostomy closure was usually performed 3 to 6 months later after the first operation [9]. Surgical site infection (SSI) was a frequent postoperative complication with an incidence varying from 0 to 41% [10,11,12,13,14]. Purse-string closure was first reported by Banerjee A and we introduced this technique in November, 2015 [15]. In brief, there were two major differences between purse-string closure and conventional linear closure. The purse-string closure made a circular incision, which was closed by purse-string suture using 2–0 Prolene™. While the conventional closure made a fusiformis incision, and it was lastly closed by interrupted sutured using 1–0 MERSILK™ non-absorbable suture. Therefore, a round skin gap was left after operation in purse-string closure group and it would get self-healed within 3 weeks [13]. Several studies, both prospective and retrospective, had reported purse-string closure reduced SSI rate to less than 10% [13, 14, 16,17,18,19]. However, the primary disease of patients enrolled in these studies included both benign (inflammation bowel disease, traumatic bowel perforation, et al.) and malignant (CRC) diseases. While there is few studies specifically discussing purse-string in CRC patients. In addition, half of the researches reported a more than 20% SSI rate in conventional closure group, which was considered unacceptable in daily clinical practice [13, 14, 16]. Therefore, we would evaluate the SSI rate in conventional closure group based on our own CRC patients.
The present study aimed to compare the short-term outcomes, including SSI rate, scar length, operation time, postoperative pain and hospital stay, between purse-string and conventional closure of ileostomy wounds in CRC patients. We set SSI rate as the primary comparative factor, while the operation time, hospital stay, postoperative pain and scar length were set as the secondary comparative factors.
2 Patients and methods
2.1 Patients
CRC patients underwent ileostomy wounds closure in the Second Affiliated Hospital of Zhejiang University (SAHZU) during November, 2015 and October, 2017 were consecutively enrolled. All patients were previously pathologically diagnosed with CRC and received radical carcinoma resection and simultaneous temporary ileostomy. In the present operation, each patient received either purse-string ileostomy closure or conventional ileostomy closure according to surgeons’ own choice. The baseline variables included: age, sex, body mass index (BMI), American Society of Anesthesiology (ASA) score, diabetes, hypertension, smoking, time from primary surgery to closure, patient-controlled analgesia (PCA) pump using, primary tumor location, radiotherapy, chemotherapy within 3 months, and pathological cancer stage. The study was approved by the Ethics Committee of SAHZU(2023-LSY-0126).
2.2 Interventions
Ileostomy wounds closure were performed within 8 months after the radical tumor resection. The operations were performed in the Department of Colorectal Surgery and Oncology of SAHZU by three experienced surgeons (Dr. Jun Li, Dr. Li-Feng Sun and Dr. Dong Xu).
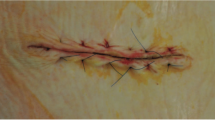
For purse-string closure, the standard operative technical consisted of a circular incision around the ileostomy (approximately 4.0 cm in diameter) with dissection into the peritoneal cavity and formal resection of the ileostomy. A side-to-side stapled anastomosis was performed with an Autosuture™ GIA™ 80 reloadable stapler to join the broken ends of ileum. The resulting enteroenterotomy was overstapled with a staple reload. Abdominal closure was achieved using 1–0 Ethicon Coated VICRYL™ suture and the subcutaneous layer was closed by 3–0 MERSILK™ suture (see in Fig. 1a). Abdominal wound was incubated with povidone iodine (PVP-I) for 30 s, and washed-out with warm sterile saline after fascial closure. At last, the circular skin incision was closed using a purse-string subcuticular suture with 2–0 Prolene™, Ethicon (see in Fig. 1b-d).
Procedure for purse-string group in skin wound closure. a the subcutaneous layer was first closed by 3–0 MERSILK™ non-absorbable suture. b the circular skin incision was closed using a purse-string subcuticular suture with 2–0 Prolene™. c the Prolene™ was tightened to shrink skin wound. d Purse-string skin closure was completed
While for conventional ileostomy closure, the surgeons made a fusiformis incision around the ileostomy (approximately 5–6 cm in length). The following steps were similar to the purse-string closure described above except the skin closure. The skin incision was interrupted sutured using 1–0 MERSILK™ non-absorbable suture.
During the operation, all patients received a single dose of intravenous antibiotics: Cefmetazole (2 g per patient). Standard intravenous anesthesia was performed and ventilation maintained with 80 percent oxygen during surgery. All patients were requested to mobilize and given a full liquid diet on the first day after surgery. They were discharged from hospital when mobile, independent in activities of daily living, and medically fit. The sutures were taken out 18–21 days and 7–10 days after operation for the purse-string and the conventional ileostomy respectively in outpatient department according to superficial recovery.
2.3 Short-term outcome measurements
The operation time was recorded in the operation system, calculated from cutting skin to suture finished. Pain score was assessed and recorded by nurses every 8:00 AM for three days after surgery using visual analogue scale (VAS) [13]. Surgical site infection (SSI) was defined as any infection occurs within 30 days after surgery and involves only skin and subcutaneous tissue of the incision by the Centers for Disease Control (CDC) [20]. It was assessed and recorded by three attending surgeons (Dr. Jun Li, Dr. Li-Feng Sun and Dr. Dong Xu) routinely until 30 days after operation. The postoperative hospital stay was calculated from the operation day to the date of discharge. The scar length was measured three weeks after operation.
2.4 Statistical analysis
All data was stored in Microsoft EXCEL 2017. Student’s t test was performed to compare continues and normal distribution data, like operation time and scar length between two groups. Data without normal distribution, like postoperation hospital stay and postoperative pain, was showed as mean + interquartile range (IQR). And nonparametric test, like Mann–Whitney test was performed. The distribution of cancer stage and ASA score was also compared by Mann–Whitney test. Categorical data, like SSI rate, tumor location were compared using Fisher’s exact test. All statistical analysis was performed using Graphpad Prism 6.0c (GraphPad Software Inc., San Diego, CA, USA). A two- sided P-value of 0.05 or less was considered to indicate statistical significance.
3 Results
3.1 Patients’ characteristics
Between November, 2015 and October, 2017, a total of 57 patients were finally enrolled. Among them, 29 patients received purse-string closure while the other 28 patients were performed conventional closure. The patient populations in both groups were well matched in most respects. The primary tumor located mostly in rectum in both groups. We also compared factors which might affect the status of ileum and anastomotic stoma recovery (like radiotherapy, chemotherapy, smoking, diabetes and hypertension) but found no significant difference. Additionally, pathological stage of the primary tumor was also analogous. As some rectal cancer patients received pathologically completely response (pCR), there had been stage 0 in both groups. There were 3 patients with stage IV. Two of them were diagnosed with liver metastasis during operation while pre-operative CT scan showed no evidence. The other patient was diagnosed with lung metastasis, we performed radical surgery because of his severe symptoms in primary tumor. It is rare to have an ileostomy after radical right colectomy. However, we have three right colon cancer patients underwent ileostomy in the present study. These three patients also had intestinal obstruction on the basis of right colon cancer. During the operation, patients showed serious intestinal edema, which would have high risk of anastomotic fistula after direct anastomosis. Therefore, we chose performed anastomosis and ileostomy to reduce the occurrence of anastomotic fistula as much as possible. More details of the patients’ baseline were shown in Table 1.
3.2 Primary comparative factor
The overall SSI rate in the whole cohort was 10.5%. A total of six patients developed SSI after operation, and each group had three. There was no significant difference of SSI rate within two groups (10.3% vs 10.7%, p = 1.000). Among the six SSI patients, half were diagnosed in-hospital. One patient in the purse-string closure group was re-admitted due to severe SSI. All SSI patients developed pain, localized swelling and erythema. Daily dressing-change was performed in all SSI patients and two of them received antibiotics therapy. Within two months, all these patients got recover.
3.3 Secondary comparative factors
The mean operation time was similar in both groups (91.45 min versus 94.54 min). There were no intraoperative complications in either group. The mean postoperative hospital stay was 8.45 days in the purse-string closure and 6.75 days in the conventional closure without significant difference. Notably, one patient in the purse-string closure group stayed 58 days after surgery due to anastomotic fistula, which was the longest postoperative hospital stay in the present study. The postoperative pain was similar and less than 2 for three days in both groups, which was tolerable for all patients.
The length of scar was measured three weeks after operation when patients came back for review. Purse-string closure had a much shorter scar length than conventional closure (1.66 cm versus 5.30 cm, p < 0.0001, see in Fig. 2). Although purse-string closure made a circular skin incision with a diameter of 4.0 cm, it resulted in a little wound after tightening Prolene™ (see in Fig. 1c and d). Therefore, it indicated purse-string might have a cosmetic effect, and it might be the only different short-term outcome. All these comparative factors were shown in Table 2.
4 Discussion
The present study compared the short-term outcomes, including SSI rate, scar length, operation time, postoperative pain and hospital stay, between purse-string and conventional closure of ileostomy wounds in CRC patients. We demonstrated purse-string showed none superiority in SSI rate control. Our research, for the first time as we know, focused on ileostomy closure specifically in CRC patients.
Several studies (three randomized controlled trails, three retrospective studies and one meta-analysis) had reported an under 10% SSI rate in purse-string group, and mostly under 5% [13, 14, 16,17,18,19, 21]. While for conventional closure, there were four studies reporting a SSI rate that was higher than 20% [13, 14, 16, 21]. In our research, the SSI rate showed no difference and the conventional closure group’s SSI rate was more acceptable in clinical practice. One major reason was our protocol required incubating abdominal wound with PVP-I for 30 s after fascial closure and before skin closure. As PVP-I is a common disinfectant used during operation, we believed it contributed to the reduction of SSI rate. Therefore, incubating abdominal wound with PVP-I, not only washout by warm saline should be considered during ileostomy closure. The other reason was our study only enrolled Chinese CRC patients. These patients had lower BMI (average < 23.0 kg/m2) and younger age (average < 60) than western countries [13, 14, 16,17,18,19]. While higher BMI was reported as a risk factor of SSI, and an older age also independently predicted a higher risk of SSI [22, 23], it might partly explain the phenomenon in our research. Nevertheless, surgeons should still carefully pay attention to the applicability of purse-string closure in CRC patients.
Except SSI rate, our data showed no difference in operation time, postoperative hospital stay, postoperative pain between two groups, which was similar to the previous studies [13, 14, 16,17,18,19]. A shorter scar length was resulted from the purse-string closure because of tightening purse-string, which indicated a cosmetic advance of purse-string closure. Even though our research only had a follow-up of three weeks, it was confirmed by longer follow-up in other studies [13, 21]. However, scar length was not the primary comparative factor in our study, and cosmetic effect was evaluated not only by scar length. In the future study, a more scientific scar assessment system, like Vancouver Scar Scale should be applied [24].
There were still some limitations in the present study. Firstly, it was a single center retrospective study with limited patients. Therefore, the baseline data of the two groups of patients was not very balanced, even though with no statically significance. While as the purse-string closure showed no superiority in CRC patients, a larger population randomized controlled trail might be carefully considered in the future. Furthermore, as a retrospective study, patients were not randomly assigned to each group. And it might inevitably lead to selection bias.
In conclusion, the present study compared purse-string closure and conventional closure of ileostomy wound in Chinese CRC patients. It did not find superiority of Purse-string closure in SSI rate control, but seemed only have a cosmetic effect. Therefore, surgeons should carefully recommend purse-string ileostomy closure to CRC patients.
Availability of data and materials
The datasets generated or analyzed during this study are available from the corresponding author on reasonable request.
References
Carlsson E, Berndtsson I, Hallen AM, Lindholm E, Persson E. Concerns and quality of life before surgery and during the recovery period in patients with rectal cancer and an ostomy. J Wound Ostomy Continence Nurs. 2010;37:654–61.
Dabirian A, Yaghmaei F, Rassouli M, Tafreshi MZ. Quality of life in ostomy patients: a qualitative study. Patient Prefer Adherence. 2010;5:1–5.
Anaraki F, Vafaie M, Behboo R, Maghsoodi N, Esmaeilpour S, et al. Quality of life outcomes in patients living with stoma. Indian J Palliat Care. 2012;18:176–80.
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, et al. Global cancer statistics, 2012. CA Cancer J Clin. 2015;65:87–108.
Chen W, Sun K, Zheng R, Zeng H, Zhang S, et al. Cancer incidence and mortality in China, 2014. Chin J Cancer Res. 2018;30:1–12.
Daams F, Luyer M, Lange JF. Colorectal anastomotic leakage: aspects of prevention, detection and treatment. World J Gastroenterol. 2013;19:2293–7.
Banaszkiewicz Z, Woda LP, Zwolinski T, Tojek K, Jarmocik P, et al. Intestinal stoma in patients with colorectal cancer from the perspective of 20-year period of clinical observation. Przeglad gastroenterologiczny. 2015;10:23–7.
Qin Q, Ma T, Deng Y, Zheng J, Zhou Z, et al. Impact of preoperative radiotherapy on anastomotic leakage and stenosis after rectal cancer resection: post hoc analysis of a randomized controlled trial. Dis Colon Rectum. 2016;59:934–42.
Herrle F, Sandra-Petrescu F, Weiss C, Post S, Runkel N, et al. Quality of life and timing of stoma closure in patients with rectal cancer undergoing low anterior resection with diverting stoma: a multicenter longitudinal observational study. Dis Colon Rectum. 2016;59:281–90.
Hackam DJ, Rotstein OD. Stoma closure and wound infection: an evaluation of risk factors. Can J Surg. 1995;38:144–8.
Sutton CD, Williams N, Marshall LJ, Lloyd G, Thomas WM. A technique for wound closure that minimizes sepsis after stoma closure. ANZ J Surg. 2002;72:766–7.
Lahat G, Tulchinsky H, Goldman G, Klauzner JM, Rabau M. Wound infection after ileostomy closure: a prospective randomized study comparing primary vs. delayed primary closure techniques. Tech Coloproctol. 2005;9:206–8.
Reid K, Pockney P, Pollitt T, Draganic B, Smith SR. Randomized clinical trial of short-term outcomes following purse-string versus conventional closure of ileostomy wounds. Br J Surg. 2010;97:1511–7.
Alvandipour M, Gharedaghi B, Khodabakhsh H, Karami MY. Purse-string versus linear conventional skin wound closure of an ileostomy: a randomized clinical trial. Ann Coloproctol. 2016;32:144–9.
Banerjee A. Pursestring skin closure after stoma reversal. Dis Colon Rectum. 1997;40:993–4.
Dusch N, Goranova D, Herrle F, Niedergethmann M, Kienle P. Randomized controlled trial: comparison of two surgical techniques for closing the wound following ileostomy closure: purse string vs direct suture. Colorectal Dis. 2013;15:1033–40.
Habbe N, Hannes S, Liese J, Woeste G, Bechstein WO, et al. The use of purse-string skin closure in loop ileostomy reversals leads to lower wound infection rates–a single high-volume centre experience. Int J Colorectal Dis. 2014;29:709–14.
Suh YJ, Park JW, Kim YS, Park SC, Oh JH. A beneficial effect of purse-string skin closure after ileostomy takedown: a retrospective cohort study. Int J Surg. 2014;12:615–20.
Wada Y, Miyoshi N, Ohue M, Noura S, Fujino S, et al. Comparison of surgical techniques for stoma closure: a retrospective study of purse-string skin closure versus conventional skin closure following ileostomy and colostomy reversal. Mol Clin Oncol. 2015;3:619–22.
National Healthcare Safety Network, Centers for Disease Control and Prevention. Surgical site infection (SSI) event. 2017. http://www.cdc.gov/nhsn/pdfs/pscmanual/9pscssicurrent.pdf.
McCartan DP, Burke JP, Walsh SR, Coffey JC. Purse-string approximation is superior to primary skin closure following stoma reversal: a systematic review and meta-analysis. Tech Coloproctol. 2013;17:345–51.
Kaye KS, Schmit K, Pieper C, Sloane R, Caughlan KF, et al. The effect of increasing age on the risk of surgical site infection. J Infect Dis. 2005;191:1056–62.
Abdallah DY, Jadaan MM, McCabe JP. Body mass index and risk of surgical site infection following spine surgery: a meta-analysis. Eur Spine J. 2013;22:2800–9.
Bae SH, Bae YC. Analysis of frequency of use of different scar assessment scales based on the scar condition and treatment method. Arch Plast Surg. 2014;41:111–5.
Acknowledgements
We gratefully thank Dr. Hai-Ting Xie, Dr. Zhan-Huai Wang, Dr. Shao-Jun Yu, Dr. Ye-Ting Hu, Dr. Dong Xu and Dr. Li-Feng Sun in helping perform the operations.
Funding
This work was supported by the Huadong Medicine Joint Funds of the Zhejiang Provincial Natural Science Foundation of China under Grant No. LHDMY22C060002, the National Natural Science Foundation of China (82103684, 11932017, 82172851), the Fundamental Research Funds for the Central Universities (No. 226–2022-00009) and the Natural Science Foundation of Zhejiang Province (LQ20H180014).
Author information
Authors and Affiliations
Contributions
Xiang-Xing Kong, Ke-Feng Ding and Jun Li designed the study. Yu-Rong Jiao analyzed the data and writes the manuscript. Xin-Bin Zhou, Yao Ye and Qian Xiao collected the data and figures. The author(s) read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Written informed consent for publication of this paper was obtained from the Second Affiliated Hospital of Zhejiang University, School of Medicine. Written informed consent was obtained from all the participants prior to the enrollment of this study.
Consent for publication
Written informed consent was obtained from all the participants for publication.
Competing interests
The authors have declared no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jiao, YR., Zhou, XB., Ye, Y. et al. Short-term outcomes following purse-string versus conventional closure of ileostomy wounds in Chinese colorectal cancer patients — a single center retrospective study. Holist Integ Oncol 2, 2 (2023). https://doi.org/10.1007/s44178-023-00025-0
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44178-023-00025-0