Abstract
Purpose
We estimated cross-sectional and longitudinal associations between depression symptoms and night eating in young adults.
Methods
Data were drawn from a longitudinal investigation of students age 12–13 years at inception in 1999–2000, in Montreal, Canada. Depression symptoms were measured with the Depressive Symptoms Scale (DSS) 20 times from age 12 to 17, and with the Major Depression Inventory (MDI) post-high school at ages 20 and 24. Night eating was measured at age 24. The association between depression symptoms and night eating was estimated in multivariable logistic regression models adjusted for sex, age and mother university-educated.
Results
9% of 829 participants (n = 77) reported night eating. In cross-sectional analysis, the adjusted odds ratio (OR) estimate for MDI scores (range 0–50) was 1.04 (1.01, 1.07). In longitudinal analyses, the OR estimates were 1.75 (1.20, 2.55) for DSS scores (range 1–4) and 1.03 (1.002, 1.06) for the MDI.
Conclusions
Depression symptoms are associated with night eating in young adults cross-sectionally and possibly longitudinally. Treatment of depression symptoms may be important in preventing night eating, a core symptom of the Night Eating Syndrome.
Level of evidence
Level III, cohort analytic study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Disordered eating behaviors are common in young adults [1, 2]. One such disorder, the Night Eating Syndrome (NES), typically begins in early adulthood [3] and is characterized by a delay in the circadian rhythm of food intake [4], symptoms of pathological eating, and sleep and mood disturbances [5,6,7,8]. Night eating (NE) has garnered interest for its possible role in the development and maintenance of obesity [5, 9, 10] and its association with pathologies such as binge eating, psychological distress [11], sleep disturbances [12, 13], altered lipid profile [14] and diabetes [15].
NES is defined by evening hyperphagia (i.e., intake of ≥ 25% of total daily energy after the evening meal) and/or conscious nocturnal ingestions (i.e., eating after waking at night) occurring twice weekly or more [16]. The diagnostic criteria also include presence of distress or impairment in functioning and that nighttime eating episodes cannot be attributed to other psychiatric or medical disorders or the side effects of medication [17]. Associated features of NES include morning anorexia, frequent depressed mood and/or mood that worsens as the day progresses, insomnia, a strong desire to eat in the evening or at night, and/or the belief that one needs to eat to fall asleep [16].
In a recent survey of 1514 Swiss adults ages 18–26, the prevalence of NES was 1.3% [18]. Estimates were higher in university students, ranging from 2.9 to 5.7% among US college students [19, 20] to 9.5% among Turkish university students [21]. NES occurs equally in males and females [9, 13], but females are more likely to report the full range of NES symptoms and to experience impairment in functioning in relation to their symptoms [22]. Familial aggregation of NES has been reported [23], with an odds ratio (OR) = 4.9 for NES among first degree relatives [24].
Although the role of NES in the obesity epidemic is a concern [5, 10, 25,26,27], there is evidence that depression symptoms are positively associated with NES [11, 21, 25,26,27,28,29,30,31,32]. Compared to persons without NES, those with NES report higher levels of depression [27, 31, 33, 34] and are more likely to meet criteria for a major depression disorder (52.6% vs. 9.1%) [28]. An elevated prevalence of NES among adults diagnosed with depression is documented, ranging from 21.3 [33] to 35.2% [35]. Further, use of anti-depressants can affect hunger and satiety which may increase the risk of NE [35]. However, few studies examine the relationship between NES and depression in young people [18, 21, 36] and all studies to date are cross-sectional, so that the directionality of the association is unknown. To inform clinical management and prevention efforts, longitudinal studies distinguishing the temporality of exposure and outcome are needed.
This current study begins to address these issues. Using data from the Nicotine Dependence in Teens (NDIT) Study [37], an ongoing longitudinal investigation of grade 7 students age 12–13 years at inception in 1999–2000, we investigated the association between depression symptoms and NE both cross-sectionally and longitudinally.
Materials and methods
NDIT participants were recruited in 1999–2000 in ten Montreal-area high schools purposively selected to include English and French schools, schools in advantaged and disadvantaged neighbourhoods, and schools in rural, suburban and urban areas. Its main objective was to document the natural course of cigarette smoking in adolescents. However, data on a wide range of health, psychosocial, and behavior-related variables were also collected. Data were obtained in self-report questionnaires administered at school every 3–4 months from grade 7 to 11 (i.e., 4 data collections per grade) for a total of 20 data collections during high school. Data were also collected in self-report questionnaires twice post-high school when participants were age 20 and 24 years, on average. Body mass index (BMI) was measured at baseline (age 12–13 years) and at age 24. Parents completed mailed self-report questionnaires when participants were age 22 years on average.
Parents/guardians provided written informed consent at inception, and participants (who had attained legal age) provided consent post-high school. NDIT received ethics approval from the Montreal Department of Public Health, McGill University and the Centre de Recherche du Centre Hospitalier de l’Université de Montréal. Characteristics of NDIT participants resembled those of a provincially representative sample of same-age adolescents [38].
Study variables
Frequency of NE, a core feature of the clinical criteria for NES [16], was measured at age 24 by: “In the past month, how often did you eat snacks when you woke up at night?” (never, rarely, sometimes, often). The single item measuring NE is strongly correlated with the total NES score [39] and is sometimes used as a proxy measure for NES [30]. For analysis, participants were categorized as night-eaters (sometimes, often) or non-night-eaters (never, rarely).
Morning anorexia was measured at age 24 by: “How hungry are you in the morning?” (not at all, a little, somewhat, moderately, very). For analysis, participants were categorized as having morning anorexia (not at all hungry) or no morning anorexia (all other responses).
Evening snacking was measured at age 24 by: “In the past month, how often did you eat snacks after supper, but before bedtime.” (never, rarely, sometimes, often). For analysis, participants were categorized as snackers (sometimes, often) or non-snackers (never, rarely).
Depression symptoms were measured using two scales. During high school, adolescents completed the validated 6-item Depressive Symptoms Scale (DSS) [40, 41]. They reported how often (never; rarely; sometimes; often) in the past 3 months they: (i) felt too tired to do things; (ii) had trouble going to sleep or staying asleep; (iii) felt unhappy, sad or depressed; (iv) felt hopeless about the future; (v) felt nervous or tense; and (vi) worried too much about things. Responses were summed and divided by the number of items responded to, to yield a score that ranged from 1 to 4, with higher values indicating more frequent symptoms. Cronbach’s alpha for the DSS ranged from 0.74 at baseline to 0.89 at age 20 years. A mean DSS score during high school was obtained by taking the highest DSS score in the four data collections completed in each grade, and computing a mean of the highest scores. For descriptive analyses, scores were categorized into groups defined by tertile cut-offs (1.00–2.09; 2.10–2.69; 2.70–4.00). The DSS was used as a continuous variable in multivariate analyses.
Post-high school, depression symptoms were assessed using the Major Depression Inventory (MDI) [42], a self-report mood questionnaire developed by the World Health Organization which can yield a diagnosis of clinical depression in adults [43, 44]. Participants reported how often in the past 2 weeks they had experienced each of 12 depression symptoms, using a 6-point Likert scale ranging from 1 (“at no time”) to 6 (“all the time”). Symptoms included items such as “felt low in spirits or sad”, “felt lacking in energy and strength”, “had trouble sleeping at night or waking up too early” and “felt that life wasn’t worth living”. MDI scores range from 0 to 50, with higher scores indicating more frequent depression symptoms. The scale is validated and reliable in adults [42, 43]. In NDIT, Cronbach’s alpha for the MDI was 0.88 at age 20 and 0.90 at age 24. For descriptive analyses, MDI scores were grouped as: no or doubtful depression (MDI score < 20), mild (20–24), moderate (25–29) or severe depression (≥ 30) depression [42]. The MDI was used as a continuous variable in multivariate analyses. The correlation between the mean DSS score and the MDI at age 20 was 0.434 (p < 0.001). The correlation between the mean DSS score and the MDI at age 24 was 0.404 (p < 0.001).
Sociodemographic data including age, sex, French-speaking (yes, no), single-parent family (yes, no) and country of birth (Canada, other) were collected at baseline. Mother university-educated (yes, no, missing) was measured in both participant and parent questionnaires, and data from both questionnaires were used to reduce missing data.
Height and weight were measured by trained technicians. If there was a discrepancy between duplicate measures (i.e., > 0.5 cm for height; > 0.5 lbs for weight), a third measure was taken. The mean was calculated using the two (closest) measures. BMI was computed as weight divided by height squared (kg/m2).
Past-month use of anti-depressants was measured at ages 20 and 24 by “In the past month, did you take any of the following medication, either prescription or over-the-counter…anti-depressants (Prozac, Paxil, Effexor)” (yes, no).
Data analysis
The analytical sample comprised participants (n = 829, 64% of 1294) with data on NE and depression symptoms. Potential confounders of the association of interest were identified in the literature [45,46,47] as variables related to both depression and NES (but likely not on the causal pathway), and included sex, age and mother university-educated as a proxy for family SES [48,49,50]. Although sex is associated with depression [51, 52], the literature suggests that there is no association between sex and NES [9]. However, more males than females in NDIT reported NE and sex is therefore considered a potential confounder. Obesity is a risk factor for depression [53], but not for NES, at least in young people [10, 13, 25, 54] and was not considered a potential confounder.
The association between depression symptoms and NES was investigated in three multivariate logistic regression models controlling for potential confounders. First, we studied the association in a cross-sectional design using exposure and outcome data collected contemporaneously at age 24. We then undertook two analyses using a longitudinal design. First we investigated the association between DSS depressive symptoms measured during high school and NE measured at age 24. Second we investigated MDI depression symptoms measured at age 20, and NE measured at age 24. Mixed models could not be estimated because NES was measured only once. Therefore, we needed to summarize depression histories to include them as the exposure in the regression model with NES as the outcome.
We examined a depressive symptoms by sex interaction term in each model. The interaction term was significant in the longitudinal model using MDI data at age 20 (p = 0.023) only. Because this could be a chance finding, we did not consider sex interaction further. Similarly, none of the interaction terms for age by depression symptoms were significant.
Because there were few missing data (Online Resource A), the analyses were undertaken using participants with complete data only. All analyses were conducted using SPSS software, Version 24.0 (IBM Corp., Armonk, NY).
Results
Table 1 compares characteristics of the 829 participants retained for analyses with those of the 465 participants not retained because of loss to follow-up (n = 195), refusal to continue to participate (n = 241), or missing data on NE (n = 29). Those not retained were older, a higher proportion was male, lower proportions had university-educated mothers and were born in Canada, and mean BMI was higher than among those retained. Mean DSS scores were lower, although there were no significant differences in MDI scores.
Overall, 9% of 829 participants (n = 77) reported NE in the past month. To assess features associated with NES [16], we compared the distribution of snacking after supper and morning anorexia in night-eaters and non-night-eaters. Compared to 70% of non-night-eaters, 92% of night-eaters reported snacking sometimes/often after supper, but before bedtime (p ≤ 0.001); and 22% of night-eaters reported morning anorexia, compared to 17% of non-night-eaters (p = 0.214).
In contrast to the literature, more night-eaters than non-night-eaters in NDIT were male (Table 2). However, night-eaters did not differ in other sociodemographic characteristics or in BMI at baseline or at age 24.
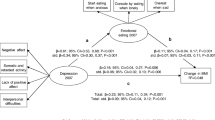
Table 3 presents descriptive data and unadjusted and adjusted estimates of the association between the depression indicators and NE. In cross-sectional analyses, the adjusted model suggested a 4% increase in the odds of NE with each unit increase in MDI scores (range 0–50). In longitudinal analyses, the adjusted model suggested a 75% increase in the odds of NE with each unit increase in the DSS (range 1–4). Finally, the adjusted OR estimate in the longitudinal analysis suggested a 3% increase in the odds of NE with each unit increase in the MDI (measured 4 years earlier).
We undertook three sensitivity analyses. First, we excluded participants taking anti-depressants (n = 16 and 30 at age 20 and 24, respectively), with little difference in the OR estimates (Online Resource B). Second, we removed items measuring sleep disturbances from the depression indicators (Online Resource C). The results for the MDI in both cross-sectionl and longitudinal analyses were unchanged. The adjusted OR estimates for mean DSS scores were attenuated, but the confidence interval for the adjusted estimate excluded 1. Finally, we repeated the analyses using only the sleep items from the depression indicators as the exposure (Online Resource D). The MDI and DSS sleep items were associated with NE in the adjusted models. The OR estimates are not comparable to the OR estimates in the primary analyses, since the sleep items in the MDI ranged from 0 to 5; and the sleep item in the DSS score had four categories (never, rarely, sometimes, often).
Discussion
Interest in NES has increased because of the obesity epidemic and concerns that it may signal psychological distress. Although the prevalence ranges from 1 to 1.6% in the general population [55, 56], 9% of young adults in NDIT reported NE occasionally or frequently. This concurs with the prevalence of NES in studies of college students [13, 19,20,21], suggestive that our NE indicator was meaningful. Further, and concordant with our hypothesis, depression symptoms were associated with NE in young adults cross-sectionally and possibly longitudinally, as well as using different indicators of depression symptoms.
The relationship between depression symptoms and NES is well-documented in cross-sectional studies [18, 19, 21, 57, 58], which note that, because of the cross-sectional design, it remains uncertain whether depressed mood is a (causal) risk factor for NES or a clinical feature [9, 55, 59]. Longitudinal evidence can help establish the temporality of the exposure outcome association such that inferences about causality are stronger than in cross-sectional analysis. Our study helps address this uncertainty by demonstrating that depression symptoms measured in adolescence are associated with NE in young adulthood. Although we did not measure age of NE onset, when it occurs as a symptom of NES, NE typically begins in early adulthood [3, 9]. It is plausible that depression symptoms measured during adolescence in NDIT preceded the onset of NE.
Different levels of severity of mood disruption have been reported in night-eaters with depression [9]. One type comprises a unique circadian pattern wherein mood worsens during the evening and night [4]. This contrasts with major depression disorder in which mood usually improves throughout the day [60, 61]. Worsening mood during the evening and night may result from food restriction during the day [9], or since NE is prominent in periods of high stress and weight gain [4], it may reflect frustration over nocturnal hyperphagia and/or weight gain [9]. Research on the pathophysiology of NES suggests that the serotonin system plays a major role in regulating appetite and food intake, and could be one mechanistic underpinning [3, 62]. Higher levels of serotonin transporter (SERT) in the brains of persons with NES might lead to increased reuptake of serotonin [63]. The resultant impaired post-synaptic serotonin transmission leads to delayed circadian rhythms and decreased satiety, thereby increasing the risk of NES [3]. Several clinical trials [64,65,66,67] have focused on blocking SERT with antidepressant medication (i.e., selective serotonin reuptake inhibitors (SSRIs)) and have reported decreases in NES symptoms. However, these improvements appear to be independent of the effect of the drug on mood [61], suggesting that depression could contribute to the development of NES [59]. Overall, researchers suggest that the relationship between depression and NE is complex and likely also involves obesity/overweight and impaired sleep, although how these variables inter-relate is not yet understood [33, 60, 61].
Sleep disturbances are important risk factors for NE, but again whether the association is causal or bidirectional is unknown [33]. It is possible that disturbed sleep among individuals suffering from depression increases nocturnal snacking [35]. In our study, the longitudinal relationship between depression symptoms measured with the DSS and NE was attenuated when sleep items were removed from the depression scales, and the sleep items themselves were independently associated with NE. Overall, caution is needed in interpreting the associations observed in this study until further research clarifies the specific roles of each of obesity, sleep disturbances and depression in NE. It may be important to empirically test alternative directed acyclic graphs of these relationships and examine the causal links between these variables.
Limitations of this analysis include that self-report data are subject to misclassification. NE was measured using a single item. However, this item is strongly correlated with the NEQ score [39] and is likely a good proxy for NES. Also, the prevalence of NE in NDIT (9%) is similar to that reported in other student populations [19,20,21], suggestive that it is a reliable proxy for NES. Misclassification of NE may have attenuated the observed estimates (i.e., NE may be more normative in young adults and participants who reported NE may not have had pathological NES). Our NE measure did not incorporate frequency of NE, type or amount of food consumed, or whether NE is related to an underlying medical condition such as diabetes or sleep apnea. We selected to use the highest DSS score in each grade because these values could represent worrisome departures from the usual pattern of depression symptoms, and then we averaged the highest scores across grade to capture consistent patterns of these departures over time. This likely resulted in a loss of information. However, suggestive that this was not a critical issue, the confidence intervals generally excluded 1, and the results were robust across sensitivity analyses. In addition, the intraclass correlation coefficient across cycles was 0.59, indicating that depression symptoms scores were moderately correlated within individuals across adolescence. Selection bias related to loss-to-follow-up may have affected the estimates and use of a purposive sample could limit generalizability. Because we did not collect data on age at which NE began, the temporality between depression symptoms and NE remains uncertain. However, we began collecting DSS data in early adolescence and NE generally begins in late adolescence to the late 20s [3, 9, 10].
Conclusion
In NDIT, 9% of young adults reported NE in the past month, a behavior that could signal NES. Depression symptoms, even at an early age, are associated with NE cross-sectionally and possibly longitudinally in young adulthood. Research is needed to discern whether the relationship is bidirectional, whether depression is a clinical feature of NES, and whether the relationship between depression and NES is confounded or mediated by BMI or weight perception. When the mechanistic underpinnings of the association are better understood, treatment of depression symptoms in adolescence could be key in preventing the NE that is a core feature of NES.
Data availability
Data are available on request. To gain access, applicants must complete a data request form available on the NDIT website (www.nditstudy.ca) and return it to the principal investigator (jennifer.oloughlin@umontreal.ca). The procedure to obtain access to NDIT data is described in O’Loughlin, J., Dugas, E.N., Brunet, J., DiFranza, J., Engert, J.C., Gervais, A., Gray-Donald, K., Karp, I., Low, N.C., Sabiston, C., Sylvestre, M.P., Tyndale, R.F., Auger, N., Belanger, M., Barnett, T., Chaiton, M., Chenoweth, M.J., Constantin, E., Contreras, G., Kakinami, L., Labbe, A., Maximova, K., McMillan, E., O’Loughlin, E.K., Pabayo, R., Roy-Gagnon, M.H., Tremblay, M., Wellman, R.J., Hulst, A., Paradis, G., 2015. Cohort Profile: The Nicotine Dependence in Teens (NDIT) Study. Int J Epidemiol. 44(5), 1537–1546. https://doi.org/10.1093/ije/dyu135. The relevant paragraph is described below. This process has been approved by the ethics committee at the CRCHUM. Access to NDIT data is open to any university-appointed or affiliated investigator upon successful completion of the application process. Masters, doctoral and postdoctoral students may apply through their primary supervisor. For more information, visit www.nditstudy.ca or contact the principal investigator.
Abbreviations
- BMI:
-
Body mass index
- CI:
-
Confidence interval
- DSS:
-
Depressive Symptoms Scale
- MDI:
-
Major Depression Inventory
- NDIT Study:
-
Nicotine Dependence in Teens Study
- NE:
-
Night eating
- NES:
-
Night Eating Syndrome
- NEQ:
-
Night Eating Questionnaire
- OR:
-
Odds ratio
- ORadj :
-
Adjusted odds ratio
- SD:
-
Standard deviation
- SERT:
-
Serotonin transporter
- SSRI:
-
Selective serotonin reuptake inhibitor
References
Neumark-Sztainer D, Wall M, Larson NI et al (2011) Dieting and disordered eating behaviors from adolescence to young adulthood: findings from a 10-year longitudinal study. J Am Diet Assoc 111(7):1004–1011. https://doi.org/10.1016/j.jada.2011.04.012
Nurkkala M, Keränen AM, Koivumaa-Honkanen H et al (2016) Disordered eating behavior, health and motives to exercise in young men: cross-sectional population-based MOPO study. BMC Public Health 16:483. https://doi.org/10.1186/s12889-016-3162-2
McCuen-Wurst C, Ruggieri M, Allison KC (2018) Disordered eating and obesity: associations between binge-eating disorder, night-eating syndrome, and weight-related comorbidities. Ann N Y Acad Sci 1411(1):96–105. https://doi.org/10.1111/nyas.13467
Stunkard AJ, Grace WJ, Wolff HG (1955) The night-eating syndrome: a pattern of food intake among certain obese patients. Am J Med 19(1):78–86. https://doi.org/10.1016/0002-9343(55)90276-X
Gallant AR, Lundgren J, Drapeau V (2012) The night-eating syndrome and obesity. Obes Rev 13(6):528–536. https://doi.org/10.1111/j.1467-789X.2011.00975.x
Chaput JP, Dutil C (2016) Lack of sleep as a contributor to obesity in adolescents: impacts on eating and activity behaviors. Int J Behav Nutr Phys Act 13(1):103. https://doi.org/10.1186/s12966-016-0428-0
Gariepy G, Nitka D, Schmitz N (2010) The association between obesity and anxiety disorders in the population: a systematic review and meta-analysis. Int J Obes (Lond) 34(3):407–419. https://doi.org/10.1038/ijo.2009.252
Luppino FS, de Wit LM, Bouvy PF et al (2010) Overweight, obesity, and depression: a systematic review and meta-analysis of longitudinal studies. Arch Gen Psychiatry 67(3):220–229. https://doi.org/10.1001/archgenpsychiatry.2010.2
Vander Wal JS (2012) Night eating syndrome: a critical review of the literature. Clin Psychol Rev 32(1):49–59. https://doi.org/10.1016/j.cpr.2011.11.001
Bruzas MB, Allison KC (2019) A review of the relationship between night eating syndrome and body mass index. Curr Obes Rep 8(2):145–155. https://doi.org/10.1007/s13679-019-00331-7
Colles SL, Dixon JB, O’brien PE (2007) Night eating syndrome and nocturnal snacking: association with obesity, binge eating and psychological distress. Int J Obes (Lond) 31(11):1722–1730. https://doi.org/10.1038/sj.ijo.0803664
Rogers NL, Dinges DF, Allison KC et al (2006) Assessment of sleep in women with night eating syndrome. Sleep 29(6):814–819. https://doi.org/10.1093/sleep/29.6.814
Yahia N, Brown C, Potter S et al (2017) Night eating syndrome and its association with weight status, physical activity, eating habits, smoking status, and sleep patterns among college students. Eat Weight Disord 22(3):421–433. https://doi.org/10.1007/s40519-017-0403-z
Gallant A, Lundgren J, Drapeau V (2014) Nutritional aspects of late eating and night eating. Curr Obes Rep 3(1):101–107. https://doi.org/10.1007/s13679-013-0081-8
Morse SA, Ciechanowski PS, Katon WJ et al (2006) Isn’t this just bedtime snacking?: the potential adverse effects of night-eating symptoms on treatment adherence and outcomes in patients with diabetes. Diabetes Care 29(8):1800–1804. https://doi.org/10.2337/dc06-0315
Allison KC, Lundgren JD, O’Reardon JP et al (2010) Proposed diagnostic criteria for night eating syndrome. Int J Eat Disord 43(3):241–247. https://doi.org/10.1002/eat.20693
American Psychiatric Association (2013) Diagnostic and statistical manual of mental disorders, 5th edn. American Psychiatric Association, Arlington, VA
Fischer S, Meyer AH, Hermann E et al (2012) Night eating syndrome in young adults: delineation from other eating disorders and clinical significance. Psychiatry Res 200(2–3):494–501. https://doi.org/10.1016/j.psychres.2012.07.028
Runfola CD, Allison KC, Hardy KK et al (2014) Prevalence and clinical significance of night eating syndrome in university students. J Adolesc Health 55(1):41–48. https://doi.org/10.1016/j.jadohealth.2013.11.012
Nolan LJ, Geliebter A (2012) Night eating is associated with emotional and external eating in college students. Eat Behav 13(3):202–206. https://doi.org/10.1016/j.eatbeh.2012.02.002
Sevincer GM, Ince E, Taymur I et al (2016) Night eating syndrome frequency in university students: association with impulsivity, depression, and anxiety. Bull Clin Psychpharmacol 26(3):238–247. https://doi.org/10.5455/bcp.20160322093750
Allison KC, Lundgren JD, Stunkard AJ et al (2014) Validation of screening questions and symptom coherence of night eating in the Swedish Twin Registry. Compr Psychiatry 55(3):579–587. https://doi.org/10.1016/j.comppsych.2013.01.006
Lundgren JD, Drapeau V, Allison KC et al (2012) Prevalence and familial patterns of night eating in the Québec Adipose and Lifestyle Investigation in Youth (QUALITY) study. Obesity (Silver Spring) 20(8):1598–1603. https://doi.org/10.1038/oby.2012.80
Lundgren JD, Allison KC, Stunkard AJ (2006) Familial aggregation in the night eating syndrome. Int J Eat Disord 39(6):516–518. https://doi.org/10.1002/eat.20269
Marshall HM, Allison KC, O’Reardon JP et al (2004) Night eating syndrome among nonobese persons. Int J Eat Disord 35(2):217–222. https://doi.org/10.1002/eat.10241
de Zwaan M, Roerig DB, Crosby RD et al (2006) Nighttime eating: a descriptive study. Int J Eat Disord 39(3):224–232. https://doi.org/10.1002/eat.20246
Gluck ME, Geliebter A, Satov T (2001) Night eating syndrome is associated with depression, low self-esteem, reduced daytime hunger, and less weight loss in obese outpatients. Obes Res 9(4):264–267. https://doi.org/10.1038/oby.2001.31
Lundgren JD, Allison KC, O’Reardon JP et al (2008) A descriptive study of non-obese persons with night eating syndrome and a weight-matched comparison group. Eat Behav 9(3):343–351. https://doi.org/10.1016/j.eatbeh.2007.12.004
Birketvedt GS, Florholmen J, Sundsfjord J et al (1999) Behavioral and neuroendocrine characteristics of the night-eating syndrome. JAMA 282(7):657–663. https://doi.org/10.1001/jama.282.7.657
Striegel-Moore RH, Rosselli F, Wilson GT et al (2010) Nocturnal eating: association with binge eating, obesity, and psychological distress. Int J Eat Disord 43(6):520–526. https://doi.org/10.1002/eat.20735
Allison KC, Ahima RS, O’Reardon JP et al (2005) Neuroendocrine profiles associated with energy intake, sleep, and stress in the night eating syndrome. J Clin Endocrinol Metab 90(11):6214–6217. https://doi.org/10.1210/jc.2005-1018
Lundgren JD, Allison KC, Crow S et al (2006) Prevalence of the night eating syndrome in a psychiatric population. Am J Psychiatry 163(1):156–158. https://doi.org/10.1176/appi.ajp.163.1.156
Kucukgoncu S, Tek C, Bestepe E et al (2014) Clinical features of night eating syndrome among depressed patients. Eur Eat Disord Rev 22(2):102–108. https://doi.org/10.1002/erv.2280
Grave RD, Calugi S, Ruocco A et al (2011) Night eating syndrome and weight loss outcome in obese patients. Int J Eat Disord 44(2):150–156. https://doi.org/10.1002/eat.20786
Orhan FÖ, Özer UG, Özer A et al (2011) Night eating syndrome among patients with depression. Isr J Psychiatry Relat Sci 48(3):212–217
Thompson SH, DeBate RD (2009) An exploratory study of the relationship between night eating syndrome and depression among college students. J College Stud Psychother 24(1):39–48. https://doi.org/10.1080/87568220903400161
O’Loughlin J, Dugas EN, Brunet J et al (2015) Cohort profile: the Nicotine Dependence in Teens (NDIT) study. Int J Epidemiol 44(5):1537–1546. https://doi.org/10.1093/ije/dyu135
Paradis G, Lambert M, O’Loughlin J et al (2003) The Québec Child and Adolescent Health and Social Survey: design and methods of a cardiovascular risk factor survey for youth. Can J Cardiol 19(5):523–531
Allison KC, Lundgren JD, O’Reardon JP et al (2008) The night eating questionnaire (NEQ): psychometric properties of a measure of severity of the night eating syndrome. Eat Behav 9(1):62–72. https://doi.org/10.1016/j.eatbeh.2007.03.007
Kandel DB, Davies M (1982) Epidemiology of depressive mood in adolescents: an empirical study. Arch Gen Psychiatry 39(10):1205–1212. https://doi.org/10.1001/archpsyc.1982.04290100065011
Choi WS, Patten C, Gillin CJ et al (1997) Cigarette smoking predicts development of depressive symptoms among US adolescents. Ann Beh Med 19:42–50. https://doi.org/10.1007/BF02883426
Bech P, Stage KB, Nair NP et al (1997) The major depression rating scale (MDS) Inter-rater reliability and validity across different settings in randomized moclobemide trials. J Affect Disord 42(1):39–48. https://doi.org/10.1016/S0165-0327(96)00094-8
Bech P, Rasmussen NA, Olsen LR et al (2001) The sensitivity and specificity of the major depression inventory, using the present state examination as the index of diagnostic validity. J Affect Disord 66(2–3):159–164. https://doi.org/10.1016/S0165-0327(00)00309-8
Olsen LR, Jensen DV, Noerholm V et al (2003) The internal and external validity of the major depression inventory in measuring severity of depressive states. Psychol Med 33(2):351–356. https://doi.org/10.1017/S0033291702006724
Kim OS, Kim MS, Lee JE et al (2016) Night-eating syndrome and the severity of self-reported depressive symptoms from the Korea Nurses’ Health Study: analysis of propensity score matching and ordinal regression. Public Health 141:80–87. https://doi.org/10.1016/j.puhe.2016.08.018
Lundgren JD, Allison KC, Stunkard AJ et al (2012) Lifetime medical and psychiatric comorbidity of night eating behavior in the Swedish Twin Study of Adults: genes and Environment (STAGE). Psychiatry Res 199(2):145–149. https://doi.org/10.1016/j.psychres.2012.04.010
Striegel-Moore RH, Franko DL, Thompson D et al (2006) Night eating: prevalence and demographic correlates. Obesity 14(1):139–147. https://doi.org/10.1038/oby.2006.17
Ritsher JE, Warner V, Johnson JG et al (2001) Inter-generational longitudinal study of social class and depression: a test of social causation and social selection models. Br J Psychiatry Suppl 178(S40):s84–s90. https://doi.org/10.1192/bjp.178.40.s84
Nevonen L, Norring C (2004) Socio-economic variables and eating disorders: a comparison between patients and normal controls. Eat Weight Disord 9(4):279–284. https://doi.org/10.1007/BF03325082
Rogers L, Resnick MD, Mitchell JE et al (1997) The relationship between socioeconomic status and eating-disordered behaviors in a community sample of adolescent girls. Int J Eat Disord 22(1):15–23. https://doi.org/10.1002/(SICI)1098-108X(199707)22:1%3c15:AID-EAT2%3e3.0.CO;2-5
Weissman MM, Klerman GL (1997) Sex differences and the epidemiology of depression. Arch Gen Psychiatry 34(1):98–111. https://doi.org/10.1001/archpsyc.1977.01770130100011
McGuinness TM, Dyer JG, Wade EH (2012) Gender differences in adolescent depression. J Psychosoc Nurs Ment Health Serv 50(12):17–20. https://doi.org/10.3928/02793695-20121107-04
Faith MS, Butryn M, Wadden TA et al (2011) Evidence for prospective associations among depression and obesity in population-based studies. Obes Rev 12(5):e438–e453. https://doi.org/10.1111/j.1467-789X.2010.00843.x
Meule A, Allison KC, Brähler E et al (2014) The association between night eating and body mass depends on age. Eat Behav 15(4):683–685. https://doi.org/10.1016/j.eatbeh.2014.10.003
de Zwaan M, Müller A, Allison KC et al (2014) Prevalence and correlates of night eating in the German general population. PLoS One 9(5):e97667. https://doi.org/10.1371/journal.pone.0097667
Striegel-Moore RH, Dohm FA, Hook JM et al (2005) Night eating syndrome in young adult women: prevalence and correlates. Int J Eat Disord 37(3):200–206. https://doi.org/10.1002/eat.20128
Striegel-Moore RH, Franko DL, Thompson D et al (2008) Exploring the typology of night eating syndrome. Int J Eat Disord 41(5):411–418. https://doi.org/10.1002/eat.20514
Nolan LJ, Geliebter A (2017) Validation of the night eating diagnostic questionnaire (NEDQ) and its relationship with depression, sleep quality, “food addiction”, and body mass index. Appetite 111:86–95. https://doi.org/10.1016/j.appet.2016.12.027
Vinai P, Allison KC, Cardetti S et al (2008) Psychopathology and treatment of night eating syndrome: a review. Eat Weight Disord 13(2):54–63. https://doi.org/10.1007/BF03327604
Cleator J, Abbott J, Judd P et al (2012) Night eating syndrome: implications for severe obesity. Nutr Diabetes 2(9):e44. https://doi.org/10.1038/nutd.2012.16
Stunkard AJ, Allison KC (2003) Two forms of disordered eating in obesity: binge eating and night eating. Int J Obes Relat Metab Disord 27(1):1–12. https://doi.org/10.1038/sj.ijo.0802186
Stunkard AJ, Allison KC, Lundgren JD et al (2009) A biobehavioural model of the night eating syndrome. Obes Rev 10(Suppl 2):69–77. https://doi.org/10.1111/j.1467-789X.2009.00668.x
Lundgren JD, Newberg AB, Allison KC et al (2008) 123I-ADAM SPECT imaging of serotonin transporter binding in patients with night eating syndrome. Psychiatry Res 162(3):214–220. https://doi.org/10.1016/j.pscychresns.2007.07.006
O’Reardon JP, Stunkard AJ, Allison KC (2004) Clinical trial of sertraline in the treatment of night eating syndrome. Int J Eat Disord 35(1):16–26. https://doi.org/10.1002/eat.10224
O’Reardon JP, Allison KC, Martino NS et al (2006) A randomized, placebo-controlled trial of sertraline in the treatment of night eating syndrome. Am J Psychiatry 163(5):893–898. https://doi.org/10.1176/ajp.2006.163.5.893
Stunkard AJ, Allison KC, Lundgren JD et al (2006) A paradigm for facilitating pharmacotherapy at a distance: sertraline treatment of the night eating syndrome. J Clin Psychiatry 67(10):1568–1572. https://doi.org/10.4088/JCP.v67n1011
Allison KC, Studt SK, Berkowitz RI et al (2013) An open-label efficacy trial of escitalopram for night eating syndrome. Eat Behav 14(2):199–203. https://doi.org/10.1016/j.eatbeh.2013.02.001
Acknowledgements
Jennifer O’Loughlin holds a Canada Research Chair in the Early Determinants of Adult Chronic Disease. The authors thank the NDIT Study participants.
Funding
This study was supported by the Canadian Cancer Society Research Institute grants (grant numbers 010271, 017435, 704031). Views expressed in this document do not necessarily reflect those of the funding agency. The funders were not involved in the design or conduct of the study, data collection, management, analysis, or interpretation, or preparation, review or approval of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of topical collection on Sleep and Eating and Weight disorders.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Guentcheva, I., Dugas, E.N., Hanusaik, N. et al. Depression symptoms and night eating in young adulthood. Eat Weight Disord 25, 1593–1600 (2020). https://doi.org/10.1007/s40519-019-00796-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-019-00796-4