Abstract
Purpose
General and eating disorder (ED)-specific ruminations have been identified as key factors that may contribute to eating pathology. Positive beliefs about rumination (e.g., “Ruminating helps me to prevent future mistakes") may impact this association. However, the effect of positive beliefs about rumination on the links between rumination and ED symptom severity has not been investigated. This study sought to clarify relations between rumination and ED symptom severity and to evaluate the potential moderating effect of positive beliefs about rumination on these associations.
Methods
During a laboratory visit, undergraduate participants (N = 473, MAge = 18.90 ± 2.27, MBMI = 23.45 kg/m2 ± 4.31, 54.8% female) completed an online battery of questionnaires assessing general and ED-specific ruminative processes (e.g., brooding, reflection), positive beliefs about rumination, and global ED symptoms. Hierarchical multiple regression analyses assessed the unique contributions of specific ruminative processes, and the moderating effect of positive beliefs on associations between ruminative processes and ED symptom severity.
Results
Hierarchical multiple regression results suggest that, after controlling for gender and BMI, ED-specific brooding, b = 1.32, SE = 0.13, β = 0.46, p < 0.0001, and reflection, b = 1.44, SE = 0.33, β = 0.19, p < 0.0001, accounted for unique variance in ED symptom severity. Moderation model results indicate that, at low levels of general reflection, b = − 0.06, SE = 0.02, β = − 0.51, p = 0.003, and ED-specific reflection, b = − 0.15, SE = 0.03, β = − 0.59, p < 0.0001, increased positive beliefs about rumination were associated with greater ED symptom severity.
Conclusion
Findings suggest ED-specific rumination accounts for ED symptom severity above and beyond general rumination, and that rumination-related expectancies influence the association between reflection and ED symptom severity.
Level of evidence
Level III, evidence obtained from a well-designed cohort study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rumination is a type of repetitive thinking that focuses on the past and often involves self-blame or criticism. This process has been implicated in numerous psychological disorders [1, 2]. Prior literature has demonstrated a positive association between rumination and eating disorder (ED) symptom severity: individuals with EDs report greater rumination following stressful life events than healthy controls [3], and increased rumination predicts greater bulimic symptom severity in female adolescents and adults with EDs [4, 5]. Ruminative thought has been associated with increased ED symptoms, including restraint, eating concerns, weight concerns, and shape concerns, in both anorexia nervosa and bulimia nervosa [5]. Additionally, recent findings suggest that rumination may interfere with corrective learning processes critical to the success of behavioral ED treatments [6].
Rumination is an overarching construct that consists of two discrete components—reflection and brooding. Reflection (i.e., contemplative, intentional pondering with a focus on problem-solving) and brooding (i.e., self-thought with an anxious or gloomy focus) exhibit distinct relationships with internalizing psychopathology [7]. However, each ruminative process appears to differentially relate to symptom severity. For example, unlike reflection, which is often conceptualized as an adaptive ruminative process, brooding is associated with greater symptom severity in mood and anxiety-related disorders [7,8,9]. To date, limited research has examined the unique associations between each process and EDs. Therefore, additional research is needed to examine the extent to which brooding and reflection may differentially relate to ED symptom severity.
Rumination about content or behaviors related to a psychological disorder, or disorder-specific rumination, has emerged as a potentially important process in EDs. Recent meta-analytic evidence indicates that larger associations between rumination and ED psychopathology were observed in studies employing ED-specific measures of rumination [10]. For instance, one prior experimental study demonstrated that when encouraged to ruminate about ED-specific content (e.g., images of thin models), adults with EDs reported increased ED symptom severity [11]. Other research suggests that disorder-specific ruminative brooding uniquely contributes to ED severity [12]. Together, these preliminary findings suggest that both general and ED-specific ruminative processes are associated with ED symptom severity. However, additional investigation is still needed to establish the extent to which each ruminative process (e.g., general brooding, general reflection, ED-specific brooding, ED-specific reflection) relates to ED symptoms.
Beliefs about the effects of rumination may reinforce ruminative thinking in EDs. Positive expectations related to rumination (e.g., “Thinking about the causes of my problems will help me solve them”) are posited to maintain rumination in psychopathology due to the perceived functional importance of this cognitive process [13]. For example, greater positive beliefs about rumination are associated with greater rumination in depression-prone groups [14, 15]. Positive beliefs about rumination also appear to partially mediate the relationship between rumination and social anxiety symptoms in undergraduate students [16]. Together, these findings suggest that stronger beliefs about rumination may strengthen the relationship between ruminative processes and psychiatric symptom presentations. However, the role of positive beliefs has not yet been investigated in relation to ED symptoms.
To address the aforementioned gaps in the literature on rumination and ED symptoms, the current study sought to clarify the relations between unique components of general and ED-specific rumination (e.g., reflection and brooding), beliefs about rumination, and ED symptoms in a sample of college-aged individuals—a demographic group at increased risk for ED onset, as well as rumination and its associated negative effects [17]. To date, few studies have examined the association between disorder-specific rumination and ED symptoms in higher-risk populations, such as college-aged individuals, rather than clinical samples [18]. However, given the increased risk for ED pathology in this age group, we expected to observe similar associations between constructs of interest as might be hypothesized based on work conducted in clinical samples. Specifically, we investigated three hypotheses: (1) brooding would be more strongly associated with ED symptoms than reflection; (2) ED-specific brooding would account for unique variance in ED symptom severity beyond that of general brooding; and (3) positive beliefs about rumination would moderate the relations between all forms of rumination and ED symptoms, such that these associations would be stronger in individuals with greater positive beliefs about rumination. Understanding the unique associations between ED-specific and general ruminative processes (e.g., brooding, reflection) and ED symptoms may inform future efforts to increase specificity in ED treatment and prevention approaches targeting rumination processes in young adults.
Methods
Participants and procedures
Participants were 473 adult men and women (54.8% women, n = 259). Participants were required to be 18 years or older and a current undergraduate student enrolled in psychology courses at a large northeastern university. Participants were recruited using online postings through the university’s research pool. Online postings recruited participants for a research study investigating the relations between cognitive style and various eating and weight-related behaviors and attitudes. Participants attended one in-laboratory visit as a part of a larger study [19], of which this is a secondary analysis. During this visit, participants completed informed consent and an online battery of self-report questionnaires via SurveyMonkey.com. Measures used in the current study were completed as part of a larger battery of online questionnaires, which included self-report questionnaires assessing cognitive rumination patterns and beliefs about rumination, as well as additional self-report questionnaires that assessed other clinical and personality characteristics (e.g., affective impulsivity, emotion regulation, perfectionism); assessments used in the current study are listed in the “Measures” subsection, below. All participants received course credit for their participation. All study procedures were approved by the university’s Institutional Review Board and were conducted in accordance with the Declaration of Helsinki.
Measures
Rumination response scale (RRS) [7]
The RRS is a self-report scale used to assess ruminative processes—brooding and reflection [7]. Participants report the frequency of each event on a 4-point Likert-type scale, ranging from 1 (“almost never”) to 4 (“almost always”), with higher scores indicating greater ruminative thought. The RRS consists of three subscales, Brooding (e.g., “How often do you think, ‘why can’t I handle things better?’”), Reflection (e.g., “How often do you write down what you are thinking and analyze it”), and Depression-related, designed to assess unique ruminative processes. Brooding and Reflection subscale items were used in the current study. Subscales demonstrated good internal reliability within the current sample (Brooding α = 0.86; Reflection α = 0.82).
Rumination Response Scale for Eating Disorders (RRS-ED) [20]
The RRS-ED is a self-report questionnaire adapted from the RRS to capture ED-specific rumination; unlike the RRS, this measure consists of only Reflection and Brooding subscales [20]. Responses are assessed using a 4-point Likert-type scale (“almost never” to “almost always”). Items capture ED-specific ruminative thoughts (e.g., “How often do you write down what you think about your eating, weight, and/or shape and analyze it?”). Higher scores indicate greater ED-specific ruminative thought. In this study, the ED-specific Brooding and Reflection subscales were used to assess each disorder-specific ruminative process. Cronbach’s alphas for ED-specific Brooding and ED-specific Reflection were α = 0.91 and 0.80, respectively.
Positive beliefs about rumination scale (PBRS) [14]
The PBRS is a self-report 4-point Likert scale assessing the degree (“1—do not agree” to “4—agree very much”) to which individuals believe ruminative thought is beneficial (e.g., “I need to ruminate about the bad things that have happened in the past to make sense of them”) [14]. Higher scores indicate stronger belief in the benefits of rumination. PBRS sum scores were used to assess positive expectancies about rumination, which was examined as a potential moderator of the association between rumination constructs and ED symptom severity. In this sample, PBRS demonstrated excellent internal consistency (α = 0.94).
Eating disorder diagnostic scale (EDDS) [21]
The EDDS is a self-report questionnaire that provides behavioral frequency counts for specific ED symptoms (e.g., objective binge-eating episodes, self-induced vomiting, diuretics/laxative use, excessive exercise). The EDDS also provides a measure of global ED symptom severity (e.g., Symptom Composite score), which is computed based on the sum of EDDS items that assess various behavioral and cognitive ED symptoms through a combination of Likert-type scales, frequency scores, and dichotomous scores [21]. Higher EDDS Symptom Composite scores represent greater ED symptom severity. EDDS Symptom Composite scores were used to assess overall ED symptom severity (α = 0.82).
Demographics
Participants completed a self-report demographics questionnaire that assessed self-reported gender identity, racial/ethnic identity, current weight (in pounds) and current height (in inches). Participant self-reported height and weight values were used to compute self-reported body mass index (BMI; kg/m2). Demographic variables were examined as potential covariates in the current study.
Analytic approach
Preliminary analyses
Covariates of interest (age, gender, and BMI) were examined prior to conducting primary analyses. Pearson-product bivariate correlations were conducted to examine associations between variables of interest. Bivariate correlation analyses indicated that age was not significantly associated with EDDS Symptom Composite scores (p > 0.05); therefore, gender and BMI were included in the final models as covariates of interest. Prior to conducting primary analyses of interest, preliminary assumption testing was conducted to ensure no serious violations of OLS assumptions among variables (e.g., homoscedasticity, normality, multicollinearity). Tolerance (1-R2) and variance inflation factor (VIF) data were examined to assess for potential multicollinearity among independent variables. Following recommendations when assessing for multicollinearity [22], problematic multicollinearity was defined as cases where tolerance was less than 0.2 and the corresponding VIF value was 10 or greater.
Primary analyses
The current investigation used hierarchical multiple regression analyses to examine the degree to which general and ED-specific rumination processes accounted for unique variance in EDDS Symptom Composite scores (hypotheses 1 and 2). In the three-step hierarchical multiple regression model, covariates were entered in the first step, general brooding and reflection variables were entered in the second step, and ED-specific brooding and reflection variables were entered in the third step. Predictor variables of interest were mean-centered prior to being added to regression models.
Four separate moderation analyses were conducted using PROCESS [23] for SPSS to evaluate our third hypothesis, examining the extent to which positive beliefs about rumination influence the association between ruminative processes and ED symptoms. One model was constructed per interaction term (e.g., Positive Beliefs x Reflection; Positive Beliefs x Brooding; Positive Beliefs x ED-specific Reflection; Positive Beliefs x ED-specific Brooding) to examine the extent to which positive beliefs about rumination impacted the association between ruminative processes and ED symptom severity. In each model, covariates and RRS variables were entered in Step 1, positive beliefs about rumination was entered in Step 2, and the interaction term for positive beliefs by ruminative process was entered in Step 3. Follow-up analyses using the Johnson–Neyman (J–N) technique were used to probe statistically significant interaction effects, to identify regions of significance, or the values of the moderator (e.g., Positive Beliefs about Rumination Scale) for which association between the level of ruminative response (e.g., RRS-ED Reflection) and eating disorder symptom severity (EDDS Symptom Composite) is statistically significant.
Data were assessed for missingness prior to primary analyses; we found low amounts of missing data in the study sample (0.8–6.1% missing data, per measure used), no patterns of missing data, and utilized listwise deletion in the current analyses. In total, we applied a familywise Bonferroni correction to each of the primary analyses of interest (hierarchical multiple regression and moderation models) in an effort to account for multiple comparisons (α = 0.05/6). The critical significance threshold for the current investigation was set at p < 0.008. All analyses were conducted using IBM SPSS Statistics, Version 27.
Results
Sample descriptives
The current sample included 473 adult participants (Mean Age = 18.90 years, SD = 2.27, range = 18–28). Slightly more than half of participants self-identified as women (54.8%, n = 259), and participants reported a mean BMI of 23.45 kg/m2 (SD = 4.31, range = 13.32–44.93) The sample was relatively diverse, with 47.1% identifying as Caucasian (n = 223), 21.8% Asian/Pacific Islander (n = 103), 12.1% Hispanic (n = 57), 18.0% Black (n = 85), and 0.8% American Indian or Alaskan Native (n = 4). The mean EDDS Symptom Composite score of participants was 18.47 (SD = 14.2); approximately 47% (n = 224) of participants met or exceeded the threshold (16.5) for clinically significant ED psychopathology [24]. Specific behavioral frequency data from the EDDS indicated that the majority of participants reported engaging in at least one objective binge episode at least once per week over the past 3 months (61.5%, n = 291), and a portion of participants endorsed self-induced vomiting (8.3%, n = 39); laxative/diuretic use (8.3%, n = 39); fasting (i.e., skipped at least two meals in a row) (24.1%, n = 114); or excessive exercise (33.2%, n = 157) at least once per week over the past 3 months.
Mean RRS subscale and PBRS scores are presented in Table 1. Bivariate Pearson-product correlations were statistically significant between all RRS subscales, PBRS scores, and EDDS Symptom Composite scores (all ps < 0.01; see Table 1). We found no evidence for problematic multicollinearity among predictor variables in the current study (Tolerance values: 0.38–0.83; VIF values: 1.2–2.6).
Hierarchical multiple regression
The overall hierarchical multiple regression model examining the unique contributions of general and ED-specific ruminative constructs to ED symptom severity was statistically significant, R = 0.78, Adjusted R2=0.61, ΔR2 = 0.22, p < 0.0001. Entered in Step 1, gender and BMI were statistically significant covariates (see Table 2 for full model output). In Step 2, Brooding accounted for significant unique variance in EDDS Symptom Composite scores, b = 1.52, SE(b) = 0.21, β = 0.40, p < 0.0001. Reflection did not account for significant unique variance in EDDS Symptom Composite scores (p > 0.008). When entered in Step 3, Brooding remained statistically significant, b = 0.86, SE(b) = 0.18, β = 0.23, p < 0.0001; ED-specific Brooding, b = 1.32, SE(b) = 0.13, β = 0.46, p < 0.0001, and ED-specific Reflection, b = 1.44, SE(b) = 0.33, β = 0.19, p < 0.0001, each accounted for unique variance in EDDS Symptom Composite scores after accounting for covariates and general rumination constructs.
Moderation analyses
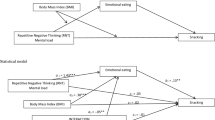
Full results for all four moderation models are presented in Table 3. Visually depicted in Fig. 1, two interaction effects were significant. Specifically, PBRS scores significantly moderated the relations between ED-specific Reflection and ED symptoms, b = − 0.15, SE(b) = 0.03, β = − 0.59, p < 0.0001, as well as the relationship between General Reflection and ED symptoms, b = − 0.06, SE(b) = 0.02, β = − 0.51, p = 0.003. Visual inspection of slopes revealed that the association between ED-specific reflection and ED symptom severity was stronger at lower positive beliefs about rumination (Fig. 1), suggesting that the association between ED-specific Reflection and ED symptom severity is stronger among individuals who endorse lower positive beliefs about rumination. When examined using the Johnson-Neyman approach, results indeed indicated that the association between ED-specific Reflection and ED symptoms was significant only when PBRS scores were equal to or lower than 30.08. Visual inspection of slopes also suggested that the association between general reflection and EDDS Symptom Composite scores was stronger at lower positive beliefs about rumination (Fig. 1). However, follow-up Johnson–Neyman analyses used to further probe the significant interaction effects revealed no regions of significance, indicating that the association between General Reflection and ED symptoms was significant across all values of the moderator (PBRS).
Moderation effects of positive beliefs on the associations between a general and b disorder-specific ruminative reflection and eating disorder symptoms. Note. Figure 1 depicts the association between eating disorder symptom severity and RRS or RRS-ED scores (a, b, respectively) by strength of positive beliefs about rumination. Interaction effects indicate the relation between ruminative reflection and eating disorder symptom severity is stronger when positive belief about rumination is lower. EDDS eating disorder diagnostic scale, positive beliefs positive beliefs about rumination scale, RRS ruminative response scale, RRS-ED rumination response scale for eating disorders, SD standard deviation, Graphics program SPSS v.27
PBRS scores did not significantly interact with ED-specific brooding to influence the relationship between general or ED-specific rumination processes and EDDS Symptom Composite scores (see Table 3).
Discussion
This study expands upon prior examinations of the links between rumination processes and eating pathology in a large sample of young adults. To our knowledge, this study also provides the first evaluation of the role of positive beliefs about rumination as a moderator of the associations between both general and ED-specific rumination and ED symptom severity. In this investigation, we found that general brooding demonstrated a significant positive relationship with ED symptoms, while general reflection did not. Moreover, the association between general brooding and EDDS Symptom Composite scores remained statistically significant within the final model after including ED-specific rumination constructs. This finding is consistent with our hypothesis and coincides with previous research that suggests that brooding, but not reflection, often exhibits a unique association with psychopathology [7,8,9]. The present findings suggest that general brooding may indeed play a particularly maladaptive role in eating pathology among young adults. General brooding may also represent a transdiagnostic mechanism accounting for the co-occurrence of EDs and other pathologies (e.g., mood and anxiety disorders); however, this hypothesis remains to be tested in future investigations.
In addition to general brooding, both ED-specific brooding and ED-specific reflection uniquely accounted for significant variance in EDDS Symptom Composite scores. These results are consistent with our hypothesis that ED-specific rumination would account for unique variance in ED symptoms, above general ruminative processes. These findings are consistent with prior research, which demonstrated that disorder-specific ruminative processes increase subsequent ED symptom severity in clinical populations [6]. However, the finding that both ED-specific reflection and brooding were significantly associated with ED symptoms only partially coincides with the previous correlational study that did not find significant associations between ED-specific reflection and eating pathology [12]. It is possible that distinctions between study designs contributed to differential findings. Our study examined a larger and more diverse sample of young adults than examined in prior work [12]; consequently, differences in statistical power or sample variance may explain divergent findings. Increased clarity regarding the relation between disorder-specific reflection and ED symptoms is warranted, given that reflection is commonly conceptualized as adaptive. However, our results suggest that both disorder-specific brooding and reflection may be maladaptive.
Partially consistent with our third hypothesis, findings from the moderation analyses indicate that positive beliefs about rumination significantly moderated the association between reflection, both general and ED-specific, and global ED symptom severity. Specifically, results suggest that the association between both general and ED-specific reflection and EDDS Symptom Composite scores is stronger among individuals who endorse lower positive beliefs about rumination. In addition, results from Johnson–Neyman follow-up analyses indicated that the association between ED-specific reflection and ED symptom severity was only statistically significant when individuals endorsed lower levels of positive beliefs about rumination (e.g., PBRS scores below 30.8). Considered alongside findings that suggest that general reflection and ED-specific reflection demonstrate significant positive main effects on EDDS Symptom Composite scores (e.g., higher levels of reflection are associated with greater ED symptom severity), these findings provide initial evidence that the associations between cognitive reflection and ED symptomatology are influenced by the degree to which an individual believes that ruminative processes are beneficial or may result in positive outcomes. Altogether, these findings suggest that reflection may not be an adaptive ruminative process and that positive beliefs about the benefits of rumination may need to be assessed to better understand the relationship between reflection and ED risk. It seems plausible that, if ruminative patterns—including reflection—are associated with maladaptive ED symptoms, an individual may not hold strong positive beliefs about the outcome or benefits of reflective cognitive processes. Future efforts to identify the point at which the association between reflection and ED symptoms is differentially impacted by positive expectancies may ultimately inform prevention modeling that incorporates rumination and rumination-related expectancies relevant to ED risk. In addition, research should continue to evaluate differences between general and ED-specific reflection associations with ED symptomology.
In contrast to our hypotheses, which posited that positive beliefs about rumination would moderate the associations between brooding and ED symptom severity, the moderation effects of positive beliefs about rumination in both general and ED-specific brooding models were not statistically significant. These results were unexpected, as they were not consistent with findings from other fields (e.g., depression, social anxiety) [7,8,9], which suggest that positive expectancies about rumination strengthen associations between rumination and psychopathology [14,15,16]. Although surprising, the lack of moderation effect of positive beliefs about rumination on the brooding-ED symptom severity association and the presence of moderation effect for reflection might be explained by several factors. For instance, brooding may not be frequently associated with beneficial outcomes (e.g., brooding may more frequently precede, co-occur with, or follow negative cognitions and events), thereby altering the influence of positive beliefs about rumination on the relationship between brooding and ED symptoms. Given that emerging evidence suggests that rumination operates at a momentary level to maintain and exacerbate subsequent ED symptomatology [25], it is possible that positive beliefs or expectancies interact with ruminative processes to influence ED symptomatology. However, because the current study assessed cross-sectional associations, limiting the ability to draw conclusions regarding the temporal associations between ruminative processes and ED symptom severity. Future efforts to clarify the temporal associations between ruminative processes and ED symptoms should utilize prospective, ecologically valid study designs for a more nuanced assessment of rumination processes in EDs.
Clinically, our findings challenge the assumption that planned reflection could serve as beneficial. Rumination-Focused Cognitive Behavioral Therapy (RFCBT) [26], which focuses on shifting unconstructive rumination (e.g., brooding processes) to focus on constructive thinking while decreasing avoidance, appears to lead to decreases in depression and relapse among adults with residual depression [26, 27]. RFCBT has been hypothesized to be beneficial in EDs given the relevance of brooding to eating pathology [10]. However, the finding that ED-specific reflection is associated with ED symptom severity and appears to be moderated by positive beliefs about rumination suggests that planned reflection may not necessarily prove beneficial.
Altogether, these results indicate that conceptualizing reflection and brooding as universally adaptive or maladaptive may be a vast oversimplification: it appears that the relationship between these variables and ED symptom severity could vary based on ruminative content or other moderating variables. For instance, the current findings suggest that it may be helpful to assess the content of ruminative thought patterns, given that ruminative thoughts specific to ED-related concerns (e.g., body shape, size, eating attitudes, or behaviors) appear closely associated with elevated ED symptom severity. In addition, evaluation of expectancies or beliefs about rumination may be useful for determining the extent to which an individual might demonstrate a stronger association between ruminative processes and ED symptoms. Such knowledge may also inform future research and current clinical efforts that aim to target ED-specific ruminative processes such as RFCBT [26]. However, because the current study utilized cross-sectional data in a non-clinical sample, research employing a prospective study design is needed to clarify the role of ruminative processes for individuals with EDs. In addition, although approximately 47% of participants met or exceeded the EDDS threshold for clinically significant ED psychopathology, a formal examination of the associations among rumination, positive beliefs about rumination, and eating pathology among clinical ED samples is warranted.
Limitations
Despite several strengths of the current study (e.g., large, relatively diverse sample), there are several notable limitations. Rumination-related constructs were reflected by self-report measures that assessed global, trait-level rumination constructs; therefore, our assessments are not reflective of the momentary nature of cognitive ruminative processes. Additionally, the PBRS broadly assesses positive beliefs about rumination. Therefore, it is possible that the current study did not explicitly assess whether positive beliefs endorsed were ED-specific (e.g., positive beliefs about engaging in ED-specific rumination processes, but not general rumination processes). Because conclusions based on our moderation results may not capture ED specificity, future research should aim to investigate the role of positive beliefs about ED-specific rumination processes. An additional key limitation of this study includes the use of cross-sectional data, temporal associations between rumination and ED symptom severity cannot be assumed. Finally, our findings may not generalize to other samples. More research is needed to evaluate the extent to which these associations are evident among individuals with varying ED symptom severity (e.g., clinical samples, treatment-seeking individuals), comorbid psychiatric disorders often characterized by ruminative processes (e.g., generalized anxiety disorder, other anxiety-related disorders), or different demographic groups (e.g., across gender or sexual orientations). Because the current study did not account for co-occurring symptom presentations (e.g., depressive symptoms) or diagnoses, future studies should aim to assess and account for comorbid symptom severity and co-occurring psychiatric diagnoses.
Conclusion
This study evaluated the extent to which general and ED-specific ruminative processes and their interactions with positive beliefs about rumination relate to eating pathology in college-aged adults with varied ED symptom severity. Results generally coincide with the broader body of research that suggests brooding is particularly maladaptive and contributes to increased psychopathology [7,8,9], while also suggesting that any form of disorder-specific rumination (brooding or reflection) relates to elevated eating pathology. Findings also suggest that the association between both general and ED-specific reflection and ED symptom severity is stronger among individuals who endorse lower positive beliefs about rumination. Overall, findings suggest that future research must consider the unique roles that these variables may play in EDs.
What is already known on this subject?
Rumination is a transdiagnostic cognitive factor comprised of two subfactors, brooding and reflection, each of which uniquely relates to psychopathology (e.g., mood and anxiety disorders). Prior research suggests that brooding and reflection differentially relate to ED symptoms, with initial evidence suggesting that disorder-specific brooding may have a particularly strong association with eating pathology. Mood and anxiety disorders research suggests that positive beliefs about the benefits of rumination may moderate the associations between rumination constructs and psychopathology; however, the role of positive beliefs has not yet been explored in EDs.
What does this study add?
Prior research established that brooding and reflection uniquely relate to eating pathology. However, the specific relations between disorder-specific and general forms of ruminative constructs and ED symptom severity remain relatively unknown. This study provides evidence that disorder-specific ruminative processes (both brooding and reflection) relate to ED symptoms, above and beyond general ruminative processes. This is also the first investigation to evaluate the extent to which positive beliefs about rumination impact the association between rumination and ED symptom severity.
Data availability
The datasets generated during and/or analyzed during the current study are available from Lisa M. Anderson (ande8936@umn.edu) upon reasonable request.
Code availability
Available upon reasonable request.
References
McEvoy P (2013) The relationship between worry, rumination, and comorbidity: evidence for repetitive negative thinking as a transdiagnostic construct. J Affect Disord 151(2013):313–320. https://doi.org/10.1016/j.jad.2013.06.014
Nolen-Hoeksema S, Watkins E (2011) A heuristic for developing transdiagnostic models of psychopathology: explaining multifinality and divergent trajectories. Perspect Psychol Sci 6(6):589–609. https://doi.org/10.1177/1745691611419672
Troop N, Holbrey A, Treasure J (1998) Stress, coping, and crisis support in eating disorders. Int J Eat Disord 24(2):157–166. https://doi.org/10.1002/(SICI)1098-108X(199809)24:2%3c157::AID-EAT5%3e3.0.CO;2-D
Nolen-Hoeksema S, Stice E, Wade E, Bohon C (2007) Reciprocal relations between rumination and bulimic, substance abuse, and depressive symptoms in female adolescents. J Abnorm Psychol 116(1):198–207. https://doi.org/10.1037/0021-843X.116.1.198
Naumann E, Tuschen-Caffier B, Voderholzer U, Caffier D, Svaldi J (2015) Rumination but not distraction increases eating-related symptoms in anorexia and bulimia nervosa. J Abnorm Psychol 124(2):412–420. https://doi.org/10.1037/abn0000046
Reilly E, Lavender J, Berner L, Brown T, Wierenga C, Kaye W (2019) Could repetitive negative thinking interfere with corrective learning? The example of anorexia nervosa. Int J Eat Disord 52:36–41. https://doi.org/10.1002/eat.22997
Treynor W, Gonzalez R, Nolen-Hoeksema S (2003) Rumination reconsidered: a psychometric analysis. Cogn Ther Res 27(3):247–259. https://doi.org/10.1023/A:1023910315561
Burwell R, Shirk S (2007) Subtypes of rumination in adolescence: Associations between brooding, reflection, depressive symptoms, and coping. J Clin Child Adolesc Psychol 36(1):56–65. https://doi.org/10.1080/15374410709336568
Schoofs H, Hermans D, Raes F (2010) Brooding and reflection as subtypes of rumination: Evidence from confirmatory factor analysis in nonclinical samples using the Dutch ruminative response scale. J Psychopathol Behav Assess 32(4):609–617. https://doi.org/10.1007/s10862-010-9182-9
Smith K, Mason T, Lavender J (2018) Rumination and eating disorder psychopathology: a meta-analysis. Clin Psychol Rev 61:9–23. https://doi.org/10.1016/j.cpr.2018.03.004
Naumann E, Tuschen-Caffier B, Voderholzer U, Schäfer J, Svaldi J (2016) Effects of emotional acceptance and rumination on media-induced body dissatisfaction in anorexia and bulimia nervosa. J Psychiatr Res 82:119–125. https://doi.org/10.1016/j.jpsychires.2016.07.021
Dondzilo L, Rieger E, Palermo R, Byrne S, Bell J (2016) Association between rumination factors and eating disorder behaviours in young women. Adv Eat Disord 4(1):84–98. https://doi.org/10.1080/21662630.2015.1118642
Jong-Meyer R, Beck B, Riede K (2009) Relationships between rumination, worry, intolerance of uncertainty and metacognitive beliefs. Personality Individ Differ 46(4):547–551. https://doi.org/10.1016/j.paid.2008.12.010
Papageorgiou C, Wells A (2001) Positive beliefs about depressive rumination: development and preliminary validation of a self-report scale. Behav Ther 32(1):13–26. https://doi.org/10.1016/S0005-7894(01)80041-1
Watkins E, Moulds M (2005) Positive beliefs about rumination in depression: a replication and extension. Personal Individ Differ 39(1):73–82. https://doi.org/10.1016/j.paid.2004.12.006
Wong Q, Moulds M (2010) Do socially anxious individuals hold positive metacognitive beliefs about rumination? Behav Chang 27(2):69–83. https://doi.org/10.1375/bech.27.2.69
Sütterlin S, Paap M, Babic S, Kübler A, Vögele C (2012) Rumination and age: some things get better. J Aging Res 2012:267327. https://doi.org/10.1155/2012/267327
Eisenberg D, Nicklett EJ, Roeder K (2011) Eating disorder symptoms among college students: prevalence, persistence, correlates, and treatment-seeking. J Am Coll Health 59(8):700–707. https://doi.org/10.1080/07448481.2010.546461
Ehrlich LE (2018) Perseverative thinking in eating pathology: do rumination patterns differ according to symptom type? [Master's Thesis, University at Albany]. ProQuest Dissertations and Theses Global.
Cowdrey F, Park R (2011) Assessing rumination in eating disorders: Principal component analysis of a minimally modified ruminative response scale. Eat Behav 12(4):321–324. https://doi.org/10.1016/j.eatbeh.2011.08.001
Stice E, Telch C, Rizvi S (2000) Development and validation of the eating disorder diagnostic scale: a brief self-report measure of anorexia, bulimia, and binge-eating disorder. Psychol Assess 12(2):123–131. https://doi.org/10.1037//1040-3590.12.2.123
Field A (2009) Discovering Statistics Using SPSS, Third Edition.
Hayes AF (2012) PROCESS: A versatile computational tool for observed variable mediation, moderation, and conditional process modeling. https://www.afhayes.com. Accessed 15 September 2020
Krabbenborg MA, Danner UN, Larsen JK et al (2012) The eating disorder diagnostic scale: psychometric features within a clinical population and a cut-off point to differentiate clinical patients from healthy controls. Eur Eat Disord Rev 20(4):315–320. https://doi.org/10.1002/erv.1144
Smith K, Schaumberg K, Reilly E et al (2020) The ecological validity of trait-level rumination measures among women with binge eating symptoms. Eat Weight Disord-Stud Anorexia Bulimia Obesity 26(1):181-190. https://doi.org/10.1007/s40519-019-00838-x
Watkins E, Scott J, Wingrove J et al. (2007) Rumination-focused cognitive behaviour therapy for residual depression: a case series. Behav Res Ther 45(9):2144–2154. https://doi.org/10.1016/j.brat.2006.09.018
Watkins E, Mullan E, Wingrove J et al. (2011) Rumination-focused cognitive–behavioural therapy for residual depression: Phase II randomised controlled trial. Br J Psychiatry 199(4):317–322. https://doi.org/10.1192/bjp.bp.110.090282
Acknowledgements
This work was supported by the National Institute of Mental Health of the National Institutes of Health under award numbers T32 MH082761 (L. Anderson), K23 MH123910 (L. Anderson), and K23 MH112867 (Haynos). It was additionally supported by the University of Minnesota Office of Undergraduate Research (Rich), Klarman Family Foundation (Haynos), and Hilda and Preston Davis Foundation (Haynos). This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Funding
This work was supported by the National Institute of Mental Health of the National Institutes of Health under award numbers T32 MH082761 (L. Anderson), K23 MH123910 (L. Anderson), and K23 MH112867 (Haynos). It was additionally supported by the University of Minnesota Office of Undergraduate Research (Rich), Klarman Family Foundation (Haynos), and Hilda and Preston Davis Foundation (Haynos). This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection was conducted by LEE and DAA. Material preparation and data analysis were performed by ACR and LMA. The first draft of the manuscript was written by ACR and LMA, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no conflicts of interest to disclose
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent to publish
Participants signed informed consent regarding publishing their data.
Ethics approval
This study was approved by the University at Albany, State University of New York’s Institutional Review Board. Study procedures were performed in accordance with the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Rich, A.C., Haynos, A.F., Anderson, D.A. et al. The role of rumination and positive beliefs about rumination in eating pathology. Eat Weight Disord 27, 979–988 (2022). https://doi.org/10.1007/s40519-021-01209-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-021-01209-1