Abstract
HbA1c and fasting plasma glucose (FPG) levels are commonly recognized as diagnostic indices for diabetes and glucose intolerance. However, they are not sufficient for clear detection of glucose intolerance in the early stage unless an oral glucose tolerance test (OGTT) is performed. Moreover, even in case of an OGTT, 2-h postprandial plasma glucose (PG) levels, a criterion for glucose intolerance in OGTTs, may not provide complete information regarding glucose tolerance. Whole glucose excursion after OGTT is considered to represent glucose tolerance well, and the glucose area under the curve (AUC) can be an index of glucose excursion. However, few studies have investigated measurement of the glucose AUC in glucose intolerance screening. In the present study, data from 520 OGTTs were analyzed to define the cutoff value for the glucose AUC for glucose intolerance screening. Our results showed that a cutoff value of 290 mg h/dl for the glucose AUC was highly sensitive and specific (90 and 93 %, respectively) for detecting diabetes, impaired glucose tolerance (IGT), and group at increased risk of diabetes (normal glucose tolerance with 1-h PG levels of ≥180 mg/dl after glucose load) and showed a better concordance rate than the use of HbA1c, FPG, or 2-h PG levels. Moreover, the cutoff value for the glucose AUC calculated using the diagnostic criteria in the OGTT (305 mg h/dl) was consistent with the value determined from OGTT analysis. These data suggest a possibility that glucose intolerance screening using a glucose AUC cutoff value of 290 mg h/dl could be useful.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is important to manage blood glucose levels in patients with diabetes to suppress the progression of diabetes mellitus (DM) and prevent complications [1]. Recent studies conducted by the Diabetes Prevention Program [2] and Japan Diabetes Prevention Program [3] have demonstrated that interventions for patients with impaired glucose tolerance (IGT) are effective in suppressing DM progression; therefore, detection of glucose intolerance at an early stage is essential. However, neither fasting plasma glucose (FPG) nor HbA1c levels, which are used as indices for DM and glucose intolerance screening, have sufficient sensitivity for detection during the early stage of glucose intolerance because of a large overlap of these indices in normal glucose tolerance (NGT) and IGT [4].
The oral glucose tolerance test (OGTT) is highly sensitive and specific for detecting glucose intolerance because it can demonstrate postchallenge glucose excursion. However, the 2-h plasma glucose (PG) levels, a criterion for glucose intolerance on the OGTT, may not provide complete information regarding the processing of PG after glucose loading. Whole glucose excursion, rather than PG levels at a point, is considered to provide more information about glucose tolerance. For instance, glycemic variability, which is proposed to be harmful for blood vessels and affect the development of complications, could be reflected by whole glucose excursion. The glucose area under the curve (AUC), which is an index of whole glucose excursion after glucose loading, has been widely used for calculating the glycemic index [5] and for evaluating the efficacy of medications for postprandial hyperglycemia [6]. However, few studies have evaluated the application of the glucose AUC to glucose tolerance testing and examined the appropriate cutoff value for diagnosis [7]. Therefore, in the present study, our aim was to evaluate the possible usefulness of glucose AUC measurements in identifying cases of early stage diabetes. We analyzed the cutoff value and screening concordance rates using glucose AUC values calculated from our OGTT data.
Materials and methods
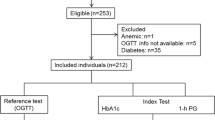
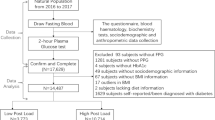
Anonymous OGTT data (N = 520) were obtained from the Kyoto Industrial Health Association (Kyoto, Japan) and IHI Harima Hospital (Aioi, Japan) and analyzed. Plasma was used for measurement of blood glucose levels, while whole blood was used for that of HbA1c. The measurements were carried out in each institute using standard laboratory methods.
Seventy-five-gram OGTT data were classified using the diagnostic criteria of the Japan Diabetes Society (JDS) [8]. DM was defined as FPG levels ≥126 mg/dl or 2-h PG levels ≥200 mg/dl. NGT was defined as FPG levels <110 mg/dl and 2-h PG levels <140 mg/dl. Impaired fasting glucose (IFG) was defined as only FPG levels in the impaired range (i.e., 110 ≤ FPG < 126 mg/dl and 2-h PG < 140 mg/dl). IGT was defined as FPG < 126 mg/dl and 140 ≤ 2-h PG < 200 mg/dl. In addition, groups at increased risk of diabetes (1-h PG levels ≥180 mg/dl with normal 2-h PG) were included in IGT according to the criteria of JDS. In this study, the National Glycohemoglobin Standardization Program (NGSP) HbA1c values were used for analysis by conversion to JDS HbA1c values [9].
PG-AUCs were calculated by trapezoidal approximation of PG levels. PG levels at x min were defined as PG(x), and PG-AUC was calculated as follows:
Results
Table 1 shows 75-g OGTT data classified by NGT, IFG, IGT, and DM, which represented 48, 2, 38, and 12 % of patients, respectively. The mean PG levels after glucose loading and PG-AUC in IGT were much higher than those in NGT, whereas the mean HbA1c and FPG levels in IGT were similar to those in NGT.
Figure 1 shows the distribution frequencies of (a) PG-AUC and (b) HbA1c levels in NGT, IFG, IGT, and DM. IGT was clearly distinguished from NGT at a PG-AUC of ~300 mg h/dl. The large overlap in HbA1c levels between NGT and IGT made it difficult to separate IGT from NGT according to HbA1c levels. This HbA1c overlap corresponded well to the findings of a previous analysis of over 18,000 75-g OGTT results in a Japanese study by Kuzuya et al. [4], indicating that our data are representative of Japanese OGTT profiles.
Receiver-operating characteristic (ROC) curves for PG-AUC, HbA1c levels, FPG levels, and 2-h PG levels are shown in Fig. 2, with IFG, IGT, and DM defined as positive in the analysis. The area under the ROC curves for HbA1c and FPG levels was 0.7–0.8, in agreement with previously reported results [10]. On the other hand, the area under the ROC curve for PG-AUC was much higher than that for HbA1c and FPG levels (Fig. 2). When the cutoff value was set to 290 mg h/dl, the sensitivity and specificity of PG-AUC were 90 and 93 %, respectively. The glucose profiles of all false-negative and -positive cases as classified by PG-AUC (290 mg h/dl) are shown in Fig. 3. False-positive profiles showed high 0.5- and 1-h PG levels; on the other hand, false-negative profiles showed slightly increased FPG or 2-h PG levels. These results indicate some discrepancy between the diagnostic criteria and glucose excursion after OGTT.
The correlations between peak glucose levels and PG-AUC, FPG levels, 1-h PG levels, and 2-h PG levels during OGTTs are shown in Fig. 4. The correlation between peak glucose levels and the PG-AUC was the highest (R 2 = 0.90), which was reasonable from the formula to calculate the area. Moreover, the correlations between PG-AUC and 1-h PG levels, 2-h PG levels and FPG levels during the OGTT are shown in Fig. 5. The correlation between the 1-h PG levels and PG-AUC was the highest (R 2 = 0.91). In most cases, plasma glucose levels reach the peak 30 min or 1-h after glucose loading; therefore, these results were again reasonable.
Discussion
Cutoff glucose AUC value for glucose intolerance screening
The cutoff value of the glucose AUC for glucose intolerance screening was set to 290 mg h/dl on the basis of analysis of ROC curves.
As diagnostic criteria, the upper glucose limits of NGT during OGTT are 110 mg/dl at fasting, 180 mg/dl 1-h after glucose load, and 140 mg/dl 2-h after glucose load. As reported previously, using these levels, the upper limit of the glucose AUC in NGT is 305 mg h/dl [11], which is 5 % higher than the cutoff value defined by the ROC curve. If the PG-AUC is >305 mg h/dl, then all patients are positive (glucose intolerant) in principle, indicating that the PG-AUC has the highest specificity with this cutoff value. However, this value is not suitable for screening because of the corresponding low sensitivity (78 %). Therefore, we determined that 290 mg h/dl is an appropriate glucose AUC cutoff value for glucose intolerance screening. We regard the proposal of this hopeful cutoff as one of the strengths of this study. Previously, we proposed the possible cutoff of the glucose AUC measured by our developing system described in a later section, but examinations were conducted with only a small number of subjects [11]. However, further validation of the cutoff value using a larger OGTT data set and/or in daily practice would be required in the future. Moreover, from the viewpoint of global consensus, using a data set including other races would also be required. Besides, each country might give importance to a different population to pick up at screening; investigation of this point is necessary.
Screening for glucose intolerance with glucose AUC
The area under the ROC curves for glucose intolerance screening was 0.96 for PG-AUC, 0.71 for HbA1c levels, 0.81 for FPG levels, and 0.86 for 2-h PG levels, indicating the usefulness of the glucose AUC for glucose intolerance screening. Using a cutoff value of 290 mg h/dl, PG-AUC screening was highly consistent with the diagnostic criteria (sensitivity, 90 %; specificity, 93 %). We examined the reason for this high concordance between PG-AUC screening and the diagnostic criteria. The group at increased risk of diabetes, IGT, and DM with normal FPG levels cannot be detected by FPG screening. The group at increased risk of diabetes with 1-h high glucose levels but normal 2-h PG levels cannot be detected by measuring only 2-h PG levels. On the other hand, PG-AUC includes whole glucose excursion, namely FPG, 1-h PG, and 2-h PG levels; thus, it yields superior information for high sensitivity/specificity screening. As mentioned in the “Materials and methods” section, the group at increased risk of diabetes based on the JDS criteria was classified as positive because these subjects have a higher risk of developing DM than those with NGT [4]. Regarding the early stage of glucose intolerance, the adequacy of this classification and treatment of NGT with high FPG levels (100 ≤ FPG < 110 mg/dl) require further investigation in a future study.
False-positive profiles showed high 0.5- and 1-h PG levels, indicating that large glucose AUCs were induced by delayed insulin secretion, a phenomenon known to occur during the early stage of glucose intolerance. On the other hand, false-negative profiles showed slightly increased FPG or 2-h PG levels and postload glucose excursion was relatively small, indicating a slight decrease in glucose tolerance in false-negative cases. DM sensitivity using this cutoff value was 98 %, and only one patient was classified as false negative. The glucose profile of this patient, which varied from 160 mg/dl before loading to 132 mg/dl at 30 min, 148 mg/dl at 60 min, and 103 mg/dl at 120 min, showed a typical pattern of insufficient fasting before the start of the 75-g OGTT.
The results of this study illustrate the usefulness of the glucose AUC during OGTT for glucose intolerance screening. We regard this point as another strength of our study; To our knowledge, this is the first examination of screening by the AUC calculated from blood sampling. Moreover, concerning cost-effectiveness, the Japanese medical service system does not admit the additional medical remuneration point because of the increase of blood sampling points. Hence, multiple blood sampling for calculation of the AUC requires the same cost as usual OGTT. However, although the glucose AUC may be a superior index for glucose intolerance compared with the existing indices, the need for multiple blood samples is burdensome on patients and the medical staff. Therefore, we have developed a minimally invasive glucose AUC monitoring system that allows convenient monitoring of postprandial glucose levels without blood sampling, and this system can be useful as a prescreening method for glucose intolerance before OGTT for diagnosis [11–14].
Usefulness of glucose AUC measurement
Peak glucose levels correlated with the PG-AUC most strongly (R 2 = 0.90), and the correlation was independent of glucose tolerance, indicating that the PG-AUC is a good surrogate marker for peak glucose levels. Although the OGTT was used for glucose loading in this study, it is also possible to apply this correlation between PG-AUC and peak glucose levels to daily meals. The American Diabetes Association and International Diabetes Federation guidelines describe the importance of peak postprandial glucose management [15, 16]. However, it is difficult to monitor peak glucose levels after a meal in daily practice, because the peak glucose time is strongly dependent on diet and glucose tolerance. Because the glucose AUC includes the whole postprandial glucose and peak glucose levels, the correlation between the peak glucose levels and glucose AUC was high but not dependent on the peak time, suggesting that peak glucose levels can be predicted by the presented minimally invasive glucose AUC monitoring system without consideration of the timing of measurement.
Moreover, the correlations among the PG-AUC and 1-h PG levels, 2-h PG levels, and FPG levels during the OGTT were examined. Although the PG-AUC correlated strongly with 1-h PG levels, the correlation of diabetes patients seemed to be dissociated from that of the others.
In the present study, the PG-AUC and peak glucose levels were based on glucose data measured 0, 30, 60, and 120 min after glucose loading. A detailed evaluation of the adequacy of this method in future studies would require continuous glucose monitoring to calculate the PG-AUC and detection of peak glucose levels.
Limitations
As already discussed, we consider the weaknesses of this study to be the limited population and number of races in the OGTT data as well as the limited examination of cost-effectiveness. These will be subjects of future investigations.
Conclusion
High screening sensitivity (90 %) and specificity (93 %) were obtained using a glucose AUC cutoff value of 290 mg h/dl according to OGTT data analysis with diagnostic criteria, and the screening rate was improved compared with those obtained using HbA1c, FPG, and 2-h PG levels. From these findings, we propose that the glucose AUC, which reflects the entire glucose excursion, could be useful as an index of glucose tolerance.
References
The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329:977–86.
Diabetes Prevention Program Research Group. Reduction in the incidence of type 2 diabetes with lifestyle intervention of metformin. N Engl J Med. 2002;246:393–403.
Sakane N, Sato J, Tsushita K, Tsujii S, Kotani K, Tsuzaki K, Tominaga M, Kawazu S, Sato Y, Usui T, Kamae I, Yoshida T, Kiyohara Y, Sato S, Kuzuya H, Japan Diabetes Prevention Program (JDPP) Research Group. Prevention of type 2 diabetes in a primary healthcare setting: three-year results of lifestyle intervention in Japanese subjects with impaired glucose tolerance. BMC Public Health. 2011;11:40–7.
Kuzuya T, Nakagawa S, Satoh J, Kanazawa Y, Iwamoto Y, Kobayashi M, Nanjo K, Sasaki A, Seino Y, Ito C, Shima K, Nonaka K, Kadowaki T, Committee of the Japan Diabetes Society on the diagnostic criteria of diabetes mellitus. Report of the Committee on the classification and diagnostic criteria of diabetes mellitus. Diabetes Res Clin Pract. 2002;55:65–85.
Standards Australia. Australian standard glycemic index of food. Sydney: Standards Australia; 2007.
Terra SG, Somayaji V, Schwartz S, Lewin AJ, Teeter JG, Dai H, Nguyen TT, Calle RA. A dose-ranging study of the DPP-IV inhibitor PF-734200 added to metformin in subjects with type 2 diabetes. Exp Clin Endocrinol Diabetes. 2011;119:401–7.
Sosenko JM, Palmer JP, Greenbaum CJ, Mahon J, Cowie C, Krischer JP, Chase HP, White NH, Buckingham B, Herold KC, Cuthbertson D, Skyler JS, Diabetes Prevention Trial-Type 1 Study Group. Increasing the accuracy of oral glucose tolerance testing and extending its application to individuals with normal glucose tolerance for the prediction of type 1 diabetes: the Diabetes Prevention Trial-Type 1. Diabetes Care. 2007;30:38–42.
Japan Diabetes Society. Guidance for standard treatment of diabetes mellitus 2014–2015. Bunkodo; 2014.
Kashiwagi A, Kasuga M, Araki E, Oka Y, Hanafusa T, Ito H, Tominaga M, Oikawa S, Noda M, Kawamura T, Sanke T, Namba M, Hashiramoto M, Sasahara T, Nishio Y, Kuwa K, Ueki K, Takei I, Uemoto M, Murakami N, Yamakado M, Yatomi Y, Ohashi H, Committee on the Standardization of Diabetes Mellitus-Related Laboratory Testing of Japan Diabetes Society. International clinical harmonization of glycated hemoglobin in Japan: from Japan Diabetes Society to National Glycohemoglobin Standardization Program values. J Diabetes Investig. 2012;3:39–40.
Olson DE, Rhee MK, Herrick K, Ziemer DC, Twombly JG, Phillips LS. Screening for diabetes and pre-diabetes with proposed A1C-based diagnostic criteria. Diabetes Care. 2010;33:2184–9.
Sakamoto K, Kubo F, Yoshiuchi K, Ono A, Sato T, Tomita K, Sakaguchi K, Matsuhisa M, Kaneto H, Maegawa H, Nakajima H, Kashiwagi A, Kosugi K. Usefulness of a novel system for measuring glucose area under the curve while screening for glucose intolerance in outpatients. J Diabetes Investig. 2013;4:552–9.
Sato T, Okada S, Hagino K, Asakura Y, Kikkawa Y, Kojima J, Watanabe T, Maekawa Y, Isobe K, Koike R, Nakajima H, Asano K. Measurement of glucose area under the curve using minimally invasive interstitial fluid extraction technology: evaluation of glucose monitoring concepts without blood sampling. Diabetes Technol Ther. 2011;13:1194–200.
Sakaguchi K, Hirota Y, Hashimoto N, Ogawa W, Sato T, Okada S, Hagino K, Asakura Y, Kikkawa Y, Kojima J, Maekawa Y, Nakajima H. A minimally invasive system for glucose area under the curve measurement using interstitial fluid extraction technology: evaluation of the accuracy and usefulness with oral glucose tolerance tests in subjects with and without diabetes. Diabetes Technol Ther. 2012;14:485–91.
Sakaguchi K, Hirota Y, Hashimoto N, Ogawa W, Hamaguchi T, Matsuo T, Miyagawa J, Namba M, Sato T, Okada S, Tomita K, Matsuhisa M, Kaneto H, Kosugi K, Maegawa H, Nakajima H, Kashiwagi A. Evaluation of a minimally invasive system for measuring glucose area under the curve during oral glucose tolerance tests: usefulness of sweat monitoring for precise measurement. J Diabetes Sci Technol. 2013;7:678–88.
American Diabetes Association. Standards of medical care in diabetes-2014. Diabetes Care. 2014;37:S14–80.
International Diabetes Federation. Guideline for Management of Postmeal Glucose: Brussels; 2011.
Acknowledgments
This study was conducted by the Minimally Invasive Interstitial Fluid Extraction Technology (MIET) Study Group, which includes the following members: A. Kashiwagi, H. Maegawa (Shiga University of Medical Science), H. Kaneto (Osaka University), K. Kosugi (Osaka Police Hospital), H. Nakajima, K. Tomita (Osaka Medical Center for Cancer and Cardiovascular Diseases), M. Matsuhisa (Tokushima University), and K. Sakaguchi. This study was sponsored by Sysmex Corp.
Conflict of interest
Regarding this article, K. Sakaguchi received research funding from Sysmex Corp. H. Nakajima is a medical advisor for GlaxoSmithKline K.K. T. Sato, S. Okada, and Y. Ohnishi are employees of Sysmex Corp. No other potential conflicts of interest relevant to this article were reported.
Human rights statement and informed consent
All the data used for this study were unlinkable and anonymous. Therefore, this study is exempt from the institutional and national standards of ethics.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Sakaguchi, K., Takeda, K., Maeda, M. et al. Glucose area under the curve during oral glucose tolerance test as an index of glucose intolerance. Diabetol Int 7, 53–58 (2016). https://doi.org/10.1007/s13340-015-0212-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-015-0212-4