Abstract
Background
Trichloroethylene (TCE) is a common industrial solvent and an occupational toxicant. TCE exposure can cause severe hepatotoxicity, but its mode of action is poorly understood. Many studies have shown TCE-induced liver damage in mice, while few have examined the effects of TCE in rats.
Objective
To explore the effects of TCE in Sprague–Dawley (SD) rats and the potential mechanisms in TCE-induced hepatocytotoxicity.
Results
The liver index and activities of liver damage marker enzymes (ALT, AST and ALP) in rat serum were elevated along with the increase in TCE dose, while the levels of total proteins and albumin in serum were reduced. The results suggest that TCE is hepatotoxic in rats. 2D-DIGE electrophoresis showed that the levels of 66 liver proteins in TCE-treated rats were abnormally altered (39 up-regulated and 27 down-regulated). In these proteins, six enzymes were related to liver damage and carcinogenesis as indicated by bioinformatics analysis, and Western blot analysis confirmed the alterations of three of them, i.e., aldehyde dehydrogenase 2 (Aldh2), glutathione S-transferase Mu 1 (Gstm1) and peroxisomal bifunctional enzyme (PBE, also named as Ehhadh). PBE was the only protein elevated in a dose dependent manner. Whether PBE can be a biomarker of TCE hepatotoxicity needs to be further studied.
Conclusion
These findings indicate that TCE induces liver injury in rats.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Trichloroethylene (TCE) is a chlorinated hydrocarbon widely used as a solvent in industrial applications. Because of inappropriate usage and transportation, TCE is now a major pollutant in soil and ground water (Wu and Schaum 2000). TCE exposure can cause severe toxic effects to humans, and the EPA (US Environmental Protection Agency) characterized TCE as carcinogenic in 2011 (Chiu et al. 2013). Exposure to TCE is therefore a human health risk in China and other regions of the world (Kamijima et al. 2007).
Liver is the major organ where TCE is typically metabolized into oxidative metabolites by cytochrome P450-dependent oxidation pathways. These metabolites play important roles in TCE-induced hepatotoxicity and carcinogenesis (Allemand et al. 1978; Lash et al. 2000). However, the precise mechanisms underlying TCE hepatotoxicity are unclear.
TCE appears to induce toxic responses in human hepatocytes (L-02 line) by dysregulating the expression of genes encoding CYP1A2 and BAX (BAX is associated with apoptosis) (Xu et al. 2012). Repeated administration of TCE to mice by oral gavage can produce hepatocellular proliferation, mitochondrial dysfunction and glycogen depletion (Sano et al. 2009). Proteome profiles of TCE-induced protein dysregulation in cultured hepatocytes indicate that specific proteins are related to TCE toxicity in human hepatocytes (Liu et al. 2007; Huang et al. 2009). Although there have been numerous studies on TCE-induced liver damage in either mouse in vivo or hepatocytes in vitro, few studies of TCE-induced toxicity in rat liver have been reported.
We studied TCE-induced liver toxicity in rats by exposing rats to TCE by gastric gavage and evaluating its effects on the liver. We then performed a comparative proteomics analysis, focusing on the profiles of liver proteins in TCE-treated SD rats. These studies were followed by analysis of the potential roles of the alterations in protein expression in TCE-induced liver toxicity.
Materials and methods
Animals and treatment
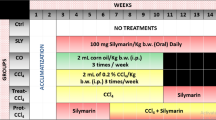
Male Sprague–Dawley (SD) rats, aged 7 weeks with body weights of 103–119 g, were purchased from the Experimental Animal Center of Guangdong Province (Guangzhou, China) and housed under specific pathogen-free (SPF) conditions. The animal experiments were approved by the Committee of Ethnics in the Shenzhen Center for Disease Control and Prevention. Animals were acclimatized to the laboratory conditions for 4 days prior to being randomly divided into four groups with ten rats per group. TCE was purchased from Sigma-Aldrich (Shanghai, China). The animals were fasted for 12 h before each administration, and food was provided 2 h after dosing. Tap water was available ad libitum. TCE was dissolved in corn oil at different doses (0, 250, 500 and 1000 mg/kg per day), with dosage being based on a previous report (Khan et al. 2009). TCE was administered by gastric gavage for 14 consecutive days. The body weight of each rat was recorded every other day during, and at the end of, the study. Animal care and treatments were performed in accordance with the Institutional Animal Care and the NIH Guide for the Care and Use of Laboratory Animals. At the end of the experiment (14 days), blood samples were collected and allowed to coagulate. The serum samples were then obtained and used for analyzing biochemical parameters. During necropsy, samples of liver tissue were taken, weighed and snap-frozen in liquid nitrogen to minimize proteolysis before storing at − 80 °C for analyses.
Serum biochemistry profile
The activities of alanine aminotransferase (ALT), aspartate aminotransferase (AST) and alkaline phosphatase (ALP), and the concentrations of total protein (TP) and albumin (ALB) in serum were analyzed using standard methodology (Bergmeyer et al. 1978), with commercially available kits obtained from Shanghai KEHUA bio-engineering (Shanghai, China). All analyses were performed on an Olympus AU 400 autoanalyzer (Hamburg, Germany).
Protein extraction and CyDye minimal labeling
Frozen liver samples were ground in liquid nitrogen and homogenized in a lysis buffer containing urea (7 M), thiourea (2 M), CHAPS [2% (w/v)], Tris (30 mM) and protease inhibitor cocktail (Thermo Scientific, Rockford, IL, USA). Homogenized samples were sonicated for 30 s, incubated on ice for 30 min and centrifuged at 20,000g for 30 min at 4 °C. Supernatants were precipitated with three volumes of ice-cold acetone at − 20 °C for 2 h, followed by centrifugation at 10,000g for 10 min at 4 °C. The resulting pellets were re-suspended in lysis buffer and centrifuged at 10,000g for 5 min. Protein concentrations of the supernatants were determined with the 2-D Quant kit (GE Healthcare, Pittsburgh, PA, USA) according to manufacturer instructions.
The purified samples were labeled with Cy2, Cy3 or Cy5 fluorescent dyes (200 pmol dyes per 25 μg protein) (GE healthcare, Pittsburgh, PA, USA) according to manufacturer instructions. Briefly, one half of individual samples from the same group were either labeled with Cy3 or Cy5 to avoid any dye-specific staining bias. An internal standard, made by pooling equal aliquots of all experimental samples, was labeled with Cy2. The labeling reaction was conducted on ice in darkness for 30 min and then quenched with 1 μL of 10 mM lysine (Sigma-Aldrich, Shanghai, China) for 10 min on ice shielded from light.
2D-DIGE electrophoresis
The Cy3- and Cy5-labeled samples were mixed together with an aliquot (25 μg) of Cy2-labeled internal standard. An equal volume of 2 × sample buffer containing urea (7 M), thiourea (2 M), CHAPS [4% (w/v)], dithiothreitol [DTT, 2% (w/v)], and IPG buffer [2% (v/v), at pH 3–11] was added to each mixed sample and incubated on ice for 10 min prior to bringing the total sample volume to 450 μL with rehydration buffer (8 M of urea, 2% w/v of CHAPS, 0.28% w/v of DTT, 0.5% v/v of IPG Buffer at pH 3–10, and 0.002% w/v of bromophenol blue). Twelve differently pooled samples were loaded onto individual IPG strips (pH 3–11, nonlinear gradient, 24 cm) (GE Healthcare, Pittsburgh, PA, USA) for isoelectric focusing (IEF) using an Ettan IPGphor 3 system (GE Healthcare, Pittsburgh, PA, USA). The IEF was programmed in the following five steps: 30 V for 12 h, 500 V for 1 h, 1000 V for 1 h, 8000 V gradient for 6 h, and then the unit was maintained at 8000 V until a total of 90,000 V-hours was reached. After IEF, the strips went through two steps of equilibration before applying on 12.5% SDS-PAGE gels. The second-dimension separation was conducted on an Ettan DALT six electrophoresis system (GE Healthcare, Pittsburgh, PA, USA) at 15 °C at 1 W per gel for 1 h, followed by 11 W per gel for 6 h. All electrophoresis procedures were performed in darkness.
Image acquisition and analysis
After electrophoresis, gels were immediately scanned by a Typhoon Trio Variable Mode Imager (GE Healthcare, Pittsburgh, PA, USA) at 100 μm resolution with excitation/emission wavelengths of 488 (Blue)/520, 532 (Green)/580 and 633 (Red)/670 nm for Cy2, Cy3 and Cy5, respectively. The images were processed by DeCyder 2D v6.5 (GE Healthcare, Pittsburgh, PA, USA) for differential analysis. Student’s t test and one-way ANOVA were used to compare the strength of spots between each treatment and the control. Statistically significant spots (p < 0.05) with an average ratio ≥ 1.2 or ≤ − 1.2 were marked for further analysis.
In-gel digestion and protein identification by MALDI-TOF–MS/MS
The significantly different protein spots were manually excised from a 2-DE gel stained with Coomassie brilliant blue G-250 staining solution. Gel plugs were de-stained with 50% acetonitrile in ammonium bicarbonate aqueous solution (25 mM) followed by dehydration in 100% acetonitrile. After removal of acetonitrile, each gel piece was digested overnight at 37 °C with 0.03 μg of sequencing-grade trypsin (Promega, Madison, WI, USA) in 15 μL of ammonium bicarbonate aqueous solution (25 mM). The extracted peptides were stored at − 80 °C prior to mass spectrometry analysis.
Peptides released from digestion were analyzed by an UltrafleXtreme MALDI-TOF/TOF mass spectrometer (Bruker Daltonics Inc., Billerica, MA, USA). Briefly, 2 µL of extracted peptide mixtures were spotted onto a polished steel MTP 384 target plate (Bruker Daltonics Inc., Billerica, MA, USA), air dried and covered with a 1 µL CHCA matrix (5 mg/mL in 50% ACN and 0.1% TFA). External calibration was performed using standard peptide calibration mixtures covering peaks between ~ 700 and 4000 Da (Bruker Daltonics Inc., Billerica, MA, USA). The peptide mass fingerprint (PMF) spectra were acquired in the positive reflection mode and the strongest seven peptides per spot were selected automatically for MS/MS analysis in LIFT mode. Protein identification by PMF and MS/MS spectra was performed using the Mascot search engine 2.2 (Matrix Science, Boston, MA, USA) and BioTools software (Bruker Daltonics Inc., Billerica, MA, USA). Confident matches in SwissProt database were defined by the Mascot score, the sequence coverage by matching peptides and statistical significance (p < 0.05).
Bioinformatics analysis
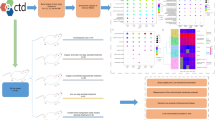
To determine the potential mechanisms mediating hepatotoxicity of TCE, PANTHER (http://pantherdb.org/) was used to classify protein families according to their cellular components, molecular functions and biological processes. STRING (http://string-db.org/, version 9.1) was used to identify protein networks of known and enrich proteins may be modulated in response to TCE exposure. Pathways with p values lower than 0.05 were considered to be significant (Franceschini et al. 2013).
Immunoblotting
To confirm the 2D-DIGE results, proteins with absolute values of average ratio > 1.2 and t values < 0.05 were selected for Western-blot analysis. Liver lysates were prepared with lysis buffer (Beyotime, Shanghai, China), homogenized, and centrifuged at 15,000g for 30 min. Extracts were mixed with protein loading buffer purchased from Thermo Scientific (Rockford, IL, USA) and heated for 5 min at 95 °C. The protein samples were separated by SDS-PAGE and transferred to PVDF membranes (Millipore, Darmstadt, Germany) in a semi-dry transfer unit (GE Healthcare, Pittsburgh, PA, USA). The blotted membranes were subsequently blocked in 5% (w/v) nonfat dry milk in TBS-T buffer (20 mM Tris–HCl, 150 mM NaCl, 0.2% Tween-20, pH 7.5) for 60 min. After being washed in TBS-T, the membranes were incubated with a mixture of several primary antibodies, including anti-GSTM1, anti-PBE, anti-β-Actin, anti-ALDH2, anti-CPS1, anti-ENO1, and anti-DDT antibodies (all from Boster Immunoleader, Pleasanton, CA, USA). After rewashing in TBS-T, the membranes were incubated with horseradish peroxidase-conjugated anti-rabbit IgG (Thermo Scientific, Rockford, IL, USA), and anti-goat IgG (Santa Cruz Biotechnology, CA, USA) secondary antibodies. The membranes were then developed using SuperSignal West Dura Substrate (Thermo Scientific, Rockford, IL, USA), and scanned with an Image Quant RT ECL scanner (GE Healthcare, Pittsburgh, PA, USA) for visualization of the proteins bound to the primary antibodies. The relative level of each protein was calculated as a ratio between the grey value of the target band and that of the reference (β-actin).
Statistical analysis
The level of each observed parameter was expressed as mean ± standard deviation (n = 10) and analyzed by SPSS statistical software (version 20.0, Chicago, IL, USA). Differences between multiple groups were calculated using one-way ANOVA followed by a Dunnett’s (two-sided) test. A p < 0.05 value was considered as statistically significant. Figures were generated by GraphPad Prism (version 7.0, GraphPad Software Inc., San Diego, CA, USA).
Results
TCE induces liver injury in rats
At terminal killing, the body weights of test animals in the TCE-treated groups and the control were similar (p > 0.05). However, the liver index significantly increased with the increase in TCE level (dose-dependence) (Table 1; Fig. 1). Additionally, the activities of the liver damage marker enzymes (ALT, AST and ALP) in the serum of TCE-treated rats increased significantly (p < 0.001, compared to the control), in a dose-dependent manner (Fig. 2). The total protein and albumin levels in serum in TCE-treated rats were both significantly (p < 0.001) lowered, compared with their levels in the control (Fig. 2).
Alterations of serum indicators of liver injury in SD rats exposed to TCE. See legend of Fig. 1; ***p < 0.001, compared with the control
Differentially expressed proteins in the livers of TCE-exposed rats
To study the mechanism underlining TCE-induced hepatotoxicity, we evaluated the changes in the expression of hepatic proteins using 2D-DIGE. A total of 2000 protein spots were detected. Among these, 66 proteins were differentially expressed in TCE-treated rats (by one-way ANOVA, p < 0.05 combined with more than a 1.2-fold intensity difference) as identified by MALDI-TOF/TOF mass spectrometry (Fig. 3). The presence of different spots corresponding to the same protein was related to the occurrence of different isoforms, mainly due to post-translational modifications. Among the differentially expressed protein spots, 50 (belonging to 39 different proteins) were up-regulated, while 33 spots (27 different proteins) were down-regulated. The results of protein identification are summarized in Table 2.
Protein classification and functional analysis
PANTHER was used for protein classification analysis. Most of the differentially expressed proteins were mainly localized in the cytoplasm (63%) and mitochondrion (26%). The majority of proteins were associated with catalytic (68%) and binding activities (12%). Altered proteins were mainly involved in metabolic processes (55%) (Fig. 4).
Protein–protein interactions were analyzed by STRING (Franceschini et al. 2013). The data suggested a combined effect of these proteins in TCE-induced hepatotoxicity (Fig. 5). We categorized these proteins by their involvement in KEGG pathways (p < 0.05) using the “Enrichment” module integrated within STRING. As shown in Table 2, the pathways perturbed by TCE included fatty acid metabolism, PPAR signaling pathway, glycolysis/gluconeogenesis, and glutathione metabolism.
Verification of PBE as differentially expressed in TCE-induced hepatic injury
Six metabolic enzymes (aldehyde dehydrogenase (Aldh2), alpha-enolase (Eno1), d-dopachrome decarboxylase (Ddt), carbamoyl-phosphate synthase (Cps1), glutathione S-transferase Mu 1 (Gstm1) and peroxisomal bifunctional enzyme (PBE) appeared to be associated with TCE-induced hepatotoxicity. Their levels were evaluated by Western-blot analysis. Aldh2 was down-regulated in the livers of the rats exposed to TCE for 14 days at doses of 250 and 1000 mg/kg (Fig. 6), while Gstm1 was up-regulated at doses of 500 and 1000 mg/kg. PBE was significantly up-regulated by TCE at doses of 500 and 1000 mg/kg. PBE was the only protein that demonstrated TCE dose-dependent enhancement of expression in the livers of rats.
Verification of TCE-targeted proteins in the rat liver. The levels of identified proteins in the liver samples from three rats in each group were confirmed by Western blot analysis. β-Actin was used as the loading control. a Protein bands of Aldh2, Eno1, Ddt, Cps1, Gstm1, and PBE. b Relative levels of Aldh2, Eno1, Ddt, Cps1, Gstm1, and PBE. Data are means and SD of three replicates; *p < 0.05, **p < 0.01, ***p < 0.001, compared with the control
Discussion
Following exposure of SD rats to TCE by gastric gavage (for 14 days), significant increases in the liver index and the activities of liver damage marker enzymes (ALT, AST and ALP) were observed. This indicates that rats, in addition to mice, are vulnerable to TCE-induced liver injury. Furthermore, albumin and total protein in serum were decreased after treatment of TCE. Albumin in serum is mainly produced by the liver. Moreover, liver is also the major organ where TCE is metabolized for hepatotoxicity. The active metabolites of TCE may impair hepatocellular function and decrease albumin synthesis, which contributes to the reduction of albumin in serum (Carvalho and Verdelho Machado 2018; Alves de Mattos 2011). Because albumin is the most abundant protein in serum, its reduction usually leads to a drop of the total protein in serum.
Quantitative analysis by proteomic approaches suggested that the expression levels of 66 individual proteins were altered in the livers of TCE-treated rats. Bioinformatic analysis revealed that many of these proteins are metabolic enzymes mainly participating in glycolysis and the metabolism of lipids and glutathione. This result is consistent with other studies (Lash et al. 2014). The levels of 6 proteins, among 39 different proteins enhanced for expression, were further verified by Western blot analysis. After functional analysis, the six proteins were involved in different biological processes associated with liver injury or hepatic carcinogenesis (Puri 2019; He et al. 2020; Seo et al. 2019; Park et al. 2019; Yu et al. 2018; Gao et al. 2018; Panisello-Rosello 2018; Koen et al. 2016; Kumar et al. 2009). Thus, these proteins were selected for further verification. Of these proteins, the levels of Eno1, Ddt and Cps1 did not change; Aldh2 and Gstm1 were down- and up-regulated, respectively, without a typical dose–response relationship. However, the expression of PBE increased in a dose-dependent manner in the livers of rats exposed to TCE.
Aldh2 is the main enzyme responsible for acetaldehyde oxidation in ethanol metabolism, which implies that its down-regulation in the livers of rats by TCE may increase the oxidative burdens in the body and potentially inhibit ethanol metabolism. This observation is consistent with previous reports demonstrating induction of oxidative stress in the liver of mice by TCE (Atkinson et al. 1993) and decreased expression of Aldh2 and its enzymatic activity (Wang et al. 2010). Gstm1 (a critical enzyme for glutathione (GSH) metabolism) was up-regulated in the livers of rats exposed to TCE. A major function of GSH in mammalian cells is to attenuate oxidative stress, a factor implicated in cancer development and progression (Watanabe and Nagashima 1983). Thus, enhanced expression of Gstm1 might mediate multiple pathologic processes, such as the liver injury induced by TCE.
PBE is a bifunctional enzyme, which has two functional domains, the N-terminal region with enoyl-CoA hydratase activity and the C-terminal region with 3-hydroxyacyl-CoA dehydrogenase activity (Uchida et al. 1992). It is one of the four enzymes in the peroxisomal β-oxidation pathway. PBE is indispensable for the production of medium-chain dicarboxylic acids, which are essential for the coordinated induction of mitochondrial and peroxisomal oxidative pathways during fasting (Houten et al. 2012). Deficiency of this protein can cause peroxisomal disorders such as Zellweger syndrome (Itoh et al. 2000). PBE is also a potential biomarker for hepatocellular carcinoma, as indicated by high-throughput RNA-seq analysis (Gao et al. 2018; Jiang et al. 2019). PBE binds and activates the activation function-1 region of PPARα, a nuclear receptor associated with hepatotoxicity (Juge-Aubry et al. 2001). Interestingly, TCE-induced liver toxicity and carcinogenesis are also mediated partly by activation of PPARα (Mandard et al. 2004; Kyrklund et al. 1983; Klaunig et al. 2003). Therefore, the enhanced expression of PBE in the livers of rats exposed to TCE is likely induced via activation of PPARα by TCE, and PBE may contribute to the hepatotoxicity of TCE.
In summary, the results of this study indicate that TCE induces liver injury in rats. In this model, the expression of 66 liver proteins was altered, among which, PBE, a peroxisomal bifunctional enzyme, can be enhanced for expression, possibly in response to oxidative stress caused by TCE exposure. The role of PBE in TCE-induced liver injury is worth further investigation.
References
Allemand H et al (1978) Metabolic activation of trichloroethylene into a chemically reactive metabolite toxic to the liver. J Pharmacol Exp Ther 204:714–723
Alves de Mattos A (2011) Current indications for the use of albumin in the treatment of cirrhosis. Ann Hepatol 10(Suppl 1):S15–S20
Atkinson A, Meeks RG, Roy D (1993) Increased oxidative stress in the liver of mice treated with trichloroethylene. Biochem Mol Biol Int 31:297–304
Bergmeyer HU, Scheibe P, Wahlefeld AW (1978) Optimization of methods for aspartate aminotransferase and alanine aminotransferase. Clin Chem 24:58–73
Carvalho JR, Verdelho Machado M (2018) New insights about albumin and liver disease. Ann Hepatol 17:547–560
Chiu WA et al (2013) Human health effects of trichloroethylene: key findings and scientific issues. Environ Health Perspect 121:303–311
Franceschini A et al (2013) STRING v9.1: protein–protein interaction networks, with increased coverage and integration. Nucleic Acids Res 41:D808–D815
Gao X, Wang X, Zhang S (2018) Bioinformatics identification of crucial genes and pathways associated with hepatocellular carcinoma. Biosci Rep 38 (2018)
He J et al (2020) Screening of significant biomarkers related with prognosis of liver cancer by lncRNA-associated ceRNAs analysis. J Cell Physiol 235:2464–2477
Houten SM et al (2012) Peroxisomal L-bifunctional enzyme (Ehhadh) is essential for the production of medium-chain dicarboxylic acids. J Lipid Res 53:1296–1303
Huang HY et al (2009) An investigation of hormesis of trichloroethylene in L-02 liver cells by differential proteomic analysis. Mol Biol Rep 36:2119–2129
Itoh M et al (2000) Developmental and pathological expression of peroxisomal enzymes: their relationship of d-bifunctional protein deficiency and Zellweger syndrome. Brain Res 858:40–47
Jiang W et al (2019) Identification of the pathogenic biomarkers for hepatocellular carcinoma based on RNA-seq analyses. Pathol Oncol Res 25:1207–1213
Juge-Aubry CE, Kuenzli S, Sanchez JC, Hochstrasser D, Meier CA (2001) Peroxisomal bifunctional enzyme binds and activates the activation function-1 region of the peroxisome proliferator-activated receptor alpha. Biochem J 353:253–258
Kamijima M, Hisanaga N, Wang H, Nakajima T (2007) Occupational trichloroethylene exposure as a cause of idiosyncratic generalized skin disorders and accompanying hepatitis similar to drug hypersensitivities. Int Arch Occup Environ Health 80:357–370
Khan S et al (2009) Effect of trichloroethylene (TCE) toxicity on the enzymes of carbohydrate metabolism, brush border membrane and oxidative stress in kidney and other rat tissues. Food Chem Toxicol 47:1562–1568
Klaunig JE et al (2003) PPARalpha agonist-induced rodent tumors: modes of action and human relevance. Crit Rev Toxicol 33:655–780
Koen YM, Galeva NA, Metushi IG, Uetrecht J, Hanzlik RP (2016) Protein targets of isoniazid-reactive metabolites in mouse liver in vivo. Chem Res Toxicol 29:1064–1072
Kumar M et al (2009) Study of genetic polymorphism in solvent exposed population and its correlation to in vitro effect of trichloroethylene on lymphocytes. J Environ Biol 30:685–691
Kyrklund T, Alling C, Haglid K, Kjellstand P (1983) Chronic exposure to trichloroethylene: lipid and acyl group composition in gerbil cerebral cortex and hippocampus. Neurotoxicology 4:35–42
Lash LH, Fisher JW, Lipscomb JC, Parker JC (2000) Metabolism of trichloroethylene. Environ Health Perspect 108(Suppl 2):177–200
Lash LH, Chiu WA, Guyton KZ, Rusyn I (2014) Trichloroethylene biotransformation and its role in mutagenicity, carcinogenicity and target organ toxicity. Mutat Res Rev Mutat Res 762:22–36
Liu J et al (2007) Comparative proteomic analysis on human L-02 liver cells treated with varying concentrations of trichloroethylene. Toxicol Ind Health 23:91–101
Mandard S, Muller M, Kersten S (2004) Peroxisome proliferator-activated receptor alpha target genes. Cell Mol Life Sci 61:393–416
Panisello-Rosello A et al (2018) Aldehyde dehydrogenase 2 (ALDH2) in rat fatty liver cold ischemia injury. Int J Mol Sci 19
Park MJ et al (2019) Constitutive release of CPS1 in bile and its role as a protective cytokine during acute liver injury. Proc Natl Acad Sci USA 116:9125–9134
Puri L et al (2019) GSTM1 and liver iron content in children with sickle cell anemia and iron overload. J Clin Med 8
Sano Y et al (2009) Trichloroethylene liver toxicity in mouse and rat: microarray analysis reveals species differences in gene expression. Arch Toxicol 83:835–849
Seo W et al (2019) ALDH2 deficiency promotes alcohol-associated liver cancer by activating oncogenic pathways via oxidized DNA-enriched extracellular vesicles. J Hepatol 71:1000–1011
Uchida Y, Izai K, Orii T, Hashimoto T (1992) Novel fatty acid beta-oxidation enzymes in rat liver mitochondria II Purification and properties of enoyl-coenzyme A (CoA) hydratase/3-hydroxyacyl-CoA dehydrogenase/3-ketoacyl-CoA thiolase trifunctional protein. J Biol Chem 267:1034–1041
Wang J et al (2010) Inhibition of aldehyde dehydrogenase 2 by oxidative stress is associated with cardiac dysfunction in diabetic rats. Mol Med 17:172
Watanabe A, Nagashima H (1983) Glutathione metabolism and glucose 6-phosphate dehydrogenase activity in experimental liver injury. Acta Med Okayama 37:463–470
Wu C, Schaum J (2000) Exposure assessment of trichloroethylene. Environ Health Perspect 108(Suppl 2):359–363
Xu XY et al (2012) Altered expression of hepatic metabolic enzyme and apoptosis-related gene transcripts in human hepatocytes treated with trichloroethylene. Hum Exp Toxicol 31:861–867
Yu S et al (2018) A novel lncRNA, TCONS_00006195, represses hepatocellular carcinoma progression by inhibiting enzymatic activity of ENO1. Cell Death Dis 9:1184
Acknowledgements
This work was supported by the National Natural Science Foundation of China (NSFC) (No. 81872666), and Sanming Project of Medicine in Shenzhen (No. SZSM201611090).
Author information
Authors and Affiliations
Contributions
Nuanyuan Luo and Qunqun Chang analyzed the data and performed statistical tests. Nuanyuan Luo wrote the manuscript. Peiwu Huang extracted protein and conducted 2D-DIGE. Xiaohu Ren conducted protein quantitation and identification. Wei Liu measured Serum biochemical index. Li Zhou and Peiwu Huang were responsible for animal treatment. Yungang Liu revised the manuscript and provided technical support. Jianjun Liu designed the study and provided technical support. All authors have read and approved the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors do not have any conflicts of interest or financial interests to disclose.
Animal rights
All experimental procedures about animal treatment and sample collection were conducted according to the Institutional Animal Care Guidelines and the animal experiments were approved by the committee of ethnics in the Shenzhen Center for Disease Control and Prevention.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Luo, N., Chang, Q., Ren, X. et al. Trichloroethylene injures rat liver and elevates the level of peroxisomal bifunctional enzyme (Ehhadh). Mol. Cell. Toxicol. 16, 331–345 (2020). https://doi.org/10.1007/s13273-020-00075-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13273-020-00075-9