Abstract
Purpose of Review
To review contemporary considerations regarding upper facial esthetics and modern brow lifting techniques, including their selection criteria and efficacy.
Recent Findings
Mitek suture anchor and K-wire fixation were found to be viable endoscopic fixation techniques with various advantages over other methods. There has been a significant focus on developing minimally invasive lateral brow lifts. These often vary in degrees of lift and durability, with techniques such as browpexy/transblepharoplasty lifts having questionable efficacy, to subcutaneous temporal and combination lifts which appear to produce reliable results with maximum accessibility due to minimal anesthesia requirements. Botulinum toxin injection remains the gold standard for brow lifting when compared to other non-surgical techniques, such as thread lifts and skin tightening.
Summary
The overall trend regarding recent upper facial esthetics often focuses on maximizing the accessibility of lateral temporal brow lifts. As such, several techniques and variations have been recently developed which are less invasive and easier to perform. While some variations, such as subcutaneous temporal lifts, appear to be flexible and effective techniques, others have questions regarding their efficacy and durability. Selection will often depend on patient/surgeon’s preference and the degree of brow ptosis. These decisions can also continually evolve with changing esthetic standards. This review should help surgeons in their decision-making when choosing a particular treatment for upper facial esthetic patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The upper face undergoes many changes over time—the brow becomes ptotic, with resultant redundancy of the glabella and subsequent deepening and lengthening of facial rhytids. These changes, compounded effects of gravitational and facial muscle forces, cause upper facial aging and a fatigued appearance [1]. Removal of these signs is the goal of facial plastic surgeons. Available techniques include a wide range of surgical and non-surgical therapies, some of which are well-established while others are novel. Brow lifting in particular has become a common rejuvenation procedure used to elevate the brows and remove rhytids, thereby providing a more youthful appearance. However, even within the realm of brow lifts, there are several techniques available, each with its specific drawbacks and benefits and without a clear consensus of a particular technique’s superiority [2]. Furthermore, with emerging technologies and anatomical understanding comes a continuous search for a less invasive, more efficient treatment of the aging face. These forces yield continuous innovations and adjustments in current practice. This study will review the current techniques used in the management of upper facial esthetics, relative indications, and specific considerations.
Methods
A review of the current literature was performed using MEDLINE and PubMed databases employing combinations of terms including one of the following: “brow,” “eyebrow,” “forehead,” or “periorbital,” and one of the following: “lift,” “lifting,” or “rejuvenation.” Focus was given to articles published since 2015, specifically with regard to modern brow lifting techniques, and a summary of key findings is presented.
Anatomical Considerations
A patient’s specific pattern of rhytids is caused by correlating facial muscle actions on particular skin lines, which weaken and thin over time. Knize [3] describes how specific muscle actions contribute to the aging of the upper face. Transverse heads of the corrugator supercilii muscle move the eyebrow medially and produce vertical glabellar lines. In conjunction with the lateral orbicularis oculi muscle, they cause lateral eyebrow ptosis, which leads to lateral eyelid hooding. In addition, the superficial temporal fascia slides inferiorly over the deep temporal fascia over time, particularly laterally where it is furthest from support via the zone of adhesion and orbital ligament. This drift pulls down the lateral brow skin and eyebrow, which lacks concomitant frontalis muscle support or any elevator lateral to it [4]. Medial eyebrow depressors—oblique head of the corrugator and depressor supercilii muscles and the medial orbicularis oculi muscle—produce oblique glabellar skin lines, while the procerus muscle produces transverse dorsal skin lines, and action of the frontalis muscle creates transverse forehead skin lines.
Other contributors of the aging face include volume loss of the brow fat pad and orbital bone, causing brow ptosis, and ablation of the three-dimensional contours associated with youth [4]. Tight fascial attachments, including the zone of adhesion and orbital ligament, may require release and resuspension to treat specific areas of brow ptosis. Drolet et al. [5] describe the necessity of fully releasing the orbital ligament laterally but only limited release of the medial ligament, with particular care of the medial retaining ligaments, in order to avoid a “surprised” look. Such analysis helps target specific mechanisms causing an aged face, provides target areas for appropriate treatment, and should be kept in mind when considering a particular technique for patients.
The structures at risk during dissection, depending on the brow-lifting technique, are also described [3]. The supraorbital nerve trunk comes across the supraorbital rim, where it is at risk particularly in endoscopic cases. The deep division, found in the subgaleal plane, is generally transected during the coronal incision and is at risk during subgaleal dissection as it leaves the periosteum to enter the plane at the superior edge of the galeal fat pad. A study by Agarwal et al. [6] details the course of the frontal branch of the facial nerve, beginning within the fibrofatty tissue over the zygomatic arch to its destination in the superficial temporal fascia 1 to 1.5 cm lateral to the canthus. It is crucial to note its relation to the orbicularis-temporal ligament, formed by fusion of superficial and deep temporal plane. The main trunk runs parallel to this, either within the ligament or inferior to it, while branches run in the superficial temporal plane [3]. For endoscopic techniques, in particular, it is important to navigate the sentinel vein, as damage to it can inhibit visualization as well as cause ecchymosis, and it is a valuable reference point for localization of the frontal branch inferior to it [5, 7].
Current Surgical Techniques
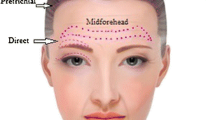
Brow lifting has undergone significant evolution since the initial inception, and several traditional techniques have been developed and disseminated variably by both facial and oculoplastic surgeons [8,9,10]. These include the direct brow lift, midforehead brow lift, coronal brow lifts, and the endoscopic brow lift, as well as modifications for the tail of brow elevation. Direct brow lift offers significant advantages including predictable results, control over the brow shape, can correct asymmetries, and can be done with local anesthesia. However, this technique is limited in the medial brow elevation and fails to treat glabellar pathology. The midforehead brow lift allows for good brow elevation utilizing an existing scar or deep rhytid. The open forehead lift can elevate the brows in a near-symmetric fashion but requires more dissection and careful hairline planning. While the coronal lift elevates the brow and hairline together as one unit, the trichophytic lift elevates the brow while maintaining the hairline (forehead reduction). These lifts do carry higher risks of scalp anesthesia and require more dissection by the surgeon. The endoscopic forehead lift allows subperiosteal elevation of the brow and hairline utilizing specific endoscopic equipment. Also, the glabellar musculature can be addressed by myectomy. Similar to the coronal brow lift, the brow and hairline are elevated together. While the rate of postoperative scalp anesthesia is believed to be lower than the open approaches, this is controversial.
Endoscopic Fixation Methods
When performing an endoscopic brow lift, the surgeon is faced with selecting between a range of fixation methods—suture, cortical bone tunnels, implantable plates, etc.—with inadequate data of superiority other than the disadvantages of fibrin glue and absorbable suture [11,12,13,14].
Absorbable implant fixation, such as the Endotine (MicroAire, Charlottesville, Virginia) multi-point plate, has often been cited as being advantageous due to not requiring later removal, intraoperative speed, and ease of use [15,16,17]. However, it also carries significant disadvantages, as it can be limited to patients with thicker scalps, is expensive, can have an inadequate lift, and has a significant incidence of residual palpability requiring removal [15, 18,19,20]. Adetayo et al. [21] studied 82 patients using the alternative Mitek Microfix QuickAnchor (DePuy Synthes, Raynham, MA) resorbable suture anchor, used in various surgical applications, and found satisfactory durability without instances of palpability or alopecia. The Mitek system was also found to be more cost-effective than the Endotine implant due to the latter’s specialized equipment. This presents an option which is similar in principle to cortical bone tunnel suturing but is easier to use, although the cost-effectiveness and durability against all other options warrant further study.
A recent study by Chasan et al. [22] describes satisfactory outcomes using K-wire fixation in 284 patients over a 20-year period. The K-wire gives flexibility in placement along small endoscopic incisions, is low profile compared to screws, and did not result in any alopecia or palpability. This technique combines the durability and minimal palpability and dependability of bone tunnels with the ease and speed of a screw technique [23, 24]. The authors observed improved fixation duration, particularly in lateral elevation, compared to prior studies [14, 25]. These findings make the K-wire technique an interesting option in endoscopic brow lifts that is inexpensive, readily available, and easy to use.
Lateral Brow Lift
As discussed, the temporal brow is prone to descent due to several factors including increased tissue laxity, continued volume loss particularly at the lateral orbit, and the relatively-unopposed action of the lateral orbicularis oculi [3, 4], while many patients may present for upper blepharoplasty with pseudoexcess of upper eyelid skin due to the ptotic lateral brow [8, 26]. An overly arched lateral brow which was previously described as “Mephisto sign,” a complication during botulinum toxin treatment, has become increasingly in line with modern beauty [27]. Several surgical and non-surgical techniques have been described for addressing this lateral lift.
Browpexy
Trans-blepharoplasty brow suspension, or browpexy, is a well-described technique that can be useful in both the aging patient and the facial paralysis patient. The technique involves a temporal dissection down to the deep layer of the superficial temporal fascia. Then, a small upper lip incision is made deep to the orbicularis oculi. A passer needle is then used to dissect a small tunnel through the subperiosteal plane and into the lateral upper lid incision. The suture is then passed through the deep layer of the lateral brow and fixated back to the superficial layer of the deep temporal fascia. This technique is limited by the need for initial overcorrection due to the subsequent stretching of the temporalis fascia and loss of lift.
Similar procedures involving more extensive dissection of the deep layer of the superficial temporal fascia and release of the lateral orbital septum have grown in popularity particularly when combined with upper blepharoplasty. This procedure can be performed with the assistance of endoscopic equipment [5, 44] depending on surgeon preference [5, 28]. This procedure can be combined with temporal skin excision as well as lysis of the corrugator musculature as described by Turin et al. [29] The study noted resolution of hooding in all 150 patients, and while almost all (93%) were done with conscious sedation, only 35% of these were in-office procedures. The lateral brow lift can be combined with a small direct brow excision [20].
An internal browpexy can also be performed by performing a transblepharoplasty approach to the lateral frontal bone. There, an absorbable fixation device such as endotine can be placed to allow for subperiosteal fixation of the brow.
While these techniques have demonstrated good short-term results, the longevity of these lateral brow lift techniques is still unknown as many studies lack long-term follow-up. [28, 30, 31]
Subcutaneous Lateral Brow Lift
Another minimally invasive option for temporal brow lifting is the subcutaneous brow lift, in which subcutaneous dissection is performed via temporal incision to the upper brow edges and redundant skin excised, typically under local anesthesia. A recent study by Savetsky and Matarasso presents the largest cohort using this technique [32••]. While this particular study lacks objective measures and follow-up standards, the authors note the overall high satisfactory rates and a lack of complications, which coincides with the findings of their literature review. In fact, an earlier study by Miller et al. describes the transition to the subcutaneous brow lift due to previous rates of numbness and difficulty in raising the galea [33]. Upon its adoption, he noted improved rhytid removal, hairline position, wound healing, and lower rates of numbness, as well as a consistent 5 − 7 mm of lift—although he noted a possible limitation in the vector of pull [34]. Adjustments include expanding dissection to elevate and reposition the malar fat pad, as well as concurrent blepharoplasty with disruption of the lateral orbicularis oculi to obliterate crow’s feet [35]. More recently, Mahmood et al. describe extending dissection to the lateral canthus for increased lift and greater flexibility in vector of pull [36]. In their response to comments advocating a subcutaneous “redistribution” of skin via a blepharoplasty incision rather than skin excision, they note their successfully maintained lift [37]. Furthermore, they note the difficulty in attaining and maintaining adequate brow elevation without skin excision, particularly in women [38]. These concerns are valid given the previous discussion regarding internal browpexy, and as such, a trans-blepharoplasty approach may be limited to males, who do not require as much elevation, with a potential indication in those with poor hairlines. Throughout the current literature, subcutaneous temporal lifting represents a simple, minimally invasive, and low-risk method to produce a predictable lateral temporal lift, which has a wide patient range and accessibility due to its performance as an in-office procedure [38]. Further study comparing these techniques and their effects on esthetic optimization secondary to factors such as vector control would be welcome.
Lateral Brow Lift—Combination Temporal and Trans-Blepharoplasty Lift
Turin et al. recently described a unique combination lift also directed at correcting lateral orbital hooding [29]. The technique begins with an upper blepharoplasty incision, through which dissection is carried deep to the orbicularis oculi and the corrugators are divided. Next, a temporal incision is used to access the forehead and superior temporal septum. Dissection is performed between the superficial and deep temporal fascia below the superior temporal septum, and in a subperiosteal plane above it. These pockets are then joined by releasing the septum, and the periorbital ligaments are released. Then, through the lateral portion of the blepharoplasty incision, a subperiosteal dissection is performed. These combine to release the galea, which is fixed with suture, while crescents of temporal skin are removed. The study noted resolution of hooding in all 150 patients, and while almost all (93%) were done with conscious sedation, only 35% of these were in-office procedures. This is an interesting technique which should provide great brow mobility and has the potential to correct some medial ptosis/rhytids in addition to the noted temporal lift. The cost of this more extensive sub-periosteal dissection appears to include the addition of increased anesthesia, limiting its accessibility when compared to the subcutaneous technique. It would be interesting to elucidate the degree of medial ptosis and rhytid correction, as well as lift durability, to determine if the expense is worthwhile. Regardless, this technique would seem to provide a more reliable lift than previously discussed internal browpexy techniques due to extensive brow release and skin excision, and presents an interesting option particularly for patients who also require blepharoplasty.
Non-surgical Techniques
The goal of non-surgical techniques is to achieve a similar result without scars and minimal downtime. While many of these results can be quite pleasing, many are not durable. As such, several techniques have been utilized including botulinum toxin and skin tightening.
Botulinum toxin injection is the most common method utilized for the correction of the aging brow worldwide. The toxin causes a temporary paresis or paralysis of muscles by affecting the neuronal input to musculature [39]. For the upper face, injection into the corrugator supercilii and procerus muscle can decrease the glabellar dynamic rhytidosis and by weakening the brow depressor action, leads to slight brow elevation. Lateral brow lift can be achieved by causing paresis to the depressing portion of the orbicularis oculi.8 Botulinum toxin is more effective at lateral brow elevation than medial brow elevation as demonstrated by Ahn et al. who noted an average medial brow elevation of 1 mm compared to 4.8 mm of the lateral brow when using botulinum toxin [40].
Skin tightening and resurfacing can also be used to achieve a small degree of brow lift by contracting forehead tissues. Microneedle radiofrequency and microfocused ultrasound (MFU) are two techniques that have been described [41]. While these techniques improve skin texture and thickness, the actual degree of durable lift is quite variable. These techniques offer a minimally invasive improvement with minimal downtime, although the microfocused ultrasound tends to be more painful for patients.
Barbed suture lift, also known as thread lift, is another non-surgical technique that has gained greater popularity in recent years. By using a barbed suture, usually in a subcutaneous plane, the lateral brow can be elevated. The longevity of the treatment is dependent on the degree of fibrosis produced during the degradation of this suture [42, 43, 44]. However, a recent systematic review found a lack of evidence to support the techniques’ durability or efficacy [45]. Meanwhile, others have noted the technique’s significant rate of complications for minimal benefit [46, 47•]. This technique has many limitations including the unsightly appearance of bunching in the lateral suprabrow/anterior temporal region. As such, this technique tends to be more popular by non-cosmetic surgeons.
Modern Esthetic Considerations
As mentioned, recent upper facial esthetic literature has often focused on minimally invasive temporal lifting. One reason for this trend is the wide range of patients who could benefit from such procedures, including younger patients. However, while these techniques are based on achieving ideal brow position, there had been a lack of studies regarding ideal modern brow esthetics. As such, there is no consensus on the ideal vector of pull used to position the brow arch, and these vary between surgeons without definition of the factors which would determine whether a brow should be pulled along a vector from ala to the pupil, the lateral canthus, the lateral limbus, [45] etc.[5, 22, 48] A recent study determined the Westmore model to be inaccurate with regard to modern esthetic ideals and seeks to provide an updated model [49•]. However, this study and others rely on subjective interpretations of unreliable landmarks, such as the hairline, without objective measures, and so are not ideal. The ideal brow position seems to change over time, and as such, there will never be a single treatment for the aging brow. Instead, various surgical and non-surgical techniques will be vital for achieving consistent beautiful outcomes.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Terella AM, Wang TD. Technical considerations in endoscopic brow lift. Clin Plast Surg. 2013;40(1):105–15.
Graham DW, Heller J, Kirkjian TJ, Schaub TS, Rohrich RJ. Brow lift in facial rejuvenation: a systematic literature review of open versus endoscopic techniques. Plast Reconstr Surg. 2011;128(4):335e–41e.
Knize DM. Anatomic concepts for brow lift procedures. Plast Reconstr Surg. 2009;124(6):2118–26.
Fitzgerald R. Contemporary concepts in brow and eyelid aging. Clinics in plastic surgery. 2013;40:21–42.
Drolet BC, Phillips BZ, Hoy EA, Chang J, Sullivan PK. Finesse in forehead and brow rejuvenation: modern concepts, including endoscopic methods. Plast Reconstr Surg. 2014;134(6):1141–50.
Agarwal CA, Mendenhall SD 3rd, Foreman KB, Owsley JQ. The course of the frontal branch of the facial nerve in relation to fascial planes: an anatomic study. Plast Reconstr Surg. 2010;125(2):532–7.
Trinei FA, Januszkiewicz J, Nahai F. The sentinel vein: an important reference point for surgery in the temporal region. Plast Reconstr Surg. 1998;101(1):27–32.
Karimi N, Kashkouli MB, Sianati H, Khademi B. Techniques of eyebrow lifting: a narrative review. J Ophthalmic Vis Res. 2020;15(2):218–35.
Patel BC, Malhotra R. Mid forehead brow lift. StatPearls. Treasure Island (FL): StatPearls Publishing Copyright © 2021, StatPearls Publishing LLC. 2021.
Raggio BS, Winters R. Endoscopic brow lift. StatPearls. Treasure Island (FL): StatPearls Publishing Copyright © 2021, StatPearls Publishing LLC. 2021.
Rohrich RJ, Beran SJ. Evolving fixation methods in endoscopically assisted forehead rejuvenation: controversies and rationale. Plast Reconstr Surg. 1997;100(6):1575–1582. Discussion 1583–1574.
Kennedy BD, Pogue MD. Fixation techniques for endoscopic browlift. Journal of oral and maxillofacial surgery: Official Journal of the American Association of Oral and Maxillofacial Surgeons. 1999;57(5):588–94.
Romo T 3rd, Jacono AA, Sclafani AP. Endoscopic forehead lifting and contouring. Facial plastic surgery: FPS. 2001;17(1):3–10.
Jones BM, Grover R. Endoscopic brow lift: a personal review of 538 patients and comparison of fixation techniques. Plast Reconstr Surg. 2004;113(4):1242–1250. Discussion 1251–1242.
Stevens WG, Apfelberg DB, Stoker DA, Schantz SA. The endotine: a new biodegradable fixation device for endoscopic forehead lifts. Aesthetic surgery journal / the American Society for Aesthetic Plastic surgery. 2003;23(2):103–7.
Evans GR, Kelishadi SS, Ho KU. “Heads up” on brow lift with Coapt Systems’ Endotine Forehead technology. Plast Reconstr Surg. 2004;113(5):1504–5.
Hönig JF, Frank MH, Knutti D, de La Fuente A. Video endoscopic-assisted brow lift: comparison of the eyebrow position after Endotine tissue fixation versus suture fixation. J Craniofac Surg. 2008;19(4):1140–7.
Walden JL, Orseck MJ, Aston SJ. Current methods for brow fixation: are they safe? Aesthetic Plast Surg Sep-Oct. 2006;30(5):541–8.
Chowdhury S, Malhotra R, Smith R, Arnstein P. Patient and surgeon experience with the endotine forehead device for brow and forehead lift. Ophthalmic Plast Reconstr Surg Sep-Oct. 2007;23(5):358–62.
Langsdon PR, Williams GB, Rajan R, Metzinger SE. Transblepharoplasty brow suspension with a biodegradable fixation device. Aesthetic surgery journal / The American Society for Aesthetic Plastic surgery. 2010;30(6):802–809.
Adetayo OA, Wong WW, Motakef S, Frew TG, Campwala I, Gupta SC, et al. Endoscopic brow lift fixation with Mitek suture anchors: a 9-year experience of a new “ideal” technique. Plast Surg (Oakv). 2019;27(2):100–6.
Chasan PE, Hauch AT. The K-wire fixation technique for endoscopic brow lift: a long-term follow-up. Aesthetic surgery journal / the American Society for Aesthetic Plastic surgery. 2020;40(10):1051–60.
Hoenig JF. Rigid anchoring of the forehead to the frontal bone in endoscopic facelifting: a new technique. Aesthetic Plast Surg. 1996;20(3):213–5.
Malata CM, Abood A. Experience with cortical tunnel fixation in endoscopic brow lift: the “bevel and slide” modification. Int J Surg. 2009;7(6):510–5.
Behmand RA, Guyuron B. Endoscopic forehead rejuvenation: II. Long-term results. Plast Reconstr Surg. 2006;117(4):1137–1143. Discussion 1144.
Dar SA, Rubinstein TJ, Perry JD. Eyebrow position following upper blepharoplasty. Orbit. 2015;34(6):327–30.
Angelo-Khattar M. A novel onabotulinumtoxinA treatment technique to obtain predictable outcomes in eyebrow position and shape. Clin Cosmet Investig Dermatol. 2020;13:781–7.
Baker MS, Shams PN, Allen RC. The quantitated internal suture browpexy: comparison of two brow-lifting techniques in patients undergoing upper blepharoplasty. Ophthalmic Plast Reconstr Surg. 2016;32(3):204–6.
Turin SY, Vaca EE, Cheesborough JE, Sinno S, Mustoe TA. Simplified lateral brow lift under local anesthesia for correction of lateral hooding. Plast Reconstr Surg Glob Open. 2019;7(6):e2098.
Georgescu D, Anderson RL, McCann JD. Brow ptosis correction: a comparison of five techniques. Facial plastic surgery: FPS. 2010;26(3):186–92.
Mokhtarzadeh A, Massry GG, Bitrian E, Harrison AR. Quantitative efficacy of external and internal browpexy performed in conjunction with blepharoplasty. Orbit. 2017;36(2):102–9.
••Savetsky IL, Matarasso A. Lateral temporal subcutaneous brow lift: clinical experience and systematic review of the literature. Plast Reconstr Surg Glob Open. Apr 2020;8(4):e2764. Findings in this study show the feasibility and effectiveness of minimally invasive subcutaneous lateral temporal brow lift, and reviews its results within prior studies.
Miller TA, Rudkin G, Honig M, Elahi M, Adams J. Lateral subcutaneous brow lift and interbrow muscle resection: clinical experience and anatomic studies. Plast Reconstr Surg. Mar 2000;105(3):1120–1127. Discussion 1128.
Miller TA. Lateral subcutaneous brow lift. Aesthetic surgery journal / the American Society for Aesthetic Plastic surgery. 2003;23(3):205–10.
Guerrissi JO. Periorbital rejuvenation: a safe subcutaneous approach to forehead, eyebrow, and orbicularis oculis muscle mobilization. Aesthetic Plast Surg. 2010;34(2):147–52.
Mahmood U, Baker JL Jr. Lateral subcutaneous brow lift: updated technique. Aesthetic surgery journal / the American Society for Aesthetic Plastic surgery. 2015;35(5):621–4.
Mahmood U, Baker JL, Jr. Response to “Comments on ‘Lateral subcutaneous brow lift: updated technique’”. Aesthetic surgery journal / the American Society for Aesthetic Plastic surgery. 2016;36(2):Np86.
Bidros RS, Salazar-Reyes H, Friedman JD. Subcutaneous temporal browlift under local anesthesia: a useful technique for periorbital rejuvenation. Aesthetic surgery journal / the American Society for Aesthetic Plastic surgery. 2010;30(6):783–788.
Satriyasa BK. Botulinum toxin (Botox) A for reducing the appearance of facial wrinkles: a literature review of clinical use and pharmacological aspect. Clin Cosmet Investig Dermatol. 2019;12:223–8.
Ahn MS, Catten M, Maas CS. Temporal brow lift using botulinum toxin A. Plast Reconstr Surg. 2000;105(3):1129–1135. Discussion 1136–1129.
Ukoha U, Malone CH, Munavalli G. Nonsurgical brow lift with a temperature-controlled, fractionated radiofrequency needle device. Dermatologic surgery: official publication for American Society for Dermatologic Surgery [et al.]. 2021;47(2):296–298.
Sulamanidze MA, Fournier PF, Paikidze TG, Sulamanidze GM. Removal of facial soft tissue ptosis with special threads. Dermatologic surgery: official publication for American Society for Dermatologic Surgery [et al.]. 2002;28(5):367–371.
Lycka B, Bazan C, Poletti E, Treen B. The emerging technique of the antiptosis subdermal suspension thread. Dermatologic surgery: official publication for American Society for Dermatologic Surgery [et al.]. 2004;30(1):41–44. Discussion 44.
Flynn J. Suture suspension lifts: a review. Oral Maxillofac Surg Clin North Am. 2005;17(1):65–76, vi.
Gülbitti HA, Colebunders B, Pirayesh A, Bertossi D, van der Lei B. Thread-lift sutures: still in the lift? A systematic review of the literature. Plast Reconstr Surg. 2018;141(3):341e–7e.
Rachel JD, Lack EB, Larson B. Incidence of complications and early recurrence in 29 patients after facial rejuvenation with barbed suture lifting. Dermatologic surgery: official publication for American Society for Dermatologic Surgery [et al.]. 2010;36(3):348–354.
•Obourn CA, Williams EF, 3rd. A decade of thread-lifting-what have we learned over the last 10 years? JAMA facial plastic surgery. 2018;20(5):349–350. Findings from this study show thread-lifting techniques to be inefficacious and not durable, while having higher complication rates than many other techniques.
Briceño CA, Zhang-Nunes SX, Massry GG. Minimally invasive surgical adjuncts to upper blepharoplasty. Facial Plast Surg Clin North Am. 2015;23(2):137–51.
•Jabbour S, Nasr M, Kechichian E, et al. “The evolution of eyebrow morphology: the Westmore model revisited”. Int J Dermatol. 2018;57(8):928–932. Findings from this study show the Westmore model to be largely outdated and was part of the impetus for investigating the changes in eyebrow esthetics.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
Aron Kandinov, Armela Hasa, Boris Paskhover, and Eric Carniol declare that they have no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical collection on FACIAL PLASTICS: FacialSkin Rejuvenation
Rights and permissions
About this article
Cite this article
Kandinov, A., Hasa, A., Paskhover, B. et al. Brow Lifting and Upper Facial Esthetics: Current Techniques and Considerations. Curr Otorhinolaryngol Rep 9, 442–447 (2021). https://doi.org/10.1007/s40136-021-00376-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40136-021-00376-0