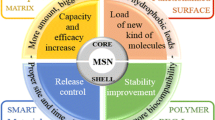
Abstract
The biocompatible nature of mesoporous silica nanoparticles (MSN) attracted researchers’ attention to deliver therapeutic agents in the treatment of various diseases, where their porous nature, high drug loading efficiency, and suitability to functionalize with a specific ligand of MSN helped to obtain the desired outcome. The application of MSN has been extended to deliver small chemicals to large-sized peptides or proteins to fight against complex diseases. Recently, formulation researches with MSN have been progressed for various non-conventional drug delivery systems, including liposome, microsphere, oro-dispersible film, 3D-printed formulation, and microneedle. Low bulk density, retaining mesoporous structure during downstream processing, and lack of sufficient in vivo studies are some of the important issues towards the success of mesoporous silica-based advanced drug delivery systems. The present review has aimed to evaluate the application of MSN in advanced drug delivery systems to critically analyze the role of MSN in the respective formulation over other functionalized polymers. Finally, an outlook on the future direction of MSN-based advanced drug delivery systems has been drawn against the existing challenges with this platform.
Graphical abstract

Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
For decades, researchers are exploring different drug delivery strategies to achieve better efficacy and safety via a suitable dosage form. The transition from the conventional dosage forms to a novel drug delivery system (NDDS) has crossed a long way. Various NDDS have conferred the term “advanced drug delivery system (ADDS)” due to their modified approach from conventional systems. Conventional formulations, tablets for oral administration, or a solution for intravenous administration has been encountered with various limitations like the requirement of high dosage, poor bioavailability issue, improper pharmacokinetic profile, unfavorable toxicities, and adverse effects. NDDS or ADDS could have the capacity to overcome these limitations of conventional deliveries [1]. The emergence of NDDS in the last two decades has been explored for the development of newer synthetic techniques with high-throughput screening in an ability to manipulate molecules for better performance [2, 3]. The objectives of most of the NDDS or ADDS include targeting the site of action, enhancement of systemic bioavailability, prolongation in the duration of action, enhancement of drug loading, specificity towards the target site, and safety concern of the users. Approaches to meet these objectives have brought to us targeted drug delivery systems, controlled drug delivery systems, and modulated drug delivery systems in modern formulation research. Not only are these approaches are confined within the laboratory but also several formulations have successfully reached the “bedside” for improved therapy [4].
Consequently, an increasing number of poorly aqueous soluble drugs within the list of new chemical entities (NCEs) create the major challenge of increasing solubility and dissolution in the aqueous medium, which needs to be addressed during formulation development, especially meant for oral delivery [5]. Approaches like reducing particle size, modification of the crystal habit, complexation, drug dispersion in a carrier, lipid-based formulation, and addition of hydrophilic excipients are some of the well-adopted techniques [6,7,8,9]. Whatever the novel delivery approached, the role of excipients is immense. Newer excipients or application of established excipients is being explored by the researchers. Moreover, a perfect excipient can promote drug solubility and dissolution, whereas, on the other side, it is expected to enhance the drug loading. It has always remained a thirst area in the excipient research while formulating a novel delivery for improved efficacy [10].
Mesoporous silica is considered as one of the popular excipients in increasing drug dissolution with a minimum required quantity [10, 11]. The mesoporous form termed “mesoporous silica” with the most popular type named MCM 41, SBA 15, and TUD-1 is now used widely in pharmaceutical research [12,13,14]. The point of difference between silica and mesoporous silica is its highly porous structure with a large number of empty channels which helps in the entrapment of bioactive molecules [15]. Here, in this review, a focus has been made on mesoporous silica as a suitable excipient for delivering drugs via different novel drug delivery platforms.
Mesoporous silica as an excipient
With drug loading being an important perspective of drug delivery, the excipient plays the role to entrap the drug within their structure; thus, there is a requirement of a suitable quantity of drug and carriers. Additionally, the premature release of the loaded drug during transportation within the biological system limits their application in several site-specific deliveries of therapeutics or peptides via oral routes of administration, as the peptides will be degraded in the gastric environment, whereas insoluble therapeutics might precipitate within the gastrointestinal tract. Emerging progress of NDDS towards the effective delivery of therapeutics or peptides urges the need for an effective excipient to accomplish both of the roles and high loading without premature release. Among various structurally stable components investigated for the purpose, silica materials were found to have suitable surface properties with a well-defined structure for drug delivery. The silica materials are usually biocompatible and are chosen to deliver therapeutic components using various nanocarriers [16,17,18,19].
Silica is regarded as a “generally regarded as safe” (GRAS) material, which can be readily surface-modified to optimize drug loading and subsequent release in the human body [20]. Mesoporous silica possesses unique characteristics of huge pore volume (> 0.9 cm3 g−1) and high surface area (> 900 m2 g−1), where the pore size of the particles could be adjusted [2]. These unique structures of mesoporous silica allow the loading of a high amount of drug, where the final requirement of the carrier is less. Mesoporous silica nanoparticle (MSN), under its advantageous properties, attracted more attention and has been intensively investigated for targeted drug delivery. Various distinctive properties of MSN, like substantial surface area, large pore size, nontoxicity, biocompatibility, biodegradability, low density, adsorption capacity, capacity for encapsulation, chemical and thermal stability, even distribution of target molecules on the porous space, controllable superficial charge, and free distribution in the whole body, have indicated its multifunctional usage in drug delivery systems [21,22,23]. The particle size of MSN is tunable at a range of 30–500 nm, granting effortless endocytosis by living creatures beyond any compelling cytotoxicity [3]. The pore size can be controlled at 2–8 nm by using different soft templates, and the pore structure can have a 2-dimensional cylindrical structure or interconnecting structure [24, 25]. Both of the large internal and external surfaces of MSN can be modified and functionalized with different moieties. The differentiating point of MSN from many other inorganic nanomaterials is the low toxicity potential. The indication of low or no toxicity was established by the in vitro studies on the healthy and cancer cell lines [26].
There are various grades of MSN available to use in drug delivery systems. It belongs to four major different MSN families like M41S (MCM-Mobil Crystalline Materials), SBA (Santa Barbara Amorphous), KIT (Korea Advanced Institute of Science and Technology), and COK (Centre for Research Chemistry and Catalysis). All of these different families have different types of MSN with varying pore sizes, pore volumes, and pore dimensions. MCM-41, MCM-48, and MCM-50 belonging to the M41S family have pore sizes of 2.5–4.5 nm, 2–5 nm, and 2–5 nm in diameter, respectively. SBA-11, SBA-12, and SBA-15 belonging to the SBA family have pore sizes of 5–15 nm, 1–3.1 nm, 5–15 nm, and 5–15 nm in diameter, respectively. KIT-5 belonging to the KIT family has a pore size of 1–9.3 nm in diameter. COK-12 belonging to the COK family has a pore size of 6–9 nm in diameter. Readers can find a detailed account of MSN grades in a comprehensive review by Narayan and team [27].
Advancement of MSN in drug delivery from its inception
The structures of mesoporous silica have become familiar to material scientists for 40 years. However, the origin of mesoporous silica was recorded by patenting an unknown compound producing it around 1970 [28, 29]. The first independent synthesis of mesoporous silica was achieved in 1990, which was conducted by researchers in Japan. Later in 1992, it was synthesized by Mobil Corporation Laboratories, where it was named as “molecular 41 sieves” (M41S) [30]. Since the M41S family of ordered mesoporous silica was first reported in the early 1990s [31], the number of studies on MSN was extensively increased, the outcome of which, in 1995, depicted the development of new families of mesoporous silica material like Santa Barbara Amorphous (SBA) [32], mesoporous MSU [33], and FSM [34]. In subsequent research, silica nanoparticles with much larger (4.6 to 30 nm) pores were developed by the University of California in 1998, which was designated as Santa Barbara Amorphous type material, or SBA-15. This was indeed a research gambit in mesoporous material development [32]. The researchers used this SBA-15 as molecular sieves owing to the well-defined and uniformly sized pores, larger surface area, high hydrothermal and thermal stability, and functionalization facility with metal oxides [35]. Concurrently, in 1998, a patent expressing the loading of pharmacologically active substances in mesoporous silicates to be used as drug delivery devices was filed [36] and again speculated upon by another group [37] in 1999. Later in 2001, Balkus and colleagues developed the first MSNs with the capability to release a drug molecule within the physiological conditions [38]. The hexagonal mesoporous silica material used was defined as Dallas Amorphous Material-1 (DAM-1). This research propelled the development of MSNs about the drug delivery platforms. Since its inception, MSNs have been extensively used for biomedical applications, specifically photodynamic therapy [39, 40], cell tracking [41], controlled drug release [42, 43], and tumor targeting [44].
The reports related to the adsorption of drugs onto silica-based materials since the 1970s became the pathfinder for Vallet-Regi et al. in 2001 that instigated the interest in MSN as a controlled drug delivery system [45]. The capability to load and control the release of ibuprofen for more than 3 days through MCM-41-based MSNs had reshaped the prospective applications of MSNs in biomedical engineering and nanomedicine which remarkably increased the scrutiny of scientists. The potential application of MSN in drug delivery was then focused on developments on mesoporous silica-based immediate release drug delivery systems (IDDSs), sustained drug delivery systems, stimulus-responsive controlled drug delivery systems (CDDSs), and targeted drug delivery systems (TDDSs) [46]. Additionally, these MSNs had also been widely incorporated in conventional drug delivery systems, such as tablets and capsules [47]. MSNs in both modified and unmodified forms have been explored for controlled drug release, where the sustained drug release utilizing unmodified silica was attained by controlling the pore structure, pore diameter, and particle size of the carrier. The modified silica materials conjugated to silanes and the interactivity between functional groups and the drug molecules were reported to prolong drug dissolution from MSNs (e.g., resveratrol [48], telmisartan [49], carbamazepine [50], curcumin [51], paclitaxel [52], and others [53, 54]), and it also produced a prolonged sustained release. With increasing research, the application of MSN has been more focused on functionally targeted drug delivery to the cancer cells through modification of the pore openings, where more advanced devices are approached with the stimulus-responsive release of entrapped therapeutics wherein the release of the drug could be set off with regards to its environmental changes [55,56,57,58]. Amid a range of drug-delivery systems, mesoporous silica materials persist attractive features for use in the delivery of water-insoluble drugs, where it can serve as a reservoir of the hydrophobic drugs with its large surface areas and porous interiors [59, 60]. Further, groups of researchers developed spherical MSNs for the immediate release of drugs [61, 62]. When correlating with various types of carriers as IDDSs, MSNs’ large surface area and high pore volume provide the advantages for being promising IDDSs. MSN-based CDDSs had been developed by implementing controls like “gatekeepers.” Only when the drug-loading system is revealed to external impulse does it trigger the withdrawal of the “gate,” and the drugs leak out from silica carriers releasing the drug in a controlled manner. Among the stimuli, like pH, temperature, magnetic field, and ionic strength glucose, pH-responsive CDDSs have been extensively explored as pH gradients are available in various tissues and subcellular compartments [63]. MSNs have also been developed as potential candidates for TDDS, where the MSNs with the nanoscale range particles could accumulate in the tumor microenvironment via the enhanced permeation and retention (EPR) effect and deliver the entrapped drug from the TDDS [64, 65].
During the last decade, the potential use of MSN has created thrust in the most attractive areas of nanobiotechnology and nanomedicine for various disease diagnosis and/or therapy, including bone/tendon tissue engineering, infectious diseases, diabetes, inflammation, and cancer [3, 60, 66,67,68,69,70,71,72]. With increased drug loading capability and the possibility of active targeting and stimulus-responsive delivery, the application of MSNs has been investigated within several areas of the biomedical field [46]. The advantage of utilizing MSNs went beyond the enhancement of poor water solubility, generally seen among anticancer therapeutics. MSNs have also been explored to act as therapeutic agents, in the case of photodynamic therapy, as an alternative to radio- and chemotherapy. To achieve improved efficiency of the MSN-based treatment strategies, for increased cancer cells specific uptake and selectivity, photosensitizers could be tagged to the MSNs while functionalizing them with mannose. The outcome was relatively higher in vitro photo-efficiency in MDA-MB-231 cancer cells by mannose-dependent endocytosis compared with the un-functionalized MSN [73]. Recently, MSNs have been investigated for infection treatment as well, where, MSNs’ delivery systems are easily adapted to combination therapies for successful antibiotic treatment [74]. MSNs for siRNA delivery has also made an edge in recent times. MSNs can potentially deliver siRNA into the cells to permit gene silencing, where the MSNs demonstrate support in siRNA delivery by generally hurdled by low transfection ability and short half-life [75].
A few review articles on the application of MSN in the drug delivery system are available in the literature [22, 76,77,78]. However, the scope and application of MSN in NDDS have rarely been addressed despite a handful of research works. As the applications of MSN have been extended widely portraying the use of MSN in NDDS or ADDS [25, 54, 79]; the objective of the present article is to evaluate and summarize the applicability of MSNs in NDDSs, including liposomes, microspheres, hydrogels, dendrimers, erythrocytes, magnetic microparticles, and advanced technology like 3D printing. The connecting section of this review has emphasized different types of drug delivery systems that could be approached using MSN.
Novel drug delivery systems using MSN
In 1992, Kresge and team developed the surfactant-templated mesoporous silica using a liquid-crystal “templating” platform [80], which has opened up its exploration in preparation and utilization of these mesoporous components via functionalization of the materials to obtain micron to submicron size range [81, 82]. The first use of mesoporous silica for drug delivery was done by a group of researchers in 2001 [45]. Following these researches, advancement has been made in the therapeutic application of the MSN to obtain advanced drug delivery with the desired potential.
Mesoporous silica in microspheres
Microspheres are spherical microparticles with a diameter in the micrometer range (1 to 100 µm), composed of various polymers. They can encapsulate drugs or therapeutically active molecules for controlled or sustained release with improved bioavailability and biocompatibility [83]. The formulation of microspheres offers myriad opportunities for the desired release of a therapeutic molecule onto a targeted site [84]. The advantage that the microsphere offers over other formulations is its provision of stability for unstable compounds [85, 86]. Various polymers could be incorporated in formulating microspheres (e.g., albumin, gelatine, modified starch, polypropylene, dextran, polylactic acid, polylactide-co-glycoside, etc.), which are either biodegradable or non-biodegradable and could be incorporated according to the design of the experiment [87]. Recently, MSNs are incorporated within the configuration of the microspheres to impart its promising characteristics like large specific surface area, good biocompatibility, and easy functionalization with the presence of many Si–OH groups on the surface [24]. Among various methods employed to formulate mesoporous incorporated microspheres, the surfactant-assisted method was found to be the most popular one [88]. With the increasing number of NCEs with low half-life or to prolong systemic exposure of existing drugs with a shorter half-life, it is an urge to formulate drug delivery with a controlled and sustained release manner. The formulation of microspheres is a way not only to control the release of the drug but also to modulate various physical properties of the drug. In some researches, it had been observed that MSNs are entrapped within the core material with coated polymer, which forms a shell and ultimately resulting in the development of microspheres [89].
MSN in alginate microsphere
A study by Song and the team reported the development of a microsphere using SBA-15 and sodium-alginate, which were finally cross linked with calcium chloride. However, they applied the mesoporous-coated microspheres in the efficient removal of lead (Pb(II)) from water, where they have also shown that the microspheres could be regenerated and reused at least six times [90]. Another report formulated the mesoporous silica nanospheres following the organic template method, where the researchers modified the structure with aminopropyl groups for functionalization. Indomethacin was incorporated within the microsphere through ionic interaction, which had revealed a sustained release of the drug from the microsphere. This sustained release was predicted by the fact of blockage of the drug by the coated layer of alginate [91].
An advanced microsphere formulation composed of MSN and alginate was reported by Liao and team, where the authors reported the advantage of high drug loading due to the presence of MSN [92]. The excellent biocompatibility of the formulation and the –COOH group functionality for the specific binding property of alginate was achieved for the treatment of liver cancer [92]. Due to the course of the study, rhodamine 6G–loaded MSN-encapsulated alginate (MSN-Alg) microspheres for sustained release were studied for targeted treatment of lung cancer therapy. Air dynamic atomization was used to fabricate MSN-Alg microspheres. The developed MSN-Alg microspheres exhibited sustained release features, excellent biocompatibility, enhanced drug release efficacy, and good drug loading capacity. Several therapeutic and diagnostic molecules, anticancer drugs, and organic dyes were loaded efficiently into MSN and released via controllable kinetics. Due to the high surface area of MSN, doxorubicin (DOX) or Rhodamine 6G could be loaded competently, and afterward, it was introduced into alginate for gelation. After optimization of the reaction conditions of atomization, microspherical morphology was obtained within the desired quality, where the release behavior of the entrapped component was converted from the typical zero-order to first order. Further modification of the microsphere with the arginine–glycine–aspartic acid (RGD) ligand on the surface has shown to possess the potential to target αvβ3 receptor overexpressed cancer cells. The schematic illustration of this research is shown in Fig. 1. [92]. Thus, it can be said that the MSN-Alg microsphere could be used in the pharmaceutical formulation for its noteworthy potential as an efficient transmembrane delivery system for intracellular controlled release of cell membrane-impermeable drugs.
Illustration representing the drug-adsorbed mesoporous silica nanoparticles (doxorubicin-MSN) encapsulated into RGD-containing peptide functionalized alginate microspheres. Reproduced with permission [92]
MSN with thermo-responsive polymer
A group of researchers synthesized novel microspheres by coating the magnetic mesoporous silica with a thermosensitive polymer. This strategy combining the advantage of the thermo-sensitive ((P(NIPAM-co-N hydroxyl methyl acrylamide) (P(NIPAM-co-MAA)) copolymer on the outer shell, mesoporous silica as the sandwiched layer, and Fe3O4 magnetic nanoparticle acting as the core was developed to form a controlled release microsphere system. Such explicit composite microspheres (core/shell) are assuring for payload and temperature-triggered release of the chosen components. This could be led by the applied magnetic field and perceive the release of therapeutic agents at the target specific sites. Volume phase-transition temperature (VPTT) and the behavior of the temperature-sensitive drug release was affected by the content of the hydrophilic co-monomer. The results depicted that the drug release behavior was dependent on the temperature with a close correlation with the VPTT, whereas above the VPTT, the drug release rate was much faster than that of below the VPTT, demonstrating potential application in tumor therapy [93].
A dual stimulus-sensitive (thermal and pH responsive) core–shell composite microsphere was reported by Chang et al. (2011) [94]. The researchers used the same thermo-responsive copolymer (P(NIPAM-co-MAA) as used by the previous group of researchers. The composite microsphere showed a thermal/pH-coupling sensitivity, and the volume phase transition could be correctly controlled by the molar ratio of methyl acrylic acid to NIPAM. It was found that the composite microsphere could, in principle, be utilized for cancer treatment with the fast release of the drug upon arriving at tumor sites and a very low premature drug release during blood circulation.
Not only as a microsphere, but a stimulus-sensitive MSN-based system (nanoparticles within the size range of 255 ± 28 nm) was also developed using PNIPAM-based polymer [95]. A notable example is the work of Tian et al. (2018), where the chemo- and magnetic hyperthermia platform was created by the P(NIPAM-co-MAA) copolymer [95]. P(NIPAM-co-MAA) was found to regulate the release of entrapped drug within the mesoporous silica through the gatekeeper control mechanism.
The benefits of the high drug storage capacity of mesoporous carrier and the aspect of stimulus-sensitive controlled release could be well combined through the use of temperature-sensitive thermo-responsive polymer, where additional control will potentially enhance the control of drug delivery.
MSN in a pH-responsive microsphere
In cases of anticancer treatment, it is always beneficial to formulate a targeted drug delivery system to the cancer cells and to release the drug in a controlled manner. It has been established that the cancer tissues usually contain acidic pH than normal tissues. Hence, targeting a way to release the drug only at a particular change in the pH will reduce the drug distribution at the normal tissue sites; thereby, we can approach delivery at cancer tissue sites [96].
A study proposed a way to apply the property of mesoporous silica as an efficient drug carrier with a polymer, which showcased pH responsiveness for the drug release. Wen and the team proposed a method to formulate pH-responsive microspheres of magnetic MSN. It consists of the ferric oxide (Fe3O4) nanoparticle as the core with MSN as a middle layer and cross linked poly(methacrylic acid) (PMAA) as the outer shell. The drug was stored in the mesoporous silica layer, and the core Fe3O4 was responsible for the magnetic response whereas the outer layer of PMAA endowed the pH-responsiveness. DOX was chosen as the model drug to understand drug storage and release behavior. In tumor therapy, the pH-responsive composite microspheres with MSN were found to be intriguing candidate carriers with a faster drug release rate below its pKa [97].
In another novel strategy, thermosensitivity and pH sensitivity were depicted by a volume phase transition, which indicated the transition of the microsphere from the swollen state at the physiological condition to collapsed state at tumor sites. The collapsed state moderated the active release of the drug at that site [21]. A microsphere with MSN was engineered in a way to reciprocate to the slightest difference in temperature/pH existence between healthy tissue and tumor tissue in the physiological surroundings. With DOX as a model drug, the authors proposed a way to synthesize a temperature/pH-sensitive microsphere made with MSN as a core to control the premature release of the DOX in the bloodstream. Here, magnetic MSNs were employed as the core and the outer shell consisted of cross-linked poly(N-isopropyl acrylamide-co methacrylic acid) polymer. Below VPTT, a composite microsphere loaded with DOX indicated a lower degree of leakage with a thermal/pH response–controlled drug release. A rapid drug release upon reaching the reduced pH 6.5 and 5.0 followed by a very low release at pH 7.4 has proven the microsphere to be a multi-pH-responsive smart drug delivery system [21]. Additionally, to control the release of the entrapped DOX from the MSN, α-cyclodextrin was incorporated as a gatekeeper, where multifunctional ligand, RGD peptide, was attached to it for targeting purposes. The red fluoresces in Fig. 2a (2) and b (2) indicated the internalization of the formulation in COS7 and HeLa cells, respectively. A comparative higher uptake of the formulation in HeLa cell could be explained by the overexpression of αvβ3 and αvβ5 [98]. Pre-incubation of the cells with RGD peptides had shown extremely low uptake of the formulations by the HeLa cells in Fig. 2c (2). Further, the absence of any barrier in free DOX resulted in a similar pattern of internalization of DOX in both the experimental cells (Fig. 2d (2) and e (2)). It would be important to mention that the exposure-free DOX resulted in higher internalization to the HeLa cells as shown in Fig. 2e (2), whereas it is less from the developed formulation (Fig. 2b (2)), which could be explained by the fact of a higher rate of concentration gradient diffusion than the process of endocytosis [21]. In this way, the major limitation of the absence of selectivity towards anti-cancer drugs could be addressed.
Confocal scanning laser microscopic results. Incubation of COS7 a and HeLa cells b with the surface engineered DOX-loaded mesoporous nanoparticles. Incubation of HeLa cells with RGD and surface engineered mesoporous nanoparticles. Incubation of COS7 a and HeLa cells b with the free-DOX. Reproduced with permission [21]
MSN with grafted polymer in the nanoshell
Grafting of a copolymer with MSN backbone could be used to develop a specially designed microsphere. A grafted copolymer can be attached to an MSN structure to form a stimulus-responsive nanoshell, such as pH-sensitive nanoshell. This nanoshell perhaps can be opened and closed reversibly with triggered pH because of its pH sensitivity. Consequently, the uptake and release of therapeutic agents could be completely controlled through the pH-stimulated reversible opening and closing. A group of researchers developed a microsphere using MSN, which was modified by RAFT polymerization for the grafting of the poly(acrylic acid) (PAA) nanoshell onto the MSN container [99]. PAA, being pH-sensitive, i.e., soluble at pH 8.0 and insoluble at pH 4.0, gave rise to an agile microsphere with a nano valve for smart uptake and release of the therapeutic agent from the “MSN container.” “MSN container” is the term indicated for a drug-loaded mesoporous silica nanocarrier. The pH-sensitive nanoshell was grafted by surface reversible addition-fragmentation chain transfer (RAFT) polymerization of acrylic acid onto the external surface of MSNs by an efficient free radical polymerization method [100]. This method is very efficient in regulating the polymerization of “smart” polymer chains and functional monomers, including polyelectrolytes, which are grafted on the surfaces of carbon nanotubes, nanospheres, and wafers by surface RAFT polymerization [100,101,102,103]. The mechanism of action of the smart microsphere is that, at comparatively elevated pH (pH 8.0), more or less all of carboxylate groups of the PAA nanoshell are deprotonated, and it becomes soluble in an aqueous environment, leading to an “open” nanoshell, whereas at pH below 4.0, its solubility becomes poor and the insoluble PAA nanoshell crashes onto the external surface of MSN, developing a “closed” and compact nanoshell. Thereby, an innovative smart nanocontainer with MSN as the drug-loaded matrix and a pH-triggered polymeric nanoshell as the nano valve could be attained.
Mesoporous silica-based hydrogels
The issues referring to the systemic toxicity and higher dosing frequency limit conventional drug delivery approaches. Hydrogels pave the way for convenient drug delivery vehicles to make sure these disadvantages are underrated with the desired therapeutic efficiency of the drug. With extensive modifiable physical properties rendering the controlled drug release, hydrogels have made their mark as effective drug delivery systems [104]. Any swellable hydrophilic polymer, extended with a wide range of chemical compositions and bulk physical properties, can effectively be used to make hydrogels. Hydrogels are further formulated into various physical forms, such as films, injectables, and nanoparticles. MSN-based delivery vehicles are built to achieve endocytosis and follow stimulus-triggered bursts of drug release from hydrogel [104]. MSN can formulate a high drug-loaded stimulus-responsive sol–gel system with a combination of a gelling polymer. It offers to prolong retention of the formulation on the delivery site as well as targeted stimulus-sensitive release. The specific properties of a hydrogel such as a 3-dimensional cross-linked network and a high amount of water content are designed for the restriction of the nanocarrier movements from the target site, but it also makes sure that there is no hindrance for the release of small drug molecules. Taking these points into account, MSN can be a valuable addition to the hydrogel system with its exceptional properties.
In the hydrogel-based system, MSN is used as a drug “container.” By its porous structure, it can hold a high amount of drug within its 3-dimensional structure. Such drug-loaded MSN forms nanocomposite with hyaluronic acid, where DOX and gold nano bipyramids were enclosed within the hyaluronic acid network at the cancer site. Upregulation of hyaluronidase production at the cancer site was found to result in a release to produce a theranostic approach [105]. Alternatively, an electro- and pH-responsive hydrogel system was developed using chitosan by Zhao and the team, where they incorporated ibuprofen with embedded MSNs [106]. The tunable release characteristics of the incorporated ibuprofen were found to pH and electric condition-dependent. The release of drug from the formulation at different pH was reported to be near the zero-order profile (Fig. 3). Release of ibuprofen from the MSN at basic pH (pH 7.4 and pH 10) is faster because of the low solubility of the drug in an acidic environment (Fig. 3a), whereas the release pattern of the drug from the MSN-hydrogel demonstrated a linear behavior (Fig. 3b) [106]. When these in situ hydrogel-forming systems become localized inside the targeted tumor tissue, the MSN payloads are released. Due to the hydrogel nature, the system retains on the delivery site for a longer time and controlled drug release from MSN “container” could be possible.
Cumulative release profiles of ibuprofen from a ibuprofen-MSNs and b chitosan/ibuprofen-MSNs in different pH buffers. Error bars showed standard deviations among triplicate experiments. Reproduced with permission [106]
A chitosan/MSN composite hydrogel was formed by using chitosan as a hydrogel-forming polymer to target antimicrobial therapy [107]. Hypothesized with the ability of MSN to load drug and release over a period, the introduction of MSN into chitosan will also increase the gel mechanical strength. MSNs were loaded into injectable chitosan to develop the chitosan/MSN composite hydrogels. The results depicted that the gelation procedure at body temperature was hastened and a rise in the elastic modulus G0 from 1000 to 1800 Pa was observed. When bovine serum albumin (BSA) and gentamicin are used as model drugs, the sustained release was observed from the CS/MSN hydrogel.
MSN in self-healing hydrogel
The increased research in hydrogels with their unique property has given rise to self-healing hydrogels. The optimal self-healing hydrogel must have high mechanical strength with instant rapid self-healing property, occurring within seconds of a wound. The faster the self-healing occurs, the better it is in most cases. Usually, faster self-healing is desired with hydrogels. With large pore volume, high specific surface area, morphology, and controllable particle size, hydrogels are considered to be effective in the healing process. MSNs have been broadly used not only to promote drug release but also in the adsorption of the drug at the site. Hence, the applicability of the MSNs will efficiently enhance self-healing characteristics. Following this, Rao and the team had reported a double network self-healing Alg/guar gum (GG) hydrogels consisting of polydopamine (PDA)-type microcapsules using MSN [108]. Glutaraldehyde (GA) was loaded within the stellate mesoporous silica (STMS) and was encapsulated with PDA to regulate the release of GA as a cross linking agent. The microcapsules (STMS-GA@PDA) were incorporated within the hydrogel to facilitate the formation of a double self-healing system of GG/sodium Alg. The self-healing and mechanical properties were remarkably improved by the union of GA and metal-ligand interactions between Fe3+, PDA, and sodium Alg. The network reformation and energy expenditure are the results of the reversible non-covalent bond formed. Therefore, the healing ability and tensile strength of self-healing hydrogels can make a remarkable difference in the performance.
Mesoporous silica-based orodispersible films
Orodispersible films (ODF) act as surrogates for conventional capsules and tablets to avoid the difficulty of swallowing, as ODFs are intraoral dosage forms facilitating instant dissolution/disintegration. The main crack point of ODF is the remarkably fast dissolution of the film. MSN can be efficiently used as a booster for dissolution with the constrained effect rendered by the molecularly sized (2–50 nm) pores to avoid the crystallization of loaded drug molecules.
Using the tunable feature of MSN making it an appropriate candidate as a solubility enhancer and drug carriers, Karaman and the team proposed a technique to come up with MSNs-incorporated ODF formulations for improved drug dissolution [109]. MSN, an excipient, resulted in the instant release of drugs from the ODF, wherein 90% of the drug could be released in the initial few minutes itself (Fig. 4). The improved mechanical characteristics of the resulting film were accompanied by the loading enhancement [109]. The opportunity of the delivery of poorly water-soluble drugs with more precise dosing with the use of MSN in the ODF could be an attractive approach to future researchers.
Relative drug release percentage from MSN incorporated ODFs. Reproduced with permission [83]
Mesoporous silica nanoparticle in liposomal drug delivery
Hybrid structures of liposome and mesoporous silica have been progressed extensively in pharmaceutical drug delivery. A combination of liposomal structure with the MSNs has several advantages of increased loading capabilities of the drugs with retention and biocompatibility in one drug delivery platform [110]. With the mesoporous silica core, the articulateness of the lipid bilayer is well defeated, and the composite nanoparticle can concurrently load numerous drugs, which remarkably enhances the drug loading scope. Along with the great biocompatibility and hassle-free surface functionalization of liposomes, it can also release drugs efficiently and in a controllable manner. The mesoporous silica nanoparticle-supported lipid bilayer is generally termed as “protocells,” which collectively combines attributes of both mesoporous silica particles and liposomes to manifest various attributes of a perfect targeted therapeutic delivery [111]. With the concern that liposomal carriers might fail in improving the safety of highly toxic drugs, using a hybrid lipid bilayer with MSN could be developed to obtain a stable, efficacious, and safe carrier. In this way, the composites could overcome a series of problems such as low solubility, limited stability, and poor bio-distribution. A recent patent on MSN with lipid bilayer coating for cargo delivery was approved in the USA [112].
A pH- and thermo-dual stimulus-responsive drug carrier based on MSN encapsulated in copolymer-lipid bilayers was developed as a trigger-sensitive drug delivery carrier [113]. Not only does the application of this concept lead to high drug loading capacity but also a sustained release effect was achieved which was reinforced by the MSN. A group of researchers developed a triple-model imaging-guided synergistic cancer therapy tool based on liposome-conjugated MSN [114]. In another study, DOX-loaded MSN-supported lipid bilayers were developed by Yang and team [115]. MSNs have now been successfully employed as platforms in bioimaging and delivery of the anticancer drug in the nanomedicine field. A polymer-lipid backed MSN was developed to enhance the antitumor efficacy by aiding intracellular delivery of an anticancer drug [116]. In this study, an anticancer agent irinotecan was incorporated within the polymer-lipid combined layer-coated MSNs to protect and retain the guest molecules within the complex structure until it reaches the site of action. At the cancer site, the drug was found to be released upon disruption of the coated layer within the cancer cells following internalization. Thus, it could minimize exposure to normal healthy cells as well as toxic manifestations (Fig. 5) [116].
Schematic illustration of the cooperation between responsive intracellular storm release of irinotecan and the ability to overcome drug resistance by blocking the efflux transporter. Reproduced with permission [116]
A similar approach was aimed at using a custom-designed MSN platform to reduce the toxicity of irinotecan, which was then used as a proton gradient for high-dose irinotecan loading across a coated lipid bilayer. By this approach, it was made possible to improve the stability of the carrier, allowing minimum drug leakage systemically with improved drug retention at the tumor sites [117]. Another approach was made to obtain hemoglobin (Hb)-loaded MSNs. These Hb-loaded MSNs were then coated with a lipid bilayer (LB-MSNs) which was then investigated as an erythrocyte mimic. Concerning MSNs’ large pore size, it acted as a rigid core and provided a protective surrounding for Hb encapsulated within the pores [118].
A group of researchers described the synthesis and application of PEGylated liposome-coated quantum dots/mesoporous silica core-shell nanoparticles for molecular imaging [119]. Besides, MSN-supported-lipid bilayers, termed “protocells,” represented a potential therapeutic and theranostic delivery [111]. The use of a lipid-coated MSN platform for synergistic gemcitabine and paclitaxel delivery to human pancreatic cancer in a mouse model was well investigated, and positive outcomes were documented [120]. Apart from MSNs, the studies with mesoporous silica were also progressed to form a hybrid structure with liposome for improved efficacy and safety. In research work, the liposome was fused to silica cores followed by the lipid exchange between silica-supported bilayers and oppositely charged free liposomes, in turn reducing the bilayer defects, allowing cargo retention, delivery, and release intracellularly [121]. Extension of their research had shown that the fusion of a positively charged liposome with a negatively charged mesoporous silica core synergistically load and seal a negatively charged drug inside the core [122]. This platform showed advantages in cargo loading, delivery, and release over other nanoformulations, which made it a useful vector in the delivery of therapeutics under the umbrella of nanotechnology.
Mesoporous silica-based microneedle delivery
Microneedles (MNs) are hypodermic needles like delivery system within micrometer size (25–2000 µm) [123], whereas the conventional hypodermic needles are about 6–8 mm in length. Usually, the length of the MNs is as long as the width of a hypodermic needle. These MNs allow the transportation of larger and/or hydrophilic molecules by forming microscopic holes in the skin and penetrating through the stratum corneum to deliver drugs into the epidermis [123]. It reaches the epidermis but not the nerve endings, being painless. As this painless delivery allows the transportation of drugs, these are more accepted by the patients than the delivery by a hypodermic needle [124]. This demonstrates that the array of MNs should be strong enough to create the microscopic holes in the skin for the permeation of drugs but not long enough to reach the nerve endings causing pain. As the skin consists of a large number of antigen-presenting cells, the microneedle-mediated intradermal delivery of vaccines has great capability for efficacious vaccine delivery. MSN has achieved huge attention to vaccine delivery because of its controlled size and mesostructured, excellent in vivo biocompatibility, and high loading capacity.
Antigen-loaded MSN microneedle
The modified and functionalized high surface of mesoporous silica helps in effective loading of antigens, where research had proved that antigen-loaded MSNs are capable of enhancing immune responses in experimental mice and augment the uptake of antigens by antigen-presenting cells [125].
Intradermal delivery of diphtheria toxoid (DT) loaded within the MSNs through the use of either a single hollow microneedle or coated microneedle array platform has been recently reported in the literature. The researchers loaded the DT in MSN, and the lipid bilayer (LB) was used to coat the nanoparticle surface (LB-MSN-DT), which was again coated layer by layer on a microneedle array [125]. The antibody response in ex vivo human skin, induced by LB-MSN-DT-coated microneedles, was analyzed after injection of a suspension containing LB-MSN-DT using hollow microneedles. With the aid of MSNs’ higher drug loading, the researchers showed that LB-MSN-DT persuades distinctly greater total IgG and IgG1 titters when compared with a solution of plain DT. When coated microneedles were inserted into the skin, the multiple insertion approach of the applicator more effectively improved the release efficacy of the coating compared with the single-insertion approach [125].
Doxorubicin- and indocyanine green–loaded microneedle
Many reports have shown that MSN is an effective protectant of indocyanine green (ICG). The protective role of MSN includes protection from high plasma protein binding, photo-thermal degradation, aqueous instability, and diminution of photo-thermal therapy (PTT) efficiency because of irreversible degradation and aggregation of ICG in blood plasma or the aqueous solution [126,127,128].
Taking into account ICG instability, Pei and the team used MSN as carriers for protecting it for PTT, photodynamic therapy, and in vivo imaging, which was loaded onto microneedle for evaluating anticancer efficiency. They fabricated ICG and DOX-loaded microneedle patches (PVP@DOX/MSN@ICG) for a combination of PTT and chemotherapy [129]. Here MSN was used to circumvent the reduction of PTT efficiency and improve in vivo ICG stability. Dissolving microneedle patches were used as therapy for superficial tumors with the combination of PTT and chemotherapy. The dissolution of microneedle tips in the interstitial fluid released DOX and ICG when it was applied at tumor sites. As depicted in Fig. 6, the temperature of the tumor site was raised through the topical administration of the PVP@DOX/MSN@ICG microneedle patch to the experimental animals. It is important to mention that the rise of temperature in the PVP@MSN microneedle patch was changed slightly, indicating the potential of PVP@DOX/MSN@ICG microneedle patches in the treatment of cancer. This was further demonstrated by the in vivo anticancer effect of the formulations in tumor-induced mice (Fig. 6c) [129].
Microneedle patches increased the topical temperature in tumors. a Representative images of infrared thermal camera in topical temperature of tumors. b Continuous temperature of tumors after treatment. c Antitumor effects of PVP/MSN, PVP@DOX/MSN, PVP/MSN@ICG, and PVP@DOX/MSN@ICG microneedle patches. Reproduced with permission [129]
The researchers had pointed out that due to the presence of negatively charged groups on both carriers (MSN) and the molecule (ICG) of interest, sufficient loading of ICG into MSN mesopores was not easy. Therefore, there was a need for MSN surface modification with amino groups to develop a surface with a positive charge, facilitating the binding of negatively charged ICG to MSNs via electrostatic interactions. In vivo studies and in vitro cell studies on human osteosarcoma MG-63 cells depicted that PVP@DOX/MSN@ICG MN patches showed an effective antitumor effect with the synergistic effects of chemotherapy and PTT for the treatment of superficial tumor [129].
MSN microneedle for insulin
The precise incorporation of the host-guest complexes constructed by cyclodextrins and the hydrophobic “guests” onto MSN often lets the development of complex hybrid structures with predefined properties. Xu and the team presented an innovative microneedle delivery device unified with insulin-loaded and H2O2-responsive MSNs. This was developed to obtain instant and painless administration of insulin [130]. For the loading of glucose oxidase (GOx) and insulin into the structure of MSN, the authors reported that modification of MSNs with 4-(imidazolyl carbamate) phenylboronic acid pinacol ester (ICBE) would be required. GOx loaded in the MSNs could transform glucose into gluconic acid and produce hydrogen peroxide (H2O2). The phenylboronic ester on the surface of the MSNs could be oxidized in the existence of H2O2. This could be resulted in the abolition of host-guest complexation, resulting in the de-assembly of the drug-loaded MSN and subsequent release of the preloaded insulin. The microneedle released insulin in vivo as a response to H2O2 stimuli and glucose. This has been established as an efficient drug delivery system in the treatment of diabetes. This H2O2-responsive artificial microneedle system can be successfully applied as an effective platform for delivering various therapeutic drugs to treat other diseases as well [130].
Mesoporous silica-based 3-dimensional printed drug deliveries
Nowadays, digital (2-dimensional and 3-dimensional) printing technologies are in the focus for the design and manufacture of pharmaceuticals by deposition of various solid materials, semi-solid and liquid consisting of one or several APIs [131,132,133,134]. Printing technologies used to manufacture personalized doses offer myriad opportunities in the drug delivery systems. Customization of the medicine following the patient’s specific needs and the pliability in production volumes makes up for the decentralized production of pharmaceuticals. The individual treatment solutions offered by 3D printing is expected to have even closer coordination between researchers and industry to improve this new manufacturing approach that can facilitate flexible dose adjustments, based on the patients’ need [135]. MSN has been reported for printing using inkjet printing soft-lithography as a top-down method for the formation of micro-and nanostructures in the drug delivery.
Inkjet printing using non-functionalized and functionalized MSN
Inkjet printing is considered to be a non-contact method of forming 2-dimensional and 3-dimensional through the processing of 1–100 pl droplets of liquid [136]. In this context, Wickström and team had reported a study wherein MSN based ink was formulated with the deposition of BCS class IV drug on hydroxypropyl methylcellulose (HPMC) and polyester transparent films using digital inkjet printing technology. It was found that both polyethyleneimine (PEI) surface-functionalized and non-functionalized MSNs, together with drug-loaded and drug-free MSN–PEI suspensions, were efficiently inkjet-printed [137]. Besides, the drug entrapped within the MSNs and the suspension were reported to be physically stable while the processing time and steps are to be optimized. The study established that inkjet printing technology is a flexible deposition method for MSN suspensions to produce patterns rendering to predefined designs. The concept is applicable as an accomplished drug-screening platform in the future because of the possibility of precisely depositing controlled volumes of MSN suspensions on different materials. The study also depicted the possibility to develop and print pharmaceutical nano-ink suspensions composed of unloaded and drug-loaded MSNs utilizing non-contact, digital, and inkjet printing technology.
Nano ink formulation using MSN
The efficiency of the printability of drug-loaded MSN as a nano-ink formulation was represented in the research work presented by Lago [138]. In this project, 1% (3 aminophenyl) tri-ethoxysilane-fluorescein isothiocyanate MSN was manufactured, functionalized, and then dispersed with different concentrations inside the ink base of water: propylene glycol: isopropyl alcohol 20:20:60 (v/v), which was chosen based on the Z values obtained (Z value is used as an indicator of the printability of the material). The analysis of drug loading and colloidal stability of MSN in a medium as well as interaction with drugs is evaluated by various techniques. Lago (2018) has demonstrated in his thesis that confocal scanning laser microscopy could be used to evaluate the concentration of MSNs and to observe if there’s an increase of fluorescence signal at higher printing resolution. Therefore, upon submission to confocal scanning laser microscopy evaluation of the printed samples, the results concluded that nanoparticles, for resolution lower than 300 DPI, did not homogeneously spread on the droplet, leading rise to be deposited along the perimeter. Still, the optimization of the printer is required to ensure reproducibility, which is important to offer individual treatment solutions [138].
Existing challenges on MSN application in NDDS
It has been established that MSN has a high potential to be used as a drug loading platform for advanced drug delivery systems. This inherited advantage has made MSN a lucrative excipient in various non-conventional drug delivery systems such as microsphere, microneedle, and hydrogel. MSN was employed as a potential drug carrier for the treatment of various diseases, and often they are functionalized to impart targeted delivery of the therapeutics at the diseased site or to obtain a controlled delivery of therapeutics. However, there are few challenges ahead for developing successful MSN-based ADDS or NDDS. The major challenge of MSN-based novel drug delivery systems is the reproducibility and industrial applicability. The synthesis of MSN on small scale or in the laboratory in a reproducible manner is relatively easier, but on a large manufacturing scale attaining the same particle size, pore size, and volume for MSN is challenging. With the use of superior polymers and the extreme processing conditions, the cost becomes ungovernable. The high bulk volume or low bulk density of MSN attributes its difficulty in handling the product on the industrial scale [139]. Few in vivo studies indicated the disadvantage of MSN, where the chances of hemolysis were reported because of the interaction of the silanol groups with the surface of the phospholipids of the red blood cell membranes [140]. Another disadvantage is attributed to the reported metabolic changes created by MSN leading to melanoma promotion [141]. A study by a group of researchers showed that a comprehensive molecular mechanism for MSNs persuaded boosting of human malignant melanoma development in vivo and in vitro [141]. It was observed that MSNs promoted A375 cell proliferation via an oxidative mechanism steering suppression of NF-kB stimulation. The result of the study is an adverse impact against the use of MSNs as drug carriers for tumor therapies. However, this effect needs further study. The mesoporous structure of MSN can be damaged or lost partially or fully during downstream processing of an MSN-based delivery system. In such cases, the benefits of MSN would be compromised. Therefore, downstream processing while maintaining the desired properties of MSN is an important issue. However, every problem has a solution. We have to address the challenges faced by the researchers during their research to employ MSN in the novel drug delivery system for improved application in the medical field.
Future direction and conclusion
The review has highlighted several approaches taken by the researchers on various ADDS and NDDS containing MSN. The challenges of MSN, mentioned in the previous section, are to overcome for making it a clinically successful drug delivery platform. To do this strong chemistry, manufacturing, and control (CMC) strategies need to be implemented along with the complete drug development program incorporating MSN as an excipient. An effective CMC program shall reduce the risk of failure in terms of safety or efficacy in clinical study phases. The chemistry, structural features, and functionalization behavior of MSN have been described by many researchers [142, 143]. One major question arises on its synthesis and manufacturing on a large scale with adequate reproducibility under the Good Manufacturing Practices (GMP), from which the batches are to be used for clinical testing, trial, and use. In general, the reproducible manufacturing of nanomedicines on a large scale always remains a major roadblock towards the translation of a “laboratory-developed” nanoparticulate drug delivery system into a clinically useful system. Similarly, the translation of MSN-based delivery systems into clinically applicable system depends on the success of its commercial manufacturing ability and stability. Therefore, future research on MSN should focus on achieving reproducible physical properties on a large scale. To identify the processing parameters and critical quality attributes, application of the “Quality by Design” (QbD) principle should be adopted. Percentage drug loading into the MSN, method of impregnation, pore size, and specific surface area, parameters related to downstream processing, are some of the important parameters that should be taken into consideration during designing commercial-scale production. Stability evaluation must be another future consideration. During long-term storage, the pore volume and surface area of MSN might change as a result of nanoparticle aggregation, which can significantly affect the drug release and absorption. So, a detailed evaluation of the storage stability of the final deliverable product is required.
Another concern is the safety and biodistribution of MSN loaded with the therapeutic agent. Despite few repeated dose toxicity studies such as a 14-day intravenous toxicity study with hollow MSN reported by Liu et al. (2011) [144], there is a significant requirement of toxicity studies of drug loaded MSN. To ensure safety, single-dose and multiple dose-toxicity studies or acute and sub-chronic toxicity studies in animal models are to be done. The route of drug administration also needs to be considered because MSN has been exploited for various routes of drug administration. There is an immense variation of physicochemical characteristics (size, pore volume, specific surface area) of MSN that depends on several factors such as the mode and conditions of synthesis, starting materials, surfactants, and hydration time and temperature. Such variation can modulate drug absorption from MSN, and so, safety and efficacy may vary. For instance, in an investigation of acute toxicity of MSN by Yu et al. (2012), it has been observed that the in vivo toxicity in mice was variably affected by porosity and surface area [144]. The researchers also demonstrated that the hydrodynamic sizes of silica are closely related to the vasculature impact and resultant tolerance threshold. The maximum tolerated dose and no observed adverse effect level (NOAEL) should be determined in acute and repeated dose toxicity studies.
Biodistribution of the MSN-based system is another concern that must be given attention, especially for tumor-targeted drug delivery. Like other nanoparticulate systems, very small diameter (5–6 nm) MSN also suffers from faster clearance by the kidney and reticuloendothelial uptake. The shape and aspect ratio of MSN affect the tissue distribution of MSN. Such phenomena adversely affect the targeting potential and the duration of action of drugs. Therefore, the distribution of MSN to various tissues, specially functionalized and targeted to the desired sites/tissue, must be studied experimentally. Radioactive or fluorescent marker-labeled MSN distribution can be studied by Gamma scintigraphy or MRI.
After all of these considerations in pre-clinical studies MSN-based drug delivery systems should be forwarded to clinical trials. In one of the very few studies in healthy human volunteers, ordered mesoporous silica was observed to improve the rate and extent of absorption by 77% and 54%, respectively compared with marketed formulation delivered orally [145]. Such studies are limited to solid dispersion formulation using mesoporous silica as a carrier. In the field of nanomedicine, at present more than 50 formulations indicated for cancer, fungal treatment, rare genetic disorders, etc., are being used clinically. Although the number of approved nanomedicine products for therapeutic uses is quite lesser compared with the huge volume of researches, there is a steady increase in the number from 1995 [146]. So far no clinical trial has been reported where the MSN-based drug delivery system is being evaluated. Moving towards clinical trials with the MSN-based drug delivery system is a delicate step unless the safety and efficacy of such a system are ensured in human beings.
Apart from all these aspects, the loading of large protein or biologics molecules into MSN could be another future direction. A small synthetic molecule is relatively easier to load in an “MSN container” than large biologics. Therefore, more focus should be needed on the biologics delivery system by availing benefits of MSN.
It could be concluded that the applicability of MSN is not only limited to conventional tablets or simple nanoparticulate drug delivery systems. Rather, it has been explored as ADDS or NDDS meant for synthetic or biologics, or protein molecules. The enhanced drug loading capability and targeting ability of MSN have been proved, but less reproducibility in large-scale manufacturing, inadequate safety and biodistribution studies, and lack of stability reports with final dosage forms are some of the “roadblocks” that are to be overcome by advanced researches followed by clinical studies.
References
Zahedi P, Yoganathan R, Piquette-Miller M, Allen C. Recent advances in drug delivery strategies for treatment of ovarian cancer. Expert Opin Drug Deliv. Taylor & Francis. 2012;9:567–83.
Slowing II, Vivero-Escoto JL, Wu CW, Lin VSY. Mesoporous silica nanoparticles as controlled release drug delivery and gene transfection carriers. Adv Drug Deliv Rev Elsevier. 2008;60:1278–88.
Mai WX, Meng H. Mesoporous silica nanoparticles: a multifunctional nano therapeutic system. Integr Biol (United Kingdom). Royal Society of Chemistry. 2013;5:19–28.
Choudhury H, Maheshwari R, Pandey M, Tekade M, Gorain B, Tekade RK. Advanced nanoscale carrier-based approaches to overcome biopharmaceutical issues associated with anticancer drug ‘Etoposide.’ Mater Sci Eng C. Elsevier. 2020;106:110275.
Kanaujia P, Poovizhi P, Ng WK, Tan RBH. Amorphous formulations for dissolution and bioavailability enhancement of poorly soluble APIs. Powder Technol. 2015.
Chatterjee B, Hamed Almurisi S, Ahmed Mahdi Dukhan A, Mandal UK, Sengupta P. Controversies with self-emulsifying drug delivery system from pharmacokinetic point of view. Drug Deliv. 2016;23:3639–52.
Karashima M, Sano N, Yamamoto S, Arai Y, Yamamoto K, Amano N, et al. Enhanced pulmonary absorption of poorly soluble itraconazole by micronized cocrystal dry powder formulations. Eur J Pharm Biopharm. Elsevier BV. 2017;115:65–72.
Gorain B, Choudhury H, Biswas E, Barik A, Jaisankar P, Pal TKTK. A novel approach for nanoemulsion components screening and nanoemulsion assay of olmesartan medoxomil through a developed and validated HPLC method. RSC Adv. The Royal Society of Chemistry. 2013;3:10887–93.
Gorain B, Choudhury H, Pandey M, Kesharwani P. Paclitaxel loaded vitamin E-TPGS nanoparticles for cancer therapy. Mater Sci Eng C. 2018;91:868–80.
Shen S-C, Ng W, Onn Chia L, Dong Y-C, Hee Tan R. Applications of mesoporous materials as excipients for innovative drug delivery and formulation. Curr Pharm Des. Bentham Science Publishers Ltd. 2013;19:6270–89.
Bremmell KE, Prestidge CA. Enhancing oral bioavailability of poorly soluble drugs with mesoporous silica based systems: opportunities and challenges. Drug Dev Ind Pharm. Taylor and Francis Ltd. 2019;45:349–58.
Jesus RA, Rabelo AS, Figueiredo RT, Cides Da Silva LC, Codentino IC, Fantini MCA, et al. Synthesis and application of the MCM-41 and SBA-15 as matrices for in vitro efavirenz release study. J Drug Deliv Sci Technol. Editions de Sante. 2016;31:153–9.
Tzankov B, Tzankova V, Aluani D, Yordanov Y, Spassova I, Kovacheva D, et al. Development of MCM-41 mesoporous silica nanoparticles as a platform for pramipexole delivery. J Drug Deliv Sci Technol. Editions de Sante. 2019;51:26–35.
Li Z, Zhang Y, Feng N. Mesoporous silica nanoparticles: synthesis, classification, drug loading, pharmacokinetics, biocompatibility, and application in drug delivery. Expert Opin Drug Deliv. Taylor and Francis Ltd. 2019;16:219–37.
Jia L, Shen J, Li Z, Zhang D, Zhang Q, Liu G, et al. In vitro and in vivo evaluation of paclitaxel-loaded mesoporous silica nanoparticles with three pore sizes. Int J Pharm Int J Pharm. 2013;445:12–9.
Li X, Zhang X, Zhao Y, Sun L. Fabrication of biodegradable Mn-doped mesoporous silica nanoparticles for pH/redox dual response drug delivery. J Inorg Biochem. Elsevier Inc. 2020;202:110887.
Kesse S, Boakye-Yiadom K, Ochete B, Opoku-Damoah Y, Akhtar F, Filli M, et al. Mesoporous silica nanomaterials: versatile nanocarriers for cancer theranostics and drug and gene delivery. Pharmaceutics. MDPI AG. 2019;11:77.
Yan Q, Guo X, Huang X, Meng X, Liu F, Dai P, et al. Gated mesoporous silica nanocarriers for hypoxia-responsive cargo release. ACS Appl Mater Interfaces. American Chemical Society. 2019;11:24377–85.
Shao M, Chang C, Liu Z, Chen K, Zhou Y, Zheng G, et al. Polydopamine coated hollow mesoporous silica nanoparticles as pH-sensitive nanocarriers for overcoming multidrug resistance. Colloids Surfaces B Biointerfaces. Elsevier BV. 2019;183:110427.
Maleki A, Kettiger H, Schoubben A, Rosenholm JM, Ambrogi V, Hamidi M. Mesoporous silica materials: from physico-chemical properties to enhanced dissolution of poorly water-soluble drugs. J Control Release. Elsevier BV. 2017;262:329–47.
Cheng YJ, Luo GF, Zhu JY, Xu XD, Zeng X, Cheng DB, et al. Enzyme-induced and tumor-targeted drug delivery system based on multifunctional mesoporous silica nanoparticles. ACS Appl Mater Interfaces. American Chemical Society. 2015;7:9078–87.
Bagheri E, Ansari L, Abnous K, Taghdisi SM, Charbgoo F, Ramezani M, et al. Silica based hybrid materials for drug delivery and bioimaging. J Control Release. Elsevier BV. 2018;277:57–76.
Bitar A, Ahmad NM, Fessi H, Elaissari A. Silica-based nanoparticles for biomedical applications. Drug Discov Today Elsevier Current Trends. 2012;17:1147–54.
Wang Y, Zhao Q, Han N, Bai L, Li J, Liu J, et al. Mesoporous silica nanoparticles in drug delivery and biomedical applications. Nanomedicine Nanotechnology, Biol Med. Elsevier Inc. 2015;11:313–27.
Slowing II, Trewyn BG, Giri S, Lin VSY. Mesoporous silica nanoparticles for drug delivery and biosensing applications. Adv Funct Mater. John Wiley & Sons, Ltd. 2007;17:1225–36.
Nigro A, Pellegrino M, Greco M, Comandè A, Sisci D, Pasqua L, et al. Dealing with skin and blood-brain barriers: the unconventional challenges of mesoporous silica nanoparticles. Pharmaceutics. MDPI AG. 2018;10:250.
Narayan R, Nayak UY, Raichur AM, Garg S. Mesoporous silica nanoparticles: a comprehensive review on synthesis and recent advances. Pharmaceutics. 2018.
V Chiola, JE Ritsko CV. Process for producing low-bulk density silica. U.S. Patent and Trademark Office. 1971.
Le Page, Madeleine, Raymond Beau, Duchene. J. Porous silica particles containing a crystallized phase and method. U.S. Patent and Trademark Office. 1970.
Yanagisawa T, Shimizu T, Kuroda K, Kato C. The preparation of alkyltriinethylaininonium–kaneinite complexes and their conversion to microporous materials. Bull Chem Soc Jpn. The Chemical Society of Japan. 1990;63:988–92.
Kresge CT, Leonowicz ME, Roth WJ, Vartuli JC, Beck JS. Ordered mesoporous molecular sieves synthesized by a liquid-crystal template mechanism. Nature. 1992.
Zhao D, Feng J, Huo Q, Melosh N, Fredrickson GH, Chmelka BF, et al. Triblock copolymer syntheses of mesoporous silica with periodic 50 to 300 angstrom pores. Science. (80). 1998.
Bagshaw SA, Di Renzo F, Fajula F. Preparation of metal-incorporated MSU mesoporous silica molecular sieves. Ti incorporation via a totally non-ionic route. Chem Commun. Royal Society of Chemistry. 1996;2209–10.
Ishikawa T, Matsuda M, Yasukawa A, Kandori K, Inagaki S, Fukushima T, et al. Surface silanol groups of mesoporous silica FSM-16. J Chem Soc - Faraday Trans. 1996;
da Silva F das CM, Costa MJ dos S, da Silva LKR, Batista AM, da Luz GE. Functionalization methods of SBA-15 mesoporous molecular sieve: a brief overview. SN Appl Sci. Springer Science and Business Media LLC. 2019;1:654.
Walstra P. Dispersed systems: basic considerations. Food Chem. 1996. p. 143–6.
Schüth F, Ciesla U, Schacht S, Thieme M, Huo Q, Stucky G. Ordered mesoporous silicas and zirconias: control on length scales between nanometer and micrometer. Mater Res Bull. 1999.
Balkus KJ, Coutinho D, Lucas J, Washmon-Kriel L. Synthesis and characterization of DAM-1 type materials. MRS Online Proc Libr Arch. Cambridge University Press. 2000;628.
Miletto I, Fraccarollo A, Barbero N, Barolo C, Cossi M, Marchese L, et al. Mesoporous silica nanoparticles incorporating squaraine-based photosensitizers: a combined experimental and computational approach. Dalt Trans. 2018.
Abrahamse H, Hamblin MR. New photosensitizers for photodynamic therapy. Biochem J. 2016.
Kempen PJ, Greasley S, Parker KA, Campbell JL, Chang H-Y, Jones JR, et al. Theranostic mesoporous silica nanoparticles biodegrade after pro-survival drug delivery and ultrasound/magnetic resonance imaging of stem cells. Theranostics. Ivyspring International Publisher. 2015;5:631.
Baeza A, Colilla M, Vallet-Regí M. Advances in mesoporous silica nanoparticles for targeted stimuli-responsive drug delivery. Expert Opin. Drug Deliv. 2015.
Möller K, Müller K, Engelke H, Bräuchle C, Wagner E, Bein T. Highly efficient siRNA delivery from core-shell mesoporous silica nanoparticles with multifunctional polymer caps. Nanoscale. 2016.
Martínez-Carmona M, Lozano D, Colilla M, Vallet-Regí M. Lectin-conjugated pH-responsive mesoporous silica nanoparticles for targeted bone cancer treatment. Acta Biomater. 2018.
Vallet-Regi M, Rámila A, Del Real RP, Pérez-Pariente J. A new property of MCM-41: Drug delivery system. Chem Mater. 2001.
Li Z, Barnes JC, Bosoy A, Stoddart JF, Zink JI. Mesoporous silica nanoparticles in biomedical applications. Chem Soc Rev. 2012.
Singh SY, Verma R, Kumar L. Porous oral drug delivery system: tablets. Pharm Chem J. Springer New York LLC. 2018;52:553–61.
Summerlin N, Qu Z, Pujara N, Sheng Y, Jambhrunkar S, McGuckin M, et al. Colloidal mesoporous silica nanoparticles enhance the biological activity of resveratrol. Colloids Surfaces B Biointerfaces. Elsevier BV. 2016;144:1–7.
Zhang Y, Zhi Z, Jiang T, Zhang J, Wang Z, Wang S. Spherical mesoporous silica nanoparticles for loading and release of the poorly water-soluble drug telmisartan. J Control Release J Control Release. 2010;145:257–63.
Wang Z, Chen B, Quan G, Li F, Wu Q, Dian L, et al. Increasing the oral bioavailability of poorly water-soluble carbamazepine using immediate-release pellets supported on SBA-15 mesoporous silica. Int J Nanomedicine. 2012;7:5807–18.
Gangwar RK, Tomar GB, Dhumale VA, Zinjarde S, Sharma RB, Datar S. Curcumin conjugated silica nanoparticles for improving bioavailability and its anticancer applications. J Agric Food Chem. American Chemical Society. 2013;61:9632–7.
He Y, Liang S, Long M, Xu H. Mesoporous silica nanoparticles as potential carriers for enhanced drug solubility of paclitaxel. Mater Sci Eng C Elsevier. 2017;78:12–7.
Takeuchi H, Nagira S, Yamamoto H, Kawashima Y. Solid dispersion particles of amorphous indomethacin with fine porous silica particles by using spray-drying method. Int J Pharm Elsevier. 2005;293:155–64.
Zhang Y, Wang J, Bai X, Jiang T, Zhang Q, Wang S. Mesoporous silica nanoparticles for increasing the oral bioavailability and permeation of poorly water soluble drugs. Mol Pharm Mol Pharm. 2012;9:505–13.
Keasberry NA, Yapp CW, Idris A. Mesoporous silica nanoparticles as a carrier platform for intracellular delivery of nucleic acids. Biochem. Maik Nauka Publishing / Springer SBM. 2017;82:655–62.
Peng H, Dong R, Wang S, Zhang Z, Luo M, Bai C, et al. A pH-responsive nano-carrier with mesoporous silica nanoparticles cores and poly(acrylic acid) shell-layers: fabrication, characterization and properties for controlled release of salidroside. Int J Pharm Elsevier. 2013;446:153–9.
Yamamoto E, Kuroda K. Colloidal mesoporous silica nanoparticles. Bull Chem Soc Jpn. Chemical Society of Japan. 2016;89:501–39.
Lai CY, Trewyn BG, Jeftinija DM, Jeftinija K, Xu S, Jeftinija S, et al. A mesoporous silica nanosphere-based carrier system with chemically removable CdS nanoparticle caps for stimuli-responsive controlled release of neurotransmitters and drug molecules. J Am Chem Soc. 2003.
Thomas MJK, Slipper I, Walunj A, Jain A, Favretto ME, Kallinteri P, et al. Inclusion of poorly soluble drugs in highly ordered mesoporous silica nanoparticles. Int J Pharm Elsevier. 2010;387:272–7.
Lu J, Liong M, Zink JI, Tamanoi F. Mesoporous silica nanoparticles as a delivery system for hydrophobic anticancer drugs. Small. 2007;3:1341–6.
Colilla M, Manzano M, Izquierdo-Barba I, Vallet-Reg M, Boissiére C, Sanchez C. Advanced drug delivery vectors with tailored surface properties made of mesoporous binary oxides submicronic spheres. Chem Mater. 2010.
Wang Y, Sun L, Jiang T, Zhang J, Zhang C, Sun C, et al. The investigation of MCM-48-type and MCM-41-type mesoporous silica as oral solid dispersion carriers for water insoluble cilostazol. Drug Dev Ind Pharm. 2014;40:819–28.
Gao W, Chan JM, Farokhzad OC. PH-responsive nanoparticles for drug delivery. Pharm: Mol; 2010.
Meng H, Xue M, Xia T, Ji Z, Tarn DY, Zink JI, et al. Use of size and a copolymer design feature to improve the biodistribution and the enhanced permeability and retention effect of doxorubicin-loaded mesoporous silica nanoparticles in a murine xenograft tumor model. ACS Nano. 2011.
Tang L, Gabrielson NP, Uckun FM, Fan TM, Cheng J. Size-dependent tumor penetration and in vivo efficacy of monodisperse drug-silica nanoconjugates. Mol Pharm. 2013.
Gary-Bobo M, Mir Y, Rouxel C, Brevet D, Hocine O, Maynadier M, et al. Multifunctionalized mesoporous silica nanoparticles for the in vitro treatment of retinoblastoma: drug delivery, one and two-photon photodynamic therapy. Int J Pharm. 2012;432:99–104.
Singh P, Singh H, Castro-Aceituno V, Ahn S, Kim YJ, Farh MEA, et al. Engineering of mesoporous silica nanoparticles for release of ginsenoside CK and Rh2 to enhance their anticancer and anti-inflammatory efficacy: in vitro studies. J Nanoparticle Res. Springer Netherlands. 2017;19:1–14.
Eivazzadeh-Keihan R, Chenab KK, Taheri-Ledari R, Mosafer J, Hashemi SM, Mokhtarzadeh A, et al. Recent advances in the application of mesoporous silica-based nanomaterials for bone tissue engineering. Mater Sci Eng C. Elsevier Ltd. 2020;107:110267.
Huang C, Zhang Z, Guo Q, Zhang L, Fan F, Qin Y, et al. A dual-model imaging theragnostic system based on mesoporous silica nanoparticles for enhanced cancer phototherapy. Adv Healthc Mater. Adv Healthc Mater. 2019;8:e1900840.
Huang PK, Lin SX, Tsai MJ, Leong MK, Lin SR, Kankala RK, et al. Encapsulation of 16-hydroxycleroda-3,13-dine-16,15-olide in mesoporous silica nanoparticles as a natural dipeptidyl peptidase-4 inhibitor potentiated hypoglycemia in diabetic mice. Nanomaterials. MDPI AG. 2017;7.
Xi C, Zhou J, Du S, Peng S. Autophagy upregulation promotes macrophages to escape mesoporous silica nanoparticle (MSN)-induced NF-κB-dependent inflammation. Inflamm Res Birkhauser Verlag AG. 2016;65:325–41.
Wang Q, Chen C, Liu W, He X, Zhou N, Zhang D, et al. Levofloxacin loaded mesoporous silica microspheres/nanohydroxyapatite/ polyurethane composite scaffold for the treatment of chronic osteomyelitis with bone defects. Sci Rep. Nature Publishing Group. 2017;7.
Brevet D, Gary-Bobo M, Raehm L, Richeter S, Hocine O, Amro K, et al. Mannose-targeted mesoporous silica nanoparticles for photodynamic therapy. Chem Commun. 2009.
Vallet-Regí M, González B, Izquierdo-Barba I. Nanomaterials as promising alternative in the infection treatment. Sci Int J Mol; 2019.
Mora-Raimundo P, Lozano D, Manzano M, Vallet-Regí M. Nanoparticles to knockdown osteoporosis-related gene and promote osteogenic marker expression for osteoporosis treatment. ACS Nano. 2019.
Anglin EJ, Cheng L, Freeman WR, Sailor MJ. Porous silicon in drug delivery devices and materials. Adv Drug Deliv Rev. 2008;60:1266–77.
Tang L, Cheng J. Nonporous silica nanoparticles for nanomedicine application. Nano Today. Elsevier BV. 2013;8:290–312.
Santos HA, Hirvonen J. Nanostructured porous silicon materials: potential candidates for improving drug delivery. Nanomedicine Nanomedicine (Lond). 2012;7:1281–4.
Argyo C, Weiss V, Bräuchle C, Bein T. Multifunctional mesoporous silica nanoparticles as a universal platform for drug delivery. Chem Mater American Chemical Society. 2014;26:435–51.
Kresge CT, Leonowicz ME, Roth WJ, Vartuli JC, Beck JS. Ordered mesoporous molecular sieves synthesized by a liquid-crystal template mechanism. Nature Nature Publishing Group. 1992;359:710–2.
Grün M, Lauer I, Unger KK. The synthesis of micrometer- and submicrometer-size spheres of ordered mesoporous oxide MCM-41. Adv Mater Wiley-VCH Verlag. 1997;9:254–7.
Unger KK, Kumar D, Grün M, Büchel G, Lüdtke S, Adam T, et al. Synthesis of spherical porous silicas in the micron and submicron size range: challenges and opportunities for miniaturized high-resolution chromatographic and electrokinetic separations. J Chromatogr A Elsevier. 2000;892:47–55.
Freiberg S, Zhu XX. Polymer microspheres for controlled drug release. Int J Pharm Elsevier. 2004;282:1–18.
Noguez Méndez NA, Quirino Barreda CT, Vega AF, Miranda Calderon JE, Urioste CG, Palomec XC, et al. Design and development of pharmaceutical microprocesses in the production of nanomedicine. Nanostructures Oral Med. Elsevier Inc. 2017. p. 669–97.
Sharma N, Purwar N, Gupta PC. Microspheres as drug carriers for controlled drug delivery : a review. Int J Pharm Sci Res. 2015;6:4579–87.
Chouhan R, Goswami S, Bajpai AK. Recent advancements in oral delivery of insulin: from challenges to solutions. Nanostructures Oral Med. Elsevier Inc. 2017. p. 409–33.
Jayant RD, McShane MJ, Srivastava R. Polyelectrolyte-coated alginate microspheres as drug delivery carriers for dexamethasone release coated alginate microspheres for dexamethasone delivery R.D. Jayant et al. Drug Deliv. 2009;16:331–40.
Yamauchi Y, Kuroda K. Rational design of mesoporous metals and related nanomaterials by a soft-template approach. Chem - An Asian J. Chem Asian J. 2008;3:664–76.
Hegazy M, Zhou P, Wu G, Wang L, Rahoui N, Taloub N, et al. Construction of polymer coated core-shell magnetic mesoporous silica nanoparticles with triple responsive drug delivery. Polym Chem. 2017.
Song Y, Yang LY, Wang Y guang, Yu D, Shen J, Ouyang X kun. Highly efficient adsorption of Pb(II) from aqueous solution using amino-functionalized SBA-15/calcium alginate microspheres as adsorbent. Int J Biol Macromol. Elsevier BV. 2019;125:808–19.
Hu L, Sun C, Song A, Chang D, Zheng X, Gao Y, et al. Alginate encapsulated mesoporous silica nanospheres as a sustained drug delivery system for the poorly water-soluble drug indomethacin. Asian J Pharm Sci. Shenyang Pharmaceutical University. 2014;9:183–90.
Liao Y Te, Liu CH, Yu J, Wu KCW. Liver cancer cells: targeting and prolonged-release drug carriers consisting of mesoporous silica nanoparticles and alginate microspheres. Int J Nanomedicine. Dove Medical Press Ltd. 2014;9:2767–78.
Liu C, Guo J, Yang W, Hu J, Wang C, Fu S. Magnetic mesoporous silica microspheres with thermo-sensitive polymer shell for controlled drug release. J Mater Chem. The Royal Society of Chemistry. 2009;19:4764–70.
Chang B, Sha X, Guo J, Jiao Y, Wang C, Yang W. Thermo and pH dual responsive, polymer shell coated, magnetic mesoporous silica nanoparticles for controlled drug release. J Mater Chem. 2011.
Tian Z, Yu X, Ruan Z, Zhu M, Zhu Y, Hanagata N. Magnetic mesoporous silica nanoparticles coated with thermo-responsive copolymer for potential chemo- and magnetic hyperthermia therapy. Microporous Mesoporous Mater. Elsevier BV. 2018;256:1–9.
Shen Y, Tang H, Radosz M, Van Kirk E, Murdoch WJ. PH-responsive nanoparticles for cancer drug delivery. Methods Mol Biol Humana Press. 2008;437:183–216.
Wen H, Guo J, Chang B, Yang W. PH-responsive composite microspheres based on magnetic mesoporous silica nanoparticle for drug delivery. Eur J Pharm Biopharm Elsevier. 2013;84:91–8.
Gandavarapu NR, Azagarsamy MA, Anseth KS. Photo-click living strategy for controlled, reversible exchange of biochemical ligands. Adv Mater Wiley-VCH Verlag. 2014;26:2521–6.
Li X, Hong CY, Pan CY. Preparation and characterization of hyperbranched polymer grafted mesoporous silica nanoparticles via self-condensing atom transfer radical vinyl polymerization. Polymer (Guildf). Elsevier BV. 2010;51:92–9.
Hong CY, Li X, Pan CY. Smart core-shell nanostructure with a mesoporous core and a stimuli-responsive nanoshell synthesized via surface reversible addition-fragmentation chain transfer polymerization. J Phys Chem C. American Chemical Society. 2008;112:15320–4.
Hong CY, You YZ, Pan CY. Synthesis of water-soluble multiwalled carbon nanotubes with grafted temperature-responsive shells by surface RAFT polymerization. Chem Mater American Chemical Society. 2005;17:2247–54.
You YZ, Hong CY, Pan CY. Directly growing ionic polymers on multi-walled carbon nanotubes via surface RAFT polymerization - IOPscience. Nanotechnology. 2006;17:2350.
Stenzel MH, Zhang L, Huck WTS. Temperature-responsive glycopolymer brushes synthesized via RAFT polymerization using the Z-group approach. Macromol Rapid Commun. John Wiley & Sons, Ltd. 2006;27:1121–6.
Narayanaswamy R, Torchilin VP. Hydrogels and their applications in targeted drug delivery. Molecules. MDPI AG. 2019;24:603.
Chen X, Liu Z, Parker SG, Zhang X, Gooding JJ, Ru Y, et al. Light-induced hydrogel based on tumor-targeting mesoporous silica nanoparticles as a theranostic platform for sustained cancer treatment. ACS Appl Mater Interfaces. American Chemical Society. 2016;8:15857–63.
Zhao P, Liu H, Deng H, Xiao L, Qin C, Du Y, et al. A study of chitosan hydrogel with embedded mesoporous silica nanoparticles loaded by ibuprofen as a dual stimuli-responsive drug release system for surface coating of titanium implants. Colloids Surfaces B Biointerfaces Elsevier. 2014;123:657–63.
Zhu M, Zhu Y, Zhang L, Shi J. Preparation of chitosan/mesoporous silica nanoparticle composite hydrogels for sustained co-delivery of biomacromolecules and small chemical drugs. Sci Technol Adv Mater. Taylor & Francis. 2013;14:45005–14.
Rao Z, Liu S, Wu R, Wang G, Sun Z, Bai L, et al. Fabrication of dual network self-healing alginate/guar gum hydrogels based on polydopamine-type microcapsules from mesoporous silica nanoparticles. Int J Biol Macromol. Elsevier BV. 2019;129:916–26.
Karaman D Ṣen, Patrignani G, Rosqvist E, Smått JH, Orłowska A, Mustafa R, et al. Mesoporous silica nanoparticles facilitating the dissolution of poorly soluble drugs in orodispersible films. Eur J Pharm Sci. Elsevier BV. 2018;122:152–9.
LaBauve AE, Rinker TE, Noureddine A, Serda RE, Howe JY, Sherman MB, et al. Lipid-coated mesoporous silica nanoparticles for the delivery of the ML336 antiviral to inhibit encephalitic alphavirus infection. Sci Rep Nature Publishing Group. 2018;8:1–13.
Butler KS, Durfee PN, Theron C, Ashley CE, Carnes EC, Brinker CJ. Protocells: modular mesoporous silica nanoparticle-supported lipid bilayers for drug delivery. Small. 2016;12:2173–85.
Nel AE, Meng H, Xiangsheng L. Mesoporous silica nanoparticles with lipid bilayer coating for cargo delivery [Internet]. 2018. Available from: https://patents.google.com/patent/US10143660B2/en?q=Mesoporous+silica+nanoparticle+lipid+bilayer+coating+cargo+delivery&oq=+Mesoporous+silica+nanoparticle+with+lipid+bilayer+coating+for+cargo+delivery
Wu X, Wang Z, Zhu D, Zong S, Yang L, Zhong Y, et al. PH and thermo dual-stimuli-responsive drug carrier based on mesoporous silica nanoparticles encapsulated in a copolymer-lipid bilayer. ACS Appl Mater Interfaces. American Chemical Society. 2013;5:10895–903.
Sun Q, You Q, Wang J, Liu L, Wang Y, Song Y, et al. Theranostic nanoplatform: Triple-modal imaging-guided synergistic cancer therapy based on liposome-conjugated mesoporous silica nanoparticles. ACS Appl Mater Interfaces. American Chemical Society. 2018;10:1963–75.
Yang S, Song S, Han K, Wu X, Chen L, Hu Y, et al. Characterization, in vitro evaluation and comparative study on the cellular internalization of mesoporous silica nanoparticle-supported lipid bilayers. Microporous Mesoporous Mater. Elsevier BV. 2019;284:212–24.
Zhang X, Li F, Guo S, Chen X, Wang X, Li J, et al. Biofunctionalized polymer-lipid supported mesoporous silica nanoparticles for release of chemotherapeutics in multidrug resistant cancer cells. Biomaterials Elsevier. 2014;35:3650–65.
Liu X, Situ A, Kang Y, Villabroza KR, Liao Y, Chang CH, et al. Irinotecan delivery by lipid-coated mesoporous silica nanoparticles shows improved efficacy and safety over liposomes for pancreatic cancer. ACS Nano American Chemical Society. 2016;10:2702–15.
Tu J, Bussmann J, Du G, Gao Y, Bouwstra JA, Kros A. Lipid bilayer-coated mesoporous silica nanoparticles carrying bovine hemoglobin towards an erythrocyte mimic. Int J Pharm. Elsevier BV. 2018;543:169–78.
Pan J, Wan D, Gong J. PEGylated liposome coated QDs/mesoporous silica core-shell nanoparticles for molecular imaging. Chem Commun. The Royal Society of Chemistry. 2011;47:3442–4.
Meng H, Wang M, Liu H, Liu X, Situ A, Wu B, et al. Use of a lipid-coated mesoporous silica nanoparticle platform for synergistic gemcitabine and paclitaxel delivery to human pancreatic cancer in mice. ACS Nano American Chemical Society. 2015;9:3540–57.
Liu J, Jiang X, Ashley C, Brinker CJ. Electrostatically mediated liposome fusion and lipid exchange with a nanoparticle-supported bilayer for control of surface charge, drug containment, and delivery. J Am Chem Soc. American Chemical Society. 2009;131:7567–9.
Liu J, Stace-Naughton A, Jiang X, Brinker CJ. Porous nanoparticle supported lipid bilayers (protocells) as delivery vehicles. J Am Chem Soc. American Chemical Society. 2009;131:1354–5.
Donnelly RF, Raj Singh TR, Woolfson AD. Microneedle-based drug delivery systems: microfabrication, drug delivery, and safety. Drug Deliv Europe PMC Funders. 2010;17:187–207.
Yang J, Liu X, Fu Y, Song Y. Recent advances of microneedles for biomedical applications: drug delivery and beyond. Acta Pharm Sin B. Chinese Academy of Medical Sciences. 2019;9:469–83.
Du G, Woythe L, van der Maaden K, Leone M, Romeijn S, Kros A, et al. Coated and hollow microneedle-mediated intradermal immunization in mice with diphtheria toxoid loaded mesoporous silica nanoparticles. Pharm Res. Springer New York LLC. 2018;35:189.
Lee CH, Cheng SH, Wang YJ, Chen YC, Chen NT, Souris J, et al. Near-infrared mesoporous silica nanoparticles for optical imaging: characterization and in vivo biodistribution. Adv Funct Mater. John Wiley & Sons, Ltd. 2009;19:215–22.
Lei Q, Qiu WX, Hu JJ, Cao PX, Zhu CH, Cheng H, et al. Multifunctional mesoporous silica nanoparticles with thermal-responsive gatekeeper for NIR light-triggered chemo/photothermal-therapy. Small Wiley-VCH Verlag. 2016;12:4286–98.
Sheng Z, Hu D, Xue M, He M, Gong P, Cai L. Indocyanine green nanoparticles for theranostic applications. Nano-Micro Lett. Springer Science and Business Media LLC. 2013;5:145–50.
Pei P, Yang F, Liu J, Hu H, Du X, Hanagata N, et al. Composite-dissolving microneedle patches for chemotherapy and photothermal therapy in superficial tumor treatment. Biomater Sci Royal Society of Chemistry. 2018;6:1414–23.
Xu B, Jiang G, Yu W, Liu D, Zhang Y, Zhou J, et al. H2O2-responsive mesoporous silica nanoparticles integrated with microneedle patches for the glucose-monitored transdermal delivery of insulin. J Mater Chem B. Royal Society of Chemistry. 2017;5:8200–8.
Zeeshan F, Madheswaran T, Pandey M, Gorain B. Three-dimensional (3-D) printing technology exploited for the fabrication of drug delivery systems. Curr Pharm Des. 2018;24:5019–28.
Pandey M, Choudhury H, Fern JLC, Kee ATK, Kou J, Jing JLJ, et al. 3D printing for oral drug delivery: a new tool to customize drug delivery. Drug Deliv Transl Res Springer. 2020;10:986–1001.
Planchette C, Pichler H, Wimmer-Teubenbacher M, Gruber M, Gruber-Woelfler H, Mohr S, et al. Printing medicines as orodispersible dosage forms: effect of substrate on the printed micro-structure. Int J Pharm Elsevier. 2016;509:518–27.
Genina N, Janßen EM, Breitenbach A, Breitkreutz J, Sandler N. Evaluation of different substrates for inkjet printing of rasagiline mesylate. Eur J Pharm Biopharm. 2013;85:1075–83.
Preis M, Rosenholm JM. Printable nanomedicines: the future of customized drug delivery? Ther Deliv Future Medicine Ltd. 2017;8:721–3.
Boehm RD, Miller PR, Daniels J, Stafslien S, Narayan RJ. Inkjet printing for pharmaceutical applications. Mater Today Elsevier Ltd. 2014;17:247–52.
Wickstrm H, Hilgert E, Nyman JO, Desai D, Karaman DŞ, De Beer T, et al. Inkjet printing of drug-loaded mesoporous silica nanoparticles—a platform for drug development. Molecules. MDPI AG. 2017;22:2020.
Lago M. Inkjet printing of nirogacestat loaded mesoporous silica nanoparticles. [Italy]: Universita Degli Studi Di Padova. 2018.
Rosenholm JM, Sahlgren C, Lindén M. Towards multifunctional, targeted drug delivery systems using mesoporous silica nanoparticles - opportunities & challenges. Nanoscale Nanoscale. 2010;2:1870–83.
Zhao Y, Sun X, Zhang G, Trewyn BG, Slowing II, Lin VSY. Interaction of mesoporous silica nanoparticles with human red blood cell membranes: Size and surface effects. ACS Nano American Chemical Society. 2011;5:1366–75.
Huang X, Zhuang J, Teng X, Li L, Chen D, Yan X, et al. The promotion of human malignant melanoma growth by mesoporous silica nanoparticles through decreased reactive oxygen species. Biomaterials. 2010.
Mamaeva V, Sahlgren C, Lindén M. Mesoporous silica nanoparticles in medicine-recent advances. Rev: Adv. Drug Deliv; 2013.
Vallet-Regí M, Colilla M, Izquierdo-Barba I, Manzano M. Mesoporous silica nanoparticles for drug delivery: current insights. Molecules. Multidisciplinary Digital Publishing Institute. 2018;23:47.
Liu T, Li L, Teng X, Huang X, Liu H, Chen D, et al. Single and repeated dose toxicity of mesoporous hollow silica nanoparticles in intravenously exposed mice. Biomaterials. 2011.
Bukara K, Schueller L, Rosier J, Martens MA, Daems T, Verheyden L, et al. Ordered mesoporous silica to enhance the bioavailability of poorly water-soluble drugs: Proof of concept in man. Eur J Pharm Biopharm. 2016.
Germain M, Caputo F, Metcalfe S, Tosi G, Spring K, Åslund AKO, et al. Delivering the power of nanomedicine to patients today. J Control Release. 2020.
Acknowledgements
The authors wish to acknowledge the support of SPPSPTM, SVKM’s NMIMS, Mumbai (India), in completion of the article.
Author information
Authors and Affiliations
Contributions
All the authors have a significant contribution to the article as mentioned in the following (author-wise). First author: construction of the manuscript and writing of the main body, formatting. Second and third author: overall technical review and editing, scientific input for modification of some major sections. Corresponding author: concept, article construction, section-wise review and technical modification, abstract. All the four authors have contributed to the article. The final submitted version has been reviewed by all authors, and all of them agreed on the submission.
Corresponding author
Ethics declarations
Informed consent
On behalf of the authors, the corresponding author hereby ensures the consent of all authors for submitting the article to Drug Delivery and Translational Research Journal.
Competing interests
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Stephen, S., Gorain, B., Choudhury, H. et al. Exploring the role of mesoporous silica nanoparticle in the development of novel drug delivery systems. Drug Deliv. and Transl. Res. 12, 105–123 (2022). https://doi.org/10.1007/s13346-021-00935-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-021-00935-4