Abstract
Purpose
Graves’ disease (GD) is an autoimmune thyroid disease, and the most important characteristic of it is the presence of the thyroid-stimulating antibody (TSAb). The mechanisms of the TSAb elevation are still uncertain. Recent studies have suggested that the dysregulation of regulatory T cell (Treg) and T helper 17 (Th17) might stimulate the production of TSAb and be a pathogenesis of GD. However, the role of Treg and Th17 cells in the pathogenesis of GD is still debated. Our aim is to assess changes of Treg and Th17 cells in the spleen of a mouse in an in vivo GD model and try to explain the pathogenesis of GD.
Methods
We used an adenovirus expressing the autoantigen thyroid-stimulating hormone receptor (Ad-TSHR289) to immunise mice in order to induce GD in the model. Flow cytometry was used to measure the frequencies of splenic Treg and Th17 cells and real-time PCR to analyse the mRNA expression of forkhead box P3(Foxp3) and interleukin-17(IL-17).
Results
Compared with the Ad-Control group, the frequencies of CD4+CD25+Foxp3+ Treg cells were significantly decreased (p = 0.007) and gene expression of Foxp3 was down-regulated (p = 0.001) in the Ad-TSHR289 group. Though there was no significant difference in CD4+IL-17+ T cell subpopulation between the two groups (p = 0.336), the IL-17 mRNA expression was significantly up-regulated in the Ad-TSHR289 group (p = 0.001).
Conclusions
The pathogenesis of GD may be associated with reduced Treg cells and increased IL-17 gene expression. The increased IL-17 mRNA needs to be explained by other mechanisms but not Th17 cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Graves’ disease (GD) is an autoantibody-mediated autoimmune thyroid disease (AITD). It affects primarily women, with an annual incidence of approximately 14 per 100,000 [1]. In America, the incidence of hyperthyroidism is approximately 1.2% [2]. In China and Western countries, the prevalence of GD is approximately 2–3.0 and 0.5–2%, respectively [3, 4]. In England, the incidence of GD is 1–2‰ per year, higher than the rate of 0.3‰ per year reported before [5]. In general, the incidence of GD is increasing steadily. Though the pathogenesis of GD remains elusive, it is associated with a complex interplay of both genetic and non-genetic factors. HLA complex, CTLA-4, CD40, FCRL3, PTPN22 and TSHR may be involved in genetic factors, while iodine, infections, psychological stress, gender, smoking, thyroid damage, vitamin D, selenium, immune-modulating agents and periods of immune reconstitution may contribute to the development of GD among non-genetic factors [6].
There are many medical treatments for GD: some methods are used to inhibit hormone synthesis and/or release, such as thionamides, iodine and compounds containing iodine, perchlorate, lithium, β-adrenergic antagonists and glucocorticoids [7], and other methods are used to eliminate functional thyroid tissue, such as surgery, radioiodine or both. In general, anti-thyroid drugs (ATDs), radioactive iodine (RAI) and surgery are the main methods used by experts. The treatments are different if the patients are in diverse circumstances, including pregnancy, childhood or the manifestation of Graves’ orbitopathy (GO) or thyroid-associated orbitopathy (TAO) [8] that is frequently termed Graves’ ophthalmopathy.
In GD patients, thyroid-stimulating antibodies (TSAbs) combine with the thyroid-stimulating hormone receptor (TSHR) and mimic the effects of the hormone on thyroid cells. They stimulate excessive production of triiodothyronine and thyroxine (T3 and T4) causing some patients to have symptoms of weight loss, tachycardia and anxiety [9]. Kampmann et al. [10] found that 90% patients of GD were TSAb positive in their research and TSAb was highly prevalent in severe/active TAO. Diana et al. [11] conducted a cross-sectional retrospective study and found that the TSAb level was a sensitive, specific and reproducible biomarker for paediatric GD, and it correlated well with disease severity and extrathyroidal manifestations. The presence of TSAb in GD patients has been recognised for a long time; however, the mechanisms that lead to its production are still uncertain.
For a long time, GD has been assumed to be the type 2 helper T cells (Th2)-dominant autoimmune disease. However, some researchers have found that TSAb in many patients are IgG1, the type 1 helper T cells (Th1) subtype in humans [12]. In the mouse model, most TSAb monoclonal antibodies are a Th1 subclass [13]. In addition, among distinct GD models induced by different methods, the types of immune response are different. In Shimojo and the M12-TSHR models, the Th2 immune response seems to be predominant. In mouse GD models induced by immunising with DNA-TSHR, Ad-TSHR or DC-TSHR, Th1 is likely to be important in the immune response [14]. In summary, these controversial data suggest that GD cannot be explained only by the classical Th1/Th2 theory.
Recently, Treg and Th17 lymphocytes have been reported to play apparent roles in the pathogenesis of autoimmune thyroid diseases [15, 16]. The Th17 cell, a recently described T helper cell [17], has been reported to be involved in many autoimmune diseases, such as diabetes mellitus type 1, collagen-induced arthritis, inflammatory bowel diseases [18], multiple sclerosis (MS) and systemic lupus erythematosus (SLE) [19–21]. The association between Th17 cell and GD pathogenesis has also been reported [22, 23].
Treg cell is also important for the regulation of autoimmune diseases [24]. However, conclusions on the changes of the Treg and Th17 cells in a mouse GD model are still controversial. So we used a mouse GD model, which was induced by immunising with an adenovirus expressing thyrotropin receptor (5.62 × 107 PFU/mouse, three times at a three-week interval), and detected the changes of Treg and Th17 cells in these mice 3 weeks after the third immunisation. We tried to explain the possible mechanisms of GD.
Materials and methods
Construction of the recombinant adenovirus expressing TSHR289
We amplified the TSHR289 gene from the plasmid of pSV2neoECE-TSHR289-6H-dhfr (kindly provided by Basil Rapoport at University of California-Los Angeles) to attB1-Kozak-TSHR289/6xHis/IRES/eGFP-attB2 vector with overlapping polymerase chain reaction (PCR). We collected the PCR products that were purified by agarose gel electrophoresis. We used Gateway® technology to recombine the adenovirus vector pAV.EX1d-TSHR289/6xHis/IRES/eGFP (Ad-TSHR289) and translated the recombined adenovirus vector into Escherichia coli Stbl3. We screened out the positive clones by PCR before sequencing. Ad-TSHR289 and null adenovirus (Ad-Control) were transferred into HEK293A cells to produce recombinant adenovirus and null adenovirus. Then, we purified adenovirus by CsCl density gradient centrifugation and measured the titre of the virus by TCID50. We measured the mRNA expression of TSHR289 in HEK293 by RT-PCR. And the titre of the recombinant adenovirus was 3.16 × 1010 PFU/ml. We use Ad-Control as a negative control.
Mice
We purchased BALB/c 6-week-old mice from Vital River Laboratory Animal Technology Co. Ltd. (Beijing, China). All animal experiments were conducted in accordance with regulations in the Institutional Animal Care and Use Committee in Guang’anmen Hospital (Beijing, China). And all the animal studies were conducted in a specific pathogen-free facility.
Immunisation protocols
All the mice were injected intramuscularly (i.m.) with 100 μl phosphate-buffered saline (PBS) (n = 9), 100 μl PBS containing 5.62 × 107 PFU of Ad-TSHR289 (n = 9) or Ad-Control (n = 9). Mice were i.m. injected three times at 3-week intervals. Three weeks after the last injection, blood, spleens and thyroid tissues were obtained for further tests.
Thyroid function test
We measured total thyroxine (T4) and TSH receptor autoantibodies (TRAb) in mouse sera with a commercially available radioimmunoassay kit (Cisbio Bioassays, Codolet, France) and a commercially available TRAb kit (Cisbio Bioassays, Codolet, France), respectively. The normal range of T4 and TRAb was defined as the mean ± 3 SD of Ad-Control mice.
Thyroid histology
Observed primarily
Thyroid glands were obtained and observed directly with a measuring scale.
Observed under light microscope
We obtained mice thyroid glands and fixed them with 10% formalin in PBS, then embedded the tissues in paraffin and cut them into 5-μm-thick sections, and stained them with haematoxylin and eosin (H&E). At last, we observed the thyroid tissues under light microscope (Nikon eclipse Ti, Japan).
Observed under transmission electron microscope (TEM)
Thyroid tissues were cut into small blocks about 1 mm3 and fixed in 2% osmic acid solution immediately. We immersed them in 0.2 M PBS (pH 7.4) for 10 min three times and fixed the samples in 2% osmic acid solution. Then, we embedded the specimens, and positioned, sliced, and stained them. We made the ultrathin sections 100 nm thick and 0.5 mm2. Finally, we observed the changes in thyroid follicular epithelial cells by a Hitachi-7650 microscope (Hitachi, China). We obtained all the images using a Gatan 832CCD camera (Gatan).
Flow cytometry
We pressed mice spleen tissues through a nylon mesh and removed red cells with lysing buffer (BD Pharm Lyse, San Diego, CA, USA) to prepare a single-cell suspension of splenic cells. First, we stimulated the splenic cell suspension (1 × 106 cells/ml) and cultured it for 5 h with leucocyte activation cocktail (BD PharMingen, San Diego, CA, USA) in the DMEM (HyClone, Utah, USA) at 37 °C. Then, we stained them with FITC-CD4 antibody (BD PharMingen, San Diego, CA, USA) and APC-CD25 antibody (BD PharMingen, San Diego, CA, USA). After 20-min incubation at 4 °C, we washed them by stain buffer (FBS) (BD PharMingen, San Diego, CA, USA). We fixed and permeabilised them with Transcription Factor Buffer Set (BD PharMingen, San Diego, CA, USA) with reference to the recommended assay procedure. We then proceeded with the intracellular staining. All the cells were incubated with PerCP-Cy™ 5.5-labelled rat anti-mouse IL-17A antibody (BD PharMingen, San Diego, CA, USA) and PE-labelled rat anti-mouse Foxp3 antibody (BD PharMingen, San Diego, CA, USA) at 4 °C for 45 min, protected from light. Then, by washing and re-suspending all the cells, we analysed and acquired data using CellQuest software (BD Biosciences, Mountain View, CA, USA). We set quadrants referring to the staining of FITC Rat IgG2a,κisotype control (BD PharMingen, San Diego, CA, USA), APC Rat IgG1,λisotype control (BD PharMingen, San Diego, CA, USA) and PE Rat IgG2a,κisotype control (BD PharMingen, San Diego, CA, USA).
Quantitative real-time RT-PCR analysis
We isolated the total RNA from 0.09 to 0.18 g fresh splenocytes with 1 ml Trizol reagent (Tiangen Biotech, Beijing, China) and synthesised cDNA with an RT Reagent Kit (Tiangen Biotech, Beijing, China) by PEQSTAR 96 universal gradient PCR System (PeqLab GmbH, Germany). We performed real-time PCR by 7500 Fast Real-time PCR System (Applied Biosystems, USA) with a Real-time PCR Kit (Tiangen Biotech, Beijing, China). We designed the primers for IL17, Foxp3 (Treg-specific transcription factor) and GAPDH mRNA by Primer Premier 5.0 as follows: Foxp3, forward primer, 5′-TAC CTC AAC CGT TCC AC-3′; reverse primer, 5′-TCT CAG GCT CCC TCT TC-3′; IL-17, forward primer, 5′-GGA GAA AGC GGA TAC CAA-3′; reverse primer, 5′-TGT GAG GAC TAC CGA GCC-3′. Reference primer of GAPDH was as follows: forward primer, 5′-AGG TCG GTG TGA ACG GAT TTG-3′; reverse primer, 5′-TGT AGA CCA TGT AGT TGA GGT CA-3′. With the above primers, PCR amplification was carried out under the following conditions: 94 °C for 10 min, followed by 40 cycles of 94 °C for 15 s, and 60 °C for 30 s. We used approximately 50 ng of cDNA in every reaction. We obtained all the data as Ct values and determined ΔCt values. We performed the reactions in triplicate and expressed them as mean ± SEM ΔCt values.
Data analysis
We performed the statistical analysis by SPSS 22.0 software. All data were expressed as mean ± standard deviation (SD). The normality of data was tested by Kolmogorov–Smirnov test. Differences between groups were analysed by one-way analysis of variance (ANOVA) with LSD test. p value less than 0.05 was considered to indicate statistical significance. The Kruskal–Wallis tests were used when data were not normally distributed.
Results
TRAb and T4 titre in Serum
Mean ± SD of T4 and TRAb in murine serum were 106.29 ± 13.05 ng/ml (ranging from 30.62 to 153.36) and 0.69 ± 0.10 u/l (ranging from 0.38 to 1.13) in the Ad-Control group. There were no significant differences between the Control group and Ad-Control group in serum T4 and TRAb. T4 and TRAb increased in all the mice of Ad-TSHR289 group (immunised with Ad-TSHR289 adenovirus). Both of them were above the mean ± 3SD of Ad-Control group (immunised with null adenovirus). The Ad-TSHT289 group had significant differences with the Control group (p < 0.001) and the Ad-Control group (p < 0.001). Thus, in all results, 9 (100%) female BALB/c mice have been induced to develop GD (as shown in Fig. 1).
Serum thyroxine (T4) and TRAb levels: T4 (a) and TRAb (b) levels were measured 3 weeks after the last immunisation. BALB/c mice were injected intramuscularly with Ad-TSHR289 adenovirus (Ad-TSHR289), null adenovirus (Ad-Control) or PBS (Control). Area below the horizontal lines indicates the mean ± 3 SD of T4 and TRAb values for 9 mice in Ad-Control group. Significant differences: aControl versus Ad-TSHR289, bAd-Control versus Ad-TSHR289
Thyroid histology in mice
Differences in the appearance of mice thyroid tissues were observed in three groups. Thyroid tissues in Ad-TSHR289 were darker and heavier than in Ad-Control and Control (Fig. 2a–c). Thyroid weight (TW) and body weight (BW) of mice were measured, and TW/BW was calculated. The TW/BW was 0.0002571 ± 0.0000831, 0.0002243 ± 0.0000629 and 0.000572 ± 0.00012 in Control, Ad-Control and Ad-TSHR289, respectively. There was no significant difference between Ad-Control and Control (p > 0.05), but a significant difference between Ad-Control and Ad-TSHR289 in TW/BW (p < 0.001) (Fig. 2d).
Appearance of mice thyroid tissues and TW/BW: Thyroid tissues in Ad-TSHR289 (a) were 1 mm wider than Ad-Control (b) and Control (c). TW/BW of Ad-TSHR289 was higher than Ad-Control and Control, and Ad-TSHR289 had a significant statistical difference when compared with Ad-Control and Control (d). Significant differences: aControl versus Ad-TSHR289, bAd-Control versus Ad-TSHR289
In the Ad-TSHR289 group (Fig. 3c), the thyroid tissues that were stained by H&E showed diffuse enlargement, and the thyroid follicular epithelia were hypertrophied and hypercellular. Compared with the Ad-Control group (Fig. 3b) and the Control group (Fig. 3a), we observed that the follicular lumen had some protrusion and the colloid in it was also decreased. These changes are similar to those observed in GD patients [5]. However, we did not observe inflammatory cell infiltration in mice thyroid.
Histographs of thyroid observed by light microscope (Stained by H&E) (×200 magnification): In contrast to Control (a) and Ad-Control (b), thyroid tissues from Ad-TSHR289 (c) were consistent with hyperthyroidism. They were more vacuolated with less amounts of colloid, and the thyroid follicular epithelia were hypertrophied and hypercellular. Protrusion was observed in the follicular lumen. There was no inflammatory infiltration in thyroid tissues
The ultrastructure of mice thyroid glands from the Ad-TSHR289 group was also changed as observed by TEM. They showed irregular nucleus, nuclear membrane invaginates, chromatin condensation and aggregation at the periphery of the nucleons when compared with the Control and Ad-Control groups. Increased number and irregularly swollen morphology were observed in the mitochondria. The cristae (infolding or convolutions) of mitochondria became fractured and fuzzy. A large number of lipid droplets filled the cytoplasm. Their rough endoplasmic reticulum was extended and wrapped around mitochondria (Fig. 4).
Histographs of thyroid observed by TEM (×1000–7000 magnification): Thyroid glands from the Ad-TSHR289 group (e) showed irregular nuclei, nuclear membrane invaginates, chromatin condensation and aggregation at the periphery of the nucleons compared with the Ad-Control group (c) and the Control group (a). The Ad-TSHR289 group (f) also showed mitochondria increase and irregular swelling. The cristae of mitochondria had fractured and become fuzzy. A large number of lipid droplets had filled their cytoplasm. Their rough endoplasmic reticulum was extended and wrapped around the mitochondria. The Ad-Control group (d) and the Control group (b) showed less mitochondria and their cristae were clear. The form of the rough endoplasmic reticulum was normal
Decreased Treg and increased IL-17 mRNA levels in spleen of Ad-TSHR289 group
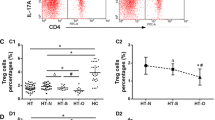
The amounts of CD4+CD25+Foxp3+ Treg cells in the Ad-TSHR289 group (2.89 ± 1.19%) depleted significantly in contrast to the Control group (5.05 ± 2.15%) (p < 0.05) and the Ad-Control group (5.36 ± 2.10%) (p < 0.05), and there were no significant differences between the Control and the Ad-Control groups (p > 0.05) (Fig. 5b). We also obtained a similar result from flow cytometry detection. In the Ad-TSHR289 group, the expression of Foxp3 mRNA (Fig. 5d) in splenic cells had also decreased (0.13 ± 0.10) as compared with the Control group (1.09 ± 0.48) (p < 0.001) and the Ad-Control group (1.19 ± 0.52) (p < 0.001). We did not find significant differences among the three groups in the proportions of CD4+IL-17+T cell in splenic cells by flow cytometry (p > 0.05) (Fig. 5c). However, the expression of IL-17 mRNA in the spleen was higher in the Ad-TSHR289 group (4.16 ± 1.29) in contrast to the Control group (1.05 ± 0.31) (p < 0.001) and the Ad-Control group (0.90 ± 0.50) (p < 0.001) (Fig. 5e).
Flow cytometric analysis of Treg cell and Th17 cell in spleen and quantitative real-time RT-PCR detection of Foxp3 and IL-17 mRNA expression. a An example of a flow cytometry result. The percentages of CD4+CD25+Foxp3+ Treg cell and CD4+IL-17+T cell were analysed by four-colour flow cytometry. Splenic cells were first stained with FITC-labelled anti-mouse CD4 and APC-labelled anti-mouse CD25. After permeabilising, they were stained with PE-labelled anti-mouse Foxp3 and PerCP-CyTM 5.5-labelled anti-mouse IL-17A. b The CD4+CD25+Foxp3+ Treg cell ratio in spleen was significantly decreased in the Ad-TSHR289 mice when compared with the Control and the Ad-Control mice. c The CD4+IL-17+ T cell ratio in spleen had no significant difference among the Ad-TSHR289, Control and Ad-Control groups. d The expression of Foxp3 mRNA was significantly down-regulated in the Ad-TSHR289 group when compared with the Control and the Ad-Control mice. e The expression of IL-17 mRNA was significantly up-regulated in the Ad-TSHR289 group as compared with the Control and the Ad-Control mice. Significant differences: aControl versus Ad-TSHR289, bAd-Control versus Ad-TSHR289
Discussion
In our research, all the mice (100%) immunised with Ad-TSHR289 became hyperthyroid. Their serum T4 and TRAb were increased above the mean ± 3SD of the Ad-Control group. The changes in thyroid histology such as diffuse enlargement, hypertrophied and hypercellular follicular epithelia, protrusion of the follicular lumen and reduced amounts of colloid were similar to previous studies. However, lymphocyte infiltration was not observed in these mice thyroids [25]. There were no significant differences between the Control group and the Ad-Control group in serum T4 and TRAb.
Besides, we observed the appearance of mice thyroid and found that thyroid tissues in the Ad-TSHR289 group were darker and heavier than in the Control and Ad-Control. This showed that the thyroid of Ad-TSHR289 had abundant blood supply, which is consistent with clinical GD patients. In addition, we also observed the thyroid tissues by TEM. The number of mitochondria had increased, and they had swelled irregularly. Besides, the rough endoplasmic reticulum was extended and wrapped around the mitochondria. These phenomena might throw light on the acceleration of thyroid hormone synthesis.
All the changes of serum markers and histology have proved the successful induction of this GD model, but how does one explain these pathogenic changes? Although Th1 and Th2 played crucial roles in the pathogenesis of GD, GD cannot be viewed simply by the balance of Th1 and Th2 immune response. Recently, more and more researches have paid greater attention to Treg and Th17 cells. These two types of lymphocytes play crucial roles in immune responses and inflammatory diseases.
In observing the changes of Th17 cell and Treg cells in the mouse GD model, we detected their functions in different aspects including cell proportions and key transcription factor or important cytokine. In our study, we found that both Treg cell proportion and expression of Foxp3 mRNA decreased in contrast to the Control and Ad-Control mice. Although the percentage of CD4+IL-17+ T cell in mice spleen had no significant difference between groups, the expression of IL-17 mRNA in spleen was higher in Ad-TSHR289 group than in the Control and Ad-Control groups.
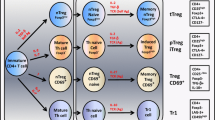
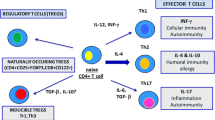
Treg cells play an important role in the regulation of immune response. It can maintain homoeostasis and prevent autoimmune diseases. And it plays a leading role in developing immune tolerance through active suppression. Treg cells can be divided into three subtypes. They are natural Treg (nTreg) lymphocytes, CD69+ Treg lymphocytes and type 1 regulatory (Tr1) lymphocytes. Regulatory T cells with an identical phenotype of nTreg cells can be generated in different places; thus, they have different names. They are called tTreg (thymus-derived Treg), pTreg (peripheral differentiated Treg) and iTreg (generated in vitro). The nTreg cells, including tTreg, pTreg and iTreg cells, are differentiated in the milieu of TGF-β and IL-2, while CD69+ Treg and Tr1 cells are differentiated in the milieu of IL-27 and IL-10, respectively. The nTreg cells express Foxp3, while CD69+ Treg and Tr1 cells do not. As the Treg cells mainly expressing Foxp3 can suppress adaptive T cell and prevent autoimmunity [26, 27], our study was fixed on CD4+CD25+Foxp3+ Treg cells. Some researchers have verified that deficiency in or dysfunction of Treg cell can be a cause of autoimmune disease [28]. The reduction in Treg cell or attenuation of its suppressive activity may elicit immunodeficiency. In Bossowski et al.’s report [29], a significant decrease in CD4+Foxp3+ and CD4+CD25 (high) T lymphocytes was found in untreated patients with GD and Hashimoto’s thyroiditis as compared to the healthy control subjects. Chaoming Mao found that the proportion of CD4+CD25+Foxp3+ Treg cells in the peripheral blood of untreated GD group is lower than the control donor group [30]. In Saitoh and Nagayamas research [31], they also found the depletion of CD4+CD25+ T cell aggravated hyperthyroidism in mice GD models. Overall, the changes of Treg cells in different researches were similar, and our results were consistent with their conclusions. The decreased proportion of CD4+CD25+Foxp3+ Treg cells may reduce the suppression of immune response by four mechanisms. Firstly, it can affect the function and maturation of antigen-presenting cell (APC). Qureshi et al. [32] found that CTLA-4 that expressed by Treg cells can lead to physical removal of CD80 and CD86 from the APC cell surface by trans-endocytosis and degradation. So the reduction of Treg cells can up-regulate the co-stimulatory molecules CD80 and CD86 and finally strengthen the immune response. Secondly, target cell apoptosis will reduce because of the diminishment of CD4+CD25+Foxp3+ Treg cells. Cao et al. [33] documented that Treg cells used granzyme B and perforin to suppress immune response against tumours. So diminished CD4+CD25+Foxp3+ Treg cells will cause less apoptosis in effector T cell and aggravate autoimmune diseases. Thirdly, the reduction of Treg cells can reduce the anti-inflammatory cytokines. Fahlén [34], Hara et al. [35] and Collison et al. [36] have reported that TGF-β, IL-10 and IL-35 secreted by Treg cells play an important role in control of immune response, respectively. The reduction of CD4+CD25+Foxp3+ Treg cells will lessen these anti-inflammatory cytokines and lead to inflammation. Fourthly, a decline in Treg cells can disrupt the metabolic pathway. In Deaglio S’ report [37], CD39 produced by Treg cell can catalyse the degradation of a pro-inflammatory molecule, adenosine triphosphate (ATP). The suppression of T cell proliferation in CD39 knockout mice was reduced. In this way, diminished CD4+CD25+Foxp3+ Treg cells will reduce the production of CD39 and disrupt the process of degradation of the ATP and aggravate autoimmune diseases. Thus, it is probable that through the mechanisms mentioned above, the absence of Treg cells may lead immune responses in thyroid tissue.
However, the study on the change of Th17 cells in GD remains controversial. Th17 cells are also differentiated from naive CD4+ T cells but that depends on a different local cytokine milieu. The differentiation of Th17 cells is mainly induced by the participation of TGF-β and IL-6, which activate transcription factors Smads and STAT3, respectively, and induce the expression of the transcription factor RORC2. IL-21 and IL-23 also participated in this process. IL-21 promotes this process in a positive feedback manner and IL-23 makes Th17 cells achieve their full function [38]. Of note, Th17 cells exert a pathogenic role when they require a further differentiation. Only when they were exposed to IL-23, were they converted into pathogenic or pro-inflammatory cells, synthesising GM-CSF and IFN-γ, which could damage the tissues in different autoimmune diseases [38–43]. However, if they were affected by TGF-β, they would convert into non-pathogenic lymphocytes, which could be a defence against bacteria and fungi. Zhou et al. [44] found that there was no significant difference between the Ad-TSHR289 and Ad-Control groups in terms of splenic Th17 cell number and the expression of transcription factor RORct mRNA. They attributed the pathogenesis of GD to the reduction of Treg cells and the increased ratio of Th17/Treg. They believed that the Th17 cell is not associated with the disease. In our research, we also found that the percentage of CD4+IL-17+ T cell in mice spleen did not show a difference between the Ad-Control and Ad-TSHR289 groups. However, the expression of IL-17 mRNA in spleen increased in the Ad-TSHR289 group. Many studies have proved that IL-17 plays an important role in autoimmune diseases. Komiyama et al. [45] found that IL-17 played a crucial role in the development of experimental autoimmune encephalomyelitis. Nakae et al. [19] demonstrated that IL-17 was responsible for the priming of collagen-specific T cells and collagen-specific IgG2a production and it played a crucial role in the development of collagen-induced arthritis. Lubberts et al. [46] also proved that IL-17 contributed to joint destruction in collagen-induced arthritis. In autoimmune thyroid diseases, IL-17 may also be a pathogenic factor. In Kim et al. research [47], they found that patients with Graves’ ophthalmopathy (GO) had high concentrations and positive detection rates of serum IL-17 compared with the Control group. The serum levels of IL-17 in active GO patients were higher than those in inactive GO patients. Zheng et al. [48] found that the expression of IL-17 mRNA and IL-17 protein levels was significantly higher in GD and euthyroid GD patients as compared with healthy people. Based on the studies above, IL-17 may be a pathogenesis in our mouse GD model, but how to explain the inconsistency between the increased IL-17 and non-notably increased CD4+IL-17+ T cell? Th17 cells are not the only source for IL-17. It is also secreted by γδT, natural killer T (NKT), CD8+ T and lymph tissue inducer cells [49]. Murine CD8+ T cells that produce IL-17 after culture in medium from dendritic cells (DCs) were exposed to Klebsiella pneumonia [50]. In the spleen of IL-6 knockout mice, the IL-17 production when stimulated with anti-CD3 and IL-23 originates largely from NKT cells [51]. Sutton et al. [52] demonstrated that γδT cells are an important source of innate IL-17 and play an important role in experimental autoimmune encephalomyelitis (EAE) induction. Therefore, we may reasonably speculate that the increased expression of IL-17 mRNA that plays an important role in GD comes from the other IL-17-producing cells but not Th17 cells. The increased IL-17 mRNA needs to be explained by other mechanisms.
In conclusion, the pathogenesis of GD may be associated with reduced Treg cells and increased IL-17 gene expression. The elevated IL-17 mRNA expression may not be associated with Th17 cells but other IL-17-producing cells.
There were certain limitations to our study. Firstly, if the increased IL-17 was secreted by other T cells, where is the source of this IL-17? We will further explore the origination of IL-17 in a mouse GD model. Secondly, recent studies have shown that IL-17 productions by γδ T cells and NKT cells are independent of IL-6 [51, 53]. This process is different from the development of Th17 cells. Some studies demonstrated that γδT cells constitutively express IL-23R. IL-23 in combination with IL-1β can promote IL-17 expression by γδT cells in the absence of additional signals. So, further studies to detect the changes of IL-6 and IL-23 in a mouse GD model are needed. Besides, as the interchange of Treg and Th17 cells has been found [54], the relationship of these two types of lymphocytes and the conditions of interchange still need further study. We will continue further research to fully elucidate the complex immunological mechanisms of GD.
References
Cooper GS, Stroehla BC (2003) The epidemiology of autoimmune diseases. Autoimmun Rev 2(3):119–125
Bahn RS, Burch HB, Cooper DS, Garber JR, Greenlee MC, Klein I, Laurberg P, McDougall IR, Montori VM, Rivkees SA, Ross DS, Sosa JA, Stan MN (2011) Hyperthyroidism and other causes of thyrotoxicosis: management guidelines of the American Thyroid Association and American Association of Clinical Endocrinologists. Endocr Pract 17(3):456–520
Zhang K, Lin Y, Fang Z, Luo C, Liu X, Zhang F, Chen G, Wensheng WU (2002) The effect of salt iodization for 10 years on the prevalences of endemic goiter and hyperthyroidism. Chin J Endocrinol Metab (5):12–14
Hollowell JG, Staehling NW, Flanders WD, Hannon WH, Gunter EW, Spencer CA, Braverman LE (2002) Serum TSH, T(4), and thyroid antibodies in the United States population (1988 to 1994): National Health and Nutrition Examination Survey (NHANES III). J Clin Endocrinol Metab 87(2):489–499. doi:10.1210/jcem.87.2.8182
DeGroot LJ (2000) Graves’ Disease and the Manifestations of Thyrotoxicosis. In: De Groot LJ, Beck-Peccoz P, Chrousos G et al (eds) Endotext. MDText.com Inc, South Dartmouth
Marino M, Latrofa F, Menconi F, Chiovato L, Vitti P (2015) Role of genetic and non-genetic factors in the etiology of Graves’ disease. J Endocrinol Invest 38(3):283–294. doi:10.1007/s40618-014-0214-2
Marino M, Latrofa F, Menconi F, Chiovato L, Vitti P (2014) An update on the medical treatment of Graves’ hyperthyroidism. J Endocrinol Invest 37(11):1041–1048. doi:10.1007/s40618-014-0136-z
Bartalena L, Chiovato L, Vitti P (2016) Management of hyperthyroidism due to Graves’ disease: frequently asked questions and answers (if any). J Endocrinol Invest. doi:10.1007/s40618-016-0505-x
Morshed SA, Latif R, Davies TF (2012) Delineating the autoimmune mechanisms in Graves’ disease. Immunol Res 54(1–3):191–203. doi:10.1007/s12026-012-8312-8
Kampmann E, Diana T, Kanitz M, Hoppe D, Kahaly GJ (2015) Thyroid stimulating but not blocking autoantibodies are highly prevalent in severe and active thyroid-associated orbitopathy: a prospective study. Int J Endocrinol 2015:678194. doi:10.1155/2015/678194
Diana T, Brown RS, Bossowski A, Segni M, Niedziela M, Konig J, Bossowska A, Ziora K, Hale A, Smith J, Pitz S, Kanitz M, Kahaly GJ (2014) Clinical relevance of thyroid-stimulating autoantibodies in pediatric graves’ disease-a multicenter study. J Clin Endocrinol Metab 99(5):1648–1655. doi:10.1210/jc.2013-4026
Weetman AP, Yateman ME, Ealey PA, Black CM, Reimer CB, Williams RC Jr, Shine B, Marshall NJ (1990) Thyroid-stimulating antibody activity between different immunoglobulin G subclasses. J Clin Invest 86(3):723–727. doi:10.1172/jci114768
McLachlan SM, Nagayama Y, Rapoport B (2005) Insight into Graves’ hyperthyroidism from animal models. Endocr Rev 26(6):800–832. doi:10.1210/er.2004-0023
Nagayama Y (2007) Graves’ animal models of Graves’ hyperthyroidism. Thyroid 17(10):981–988. doi:10.1089/thy.2007.0161
Zuniga LA, Jain R, Haines C, Cua DJ (2013) Th17 cell development: from the cradle to the grave. Immunol Rev 252(1):78–88. doi:10.1111/imr.12036
Grant CR, Liberal R, Mieli-Vergani G, Vergani D, Longhi MS (2015) Regulatory T-cells in autoimmune diseases: challenges, controversies and–yet–unanswered questions. Autoimmun Rev 14(2):105–116. doi:10.1016/j.autrev.2014.10.012
Infante-Duarte C, Horton HF, Byrne MC, Kamradt T (2000) Microbial lipopeptides induce the production of IL-17 in Th cells. J Immunol 165(11):6107–6115
Hundorfean G, Neurath MF, Mudter J (2012) Functional relevance of T helper 17 (Th17) cells and the IL-17 cytokine family in inflammatory bowel disease. Inflamm Bowel Dis 18(1):180–186. doi:10.1002/ibd.21677
Nakae S, Nambu A, Sudo K, Iwakura Y (2003) Suppression of immune induction of collagen-induced arthritis in IL-17-deficient mice. J Immunol 171(11):6173–6177
Steinman L (2005) Blocking adhesion molecules as therapy for multiple sclerosis: natalizumab. Nat Rev Drug Discov 4(6):510–518. doi:10.1038/nrd1752
Hsu HC, Yang P, Wang J, Wu Q, Myers R, Chen J, Yi J, Guentert T, Tousson A, Stanus AL, Le TV, Lorenz RG, Xu H, Kolls JK, Carter RH, Chaplin DD, Williams RW, Mountz JD (2008) Interleukin 17-producing T helper cells and interleukin 17 orchestrate autoreactive germinal center development in autoimmune BXD2 mice. Nat Immunol 9(2):166–175. doi:10.1038/ni1552
Bedoya SK, Lam B, Lau K, Larkin J 3rd (2013) Th17 cells in immunity and autoimmunity. Clin Dev Immunol 2013:986789. doi:10.1155/2013/986789
Nanba T, Watanabe M, Inoue N, Iwatani Y (2009) Increases of the Th1/Th2 cell ratio in severe Hashimoto’s disease and in the proportion of Th17 cells in intractable Graves’ disease. Thyroid 19(5):495–501. doi:10.1089/thy.2008.0423
von Spee-Mayer C, Siegert E, Abdirama D, Rose A, Klaus A, Alexander T, Enghard P, Sawitzki B, Hiepe F, Radbruch A, Burmester GR, Riemekasten G, Humrich JY (2015) Low-dose interleukin-2 selectively corrects regulatory T cell defects in patients with systemic lupus erythematosus. Ann Rheum Dis. doi:10.1136/annrheumdis-2015-207776
Chen CR, Pichurin P, Chazenbalk GD, Aliesky H, Nagayama Y, McLachlan SM, Rapoport B (2004) Low-dose immunization with adenovirus expressing the thyroid-stimulating hormone receptor A-subunit deviates the antibody response toward that of autoantibodies in human Graves’ disease. Endocrinology 145(1):228–233. doi:10.1210/en.2003-1134
Roncarolo MG, Gregori S, Bacchetta R, Battaglia M (2014) Tr1 cells and the counter-regulation of immunity: natural mechanisms and therapeutic applications. Curr Top Microbiol Immunol 380:39–68. doi:10.1007/978-3-662-43492-5_3
Marazuela M, Garcia-Lopez MA, Figueroa-Vega N, de la Fuente H, Alvarado-Sanchez B, Monsivais-Urenda A, Sanchez-Madrid F, Gonzalez-Amaro R (2006) Regulatory T cells in human autoimmune thyroid disease. J Clin Endocrinol Metab 91(9):3639–3646. doi:10.1210/jc.2005-2337
Sakaguchi S (2005) Naturally arising Foxp3-expressing CD25 + CD4 + regulatory T cells in immunological tolerance to self and non-self. Nat Immunol 6(4):345–352. doi:10.1038/ni1178
Bossowski A, Moniuszko M, Dabrowska M, Sawicka B, Rusak M, Jeznach M, Wojtowicz J, Bodzenta-Lukaszyk A, Bossowska A (2013) Lower proportions of CD4 + CD25(high) and CD4 + FoxP3, but not CD4 + CD25 + CD127(low) FoxP3 + T cell levels in children with autoimmune thyroid diseases. Autoimmunity 46(3):222–230. doi:10.3109/08916934.2012.751981
Mao C, Wang S, Xiao Y, Xu J, Jiang Q, Jin M, Jiang X, Guo H, Ning G, Zhang Y (2011) Impairment of regulatory capacity of CD4 + CD25 + regulatory T cells mediated by dendritic cell polarization and hyperthyroidism in Graves’ disease. J Immunol 186(8):4734–4743. doi:10.4049/jimmunol.0904135
Saitoh O, Nagayama Y (2006) Regulation of Graves’ hyperthyroidism with naturally occurring CD4 + CD25 + regulatory T cells in a mouse model. Endocrinology 147(5):2417–2422. doi:10.1210/en.2005-1024
Qureshi OS, Zheng Y, Nakamura K, Attridge K, Manzotti C, Schmidt EM, Baker J, Jeffery LE, Kaur S, Briggs Z, Hou TZ, Futter CE, Anderson G, Walker LS, Sansom DM (2011) Trans-endocytosis of CD80 and CD86: a molecular basis for the cell-extrinsic function of CTLA-4. Science 332(6029):600–603. doi:10.1126/science.1202947
Cao X, Cai SF, Fehniger TA, Song J, Collins LI, Piwnica-Worms DR, Ley TJ (2007) Granzyme B and perforin are important for regulatory T cell-mediated suppression of tumor clearance. Immunity 27(4):635–646. doi:10.1016/j.immuni.2007.08.014
Fahlen L, Read S, Gorelik L, Hurst SD, Coffman RL, Flavell RA, Powrie F (2005) T cells that cannot respond to TGF-beta escape control by CD4(+)CD25(+) regulatory T cells. J Exp Med 201(5):737–746. doi:10.1084/jem.20040685
Hara M, Kingsley CI, Niimi M, Read S, Turvey SE, Bushell AR, Morris PJ, Powrie F, Wood KJ (2001) IL-10 is required for regulatory T cells to mediate tolerance to alloantigens in vivo. J Immunol 166(6):3789–3796
Collison LW, Workman CJ, Kuo TT, Boyd K, Wang Y, Vignali KM, Cross R, Sehy D, Blumberg RS, Vignali DA (2007) The inhibitory cytokine IL-35 contributes to regulatory T-cell function. Nature 450(7169):566–569. doi:10.1038/nature06306
Deaglio S, Dwyer KM, Gao W, Friedman D, Usheva A, Erat A, Chen JF, Enjyoji K, Linden J, Oukka M, Kuchroo VK, Strom TB, Robson SC (2007) Adenosine generation catalyzed by CD39 and CD73 expressed on regulatory T cells mediates immune suppression. J Exp Med 204(6):1257–1265. doi:10.1084/jem.20062512
Song X, Gao H, Qian Y (2014) Th17 differentiation and their pro-inflammation function. Adv Exp Med Biol 841:99–151. doi:10.1007/978-94-017-9487-9_5
Ghoreschi K, Laurence A, Yang XP, Tato CM, McGeachy MJ, Konkel JE, Ramos HL, Wei L, Davidson TS, Bouladoux N, Grainger JR, Chen Q, Kanno Y, Watford WT, Sun HW, Eberl G, Shevach EM, Belkaid Y, Cua DJ, Chen W, O’Shea JJ (2010) Generation of pathogenic T(H)17 cells in the absence of TGF-beta signalling. Nature 467(7318):967–971. doi:10.1038/nature09447
Langrish CL, Chen Y, Blumenschein WM, Mattson J, Basham B, Sedgwick JD, McClanahan T, Kastelein RA, Cua DJ (2005) IL-23 drives a pathogenic T cell population that induces autoimmune inflammation. J Exp Med 201(2):233–240. doi:10.1084/jem.20041257
Ghoreschi K, Laurence A, Yang XP, Hirahara K, O’Shea JJ (2011) T helper 17 cell heterogeneity and pathogenicity in autoimmune disease. Trends Immunol 32(9):395–401. doi:10.1016/j.it.2011.06.007
Lee Y, Awasthi A, Yosef N, Quintana FJ, Xiao S, Peters A, Wu C, Kleinewietfeld M, Kunder S, Hafler DA, Sobel RA, Regev A, Kuchroo VK (2012) Induction and molecular signature of pathogenic TH17 cells. Nat Immunol 13(10):991–999. doi:10.1038/ni.2416
Basdeo SA, Moran B, Cluxton D, Canavan M, McCormick J, Connolly M, Orr C, Mills KH, Veale DJ, Fearon U, Fletcher JM (2015) Polyfunctional, pathogenic CD161 + Th17 lineage cells are resistant to regulatory T cell-mediated suppression in the context of autoimmunity. J Immunol 195(2):528–540. doi:10.4049/jimmunol.1402990
Zhou J, Bi M, Fan C, Song X, Yang R, Zhao S, Li L, Li Y, Teng W, Shan Z (2012) Regulatory T cells but not T helper 17 cells are modulated in an animal model of Graves’ hyperthyroidism. Clin Exp Med 12(1):39–46. doi:10.1007/s10238-011-0137-6
Komiyama Y, Nakae S, Matsuki T, Nambu A, Ishigame H, Kakuta S, Sudo K, Iwakura Y (2006) IL-17 plays an important role in the development of experimental autoimmune encephalomyelitis. J Immunol 177(1):566–573
Lubberts E, Joosten LA, Oppers B, van den Bersselaar L, Coenen-de Roo CJ, Kolls JK, Schwarzenberger P, van de Loo FA, van den Berg WB (2001) IL-1-independent role of IL-17 in synovial inflammation and joint destruction during collagen-induced arthritis. J Immunol 167(2):1004–1013
Kim SE, Yoon JS, Kim KH, Lee SY (2012) Increased serum interleukin-17 in Graves’ ophthalmopathy. Graefes Arch Clin Exp Ophthalmol 250(10):1521–1526. doi:10.1007/s00417-012-2092-7
Zheng L, Ye P, Liu C (2013) The role of the IL-23/IL-17 axis in the pathogenesis of Graves’ disease. Endocr J 60(5):591–597
Xu S, Cao X (2010) Interleukin-17 and its expanding biological functions. Cell Mol Immunol 7(3):164–174. doi:10.1038/cmi.2010.21
Happel KI, Zheng M, Young E, Quinton LJ, Lockhart E, Ramsay AJ, Shellito JE, Schurr JR, Bagby GJ, Nelson S, Kolls JK (2003) Cutting edge: roles of Toll-like receptor 4 and IL-23 in IL-17 expression in response to Klebsiella pneumoniae infection. J Immunol 170(9):4432–4436
Rachitskaya AV, Hansen AM, Horai R, Li Z, Villasmil R, Luger D, Nussenblatt RB, Caspi RR (2008) Cutting edge: NKT cells constitutively express IL-23 receptor and RORgammat and rapidly produce IL-17 upon receptor ligation in an IL-6-independent fashion. J Immunol 180(8):5167–5171
Sutton CE, Lalor SJ, Sweeney CM, Brereton CF, Lavelle EC, Mills KH (2009) Interleukin-1 and IL-23 induce innate IL-17 production from gammadelta T cells, amplifying Th17 responses and autoimmunity. Immunity 31(2):331–341. doi:10.1016/j.immuni.2009.08.001
Lochner M, Peduto L, Cherrier M, Sawa S, Langa F, Varona R, Riethmacher D, Si-Tahar M, Di Santo JP, Eberl G (2008) In vivo equilibrium of proinflammatory IL-17 + and regulatory IL-10 + Foxp3 + RORgamma t + T cells. J Exp Med 205(6):1381–1393. doi:10.1084/jem.20080034
Lee YK, Mukasa R, Hatton RD, Weaver CT (2009) Developmental plasticity of Th17 and Treg cells. Curr Opin Immunol 21(3):274–280. doi:10.1016/j.coi.2009.05.021
Acknowledgements
We thank Basil Rapoport (University of California-Los Angeles) for providing us with the plasmid of pSV2neoECE-TSHR289-6H-dhfr. We also thank National Natural Science Foundation of China for its generous support (Grant No. 81373593) without which our work would not have been possible.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving animals were in accordance with the ethical standards of the institution or practice at which the studies were conducted.
Informed consent
No informed consent.
Rights and permissions
About this article
Cite this article
Yuan, Q., Zhao, Y., Zhu, X. et al. Low regulatory T cell and high IL-17 mRNA expression in a mouse Graves’ disease model. J Endocrinol Invest 40, 397–407 (2017). https://doi.org/10.1007/s40618-016-0575-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-016-0575-9