Abstract
Purpose
Feelings of shame and social comparison focused on physical appearance have been identified as important risk factors for the engagement in disordered eating behaviours. Further, recent studies have emphasized the role of body-image psychological (in)flexibility in the association between several risk factors and eating psychopathology. The current study intended to explore, in two different path models, the effects of external shame, physical appearance-related social comparison, and body image inflexibility on the explanation of eating psychopathology severity.
Methods
This study follows a cross-sectional design and was conducted in a sample of 776 emerging-adult women, aged between 18 and 28, who completed an online battery of self-report measures. Path analyses were conducted using a structural equation modeling.
Results
Model 1’s results showed that external shame and unfavourable social comparison based on physical appearance directly accounts for 26% of the variance in disordered eating. In turn, when body image inflexibility is introduced as a mediator in the relationship presented in Model 1, variance in disordered eating increases to 60% (Model 2). These results suggest that both external shame and unfavourable physical appearance-related social comparison have an impact on disordered eating behaviours. However, when body image inflexibility is introduced, the mentioned relationships change and reveal that psychological inflexibility is a significant mediator of these associations.
Conclusion
These findings seem to demonstrate that body image inflexibility is a key process for the engagement in disordered eating, so the promotion of psychological flexibility focused on one’s body is crucial for the prevention and treatment of disordered eating behaviours and attitudes.
Level of evidence
Level IV: Cross-sectional study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Literature has recently focused on a new life period that develops in between the adolescence and adulthood stages. Particularly in Western societies, authors have characterized this as a standalone developmental phase, entitled “emerging adulthood”, that occurs between the ages of 18 and 29 years old [1]. Though this life stage depends tremendously on culture [2], emerging adults in developed countries are characterized by a focus on identity searching and formation, having reached full physical and sexual maturity, but with diverse personal, educational, and professional trajectories [3].
Known as a period of a general rapid increase in weight gain [4], this has been studied as a particularly important stage for the development of Eating Disorders (EDs; [3, 5]), presenting high ED prevalence rates ([6]; 20.3%; [7]; 15.5% in women). Another study found that prevalence rates of ED during this period are significantly higher than in older adults [8]. More notoriously, a recent systematic review has concluded that emerging adulthood is an “underused concept” in the study of EDs, highlighting the need for literature to better explore the field of eating psychopathology during this stage [5]. In a world where technology and social media have taken over, social comparison and its consequences have been the center of attention [9,10,11,12,13].
Social comparison is conceptualized as a fundamental social process, where the individual uses information about the other to draw conclusions concerning the self [14]. Despite being a core process to all individuals, its consequences and impact differ for everyone. According to this, social comparison can be defined by two dimensions: (1) comparison of strength, power, and aggressiveness and (2) comparison of social attractiveness and talent [15].
There is also evidence showing that, even before social media, the notion of attractiveness was known to define one’s social rank. Thus, while the perception of a high social rank can lead to good self-esteem and positive outcomes, unfavourable social comparisons (e.g., the propensity to perceive the self as inferior, insufficient, and unwanted [16]) can lead to negative consequences, being associated with feelings and emotions such as shame, anxiety, depression symptomatology, and engagement in disordered eating attitudes and behaviours [17,18,19,20].
Today’s emerging adults are part of a generation that grew up with new technology and social media, and, therefore, have access to others as a source of comparison like never before, stressing the need to explore the impact of perceived social rank based on attractiveness and one’s body when compared to others, for this generation. Particularly in women, appearance and physical attractiveness have been shown to represent a focus for self-evaluation and social comparison [16, 21,22,23]. Women tend to use the body—body shape and body weight—as a source of comparison with others [24], since body image has been associated not only with health, but also with personal attributes and, particularly, with shame experiences [25].
Shame is an emotion that exists solely from social comparison, either in the presence of a real or an imagined audience [26]. This self-conscious emotion is considered an aversive state accompanied by a feeling of being ridiculed, humiliated, devalued, rejected, and exposed, leading to a range of behaviours such as anger, eye contact avoidance, desire to hide or flee, blushing, and submission mannerisms [27, 28]. According to the evolutionary biopsychosocial model [28], this socially focused emotion may be categorized into two different dimensions (external and internal shame) that are particularly related to each other. Specifically, external shame arises from the perception of negative evaluations and judgements about the self in the mind of others [28]. There is a growing research on the association between shame and mental health difficulties, in particular with disordered eating symptomatology [29,30,31]. Furthermore, evidence has supported that woman tend to report higher levels of shame proneness [32, 33]. Thus, disordered eating attitudes and behaviours (e.g., pathological dieting, the use of diet pills, laxatives or diuretics, excessive exercise, and purging) may emerge as maladaptive weight control strategies to attempt to change what is considered as the source of shame—one’s body image [21].
Therefore, the first aim of the present study was to explore, in a sample of emerging-adult women, the role of feelings of external shame and unfavourable social comparison based on physical appearance on eating psychopathology severity (Model 1). We hypothesized that women who present higher levels of general feelings of external shame and report more unfavourable physical appearance-related social comparison tend to adopt more disordered eating attitudes and behaviours. Thus, disordered eating may be conceptualized as a maladaptive strategy aimed to correct what is perceived as the cause of these feelings of inferiority, and, therefore, attain a valued physical appearance (which is commonly associated with success, happiness, and a high social rank [21, 25]). However, the feelings of external shame and unfavourable social comparison based on physical appearance are considered common human experiences, which suggest that there are other processes or mechanisms involved in this relationship.
Psychological (in)flexibility is considered a central concept in Acceptance and Commitment Therapy (ACT) and refers to one's (in)capacity to accept thoughts, memories, feelings, emotions, and other inner experiences, along with the (in)ability to adapt and persist in more effective and adaptive actions committed with one’s goals and values [34]. Specifically, recent literature has explored the role that psychological (in)flexibility has on the field of eating psychopathology [35, 36]. One of the variables explored before is body image-related psychological inflexibility (i.e., body image inflexibility; [37]). Specifically, this maladaptive strategy reflects the inability to fully and openly accept difficult private experiences (e.g., emotions, thoughts, feelings, and memories) about one's body, associated with the incapacity to engage in behaviours consistent with important life values [34, 38]. According to this perspective, several studies have demonstrated the effect of body image (in)flexibility in the association between several risk factors and eating psychopathology [37,38,39,40,41,42,43]. Indeed, body image inflexibility has been recognized as a noteworthy predictor of disordered eating, suggesting that individuals with high levels of body dissatisfaction and low body image flexibility tend to overestimate the importance of being thin and tend to engage in more disordered eating attitudes and behaviours [41]. On the other hand, the ability to accept these difficult private events related to body image is associated, among others, with a lower tendency to engage in pathological dieting [37], with fewer binge eating symptoms [44], and with more adaptive emotion strategies [45].
Thus, body image inflexibility emerges as a possible process that is involved in the relationship between general feelings of external shame, unfavourable social comparison through physical appearance, and disordered eating behaviours (Model 2). We hypothesized that when body image inflexibility is introduced to Model 1, it will better explain the mentioned relationship.
Methods
Participants
The sample included 776 emerging-adult women, aged between 18 and 28 (M = 20.6, SD = 2.1), with a mean of 13.1 (SD = 1.6) years of education. Four hundred and sixty-three (60%) lived in an urban and 312 (40%) in a rural zone. The participants’ mean body mass index (BMI) was 21.9 (SD = 3.1), which corresponds to normal weight values [46].
Procedures
This cross-sectional study was developed in the context of a wider Portuguese research project investigating the impact of different emotion regulation processes on mental health and disordered eating attitudes and behaviours. The sample was collected on an online platform between October 2019 and February 2020. All ethical and deontological requirements inherent to scientific research were respected. Participants were electronically recruited through online advertisement, using social networks, and were also asked to share the study with two or more female friends aged between 18 and 30 (Snowball Sampling method). Before staring the survey, participants signed an informed consent and were fully informed about the aims and procedures of the study, the voluntary nature of their cooperation, and the confidentiality of the data collection, which was only used for research purposes. The interested participants accessed an Internet link to a secure online platform (via LimeSurvey) on which they filled a short sociodemographic questionnaire and the self-report instruments described below (approximately 15 min). Participants did not receive any incentive or compensation for their participation.
Measures
Body mass index (BMI)
Participants’ BMI was estimated by dividing self-reported weight (in kg) by height squared (in m).
The other as Shamer scale-2 (OAS-2)
The OAS-2 [47] is an 8-item self-report scale that assesses external shame (i.e., negative perceptions about how others evaluate and judge the self). Participants are asked to rate on a five-point scale (0 = “Never” to 4 = “Almost Always”) the frequency of their feelings and experiences. Higher scores on this measure reveal high external shame. This scale has demonstrated good internal consistencies both in the original (α = 0.82; [47]) and in the current study (α = 0.92).
Social comparison through physical appearance scale (SCPAS)
The SCPAS [21] assesses social comparisons based on physical appearance. The participants are asked to compare themselves with Peers (Part 1) and with Models/Other Celebrities (Part 2). Lower scores indicate more unfavourable social comparison based on psychical appearance. The scale revealed high internal consistency in its original study for both parts [21]. For the current study, we only considered the comparisons with Peers (Part 1), and scores were reversed to obtain a measure of unfavourable social comparison. In the present study, Cronbach's alpha was 0.91.
Body image-acceptance and action questionnaire (BI-AAQ)
The BI-AAQ [37] includes 12 items and assesses body image (in)flexibility. Items are scored on a seven-point Likert scale (1 = “Never True” to 7 = “Always True”), with higher scores representing higher levels of psychological inflexibility concerning body image. The BI-AAQ showed very good psychometric characteristics in its Portuguese validation studies (α = 0.95; [37]). In the current study, Cronbach's alpha was 0.94.
Eating disorder examination questionnaire (EDE-Q)
The EDE-Q [48] was used to assess disordered eating attitudes and behaviours. This self-report measure includes 36 items, providing a total score (representing eating psychopathology severity) and four subscales: Restraint, Eating Concern, Weight Concern, and Shape Concern. This measure presented good psychometric properties, both in the original [49] and in its Portuguese version [48]. For the current study, the Cronbach alpha was 0.94.
Data analysis
Descriptive and Pearson correlation analyses were performed, using the Statistical Package for the Social Science (SPSS version22.0; IBM SPSS, Chicago, IL), to examine the sample means and standard deviations and the correlations between study variables [50]. Path analysis, a particular type of Structural Equation Modelling, was conducted to estimate the associations between the study variables hypothesized in the model. It allows for the simultaneous examination of direct and indirect effects considering multiple mediators while controlling for error [51]. All analyses were performed with the Analysis of Moment Structures software (AMOS, version22.0; IBM® SPSS® Amos™ 22 [52]) using the Maximum Likelihood as estimation method. The criteria proposed for good model fit indicators were: a non-significant chi-squared (χ2; p > 0.50); a Tucker–Lewis’s Index (TLI) ≥ 0.95; a Comparative Fit Index (CFI) ≥ 0.95; and a Root Mean Square Error of Approximation (RMSEA) ≤ 0.05 [51]. The significance of the direct, indirect, and total effects was examined by chi-squared tests. To test the significance of the mediational model, the Bootstrap resampling procedure (with 5000 Bootstrap samples and 95% bias‐corrected confidence intervals around the standardized estimates of total, direct, and indirect effects) was conducted. Significant effects (p < 0.050) were found when zero was not included in the interval between the lower and upper limits of the 95% bias-corrected confidence interval [51].
Results
Preliminary analyses
The analysis of these coefficients revealed that Skewness (Sk) values ranging from 0.08 (SCPAS_peers) and 1.70 (BMI), and Kurtosis (Ku) values ranging from 0.18 (BI-AAQ) and 7.56 (BMI). These results indicated that there was no severe violation of the normal distribution of the data (Sk <|3| and Ku <|8–10| [51]).
Descriptive and correlational analyses
Descriptive statistics (means and standard deviations) and correlations between the study’s variables are reported in Table 1. Results from correlation analysis revealed positive correlations between BMI and unfavourable social comparison through physical appearance, body image psychological inflexibility, and eating psychopathology severity, with week and moderate magnitudes. No significant correlations were found between BMI and external shame. In turn, external shame correlated moderate and positively with unfavourable social comparison through physical appearance, body image inflexibility, and eating psychopathology severity. Unfavourable social comparison through physical appearance correlated moderately and positively with body image inflexibility and eating psychopathology severity. Concluding, a correlation between body image inflexibility and eating psychopathology severity was significant, positive, and strong.
Path analysis
Path Model 1: This model was examined through a fully saturated model (i.e., with zero degrees of freedom), consisting of 14 parameters. All path coefficients were statistically significant at the level of p < 0.001. Results indicated that the model accounted for 26% of the variance of eating psychopathology severity.
Findings showed that both external shame and unfavourable social comparison through physical appearance had direct effects of 0.27 (bOAS = 0.06; SEb = 0.01; Z = 8.14; p < 0.001) and of 0.18 (bSCPAS_peers = 0.01; SEb = 0.00; Z = 5.25; p < 0.001) on eating psychopathology severity, respectively (Fig. 1).
Path Model 2: The initial model comprised 20 parameters, and indicated that one path was not significant: the path from external shame to eating psychopathology severity (bOAS = −0.01; SEb = 0.01; Z = 1.88; p = 0.061). This path was removed and the model was readjusted.
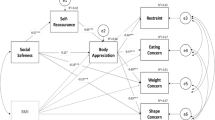
The recalculated model is presented in Fig. 2 and accounted for 25% of the variance of body image inflexibility, and 60% of the variance of eating psychopathology severity. Model fit indices were tested and provided evidence for an excellent fit to empirical data: [CMIN/df = 3.51; TLI = 0.98; CFI = 1.00; RMSEA = 0.06, p = 0.316, 95% CI = 0.00–0.13].
Path Model 2. The link between feelings of external shame and unfavourable social comparison through physical appearance on eating psychopathology severity mediated by body image inflexibility. Final path model. Standardized path coefficients among variables are presented. *p < 0.050; **p < 0.010; ***p < 0.001
External shame presented a direct effect of 0.33 (bOAS = −0.91; SE = 0.09; Z = 9.85; p < 0.001) on body image inflexibility. Also, unfavourable social comparisons through physical appearance presented a direct effect of 0.08 (bSCPAS_peers = 0.01; SE = 0.00; Z = 3.33; p < 0.001) on eating psychopathology severity and of 0.16 (bSCPAS_peers = 0.17; SE = 0.04; Z = 4.76; p < 0.001) on body image inflexibility, which in turn directly predicted eating psychopathology severity with an effect of 0.69 (bBI-AAQ = 0.05; SE = 0.00; Z = 27.79; p < 0.001).
Concerning indirect effects, external shame presented an indirect effect of 0.23 (95% CI [0.17, 0.28]; p < 0.001) on eating psychopathology severity, which was mediated by body image inflexibility. Furthermore, results revealed that unfavourable social comparisons through physical appearance presented an indirect effect on eating psychopathology severity (β = 0.11), which was partially mediated by body image inflexibility (95% CI [0.06, 0.16]; p < 0.001).
Discussion
According to the literature, feelings of shame and social comparison based on physical appearance are considered important risk factors for the engagement disordered eating attitudes and behaviours [19, 31, 53]. Further, recent studies have highlighted the role of body-image psychological (in)flexibility in the relationship between several risk factors and eating psychopathology [37, 39,40,41,42,43, 54]. Thus, the current study intended to explore, in two different path models (Model 1 and 2), the effects of external shame, social comparison based on physical appearance, and body image inflexibility on disordered eating behaviours, in a sample of emerging-adult women.
In Model 1, a mediational analysis was conducted to understand the associations between external shame and unfavourable social comparison through physical appearance on eating psychopathology severity. The results obtained with this model were aligned with our hypotheses demonstrating that, indeed, emerging-adult women who present higher levels of general feelings of shame, as well as more unfavourable social comparison related to physical appearance tend to report more disordered eating attitudes and behaviours. This suggests that when young women consider that others see and judge them as inferior or inadequate, as well as engage in unfavourable social comparison with others (focused on one's body and appearance), they will more likely adopt maladaptive behaviours related to eating psychopathology. Results from path analyses showed that external shame and unfavourable comparison based on physical appearance directly accounted for 26% of eating psychopathology severity’s variance. These findings arise per previous literature, which has explored the effect of external shame [29,30,31] and social comparison based on physical appearance [19, 53] on disordered eating.
Though the previously mentioned results are not considered completely new, few studies have included a sample of young adults. Moreover, it allows us to conclude that other processes might be involved in the association between feelings of external shame and unfavourable social comparison based on physical appearance and eating psychopathology severity. Following this, Model 2 emerged as a way to explore the possible role of body image inflexibility in the previously mentioned relationship. We hypothesized that when body image inflexibility is introduced to Model 1, eating psychopathology severity’s variance will increase. In fact, not only did body image inflexibility mediate this relationship, but it also significantly impacted disordered eating behaviours’ variance, increasing it to 60%. These findings, when considered along with Model 1, suggest that both external shame and unfavourable social comparison based on physical appearance have an impact on disordered eating behaviors. However, when body image inflexibility is introduced, the mentioned relationships change: (a) the relationship between external shame and eating psychopathology severity becomes completely mediated by body image inflexibility and (b) the association between unfavourable social comparison based on physical appearance and eating psychopathology severity becomes partially mediated by the same process. The path analysis findings corroborated prior research regarding the association between maladaptive emotion strategies (i.e., body-image psychological inflexibility) and increased eating psychopathology symptoms [37, 39,40,41,42,43, 54] and extend them to a sample of emerging-adult women.
These findings highlight the powerful effect that body-image psychological inflexibility (meaning the inability to: (a) accept unwanted memories, thoughts, emotions, or sensations related to body image as contextual, and to (b) adopt congruent actions with one’s life values) has on the field of eating psychopathology. Additionally, this study places emerging-adult women at the center of the discussion, which is a clear focal point, as previous research has shown this specific life stage to be vulnerable to mental health issues, including disordered eating symptomatology [1, 5]. Concluding, this study suggests that the relationship between external shame and unfavourable social comparison through physical appearance with eating psychopathology severity depends both on the ability to accept unwanted body image-focused experiences as contextual and transient and the ability to adopt behaviours and actions congruent with one’s life values, even in the presence of such unwanted body image-focused experiences.
Some limitations need to be considered. First, the cross-sectional design prevents the establishment of causal relationships between the examined variables, suggesting the need for and/or experimental designs. Also, the selection of a sample composed solely of women prevents the generalization of the results to other genders. Third, the sample included only Portuguese women, which compromises the generalization of the results to other nationalities. Cross-cultural investigations with multi-group analyses should be explored. Moreover, the exclusive use of self-report measures may be susceptible to biases (e.g., social desirability). To support our findings, it would be important to include other assessment methodologies (e.g., structured interviews). Finally, it is possible that other processes or mechanisms (such as automatic pilot and cognitive fusion) are involved in this relationship and were not accounted for in Models 1 and 2.
Nowadays, more than ever, with the rise of social media and its presence in everyday life, women are constantly faced with images of others, and social comparison is inevitable. The problem is that, more often than not, this comparison is unfavourable or problematic. Today’s emerging adults are the first generation that was brought up in this social media era, so research centred on its impact is essential. Though it is impossible to stop external shame or social comparison, as they are universal processes and feelings, it is of the utmost importance to develop clinical guidelines and interventions that target these risk factors. In this sense, ACT emerges as promising prevention and intervention for this goal, with its core principle being to promote more adaptive emotional mechanisms, such as psychological flexibility [34]. In that line, the present study shows that body image inflexibility is a key process for the engagement in disordered eating behaviours, so the promotion of body image flexibility seems to be crucial for the prevention and treatment of disordered eating behaviours and attitudes.
What is already known on this subject?
Today’s emerging adults are the first generation that was brought up around social media. Its effects on this generation are still being investigated. At the same time, shame and unfavourable social comparison have been studied as undesirable experiences that are associated with the adoption of more maladaptive eating behaviours. However, the processes involved in this relationship remain underexplored in a sample of emerging adults.
What does this study add?
This study shows that in a sample of emerging adults, body image inflexibility emerges as a key mediating process for eating psychopathology severity, when in the presence of shame and unfavourable social comparison experiences. This underlines the importance of promoting body image flexibility for the prevention and treatment of disordered eating behaviours and attitudes in emerging adults, meaning that ACT, where psychological flexibility represents a core principle, should be highlighted as a promising intervention.
References
Arnett JJ (2014) Emerging adulthood: The winding road from the late teens through the twenties. Oxford University Press, Oxford
Nelson LJ, Badger S, Wu B (2004) The influence of culture in emerging adulthood: perspectives of Chinese college students. Int J Behav Dev 28(1):26–36. https://doi.org/10.1080/01650250344000244
Arnett JJ, Žukauskienė R, Sugimura K (2014) The new life stage of emerging adulthood at ages 18–29 years: implications for mental health. Lancet Psychiatry 1(7):569–576. https://doi.org/10.1016/S2215-0366(14)00080-7
Ng M, Fleming T, Robinson M, Thomson B, Graetz N, Margono C, Abera SF (2014) Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet 384(9945):766–781. https://doi.org/10.1016/S0140-6736(14)60460-8
Potterton R, Richards K, Allen K, Schmidt U (2020) Eating disorders during emerging adulthood: a systematic scoping review. Front Psychol 10:3062. https://doi.org/10.3389/fpsyg.2019.03062
Hasselle AJ, Howell KH, Dormois M, Miller-Graff LE (2017) The influence of childhood polyvictimization on disordered eating symptoms in emerging adulthood. Child Abuse Negl 68:55–64. https://doi.org/10.1016/j.chiabu.2017.04.003
Gonidakis F, Lemonoudi M, Charila D, Varsou E (2018) A study on the interplay between emerging adulthood and eating disorder symptomatology in young adults. Eat Weight Disord 23(6):797–805. https://doi.org/10.1007/s40519-018-0552-8
Preti A, de Girolamo G, Vilagut G, Alonso J, de Graaf R, Bruffaerts R, ESEMeD-WMH Investigators (2009) The epidemiology of eating disorders in six European countries: results of the ESEMeD-WMH project. J Psychiatr Res 43(14):1125–1132. https://doi.org/10.1016/j.jpsychires.2009.04.003
Warrender D (2020) How use of social media and social comparison affect mental health. Nurs Times 116(3):58–61
Verduyn P, Gugushvili N, Massar K, Täht K, Kross E (2020) Social comparison on social networking sites. Curr Opin Psychol. https://doi.org/10.1016/j.copsyc.2020.04.002
Nesi J, Prinstein MJ (2015) Using social media for social comparison and feedback-seeking: gender and popularity moderate associations with depressive symptoms. J Abnorm Child Psychol 43(8):1427–1438. https://doi.org/10.1007/s10802-015-0020-0
Jiang S, Ngien A (2020) The effects of instagram use, social comparison, and self-esteem on social anxiety: a survey study in Singapore. Social Media Soc 6(2):205630512091248. https://doi.org/10.1177/2056305120912488
Vogel EA, Rose JP, Roberts LR, Eckles K (2014) Social comparison, social media, and self-esteem. Psychol Pop Media Cult 3(4):206–222. https://doi.org/10.1037/ppm0000047
Festinger L (1954) A theory of social comparison processes. Hum Relat 7:117–140. https://doi.org/10.1177/001872675400700202
Allan S, Gilbert P (1995) A social comparison scale: psychometric properties and relationship to psychopathology. Pers Indiv Differ 19(3):293–299. https://doi.org/10.1016/0191-8869(95)00086-L
Troop NA, Allan S, Treasure JL, Katzman M (2003) Social comparison and submissive behaviour in eating disorder patients. Psychol Psychother 76(3):237–249. https://doi.org/10.1348/147608303322362479
Lim M, Yang Y (2015) Effects of users’ envy and shame on social comparison that occurs on social network services. Comput Human Behav 51:300–311. https://doi.org/10.1016/j.chb.2015.05.013
Mitchell MA, Schmidt NB (2014) An experimental manipulation of social comparison in social anxiety. Cogn Behav Ther 43(3):221–229. https://doi.org/10.1080/16506073.2014.914078
Hamel AE, Zaitsoff SL, Taylor A, Menna R, Grange DL (2012) Body-related social comparison and disordered eating among adolescent females with an eating disorder, depressive disorder, and healthy controls. Nutrients 4(9):1260–1272. https://doi.org/10.3390/nu4091260
Fitzsimmons-Craft EE (2017) Eating disorder-related social comparison in college women’s everyday lives. Int J Eat Disorders 50(8):893–905. https://doi.org/10.1002/eat.22725
Ferreira C, Pinto-Gouveia J, Duarte C (2013) Physical appearance as a measure of social ranking: the role of a new scale to understand the relationship between weight and dieting. Clin Psychol Psychother 20(1):55–66. https://doi.org/10.1002/cpp.769
Buote VM, Wilson AE, Strahan EJ, Gazzola SB, Papps F (2011) Setting the bar: divergent sociocultural norms for women’s and men’s ideal appearance in real-world contexts. Body Image 8(4):322–334. https://doi.org/10.1016/j.bodyim.2011.06.002
Homan KJ, Tylka TL (2015) Self-compassion moderates body comparison and appearance self-worth’s inverse relationships with body appreciation. Body Image 15:1–7. https://doi.org/10.1016/j.bodyim.2015.04.007
Trottier K, Polivy J, Herman CP (2007) Effects of exposure to thin and overweight peers: evidence of social comparison in restrained and unrestrained eaters. J Soc Clin Psychol 26(2):155–172. https://doi.org/10.1521/jscp.2007.26.2.155
Sypeck MF, Gray JJ, Etu SF, Ahrens AH, Mosimann JE, Wiseman CV (2006) Cultural representations of thinness in women, redux: playboy magazine’s depiction of beauty from 1979 to 1999. Body Image 3(3):229–235. https://doi.org/10.1016/j.bodyim.2006.07.001
Allan S, Gilbert P, Goss K (1994) An exploration of shame measures: II. Psychopathology. Personality Indiv Differ 17(5):719–722. https://doi.org/10.1016/0191-8869(94)90150-3
Gilbert P (2002) Body shame: A biopsychosocial conceptualization and overview, with treatment implications. In: Gilbert P, Miles J (eds) Body shame: conceptualisation, research and treatment. Brunner Routledge, New York, pp 3–54
Gilbert P (2007) The evolution of shame as a marker for relationship security. In: Tracy JL, Robins RW, Tangney JP (eds) The self-conscious emotions: theory and research. Guilford, New York, NY, pp 283–309
Gee A, Troop NA (2003) Shame, depressive symptoms and eating, weight and shape concerns in a non-clinical sample. Eat Weight Disord 8(1):72–75. https://doi.org/10.1007/bf03324992
Murray C, Waller G, Legg C (2000) Family dysfunction and bulimic psychopathology: the mediating role of shame. Int J Eat Disord 28(1):84–89. https://doi.org/10.1002/(sici)1098-108x(200007)28:1%3c84::aid-eat10%3e3.0.co;2-r
Troop NA, Allan S, Serpell L, Treasure JL (2008) Shame in women with a history of eating disorders. Eur Eat Disord Rev 16(6):480–488. https://doi.org/10.1002/erv.858
Benetti-McQuoid J, Bursik K (2005) Individual differences in experiences of and responses to guilt and shame: examining the lenses of gender and gender role. Sex Roles 53(1–2):133–142. https://doi.org/10.1007/s11199-005-4287-4
Galhardo A, Cunha M, Pinto-Gouveia J, Matos M (2013) The mediator role of emotion regulation processes on infertility-related stress. J Clini Psychol Med Settings 20(4):497–507. https://doi.org/10.1007/s10880-013-9370-3
Hayes SC, Luoma JB, Bond FW, Masuda A, Lillis J (2006) Acceptance and commitment therapy: model, process and outcomes. Behav Res Therapy 44:1–25. https://doi.org/10.1016/j.brat.2005.06.006
Rawal A, Park RJ, Williams JMG (2010) Rumination, experiential avoidance, and dysfunctional thinking in eating disorders. Behav Res Ther 48(9):851–859. https://doi.org/10.1016/j.brat.2010.05.009
Levin ME, MacLane C, Daflos S, Seeley JR, Hayes SC, Biglan A, Pistorello J (2014) Examining psychological inflexibility as a transdiagnostic process across psychological disorders. J Contextual Behav Sci 3(3):155–163. https://doi.org/10.1016/j.jcbs.2014.06.003
Ferreira C, Pinto-Gouveia J, Duarte C (2011) The validation of the body image acceptance and action questionnaire: exploring the moderator effect of acceptance on disordered eating. Rev Int Psicol Ter Psicol 11:327–345
Sandoz EK, Wilson KG, Merwin RM, Kellum KK (2013) Assessment of body image flexibility: the body image-acceptance and action questionnaire. J Contextual Behav Sci 2(1–2):39–48. https://doi.org/10.1016/j.jcbs.2013.03.002
Cardoso A, Oliveira S, Ferreira C (2020) Negative and positive affect and disordered eating: the adaptive role of intuitive eating and body image flexibility. Clin Psychol 24(2):176–185. https://doi.org/10.1111/cp.12224
Duarte C, Pinto-Gouveia J (2016) Body image flexibility mediates the effect of body image-related victimization experiences and shame on binge eating and weight. Eat Behav 23:13–18
Hill ML, Masuda A, Latzman RD (2013) Body image flexibility as a protective factor against disordered eating behavior for women with lower body mass index. Eat Behav 14(3):336–341. https://doi.org/10.1016/j.eatbeh.2013.06.003
Morton C, Mooney TA, Lozano LL, Adams EA, Makriyianis HM, Liss M (2020) Psychological inflexibility moderates the relationship between thin-ideal internalization and disordered eating. Eat Behav 36:101345. https://doi.org/10.1016/j.eatbeh.2019.101345
Wendell JW, Masuda A, Le JK (2012) The role of body image flexibility in the relationship between disordered eating cognitions and disordered eating symptoms among non-clinical college students. Eat Behav 13(3):240–245. https://doi.org/10.1016/j.eatbeh.2012.03.006
Duarte C, Pinto-Gouveia J, Ferreira C (2014) Escaping from body image shame and harsh self-criticism: exploration of underlying mechanisms of binge eating. Eat Behav 15(4):638–643. https://doi.org/10.1016/j.eatbeh.2014.08.025
Kelly AC, Vimalakanthan K, Miller KE (2014) Self-compassion moderates the relationship between body mass index and both eating disorder pathology and body image flexibility. Body Image 11(4):446–453. https://doi.org/10.1016/j.bodyim.2014.07.005
WHO (1995) Physical status: the use and interpretation of anthropometry. Reports of a 5 WHO Expert Committee. WHO technical report series 854. World Health Organization, Geneva
Matos M, Pinto-Gouveia J, Gilbert P, Duarte C, Figueiredo C (2015) The other as Shamer Scale-2: development and validation of a short version of a measure of external shame. Pers Individ Differ 74:6–11. https://doi.org/10.1016/j.paid.2014.09.037
Machado PP, Martins C, Vaz AR, Conceição E, Bastos AP, Gonçalves S (2014) Eating disorder examination questionnaire: psychometric properties and norms for the Portuguese population. Eur Eat Disord Rev 22(6):448–453
Fairburn C, Beglin S (1994) Assessment of eating disorders: interview or self-report questionnaire? Int J Eat Disord 16(4):363–370. https://doi.org/10.1002/1098-108X(199412)16:4%3c363::AID-EAT2260160405%3e3.0.CO;2-#
Cohen J, Cohen P, West SG, Aiken LS (2003) Applied multiple regression/correlation analysis for the behavioral sciences, 3rd edn. Lawrence Erlbaum Associates Publishers, New Jersey
Kline RB (2011) Principles and practice of structural equation modelling, 3rd edn. Guilford Press, New York
Arbuckle JL (2013) Amos (Version 22.0) [Computer Program]. SPSS
Fitzsimmons-Craft EE (2017) Eating disorder-related social comparison in college women’s everyday lives. Int J Eat Disord 50(8):893–905. https://doi.org/10.1002/eat.22725
Sandoz EK, Wilson KG, Merwin RM, Kellum KK (2013) Assessment of body image acceptance: the body image-acceptance questionnaire. J Context Behav Sci 2(1–2):39–48. https://doi.org/10.1016/j.jcbs.2013.03.002
Funding
Research by Ana Laura Mendes is supported by a Ph.D. Grant (SFRH/BD/119286/2016) sponsored by the Portuguese Foundation for Science and Technology (FCT), the Human Capital Operational Programme (POCH), and the European Union (UE).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures followed were under the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975, as revised in 2000.
Informed consent
Informed consent was obtained from all participants for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mendes, A.L., Coimbra, M., Canavarro, M.C. et al. The powerful effect of body image inflexibility on the explanation of eating psychopathology severity. Eat Weight Disord 27, 961–968 (2022). https://doi.org/10.1007/s40519-021-01233-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-021-01233-1