Abstract
Purpose of Review
Transoral robotic thyroidectomy (TORT) is one of the latest approaches in remote-access thyroid surgery. This review presents the current indications for TORT, an in-depth description of the surgical procedure, and discusses the advantages, disadvantages, potential complications, and latest advances for this procedure.
Recent Findings
TORT has the advantages of excellent cosmesis, short distance from oral vestibule to the neck, and midline approach which allows easy access to bilateral thyroid glands and central compartment. In addition, the use of robotic arms ensures wristed instruments, tremor elimination, and reduced clashing of instruments with endoscope. Complication rates are low; however, the use of robotic systems is costly and there may be a steep learning curve.
Summary
TORT can be performed safely with careful patient selection and with an experienced robotic surgeon and it is an acceptable alternative for the treatment of certain thyroid conditions.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Conventional open thyroidectomy with a cervical incision has always been the gold standard for the management of a multitude of thyroid diseases. However, with the increase in demand for cosmesis in the young female-predominant population and also the concern of the impact of a visible cervical scar on quality of life [1, 2], there has been a quest for alternative surgical approaches that can cater to these concerns and hence the birth of remote-access thyroid surgery.
Remote-access thyroid surgery has been gaining popularity over the past decade. In order to avoid the need for a cervical scar, several approaches have been developed. The transoral approach is the latest approach and has been gaining steady popularity in recent years. This approach has the advantages of a shorter distance from the oral vestibule to the neck, which reduces the amount of tissue dissection, a midline approach which allows easy access to bilateral thyroid glands and central compartment, and remote incisions, which are made in the mucosa of the lower lip, eliminating any cutaneous scarring over the head and neck [1].
The development of transoral robotic thyroidectomy (TORT) has further added advantages such as a high-definition three-dimensional view, wristed instruments, tremor elimination, and reduced clashing of instruments, [4].
Currently our centre is one of the leading international centres specialized in TORT and holds the highest number of publications regarding this technique. We herein present this review of our experience.
History
Several endoscopic and remote-access approaches to the thyroid have been introduced to try to minimize the need for a cervical scar. These include the bilateral axillary breast approach [5], axillo-breast approach [6], lateral neck approach [7], and post-auricular axillary approach [8].
With the advancement in technology, the Da Vinci robotic system (Intuitive Surgical, Sunnyvale, California) was adapted to remote-access thyroid surgery and has been successful in the transaxillary approach [9], retroauricular approach [10], and transoral approach [11].
The transoral approach is the latest approach for remote-access thyroid surgery. Transoral endoscopic thyroidectomy was first described by Witzel et al. in 2008 [12, 13]. In 2010, the Da Vinci robot was adopted to this approach by Richmon et al. where the central endoscope was passed via a sublingual incision and the two lateral arms were passed via vestibular incisions made anterior to the mandible [14]. However, the sublingual approach was unattractive as there was restricted camera movement and also there were reports of high complication rates. In 2011, Richmon et al. modified this approach by placing all three ports via the vestibule anterior to the mandible to avoid the floor of the mouth and this resulted in excellent visibility of the central cavity and mobility of instruments [11]. However surgical outcomes were still unsatisfactory when compared to the open conventional thyroidectomy, with incidences of transient and permanent recurrent laryngeal nerve palsy rates of 25% and 13%, respectively. Subsequently, a study in 2016 by Anuwong et al. that included 60 patients undergoing endoscopic transoral thyroidectomy showed promising results, in which there were no instances of permanent hoarseness, mental neve injury, or infection [15].
Our initial experience with TORT on four human patients was published in 2015 [12]. Though all surgeries were successful, three patients developed temporary mental nerve palsy with paraesthesia over the chin or lower lip. This was due to the placement of the trocars close to the emergence of the mental nerves, causing nerve injury during surgery. Since then we have continually modified and refined our surgical techniques and procedures with much success to demonstrate that TORT is indeed feasible in a wide range of patients.
Indications for Surgery
Inclusion criteria for TORT includes the following: [16, 17]
Benign or atypical thyroid nodules, preferably less than 6 cm
Follicular neoplasms, preferably less than 6 cm
Malignant or suspicious malignant nodules, preferably less than 4 cm
Exclusion criteria for TORT includes the following: [16, 17]
Patients with extensive lymph node metastasis in lateral cervical compartment on preoperative ultrasound or computed tomography
History of neck radiation
History of neck surgery
According to the American Thyroid Association guidelines, lobectomy or total thyroidectomy is recommended for patients with papillary thyroid carcinoma (PTC) of 1–4 cm; however, prophylactic central neck dissection (CND), ipsilateral or bilateral, is only recommended for patients with advanced primary tumours (T3 or T4) or clinically involved lateral neck lymph nodules (cN1b) [••18]. At our institution, we routinely perform prophylactic ipsilateral CND for lobectomy cases and bilateral CND for total thyroidectomy cases because in TORT the cranial-caudal view allows for easy access and dissection of the central compartment and it is not technically difficult [16]. In addition, the prophylactic CND may reduce the need for reoperation which may be difficult and dangerous.
There is no limitation on the age or the gender of the patient when performing TORT. However, with the increasing popularity of TORT worldwide, there has been concerns on whether obesity would affect the technical difficulty or outcomes of TORT. Russell et al. performed a prospective study on 14 cases that underwent either endoscopic or robotic transoral thyroidectomy and/or parathyroidectomy and concluded that this approach did not appear to be limited by obesity as they were able to successfully operate on patients with BMI as high as 44 kg/m2 [19]. We have also addressed this issue by performing a subset analysis of 304 patients in our hospital that underwent TORT. We compared the surgical outcomes of patients with BMI < 30 kg/m2 and BMI ≥ 30 kg/m2. It was found that there were no statistically significant differences between the two groups in terms of operative time, length of stay, pain score, or postoperative complications. Although there were limitations to this study, such as the small number of obese patients relative to the non-obese patients and the need for a longer follow-up time to evaluate oncological outcomes, the results of this study showed that obesity did not appear to affect the technical difficulty or surgical outcomes of TORT [•20].
Operative Procedures and Preparation
Preoperative Preparation
A preoperative ultrasound and computed tomography (CT) is performed for all patients to evaluate the size and location of the thyroid nodule or tumour, lymph node status, and potential blood vessels that may be injured during dissection. The CT scan is also beneficial in the detection of aberrant subclavian artery suggesting the presence of non-recurrent laryngeal nerve [16]. Indirect laryngoscopy is performed to evaluate the vocal cord status. Patients with oral hygiene issues may be referred to a dentist before surgery. A single dosage of prophylactic antibiotic (cefazedone 1 g) is administered before surgery [16].
Surgical Procedure
The patient is intubated with an electromyogram tube (Medtronic, Minneapolis, Minnesota) that can enable intraoperative nerve monitoring. The patient’s neck is placed in a slightly extended position. The oral cavity is irrigated with chlorhexidine and povidone-iodine solution after draping [16].
Incision and Flap Creation
10 ml epinephrine-saline solution diluted to a ratio of 1:200,000 is injected via the lower lip down to the tip of the chin. An inverted U-shaped 1 cm incision is made at the midline of the lower lip 2 cm above the frenulum and another two 0.5 cm incisions are made at the lateral angles of the mouth.
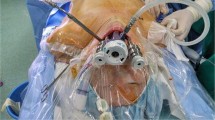
Blunt dissection is performed via the midline incision with mosquito and Kelly forceps past the mandible to the neck. A vascular tunneler is used to further create the tunnel to the level of the cricoid cartilage. A midline trocar (8 mm for da Vinci Xi and 12 mm for da Vinci Si) is inserted with carbon dioxide (CO2) insufflation at a pressure of 5-7 mmHg. Blunt dissection is performed for the lateral ports and trocars are subsequently inserted (Fig. 1). 8 mm ports are used for da Vinci Xi and 5 mm ports for da Vinci Si [3, 16].
Further dissection of the platysmal flap is performed using ultrasonic energy device (Harmonic Ace + , Ethion Endo-Surgery, Cincinnati, Ohio) inferiorly to the level of the sternal notch and laterally to the sternocleidomastoid muscles [16].
A 1 cm incision is made at the right axillary fold and an 8 mm trocar is inserted to facilitate traction of the thyroid gland and drain insertion after the operation [16].
Patient Positioning and Docking
TORT can be performed using both the da Vinci Si and da Vinci Xi systems (Intuitive Surgical, Sunnydale, CA).
For the da Vinci Si system, the patient is placed in lithotomy position with the reversed Trendelenberg status of 15 degrees, and the robot is docked at the midline between the patient’s legs. For the da Vinci Xi system, the patient is placed in supine position with the reversed Trendelenberg status of 15 degrees, and the robot is docked left lateral to the patient with the boom laser point targeted to 1 cm right lateral to the cricoid cartilage [3].
Once the robotic arms are docked to the ports, the endoscope is placed in the midline cannula (30-degree scope). Harmonic scalpel is inserted via the right port and the Maryland bipolar forcep is inserted into the left port. The Prograsp bipolar forcep is placed via the axillary port [16].
Console Stage
After the midline raphe is opened, the thyroid is exposed and the pyramidal lobe and Delphian lymph nodes are dissected free and removed. Isthmusectomy is subsequently performed. The strap muscles are dissected away from the thyroid lobe. The sternothyroid muscle is retracted and the superior pole vessels are divided individually with ultrasonic curved shears. The superior pole parathyroid gland is identified and dissected away from the thyroid. The thyroid lobe is then retracted contralaterally and anteriorly and the recurrent laryngeal nerve is identified around cricoid articulation where the nerve inserts. Intraoperative nerve monitoring is used to confirm the course and the integrity of the recurrent laryngeal nerve. Lobectomy is completed whilst safeguarding the recurrent laryngeal nerve and the inferior parathyroid glands. For total thyroidectomy, the same procedure is performed on the contralateral lobe.
Central compartment lymph node dissection can be performed and retrieved en bloc with the resected thyroid lobe.
The specimen is retrieved using an endo-plastic bag via the right axilla port. Hemostasis is ascertained and a Jackson-Pratt drain is placed in the thyroid bed. Strap muscles are re-opposed with self-locking absorbable sutures. All incisions are closed with a single layer of absorbable sutures [3, 16, •20].
Postoperative Management
Compression dressing is applied to the submandibular area for 12 h. Patients are allowed sips of water, and then soft diet, 4 h after the operation. The drain is usually removed on postoperative day 1 or 2 depending on the output. Patients are usually discharged on postoperative day 2 and are followed up on the second week in the outpatient clinic [•20].
Advantages of TORT
Cosmesis
Cosmesis is excellent as the incisions are made in the mucosa of the lower lip which heal within 2–3 weeks and hence leaves no cutaneous scarring over the head or neck, thus making it truly scarless. The small axillar scar in the skin fold becomes indistinct and is never complained of [4, • 21].
Surgical Efficacy
The transoral approach has several advantages compared to other remote-access approaches. The distance from the oral vestibule to the neck is short, which minimizes the amount of tissue dissection required [4, 22, 23]. This may result in the accentuation of potential benefits of minimally invasive surgery, which are decreased postoperative pain, decreased need for analgesics, faster recovery, and shorter hospital stay [4]. Secondly the cranial-caudal approach allows easy access to bilateral thyroid glands, bilateral parathyroid glands, and central compartment, and also allows easy identification of the bilateral laryngeal nerves which facilitates total thyroidectomy when necessary [4, 16, 24]. Central compartment dissection has been proven to be safe and technically feasible [24].
Though both TOETVA and TORT can be used to perform the same operation, there are definite limitations of the endoscopic approach. Endoscopic instruments used in TOETVA are rigid. Hence only linear movements can be performed. The two-dimensional endoscope is held by an assistant surgeon, which can make visualization of the surgical field difficult to control. In addition, TOETVA cannot cancel out any natural tremors that the surgeon may have during the operation [4]. Another limitation is that the specimen is usually removed via the midline intraoral incision. If the specimen is larger or hard in consistency, there is a chance that retrieval will be difficult and result in fragmentation of the specimen which increases the risk of tumour spillage.
TORT overcomes the limitations of the endoscopic approach with the use of articulated instrumentation, high-definition three-dimensional view, tremor elimination, and individual camera operation that prevents clashing of instruments with the endoscope during operation [4, • 20, 24]. The articulated movements of the EndoWrist are essential in facilitating the complete resection of the superior pole and pyramidal lobe of the thyroid [4]. With the robotic system, it is much easier to identify and preserve the recurrent laryngeal nerves and parathyroid glands [4, 25, 26]. The axillary arm allows for counter traction of the perithyroidal and perineural tissues to facilitate better visualization and dissection. In addition, with appropriate subcutaneous tunnelling and dissection, the axilla incision can be used for complete non-fragmented specimen removal, even for large or hard specimens [4, 24].
TORT and Oncologic Efficacy
We previously analysed the perioperative outcomes of 100 consecutive patients with papillary thyroid carcinoma who underwent TORT. It was found that for the patients who required radioactive iodine ablation (RAI), the dosage was similar to that for open thyroidectomy. In addition, post-ablation thyroglobulin levels were almost undetectable. There were no major complications detected and there was no recurrence or mortality during follow-up [24].
Another study by our group compared patients who underwent TORT with patients who underwent open thyroidectomy using propensity score matching with 10 clinico-pathologic factors including tumor size, multifocality, bilaterality, extrathyroidal extension, radioactive iodine ablation, and extent of central neck dissection. Results showed that surgical outcomes were similar, except a longer operative time for TORT [27].
Overall, we believe TORT is safe for selected low-risk or intermediate-risk cancer patients; however, due to the indolent nature of thyroid carcinoma, longer follow-up is required in order to compare long-term outcomes to open thyroidectomy.
Postoperative Recovery
The postoperative recovery for TORT patients is simple and consistent. Compression dressing to the submandibular area is only required for 12 h. As described previously, patients are allowed water and soft diet 4 h after the operation. Patients are usually allowed to return home on postoperative day 2 [•20].
Potential Complications and Disadvantages of TORT
Potential Complications
The vestibular approach is the latest approach to remote-access thyroid surgery. As with all new approaches, new complications can be encountered that are rarely seen in open thyroidectomy. We have performed over 500 TORT cases and here we share our experience of the potential complications of this procedure and how we have modified our surgical technique and procedures thereafter.
In the patients with TORT performed in our hospital, mental nerve injury has only occurred in the initial experience of this procedure. Our initial consecutive series of 24 patients found that 6 patients had transient mental nerve injury with paraesthesia over the lower lip and chin that resolved within 6 months, and in 3 patients that had permanent mental nerve injury [•21]. This was attributed to the placement of the midline incisions at the gingival-buccal sulcus and the lateral incisions at the first molar, causing a high rate of mental nerve injury. Since then, we have modified our technique such that the midline incision is over the end of the frenulum of the lower lip and the lateral incisions are 1 cm medial to both lateral oral commissures [•21, 24]. Since this modification, no further mental nerve injuries have been reported in our patients.
The study by Tai et al. consists of 304 patients undergoing TORT at our institution and represents the largest series to date. Regarding TORT-specific complications in this series, 2 patients developed cornea abrasion, 3 patients developed zygomatic bruising, 2 patients developed mandible abrasion, 2 patients had oral commissure tearing, and one patient experienced flap burn [•20].
Zygomatic bruising and corneal abrasions were mainly observed in our earlier experience and were attributed to compression of the patient’s face by the robotic arms. We have since been applying dressing over the eyes, reinforced by a thick foam covering over the upper face and eyes to prevent these complications [•20, •21, 24].
Oral commissure tearing is a complication unique to TORT and occurs most frequently during the dissection of the upper pole because there is excessive lateral movement of the robotic arms. We were able to overcome this by firstly reinforcing the corners of the mouth with sutures and also adapting to the range of movement of the robotic arms. It is also important for the assistant surgeon to be aware of the degree of movement of the robotic arms and to have regular communication with the chief surgeon [•20, •21, 24].
Chin flap perforation and flap burn is related to the electrocautery used during dissection of the skin flap. We have modified the procedure by initially using blunt mosquito clamps for dissection before switching to electrocautery [•20].
Chin dimpling was only seen in the cases where da Vinci Si was used. The dimpling can be due to the movement of the large 12 mm midline trocar; however, since switching to the da Vinci Xi system where 8 mm midline trocars are used, no further cases of chin dimpling have occurred [•20, 24].
In terms of general complications, only three patients developed transient vocal cord palsy which recovered within 3 months and only one patient developed transient hypoparathyroidism. No wound infections were encountered in this series [•20].
Cost
The da Vinci system comes at a high cost. In South Korea, the national and private medical insurance systems are well established. Hence the patient does not need to harbour a huge financial burden if they choose to undergo TORT [27]. Depending on the insurance coverage and government healthcare subsidies in different countries, we hope to see more patients benefit from robotic surgery in the future.
Reproducibility
Unlike endoscopic and open thyroidectomy, TORT lacks tactile feedback. In addition, operative times are also longer than that for endoscopic or open thyroidectomy, which is attributed to the time needed to create the working space, dock the system, and also for exchanging tools during the operation [4, 26].
TORT requires a steep learning curve. It has been suggested that a steep learning curve of 40 to 45 cases is required to master transaxillary robotic thyroidectomy [28, 29], and we believe that it is similar for TORT. This procedure will benefit patients best if performed by well-trained robotic surgeons. We believe that attending training courses especially those with hands-on cadaveric workshops would be beneficial to inexperienced surgeons.
Advances in Technology
Though TORT can be performed with both the da Vinci Si and Xi system, there are certain advantages that the newer da Vinci Xi system has over the Si system. Firstly, the endoscopic camera can be attached to any arm in the Xi system. The joint arms of the Xi system are slimmer which helps to reduce external collisions and also reduces the risk of oral commissure tearing during manipulation of the upper pole of the thyroid which is caused by excessive lateral movement of the robotic arms. Furthermore, the midline port for the Xi system is smaller, which reduces the chance of chin dimpling. The overhead boom rotation system of the Xi system allows for the patient to be in supine position rather than lithotomy position. In addition to these mentioned advantages, we compared the outcomes of patients that underwent TORT using da Vinci Si and Xi surgical systems and found that for the Xi group the postoperative pain scores at post-operation day 0 were lower, the length of hospital stay was shorter, and the number of retrieved lymph nodes from the central compartment for papillary thyroid carcinoma patients was higher [3].
With the emergence of the Intuitive da Vinci single port robotic surgical system (Intuitive, Inc. Sunnyvale, CA), a preclinical feasibility study was performed in which TORT was performed on two human cadavers using this system. The initial experience found that collision of robotic arms was minimized as all the extensions could enter the operative field via the central oral incision. This also helped to reduce the risk of oral commissure tear when manipulating the superior pole. In addition, there was no need for an axillary incision. However, in order for arm triangulation, an additional 10 cm advancement of the robotic arms past the cannula was required which is challenging with the limited working space. In addition, a larger incision is required to insert the 2.5 cm trocar, which can potentially cause mental nerve traction resulting in paraesthesia of the lower lip and chin, as well as the dimpling of the chin in the patients postoperatively [30]. Further studies will be required before this technique can be introduced to live human patients.
Conclusion
TORT is one of the latest minimally invasive approaches, which can be performed safely by an experienced surgeon with careful patient selection. As there is a consistent demand for scarless thyroid surgery, we believe that TORT can be an acceptable alternative for the treatment of certain thyroid conditions.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Dionigi G, Lavazza M, Wu CW, et al. Transoral thyroidectomy: why is it needed? Gland Surg. 2017;6(3):272–6. https://doi.org/10.21037/gs.2017.03.21.
Arora A, Swords C, Garas G, et al. The perception of scar cosmesis following thyroid and parathyroid surgery: a prospective cohort study. Int J Surg. 2016;25:38–433. https://doi.org/10.1016/j.ijsu.2015.11.021.
Kim HK, Kim HY, Chai YJ, Dionigi G, Berber E, Tufano RP. Transoral robotic thyroidectomy: comparison of surgical outcomes between the da Vinci Xi and Si. Surg Laparosc Endosc Percutan Tech. 2018;28(6):404–9. https://doi.org/10.1097/SLE.0000000000000587.
Zhang D, Park D, Sun H, et al. Indications, benefits and risks of transoral thyroidectomy. Best Pract Res Clin Endocrinol Metab. 2019;33(4):101280. https://doi.org/10.1016/j.beem.2019.05.004.
Choe JH, Kim SW, Chung KW, et al. Endoscopic thyroidectomy using a new bilateral axillo-breast approach. World J Surg. 2007;31(3):601–6. https://doi.org/10.1007/s00268-006-0481-y.
Koh YW, Kim JW, Lee SW, Choi EC. Endoscopic thyroidectomy via a unilateral axillo-breast approach without gas insufflation for unilateral benign thyroid lesions. Surg Endosc. 2009;23(9):2053–60. https://doi.org/10.1007/s00464-008-9963-3.
Sebag F, Palazzo FF, Harding J, Sierra M, Ippolito G, Henry JF. Endoscopic lateral approach thyroid lobectomy: safe evolution from endoscopic parathyroidectomy. World J Surg. 2006;30(5):802–5. https://doi.org/10.1007/s00268-005-0353-x.
Lee KE, Kim HY, Park WS, et al. Postauricular and axillary approach endoscopic neck surgery: a new technique. World J Surg. 2009;33(4):767–72. https://doi.org/10.1007/s00268-009-9922-8.
Kang SW, Jeong JJ, Yun JS, et al. Robot-assisted endoscopic surgery for thyroid cancer: experience with the first 100 patients. Surg Endosc. 2009;23(11):2399–406. https://doi.org/10.1007/s00464-009-0366-x.
Sung ES, Ji YB, Song CM, Yun BR, Chung WS, Tae K. Robotic thyroidectomy: comparison of a postauricular facelift approach with a gasless unilateral axillary approach. Otolaryngol Head Neck Surg. 2016;154(6):997–1004. https://doi.org/10.1177/0194599816636366.
Richmon JD, Holsinger FC, Kandil E, Moore MW, Garcia JA, Tufano RP. Transoral robotic-assisted thyroidectomy with central neck dissection: preclinical cadaver feasibility study and proposed surgical technique. J Robot Surg. 2011;5(4):279–82. https://doi.org/10.1007/s11701-011-0287-2.
Lee HY, You JY, Woo SU, et al. Transoral periosteal thyroidectomy: cadaver to human. Surg Endosc. 2015;29(4):898–904. https://doi.org/10.1007/s00464-014-3749-6.
Witzel K, von Rahden BH, Kaminski C, Stein HJ. Transoral access for endoscopic thyroid resection. Surg Endosc. 2008;22(8):1871–5. https://doi.org/10.1007/s00464-007-9734-6.
Richmon JD, Pattani KM, Benhidjeb T, Tufano RP. Transoral robotic-assisted thyroidectomy: a preclinical feasibility study in 2 cadavers. Head Neck. 2011;33(3):330–3. https://doi.org/10.1002/hed.21454.
Anuwong A. Transoral endoscopic thyroidectomy vestibular approach: a series of the first 60 human cases. World J Surg. 2016;40(3):491–7. https://doi.org/10.1007/s00268-015-3320-1.
Kim HK, Park D, Kim HY. Robotic transoral thyroidectomy: total thyroidectomy and ipsilateral central neck dissection with da Vinci Xi Surgical System. Head Neck. 2019;41(5):1536–40. https://doi.org/10.1002/hed.25661.
Kim HK, Park D, Kim HY. Robotic transoral thyroidectomy for papillary thyroid carcinoma. Ann Surg Treat Res. 2019;96(5):266–8. https://doi.org/10.4174/astr.2019.96.5.266.
••Haugen BR. 2015 American thyroid association management guidelines for adult patients with thyroid nodules and differentiated thyroid cancer: what is new and what has changed?. Cancer 2017:123(3):372–381. https://doi.org/10.1002/cncr.30360. The treatment of differentiated thyroid tumours has changed due to these updated guidelines in which for a certain tumour size and criteria patients may have the option of performing a hemithyroidectomy rather than a total thyroidectomy, this has a great impact on the management of thyroid cancer patients including their options for remote access surgery, quality of life and need for adjuvant therapy.
Russell JO, Clark J, Noureldine SI, et al. Transoral thyroidectomy and parathyroidectomy—A North American series of robotic and endoscopic transoral approaches to the central neck. Oral Oncol. 2017;71:75–80. https://doi.org/10.1016/j.oraloncology.2017.06.001.
•Tai DKC, Kim HY, Park D, et al. Obesity may not affect outcomes of transoral robotic thyroidectomy: subset analysis of 304 patients [published online ahead of print, 2019 Aug 13]. Laryngoscope 2019. https://doi.org/10.1002/lary.28239. This study includes the largest number of TORT patients to date and also addresses whether obesity would affect the difficulty and outcomes of performing TORT.
•Kim HY, Chai YJ, Dionigi G, Anuwong A, Richmon JD. Transoral robotic thyroidectomy: lessons learned from an initial consecutive series of 24 patients. Surg Endosc 2018:32(2):688–694. https://doi.org/10.1007/s00464-017-5724-5. Our initial experience with using the da Vinci robot to perform thyroidectomy helped us to face and address certain difficulties and complications and also helped us to alter our surgical methods to reduce complications and streamline subsequent TORT surgeries.
Dionigi G, Chai YJ, Tufano RP, Anuwong A, Kim HY. Transoral endoscopic thyroidectomy via a vestibular approach: why and how? Endocrine. 2018;59(2):275–9. https://doi.org/10.1007/s12020-017-1451-x.
Dionigi G, Tufano RP, Russell J, Kim HY, Piantanida E, Anuwong A. Transoral thyroidectomy: advantages and limitations. J Endocrinol Inves. 2017;40(11):1259–63. https://doi.org/10.1007/s40618-017-0676-0.
Kim HK, Chai YJ, Dionigi G, Berber E, Tufano RP, Kim HY. Transoral robotic thyroidectomy for papillary thyroid carcinoma: perioperative outcomes of 100 consecutive patients. World J Surg. 2019;43(4):1038–46. https://doi.org/10.1007/s00268-018-04877-w.
Ban EJ, Yoo JY, Kim WW, et al. Surgical complications after robotic thyroidectomy for thyroid carcinoma: a single center experience with 3,000 patients. Surg Endosc. 2014;28(9):2555–633. https://doi.org/10.1007/s00464-014-3502-1.
Chang EHE, Kim HY, Koh YW, Chung WY. Overview of robotic thyroidectomy. Gland Surg. 2017;6(3):218–28. https://doi.org/10.21037/gs.2017.03.18.
You JY, Kim HY, Park DW, et al. Transoral robotic thyroidectomy versus conventional open thyroidectomy: comparative analysis of surgical outcomes using propensity score matching [published online ahead of print, 2020 Jan 10]. Surg Endosc 2020. https://doi.org/10.1007/s00464-020-07369-y
Kandil EH, Noureldine SI, Yao L, Slakey DP. Robotic transaxillary thyroidectomy: an examination of the first one hundred cases. J Am Coll Surg. 2012;214(4):558–66. https://doi.org/10.1016/j.jamcollsurg.2012.01.002.
Lee J, Yun JH, Nam KH, Soh EY, Chung WY. The learning curve for robotic thyroidectomy: a multicenter study. Ann Surg Oncol. 2011;18(1):226–32. https://doi.org/10.1245/s10434-010-1220-z.
Park D, Shaear M, Chen YH, Russell JO, Kim HY, Tufano RP. Transoral robotic thyroidectomy on two human cadavers using the Intuitive da Vinci single port robotic surgical system and CO2 insufflation: preclinical feasibility study. Head Neck. 2019;41(12):4229–333. https://doi.org/10.1002/hed.25939.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
HYK reports support from Medtronic outside of the submitted work. DP and DT declare no conflicts of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Robotic Surgery.
Rights and permissions
About this article
Cite this article
Tai, D.K.C., Park, D. & Kim, H.Y. The Recent Advances in Robotic Transoral Thyroidectomy. Curr Surg Rep 8, 8 (2020). https://doi.org/10.1007/s40137-020-00253-7
Published:
DOI: https://doi.org/10.1007/s40137-020-00253-7