Abstract
Objective
To compare parameters of insulin resistance, with special reference to McAuley index, in urban Indian adolescents, and to establish their cut-off values for defining metabolic syndrome.
Design
Cross-sectional study.
Setting
Schools located in four different geographical zones of Delhi, India.
Participants
695 apparently healthy adolescents grouped as normal weight (298), overweight (205) and obese (192).
Outcome measures
Cut-off point for indices of insulin resistance was assessed by fasting insulin, insulin glucose ratio, and other methods (HOMA model, QUICKI, McAuley index) to define metabolic syndrome.
Results
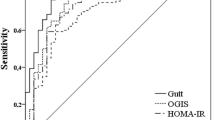
The McAuley index increased progressively from normal weight to obese adolescents in both sexes. McAuley index was significantly lower in adolescents with metabolic syndrome (5.36 ± 1.28 vs. 7.05 ± 1.88; P<0.001). McAuley index had the highest area under curve of receiver operator characteristics [0.82 (0.02)] as compared to other indices of insulin resistance. McAuley index of 6.23 had the highest specificity (88%) with sensitivity of 63.3% for diagnosing metabolic syndrome, whereas insulin glucose ratio had the highest sensitivity (79.7%) but low (55.5%) specificity. McAuley index was negatively correlated with height (r= −0.257, P=<0.001), weight (r= −0.537, P=<0.001), body mass index (r= −0.579, P<0.001), waist circumference (r= −0.542, p<0.001), and waist hip ratio (r= −0.268, P<0.001).
Conclusions
Among various parameters of insulin resistance, McAuley index had the highest specificity, and insulin glucose ratio had the highest sensitivity in diagnosing metabolic syndrome in urban Indian adolescents.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Gupta N, Goel K, Shah P, Misra A. Childhood obesity in developing countries: epidemiology, determinants, and prevention. Endocr Rev. 2012;33:48–70.
Muniyappa R, Lee S, Chen H, Quon MJ. Current approaches for assessing insulin sensitivity and resistance in vivo: advantages, limitations, and appropriate usage. Am J Physiol Endocrinol Metab. 2008;294:E15–E26.
Matthews DR, Hosker JP, Rudenski AS, Burnett MA, Darling P, Bown EG, et al. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia. 1985;28:412–419.
Katz A, Nambi SS, Mather K, Baron AD, Follmann DA, Sullivan G, et al. Quantitative insulin sensitivity check index: a simple, accurate method for assessing insulin sensitivity in humans. J Clin Endocrinol Metab. 2000;85:2402–2410.
McAuley KA, Williams SM, Mann JI, Walker RJ, Ledwis-Barned NJ, Temple LA, et al. Diagnosing insulin resistance in the general population. Diabetes Care. 2001;24:460–464.
Ascaso JF, Pardo S, Real JT, Lorente RI, Priego A, Carmena R. Diagnosing insulin resistance by simple quantitative methods in subjects with normal glucose metabolism. Diabetes Care. 2003;26:3320–3325.
Ruige JB, Mertens IL, Bartholomeeusen E, Dirinck E, Ferrannini E, Van Gaal LF. Fasting-based estimates of insulin sensitivity in overweight and obesity: a critical appraisal. Obesity (Silver Spring). 2006;14:1250–1256.
Hettihawa LM, Palangasinghe S, Jayasinghe SS, Gunasekara SW, Weerarathna TP. Comparison of insulin resistance by indirect methods — HOMA, QUICKI and McAuley -with fasting insulin in patients with type 2 diabetes in Galle, Sri Lanka: A pilot study. Online J Health Allied Sc. 2006;1:2.
Shand BI, Scott RS, Lewis JG, Elder PA, Frampton CM. Comparison of indices of insulin resistance with metabolic syndrome classifications to predict the development of impaired fasting glucose in overweight and obese subjects: a 3-year prospective study. Int J Obes (Lond). 2009;33:1274–1279.
Antuna-Puente B, Disse E, Faraj M, Lavoie ME, Laville M, Rabasa-Lhoret R, et al. Evaluation of insulin sensitivity with a new lipid-based index in non-diabetic postmenopausal overweight and obese women before and after a weight loss intervention. Eur J Endocrinol. 2009;161:51–56.
Lorenzo C, Haffner SM, Stancáková A, Laakso M. Relation of direct and surrogate measures of insulin resistance to cardiovascular risk factors in nondiabetic Finnish offspring of type 2 diabetic individuals. J Clin Endocrinol Metab. 2010;95:5082–5090.
Tandon N, Garg MK, Singh Y, Marwaha RK. Prevalence of metabolic syndrome in urban Indian adolescents and its relation with insulin resistance (HOMA-IR). J Pediatr Endocrinol Metab. 2013;26:1123–1130.
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH. Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ. 2000;320:1240–1243.
Kurian R, Thomas T, Lokesh DP, Sheth NR, Mahendra A, Joy R, et al. Waist circumference and waist for height percentiles in urban South Indian children aged 3–16 years. Indian Pediatr. 2011;48:765–771.
The fourth report on the diagnosis, evaluation, and treatment of high blood pressure in children and adolescents. Pediatrics. 2004;114:555–576.
P Zimmet. The IDF Consensus Definition of the Metabolic Syndrome in Children and Adolescents. Available from: www.idf.org/webdata/docs/Mets_definition_children.pdf . Assessed August 23, 2013.
Third report of the National Cholesterol Education Program Expert Panel on Detection, Evaluation and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Bethesda, Md.: National Heart, Lung, and Blood Institute, May 2001.
Marwaha RK, Khadgawat R, Tandon N, Kanwar R, Narang A, Sastry A, et al. Reference interval of lipid profile in healthy school children and adolescents. Clin Biochem. 2011;44:760–766.
Martínez-Larrad MT, Lorenzo C, González-Villalpando C, Gabriel R, Haffner SM, Serrano-Ríos M. Associations between surrogate measures of insulin resistance and waist circumference, cardiovascular risk and the metabolic syndrome across Hispanic and non-Hispanic white populations. Diabet Med. 2012;29:1390–1394.
Thompson WG, Slezak JM. Correlations between measures of insulin sensitivity and weight loss. Diabetes Res Clin Pract. 2006;74:129–134.
Hancox RJ, Landhuis CE. Correlation between measures of insulin resistance in fasting and non-fasting blood. Diabetol Metab Syndr. 2011 7;3:23.
Grant AM, Taungapeau FK, McAuley KA, Taylor RW, Williams SM, Waldron MA, et al. Body mass index status is effective in identifying metabolic syndrome components and insulin resistance in Pacific Island teenagers living in New Zealand. Metabolism. 2008;57:511–516.
Hettihewa LM, Weerarathna TP. Comparison of McAuley/fasting insulin indices with ATP III clinical criteria for the diagnosis of insulin resistance in type 2 diabetes mellitus. J Pharmacol Pharmacother. 2011;2:165–169.
Vyssoulis GP, Liakos CI, Karpanou EA, Triantafyllou AI, Michaelides AP, Tzamou VE, et al. Impaired glucose homeostasis in non-diabetic Greek hypertensives with diabetes family history. Effect of the obesity status. J Am Soc Hypertens. 2013;7:294–304.
Hydrie MZI, Basit A, Fawwad A, Ahmedani MY, Shera AS, Hussain A. Detecting insulin resistance in Pakistani subjects by fasting blood samples. Open Diab J. 2012;5:20–24.
Snehalatha C, Nanditha A, Shetty AS, Ramachandran A. Hypertriglyceridaemia either in isolation or in combination with abdominal obesity is strongly associated with atherogenic dyslipidaemia in Asian Indians. Diabetes Res Clin Pract. 2011;94:140–145.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Garg, M.K., Tandon, N., Marwaha, R.K. et al. Evaluation of surrogate markers for insulin resistance for defining metabolic syndrome in urban Indian adolescents. Indian Pediatr 51, 279–284 (2014). https://doi.org/10.1007/s13312-014-0401-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-014-0401-4