Abstract
The selective and efficient drug delivery to tumor cells can remarkably improve different cancer therapeutic approaches. There are several nanoparticles (NPs) which can act as a potent drug carrier for cancer therapy. However, the specific drug delivery to cancer cells is an important issue which should be considered before designing new NPs for in vivo application. It has been shown that cancer cells over-express folate receptor (FR) in order to improve their growth. As normal cells express a significantly lower levels of FR compared to tumor cells, it seems that folate molecules can be used as potent targeting moieties in different nanocarrier-based therapeutic approaches. Moreover, there is evidence which implies folate-conjugated NPs can selectively deliver anti-tumor drugs into cancer cells both in vitro and in vivo. In this review, we will discuss about the efficiency of different folate-conjugated NPs in cancer therapy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Nanomedicine is a recent expanded novel technology, with various advantages for diagnosis and treatment of several disorders such as autoimmunity and cancer. Since the current therapeutic methods are usually ineffective for cancer, it seems that the identification of novel methods, which are safe and effective, is required [1]. Surgery, radiation, and chemotherapy are conventional tumor therapeutic approaches, which destruct both tumor and normal cells. As nanoscale therapeutic materials demonstrate several features such as nontoxic, biodegradable, non-immunogenic, biocompatible, and gradual long-time drug release, they can be considered as potent candidates in cancer therapy [2]. It has been shown that nanoparticles (NPs) can be applied for various purposes, including drug delivery, diagnosis, and regenerative medicine. NPs can act as worthy drug carriers, which is in part due to their unique properties such as protection of drugs against degradation in the circulation before they reach their target site, promotion of drug absorption in cancer cells and tissues, and gradual drug release [3].
As mentioned, non-specific action of common anti-cancer drugs leads to destruction of both tumor and normal cells. Thus, targeted cancer therapy can increase the efficiency of current therapeutic approaches. Consistently, modification of different NPs for specific targeting is of great importance for a targeted therapy [4]. There are two general targeting methods, including passive and active targeting approaches. The unique physiologic properties of tumor microenvironment and physicochemical features of NPs facilitate the preferred accumulation of nanocarriers in tumor tissues. This is the main objective of passive targeting. In spite of preferred accumulation of nanocarriers through passive mechanisms, there is some degree of non-specific action in this method. Moreover, passive targeting does not guarantee the cellular uptake of drug-loaded NPs. Furthermore, although the passively targeted NPs can accumulate within the tumor site, they can also diffuse out of the tumor region and back into the blood circulation. Active targeting approaches can significantly decrease the non-specific action of passively targeted nanocarriers. Active targeting can be performed through surface conjugation of nanocarriers to various targeting molecules such as antibodies against tumor markers, aptamers, carbohydrates, vitamins and peptides or ligands of some overexpressed molecules on tumor cells such as transferrin and folate (vitamin B9) [5]. It has been reported that folate receptor (FR) is overexpressed on the surface of several cancers, including breast, kidney, lung, brain, and ovary cancers [6]. Folate can bind to FR and facilitate the transfer of folate-targeted NPs through receptor-mediated endocytosis. Folic acid is an essential nutrient needed by all cells for biosynthesis of nucleotide and normal action of some metabolic pathways. It has been shown that FR has high affinity (Kd»10−10 M) for the folic acid (FA) [7] and mediates the cellular uptake via a non-destructive [6], endosomal pathway [3]. Regarding the limited expression of FR on normal tissues and its overexpression on tumor cells [6], it seems that folate may be an appropriate choice for targeting tumor cells in NP-based cancer therapies. FR can internalize its ligand into the cytosol, because it is linked to the lipid region of the cell membrane. Following migration of FR and its contents to inner side of membrane, the acidic microenvironment of interior side (pH of approximately 5) leads to dissociation of FR from the folate-conjugated NPs. Thus, folate-conjugated NPs can then release into the cytosol of the tumor cells following migration to the interior surface of the cell membrane (Fig. 1) [7]. As mentioned, folate-targeting can effectively increase the efficiency of cancer therapy, as several tumor cells over-express FR on their surface. Consistently, several drugs have conducted toward tumor tissues through various FA-conjugated NPs (Fig. 2) [8]. In here, we summarize the recent advances regarding the use of folate-conjugated NPs in cancer therapy.
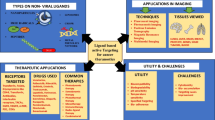
The representative schematic platform for site-specific drug delivery through folate-conjugated pH-sensitive NPs. Folate-targeted NPs reach and bind to tumor cells with high affinity due to the overexpression of folate receptors on tumor cells. Tumor cells take these multifunctional NPs via FR-mediated endocytosis mechanism, by which these nanocarriers enter into the endosomal vesicles in which they are exposed to an acidic microenvironment. In the acidic pH of endosomes (or cytoplasm), NPs release encapsulated drug (doxorubicin) and kill cancer cell. Drugs may simply be loaded in targeted NPs or conjugated to reactive groups in NPs directly or by some environment-sensitive drug-binding linkers. These linkers will be broken in the reductive/acidic microenvironment of cytoplasm of tumor cells, which then leads to drug release and death of tumor cells
A schematic representation of some NPs used as drug delivery systems. a Micelles are self-assembled amphiphilic NPs that can encapsulate both lipophilic or lipophobic drugs. b Albumin can deliver lipophilic molecules to cancer cells. c Drug-loaded magnetic NPs can be magnetically conducted into cancer cells using an external magnet. d Mesoporous silica NPs can be used as multifunctional drug delivery system. e Gold NPs can be used as multifunctional imaging and therapeutic agents. f Dendrimers have ability to encapsulate or covalently conjugate drugs, targeting moieties, and imaging agents. g Chitosan NPs have wide variety of advantages to deliver several therapeutic molecules to cancer cells
Polymeric micelles
Polymeric micelles are nanosized core/shell particles constituted by amphiphilic block copolymers [9]. The hydrophilic shell of the micelle increases its circulation time in the body and inhibits its uptake by the mononuclear phagocyte system [10]. Micelles with a size range of 5–100 nm have the inner hydrophobic core, which enables them to engulf poorly water-soluble drugs [9]. Polyesters, polyethers, and polyamino acids are commonly used polymers for hydrophobic core of micelles [11]. Polymeric micelles possess several strong advantages, such as their physicochemical properties for tumor targeting by a passive targeting mechanism called the enhanced permeability and retention effect [12]. For targeting the tumor at inaccessible sites, the drug should be administered by the parenteral route, and pharmaceutical drug carriers carrying drug in plasma should possess properties like biodegradability, small particle size, high loading capacity, prolonged circulation, and accumulation in the required pathological site in the body [12]. Compared with other drug carriers, micelles have the advantage because of their very small size, which is critical for passive targeting to solid tumors, particularly the poorly vascularized tumors. Micelles have demonstrated a variety of shapes such as spheres, rods, vesicles, tubules, and lamellae, which lead to a significant impact on the pharmacokinetic properties of micelles [13]. These nanocarriers can act as potent drug reservoirs and are able to provide the high concentrations of the drug in tumor tissues. Micelles are mainly applied for drug solubilization, controlled drug release, and drug targeting [13]. Drug release from micelles at target site can be managed through various mechanisms such as pH-, thermo-, ultrasound-, and light-sensitivity [14, 15].
It is demonstrated that folate conjugation can increase the stability of FA-poly(ethylene glycol) (PTL-PLA-MPEG/PEG-FA) micelle compared to poly(L-lactic acid)-block-methoxy poly(ethylene glycol) copolymer (PLA-MPEG), which was in part due to the lower micelle concentration [16]. Similarly, it is reported that FA-conjugated doxorubicin (DOX)-loaded PLA-PEG-based polymeric micelles exhibit a potent cytotoxicity against FR-expressing SKOV3 human ovarian cancer cells, in vitro [17].
FA-conjugated micelles have been shown to exert potent anti-tumor effect both in vitro and in vivo. Scarano and colleagues have shown that both small and large FA-conjugated micelles loaded with platinum drugs exert higher anti-tumor effects on FR-expressing cell line OVCAR-3 compared to FR-negative A549 cells [18]. In another study, Gao et al. showed the inhibition of tumor cells metastasis in 4T1 tumor-bearing mice by DOX-loaded FA-targeted pH-sensitive polymeric micelles. FA-conjugated micelles could effectively inhibit tumor growth and metastasis and increase mice survival [14]. Gue et al. have also showed that DOX-conjugated FA-conjugated PEG-poly(ε-caprolactone) micelles exert potent anti-tumor function in both in vitro and in vivo. In this nanoformulation, DOX was connected with a hydrazone linker (FA-hyd) for a pH-mediated drug release. They demonstrated that FA-hyd micelles had significantly more circulation time and enriched drug into the tumors rather than normal tissues [19]. The similar results were reached in another investigation using two series of FA-targeted pH-sensitive amphiphilic block copolymers, poly(ε-caprolactone)-b-poly[triethylene glycol methacrylate-co-N-methacryloyl caproic acid] and poly(ε-caprolactone)-b-poly[triethylene glycol methacrylate-co-N-(2-(methacrylamido)ethyl] in vitro in FR-positive (HeLa) and FR-negative (HT-29) tumor cell lines [20]. There are other reports, which applied pH-dependent drug release approach for the control of tumor growth in FA-targeted micelles. For example, while Bae et al. used FA-PEG-poly(aspartate hydrazone adriamycin) [FA-PEG-P(Asp-Hyd-ADR)] to stop the growth of human pharyngeal cancer cells (KB cell) in vitro [21], Liu and coworkers developed DOX-loaded poly(N-isopropylacrylamide-co-N,N-dimethylacrylamide-co-2-aminoethyl methacrylate)-b-poly(10-undecenoic acid) (P(NIPAAm-co-DMAAm-co-AMA)-b-PUA) micelles in order to attenuate tumor burden in 4T1 tumor-bearing mice and KB cells [22]. Song and colleagues developed redox- and pH-sensitive FA-targeted DOX-loaded polyurethane nanomicelles, which controlled the growth of FR-positive HeLa cells in vitro [23].
In addition to pH-sensitive NPs, thermosensitive FA-conjugated micelles are also developed, which showed good stability. For instance, 5-fluorouracil (5-FU)-loaded poly(N-vinylcaprolactam)-b-PEG-FA micelles with a lower critical solution temperature of 33 °C were generated, which showed a slow and sustained release at 37 °C up to 30 h. Moreover, while FA-targeted micelles exerted remarkable toxicity against FR-positive 4T1 cells, they had no significant toxicity on FR-negative EA.hy 926 human endothelial cell line [24]. Interestingly, it has been demonstrated that polymeric micelles can also be used for photodynamic therapy (PDT). In this method, a tumor tissue is destroyed through light-induced chemical reaction. Consistently, Syu et al. generated a FA-conjugated meta-tetra (hydroxyphenyl)chlorin (m-THPC)-loaded micelles. They showed that FA-conjugated m-THPC-loaded micelles are engulfed and accumulated by FR-expressing KB cells both in vitro and in vivo. Moreover, the encapsulated m-THPC had no remarkable side effects on the body weight of mice [25]. Regarding these reports (Table 1), it seems that FA-targeted nanomicelles may be considered as potent devices in drug delivery into FR-positive tumors. However, little is known regarding the efficiency of these NPs in in vivo human tumors, and this issue needs further investigations.
Albumin nanoparticles
The protein nanoparticles can bind to a large number of drugs in a relatively non-specific manner. Because of their surface charge, drugs can physically adsorb onto the protein surface or can covalently bind to the matrix. Bovine serum albumin (BSA) and human serum albumin (HSA) have been widely used over the past 30 years to prepare micro- and NPs [26]. HSA is a negatively charged plasma protein (42–54 g/l) with a small size, which is produced in the liver and involved in different physiological processes such as long-chain fatty acids solubilization, nutrients delivery to cells, induction of colloidal osmotic pressure in the blood, controlling plasma pH, and binding to bilirubin and drugs. As HSA is a source of amino acid for metabolism of cells, albumin can be used as a carrier for the drug delivery to tumor cells [27]. Tumor cells secrete an albumin-binding protein (also known as BM-40), which can help to the preferential uptake of albumin NPs by these cells [28]. Albumin NPs have several advantages such as biodegradability, less toxicity and antigenicity, high stability, controllable drug release, shelf life, and high loading potential for hydrophilic drugs, which make them a potent candidate in drug delivery to tumor cells [29]. Conjugation of albumin NPs with folate can provide site-specific targeting properties for these NPs [4]. Consistently, there is evidence, which implies the effectiveness of FA-conjugated albumin NPs in drug delivery to cancer cells [29, 30] (Table 1). Zhang et al. showed that FA-conjugated BSA NPs could effectively uptake SKOV3 cells in vitro [29]. It has also been reported that FA-conjugated paclitaxel-loaded BSA NPs selectively deliver anti-cancer drug into a human prostate cancer PC3 cells [30]. The first HSA-based NP formulation, ABI 007 (Abraxane®), was approved by the Food and Drug Administration (FDA) in 2005 [31]. ABI-007 is a novel, albumin-bound, 130-nm particle formulation of paclitaxel, free from any kind of solvent (polyethoxylated castor oil—Cremophor-free). It is used as a colloidal suspension derived from the lyophilized formulation of paclitaxel and HSA diluted in saline solution. In detail, HSA stabilizes the drug particle at an average size of 130 nm which prevents any risk of capillary obstruction and does not necessitate any particular infusion systems or steroid/antihistamine premedication before the infusion [32]. There are some trials related to the use of albumin-based NPs for treatment and diagnosis of breast and brain tumors, respectively [33, 34]. Hao et al. have recently prepared FA-conjugated DOX-loaded BSA-dextran NPs for cancer drug delivery. It should be noted that the dextran shell makes the NPs more dispersible in solution. They showed that these NPs allow to the administration of the higher doses of DOX and exert remarkable anti-tumor activity in murine ascites hepatoma H22 tumor-bearing mice [35]. The similar results have been observed following the use of DOX-loaded FA-conjugated albumin nanospheres in FR-positive HeLa cells and FR-negative aortic smooth muscle cells (AoSMC) [36]. FA-targeted 5-FU-loaded BSA-carboxymethyl-β-cyclodextrin NPs have also exhibited high inhibition and promote apoptosis in FR-expressing HeLa cells as compared to free drug and non-targeted NPs [37]. It has recently been demonstrated that FA-conjugated ergosta-4,6,8(14),22-tetraen-3-one (ergone)-loaded albumin nanospheres could selectively kill KB tumor cells, in vitro. In vivo experiments using murine animal models more substantiated the efficacy of these NPs in tumor targeting [38]. FA-conjugated albumin NPs could selectively deliver vinblastine sulfate (VBLS) anti-cancer drug to tumor cells [39]. The intravenous administration of tamoxifen-loaded FA-conjugated albumin NPs to nude mice carrying xenograft MCF-7 tumors was associated with potent anti-tumor effects and the lowest levels of drug accumulated in non-targeted tissues [40]. On the other hand, Yang and colleagues have shown that administration of FA-conjugated BSA nanospheres comprising DOX and encapsulated magnetic iron oxide in combination with hyperthermia significantly decreases the adverse effects and improves the therapeutic effect of anti-tumor drugs in both in vitro and in vivo [41]. Similarly, mitoxantrone-loaded FA-conjugated albumin NPs could effectively control the growth of SKOV3 tumor cells both in vitro and in vivo [42].
Regarding high compatibility, availability, and drug loading, it seems that FA-conjugated albumin NPs may have a potent therapeutic potential as the vector of anti-cancer drugs.
Magnetic nanoparticles
Superparamagnetic NPs made from ferrite oxide-magnetite (Fe3O4) are the most magnetic NPs used in biological applications [43]. Magnetic NPs can be manipulated through magnetic field [44]. Although the application of magnetic NPs dates back to the 1970s [45], high attention has recently been focused on them, which is in part related to their unique features such as high surface to volume ratio, quantum size effect, and magnetic character [45, 46]. Although the size and surface functionality of magnetic NPs remarkably affect their efficiency, superparamagnetic iron oxide NPs (SPIOs) diameters mainly affect their in vivo biodistribution. Moreover, ultra-small SPIOs with diameters of 10 to 40 nm show prolonged blood circulation and cross capillary walls and are usually engulfed by macrophages [47]. Magnetic NPs can be applied in several ways, including magnetic drug targeting [46], magnetic fluid hyperthermia [48], and contrast agents for magnetic resonance imaging (MRI) [49, 50, 46, 51, 52]. Among the magnetic NPs, Fe3O4 NPs are only approved by the US FDA for clinical use [53, 45]; however, it has a short half-life, no specific tumor-targeting effect, and readily phagocytosed by mononuclear phagocyte system and removed by macrophages [41]. Magnetic NPs are usually composed of inner magnetic core (Fe3O4 or Fe2O3) and an outer polymeric shell. The polymeric shell provides biocompatibility, prevents agglomeration, and acts as a drug reservoir. Several polymers such as starch, dextran [54, 55], PEG [51, 56], fatty acids, polyvinyl alcohol [57], polyacrylic acid, poly lactides, gelatin, silica [58, 59, 56], oleic acid [60, 61], PLGA or poly(D,L-lactic-co-glycolic acid) [62], polyethylene imine (PEI) [63], poly methyl methacrylate (PMMA), and polyacrylic acid (PAA) [59, 64], albumin [50, 41], and chitosan [64] have been used as coating materials for different purposes. Conjugation of outer shell with different targeting molecules can promote site-specific function of magnetic NPs. It has been shown that conjugation of SPIOs with amino-terminal fragment [65] and RGD peptides [66] could specifically target tumor cells. Moreover, the amino-functionalized Fe3O4, MnFe2O4, and Mn3O4 magnetic NPs conjugated with rhodamine B (a fluorescent dye) and FA could specifically target cancer cells overexpressing FRs [67]. Similarly, it is reported that FA-conjugated Fe3O4 NPs modified by dopamine-PEG-NH2 and fluorescein isothiocyanate (FITC) could effectively recognize the FR-positive MCF-7 cells, but not the FR-negative A549 cells [49]. Interestingly, it is suggested that microbial exopolysaccharides can be applied as biocompatible shell polymers for magnetic NPs. Sivakumar and colleagues have recently demonstrated that 5-FU-loaded FA-conjugated magnetic NPs coated with bacterial exopolysaccharides mauran and gellan gum in combination with hyperthermia effectively killed cancer cells. They have recommended that mauran and gellan gum coated magnetic NPs have high biocompatibility, low cytotoxicity, high therapeutic potential, and superparamagnetic behavior that can be applied as worthy tools for bacterial exopolysaccharide-based targeted drug delivery, cancer cell imaging, and magnetic hyperthermia [68]. Most recently, Ma and coworkers generated FA-albumin conjugated SPIO NPs, which had a strong MRI efficacy in MCF-7 and SPC-A-1 cells due to the recognition of FR [50]. DOX-loaded FA-targeted magnetic Fe3O4 NPs could also significantly kill C30 and CP70 human ovarian cancer cells in vitro, which was associated with downregulation of bcl-2 and survivin and upregulation of caspase-3 [69]. Similar results were observed when FA-conjugated SPIO-based magnetic NPs were incubated with human leukemic CCRF-CEM cells [70]. Similarly, idarubicin-loaded PEG-covered magnetic NPs showed higher toxicity in MCF-7 cells compared to free idarubicin [71]. Interestingly, it has recently been demonstrated that the peroxidase-like activity of Fe3O4@ carbon NPs can modulate oxidative stress induced by ascorbic acid for the selective killing of PC-3 prostate cancer cells through production of high levels of endogenous ROS [72]. In addition, Li et al. have demonstrated that amine-modified group in the surface of core-shell Fe2O3@ carbon NPs can be functionalized with PEG and FA to enhance their solubility in aqueous solution and target cancer cells [73].
It is suggested that incorporation of Fe3O4 into FA-conjugated BSA NPs inhibits their clearing by mononuclear phagocyte system [41, 50]. Active targeting through FA-conjugated magnetic NPs is mainly dependent to density of FA on magnetic NPs and FR on the tumor cells as assessed in 4T1 bearing BALB/c mice [74].
The higher sensitivity of tumor cells to high temperatures compared to normal cells, which is in part due to hypoxic condition of tumor area, led to a combinatorial application of magnetic NPs and hyperthermia to destroy tumor cells [75, 76, 68]. Addition of some chemotherapeutic drugs in the above-mentioned combination therapy could increase the efficacy of tumor cell killing [77–79, 68]. There are studies which indicate the administration of chemotherapeutic drugs (daunorubicin and 5-bromotetrandrine)-loaded Fe3O4 magnetic NPs suppresses tumor proliferation and enhances apoptosis in a dose- and time-dependent manner, both in vitro and in vivo [80, 81].
Several other biocompatible magnetic NPs such as dextran-stabilized magnetic fluid, aminosilane-modified NPs, cationic magnetoliposomes, and affinity magnetoliposomes have also been used for hyperthermia treatment [82, 83]. Magnetic hyperthermia makes it possible for the heating to be limited to the tumor site [84, 85, 68]. The use of external magnetic field in combination with magnetic NPs can conduct magnetic nanocarrier to the desired tumor site, fix them, and release the drug locally [86–88]. It is demonstrated that combination of hyperthermia and chemotherapy not only increases the drug concentration in tumor cells but also decreases the drug-related adverse effects to normal tissue and inhibits the drug resistance [89, 79]. The unique feature of tumor cells to absorb magnetic NPs (8–400-fold more than normal cells) makes them highly susceptible to magnetic fluid hyperthermia [41].
Electromagnetic fields (EMFs) are other noninvasive useful devices, which can be applied in combination with magnetic NPs. It is demonstrated that frequencies lesser than 300 Hz (known as extremely low frequency or ELF) do not exert damage to deoxyribonucleic acid (DNA) [62]. Using this approach, Wen and colleagues have shown that FA-conjugated magnetic NPs in combination with ELF-EMF could selectively induce apoptosis in BEL-7402 liver cancer cells [53]. ELF-EMF enhances anti-tumor function of magnetic NPs in part through affecting cell ion metabolism via the reduction of cation-exchange across the cell membrane [90]. The possibility of combining magnetic NPs with other cancer therapeutic methods makes them as worthy candidates for cancer therapy (Table 2).
Mesoporous silica nanoparticles (MSN)
Silica has more biocompatibility and lower cytotoxicity than other metal oxides such as titania and iron oxide [91]. The high levels of silanol groups in silica enhance its affinity to phospholipids, so it can be easily taken up by the cells. The high surface area (>900 m2/g) and pore volume (>0.9 cm3/g) make it possible to load high doses of different drugs [92]. Due to the presence of strong Si–O bond [93] in silica NPs, they have high resistance against mechanical stress, heat, pH, and hydrolysis-induced degradations compared to liposomes and dendrimers [92, 94, 95]. The sol-gel process is a common methodology to create mesoporous silica NPs [96]. The rate of drug release from mesoporous silica NPs depends on the size of pores, which can be controlled by the processing parameters, such as temperature, pH, solvents, raw materials, catalysts, precursor, and additives in different concentrations [97, 91]. MCM-41 and SBA-15 are two common mesoporous silica materials, which have different pore sizes, including 2–5 nm and 5–10 nm, respectively. The smaller pore size helps to slow drug release and provides higher stability in mesoporous silica NPs [98, 97, 92]. In addition, the surface functionalization of silica NPs with different molecules allows developing silica NPs with various surface properties [96, 99]. Regarding the high expression of FR on tumor cells, several studies have tried to conjugate mesoporous silica NPs with FA to achieve effective drug delivery to tumor cells [100, 93, 101, 102] (Table 3). Consistently, it is reported that FA-targeted camptothecin or paclitaxel-loaded multifunctional mesoporous silica NPs could be effectively used for cancer imaging, targeting, and drug delivery in FR-expressing human pancreatic cancer cells PANC-1 and BxPC-3 [93]. Fan and colleagues have developed the pH-sensitive FA-conjugated DOX-loaded mesoporous silica NPs, which could selectively kill FR-expressing HeLa cells, but not FR-negative A549 and L929 cells [100]. Mahapatra and coworkers have also produced FA-conjugated hybrid NPs composed of multifunctional mesoporous hollow silica NPs, which encapsulated superparamagnetic CoFe2O4 NPs for targeted co-delivery of cisplatin-pemetrexed and MR imaging. Their generated drug-loaded nanospheres exhibited enhanced cytotoxicity against FR-positive HeLa cells, but not HaCat and 3T3 cells [101]. Sahoo and colleagues have similarly prepared mesoporous silica-coated super paramagnetic manganese ferrite (MnFe2O4) NPs conjugated with FA for targeted drug delivery and MR imaging applications. The DOX-loaded NPs could selectively kill HeLa cancer cells both in vitro and in vivo [58]. Other investigators have designed mechanized nanocontainers via conjugating interlocked molecules, rotaxanes, onto the orifices of mesoporous silica NPs through disulfide bond. They showed that DOX-loaded mechanized nanocarriers could selectively kill tumor cells in vitro and in vivo [102]. MA and coworkers have recently developed FA-conjugated hollow mesoporous silica NPs for simultaneously delivering both DOX and small interfering RNA (siRNA) against the Bcl-2 protein into tumor cells. Their results showed that FA-conjugated NPs could potently kill high-expressing FR cells (HeLa) compared to low-expressing FR cells (MCF-7) [99]. Moreover, Teng et al. developed folate-targeted phospholipid-functionalized mesoporous silica NPs for selective photodynamic therapy of tumor cells in vitro and in vivo. They showed that their developed nano-photodynamic therapy systems could effectively enter into the FR-overexpressed HeLa cells. In addition, this therapeutic method could significantly decrease tumor growth in nude mice inoculated with B16F10 cells [103].
Gold nanoparticles
Gold NPs have been used for far years in techniques such as transmission electron microscopy (TEM) and atomic force microscopy (AFM) [104]. There are conflicting reports regarding the toxicity of gold NPs both in vitro and in vivo [105]. Gold NPs have successfully been used for several biomedical approaches such as photo-thermal therapy [106, 107], cancer diagnosis [108], tumor imaging [109, 110], and drug delivery [111, 108]. The plasmon resonance features of gold NPs enable their detection in biological systems [112]. Gold NPs can bind to amine and thiol groups, which make it possible to modify their surface and their usage in medical applications [113]. The high surface to volume ratio provides an optimum condition in which hundreds of molecules such as drugs, targeting agents, and anti-fouling polymers can be coated on the surface of gold NPs. As gold NPs can pass across leaky blood vessels, they may be considered as potent nanocarriers for drug delivery into solid tumors with high angiogenesis potential [114]. It is suggested that gold NPs enter into the cells through non-specific receptor-mediated endocytosis mechanism [115]. Since the systemic administration of gold NPs without targeting moieties can be associated with toxic side effects against normal tissues, its surface modification with targeting molecules such as FA can increase their efficiency and decrease their adverse effects [116, 117] (Table 3). Pandey and coworkers have developed FA-conjugated berberine hydrochloride-loaded gold NPs, which can selectively kill FR-expressing HeLa cells [118]. Another group used BSA-conjugated gold NPs, which was surface modified by FA. They showed that while the BSA-gold NPs had no effects on the MGC803 gastric cancer cells, FA-modified NPs could selectively target them [110]. Similarly, FA-conjugated 6-mercaptopurine (6MP)-loaded gold NPs could potently kill FR-expressing HeLa and KB cells both in vitro and in vivo [119]. It has also been shown that FA-targeted 5-FU-loaded pullulan stabilized gold NPs could significantly decrease the amount of 50 % of growth of inhibition (IC50) when incubated with HepG2 cancer cells. Moreover, these NPs had higher concentrations in liver of zebrafish embryo, as an in vivo model, compared to non-targeted gold NPs [120]. Zhu and colleagues recently developed multifunctional dendrimer-entrapped gold NPs, which were conjugated with PEGylated FA and linked with α-tocopheryl succinate (α-TOS) as a platform for targeted cancer imaging and therapy. The theranostic potential of their targeted NPs was approved both in vitro and in vivo using U87MG and L929 cancer cells [121].
The thermal characteristics of gold NPs, which let them to convert the absorbed laser light energy into localized heat, make them as worthy tools for application in combination with photo-thermal therapy for selective destruction of cancer cells [122–125]. Mehdizadeh and colleagues have used the combination of FA-conjugated gold nanorods with the photothermal therapy for the selective targeting and destruction of mouth epidermal carcinoma KB cells. While none of the treatments alone had effects on the cancer cells, their combination could significantly kill them [126]. FA-conjugated gold nanoclusters have also been used as fluorescence enzyme mimetic nanoprobes for tumor diagnosis and distinguishing tumor cells from normal cells [127]. Moreover, Xu et al. have designed an electrochemical cytosensor containing FA-conjugated gold NPs and signal indicator (ferrocene), which was able to effectively detect specific cancer cell and signal magnification for improving detection sensitivity [128].
Regarding the above-discussed studies, it seems that FA-conjugated NPs in combination with photo-thermal therapy may be effective for specific cancer therapy.
Dendrimers
Dendrimers are branched polymeric molecules with several arms extending from a center, leading to almost perfect three-dimensional geometric pattern. Two common strategies, including divergent and convergent methods, have usually been used for synthesis of dendrimers, which differ in direction of production, either core to out or inwardly out to core, respectively [129]. While the branches of dendrimers increase exponentially with their generation (G), their diameter increases up to about 1 nm with the generation.
Polyamidoamine (PAMAM) is an important subtype of dendrimers, which has a high efficiency to carry small therapeutic drugs. The cationic form of PAMAM is a worthy tool for delivery of therapeutic oligonucleotides. The tertiary amines and amide linkages of PAMAMs facilitate the attachment of numerous targeting and guest molecules. The hydrophobic core of PAMAMs enables them for the encapsulation of different therapeutic molecules [130]. Modification of terminal groups of dendrimers can create both a hydrophilic or lipophilic molecules for the desired biological and drug delivery application [131]. Since there are several reactive groups on dendrimers, their surface modification can be easily performed for specific targeting. It is reported that conjugation of dendrimers with biological targeting moieties such as FA can significantly increase their specific function on tumor cells in vitro (using KB cells) [132] (Table 4). The selective in vitro cytotoxicity of FA-conjugated methotrexate-loaded dendrimers against tumor cells confirms former report [133]. Kesharwani et al. have recently analyzed the anti-tumor potential of different generations of FA-targeted Melphalan-loaded poly(propyleneimine) (PPI) dendrimers both in vitro (MCF-7 cells) and in vivo. They have suggested that the fourth generation PPI dendrimer is a better carrier for targeted cancer therapy compared to the third and fifth generations [134]. Other investigators have investigated the effect of surface capping via different groups (including -OH, -COOH, and -NH2) on tumor-targeting efficiency of FA-conjugated PPI dendrimers. Their results showed that COOH-capped dendrimers have the highest tumor-targeting potential (as assessed in HeLa and SiHa cells) compared to other formulations [135]. The high anti-tumor gene delivery potential of FA-conjugated fifth generation (G5) PAMAM dendrimers into KB cancer cells has been demonstrated by other investigators [136]. Consistently, Arima and colleagues have reported that FA-PEG-appended polyamidoamine dendrimer (G3) conjugate with α-cyclodextrin exhibits high efficiency for gene delivery into FR-overexpressing (KB), but not FR-negative (A549), cells, both in vitro and in vivo [137]. The high gene transfection potential of dendrimers was also demonstrated using a pH-sensitive FA-PEG-chitosan-PAMAM-plasmid DNA (containing a high mobility group box 1, HMGB1) complexes both in vitro (in KB cells) and in vivo (S180 xenograft nude mice) [138]. The rapid elimination of such a small NPs is one of their important limitations. Thus, Sunoqrot and coworkers have developed a multi-scale hybrid NP platform that loads PAMAM dendrimers into PEG-PLA NPs. Their generated hybrid NPs had higher circulation time compared to dendrimer. Moreover, these hybrid NPs could selectively reach to FR-expressing KB tumor cells, in vivo [139].
It seems that dendrimers can be considered as potent therapeutic gene carriers in biomedical applications. Moreover, hybridization of dendrimers with some polymers could promote their efficiency for in vivo approaches.
Chitosan nanoparticles
Chitosan is a linear polysaccharide derived from alkaline N-deacetylation of chitin and composed of randomly distributed N-acetyl-glucosamine and glucosamine residues with β-1,4-linkage [140]. As chitosan is soluble in acid condition, it can be applied for drug delivery in an acidic environment [141, 8]. In addition to pH, degree of deacetylation, molecular weight, and ionic strength of the solution can potently affect the chitosan solubility [142]. Chitosan exhibited several features, including high biocompatibility and low cytotoxicity, which made it as a potent nanocarrier for targeted cancer therapy. However, due to the lack of cell-targeting ability and low transfection efficiency, it shows low therapeutic potential in common form. Thus, different derivatives of chitosan such as trimethyl chitosan (TMC), 6-amino-6-deoxy-chitosan (6ACT) (both are hydrophilic derivatives), N-alkylated chitosan (ACS), and hydrophobically modified glycol chitosan (HGC) (both are hydrophobic derivatives) have been developed in order to improve the therapeutic potential of chitosan [143]. Moreover, several targeting molecules such as FA have also been conjugated with chitosan NPs in order to facilitating their selective function (Table 4). It is reported that FA-conjugated DOX-loaded chitosan NPs could potently kill FR-expressing SMMC-7221 cells, in vitro [144]. FA-tagged copper ion and acetylacetone-encapsulated chitosan NPs were also exerted anti-tumor effects on the several FR-overexpressing cancer cells, in vitro [145]. The similar results were observed using FA-conjugated gemcitabine-loaded PEG-chitosan NPs in COLO357 pancreatic cancer cells both in vitro and in vivo [146]. Zheng and colleagues have shown that FA-conjugated DNA-loaded TMC NPs exhibit the higher cellular uptake in FR-expressing (KB and SKOV3) cells compared to non-targeted NPs. The cellular uptake of FA-conjugated NPs was significantly decreased in FR-negative (A549 and NIH/3T3) cells. Moreover, they suggested that FR-mediated uptake of NPs could be done through both FR-dependent and FR-independent endocytosis mechanisms [147]. The FA-targeted DOX-loaded chitosan-dextran NPs could also inhibit the growth of cancer (KB) cells both in vitro and in vivo [148]. Gaspar et al. reported that the use of FA-PEG-conjugated p53 DNA-loaded amino acid-modified chitosan NPs significantly increased gene transfer into FR-positive cancer cells, both in 3D spheroids and in vivo-mimicking 2D co-cultures, which led to the decreased tumor-spheroids volume [149]. Interestingly, it is suggested that methotrexate, as a FA analogue, can effectively target cancer cells through binding to FR [150]. Shi and coworkers have recently developed FA-conjugated DOX-loaded chitosan-deoxycholic acid–MPEG NPs, which exerted high toxicity against FR-positive HeLa but not FR-negative fibroblast 3T3 cells, in vitro [151]. It should be noted that deoxycholic acid contains the hydrophilic moieties and the hydrophobic nucleus, which allows forming micelles in water because of its amphiphilicity. Thus, deoxycholic acid can help in the self-association of chitosan and physical incorporation of hydrophobic drugs. In order to escape from the mononuclear phagocyte system, PEG molecules can be added to this complex. The systemic administration of FA-targeted HIF-1α siRNA encapsulated-PEG-chitosan oligosaccharide lactate (FA-PEG-COL) NPs into BALB/c mice bearing OVK18 #2 tumor xenograft was associated with remarkable tumor hindrance compared to non-targeted NPs that implies chitosan as a potent carrier for siRNA delivery, in vivo [152].
Conclusion
Site-specific drug delivery is an important issue in cancer therapy because it can decrease drug toxicity and enhance therapeutic effects [29, 153]. The effective nanocarriers, which can be applied in cancer therapy should exhibit some features, including high biocompatibility and less toxicity, efficient drug loading, long-time circulation in bloodstream, and selective targeting of tumor cells [154, 155, 29, 156–160]. There are three main pathways by which NPs can be uptaken by cells, including endocytosis, phagocytosis, and receptor-mediated endocytosis. In order to improve the internalization of NPs, their surface can be modified with some ligands that can selectively bind to their receptors on target cells.
Regarding the high expression of FR on cancer cells and the lack of FR on normal cells, it seems that folate can be a potent targeting molecule that can be applied in NP-based cancer therapy [161]. Folate exhibits several properties such as possibility of conjugation, non-immunogenicity, and essential factor for tumor growth, which make it a novel targeting molecule for various tumors [162]. FA-targeted NPs can be also conjugated with some other targeting molecules that may enhance their cellular penetration. For example, trans-activating transcriptional activator peptide (Tat) is a well-known cell-penetrating peptide (CPP), which can enhance the efficient uptake of nanocarriers by target cells. Therefore, the combination of FR-mediated specificity and CPP-mediated penetration may increase the efficiency of current FA-targeted nanocarriers for cancer therapy [163]. Dual targeting through FA and some anti-tumor antigen monoclonal antibodies is another approach in improving tumor site-specific cancer therapy.
As discussed earlier, several FA-targeted NPs have successfully been used for cancer therapy in vitro and in experimental tumor models. Unfortunately, little is known regarding the efficiency of these FA-targeted NPs in human tumors, and this issue should be investigated in future studies.
References
Kazemi T, Younesi V, Jadidi-Niaragh F, Yousefi M. Immunotherapeutic approaches for cancer therapy: an updated review. Artificial Cells, Nanomed Biotechnol. 2015(0):1-11.
Hosseini M, Haji-Fatahaliha M, Jadidi-Niaragh F, Majidi J, Yousefi M. The use of nanoparticles as a promising therapeutic approach in cancer immunotherapy. Artif cells, Nanomed Biotechnol. 2015(0):1-11.
Murthy SK. Nanoparticles in modern medicine: state of the art and future challenges. Int J Nanomedicine. 2007;2(2):129–41.
Talekar M, Kendall J, Denny W, Garg S. Targeting of nanoparticles in cancer: drug delivery and diagnostics. Anti-Cancer Drugs. 2011;22(10):949–62.
Conniot J, Silva JM, Fernandes JG, Silva LC, Gaspar R, Brocchini S et al. Cancer immunotherapy: nanodelivery approaches for immune cell targeting and tracking. Frontiers Chem. 2014;2(105).
Parker N, Turk MJ, Westrick E, Lewis JD, Low PS, Leamon CP. Folate receptor expression in carcinomas and normal tissues determined by a quantitative radioligand binding assay. Anal Biochem. 2005;338(2):284–93.
Mansoori GA, Brandenburg KS, Shakeri-Zadeh A. A comparative study of two folate-conjugated gold nanoparticles for cancer nanotechnology applications. Cancers. 2010;2(4):1911–28.
Ye W, Du J, Na R, Song Y, Mei Q, Zhao M. Cellular uptake and antitumor activity of DOX-hyd-PEG-FA nanoparticles. PLoS One. 2014;9(5):e97358.
Xu W, Ling P, Zhang T. Polymeric micelles, a promising drug delivery system to enhance bioavailability of poorly water-soluble drugs. J Drug Del. 2013;2013(340315).
Wang J, Yao K, Wang C, Tang C, Jiang X. Synthesis and drug delivery of novel amphiphilic block copolymers containing hydrophobic dehydroabietic moiety. J Mat Chem B. 2013;1(17):2324–32.
Khoee S, Kavand A. Preparation, co-assembling and interfacial crosslinking of photocurable and folate-conjugated amphiphilic block copolymers for controlled and targeted drug delivery: smart armored nanocarriers. Eur J Med Chem. 2014;73:18–29.
Miyata K, Christie RJ, Kataoka K. Polymeric micelles for nano-scale drug delivery. React Funct Polym. 2011;71(3):227–34.
Aliabadi HM, Lavasanifar A. Polymeric micelles for drug delivery. Expert Opin Drug Del. 2006;3(1):139–62.
Gao Z-G, Tian L, Hu J, Park I-S, Bae YH. Prevention of metastasis in a 4T1 murine breast cancer model by doxorubicin carried by folate conjugated pH sensitive polymeric micelles. J Control Release. 2011;152(1):84–9.
Rapoport N. Physical stimuli-responsive polymeric micelles for anti-cancer drug delivery. Prog Polym Sci. 2007;32(8):962–90.
Zhu J, Zhou Z, Yang C, Kong D, Wan Y, Wang Z. Folate-conjugated amphiphilic star-shaped block copolymers as targeted nanocarriers. J Biomed Mat Res Part A. 2011;97(4):498–508.
Hami Z, Amini M, Ghazi-Khansari M, Rezayat SM, Gilani K. Doxorubicin-conjugated PLA-PEG-Folate based polymeric micelle for tumor-targeted delivery: synthesis and in vitro evaluation. DARU J Pharmaceut Sci. 2014;22(1):22–30.
Scarano W, Duong HT, Lu H, De Souza PL, Stenzel MH. Folate conjugation to polymeric micelles via boronic acid ester to deliver platinum drugs to ovarian cancer cell lines. Biomacromolecules. 2013;14(4):962–75.
Guo X, Shi C, Wang J, Di S, Zhou S. pH-triggered intracellular release from actively targeting polymer micelles. Biomaterials. 2013;34(18):4544–54.
Wu W-C, Huang C-M, Liao P-W. Dual-sensitive and folate-conjugated mixed polymeric micelles for controlled and targeted drug delivery. React Funct Polym. 2014;81:82–90.
Bae Y, Jang W-D, Nishiyama N, Fukushima S, Kataoka K. Multifunctional polymeric micelles with folate-mediated cancer cell targeting and pH-triggered drug releasing properties for active intracellular drug delivery. Mol BioSyst. 2005;1(3):242–50.
Liu S-Q, Wiradharma N, Gao S-J, Tong YW, Yang Y-Y. Bio-functional micelles self-assembled from a folate-conjugated block copolymer for targeted intracellular delivery of anticancer drugs. Biomaterials. 2007;28(7):1423–33.
Song N, Ding M, Pan Z, Li J, Zhou L, Tan H, et al. Construction of targeting-clickable and tumor-cleavable polyurethane nanomicelles for multifunctional intracellular drug delivery. Biomacromolecules. 2013;14(12):4407–19.
Prabaharan M, Grailer JJ, Steeber DA, Gong S. Thermosensitive micelles based on folate conjugated poly (N-vinylcaprolactam) block-poly (ethylene glycol) for tumor targeted drug delivery. Macromol Biosci. 2009;9(8):744–53.
Syu WJ, Yu HP, Hsu CY, Rajan YC, Hsu YH, Chang YC, et al. Improved photodynamic cancer treatment by folate conjugated polymeric micelles in a KB xenografted animal model. Small. 2012;8(13):2060–9.
Fanciullino R, Ciccolini J, Milano G. Challenges, expectations and limits for nanoparticles-based therapeutics in cancer: a focus on nano-albumin-bound drugs. Criti Rev Oncol/Hematol. 2013;88(3):504–13.
Quinlan GJ, Martin GS, Evans TW. Albumin: biochemical properties and therapeutic potential. Hepatology. 2005;41(6):1211–9.
Lindner J, Loibl S, Denkert C, Ataseven B, Fasching P, Pfitzner B, et al. Expression of secreted protein acidic and rich in cysteine (SPARC) in breast cancer and response to neoadjuvant chemotherapy. Ann Oncol. 2014;26(1):95–100.
Zhang L, Hou S, Mao S, Wei D, Song X, Lu Y. Uptake of folate-conjugated albumin nanoparticles to the SKOV3 cells. Int J Pharm. 2004;287(1):155–62.
Zhao D, Zhao X, Zu Y, Li J, Zhang Y, Jiang R, et al. Preparation, characterization, and in vitro targeted delivery of folate-decorated paclitaxel-loaded bovine serum albumin nanoparticles. Int J Nanomedicine. 2010;20(5):669–77.
Hoffman RM, Bouvet M. Nanoparticle albumin-bound-paclitaxel: a limited improvement under the current therapeutic paradigm of pancreatic cancer. Expert Opin Pharmacother. 2015;16(7):943–7.
Miele E, Spinelli GP, Miele E, Tomao F, Tomao S. Albumin-bound formulation of paclitaxel (Abraxane® ABI-007) in the treatment of breast cancer. Int J Nanomedicine. 2009;4:99–105.
Ren K, Dusad A, Dong R, Quan L. Albumin as a delivery carrier for rheumatoid arthritis. J Nanomed Nanotechol. 2013;4(4):176.
Kratz F, Elsadek B. Clinical impact of serum proteins on drug delivery. J Control Release. 2012;161(2):429–45.
Hao H, Ma Q, Huang C, He F, Yao P. Preparation, characterization, and in vivo evaluation of doxorubicin loaded BSA nanoparticles with folic acid modified dextran surface. Int J Pharm. 2013;444(1):77–84.
Shen Z, Li Y, Kohama K, Oneill B, Bi J. Improved drug targeting of cancer cells by utilizing actively targetable folic acid-conjugated albumin nanospheres. Pharmacol Res. 2011;63(1):51–8.
Su C, Li H, Shi Y, Wang G, Liu L, Zhao L, et al. Carboxymethyl-β-cyclodextrin conjugated nanoparticles facilitate therapy for folate receptor-positive tumor with the mediation of folic acid. Int J Pharm. 2014;474(1):202–11.
Liang X, Sun Y, Liu L, Ma X, Hu X, Fan J, et al. Folate-functionalized nanoparticles for controlled ergosta-4, 6, 8 (14), 22-tetraen-3-one delivery. Int J Pharm. 2013;441(1):1–8.
Zu Y, Zhang Y, Zhao X, Zhang Q, Liu Y, Jiang R. Optimization of the preparation process of vinblastine sulfate (VBLS)-loaded folateconjugated bovine serum albumin (BSA) nanoparticles for tumor-targeted drug delivery using response surface methodology (RSM). Int J Nanomedicine. 2009;4:321.
Martínez A, Muñiz E, Teijón C, Iglesias I, Teijón J, Blanco M. Targeting tamoxifen to breast cancer xenograft tumours: preclinical efficacy of folate-attached nanoparticles based on alginate-cysteine/disulphide-bond-reduced albumin. Pharm Res. 2014;31(5):1264–74.
Yang R, An Y, Miao F, Li M, Liu P, Tang Q. Preparation of folic acid-conjugated, doxorubicin-loaded, magnetic bovine serum albumin nanospheres and their antitumor effects in vitro and in vivo. Int J Nanomedicine. 2014;9:4231–43.
Zhang L, Hou S, Zhang J, Hu W, Wang C. Preparation, characterization, and in vivo evaluation of mitoxantrone-loaded, folate-conjugated albumin nanoparticles. Arch Pharm Res. 2010;33(8):1193–8.
Akbarzadeh A, Samiei M, Davaran S. Magnetic nanoparticles: preparation, physical properties, and applications in biomedicine. Nanoscale Res Lett. 2012;7(1):1–13.
Jing Y, Dong-Yan H, Yousaf MZ, Yang-Long H, Song G. Magnetic nanoparticle-based cancer therapy. Chin Physics B. 2013;22(2):027506.
Wang J, Chen Y, Chen B, Ding J, Xia G, Gao C, et al. Pharmacokinetic parameters and tissue distribution of magnetic Fe3O4 nanoparticles in mice. Int J Nanomedicine. 2010;5:861–6.
Tang Q, An Y, Liu D, Liu P, Zhang D. Folate/NIR 797-conjugated albumin magnetic nanospheres: synthesis, characterisation, and in vitro and in vivo targeting evaluation. PLoS One. 2014;9(9):e106483.
Lu AH, Salabas EL, Schüth F. Magnetic nanoparticles: synthesis, protection, functionalization, and application. Angew Chem Int Ed. 2007;46(8):1222–44.
Ito A, Shinkai M, Honda H, Kobayashi T. Medical application of functionalized magnetic nanoparticles. J Biosci Bioeng. 2005;100(1):1–11.
Majd MH, Barar J, Asgari D, Valizadeh H, Rashidi MR, Kafil V, et al. Targeted fluoromagnetic nanoparticles for imaging of breast cancer MCF-7 cells. Adv Pharmaceut Bull. 2013;3(1):189–95.
Ma X, Gong A, Chen B, Zheng J, Chen T, Shen Z, et al. Exploring a new SPION-based MRI contrast agent with excellent water-dispersibility, high specificity to cancer cells and strong MR imaging efficacy. Colloids Surf B: Biointerfaces. 2014;126:44–9.
Li J, Zheng L, Cai H, Sun W, Shen M, Zhang G, et al. Polyethyleneimine-mediated synthesis of folic acid-targeted iron oxide nanoparticles for in vivo tumor MR imaging. Biomaterials. 2013;34(33):8382–92.
Shi J, Wang L, Gao J, Liu Y, Zhang J, Ma R, et al. A fullerene-based multi-functional nanoplatform for cancer theranostic applications. Biomaterials. 2014;35(22):5771–84.
Wen J, Jiang S, Chen Z, Zhao W, Yi Y, Yang R, et al. Apoptosis selectively induced in BEL-7402 cells by folic acid-modified magnetic nanoparticles combined with 100 Hz magnetic field. Int J Nanomedicine. 2014;9:2043.
Majetich SA. Magnetic nanoparticles for biomedicine. Conf Proc IEEE Eng Med Biol Soc. 2009;2009:4477–8.
Varshosaz J, Hassanzadeh F, Sadeghi Aliabadi H, Nayebsadrian M, Banitalebi M, Rostami M. Synthesis and characterization of folate-targeted dextran/retinoic acid micelles for doxorubicin delivery in acute leukemia. BioMed Res Int. 2014;2014.
Krais A, Wortmann L, Hermanns L, Feliu N, Vahter M, Stucky S, et al. Targeted uptake of folic acid-functionalized iron oxide nanoparticles by ovarian cancer cells in the presence but not in the absence of serum. Nanomed: Nanotechnol, Biol Med. 2014;10(7):1421–31.
Laurent S, Forge D, Port M, Roch A, Robic C, Vander Elst L, et al. Magnetic iron oxide nanoparticles: synthesis, stabilization, vectorization, physicochemical characterizations, and biological applications. Chem Rev. 2008;108(6):2064–110.
Sahoo B, Devi KSP, Dutta S, Maiti TK, Pramanik P, Dhara D. Biocompatible mesoporous silica-coated superparamagnetic manganese ferrite nanoparticles for targeted drug delivery and MR imaging applications. J Colloid Interface Sci. 2014;431:31–41.
Wu W, He Q, Jiang C. Magnetic iron oxide nanoparticles: synthesis and surface functionalization strategies. Nanoscale Res Lett. 2008;3(11):397–415.
Guan Y-Q, Zheng Z, Huang Z, Li Z, Niu S, Liu J-M. Powerful inner/outer controlled multi-target magnetic nanoparticle drug carrier prepared by liquid photo-immobilization. Scientific reports. 2014;4(4990).
Badruddoza AZM, Rahman MT, Ghosh S, Hossain MZ, Shi J, Hidajat K, et al. β-Cyclodextrin conjugated magnetic, fluorescent silica core–shell nanoparticles for biomedical applications. Carbohydr Polym. 2013;95(1):449–57.
Erdal N, Gürgül S, Tamer L, Ayaz L. Effects of long-term exposure of extremely low frequency magnetic field on oxidative/nitrosative stress in rat liver. J Radiat Res. 2008;49(2):181–7.
Qu J, Liu G, Wang Y, Hong R. Preparation of Fe3O4–chitosan nanoparticles used for hyperthermia. Adv Powder Technol. 2010;21(4):461–7.
Viota J, Carazo A, Munoz-Gamez J, Rudzka K, Gómez-Sotomayor R, Ruiz-Extremera A, et al. Functionalized magnetic nanoparticles as vehicles for the delivery of the antitumor drug gemcitabine to tumor cells. Physicochemical in vitro evaluation. Mater Sci Eng C. 2013;33(3):1183–92.
Lee GY, Qian WP, Wang L, Wang YA, Staley CA, Satpathy M, et al. Theranostic nanoparticles with controlled release of gemcitabine for targeted therapy and MRI of pancreatic cancer. ACS Nano. 2013;7(3):2078–89.
Zhang F, Huang X, Zhu L, Guo N, Niu G, Swierczewska M, et al. Noninvasive monitoring of orthotopic glioblastoma therapy response using RGD-conjugated iron oxide nanoparticles. Biomaterials. 2012;33(21):5414–22.
Hu H, Zhang C, An L, Yu Y, Yang H, Sun J, et al. General protocol for the synthesis of functionalized magnetic nanoparticles for magnetic resonance imaging from protected metal–organic precursors. Chem-A Europ J. 2014;20(23):7160–7.
Sivakumar B, Aswathy RG, Sreejith R, Nagaoka Y, Iwai S, Suzuki M, et al. Bacterial exopolysaccharide based magnetic nanoparticles: a versatile nanotool for cancer cell imaging, targeted drug delivery and synergistic effect of drug and hyperthermia mediated cancer therapy. J Biomed Nanotechnol. 2014;10(6):885–99.
Fazilati M. Folate decorated magnetite nanoparticles: synthesis and targeted therapy against ovarian cancer. Cell Biol Int. 2014;38(2):154–63.
Mehrabi M, Javid A, Hashemi A, Rezaei-Zarchi S. Investigation of the effect of folic acid based iron oxide nanoparticles on human leukemic CCRF-CEM cell line. Iran J Pediatr Hematol Oncol. 2013;3(2):47–53.
Gunduz U, Keskin T, Tansık G, Mutlu P, Yalcın S, Unsoy G, et al. Idarubicin-loaded folic acid conjugated magnetic nanoparticles as a targetable drug delivery system for breast cancer. Biomed Pharmacotherapy. 2014;68(6):729–36.
An Q, Sun C, Li D, Xu K, Guo J, Wang C. Peroxidase-like activity of Fe3O4@ carbon nanoparticles enhances ascorbic acid-induced oxidative stress and selective damage to PC-3 prostate cancer cells. ACS Appl Mater Interfaces. 2013;5(24):13248–57.
Li X, Ding J, Wang X, Wei K, Weng J, Wang J. One-pot synthesis and functionalisation of Fe 2 O 3@ CNH 2 nanoparticles for imaging and therapy. Nanobiotechnol, IET. 2014;8(2):93–101.
Tang Z, Li D, Sun H, Guo X, Chen Y, Zhou S. Quantitative control of active targeting of nanocarriers to tumor cells through optimization of folate ligand density. Biomaterials. 2014;35(27):8015–27.
Mikhaylova M, Kim DK, Bobrysheva N, Osmolowsky M, Semenov V, Tsakalakos T, et al. Superparamagnetism of magnetite nanoparticles: dependence on surface modification. Langmuir. 2004;20(6):2472–7.
Kim J, Park S, Lee JE, Jin SM, Lee JH, Lee IS, et al. Designed fabrication of multifunctional magnetic gold nanoshells and their application to magnetic resonance imaging and photothermal therapy. Angew Chem. 2006;118(46):7918–22.
Wu W, Chen B, Cheng J, Wang J, Xu W, Liu L, et al. Biocompatibility of Fe3O4/DNR magnetic nanoparticles in the treatment of hematologic malignancies. Int J Nanomedicine. 2010;5:1079.
Hervault A, Thanh NTK. Magnetic nanoparticle-based therapeutic agents for thermo-chemotherapy treatment of cancer. Nanoscale. 2014;6(20):11553–73.
Sivakumar Balasubramanian ARG, Nagaoka Y, Iwai S, Suzuki M, Kizhikkilot V, Yoshida Y, et al. Curcumin and 5-Fluorouracil-loaded, folate-and transferrin-decorated polymeric magnetic nanoformulation: a synergistic cancer therapeutic approach, accelerated by magnetic hyperthermia. Int J Nanomedicine. 2014;9:437–59.
Chen B, Cheng J, Wu Y, Gao F, Xu W, Shen H, et al. Reversal of multidrug resistance by magnetic Fe3O4 nanoparticle copolymerizating daunorubicin and 5-bromotetrandrine in xenograft nude-mice. Int J Nanomedicine. 2009;4:73–8.
Chen B, Cheng J, Shen M, Gao F, Xu W, Shen H, et al. Magnetic nanoparticle of Fe3O4 and 5-bromotetrandrin interact synergistically to induce apoptosis by daunorubicin in leukemia cells. Int J Nanomedicine. 2009;4:65–71.
Goya G, Grazu V, Ibarra M. Magnetic nanoparticles for cancer therapy. Curr Nanosci. 2008;4(1):1–16.
Safarik I, Safarikova M. Magnetically responsive nanocomposite materials for bioapplications. Solid State Phenom. 2009;151:88–94.
Jeong U, Teng X, Wang Y, Yang H, Xia Y. Superparamagnetic colloids: controlled synthesis and niche applications. Adv Mater. 2007;19(1):33–60.
Tang Q, Chen D. Study of the therapeutic effect of 188Re labeled folate targeting albumin nanoparticle coupled with cis-diamminedichloroplatinum cisplatin on human ovarian cancer. Bio-Med Mat Eng. 2014;24(1):711–22.
Yoo H, Moon S-K, Hwang T, Kim YS, Kim J-H, Choi S-W, et al. Multifunctional magnetic nanoparticles modified with polyethylenimine and folic acid for biomedical theranostics. Langmuir. 2013;29(20):5962–7.
Varshosaz J, Sadeghi-Aliabadi H, Ghasemi S, Behdadfar B. Use of magnetic folate-dextran-retinoic acid micelles for dual targeting of doxorubicin in breast cancer. BioMed Res Int. 2013;2013:680712.
Yang H-W, Hua M-Y, Liu H-L, Huang C-Y, Wei K-C. Potential of magnetic nanoparticles for targeted drug delivery. Nanotechnol Sci Appl. 2012;5:73–86.
Franckena M, Wit RD, Ansink AC, Notenboom A, Canters RA, Fatehi D, et al. Weekly systemic cisplatin plus locoregional hyperthermia: an effective treatment for patients with recurrent cervical carcinoma in a previously irradiated area. Int J Hyperth. 2007;23(5):443–50.
Chen ZQ, Wen J, Tu WY, Xiao L, Fang Z. A study on early apoptosis of hepatoma Bel-7402 cells in vitro treated by altering-electric magnetic field exposure of extremely low frequency combined with magnetic nano-Fe3O4 powders. Appl Mech Mat. 2013;364:742–8.
Klichko Y, Liong M, Choi E, Angelos S, Nel AE, Stoddart JF, et al. Mesostructured silica for optical functionality, nanomachines, and drug delivery. J Am Ceram Soc. 2009;92(s1):S2–S10.
Slowing II, Vivero-Escoto JL, Wu C-W, Lin VS-Y. Mesoporous silica nanoparticles as controlled release drug delivery and gene transfection carriers. Adv Drug Deliv Rev. 2008;60(11):1278–88.
Liong M, Lu J, Kovochich M, Xia T, Ruehm SG, Nel AE, et al. Multifunctional inorganic nanoparticles for imaging, targeting, and drug delivery. ACS Nano. 2008;2(5):889–96.
Trewyn BG, Slowing II, Giri S, Chen H-T, Lin VS-Y. Synthesis and functionalization of a mesoporous silica nanoparticle based on the sol–gel process and applications in controlled release. Acc Chem Res. 2007;40(9):846–53.
Safari J, Zarnegar Z. Advanced drug delivery systems: nanotechnology of health design a review. J Saudi Chem Soc. 2014;18(2):85–99.
Kwon S, Singh RK, Perez RA, Neel EAA, Kim H-W, Chrzanowski W. Silica-based mesoporous nanoparticles for controlled drug delivery. J Tiss Eng. 2013;4:2041731413503357.
Wang S. Ordered mesoporous materials for drug delivery. Microporous Mesoporous Mater. 2009;117(1):1–9.
Halamová D, Zeleňák V. NSAID naproxen in mesoporous matrix MCM-41: drug uptake and release properties. J Incl Phenom Macrocycl Chem. 2012;72(1-2):15–23.
Ma X, Zhao Y, Ng KW, Zhao Y. Integrated hollow mesoporous silica nanoparticles for target drug/siRNA co-delivery. Chem-A Europ J. 2013;19(46):15593–603.
Fan J, Fang G, Wang X, Zeng F, Xiang Y, Wu S. Targeted anticancer prodrug with mesoporous silica nanoparticles as vehicles. Nanotechnology. 2011;22(45):455102.
Mohapatra S, Rout SR, Narayan R, Maiti TK. Multifunctional mesoporous hollow silica nanocapsules for targeted co-delivery of cisplatin-pemetrexed and MR imaging. Dalton Trans. 2014;43(42):15841–50.
Luo Z, Ding X, Hu Y, Wu S, Xiang Y, Zeng Y, et al. Engineering a hollow nanocontainer platform with multifunctional molecular machines for tumor-targeted therapy in vitro and in vivo. ACS Nano. 2013;7(11):10271–84.
Teng I, Chang Y-J, Wang L-S, Lu H-Y, Wu L-C, Yang C-M, et al. Phospholipid-functionalized mesoporous silica nanocarriers for selective photodynamic therapy of cancer. Biomaterials. 2013;34(30):7462–70.
Jain S, Hirst D, O’sullivan J. Gold nanoparticles as novel agents for cancer therapy. Br J Radiol. 2014;85(1010):101–13.
Nel A, Xia T, Mädler L, Li N. Toxic potential of materials at the nanolevel. Science. 2006;311(5761):622–7.
Lal S, Clare SE, Halas NJ. Nanoshell-enabled photothermal cancer therapy: impending clinical impact. Acc Chem Res. 2008;41(12):1842–51.
Niidome T, Yamagata M, Okamoto Y, Akiyama Y, Takahashi H, Kawano T, et al. PEG-modified gold nanorods with a stealth character for in vivo applications. J Control Release. 2006;114(3):343–7.
Llevot A, Astruc D. Applications of vectorized gold nanoparticles to the diagnosis and therapy of cancer. Chem Soc Rev. 2012;41(1):242–57.
Kim D, Jeong YY, Jon S. A drug-loaded aptamer-gold nanoparticle bioconjugate for combined CT imaging and therapy of prostate cancer. ACS Nano. 2010;4(7):3689–96.
Lin J, Zhou Z, Li Z, Zhang C, Wang X, Wang K, et al. Biomimetic one-pot synthesis of gold nanoclusters/nanoparticles for targeted tumor cellular dual-modality imaging. Nanoscale Res Lett. 2013;8(1):1–7.
Brown SD, Nativo P, Smith J-A, Stirling D, Edwards PR, Venugopal B, et al. Gold nanoparticles for the improved anticancer drug delivery of the active component of oxaliplatin. J Am Chem Soc. 2010;132(13):4678–84.
Jain PK, Huang W, El-Sayed MA. On the universal scaling behavior of the distance decay of plasmon coupling in metal nanoparticle pairs: a plasmon ruler equation. Nano Lett. 2007;7(7):2080–8.
Park JH, von Maltzahn G, Ruoslahti E, Bhatia SN, Sailor MJ. Micellar hybrid nanoparticles for simultaneous magnetofluorescent imaging and drug delivery. Angew Chem. 2008;120(38):7394–8.
Sezgin E, Karatas ÖF, Çam D, Sur İ, Sayin İ, Avci E, et al. Interaction of gold nanoparticles with living cells. Sigma. 2008;26:227–46.
Chithrani BD, Ghazani AA, Chan WC. Determining the size and shape dependence of gold nanoparticle uptake into mammalian cells. Nano Lett. 2006;6(4):662–8.
De Jong WH, Hagens WI, Krystek P, Burger MC, Sips AJ, Geertsma RE. Particle size-dependent organ distribution of gold nanoparticles after intravenous administration. Biomaterials. 2008;29(12):1912–9.
Semmler‐Behnke M, Kreyling WG, Lipka J, Fertsch S, Wenk A, Takenaka S, et al. Biodistribution of 1.4 and 18 nm gold particles in rats. Small. 2008;4(12):2108–11.
Pandey S, Mewada A, Thakur M, Shah R, Oza G, Sharon M. Biogenic gold nanoparticles as fotillas to fire berberine hydrochloride using folic acid as molecular road map. Mater Sci Eng C. 2013;33(7):3716–22.
Park J, Jeon WI, Lee SY, Ock KS, Seo JH, Park J, et al. Confocal Raman microspectroscopic study of folate receptor targeted delivery of 6 mercaptopurine embedded gold nanoparticles in a single cell. J Biomed Mat Res Part A. 2012;100(5):1221–8.
Ganeshkumar M, Ponrasu T, Raja MD, Subamekala MK, Suguna L. Green synthesis of pullulan stabilized gold nanoparticles for cancer targeted drug delivery. Spectrochim Acta A Mol Biomol Spectrosc. 2014;130:64–71.
Zhu J, Zheng L, Wen S, Tang Y, Shen M, Zhang G, et al. Targeted cancer theranostics using alpha-tocopheryl succinate-conjugated multifunctional dendrimer-entrapped gold nanoparticles. Biomaterials. 2014;35(26):7635–46.
Kattumuri V, Katti K, Bhaskaran S, Boote EJ, Casteel SW, Fent GM, et al. Gum arabic as a phytochemical construct for the stabilization of gold nanoparticles: in vivo pharmacokinetics and x-ray contrast imaging studies. Small. 2007;3(2):333–41.
Fent GM, Casteel SW, Kim DY, Kannan R, Katti K, Chanda N, et al. Biodistribution of maltose and gum arabic hybrid gold nanoparticles after intravenous injection in juvenile swine. Nanomed: Nanotechnol, Biol Med. 2009;5(2):128–35.
Triulzi RC, Dai Q, Zou J, Leblanc RM, Gu Q, Orbulescu J, et al. Photothermal ablation of amyloid aggregates by gold nanoparticles. Colloids Surf B: Biointerfaces. 2008;63(2):200–8.
Jain PK, El-Sayed IH, El-Sayed MA. Au nanoparticles target cancer. Nano Today. 2007;2(1):18–29.
Mehdizadeh A, Pandesh S, Shakeri-Zadeh A, Kamrava SK, Habib-Agahi M, Farhadi M, et al. The effects of folate-conjugated gold nanorods in combination with plasmonic photothermal therapy on mouth epidermal carcinoma cells. Lasers Med Sci. 2014;29(3):939–48.
Hu D, Sheng Z, Fang S, Wang Y, Gao D, Zhang P, et al. Folate receptor-targeting gold nanoclusters as fluorescence enzyme mimetic nanoprobes for tumor molecular colocalization diagnosis. Theranostics. 2014;4(2):142.
Xu S, Liu J, Wang T, Li H, Miao Y, Liu Y, et al. A simple and rapid electrochemical strategy for non-invasive, sensitive and specific detection of cancerous cell. Talanta. 2013;104:122–7.
Bharali DJ, Khalil M, Gurbuz M, Simone TM, Mousa SA. Nanoparticles and cancer therapy: a concise review with emphasis on dendrimers. Int J Nanomedicine. 2009;4:1–7.
Eichman JD, Bielinska AU, Kukowska-Latallo JF, Baker Jr JR. The use of PAMAM dendrimers in the efficient transfer of genetic material into cells. Pharmaceut Sci Technol. 2000;3(7):232–45.
Gillies ER, Frechet JM. Dendrimers and dendritic polymers in drug delivery. Drug Discov Today. 2005;10(1):35–43.
Hong S, Leroueil PR, Majoros IJ, Orr BG, Baker Jr JR, Banaszak Holl MM. The binding avidity of a nanoparticle-based multivalent targeted drug delivery platform. Chem Biol. 2007;14(1):107–15.
Myc A, Douce TB, Ahuja N, Kotlyar A, Kukowska-Latallo J, Thomas TP, et al. Preclinical antitumor efficacy evaluation of dendrimer-based methotrexate conjugates. Anti-Cancer Drugs. 2008;19(2):143–9.
Kesharwani P, Tekade RK, Jain NK. Generation dependent safety and efficacy of folic acid conjugated dendrimer based anticancer drug formulations. Pharm Res. 2014;32(4):1438–50.
Birdhariya B, Kesharwani P, Jain NK. Effect of surface capping on targeting potential of folate decorated poly (propylene imine) dendrimers. Drug Dev Indust Pharma. 2014(0):1-7.
Wong PT, Tang K, Coulter A, Tang S, Baker Jr JR, Choi SK. Multivalent dendrimer vectors with DNA intercalation motifs for gene delivery. Biomacromolecules. 2014;15(11):4134–45.
Arima H, Arizono M, Higashi T, Yoshimatsu A, Ikeda H, Motoyama K, et al. Potential use of folate-polyethylene glycol (PEG)-appended dendrimer (G3) conjugate with α-cyclodextrin as DNA carriers to tumor cells. Cancer Gene Ther. 2012;19(5):358–66.
Wang M, Hu H, Sun Y, Qiu L, Zhang J, Guan G, et al. A pH-sensitive gene delivery system based on folic acid-PEG-chitosan–PAMAM-plasmid DNA complexes for cancer cell targeting. Biomaterials. 2013;34(38):10120–32.
Sunoqrot S, Bugno J, Lantvit D, Burdette JE, Hong S. Prolonged blood circulation and enhanced tumor accumulation of folate-targeted dendrimer-polymer hybrid nanoparticles. J Control Release. 2014;191:115–22.
Liu W, Sun S, Cao Z, Zhang X, Yao K, Lu WW, et al. An investigation on the physicochemical properties of chitosan/DNA polyelectrolyte complexes. Biomaterials. 2005;26(15):2705–11.
Sadigh-Eteghad S, Talebi M, Farhoudi M, Mahmoudi J, Reyhani B. Effects of Levodopa loaded chitosan nanoparticles on cell viability and caspase-3 expression in PC12 neural like cells. Neurosciences. 2013;18(3):281–3.
Bowman K, Leong KW. Chitosan nanoparticles for oral drug and gene delivery. Int J Nanomedicine. 2006;1(2):117–28.
Xu Q, Wang C-H, Pack DW. Polymeric carriers for gene delivery: chitosan and poly (amidoamine) dendrimers. Curr Pharm Des. 2010;16(21):2350.
Song H, Su C, Cui W, Zhu B, Liu L, Chen Z, et al. Folic acid-chitosan conjugated nanoparticles for improving tumor-targeted drug delivery. BioMed Res Int. 2013;2013.
Pramanik A, Laha D, Pramanik P, Karmakar P. A novel drug “copper acetylacetonate” loaded in folic acid-tagged chitosan nanoparticle for efficient cancer cell targeting. J Drug Target. 2013;22(1):23–33.
Zhou J, Wang J, Xu Q, Xu S, Wen J, Yu Z, et al. Folate-chitosan-gemcitabine core-shell nanoparticles targeted to pancreatic cancer. Chin J Cancer Res. 2013;25(5):527.
Zheng Y, Cai Z, Song X, Yu B, Bi Y, Chen Q, et al. Receptor mediated gene delivery by folate conjugated N-trimethyl chitosan in vitro. Int J Pharm. 2009;382(1):262–9.
Lee KD, Choi S-H, Kim DH, Lee H-Y, Choi K-C. Self-organized nanoparticles based on chitosan-folic acid and dextran succinate-doxorubicin conjugates for drug targeting. Arch Pharmacal Res. 2014:1-8.
Gaspar VM, Costa EC, Queiroz JA, Pichon C, Sousa F, Correia IJ. Folate-targeted multifunctional amino acid-chitosan nanoparticles for improved cancer therapy. Pharm Res. 2014;1–16.
Jia M, Li Y, Yang X, Huang Y, Wu H, Huang Y, et al. Development of both methotrexate and mitomycin C loaded pegylated chitosan nanoparticles for targeted drug codelivery and synergistic anticancer effect. ACS Appl Mater Interfaces. 2014;6(14):11413–23.
Shi Z, Guo R, Li W, Zhang Y, Xue W, Tang Y, et al. Nanoparticles of deoxycholic acid, polyethylene glycol and folic acid-modified chitosan for targeted delivery of doxorubicin. J Mater Sci Mater Med. 2014;25(3):723–31.
Li TSC, Yawata T, Honke K. Efficient siRNA delivery and tumor accumulation mediated by ionically cross-linked folic acid–poly (ethylene glycol)–chitosan oligosaccharide lactate nanoparticles: for the potential targeted ovarian cancer gene therapy. Eur J Pharm Sci. 2014;52:48–61.
Allen TM, Brandeis E, Hansen CB, Kao GY, Zalipsky S. A new strategy for attachment of antibodies to sterically stabilized liposomes resulting in efficient targeting to cancer cells. Biochimica et Biophysica Acta (BBA)-Biomembranes. 1995;123(2):99–108.
Liu Y, Li K, Pan J, Liu B, Feng S-S. Folic acid conjugated nanoparticles of mixed lipid monolayer shell and biodegradable polymer core for targeted delivery of Docetaxel. Biomaterials. 2010;31(2):330–8.
Cho K, Wang X, Nie S, Shin DM. Therapeutic nanoparticles for drug delivery in cancer. Clin Cancer Res. 2008;14(5):1310–6.
Torchilin VP. Recent advances with liposomes as pharmaceutical carriers. Nat Rev Drug Discov. 2005;4(2):145–60.
Tong R, Cheng J. Anticancer polymeric nanomedicines. J Macromol Sci Polym Rev. 2007;47(3):345–81.
S-s F, Huang G. Effects of emulsifiers on the controlled release of paclitaxel (Taxol®) from nanospheres of biodegradable polymers. J Control Release. 2001;71(1):53–69.
Wang X, Yang L, Chen ZG, Shin DM. Application of nanotechnology in cancer therapy and imaging. CA: Cancer J Clin. 2008;58(2):97–110.
Campbell IG, Jones TA, Foulkes WD, Trowsdale J. Folate-binding protein is a marker for ovarian cancer. Cancer Res. 1991;51(19):5329–38.
Zhang Z, Jia J, Lai Y, Ma Y, Weng J, Sun L. Conjugating folic acid to gold nanoparticles through glutathione for targeting and detecting cancer cells. Bioorg Med Chem. 2010;18(15):5528–34.
Ai J, Xu Y, Li D, Liu Z, Wang E. Folic acid as delivery vehicles: targeting folate conjugated fluorescent nanoparticles to tumors imaging. Talanta. 2012;101:32–7.
Zhu Y, Cheng L, Cheng L, Huang F, Hu Q, Li L, et al. Folate and TAT peptide co-modified liposomes exhibit receptor-dependent highly efficient intracellular transport of payload in vitro and in vivo. Pharm Res. 2014;31(12):3289–303.
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bahrami, B., Mohammadnia-Afrouzi, M., Bakhshaei, P. et al. Folate-conjugated nanoparticles as a potent therapeutic approach in targeted cancer therapy. Tumor Biol. 36, 5727–5742 (2015). https://doi.org/10.1007/s13277-015-3706-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-015-3706-6