Abstract
Interventions targeting anhedonia in depression demonstrate encouraging results in adults but are lacking for adolescents. Here, we have adapted a brief imagery-based intervention (IMAGINE), which has shown promising results in reducing symptoms of depression in young people, to focus specifically on reducing symptoms of anhedonia (IMAGINE-Positive). We augment positive mental imagery generation with techniques to upregulate positive affect. Eight participants completed the four-session intervention. Data on feasibility and acceptability were collected. Questionnaires of symptomology and cognitive mechanisms (e.g. depression, anhedonia and future imagery vividness) were administered at pre-intervention, post-intervention and 3-month follow-up. The intervention was feasible to deliver and acceptable to participants. There was a large reduction in depression symptom scores from pre- to post-intervention (d = 1.12) and 63% of participants showed reliable improvement (RI), which was maintained at follow-up (d = 2.51, RI = 86%). Although there were only small reductions in anhedonia from pre to post (d = 0.38, RI = 0), there was a large reduction from pre to follow-up (d = 1.28, RI = 29%). There were also large increases in positive future imagery vividness (post, d = − 1.08, RI = 50%; follow-up, d = − 2.02, RI = 29%). Initial evidence suggests that IMAGINE-Positive is feasible and acceptable and may have clinical utility, but future randomised controlled trials are needed to further evaluate efficacy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Depression in adolescents is common (Thapar et al., 2012) and a leading cause of illness and disability (World Health Organization [WHO], 2021a). Early onset of depression is associated with poor psychosocial outcomes (Clayborne et al., 2019) including social dysfunction, academic difficulties and unemployment (Fombonne et al., 2001; Kim-Cohen et al., 2003), as well as recurrent episodes and increased risk of chronicity (Angst et al., 2009; Essau et al., 2010; Richards, 2011). Despite this, young people may struggle to access the right level of support when they require it. There has been a global lack of investment in mental health services in the face of increased service demands (WHO, 2021b) which, in the UK, has led to long waiting lists, increased eligibility criteria of specialist services and disparities in service provision (Care Quality Commission [CQC], 2018). Consequently, young people often only receive access to services once their mental health has deteriorated or they reach a point of crisis (CQC, 2018). Research with adolescents suggests that intervening when symptoms of depression are subthreshold may reduce the risk of developing clinical symptoms (Garber et al., 2009). However, effect sizes for school-based early interventions of depression, compared to control groups, are small (Gee et al., 2020). So, whilst preventative and early intervention support for young people is much needed, effective programmes are lacking (Zonca, 2021). One key target that might improve the effectiveness of treatments for adolescent depression is anhedonia, and in particular the cognitive mechanisms that contribute to and maintain it (Craske et al., 2016, 2019; Dunn, 2012).
Anhedonia is a cardinal feature of depression, which has been shown to be common in young people’s experience of depression (Goodyer et al., 2017; Orchard et al., 2016) and predicts poor outcomes (Ducasse et al., 2018; Dunn et al., 2019; McMakin et al., 2012; Morris et al., 2009; Watson et al., 2020; Winer et al., 2014). Anhedonia is defined in the DSM-5 as a ‘markedly diminished interest or pleasure in all, or almost all, activities’ (APA, 2013). It is proposed that symptoms of anhedonia are associated with deficits in positive affect due to altered reward processing in the Positive Valence Systems (PVS), including reward motivation (‘wanting’), reward attainment (‘liking’) and reward learning (Insel et al., 2010). Initial research with adults has indicated that cognitive therapeutic techniques and augmented behavioural approaches can be harnessed to target aspects of the PVS, including reward anticipation, attainment and learning. For example, Positive Affect Treatment (PAT) and Augmented Depression Therapy (ADepT) demonstrate efficacy in reducing anhedonia in adults with depression (Craske et al., 2016, 2019; Dunn et al., 2019; Sandman & Craske, 2022). Upregulating the PVS to increase positive affect is likely to be an important early intervention target for adolescent depression, yet no interventions have been developed to directly target it in this age group. In young people, positive affect is linked to increased resilience to negative life events and may protect from an initial depressive episode or prevent future relapse (Fredrickson & Levenson, 1998; Tugade & Fredrickson, 2004; Werner-Seidler et al., 2013). In addition to loss of pleasure, phenomenological research into depressed adolescents’ experiences of anhedonia highlights that difficulties with motivation, losing a sense of connection and belonging and questioning one’s sense of self and purpose are also experienced (Watson et al., 2020). This suggests that treatments for anhedonia in adolescent depression should focus on a broad range of facets of anhedonia.
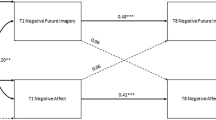
A particularly powerful and developmentally appropriate method to target the PVS might be to use emotional mental imagery. Mental imagery is described as the perception of sensory information without external information, such as seeing with ‘the mind’s eye’ or hearing with the ‘mind’s ear’ (Kosslyn et al., 2001). The component most frequently explored is visual imagery vividness, e.g. how clear and detailed an image is. Research has consistently shown that reduced vividness of positive mental imagery is uniquely associated with depression (as opposed to anxiety) (MacLeod & Byrne, 1996; Morina et al., 2011; Pile & Lau, 2018; Stöber, 2000), whereas the relationship between negative mental imagery and depression is more mixed (Holmes et al., 2007, 2008a; MacLeod & Byrne, 1996; Morina et al., 2011; Pile & Lau, 2018; Stöber, 2000). Additionally, research suggests that positive future imagery may be protective against depression following a negative life event due to its associations with optimism, psychological wellbeing and resilience to stress (Blackwell et al., 2013; Ji et al., 2017; Pile & Lau, 2018). More specifically in relation to negative and positive affect, research in young people has shown that whilst increased negative future imagery and reduced positive future imagery are associated with negative affect, only reduced positive future imagery is associated with anhedonia (Hutchinson et al., 2023). Furthermore, findings from experimental studies have shown that imagining positive events increases positive affect over time in both healthy and dysphoric individuals (Holmes et al., 2008b; Pictet et al., 2011; Pile et al., 2021d). This suggests that positive future imagery may be a useful target for symptoms of anhedonia in depression.
Recent research in adults has examined the use of mental imagery to enhance the ability to imagine future events, as a means of targeting anhedonia in depression. The ability to imagine future events is supported by autobiographical memories, as demonstrated by evidence from neuroimaging studies showing that the same neural pathways that are involved in remembering memories are activated when imagining future events (Schacter et al., 2007). Overgeneral autobiographical memory, which refers to a difficulty in generating specific memories, is reported in depressed individuals and predicts a poorer course of depressive symptoms (Hallford & Sharma, 2019; Sumner et al., 2010; Williams et al., 2007). In relation to anhedonia, difficulties with evoking past memories and generating future events may contribute to low anticipatory pleasure (Kring & Caponigro, 2010; Werner-Seidler & Moulds, 2012) and thus reduce reward motivation (Sherdell et al., 2012). Future Event Specificity Training (FEST) aims to increase anticipatory pleasure through enhancing episodic future thinking by increasing the specificity and detail of positive future events, as well as using mental imagery and emphasising emotions that are associated with imagined future events (Hallford et al., 2020, 2023). Results from a randomised controlled trial found that, compared to a control group, depressed adults who received FEST were less likely to meet criteria for anhedonia and depression at follow-up and FEST was associated with increased anticipatory and consummatory pleasure, as well as increased behavioural activation (Hallford et al., 2023). Whilst these results are encouraging for adult populations, it highlights a need to explore these further in young people.
Simulating positive events and associated emotions, through mental imagery, allows individuals to ‘pre-live’ them, which may enhance positive affect and promote more adaptive behaviours in depression (Holmes et al., 2016; Moulton & Kosslyn, 2011; Renner al., 2017). However, to generate the greatest therapeutic effect, research suggests that it is not only important to generate these positive experiences but also acknowledge and shape the way in which young people respond to the experience of positive affect. Recognising and reducing dampening appraisals, as well as enhancing self-compassion and savouring, have all been suggested to be important in preserving and enhancing positive affect in adults and adolescents. Dampening appraisals (e.g. kill-joy thinking, fault-finding and minimising) (Bryant & Veroff, 2007; Quoidbach et al., 2010) down-regulate positive emotions through negative appraisals of positive emotional experiences and are associated with low levels of positive affect (Bean et al., 2022; Feldman et al., 2008; Yilmaz et al., 2019, 2021). Dampening appraisals in response to positive affect may increase anhedonia through undermining the production of positive emotions and therefore reduce the mood-enhancing effects of positive stimuli, thus diminishing reactivity to positive experiences (Bean et al., 2022). Self-compassion has been shown to attenuate negative affective responses that interfere with emotion regulation and protect against the negative consequences of self-criticism, such as rumination (Neff, 2003; Odou & Brinker, 2014; Terry & Leary, 2011), and greater self-compassion is associated with higher levels of positive affect (Galla, 2016; Neff, 2003; Neff et al., 2007). Finally, savouring, which involves attending to and appreciating positive aspects of experience (Bryant & Veroff, 2007), has been shown to increase positive affect during positive memory recall (Bryant et al., 2005; Gadeikis et al., 2017) and predict positive affect when imaging and anticipating future events (Quoidbach et al., 2010), in adults. In adolescents, greater savouring predicts reduced symptoms of anhedonia over time (Nelis et al., 2018; Yilmaz et al., 2021).
Developing an Early Intervention for Symptoms of Anhedonia in Adolescent Depression
Building on understanding (from cognitive science and young people with lived experience) of which treatment targets and techniques might be particularly valued and effective for adolescents, we have developed a positive imagery intervention (IMAGINE-Positive) that targets symptoms of anhedonia in adolescent depression. To improve access, this brief manualised intervention is designed to be delivered in secondary schools by a non-specialist practitioner. We combined elements of a co-developed intervention for depressed adolescents (IMAGINE, Integrating Memories and Generating Images of New Experiences; Pile et al., 2021a, b) with techniques hypothesised to target the positive valence system (Craske et al., 2016, 2019; Dunn et al., 2019). Results from a recent feasibility randomised controlled trial found IMAGINE reduced symptoms of depression and increased memory specificity compared to a control group (Pile et al., 2021b). IMAGINE combines psychological techniques of imagery rescripting with memory specificity training (MEST) to target dysfunctional autobiographical memory processes that have been linked to depression, including distress/intrusive negative memories, impoverished positive future images and over-general memory). As autobiographical memories support our ability to recall memories and imagine positive future events (Pile et al., 2021a; Schacter et al., 2007), aspects of positive future imagery generation and MEST from IMAGINE were retained for IMAGINE-Positive. Positive future imagery generation was augmented with strategies to target cognitive mechanisms that impair the PVS and reduce positive affect. These included identifying dampening cognitions (during positive future imagery generation) that reduce positive affect in the present moment, identifying self-critical thoughts that arise from dampening appraisals and imagery generation of a compassionate other to increase self-compassion. Positive imagery generation (past and future) was also supplemented with cognitive strategies from adult literature to enhance positive affect. These included encouraging savouring during imagery generation (absorption, in addition to positive mental time travel), increasing attention to personal values and making links between memories and future images.
A key aspect of IMAGINE that was removed for IMAGINE-Positive is imagery rescripting of negative memories (Pile et al., 2021c). The rationale for this is three-fold. Firstly, imagery rescripting may be more useful for reducing negative affect than directly targeting positive affect. This is because imagery rescripting involves focusing on an intrusive image/memory in high detail and vividly imaging an alternative outcome (Hackmann, 1998) to reduce negative affect (Clark & Watson, 1991). Secondly, imagery rescripting is not appropriate for all young people (e.g. high levels of current risk) and some practitioners do not feel confident in delivering imagery rescripting. Finally, young people state a preference to have a range of options for treatment and to be able to choose between them (Pile et al., 2022). Therefore, our objective in developing IMAGINE-Positive was partly to broaden the range of treatments available to young people and increase their agency over their care.
The aims of the present study were to (1) gather data on the feasibility and acceptability of IMAGINE-Positive, to refine the protocol, and (2) establish proof of concept of IMAGINE-Positive by (i) showing no evidence of harm and (ii) initial evidence of clinical gain and changes to targeted cognitive mechanisms at post-assessment (immediately after completing the intervention) and at 3-month follow-up. Changes to symptoms of depression and anhedonia will inform clinical gain. Other measures of emotional symptoms were also collected, including post-traumatic stress symptoms, anxiety, positive and negative affect and self-esteem. Measures of positive and negative future imagery, memory specificity, self-compassion and cognitive responses to low mood (rumination, distraction and problem-solving) will inform changes on cognitive mechanisms. Results from this case series will inform on whether a feasibility randomised controlled trial is warranted and allow for refinements to the protocol if a trial is indicated.
Methods
Design
A single case series, with an A-B-A design, was used. A1 was a no-intervention baseline of varying lengths (3–12 weeks); B was the intervention phase comprising four 90-min sessions; A2 is the follow-up period of 3 months.
Participants
Ten young people (9 females, mean age = 17.69 years, SD = 0.57, range = 16.68–18.48; see Tables 1 for ethnicities) were recruited from one secondary school in London, United Kingdom. As this study aimed to assess feasibility and not efficacy, a power calculation to determine sample size was not appropriate. Instead, we followed other similar studies formatively evaluating novel psychological interventions, e.g. Pile et al. (2021a). To identify participants, schools were approached, and pupils aged 16–19 years were invited to complete the screening questionnaire. Inclusion criteria for participants included the following: (1) aged 16–19, (2) informed consent, (3) willing and able to engage in psychological therapy and complete assessments and (4) scoring above a clinical cut-off for depression at two timepoints (scoring 17 or above at screen and 20 or above at pre-assessment on the MFQ) and showing symptoms of anhedonia (scoring at least 2 on the SHAPS) at the screening stage. Exclusion criteria included the following: (1) diagnosis of learning disability (but not difficulty, e.g. dyslexia), diagnosis of Autism Spectrum Disorder, or significant head injury, neurological disorder or epilepsy; (2) unable to fluently communicate in English; (3) unable to give informed consent; (4) high levels of risk, which were verbally assessed during the pre-intervention assessment; (5) receiving another psychological intervention (including school counselling) and (6) experiencing psychotic or postnatal depressive symptoms. Two participants (one completed (ID: 3) and one discontinued) reported having mental health diagnoses (major depressive disorder, anxiety and an eating disorder) and six participants (ID: 1, 6, 7, 8 and two discontinued) reported having previous psychological support (school mentoring, school counselling, CAMHS, holistic therapy, art therapy, private therapy).
Procedures
The study received ethical approval from the Psychiatry, Nursing and Midwifery Research Ethics Committee at King’s College London (HR-19/20–14899). Participants were identified as those scoring above the clinical cut-off on a measure of depression and were assigned to a no-intervention phase for between 3 to 12 weeks; these varying baseline periods arose because of practical and logistical difficulties of assessing young people during the school term but may actually help to enhance inferences of causality in case series designs (Dunn et al., 2019; Kratochwill & Levin, 2010; Slocum et al., 2022). Consistent with similar studies (Smith et al., 2015), a cut-off score of 20 on the MFQ was applied to confirm eligibility into the study. At the screening stage, four items measuring risk were removed due to ethical considerations for group testing and so an adjusted cut-off of 17 was used. The full MFQ (33 items, cut-off of 20) was completed again at pre-intervention assessment, alongside a clinical interview for risk. Participants completed a pre-assessment and then received the intervention which consisted of four, 90-min, sessions. Following completion of the intervention, participants completed a post-intervention assessment and participants then completed a 3-month follow-up assessment. All assessments and intervention sessions took place in a quiet room within the school, during the school day. All participants provided written informed consent.
Intervention
The intervention was delivered by the first author (Psychological Wellbeing Practitioner) and the third author provided clinical supervision (Consultant Clinical Psychologist). As with IMAGINE (Pile et al., 2021a, b), the intervention was designed to be delivered on a weekly basis for four sessions, lasting up to 90 min, and uses cognitive behavioural techniques (e.g. agenda setting, homework tasks and accompanying worksheets).
In session 1, as in IMAGINE, participants are introduced to the rationale of ‘training memories’, based on the concept that memories compete for retrieval (Brewin, 2006) and the relationship between memories (and the meaning of memories) and emotions, thoughts and behaviours. Participants generate an image of a positive past memory in high-level levels of detail, including prompts for sensory information (smells, sounds, etc.). Imagery generation is in first person, present tense and with their eyes closed (if comfortable to).
In session 2, we removed imagery-rescripting to instead focus on the introduction of positive future images, with a focus on short-term future goals (e.g. an event that will take place in the next week). Participants are encouraged to savour positive emotions that are identified during the generation of their positive future image, in order to prolong and harness positive affect (Bryant et al., 2011; Quoidbach et al., 2010). Participants are also asked to identify any dampening cognitions that are reducing these positive emotions, and psychoeducation on dampening appraisals, based on research in adults and adolescents, is provided (Burr et al., 2017; Dunn et al., 2018; Yilmaz et al., 2019, 2021). We aimed to disrupt the effects of dampening appraisals on positive emotions in two ways. Firstly, we asked participants to re-focus their attention on positive aspects of their positive future image. Second, we aimed to increase self-compassion through a modified version of the Gestalt ‘two chairs’ exercise (Greenberg et al., 1993; Perls, 1973), using mental imagery. In the first step, participants respond to their positive future image as the voice of their inner ‘self-critic’. They then stand up, pace the room and focus on their breath, before sitting back in the same chair, taking on the perspective of their ‘criticised’ self. Participants are encouraged to explain how they feel to hear their self-critical thoughts out loud. To facilitate self-compassion, participants are asked to identify a compassionate person in their lives and use mental imagery to build up a detail image of them, including their facial expression and tone of voice. Participants then stand and pace the room again, before sitting back down and imagining themselves as their ‘compassionate other’. The practitioner takes on the voice of the participant’s ‘inner critic’ and participants are asked to respond to these thoughts from the perspective of the ‘compassionate other’.
As with IMAGINE, in session 3, participants generate positive future images for long-term goals (e.g. graduating from university). Participants generate an image of achieving their future goal and speak to their current self about the journey to achieving this goal, including the ‘good bits’ and the ‘tough bits’, as well as what has helped them achieve their goal and what advice they would give to their current self. Focusing on the ‘good bits’, and their individual contributions to achieving their goal, aims to target approach motivation and reward learning in the reward system (Craske et al., 2019). Identifying the ‘tough bits’, and how they overcame any obstacles, aims to build self-efficacy and resilience. Self-efficacy beliefs enable individuals to reframe challenges and setbacks in order to preserve in the face of difficulty, thus increasing resilience (Djourova et al., 2020; Luthans et al., 2006).
The final session reviews the intervention and how to continue using the intervention strategies in the future. Participants also generate images of past memories and future events (added to IMAGINE-Positive) that link to their personal values, as achievement and self-direction personal values are related to affective wellbeing (positive affect) (Sagiv & Schwartz, 2000).
Each session is accompanied with homework tasks, including memory specificity training (MEST) to increase specificity and access to memories, and a positive data log to increase attention to positive aspects of experience. For an overview of the sessions and homework tasks, see Table 2. Tasks were completed via a mobile phone application, Ethica, which participants downloaded for free onto their phones and were notified to complete the tasks at 6 pm each evening. One participant completed these tasks in their work booklet instead (see Table 3, for homework compliance). Ethica was chosen to collect the homework task data for several reasons: (i) it is free for participants to download; (ii) it has a website interface for researchers, which allows researchers to invite participants to the study, to send different daily notifications to participants relative to when they join the study, and to view whether participants have completed these homework tasks; (iii) it complies with GDPR regulations and (iv) it was cost-effective at the time completing the study.
Measures
Our primary outcomes were feasibility and acceptability, but we also had a secondary interest in quantifying possible effect sizes of the changes in depression and anhedonia symptoms and other relevant symptom dimensions (anxiety, trauma, self-esteem) and cognitive targets (positive and negative mental imagery, memory specificity, self-compassion, rumination, distraction and problem-solving). Although not directly targeted, anxiety, intrusive images and self-esteem have all been implicated in depression, and imagery interventions are likely to have transdiagnostic effects, so we included measures of these to understand if there was any indication of change in these symptoms. We also explored whether IMAGINE-Positive targeted the symptoms that we expected, such as depression and anhedonia. The cognitive measures were chosen to reflect the cognitive mechanisms we aimed to target in IMAGINE-Positive.
Feasibility
Recruitment and retention were measured throughout the study, including the number of schools contacted, the number of students completing the screening questionnaire and scoring above cut-off at two timepoints, the number invited to pre-assessment and consenting to take part and the number of participants completing post- and follow-up assessments and reasons for drop-out. Uptake to the study was measured by the number of students who consented to take part in the pre-assessment versus the number of students who were eligible to take part and retention was measured by the number of students who completed the post-assessments versus the number of students who started the intervention. We set a priori uptake and retention rates of 80% or above to indicate feasibility (Pile et al., 2021b). We also collected data on homework task compliance.
Acceptability
To measure acceptability, participants completed a feedback questionnaire which consisted of rating scales and written responses. Participants were presented with four questions on a five-point Likert scale (see Table 4, for scale response options). These included the following: (1) overall satisfaction, (2) how much the intervention helped them, (3) whether they would recommend the intervention to a friend and (4) feedback on the number of sessions. Mean scores for each scale will be compared with results from a previous similar study, which used the same scales and demonstrated acceptability, to give an indication of acceptability (Pile et al., 2021a). Participants also provided qualitative feedback through written responses.
Indicators of Harm
Indicators of harm were recorded, including adverse events, risk concerns and changes in symptoms/distress. These were differentiated by whether harm was caused as a result of participating in the intervention or due to external factors, whilst a holistic approach was taken, the main consideration for relatedness being whether the risk concerns were consistent with the participant’s history or not. The procedure for managing risk (which did not require immediate action) was for the researcher to discuss the concerns with the clinical supervisor (Consultant Clinical Psychologist) and, if indicated and following discussion with the participant, to share the concerns with the school’s safeguarding team.
Symptom Measures
The Mood and Feelings Questionnaire (Angold et al., 1995) (MFQ) was used to measure depression, one of the designated primary outcomes of the intervention. At screening a 29-item version of the MFQ was used, due to the removal of the risk items. At pre, post and follow-up, the full MFQ (33 items) was completed. At the beginning of each intervention session, the Short MFQ (12 items) was completed. The Snaith-Hamilton Pleasure Scale (Snaith et al., 1995) (SHAPS) was used to measure anhedonia, as the other primary outcome. Participants indicated how much they agree or disagree with each statement on a four-point scale. At screening, the original dichotomous scoring (1, strongly disagree; 1, disagree; 0, agree; 0, strongly agree) (Snaith et al., 1995) was used to identify participants with abnormal hedonic tones, as indicated by a score of greater than 2. At the assessments, a four-point Likert scale (4, strongly disagree; 3, disagree; 2, agree; 1, strongly agree) was used to generate a greater dispersion of the data (Franken et al., 2007). The Screen for Child Anxiety Related Disorders (Birmaher et al. 1997) (SCARED) was used to measure anxiety. To measure post-traumatic stress symptoms (PTSS) in reference to a recent negative event, the Child Revised Impact of Event Scale (Perrin et al., 2005) (CRIES) was employed. The Positive and Negative Affect Schedule (Watson et al., 1988) (PANAS) was used to measure positive and negative affect. The Rosenberg Self Esteem Scale (Rosenberg, 1965) (RSES) measured self-esteem.
Measures of Cognitive Processes
An adapted version of the Prospective Imagery Task (Holmes et al., 2008a; Stöber, 2000) (PIT) for use in young people (Pile & Lau, 2018) was used to measure the vividness of positive and negative future images. The Autobiographical Memory Task (Williams & Broadbent, 1986) (AMT) was used to measure specificity to ten cue words (five positive, five negative). The Children’s Response Style Questionnaire (Abela et al., 2004) (C-RSQ) measured young people’s cognitive responses to low mood, with three response style subscales: rumination, distraction and problem-solving. The Self-Compassion Scale (Neff, 2003) (SCS) measured self-compassion.
Data Analysis
Feasibility data is presented in a modified CONSORT flow diagram and acceptability data are presented descriptively. Descriptive statistics are reported for measures of symptoms and cognitive processes at each time-point. These are reported for each participant to observe any changes from pre- to post-intervention and whether these changes are maintained at follow-up. Additional measures of change, including effect sizes and reliable change (RC), were calculated to reduce the chances of making biased interpretations of changes in outcome measures. Formal statistical testing was not performed as the primary aim of the study was to assess feasibility and acceptability. To give an indication of whether there was a change with the intervention, within-group effect sizes were estimated using Cohen’s d from pre-intervention to post-intervention and from pre-intervention to follow-up, using IBM SPSS Statistics (version 28). Negative effect sizes represent an increase in scores from pre to post/pre to follow-up and positive effect sizes indicate a decrease in scores. The number of participants that showed RC was calculated using The Leeds Reliable Change Indicator by Morley and Dowzer (2014). Reliability estimates for each scale were informed by previous publications, with similar sample characteristics (e.g. adolescents, non-clinical populations) where possible: MFQ (33 items) Cronbach’s α = 0.91 (Thabrew et al., 2018); MFQ (29 items) Cronbach’s α = 0.87 (Pile et al., 2021a); SHAPS Cronbach’s α = 0.91 (Franken et al., 2007); SCARED Cronbach’s α = 0.91 (Bucur et al., 2022); CRIES Cronbach’s α = 0.82 (Dyregrov et al., 1996); PANAS Negative Subscale Cronbach’s α = 0.87 and PANAS Positive Subscale Cronbach’s α = 0.91 (Hutchinson et al., 2023); RSES Cronbach’s α = 0.86 (Wongpakaran & Wongpakaran, 2012); SCS Cronbach’s α = 0.93 (Neff & Pommier, 2013); PIT Positive Subscale Cronbach’s α = 0.83 and PIT Negative Subscale Cronbach’s α = 0.75 (Hutchinson et al., 2023); AMT Cronbach’s α = 0.76 (Stewart et al., 2018); CRSQ Rumination Subscale Cronbach’s α = 0.75, CRSQ Distraction Subscale Cronbach’s α = 0.66 and CRSQ Problem Solving Subscale Cronbach’s α = 0.73 (Abela et al., 2004). RC is found when the magnitude of change (improvement or deterioration) is greater than can be explained by measurement error, as calculated using the Morley and Dowzer (2014) excel application (Pile et al., 2021a). Three outcome categories were allocated to participants: ‘yes’ when reliable improvement (RI) is noted, ‘no’ when there is no RC indicated and ‘deteriorate’ when a reliable deterioration (RD) is shown in participants’ scores.
Results
Feasibility
As school recruitment was impacted by the coronavirus pandemic, school recruitment took place between March 2020 and February 2022. Twenty-six schools were contacted directly through email and 13 schools contacted the research team following advertising the study on social media. One school was recruited, and pre-assessments were completed in terms 2 and 3 (February to April 2022), with post- and follow-up assessments completed in term 3 (April to July 2022) and term 1 (September 2022) of the following school year. Attempts to complete the intervention within one school term were made, to ensure regular intervention sessions; however, this was not possible for all participants. Four hundred young people were presented with the opportunity to complete the screening questionnaire, which included the MFQ (29 items) and SHAPS. A modified CONSORT flow diagram of study participation is presented in Fig. 1. Uptake (the number of students who consented to take part in the pre-assessment versus the number of students who were eligible to take part) was 83%. Retention (the number of students who completed the post-assessments versus the number of students who started the intervention) was 80%. Of the two participants who discontinued the intervention, one participant requested to withdraw because they wished to prioritise their A-Levels and one participant cancelled their second session and did not respond to invitations to rearrange, meaning the reason for their discontinuation is unknown. Together these results suggest that uptake and retention to IMAGINE-Positive are feasible. In terms of homework compliance, for the memory specificity task (MEST), 63% participants completed all 21 days, with two participants completing only 11 and 18 days. For the positive data log, 75% participants completed all 14 days and one participant completed 6 days. For means and standard deviations, see Table 3.
Acceptability
Acceptability was measured by the feedback questionnaire consisting of rating scales and written responses. Overall, participants were satisfied with the intervention (M = 4.24, SD = 0.45), felt that the intervention helped them (M = 4.12, SD = 0.35) and would recommend the intervention to a friend (M = 4.00, SD = 0.53). Six of the eight participants were ‘happy with the number of sessions’, whilst one participant ‘would have like 1–2 more’ and one ‘would have liked 2 + more’ sessions. See Table 4 for individual responses.
The written responses provided qualitative information on participants’ experiences of the programme, including how they found completing the programme at school, what they liked or disliked about the programme and what was most important to them, as well as whether they would recommend the programme to other young people experiencing difficulties with mood and self-esteem. As this data was collected as part of the feedback questionnaire, formal qualitative analysis was not felt appropriate; instead, we have summarised these responses and provided quotes.
Overall, participants reported that IMAGINE-Positive helped them think in new ways and put their thinking and feelings in perspective:
I enjoyed thinking about memories in an alternate way. (Participant 4)
It makes you see things in a different perspective. (Participant 5)
I liked the activities and I felt I was able to engage and understand them well, being able to relate myself to the topics of discussion such as future events and critical thinking. I felt it was a good way of putting feelings that we don’t often talk about into perspective. (Participant 6)
It helps you sees things in a new way that you probably haven’t before (Participant 7)
Participants also identified that the intervention helped with dealing with problems and emotions:
It is good as it helps you find different ways in which you can help your mood… Being guided to see what I might get from my memories and what they may mean, and how they could improve my mood. (Participant 1).
I think it was useful as it opens your eyes to ways of dealing with things. (Participant 5)
It helped me put a lot of my issues into perspective and understand them better in terms of how to deal with them. (Participant 7)
It was very helpful in changing the way I approach my thoughts and feelings. (Participant 8)
Most participants were positive about completing the intervention at school:
It was a lot easier and it’s an environment where i can properly focus (Participant 4)
It was somewhere I was familiar with but knew. It is in a place I can relax and be more open I felt. (Participant 1)
But one participant reported that they would have preferred a different setting:
Was ok but maybe a different environment would’ve been better. As after the sessions you’re thinking about things, but you have to switch it off because we’re at school. (Participant 5)
In terms of responses that suggested changes to the methodology or intervention, one participant reported that there could have been more depth due to the intervention only being four sessions:
There was nothing I didn’t like particularly about the programme, I just feel that because of it only being 4 sessions it felt like some things could’ve been more in depth perhaps. (Participant 7)
One participant reported that the times of day that the homework tasks are prompted could be adjusted, as they found 6 pm too late and would have preferred to complete the positive data log in the morning:
There’s wasn’t anything I didn’t like, but I felt the homework task timings of day could be adjusted as having it at 6pm I felt was too late. I feel if it was in the morning then I could think of something positive able myself and possibly that could help with my mood for the rest of day if I start my day off positively rather than ending it positively. (Participant 6)
Finally, one participant reported that when long explanations were involved, it was hard to focus on:
Some parts I found long and hard to focus on, especially when there were longer explanations involved. (Participant 1)
Indicators of Harm
There were concerns of risk recorded for two participants (ID2 and ID7), both having a history of self-harm. One participant (ID2) disclosed self-harm at pre-assessment but did not report any subsequent risk during treatment. One participant (ID7) reported historic self-harm prior to the study and one incident of self-harm during the study, but this was assessed as unrelated to the intervention. Risk issues were discussed with the larger team to understand the context and assess whether the incident was related or unrelated to the intervention, taking into consideration whether the risk concern was consistent with the participant’s history or not. For the second participant (ID7), in the final session, they reported that a risk incident had taken place during the school holidays (which occurred between the third session and the final session). From discussions with the young person, this incident was consistent with their previous history of self-harm and so it was deemed by the clinical team to not be associated with the intervention. Additionally, in their qualitative feedback, this participant (ID7) identified that the most important part of the programme for them was that they ‘felt safe confiding in things’ because their ‘feelings were always met with validation and explanation’, suggesting that, anecdotally, participation in the intervention enabled them to feel able to disclose their risk and get extra support.
In terms of changes in symptoms/distress, one participant (ID2) presented with elevated symptoms of depression at the start of the programme and their depression score increased at post-assessment, but this was not a RD. They did show RD in symptoms of anxiety and self-compassion. At pre-assessment, this participant also disclosed risk due to increasing stress about their upcoming A-Level examinations. At post-assessment, this participant had completed their examinations and reported that they had not gone well, which they were distressed by, and hoped school would allow them to re-sit. In their qualitative feedback, this participant (ID2) reported that ‘having someone to talk to’ was the most important part of the programme for them and that they found the programme ‘helpful’ because it gave them ‘someone to talk to as well as learn methods to control emotions’. These deteriorations in symptoms are therefore unlikely to be associated with the taking part in the intervention. Unfortunately, this participant did not attend the follow-up as they had left school.
Changes in Symptomology
Due to the variable time between screen and pre-intervention assessment, depression scores on the MFQ (risk items removed from pre-assessment to allow for comparison) were compared to explore if there were any changes in scores during this period. Differences in scores were small (d = − 0.20) but three participants showed RD (time between screen and pre-assessment was 4 weeks for two participants and 12 weeks for one participant).
There was a large effect from pre to post (d = 1.12) and from pre to follow-up (d = 2.51) for depression scores. Of the eight participants, seven showed a decrease in depressive symptoms from pre to post, with 5 showing RI (63%). From pre to follow-up, all seven remaining participants showed a decrease in depressive symptoms, with six showing RI (86%). At post-assessment, four out of eight participants scored below the clinical cut-off on the MFQ, and at follow-up, six out of seven participants were below the clinical cut-off. Individual changes in symptoms are presented in Table 5 and Fig. 2. The short MFQ was administered at each session, and whilst caution should be employed when interpreting these scores, they could suggest a trend in decreasing depressive symptoms across the sessions for most participants, with a slightly larger decrease in symptoms from session one to session two (See Fig. 3).
Scores of anhedonia, as measured by the SHAPS, were compared at screen and pre, with small differences observed (d = 0.24) and two participants showing RI (time between screen and pre-assessment was 4 weeks for one participant and one week for the other participant). Within-subject effect sizes indicated a small decrease in anhedonic symptoms from pre to post (d = 0.38) but a large decrease from pre to follow-up (d = 1.28). Six (of eight) participants showed a decrease in anhedonia pre to post, but none showed RI (0%). Six (of seven) participants showed a decrease in anhedonia pre to follow-up, with two showing RI (29%). Individual changes in symptoms of anhedonia are presented in Fig. 4.
Within-subject effect sizes for anxiety scores, as measured by the SCARED, indicated a medium decrease in symptoms from pre to post (d = 0.53) and a large decrease from pre to follow-up (d = 1.53). Five of eight participants showed a decrease in anxiety from pre to post, with two participants showing RI (25%) and one participant showing RD (13%). All seven participants showed a decrease in anxiety from pre to follow-up, with five participants showing RI (71%).
For PTSS, which was measured by the CRIES, the within-subject effect sizes indicated a small decrease from pre to post (d = 0.48) and a large decrease from pre to follow-up (d = 0.84). Five out of eight participants showed a decreased in PTSS from pre to post, with three participants showing RI (38%) and one participant showing RD (13%). Six out of seven participants showed a decrease in PTSS from pre to follow-up with four participants showing RI (47%) and one participant showing RD (14%).
For negative affect, measured by the PANAS-N, the within-subject effect sizes indicated a large decrease from pre to post (d = 0.75) and a large decrease from pre to follow-up (d = 1.92). Seven out of eight participants showed a decreased in negative affect from pre to post, with five participants showing RI (63%) and one participant showing RD (13%). All seven participants showed a decrease in negative affect from pre to follow-up, with all participants showing RI (100%).
Higher scores on the PANAS-P represent a greater positive affect. The within-subject effect sizes indicated a small increase from pre to post (d = − 0.29) and a large increase from pre to follow-up (d = − 2.87). Five out of eight participants showed an increase in positive affect from pre to post, with two participants showing RI (25%) and two participants showing RD (25%). All seven participants showed an increase in positive affect from pre to follow-up, with all participants showing RI (100%).
Higher scores on the RSES also represent greater self-esteem. The within-subject effect sizes indicated a medium increase from pre to post (d = − 0.54) and from pre to follow-up (d = − 0.68). Six out of eight participants showed an increase in self-esteem from pre to post, with one participant showing RI (13%). Five out of seven participants showed an increase in self-esteem from pre to follow-up, with three participants showing RI (43%).
Changes in Cognitive Mechanisms
The prospective imagery task (PIT) measured vividness of future images. For the vividness of positive future imagery, the within-subject effect sizes showed a large increase from pre to post (d = − 1.08) and pre to follow-up (d = − 2.02). Six out of eight participants showed an increase in positive future imagery vividness from pre to post, with four participants showing RI (50%). From pre to follow-up, two of seven participants showed RI (29%). For the vividness of negative future imagery, there were small decreases in effect size from pre to post (d = 0.31) and pre to follow-up (d = 0.33). Five participants showed a decrease in vividness of negative future imagery from pre to post, with one participant showing RI (13%). From pre to follow-up, there were decreases for four of seven participants, with one participant showing RI (14%).
For memory specificity, which was measured by the AMT, the within-subject effect sizes showed a large increase from pre to post (d = − 0.91) but a small increase from pre to follow-up (d = − 0.42). From pre to post, five out of eight participants showed increased memory specificity and one participant showed RI (13%). From pre to follow-up, four out of seven participants showed increased memory specificity and one participant showed RI (14%). Individual changes in scores on measures of cognitive mechanisms are presented in Table 6.
In terms of cognitive responses to low mood, rumination, distraction and problem-solving were measured using the C-RSQ. For rumination, the within-subjects effect sizes showed a small decrease from pre to post (d = 0.34) but a large decrease from pre to follow-up (d = 0.83). Seven out of eight participants showed decreased rumination from pre to post, but no participants showed RI. Five out of seven participants showed a decrease from pre to follow-up, with two participants showing RI (29%). For distraction, there were small within-subject effect sizes from pre to post (d = 0.29) and from pre to follow-up (d = 0.17), with only one participant showing RI at pre to post (13%) and pre to follow-up (14%) and one participant showing RD at pre to follow-up (14%). For problem-solving, the within-subject effect sizes showed a medium increase in problem-solving from pre to post (d = − 0.53) and large increases from pre to follow-up (− 1.27). From pre to post, four of eight participants showed increased problem-solving, with two participants showing RI (25%). From pre to follow-up, six of seven participants show an increase, with three participants showing RI (43%).
Higher scores on the SCS also represent greater self-compassion. The within-subject effect sizes indicated a medium increase from pre to post (d = − 0.54) and from pre to follow-up (d = − 0.64). Seven out of eight participants showed an increase in self-compassion from pre to post, with three participants showing RI (38%). Six out of seven participants showed an increase in self-compassion from pre to follow-up, with two participants showing RI (29%) and one participant showing RD (14%).
Discussion
The present study aimed to adapt a novel-imagery based intervention for adolescent depression (IMAGINE), to specifically target symptoms of anhedonia. We aimed to gather data on the feasibility and acceptability of IMAGINE-Positive and establish proof of concept of the intervention through showing no evidence of harm related to the intervention. We also aimed to demonstrate evidence of clinical gain (on measures of depression and anhedonia) and changes to targeted cognitive mechanisms of mental imagery, memory specificity and self-compassion.
In terms of feasibility, uptake (83%) and retention rates (80%) indicated that participants were willing to take part in the programme, to complete the intervention and complete the post-intervention outcome measures. Of the fifteen participants that were invited to pre-assessment, twelve (80%) participants responded to take part, which is higher than studies of similar samples (Pile et al., 2021a; Smith et al., 2015). Of the three participants who did not take part, one no longer wished to take part, one did not respond to the invite, and one initially accepted the invitation but did not attend their pre-assessment and did not respond to invites to rearrange. Literature from previous studies of similar samples (Pile et al., 2021a) and discussions with young people with lived experiences from advisory groups suggest that possible reasons for withdrawing or not responding may include the following: concerns about stigma (e.g. being seen with the research team in school), worries about confidentiality, concerns about what participation involves, beliefs that the intervention may not be beneficial to them and not receiving the invitation (e.g. emails going to their junk folder). These reasons may also explain why only a small proportion of students (20 out of 400) chose to take part in the initial screening questionnaire. It is also worth noting that changes to the screening process may explain why uptake to the screen was lower than previous similar studies (Pile et al., 2021a, b). Firstly, as in any school intervention, procedures were discussed and co-created with teachers. Due to a preference amongst teachers to organise an assembly around mental health (for maximum exposure) and also curriculum demands, the screen was delivered to whole year groups rather than smaller form tutor groups. Secondly, at the request of the school, a link to the screening questionnaire was provided to allow students to complete the screen after the session (that they could complete in privacy), rather than completing a paper questionnaire during the session. This may have meant that students forgot to complete the screening questionnaire after the session. It is possible that asking teachers to remind students about the screening questionnaire may increase completion, but it is important to be mindful of placing additional demands on teachers, as well as whether this would make students feel pressured to participate by their teachers. Students completing the screen during the session may overcome this barrier, but students may struggle to do this in larger groups of their peers with smaller tutor groups being preferable. Our subsequent work with young people with lived experience has suggested an active approach to screening, i.e. asking all young people to complete a questionnaire in school lessons rather than rely on young people to self-identify. Future studies that could explore the best methodology for identifying young people with high symptoms of depression would be valuable.
Overall, compliance with the homework tasks was good. Most participants completed their homework tasks in Ethica, meaning they were prompted with daily notifications, which may have facilitated homework completion as previously suggested in Pile et al. (2021a). One participant completed their homework tasks in their booklet, as they had only a family iCloud account and wanted to maintain privacy. Regarding acceptability, participants reported being satisfied with the intervention, that the intervention helped them, that they would recommend the intervention to a friend and that they were happy with the number of sessions. These results are consistent with findings from a previous study which demonstrated acceptability through using the same scales (Pile et al., 2021a). Overall, these results suggested that IMAGINE-Positive and the trial design are feasible and acceptable.
To establish proof of concept, it was important to monitor for any evidence of harm, including adverse events, risk issues or significant deterioration of mood, and to identify any change in symptoms of depression. There was one adverse event reported during the case series although this was deemed not related to the intervention. Two participants (ID2, 1D7) disclosed risk issues and one (ID2) showed an increase in depression scores from pre to post (although this was not a reliable deterioration), but when taking into consideration external factors related to the participants, as well as their qualitative feedback about the programme, it is unlikely that these concerns were a result of taking part in the intervention.
In terms of clinical gain, across all participants, this study found a 14-point decrease in depression scores from pre to post and a 24-point decrease from pre to follow-up, which is consistent with (and larger than) previous studies (Pile et al., 2021a; Smith et al., 2015). Only one participant did not demonstrate therapeutic gain in depressive symptoms at follow-up, but it should be noted that their MFQ score was low at pre-assessment. There was only a 1-point decrease in scores of anhedonia from pre to post, but a 7-point decrease from pre to follow-up. As anhedonia is conceptualised by a lack of positive affect, we also recorded changes in scores for positive affect, Similarly, there was a small increase in scores from pre to post (1.5 points) but a larger increase from pre to follow-up (9 points). This pattern of results suggests that the benefits of positive future imagery on anhedonia and positive affect may be more gradual. For self-esteem, whilst there were medium within-subjects effect sizes, increases in scores were small from pre to post (2 points) and pre to follow-up (4 points). In terms of PTSS, anxiety and negative affect, there were (respectively) small, medium and large reductions from pre to post, and large reductions from pre to follow-up. Whilst caution should be taken when interpreting these results, due to the small sample and lack of effect sizes relative to a control, it is promising that initial results suggest that depressive symptoms reduce following completing IMAGINE-Positive and over time symptoms of anhedonia, PTSS, anxiety and negative affect reduce whilst symptoms of positive affect and self-esteem improve.
An additional aim was to target underlying cognitive mechanisms that perpetuate and maintain anhedonia in adolescent depression. As expected, there were notable changes in positive future imagery but not negative future imagery. There were large increases in positive future imagery from pre to post and further increases from pre to follow-up, with most participants showing reliable improvement overtime. Whilst interpreting these results with caution, they are encouraging as IMAGINE-Positive was developed to be a positive future imagery-based early intervention. As imagery rescripting of negative memories was removed, we did not expect to see the changes in negative future imagery that were reported in participants who received IMAGINE (Pile et al., 2021a, b). Furthermore, as previous research suggests that negative future imagery is not associated with anhedonia (Hutchinson et al., 2023), we did not expect changes in vividness of negative future imagery to be linked to changes in symptoms of anhedonia. For memory specificity, the improvements were larger from pre to post, than from pre to follow-up. These results are consistent with findings in the IMAGINE case series study (Pile et al., 2021a), suggesting that the training effects of memory specificity might be lost over time when regular prompts are stopped. With regard to self-compassion, whilst there were medium increases from both pre to post and pre to follow-up, most participants showed reliable improvement. This is encouraging because we specifically aimed to target the generation of self-compassion in session 2. However, again, these results should be interpreted with caution due to the small sample size.
In terms of changes to cognitive responses to low mood, results were broadly consistent with what we expected. Whilst reductions in rumination were small from pre to post, they were large from pre to follow-up. We aimed to disrupt the effects of dampening appraisals on positive affect and so expected to see reductions in rumination as dampening cognitions have been associated with increase rumination (Feldman et al., 2008). There were only small increases in distraction, which is promising as research suggests that distraction in relation to positive affect can dampen positive affect (Quoidbach et al., 2010), as continual attending to information unrelated to positive events has been associated with longer-term negative effects on affective well-being (Carriere et al., 2008). For problem-solving, there were medium increases from pre to post and larger increases from pre to follow-up. It is possible that problem-solving skills were activated during imagery generation for long-term future goals, particularly when focusing on obstacles and how to overcome these, through generating self-efficacy beliefs.
It is also important to highlight the context with which this study took place in to explain the extended duration for recruiting a school and the high proportion of schools that were contacted versus the one that was recruited, as these are greater than previous studies of similar populations (Pile et al., 2021a; Smith et al., 2015). School recruitment was severely disrupted by the coronavirus pandemic, with numerous school closures between March 2020 and January 2022. During this time, we were in contact with several schools, but a variety of challenges prevented recruitment from starting sooner. These included the following: (a) a preference from schools to start recruitment when in-person teaching resumed, (b) gate keepers who had initially expressed an interest in the study had left their positions by the time in-person teaching was more stable and (c) increased workload demands for teachers due to moving between online teaching and in-person teaching. It is important to highlight that these challenges represented the unique situation of the pandemic, and whilst it is still uncertain how schools are recovering from the pandemic, young people in this study and in previous research (Pile et al., 2021a) report positive feedback about completing brief psychological interventions in school.
There are several limitations to the current study. Firstly, though this study was not designed to test efficacy, as we used a single case series design, the sample size is small, and we do not have a control group. We therefore cannot exclude the possibility that symptom improvement may have been due to common factor skills, such as empathy, active listening and building a therapeutic alliance. Future studies should replicate these results using larger sample sizes and include a therapeutic control group. Secondly, whilst we had a varied baseline period, due to practical and logistical issues, we did not collect additional baseline data which is recommended for single-subject designs (Ritter & Stangier, 2016) and would be helpful to infer causality during the no-treatment phase. Third, as we did not include measures of dampening and savouring strategies, it is unclear to what extent these mechanisms were targeted and whether they contributed to changes in symptomology. To better understand this, future studies could consider including measures of savouring and dampening. Relatedly, as there were several targets in IMAGINE-Positive, we cannot definitively know which mechanisms were driving the changes observed, although this study was not designed for statistical testing of mechanisms. Future studies could consider using qualitative methods to collect rich data from participants on their experiences of the proposed therapeutic mechanisms, which may inform on active ingredients. This is particularly important because if future research can match key mechanisms and interventions on a larger scale and improve our understanding of ‘what works for who’, this could provide a range of tailored interventions for young people with depression and allow them to make an informed choice of their treatment. Fourth, because of limited funding resources, the intervention was only delivered by one practitioner, who also collected the assessment data at pre, post and follow-up, and whilst self-report measures are considered to be less vulnerable to assessor bias, this still may have introduced a bias of social desirability, whereby participants may have skewed their answers to meet their perceived expectations of the practitioner. To reduce this risk of bias in the future, outcome assessments could be administered by practitioners who are independent of the intervention delivery. Fifth, whilst our sample is ethnically diverse, participants were predominantly female which may affect the generalisability of our findings. Finally, as we only recruited from one school, it is possible that the increased attendance at pre-assessment (compared to previous studies) may reflect the nature of the school and students.
Conclusions
This study provides initial evidence that IMAGINE-Positive is feasible to deliver in schools and is acceptable to participants. Results also indicate that receiving IMAGINE-Positive led to reductions in symptoms of depression and anhedonia, which may be due to changes in key cognitive mechanisms. Together, these findings suggest that a feasibility randomised controlled trial is warranted to gather data on IMAGINE-Positive in relation to an appropriate control group.
Data availability
The data that support the findings of this study are openly available at Hutchinson, Taryn (2023), ‘Targeting anhedonia in adolescents: A single case series of a positive imagery-based early intervention’, Mendeley Data, V1, doi: https://doi.org/10.17632/3wmy67nszx.1.
References
Abela, J. R. Z., Vanderbilt, E., & Rochon, A. (2004). A test of the integration of the response styles and of depression in third and seventh grade children. Journal of Social and Clinical Psychology, 23(5), 653–674. https://doi.org/10.1521/jscp.23.5.653.50752
American Psychiatric Association, DSM-5 Task Force. (2013). Diagnostic and statistical manual of mental disorders: DSM-5™ (5th ed.). American Psychiatric Publishing, Inc.. https://doi.org/10.1176/appi.books.9780890425596
Angold, A., Costello, E. J., Messer, S. C., Pickles, A., Winder, F., & Silver, D. (1995). The development of a short questionnaire for use in epidemiological studies of depression in children and adolescents. International Journal of Methods in Psychiatric Research, 5, 237–249.
Angst, J., Gamma, A., Rössler, W., Ajdacic, V., & Klein, D. N. (2009). Long-term depression versus episodic major depression: Results from the prospective Zurich study of a community sample. Journal of Affective Disorders, 115(1), 112–121. https://doi.org/10.1016/j.jad.2008.09.023
Bean, C. A. L., Summers, C. B., & Ciesla, J. A. (2022). Dampening of positive affect and depression: A meta-analysis of cross-sectional and longitudinal relationships. Behaviour Research and Therapy, 156, 104153. https://doi.org/10.1016/j.brat.2022.104153
Birmaher, B., Khetarpal, S., Brent, D., Cully, M., Balach, L., Kaufman, J., et al. (1997). The Screen for Child Anxiety Related Emotional Disorders (SCARED): Scale construction and psychometric characteristics. Journal of the American Academy of Child and Adolescent Psychiatry, 36(4), 545–553. https://doi.org/10.1097/00004583-199704000-00018
Blackwell, S. E., Rius-Ottenheim, N., Schulte-van Maaren, Y. W., Carlier, I. V., Middelkoop, V. D., Zitman, F. G., Spinhoven, P., Holmes, E. A., & Giltay, E. J. (2013). Optimism and mental imagery: A possible cognitive marker to promote well-being? Psychiatry Research, 206(1), 56–61. https://doi.org/10.1016/j.psychres.2012.09.047
Bryant, F., Chadwick, E., & Kluwe, K. (2011). Understanding the processes that regulate positive emotional experience: Unsolved problems and future directions for theory and research on savoring. International Journal of Wellbeing, 1. https://doi.org/10.5502/ijw.v1i1.18
Bryant, F. B., & Veroff, J. (2007). Savoring: A new model of positive experience. Lawrence Erlbaum.
Bryant, F. B., Smart, C. M., & King, S. P. (2005). Using the past to enhance the present: Boosting happiness through positive reminiscence. Journal of Happiness Studies, 6(3), 227–260. https://doi.org/10.1007/s10902-005-3889-4
Brewin, C. R. (2006). Understanding cognitive behaviour therapy: A retrieval competition account. Behaviour Research and Therapy, 44(6), 765–784. https://doi.org/10.1016/j.brat.2006.02.005
Bucur, S. M., Moraru, A., Adamovits, B., Bud, E. S., Olteanu, C. D., & Vaida, L. L. (2022). Psychometric Properties of Scared-C Scale in a Romanian Community Sample and Its Future Utility for Dental Practice. Children, 9(1), 34. https://doi.org/10.3390/children9010034
Burr, L. A., Javiad, M., Jell, G., Werner-Seidler, A., & Dunn, B. D. (2017). Turning lemonade into lemons: Dampening appraisals reduce positive affect and increase negative affect during positive activity scheduling. Behaviour Research and Therapy, 91, 91–101. https://doi.org/10.1016/j.brat.2017.01.010
Carriere, J. S., Cheyne, J. A., & Smilek, D. (2008). Everyday attention lapses and memory failures: The affective consequences of mindlessness. Consciousness and Cognition, 17(3), 835–847. https://doi.org/10.1016/j.concog.2007.04.008
Care Quality Commission. (2018). Are we listening? A review of children and young people’s mental health services. Retrieved 5th February 2023 from: https://www.discoveringstatistics.com/repository/sem.pdf
Clark, L. A., & Watson, D. (1991). Tripartite model of anxiety and depression: Psychometric evidence and taxonomic implications. Journal of Abnormal Psychology, 100(3), 316–336. https://doi.org/10.1037/0021-843X.100.3.316
Clayborne, Z. M., Varin, M., & Colman, I. (2019). Systematic review and meta-analysis: Adolescent depression and long-term psychosocial outcomes. Journal of the American Academy of Child and Adolescent Psychiatry, 58(1), 72–79. https://doi.org/10.1016/j.jaac.2018.07.896
Craske, M. G., Meuret, A. E., Ritz, T., Treanor, M., Dour, H. J., & Rosenfield, D. (2019). Positive affect treatment for depression and anxiety: A randomized clinical trial for a core feature of anhedonia. Journal of Consulting and Clinical Psychology., 87(5), 457–471.
Craske, M. G., Meuret, A. E., Ritz, T., Treanor, M., & Dour, H. J. (2016). Treatment for anhedonia: A neuroscience driven approach. Depression and Anxiety, 33, 927–936. https://doi.org/10.1002/da.22490
Djourova, N. P., Rodríguez Molina, I., TorderaSantamatilde, N., & Abate, G. (2020). Self-efficacy and resilience: Mediating mechanisms in the relationship between the transformational leadership dimensions and well-being. Journal of Leadership & Organizational Studies, 27(3), 256–270. https://doi.org/10.1177/1548051819849002
Ducasse, D., Loas, G., Dassa, D., Gramaglia, C., Zeppegno, P., Guillaume, S., Olié, E., & Courtet, P. (2018). Anhedonia is associated with suicidal ideation independently of depression: A meta-analysis. Depression and Anxiety, 35(5), 382–392. https://doi.org/10.1002/da.22709
Dunn, B. D., Widnall, E., Reed, N., Owens, C., Campbell, J., & Kuyken, W. (2019). Bringing light into darkness: A multiple baseline mixed methods case series evaluation of Augmented Depression Therapy (ADepT). Behaviour Research and Therapy, 120, 103418. https://doi.org/10.1016/j.brat.2019.103418
Dunn, B. D., Burr, L. A., Smith, H. B., Hunt, A., Dadgostar, D., Dalglish, L., Smith, S., Attree, E., Jell, G., Martyn, J., Bos, N., & Werner-Seidler, A. (2018). Turning gold into lead: Dampening appraisals reduce happiness and pleasantness and increase sadness during anticipation and recall of pleasant activities in the laboratory. Behaviour Research and Therapy, 107, 19–33. https://doi.org/10.1016/j.brat.2018.05.003
Dunn, B. D. (2012). Helping depressed clients reconnect to positive emotion experience: Current insights and future directions. Clinical Psychology and Psychotherapy, 19, 326–340. DOI: 10.1002
Dyregrov, A., Kuterovac, G., & Barath, A. (1996). Factor analysis of the impact of event scale with children in war. Scandinavian Journal of Psychology, 36, 339–350.
Essau, C. A., Lewinsohn, P. M., Seeley, J. R., & Sasagawa, S. (2010). Gender differences in the developmental course of depression. Journal of Affective Disorders, 127(1), 185–190. https://doi.org/10.1016/j.jad.2010.05.016
Feldman, G., Joormann, J., & Johnson, S. (2008). Responses to positive affect: A self-report measure of rumination and dampening. Cognitive Therapy and Research, 32, 507–525.
Fombonne, E., Wostear, G., Cooper, V., Harrington, R., & Rutter, M. (2001). The Maudsley long-term follow-up of child and adolescent depression. 1. Psychiatric outcomes in adulthood. British Journal of Psychiatry, 179, 210–217. https://doi.org/10.1192/bjp.179.3.210
Franken, I. H. A., Rassin, E., & Muris, P. (2007). The assessment of anhedonia in clinical and non-clinical populations: Further validation of the Snaith-Hamilton Pleasure Scale (SHAPS). Journal of Affective Disorders, 99(1), 83–89. https://doi.org/10.1016/j.jad.2006.08.020
Fredrickson, B. L., & Levenson, R. W. (1998). Positive emotions speed recovery from the cardiovascular sequelae of negative emotions. Cognition & Emotion, 12(2), 191–220. https://doi.org/10.1080/026999398379718
Gadeikis, D., Bos, N., Schweizer, S., Murphy, F., & Dunn, B. (2017). Engaging in an experiential processing mode increases positive emotional response during recall of pleasant autobiographical memories. Behaviour Research and Therapy, 92, 68–76. https://doi.org/10.1016/j.brat.2017.02.005
Galla, B. M. (2016). Within-person changes in mindfulness and self-compassion predict enhanced emotional well-being in healthy, but stressed adolescents. Journal of Adolescence, 49, 204–217. https://doi.org/10.1016/j.adolescence.2016.03.016
Garber, J., Clarke, G. N., Weersing, V. R., Beardslee, W. R., Brent, D. A., Gladstone, T. R., DeBar, L. L., Lynch, F. L., D’Angelo, E., Hollon, S. D., Shamseddeen, W., & Iyengar, S. (2009). Prevention of depression in at-risk adolescents: A randomized controlled trial. JAMA, 301(21), 2215–2224. https://doi.org/10.1001/jama.2009.788
Gee, B., Reynolds, S., Carroll, B., Orchard, F., Clarke, T., Martin, D., Wilson, J., & Pass, L. (2020). Practitioner review: Effectiveness of indicated school-based interventions for adolescent depression and anxiety–a meta-analytic review. Journal of Child Psychology and Psychiatry, 61, 739–756. https://doi.org/10.1111/jcpp.13209
Goodyer IM, Reynolds S, Barrett B, Byford S, Dubicka B, Hill J et al (2017) Cognitive behavioural therapy and short-term psychoanalytical psychotherapy versus a brief psychosocial intervention in adolescents with unipolar major depressive disorder (IMPACT): A multicentre, pragmatic, observer-blind, randomised controlled superiority trial. Lancet Psychiatry 4(2):109–119. https://doi.org/10.1016/S2215-0366(16)30378-9
Greenberg, L. S., Rice, L. N., & Elliot, R. (1993). Facilitating emotional change: The moment by moment process. Guilford Press.
Hackmann, A. (1998). Working with images in clinical psychology. In A. S. Bellack, &M. Hersen (Eds.), Comprehensive clinical psychology, Vol. 6(pp. 301–318). Elsevier
Hallford, D. J., Rusanov, D., Yeow, J. J. E., Austin, D. W., D’Argembeau, A., Fuller-Tyszkiewicz, M., & Raes, F. (2023). Reducing anhedonia in major depressive disorder with Future Event Specificity Training (FEST): A randomized controlled trial. Cognitive Therapy and Research, 47(1), 20–37. https://doi.org/10.1007/s10608-022-10330-z
Hallford, D. J., Sharma, M. K., & Austin, D. W. (2020). Increasing anticipatory pleasure in major depression through enhancing episodic future thinking: A randomized single-case series trial. Journal of Psychopathology and Behavioral Assessment, 42(4), 751–764. https://doi.org/10.1007/s10862-020-09820-9
Hallford, D. J., & Sharma, M. K. (2019). Anticipatory pleasure for future experiences in schizophrenia spectrum disorders and major depression: A systematic review and meta-analysis. The British Journal of Clinical Psychology, 58(4), 357–383. https://doi.org/10.1111/bjc.12218
Holmes, E. A., Lang, T. J., Moulds, M. L., & Steele, A. M. (2008a). Prospective and positive mental imagery deficits in dysphoria. Behaviour Research and Therapy, 46(8), 976–981. https://doi.org/10.1016/j.brat.2008.04.009
Holmes, E. A., Coughtrey, A. E., & Connor, A. (2008b). Looking at or through rose-tinted glasses? Imagery perspective and positive mood. Emotion, 8, 875–879. https://doi.org/10.1037/a0013617
Holmes, E. A., Crane, C., Fennell, M. J., & Williams, J. M. (2007). Imagery about suicide in depression—“Flash-forwards”? Journal of Behavior Therapy and Experimental Psychiatry, 38(4), 423–434. https://doi.org/10.1016/j.jbtep.2007.10.004
Holmes, E. A., Blackwell, S. E., Burnett Heyes, S., Renner, F., & Raes, F. (2016). Mental Imagery in Depression: Phenomenology, Potential Mechanisms, and Treatment Implications. Annu Rev Clin Psychol, 12, 249–280. https://doi.org/10.1146/annurev-clinpsy-021815-092925
Hutchinson, T., Riddleston, L., Pile, V., Meehan, A., Shukla, M., & Lau, J. (2023). Is future mental imagery associated with reduced impact of the COVID-19 pandemic on negative affect and anhedonic symptoms in young people? Cognitive Therapy and Research, 1–13. https://doi.org/10.1007/s10608-023-10352-1
Insel, T., Cuthbert, B., Garvey, M., Heinssen, R., Pine, D. S., Quinn, K., Sanislow, C., & Wang, P. (2010). Research domain criteria (RDoC): Toward a new classification framework for research on mental disorders. The American Journal of Psychiatry, 167(7), 748–751. https://doi.org/10.1176/appi.ajp.2010.09091379
Ji, J. L., Holmes, E. A., & Blackwell, S. E. (2017). Seeing light at the end of the tunnel: Positive prospective mental imagery and optimism in depression. Psychiatry Research, 247, 155–162. https://doi.org/10.1016/j.psychres.2016.11.025
Kim-Cohen, J., Caspi, A., Moffitt, T. E., Harrington, H., Milne, B. J., & Poulton, R. (2003). Prior juvenile diagnoses in adults with mental disorder: Developmental follow-back of a prospective-longitudinal cohort. Archives of General Psychiatry, 60(7), 709–717. https://doi.org/10.1001/archpsyc.60.7.709
Kosslyn, S. M., Ganis, G., & Thompson, W. L. (2001). Neural foundations of imagery. Nature Reviews: Neuroscience, 2, 635–642.
Kring, A. M., & Caponigro, J. M. (2010). Emotion in schizophrenia: Where feeling meets thinking. Current Directions in Psychological Science, 19(4), 255–259. https://doi.org/10.1177/0963721410377599
Kratochwill, T. R., & Levin, J. R. (2010). Enhancing the scientific credibility of single-case intervention research: Randomization to the rescue. Psychological Methods, 15(2), 124–144. https://doi.org/10.1037/a0017736
Luthans, F., Avey, J., Avolio, B., Norman, S. M., & Combs, G. M. (2006). Psychological capital development: Toward a micro-intervention. Journal of Organizational Behavior, 27, 387–393.
MacLeod, A. K., & Byrne, A. (1996). Anxiety, depression, and the anticipation of future positive and negative experiences. Journal of Abnormal Psychology, 105(2), 286–289. https://doi.org/10.1037/0021-843X.105.2.286
McMakin, D. L., Olino, T. M., Porta, G., Dietz, L. J., Emslie, G., Clarke, G., Wagner, K. D., Asarnow, J. R., Ryan, N. D., Birmaher, B., Shamseddeen, W., Mayes, T., Kennard, B., Spirito, A., Keller, M., Lynch, F. L., Dickerson, J. F., & Brent, D. A. (2012). Anhedonia predicts poorer recovery among youth with selective serotonin reuptake inhibitor treatment-resistant depression. Journal of the American Academy of Child and Adolescent Psychiatry, 51(4), 404–411. https://doi.org/10.1016/j.jaac.2012.01.011
Morina, N., Deeprose, C., Pusowski, C., Schmid, M., & Holmes, E. A. (2011). Prospective mental imagery in patients with major depressive disorder or anxiety disorders. Journal of Anxiety Disorders, 25(8), 1032–1037. https://doi.org/10.1016/j.janxdis.2011.06.012
Morley, S., & Dowzer, C. N. (2014). Manual for the Leeds reliable change indicator: Simple excel applications for the analysis of individual patient and group data (pp. 1–13). University of Leeds.
Morris, B. H., Bylsma, L. M., & Rottenberg, J. (2009). Does emotion predict the course of major depressive disorder? A review of prospective studies. British Journal of Clinical Psychology, 48, 255–273. https://doi.org/10.1348/014466508X396549
Moulton, S. T., & Kosslyn, S. M. (2011). Imagining predictions: Mental imagery as mental emulation. In M. Bar (Ed.), Predictions in the brain: Using our past to generate a future (pp. 95–106). Oxford University Press. https://doi.org/10.1093/acprof:oso/9780195395518.003.0040
Neff, K. D., & Pommier, E. (2013). The relationship between self-compassion and other-focused concern among college undergraduates, community adults, and practicing meditators. Self and Identity, 12(2), 160–176. https://doi.org/10.1080/15298868.2011.649546
Neff, K. D., Kirkpatrick, K. L., & Rude, S. S. (2007). Self-compassion and adaptive psychological functioning. Journal of Research in Personality, 41, 139–154. https://doi.org/10.1016/j.jrp.2006.03.004
Neff, K. (2003). Self-compassion: An alternative conceptualization of a healthy attitude toward oneself. Self and Identity, 2(2), 85–101. https://doi.org/10.1080/15298860309032
Nelis, S., Bastin, M., Raes, F., & Bijttebier, P. (2018). When do good things lift you up? Dampening, enhancing, and uplifts in relation to depressive and anhedonic symptoms in early adolescence. Journal of Youth and Adolescence, 47, 1712–1730. https://doi.org/10.1007/s10964-018-0880-z
Odou, N., & Brinker, J. (2014). Exploring the relationship between rumination, self-compassion, and mood. Self and Identity, 13(4), 449–459. https://doi.org/10.1080/15298868.2013.840332
Orchard, F., Pass, L., Marshall, T., & Reynolds, S. (2016). Clinical characteristics of adolescents referred for treatment of depressive disorders. Child and Adolescent Mental Health, 22, 61–68. https://doi.org/10.1111/camh.12178
Perls, F. (1973). The gestalt approach and eye witness to therapy. Science and Behavior Books.
Perrin, S., Meiser-Stedman, R., & Smith, P. (2005). The Children’s Revised Impact of Event Scale (CRIES): Validity as a screening instrument for PTSD. Behavioural and Cognitive Psychotherapy, 33(04), 487. https://doi.org/10.1017/S1352465805002419
Pictet, A., Coughtrey, A. E., Mathews, A., & Holmes, E. A. (2011). Fishing for happiness: The effects of generating positive imagery on mood and behaviour. Behaviour Research and Therapy, 49(12), 885–891. https://doi.org/10.1016/j.brat.2011.10.003
Pile, V., Herring, G., Bullard, A., Loades, M., Chan, S. W. Y., Reynolds, S., & Orchard, F. (2022). A multi-stakeholders perspective on how to improve psychological treatments for depression in young people. European Child and Adolescent Psychiatry. https://doi.org/10.1007/s00787-022-02001-x
Pile, V., Smith, P., Leamy, M., Oliver, A., Blackwell, S. E., Meiser-Stedman, R., Dunn, B. D., Holmes, E. A., & Lau, J. Y. F. (2021a). Harnessing mental imagery and enhancing memory specificity: Developing a brief early intervention for depressive symptoms in adolescence. Cognitive Therapy and Research, 45(5), 885–901. https://doi.org/10.1007/s10608-020-10130-3
Pile, V., Smith, P., Leamy, M., Oliver, A., Bennett, E., Blackwell, S. E., Meiser-Stedman, R., Stringer, D., Dunn, B. D., Holmes, E. A., & Lau, J. Y. F. (2021b). A feasibility randomised controlled trial of a brief early intervention for adolescent depression that targets emotional mental images and memory specificity (IMAGINE). Behaviour Research and Therapy, 143, 103876. https://doi.org/10.1016/j.brat.2021.103876
Pile, V., Smith, P., & Lau, J. Y. F. (2021c). Using imagery rescripting as an early intervention for depression in young people. Front Psychiatry, 12, 651115. https://doi.org/10.3389/fpsyt.2021.651115
Pile, V., Williamson, G., Saunders, A., Holmes, E. A., & Lau, J. Y. F. (2021d). Harnessing emotional mental imagery to reduce anxiety and depression in young people: An integrative review of progress and promise. The Lancet Psychiatry, 8(9), 836–852. https://doi.org/10.1016/S2215-0366(21)00195-4
Pile, V., & Lau, J. Y. F. (2018). Looking forward to the future: Impoverished vividness for positive prospective events characterises low mood in adolescence. Journal of Affective Disorders, 238, 269–276. https://doi.org/10.1016/j.jad.2018.05.032
Quoidbach, J., Berry, E. V., Hansenne, M., & Mikolajczak, M. (2010). Positive emotion regulation and well-being: Comparing the impact of eight savoring and dampening strategies. Personality and Individual Differences, 49(5), 368–373. https://doi.org/10.1016/j.paid.2010.03.048
Renner, F., Ji, J. L., Pictet, A., et al. (2017). Effects of engaging in repeated mental imagery of future positive events on behavioural activation in individuals with major depressive disorder. Cognitive Therapy and Research, 41, 369–380. https://doi.org/10.1007/s10608-016-9776-y
Ritter, V., & Stangier, U. (2016). Seeing in the mind’s eye: Imagery rescripting for patients with body dysmorphic disorder. A single case series. Journal of Behavior Therapy and Experimental Psychiatry, 50, 187–195. https://doi.org/10.1016/j.jbtep.2015.07.007
Richards, D. (2011). Prevalence and clinical course of depression: A review. Clinical Psychology Review, 31, 1117–1125.
Rosenberg, M. (1965). Society and the adolescent self-image. Princeton University Press.
Sandman, C. F., & Craske, M. G. (2022). Psychological treatments for anhedonia. Current Topics in Behavioral Neurosciences, 58, 491–513. https://doi.org/10.1007/7854_2021_291
Sagiv, L., & Schwartz, S. H. (2000). Value priorities and subjective well-being: Direct relations and congruity effects. European Journal of Social Psychology, 30, 177–198. https://doi.org/10.1002/(SICI)1099-0992(200003/04)30:2%3c177::AID-EJSP982%3e3.0.CO;2-Z
Schacter, D. L., Addis, D. R., & Buckner, R. L. (2007). Remembering the past to imagine the future: The prospective brain. Nature Reviews. Neuroscience, 8(9), 657–661. https://doi.org/10.1038/nrn2213
Sherdell, L., Waugh, C. E., & Gotlib, I. H. (2012). Anticipatory pleasure predicts motivation for reward in major depression. Journal of Abnormal Psychology, 121(1), 51–60. https://doi.org/10.1037/a0024945
Slocum, T. A., Pinkelman, S. E., Joslyn, P. R., et al. (2022). Threats to internal validity in multiple-baseline design variations. Perspect Behav Sci, 45, 619–638. https://doi.org/10.1007/s40614-022-00326-1
Snaith, R. P., Hamilton, M., Morley, S., Humayan, A., Hargreaves, D., & Trigwell, P. (1995). A scale for the assessment of hedonic tone the snaith-Hamilton pleasure scale. British Journal of Psychiatry, 167(1), 99–103. https://doi.org/10.1192/bjp.167.1.99
Smith, P., Scott, R., Eshkevari, E., Jatta, F., Leigh, E., Harris, V., Robinson, A., Abeles, P., Proudfoot, J., Verduyn, C., & Yule, W. (2015). Computerised CBT for depressed adolescents: Randomised controlled trial. Behaviour Research and Therapy, 73, 104–110. https://doi.org/10.1016/j.brat.2015.07.009
Stewart, T. M., Hunter, S. C., & Rhodes, S. M. (2018). A prospective investigation of rumination and executive control in predicting overgeneral autobiographical memory in adolescence. Memory & Cognition, 46(3), 482–496. https://doi.org/10.3758/s13421-017-0779-z
Stöber, J. (2000). Prospective cognitions in anxiety and depression: Replication and methodological extension. Cognition and Emotion, 14(5), 725–729. https://doi.org/10.1080/02699930050117693
Sumner, J. A., Griffith, J. W., & Mineka, S. (2010). Overgeneral autobiographical memory as a predictor of the course of depression: A meta-analysis. Behaviour Research and Therapy, 48(7), 614–625. https://doi.org/10.1016/j.brat.2010.03.013
Terry, M. L., & Leary, M. R. (2011). Self-compassion, self-regulation, and health. Self and Identity, 10(3), 352362. https://doi.org/10.1080/15298868.2011.558404
Thabrew, H., Stasiak, K., Bavin, L. M., Frampton, C., & Merry, S. (2018). Validation of the Mood and Feelings Questionnaire (MFQ) and Short Mood and Feelings Questionnaire (SMFQ) in New Zealand help-seeking adolescents. International Journal of Methods in Psychiatric Research, 27(3), 1–9.
Thapar, A., Collishaw, S., Pine, D. S., & Thapar, A. K. (2012). Depression in adolescence. Lancet (London, England), 379(9820), 1056–1067. https://doi.org/10.1016/S0140-6736(11)60871-4
Tugade, M. M., & Fredrickson, B. L. (2004). Resilient individuals use positive emotions to bounce back from negative emotional experiences. Journal of Personality and Social Psychology, 86(2), 320–333. https://doi.org/10.1037/0022-3514.86.2.320
Watson, R., Harvey, K., McCabe, C., & Reynolds, S. (2020). Understanding anhedonia: A qualitative study exploring loss of interest and pleasure in adolescent depression. European Child and Adolescent Psychiatry, 29(4), 489–499. https://doi.org/10.1007/s00787-019-01364-y
Watson, D., Clark, L. A., & Tellegen, A. (1988). Development and validation of brief measures of positive and negative affect: The PANAS scales. Journal of Personality and Social Psychology, 54(6), 1063–1070. https://doi.org/10.1037/0022-3514.54.6.1063
Werner-Seidler, A., Banks, R., Dunn, B. D., & Moulds, M. L. (2013). An investigation of the relationship between positive affect regulation and depression. Behaviour Research and Therapy, 51(1), 46–56. https://doi.org/10.1016/j.brat.2012.11.001
Werner-Seidler, A., & Moulds, M. L. (2012). Mood repair and processing mode in depression. Emotion, 12(3), 470–478. https://doi.org/10.1037/a0025984
Williams, J. M., Barnhofer, T., Crane, C., Herman, D., Raes, F., Watkins, E., & Dalgleish, T. (2007). Autobiographical memory specificity and emotional disorder. Psychological Bulletin, 133(1), 122–148. https://doi.org/10.1037/0033-2909.133.1.122
Williams, J. M. G., & Broadbent, K. (1986). Autobiographical memory in suicide attempters. Journal of Abnormal Psychology, 95(2), 144–149. https://doi.org/10.1037/0021-843X.95.2.144
Wongpakaran, T., & Wongpakaran, N. (2012). A comparison of reliability and construct validity between the original and revised versions of the Rosenberg self-esteem scale. Psychiatry Investigation, 9(1), 54–58. https://doi.org/10.4306/pi.2012.9.1.54
Winer, E. S., Nadorff, M. R., Ellis, T. E., Allen, J. G., Herrera, S., & Salem, T. (2014). Anhedonia predicts suicidal ideation in a large psychiatric inpatient sample. Psychiatry Research, 218, 124–128. https://doi.org/10.1016/j.psychres.2014.04.016
Yilmaz, M., Psychogiou, L., Ford, T., & Dunn, B. D. (2021). Examining the relationship between anhedonia symptoms and trait positive appraisal style in adolescents: A longitudinal survey study. Journal of Adolescence, 91, 71–81. https://doi.org/10.1016/j.adolescence.2021.07.007
Yilmaz, M., Psychogiou, L., Javaid, M., Ford, T., & Dunn, B. D. (2019). Making the worst of a good job: Induced dampening appraisals blunt happiness and increase sadness in adolescents during pleasant memory recall. Behaviour Research and Therapy, 122, 103476. https://doi.org/10.1016/j.brat.2019.103476
Zonca, V. (2021). Preventive strategies for adolescent depression: What are we missing? A focus on biomarkers. Brain, Behavior, & Immunity - Health, 18, 100385. https://doi.org/10.1016/j.bbih.2021.100385
World Health Organization. (2021a). Adolescent Mental Health. Retrieved January, 2022 from https://www.who.int/news-room/fact-sheets/detail/adolescent-mental-health
World Health Organization. (2021b). WHO report highlights global shortfall in investment in mental health. Retrieved May 2022 from https://www.who.int/news/item/08-10-2021-who-report-highlights-global-shortfall-in-investment-in-mental-health
Acknowledgements
We wish to acknowledge the students and staff members who participated in or facilitated this research. For the purposes of open access, the author has applied a Creative Commons Attribution (CC BY) licence to any Accepted Author Manuscript version arising from this submission.
Funding
This study represents research from a Doctoral Scholarship, supported by a grant from Mental Health Research UK and the Schizophrenia Research Fund. Dr Victoria Pile (Advanced Fellowship, NIHR301312) is funded by the NIHR for this research project. The views expressed in this publication are those of the author(s) and not necessarily those of the NIHR, NHS or the UK Department of Health and Social Care.
Author information
Authors and Affiliations
Contributions
Taryn Hutchinson: conceptualization, data curation, formal analysis, investigation, project administration, software, validation, visualisation, writing—original draft, writing—review and editing.
Jennifer Lau: conceptualization, funding acquisition, methodology, project administration, supervision, validation, writing—review and editing.
Patrick Smith: project administration, supervision, validation, writing—review and editing.
Victoria Pile: conceptualization, funding acquisition, methodology, project administration, resources, supervision, validation, writing—review and editing.
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Psychiatry, Nursing and Midwifery Research Ethics Committee at King’s College London (HR-19/20–14899).
Research involving animal rights
No animal participants were included in this study.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Hutchinson, T., Lau, J.Y.F., Smith, P. et al. Targeting Anhedonia in Adolescents: A Single Case Series of a Positive Imagery-Based Early Intervention. J Cogn Ther 17, 429–465 (2024). https://doi.org/10.1007/s41811-024-00202-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41811-024-00202-7