Abstract
P21-activated protein kinase1 (PAK1), a main downstream effector of small Rho GTPases, Rac1, and Cdc42, plays an important role in the regulation of cell morphogenesis, motility, mitosis, and angiogenesis. Despite its importance, the molecular mechanisms of PAK1 that contributed to colorectal carcinogenesis remain unclear. Our immunohistochemistry showed that PAK1 expression was increased with colorectal cancer (CRC) progression through the adenoma to carcinoma sequence. Furthermore, our results suggested a relationship between PAK1 nuclear localization and the Dukes staging. In the present study, we showed that PAK1 knockdown decreased proliferation and delayed the G1/S cell-cycle transition, and increased apoptosis in vivo and in vitro. In addition, PAK1 knock-down downregulated c-Jun amino terminal kinases (JNK) activity and the levels of cyclinD1, CDK4/6. Inhibition of the JNK activity by chemical inhibitor (SP600125) significantly reduced the effects of PAK1 on CRC proliferation via accumulation of phosphatase and tensin homolog deleted on chromosome 10 (PTEN). In conclusion, our results demonstrate that knockdown of PAK1 could enhance the chemosensitivity of CRCs to 5-fluorouracil through G1 arrest. The mechanism by which PAK1 induced cancer growth might involve activation of JNK as well as downregulation of PTEN. Targeting PAK1 may represent a novel treatment strategy for developing novel chemotherapeutic agents.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Colorectal cancer (CRC) is one of the major causes of premature death worldwide, and the overall incidence is increasing in China. Despite our growing understanding of oncogenesis and successful identification of proto-oncogenes and tumor suppressor genes involved in the tumorigenesis of CRC, the biologic and molecular mechanisms in CRC are poorly understood. Currently, chemotherapy using 5-fluorouracil (5-FU) and associated adjuvant agents remains to be the standard chemotherapeutic agent used in the treatment of colorectal cancer [1, 2]. However, response rates for 5-FU-based chemotherapy as a first-line treatment for advanced colorectal cancer are only 10–15% (Johnston and Kaye 2001). To find more effective treatment strategies, some studies have tried to investigate the effects molecular targeted agents.
P21-activated kinases (PAKs), a serine/threonine kinases, is a small GTPase effector that plays critical roles in many fundamental cellular processes, including proliferation, survival, and differentiation. Six PAKs have been identified in mammals, which are classified into two groups: PAK1–PAK3 in group I and PAK4–PAK6 in group II. Recently, there is mounting evidence suggesting the involvement of PAK1 in tumorigenesis. Several studies also report that PAK1 either upregulated or hyperactivated in multiple human cancers, such as breast, stomach, and ovarian [3, 4]. Sullivan reports that PAK1 plays a role in renal tumor growth in vivo and in vitro [5]. In mitotic cells, PAK1 is localized on centrosomes, spindles, or contractile ring, suggesting that PAK1 may contribute to cell proliferation via affecting cell-cycle progression [6–8]. Phosphorylated PAK1 inhibition by an auto-inhibitory peptide (amino acids 83–149) or PAK1 knockdown by short interference RNA markedly reduced the expression of cyclinD1 in breast cancer cells, suggesting that PAK1 function is beneficial to cell proliferation [9]. In a mouse model, PAK1 hyperactivation is sufficient for the formation of mammary gland tumors [10]. The presence of phosphorylated Pak1 in the cytoplasm of glioblastoma cells is associated with shorter survival, and knockdown of Pak1 suppressed the invasiveness of glioblastoma [11]. PAK1 is believed to be involved in several survival signaling pathways, such as mitogen-activated protein kinases (MAPK), which are believed to be important in carcinogenesis [12].
Despite its importance, the molecular mechanisms of PAK1 contributes to colorectal carcinogenesis are largely undefined. In the present study, we aimed to elucidate the functional connection of PAK1 to colorectal cancer. In our previous study, we found that PAK5 expression increased significantly with malignant progression of CRC and that PAK5 might promote CRC metastasis by regulating CRC cell adhesion and migration [13]. In this study, our data indicated that PAK1 expression was also significantly up-regulated in human CRCs, and this up-regulation was associated with more aggressive tumor behavior. Our studies showed that PAK1 played a critical role in colorectal cancer growth in vivo and in vitro. We provided the first evidence that PAK1 knockdown decreased the rate of colorectal tumor growth and the volume of tumors. PAK1 downregulation caused a delay in the G1 transition of the cell cycle. Increased levels of PAK1 might augment chemoresistance to 5-FU in colon cancer cells though regulating G1 phase transition. Our result showed that JNK activity and PTEN repression were required for the proliferation and cell cycle effects of PAK1 as well as the expression of PTEN were regulated by JNK pathway.
Materials and methods
Reagents
Anti-JNK, anti-phospho-JNK antibodies, U0126 (Cell Signaling Technology), rabbit anti-PAK1 and anti-GAPDH, anti-CDK4, anti-CDK6 antibodies (Santa Cruz, USA), rabbit anti-PTEN antibodies (Millipore Corporation), and SB203580 and SP600125,5-fluorouracil (Sigma Aldrich) were obtained from the indicated sources.
Constructs
Double-strand oligonucleotides corresponding to the target sequences were cloned into pGPU6/GFP/Neo plasmid (Shanghai GenePharma Co., China). In this study, the target sequences for human PAK1 cDNA are AAGATTGGACAAGGTGCTTCA and for human PTEN cDNA 5′-AAGGTGAAGATATATTCCTCC-3′ [14]. Mammalian expression plasmids for PAK1 and control empty plasmids were generous gifts from Prof. Hongquan Zhang (Peking University Health Science Center, Beijing).
Tissue culture and stable clone selection
The SW480, LoVo cells from the American Type Culture Collection (Manassas, VA, USA) were cultured in the RPMI 1640 media supplemented with 10% fetal bovine serum and 100 U each of penicillin and streptomycin. Cells were transfected with 4 μg DNA constructs using LipofectAMINE 2000 reagent (Invitrogen, Carlsbad, CA, USA) as per protocols recommended by the manufacturer. For RNA interference (RNAi) of Pak1, 150 pmol of PTEN small interfering RNA (siPTEN) and control siRNA (both from Shanghai GenePharma Co.) was used for each transfection using LipofectAMINE 2000 reagent. For constructing the stable transfectant, pGPU6/GFP/Neo and pGPU6/GFP/Neo shPak1 were separately transfected into LoVo. Forty-eight hours after transfection, G418 at 1.0 mg/ml (Merck) was added for the selection of stable clones.
Cell proliferation assays
Stable LoVo clones were obtained by transfection with the PAK1 shRNA expression vector and empty vector, followed by selection in 1 mg/ml G418 media. To measure the effects of knockdown on cell proliferation, PAK1 shRNA-transfected cells were seeded at concentrations of 2 × 103 per well in 96-well plates. After 0, 1, 2, and 3 days, cell proliferation was measured by cell counting kit-8 (CCK-8) (Beyotime Institute of Biotechnology) according to the manufacturer's instructions. SW480 cells were transfected in six-well plates. Twenty-four hours later, the transfected cells were trypsinized and plated in 96-well plates with 1.0 × 103 cells in 100 μl of the medium and allowed to attach for 24 h before initiating treatment. Either 20 mM SP600125 or DMSO alone was added to fresh media then used to culture cells. After 48 h, CCK-8 (10 μl) was added to each well at different time points and incubated at 37°C for 1.5 h and absorbance at 450 nm was measured after 1 h of incubation, following the manufacturer’s instructions.
Colony forming efficiency in soft agar
To examine the anchorage-independent growth, 1 ml of 0.5% agarose in high-fertility culture medium was allowed to solidify in 35-mm culture dishes. These were overlaid with 1 ml of 0.33% agarose containing 1 × 103 cells/ml in middle fertility culture medium. One milliliter of low-fertility culture medium was added to each well the next day. Cells from different stably transfected cell strains were incubated for 2 weeks at 37°C. The cell colonies (more than 15 cells) were counted under the microscope. The average of three independent experiments was shown.
Serum starvation and analysis of apoptosis
Cell-cycle distribution or apoptosis was measured with and without exposure to 5-FU. Then 1 × 106 vector-shPAK1 or shPAK1 LoVo cells were grown to confluence in six-well plates in 10% FBS for 24 h, when media was replaced to 0.2% FBS for an additional 48 h. Apoptosis was measured simultaneously by staining cells with Annexin-V-PE (BioVision) and 7AAD (BD Pharmingen) according to the manufacturer's protocol. After culture at different time points, samples were harvested (including detached cells), suspended in PBS and fixed in 70% ethanol, and their DNA content was evaluated after propidium iodide staining. Fluorescence-activated cell sorting analysis was carried out using a FACScan flow cytometer (Beckton Dickinson, San Diego, CA, USA) and Cell Quest software. Cell debris and fixation artifacts were gated out.
Western blot analysis
Total cell lysates were extracted by PBSTDS (100 ml 10 3 PBS, 10 ml 100% Triton X-100, 5 g nadeoxycholate, 1 g SDS, 1 nM EDTA, up to 1,000 ml/day H2O) on ice and were centrifuged at 20,000 rpm for 30 min at 4°C. Concentration of the protein was measured. Protein (50 μg) was mixed with loading buffer with final concentration of 1×. After boiling for 8 min, proteins were separated by running in SDS–polyacrylamide gel. Proteins were then transferred to a nitrocellulose membrane and then blocked for 1 h at room temperature in TBS-T [50 mmol/l Tris–HCl (pH 7.5), 150 mmol/l NaCl, 0.1% Tween 20 buffer containing 5% nonfat milk]. Membranes were then incubated overnight at 4°C or 1 h at room temperature with the respective primary antibodies: phospho-JNK (1:500), JNK (1:500), cyclinD1 (1:500), CDK4 (1:500), CDK6 (1:500), GAPDH (1:500), PTEN (1:500), PAK1 (1:500), Bcl-2 (1:500), Bcl-xl (1:500), XIAP (1:500), and phosphorylated Badser112 (1:500). Anti-mouse IgG-HRP, anti-rabbit IgG-HRP antibody (Santa Cruz), and the blots were developed with a Pierce ECL Western Blotting Substrate (Pierce, Rockford, IL, USA).
Drug treatment
Cells were seeded in six-well plates at 20–30% density 48 h before treatment. Cells were then incubated in culture medium containing 5-FU (Sigma Chemical Co.) in dimethyl sulfoxide (final concentration <0.1%) or no addition (control). For in vitro studies, unless noted, the final concentrations used for MAPK inhibitors and 5-fluorouracil were 20 μM or 50 μM, respectively.
Tumor cell xenotransplantation
LoVo cells stably expressing PAK1 shRNA and empty vector controls were s.c. injected into the lower flanks of NCr nu/nu mice (Taconic Farms) at a dose of 5 × 106 viable tumor cells. There are five mice for each group. Mouse tumor growth was measured with a digital caliper and calculated by using the formula of a rotational ellipsoid: V = π/6 × A × B2, where V is volume, A is the longest tumor axis, and B is the perpendicular shorter tumor axis. In vivo chemotherapy with 5-fluorouracil was started after 2 weeks once xenografts reached an average volume of at least 100 mm3. 5-Fluorouracil was administered at a dose of 50 mg/kg i.p. every third day for 2 weeks. All animal experiments were done according to the institutional guidelines of Lifespan Animal Welfare Committee of Nanfang Hospital.
Results
PAK1 protein is elevated in colorectal cancer cells
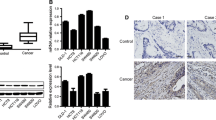
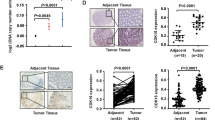
Previous data shows that PAK1 expression is increased significantly with malignant progression of human colorectal carcinoma [9]. We found that PAK1 expression increased gradually from normal colon mucosa to invasive and metastatic carcinomas (Table 1), with the highest expression in metastatic tumors. According to the Dukes grading, PAK1 was found lower expressed in less malignant Dukes A CRCs compared with invasive Dukes D (Table 1, P < 0.0001). However, PAK1 expression level was not correlated with the different differentiated state of CRCs (Table 1, P = 0.373). A marked difference was observed in the same section having both normal colon mucosa and atypical hyperplastic adenomas, where PAK1 expression is markedly higher than in normal mucosa, suggesting that PAK1 is overexpressed in the atypical hyperplastic adenomas that may occur in the early stage of CRC progression (Table 1). Apart from the cytoplasmic expression of PAK1, we were impressed by the nuclear translocation of PAK1 in some CRC cases (Supplementary Fig. 1a, b). Importantly, by examination of more nuclei-localized CRC cases and linking them to Dukes stages, we found a correlation between PAK1 nuclear localization and the Dukes staging; that is, higher Dukes corresponds to a higher percentage of PAK1 nuclear localization (Table 2, P = 0.001). Intriguingly, PAK1 nuclear localization in breast cancer is found to contribute to the tamoxifen resistance and to breast cancer development from ductal hyperplasia to ductal carcinoma and to adenocarcinoma [11]. This was reminiscent of increased PAK1 nuclear localization in CRC which might predict a poor prognosis for the CRC patients.
Effect of PAK1 expression on cell proliferation and apoptosis
To assess the role of PAK1 in CRC cell proliferation, we knocked down PAK1 expression using short hairpin RNAs, which effectively downregulated PAK1 expression in LoVo cells (Fig. 1a). Growth of LoVo cells was obviously decreased after transfection of PAK1 shRNA compared with transfected empty vector (Fig. 1b). There was statistical difference between PAK1 shRNA and empty vector after 48 h (P < 0.05). As shown in Fig. 1c, shPAK1 transfectants were 3-fold more apoptotic when compared with vector (P < 0.05). Next, we analyzed the effect of PAK1 knockdown on the tumorigenic potential of LoVo cells. As shown in Fig. 1d, LoVo shPAK1 presented significantly inhibited anchorage-independent growth in soft agar compared with empty vector. Figure 1e showed that PAK1 knockdown resulted in decreased Bcl-2, Bcl-xl, XIAP, and phosphorylated Badser112.
PAK1 knockdown decreased proliferation and promotes apoptosis of colon cancer cells. PAK1 inhibition caused colon cancer cell cycle arrest at G1 phase. a Immunoblot analysis of PAK1 in stable vector and PAK1 shRNA LoVo cells. b PAK1 inhibition in LoVo cells decreased proliferation, as measured with the CCK-8 assay. Significant inhibition of proliferation was seen in cells transfected with PAK1 shRNA relative to those transfected with the empty vector (Student’s t test, P < 0.05). c The apoptosis rate of PAK1 shRNA LoVo cells significantly increased by almost 10% (Student’s t test, P < 0.05 for both cell lines). d Compared with control, the number of colonies was significantly reduced in PAK1 shRNA LoVo cells (Student’s t test, P < 0.05). Data are from at least three independent experiments carried out in triplicate. e Immunoblot analyses showed that PAK1 knockdown in LoVo cells affected the levels of Bcl-2, Bcl-xl, XIAP, or phosphorylated Badser112. In immunoblots, the numbers underneath each band indicate the fold change in intensity of the corresponding band relative to the control. f DNA content analysis by flow cytometry. Samples were fixed and stained with propidium iodide (PI). PI-stained cells were gated on the basis of their DNA content. The percentage of cells with 2 N-DNA content, indicative of G1 phase of the cell cycle, is indicated. PAK1 knockdown increased the number of cells at G1 (Student’s t test, P < 0.05). g Immunoblot analyses showed that PAK1 knockdown in LoVo cells affects the levels of proteins crucial in G1 transition including cyclinD1, CDK4/6. In immunoblots, the numbers underneath each band indicated the fold change in intensity of the corresponding band relative to the control
PAK1 knockdown induced a delay in the G1 phase of the cell cycle and decreased the expression of cyclinD1, CDK4/6
To investigate the effects of PAK1 on the cell cycle, we analyzed the number and distribution of cells in the phases of the cell cycle by flow cytometry. As shown in Fig. 1f, PAK1 knockdown significantly increased the number of cells at the G1 transition. PAK1 knockdown resulted in almost a 12% increase in the number of cells in G1 compared with empty vector-transfected cells (P < 0.05). We next investigated the effect of PAK1 on crucial G1 checkpoint proteins. The cell lysate of LoVo PAK1 shRNA and vector controls were analyzed for the level of cyclinD1, CDK4/6. As shown in Fig. 1g, knockdown of PAK1 in LoVo cells reduced the expression of cyclinD1, CDK4/6.
PAK1 effects on cell proliferation and G1 transition required activity of JNK
Recently, Fang et al. reported that direct phosphorylation of MAPKs play an important role in the regulation of proliferation in cancer [15]. In light of this, we next tested the hypothesis that PAK1 might promote colon tumorigenesis by regulating MAPK in CRC. As shown in Fig. 2a, overexpression of PAK1 effectively increased the expression of phosphorylated JNK. To investigate whether the effects of PAK1 on cell proliferation and transition from the G1 phase to mitosis necessitated JNK activity, we employed SP600125, an inhibitor of JNK activity by a pharmacologic JNK inhibitor, which significantly reduced proliferation, the number of cells in G1 cells, and the level of CDK4/6, cyclinD1 in SW480 cells with PAK1 upregulation. U0126 or SB20358 had no effects on proliferation transition (Fig. 2b).
PAK1-mediated colon cancer proliferation and G1 transition required activity of JNK. PTEN blocked PAK1/JNK-induced proliferation and apoptosis in CRC cells. a SP600125 inhibited the effect of PAK1 on G1 phase by DNA content analysis by flow cytometry. Samples were fixed and stained with propidium iodide (PI). PI-stained cells were gated on the basis of their DNA content (one-way ANOVA, P < 0.05). b PAK1 upregulation in SW480 cells increased proliferation, as measured with the CCK-8 assay. Significant inhibition of proliferation was seen in cells transfected with PAK1 T423E relative to those transfected with the empty vector (one-way ANOVA, P < 0.05). SP600125, but not U0126, SB20358, inhibited the effect of PAK1. c Immunoblot analyses showed that PAK1 downregulation in LoVo cells affected the activity of JNK. d At 48 h after transfection with control or PAK1 T423E or treatment with 20 μM SP600125 for 24 h, CDK4/6, cyclinD1 and GAPDH levels in the cellular extracts were assayed by immunoblotting. e Immunoblot analysis of PTEN in PAK1 shRNA LoVo cells after transfection with PTEN siRNA or not. f At 48 h after transfection with control or PAK1 T423E or incubated with SP600125 for 24 h, PTEN and GAPDH levels in the cellular extracts were assayed by immunoblotting. g The apoptosis rate of PAK1 shRNA LoVo cells transfected with PTEN siRNA significantly decreased by nearly 8% (one-way ANOVA). h PTEN inhibition in PAK1 shRNA LoVo cells increased proliferation, as measured with the CCK-8 assay. Significant effect was seen in cells transfected with PTEN siRNA relative to those transfected with control (one-way ANOVA). Data were from at least three independent experiments carried out in triplicate. *P < 0.05
PTEN inhibits PAK1/JNK-induced proliferation in CRC cells
Increasing evidences indicated that JNK might suppress tumor development [16]. But our study suggested that the activation of JNK-mediated signal pathway was involved in the effects of PAK1 on CRC proliferation. To understand how PAK1/JNK induced CRC cell proliferation and mitosis, we next investigated the possible correlation between PAK1/JNK and PTEN levels in CRC cells.
In PAK1 shPAK1 cells, PAK1 knockdown effectively increased PTEN expression (Fig. 2e). To further confirm the role of PAK1/JNK in PTEN regulation, SW480 cells were co-transfected with siRNA directed to PTEN or PAK1-T423E. Twenty-four hours after transfection, cells were treated with SP600125 for an additional 48 h. PTEN expression was determined by Western blotting. Figure 2f shows that transfection with PAK1-T423E decreased the level of PTEN; SP600125 attenuated the effect. To ascertain the function of PTEN in PAK1-mediated cell proliferation, we subjected these colon cancer cells to proliferation assays and flow cytometry. Figure 2g and h show that PTEN knockdown in shPAK1 LoVo cells was sufficient to completely rescue the reduction in cell proliferation and apoptosis caused by PAK1 downregulation.
These data suggested that PAK1 decreased PTEN via JNK, and JNK inactivity appeared to be required for the expression of PTEN.
Knockdown of PAK1 significantly enhances cytotoxicity of 5-fluorouracil
Drug resistance to 5-fluorouracil (5-FU) is still a major limitation to its clinical use. Several reports show that LoVo cells have low sensitivity incubated with 5-FU (50 μM, 72 h) [17]. Based on our finding that PAK1 RNAi induced apoptosis in CRC cells, we then investigated whether the combination of PAK1 RNAi and 5-fluorouracil would enhance the cytotoxicity of 5-FU. The LoVo shPAK1 cells and control cells were treated with 50 μM 5-fluorouracil for 24 h, 48 h, and 72 h. Then proliferation and apoptosis were measured by CCK-8 and flow cytometry analyses. Consistent with previous reports, in both CCK-8 and flow cytometry analyses, knockdown of PAK1 in LoVo cells significantly enhanced apoptosis induced by 5-fluorouracil (50 μM, P < 0.05) (Fig. 3a). These data demonstrated that the enhancement of apoptotic effect of 5-fluorouracil was correlated with the knockdown of PAK1 (Fig. 3b). As shown in Fig. 3c, PAK1 knockdown resulted in G1 arrest and decreased the protein level of cyclinD1,CDK4/6. These results indicate that the knockdown of PAK1 could synergistically enhance the chemosensitivities of LoVo cells to 5-fluorouracil.
The contribution of PAK1 in 5-FU-mediated proliferation and apoptosis. a The proliferation of LoVo cells transiently transfected with PAK1 shRNA in the absence or presence of 5-FU (50 μM) for 0, 24 h, 48 h, and 72 h were measured with the CCK-8 assay (ANOVA, *P < 0.05). b After stable shRNA expression targeting PAK1, LoVo cells were treated with 5-FU or equal volume DMSO for 72 h, and apoptosis was determined by flow cytometry (Student's t test, *P < 0.05). c Immunoblot analyses showed that PAK1 knockdown in LoVo cells in the absence or presence of 5-FU affected the levels of proteins crucial in G1 transition including cyclinD1, CDK4/6. In immunoblots, the numbers underneath each band indicated the fold change in intensity of the corresponding band relative to the control
PAK1 knockdown decreased proliferation and tumorigenicity in vivo
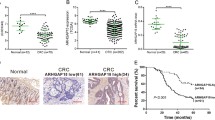
Next, we analyzed the effects of PAK1 on 5-fluorouracil resistance of colon cancer cells in vivo. We generated s.c. xenografts in NCr nu/nu mice by using LoVo shPAK1 cells compared with empty vector controls. Once xenografts reached an average volume of at least 100 mm3, animals were divided into four groups: vector, shPAK1, vector + 5-FU, and shPAK1 + 5-FU. Xenograft tumors were monitored for 30 days. As shown in Fig. 4a, tumor growth was significantly suppressed in PAK1 shRNA group compared to that in empty vector group (P < 0.05). Tumor growth markedly regressed in response to treatment with 5-fluorouracil in mice that received xenografts of LoVo shPAK1 cells (P < 0.05). In contrast, LoVo empty vectors cells were much more resistant to 5-fluorouracil. Significant downregulation PAK1 staining was observed in the combination group, PAK1 shRNA group, and 5-fluorouracil treatment group, but not in the empty vector (Fig. 4b). As shown in Fig. 4b, Ki-67 was lower in shPAK1 and the combination tumor specimens when compared with vector and 5-fluorouracil specimens. These data suggest that PAK1 knockdown might suppress tumor growth in vivo. Furthermore, increased levels of PAK1 might augment chemoresistance in colon cancer cells.
Effects of tumor cell growth in vivo by PAK1 knockdown. a Growth curves of LoVo tumor in nude mice in different treated groups. Values presented as mean ± SEM (ANOVA, *P < 0.05, shPAK1 vs. vector following 5FU treatment or not). Data table lists mean value for four groups: vector, 5-FU, shPAK1, and 5-FU + shPAK1. b Immunohistochemical analysis of xenograft slides blotted with Ki-67 and PAK1 antibodies. Original magnification ×100
Discussion
In this study, we found that the expression of PAK1 expression was increased significantly with malignant progression of human colorectal carcinoma (Table 1), suggesting that PAK1 might play an important role in the carcinogenesis and progression of colorectal cancer. Furthermore, we found a significant correlation between PAK1 nuclear localization and the Dukes staging (Table 2). We hypothesized that the nuclear translocation of PAK1 might contribute to metastasis, proliferation, and chemosensitivities in colorectal cancer. Further studies are required to investigate the nuclear PAK1 functions and identify putative PAK1-interacting nuclear proteins.
However, direct demonstration of PAK1’s function in colon cancer tumorigenesis is currently lacking. To elucidate the role that PAK1 may have in CRC progression, we used small interfering RNA technique to knock down PAK1 in colorectal cancer cell lines. A major novel finding presented in our study was that PAK1 downregulation in CRC cancer cells greatly decreased their proliferative capacity (Fig. 1b). Targeted downregulation of PAK1 in LoVo cells resulted in significant reduction of mammary tumor size (P < 0.05) (Fig. 4a). These observations suggested that colorectal cancer cells can become dependent on PAK1 for survival.
Next, we found that PAK1 knockdown prolonged the doubling time of CRC cells and caused an arrest at the G1 transition of the cell cycle (Fig. 1f). It has been reported that entry into G1 from a quiescent state (G0) is associated with the expression and activation of cyclinD:Cdk4/Cdk6, which phosphorylate and inactivate the retinoblastoma protein (Rb) during the first half of G1 [18–20]. This hypophosphorylated form of Rb is now capable of binding to E2F family members, which is necessary for G1/S phase transition and cell-cycle progression [21, 22]. As expected, the data in Fig. 1g implied that Pak1 could regulate the expression of cyclinD:Cdk4/Cdk6. JNK has been shown to modulate the expression of cyclinD1/Cdk4 in many cells [23–25]. The JNK/c-Jun pathway is a critical component of the proliferative response and induces G0 to G1 cell-cycle progression in many cell types [26]. The JNK pathway has also been shown to be closely linked to apoptosis [27]. Activation of the JNK pathway leads to regulation of cellular survival or cellular apoptosis, and the decision appears to be cell-type specific as well as stimulating signal specific [16, 28–30]. Recently, it has been shown that c-Jun contributes to the promotion of cellular survival by regulating the expression of PTEN [13]. Several studies report that Pak1 induces cancer carcinogenesis and may involve activation of JNK [15, 31, 32]. In this study, we showed that the level of phosphorylated JNK was decreased in LoVo shPAK1 cells (Fig. 2c). We hypothesized that PAK1 induces transcription of cyclinD1, CDK4/6 depending on JNK pathway activity. Indeed, we found that the observed effects of PAK1 downregulation on LoVo cells proliferation and G1 transition require JNK pathway activity, as inhibition of c-Jun amino terminal kinases (JNK) by SP600125, the first selective JNK inhibitor, abolished PAK1-induced cell proliferation in CRC cells (Fig. 2b). U0126 or SB20358 had no effects on cell proliferation regulated by PAK1 upregulation. PAK1 downregulation has been shown to downregulate several important pro-apoptotic pathways [33–37]. In this study, we also showed that the apoptosis rate was increased in LoVo shPAK1 (Fig. 1c). The level of Bcl-2, Bcl-xl, XIAP, or phosphorylated Badser112 was decreased in LoVo shPAK1 (Fig. 1e). Interestingly, we found that inhibition of PTEN expression was important for shPAK1-mediated apoptosis of CRC cells (Fig. 2g). Consistent with this notion, we also noticed that the PTEN protein level in LoVo shPAK1 cells was high (Fig. 2e) and correlated with the lowly proliferate property of the cells (Fig. 2h). Although PTEN is regulated by other kinases, it has been reported that JNK is the important kinase regulating the expression of PTEN. Our data established the first evidence that PTEN might be associated with PAK1/JNK-mediated proliferation of CRC.
5-Fluorouracil (5-FU) is one of the most widely used chemotherapeutic agents for breast cancer, colorectal cancer (CRC), and GC [38]. Unfortunately, some patients, especially with late-stage colorectal cancer, showed a poor response, possibly owing to inefficiency of the chemotherapy [17]. Recently, it has been shown that the balance of Bax, Bcl-2, and Bcl-xl could be used as a marker to predict 5-FU treatment response of colon tumors whatever their p53 status [17, 39, 40]. Our data demonstrated that PAK1 knockdown inhibited the expression of Bcl-2 and Bcl-xl (Fig. 1e). Therefore, we hypothesized that knockdown of PAK1 might enhance the response of CRC to 5-FU because LoVo cells expressed high levels of Bcl-2/Bcl-xl combined with a low level of Bax for the resistance of 5-FU to CRC [40]. So, we invested the chemoresistance mechanism via LoVo cells. Indeed, we found that the combination of PAK1 knockdown and 5-fluorouracil resulted in strong impairment of G1 phase progression and the synergistic induction of apoptosis (Fig. 3a, b). Our xenograft mouse models thus suggested that PAK1 inhibition and 5-fluorouracil combination group might have potential utility in treating colon cancer patients.
In conclusion, we provided convincing evidence that knockdown of PAK1 in colorectal cancer cells attenuated the tumorigenic properties. Our study implied that PAK1 knockdown decreased tumor growth in vivo and in vitro by arresting the transition from G1 phase to mitosis and promoting apoptosis. We provided the first functional link between PAK1 and JNK and showed that PAK1 knockdown led to JNK downregulation and subsequently decreased colon cancer proliferation and progression through G1 arrest. The effect of PAK1/JNK-mediated proliferation and mitosis might be repressed by PTEN. Knockdown of PAK1 could enhance the chemosensitivity of CRCs to 5-fluorouracil though G1 arrest. We thus provided a new lead toward future development of specific strategies to downregulate PAK1 levels and function, and for possible prevention of colorectal cancer.
References
Jones Jr DV, Winn RJ, Brown BW, Levy LB, Pugh RP, Wade 3rd JL, Gross HM, Pendergrass KB, Levin B, Abbruzzese JL. Randomized phase III study of 5-fluorouracil plus high dose folinic acid versus 5-fluorouracil plus folinic acid plus methyl-lomustine for patients with advanced colorectal cancer. Cancer. 1995;76:1709–14.
Marsoni S. Fluorouracil and folinic acid in colon cancer. IMPACT Investigators. Lancet. 1995;345:1582–3.
Adam L, Vadlamudi R, Mandal M, Chernoff J, Kumar R. Regulation of microfilament reorganization and invasiveness of breast cancer cells by kinase dead p21-activated kinase-1. J Biol Chem. 2000;275:12041–50.
Liu F, Li X, Wang C, Cai X, Du Z, Xu H, Li F. Downregulation of p21-activated kinase-1 inhibits the growth of gastric cancer cells involving cyclin B1. Int J Cancer. 2009;125:2511–9.
O'Sullivan GC, Tangney M, Casey G, Ambrose M, Houston A, Barry OP. Modulation of p21-activated kinase 1 alters the behavior of renal cell carcinoma. Int J Cancer. 2007;121:1930–40.
Li F, Adam L, Vadlamudi RK, Zhou H, Sen S, Chernoff J, Mandal M, Kumar R. p21-activated kinase 1 interacts with and phosphorylates histone H3 in breast cancer cells. EMBO Rep. 2002;3:767–73.
Maroto B, Ye MB, von Lohneysen K, Schnelzer A, Knaus UG. P21-activated kinase is required for mitotic progression and regulates Plk1. Oncogene. 2008;27:4900–8.
Zhao ZS, Lim JP, Ng YW, Lim L, Manser E. The GIT-associated kinase PAK targets to the centrosome and regulates Aurora-A. Mol Cell. 2005;20:237–49.
Balasenthil S, Sahin AA, Barnes CJ, Wang RA, Pestell RG, Vadlamudi RK, Kumar R. p21-activated kinase-1 signaling mediates cyclin D1 expression in mammary epithelial and cancer cells. J Biol Chem. 2004;279:1422–8.
Wang RA, Zhang H, Balasenthil S, Medina D, Kumar R. PAK1 hyperactivation is sufficient for mammary gland tumor formation. Oncogene. 2006;25:2931–6.
Aoki H, Yokoyama T, Fujiwara K, Tari AM, Sawaya R, Suki D, Hess KR, Aldape KD, Kondo S, Kumar R, Kondo Y. Phosphorylated Pak1 level in the cytoplasm correlates with shorter survival time in patients with glioblastoma. Clin Cancer Res. 2007;13:6603–9.
Schraml P, Schwerdtfeger G, Burkhalter F, Raggi A, Schmidt D, Ruffalo T, King W, Wilber K, Mihatsch MJ, Moch H. Combined array comparative genomic hybridization and tissue microarray analysis suggest PAK1 at 11q13.5–q14 as a critical oncogene target in ovarian carcinoma. Am J Pathol. 2003;163:985–92.
Gong W, An Z, Wang Y, Pan X, Fang W, Jiang B, Zhang H. P21-activated kinase 5 is overexpressed during colorectal cancer progression and regulates colorectal carcinoma cell adhesion and migration. Int J Cancer. 2009;125:548–55.
Li Z, Dong X, Wang Z, Liu W, Deng N, Ding Y, Tang L, Hla T, Zeng R, Li L, Wu D. Regulation of PTEN by Rho small GTPases. Nat Cell Biol. 2005;7:399–404.
Fang JY, Richardson BC. The MAPK signalling pathways and colorectal cancer. Lancet Oncol. 2005;6:322–7.
Manning AM, Davis RJ. Targeting JNK for therapeutic benefit: from junk to gold? Nat Rev Drug Discov. 2003;2:554–65.
Mariadason JM, Arango D, Shi Q, Wilson AJ, Corner GA, Nicholas C, Aranes MJ, Lesser M, Schwartz EL, Augenlicht LH. Gene expression profiling-based prediction of response of colon carcinoma cells to 5-fluorouracil and camptothecin. Cancer Res. 2003;63:8791–812.
Dowdy SF, Hinds PW, Louie K, Reed SI, Arnold A, Weinberg RA. Physical interaction of the retinoblastoma protein with human D cyclins. Cell. 1993;73:499–511.
Ezhevsky SA, Ho A, Becker-Hapak M, Davis PK, Dowdy SF. Differential regulation of retinoblastoma tumor suppressor protein by G(1) cyclin-dependent kinase complexes in vivo. Mol Cell Biol. 2001;21:4773–84.
Ezhevsky SA, Nagahara H, Vocero-Akbani AM, Gius DR, Wei MC, Dowdy SF. Hypo-phosphorylation of the retinoblastoma protein (pRb) by cyclin D:Cdk4/6 complexes results in active pRb. Proc Natl Acad Sci USA. 1997;94:10699–704.
Harbour JW, Luo RX. Dei Santi A, Postigo AA, Dean DC. Cdk phosphorylation triggers sequential intramolecular interactions that progressively block Rb functions as cells move through G1. Cell. 1999;98:859–69.
Lundberg AS, Weinberg RA. Functional inactivation of the retinoblastoma protein requires sequential modification by at least two distinct cyclin–cdk complexes. Mol Cell Biol. 1998;18:753–61.
Schwabe RF, Bradham CA, Uehara T, Hatano E, Bennett BL, Schoonhoven R, Brenner DA. c-Jun-N-terminal kinase drives cyclin D1 expression and proliferation during liver regeneration. Hepatology. 2003;37:824–32.
Pedram A, Razandi M, Levin ER. Extracellular signal-regulated protein kinase/Jun kinase cross-talk underlies vascular endothelial cell growth factor-induced endothelial cell proliferation. J Biol Chem. 1998;273:26722–8.
Zhang JY, Tao S, Kimmel R, Khavari PA. CDK4 regulation by TNFR1 and JNK is required for NF-kappaB-mediated epidermal growth control. J Cell Biol. 2005;168:561–6.
Shaulian E, Karin M. AP-1 in cell proliferation and survival. Oncogene. 2001;20:2390–400.
Davis RJ. Signal transduction by the JNK group of MAP kinases. Cell. 2000;103:239–52.
Kuntzen C, Sonuc N, De Toni EN, Opelz C, Mucha SR, Gerbes AL, Eichhorst ST. Inhibition of c-Jun-N-terminal-kinase sensitizes tumor cells to CD95-induced apoptosis and induces G2/M cell cycle arrest. Cancer Res. 2005;65:6780–8.
Potapova O, Gorospe M, Bost F, Dean NM, Gaarde WA, Mercola D, Holbrook NJ. c-Jun N-terminal kinase is essential for growth of human T98G glioblastoma cells. J Biol Chem. 2000;275:24767–75.
Sabapathy K, Hochedlinger K, Nam SY, Bauer A, Karin M, Wagner EF. Distinct roles for JNK1 and JNK2 in regulating JNK activity and c-Jun-dependent cell proliferation. Mol Cell. 2004;15:713–25.
Poitras L, Jean S, Islam N, Moss T. PAK interacts with NCK and MLK2 to regulate the activation of jun N-terminal kinase. FEBS Lett. 2003;543:129–35.
Zhou L, Yan C, Gieling RG, Kida Y, Garner W, Li W, Han YP. Tumor necrosis factor-alpha induced expression of matrix metalloproteinase-9 through p21-activated kinase-1. BMC Immunol. 2009;10:15.
Dummler B, Ohshiro K, Kumar R, Field J. Pak protein kinases and their role in cancer. Cancer Metastasis Rev. 2009;28:51–63.
Denning MF, Wang Y, Tibudan S, Alkan S, Nickoloff BJ, Qin JZ. Caspase activation and disruption of mitochondrial membrane potential during UV radiation-induced apoptosis of human keratinocytes requires activation of protein kinase C. Cell Death Differ. 2002;9:40–52.
Zang M, Hayne C, Luo Z. Interaction between active Pak1 and Raf-1 is necessary for phosphorylation and activation of Raf-1. J Biol Chem. 2002;277:4395–405.
Jin S, Zhuo Y, Guo W, Field J. p21-activated Kinase 1 (Pak1)-dependent phosphorylation of Raf-1 regulates its mitochondrial localization, phosphorylation of BAD, and Bcl-2 association. J Biol Chem. 2005;280:24698–705.
Schurmann A, Mooney AF, Sanders LC, Sells MA, Wang HG, Reed JC, Bokoch GM. p21-activated kinase 1 phosphorylates the death agonist bad and protects cells from apoptosis. Mol Cell Biol. 2000;20:453–61.
Longley DB, Harkin DP, Johnston PG. 5-fluorouracil: mechanisms of action and clinical strategies. Nat Rev Cancer. 2003;3:330–8.
Tokunaga E, Oda S, Fukushima M, Maehara Y, Sugimachi K. Differential growth inhibition by 5-fluorouracil in human colorectal carcinoma cell lines. Eur J Cancer. 2000;36:1998–2006.
Violette S, Poulain L, Dussaulx E, Pepin D, Faussat AM, Chambaz J, Lacorte JM, Staedel C, Lesuffleur T. Resistance of colon cancer cells to long-term 5-fluorouracil exposure is correlated to the relative level of Bcl-2 and Bcl-X(L) in addition to Bax and p53 status. Int J Cancer. 2002;98:498–504.
Acknowledgments
Grant support: The Nature Science Foundation of China grant 30830048 and 973 Program of the Ministry of Science and Technology of China (2010CB912203) to Hongquan Zhang. We thank Dr. Feici Diao for critical reading of the manuscript, Dr. Hua Tian for providing the pcDNA3.1(+)-PTEN and vector plasmids, and Dr. Yan Sun for helpful advice with the siRNA, cell cycle, and apoptosis experiments.
Conflicts of interest
None
Author information
Authors and Affiliations
Corresponding author
Additional information
Haitao Qing and Wei Gong contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary Fig. 1
Nuclear localization of PAK1. (a) and (b) are representatives which have strong PAK1 immunoactivity in the nucleus as well as in the cytoplasm. a, b: ×400 (JPEG 26 kb)
Rights and permissions
About this article
Cite this article
Qing, H., Gong, W., Che, Y. et al. PAK1-dependent MAPK pathway activation is required for colorectal cancer cell proliferation. Tumor Biol. 33, 985–994 (2012). https://doi.org/10.1007/s13277-012-0327-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-012-0327-1