Abstract
Purpose of review
The preferred treatment of systemic sclerosis (SSc) is unclear due to an incomplete understanding of disease pathogenesis, variations in disease manifestations and variable quality of evidence to support treatment decisions. The objectives of this article are to discuss the value of clinical practice guidelines, critique guideline development and uptake, compare SSc-specific guidelines and highlight consensus-based treatment algorithms to complement guidelines when recommendations and/or high-quality evidence are lacking.
Recent finding
Thirty-nine guidelines or recommendations for the screening, diagnosis, treatment and conduct of trials in SSc have been published. Four publications contained guidance on the treatment of multiple domains. The European League Against Rheumatism and the EULAR Scleroderma Trial and Research group guidelines were published in 2009 and updated in 2017. The British Society of Rheumatology and the British Health Professionals in Rheumatology published guidelines in 2016. The Brazilian Society of Rheumatology published SSc guidelines in 2013. The absence of recommendations for the preferred order of therapy is a limitation of all published guidelines. Treatment algorithms, based on SSc expert consensus, were proposed in 2012 and updated in 2018. These algorithms are complementary to the guidelines, as they provide expert consensus in areas of uncertainty.
Summary
SSc-specific guidelines and treatment algorithms provide evidence-based and/or expert consensus-based recommendations on how to treat patients with the intention of reducing inappropriate practice variability and improving patient outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
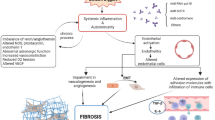
Systemic sclerosis (SSc, also called scleroderma) is a systemic autoimmune rheumatic disease characterized by immune activation with antibody production, vasculopathy and fibrosis. It can not only affect the skin but affect the lungs, heart, gastrointestinal tract, joints and kidneys. It is a progressive disease without a cure. The diagnosis is made by recognition of characteristic signs and symptoms. In order to identify more homogeneous groups of patients for research purposes, the American College of Rheumatology (ACR) and European League Against Rheumatism (EULAR) have developed classification criteria for SSc [1]. Once classified as SSc, patients can be further subdivided into limited or diffuse cutaneous subsets, based on extent of skin involvement [2]. New subset criteria are under development [3,4,5].
SSc has a female preponderance with a female:male ratio of 4.7:1 [6]. However, males more frequently have the diffuse cutaneous form of SSc (relative risk (RR) 1.44) and interstitial lung disease (RR 1.24). Male sex confers an increased risk of mortality (hazard ratio 1.16) compared to males in the general population [6]. Disease manifestations can vary across ethnic groups [7]. Compared to European-descent Caucasian subjects, East Asians less frequently have calcinosis cutis and esophageal dysmotility, Afro-Caribbeans more frequently have interstitial lung disease and First Nations patients more frequently have diffuse cutaneous disease [7]. SSc can confer pain, disability and adversely impact self-esteem, social and occupational ability. SSc is more disabling than joint involvement in psoriatic arthritis, and patients with SSc experience more severe pain than patients with rheumatoid arthritis [8]. SSc diminishes quality of life [8].
The optimal treatment of SSc is often unclear due to an incomplete understanding of the disease pathogenesis, variations in disease manifestations and disease trajectory and insufficient or variable quality of evidence to support treatment decisions [9]. This is further compounded by the rarity of the disease, resulting in non-expert rheumatologists having less experience with its diagnosis and management [10•]. Given the high morbidity, mortality and poor prognosis associated with SSc [11], high-quality guidelines are needed to reduce inappropriate practice variability, expedite uptake of effective advances and achieve better outcomes [12, 13]. The objectives of this article are to discuss the value of clinical practice guidelines, critique challenges of guideline development and uptake, compare and contrast SSc-specific clinical practice guidelines and highlight the utility of consensus-based treatment algorithms to complement guidelines when recommendations and/or high-quality evidence are lacking.
The value of clinical practice guidelines
Clinical practice guidelines are important to both health care professionals and professional organizations. Guidelines provide synthesis of the published literature regarding diagnosis, screening, prevention and/or treatment options. Guidelines often include expert consultation and consideration of the weight and quality of the evidence [14]. A ranking system is often used to indicate the strength of the results of a study. The strength of evidence can be impacted by the study design (randomized trial, cohort study, case series), implementation of bias reduction strategies and outcome measures used. A recommendation with high-quality evidence is supported by several high-quality studies with consistent results or one large high-quality multicentre trial. Additional research is unlikely to change confidence in the estimated treatment effect. This process of evidence synthesis and grading of evidence strength/quality, complemented by expert panel oversight, often results in recommendations.
Although the terms ‘guidelines’ and ‘recommendations’ are frequently used interchangeably, most guidelines contain recommendations. In Europe, the term recommendation is preferred for the overall document since guideline may have medico-legal implications. A physician could be exposed to litigation if not following a guideline even though the guideline may be of low quality or may not always reflect current or standard practice. For health care professionals, clinical practice guidelines or recommendations provide reasonable certainty about what works, based on good quality evidence. Guidelines can facilitate making us better doctors. Furthermore, guidelines communicate to frontline providers’ information that is trustworthy and concise.
Guidelines also provide value to professional organizations. The guideline can be a tool to advocate for the disease, for access to investigations or for access to therapy. Guidelines can affect the international reputation of an organization by conferring gravitas and provides evidence of organizational impact. Guidelines can improve the credibility of the organization. This is particularly true of small organizations with a small professional membership. Guidelines can elevate the standing of the organization by providing better access to government and influence partner organizations. Together, they can form a brotherhood of organizations that trusts each other. For professional organizations, guidelines can set an objective foundation for clear policy, as opposed to the opinion of a few people in leadership positions. For example, guidelines can set a foundation for an organization’s policies relating to corporate relationships (do not enter due to lack of science), patient communications, human resources and guidance to insurance companies. For professional organizations, guidelines can demonstrate ownership of the disease. It demonstrates that the organization is at the forefront of knowledge translation and can be used for raising funds.
The challenges of guideline development and uptake
Critics of guidelines note that the development of good quality guidelines requires significant resources [15]. Historically, guideline development is a multi-year process, requiring staff and face-to-face meetings, at a cost of approximately US$200,000 per year [15]. Many guidelines have relied on teams of volunteers who have full-time research enterprises. In addition, there are insufficient numbers of methodologists trained in guideline development. Critics have also noted that guidelines are often outdated by the time they are published due to the time required to develop the guideline and long publication times. Once published, they are difficult to maintain. Guidelines are not easily modified in a timely manner without loss of rigour. In a complex and heterogeneous disease like SSc, they may lag behind the concept of personalized or precision medicine if treatment recommendations become too generic, especially in the era of targeted biological therapies that may in the future be characterized by subgroup responses.
In addition, it has been recognized that despite wide dissemination, guidelines do not necessarily change physician behaviour.[13]. Potential barriers to physician uptake and adherence may include lack of awareness, lack of familiarity, lack of agreement, lack of self-efficacy, lack of outcome expectancy, inertia of previous practice and external barriers [13, 16]. Casual familiarity of the guideline’s existence does not ensure knowledge of the recommendations nor ability to apply them [13]. External barriers may be related to the guideline itself (e.g. poorly written, difficult to use), patient-related factors (e.g. the recommendation is not in line with patient preferences) or environmental factors (lack of access to resources such as recommended investigations, therapists or treatments) [13, 16].
Guidelines and recommendations in systemic sclerosis
A systematic review of the literature evaluating clinical practice guidelines and recommendations in SSc was recently published by Smith et al. under the auspices of the European Reference Network on Rare and Complex Connective Tissue and Musculoskeletal Diseases (ReCONNET) [10•]. They identified 39 guidelines or recommendations for the screening and diagnosis [17,18,19,20,21,22,23], treatment [9, 19, 22,23,24,25, 26••, 27••, 28,29,30,31,32,33,34] and conduct of clinical trials [35,36,37,38,39,40,41,42,43,44,45,46] of SSc-specific manifestations (Table 1). While most publications were domain-specific (e.g. cardiac, vascular) [19, 23, 25, 33, 34], four publications contained guidance on the treatment of multiple domains within one document [9, 26••, 27••, 28]. The investigators critiqued that many recommendations were based on non-systematic review of the published literature. The investigators considered five guidelines as strong evidence and consensus-based, developed by a representative committee, a systematic review of the literature and synthesis of the evidence [9, 19, 22, 26••, 36, 49].
Three sets of guidelines provided treatment recommendations for multiple SSc-specific domains (Table 1). The European League Against Rheumatism (EULAR) and the EULAR Scleroderma Trial and Research (EUSTAR) group initially published guidelines in 2009, with an update in 2017 [9, 26••]. The British Society of Rheumatology (BSR) and the British Health Professionals in Rheumatology (BHPR) published guidelines in 2016 [27••]. Both sets of guidelines were comparatively evaluated by Peller and Pope in 2017 [55]. The Brazilian Society of Rheumatology Committee on Systemic Sclerosis also published guidelines in 2013 [28].
The EULAR/EUSTAR guidelines contain recommendations the management of SSc-related digital vasculopathy, pulmonary arterial hypertension, skin involvement, interstitial lung disease, scleroderma renal crisis and gastrointestinal disease. The EULAR/EUSTAR guidelines did not include recommendations on the treatment of calcinosis cutis, telangiectasia, pruritus, inflammatory arthritis or fatigue, exercise, occupational therapy nor nutritional issues [55, 56]. However, the EULAR/EUSTAR guidelines contain a research agenda, supported by the expert committee, of questions for consideration by future investigators. Agreement with the EULAR/EUSTAR guidelines was evaluated by cross-sectional survey of international SSc experts who were members of the Scleroderma Clinical Trials Consortium and the Canadian Scleroderma Research Group, some of whom were also EUSTAR members [56]. Many of the recommendations were strongly supported [56]. However, North American and European SSc experts differed on the strength of support on the use of iloprost for the management of SSc-associated vasculopathy and the use of bosentan for the prevention of SSc-associated digital ulceration. This regional variation has been attributed to the lack of availability of iloprost in North American and the lack of regulatory approval for the use of bosentan for digital ulcer prevention in North America [10•, 56]. Agreement may also be affected by the strength of evidence, particularly when the effect size was modest (e.g. use of methotrexate for skin involvement) [56,57,58].
The BSR/BHPR guidelines similarly provided recommendations for the treatment of SSc-related digital vasculopathy, pulmonary arterial hypertension, skin involvement, interstitial lung disease, scleroderma renal crisis and gastrointestinal disease. The treatment recommendation is generally comparable to the EULAR/EUSTAR guidelines, but the BSR/BHPR guidelines provide recommendations on more treatment options [55]. These guidelines are considered more comprehensive in disease management as they include recommendations on general measures (e.g. early recognition of diffuse cutaneous SSc, referral to specialist centres), education (e.g. cold avoidance and smoking cessation for management of Raynaud’s phenomenon) and non-pharmacologic strategies (e.g. moisturization, laser therapy, physiotherapy, massage therapy, exercise) [55]. The BSR/BHPR guidelines also provide recommendations on the management of SSc-associated cardiac disease, calcinosis cutis and musculoskeletal involvement. However, these guidelines do not provide evidence-based recommendations for the treatment of SSc-associated erectile dysfunction, cardiac dysrhythmias, heart failure and pain [55].
The Brazilian Society of Rheumatology guidelines provide recommendations on classification of SSc: role of nailfold capillaroscopy and autoantibodies in the early diagnosis and follow-up of SSc and treatment of SSc-associated skin involvement, calcinosis cutis, vasculopathy, ulceration, gastrointestinal manifestations, pulmonary arterial hypertension, interstitial lung disease, scleroderma renal crisis and cardiac involvement [28]. The Brazilian Society of Rheumatology guidelines also provide recommendations on non-pharmacologic strategies (e.g. laser therapy and extracorporeal shock wave lithotripsy for calcinosis cutis). Grading of the recommendations is provided based on the strength of evidence [28].
SSc clinical practice guidelines: unmet needs
The currently published guidelines and recommendations address the major issues relating to the screening of internal organ manifestations of SSc, treatment and clinical trial design. However, these issues reflect disease severity and relative importance from a physician perspective. Other SSc-specific issues are deemed important by patients [59, 60], such as sexual dysfunction, loss of self-esteem, relationships and occupational ability lack recommendations or guidelines [10•]. Furthermore, there is an absence of recommendations for psycho-social or behavioural interventions, particularly with the goal of improving health-related quality of life [10•].
The uptake of the SSc clinical practice guidelines into real-world practice has been questioned [61]. Adherence may be affected by physician level characteristics (practice size, physician experience), patient characteristics, socio-economic factors (geographic location, access to medication, health insurance coverage) and lack of a clear algorithm [56]. Indeed, when a patient does not have access to a first-line therapy or it has been ineffective, treatment algorithms can provide guidance on the next appropriate treatment option [62, 63••]. The absence of recommendations for the preferred order for initiation of therapy is a limitation of published guidelines [62, 63••]. Treatment algorithms for SSc, based on international SSc expert consensus, were proposed in 2012 and updated in 2018 [62, 63••]. Treatment algorithms are provided for SSc-associated vasculopathy, inflammatory arthritis, scleroderma renal crisis, pulmonary arterial hypertension, interstitial lung disease, gastrointestinal, skin and cardiac involvement. These algorithms are complementary to the guidelines, as they provide expert consensus in areas of uncertainty and paucity of evidence.
Conclusion
In summary, SSc is a complex multisystem disease resulting in significant morbidity, disability, diminished health-related quality of life and mortality. SSc-specific clinical practice guidelines provide evidence-based recommendations on how to treat patients with the intention of reducing inappropriate practice variability and improving patient outcomes. When first-line treatment has been ineffective or not accessible, SSc expert consensus-based treatment algorithms can provide guidance on the next appropriate treatment option(s). These algorithms are complementary to the guidelines, as they provide expert consensus in areas of uncertainty and paucity of evidence.
References and Recommended Reading
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
van den Hoogen F, Khanna D, Fransen J, Johnson SR, Baron M, Tyndall A, et al. 2013 classification criteria for systemic sclerosis: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum. 2013;65(11):2737–47. https://doi.org/10.1002/art.38098.
LeRoy EC, Black C, Fleischmajer R, Jablonska S, Krieg T, Medsger TA Jr, et al. Scleroderma (systemic sclerosis): classification, subsets and pathogenesis. J Rheumatol. 1988;15(2):202–5.
Johnson SR, Feldman BM, Hawker GA. Classification criteria for systemic sclerosis subsets. J Rheumatol. 2007;34(9):1855–63.
Johnson SR, Soowamber ML, Fransen J, Khanna D, Van Den Hoogen F, Baron M, et al. There is a need for new systemic sclerosis subset criteria. A content analytic approach. Scand J Rheumatol. 2018;47(1):62–70. https://doi.org/10.1080/03009742.2017.1299793.
Johnson SR. Progress in the clinical classification of systemic sclerosis. Curr Opin Rheumatol. 2017;29(6):568–73. https://doi.org/10.1097/BOR.0000000000000443.
Hussein H, Lee P, Chau C, Johnson SR. The effect of male sex on survival in systemic sclerosis. J Rheumatol. 2014;41(11):2193–200. https://doi.org/10.3899/jrheum.140006.
Al Sheikh H, Ahmad Z, Johnson SR. Ethnic variations in systemic sclerosis disease manifestations, internal organ involvement and mortality. The Journal of Rheumatology 2019;In Press.
Johnson SR, Glaman DD, Schentag CT, Lee P. Quality of life and functional status in systemic sclerosis compared to other rheumatic diseases. J Rheumatol. 2006;33(6):1117–22.
Kowal-Bielecka O, Landewé R, Avouac J, Chwiesko S, Miniati I, Czirjak L, et al. EULAR recommendations for the treatment of systemic sclerosis: a report from the EULAR Scleroderma Trials and Research group (EUSTAR). Ann Rheum Dis. 2009;68(5):620–8. https://doi.org/10.1136/ard.2008.096677.
Smith V, Scire CA, Talarico R, Airo P, Alexander T, Allanore Y, et al. Systemic sclerosis: state of the art on clinical practice guidelines. RMD Open, This article provides a concise overview of clinical practice guidelines in systemic sclerosis. 2018;4(Suppl 1):e000782. https://doi.org/10.1136/rmdopen-2018-000782.
Johnson SR, Swiston JR, Granton JT. Prognostic factors for survival in scleroderma associated pulmonary arterial hypertension. J Rheumatol. 2008;35(8):1584–90.
Reed J, Pope J. A comparison between general rheumatologists and scleroderma experts with respect to following systemic sclerosis guidelines. Clin Exp Rheumatol. 2015;33(4 Suppl 91):S40–6.
Cabana MD, Rand CS, Powe NR, Wu AW, Wilson MH, Abboud PA, et al. Why don’t physicians follow clinical practice guidelines? A framework for improvement. Jama. 1999;282(15):1458–65.
Guyatt G, Oxman AD, Akl EA, Kunz R, Vist G, Brozek J, et al. GRADE guidelines: 1. Introduction-GRADE evidence profiles and summary of findings tables. J Clin Epidemiol. 2011;64(4):383–94. https://doi.org/10.1016/j.jclinepi.2010.04.026.
Guidelines IoMUCoSfDTCP. Clinical practice guidelines we can trust. Washington (DC): National Academies Press (US); 2011.
Birrenbach T, Kraehenmann S, Perrig M, Berendonk C, Huwendiek S. Physicians’ attitudes toward, use of, and perceived barriers to clinical guidelines: a survey among Swiss physicians. Adv Med Educ Pract. 2016;7:673–80. https://doi.org/10.2147/AMEP.S115149.
Maverakis E, Patel F, Kronenberg DG, Chung L, Fiorentino D, Allanore Y, et al. International consensus criteria for the diagnosis of Raynaud’s phenomenon. J Autoimmun. 2014;48–49:60–5. https://doi.org/10.1016/j.jaut.2014.01.020.
Mavrogeni SI, Kitas GD, Dimitroulas T, Sfikakis PP, Seo P, Gabriel S, et al. Cardiovascular magnetic resonance in rheumatology: current status and recommendations for use. Int J Cardiol. 2016;217:135–48. https://doi.org/10.1016/j.ijcard.2016.04.158.
Pain CE, Constantin T, Toplak N, Moll M, Iking-Konert C, Piotto DP, et al. Raynaud’s syndrome in children: systematic review and development of recommendations for assessment and monitoring. Clin Exp Rheumatol. 2016;34(Suppl 100(5)):200–6.
Lazzaroni MG, Cavazzana I, Colombo E, Dobrota R, Hernandez J, Hesselstrand R, et al. Malignancies in patients with anti-RNA polymerase III antibodies and systemic sclerosis: analysis of the EULAR scleroderma trials and research cohort and possible recommendations for screening. J Rheumatol. 2017;44(5):639–47. https://doi.org/10.3899/jrheum.160817.
Avouac J, Huscher D, Furst DE, Opitz CF, Distler O, Allanore Y, et al. Expert consensus for performing right heart catheterisation for suspected pulmonary arterial hypertension in systemic sclerosis: a Delphi consensus study with cluster analysis. Ann Rheum Dis. 2014;73(1):191–7. https://doi.org/10.1136/annrheumdis-2012-202567.
Galie N, Humbert M, Vachiery JL, Gibbs S, Lang I, Torbicki A, et al. 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension: the Joint Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European Society of Cardiology (ESC) and the European Respiratory Society (ERS): Endorsed by: Association for European Paediatric and Congenital Cardiology (AEPC), International Society for Heart and Lung Transplantation (ISHLT). Eur Heart J. 2016;37(1):67–119. https://doi.org/10.1093/eurheartj/ehv317.
Lynch BM, Stern EP, Ong V, Harber M, Burns A, Denton CP. UK Scleroderma Study Group (UKSSG) guidelines on the diagnosis and management of scleroderma renal crisis. Clin Exp Rheumatol. 2016;34(Suppl 100(5)):106–9.
Bissell LA, Anderson M, Burgess M, Chakravarty K, Coghlan G, Dumitru RB, et al. Consensus best practice pathway of the UK Systemic Sclerosis Study group: management of cardiac disease in systemic sclerosis. Rheumatology (Oxford). 2017;56(6):912–21. https://doi.org/10.1093/rheumatology/kew488.
Knobler R, Berlin G, Calzavara-Pinton P, Greinix H, Jaksch P, Laroche L, et al. Guidelines on the use of extracorporeal photopheresis. J Eur Acad Dermatol Venereol. 2014;28(Suppl 1):1–37. https://doi.org/10.1111/jdv.12311.
•• Kowal-Bielecka O, Fransen J, Avouac J, Becker M, Kulak A, Allanore Y, et al. Update of EULAR recommendations for the treatment of systemic sclerosis. Ann Rheum Dis. 2017;76(8):1327–39. https://doi.org/10.1136/annrheumdis-2016-209909. This article presents the updated EULAR recommendations for the treatment of systemic sclerosis.
Denton CP, Hughes M, Gak N, Vila J, Buch MH, Chakravarty K, et al. BSR and BHPR guideline for the treatment of systemic sclerosis. Rheumatology (Oxford), These guidelines present comprehensive recommendations for the management of systemic sclerosis. 2016;55(10):1906–10. https://doi.org/10.1093/rheumatology/kew224.
Sampaio-Barros PD, Zimmermann AF, Muller Cde S, Borges CT, Freire EA, Maretti GB, et al. Recommendations for the management and treatment of systemic sclerosis. Rev Bras Reumatol. 2013;53(3):258–75.
Distler JH, Jordan S, Airo P, Alegre-Sancho JJ, Allanore Y, Balbir Gurman A, et al. Is there a role for TNFalpha antagonists in the treatment of SSc? EUSTAR expert consensus development using the Delphi technique. Clin Exp Rheumatol. 2011;29(2 Suppl 65):S40–5.
Rodrigues MC, Hamerschlak N, de Moraes DA, Simoes BP, Rodrigues M, Ribeiro AA, et al. Guidelines of the Brazilian Society of Bone Marrow Transplantation on hematopoietic stem cell transplantation as a treatment for the autoimmune diseases systemic sclerosis and multiple sclerosis. Rev Bras Hematol Hemoter. 2013;35(2):134–43. https://doi.org/10.5581/1516-8484.20130035.
Saccardi R, Tyndall A, Coghlan G, Denton C, Edan G, Emdin M, et al. Consensus statement concerning cardiotoxicity occurring during haematopoietic stem cell transplantation in the treatment of autoimmune diseases, with special reference to systemic sclerosis and multiple sclerosis. Bone Marrow Transplant. 2004;34(10):877–81. https://doi.org/10.1038/sj.bmt.1704656.
Farge D, Burt RK, Oliveira MC, Mousseaux E, Rovira M, Marjanovic Z, et al. Cardiopulmonary assessment of patients with systemic sclerosis for hematopoietic stem cell transplantation: recommendations from the European Society for Blood and Marrow Transplantation Autoimmune Diseases Working Party and collaborating partners. Bone Marrow Transplant. 2017;52(11):1495–503. https://doi.org/10.1038/bmt.2017.56.
Baron M, Bernier P, Cote LF, Delegge MH, Falovitch G, Friedman G, et al. Screening and therapy for malnutrition and related gastro-intestinal disorders in systemic sclerosis: recommendations of a North American expert panel. Clin Exp Rheumatol. 2010;28(2 Suppl 58):S42–6.
Alantar A, Cabane J, Hachulla E, Princ G, Ginisty D, Hassin M, et al. Recommendations for the care of oral involvement in patients with systemic sclerosis. Arthritis Care Res (Hoboken). 2011;63(8):1126–33. https://doi.org/10.1002/acr.20480.
Johnson SR, Khanna D, Allanore Y, Matucci-Cerinic M, Furst DE. Systemic sclerosis trial design moving forward. J Scleroderma Relat Dis. 2016;1(2):177–80. https://doi.org/10.5301/jsrd.5000198.
Khanna D, Furst DE, Allanore Y, Bae S, Bodukam V, Clements PJ, et al. Twenty-two points to consider for clinical trials in systemic sclerosis, based on EULAR standards. Rheumatology (Oxford). 2015;54(1):144–51. https://doi.org/10.1093/rheumatology/keu288.
Khanna D, Brown KK, Clements PJ, Elashoff R, Furst DE, Goldin J, et al. Systemic sclerosis-associated interstitial lung disease-proposed recommendations for future randomized clinical trials. Clin Exp Rheumatol. 2010;28(2 Suppl 58):S55–62.
Clements P, Allanore Y, Furst DE, Khanna D. Points to consider for designing trials in systemic sclerosis patients with arthritic involvement. Rheumatology (Oxford). 2017;56(suppl_5):v23–v6. https://doi.org/10.1093/rheumatology/kex194.
Furst DE, Braun-Moscovic Y, Khanna D. Points to consider for clinical trials of the gastrointestinal tract in systemic sclerosis. Rheumatology (Oxford). 2017;56(suppl_5):v4–v11. https://doi.org/10.1093/rheumatology/kex195.
Humbert M, Singh M, Furst DE, Khanna D, Seibold JR. Pulmonary hypertension related to systemic sclerosis: points to consider for clinical trials. Rheumatology (Oxford). 2017;56(suppl_5):v33–v7. https://doi.org/10.1093/rheumatology/kex197.
Walker UA, Clements PJ, Allanore Y, Distler O, Oddis CV, Khanna D, et al. Muscle involvement in systemic sclerosis: points to consider in clinical trials. Rheumatology (Oxford). 2017;56(suppl_5):v38–44. https://doi.org/10.1093/rheumatology/kex196.
Allanore Y, Distler O, Walker UA, Khanna D, Furst DE, Meune C. Points to consider when doing a trial primarily involving the heart. Rheumatology (Oxford). 2017;56(suppl_5):v12–v6. https://doi.org/10.1093/rheumatology/kex198.
Galluccio F, Allanore Y, Czirjak L, Furst DE, Khanna D, Matucci-Cerinic M. Points to consider for skin ulcers in systemic sclerosis. Rheumatology (Oxford). 2017;56(suppl_5):v67–71. https://doi.org/10.1093/rheumatology/kex200.
Galluccio F, Muller-Ladner U, Furst DE, Khanna D, Matucci-Cerinic M. Points to consider in renal involvement in systemic sclerosis. Rheumatology (Oxford). 2017;56(suppl_5):v49–52. https://doi.org/10.1093/rheumatology/kex201.
Khanna D, Seibold J, Goldin J, Tashkin DP, Furst DE, Wells A. Interstitial lung disease points to consider for clinical trials in systemic sclerosis. Rheumatology (Oxford). 2017;56(suppl_5):v27–32. https://doi.org/10.1093/rheumatology/kex203.
Cutolo M, Smith V, Furst DE, Khanna D, Herrick AL. Points to consider—Raynaud’s phenomenon in systemic sclerosis. Rheumatology (Oxford). 2017;56(suppl_5):v45–v8. https://doi.org/10.1093/rheumatology/kex199.
Khanna D, Hays RD, Furst DE. Functional disability and other health-related quality-of-life domains: points to consider for clinical trials in systemic sclerosis. Rheumatology (Oxford). 2017;56(suppl_5):v17–22. https://doi.org/10.1093/rheumatology/kex193.
Hansi N, Thoua N, Carulli M, Chakravarty K, Lal S, Smyth A, et al. Consensus best practice pathway of the UK scleroderma study group: gastrointestinal manifestations of systemic sclerosis. Clin Exp Rheumatol. 2014;32(6 Suppl 86):S-214–21.
Khanna D, Gladue H, Channick R, Chung L, Distler O, Furst DE, et al. Recommendations for screening and detection of connective tissue disease-associated pulmonary arterial hypertension. Arthritis Rheum. 2013;65(12):3194–201. https://doi.org/10.1002/art.38172.
Knobler R, Moinzadeh P, Hunzelmann N, Kreuter A, Cozzio A, Mouthon L, et al. European Dermatology Forum S1-guideline on the diagnosis and treatment of sclerosing diseases of the skin, part 1: localized scleroderma, systemic sclerosis and overlap syndromes. J Eur Acad Dermatol Venereol. 2017;31(9):1401–24. https://doi.org/10.1111/jdv.14458.
Baron M, Chung L, Gyger G, Hummers L, Khanna D, Mayes MD, et al. Consensus opinion of a North American Working Group regarding the classification of digital ulcers in systemic sclerosis. Clin Rheumatol. 2014;33(2):207–14. https://doi.org/10.1007/s10067-013-2460-7.
Fujimoto M, Asano Y, Ishii T, Ogawa F, Kawakami T, Kodera M, et al. The wound/burn guidelines - 4: guidelines for the management of skin ulcers associated with connective tissue disease/vasculitis. J Dermatol. 2016;43(7):729–57. https://doi.org/10.1111/1346-8138.13275.
Hughes M, Ong VH, Anderson ME, Hall F, Moinzadeh P, Griffiths B, et al. Consensus best practice pathway of the UK Scleroderma Study Group: digital vasculopathy in systemic sclerosis. Rheumatology (Oxford). 2015;54(11):2015–24. https://doi.org/10.1093/rheumatology/kev201.
Pistorius MA, Carpentier PH. le groupe de travail de la Societe francaise de medecine v. [Minimal work-up for Raynaud syndrome: a consensus report. Microcirculation Working Group of the French Vascular Medicine Society]. J Mal Vasc. 2012;37(4):207–12. https://doi.org/10.1016/j.jmv.2012.05.005.
Pellar RE, Pope JE. Evidence-based management of systemic sclerosis: navigating recommendations and guidelines. Semin Arthritis Rheum. 2017;46(6):767–74. https://doi.org/10.1016/j.semarthrit.2016.12.003.
Walker KM, Pope J, Scleroderma Clinical Trials C, Canadian Scleroderma Research G. Expert agreement on EULAR/EUSTAR recommendations for the management of systemic sclerosis. J Rheumatol. 2011;38(7):1326–8. https://doi.org/10.3899/jrheum.101262.
Johnson SR, Feldman BM, Pope JE, Tomlinson GA. Shifting our thinking about uncommon disease trials: the case of methotrexate in scleroderma. J Rheumatol. 2009;36(2):323–9. https://doi.org/10.3899/jrheum.071169.
Pope JE, Bellamy N, Seibold JR, Baron M, Ellman M, Carette S, et al. A randomized, controlled trial of methotrexate versus placebo in early diffuse scleroderma. Arthritis Rheum. 2001;44(6):1351–8. https://doi.org/10.1002/1529-0131(200106)44:6<1351::AID-ART227>3.0.CO;2-I.
Nakayama A, Tunnicliffe DJ, Thakkar V, Singh-Grewal D, O’Neill S, Craig JC, et al. Patients’ perspectives and experiences living with systemic sclerosis: a systematic review and thematic synthesis of qualitative studies. J Rheumatol. 2016;43(7):1363–75. https://doi.org/10.3899/jrheum.151309.
Johnson SR, O’Brien KK. Qualitative methods in systemic sclerosis research. J Rheumatol. 2016;43(7):1265–7. https://doi.org/10.3899/jrheum.160602.
Pope J, Harding S, Khimdas S, Bonner A, Canadian Scleroderma Research G, Baron M. Agreement with guidelines from a large database for management of systemic sclerosis: results from the Canadian Scleroderma Research Group. J Rheumatol. 2012;39(3):524–31. https://doi.org/10.3899/jrheum.110121.
Walker KM, Pope J, participating members of the Scleroderma Clinical Trials C, Canadian Scleroderma Research G. Treatment of systemic sclerosis complications: what to use when first-line treatment fails--a consensus of systemic sclerosis experts. Semin Arthritis Rheum. 2012;42(1):42–55. https://doi.org/10.1016/j.semarthrit.2012.01.003.
•• Fernandez-Codina A, Walker KM, Pope JE, Scleroderma Algorithm G. Treatment algorithms for systemic sclerosis according to experts. Arthritis Rheumatol. 2018;70(11):1820–8. https://doi.org/10.1002/art.40560. This article provides expert-based consensus on the management of systemic sclerosis and is particularly informative with regards to second-line strategeis.
Funding
Dr. Johnson is supported by the Oscar and Eleanor Markovitz Fund for Scleroderma Research of the Arthritis Research Foundation and a Canadian Institutes of Health Research New Investigator Award.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Dr. Johnson reports grants from the American College of Rheumatology, European League Against Rheumatism, and the Canadian Institutes of Health Research during the conduct of the study and was a site investigator for scleroderma clinical trials supported by Boehringer Ingelheim, National Institutes of Health (US), Bristol Myers Squibb, Roche, Merck, and Bayer outside the submitted work.
Keshini Devakandan declares that she has no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Scleroderma
Rights and permissions
About this article
Cite this article
Johnson, S.R., Devakandan, K. Guidelines and Recommendations Towards Evidence-Based Management of Systemic Sclerosis. Curr Treat Options in Rheum 5, 115–126 (2019). https://doi.org/10.1007/s40674-019-00120-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40674-019-00120-2