Abstract
Purpose of Review
The purpose of this paper is to review skin cancer screening guidelines from major public health/medical organizations.
Recent Findings
No consensus exists on whether or not screening to prevent skin cancer is warranted.
Summary
The best evidence of screening efficacy should come from population-based randomized trials, but is unlikely to exist due to feasibility constraints. Consequently, consensus should be built from observational/non-randomized designs, such as the SCREEN study in Germany. Current guidelines often focus on melanoma alone, while potential benefits of screening for non-melanoma skin cancers (NMSC) are largely overlooked. There may be less room for doubt regarding the value of screening, if both diseases were considered. Further, targeted approaches, i.e., screening only in high-risk populations, remain poorly defined and untested. Continuing to state that there is insufficient evidence to recommend screening leads to confusion about whether or not to screen and is unlikely to result in substantial changes to the morbidity of NMSC and significant mortality from melanoma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Melanoma is the most lethal form of skin cancer, and while it has a relatively high 5-year survival rate [1], there is considerable variance in the prognosis according to the stage of disease at diagnosis (99, 64, and 18% for localized, regional, and distant stages, respectively) [2, 3] indicating the potential importance of early detection. Most melanomas are found incidentally through clinical skin examinations [4], and several studies have supported the effectiveness of skin examination in the early diagnosis of melanoma [5, 6]; yet, skin cancer screening is underutilized in the USA [7,8,9].
Current skin cancer screening recommendations from different expert, clinical, and academic groups are conflicting despite often being based on the same set of studies. For example, the US Preventive Services Task Force (USPSTF) confirms that skin cancer screening consistently identifies melanomas at an earlier stage than those identified through usual care. However, lack of randomized controlled trials (RCTs) showing reduced skin cancer mortality from screening precludes their recommendation for or against routine skin cancer screening through whole-body examination [10,11,12]. This review critically analyzes current skin cancer screening guidelines proposed by major public health and medical organizations in the USA, summarizes the differences, and, by including new information from a skin screening study underway in the USA, seeks to provide a clarified rationale for a prudent approach to screening activities.
Methods
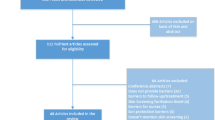
An online search was performed with the PubMed and Google to identify information concerning skin cancer screening guidelines released by public health and medical organizations using the following inclusion criteria: (1) published between 2008 and 2017, (2) available in English, and (3) type of publication could be position statements and guidelines, original research, review articles, perspective, opinion, or commentary. Existing recommendations were compared and summarized with supporting literature into three categories: (1) no recommendation of screening in the general (asymptomatic) population, (2) screening recommended in the general population, and (3) selective screening recommended among high-risk populations.
Results and Discussion
From 2008 to 2017, position statements or guidelines addressing skin cancer screening were released by several US entities including the USPSTF [13], the National Cancer Institute (NCI) [14], the Centers for Disease Control and Prevention (CDC) [15], the American Academy of Dermatology (AAD) [16], the American Academy of Family Physicians (AAFP) [17], the American Cancer Society (ACS) [18], and the US Surgeon General [19], as well as international entities including the Cancer Research in the UK [20], the Cancer Council of Australia [21], and the Canadian Cancer Society [22]. A summary of their positions or recommendations is provided in Table 1.
The Case for Not Screening in the General “Asymptomatic” Adult Population
The 2016 recommendation statement from the USPSTF, which concentrated its review on whole or partial visual skin examination conducted by primary care physicians or dermatologists and which focused on potential impact on melanoma morbidity and mortality, stated that insufficient evidence exists to determine the benefits and harms of visual skin examinations by clinicians as a screening tool for skin cancer [13]. The USPSTF conducts rigorous systematic reviews and publishes letter grades for preventive services reflecting the strength of evidence and balance of benefits and harms. A grade of “I” is reserved for preventive services with insufficient supporting evidence and for which the balance of benefits and harms cannot be established, while grades of “A” or “B” are given for recommended services with a substantial or moderate, respectively, net benefit; “C” is for services that are recommended based on individual preferences and have a small net benefit; and “D” is for services that are discouraged because of lack of net benefit. A letter grade of I was issued by the USPSTF in 2016 for visual skin exams to screen for skin cancer in the general population, reaffirming their prior conclusions issued in 2009.
While the USPSTF acknowledges the ability of visual examinations by clinicians to successfully detect both melanoma and non-melanoma skin cancers (NMSC), the benefit as a preventive screening tool is currently not supported for individuals who are not considered “high risk.” The decision was largely based on the lack of RCTs and observational studies (i.e., case-control or cohort studies) providing direct evidence to support that whole-body skin examinations (by a clinician) lead to improved health outcomes (i.e., reductions in morbidity and mortality from melanoma) in asymptomatic adults. Considering it was estimated that about 800,000 Americans would need to be randomized in a skin screening study to demonstrate a significant impact on mortality from melanoma [23, 24], controlled trials demonstrating mortality outcomes are not considered feasible in the USA [10, 25]. Even in a country like Australia that has extremely high incidence rates of melanoma, a randomized trial of population-based screening confirmed only 0.20% of the screened population had melanomas [26, 27]. The USPSTF also argued that there is substantial risk for overdiagnosis of skin cancer in implementing screening in the general population, making reference to the SEER-Medicare (1986–2001) data showing increases in the diagnosis of clinically insignificant cancers, but no changes in mortality rates [13].
In a similar conclusion, the NCI’s Physician Data Query (PDQ) Screening and Prevention Editorial Board reported inadequate evidence to determine whether mortality from melanomatous skin cancer is reduced from visual skin exams in individuals without symptoms [14]. Emphasis in this report was placed on the potential harms and negative outcomes from visual examination of the skin in healthy individuals including over diagnosis, misdiagnosis, and complications from diagnostic or treatment interventions [14].
A review of global guidelines by Collins et al. also did not support screenings of the general population, as it is believed that screening the general population, who are not considered high risk, may produce a high false-positive rate [28]. These recommendations are in line with statements from international entities, e.g., the Cancer Council Australia, Cancer Research UK, Cancer Council Australia, and Canadian Task Force on Preventative Health Care, which do not support annual skin checks in the general population, citing limited evidence that screening will reduce mortality, or that a mass screening program cannot be justified by either melanoma frequency or low mortality of the NMSC [21].
The Case in Support of Physician Screenings in the General Population
In a commentary to the USPSTF recommendations, Bigby argued that the benefit in screening is not disproven due to absence of direct evidence and that physicians should be doing whole-body skin screenings as part of a basic clinical examination [23]. Worldwide, population-based melanoma screening programs have largely been conducted and evaluated among populations with moderate to high incidence of melanoma such as France (age-standardized rate (ASR) = 10.2), Germany (ASR = 11.4), Italy (ASR = 11.4), Australia (ASR = 34.9), and New Zealand (ASR = 35.8); in the USA, the ASR = 14.3 and considered moderate [27, 29,30,31,32,33,34].
Early results published in 2017 from a large screening study in the USA demonstrated greater likelihood of melanoma detection in screened vs unscreened persons, as well as greater likelihood of detecting thinner tumors (0.37 vs 0.65 mm) [35•]. The SCREEN project conducted in Northern Germany implemented a population-based systematic skin cancer surveillance program with over 360,000 participants finding a 34% increase in invasive melanoma incidence at a population level. Importantly, melanoma mortality 5 years after the SCREEN decreased by nearly half in men and women [30]. However, the mortality decrease did not appear to be durable in a subsequent study, which included an additional 5 years of follow-up data [36]. This may be explained by a variety of factors, including the potentially less intensive national protocol and the 4-year lag time between the end of the SCREEN pilot study and the launch of the National Skin Screening program [36, 37•]. Other well-designed observational studies have found correlations between physician skin examinations and thinner melanomas at diagnosis and decreased mortality rates [35•, 38, 39]. Due to these results, numerous studies have suggested screening recommendations stratified by patient risk level [28, 40, 41], calculated based on skin type, hair and eye color, family history, previous history of skin cancer, sun exposure, and presence of nevi [40].
The ACS currently advocates for the addition of skin checks during a health exam with a primary care provider for men and women 20 years of age and older [18] and recommends monthly self-skin examination (SSE) for all individuals. The Skin Cancer Foundation provided their own recommendations of monthly SSE, yearly physician-directed total body skin exams (TBSE), and patient education, after citing a study that showed 56% of the melanomas discovered by dermatologists were not the primary reason for the patient’s visit and detection initiated by dermatologists was associated with thinner melanomas [39]. The AAD has voiced its disappointment in the recommendations made by the USPSTF, stating that the scope of the USPSTF’s recommendations were limited to studies of primary care physicians performing skin checks, while dermatologists are the best trained to diagnose skin cancer [42]. However, USPSTF states there is insufficient data to draw any conclusion about differences in accuracy by specialty [13, 24]. In addition, the AAD recommends SSE and encourages dermatologists to hold public skin cancer screenings, emphasizing their conclusion that research has shown early detection can significantly reduce morbidity and mortality related to melanoma [42]. The Canadian Cancer Society recommends that everyone gets a physician skin check done yearly. Other proposed skin cancer recommendations include yearly screening based on risk factors (i.e., personal history, family history, physical features, and UV overexposure) [43•]. The Blue Cross Blue Shield in Massachusetts recommends total skin exams every 3 years at the clinician’s discretion from ages 19–49 and yearly total skin exam at the clinician’s discretion for ages 50 and up.
A common point of argument for skin cancer screening has been costs. However, in a study conducted in the community practice setting, assessment of the “downstream consequences” (i.e., skin surgeries and dermatology visits) of a melanoma screening program reported that although more melanomas were diagnosed, no appreciable impact on either skin surgeries or dermatological visits was observed, suggesting that early melanoma detection can be achieved with greater screening by primary care physicians (PCPs) in a community setting, with little increase to downstream elements of cost in either skin surgeries or dermatology visits [44].
While there is potential for additional financial cost to the patient in order to get a skin exam from either their PCP or a dermatologist, there is relatively minimal impact from a skin cancer screening, when contrasted with PSA testing to screen for prostate cancer. If a suspicious growth is noticed as a result of the skin screening, it will likely be removed with a minimally invasive biopsy procedure during that visit, and the biopsy site often heals within a week or so. The majority of these lesions are also likely benign in nature, and if an early stage skin cancer is detected, there may only be an additional clinic visit for a subsequent biopsy that shows clear margins. In contrast, a biopsy resulting from a positive PSA screening test may have relatively higher treatment consequences, including impotence, incontinence, or even death.
Selective Screening/Screening of High-Risk Individuals
To provide maximum efficiency, some recommendations are focused on screening individuals who are determined to be at risk for melanoma and likely to benefit most from these screenings, where the cost-effectiveness may also be optimized [36, 45]. A cohort study published in 2017 found that specialized surveillance is a cost-effective strategy for individuals at high risk for developing melanoma [46]. The USPSTF concluded its 2016 review with a recommendation: “future research on skin cancer screening should focus on evaluating the effectiveness of targeted screening in those considered to be at higher risk for skin cancer” [47]. Unfortunately, this recommendation does not include a strategy for persons at high risk for NMSC, even though persons who get an NMSC are at higher risk of a subsequent primary melanoma [48], a point that was strongly emphasized in both initial [16] and follow-up [42, 49] statements released by AAD in response to the USPSTF’s 2016 recommendations.
A systematic review of the melanoma screening guidelines of 20 countries reported significant evidence to support screening and monitoring measures for individuals considered to be high risk, but did not assess recommendations in the general population [50]. Those at greatest risk, and who would receive the most benefit from screening measures, are predominantly elderly men due to their melanoma incidence and melanoma-related mortality [28]. While the AAD supports broader screening efforts in the general population, they similarly note that the members of high-risk groups, including men older than 50, as well as people with more than 50 moles, large or unusual moles, fair skin, or history of skin cancer, should discuss with a dermatologist the frequency of receiving physician skin examinations [42]. This approach is also endorsed by the American College of Preventive Medicine, which recommends total skin examinations targeting high-risk populations, as does American College of Obstetricians and Gynecologists, which additionally specifies females 13 years and older as among those at high risk [34].
Minority groups, including individuals of Hispanic, Black, or Asian background, should be considered high risk and recommended for selective screening due to experiencing greater morbidity and mortality from skin cancer, despite lower rates of skin cancer than white individuals [51,52,53,54]. When melanoma occurs among ethnic and racial minorities, it is more likely to be present as advanced stage disease [52,53,54], and risk misperceptions in minority groups (i.e., believing pain or other symptoms should occur with skin cancer, or that there is nothing one can do to decrease skin cancer risk) may contribute to the observed disparities for morbidity and mortality [51]. Further, the incidence of melanoma among Hispanic individuals increased by 11.6 and 8.9% per year for males and females, respectively [53], with a detection of thicker tumors (> 1.5 mm) notable for those of lower socioeconomic status (SES), particularly for Hispanic males [54]. SES is an established risk factor for melanoma in white populations, among whom increasing levels of wealth are strongly associated with increasing incidence of melanoma [55], while the opposite trend of higher incidence among lower levels of SES has been observed for individuals of Hispanic ethnicity [54]. Because NMSC is not a reportable cancer, reliable information regarding incidence and impact of NMSC in persons of color or Hispanic ethnicity remains largely unknown [52, 56].
Economic and Other Considerations
A study of the impact on years of potential life lost (YPLL), estimated that for melanoma, men had 17–18 YPLL and women had 18–23 YPLL, and for NMSC, the impact was lower but still appreciable (both men and women had 9–11 YPLL) [57]. The indirect morbidity costs (i.e., lost work days, restricted activity days, etc.) were also described and observed to be higher for NMSC than for melanoma in the USA (7–19 vs 20–29 million, as annual indirect costs per population) [57]. Perhaps this higher estimate for NMSC is in part owing to the significant recurrence that ensues, once initially diagnosed [58]. A systematic review by Barton et al. suggests that NMSC is associated with higher all-cause mortality and cancer-specific mortality, but this relationship requires more rigorous study with adequate control for confounding and potential mechanisms have not yet been tested [59]. Earlier detection, perhaps through greater screening efforts, could reduce some of the impact on YPLL for patients diagnosed with skin cancer.
Although both CDC and NCI defer to the USPSTF’s recommendation that no population-wide screening be initiated at this time for the general public, they both emphasized that these recommendations are not applicable to people with history of skin cancer or suspicious lesions. Instead, those individuals should talk to their doctor to evaluate if they are at high risk for skin cancer [60] and should seek regular screening. However, the general population consists of people who are unaware of their history of NMSC, melanoma, or atypical moles. Likewise, primary care physicians may be unaware of their patient’s status in an at-risk category, especially as physician knowledge of the patient’s health history (unless they are the original diagnosing physician) largely relies on patient self-report.
Conclusions
There is currently no consensus from leading expert, clinical, and academic groups on whether or not screening to prevent melanoma is warranted. While some groups recommend general population screening, other groups do not, despite the fact that both have reached their conclusion based on essentially the same data from the same studies. A large-scale randomized trial of screening with melanoma mortality as the outcome is unlikely to be conducted due to the relative rarity of the disease; therefore, recommendations must rely on non-randomized studies, observational data, and studies that do not directly evaluate the role of screening in reducing melanoma mortality. Several studies have supported the effectiveness of skin examination in the early diagnosis of melanoma, but whether or not this approach to skin cancer screening actually has a long-term effect in lowering melanoma mortality rates has not been demonstrated [61]. Some have argued that differences in survival rates have little to do with early detection but are associated with other factors that may produce more aggressive melanomas in certain individuals (i.e., change in the biologic nature of the disease, smoking, and diet) [62, 63]. In addition, screening programs may attract more highly motivated individuals who may be more likely to be aware of their risk factors, present as early stage melanomas, and have better prognosis regardless of the availability of skin examination (selection bias) [64]. Lead-time and length-time bias may also create a false impression that early detection programs are effective in increasing survival rates by catching tumors early in their detectable preclinic phase or enrolling patients who are more likely to have a longer detectable preclinic phase.
As well as a lack of direct evidence of the efficacy of skin cancer screening programs, there are other factors that complicate the discussion regarding screening efficacy and are undoubtedly contributing to the inconsistency in recommendations from various groups. Frequently, the focus is on melanoma alone, whereas the potential benefits to screening for NMSC are largely overlooked—although NMSC is usually not as lethal a disease as melanoma, it still carries significant morbidity and has substantial impact economically. The AAD expressed similar concerns that the USPSTF’s recommendations did not account for the “potentially devastating effects of [NMSC]” including “severe tissue damage or metastasis and death.” If the impact of a screening program included cost/benefit analysis for both melanoma and NMSC, there may be less room for doubt regarding the value of implementing screening activities in the general population.
The question of screening method also confuses the discussion about the efficacy of screening. For example, a focus on whole-body skin examinations discounts studies that used histologically confirmed images of lesions to assess the accuracy of screening tests. Instead of making specific screening recommendations, some expert groups have made suggestions to improve overall skin cancer surveillance. Shellenberger et al. proposed putting more emphasis on skin cancer education for US residency programs for primary care physicians [65] who may be at the frontline of finding skin cancer at its early, thinner stages during routine annual care visits. In a study conducted at the Mayo Clinic, it was found that the most common reason for an office visit was having a skin-related concern, presenting an existing opportunity to conduct a skin check right then and there, with the impetus to do so [66]. Inspired by the SCREEN project in Germany, some authors have proposed better reimbursement; the confluence of specially trained primary care physicians, physician assistants, and nurse practitioners to assist with large-scale screening programs; and expedited skin examinations that focus on parts of the body that receive high sun exposure or are hard to see [12]. Although limited, there is evidence that nurse practitioners can effectively assist with implementing screening procedures and that the addition of a tool in the medical record may serve both as a skin exam tracking tool and a reminder for health providers that conducting the skin exam is important [67]. Other studies support efforts to emphasize patient education on self-skin examinations until more definitive evidence arises for physician skin examinations [50]. All of these approaches have different costs and effectiveness, and therefore, cost-effectiveness, and to date, there has been no comprehensive approach to evaluating one screening modality against another, nor consideration of multilevel screening approaches incorporating combinations of the above approaches.
Population-based early detection campaigns have largely been popular in settings with very high incidence rates such as Australia and Germany [30, 68]. While rates are high in certain parts of the USA, melanoma is still a fairly rare disease and this has contributed to the lack of adequately powered RCTs to examine the effects of population-based screening on melanoma outcomes [10]. For such settings where the cost-effectiveness of population-based campaigns cannot be easily established, experts are leaning toward focusing on high-risk subpopulations, such as individuals who have a personal history melanoma, middle-aged or older men, and the economically disadvantaged [32, 41, 69,70,71,72]. However, there is little agreement on what constitutes high risk and little evaluation to date on the relative benefits of screening in different high-risk populations: those details are required in order to accurately identify high-risk groups for screening, and it could be argued that recommending screening in high-risk groups without consensus on how to identify those high-risk groups is not a reasonable recommendation—especially if it is provided as the only alternative to population-based screening.
Finally, while it is important to have a standardized set of criteria for reaching consensus on whether or not to screen and how to screen (such as the USPSTF employs), and the best evidence of screening efficacy certainly comes from population-based randomized trials, those data are unlikely ever to be available for screening to reduce melanoma mortality. As a result, we may have to settle for building consensus on indirect evidence (i.e., information obtained from observational or non-randomized designs, such as the SCREEN study in Germany). The alternative approaches of recommending screening only in high-risk populations that are ill defined and among whom screening also has not been evaluated, or continuing to state that there is insufficient evidence to recommend screening, not only lead to confusion about whether or not to screen but are also unlikely to result in substantial reduction in morbidity of non-melanoma skin cancers and significant mortality from melanoma.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Jemal A, Ward EM, Johnson CJ, Cronin KA, Ma J, Ryerson B, et al. Annual report to the nation on the status of cancer, 1975–2014, featuring survival. J Natl Cancer Inst. 2017;109:1975–2014.
Azoury SC, Lange JR. Epidemiology, risk factors, prevention, and early detection of melanoma. Surg Clin North Am. 2014;94:945–62.
American Cancer Society, California Department of Public Health, California Cancer Registry. California Cancer Facts & Figures 2017. Alameda, CA: American Cancer Society, Inc., California Division; 2017.
Chiaravalloti AJ, Laduca JR. Melanoma screening by means of complete skin exams for all patients in a dermatology practice reduces the thickness of primary melanomas at diagnosis. J Clin Aesthet Dermatol. 2014;7:18–22.
Di Quinzio ML, Dewar RA, Burge FI, Veugelers PJ. Family physician visits and early recognition of melanoma. Can J Public Health. 2005;96:136–9.
Aitken M, Elwood PD, Baade P, Youl D, English JF. Clinical whole-body skin examination reduces the incidence of thick melanomas. Int J Cancer. 2010;126:450–8.
Saraiya M, Hall HI, Thompson T, Hartman A, Glanz K, Rimer B, et al. Skin cancer screening among U.S. adults from 1992, 1998, and 2000 National Health Interview Surveys. Prev Med (Baltim). 2004;39:308–14.
Geller AC, Zhang Z, Sober AJ, Halpern AC, Weinstock MA, Daniels S, et al. The first 15 years of the American Academy of Dermatology skin cancer screening programs: 1985–1999. J Am Acad Dermatol. 2003;48:34–41.
Lakhani NA, Saraiya M, Thompson TD, King SC, Guy GP. Total body skin examination for skin cancer screening among U.S. adults from 2000 to 2010. Prev. Med. (Baltim). 2014;61:75–80.
Wolff T, Tai E, Miller T. Screening for skin cancer: an update of the evidence for the U.S. Preventive Services Task Force. Ann Intern Med. 2009;150:194–8.
Calonge DB, Petitti TG, DeWitt L, US, Gordis N. Screening for skin cancer: Services Task Force recommendation statement. Ann Intern Med. 2009;150(3):188–93.
Wickenheiser MR, Bordeaux JS, Robinson JK. Melanoma screening by physicians: time for a policy change in the United States. JAMA Dermatol. 2014;150:1045–6.
U.S. Preventive Services Task Force. Screening for skin cancer: U.S. Preventive Services Task Force recommendation statement. Ann. Intern. Med. 2009;150:188–93.
National Cancer Institute: PDQ Screening and Prevention Editorial Board. Skin Cancer Screenings (PDQ®). Bethesda: PDQ Cancer Inf. Summ; 2017.
Centers for Disease Control and Prevention. Cancer Prevention and Control: Cancer screening tests (Internet). Division of cancer prevention and prevention, Centers for Disease Control and Prevention; 2016 Available from: https://www.cdc.gov/cancer/dcpc/prevention/screening.htm. Accessed 17 Aug 2017.
Lebwhol MG. AAD statement on skin cancer screening. News releases. Schaumburg: American Academy of Dermatology; 2015 Nov.
American Academy of Family Physicians. Clinical preventive service recommendation: Skin Cancer (Internet). American Academy of Family Physicians; 2016. Available from: http://www.aafp.org/patient-care/clinical-recommendations/all/skin-cancer.html. Accessed 17 Aug 2017.
American Cancer Society. Cancer Screening Guidelines (Internet). American Cancer Society; 2017. Available from: https://www.cancer.org/healthy/find-cancer-early/cancer-screening-guidelines.html. Accessed 17 Aug 2017.
U.S. Department of Health and Human Services. The Surgeon General’s call to action to prevent skin cancer. Washington, DC: U.S. Department of Health and Human Services; 2014.
Cancer Research UK. Melanoma skin cancer: Getting diagnosed (Internet). Cancer Research UK. Cancer Research UK; 2016 . Available from: http://aboutcancer.cancerresearchuk.org/about-cancer/melanoma/getting-diagnosed. Accessed 17 Aug 2017.
Cancer Council Australia. Position Statement: Sun Smart (Internet). Cancer Council Australia; 2017 Available from: http://www.cancer.org.au/policy-and-advocacy/position-statements/sun-smart/Accessed 17 Aug 2017.
Canadian Cancer Society. Skin exam (Internet). Can. Cancer Soc. 2017. Available from: http://www.cancer.ca/en/cancer-information/cancer-type/skin-melanoma/finding-cancer-early/skin-examination/?region=on. Accessed 17 Aug 2017.
Bigby M. Why the evidence for skin cancer screening is insufficient: lessons from prostate cancer screening. Arch Dermatol. 2010;146:322–4.
U.S. Preventive Services Task Force. Screening for skin cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2009;150:188–93.
Geller AC. Educational and screening campaigns to reduce deaths from melanoma. Hematol Oncol Clin North Am. 2009;23:515–27.
Aitken JF, Janda M, Elwood M, Youl PH, Ring IT, Lowe JB. Clinical outcomes from skin screening clinics within a community-based melanoma screening program. J Am Acad Dermatol. 2006;54:105–14.
Aitken JF, Elwood JM, Lowe JB, Firman DW, Balanda KP, Ring IT. A randomised trial of population screening for melanoma. J Med Screen. 2002;9:33–7.
Collins M-KM, Secrest AM, Ferris LK. Screening for melanoma. Melanoma Res. 2014;24:428–36.
Ferlay J, Steliarova-Foucher E, Lortet-Tieulent J, Rosso S, Coebergh JWW, Comber H, et al. Cancer incidence and mortality patterns in Europe: estimates for 40 countries in 2012. Eur J Cancer. 2013;49:1374–403.
Breitbart EW, Waldmann A, Nolte S, Capellaro M, Greinert R, Volkmer B, et al. Systematic skin cancer screening in Northern Germany. J Am Acad Dermatol. 2012;66:201–11.
De Giorgi V, Gori A, Alfaioli B, Rossari S, Grazzini M, Pata MA, et al. Early diagnosis for melanoma: is open access to skin cancer clinics really significant? A prospective study. Prev Med (Baltim). 2010;51:334–5.
Geller AC, Greinert R, Sinclair C, Weinstock MA, Aitken J, Boniol M, et al. A nationwide population-based skin cancer screening in Germany: proceedings of the first meeting of the International Task Force on Skin Cancer Screening and Prevention (September 24 and 25, 2009). Cancer Epidemiol. 2010;34:355–8.
Guther K, Ramrath D, Dyall-Smith M, Landthaler W, Guther S, Ramrath K, et al. Development of a targeted risk-group model for skin cancer screening based on more than 100,000 total skin examinations. J Eur Acad Dermatol Venereol. 2012;26:86–94.
Sneyd M, Cox B. The control of melanoma in New Zealand. N Z Med J. 2006;119:U2169.
• Ferris LK, Saul MI, Lin Y, Ding F, Weinstock MA, Geller AC, et al. A large skin cancer screening quality initiative. JAMA Oncol. 2017;3:1112. This manuscript highlights a rare, large-scale and recent study of a skin cancer screening initiative in the US, exploring feasibility of conducting total body skin exams to detect thinner melanomas and assesses cost impacts, which could be used to inform future population-based screening programs.
Stratigos AJ, Forsea AM, van der Leest RJT, de Vries E, Nagore E, Bulliard J-L, et al. Euromelanoma: a dermatology-led European campaign against nonmelanoma skin cancer and cutaneous melanoma. Past, present and future. Br J Dermatol. 2012;167:99–104.
• Stang A, Jöckel K-H. Does skin cancer screening save lives? A detailed analysis of mortality time trends in Schleswig-Holstein and Germany. Cancer. 2016;122:432–7. This manuscript offers valuable insights into the complexities of conducting large scale skin cancer screening to determine impact on melanoma mortality based on the SCREEN study in Germany, which is the largest skin screening effort undertaken to date.
McFarland SL, Schram SE. Physician skin examinations for melanoma screening. Cutis. 2015;96:175–82.
Kantor J, Kantor DE. Routine dermatologist-performed full-body skin examination and early melanoma detection. Arch Dermatol. 2009;145:873–6.
Sinclair R. Skin checks. Aust Fam Physician. 2012;41:464–9.
Mayer JE, Swetter SM, Fu T, Geller AC, Mayer SM, Swetter T, et al. Screening, early detection, education, and trends for melanoma: current status (2007–2013) and future directions: part I. Epidemiology, high-risk groups, clinical strategies, and diagnostic technology. J Am Acad Dermatol. 2014;71:599.e1–599.e12. quiz 610, 599.e12
American Academy of Dermatology Association. AADA provides input on skin cancer screening recommendation (Internet). Shaumburg, IL: American Academy of Dermatology Association; Jan 8, 2016 Available from: https://www.aad.org/media/news-releases/aada-provides-input-on-skin-cancer-screening-recommendation. Accessed Aug 17 2017.
• Johnson MM, Leachman SA, Aspinwall LG, Cranmer LD, Curiel-Lewandrowski C, Sondak VK, et al. Skin cancer screening: recommendations for data-driven screening guidelines and a review of the US Preventive Services Task Force controversy. Melanoma Manag. 2017;4:13–37. This manuscript is a comprehensive, data-driven review of skin screening and counseling techniques, specifically evaluating USPSTF scoring methods for skin cancer sceening in the context of how their scoring system has been applied to screening for other diseases (i.e. CT scans for smokers and lung cancer risk).
Weinstock MA, Ferris LK, Saul MI, Geller AC, Risica PM, Siegel JA, et al. Downstream consequences of melanoma screening in a community practice setting: first results. Cancer. 2016;122:3152–6.
Federman DG, Kirsner RS, Viola KV. Skin cancer screening and primary prevention: facts and controversies. Clin Dermatol Elsevier BV. 2013;31:666–70.
Watts CG, Madronio C, Morton RL, Goumas C, Armstrong BK, Curtin A, et al. Clinical features associated with individuals at higher risk of melanoma. JAMA Dermatol. 2017;153:23.
Wernli KJ, Henrikson NB, Morrison CC, Nguyen M, Pocobelli G, Blasi PR. Screening for skin cancer in adults. JAMA. 2016;316:436.
Stratigos AJ, Katsambas AD. The value of screening in melanoma. Clin Dermatol Elsevier Inc. 2009;27:10–25.
Torres A. AAD statement on USPSTF recommendation on skin cancer screening (Internet). Schaumburg, IL: American Academy of Dermatology; 2016 Available from: https://www.aad.org/media/news-releases/aad-statement-on-uspstf. Accessed 17 Aug 2017
Watts CG, Dieng M, Morton RL, Mann GJ, Menzies SW, Cust AE. Clinical practice guidelines for identification, screening and follow-up of individuals at high risk of primary cutaneous melanoma: a systematic review. Br J Dermatol. 2015;172:33–47.
Buster KJ, You Z, Fouad M, Elmets C. Skin cancer risk perceptions: a comparison across ethnicity, age, education, gender, and income. J. Am. Acad. Dermatol. Elsevier Inc. 2012;66:771–9.
Agbai ON, Buster K, Sanchez M, Hernandez C, Kundu RV, Chiu M, et al. Skin cancer and photoprotection in people of color: a review and recommendations for physicians and the public. J Am Acad Dermatol Elsevier Inc. 2014;70:748–62.
Cockburn MG, Zadnick J, Deapen D. Developing epidemic of melanoma in the Hispanic population of California. Cancer. 2006;106:1162–8.
Pollitt RA, Clarke CA, Swetter SM, Peng DH, Zadnick J, Cockburn M. The expanding melanoma burden in California hispanics. Cancer. 2011;117:152–61.
Clarke CA, Moy LM, Swetter SM, Zadnick J, Cockburn MG. Interaction of area-level socioeconomic status and UV radiation on melanoma occurrence in California. Cancer Epidemiol Biomark Prev. 2010;19:2727–33.
Miller KA, In GK, Jiang SY, Ahadiat O, Higgins S, Wysong A, et al. Skin cancer prevention among Hispanics: a review of the literature. Curr Dermatol Rep. 2017;6(3):186–95.
Guy GP, Ekwueme DU. Years of potential life lost and indirect costs of melanoma and non-melanoma skin cancer: a systematic review of the literature. PharmacoEconomics. 2011;29:863–74.
Sutton A, Crew A, Wysong A. Redefinition of skin cancer as a chronic disease. JAMA Dermatol. 2016;152:255.
Barton V, Armeson K, Hampras S, Ferris LK, Visvanathan K, Rollison D, et al. Nonmelanoma skin cancer and risk of all-cause and cancer-related mortality: a systematic review. Arch Dermatol Res Springer Berlin Heidelberg. 2017;309:243–51.
Center for Disease Control and Prevention. Skin Cancer: What screening tests are there? (Internet). 2017 Division of cancer prevention and control, Centers for disease control and prevention; Available from: https://www.cdc.gov/cancer/skin/basic_info/screening.htm Accessed 17 Aug 2017.
Melia J, Moss S, Coleman D, Frost T, Graham-Brown R, Hunter JAA, et al. The relation between mortality from malignant melanoma and early detection in the Cancer Research Campaign Mole Watcher Study. Br J Cancer. 2001;85:803–7.
Caini S, Boniol M, Tosti G, Magi S, Medri M, Stanganelli I, et al. Vitamin D and melanoma and non-melanoma skin cancer risk and prognosis: a comprehensive review and meta-analysis. Eur J Cancer. 2014;50:2649–58.
Warren GW, Kasza KA, Reid ME, Cummings KM, Marshall JR. Smoking at diagnosis and survival in cancer patients. Int J Cancer. 2013;132:401–10.
Stratigos A, Nikolaou V, Kedicoglou S, Antoniou C, Stefanaki I, Haidemenos G, et al. Melanoma/skin cancer screening in a Mediterranean country: results of the Euromelanoma Screening Day Campaign in Greece. J Eur Acad Dermatol Venereol. 2007;21:56–62.
Shellenberger R, Nabhan M, Kakaraparthi S. Melanoma screening: a plan for improving early detection. Ann Med. 2016;48:142–8.
St. Sauver JL, Warner DO, Yawn BP, Jacobson DJ, McGree ME, Pankratz JJ, et al. Why patients visit their doctors: assessing the most prevalent conditions in a defined american population. Mayo Clin. Proc. 2013;88:56–67.
Bradley HB. Implementation of a skin cancer screening tool in a primary care setting: a pilot study. J Am Acad Nurse Pract. 2012;24:82–8.
Lowe JB, Ball J, Lynch BM, Baldwin L, Janda M, Stanton WR, et al. Acceptability and feasibility of a community-based screening programme for melanoma in Australia. Health Promot Int. 2004;19:437–44.
Elwood JM. Screening for melanoma and options for its evaluation (see comment). J Med Screen 1994;1:22–38.
Youl PH, Baade PD, Parekh S, English D, Elwood M, Aitken JF. Association between melanoma thickness, clinical skin examination and socioeconomic status: results of a large population-based study. Int J Cancer. 2011;128:2158–65.
Wainstein A, Algarra SM, Bastholt L, Cinat G, Demidov L, Grob JJ, et al. Melanoma early detection and awareness: how countries developing melanoma awareness programs could benefit from melanoma-proficient countries. Am J Ther. 2015;22:37–43.
Quéreux G, N’guyen J-M, Cary M, Jumbou O, Lequeux Y, Dréno B. Validation of the Self-Assessment of Melanoma Risk Score for a melanoma-targeted screening. Eur J Cancer Prev. 2012;21:588–95.
Funding
This paper was supported in part by T32CA009492 from the National Cancer Institute and by R01CA158407 from the National Cancer Institute and the National Institute of Child Health and Human Development. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Epidemiology
Rights and permissions
About this article
Cite this article
Wojcik, K.Y., Escobedo, L.A., Miller, K.A. et al. Conflicts and Contradictions in Current Skin Cancer Screening Guidelines. Curr Derm Rep 6, 316–324 (2017). https://doi.org/10.1007/s13671-017-0205-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13671-017-0205-6