Abstract
Purpose
Limited data are available linking breakfast consumption to Heart Burn Syndrome (HBS). This study was done to investigate to find whether breakfast consumption is associated with HBS. This cross-sectional study was done to investigate the association between breakfast consumption and HBS among Iranian adults.
Methods
This cross-sectional study was performed among 4763 general adults of Isfahan, Iran. Participants’ patterns of breakfast eating were assessed by asking two questions from them. How often do you eat breakfast in a week?” Participants were able to respond as: "never or 1 day/wk", "2–4 days/wk", "5–6 days/wk", "every day". HBS was defined as the presence of HBS at sometimes, often or always using a Persian version of validated self-administered modified ROME III questionnaire.
Results
Totally, 4763 patients with HBS completed this cross-sectional study, where about 32.4% of them intake breakfast less than one time per week. After controlling for potential confounders, participants who consumed breakfast every day had a 43% lower risk for having HBS as compared with those who had breakfast ≤ 1 times/wk (OR 0.57; 95% CI 0.41–0.80). A significant inverse relationship was found between breakfast consumption and frequent than scare HBS (OR 0.57; 95% CI 0.40–0.77) among the whole population, not in patients with HBS. No significant association was observed between breakfast intake and severity of HBS (OR 0.56; 95% CI 0.31–1.04).
Conclusion
We found an inverse association between frequency of breakfast consumption and odds of HBS as well as the frequency of HBS among the adult population. Prospective studies are required to confirm these findings.
Level of evidence
Level V, cross-sectional descriptive study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Heart Burn Syndrome (HBS) is a highly prevalent condition affecting a wide range of people in the world [1]. HBS has become very common in the past three decades [2]. In the US, almost half of adult people experience reflux symptoms monthly [3]. In western nations, 10–20% of adult populations are affected [4]. Although the prevalence in Asian countries is comparatively low, recent estimates indicated the increasing trend of this condition [5]. In Iran, 1.9–52% of adult population has been reported to have the condition based on different definitions [6]. HBS is associated with several complications including esophagitis, esophageal ulcer, upper GI bleeding and Barrett esophagus [7]. Furthermore, it affects quality of life and imposes a great burden on the health care system [8].
The exact etiology of HBS is still unknown. Besides genetic predisposition, it seems that lifestyle factors greatly contribute to this condition [9]. Among several lifestyle-related factors, poor sleep quality, smoking, alcohol drinking, short meal-to-sleep interval and irregular dietary habits have been reported as strong determinants [10]. Although some studies have been conducted to identify the diet-related factors in HBS [11, 12], limited information is available about the relationship between breakfast consumption and HBS. In a cross-sectional study in Japan, it has been found that irregular dietary habits and breakfast skipping could strongly contribute to HBS symptoms; such that the effects of breakfast skipping were even stronger than smoking and alcohol consumption [13]. However, participants in that study were among wealthy peoples with specific dietary habits. Therefore, this finding might not completely reflect the population-based data from Asian people. In the current study, we hypothesized that breakfast skipping might contribute to HBS because skipping meals might exacerbate gastric acidity, a phenomenon that is observed in patients with HBS [14, 15]. Furthermore, prior studies have indicated a significant association between breakfast skipping and obesity [16, 17]. The link between obesity and the prevalence of HBS has also been shown [9]. Therefore, breakfast skipping might contribute to HBS through its effects on obesity. Given the limited evidence of the relationship between breakfast consumption and HBS as well as the increasing trend of HBS in the Asian countries, including Iran, we examined the association between breakfast skipping and prevalent HBS among a large group of Iranian adults.
Methods
Study population
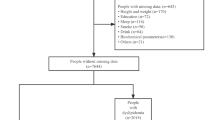
This cross-sectional study was performed among general adult population of Isfahan. The study was conducted in the framework of SEPAHAN (the study on the epidemiology of psychological, alimentary health and nutrition) project that has been designed to investigate the epidemiological aspects of functional gastrointestinal disorders (FGIDs) and their relationship with different lifestyle and psychological factors [18]. Briefly, this study was conducted among nonacademic staff working in 50 different health centers affiliated to the Isfahan University of Medical Sciences (IUMS) in Isfahan province, Iran. These participants worked in hospitals, university campuses, and health centers. The required sample size was determined based on the proposed formula for cross-sectional studies [19]. We hypothesized the prevalence of FGDIs as 15%. So, considering the type I error of 5% and the study power of 80%, and desired confidence interval of 0.03, we reached the minimum required sample size of 1387 subjects. In the SEPAHAN project, data collection was done in two main phases. In the first and second phases of the project, 10,087 and 9652 questionnaires were sent to subjects aged 18–55 years, respectively. The questionnaire in the first phase included questions on demographic information, lifestyle and nutritional factors. Totally, 8691 subjects returned the completed questionnaire (response rate: 86.16%). The questionnaire is the second phase included questions on gastrointestinal disorders; which 6239 subjects completed and returned questionnaires (response rate: 64.64%). The national identification number of participants was used to merge the questionnaires from two phases. We were unable to use 1476 questionnaires in the final analysis, due to incomplete questionnaires or lack of having national identification number in phase 1 or 2 as well as having missing information on exposure or outcome of interest. Finally, data on 4763 subjects, who had complete data on related variables, were analyzed (Fig. 1). Ethical approval of the study was provided by the Medical Research Ethics Committee of Isfahan University of Medical Sciences (IUMS). All participants provided informed written consent.
Assessment of breakfast skipping
We asked a question from participants to assess patterns of breakfast eating: 1) “How frequently do you eat breakfast during a week?” Participants were able to respond as: "never or 1 day/wk", "2–4 days/wk", "5–6 days/wk", "every day".
Assessment of HBS
A Persian version of validated self-administered modified ROME III questionnaire was applied to assess the functional gastrointestinal disorders [18]. As the rating scales used in ROME III (never, less than 1 day a month, 1 day a month, 2–3 days a month, 1 day a week, more than 1 day a week, every day) were hard to be discriminated by most participants during the face validation of the questionnaire, we modified the rating scale of the original questionnaire into a four-item rating scale (never or rarely, sometimes, often, always). In the current study, HBS was defined as the presence of reflux attack sometimes, often or always. The validity and reliability of Persian version of ROME III questionnaire in Iranian population has earlier been shown [18].
Assessment of other variables
Information on age, sex, marital status, smoking, existence of diabetes, supplement use, and Oral Contraceptive Pill (OCP) use were obtained by demographic and medical history questionnaires. The General Practice Physical Activity Questionnaire (GPPAQ) was used to assess participants’ physical activity [20]. As previous investigations have shown that even 1 h of walking per week may reduce the risk of chronic diseases [21], we classified participants as: physically active (≥ 1 h/week) and inactive (< 1 h/week). In addition, anthropometric measures including weight, height, and waist circumference (WC) were assessed using a validated self-administered questionnaire [22]. Then, body mass index (BMI) was calculated as weight in kilograms divided by height in meters squared. Furthermore, information on dietary habits including number of meals per day, chewing behaviors, eating speed, meals to sleep intervals, and consumption of spicy foods were also examined.
Statistical analysis
Participants were classified into four categories based on their frequencies of breakfast consumption "never or 1 day/wk", "2–4 days/wk", "5–6 days/wk", "every day". One-way ANOVA and Chi-square test were used to compare general characteristics of study subjects across different categories of breakfast consumption for continuous and categorical variables, respectively. Multivariable logistic regression in different models was used to find the relation between breakfast consumption and odds of HBS presence. First, we adjusted for age (years) and sex (male/female). Findings were additionally adjusted for smoking (yes/no), presence of chronic conditions (yes/no), and physical activity (less/more than 1 h per week) in Model 2. Further control for number of meals per day (one/two/three), chewing quality (not very well/well/more than adequate), quick eating (yes/no), meal to sleep interval (less than 2 h as short/more than 2 h as adequate), and spicy foods consumption (˂3/4–6/ ≥ 7 times/week) was done in the third model. Finally, additional adjustment was done for BMI (kg/m2). The first category of breakfast consumption (never or 1 day/wk) was considered as reference in the analyses. We considered the categories as ordinal variable to calculate the trend of odds ratios across increasing categories of breakfast consumption. To determine the association of breakfast consumption with severity of heartburn syndrome, we applied multivariable ordinal logistic regression. P values less than 0.05 were considered as statistically significant. All analyses were performed using Statistical Package for Social Sciences (SPSS Corp, version 18, Chicago, IL, USA).
Results
General Characteristics of study participants across various categories of frequency of breakfast consumption is shown in Table 1. Compared with those who had breakfast ≤ 1 time/wk, individuals who consumed breakfast daily were older, more likely to be females and physically active. No significant differences were found in terms of mean weight, BMI as well as distribution of smokers, supplement users and obesity across various categories of breakfast intake.
Distribution of participants in terms of diet-related behaviors across different categories of breakfast intake is provided in Table 2. Compared to those who had breakfast ≤ 1 time/wk, lower percentage of people who had breakfast daily, consumed one meal a day and a greater percentage of them had three meals per day. Greater percentage of subjects who had breakfast daily reported well chewing of foods compared with those who had breakfast ≤ 1 time/wk. Quick eating was highly prevalent among those with frequent breakfast intake. Breakfast consumers were less likely to have a short meal-to-sleep interval than breakfast skippers.
Multivariable-adjusted odds ratios for having HBS across various categories of breakfast intake are indicated in Table 3. Daily intake of breakfast was associated with a reduced risk of HBS; such that those who consumed breakfast everyday had 43% lower risk (OR 0.57; 95% CI 0.45–0.72) for having HBS as compared with those who had breakfast ≤ 1 times/wk. Adjustment for potential confounders including age, gender, smoking and physical activity did not significantly attenuate the association. Even after adjusting for all confounders, including diet-related behaviors and BMI, there was still a significant inverse association between breakfast intake and risk of HBS (OR 0.57; 95% CI 0.41–0.80). The prevalence of heart burn syndrome across categories of breakfast intake is shown in Fig. 2.
Multivariable-adjusted odds ratios for frequency of HBS across various categories of breakfast intake are shown in Table 4. When the analysis was done for the whole population, we found a significant inverse relationship between breakfast consumption and frequent HBS (OR 0.55; 95% CI 0.44–0.70). After controlling for potential confounders, including BMI, those who had breakfast everyday were 45% less likely to have frequent HBS than those who had breakfast ≤ 1 times/wk (OR 0.57; 95% CI 0.40–0.77). When the analysis was confined to those with HBS, the association disappeared (OR 0.56; 95% CI 0.28–1.13).
Multivariable-adjusted odds ratios for severity of HBS across different categories of breakfast intake among individuals with HBS are provided in Table 5. We observed an inverse association between regular breakfast consumption and severity of HBS in crude model (OR 0.57; 95% CI 0.37–0.87). However, when potential confounders were taken into account, this relationship became non-significant (OR 0.57; 95% CI 0.31–1.05). When the model was adjusted for BMI, we observed a trend toward inverse association between breakfast intake and severity of HBS (OR 0.56; 95% CI 0.31–1.04).
Discussion
In this cross-sectional study, an inverse association was found between frequency of breakfast consumption and odds of HBS as well as HBS severity among adults. This association remained significant even after controlling for a wide range of potential confounders. To the best of our knowledge, limited information is available about the relationship between breakfast consumption and HBS. Heartburn is the classic and most common symptom of GERD. However, the diagnosis of GERD usually was done by upper gastrointestinal endoscopic examination or using the GERD Symptom Assessment Scale (GSAS). In our study, we used a modified ROME III questionnaire that contain some questions about the presence of heartburn symptoms. So, we did not perform endoscopic examination. This is why we did not use GERD as the outcome instead of heartburn syndrome.
Totally gastrointestinal problems are highly prevalent among adult population which can affect quality of life [8]. Lifestyle-related factors, including dietary habits and dietary intakes might influence their occurrence and severity [23,24,25]. We found that breakfast intake was inversely associated with HBS in the Iranian adult population. In line with ours, a cross-sectional study in Japan reported a strong inverse association between breakfast consumption and HBS symptoms [13]. The direct association of breakfast skipping with HBS symptoms was also reported in another study on 1840 junior high school students in Japan [26]. However, in a cohort study on 817 Japanese patients with type 2 diabetes, the authors did not find a significant relationship between breakfast skipping and HBS. However, participants of the latter study were patients with type 2 diabetes mellitus who had been treated for diabetes for several years [27]. Therefore, many of them might have changed their eating behaviors to control hyperglycemia. Overall, it seems that breakfast consumption, along with other dietary habits, can be recommended as a preventive measure to HBS.
Breakfast is among the most important meals which provide micro- and macro-nutrients [28]. It has been shown that breakfast skippers were more likely to have a poor diet quality compared with breakfast consumers [29, 30]. The exact mechanism through which breakfast consumption might affect HBS has not been understood. However, breakfast skipping might exacerbate gastric acidity which has been considered as an important risk factor of HBS development [31, 32]. Furthermore, breakfast skipping was associated with overweight and obesity [33, 34], which is in turn associated with an elevated risk of HBS [33,34,35]. Poor dietary quality and physical inactivity which are commonly observed among breakfast skippers might explain the high prevalence of obesity in these individuals [29, 36]. Furthermore, breakfast consumption has been found to alter inflammation, mainly due to change in levels of gastrointestinal peptides [37, 38]. Changing in gastrointestinal inflammatory environment has been also linked to HBS development [39]. In addition, we found that participants with frequent breakfast intake were more likely to have some healthy diet-related behaviors including good chewing of foods and adequate meal-to-sleep interval than breakfast skippers. Imperfect chewing of foods and short meal-to-sleep interval were also found to increase HBS severity [40].
Several strengths of the study should be highlighted. This is the first study from the Middle Eastern countries with a large sample size investigating the association of breakfast consumption with HBS among adults. A wide range of potential confounders were controlled for to reach an independent association between breakfast consumption and HBS. In addition, diet-related behaviors were taken into account in the current study. Given these strengths, some limitations should also be considered. Due to the cross-sectional design of the study, it is impossible to confer causality. Further studies, in particular of prospective design, are needed to discover causality and to confirm our findings. Symptoms of HBS were examined based on a self-administrated questionnaire in this study. Although validated questionnaires were used, misclassification of study participants cannot be excluded. In addition, the study was conducted on a population from Isfahan province, therefore, generalizing the findings to Iranian adults should be done cautiously.
Conclusions
In conclusion, findings from this cross-sectional study showed an inverse association between frequency of breakfast consumption and odds of HBS and frequency of HBS among adult populations. Further prospective studies, in particular from Middle-Eastern countries, are required to confirm these findings.
What is already known on this subject?
Several lifestyle-related factors are contributed to the etiology of HBS. Among them, irregular dietary habits have been reported as strong determinants. Some studies shown that breakfast skipping increased the odds of gastrointestinal diseases while others reported no significant association. In addition, most publications in this regard were from western countries and few information are accessible from the Middle-East.
What does this study add?
We estimated that 32.4% of the participants consumed breakfast less than one time per week. We also found subjects who consumed breakfast everyday had 43% lower risk for having HBS as compared with those who had breakfast less than one time per week.
References
Leu HB, Chen JW, Wu TC, Ding YA, Lin SJ, Charng MJ (2005) Effects of fluvastatin, an HMG-CoA reductase inhibitor, on serum levels of interleukin-18 and matrix metalloproteinase-9 in patients with hypercholesterolemia. Clin Cardiol 28(9):423–428. https://doi.org/10.1002/clc.4960280907
Panichi V, Paoletti S, Mantuano E, Manca-Rizza G, Filippi C, Santi S, Taccola D, Donadio C, Tramonti G, Innocenti M, Casto G, Consani C, Sbragia G, Franzoni F, Galetta F, Panicucci E, Barsotti G (2006) In vivo and in vitro effects of simvastatin on inflammatory markers in pre-dialysis patients. Nephrol Dial Transpl 21(2):337–344. https://doi.org/10.1093/ndt/gfi224
Bruni F, Pasqui AL, Pastorelli M, Bova G, Cercignani M, Palazzuoli A, Sawamura T, Gioffre WR, Auteri A, Puccetti L (2005) Different effect of statins on platelet oxidized-LDL receptor (CD36 and LOX-1) expression in hypercholesterolemic subjects. Clin Appl Thromb Hemost 11(4):417–428. https://doi.org/10.1177/107602960501100408
Sola S, Mir MQ, Rajagopalan S, Helmy T, Tandon N, Khan BV (2005) Statin therapy is associated with improved cardiovascular outcomes and levels of inflammatory markers in patients with heart failure. J Card Fail 11(8):607–612. https://doi.org/10.1016/j.cardfail.2005.05.011
Ray KK, Cannon CP, Cairns R, Morrow DA, Rifai N, Kirtane AJ, McCabe CH, Skene AM, Gibson CM, Ridker PM, Braunwald E (2005) Relationship between uncontrolled risk factors and C-reactive protein levels in patients receiving standard or intensive statin therapy for acute coronary syndromes in the PROVE IT-TIMI 22 trial. J Am Coll Cardiol 46(8):1417–1424. https://doi.org/10.1016/j.jacc.2005.08.024
Damas JK, Boullier A, Waehre T, Smith C, Sandberg WJ, Green S, Aukrust P, Quehenberger O (2005) Expression of fractalkine (CX3CL1) and its receptor, CX3CR1, is elevated in coronary artery disease and is reduced during statin therapy. Arterioscler Thromb Vasc Biol 25(12):2567–2572. https://doi.org/10.1161/01.ATV.0000190672.36490.7b
Nakaya R, Uzui H, Shimizu H, Nakano A, Mitsuke Y, Yamazaki T, Ueda T, Lee JD (2005) Pravastatin suppresses the increase in matrix metalloproteinase-2 levels after acute myocardial infarction. Int J Cardiol 105(1):67–73. https://doi.org/10.1016/j.ijcard.2004.12.024
Meredith IT, Plunkett JC, Worthley SG, Hope SA, Cameron JD (2005) Systemic inflammatory markers in acute coronary syndrome: association with cardiovascular risk factors and effect of early lipid lowering. Coron Artery Dis 16(7):415–422
ter Avest E, Abbink EJ, Holewijn S, de Graaf J, Tack CJ, Stalenhoef AF (2005) Effects of rosuvastatin on endothelial function in patients with familial combined hyperlipidaemia (FCH). Curr Med Res Opin 21(9):1469–1476. https://doi.org/10.1185/030079905x61910
Verma A, Ranganna KM, Reddy RS, Verma M, Gordon NF (2005) Effect of rosuvastatin on C-reactive protein and renal function in patients with chronic kidney disease. Am J Cardiol 96(9):1290–1292. https://doi.org/10.1016/j.amjcard.2005.06.074
Milionis HJ, Gazi IF, Filippatos TD, Tzovaras V, Chasiotis G, Goudevenos J, Seferiadis K, Elisaf MS (2005) Starting with rosuvastatin in primary hyperlipidemia–Is there more than lipid lowering? Angiology 56(5):585–592. https://doi.org/10.1177/000331970505600510
Stalenhoef AF, Ballantyne CM, Sarti C, Murin J, Tonstad S, Rose H, Wilpshaar W (2005) A comparative study with rosuvastatin in subjects with metabolic syndrome: results of the COMETS study. Eur Heart J 26(24):2664–2672. https://doi.org/10.1093/eurheartj/ehi482
Yamamichi N, Mochizuki S, Asada-Hirayama I, Mikami-Matsuda R, Shimamoto T, Konno-Shimizu M, Takahashi Y, Takeuchi C, Niimi K, Ono S (2012) Lifestyle factors affecting gastroesophageal reflux disease symptoms: a cross-sectional study of healthy 19864 adults using FSSG scores. BMC Med 10(1):45. https://doi.org/10.1186/1741-7015-10-45
ter Avest E, Abbink EJ, de Graaf J, Tack CJ, Stalenhoef AF (2005) Effect of rosuvastatin on insulin sensitivity in patients with familial combined hyperlipidaemia. Eur J Clin Invest 35(9):558–564. https://doi.org/10.1111/j.1365-2362.2005.01549.x
Takebayashi K, Matsumoto S, Wakabayashi S, Inukai Y, Matsutomo R, Aso Y, Inukai T (2005) The effect of low-dose atorvastatin on circulating monocyte chemoattractant protein-1 in patients with type 2 diabetes complicated by hyperlipidemia. Metabolism 54(9):1225–1229. https://doi.org/10.1016/j.metabol.2005.04.008
Li JJ, Fang CH (2005) Effects of 4 weeks of atorvastatin administration on the antiinflammatory cytokine interleukin-10 in patients with unstable angina. Clin Chem 51(9):1735–1738. https://doi.org/10.1373/clinchem.2005.049700
Okopien B, Krysiak R, Kowalski J, Madej A, Belowski D, Zielinski M, Herman ZS (2005) Monocyte release of tumor necrosis factor-alpha and interleukin-1beta in primary type IIa and IIb dyslipidemic patients treated with statins or fibrates. J Cardiovasc Pharmacol 46(3):377–386
Adibi P, Keshteli AH, Esmaillzadeh A, Afshar H, Roohafza H, Bagherian-Sararoudi R, Daghaghzadeh H, Soltanian N, Feinle-Bisset C, Boyce P (2012) The study on the epidemiology of psychological, alimentary health and nutrition (SEPAHAN): overview of methodology. J Res Med Sci 17(2):292–298
Charan J, Biswas T (2013) How to calculate sample size for different study designs in medical research? Indian J Psychol Med 35(2):121
Policy PA (2009) Health improvement directorate. The General Practice Physical Activity Questionnaire (GPPAQ) A screening tool to assess adult physical activity levels, within primary care London: Department of Health. https://www.gov.uk
Oguma Y, Shinoda-Tagawa T (2004) Physical activity decreases cardiovascular disease risk in women: review and meta-analysis. Am J Prev Med 26(5):407–418. https://doi.org/10.1016/j.amepre.2004.02.007
Aminianfar S, Saneei P, Nouri M, Shafiei R, Hassanzadeh-Keshteli A, Esmaillzadeh A, Adibi P (2015) Validation study of self-reported anthropometric indices among the staff of the Isfahan University of Medical Sciences, Isfahan. Iran J Isfahan Med Sch 33(346):1318–1327
Ebrahimi-Mameghani M, Sabour S, Khoshbaten M, Arefhosseini SR, Saghafi-Asl M (2017) Total diet, individual meals, and their association with gastroesophageal reflux disease. Health Promot Perspect 7(3):155
Sethi S, Richter JE (2017) Diet and gastroesophageal reflux disease: role in pathogenesis and management. Curr Opin Gastroenterol 33(2):107–111. https://doi.org/10.1097/MOG.0000000000000337
Salari-Moghaddam A, Keshteli AH, Mousavi SM, Afshar H, Esmaillzadeh A, Adibi P (2019) Adherence to the MIND diet and prevalence of psychological disorders in adults. J Affect Disord 256:96–102
Sakaguchi K, Yagi T, Maeda A, Nagayama K, Uehara S, Saito-Sakoguchi Y, Kanematsu K, Miyawaki S (2014) Association of problem behavior with sleep problems and gastroesophageal reflux symptoms. Pediatr Int 56(1):24–30. https://doi.org/10.1111/ped.12201
Takeshita E, Furukawa S, Sakai T, Niiya T, Miyaoka H, Miyake T, Yamamoto S, Senba H, Yamamoto Y, Arimitsu E (2017) Eating behaviours and prevalence of gastroesophageal reflux disease in japanese patients with type 2 diabetes mellitus: the dogo study. Can J Diabetes. https://doi.org/10.1016/j.jcjd.2017.07.007
Nicklas TA, O’neil C, Myers L, (2004) The importance of breakfast consumption to nutrition of children, adolescents, and young adults. Nutr Today 39(1):30–39. https://doi.org/10.1097/00017285-200401000-00009
Otaki N, Obayashi K, Saeki K, Kitagawa M, Tone N, Kurumatani N (2017) Relationship between breakfast skipping and obesity among elderly: Cross-sectional analysis of the HEIJO-KYO study. J Nutr Health Aging 21(5):501–504. https://doi.org/10.1007/s12603-016-0792-0
Milajerdi A, Keshteli A, Esmaillzadeh A, Roohafza H, Afshar H, Adibi P (2018) Breakfast consumption in relation to lowered risk of psychological disorders among Iranian adults. Public Health. https://doi.org/10.1016/j.puhe.2018.05.020
Schubert ML (2008) Hormonal regulation of gastric acid secretion. Curr Gastroenterol Rep 10(6):523–527. https://doi.org/10.1007/s11894-008-0097-5
Gardner JD (2010) GERD: increased gastric acid secretion as a possible cause of GERD. Nat Rev Gastroenterol Hepatol 7(3):125–126. https://doi.org/10.1038/nrgastro.2009.240
Watanabe Y, Saito I, Henmi I, Yoshimura K, Maruyama K, Yamauchi K, Matsuo T, Kato T, Tanigawa T, Kishida T (2014) Skipping breakfast is correlated with obesity. J Rural Med 9(2):51–58. https://doi.org/10.2185/jrm.2887
Horikawa C, Kodama S, Yachi Y, Heianza Y, Hirasawa R, Ibe Y, Saito K, Shimano H, Yamada N, Sone H (2011) Skipping breakfast and prevalence of overweight and obesity in Asian and Pacific regions: a meta-analysis. Prev Med 53(4):260–267. https://doi.org/10.1016/j.ypmed.2011.08.030
Tanaka Y, Sakata Y, Hara M, Kawakubo H, Tsuruoka N, Yamamoto K, Itoh Y, Hidaka H, Shimoda R, Iwakiri R (2017) Risk factors for helicobacter pylori infection and endoscopic reflux esophagitis in healthy young Japanese volunteers. Intern Med. https://doi.org/10.2169/internalmedicine.8669-16
Mousavi SM, Shayanfar M, Rigi S, Mohammad-Shirazi M, Sharifi G, Esmaillzadeh A (2020) Adherence to the Mediterranean dietary pattern in relation to glioma: a case-control study. Clin Nutr. https://doi.org/10.1016/j.clnu.2020.05.022
McFarlin B, Carpenter K, Henning A, Venable A (2017) Consumption of a high-fat breakfast on consecutive days alters preclinical biomarkers for atherosclerosis. Eur J Clin Nutr 71(2):239–244. https://doi.org/10.1038/ejcn.2016.242
Nas A, Mirza N, Hägele F, Kahlhöfer J, Keller J, Rising R, Kufer TA, Bosy-Westphal A (2017) Impact of breakfast skipping compared with dinner skipping on regulation of energy balance and metabolic risk. Am J Clin Nutr 105(6):1351–1361. https://doi.org/10.3945/ajcn.116.151332
Kim JJ, Kim N, Choi YJ, Kim JS, Jung HC (2016) Increased TRPV1 and PAR2 mRNA expression levels are associated only with the esophageal reflux symptoms, but not with the extraesophageal reflux symptoms. Medicine. https://doi.org/10.1097/MD.0000000000004387
Asl SF, Mansour-Ghanaei F, Samadi H, Joukar F (2015) Evaluations of life style factors and the severity of gastroesophageal reflux disease; a case-control study. Int J Mol Epidemiol Genet 6(1):27
Acknowledgements
The authors acknowledge their staff, the fieldworkers, and SEPAHAN project participants that without them this work would not have been possible. This study was supported by the Vice Chancellery for Research and Technology, Isfahan University of Medical Sciences (IUMS).
Funding
SEPAHAN was financially supported by the Vice Chancellery for Research and Technology, Isfahan University of Medical Sciences (IUMS). This study was supported by funding from Isfahan University of Medical Sciences (Grant Number: 627002).
Author information
Authors and Affiliations
Contributions
AM and SMM wrote the manuscript. AE analyzed and interpreted the data. AHK, HR, HA, PA, and AE designed the study and contributed to data collection and interpretation. PA and AE revised the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical approval
Ethical approval of the study was provided by the Medical Research Ethics Committee of Isfahan University of Medical Sciences (IUMS).
Informed consent
Informed consent was obtained from all participants in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Milajerdi, A., Bagheri, F., Mousavi, S.M. et al. Breakfast skipping and prevalence of heartburn syndrome among Iranian adults. Eat Weight Disord 26, 2173–2181 (2021). https://doi.org/10.1007/s40519-020-01065-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-020-01065-5